Diagnosing Pain in Individuals with Intellectual and Developmental Disabilities: Current State and Novel Technological Solutions
Abstract
1. Introduction
2. Diagnosing Pain in Individuals with IDD
2.1. Complex Diagnosis of Pain in Individuals with IDD
2.2. Existing Pain Scales
- (a)
- Twenty-two adults diagnosed at a severe or profound IDD level were evaluated for pain behaviors presented before and during acute medical procedures assumed to produce pain and/or discomfort (procedures such as a toenail removal or a gastronomy-tube insertion).
- (b)
- The pain scores of a group of individuals with physical disabilities and painful chronic medical conditions were matched to the pain scores of a group with IDD alone (no-pain group; the scores of the former were found to be significantly higher); and
- (c)
- Eight adults diagnosed at a profound level of IDD with various concurrent medical conditions were assessed before and after pain-killer use.
2.3. Physiological Pain Assessment
3. New Technological Solutions Enabling Pain Assessment in Individuals with IDD
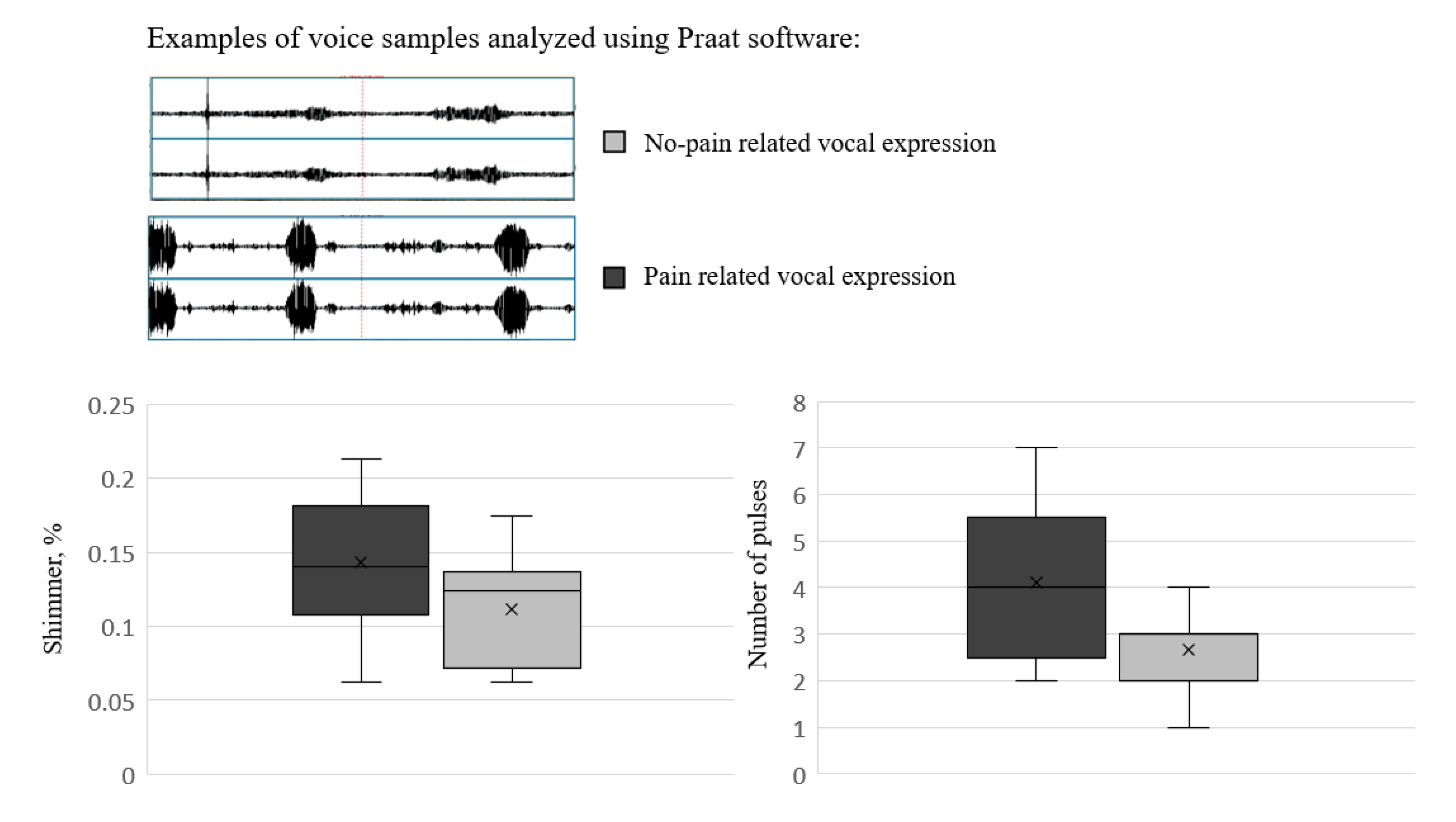
3.1. Assessing Pain Using Vocal Responses
3.2. Using Smart Shirts as a Base for Pain Assessment
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
| Name | FACS *# | ESPCP # | NCCPC # | PICIC # | PPP # | PADS * | NCAPC * |
|---|---|---|---|---|---|---|---|
| No. of items | 8 | 22; 10 | 30 | 6 | 20 | 18 | 18 |
| Source | Lachapelle et al., 1999 [10] | Giusiano et al., 1995 [37]; Collignon et al., 1997 [38] | McGrath et al., 1998 [15]; Breau et al., 2000 [40]; Breau et al., 2002 [42] | Stallard et al., 2001 [1]; Stallard et al., 2002 [26] | Hunt et al., 2004 [45] | Bodfish et al., 2001 [20]; Phan et al., 2005 [46] | Lotan et al., 2009 [49]; Lotan et al., 2010 [50] |
| Population | Adults with mild-moderate IDD | Adolescents with CP & IDD | Children with cognitive impairment | Non communicating children | Children with severe neurological and cognitive disability | Adults with severe and profound MR | Adults at all levels of IDD |
| Age range (mean) | (49.6) | 2–33 (16) | 6–29 (14.5); 3–9; 3–18 | 2 + (9.4); 2–21 (7.8) | 1–18 (9.9) | ----- | |
| N | 40 | 100 | 20; 24; 71 | 49; 34 | 140 | 22; 8 | 228 |
| Type of pain | Procedural | Not specified | Needle pain; long lasting pain | Non specific—severe pain | Not specified | Procedural; Chronic | Procedural; Chronic |
| Psycho-metric properties: | Have not been tested | Have not been tested | 0.78–0.82 | Have not been tested | 0.74–0.89 | 0.86 | 0.94–091 |
| (a) Reliability | |||||||
| (b) Internal consistency | 0.91–0.93 | 0.75–0.89 | ----- | 0.77 | |||
| (c) Validity | ----- | Construct validity | Content validity | Content validity Construct validity | |||
| (d) Specificity | 0.81–0.74 | 1.00 | ----- | ----- | |||
| (e) Sensitivity | 0.88–0.84 | 0.91 | ----- | ----- |
References
- Stallard, P.; Williams, L.; Lenton, S.; Velleman, R. Pain in cognitively impaired, non-communicating children. Arch. Dis. Child 2001, 85, 460–462. [Google Scholar] [CrossRef]
- Van Schrojenstein Lantman-De Valk, H.M.; Metsemakers, J.F.; Haveman, M.J.; Crebolder, H.F. Health problems in people with intellectual disability in general practice: A comparative study. Fam. Pract. 2000, 17, 405–407. [Google Scholar] [CrossRef] [PubMed]
- International Association for the Study of Pain—IASP. IASP Pain Terminology. 2010. Available online: https://www.iasp-pain.org/resources/terminology/ (accessed on 1 October 2022).
- International Association for the Study of Pain & Task Force on Taxonomy. Classification of Chronic Pain: Descriptions of Chronic Pain Syndromes and Definitions of Pain Terms, 2nd ed.; IASP Press: Seattle, WA, USA, 1994. [Google Scholar]
- Cousins, M.J.; Brennan, F.; Carr, D.B. Pain relief: A universal human right. Pain 2004, 112, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Regnard, C.; Mathews, D.; Gibson, L.; Clarke, C. Difficulties in identifying distress and its causes in people with severe communication problems. Int. J. Palliat. Nurs. 2003, 9, 173–176. [Google Scholar] [CrossRef] [PubMed]
- Reid, B.C.; Chenette, R.; Macek, M.D. Prevalence and predictors of untreated caries and oral pain among Special Olympic athletes. Spec. Care Dent. 2003, 23, 139–142. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, L.; Engel, J.M.; Jensen, M.P. Pain in persons with cerebral palsy. Arch. Phys. Med. Rehabil. 1999, 80, 1243–1246. [Google Scholar] [CrossRef]
- Breau, L.M.; Camfield, C.S.; McGrath, P.J.; Finley, G.A. The incidence of pain in children with severe cognitive impairments. Arch. Pediatr. Adolesc. Med. 2003, 157, 1219–1226. [Google Scholar] [CrossRef]
- LaChapelle, D.L.; Hadjistavropoulos, T.; Craig, K.D. Pain measurement in persons with intellectual disabilities. Clin. J. Pain 1999, 15, 13–23. [Google Scholar] [CrossRef]
- Malviya, S.; Voepel-Lewis, T.; Tait, A.R.; Merkel, S.; Lauer, A.; Munro, H.; Farley, F. Pain management in children with and without cognitive impairment following spine fusion surgery. Paediatr. Anaesth. 2001, 11, 453–458. [Google Scholar] [CrossRef]
- Oberlander, T.F.; O’Donnell, M.E.; Montgomery, C.J. Pain in children with significant neurological impairment. J. Dev. Behav. Pediatr. 1999, 20, 235–243. [Google Scholar] [CrossRef]
- Breau, L.M.; Camfield, C.S.; McGrath, P.J.; Finley, G.A. Risk factors for pain in children with severe cognitive impairments. Dev. Med. Child Neurol. 2004, 46, 364–371. [Google Scholar] [CrossRef] [PubMed]
- Mafrica, F.; Schifilliti, D.; Fodale, V. Pain in Down’s syndrome. Sci. World J. 2006, 6, 140–147. [Google Scholar] [CrossRef]
- McGrath, P.J.; Rosmus, C.; Camfield, C.; Campbell, M.A.; Hennigar, A.W. Behaviours caregivers use to determine pain in non-verbal, cognitively impaired individuals. Dev. Med. Child Neurol. 1998, 40, 340–343. [Google Scholar] [PubMed]
- Carr, E.G.; Owen-Deschryver, J.S. Physical illness, pain, and problem behavior in minimally verbal people with developmental disabilities. J. Autism. Dev. Disord 2007, 37, 413–424. [Google Scholar] [CrossRef]
- De Lissovoy, V. Head banging in early childhood. Child Dev. 1982, 33, 43–56. [Google Scholar] [CrossRef]
- Clements, J. “‘I can’t explain challenging behaviour’’: Towards a shared conceptual framework. Clin. Psychol. Forum 1992, 39, 29–37. [Google Scholar] [CrossRef]
- Bosch, J.; Van Dyke, D.C.; Smith, S.M.; Poulton, S. Role of medical conditions in the exacerbation of self-injurious behavior: An exploratory study. Ment. Retard. 1997, 35, 124–130. [Google Scholar] [CrossRef]
- Bodfish, J.W.; Harper, V.N.; Deacon, J.R.; Symons, F.J. Identifying and Measuring Pain in Persons with Developmental Disabilities: A Manual for the Pain and Discomfort Scale Morganton; Western Carolina Center: Morganton, NC, USA, 2001. [Google Scholar]
- Mason, J.; Scior, K. Diagnostic Overshdowing amongst clinicians working with people with intellectual disabilities in the UK. J. Appl. Res. Intellect. Disabil. 2004, 17, 75–90. [Google Scholar] [CrossRef]
- Carter, B.; McArthur, E.; Cunliffe, M. Dealing with uncertainty: Parental assessment of pain in their children with profound special needs. J. Adv. Nurs. 2002, 38, 449–457. [Google Scholar] [CrossRef]
- Donovan, J. Learning disability nurses’ experiences of being with clients who may be in pain. J. Adv. Nurs. 2002, 38, 458–466. [Google Scholar] [CrossRef]
- Fanurik, D.; Koh, J.L.; Schmitz, M.L.; Harrison, R.D.; Roberson, P.K.; Killebrew, P. Pain assessment and treatment in children with cognitive impairment: A survey of nurses’ and physicians’ beliefs. Clin. J. Pain 1999, 15, 304–312. [Google Scholar] [CrossRef] [PubMed]
- Oberlander, T.F.; O’Donnell, M.E. Beliefs about pain among professionals working with children with significant neurologic impairment. Dev. Med. Child Neurol. 2001, 43, 138–140. [Google Scholar] [CrossRef] [PubMed]
- Stallard, P.; Williams, L.; Velleman, R.; Lenton, S.; McGrath, P.J.; Taylor, G. The development and evaluation of the pain indicator for communicately impaired children (PICIC). Pain 2002, 1–2, 149. [Google Scholar]
- Ekman, P.; Friesen, W.V. Investigator’s Guide to the Facial Action Coding System; Consulting Psychologists Press: Palo Alto, CA, USA, 1978. [Google Scholar]
- Craig, K.D.; Grunau, R.V.E. Judgement of pain in newborns: Facial activity and cry as determinants. Can. J. Behav. Sci. 1988, 20, 442–451. [Google Scholar] [CrossRef]
- Craig, K.D. The facial expression of pain. In Handbook of Pain Assessment; Turk, D.C., Melzack, R., Eds.; Guilford: New York, NY, USA, 1992; pp. 257–276. [Google Scholar]
- Craig, K.D.; Hyde, S.A.; Patrick, C.J. Genuine, suppressed and faked facial behavior during exacerbation of chronic low back pain. Pain 1991, 46, 161–171. [Google Scholar] [CrossRef]
- Craig, K.D.; Korol, C.T.; Pillai, R.R. Challenges of judging pain in vulnerable infants. Clin. Perinatol. 2002, 29, 445–457. [Google Scholar] [CrossRef]
- Prkachin, K.M.; Berzins, S.; Mercer, S.R. Encoding and decoding of pain expressions: A judgement study. Pain 1994, 58, 253–259. [Google Scholar] [CrossRef]
- Hadjistavropoulos, T.; Craig, K.D.; Martin, N. Towards a research outcome measure of pain in frail elderly in chronic care. Pain Clin. 1997, 10, 71–90. [Google Scholar]
- Hurley, B.A.C.; Volier, B.J.; Harnahan, P.A. Assessment of discomfort in advanced Alzheimer patients. Res. Nurs. Health 1992, 15, 369–377. [Google Scholar] [CrossRef]
- Chambers, C.T.; Cassidy, K.L.; McGrath, P.J.; Gilbert, C.A.; Craig, K.D. Child Facial Coding System: A Manual; Dalhousie University: Halifax, NS, Canada; University of British Columbia: Vancouver, BC, Canada, 1996. [Google Scholar]
- Breau, L.M.; Finley, G.A.; Camfield, C.S.; McGrath, P.J. Facial expression of pain in children with intellectual disabilities following surgery. J. Pain Manag. 2009, 2, 51–62. [Google Scholar]
- Giusiano, B.; Jimeno, M.T.; Collignon, P.; Chau, Y. Utilization of a neural network in the elaboration of an evaluation scale for pain in cerebral palsy. Methods Inf. Med. 1995, 34, 498–502. [Google Scholar]
- Collignon, P.; Giusiano, B.; Boutin, A.M.; Combes, J.C. Utilisation d’une echelle d’heteroevaluation de la douleur chez le sujet severement polyhandicape. Doul. Analg. 1997, 10, 27–32. [Google Scholar] [CrossRef]
- Collignon, P.; Giusiano, B. Validation of a pain evaluation scale for patients with severe cerebral palsy. Eur. J. Pain 2001, 5, 433–442. [Google Scholar] [CrossRef] [PubMed]
- Breau, L.M.; McGrath, P.J.; Camfield, C.; Rosmus, C.; Finley, G.A. Preliminary validation of an observational pain checklist for persons with cognitive impairments and inability to communicate verbally. Dev. Med. Child Neurol. 2000, 42, 609–616. [Google Scholar] [CrossRef] [PubMed]
- Breau, L.M.; Finley, G.A.; McGrath, P.J.; Camfield, C.S. Validation of the Non-communicating Children’s Pain Checklist-Postoperative Version. Anesthesiology 2002, 96, 528–535. [Google Scholar] [CrossRef] [PubMed]
- Breau, L.M.; McGrath, P.J.; Camfield, C.S.; Finley, G.A. Psychometric properties of the non-communicating children’s pain checklist-revised. Pain 2002, 99, 349–357. [Google Scholar] [CrossRef]
- Breau, L.; Camfield, C.; Camfield, P. Development and initial validation of the Batten’s Observational Pain Scale: A preliminary study. J. Pain Manag. 2010, 3, 283–292. [Google Scholar]
- Burkitt, C.; Breau, L.M.; Salsman, S.; Sarsfield-Turner, T.; Mullan, R. Pilot Study of the Feasibility of the Non-Communicating Children’s Pain Checklist Revised for Pain Assessment for Adults with Intellectual Disabilities. J. Pain Manag. 2009, 2, 37–49. [Google Scholar]
- Hunt, A.; Goldman, A.; Seers, K.; Crichton, N.; Mastroyannopoulou, K.; Moffat, V.; Oulton, K.; Brady, M. Clinical validation of the paediatric pain profile. Dev. Med. Child Neurol. 2004, 46, 9–18. [Google Scholar] [CrossRef]
- Phan, A.; Edwards, C.L.; Robinson, E.L. The assessment of pain and discomfort in individuals with mental retardation. Res. Dev. Disabil. 2005, 26, 433–439. [Google Scholar] [CrossRef] [PubMed]
- Defrin, R.; Lotan, M.; Pick, C.G. The evaluation of acute pain in individuals with cognitive impairment: A differential effect of the level of impairment. Pain 2006, 124, 312–320. [Google Scholar] [CrossRef] [PubMed]
- Lotan, M.; Ljunggren, E.A.; Johnsen, T.B.; Defrin, R.; Pick, C.G.; Strand, L.I. A modified version of the non-communicating children pain checklist-revised, adapted to adults with intellectual and developmental disabilities: Sensitivity to pain and internal consistency. J. Pain 2009, 10, 398–407. [Google Scholar] [CrossRef]
- Lotan, M.; Moe-Nilssen, R.; Ljunggren, A.E.; Strand, L.I. Reliability of the Non-Communicating Adult Pain Checklist (NCAPC), assessed by different groups of health workers. Res. Dev. Disabil. 2009, 30, 735–745. [Google Scholar] [CrossRef] [PubMed]
- Lotan, M.; Moe-Nilssen, R.; Ljunggren, A.E.; Strand, L.I. Measurement properties of the Non-communicating Adult Pain Checklist (NCAPC): A pain scale for adults with Intellectual and Developmental Disabilities, scored in a clinical setting. Res. Dev. Disabil. 2010, 31, 367–375. [Google Scholar] [CrossRef] [PubMed]
- Lotan, M.; Strand, L.I.; Klave, A. A model for pain behavior in individuals with intellectual and developmental disabilities. Res. Dev. Disabil. 2012, 33, 1984–1989. [Google Scholar] [CrossRef] [PubMed]
- Blomqvist, K.; Hallberg, I.R. Pain in older adults living in sheltered accommodation–agreement between assessments by older adults and staff. J. Clin. Nurs. 1999, 8, 159–169. [Google Scholar] [CrossRef]
- Gunnar, M.R.; Porter, F.L.; Wolf, C.M.; Rigatuso, J.; Larson, M.C. Neonatal stress reactivity: Predictions to later emotional temperament. Child Dev. 1995, 66, 1–13. [Google Scholar] [CrossRef]
- Cohen, L.L.; Blount, R.L.; Cohen, R.J.; Schaen, E.R.; Zaff, J.F. Comparative study of distraction versus topical anesthesia for pediatric pain management during immunizations. Health Psychol. 1999, 18, 591. [Google Scholar] [CrossRef]
- Cordova, F.C.; Marchetti, N. Noninvasive Monitoring in the Intensive Care Unit. In Critical Care Study Guide; Criner, G., Barnette, R., D’Alonzo, G., Eds.; Springer: New York, NY, USA, 2010. [Google Scholar] [CrossRef]
- Yamaguchi, M.; Takeda, K.; Onishi, M.; Deguchi, M.; Higashi, T. Non-verbal communication method based on a biochemical marker for people with severe motor and intellectual disabilities. J. Int. Med. Res. 2006, 34, 30–41. [Google Scholar] [CrossRef]
- Zautra, A.J.; Fasman, R.; Davis, M.C.; Craig, A.D.B. The effects of slow breathing on affective responses to pain stimuli: An experimental study. Pain 2010, 149, 12–18. [Google Scholar] [CrossRef]
- Stevens, B.J.; Johnston, C.C.; Horton, L. Factors that influence the behavioral pain responses of premature infants. Pain 1994, 59, 101–109. [Google Scholar] [CrossRef] [PubMed]
- Fuller, B.F.; Roberts, J.E.; McKay, S. Acoustical analysis of maternal sounds during the second stage of labor. Appl. Nurs. Res. 1993, 6, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Herr, K.; Coyne, P.J.; McCaffery, M.; Manworren, R.; Merkel, S. Pain assessment in the patient unable to self–report: Position statement with clinical practice recommendations. Pain Manag. Nurs. 2011, 12, 230–250. [Google Scholar] [CrossRef] [PubMed]
- van Iersel, T.; Timmerman, D.; Mullie, A. Introduction of a pain scale for palliative care patients with cognitive impairment. Int. J. Palliat. Nurs. 2006, 12, 54–59. [Google Scholar] [CrossRef]
- Icht, M.; Wiznitser Ressis-tal, H.; Lotan, M. Can the vocal expression of intellectually disabled individuals be used as a pain indicator? Initial findings supporting a possible novice assessment method. Front. Psychol. 2021, 12, 2926. [Google Scholar] [CrossRef]
- Banaee, H.; Ahmed, M.U.; Loutfi, A. Data mining for wearable sensors in health monitoring systems: A review of recent trends and challenges. Sensors 2013, 13, 17472–17500. [Google Scholar]
- Koo, S.H.; Gaul, K.; Rivera, S.; Pan, T.; Fong, D. Wearable technology design for autism spectrum disorders. Arch. Des. Res. 2018, 31, 37–55. [Google Scholar] [CrossRef]
- Taj-Eldin, M.; Ryan, C.; O’Flynn, B.; Galvin, P. A Review of Wearable Solutions for Physiological and Emotional Monitoring for Use by People with Autism Spectrum Disorder and Their Caregivers. Sensors 2018, 18, 4271. [Google Scholar] [CrossRef]
- Black, M.H.; Milbourn, B.; Chen, N.T.M.; McGarry, S.; Wali, F.; Ho, A.S.V.; Lee, M.; Bölte, S.; Falkmer, T.; Girdler, S. The use of wearable technology to measure and support abilities, disabilities and functional skills in autistic youth: A scoping review. Scand. J. Child Adolesc. Psychiatry Psychol. 2020, 8, 48–69. [Google Scholar] [CrossRef]
- Simantiraki, O.; Giannakakis, G.; Pampouchidou, A.; Tsiknakis, M. Stress detection from speech using spectral slope measurements. In Pervasive Computing Paradigms for Mental Health; Springer: Cham, Switzerland, 2016; pp. 41–50. [Google Scholar]
- Chen, J.; Abbod, M.; Shieh, J.S. Pain and stress detection using wearable sensors and devices—A review. Sensors 2021, 21, 1030. [Google Scholar] [CrossRef]
- Breau, L.M.; Camfield, C.S.; McGrath, P.J.; Finley, G.A. Pain’s impact on adaptive functioning. J. Intellect. Disabil. Res. 2007, 51, 125–134. [Google Scholar] [CrossRef] [PubMed]
- Breau, L.M.; Camfield, C.S.; Symons, F.J.; Bodfish, J.W.; Mackay, A.; Finley, G.A.; McGrath, P.J. Relation between pain and self-injurious behavior in nonverbal children with severe cognitive impairments. J. Pediatr. 2003, 142, 498–503. [Google Scholar] [CrossRef] [PubMed]
- Mahon, M.; Kibirige, M.S. Patterns of admissions for children with special needs to the paediatric assessment unit. Arch Dis. Child 2004, 89, 165–169. [Google Scholar] [CrossRef] [PubMed]
- Gauthier, J.C.; Finley, G.A.; McGrath, P.J. Children’s self-report of postoperative pain intensity and treatment threshold: Determining the adequacy of medication. Clin. J. Pain 1998, 14, 116–120. [Google Scholar] [CrossRef] [PubMed]
- Breau, L.M. A bio-ecological approach to pediatric pain assessment. J. Pain Manag. 2008, 1, 247–255. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lotan, M.; Icht, M. Diagnosing Pain in Individuals with Intellectual and Developmental Disabilities: Current State and Novel Technological Solutions. Diagnostics 2023, 13, 401. https://doi.org/10.3390/diagnostics13030401
Lotan M, Icht M. Diagnosing Pain in Individuals with Intellectual and Developmental Disabilities: Current State and Novel Technological Solutions. Diagnostics. 2023; 13(3):401. https://doi.org/10.3390/diagnostics13030401
Chicago/Turabian StyleLotan, Meir, and Michal Icht. 2023. "Diagnosing Pain in Individuals with Intellectual and Developmental Disabilities: Current State and Novel Technological Solutions" Diagnostics 13, no. 3: 401. https://doi.org/10.3390/diagnostics13030401
APA StyleLotan, M., & Icht, M. (2023). Diagnosing Pain in Individuals with Intellectual and Developmental Disabilities: Current State and Novel Technological Solutions. Diagnostics, 13(3), 401. https://doi.org/10.3390/diagnostics13030401






