Multidisciplinary Consulting Team for Complicated Cases of Neurodevelopmental and Neurobehavioral Disorders: Assessing the Opportunities and Challenges of Integrating Pharmacogenomics into a Team Setting
Abstract
:1. Introduction
2. Materials and Methods
2.1. Ethics and Study Design
2.2. Patient Inclusion/Exclusion Criteria for PGx Referral
2.3. Patient Consent
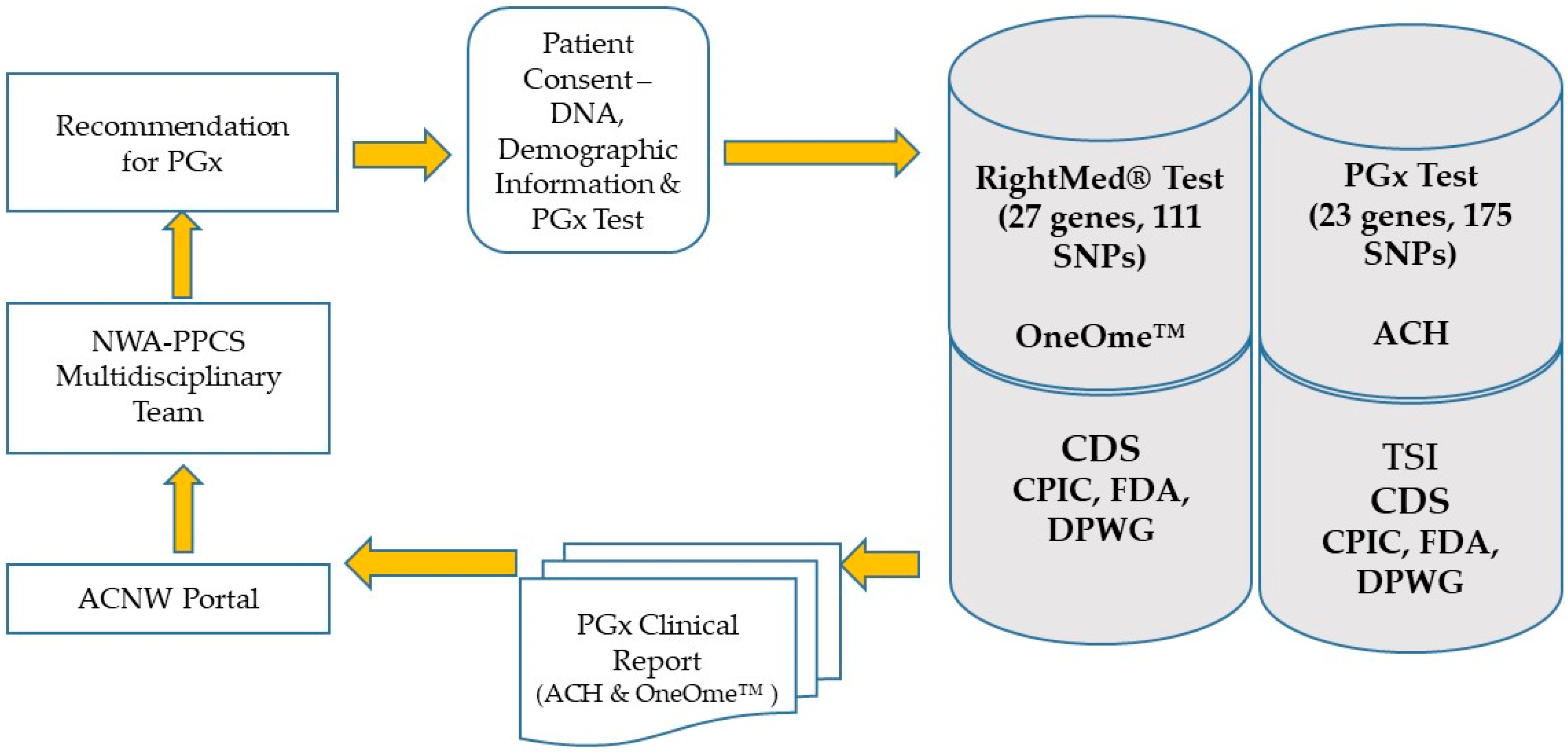
2.4. DNA Sample Collection and PGx Testing
2.5. Data Reporting
2.6. Clinical Recommendations
3. Results
3.1. Sample Demographics
3.2. Pharmacogenomic (PGx) Results
3.2.1. CYP2C19 and CYP2D6 Phenotype Metabolizer Status
3.2.2. Pharmacogenomics Actionability and Phenoconversion
3.3. NDD/NBD Diagnosis
3.4. PGx Guiding Therapy
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Available online: https://www.cdc.gov/ncbddd/developmentaldisabilities/facts.html (accessed on 2 February 2022).
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Arlington, VA, USA, 2013. [Google Scholar]
- Parenti, I.; Rabaneda, L.G.; Schoen, H.; Novarino, G. Neurodevelopmental disorders: From genetics to functional pathways. Trends Neurosci. 2020, 43, 608–621. [Google Scholar] [CrossRef] [PubMed]
- Jeste, S.S. Neurodevelopmental behavioral and cognitive disorders. Continuum Minneap Minn. 2015, 21, 690–714. [Google Scholar] [CrossRef] [PubMed]
- Poppi, L.A.; Ho-Nguyen, K.T.; Shi, A.; Daut, C.T.; Tischfield, M.A. Recurrent Implication of Striatal Cholinergic Interneurons in a Range of Neurodevelopmental, Neurodegenerative, and Neuropsychiatric Disorders. Cells 2021, 10, 907. [Google Scholar] [CrossRef] [PubMed]
- Prem, S.; Millonig, J.H.; DiCicco-Bloom, E. Dysregulation of Neurite Outgrowth and Cell Migration in Autism and Other Neurodevelopmental Disorders. In Neurodevelopmental Disorders. Advances in Neurobiology; Di-Cicco-Bloom, E., Millonig, J., Eds.; Springer: Cham, Switzerland, 2020. [Google Scholar]
- Penna, E.; Pizzella, A.; Cimmino, F.; Trinchese, G.; Cavaliere, G.; Catapano, A.; Allocca, I.; Chun, J.T.; Campanozzi, A.; Messina, G.; et al. Neurodevelopmental Disorders: Effect of High-Fat Diet on Synaptic Plasticity and Mitochondrial Functions. Brain Sci. 2020, 10, 805. [Google Scholar] [CrossRef] [PubMed]
- Niemi, M.E.K.; Martin, H.C.; Rice, D.L.; Gallone, G.; Gordon, S.; Kelemen, M.; McAloney, K.; McRae, J.; Radford, E.J.; Yu, S.; et al. Common genetic variants contribute to risk of rare severe neurodevelopmental disorders. Nature 2018, 562, 268–271. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Blesson, A.; Cohen, J.S. Genetic counseling in neurodevelopmental disorders. Cold Spring Harb. Perspect. Med. 2020, 10, a036533. [Google Scholar] [CrossRef]
- Leblond, C.S.; Le, T.-L.; Malesys, S.; Cliquet, F.; Tabet, A.-C.; Delorme, R.; Rolland, T.; Bourgeron, T. Operative list of genes associated with autism and neurodevelopmental disorders based on database review. Mol. Cell. Neurosci. 2021, 113, 103623. [Google Scholar] [CrossRef]
- Available online: https://datacenter.kidscount.org/data/tables/10668-children-whohave-one-or-more-emotional-behavioral-or-developmental-nditions?loc=5&loct=2#detailed/2/5/false/1648/any/20457,20456 (accessed on 2 February 2022).
- Gill, P.S.; Yu, F.B.; Porter-Gill, P.A.; Boyanton, B.L.; Allen, J.C.; Farrar, J.E.; Veerapandiyan, A.; Prodhan, P.; Bielamowicz, K.J.; Sellars, E.; et al. Implementing Pharmacogenomics Testing: Single Center Experience at Arkansas Children’s Hospital. J. Pers. Med. 2021, 11, 394. [Google Scholar] [CrossRef]
- Pardiñas, A.F.; Owen, M.J.; Walters, J.T.R. Pharmacogenomics: A road ahead for precision medicine in psychiatry. Neuron 2021, 109, 3914–3929. [Google Scholar] [CrossRef]
- Ampong, D.N. Landmars of pharmacogenomics and some considerations for clinical practice. Ther. Adv. Psychopharmacol. 2019, 9, 1–12. [Google Scholar] [CrossRef]
- Nicholson, W.T.; Formea, C.M.; Matey, E.T.; Wright, J.A.; Giri, J.; Moyer, A.M. Considerations when applying pharmacogenomics to your practice. Mayo Clin. Proc. 2021, 96, 218–230. [Google Scholar] [CrossRef] [PubMed]
- Dagar, A.; Cherlopalle, S.; Ahuja, V.; Senko, L.; Butler, R.S.; Austerman, J.; Anand, A.; Falcone, T. Real-world experience of using combinatorial pharmacogenomic test in children and adolescents with depression and anxiety. J. Psychiatr. Res. 2022, 146, 83–86. [Google Scholar] [CrossRef] [PubMed]
- Strawn, J.R.; Mills, J.A.; Schroeder, H.; Mossman, S.A.; Varney, S.T.; Ramsey, L.B.; Poweleit, E.A.; Desta, Z.; Cecil, K.; DelBello, M.P. Escitalopram in Adolescents with Generalized Anxiety Disorder: A Double-Blind, Randomized, Placebo-Controlled Study. J. Clin. Psychiatry 2020, 81, 6584. [Google Scholar] [CrossRef] [PubMed]
- Aldrich, S.L.; Poweleit, E.A.; Prows, C.A.; Martin, L.J.; Strawn, J.R.; Ramsey, L.B. Influence of CYP2C19 Metabolizer Status on Escitalopram/Citalopram Tolerability and Response in Youth with Anxiety and Depressive Disorders. Front. Pharmacol. 2019, 19, 99. [Google Scholar] [CrossRef] [PubMed]
- Caraballo, P.J.; Hodge, L.S.; Bielinski, S.J.; Stewart, A.K.; Farrugia, G.; Schultz, C.G.; Rohrer-Vitek, C.R.; Olson, J.E.; Sauver, J.L.S.; Roger, V.L.; et al. Multidisciplinary model to implement pharmacogenomics at the point of care. Genet. Med. 2017, 19, 421–429. [Google Scholar] [CrossRef] [Green Version]
- Dunnenberger, H.M.; Biszewski, M.; Bell, G.C.; Sereika, A.; May, H.; Johnson, S.G.; Hulick, P.J.; Khandekar, J. Implementation of a multidisciplinary pharmacogenomics clinic in a community health system. Am. J. Health Syst. Pharm. 2016, 73, 1956–1966. [Google Scholar] [CrossRef] [PubMed]
- Van der Wouden, C.H.; Cambon-Thomsen, A.; Cecchin, E.; Cheung, K.C.; Dávila-Fajardo, C.L.; Deneer, V.H.; Dolzan, V.; Ingelman-Sundberg, M.; Jonsson, S.; Karlsson, M.O.; et al. Implementing pharmacogenomics in Europe: Design and implementation strategy of the ubiquitous pharmacogenomics consortium. Clin. Pharmacol. Ther. 2017, 101, 341–358. [Google Scholar] [CrossRef] [PubMed]
- Nofziger, C.; Turner, A.J.; Sangkuhl, K.; Whirl-Carrillo, M.; Agúndez, J.A.G.; Black, J.L.; Dunnenberger, H.M.; Ruano, G.; Kennedy, M.A.; Phillips, M.S.; et al. PharmVar GeneFocus: CYP2D6. Clin. Pharmacol. Ther. 2020, 107, 154–170. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Botton, M.R.; Whirl-Carrillo, M.; Del Tredici, A.L.; Sangkuhl, K.; Cavallari, L.H.; Agúndez, J.A.G.; Duconge, J.; Lee, M.T.M.; Woodahl, E.L.; Claudio-Campos, K.; et al. PharmVar GeneFocus: CYP2C19. Clin. Pharmacol. Ther. 2021, 109, 352–366. [Google Scholar] [CrossRef]
- Hicks, J.K.; Bishop, J.R.; Sangkuhl, K.; Müller, D.J.; Ji, Y.; Leckband, S.G.; Leeder, J.S.; Graham, R.L.; Chiulli, D.L.; LLerena, A.; et al. Clinical Pharmacogenetics Implementation Consortium (CPIC) Guideline for CYP2D6 and CYP2C19 Genotypes and Dosing of Selective Serotonin Reuptake Inhibitors. Clin. Pharmacol. Ther. 2015, 98, 127–134. [Google Scholar] [CrossRef] [Green Version]
- Available online: https://www.fda.gov/medical-devices/precision-medicine/table-pharmacogenetic-associations (accessed on 2 February 2022).
- Available online: https://www.knmp.nl/downloads/pharmacogenetic-recommendations-3mei2021.pdf (accessed on 2 February 2022).
- Cicali, E.J.; Elchynski, A.L.; Cook, K.J.; Houder, J.T.; Thomas, C.D.; Smith, D.M.; Elsey, A.; Johnson, J.A.; Cavallari, L.H.; Wiisanen, K. How to Integrate CYP2D6 Phenoconversion Into Clinical Pharmacogenetics: A Tutorial. Clin. Pharmacol. Ther. 2021, 110, 677–687. [Google Scholar] [CrossRef] [PubMed]
- Al-Beltagi, M. Autism medical comorbidities. World J. Clin. Pediatr. 2021, 10, 15–28. [Google Scholar] [CrossRef] [PubMed]
- Antshel, K.M.; Russo, N. Autism Spectrum Disorders and ADHD: Overlapping Phenomenology, Diagnostic Issues, and Treatment Considerations. Curr. Psychiatry Rep. 2019, 21, 34. [Google Scholar] [CrossRef] [PubMed]
- Van Steijn, D.J.; Richards, J.S.; Oerlemans, A.M.; De Ruiter, S.W.; Van Aken, M.A.; Franke, B.; Buitelaar, J.K.; Rommelse, N.N.J. The co-occurrence of autism spectrum disorder and attention-deficit/hyperactivity disorder symptoms in parents of children with ASD or ASD with ADHD. J. Child Psychol. Psychiatry 2012, 53, 954–963. [Google Scholar] [CrossRef] [PubMed]
- Leitner, Y. The co-occurrence of autism and attention deficit hyperactivity disorder in children—What do we know? Front. Hum. Neurosci. 2014, 8, 8. [Google Scholar] [CrossRef]
- Van Steensel, F.J.; Bögels, S.M.; Perrin, S. Anxiety disorders in children and adolescents with autistic spectrum disorders: A meta-analysis. Clin. Child Fam. Psychol. Rev. 2011, 14, 302–317. [Google Scholar] [CrossRef] [Green Version]
- Available online: https://www.carautismroadmap.org/intellectual-disability-and-asd/ (accessed on 2 February 2022).
- Davis, N.O.; Kollins, S.H. Treatment for co-occurring attention deficit/hyperactivity disorder and autism spectrum disorder. Neurotherapeutics 2012, 9, 518–530. [Google Scholar] [CrossRef] [Green Version]
- Shah, R.R.; Smith, R.L. Addressing phenoconversion: The Achilles’ heel of personalized medicine. Br. J. Clin. Pharmacol. 2015, 79, 222–240. [Google Scholar] [CrossRef] [Green Version]
- Hahn, M.; Roll, S.C. The Influence of Pharmacogenetics on the Clinical Relevance of Pharmacokinetic Drug-Drug Interactions: Drug-Gene, Drug-Gene-Gene and Drug-Drug-Gene Interactions. Pharmaceuticals 2021, 14, 487. [Google Scholar] [CrossRef]
- Shah, R.R.; Gaedigk, A. Precision medicine: Does ethnicity information complement genotype-based prescribing decisions? Ther. Adv. Drug Saf. 2018, 9, 45–62. [Google Scholar] [CrossRef] [Green Version]
- Kotlyar, M.; Brauer, L.H.; Tracy, T.S.; Hatsukami, D.K.; Harris, J.; Bronars, C.A.; Adson, D.E. Inhibition of CYP2D6 Activity by Bupropion. J. Clin. Psychopharmacol. 2005, 25, 226–229. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.fda.gov/drugs/drug-interactions-labeling/drug-development-and-drug-interactions-table-substrates-inhibitors-and-inducers (accessed on 2 February 2022).
- Brown, L.; Li, J.; Katel, N.; Yu, K.; Fatourou, E.; Himmler, B.; Halaris, A. Pharmacogenetic Testing in an Academic Psychiatric Clinic: A Retrospective Chart Review. J. Pers. Med. 2021, 11, 896. [Google Scholar] [CrossRef]
- Siegel, M.; McGuire, K.; Veenstra-VanderWeele, J.; Stratigos, K.; King, B.; American Academy of Child and Adolescent Psychiatry (AACAP) Committee on Quality Issues (CQI). Practice Parameter for the Assessment and Treatment of Psychiatric Disorders in Children and Adolescents with Intellectual Disability (Intellectual Developmental Disorder). J. Am. Acad. Child Adolesc. Psychiatry 2020, 59, 468–496. [Google Scholar] [CrossRef] [PubMed]
- Volkmar, F.; Siegel, M.; Woodbury-Smith, M.; King, B.; McCracken, J.; State, M.; American Academy of Child and Adolescent Psychiatry (AACAP) Committee on Quality Issues (CQI). Practice parameter for the assessment and treatment of children and adolescents with autism spectrum disorder. J. Am. Acad. Child Adolesc. Psychiatry 2014, 53, 237–257. [Google Scholar] [PubMed] [Green Version]
- Birmaher, B.; Brent, D.; AACAP Work Group on Quality Issues; Bernet, W.; Bukstein, O.; Walter, H.; Benson, R.S.; Chrisman, A.; Farchione, T.; Greenhill, L.; et al. Practice parameter for the assessment and treatment of children and adolescents with depressive disorders. J. Am. Acad. Child Adolesc. Psychiatry 2007, 46, 1503–1526. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Connolly, S.D.; Bernstein, G.A.; Work Group on Quality Issues. Practice parameter for the assessment and treatment of children and adolescents with anxiety disorders. J. Am. Acad. Child Adolesc. Psychiatry 2007, 46, 267–283. [Google Scholar] [CrossRef] [PubMed]
- Roscizewski, L.; Henneman, A.; Snyder, T. Effect of pharmacogenomic testing on pharmacotherapy decision making in patients with symptoms of depression in an interprofessional primary care clinic. J. Am. Pharm. Assoc. 2021, 62, 569–574. [Google Scholar] [CrossRef]
| Gene | RightMed® Alleles | ACH PGx Alleles |
|---|---|---|
| CYP2C19 | * 2, * 3, * 4, * 4B, * 10, * 17 | * 2, * 3, * 4A, * 4B, * 5, * 6, * 7, * 8, * 9, * 10, * 11, * 17, * 35 |
| CYP2D6 | * 2, * 2A, * 3, * 4, * 4J, * 4K, * 4M, * 4N, * 5, * 6, * 6C, * 7, * 8, * 9, * 10, * 11, * 12,* 13, * 14, * 15, * 17, * 18, * 19, * 29, * 31, * 34, * 35, * 36, * 39, * 41, * 42, * 59, * 61, * 63, * 64, * 65, * 68, * 69, * 70, * 91, * 109, * 114, CNVs | * 4, * 6, * 7, * 8, * 9, * 10, * 11, * 12, * 14A, * 14B, * 15, * 17, * 18, * 19, * 21, * 29, * 30, * 31, * 33, * 35, * 36, * 38, * 40, * 41, * 42, * 43, * 44, * 45, * 46, * 47, * 49, * 51, * 53, * 54, * 56A, * 56B, * 58, * 62, * 70, * 84, * 100, * 101, CNVs |
| Patient Characteristics | n = 27 |
|---|---|
| Age, years (AVG ± SD) | 11 ± 4 |
| Sex (%) | |
| Males | 14 (51.9) |
| Race (%) | |
| White | 24 (88.9) |
| Other | 3 (11.1) |
| Ethnicity (%) | |
| Not Hispanic | 23 (85.2) |
| Gene (Phenotype) | n (%) |
|---|---|
| CYP2C19 Phenotype | |
| PM | 1 (3.7) |
| IM | 7 (25.9) |
| NM | 11 (40.8) |
| RM | 7 (25.9) |
| UM | 1 (3.7) |
| CYP2D6 Phenotype | |
| PM | 0 (0) |
| IM | 11 (40.7) |
| NM | 16 (59.3) |
| UM | 0 (0) |
| Gene (Phenotype) | n (%) |
|---|---|
| CYP2D6 Phenoconversion | 7 (25.9) |
| *Clinical CYP2D6 Phenotype | |
| PM | 7 (25.9) |
| IM | 8 (29.6) |
| NM | 12 (44.4) |
| UM | 0 (0) |
| Most Common Diagnosis | n (%) |
|---|---|
| ADHD | 18 (66.7) |
| Anxiety Disorder | 16 (59.3) |
| Autism | 11 (40.7) |
| Intellectual Disability | 9 (33.3) |
| Sleep Difficulties | 8 (29.6) |
| Encephalopathy | 7 (25.9) |
| PatientID | Diagnoses | Diagnostic Genetic Testing Results | Medications Before PGx | CYP2C19 Phenotype | CYP2D6 Phenotype | Medications After PGx | PGx Medication Change Classification |
|---|---|---|---|---|---|---|---|
| 7 | Encephalopathy Spastic paraparesis Panic Disorder ADHD Borderline Personality Disorder | PUM1 related disorder | None | NM | NM | Escitalopram 5 mg, 1 tablet daily Trazodone 50 mg, 1 tablet at bedtime | New Start |
| 12 | Middle cerebral artery syndrome Encephalopathy Migraine Disorder Growth Hormone Disorder ADHD Social Anxiety Mild Intellectual Disability | KAT8 related disorder | Guanfacine ER 4 mg, 1 table at night Venlafaxine ER 150 mg, 1 tablet every morning Trazodone 150 mg, 1 tablet at bedtime | IM | IM | Guanfacine ER 4mg, 1 tablet at bedtime Trazodone 150 mg, 1 tablet at bedtime Duloxetine 30 mg, 1 tablet daily | Alternative Therapy |
| 26 | Encephalopathy ASD ADHD Borderline Intellectual Functioning Sleep Difficulties | Exome sequencing non-diagnostic | Methylphenidate 10 mg, 1 tablet two times daily | IM | IM | Methylphenidate 10 mg, 1 tablet two times daily Clonidine 0.1 mg, 1 tablet at bedtime Hydroxyzine 25 mg, 1 tablet two times daily Risperidone 0.5 mg, 1 tablet two times daily | Adjunct Therapy |
| 28 | ASD ADHD Anxiety | Chromosome Microarray Analysis Normal | Risperidone 0.5 mg, 2 tablets daily Dexmethylphenidate XR 5 mg, 1 tablet daily | IM | NM | Risperidone 0.5 mg, 2 tablets daily Dexmethylphenidate XR 10mg, 1 tablet daily | Confirmed Therapy |
| 30 | ADH Anxiety Cognitive Disorder Executive Function Deficient Learn Disorder involving mathematics | No additional genetic testing | Bupropion 400 mg daily | IM | PM * | Bupropion 400 mg daily Guanfacine XR 3 mg, 3 tablets by mouth at bedtime | Adjunct Therapy |
| Utilized PGx to Guide Therapy | n = 18 (66.7) |
|---|---|
| New medication start | 6 (22.2) |
| Alternative therapy | 5 (18.5) |
| Adjunct therapy | 4 (14.8) |
| Confirmed therapy | 3 (11.1) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gill, P.S.; Elchynski, A.L.; Porter-Gill, P.A.; Goodson, B.G.; Scott, M.A.; Lipinski, D.; Seay, A.; Kehn, C.; Balmakund, T.; Schaefer, G.B. Multidisciplinary Consulting Team for Complicated Cases of Neurodevelopmental and Neurobehavioral Disorders: Assessing the Opportunities and Challenges of Integrating Pharmacogenomics into a Team Setting. J. Pers. Med. 2022, 12, 599. https://doi.org/10.3390/jpm12040599
Gill PS, Elchynski AL, Porter-Gill PA, Goodson BG, Scott MA, Lipinski D, Seay A, Kehn C, Balmakund T, Schaefer GB. Multidisciplinary Consulting Team for Complicated Cases of Neurodevelopmental and Neurobehavioral Disorders: Assessing the Opportunities and Challenges of Integrating Pharmacogenomics into a Team Setting. Journal of Personalized Medicine. 2022; 12(4):599. https://doi.org/10.3390/jpm12040599
Chicago/Turabian StyleGill, Pritmohinder S., Amanda L. Elchynski, Patricia A. Porter-Gill, Bradley G. Goodson, Mary Ann Scott, Damon Lipinski, Amy Seay, Christina Kehn, Tonya Balmakund, and G. Bradley Schaefer. 2022. "Multidisciplinary Consulting Team for Complicated Cases of Neurodevelopmental and Neurobehavioral Disorders: Assessing the Opportunities and Challenges of Integrating Pharmacogenomics into a Team Setting" Journal of Personalized Medicine 12, no. 4: 599. https://doi.org/10.3390/jpm12040599
APA StyleGill, P. S., Elchynski, A. L., Porter-Gill, P. A., Goodson, B. G., Scott, M. A., Lipinski, D., Seay, A., Kehn, C., Balmakund, T., & Schaefer, G. B. (2022). Multidisciplinary Consulting Team for Complicated Cases of Neurodevelopmental and Neurobehavioral Disorders: Assessing the Opportunities and Challenges of Integrating Pharmacogenomics into a Team Setting. Journal of Personalized Medicine, 12(4), 599. https://doi.org/10.3390/jpm12040599







