Acceptance of COVID-19 and Influenza Vaccine Co-Administration: Insights from a Representative Italian Survey
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Study Outcome
2.3. Study Variables
2.4. Data Analysis
3. Results
3.1. Characteristics of the Study Participants
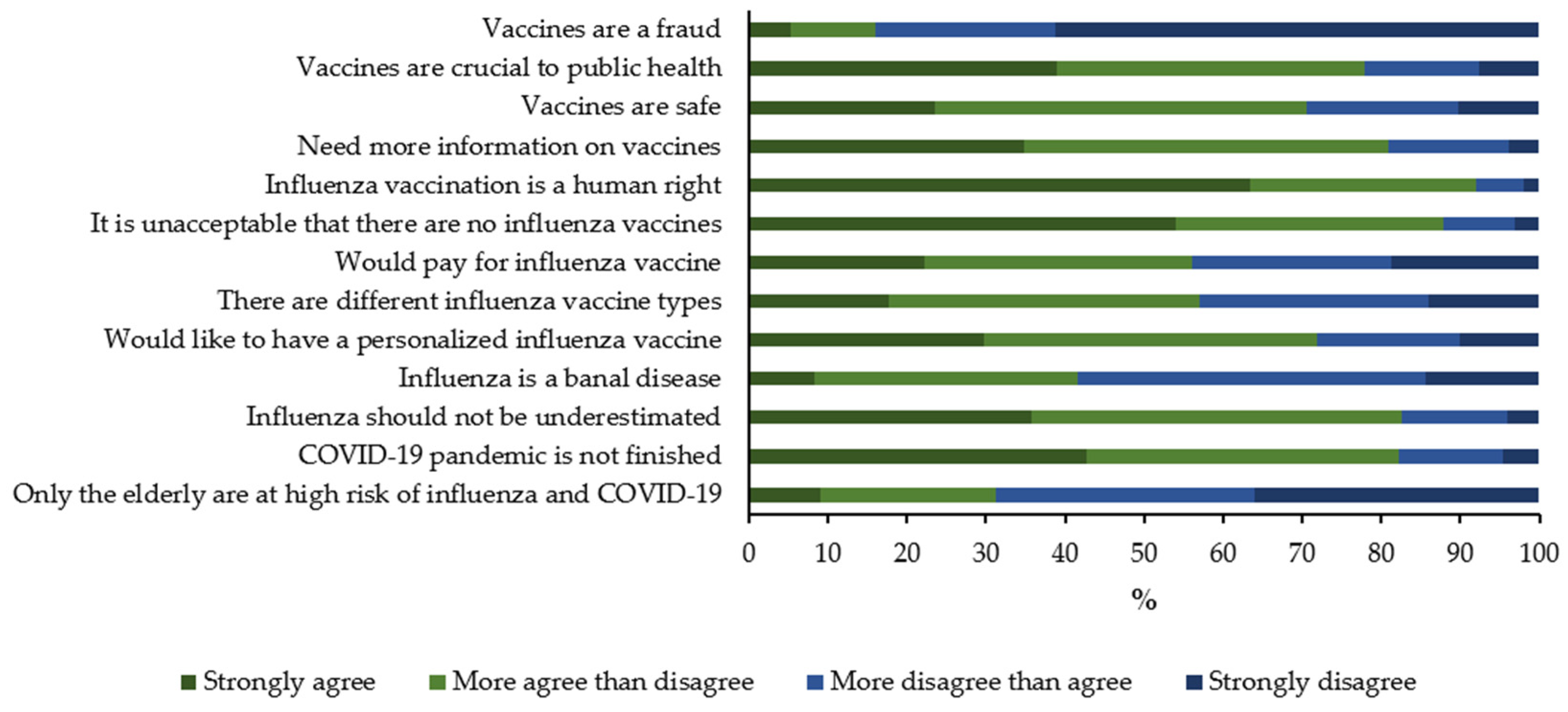
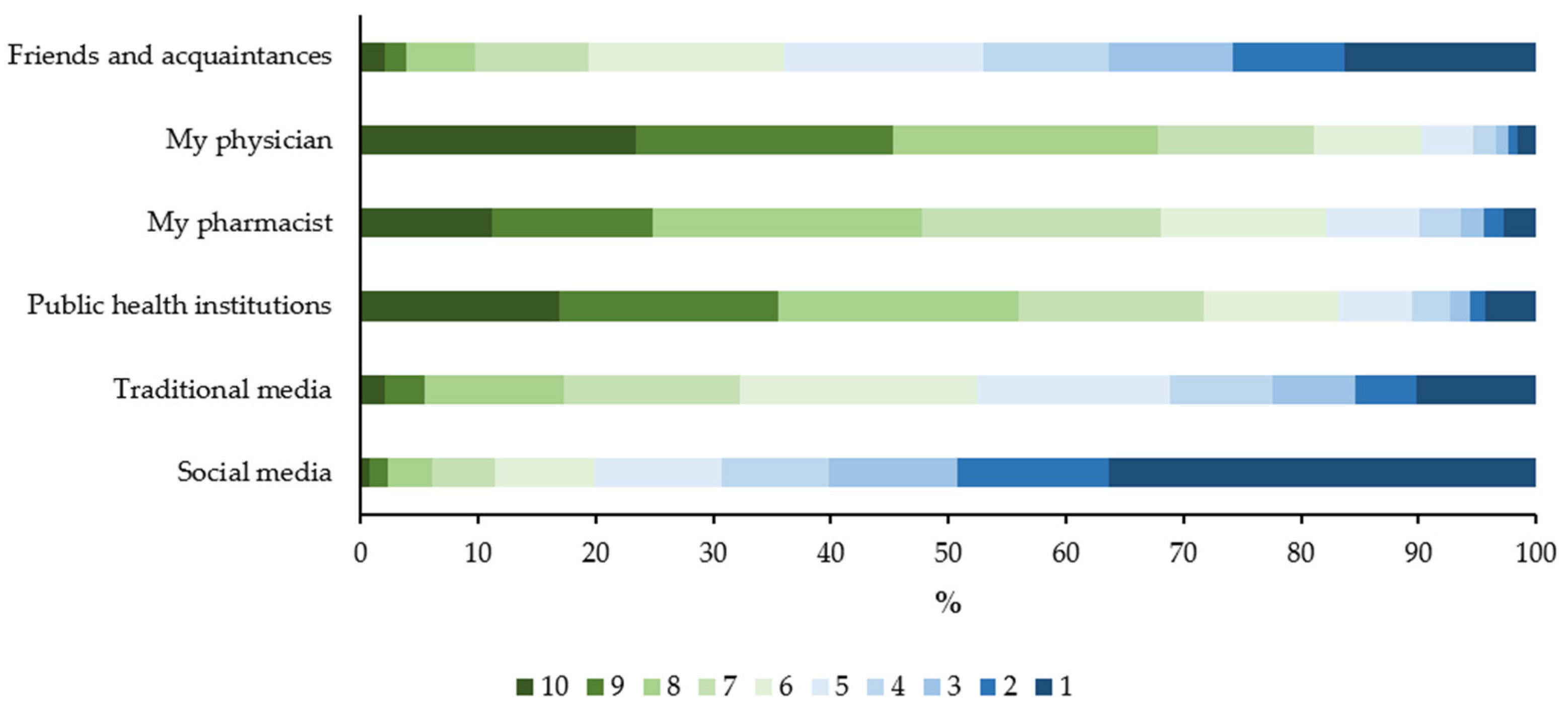
3.2. Knowledge, Attitudes and Practices concerning Influenza and Vaccination
3.3. Influenza and COVID-19 Vaccination Uptake
3.4. Attitude toward Influenza and COVID-19 Vaccine Co-Administration and Its Correlates
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization (WHO). FluNet. Available online: https://www.who.int/tools/flunet (accessed on 13 December 2021).
- The Academy of Medical Sciences. COVID-19: Preparing for the Future. Looking ahead to Winter 2021/22 and Beyond. Available online: https://acmedsci.ac.uk/file-download/4747802 (accessed on 13 December 2021).
- McCauley, J.; Barr, I.G.; Nolan, T.; Tsai, T.; Rockman, S.; Taylor, B. The importance of influenza vaccination during the COVID-19 pandemic. Influenza Other Respir. Viruses 2021, 16, 3–6. [Google Scholar] [CrossRef]
- Peacock, G.; Ryerson, A.B.; Koppaka, R.; Tschida, J. The importance of seasonal influenza vaccination for people with disabilities during the COVID-19 pandemic. Disabil. Health J. 2021, 14, 101058. [Google Scholar] [CrossRef] [PubMed]
- Bhatt, H. Improving influenza vaccination rates during COVID-19 pandemic—The need of the hour. J. Glob. Health 2021, 11, 03042. [Google Scholar] [CrossRef]
- Conlon, A.; Ashur, C.; Washer, L.; Eagle, K.A.; Hofmann Bowman, M.A. Impact of the influenza vaccine on COVID-19 infection rates and severity. Am. J. Infect. Control. 2021, 49, 694–700. [Google Scholar] [CrossRef] [PubMed]
- Wang, R.; Liu, M.; Liu, J. The Association between influenza vaccination and COVID-19 and its outcomes: A systematic review and meta-analysis of observational studies. Vaccines 2021, 9, 529. [Google Scholar] [CrossRef] [PubMed]
- Marín-Hernández, D.; Nixon, D.F.; Hupert, N. Heterologous vaccine interventions: Boosting immunity against future pandemics. Mol. Med. 2021, 27, 54. [Google Scholar] [CrossRef] [PubMed]
- Debisarun, P.A.; Gössling, K.L.; Bulut, O.; Kilic, G.; Zoodsma, M.; Liu, Z.; Oldenburg, M.; Rüchel, N.; Zhang, B.; Xu, C.J.; et al. Induction of trained immunity by influenza vaccination—Impact on COVID-19. PLoS Pathog. 2021, 17, e1009928. [Google Scholar] [CrossRef]
- Gilchrist, S.A.; Nanni, A.; Levine, O. Benefits and effectiveness of administering pneumococcal polysaccharide vaccine with seasonal influenza vaccine: An approach for policymakers. Am. J. Public Health 2012, 102, 596–605. [Google Scholar] [CrossRef] [PubMed]
- Domnich, A.; Grassi, R.; Fallani, E.; Spurio, A.; Bruzzone, B.; Panatto, D.; Marozzi, B.; Cambiaggi, M.; Vasco, A.; Orsi, A.; et al. Changes in attitudes and beliefs concerning vaccination and influenza vaccines between the first and second COVID-19 pandemic waves: A longitudinal study. Vaccines 2021, 9, 1016. [Google Scholar] [CrossRef]
- Lazarus, R.; Baos, S.; Cappel-Porter, H.; Carson-Stevens, A.; Clout, M.; Culliford, L.; Emmett, S.R.; Garstang, J.; Gbadamoshi, L.; Hallis, B.; et al. Safety and immunogenicity of concomitant administration of COVID-19 vaccines (ChAdOx1 or BNT162b2) with seasonal influenza vaccines in adults in the UK (ComFluCOV): A multicentre, randomised, controlled, phase 4 trial. Lancet 2021, 398, 2277–2287. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Coadministration of Seasonal Inactivated Influenza and COVID-19 Vaccines. Interim Guidance. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-vaccines-SAGE_recommendation-coadministration-influenza-vaccines (accessed on 13 December 2021).
- Centers for Disease Control and Prevention (CDC). Interim Clinical Considerations for Use of COVID-19 Vaccines Currently Authorized in the United States. Available online: https://www.cdc.gov/vaccines/covid-19/clinical-considerations/covid-19-vaccines-us.html#Coadministration (accessed on 13 December 2021).
- Italian Ministry of Health. Frequently Asked Questions—Influenza and Influenza Vaccination. Available online: https://www.salute.gov.it/portale/p5_1_1.jsp?lingua=italiano&faqArea=influenza&id=103 (accessed on 13 December 2021).
- Luo, C.; Yang, Y.; Liu, Y.; Zheng, D.; Shao, L.; Jin, J.; He, Q. Intention to COVID-19 vaccination and associated factors among health care workers: A systematic review and meta-analysis of cross-sectional studies. Am. J. Infect. Control 2021, 49, 1295–1304. [Google Scholar] [CrossRef] [PubMed]
- Cascini, F.; Pantovic, A.; Al-Ajlouni, Y.; Failla, G.; Ricciardi, W. Attitudes, acceptance and hesitancy among the general population worldwide to receive the COVID-19 vaccines and their contributing factors: A systematic review. EClinicalMedicine 2021, 40, 101113. [Google Scholar] [CrossRef] [PubMed]
- Domnich, A.; Cambiaggi, M.; Vasco, A.; Maraniello, L.; Ansaldi, F.; Baldo, V.; Bonanni, P.; Calabrò, G.E.; Costantino, C.; de Waure, C.; et al. Attitudes and beliefs on influenza vaccination during the COVID-19 pandemic: Results from a representative Italian survey. Vaccines 2020, 8, 711. [Google Scholar] [CrossRef] [PubMed]
- SWG, S.p.A. Activity. Available online: https://www.swg.it/activity (accessed on 17 January 2022).
- Italian National Institute of Statistics (ISTAT). Demography in Numbers. Available online: http://demo.istat.it/ (accessed on 17 January 2022).
- Italian National Institute of Statistics (ISTAT). ISTAT Classification of the Italian Education Qualifications. Available online: https://www.istat.it/it/files/2011/01/Classificazione-titoli-studio-28_ott_2005-nota_metodologica.pdf (accessed on 13 December 2021).
- R Core Team. R: A Language and Environment for Statistical Computing. Available online: http://www.R-project.org/ (accessed on 13 December 2021).
- Phillips, N. The coronavirus is here to stay—Here’s what that means. Nature 2021, 590, 382–384. [Google Scholar] [CrossRef] [PubMed]
- Giambi, C.; Fabiani, M.; D’Ancona, F.; Ferrara, L.; Fiacchini, D.; Gallo, T.; Martinelli, D.; Pascucci, M.G.; Prato, R.; Filia, A.; et al. Parental vaccine hesitancy in Italy—Results from a national survey. Vaccine 2018, 36, 779–787. [Google Scholar] [CrossRef]
- Bonanni, P.; Boccalini, S.; Bechini, A.; Varone, O.; Matteo, G.; Sandri, F.; Gabutti, G. Co-administration of vaccines: A focus on tetravalent Measles-Mumps-Rubella-Varicella (MMRV) and meningococcal C conjugate vaccines. Hum. Vaccines Immunother. 2020, 16, 1313–1321. [Google Scholar] [CrossRef] [Green Version]
- Stefanizzi, P.; Martinelli, A.; Bianchi, F.P.; Migliore, G.; Tafuri, S. Acceptability of the third dose of an-ti-SARS-CoV-2 vaccine co-administered with influenza vaccine: Preliminary data in a sample of Italian HCWs. Hum. Vaccines Immunother. 2021. [Google Scholar] [CrossRef]
- Van Buynder, P.G.; Newbound, A.; MacIntyre, C.R.; Kennedy, A.T.; Clarke, C.; Anderson, J. Australian experience of the SH21 flu vaccination program during the COVID-19 vaccine program. Hum. Vaccines Immunother. 2021, 17, 4611–4616. [Google Scholar] [CrossRef]
- Larson, H.J.; Clarke, R.M.; Jarrett, C.; Eckersberger, E.; Levine, Z.; Schulz, W.S.; Paterson, P. Measuring trust in vaccination: A systematic review. Hum. Vaccin. Immunother. 2018, 14, 1599–1609. [Google Scholar] [CrossRef]
- Prematunge, C.; Corace, K.; McCarthy, A.; Nair, R.C.; Pugsley, R.; Garber, G. Factors influencing pandemic influenza vaccination of healthcare workers-a systematic review. Vaccine 2012, 30, 4733–4743. [Google Scholar] [CrossRef]
- Wang, Q.; Yang, L.; Jin, H.; Lin, L. Vaccination against COVID-19: A systematic review and meta-analysis of acceptability and its predictors. Prev. Med. 2021, 150, 106694. [Google Scholar] [CrossRef] [PubMed]
- Jamison, A.M.; Quinn, S.C.; Freimuth, V.S. “You don’t trust a government vaccine”: Narratives of institutional trust and influenza vaccination among African American and white adults. Soc. Sci. Med. 2019, 221, 87–94. [Google Scholar] [CrossRef] [PubMed]
- Udow-Phillips, M.; Lantz, P.M. Trust in public health Is essential amid the COVID-19 pandemic. J. Hosp. Med. 2020, 15, 431–433. [Google Scholar] [CrossRef]
- Nehal, K.R.; Steendam, L.M.; Campos Ponce, M.; van der Hoeven, M.; Smit, G.S.A. Worldwide vaccination willingness for COVID-19: A systematic review and meta-analysis. Vaccines 2021, 9, 1071. [Google Scholar] [CrossRef] [PubMed]
- Kan, T.; Zhang, J. Factors influencing seasonal influenza vaccination behaviour among elderly people: A systematic review. Public Health 2018, 156, 67–78. [Google Scholar] [CrossRef]
- Yeung, M.P.; Lam, F.L.; Coker, R. Factors associated with the uptake of seasonal influenza vaccination in adults: A systematic review. J. Public Health 2016, 38, 746–753. [Google Scholar] [CrossRef] [Green Version]
- Nagata, J.M.; Hernández-Ramos, I.; Kurup, A.S.; Albrecht, D.; Vivas-Torrealba, C.; Franco-Paredes, C. Social determinants of health and seasonal influenza vaccination in adults ≥ 65 years: A systematic review of qualitative and quantitative data. BMC Public Health 2013, 13, 388. [Google Scholar] [CrossRef] [Green Version]
- Fridman, A.; Gershon, R.; Gneezy, A. COVID-19 and vaccine hesitancy: A longitudinal study. PLoS ONE 2021, 16, e0250123. [Google Scholar] [CrossRef]
- Gerussi, V.; Peghin, M.; Palese, A.; Bressan, V.; Visintini, E.; Bontempo, G.; Graziano, E.; De Martino, M.; Isola, M.; Tascini, C. Vaccine hesitancy among Italian patients recovered from COVID-19 infection towards influenza and Sars-Cov-2 vaccination. Vaccines 2021, 9, 172. [Google Scholar] [CrossRef]
- Cheung, E.K.H.; Lee, S.; Lee, S.S. Pattern of exposure to information and its impact on seasonal influenza vaccination uptake in nurses. J. Hosp. Infect. 2017, 97, 376–383. [Google Scholar] [CrossRef] [PubMed]
- Italian Ministry of Health. Prevention and Control of Influenza: Recommendations for Season 2021–2022. Available online: https://www.trovanorme.salute.gov.it/norme/renderNormsanPdf?anno=2021&codLeg=79647&parte=1%20&serie=null (accessed on 13 December 2021).
- Grohskopf, L.A.; Alyanak, E.; Ferdinands, J.M.; Broder, K.R.; Blanton, L.H.; Talbot, H.K.; Fry, A.M. Prevention and control of seasonal influenza with vaccines: Recommendations of the Advisory Committee on Immunization Practices, United States, 2021–22 influenza season. MMWR Recomm. Rep. 2021, 70, 1–28. [Google Scholar] [CrossRef] [PubMed]
- Boccalini, S.; Tacconi, F.M.; Lai, P.L.; Bechini, A.; Bonanni, P.; Panatto, D. Appropriateness and preferential use of different seasonal influenza vaccines: A pilot study on the opinion of vaccinating physicians in Italy. Vaccine 2019, 37, 915–918. [Google Scholar] [CrossRef]
- Bonanni, P.; Boccalini, S.; Zanobini, P.; Dakka, N.; Lorini, C.; Santomauro, F.; Bechini, A. The appropriateness of the use of influenza vaccines: Recommendations from the latest seasons in Italy. Hum. Vaccines Immunother. 2018, 14, 699–705. [Google Scholar] [CrossRef] [PubMed]
- Domnich, A.; Manini, I.; Calabrò, G.E.; de Waure, C.; Montomoli, E. Mapping host-related correlates of influenza vaccine-induced immune response: An umbrella review of the available systematic reviews and meta-analyses. Vaccines 2019, 7, 215. [Google Scholar] [CrossRef] [Green Version]
- McDonald, I.; Murray, S.M.; Reynolds, C.J.; Altmann, D.M.; Boyton, R.J. Comparative systematic review and meta-analysis of reactogenicity, immunogenicity and efficacy of vaccines against SARS-CoV-2. NPJ Vaccines 2021, 6, 74. [Google Scholar] [CrossRef]
- Scheibehenne, B.; Greifeneder, R.; Todd, P.M. What moderates the too-much-choice effect? Psychol. Mark. 2009, 26, 229–253. [Google Scholar] [CrossRef] [Green Version]
- Ogden, J.; Daniells, E.; Barnett, J. When is choice a good thing? An experimental study of the impact of choice on patient outcomes. Psychol. Health Med. 2009, 14, 34–47. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gofen, A.; Needham, C. Service personalization as a response to noncompliance with routine childhood vaccination. Governance 2015, 28, 269–283. [Google Scholar] [CrossRef]
- Toback, S.; Galiza, E.; Cosgrove, C.; Galloway, J.; Goodman, A.L.; Swift, P.A.; Rajaram, S.; Graves-Jones, A.; Edelman, J.; Burns, F.; et al. Safety, immunogenicity, and efficacy of a COVID-19 vaccine (NVX-CoV2373) co-administered with seasonal influenza vaccines: An exploratory substudy of a randomised, observer-blinded, placebo-controlled, phase 3 trial. Lancet Respir Med. 2021. [Google Scholar] [CrossRef]
- Izikson, R.; Brune, D.; Bolduc, J.S.; Bourron, P.; Fournier, M.; Mallett Moore, T.; Pandey, A.; Lucia Perez, L.; Sater, N.; Shrestha, A.; et al. Safety and immunogenicity of a high-dose quadrivalent influenza vaccine administered concomitantly with a third dose of the mRNA-1273 SARS-CoV-2 vaccine in adults ≥ 65 years of age: A Phase II, open-label study. medRxiv 2021. Available online: https://www.medrxiv.org/content/10.1101/2021.10.29.21265248v1 (accessed on 13 December 2021).
- Selya-Hammer, C.; Fleming, D.; Jiang, Y.; Durnall, H.; Keeping, S.; Carroll, S. Co-administration of PPV23 and influenza vaccines in England and Wales: A study based on the Royal College of General Practitioners Sentinel Surveillance Network. J. Vaccines Immun. 2015, 1, 043–049. [Google Scholar]
- Italian Institute of Statistics. Internet Use. Available online: http://dati.istat.it/index.aspx?queryid=22998 (accessed on 13 December 2021).
- Italian Ministry of Health. Influenza Vaccination Coverage. Available online: https://www.salute.gov.it/portale/influenza/dettaglioContenutiInfluenza.jsp?lingua=italiano&id=679&area=influenza&menu=vuoto (accessed on 13 December 2021).
| Variable | Level | % (n) |
|---|---|---|
| Sex | Male | 47.8 (1177) |
| Female | 52.2 (1286) | |
| Age, years | 18–24 | 7.9 (194) |
| 25–34 | 12.5 (309) | |
| 35–44 | 15.4 (380) | |
| 45–54 | 19.8 (488) | |
| 55–64 | 16.7 (412) | |
| 65–74 | 21.0 (516) | |
| ≥75 | 6.7 (164) | |
| Geographic macro-area | Northwest | 27.0 (664) |
| Northeast | 18.9 (465) | |
| Center | 20.1 (496) | |
| South | 22.9 (563) | |
| Islands | 11.2 (275) | |
| Educational level | 1 | 1.5 (38) |
| 2 | 8.0 (197) | |
| 3–4 | 48.2 (1188) | |
| 5 | 40.5 (997) | |
| 6 | 1.7 (43) | |
| Employment pattern | Employed | 55.4 (1364) |
| Student | 6.7 (165) | |
| Housekeeper | 8.3 (204) | |
| Unemployed | 5.2 (129) | |
| Retired | 23.5 (580) | |
| Other/prefer not to reply | 0.9 (21) | |
| Perceived income | Low | 1.8 (44) |
| Lower than average | 41.2 (1014) | |
| Average | 30.8 (759) | |
| Higher than average | 7.6 (187) | |
| High | 2.4 (59) | |
| No personal income | 16.2 (400) | |
| Self-rated health | Excellent | 11.5 (284) |
| Very good | 48.3 (1190) | |
| Good | 36.2 (891) | |
| Fair | 3.5 (86) | |
| Poor | 0.5 (12) |
| Influenza Vaccination | COVID-19 Vaccination, % (n) | ||||
|---|---|---|---|---|---|
| Complete | Partial | Planned | No Intention | Total | |
| Never | 35.9 (885) | 1.0 (25) | 1.5 (36) | 5.8 (142) | 44.2 (1088) |
| In the past but not in 2020/2021 | 10.7 (263) | 0.6 (14) | 0.7 (18) | 1.3 (31) | 13.2 (326) |
| In 2020/2021 but not in the past | 10.6 (262) | 0.4 (11) | 0.7 (17) | 0.2 (5) | 12.0 (295) |
| Both in 2020/2021 and in the past | 27.8 (685) | 1.3 (33) | 0.9 (22) | 0.6 (14) | 30.6 (754) |
| Total | 85.1 (2095) | 3.4 (83) | 3.8 (93) | 7.8 (192) | 100 (2463) |
| Variable | Level | aOR (95% CI) | p |
|---|---|---|---|
| Sex | Male | Ref | – |
| Female | 0.56 (0.47–0.67) | <0.001 | |
| Age | 1-year increase | 0.99 (0.98–0.99) | <0.001 |
| Previous influenza vaccination | Never | Ref | – |
| In the past but not in 2020/2021 | 1.09 (0.83–1.44) | 0.53 | |
| In 2020/2021 but not in the past | 1.52 (1.14–2.04) | 0.005 | |
| Both in 2020/2021 and in the past | 1.89 (1.49–2.41) | <0.001 | |
| COVID-19 vaccination | No intention | Ref | – |
| Planned | 4.97 (2.70–9.12) | <0.001 | |
| Partial | 3.44 (1.81–6.55) | <0.001 | |
| Complete | 7.78 (4.91–12.33) | <0.001 | |
| Recently searched for influenza vaccination information | No | Ref | – |
| Yes | 1.38 (1.13–1.69) | 0.001 | |
| Vaccines are crucial to public health 1 | Disagree 2 | Ref | – |
| Agree 3 | 1.37 (1.05–1.80) | 0.021 | |
| Vaccines are safe 1 | Disagree 2 | Ref | – |
| Agree 3 | 2.11 (1.64–2.70) | <0.001 | |
| Need more information on vaccines 1 | Disagree 2 | Ref | – |
| Agree 3 | 0.60 (0.48–0.75) | <0.001 | |
| Would pay for influenza vaccine 1 | Disagree 2 | Ref | – |
| Agree 3 | 1.79 (1.46–2.19) | <0.001 | |
| Would like to have a personalized influenza vaccine 1 | Disagree 2 | Ref | – |
| Agree 3 | 1.55 (1.25–1.94) | <0.001 | |
| Influenza is a banal disease 1 | Agree 3 | Ref | – |
| Disagree 2 | 1.36 (1.12–1.64) | 0.002 | |
| COVID-19 pandemic is not finished 1 | Disagree 2 | Ref | – |
| Agree 3 | 1.32 (1.01–1.73) | 0.043 | |
| Only the elderly are at high risk of influenza and COVID-19 1 | Agree 3 | Ref | – |
| Disagree 2 | 1.20 (0.98–1.47) | 0.078 | |
| Trust in public health institutions | 1-point increase | 1.22 (1.16–1.28) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Domnich, A.; Grassi, R.; Fallani, E.; Ciccone, R.; Bruzzone, B.; Panatto, D.; Ferrari, A.; Salvatore, M.; Cambiaggi, M.; Vasco, A.; et al. Acceptance of COVID-19 and Influenza Vaccine Co-Administration: Insights from a Representative Italian Survey. J. Pers. Med. 2022, 12, 139. https://doi.org/10.3390/jpm12020139
Domnich A, Grassi R, Fallani E, Ciccone R, Bruzzone B, Panatto D, Ferrari A, Salvatore M, Cambiaggi M, Vasco A, et al. Acceptance of COVID-19 and Influenza Vaccine Co-Administration: Insights from a Representative Italian Survey. Journal of Personalized Medicine. 2022; 12(2):139. https://doi.org/10.3390/jpm12020139
Chicago/Turabian StyleDomnich, Alexander, Riccardo Grassi, Elettra Fallani, Roberto Ciccone, Bianca Bruzzone, Donatella Panatto, Allegra Ferrari, Marco Salvatore, Maura Cambiaggi, Alessandro Vasco, and et al. 2022. "Acceptance of COVID-19 and Influenza Vaccine Co-Administration: Insights from a Representative Italian Survey" Journal of Personalized Medicine 12, no. 2: 139. https://doi.org/10.3390/jpm12020139
APA StyleDomnich, A., Grassi, R., Fallani, E., Ciccone, R., Bruzzone, B., Panatto, D., Ferrari, A., Salvatore, M., Cambiaggi, M., Vasco, A., Orsi, A., & Icardi, G. (2022). Acceptance of COVID-19 and Influenza Vaccine Co-Administration: Insights from a Representative Italian Survey. Journal of Personalized Medicine, 12(2), 139. https://doi.org/10.3390/jpm12020139






