Frailty Network in an Acute Care Setting: The New Perspective for Frail Older People
Abstract
:1. Introduction
2. Methods
2.1. The Frailty Unit: An Emergency Department Geriatrician
2.2. The Geriatric Assessment
2.3. Discharge Plan
3. Results and Discussion
3.1. The Frailty Unit Experience
3.2. From the Emergency Department to a ‘New’ Geriatric Ward: The Functional-Cognitive Unit
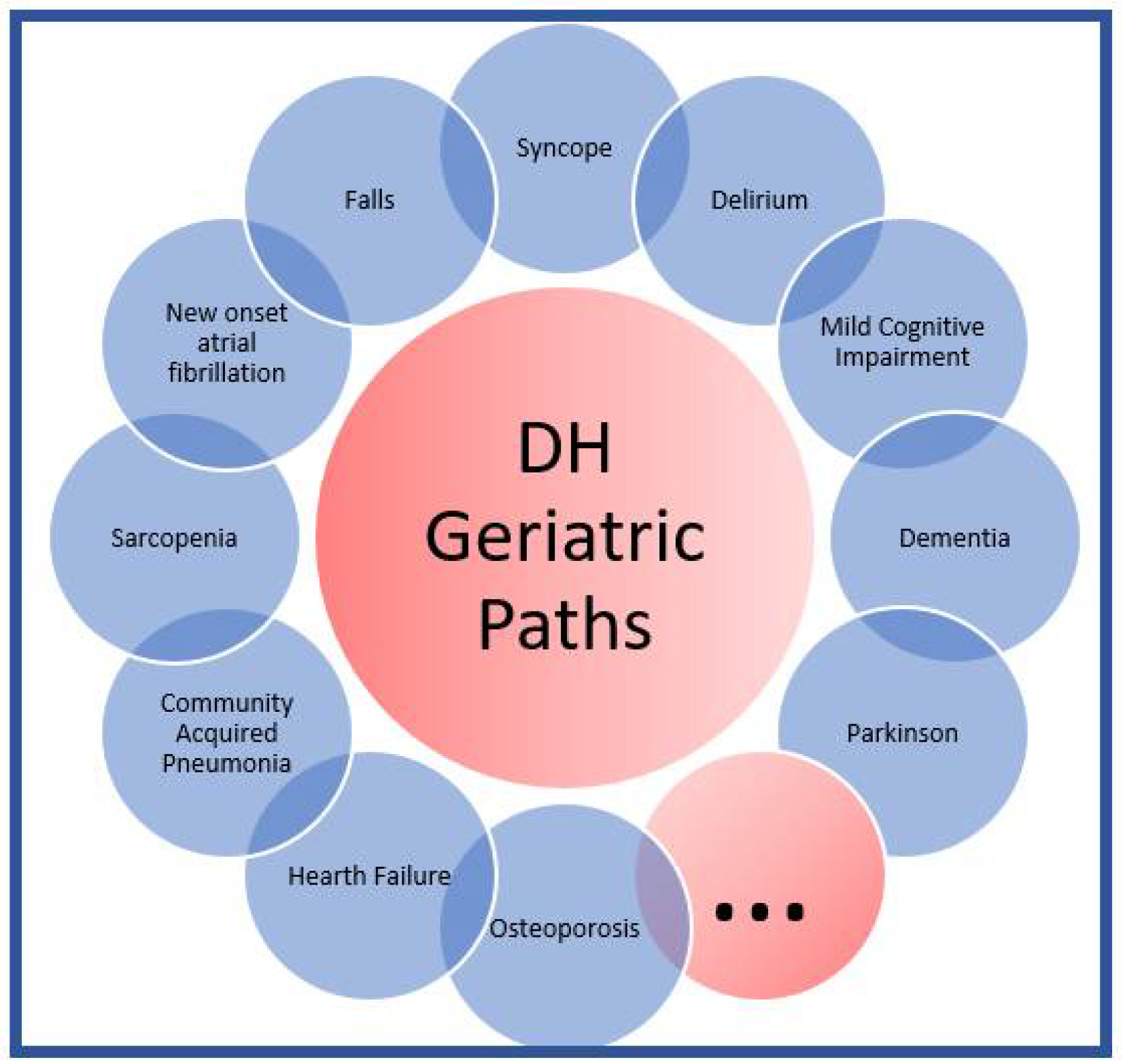
- based on the geriatric short stay observation model, patients with a clinical path or continuity of care already set up for an assumed short-term hospitalization; in these patients, a short-term hospitalization is often necessary, but it is important to guarantee particular attention from a frailty point of view (for example, to prevent geriatric syndromes typical of hospitalization, such as delirium, or falls.).
- on the long-term care model, patients with a high degree of complexity or potential bed blockers; in these patients, the geriatric approach is fundamental in the treatment of acute cases, as are knowledge of the territory and the possible services supporting safe discharge.
- the patient must be a “frail older adult” according to the previously specified criteria, when geriatric expertise can ensure more appropriate care and discharge pathway
- the patient must have been admitted to a surgery or specialized medicine department (e.g., vascular diseases, endocrinology, nephrology, neurology.), but no longer requires the specialist expertise for which it was accessed (e.g., a patient who has already undergone surgery and needs to continue medical treatment and observation)
- the diagnostic process must have been completed and the specific therapeutic process must have started;
- the continuity of the territorial care process must have been defined or at least the need for it must have been identified
3.3. Frailty Evaluation from the Emergency Department to the Wards: The Interdepartmental Geriatrician
- -
- Clinical history including the reason for the hospitalization, the remote pathological history with an evaluation of active and previous comorbidities, the drug history, and the physiological anamnesis;
- -
- Multidimensional evaluation that can make use of second-level evaluation tools:
- Functional (ADL, IADL, Barthel Index) and cognitive status (spatial and temporal orientation, Six Item screener, MMSE, specific neuropsychological tests)
- State of supervision and delirium evaluation (RASS, CAM);
- -
- Evaluation of the presence of geriatric syndromes (delirium and agitation in dementia, functional deterioration, hypomobility syndrome, risk of falls, malnutrition, pressure injury, urinary incontinence);
- -
- Assessment of the social and family network;
- -
- Evaluation of the continuity of care outside the hospital;
- -
- Interview with the patient and family members.
3.4. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Arendts, G.; Reibel, T.; Codde, J.; Frankel, J. Can Transfers from Residential Aged Care Facilities to the Emergency Department Be Avoided through Improved Primary Care Services? Data from Qualitative Interviews. Australas. J. Ageing 2010, 29, 61–65. [Google Scholar] [CrossRef] [PubMed]
- Onder, G.; Giovannini, S.; Sganga, F.; Manes-Gravina, E.; Topinkova, E.; Finne-Soveri, H.; Garms-Homolová, V.; Declercq, A.; van der Roest, H.G.; Jónsson, P.V.; et al. Interactions between Drugs and Geriatric Syndromes in Nursing Home and Home Care: Results from Shelter and IBenC Projects. Aging Clin. Exp. Res. 2018, 30, 1015–1021. [Google Scholar] [CrossRef] [PubMed]
- Dwyer, R.; Stoelwinder, J.; Gabbe, B.; Lowthian, J. Unplanned Transfer to Emergency Departments for Frail Elderly Residents of Aged Care Facilities: A Review of Patient and Organizational Factors. J. Am. Med. Dir. Assoc. 2015, 16, 551–562. [Google Scholar] [CrossRef] [PubMed]
- Pines, J.M.; Mullins, P.M.; Cooper, J.K.; Feng, L.B.; Roth, K.E. National Trends in Emergency Department Use, Care Patterns, and Quality of Care of Older Adults in the United States. J. Am. Geriatr. Soc. 2013, 61, 12–17. [Google Scholar] [CrossRef]
- Šteinmiller, J.; Routasalo, P.; Suominen, T. Older People in the Emergency Department: A Literature Review. Int. J. Older People Nurs. 2015, 10, 284–305. [Google Scholar] [CrossRef]
- Coraci, D.; Fusco, A.; Frizziero, A.; Giovannini, S.; Biscotti, L.; Padua, L. Global Approaches for Global Challenges: The Possible Support of Rehabilitation in the Management of COVID-19. J. Med. Virol. 2020, 92, 1739–1740. [Google Scholar] [CrossRef] [Green Version]
- Onder, G.; Vetrano, D.L.; Villani, E.R.; Carfì, A.; lo Monaco, M.R.; Cipriani, M.C.; Manes Gravina, E.; Denkinger, M.; Pagano, F.; van der Roest, H.G.; et al. Deprescribing in Nursing Home Residents on Polypharmacy: Incidence and Associated Factors. J. Am. Med. Dir. Assoc. 2019, 20, 1116–1120. [Google Scholar] [CrossRef]
- Wallis, S.J.; Wall, J.; Biram, R.W.S.; Romero-Ortuno, R. Association of the Clinical Frailty Scale with Hospital Outcomes. QJM Int. J. Med. 2015, 108, 943–949. [Google Scholar] [CrossRef] [Green Version]
- Di Bari, M.; Balzi, D.; Roberts, A.T.; Barchielli, A.; Fumagalli, S.; Ungar, A.; Bandinelli, S.; de Alfieri, W.; Gabbani, L.; Marchionni, N. Prognostic Stratification of Older Persons Based on Simple Administrative Data: Development and Validation of the “Silver Code,” to Be Used in Emergency Department Triage. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2010, 65, 159–164. [Google Scholar] [CrossRef] [Green Version]
- Giovannini, S.; Onder, G.; Leeuwenburgh, C.; Carter, C.; Marzetti, E.; Russo, A.; Capoluongo, E.; Pahor, M.; Bernabei, R.; Landi, F. Myeloperoxidase Levels and Mortality in Frail Community-Living Elderly Individuals. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2010, 65A, 369–376. [Google Scholar] [CrossRef] [Green Version]
- Vetrano, D.L.; Villani, E.R.; Grande, G.; Giovannini, S.; Cipriani, M.C.; Manes-Gravina, E.; Bernabei, R.; Onder, G. Association of Polypharmacy With 1-Year Trajectories of Cognitive and Physical Function in Nursing Home Residents: Results from a Multicenter European Study. J. Am. Med. Dir. Assoc. 2018, 19, 710–713. [Google Scholar] [CrossRef] [PubMed]
- Giovannini, S.; Onder, G.; Lattanzio, F.; Bustacchini, S.; di Stefano, G.; Moresi, R.; Russo, A.; Bernabei, R.; Landi, F. Selenium Concentrations and Mortality Among Community-Dwelling Older Adults: Results from IlSIRENTE Study. J. Nutr. Health Aging 2018, 22, 608–612. [Google Scholar] [CrossRef] [PubMed]
- Giovannini, S.; Tamburrano, A.; Sganga, F.; Serra, M.L.; Loreti, C.; Coraci, D.; Padua, L.; Caliandro, P.; Zega, M.; Tafani, A.; et al. A New Model of Multidimensional Discharge Planning: Continuity of Care for Frail and Complex Inpatients. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 13009–13014. [Google Scholar] [CrossRef]
- Shenvi, C.; Kennedy, M.; Austin, C.A.; Wilson, M.P.; Gerardi, M.; Schneider, S. Managing Delirium and Agitation in the Older Emergency Department Patient: The ADEPT Tool. Ann. Emerg. Med. 2020, 75, 136–145. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lorenzi, M.; Bonassi, S.; Lorenzi, T.; Giovannini, S.; Bernabei, R.; Onder, G. A Review of Telomere Length in Sarcopenia and Frailty. Biogerontology 2018, 19, 209–221. [Google Scholar] [CrossRef]
- Giovannini, S.; van der Roest, H.G.; Carfì, A.; Finne-Soveri, H.; Garms-Homolová, V.; Declercq, A.; Jónsson, P.v.; van Hout, H.; Vetrano, D.L.; Gravina, E.M.; et al. Polypharmacy in Home Care in Europe: Cross-Sectional Data from the IBenC Study. Drugs Aging 2018, 35, 145–152. [Google Scholar] [CrossRef]
- Laudisio, A.; Giovannini, S.; Finamore, P.; Loreti, C.; Vannetti, F.; Coraci, D.; Incalzi, R.A.; Zuccalà, G.; Macchi, C.; Padua, L.; et al. Muscle Strength Is Related to Mental and Physical Quality of Life in the Oldest Old. Arch. Gerontol. Geriatr. 2020, 89, 104109. [Google Scholar] [CrossRef]
- Giovannini, S.; Macchi, C.; Liperoti, R.; Laudisio, A.; Coraci, D.; Loreti, C.; Vannetti, F.; Onder, G.; Padua, L.; Bonaccorsi, G.; et al. Association of Body Fat with Health-Related Quality of Life and Depression in Nonagenarians: The Mugello Study. J. Am. Med. Dir. Assoc. 2019, 20, 564–568. [Google Scholar] [CrossRef]
- Carfì, A.; Liperoti, R.; Fusco, D.; Giovannini, S.; Brandi, V.; Vetrano, D.L.; Meloni, E.; Mascia, D.; Villani, E.R.; Manes Gravina, E.; et al. Bone Mineral Density in Adults with Down Syndrome. Osteoporos. Int. 2017, 28, 2929–2934. [Google Scholar] [CrossRef]
- Giovannini, S.; Coraci, D.; di Caro, F.; Castelli, L.; Loreti, C.; Chicco, A.; Fiori, M.; Bellieni, A.; Gerardino, L.; Nigito, C.; et al. Prehabilitation and Heart Failure: Perspective in Primary Outcomes, a Randomized Controlled Trial. Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 6684–6690. [Google Scholar] [CrossRef]
- Keene, S.E.; Cameron-Comasco, L. Implementation of a geriatric emergency medicine assessment team decreases hospital length of stay. Am. J. Emerg. Med. 2022, 55, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Southerland, L.T.; Stephens, J.A.; Carpenter, C.R.; Mion, L.C.; Moffatt-Bruce, S.D.; Zachman, A.; Hill, M.; Caterino, J.M. Study protocol for IMAGE: Implementing multidisciplinary assessments for geriatric patients in an emergency department observation unit, a hybrid effectiveness/implementation study using the Consolidated Framework for Implementation Research. Implement. Sci. Commun. 2020, 25, 28. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Leahy, A.; McNamara, R.; Reddin, C.; Corey, G.; Carroll, I.; SOLAR Team; O’Neill, A.; Flannery, D.; Devlin, C.; Barry, L.; et al. The Impact of Frailty Screening of Older Adults with Multidisciplinary Assessment of Those at Risk during Emergency Hospital Attendance on the Quality, Safety and Cost-Effectiveness of Care (SOLAR): A Randomized Controlled Trial. Trials 2021, 22, 581. [Google Scholar] [CrossRef] [PubMed]


| Variable | All n 1191 | Discharged n 723 | Hospitalized n 468 | p |
|---|---|---|---|---|
| Age | 82 (74–87) | 81 (73–87) | 83 (76–86) | <0.001 |
| Sex (Male) Clinical Frailty Scale | 516 (45.1) 7 (5–8) | 317 (46.6) 6 (4–7) | 199 (42.8) 7 (6–8) | 0.202 <0.001 |
| Emergency Department Presentation | ||||
| Delirium | 135 (11.8) | 62 (9.1) | 73 (15.7) | <0.001 |
| Dyspnea | 251 (21.9) | 148 (21.8) | 103 (22.2) | 0.877 |
| Fever | 439 (38.3) | 266 (39.1) | 173 (37.2) | 0.513 |
| Chest pain | 50 (4.4) | 36 (5.1) | 15 (3.2) | 0.118 |
| Syncope | 107 (9.3) | 67 (9.9) | 40 (8.6) | 0.475 |
| Abdominal pain | 90 (7.9) | 56 (8.2) | 34 (7.3) | 0.569 |
| Diarrhea Constipation | 35 (3.1) 27 (2.4) | 18 (2.6) 15 (2.2) | 17 (3.7) 12 (2.6) | 0.330 0.681 |
| Dizziness | 19 (1.7) | 14 (2.1) | 5 (1.1) | 0.201 |
| Neurological symptoms | 68 (5.9) | 35 (5.1) | 33 (7.1) | 0.170 |
| Malaise/fatigue | 145 (12.7) | 87 (12.8) | 58 (12.5) | 0.873 |
| Clinical History | ||||
| Charlson Comorbidity Index | 4 (2–5) | 4 (3–5) | 3 (1–5) | <0.001 |
| Ischemic heart disease | 190 (16.6) | 123 (18.1) | 67 (14.4) | 0.100 |
| Congestive heart failure | 274 (23.9) | 129 (19.0) | 145 (31.2) | <0.001 |
| Peripheral vascular disease | 66 (5.8) | 6 (0.9) | 60 (12.9) | <0.001 |
| Previous stroke Dementia | 125 (10.9) 214 (18.7) | 36 (5.3) 58 (8.5) | 89 (19.1) 156 (33.5) | <0.001 <0.001 |
| COPD | 127 (11.1) | 56 (8.2) | 71 (15.3) | <0.001 |
| Diabetes | 204 (17.8) | 96 (14.1) | 108 (23.6) | <0.001 |
| Liver chronic disease | 36 (3.1) | 6 (0.9) | 30 (6.5) | <0.001 |
| Rheumatologic disease | 15 (1.3) | 6 (0.9) | 9 (1.9) | 0.124 |
| Chronic kidney disease | 134 (11.7) | 31 (4.6) | 103 (22.2) | <0.001 |
| Malignancy | 135 (11.8) | 41 (6.0) | 94 (20.2) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Salini, S.; Giovannini, S.; Covino, M.; Barillaro, C.; Acampora, N.; Gravina, E.M.; Loreti, C.; Damiano, F.P.; Franceschi, F.; Russo, A. Frailty Network in an Acute Care Setting: The New Perspective for Frail Older People. Diagnostics 2022, 12, 1228. https://doi.org/10.3390/diagnostics12051228
Salini S, Giovannini S, Covino M, Barillaro C, Acampora N, Gravina EM, Loreti C, Damiano FP, Franceschi F, Russo A. Frailty Network in an Acute Care Setting: The New Perspective for Frail Older People. Diagnostics. 2022; 12(5):1228. https://doi.org/10.3390/diagnostics12051228
Chicago/Turabian StyleSalini, Sara, Silvia Giovannini, Marcello Covino, Christian Barillaro, Nicola Acampora, Ester Manes Gravina, Claudia Loreti, Francesco Paolo Damiano, Francesco Franceschi, and Andrea Russo. 2022. "Frailty Network in an Acute Care Setting: The New Perspective for Frail Older People" Diagnostics 12, no. 5: 1228. https://doi.org/10.3390/diagnostics12051228
APA StyleSalini, S., Giovannini, S., Covino, M., Barillaro, C., Acampora, N., Gravina, E. M., Loreti, C., Damiano, F. P., Franceschi, F., & Russo, A. (2022). Frailty Network in an Acute Care Setting: The New Perspective for Frail Older People. Diagnostics, 12(5), 1228. https://doi.org/10.3390/diagnostics12051228








