Automated Final Lesion Segmentation in Posterior Circulation Acute Ischemic Stroke Using Deep Learning
Abstract
:1. Introduction
2. Materials and Methods
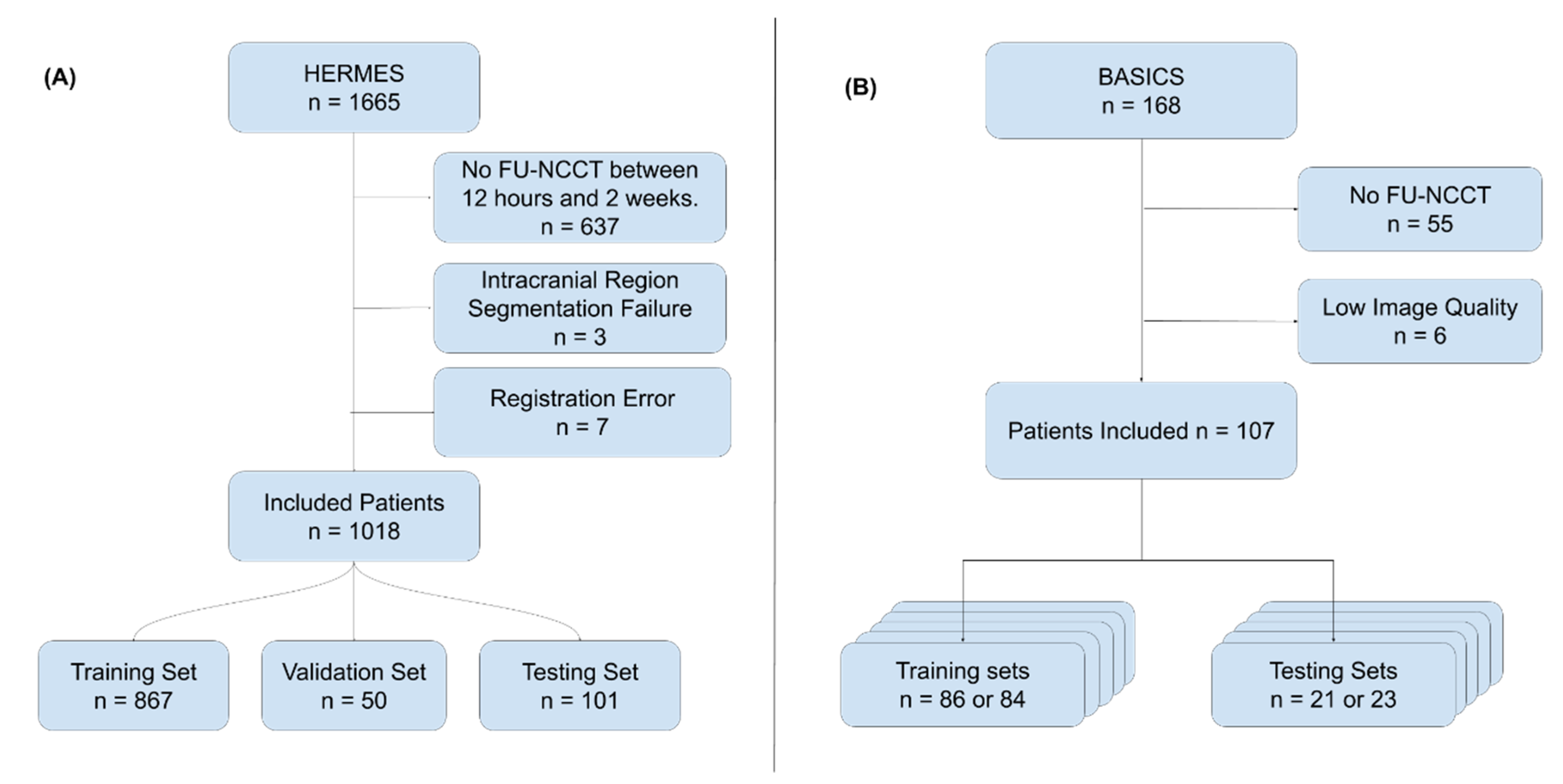
2.1. Patient and Image Data
2.2. Reference Segmentations
2.3. Preprocessing
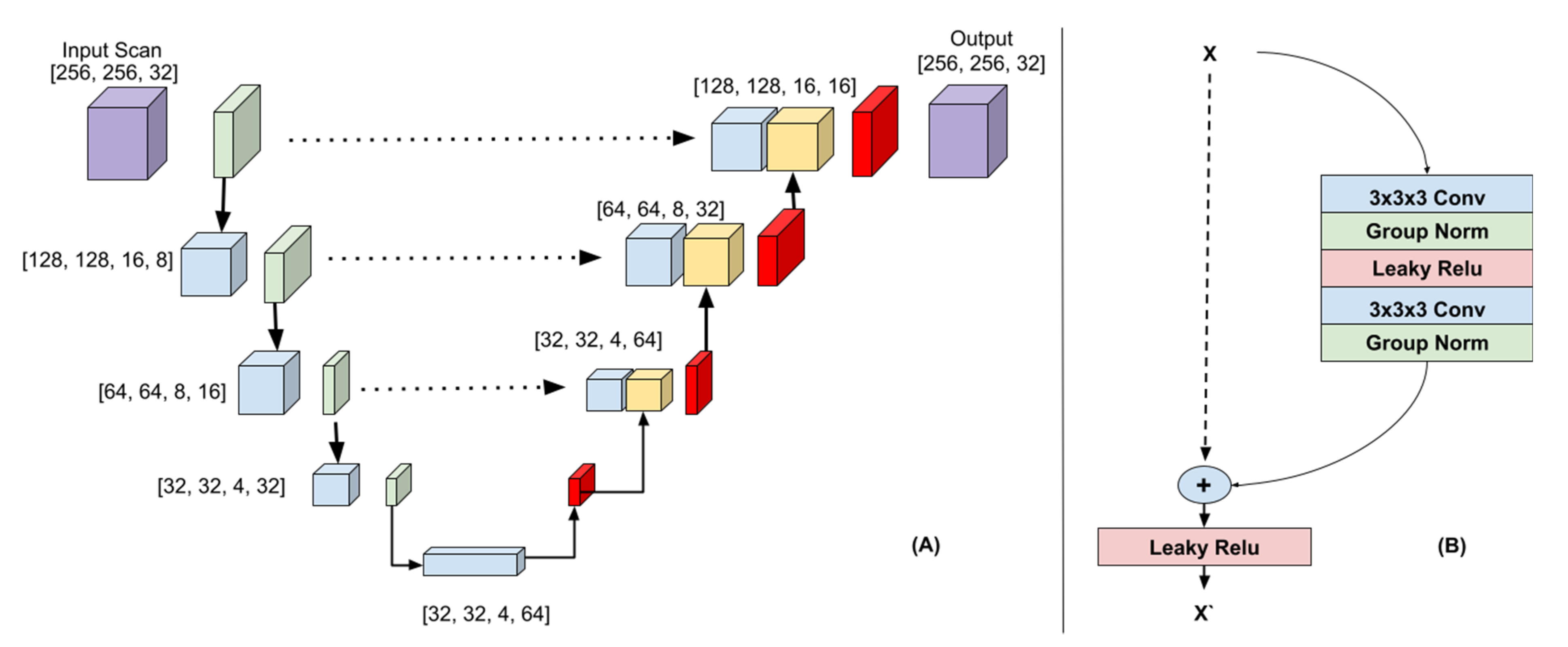
2.4. CNN for Automatic Posterior Circulation Lesion Segmentation
2.5. Experimental Setup
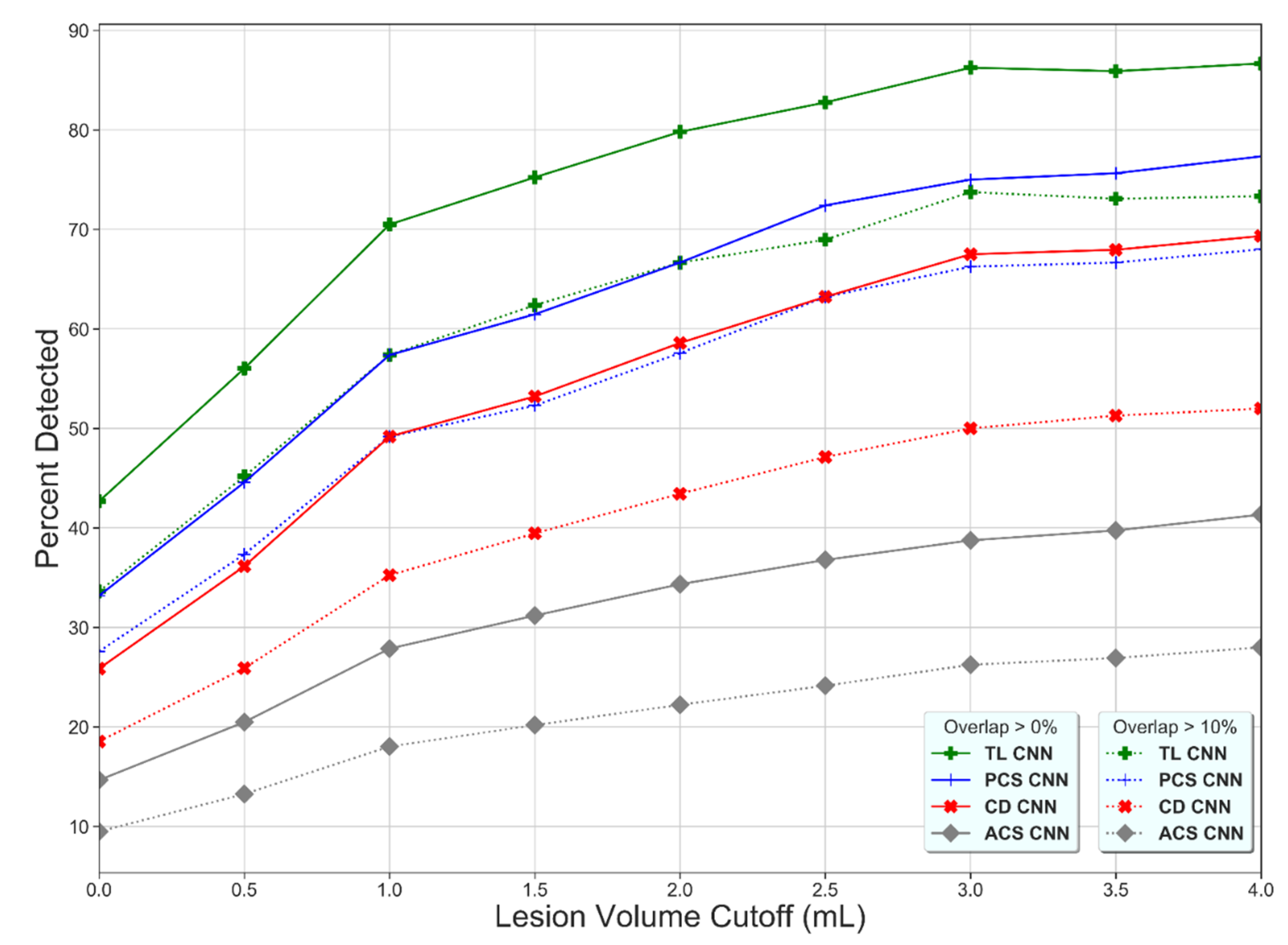
2.6. Evaluation
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Manufacturer | Model | Patients | Exposure Time (mS) | Exposure (mA) | Tube Current | kVp |
|---|---|---|---|---|---|---|
| Philips | iCT 256 | 29 | 1913 (IQR: 1025–1913) | 375 (IQR: 251–490) | 256 (IQR: 244–256) | 100 (IQR: 100–120) |
| GE | LightSpeed VCT | 17 | 1000 (IQR: 1000–2000) | 175 (IQR: 171–175) | 351 (IQR: 179–351) | 120 (IQR: 120–120) |
| SIEMENS | SOMATOM Definition Flash | 13 | 2000 (IQR: 2000–2000) | 340 (IQR: 285–430) | 172 (IQR: 143–229) | 120 (IQR: 100–120) |
| TOSHIBA | Aquilion | 11 | 750 (IQR: 750–750) | 187 (IQR: 187–225) | 250 (IQR: 250–300) | 120 (IQR: 120–120) |
| SIEMENS | Sensation 64 | 6 | 1000 (IQR: 1000–1000) | 380 (IQR: 380–380) | 352 (IQR: 323–380) | 120 (IQR: 120–120) |
| Philips | Brilliance 64 | 5 | 1678 (IQR: 1000–1678) | 351 (IQR: 250–351) | 209 (IQR: 200–209) | 120 (IQR: 120–120) |
| SIEMENS | SOMATOM Force | 4 | 2000 (IQR: 1750–2000) | 340 (IQR: 327–380) | 170 (IQR: 163.5–196) | 100 (IQR: 100–105) |
| SIEMENS | SOMATOM Definition AS+ | 4 | 1000 (IQR: 1000–1000) | 250 (IQR: 233–290) | 138 (IQR: 129–155) | 120 (IQR: 115–120) |
| Philips | IQon—Spectral CT | 4 | 1117 (IQR: 1117–1117) | 200 (IQR: 200–200) | 179 (IQR: 179–179) | 120 (IQR: 120–120) |
| Other | Various | 12 | 1000 (IQR: 1000–1000) | 260 (IQR: 158–353) | 260 (IQR: 220–325) | 120 (IQR: 120–120) |
| Lesion Location | Count/Total |
|---|---|
| No lesion | 15/107 |
| Left thalamus | 33/107 |
| Left cerebellum | 40/107 |
| Left PCA territory | 19/107 |
| Right thalamus | 26/107 |
| Right cerebellum | 40/107 |
| Right PCA territory | 19/107 |
| Midbrain | 34/107 |
| Pons | 46/107 |
| Other | 4/107 |
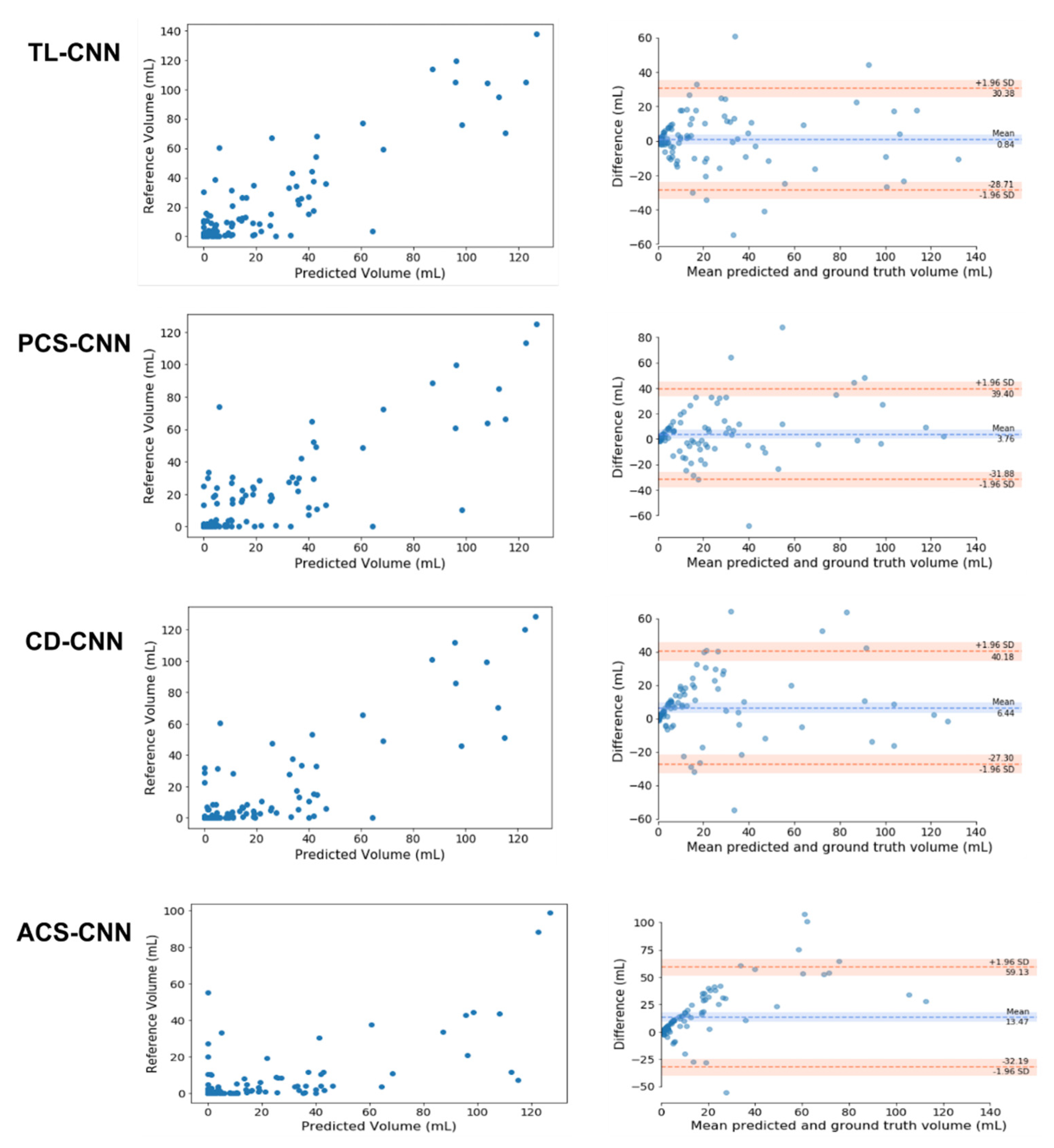
| Method | ICC | Dice | Bias | Limits of Agreement |
|---|---|---|---|---|
| TL-CNN | 0.88 (95% CI: 0.83–0.92) | 0.25 ± 0.07 | 0.84 mL | −28.7 to 30.4 mL |
| PCS-CNN | 0.80 (95% CI: 0.72–0.86) | 0.21 ± 0.06 | 3.8 mL | −31.9 to 39.4 mL |
| CD-CNN | 0.83 (95% CI: 0.76–0.88) | 0.16 ± 0.06 | 6.4 mL | −27.3 to 40.2 mL |
| ACS-CNN | 0.55 (95% CI: 0.4–0.67) | 0.07 ± 0.03 | 13.5 mL | −32.2 to 59.1 mL |
| Method 1 | Method 2 | Dice Coefficient | Bias | ||
|---|---|---|---|---|---|
| W | p-Value | W | p-Value | ||
| TL-CNN | PCS-CNN | 766 | <0.05 | 2205 | 0.28 |
| TL-CNN | CD-CNN | 216 | <0.01 | 1018 | <0.01 |
| TL-CNN | ACS-CNN | 62 | <0.01 | 938 | <0.01 |
| PCS-CNN | CD-CNN | 535 | <0.01 | 1958 | <0.05 |
| PCS-CNN | ACS-CNN | 114 | <0.01 | 1350 | <0.01 |
| CD-CNN | ACS-CNN | 88 | <0.01 | 1443 | <0.01 |
References
- Boers, A.M.; Jansen, I.G.; Beenen, L.F.; Devlin, T.G.; San Roman, L.; Heo, J.H.; Ribó, M.; Brown, S.; Almekhlafi, M.A.; Liebeskind, D.S.; et al. Association of follow-up infarct volume with functional outcome in acute ischemic stroke: A pooled analysis of seven randomized trials. J. Neurointerv. Surg. 2018, 10, 1137–1142. [Google Scholar] [CrossRef] [Green Version]
- Zaidi, S.F.; Aghaebrahim, A.; Urra, X.; Jumaa, M.A.; Jankowitz, B.; Hammer, M.; Nogueira, R.; Horowitz, M.; Reddy, V.; Jovin, T.G. Final infarct volume is a stronger predictor of outcome than recanalization in patients with proximal middle cerebral artery occlusion treated with endovascular therapy. Stroke 2012, 43, 3238–3244. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Villringer, K.; Florczak-Rzepka, M.; Grittner, U.; Brunecker, P.; Tepe, H.; Nolte, C.H.; Fiebach, J.B. Characteristics associated with outcome in patients with first-ever posterior fossa stroke. Eur. J. Neurol. 2018, 25, 818–824. [Google Scholar] [CrossRef] [PubMed]
- Schonewille, W.J.; Wijman, C.A.C.; Michel, P.; Rueckert, C.M.; Weimar, C.; Mattle, H.P.; Engelter, S.T.; Tanne, D.; Muir, K.W.; Molina, C.A.; et al. Treatment and outcomes of acute basilar artery occlusion in the Basilar Artery International Cooperation Study (BASICS): A prospective registry study. Lancet Neurol. 2009, 8, 724–730. [Google Scholar] [CrossRef]
- Banks, J.L.; Marotta, C.A. Outcomes validity and reliability of the modified rankin scale: Implications for stroke clinical trials—A literature review and synthesis. Stroke 2007, 38, 1091–1096. [Google Scholar] [CrossRef] [Green Version]
- Barros, R.S.; Tolhuisen, M.L.; Boers, A.M.M.; Jansen, I.; Ponomareva, E.; Dippel, D.W.J.; Van Der Lugt, A.; Van Oostenbrugge, R.J.; Van Zwam, W.H.; Berkhemer, O.A.; et al. Automatic segmentation of cerebral infarcts in follow-up computed tomography images with convolutional neural networks. J. Neurointerv. Surg. 2020, 12, 848–852. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, Y.C.; Lee, J.E.; Yu, I.; Song, H.N.; Baek, I.Y.; Seong, J.K.; Jeong, H.G.; Kim, B.J.; Nam, H.S.; Chung, J.W.; et al. Evaluation of Diffusion Lesion Volume Measurements in Acute Ischemic Stroke Using Encoder-Decoder Convolutional Network. Stroke 2019, 50, 1444–1451. [Google Scholar] [CrossRef]
- Bogousslavsky, J.; Van Melle, G.; Regli, F. Original Contributions The Lausanne Stroke Registry: Analysis of 1000 Consecutive Patients With First Stroke. Available online: https://www.ahajournals.org/doi/abs/10.1161/01.str.19.9.1083 (accessed on 24 August 2021).
- Moulin, T.; Tatu, L.; Vuillier, F.; Berger, E.; Chavot, D.; Rumbach, L. Role of a stroke data bank in evaluating cerebral infarction subtypes: Patterns and outcome of 1,776 consecutive patients from the Besancon Stroke Registry. Cerebrovasc. Dis. 2000, 10, 261–271. [Google Scholar] [CrossRef]
- Pan, S.J.; Yang, Q. A Survey on Transfer Learning. IEEE Trans. Knowl. Data Eng. 2009, 22, 1345–1359. [Google Scholar] [CrossRef]
- Litjens, G.; Kooi, T.; Bejnordi, B.E.; Setio, A.A.A.; Ciompi, F.; Ghafoorian, M.; van der Laak, J.A.W.M.; van Ginneken, B.; Sánchez, C.I. A survey on deep learning in medical image analysis. Med. Image Anal. 2017, 42, 60–88. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sanford, T.H.; Zhang, L.; Harmon, S.A.; Sackett, J.; Yang, D.; Roth, H.; Xu, Z.; Kesani, D.; Mehralivand, S.; Baroni, R.H.; et al. Data Augmentation and Transfer Learning to Improve Generalizability of an Automated Prostate Segmentation Model. Am. J. Roentgenol. 2020, 215, 1403–1410. [Google Scholar] [CrossRef]
- Nishio, M.; Fujimoto, K.; Matsuo, H.; Muramatsu, C.; Sakamoto, R.; Fujita, H. Lung Cancer Segmentation With Transfer Learning: Usefulness of a Pretrained Model Constructed From an Artificial Dataset Generated Using a Generative Adversarial Network. Front. Artif. Intell. 2021, 4, 694815. [Google Scholar] [CrossRef]
- Byra, M.; Wu, M.; Zhang, X.; Jang, H.; Ma, Y.-J.; Chang, E.Y.; Shah, S.; Du, J. Knee menisci segmentation and relaxometry of 3D ultrashort echo time cones MR imaging using attention U-Net with transfer learning. Magn. Reson. Med. 2020, 83, 1109–1122. [Google Scholar] [CrossRef] [Green Version]
- Goyal, M.; Menon, B.K.; Van Zwam, W.H.; Dippel, D.W.J.; Mitchell, P.J.; Demchuk, A.M.; Dávalos, A.; Majoie, C.B.L.M.; Van Der Lugt, A.; De Miquel, M.A.; et al. Endovascular thrombectomy after large-vessel ischaemic stroke: A meta-analysis of individual patient data from five randomised trials. Lancet 2016, 387, 1723–1731. [Google Scholar] [CrossRef]
- Van Der Hoeven, E.J.; Schonewille, W.J.; Vos, J.A.; Algra, A.; Audebert, H.J.; Berge, E.; Ciccone, A.; Mazighi, M.; Michel, P.; Muir, K.W.; et al. The Basilar Artery International Cooperation Study (BASICS): Study protocol for a randomised controlled trial. Trials 2013, 14, 200. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Langezaal, L.C.M.; van der Hoeven, E.J.R.J.; Mont’Alverne, F.J.A.; de Carvalho, J.J.F.; Lima, F.O.; Dippel, D.W.J.; van der Lugt, A.; Lo, R.T.H.; Boiten, J.; Lycklama à Nijeholt, G.J.; et al. Endovascular Therapy for Stroke Due to Basilar-Artery Occlusion. N. Engl. J. Med. 2021, 384, 1910–1920. [Google Scholar] [CrossRef] [PubMed]
- Yushkevich, P.A.; Piven, J.; Hazlett, H.C.; Smith, R.G.; Ho, S.; Gee, J.C.; Gerig, G. User-guided 3D active contour segmentation of anatomical structures: Significantly improved efficiency and reliability. Neuroimage 2006, 31, 1116–1128. [Google Scholar] [CrossRef] [Green Version]
- Puetz, V.; Sylaja, P.N.; Coutts, S.B.; Hill, M.D.; Dzialowski, I.; Mueller, P.; Becker, U.; Urban, G.; O’Reilly, C.; Barber, P.A.; et al. Extent of hypoattenuation on CT angiography source images predicts functional outcome in patients with basilar artery occlusion. Stroke 2008, 39, 2485–2490. [Google Scholar] [CrossRef] [Green Version]
- Mattes, D.; Haynor, D.R.; Vesselle, H.; Lewellyn, T.K.; Eubank, W. Nonrigid multimodality image registration. In Proceedings of the Medical Imaging 2001: Image Processing, San Diego, CA, USA, 17–22 February 2001; SPIE: Bellingham, WA, USA, 2001; Volume 4322, pp. 1609–1620. [Google Scholar]
- Lowekamp, B.C.; Chen, D.T.; Ibáñez, L.; Blezek, D. The design of simpleITK. Front. Neuroinform. 2013, 7, 45. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yaniv, Z.; Lowekamp, B.C.; Johnson, H.J.; Beare, R. SimpleITK Image-Analysis Notebooks: A Collaborative Environment for Education and Reproducible Research. J. Digit. Imaging 2018, 31, 290–303. [Google Scholar] [CrossRef] [Green Version]
- Ronneberger, O.; Fischer, P.; Brox, T. U-net: Convolutional networks for biomedical image segmentation. In Lecture Notes in Computer Science (Including Subseries Lecture Notes in Artificial Intelligence and Lecture Notes in Bioinformatics), Proceedings of the International Conference on Medical Image Computing and Computer-Assisted Intervention, Munich, Germany, 5–9 October 2015; Springer: Berlin/Heidelberg, Germany, 2015; Volume 9351, pp. 234–241. [Google Scholar]
- He, K.; Zhang, X.; Ren, S.; Sun, J. Deep Residual Learning for Image Recognition. In Proceedings of the 2016 IEEE Conference on Computer Vision and Pattern Recognition (CVPR), Las Vegas, NV, USA, 27–30 June 2016. [Google Scholar]
- Cicchetti, D.V. Guidelines, Criteria, and Rules of Thumb for Evaluating Normed and Standardized Assessment Instruments in Psychology. Psychol. Assess. 1994, 6, 284–290. [Google Scholar] [CrossRef]
- Vallat, R. Pingouin: Statistics in Python. J. Open Source Softw. 2018, 3, 1026. [Google Scholar] [CrossRef]
- Clèrigues, A.; Valverde, S.; Bernal, J.; Freixenet, J.; Oliver, A.; Lladó, X. Acute ischemic stroke lesion core segmentation in CT perfusion images using fully convolutional neural networks. Comput. Biol. Med. 2019, 115, 103487. [Google Scholar] [CrossRef] [PubMed]
- Öman, O.; Mäkelä, T.; Salli, E.; Savolainen, S.; Kangasniemi, M. 3D convolutional neural networks applied to CT angiography in the detection of acute ischemic stroke. Eur. Radiol. Exp. 2019, 3, 8. [Google Scholar] [CrossRef] [Green Version]
- Yu, Y.; Xie, Y.; Thamm, T.; Gong, E.; Ouyang, J.; Huang, C.; Christensen, S.; Marks, M.P.; Lansberg, M.G.; Albers, G.W.; et al. Use of Deep Learning to Predict Final Ischemic Stroke Lesions From Initial Magnetic Resonance Imaging. JAMA Netw. Open 2020, 3, e200772. [Google Scholar] [CrossRef] [Green Version]
- Qiu, W.; Kuang, H.; Teleg, E.; Ospel, J.M.; Sohn, S.I.; Almekhlafi, M.; Goyal, M.; Hill, M.D.; Demchuk, A.M.; Menon, B.K. Machine Learning for Detecting Early Infarction in Acute Stroke with Non–Contrast-enhanced CT. Radiology 2020, 294, 638–644. [Google Scholar] [CrossRef] [PubMed]
- Barman, A.; Inam, M.E.; Lee, S.; Savitz, S.; Sheth, S.; Giancardo, L. Determining ischemic stroke from ct-angiography imaging using symmetry-sensitive convolutional networks. In Proceedings of the 2019 IEEE 16th International Symposium on Biomedical Imaging, Venice, Italy, 8–11 April 2019; IEEE Computer Society: Washington, DC, USA, 2019; pp. 1873–1877. [Google Scholar]
- Pustina, D.; Branch Coslett, H.; Turkeltaub, P.E.; Tustison, N.; Schwartz, M.F.; Avants, B. Automated Segmentation of Chronic Stroke Lesions Using LINDA: Lesion Identification With Neighborhood Data Analysis. Hum. Brain Mapp. 2016, 37, 1405–1421. [Google Scholar] [CrossRef] [Green Version]
- Tomita, N.; Jiang, S.; Maeder, M.E.; Hassanpour, S. Automatic post-stroke lesion segmentation on MR images using 3D residual convolutional neural network. NeuroImage Clin. 2020, 27, 102276. [Google Scholar] [CrossRef]
- Chen, S.; Ma, K.; Zheng, Y. MED3D: Transfer learning for 3D medical image analysis. arXiv 2019, arXiv:1904.00625v4. [Google Scholar]
- Zhou, Z.; Sodha, V.; Rahman Siddiquee, M.M.; Feng, R.; Tajbakhsh, N.; Gotway, M.B.; Liang, J. Models genesis: Generic autodidactic models for 3d medical image analysis. In Lecture Notes in Computer Science (Including Subseries Lecture Notes in Artificial Intelligence and Lecture Notes in Bioinformatics), Proceedings of the International Conference on Medical Image Computing and Computer-Assisted Intervention, Shenzhen, China, 13–17 October 2019; Springer: Berlin/Heidelberg, Germany, 2019; Volume 11767, pp. 384–393. [Google Scholar]
- Russakovsky, O.; Deng, J.; Su, H.; Krause, J.; Satheesh, S.; Ma, S.; Huang, Z.; Karpathy, A.; Khosla, A.; Bernstein, M.; et al. ImageNet Large Scale Visual Recognition Challenge. Int. J. Comput. Vis. 2014, 115, 211–252. [Google Scholar] [CrossRef] [Green Version]
- Yosinski, J.; Clune, J.; Bengio, Y.; Lipson, H. How transferable are features in deep neural networks? In Proceedings of the Advances in Neural Information Processing Systems, Montreal, QC, Canada, 8–13 December 2014; Volume 4, pp. 3320–3328. [Google Scholar]
| Parameter | Posterior Stroke | Anterior Stroke |
|---|---|---|
| Clinical | ||
| Age, years, mean (Standard Deviation) | 65.65 (12.2) | 66.1 (13.3) |
| Sex, F, No. [%] | 34/107 [31.8] | 458/1018 [45] |
| NIHSS at baseline, mean [median] (N) | 21.4 [19] (107) | 17 [17] (1015) |
| Prior Conditions | ||
| Diabetes mellitus, No. [%] | 28/107 [26.2] | 169/1018 [16.6] |
| Hypertension, No. [%] | 64/107 [59.8] | 564/1018 [55.4] |
| Stroke, No. [%] | 21/107 [19.6] | 121/1018 [11.9] |
| Posterior circulation stroke, No. [%] | 7/107 [6.5] | NAV |
| TIA, No. [%] | 10/106 [9.4] | NAV |
| Posterior circulation TIA, No. [%] | 2/106 [1.9] | NAV |
| Atrial fibrillation, No. [%] | 13/107 [12.1] | 314/1018 [30.8] |
| Atrial fibrillation (history or 12 lead ECG), No. [%] | 23/107 [21.5] | NAV |
| Pre-Stroke mRS | ||
| 0, No. [%] | 80/107 [74.8] | 836/1017 [82.1] |
| 1, No. [%] | 11/107 [10.3] | 129/1017 [12.7] |
| 2, No. [%] | 13/107 [12.1] | 29/1017 [2.9] |
| 3, No. [%] | 3/107 [2.8] | 23/1017 [2.3] |
| Treatment | ||
| IVT, No. [%] | 92/107 [86] | 872/1018 [85.7] |
| Time | ||
| Stroke onset to IVT, min., mean [Standard Deviation] (N) | 176.9 [176.102] (90) | 112.2 [57.2] (871) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zoetmulder, R.; Konduri, P.R.; Obdeijn, I.V.; Gavves, E.; Išgum, I.; Majoie, C.B.L.M.; Dippel, D.W.J.; Roos, Y.B.W.E.M.; Goyal, M.; Mitchell, P.J.; et al. Automated Final Lesion Segmentation in Posterior Circulation Acute Ischemic Stroke Using Deep Learning. Diagnostics 2021, 11, 1621. https://doi.org/10.3390/diagnostics11091621
Zoetmulder R, Konduri PR, Obdeijn IV, Gavves E, Išgum I, Majoie CBLM, Dippel DWJ, Roos YBWEM, Goyal M, Mitchell PJ, et al. Automated Final Lesion Segmentation in Posterior Circulation Acute Ischemic Stroke Using Deep Learning. Diagnostics. 2021; 11(9):1621. https://doi.org/10.3390/diagnostics11091621
Chicago/Turabian StyleZoetmulder, Riaan, Praneeta R. Konduri, Iris V. Obdeijn, Efstratios Gavves, Ivana Išgum, Charles B.L.M. Majoie, Diederik W.J. Dippel, Yvo B.W.E.M. Roos, Mayank Goyal, Peter J. Mitchell, and et al. 2021. "Automated Final Lesion Segmentation in Posterior Circulation Acute Ischemic Stroke Using Deep Learning" Diagnostics 11, no. 9: 1621. https://doi.org/10.3390/diagnostics11091621
APA StyleZoetmulder, R., Konduri, P. R., Obdeijn, I. V., Gavves, E., Išgum, I., Majoie, C. B. L. M., Dippel, D. W. J., Roos, Y. B. W. E. M., Goyal, M., Mitchell, P. J., Campbell, B. C. V., Lopes, D. K., Reimann, G., Jovin, T. G., Saver, J. L., Muir, K. W., White, P., Bracard, S., Chen, B., ... Marquering, H. A. (2021). Automated Final Lesion Segmentation in Posterior Circulation Acute Ischemic Stroke Using Deep Learning. Diagnostics, 11(9), 1621. https://doi.org/10.3390/diagnostics11091621







