Salivary Protein and Electrolyte Profiles during Primary Teeth Eruption: A Cross-Sectional Study
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wise, G.E.; Frazier-Bowers, S.; D’souza, R.N. Cellular, molecular, and genetic determinants of tooth eruption. Crit. Rev. Oral Biol. Med. 2002, 13, 323–335. [Google Scholar] [CrossRef]
- Thesleff, I. The genetic basis of tooth development and dental defects. Am. J. Med. Genet. Part A 2006, 140, 2530–2535. [Google Scholar] [CrossRef]
- Barlow, B.S.; Kanellis, M.J.; Slayton, R.L. Tooth eruption symptoms: A survey of parents and health professionals. J. Dent. Child. 2002, 69, 148–150. [Google Scholar]
- Iavarone, F.; Olianas, A.; Patini, R.; Gallenzi, P.; Di Tonno, L.; Desiderio, C.; Cabras, T.; Manconi, B.; Vincenzoni, F.; Cordaro, M.; et al. Top down proteomic analysis of gingival crevicular fluid in deciduous, exfoliating and permanent teeth in children. J. Proteom. 2020, 226, 103890. [Google Scholar] [CrossRef]
- Nahajowski, M.; Hnitecka, S.; Antoszewska-Smith, J.; Rumin, K.; Dubowik, M.; Sarul, M. Factors influencing an eruption of teeth associated with a dentigerous cyst: A systematic review and meta-analysis. BMC Oral Health 2021, 21, 180. [Google Scholar] [CrossRef]
- Rao, P.V.; Reddy, A.P.; Lu, X.; Dasari, S.; Krishnaprasad, A.; Biggs, E.; Roberts, C.T., Jr.; Nagalla, S.R. Proteomic identification of salivary biomarkers of type-2 diabetes. J. Proteome Res. 2009, 8, 239–245. [Google Scholar] [CrossRef]
- Deshpande, R.R.; Panvalkar, P.S.; Kulkarni, A.A.; Gadkri, T.V. Age-related changes of the human salivary secretory total protein complex and trace elements in children between the age group of 3-16 years. J. Biomed. Sci. Res. 2011, 3, 362–367. [Google Scholar]
- Dezan, C.; Nicolau, J.; Souza, D.; Walter, L. Flow rate, amylase activity, and protein and sialic acid concentrations of saliva from children aged 18, 30 and 42 months attending a baby clinic. Arch. Oral Biol. 2002, 47, 423–427. [Google Scholar] [CrossRef]
- Messana, I.; Cabras, T.; Iavarone, F.; Manconi, B.; Huang, L.; Martelli, C.; Olianas, A.; Sanna, M.T.; Pisano, E.; Sanna, M.; et al. Chrono-Proteomics of Human Saliva: Variations of the Salivary Proteome during Human Development. J. Proteome Res. 2015, 14, 1666–1677. [Google Scholar] [CrossRef]
- Manconi, B.; Cabras, T.; Pisano, E.; Sanna, M.; Olianas, A.; Fanos, V.; Faa, G.; Nemolato, S.; Iavarone, F.; Castagnola, M.; et al. Modifications of the acidic soluble salivary proteome in human children from birth to the age of 48months investigated by a top-down HPLC–ESI–MS platform. J. Proteom. 2013, 91, 536–543. [Google Scholar] [CrossRef]
- Inzitari, R.; Vento, G.; Capoluongo, E.; Boccacci, S.; Fanali, C.; Cabras, T.; Romagnoli, C.; Giardina, B.; Messana, I.; Castagnola, M. Proteomic Analysis of Salivary Acidic Proline-Rich Proteins in Human Preterm and At-Term Newborns. J. Proteome Res. 2007, 6, 1371–1377. [Google Scholar] [CrossRef]
- Cabras, T.; Pisano, E.; Boi, R.; Olianas, A.; Manconi, B.; Inzitari, R.; Fanali, C.; Giardina, B.; Castagnola, M.; Messana, I. Age-Dependent Modifications of the Human Salivary Secretory Protein Complex. J. Proteome Res. 2009, 8, 4126–4134. [Google Scholar] [CrossRef]
- Castagnola, M.; Inzitari, R.; Fanali, C.; Iavarone, F.; Vitali, A.; Desiderio, C.; Messana, I. The surprising composition of the salivary proteome of preterm human newborn. Mol. Cell. Proteom. 2011, 10, M110.003467. [Google Scholar] [CrossRef]
- Morzel, M.; Palicki, O.; Chabanet, C.; Lucchi, G.; Ducoroy, P.; Chambon, C.; Nicklaus, S. Saliva electrophoretic protein profiles in infants: Changes with age and impact of teeth eruption and diet transition. Arch. Oral Biol. 2011, 56, 634–642. [Google Scholar] [CrossRef]
- Tabbara, N. Identification of the Salivary Proteome in Children Throughout the Course of Dental Eruption; The University of Western Ontario: London, Canada, 2013. [Google Scholar]
- Gill, J.K.; Kaur, M.; Kaur, K.; Goel, S. Salivary biomarkers as a diagnostic indicator-a brief review. J. Adv. Med. Dent. Sci. Res. 2017, 5, 87. [Google Scholar]
- Carpenter, G.H. The secretion, components, and properties of saliva. Annu. Rev. Food Sci. Technol. 2013, 4, 267–276. [Google Scholar] [CrossRef]
- Oudhoff, M.J.; Bolscher, J.G.M.; Nazmi, K.; Kalay, H.; Hof, W.V.; Amerongen, A.V.N.; Veerman, E.C.I. Histatins are the major wound-closure stimulating factors in human saliva as identified in a cell culture assay. FASEB J. 2008, 22, 3805–3812. [Google Scholar] [CrossRef]
- Oudhoff, M.J.; Kroeze, K.L.; Nazmi, K.; van den Keijbus, P.A.; van’t Hof, W.; Fernandez-Borja, M.; Veerman, E.C. Structure-activity analysis of histatin, a potent wound healing peptide from human saliva: Cyclization of histatin potentiates molar activity 1000-fold. FASEB J. 2009, 23, 3928–3935. [Google Scholar] [CrossRef]
- Morzel, M.; Jeannin, A.; Lucchi, G.; Truntzer, C.; Pecqueur, D.; Nicklaus, S.; Chambon, C.; Ducoroy, P. Human infant saliva peptidome is modified with age and diet transition. J. Proteom. 2012, 75, 3665–3673. [Google Scholar] [CrossRef]
- Bobek, L.A.; Levine, M.J. Cystatins—Inhibitors of cysteine proteinases. Crit. Rev. Oral Biol. Med. 1992, 3, 307–332. [Google Scholar] [CrossRef]
- Dickinson, D.; Thiesse, M.; Hicks, M. Expression of Type 2 Cystatin Genes CST1-CST5 in Adult Human Tissues and the Developing Submandibular Gland. DNA Cell Biol. 2002, 21, 47–65. [Google Scholar] [CrossRef]
- Katsukawa, H.; Ninomiya, Y. Capsaicin Induces Cystatin S-like Substances in Submandibular Saliva of the Rat. J. Dent. Res. 1999, 78, 1609–1616. [Google Scholar] [CrossRef]
- Fábián, T.K.; Hermann, P.; Beck, A.; Fejérdy, P.; Fábián, G. Salivary Defense Proteins: Their Network and Role in Innate and Acquired Oral Immunity. Int. J. Mol. Sci. 2012, 13, 4295–4320. [Google Scholar] [CrossRef]
- Gibbons, R.J.; Hay, D.I.; Schlesinger, D.H. Delineation of a segment of adsorbed salivary acidic proline-rich proteins which promotes adhesion of Streptococcus gordonii to apatitic surfaces. Infect. Immun. 1991, 59, 2948–2954. [Google Scholar] [CrossRef]
- Böttcher, M.F.; Häggström, P.; Björkstén, B.; Jenmalm, M. Total and allergen-specific immunoglobulin A levels in saliva in relation to the development of allergy in infants up to 2 years of age. Clin. Exp. Allergy 2002, 32, 1293–1298. [Google Scholar] [CrossRef]
- Wan, A.K.L.; Seow, W.K.; Purdie, D.M.; Bird, P.S.; Walsh, L.; Tudehope, D.I. Immunoglobulins in saliva of preterm and full-term infants. A longitudinal study from 0–18 months of age. Oral Microbiol. Immunol. 2003, 18, 72–78. [Google Scholar] [CrossRef]
- Gleeson, M.; Cripps, A.W. Development of mucosal immunity in the first year of life and relationship to sudden infant death syndrome. FEMS Immunol. Med. Microbiol. 2004, 42, 21–33. [Google Scholar] [CrossRef]
- Bellavia, S.; Moreno, J.; Sanz, E.; Picas, E.I.; Blanco, A. α-Amylase activity of human neonate and adult saliva. Arch. Oral Biol. 1979, 24, 117–121. [Google Scholar] [CrossRef]
- Ruhl, S.; Rayment, S.A.; Schmalz, G.; Hiller, K.-A.; Troxler, R.F. Proteins in Whole Saliva during the First Year of Infancy. J. Dent. Res. 2005, 84, 29–34. [Google Scholar] [CrossRef]
- Janiani, P.; Ravindran, V. Comparative evaluation of the antimicrobial effects of probiotic milk and probiotic powder on the salivary Streptococcus mutans counts and the plaque scores in children aged 3–6 years: A randomized controlled trial. Dent. Med. Probl. 2022, 59, 99–104. [Google Scholar] [CrossRef]
- De Oliveira, R.; Navas, E.; Duran, C.; Pinto, M.; Gutierrez, J.; Eblen-Zajjur, A. Aging related changes in mixed basal saliva concentration of sodium, potassium and chloride in healthy non medicated humans. Curr. Aging Sci. 2014, 7, 110–114. [Google Scholar] [CrossRef]
- Castagnola, M.; Cabras, T.; Vitali, A.; Sanna, M.T.; Messana, I. Biotechnological implications of the salivary proteome. Trends Biotechnol. 2011, 29, 409–418. [Google Scholar] [CrossRef]
- Sarvaiya, B.; Mehta, D.; Singh, V.; Arora, R.; Bhayya, D.; Singh, D. Comparison of relationship between salivary electrolyte levels and dental caries in children with Down syndrome. J. Nat. Sci. Biol. Med. 2015, 6, 144–148. [Google Scholar] [CrossRef]
- Rodrigues, V.P.; Franco, M.M.; Marques, C.P.; de Carvalho, R.C.; Leite, S.A.; Pereira, A.L.; Benatti, B.B. Salivary levels of calcium, phosphorus, potassium, albumin and correlation with serum biomarkers in hemodialysis patients. Arch. Oral Biol. 2016, 62, 58–63. [Google Scholar] [CrossRef]
- Shirzaii, M.; Heidari, F. Evaluation chemical composition of unstimulated saliva, in patients with type I diabetes mellitus. Zahedan J. Res. Med. Sci. 2013, 15, 15–18. [Google Scholar]
- Bang, J.; Cimasoni, G.; Rosenbusch, C.; Duckert, A. Sodium, Potassium and Calcium Contents of Crevicular Exudate: Their Relations to Gingivitis and Periodontitis. J. Periodontol. 1973, 44, 770–774. [Google Scholar] [CrossRef]

| Variable | Age (Month) | Weight (kg) | Gender | Total (%) | ||
|---|---|---|---|---|---|---|
| Group | Mean ± Standard Deviation | Mean ± Standard Deviation | Male Number (%) | Female Number (%) | ||
| A | 5.17 ± 6.16 | 6.59 ± 8.59 | 25 (51) | 24 (49) | 49 (100) | |
| B | 7.16 ± 14.07 | 1.95 ± 10.26 | 32 (60.4) | 21 (39.6) | 53 (100) | |
| C | 8.33 ± 42.11 | 2.19 ± 14.17 | 18 (40) | 27 (60) | 45 (100) | |
| Clinical Signs and Symptoms | Number (%) |
|---|---|
| Gastrointestinal complications | 24 (46.15) |
| Gingival swelling or redness | 27 (51.92) |
| Perioral redness | 8 (15.38) |
| Irritability | 42 (80.76) |
| Hyper-salivation | 45 (86.53) |
| Putting hand in the mouth | 50 (96.15) |
| Skin rashes | 4 (7.69) |
| Malaise | 16 (30.76) |
| Fever | 35 (67.30) |
| Molecular Weight (KD) | A | B | C | p-Value * |
|---|---|---|---|---|
| Mean ± Standard Deviation | Mean ± Standard Deviation | Mean ± Standard Deviation | ||
| <10 | 1228.80 ± 698.15 | 2181.35 ± 2021.60 | 548.79 ± 463.13 | <0.001 |
| 10 | 3082.02 ± 2201.19 | 2473.94 ± 1489.30 | 1541.47 ± 1455.47 | 0.261 |
| 15 | 5765.84 ± 6933.28 | 4821.13 ± 7565.93 | 3607.24 ± 6122.51 | 0.375 |
| 20–15 | 2910.68 ± 2313.71 | 3629.41 ± 4440.93 | 2174.24 ± 2486.53 | <0.001 |
| 30–20 | 9399.27 ± 15,960.54 | 10,672.66 ± 12,512.34 | 2143.05 ± 3643.56 | <0.001 |
| 40 | 1985.90 ± 1944.01 | 1684.75 ± 2431.67 | 1780.50 ± 2326.70 | 0.378 |
| 60–50 | 5010.35 ± 9048.58 | 3010.74 ± 6554.44 | 5547.18 ± 13,961.51 | <0.001 |
| 95–90 | 2776.19 ± 2962.21 | 2278.19 ± 2531.97 | 1921.05 ± 2001.25 | 0.169 |
| >130 | 1723.18 ± 774.50 | 1260.46 ± 725.84 | 651.98 ± 211.23 | 0.094 |
| Molecular Weight | Group | Mean | p-Value * |
|---|---|---|---|
| <10 | A vs. B | −1323.44 ± 306.42 | <0.001 |
| A vs. C | 235.02 ± 327.96 | 1 | |
| B vs. C | 1558.46 ± 323.68 | <0.001 | |
| 20–15 | A vs. B | −2127.21 ± 602.27 | 0.002 |
| A vs. C | −172.81 ± 644.61 | 1 | |
| B vs. C | 1954.39 ± 436.20 | 0.008 | |
| 30–20 | A vs. B | 3448.20 ± 1714.10 | 0.139 |
| A vs. C | 12,316.98 ± 1834.60 | <0.001 | |
| B vs. C | 8868.78 ± 1810.66 | <0.001 | |
| 50–60 | A vs. B | 2494.14 ± 907.53 | 0.020 |
| A vs. C | −4912.93 ± 971.33 | <0.001 | |
| B vs. C | −7407.07 ± 958.65 | <0.001 |
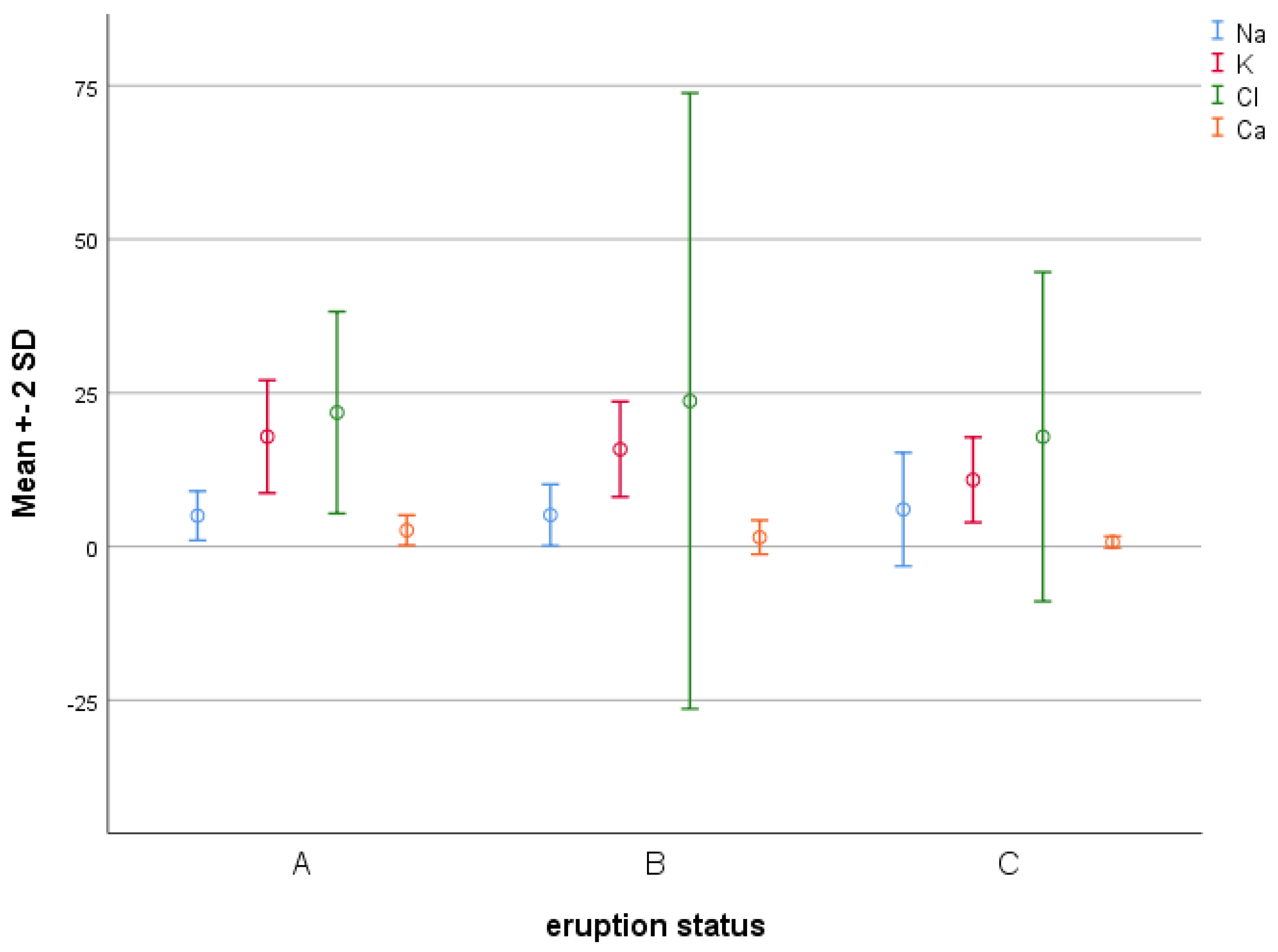
| Electrolyte | A | B | C | p-Value * |
|---|---|---|---|---|
| Mean ± Standard Deviation | Mean ± Standard Deviation | Mean ± Standard Deviation | ||
| Sodium | 2.15 ± 4.81 | 2.53 ± 5.14 | 4.58 ± 6.16 | 0.114 |
| Potassium | 4.13 ± 16.90 | 3.88 ± 16.01 | 3.79 ± 11.10 | <0.001 |
| Chloride | 8.06 ± 21.21 | 24.55 ± 23.60 | 13.25 ± 17.45 | 0.22 |
| Calcium | 1.22 ± 2.64 | 1.38 ± 1.49 | 0.46 ± 0.71 | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ahmadian, M.; Maleki Kambakhsh, S.; Einollahi, N.; Babazadeh, S.; Tofangchiha, M.; D’Amato, G.; Patini, R. Salivary Protein and Electrolyte Profiles during Primary Teeth Eruption: A Cross-Sectional Study. Diagnostics 2023, 13, 1335. https://doi.org/10.3390/diagnostics13071335
Ahmadian M, Maleki Kambakhsh S, Einollahi N, Babazadeh S, Tofangchiha M, D’Amato G, Patini R. Salivary Protein and Electrolyte Profiles during Primary Teeth Eruption: A Cross-Sectional Study. Diagnostics. 2023; 13(7):1335. https://doi.org/10.3390/diagnostics13071335
Chicago/Turabian StyleAhmadian, Mina, Sara Maleki Kambakhsh, Nahid Einollahi, Saber Babazadeh, Maryam Tofangchiha, Giuseppe D’Amato, and Romeo Patini. 2023. "Salivary Protein and Electrolyte Profiles during Primary Teeth Eruption: A Cross-Sectional Study" Diagnostics 13, no. 7: 1335. https://doi.org/10.3390/diagnostics13071335
APA StyleAhmadian, M., Maleki Kambakhsh, S., Einollahi, N., Babazadeh, S., Tofangchiha, M., D’Amato, G., & Patini, R. (2023). Salivary Protein and Electrolyte Profiles during Primary Teeth Eruption: A Cross-Sectional Study. Diagnostics, 13(7), 1335. https://doi.org/10.3390/diagnostics13071335







