Beyond the Image Frame: An Art-Based Pedagogical Framework for Teaching Diagnostic Reasoning in Breast Ultrasound to Medical Students
Abstract
1. Introduction
2. Methods
- I
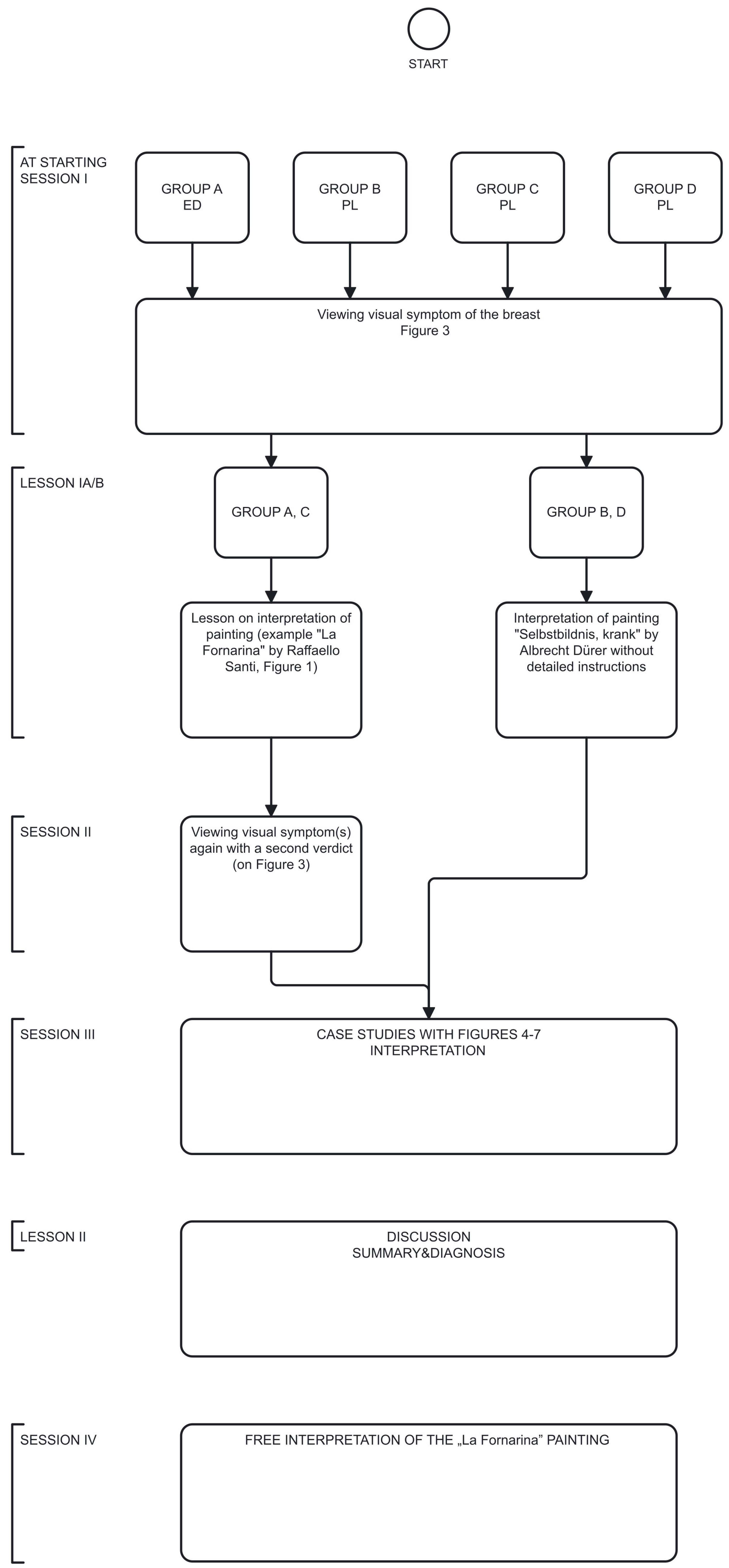
- At starting session (I session). In the initial session of the four-day workshop, all four groups (A–D) of students (Group A on day 1, Group B on day 2, etc.) were independently provided with the same clinical image of the patient with left breast abnormality that had been retrieved by the project developers (Figure 3) and assigned the task to formulate a medical diagnosis in the form of a single sentence within 5 min.
- II
- Lesson Ia on the interpretation of the painting La Fornarina by Raffaello Sanzio. This painting was used as an example of a painting with “diagnostic” properties in cases of Groups A and C but not in cases of Groups B and D. The selection of this painting for analysis was motivated by the controversy surrounding its diagnostic utility and its continued citation as a foundational reference for various medical considerations [3,4,17,22]. During this lesson, a methodology for interpreting the “medical” image from the perspectives of visual culture, art history, and visual arts was presented (Supplementary Material S1).
- III
- The second (II) session. During the second session, Groups A and C, who had received the Lesson Ia on image interpretation, were given tasks of issuing a diagnostic verdict again.
- IV
- Lesson Ib. Students in Group B and D interpreted another Renaissance artwork in the form of a drawing by Albrecht Durer entitled Selbstbildnis, krank but without detailed instructions driven by art history and semiology [23]. Students from groups A and C did not participate in this activity.
- V
- In the third (III) session, each group of medical students (Groups A, B, C, and D) displayed a case study with clinical images of four different patients: Group A—Figure 4, Group B—Figure 5, Group C—Figure 6, Group D—Figure 7. The students were then asked to formulate an interpretation of all signs and symptoms they see.
- VI
- Lesson II was a summary of the previous sessions and lessons, including an explanation of the diagnosis.After this lesson, each group of students underwent a “Be like Raphael” workshop (Supplementary Material S2).
- VII
- During the fourth (IV) session, students were tasked with creating their own interpretation of Raphael’s La Fornarina painting based on the specific case studies they analyzed in the previous session. They were given one week to complete this task. This session was conducted fully online. A summary of the proceedings and results of all sessions is provided in the Results section of this report and in the Supplementary Material S3 as well.
3. Results
3.1. At Starting Session—Initial Student Interpretation
3.2. Lesson Ia—Seminar Room (Groups A and C)
3.3. Second Session
3.4. Lesson Ib—Seminar Room (Groups B and D)
3.5. Third Session
3.5.1. Patient of Group A
3.5.2. Patient of Group B
3.5.3. Patient of Group C
3.5.4. Patient of Group D
3.6. Conclusions
3.6.1. Summary
3.6.2. Discussion
3.7. Fourth Session
4. Final Discussion
5. Recommendations
6. Limitations
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AI | Artificial intelligence |
| ARSA | Arthur Schopenhauer Research Academy |
| ARSATTM | ARSA Think Tank Meeting |
| BI-RADS | Breast Imaging-Reporting and Data System |
| BSE | breast self-examination |
| BUS | Breast ultrasound |
| BUST | Polyclinic of Gynecology and Senology, Division of Breast Ultrasound and Senological Treatment |
| COVID-19 | Coronavirus disease 2019 |
| GLOBOCAN | The Global Cancer Observatory |
| MMG | Mammography |
| MRI | Magnetic resonance imaging |
| NML | Non-mass lesion |
| SGWG | Senological Gynecology Working Group |
| US | Ultrasound |
References
- Snell, M. Was Raphael Married? ThoughtCo. Available online: https://www.thoughtco.com/was-raphael-married-3969429 (accessed on 1 June 2025).
- Espinel, K.H. The portrait of breast cancer and Raphael’s La Fornarina. Lancet 2002, 360, 2061–2063. [Google Scholar] [CrossRef]
- Baum, M. La Fornarina: Breast cancer or not? Lancet 2003, 361, 1129. [Google Scholar] [CrossRef] [PubMed]
- Śniadecki, M.; Malitowska, A.; Musielak, O.; Meyer-Szary, J.; Guzik, P.; Boyke, Z.; Danielkiewicz, M.; Konarzewska, J.; Aristei, C. on behalf of the Senological Gynecology Working Group. The Art of Medical Diagnosis: Lessons on Interpretation of Signs from Italian High Renaissance Paintings. Diagnostics 2025, 15, 380. [Google Scholar] [CrossRef]
- Bray, F.; Laversanne, M.; Sung, H.; Ferlay, J.; Siegel, R.L.; Soerjomataram, F.; Jemal, A. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2024, 74, 229–263. [Google Scholar] [CrossRef] [PubMed]
- Giaquinto, A.N.; Sung, H.; Newman, L.A.; Freedman, R.A.; Smith, R.A.; Star, J.; Jemal, A.; Siegel, R. Breast cancer statistics 2024. CA Cancer J. Clin. 2024, 74, 477–495. [Google Scholar] [CrossRef]
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef]
- Giurge, L.M.; Whillans, A.V.; West, C. Why time poverty matters for individuals, organizations and nations. Nat. Hum, Behav. 2020, 4, 993–1003. [Google Scholar] [CrossRef] [PubMed]
- Honore, C. In Praise of Slow; Orion: London, UK, 2019. [Google Scholar]
- Updates in Slow Medicine. Available online: http://slowmedupdates.com (accessed on 15 May 2025).
- de Azambuja, E.; Trapani, D.; Loibl, S.; Delaloge, S.; Senkus, E.; Criscitiello, C.; Poortman, P.; Gnant, M.; Di Cosimo, S.; Cortes, J.; et al. ESMO Management and treatment adapted recommendations in the COVID-19 era: Breast Cancer. ESMO Open 2020, 5, e000793. [Google Scholar] [CrossRef]
- Chan, J.J.; Sim, Y.; Ow, S.G.W.; Lim, J.S.J.; Kusumawidjaja, G.; Zhuang, Q.; Wong, R.X.; Wong, F.Y.; Tan, V.K.M.; Tan, T.J.Y. The impact of COVID-19 on and recommendations for breast cancer care: The Singapore experience. Endocr. Relat. Cancer 2020, 27, R307–R327. [Google Scholar] [CrossRef]
- Sonagli, M.; Cagnacci Neto, R.; Leite, F.P.M.; Makdissi, F.B.A. The use of telemedicine to maintain breast cancer follow-up and surveillance during the COVID-19 pandemic. J. Surg. Oncol. 2021, 123, 371–374. [Google Scholar] [CrossRef]
- Monaghesh, E.; Hajizadeh, A. The role of telehealth during COVID-19 outbreak: A systematic review based on current evidence. BMC Public Health 2020, 20, 1193. [Google Scholar] [CrossRef] [PubMed]
- Moskal, P.; Dulski, K.; Chug, N.; Curceanu, C.; Czerwiński, E.; Dadgar, M.; Gajewski, J.; Gajos, A.; Grudzień, G.; Hiesmayr, B.C.; et al. Positronium imaging with the novel multiphoton PET scanner. Sci. Adv. 2021, 7, eabh4394. [Google Scholar] [CrossRef]
- Hall, M.B. Classicism, Mannerism, and the Relieflike Style. In The Cambridge Companion to Raphael; Hall, M.B., Ed.; Cambridge University Press: Cambridge, UK, 2005; p. 224. [Google Scholar]
- Bianucci, R.; Perciaccante, A.; Charlier, P.; Appenzeller, O.; Lippi, D. Earliest evidence of malignant breast cancer in Renaissance paintings. Lancet Oncol. 2018, 19, 166–167. [Google Scholar] [CrossRef]
- Charlier, P.; Perciaccante, A.; Kluger, N.; Nerlich, A.G.; Appenzeller, O.; Donell, S.T.; Asensi, V.; Mackowiak, P.A.; Ferrara, V.; Bianucci, R. Iconodiagnosis: Guidelines and recommendations. Ethics Med. Public Health 2023, 31, 100951. [Google Scholar] [CrossRef]
- Nerlich, A.G.; Dewaal, J.C.; Perciaccante, A.; di Cosimo, S.; Cortesi, L.; Wimmer, J.; Donell, S.T.; Bianucci, R. Did Michelangelo paint a young adult woman with breast cancer in ”The Flood” (Sistine Chapel, Rome)? Breast 2024, 78, 103823. [Google Scholar] [CrossRef] [PubMed]
- Śniadecki, M.; Malitowska, A.; Musielak, O.; Boyke, Z.; Aristei, C. What can paintings teach us? Breast 2025, 80, 103882. [Google Scholar] [CrossRef] [PubMed]
- di Cosimo, S.; Perciaccante, A.; Donell, S.T.; Wimmer, J.; Nerlich, A.G.; DeWaal, J.C.; Cortesi, L.; Bianucci, R. Reply to the letter: What can paintings teach us? Breast 2025, 80, 103893. [Google Scholar] [CrossRef]
- Śniadecki, M.; Boyke, Z.; Kijanska, P.; Meyer-Szary, J.; Aristei, C.; Malitowska, A. How Renaissance Paintings Can be used to Teach Students to Interpret Patient Symptoms: The Example of Breast Cancer. In Proceedings of the 11th Annual International Conference on Nursing, Athens, Greece, 5–8 May 2025; Athens Institute for Education and Research: Athens, Greece, 2025. abstract no. 24. Available online: https://www.atiner.gr/abstracts/2025ABST-NUR.pdf (accessed on 13 February 2026).
- Selbstbildnis, Krank. Available online: https://onlinekatalog.kunsthalle-bremen.de/DE-MUS-027614/object/8237 (accessed on 22 February 2025).
- Digital Dante. Inferno XIV. Available online: https://digitaldante.columbia.edu/dante/divine-comedy/inferno/inferno-14 (accessed on 23 September 2025).
- Bettini, M. Il Nudo. Eros, Natura, Artificio; Fossi, G., Ed.; Giunti Editore: Florence, Italy, 2019. [Google Scholar]
- Plato. The Allegory of the Cave. Available online: https://web.sbu.edu/theology/bychkov/plato%20republic%207.pdf (accessed on 13 February 2026).
- Poprzecka, M. Inni inaczej. Obrazy obcych i obraz cudzego. Przegląd Hist. 2009, 100, 363–385. [Google Scholar]
- Jones, J. The Loves of the Artists. Art and Passion in the Renaissance; Simon & Schuster: London, UK; New York, NY, USA, 2013. [Google Scholar]
- Mulvey, L. Visual pleasure and narrative cinema. In Film Theory and Criticism: Introductory Readings; Mast, G., Cohen, M., Braudy, L., Eds.; Oxford University Press: New York, NY, USA, 1992; pp. 746–757. [Google Scholar]
- Rose, G. Visual Metodology: An Introduction to the Interpretation of Visual Materials, 4th ed.; SAGE Publications Ltd.: London, UK, 2001. [Google Scholar]
- Peirce, C.S. Collected Papers of Charles Sanders Peirce: Vol. 1–2. Principles of Philosophy and Elements of Logic; Hartshorne, C., Weiss, P., Eds.; Harvard University Press: Cambridge, MA, USA, 1932; Volume 1. [Google Scholar]
- Seitz, H.M. “Do der gelb fleck ist…” Dürers Malaria, eine Fehldiagnose. Wien. Klin. Wochenschr. 2010, 122, 10–13. [Google Scholar] [CrossRef]
- Schott, G.D. The Sick Dürer—A Renaissance prototype pain map. BMJ 2004, 329, 1492. [Google Scholar] [CrossRef] [PubMed]
- Vasari, G. Lives of the Artists. Raphael of Urbino; Penguin Books: Harmondsworth, UK, 1970; pp. 306–307. [Google Scholar]
- Wojcinski, S.; Farrokh, A.; Weber, S.; Thomas, A.; Fischer, T.; Slowinski, T.; Schmidt, W. Multicenter Study of Ultrasound Real-Time Tissue Elastography in 779 Cases for the Assessment of Breast Lesions: Improved Diagnostic Performance by Combining the BI-RADS®-US Classification System with Sonoelastography. Ultraschall Med.—Eur. J. Ultrasound 2010, 31, 484–491. [Google Scholar] [CrossRef]
- Hicks, M.J.; Davis, J.R.; Layton, J.M.; Present, A.J. Sensitivity of mammography and physical examination of the breast for detecting breast cancer. JAMA 1979, 242, 2080–2083. [Google Scholar] [CrossRef] [PubMed]
- Kolb, T.M.; Lichy, J.; Newhouse, J.H. Comparison of the Performance of Screening Mammography, Physical Examination, and Breast US and Evaluation of Factors that Influence Them: An Analysis of 27,825 Patient Evaluations. Radiology 2002, 225, 165–175. [Google Scholar] [CrossRef] [PubMed]
- Yao, M.M.-S.; Joe, B.N.; Sickles, E.A.; Lee, C.S. BI-RADS Category 5 Assessments at Diagnostic Breast Imaging: Outcomes Analysis Based on Lesion Descriptors. Acad. Radiol. 2019, 26, 1048–1052. [Google Scholar] [CrossRef]
- Carin, A.; Molière, S.; Gabriele, V.; Lodi, M.; Thiébaut, N.; Neuberger, K.; Mathelin, C. Relevance of breast MRI in determining the size and focality of invasive breast cancer treated by mastectomy: A prospective study. World J. Surg. Oncol. 2017, 15, 128. [Google Scholar] [CrossRef]
- Brem, R.F.; Lenihan, M.J.; Lieberman, J.; Torrente, J. Screening Breast Ultrasound: Past, Present, and Future. Am. J. Roentgenol. 2015, 204, 234–240. [Google Scholar] [CrossRef]
- Wang, J.; Gottschal, P.; Ding, L.; van Veldhuizen, D.W.A.; Lu, W.; Houssami, N.; Greuter, M.J.W.; de Bock, G.H. Mammographic sensitivity as a function of tumor size: A novel estimation based on population-based screening data. Breast 2021, 55, 69–74. [Google Scholar] [CrossRef]
- Shaevitch, D.; Taghipour, S.; Miller, A.B.; Montgomery, N.; Harvey, B. Tumor size distribution of invasive breast cancers and the sensitivity of screening methods in the Canadian National Breast Screening Study. J. Cancer Res. Ther. 2017, 13, 562–569. [Google Scholar] [CrossRef]
- Güth, U.; Huang, D.J.; Huber, M.; Schötzau, A.; Wruk, D.; Holzgreve, W.; Wight, E.; Zanetti-Dällenbach, R. Tumor size and detection in breast cancer: Self-examination and clinical breast examination are at their limit. Cancer Detect. Prev. 2008, 32, 224–228. [Google Scholar] [CrossRef]
- Moyle, P.; Sonoda, L.; Britton, P.; Sinnatamby, R. Incidental breast lesions detected on CT: What is their significance? Br. J. Radiol. 2010, 83, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Buta, M.G. Genetic diseases in religious painting. Med. Pharm. Rep. 2021, 94, 382–389. [Google Scholar] [CrossRef] [PubMed]
- Lazzeri, D.; Lippi, D.; Castello, M.F.; Weisz, G.M. Breast Mass in a Rubens Painting. Rambam Maimonides Med. J. 2016, 7, e0016. [Google Scholar] [CrossRef] [PubMed]
- Committee on Diagnostic Error in Health Care; Board on Health Care Services; Institute of Medicine; The National Academies of Sciences, Engineering, and Medicine; Balogh, E.P.; Miller, B.T.; Ball, J.R. (Eds.) Improving Diagnosis in Health Care; National Academies Press: Washington, DC, USA, 2015. Available online: https://www.ncbi.nlm.nih.gov/books/NBK338593/ (accessed on 23 October 2025).
- Robinson, K.M.; Christensen, K.B.; Ottesen, B.; Krasnik, A. Diagnostic delay, quality of life and patient satisfaction among women diagnosed with endometrial or ovarian cancer: A nationwide Danish study. Qual. Life Res. 2012, 21, 1519–1525. [Google Scholar] [CrossRef]
- Yang, Y.; Xu, J.; Hu, Y.; Hu, J.; Jiang, A. The experience of patients with cancer on narrative practice: A systematic review and meta-synthesis. Health Expect. 2020, 23, 274–283. [Google Scholar] [CrossRef]
- Viegas, I.S. The Role of Information Technology in Improving the Quality of Health Services in Hospitals. J. Soc. Sci. 2024, 3, 1561–1571. [Google Scholar] [CrossRef]
- Grasset, E.M.; Deshpande, A.; Lee, J.W.; Cho, Y.; Shin, S.M.; Coyne, E.M.; Hernandez, A.; Yuan, X.; Zhang, Z.; Cimino-Mathews, A.; et al. Mapping the breast tumor microenvironment: Proximity analysis reveals spatial relationships between macrophage subtypes and metastasis-initiating cancer cells. Oncogene 2024, 43, 2927–2937. [Google Scholar] [CrossRef] [PubMed]
- Fröhlich, E. The Variety of 3D Breast Cancer Models for the Study of Tumor Physiology and Drug Screening. Int. J. Mol. Sci. 2023, 24, 7116. [Google Scholar] [CrossRef]
- Majewski, L. The Mill and the Cross [Film]; Angelus Silesius: Warsaw, Poland; Telewizja Polska: Warsaw, Poland; Arkana Studio: Warsaw, Poland; Bokomotiv Filmproduktion: Stockholm, Sweden, 2011. [Google Scholar]
- Webber, P. Girl with a Pearl Earring [Film]; UK Film Council: London, UK; Archer Street Productions: London, UK; DeLux Productions: Luxembourg; Inside Track: London, UK; Film Fund Luxembourg: Luxembourg; Wild Bear Films: London, UK, 2003. [Google Scholar]






| Type of Signs | Definition | Medical Perspective | Art History/Visual Culture Perspective |
|---|---|---|---|
| Indexical sign | It represents real, physical connection between the signifier and the signified. | The naked breast with a mass, retraction, skin discoloration (deformation)— index sign of breast cancer. | The naked breast—index sign of art nude. |
| Iconic sign | It represents an object if the sign and the object are similar. | N/A | The art nude is an iconic sign of Western art as visual culture. |
| Symbolic sign | There is a convention that assigns denotations to them, which means that symbols require interpretation based on specific conventions. | N/A | Raphael uses the female body (signifiant) to symbolize sensual beauty and (unfulfilled) love (signifié); left side may also symbolize sin: Latin sinister—not right. |
| 11 Steps to Achieve the Final Portrait of the Left Breast of La Fornarina, Including 9 Pigments [2] | 11 Steps to Achieve the Final 2D Ultrasound Tumor Image | |
|---|---|---|
| 1. | Applying primer under the paint | 2D enhancement: sets the brightness of the entire 2D image |
| 2. | Sketching the outline of the shape | Penetration depth: reduces or increases the size of the 2D image |
| 3. | Black | TGC correction sliders changes the gain at certain penetration depths in the 2D projection, thus allowing for accurate compensation of echo weakening over the time (depth) |
| 4. | Gray | Frequency range: allows the operator to quickly adjust settings for high resolution/low penetration, medium resolution/medium penetration, low resolution/high penetration for a 2D image |
| 5. | Violet | Harmonic imaging: provides better grayscale contrast compared with the standard ultrasound imaging |
| 6. | Blue | Simultaneous multi-frequency operation: this function combines the use of low frequency to increase penetration and higher frequency to maintain high resolution |
| 7. | Pink | Code excitation improves image resolution and penetration of deeper areas |
| 8. | Creamy | Cross-beam imaging (XBeam-CRI): increases contrast resolution with better tissue differentiation and clearer organ contours |
| 9. | Brown | Noise reduction imaging (SRI II): smooths the final image |
| 10. | Taupe | Color Doppler application |
| 11. | Umbra | Use of elastography |
| Diagnostic Method of a Breast Tumor | Average Tumor Size (cm) | Reference |
|---|---|---|
| Magnetic resonance imaging | 0.7 | [39] |
| Ultrasonography | 1.0 | [40] |
| Mammographic screening | 1.4 | [41,42] |
| Clinical breast exam and self-examination | 2.05 and 2.1 | [43] |
| Incidental detection | 2.85 | [44] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Śniadecki, M.; Morawska, M.; Kijańska, P.; Kondratowicz, O.; Nowakowska, J.; Musielak, O.; Singla, A.; Chhabria, R.A.; Alvi, H.; Banaszak, A.; et al. Beyond the Image Frame: An Art-Based Pedagogical Framework for Teaching Diagnostic Reasoning in Breast Ultrasound to Medical Students. Diagnostics 2026, 16, 642. https://doi.org/10.3390/diagnostics16040642
Śniadecki M, Morawska M, Kijańska P, Kondratowicz O, Nowakowska J, Musielak O, Singla A, Chhabria RA, Alvi H, Banaszak A, et al. Beyond the Image Frame: An Art-Based Pedagogical Framework for Teaching Diagnostic Reasoning in Breast Ultrasound to Medical Students. Diagnostics. 2026; 16(4):642. https://doi.org/10.3390/diagnostics16040642
Chicago/Turabian StyleŚniadecki, Marcin, Maria Morawska, Patrycja Kijańska, Olga Kondratowicz, Julia Nowakowska, Oliwia Musielak, Abhishek Singla, Ritu Amit Chhabria, Hanaf Alvi, Amelia Banaszak, and et al. 2026. "Beyond the Image Frame: An Art-Based Pedagogical Framework for Teaching Diagnostic Reasoning in Breast Ultrasound to Medical Students" Diagnostics 16, no. 4: 642. https://doi.org/10.3390/diagnostics16040642
APA StyleŚniadecki, M., Morawska, M., Kijańska, P., Kondratowicz, O., Nowakowska, J., Musielak, O., Singla, A., Chhabria, R. A., Alvi, H., Banaszak, A., Grono, L., Akhmed, D., Kokot, K., Grzelak, M., Duszyński, K., Marozik, K., Jaworska, P., Majchrzak, J., Krupovich, N., ... on behalf of Senological Gynecology Working Group. (2026). Beyond the Image Frame: An Art-Based Pedagogical Framework for Teaching Diagnostic Reasoning in Breast Ultrasound to Medical Students. Diagnostics, 16(4), 642. https://doi.org/10.3390/diagnostics16040642









