A Comprehensive Approach for the Diagnosis of Primary Ciliary Dyskinesia—Experiences from the First 100 Patients of the PCD-UNIBE Diagnostic Center
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Study Population
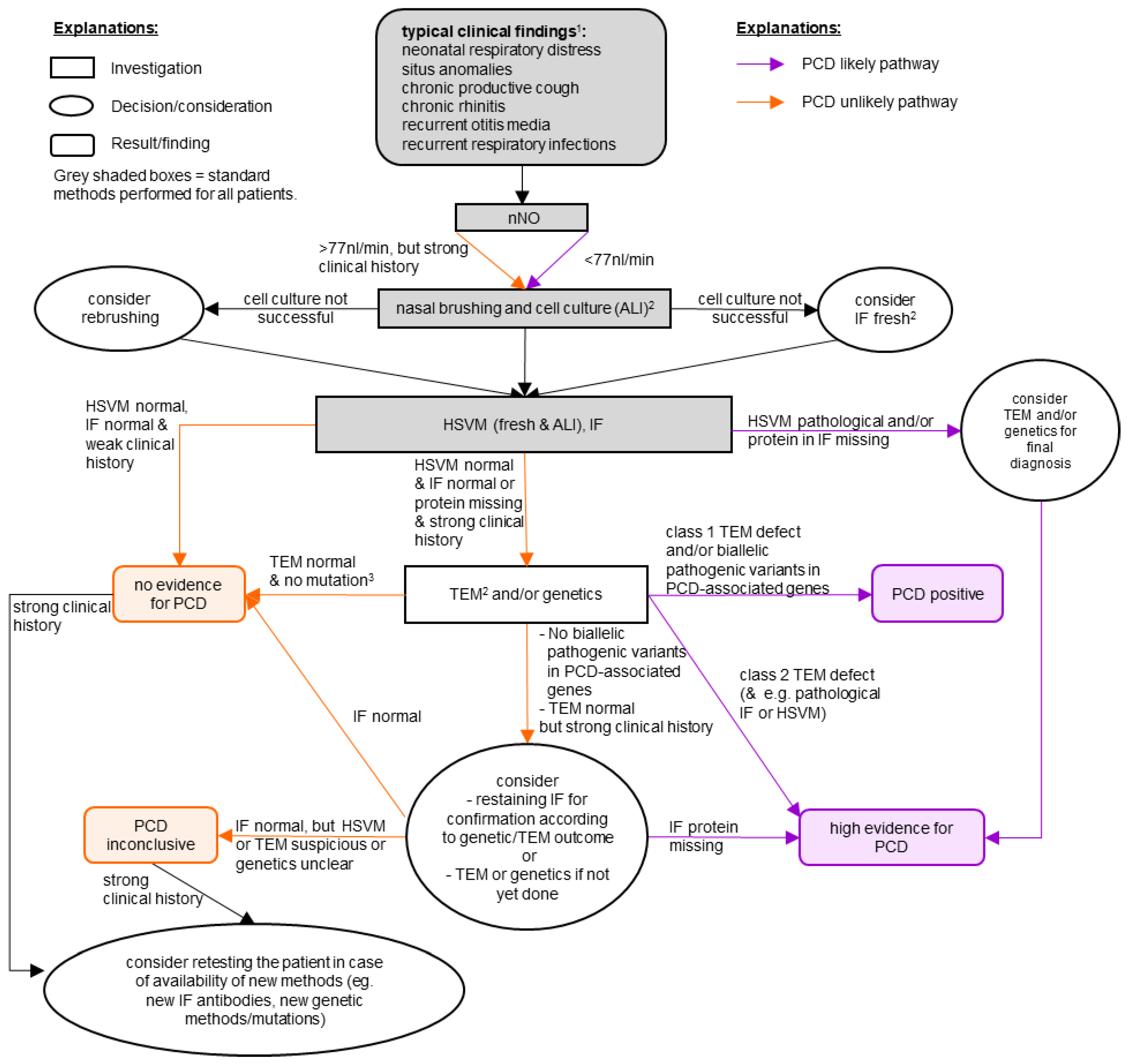
2.2. Diagnostic Workflow
2.3. Nasal Brushing and Further Processing
2.4. Cell Culture
2.5. High-Speed Videomicroscopy (HSVM)
2.6. Immunofluorescence Staining (IF)
2.7. Transmission Electron Microscopy (TEM)
2.8. Genetical Analysis
3. Results
3.1. Study Population
3.2. Overview of the Tests: HSVM, IF, TEM, Genetics
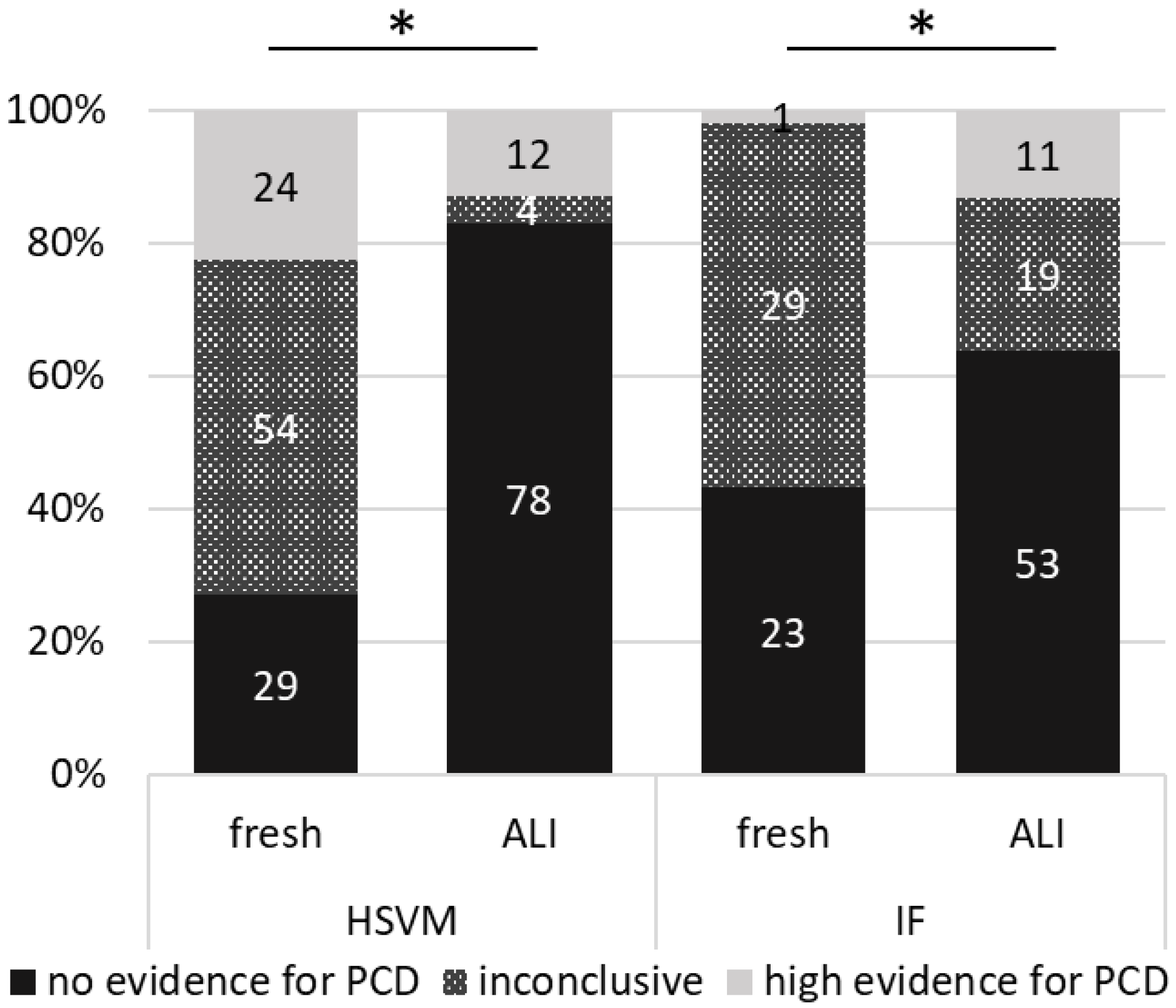
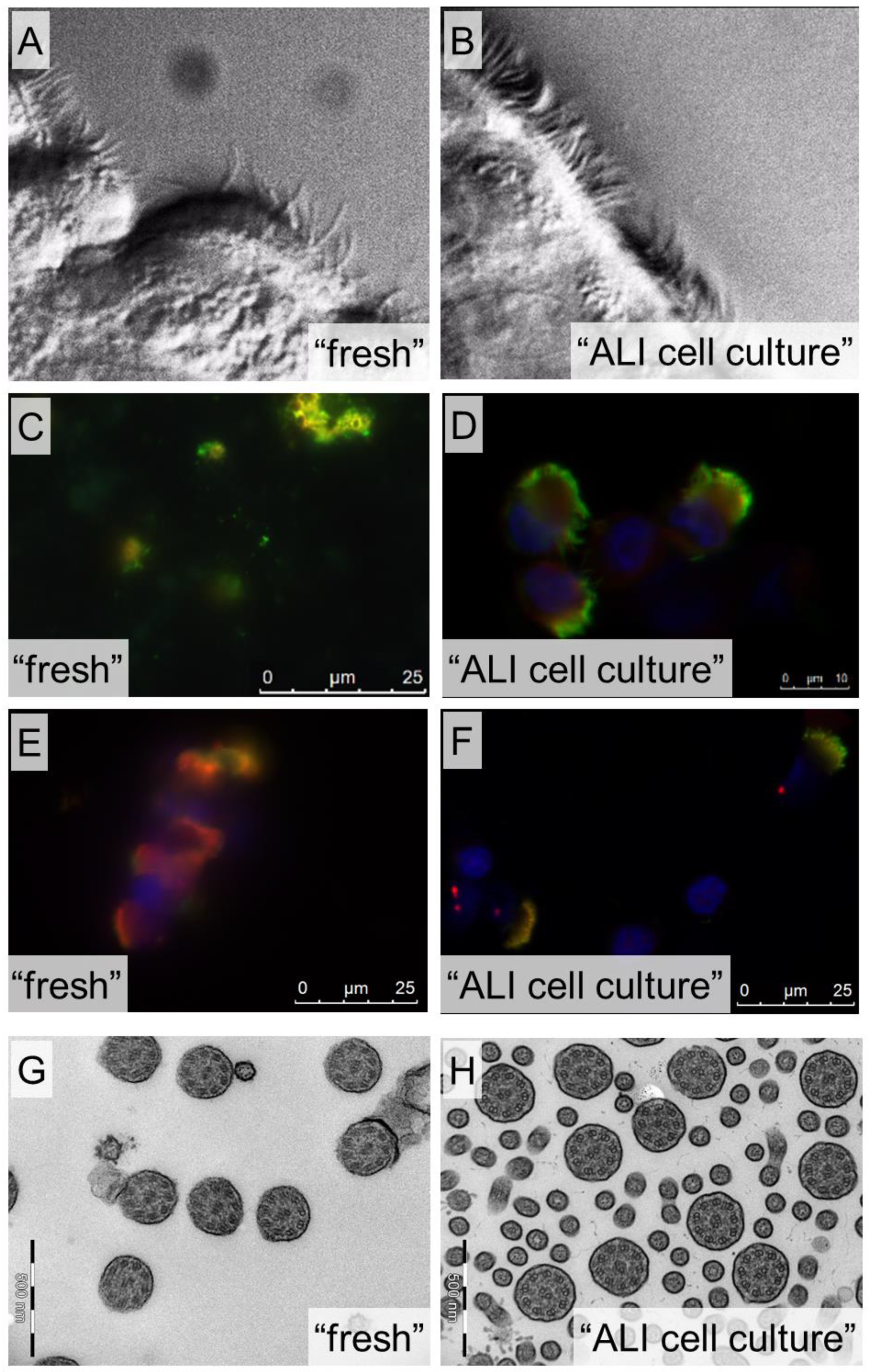
3.3. Air-Liquid Interface (ALI) Cell Culture
3.4. Results of the Performed Tests: HSVM, IF, TEM, Genetics
3.5. Overall Diagnostics Outcome
3.6. Relevance of the Different Methods for the Diagnosis of PCD
3.7. Costs
4. Discussion
4.1. Summary
4.2. Diagnostic Impact of Methods/Procedures in Our Setting
4.3. Limitations and Strengths
4.4. Comparison with the Literature
4.5. Clinical and Practical Relevance
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Supplementary Methods’ Description
Appendix A.1. Nasal Brushing: Procedure and Processing
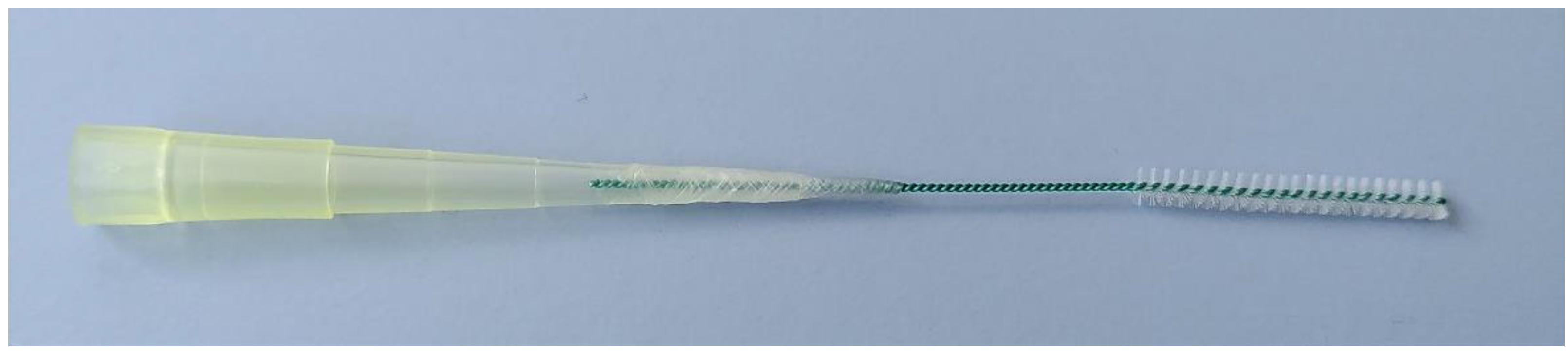
Appendix A.2. Cell Culture
Appendix A.2.1. Preparation of Media
Appendix A.2.2. Preparation of Well Plates
Appendix A.2.3. Procedure of Cell Cultivation
Appendix A.2.4. Processing of Mature ALI Cultures
Appendix A.3. High-Speed Videomicroscopy (HSVM)

Appendix A.4. Immunofluorescence (IF)
| Protein | Manufacturer | Product Number | Dilution |
|---|---|---|---|
| beta-tubulin | Sigma Aldrich | T7451 | 1:1000 |
| CCDC40 | Prestige, Sigma Aldrich | HPA022974 | 1:100 |
| DNAH5 | Prestige, Sigma Aldrich | HPA037470 | 1:100 |
| DNAH9 | Prestige, Sigma Aldrich | HPA052641 | 1:50 |
| DNAH11 | Prestige, Sigma Aldrich | HPA045880 | 1:50 |
| DNAI1 | Prestige, Sigma Aldrich | HPA021649 | 1:100 |
| DNAI2 | Prestige, Sigma Aldrich | HPA050565 | 1:100 |
| DNALI1 | Prestige, Sigma Aldrich | HPA028305 | 1:100 |
| GAS8 | Prestige, Sigma Aldrich | HPA041311 | 1:200 |
| RSPH1 | Prestige, Sigma Aldrich | HPA017382 | 1:100 |
| RSPH4a | Prestige, Sigma Aldrich | HPA031197 | 1:200 |
| RSPH9 | Novus, Bio-Techne | NBP1-86750 | 1:100 |
| goat anti-mouse 488 | Invitrogen | A21121 | 1:2500 |
| goat anti-rabbit 546 | Invitrogen | A11035 | 1:1000 |
Appendix A.5. Transmission Electron Microscopy (TEM)
Appendix A.6. Genetics—Whole Genome Sequencing at HUG
References
- Lucas, J.S.; Burgess, A.; Mitchison, H.M.; Moya, E.; Williamson, M.; Hogg, C. Diagnosis and management of primary ciliary dyskinesia. Arch. Dis. Child. 2014, 99, 850–856. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kuehni, C.E.; Frischer, T.; Strippoli, M.P.; Maurer, E.; Bush, A.; Nielsen, K.G.; Escribano, A.; Lucas, J.S.; Yiallouros, P.; Omran, H.; et al. Factors influencing age at diagnosis of primary ciliary dyskinesia in European children. Eur. Respir. J. 2010, 36, 1248–1258. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ardura-Garcia, C.; Goutaki, M.; Carr, S.B.; Crowley, S.; Halbeisen, F.S.; Nielsen, K.G.; Pennekamp, P.; Raidt, J.; Thouvenin, G.; Yiallouros, P.K.; et al. Registries and collaborative studies for primary ciliary dyskinesia in Europe. ERJ Open Res. 2020, 6. [Google Scholar] [CrossRef] [PubMed]
- Afzelius, B.A. A human syndrome caused by immotile cilia. Science 1976, 193, 317–319. [Google Scholar] [CrossRef]
- Fliegauf, M.; Benzing, T.; Omran, H. When cilia go bad: Cilia defects and ciliopathies. Nat. Rev. Mol. Cell Biol. 2007, 8, 880–893. [Google Scholar] [CrossRef]
- Leigh, M.W.; Ferkol, T.W.; Davis, S.D.; Lee, H.S.; Rosenfeld, M.; Dell, S.D.; Sagel, S.D.; Milla, C.; Olivier, K.N.; Sullivan, K.M.; et al. Clinical Features and Associated Likelihood of Primary Ciliary Dyskinesia in Children and Adolescents. Ann. Am. Thorac. Soc. 2016, 13, 1305–1313. [Google Scholar] [CrossRef]
- Holzmann, D.; Felix, H. Neonatal respiratory distress syndrome—A sign of primary ciliary dyskinesia? Eur. J. Pediatr. 2000, 159, 857–860. [Google Scholar] [CrossRef]
- Noone, P.G.; Leigh, M.W.; Sannuti, A.; Minnix, S.L.; Carson, J.L.; Hazucha, M.; Zariwala, M.A.; Knowles, M.R. Primary ciliary dyskinesia: Diagnostic and phenotypic features. Am. J. Respir. Crit. Care Med. 2004, 169, 459–467. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lucas, J.S.; Davis, S.D.; Omran, H.; Shoemark, A. Primary ciliary dyskinesia in the genomics age. Lancet. Respir. Med. 2020, 8, 202–216. [Google Scholar] [CrossRef]
- Goutaki, M.; Meier, A.B.; Halbeisen, F.S.; Lucas, J.S.; Dell, S.D.; Maurer, E.; Casaulta, C.; Jurca, M.; Spycher, B.D.; Kuehni, C.E. Clinical manifestations in primary ciliary dyskinesia: Systematic review and meta-analysis. Eur. Respir. J. 2016, 48, 1081–1095. [Google Scholar] [CrossRef] [Green Version]
- Kartagener, M.; Stucki, P. Bronchiectasis with situs inversus. Arch. Pediatr. 1962, 79, 193–207. [Google Scholar]
- Honore, I.; Burgel, P.R. Primary ciliary dyskinesia in adults. Rev. Mal. Respir. 2016, 33, 165–189. [Google Scholar] [CrossRef]
- Nyilas, S.; Bauman, G.; Pusterla, O.; Sommer, G.; Singer, F.; Stranzinger, E.; Heyer, C.; Ramsey, K.; Schlegtendal, A.; Benzrath, S.; et al. Structural and Functional Lung Impairment in Primary Ciliary Dyskinesia. Assessment with Magnetic Resonance Imaging and Multiple Breath Washout in Comparison to Spirometry. Ann. Am. Thorac. Soc. 2018, 15, 1434–1442. [Google Scholar] [CrossRef]
- Horani, A.; Ferkol, T.W. Advances in the Genetics of Primary Ciliary Dyskinesia: Clinical Implications. Chest 2018, 154, 645–652. [Google Scholar] [CrossRef]
- Lucas, J.S.; Barbato, A.; Collins, S.A.; Goutaki, M.; Behan, L.; Caudri, D.; Dell, S.; Eber, E.; Escudier, E.; Hirst, R.A.; et al. European Respiratory Society guidelines for the diagnosis of primary ciliary dyskinesia. Eur. Respir. J. 2017, 49, 1601090. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, A.J.; Davis, S.D.; Polineni, D.; Manion, M.; Rosenfeld, M.; Dell, S.D.; Chilvers, M.A.; Ferkol, T.W.; Zariwala, M.A.; Sagel, S.D.; et al. Diagnosis of Primary Ciliary Dyskinesia. An Official American Thoracic Society Clinical Practice Guideline. Am. J. Respir. Crit. Care Med. 2018, 197, e24–e39. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, A.J.; Ferkol, T.W.; Manion, M.; Leigh, M.W.; Davis, S.D.; Knowles, M.R. High-Speed Videomicroscopy Analysis Presents Limitations in Diagnosis of Primary Ciliary Dyskinesia. Am. J. Respir. Crit. Care Med. 2020, 201, 122–123. [Google Scholar] [CrossRef] [PubMed]
- Kempeneers, C.; Seaton, C.; Garcia Espinosa, B.; Chilvers, M.A. Ciliary functional analysis: Beating a path towards standardization. Pediatr. Pulmonol. 2019, 54, 1627–1638. [Google Scholar] [CrossRef] [PubMed]
- Coren, M.E.; Meeks, M.; Morrison, I.; Buchdahl, R.M.; Bush, A. Primary ciliary dyskinesia: Age at diagnosis and symptom history. Acta Paediatr. 2002, 91, 667–669. [Google Scholar] [CrossRef] [PubMed]
- Polineni, D.; Davis, S.D.; Dell, S.D. Treatment recommendations in Primary Ciliary Dyskinesia. Paediatr. Respir. Rev. 2016, 18, 39–45. [Google Scholar] [CrossRef]
- Nussbaumer, M.K.E.; Tschanz, S.A.; Savas, S.T.; Casaulta, C.; Goutaki, M.; Blanchon, S.; Jung, A.; Regamey, N.; Kuehni, C.E.; Latzin, P.; et al. Diagnosis of Primary Ciliary Dyskinesia: Discrepancy according to different algorithms. ERJ Open 2021, 197, 12. [Google Scholar] [CrossRef]
- Behan, L.; Dimitrov, B.D.; Kuehni, C.E.; Hogg, C.; Carroll, M.; Evans, H.J.; Goutaki, M.; Harris, A.; Packham, S.; Walker, W.T.; et al. PICADAR: A diagnostic predictive tool for primary ciliary dyskinesia. Eur. Respir. J. 2016, 47, 1103–1112. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schneiter, M. On the Structure and Function of Mucociliary Epithelia. Ph.D. Thesis, University of Bern, Bern, Switzerland, 2020. [Google Scholar]
- Shoemark, A.; Boon, M.; Brochhausen, C.; Bukowy-Bieryllo, Z.; De Santi, M.M.; Goggin, P.; Griffin, P.; Hegele, R.G.; Hirst, R.A.; Leigh, M.W.; et al. International consensus guideline for reporting transmission electron microscopy results in the diagnosis of primary ciliary dyskinesia (BEAT PCD TEM Criteria). Eur. Respir. J. 2020, 55. [Google Scholar] [CrossRef]
- Hirst, R.A.; Rutman, A.; Williams, G.; O’Callaghan, C. Ciliated air-liquid cultures as an aid to diagnostic testing of primary ciliary dyskinesia. Chest 2010, 138, 1441–1447. [Google Scholar] [CrossRef] [PubMed]
- Coles, J.L.; Thompson, J.; Horton, K.L.; Hirst, R.A.; Griffin, P.; Williams, G.M.; Goggin, P.; Doherty, R.; Lackie, P.M.; Harris, A.; et al. A Revised Protocol for Culture of Airway Epithelial Cells as a Diagnostic Tool for Primary Ciliary Dyskinesia. J. Clin. Med. 2020, 9, 3753. [Google Scholar] [CrossRef]
- Pifferi, M.; Bush, A.; Montemurro, F.; Pioggia, G.; Piras, M.; Tartarisco, G.; Di Cicco, M.; Chinellato, I.; Cangiotti, A.M.; Boner, A.L. Rapid diagnosis of primary ciliary dyskinesia: Cell culture and soft computing analysis. Eur. Respir. J. 2013, 41, 960–965. [Google Scholar] [CrossRef] [Green Version]
- Hirst, R.A.; Jackson, C.L.; Coles, J.L.; Williams, G.; Rutman, A.; Goggin, P.M.; Adam, E.C.; Page, A.; Evans, H.J.; Lackie, P.M.; et al. Culture of Primary Ciliary Dyskinesia Epithelial Cells at Air-Liquid Interface Can Alter Ciliary Phenotype but Remains a Robust and Informative Diagnostic Aid. PLoS ONE 2014, 9, e89675. [Google Scholar] [CrossRef] [Green Version]
- Rubbo, B.; Shoemark, A.; Jackson, C.L.; Hirst, R.; Thompson, J.; Hayes, J.; Frost, E.; Copeland, F.; Hogg, C.; O’Callaghan, C.; et al. Accuracy of High-Speed Video Analysis to Diagnose Primary Ciliary Dyskinesia. Chest 2019, 155, 1008–1017. [Google Scholar] [CrossRef] [Green Version]
- Behan, L.; Rubbo, B.; Lucas, J.S.; Dunn Galvin, A. The patient’s experience of primary ciliary dyskinesia: A systematic review. Qual. Life Res. Int. J. Qual. Life Asp. Treat. Care Rehabil. 2017, 26, 2265–2285. [Google Scholar] [CrossRef] [Green Version]
- Kobbernagel, H.E.; Buchvald, F.F.; Haarman, E.G.; Casaulta, C.; Collins, S.A.; Hogg, C.; Kuehni, C.E.; Lucas, J.S.; Moser, C.E.; Quittner, A.L.; et al. Efficacy and safety of azithromycin maintenance therapy in primary ciliary dyskinesia (BESTCILIA): A multicentre, double-blind, randomised, placebo-controlled phase 3 trial. Lancet. Respir. Med. 2020, 8, 493–505. [Google Scholar] [CrossRef]
- Stokes, A.B.; Kieninger, E.; Schogler, A.; Kopf, B.S.; Casaulta, C.; Geiser, T.; Regamey, N.; Alves, M.P. Comparison of three different brushing techniques to isolate and culture primary nasal epithelial cells from human subjects. Exp. Lung Res. 2014, 40, 327–332. [Google Scholar] [CrossRef] [PubMed]

| Characteristic of the Study Population | All Cases | PCD Cases | Non-PCD Cases |
|---|---|---|---|
| Mean age (Standard deviation), years | 12.9 (18.0) | 29.2 (26.4) | 9.1 (12.8) |
| Median age (range), years | 5.6 (0.04–68.9) | 16.9 (1.4–68.9) | 4.8 (0.04–61.7) |
| Sex (female/male), n | 44/56 | 8/91 | 36/44 1 |
| Age category 2 (children/adults), n | 83/17 | 11/6 | 70/10 |
| Referring centers, n (%) | all cases | PCD cases | non-PCD cases |
| Inselspital, Bern University Hospital (pediatrics) | 54 (54%) | 7 (41%) | 45 (56%) |
| Inselspital, Bern University Hospital (adults) | 2 (2%) | 0 (0%) | 1 (1%) |
| Cantonal Hospital Graubünden (pediatrics) | 23 (23%) | 3 (18%) | 20 (25%) |
| Children’s Hospital Lucerne | 4 (4%) | 1 (6%) | 3 (4%) |
| Fribourg Hospital (pediatrics) | 4 (4%) | 0 (0%) | 4 (5%) |
| Lausanne University Hospital (pediatrics) | 2 (2%) | 0 (0%) | 2 (3%) |
| Hospital Lindenhof (Pneumology, Bern) | 4 (4%) | 2 (12%) | 2 (3%) |
| Others 3 | 7 (7%) | 4 (24%) | 3 (4%) |
| Symptoms, n (%) | all cases | PCD cases | non-PCD cases |
| Chronic productive cough | 61 (61%) | 9 (53%) | 51 (64%) |
| Chronic rhinitis | 40 (40%) | 9 (53%) | 29 (36%) |
| Chronic sinusitis | 8 (8%) | 1 (6%) | 7 (9%) |
| Recurrent otitis media | 18 (18%) | 4 (24%) | 13 (16%) |
| Recurrent respiratory infections | 41 (41%) | 2 (12%) | 36 (45%) |
| Bronchiectasis | 12 (12%) | 3 (18%) | 8 (10%) |
| Neonatal respiratory distress | 8 (8%) | 1 (6%) | 7 (9%) |
| Situs anomalies | 10 (10%) | 5 (29%) | 5 (6%) |
| Others 4 | 42 (42%) | 9 (53%) | 32 (40%) |
| nNO3, n (%) | all cases | PCD cases | non-PCD cases |
| Reduced (<77 nL/min) | 25 (25%) | 3 (18%) | 21 (26%) |
| Borderline (<85 nL/min, >77 nL/min) | 2 (2%) | 11 (65%) | 14 (18%) |
| Normal (>85 nL/min) | 24 (24%) | 0 (0%) | 2 (3%) |
| Not performed 5 | 49 (49%) | 3 (18%) | 43 (54%) |
| Diagnostic Outcome | n (%) |
|---|---|
| no evidence for PCD | 80 (80%) |
| high evidence for PCD (=diagnosis of PCD) | 5 (5%) |
| PCD positive (=diagnosis of PCD) | 12 (12%) |
| Inconclusive a | 3 (3%) |
| n | HSVM | IF | TEM | Genetics | Remark |
|---|---|---|---|---|---|
| 8 | + | + | - | + | all DNAH11 mutations |
| 2 | + | + | + | (not done) | no genetics performed |
| 2 | - | + | + | - | no mutations found |
| 1 | + | + | - | - | one pathologic variant in DNAH11 |
| 1 | + | - | + | - | genetics still ongoing |
| 1 | + | - | (not done) | + | HYDIN mutation |
| 1 | - | + | - | - | No mutation found |
| 1 | - | - | (not done) | + | DNAH5 mutation, cell culture not successful |
| Total: 17 | 13 | 14 | 5 | 10 |
| Investigation/Method | Consumables and Fee for Equipment Use | Working Hours | Total |
|---|---|---|---|
| nasal brushing | EUR 6 | EUR 70 | EUR 76 |
| cell culture | EUR 250 | EUR 260 | EUR 510 |
| HSVM fresh | EUR 24 | EUR 180 | EUR 204 |
| HSVM ALI | EUR 24 | EUR 140 | EUR 164 |
| IF fresh 1 | EUR 155 | EUR 170 | EUR 325 |
| IF ALI 1 | EUR 155 | EUR 120 | EUR 275 |
| TEM fresh | EUR 500 | EUR 1500 | EUR 2000 |
| TEM ALI | EUR 250 | EUR 750 | EUR 1000 |
| Reporting/meetings/etc. | EUR 0 | EUR 181 | EUR 181 |
| Genetics 2 | EUR 200 | EUR 2800 | EUR 3000 |
| all standard methods 3 | EUR 459 | EUR 770 | EUR 1229 |
| all methods 4 | EUR 909 | EUR 4501 | EUR 5410 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Müller, L.; Savas, S.T.; Tschanz, S.A.; Stokes, A.; Escher, A.; Nussbaumer, M.; Bullo, M.; Kuehni, C.E.; Blanchon, S.; Jung, A.; et al. A Comprehensive Approach for the Diagnosis of Primary Ciliary Dyskinesia—Experiences from the First 100 Patients of the PCD-UNIBE Diagnostic Center. Diagnostics 2021, 11, 1540. https://doi.org/10.3390/diagnostics11091540
Müller L, Savas ST, Tschanz SA, Stokes A, Escher A, Nussbaumer M, Bullo M, Kuehni CE, Blanchon S, Jung A, et al. A Comprehensive Approach for the Diagnosis of Primary Ciliary Dyskinesia—Experiences from the First 100 Patients of the PCD-UNIBE Diagnostic Center. Diagnostics. 2021; 11(9):1540. https://doi.org/10.3390/diagnostics11091540
Chicago/Turabian StyleMüller, Loretta, Sibel T. Savas, Stefan A. Tschanz, Andrea Stokes, Anaïs Escher, Mirjam Nussbaumer, Marina Bullo, Claudia E. Kuehni, Sylvain Blanchon, Andreas Jung, and et al. 2021. "A Comprehensive Approach for the Diagnosis of Primary Ciliary Dyskinesia—Experiences from the First 100 Patients of the PCD-UNIBE Diagnostic Center" Diagnostics 11, no. 9: 1540. https://doi.org/10.3390/diagnostics11091540
APA StyleMüller, L., Savas, S. T., Tschanz, S. A., Stokes, A., Escher, A., Nussbaumer, M., Bullo, M., Kuehni, C. E., Blanchon, S., Jung, A., Regamey, N., Haenni, B., Schneiter, M., Ingold, J., Kieninger, E., Casaulta, C., Latzin, P., & on behalf of the Swiss PCD Research Group. (2021). A Comprehensive Approach for the Diagnosis of Primary Ciliary Dyskinesia—Experiences from the First 100 Patients of the PCD-UNIBE Diagnostic Center. Diagnostics, 11(9), 1540. https://doi.org/10.3390/diagnostics11091540






