FairEmbo Concept for Postpartum Hemorrhage: Evaluation of the Efficacy of Suture Fragment Compared with Gelatin Sponge Torpedo Embolization in a Post-Gravid Swine Model
Abstract
1. Introduction
2. Materials and Methods
2.1. Animal Model
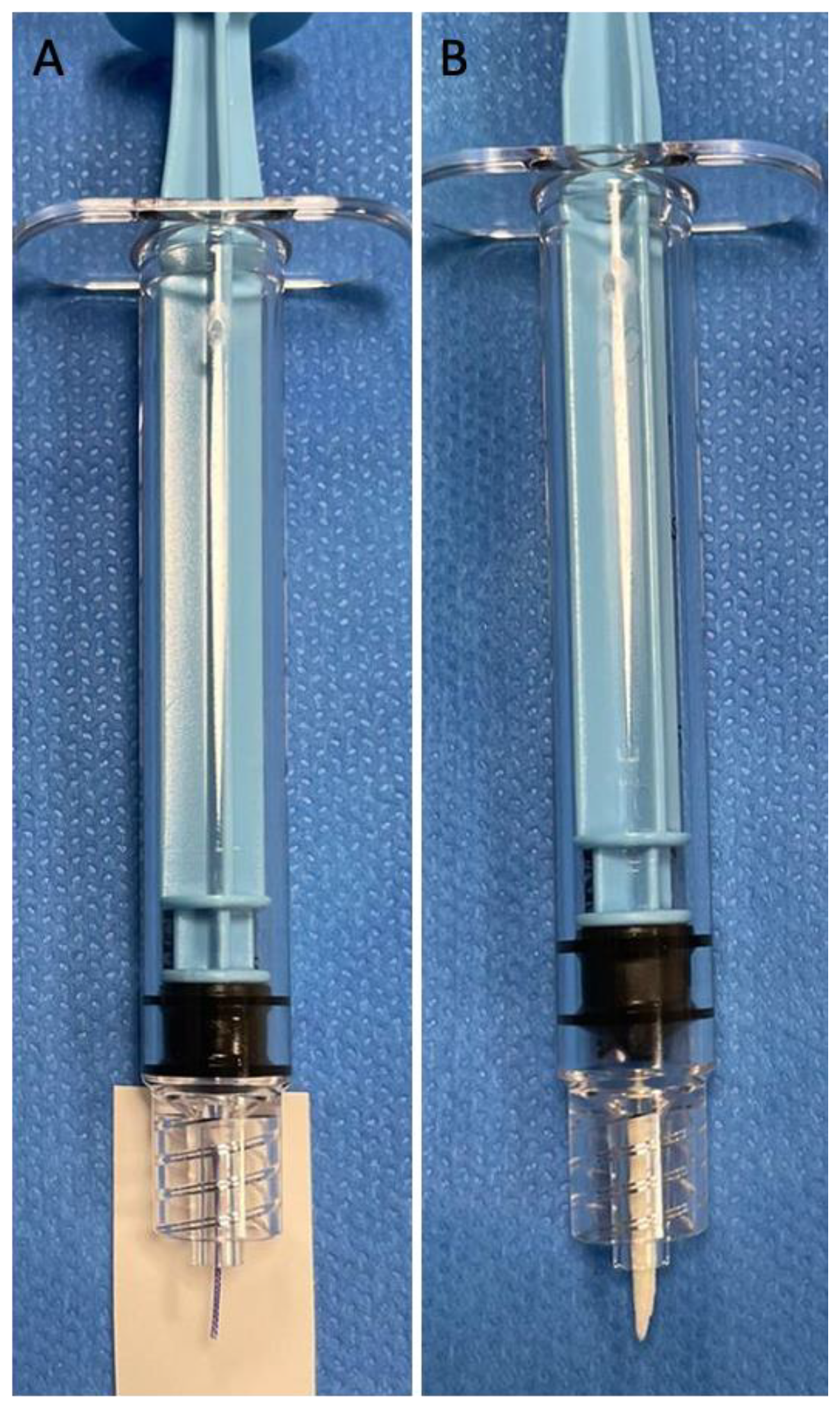
2.2. Embolization Agents
2.3. Embolization Procedure
2.4. Technical Success and Evaluation of Secondary Outcomes
2.5. Statistics
3. Results
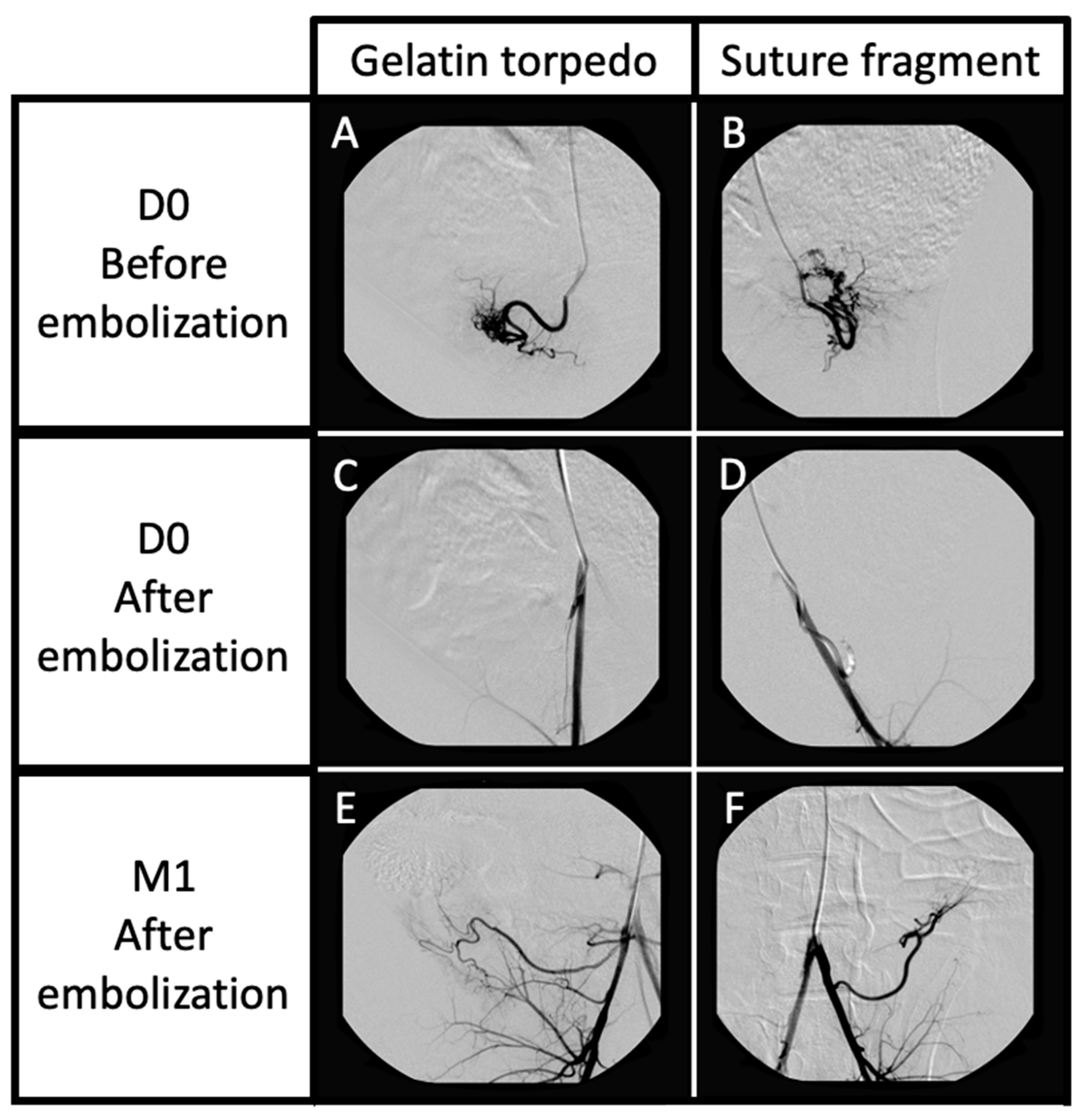
3.1. DSA Parameters, Technical Success
3.2. Short-Term Secondary Endpoints
3.3. Medium-Term Secondary Endpoints: ANGIOGRAPHIC Findings and Macroscopic Aspect
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- McLintock, C.; James, A.H. Obstetric hemorrhage. J. Thromb. Haemost. 2011, 9, 1441–1451. [Google Scholar] [CrossRef] [PubMed]
- Mercier, F.J.; Van de Velde, M. Major obstetric hemorrhage. Anesthesiol. Clin. 2008, 26, 53–66. [Google Scholar] [CrossRef]
- Say, L.; Chou, D.; Gemmill, A.; Tunçalp, Ö.; Moller, A.B.; Daniels, J.; Gülmezoglu, A.M.; Temmerman, M.; Alkema, L. Global causes of maternal death: A WHO systematic analysis. Lancet Glob. Health 2014, 2, e323–e333. [Google Scholar] [CrossRef]
- Ononge, S.; Mirembe, F.; Wandabwa, J.; Campbell, O.M. Incidence and risk factors for postpartum hemorrhage in Uganda. Reprod. Health 2016, 13, 38. [Google Scholar] [CrossRef]
- Guasch, E.; Gilsanz, F. Massive obstetric hemorrhage: Current approach to management. Med. Intensiva 2016, 40, 298–310. [Google Scholar] [CrossRef] [PubMed]
- Pelage, J.P.; Fohlen, A.; Le Pennec, V. Role of arterial embolization in the management of postpartum hemorrhage. J. Gynecol. Obstet. Biol. Reprod. (Paris) 2014, 43, 1063–1082. (In French) [Google Scholar] [CrossRef]
- Sergent, F.; Resch, B.; Verspyck, E.; Rachet, B.; Clavier, E.; Marpeau, L. Intractable postpartum haemorrhages: Where is the place of vascular ligations, emergency peripartum hysterectomy or arterial embolization? Gynecol. Obstet. Fertil. 2004, 32, 320–329. [Google Scholar] [CrossRef] [PubMed]
- Pelage, J.P.; Laissy, J.P.; Collège National des Gynécologues et Obstétriciens Français; Agence Nationale d’Accréditation et d’Evaluation en Santé. Management of life-threatening postpartum hemorrhage: Indications and technique of arterial embolization. J. Gynecol. Obstet. Biol. Reprod. (Paris) 2004, 33 (Suppl. 8), 4S93–4S102. [Google Scholar]
- Makris, G.C.; Byrne, G. Post-partum hemorrhage and maternal mortality in low-income countries and the forgotten role of interventional radiology. Cardiovasc. Intervent. Radiol. 2019, 42, 1810–1811. [Google Scholar] [CrossRef]
- Vidal, V.; Hak, J.F.; Brige, P.; Chopinet, S.; Tradi, F.; Bobot, M.; Gach, P.; Haffner, A.; Soulez, G.; Jacquier, A.; et al. In Vivo Feasibility of Arterial Embolization with Permanent and Absorbable Suture: The FAIR-Embo Concept. Cardiovasc. Intervent. Radiol. 2019, 42, 1175–1182. [Google Scholar] [CrossRef]
- Di Bisceglie, M.; Hak, J.F.; Diop, A.D.; Salazar, G.; Brige, P.; Panneau, J.; Tradi, F.; Habert, P.; Campion, J.Y.; Diop, A.N.; et al. FairEmbo Concept for Arterial Embolizations: In Vivo Feasibility and Safety Study with Suture-Based Microparticles Compared with Microspheres. Cardiovasc. Intervent. Radiol. 2021, 44, 625–632. [Google Scholar] [CrossRef]
- Diop, A.D.; Diop, A.N.; Hak, J.F.; Di Bisceglie, M.; Bartoli, J.M.; Guillet, B.; Vidal, V. Hemostatic embolization of renal artery pseudoaneurysm using absorbable surgical suture (FairEmbo concept). Diagn. Interv. Imaging 2020, 101, 757–758. [Google Scholar] [CrossRef] [PubMed]
- Sato, H.; Sonomura, T.; Onishi, S.; Koike, M.; Tanaka, R.; Ueda, S.; Okuhira, R.; Kamisako, A.; Koyama, T.; Shima, N.; et al. Comparison of Uterine Necrosis After Uterine Artery Embolization with Soluble Gelatin Sponge Particles or Tris-acryl Gelatin Microspheres in Swine. Cardiovasc. Intervent. Radiol. 2021, 44, 1780–1789. [Google Scholar] [CrossRef]
- Sonomura, T.; Kawai, N.; Ikoma, A.; Minamiguchi, H.; Ozaki, T.; Kishi, K.; Sanda, H.; Nakata, K.; Nakai, M.; Muragaki, Y.; et al. Uterine damage in swine following uterine artery embolization: Comparison among gelatin sponge particles and two concentrations of N-butyl cyanoacrylate. Jpn. J. Radiol. 2013, 31, 685–692. [Google Scholar] [CrossRef]
- Louail, B.; Sapoval, M.; Bonneau, M.; Wasseff, M.; Senechal, Q.; Gaux, J.C. A new porcine sponge material for temporary embolization: An experimental short-term pilot study in swine. Cardiovasc. Intervent. Radiol. 2006, 29, 826–831. [Google Scholar] [CrossRef]
- Schmitz-Rixen, T.; Horsch, S.; Klein, B.; Pichlmaier, H. Blood vessel wall regeneration in the use of a new monofilament, resorbable suture material for arterial anastomoses. Langenbecks Arch. Chir. 1984, 362, 53–60. [Google Scholar] [CrossRef]
- Belghiti, J.; Tassin, M.; Raiffort, C.; Zappa, M.; Poujade, O.; Bout, H.; Mandelbrot, L. Uterine necrosis after arterial embolization for postpartum hemorrhage. Gynecol. Obstet. Fertil. 2014, 42, 126–128. [Google Scholar] [CrossRef] [PubMed]
- Cottier, J.P.; Fignon, A.; Tranquart, F.; Herbreteau, D. Uterine necrosis after arterial embolization for postpartum hemorrhage. Obstet. Gynecol. 2002, 100 Pt 2, 1074–1077. [Google Scholar] [CrossRef]
- Nakamura, Y.; Aoki, S.; Takebayashi, S.; Hirahara, F. Effect of transarterial embolization for post-partum hemorrhage on subsequent pregnancy. J. Obstet. Gynaecol. Res. 2016, 42, 1186–1189. [Google Scholar] [CrossRef] [PubMed]
- Cheng, H.H.; Tsang, L.L.; Hsu, T.Y.; Kung, C.T.; Ou, C.Y.; Chang, C.D.; Tsai, C.C.; Cheng, Y.F.; Kung, F.T. Transcatheter arterial embolization as first-line rescue in intractable primary postpartum hemorrhage: Assessment, outcome, and subsequent fertility. J. Formos. Med. Assoc. 2017, 116, 380–387. [Google Scholar] [CrossRef]
- Swindle, M.M.; Makin, A.; Herron, A.J.; Clubb, F.J.; Frazier, K.S. Swine as models in biomedical research and toxicology testing. Vet. Pathol. 2012, 49, 344–356. [Google Scholar] [CrossRef] [PubMed]
- Kessler, U.; Grau, T.; Gronchi, F.; Berger, S.; Brandt, S.; Bracht, H.; Marcucci, C.; Zachariou, Z.; Jakob, S.M. Comparison of porcine and human coagulation by thrombelastometry. Thromb. Res. 2011, 128, 477–482. [Google Scholar] [CrossRef] [PubMed]
- Lechner, R.; Helm, M.; Müller, M.; Wille, T.; Riesner, H.J.; Friemert, B. In-vitro study of species-specific coagulation differences in animals and humans using rotational thromboelastometry (ROTEM). J. R. Army Med. Corps 2019, 165, 356–359. [Google Scholar] [CrossRef] [PubMed]
- Niles, J.; Williams, J. Suture materials and patterns. In Pract. 1999, 21, 308–320. [Google Scholar] [CrossRef]
- Campbell, J.R.; Marks, A. Suture materials and suturing techniques. In Pract. 1985, 7, 72–75. [Google Scholar] [CrossRef]

| Suture | Gelatin | p * | |
|---|---|---|---|
| Immediate effective embolization (n) | 7/7 (100%) | 7/7 (100%) | |
| Embolization time (min) | 10 (4–17) | 3.7 (1–6) | 0.028 |
| Numbers of fragments/torpedoes used (n) | 13.8 (4–25) | 5.7 (3–10) | 0.029 |
| Non-targeted embolization (n) | 0/7 (0%) | 0/7 (0%) |
| Suture | Gelatin | |
|---|---|---|
| Arterial recanalization at D7 (n) | 3/7 (43%) | 7/7 (100%) |
| Arterial recanalization at M1 (n) | 7/7 (100%) | 7/7 (100%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Banata Gang-Ny, A.; Panneau, J.; Brige, P.; Hak, J.-F.; Habert, P.; Vidal, V.; Tradi, F.; Di Bisceglie, M. FairEmbo Concept for Postpartum Hemorrhage: Evaluation of the Efficacy of Suture Fragment Compared with Gelatin Sponge Torpedo Embolization in a Post-Gravid Swine Model. J. Pers. Med. 2023, 13, 124. https://doi.org/10.3390/jpm13010124
Banata Gang-Ny A, Panneau J, Brige P, Hak J-F, Habert P, Vidal V, Tradi F, Di Bisceglie M. FairEmbo Concept for Postpartum Hemorrhage: Evaluation of the Efficacy of Suture Fragment Compared with Gelatin Sponge Torpedo Embolization in a Post-Gravid Swine Model. Journal of Personalized Medicine. 2023; 13(1):124. https://doi.org/10.3390/jpm13010124
Chicago/Turabian StyleBanata Gang-Ny, Amandine, Julien Panneau, Pauline Brige, Jean-François Hak, Paul Habert, Vincent Vidal, Farouk Tradi, and Mathieu Di Bisceglie. 2023. "FairEmbo Concept for Postpartum Hemorrhage: Evaluation of the Efficacy of Suture Fragment Compared with Gelatin Sponge Torpedo Embolization in a Post-Gravid Swine Model" Journal of Personalized Medicine 13, no. 1: 124. https://doi.org/10.3390/jpm13010124
APA StyleBanata Gang-Ny, A., Panneau, J., Brige, P., Hak, J.-F., Habert, P., Vidal, V., Tradi, F., & Di Bisceglie, M. (2023). FairEmbo Concept for Postpartum Hemorrhage: Evaluation of the Efficacy of Suture Fragment Compared with Gelatin Sponge Torpedo Embolization in a Post-Gravid Swine Model. Journal of Personalized Medicine, 13(1), 124. https://doi.org/10.3390/jpm13010124





