Role of Optical Coherence Tomography Imaging in Predicting Progression of Age-Related Macular Disease: A Survey
Abstract
1. Introduction
2. Grades of AMD
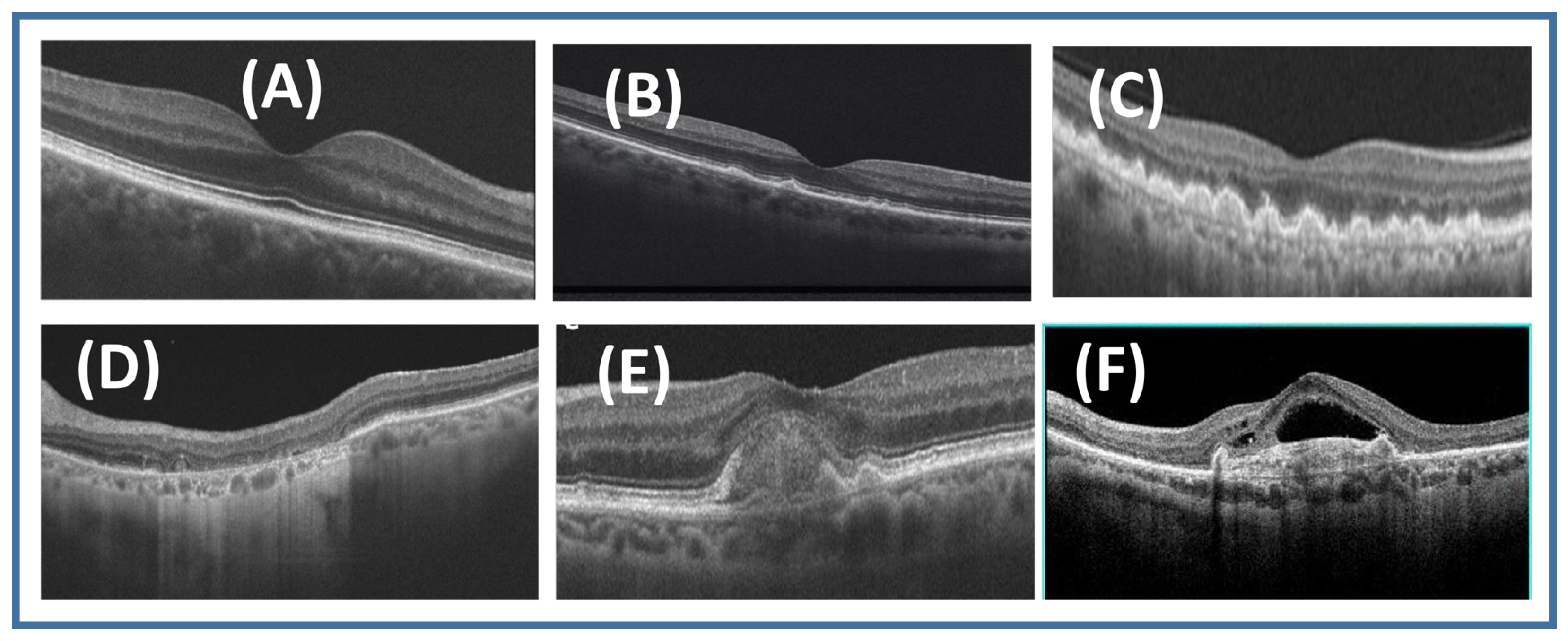
2.1. Dry AMD
2.1.1. Early Dry AMD
2.1.2. Intermediate Dry AMD
2.1.3. Advanced Dry AMD (Geographic Atrophy)
2.2. Wet AMD
2.2.1. Inactive Wet AMD
2.2.2. Active Wet AMD
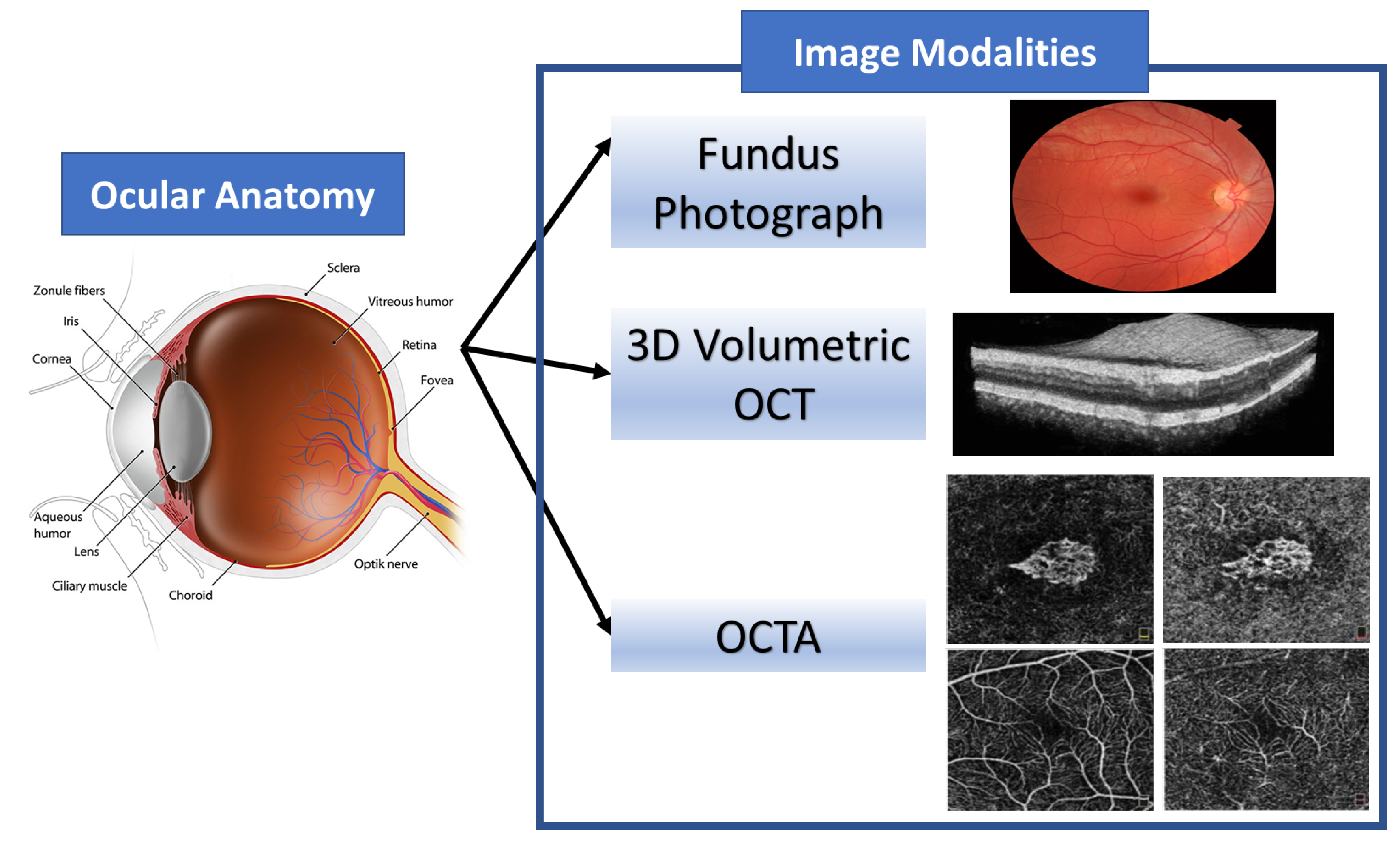
3. The Image Modalities Used for AMD Classification
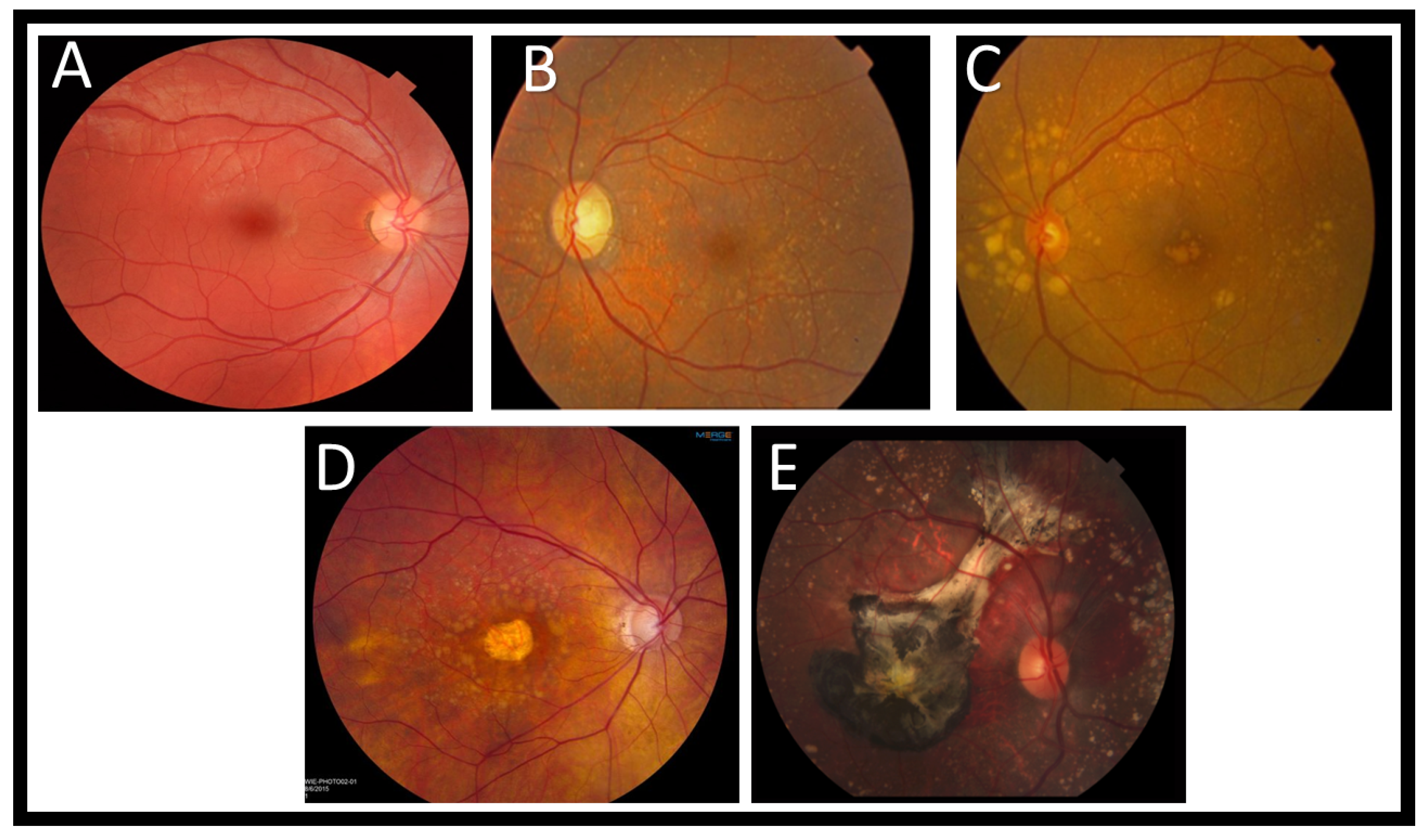
3.1. Fundus Image
3.2. Optical Coherence Tomography (OCT)
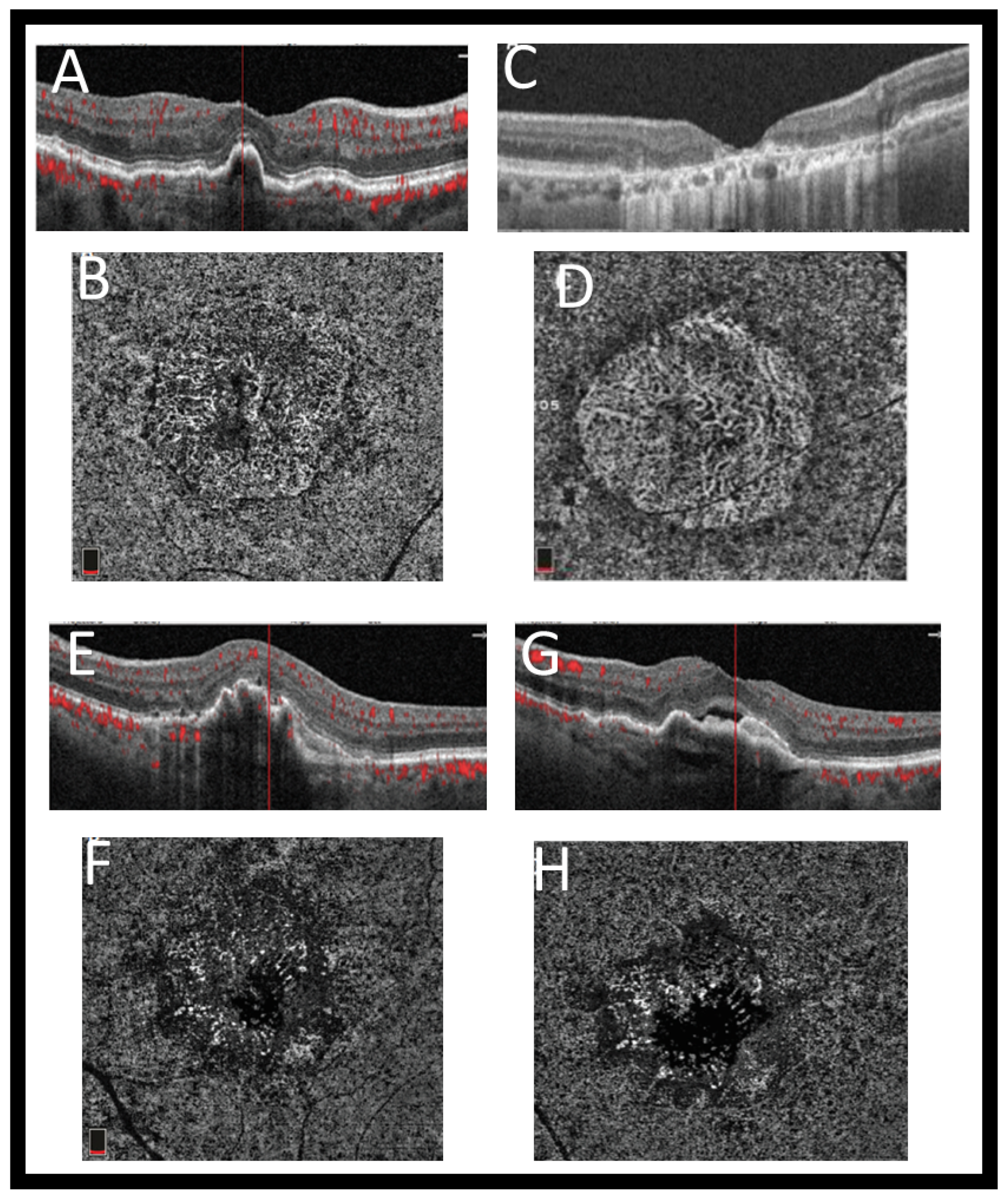
3.3. Optical Coherence Tomography Angiography (OCTA)
4. The Abnormalities of AMD
4.1. Drusen
4.2. Geographic Atrophy
4.3. Neovascular Age-Related Macular Degeneration
5. Methods
CAD System for AMD Diagnosing Based on Imaging
6. Discussion and Future Direction
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bressler, N.M. Age-Related Macular Degeneration Is the Leading Cause of Blindness…. JAMA 2004, 291, 1900–1901. [Google Scholar] [CrossRef] [PubMed]
- Pascolini, D.; Mariotti, S.; Pokharel, G.; Pararajasegaram, R.; Etya’Ale, D.; Négrel, A.D.; Resnikoff, S. 2002 global update of available data on visual impairment: A compilation of population-based prevalence studies. Ophthalmic Epidemiol. 2004, 11, 67–115. [Google Scholar] [CrossRef] [PubMed]
- Venhuizen, F.G.; van Ginneken, B.; van Asten, F.; van Grinsven, M.J.; Fauser, S.; Hoyng, C.B.; Theelen, T.; Sánchez, C.I. Automated staging of age-related macular degeneration using optical coherence tomography. Investig. Ophthalmol. Vis. Sci. 2017, 58, 2318–2328. [Google Scholar] [CrossRef]
- Hwang, D.K.; Hsu, C.C.; Chang, K.J.; Chao, D.; Sun, C.H.; Jheng, Y.C.; Yarmishyn, A.A.; Wu, J.C.; Tsai, C.Y.; Wang, M.L.; et al. Artificial intelligence-based decision-making for age-related macular degeneration. Theranostics 2019, 9, 232. [Google Scholar] [CrossRef]
- An, G.; Yokota, H.; Motozawa, N.; Takagi, S.; Mandai, M.; Kitahata, S.; Hirami, Y.; Takahashi, M.; Kurimoto, Y.; Akiba, M. Deep learning classification models built with two-step transfer learning for age related macular degeneration diagnosis. In Proceedings of the 2019 41st Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Berlin, Germany, 23–27 July 2019; pp. 2049–2052. [Google Scholar]
- Motozawa, N.; An, G.; Takagi, S.; Kitahata, S.; Mandai, M.; Hirami, Y.; Yokota, H.; Akiba, M.; Tsujikawa, A.; Takahashi, M.; et al. Optical coherence tomography-based deep-learning models for classifying normal and age-related macular degeneration and exudative and non-exudative age-related macular degeneration changes. Ophthalmol. Ther. 2019, 8, 527–539. [Google Scholar] [CrossRef]
- Treder, M.; Lauermann, J.L.; Eter, N. Automated detection of exudative age-related macular degeneration in spectral domain optical coherence tomography using deep learning. Graefe’s Arch. Clin. Exp. Ophthalmol. 2018, 256, 259–265. [Google Scholar] [CrossRef]
- Ambati, J.; Ambati, B.K.; Yoo, S.H.; Ianchulev, S.; Adamis, A.P. Age-related macular degeneration: Etiology, pathogenesis, and therapeutic strategies. Surv. Ophthalmol. 2003, 48, 257–293. [Google Scholar] [CrossRef]
- Lim, L.S.; Mitchell, P.; Seddon, J.M.; Holz, F.G.; Wong, T.Y. Age-related macular degeneration. Lancet 2012, 379, 1728–1738. [Google Scholar] [CrossRef]
- Yannuzzi, L.A.; Negrão, S.; Tomohiro, I.; Carvalho, C.; Rodriguez-Coleman, H.; Slakter, J.; Freund, K.B.; Sorenson, J.; Orlock, D.; Borodoker, N. Retinal angiomatous proliferation in age–related macular degeneration. Retina 2012, 32, 416–434. [Google Scholar] [CrossRef]
- Chakravarthy, U.; Wong, T.Y.; Fletcher, A.; Piault, E.; Evans, C.; Zlateva, G.; Buggage, R.; Pleil, A.; Mitchell, P. Clinical risk factors for age-related macular degeneration: A systematic review and meta-analysis. BMC Ophthalmol. 2010, 10, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Klein, R.; Klein, B.E.; Linton, K.L. Prevalence of age-related maculopathy: The Beaver Dam Eye Study. Ophthalmology 1992, 99, 933–943. [Google Scholar] [CrossRef]
- Leibowitz, H.M.; Krueger, D.; Maunder, L.R.; Milton, R.; Kini, M.; Kahn, H.; Nickerson, R.; Pool, J.; Colton, T.; Ganley, J.; et al. The Framingham Eye Study monograph: An ophthalmological and epidemiological study of cataract, glaucoma, diabetic retinopathy, macular degeneration, and visual acuity in a general population of 2631 adults, 1973–1975. Surv. Ophthalmol. 1980, 24, 335–610. [Google Scholar] [PubMed]
- Chou, R.; Dana, T.; Bougatsos, C.; Grusing, S.; Blazina, I. Screening for impaired visual acuity in older adults: Updated evidence report and systematic review for the US Preventive Services Task Force. JAMA 2016, 315, 915–933. [Google Scholar] [CrossRef] [PubMed]
- Adams, M.K.; Simpson, J.A.; Aung, K.Z.; Makeyeva, G.A.; Giles, G.G.; English, D.R.; Hopper, J.; Guymer, R.H.; Baird, P.N.; Robman, L.D. Abdominal obesity and age-related macular degeneration. Am. J. Epidemiol. 2011, 173, 1246–1255. [Google Scholar] [CrossRef]
- Dasari, B.; Prasanthi, J.R.; Marwarha, G.; Singh, B.B.; Ghribi, O. Cholesterol-enriched diet causes age-related macular degeneration-like pathology in rabbit retina. BMC Ophthalmol. 2011, 11, 1–11. [Google Scholar] [CrossRef]
- Sandberg, M.A.; Tolentino, M.J.; Miller, S.; Berson, E.L.; Gaudio, A.R. Hyperopia and neovascularization in age-related macular degeneration. Ophthalmology 1993, 100, 1009–1013. [Google Scholar] [CrossRef]
- Khan, J.; Shahid, H.; Thurlby, D.; Bradley, M.; Clayton, D.; Moore, A.; Bird, A.; Yates, J. Age related macular degeneration and sun exposure, iris colour, and skin sensitivity to sunlight. Br. J. Ophthalmol. 2006, 90, 29–32. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Feskanich, D.; Cho, E.; Schaumberg, D.A.; Colditz, G.A.; Hankinson, S.E. Menopausal and reproductive factors and risk of age-related macular degeneration. Arch. Ophthalmol. 2008, 126, 519–524. [Google Scholar] [CrossRef]
- Chong, E.W.T.; Kreis, A.J.; Wong, T.Y.; Simpson, J.A.; Guymer, R.H. Alcohol consumption and the risk of age-related macular degeneration: A systematic review and meta-analysis. Am. J. Ophthalmol. 2008, 145, 707–715. [Google Scholar] [CrossRef]
- Gopinath, B.; Flood, V.M.; Rochtchina, E.; Wang, J.J.; Mitchell, P. Homocysteine, folate, vitamin B-12, and 10-y incidence of age-related macular degeneration. Am. J. Clin. Nutr. 2013, 98, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Millen, A.E.; Voland, R.; Sondel, S.A.; Parekh, N.; Horst, R.L.; Wallace, R.B.; Hageman, G.S.; Chappell, R.; Blodi, B.A.; Klein, M.L.; et al. Vitamin D status and early age-related macular degeneration in postmenopausal women. Arch. Ophthalmol. 2011, 129, 481–489. [Google Scholar] [CrossRef]
- Wong, W.L.; Su, X.; Li, X.; Cheung, C.M.G.; Klein, R.; Cheng, C.Y.; Wong, T.Y. Global prevalence of age-related macular degeneration and disease burden projection for 2020 and 2040: A systematic review and meta-analysis. Lancet Glob. Health 2014, 2, e106–e116. [Google Scholar] [CrossRef]
- Victor, A.A. The Role of Imaging in Age-Related Macular Degeneration. In Visual Impairment and Blindness-What We Know and What We Have to Know; IntechOpen: London, UK, 2019. [Google Scholar]
- Ooto, S.; Hangai, M.; Tomidokoro, A.; Saito, H.; Araie, M.; Otani, T.; Kishi, S.; Matsushita, K.; Maeda, N.; Shirakashi, M.; et al. Effects of age, sex, and axial length on the three-dimensional profile of normal macular layer structures. Investig. Ophthalmol. Vis. Sci. 2011, 52, 8769–8779. [Google Scholar] [CrossRef] [PubMed]
- Keane, P.A.; Patel, P.J.; Liakopoulos, S.; Heussen, F.M.; Sadda, S.R.; Tufail, A. Evaluation of age-related macular degeneration with optical coherence tomography. Surv. Ophthalmol. 2012, 57, 389–414. [Google Scholar] [CrossRef]
- Ahlers, C.; Götzinger, E.; Pircher, M.; Golbaz, I.; Prager, F.; Schütze, C.; Baumann, B.; Hitzenberger, C.K.; Schmidt-Erfurth, U. Imaging of the retinal pigment epithelium in age-related macular degeneration using polarization-sensitive optical coherence tomography. Investig. Ophthalmol. Vis. Sci. 2010, 51, 2149–2157. [Google Scholar] [CrossRef] [PubMed]
- Ma, J.; Desai, R.; Nesper, P.; Gill, M.; Fawzi, A.; Skondra, D. Optical coherence tomographic angiography imaging in age-related macular degeneration. Ophthalmol. Eye Dis. 2017, 9, 1179172116686075. [Google Scholar] [CrossRef]
- Nagiel, A.; Sadda, S.R.; Sarraf, D. A promising future for optical coherence tomography angiography. JAMA Ophthalmol. 2015, 133, 629–630. [Google Scholar] [CrossRef] [PubMed]
- Burlina, P.M.; Joshi, N.; Pekala, M.; Pacheco, K.D.; Freund, D.E.; Bressler, N.M. Automated grading of age-related macular degeneration from color fundus images using deep convolutional neural networks. JAMA Ophthalmol. 2017, 135, 1170–1176. [Google Scholar] [CrossRef] [PubMed]
- Stahl, A. The Diagnosis and Treatment of Age-Related Macular Degeneration. Dtsch. ÄRzteblatt Int. 2020, 117, 513. [Google Scholar] [CrossRef]
- Bird, A.C.; Bressler, N.M.; Bressler, S.B.; Chisholm, I.H.; Coscas, G.; Davis, M.D.; de Jong, P.T.; Klaver, C.; Klein, B.; Klein, R.; et al. An international classification and grading system for age-related maculopathy and age-related macular degeneration. Surv. Ophthalmol. 1995, 39, 367–374. [Google Scholar] [CrossRef]
- Joachim, N.; Mitchell, P.; Burlutsky, G.; Kifley, A.; Wang, J.J. The incidence and progression of age-related macular degeneration over 15 years: The Blue Mountains Eye Study. Ophthalmology 2015, 122, 2482–2489. [Google Scholar] [CrossRef] [PubMed]
- Vitale, S.; Agrón, E.; Clemons, T.E.; Keenan, T.D.; Domalpally, A.; Danis, R.P.; Chew, E.Y. Association of 2-Year Progression Along the AREDS AMD Scale and Development of Late Age-Related Macular Degeneration or Loss of Visual Acuity: AREDS Report 41. JAMA Ophthalmol. 2020, 138, 610–617. [Google Scholar] [CrossRef] [PubMed]
- Coleman, H.R.; Chan, C.C.; Ferris III, F.L.; Chew, E.Y. Age-related macular degeneration. Lancet 2008, 372, 1835–1845. [Google Scholar] [CrossRef]
- Davis, M.D.; Gangnon, R.E.; Lee, L.Y.; Hubbard, L.D.; Klein, B.E.; Klein, R.; Ferris, F.L.; Bressler, S.B.; Milton, R.C.; Age-Related Eye Disease Study Group. The Age-Related Eye Disease Study severity scale for age-related macular degeneration: AREDS report no. 17. Arch. Ophthalmol. 2005, 123, 1484–1498. [Google Scholar] [PubMed]
- Age-Related Eye Disease Study Research Group. A randomized, placebo-controlled, clinical trial of high-dose supplementation with vitamins C and E, beta carotene, and zinc for age-related macular degeneration and vision loss: AREDS report no. 8. Arch. Ophthalmol. 2001, 119, 1417–1436. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.G.; Lee, S.C.; Seong, Y.S.; Kim, S.W.; Kwon, O.W. Optical coherence tomography. Yonsei Med. J. 2003, 44, 821–827. [Google Scholar] [CrossRef] [PubMed]
- Podoleanu, A.G. Optical sources for optical coherence tomography (OCT). In Lasers for Medical Applications; Elsevier: Amsterdam, The Netherlands, 2013; pp. 253–285. [Google Scholar]
- Fujimoto, J.G.; Pitris, C.; Boppart, S.A.; Brezinski, M.E. Optical coherence tomography: An emerging technology for biomedical imaging and optical biopsy. Neoplasia 2000, 2, 9–25. [Google Scholar] [CrossRef] [PubMed]
- De Carlo, T.E.; Romano, A.; Waheed, N.K.; Duker, J.S. A review of optical coherence tomography angiography (OCTA). Int. J. Retin. Vitr. 2015, 1, 5. [Google Scholar] [CrossRef] [PubMed]
- Hee, M.R.; Baumal, C.R.; Puliafito, C.A.; Duker, J.S.; Reichel, E.; Wilkins, J.R.; Coker, J.G.; Schuman, J.S.; Swanson, E.A.; Fujimoto, J.G. Optical coherence tomography of age-related macular degeneration and choroidal neovascularization. Ophthalmology 1996, 103, 1260–1270. [Google Scholar] [CrossRef]
- Pieroni, C.; Witkin, A.; Ko, T.; Fujimoto, J.; Chan, A.; Schuman, J.; Ishikawa, H.; Reichel, E.; Duker, J. Ultrahigh resolution optical coherence tomography in non-exudative age related macular degeneration. Br. J. Ophthalmol. 2006, 90, 191–197. [Google Scholar] [CrossRef]
- Sandhu, H.S.; Elmogy, M.; Sharafeldeen, A.T.; Elsharkawy, M.; El-Adawy, N.; Eltanboly, A.; Shalaby, A.; Keynton, R.; El-Baz, A. Automated diagnosis of diabetic retinopathy using clinical biomarkers, optical coherence tomography, and optical coherence tomography angiography. Am. J. Ophthalmol. 2020, 216, 201–206. [Google Scholar] [CrossRef] [PubMed]
- Sharafeldeen, A.; Elsharkawy, M.; Khalifa, F.; Soliman, A.; Ghazal, M.; AlHalabi, M.; Yaghi, M.; Alrahmawy, M.; Elmougy, S.; Sandhu, H.; et al. Precise higher-order reflectivity and morphology models for early diagnosis of diabetic retinopathy using OCT images. Sci. Rep. 2021, 11, 4730. [Google Scholar] [CrossRef]
- Gorczynska, I.; Srinivasan, V.J.; Vuong, L.N.; Chen, R.W.; Liu, J.J.; Reichel, E.; Wojtkowski, M.; Schuman, J.S.; Duker, J.S.; Fujimoto, J.G. Projection OCT fundus imaging for visualising outer retinal pathology in non-exudative age-related macular degeneration. Br. J. Ophthalmol. 2009, 93, 603–609. [Google Scholar] [CrossRef] [PubMed]
- Sikorski, B.L.; Bukowska, D.; Kaluzny, J.J.; Szkulmowski, M.; Kowalczyk, A.; Wojtkowski, M. Drusen with accompanying fluid underneath the sensory retina. Ophthalmology 2011, 118, 82–92. [Google Scholar] [CrossRef]
- Spaide, R.F.; Curcio, C.A. Drusen characterization with multimodal imaging. Retina (Philadelphia, Pa.) 2010, 30, 1441. [Google Scholar] [CrossRef] [PubMed]
- Klein, R.; Davis, M.D.; Magli, Y.L.; Segal, P.; Klein, B.E.; Hubbard, L. The Wisconsin age-related maculopathy grading system. Ophthalmology 1991, 98, 1128–1134. [Google Scholar] [CrossRef]
- Klein, R.; Meuer, S.M.; Knudtson, M.D.; Iyengar, S.K.; Klein, B.E. The epidemiology of retinal reticular drusen. Am. J. Ophthalmol. 2008, 145, 317–326. [Google Scholar] [CrossRef] [PubMed]
- Arnold, J.J.; Sarks, S.H.; Killingsworth, M.C.; Sarks, J.P. Reticular pseudodrusen. A risk factor in age-related maculopathy. Retina (Philadelphia, Pa.) 1995, 15, 183–191. [Google Scholar] [CrossRef]
- Cohen, S.Y.; Dubois, L.; Tadayoni, R.; Delahaye-Mazza, C.; Debibie, C.; Quentel, G. Prevalence of reticular pseudodrusen in age-related macular degeneration with newly diagnosed choroidal neovascularisation. Br. J. Ophthalmol. 2007, 91, 354–359. [Google Scholar] [CrossRef]
- Gass, J.D.M. Stereoscopic atlas of macular diseases. Diagn. Treat. 1997, 158–165. [Google Scholar]
- Gass, J. A clinicopathologic study of a peculiar foveomacular dystrophy. Trans. Am. Ophthalmol. Soc. 1974, 72, 139. [Google Scholar] [PubMed]
- Finger, R.P.; Issa, P.C.; Kellner, U.; Schmitz-Valckenberg, S.; Fleckenstein, M.; Scholl, H.P.; Holz, F.G. Spectral domain optical coherence tomography in adult-onset vitelliform macular dystrophy with cuticular drusen. Retina 2010, 30, 1455–1464. [Google Scholar] [CrossRef]
- Leng, T.; Rosenfeld, P.J.; Gregori, G.; Puliafito, C.A.; Punjabi, O.S. Spectral domain optical coherence tomography characteristics of cuticular drusen. Retina 2009, 29, 988–993. [Google Scholar] [CrossRef]
- Schmitz-Valckenberg, S.; Steinberg, J.S.; Fleckenstein, M.; Visvalingam, S.; Brinkmann, C.K.; Holz, F.G. Combined confocal scanning laser ophthalmoscopy and spectral-domain optical coherence tomography imaging of reticular drusen associated with age-related macular degeneration. Ophthalmology 2010, 117, 1169–1176. [Google Scholar] [CrossRef] [PubMed]
- Zweifel, S.A.; Spaide, R.F.; Curcio, C.A.; Malek, G.; Imamura, Y. Reticular pseudodrusen are subretinal drusenoid deposits. Ophthalmology 2010, 117, 303–312. [Google Scholar] [CrossRef] [PubMed]
- Freeman, S.R.; Kozak, I.; Cheng, L.; Bartsch, D.U.; Mojana, F.; Nigam, N.; Brar, M.; Yuson, R.; Freeman, W.R. Optical coherence tomography-raster scanning and manual segmentation in determining drusen volume in age-related macular degeneration. Retina 2010, 30, 431–435. [Google Scholar] [CrossRef]
- Gregori, G.; Wang, F.; Rosenfeld, P.J.; Yehoshua, Z.; Gregori, N.Z.; Lujan, B.J.; Puliafito, C.A.; Feuer, W.J. Spectral domain optical coherence tomography imaging of drusen in nonexudative age-related macular degeneration. Ophthalmology 2011, 118, 1373–1379. [Google Scholar] [CrossRef] [PubMed]
- Holz, F.G.; Pauleikhoff, D.; Klein, R.; Bird, A.C. Pathogenesis of lesions in late age-related macular disease. Am. J. Ophthalmol. 2004, 137, 504–510. [Google Scholar] [CrossRef]
- Sunness, J.S. The natural history of geographic atrophy, the advanced atrophic form of age-related macular degeneration. Mol. Vis. 1999, 5, 25. [Google Scholar]
- Wolf-Schnurrbusch, U.E.; Enzmann, V.; Brinkmann, C.K.; Wolf, S. Morphologic changes in patients with geographic atrophy assessed with a novel spectral OCT–SLO combination. Investig. Ophthalmol. Vis. Sci. 2008, 49, 3095–3099. [Google Scholar] [CrossRef]
- Brar, M.; Kozak, I.; Cheng, L.; Bartsch, D.U.G.; Yuson, R.; Nigam, N.; Oster, S.F.; Mojana, F.; Freeman, W.R. Correlation between spectral-domain optical coherence tomography and fundus autofluorescence at the margins of geographic atrophy. Am. J. Ophthalmol. 2009, 148, 439–444. [Google Scholar] [CrossRef] [PubMed]
- Lujan, B.J.; Rosenfeld, P.J.; Gregori, G.; Wang, F.; Knighton, R.W.; Feuer, W.J.; Puliafito, C.A. Spectral domain optical coherence tomographic imaging of geographic atrophy. Ophthalmic Surg. Lasers Imaging Retin. 2009, 40, 96–101. [Google Scholar] [CrossRef]
- Grossniklaus, H.E.; Green, W.R. Choroidal neovascularization. Am. J. Ophthalmol. 2004, 137, 496–503. [Google Scholar] [CrossRef]
- Green, W.R. Clinicopathologic studies of treated choroidal neovascular membranes. A review and report of two cases. Retina (Philadelphia, Pa.) 1991, 11, 328–356. [Google Scholar] [CrossRef]
- Green, W.R. Histopathology of age-related macular degeneration. Mol. Vis. 1999, 5, 1–10. [Google Scholar]
- Green, W.R.; Enger, C. Age-related macular degeneration histopathologic studies: The 1992 Lorenz E. Zimmerman Lecture. Ophthalmology 1993, 100, 1519–1535. [Google Scholar] [CrossRef]
- Matsui, M.; Tashiro, T.; Matsumoto, K.; Yamamoto, S. [A study on automatic and quantitative diagnosis of fundus photographs. I. Detection of contour line of retinal blood vessel images on color fundus photographs (author’s transl)]. Nippon Ganka Gakkai Zasshi 1973, 77, 907–918. [Google Scholar] [PubMed]
- Baudoin, C.; Lay, B.; Klein, J. Automatic detection of microaneurysms in diabetic fluorescein angiography. Revue d’épidémiologie et de santé publique 1984, 32, 254–261. [Google Scholar] [PubMed]
- Narasimha-Iyer, H.; Can, A.; Roysam, B.; Stewart, V.; Tanenbaum, H.L.; Majerovics, A.; Singh, H. Robust detection and classification of longitudinal changes in color retinal fundus images for monitoring diabetic retinopathy. IEEE Trans. Biomed. Eng. 2006, 53, 1084–1098. [Google Scholar] [CrossRef] [PubMed]
- Sleman, A.A.; Soliman, A.; Elsharkawy, M.; Giridharan, G.; Ghazal, M.; Sandhu, H.; Schaal, S.; Keynton, R.; Elmaghraby, A.; El-Baz, A. A novel 3D segmentation approach for extracting retinal layers from optical coherence tomography images. Med. Phys. 2021, 48, 1584–1595. [Google Scholar] [CrossRef]
- Quellec, G.; Lee, K.; Dolejsi, M.; Garvin, M.K.; Abramoff, M.D.; Sonka, M. Three-dimensional analysis of retinal layer texture: Identification of fluid-filled regions in SD-OCT of the macula. IEEE Trans. Med. Imaging 2010, 29, 1321–1330. [Google Scholar] [CrossRef]
- Liu, J.; Wong, D.; Lim, J.; Li, H.; Tan, N.; Zhang, Z.; Wong, T.; Lavanya, R. ARGALI: An automatic cup-to-disc ratio measurement system for glaucoma analysis using level-set image processing. In Proceedings of the 13th International Conference on Biomedical Engineering, Singapore, 3–6 December 2008; Springer: Berlin/Heidelberg, Germany, 2009; pp. 559–562. [Google Scholar]
- Huang, W.; Chan, K.L.; Li, H.; Lim, J.H.; Liu, J.; Wong, T.Y. A computer assisted method for nuclear cataract grading from slit-lamp images using ranking. IEEE Trans. Med Imaging 2010, 30, 94–107. [Google Scholar] [CrossRef]
- LeCun, Y.; Bengio, Y.; Hinton, G. Deep learning. Nature 2015, 521, 436–444. [Google Scholar] [CrossRef] [PubMed]
- Li, F.; Chen, H.; Liu, Z.; Zhang, X.; Wu, Z. Fully automated detection of retinal disorders by image-based deep learning. Graefe’s Arch. Clin. Exp. Ophthalmol. 2019, 257, 495–505. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.S.; Baughman, D.M.; Lee, A.Y. Deep learning is effective for classifying normal versus age-related macular degeneration OCT images. Ophthalmol. Retin. 2017, 1, 322–327. [Google Scholar] [CrossRef]
- García-Floriano, A.; Ferreira-Santiago, Á.; Camacho-Nieto, O.; Yáñez-Márquez, C. A machine learning approach to medical image classification: Detecting age-related macular degeneration in fundus images. Comput. Electr. Eng. 2019, 75, 218–229. [Google Scholar] [CrossRef]
- Tan, J.H.; Bhandary, S.V.; Sivaprasad, S.; Hagiwara, Y.; Bagchi, A.; Raghavendra, U.; Rao, A.K.; Raju, B.; Shetty, N.S.; Gertych, A.; et al. Age-related macular degeneration detection using deep convolutional neural network. Future Gener. Comput. Syst. 2018, 87, 127–135. [Google Scholar] [CrossRef]
- Burlina, P.M.; Joshi, N.; Pacheco, K.D.; Liu, T.A.; Bressler, N.M. Assessment of deep generative models for high-resolution synthetic retinal image generation of age-related macular degeneration. JAMA Ophthalmol. 2019, 137, 258–264. [Google Scholar] [CrossRef]
- Srinivasan, P.P.; Kim, L.A.; Mettu, P.S.; Cousins, S.W.; Comer, G.M.; Izatt, J.A.; Farsiu, S. Fully automated detection of diabetic macular edema and dry age-related macular degeneration from optical coherence tomography images. Biomed. Opt. Express 2014, 5, 3568–3577. [Google Scholar] [CrossRef]
- Hassan, T.; Akram, M.U.; Akhtar, M.; Khan, S.A.; Yasin, U. Multilayered deep structure tensor delaunay triangulation and morphing based automated diagnosis and 3D presentation of human macula. J. Med Syst. 2018, 42, 1–17. [Google Scholar] [CrossRef]
- Fraccaro, P.; Nicolo, M.; Bonetto, M.; Giacomini, M.; Weller, P.; Traverso, C.E.; Prosperi, M.; O’Sullivan, D. Combining macula clinical signs and patient characteristics for age-related macular degeneration diagnosis: A machine learning approach. BMC Ophthalmol. 2015, 15, 1–9. [Google Scholar] [CrossRef]
- Liu, Y.Y.; Ishikawa, H.; Chen, M.; Wollstein, G.; Duker, J.S.; Fujimoto, J.G.; Schuman, J.S.; Rehg, J.M. Computerized macular pathology diagnosis in spectral domain optical coherence tomography scans based on multiscale texture and shape features. Investig. Ophthalmol. Vis. Sci. 2011, 52, 8316–8322. [Google Scholar] [CrossRef]
- Ting, D.S.W.; Cheung, C.Y.L.; Lim, G.; Tan, G.S.W.; Quang, N.D.; Gan, A.; Hamzah, H.; Garcia-Franco, R.; San Yeo, I.Y.; Lee, S.Y.; et al. Development and validation of a deep learning system for diabetic retinopathy and related eye diseases using retinal images from multiethnic populations with diabetes. JAMA 2017, 318, 2211–2223. [Google Scholar] [CrossRef]
- Li, H.K. Telemedicine and ophthalmology. Surv. Ophthalmol. 1999, 44, 61–72. [Google Scholar] [CrossRef]
- Saleem, S.M.; Pasquale, L.R.; Sidoti, P.A.; Tsai, J.C. Virtual ophthalmology: Telemedicine in a COVID-19 era. Am. J. Ophthalmol. 2020, 216, 237–242. [Google Scholar] [CrossRef]
- Tanna, P.; Strauss, R.W.; Fujinami, K.; Michaelides, M. Stargardt disease: Clinical features, molecular genetics, animal models and therapeutic options. Br. J. Ophthalmol. 2017, 101, 25–30. [Google Scholar] [CrossRef]
- Rahman, N.; Georgiou, M.; Khan, K.N.; Michaelides, M. Macular dystrophies: Clinical and imaging features, molecular genetics and therapeutic options. Br. J. Ophthalmol. 2020, 104, 451–460. [Google Scholar] [CrossRef]
- Spaide, R.F.; Jaffe, G.J.; Sarraf, D.; Freund, K.B.; Sadda, S.R.; Staurenghi, G.; Waheed, N.K.; Chakravarthy, U.; Rosenfeld, P.J.; Holz, F.G.; et al. Consensus nomenclature for reporting neovascular age-related macular degeneration data: Consensus on neovascular age-related macular degeneration nomenclature study group. Ophthalmology 2020, 127, 616–636. [Google Scholar] [CrossRef]
| Study | Methodology | Year | # of Grades | Weakness | # of Images |
|---|---|---|---|---|---|
| An et al. [5] | Develop deep learning techniques using OCT images to AMD classification | 2019 | They are able to differentiate between AMD with fluids and AMD without fluids | They cannot differentiate between all AMD grades | 1625 |
| Motozawa et al. [6] | Separate DL methods tailored to active wet AMD and inactive wet AMD | 2019 | They are able to distinguish between normal cases and active wet AMD in addition to inactive wet AMD. | They cannot identify the early stages of AMD | 1621 |
| Treder et al. [7] | Pretrained InceptionV3 DCNN, multiple computational layers are used to process the input image | 2018 | They are able to differentiate between healthy and exudative AMD cases | Wet AMD can present with no exudation | 1112 |
| Lee et al. [79] | A modified VGG19 DCNN with changed the last fully connected layer to be more adjustable with the two output classes | 2017 | They are able to differentiate between normal and AMD cases | They cannot differentiate between all AMD grades | 43,328 |
| Garcia et al. [80] | Combining mathematical Morphology, Image Processing, and a reliable and effective ML model: a Support Vector Machine (SVM) | 2019 | They differentiated between healthy and AMD with drusen | Drusen have different sizes which indicates that this is early or intermediate AMD | 397 |
| Tan et al. [81] | Develop a deep convolutional neural network (CNN) model capable of detecting AMD autonomously and accurately at the earliest stage | 2018 | They differentiated between dry and wet AMD | Dry AMD can be in either early or intermediate form and wet AMD can be active or inactive | 1110 |
| Hwang et al. [4] | Three pretrained CNN (VGG16, InceptionV3, ResNet50) are used for diagnosis and proposed treatment of AMD | 2019 | They differentiated between healthy, dry, active wet and in active wet AMD | Dry AMD can be in either early or intermediate form or in its advanced form (GA) | 35,900 |
| Li et al. [78] | Investigate how deep learning methods built on the VGG-16 network can enhance OCT’s ability to classify AMD and DME | 2019 | They differentiated between normal, drusen, CNV and DME | CNV can itself be active or inactive and drusen can be in an earlier form or an intermediate form or in an advanced form (GA) | 109,312 |
| Burlina et al. [82] | Generational adversarial networks (GAN) trained on Age-Related Eye Disease Study (AREDS) color fundus images | 2019 | They distinguished between early, intermediate, and Advanced Stage of AMD | CFP cannot identify subtle amounts of IRF or SRF, early discontinuities of the outer retinal layers or RPE | 133,821 |
| Srinivasan et al. [83] | Support vector machines based on multiscale histograms of oriented gradient descriptors are employed as feature vectors | 2014 | They distinguished between healthy, Dry AMD, and DME | They cannot identify wet AMD; in addition, dry AMD can be in either early or intermediate form or in its advanced form (GA) | 90 |
| Hassan et al. [84] | CNNs with multilayered structures that perform Delaunay triangulation and morphing to extract nine layers of retina and choroidal tissue along with macular fluids are employed in this fully autonomous system. | 2018 | They distinguished between normal, dry AMD, and wet AMD | Wet AMD can be active or inactive; in addition, dry AMD can be in either early or intermediate form or in its advanced form (GA) | 46,913 |
| Fraccaro et al. [85] | Models for diagnosing AMD involved a combination of white box methodologies such as logistic regression and decision trees and black box methodologies such as SVM, random forests, and AdaBoost | 2015 | They distinguished between normal, dry AMD, and wet AMD | Wet AMD can be active or inactive; in addition, dry AMD can be in either early or intermediate form or in its advanced form (GA) | 974 |
| Liu et al. [86] | Two SVM classifiers are used to train the OCTs to identify three retinal diseases (AMD, macular hole, macular edema) | 2011 | They were able to distinguish between normal and AMD cases | They cannot identify or grade each type of AMD | 326 |
| Burlina et al. [30] | DL and DCNN were utilized to train fundus images to solve 2-class AMD problem (no/early AMD vs. advanced AMD) | 2017 | They are able to differentiate between early AMD and advanced AMD | They cannot identify the intermediate stage of AMD in addition to the advanced AMD may contain active wet or inactive wet AMD | 67,401 |
| Ting et al. [87] | DL system was used to train the OCT images to diagnose three different eye disease(diabetic retinopathy (DR), glaucoma, and AMD) | 2017 | They are able to identify intermediate AMD according to AREDS grading system | They cannot identify all categories of AMD | 108,558 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Elsharkawy, M.; Elrazzaz, M.; Ghazal, M.; Alhalabi, M.; Soliman, A.; Mahmoud, A.; El-Daydamony, E.; Atwan, A.; Thanos, A.; Sandhu, H.S.; et al. Role of Optical Coherence Tomography Imaging in Predicting Progression of Age-Related Macular Disease: A Survey. Diagnostics 2021, 11, 2313. https://doi.org/10.3390/diagnostics11122313
Elsharkawy M, Elrazzaz M, Ghazal M, Alhalabi M, Soliman A, Mahmoud A, El-Daydamony E, Atwan A, Thanos A, Sandhu HS, et al. Role of Optical Coherence Tomography Imaging in Predicting Progression of Age-Related Macular Disease: A Survey. Diagnostics. 2021; 11(12):2313. https://doi.org/10.3390/diagnostics11122313
Chicago/Turabian StyleElsharkawy, Mohamed, Mostafa Elrazzaz, Mohammed Ghazal, Marah Alhalabi, Ahmed Soliman, Ali Mahmoud, Eman El-Daydamony, Ahmed Atwan, Aristomenis Thanos, Harpal Singh Sandhu, and et al. 2021. "Role of Optical Coherence Tomography Imaging in Predicting Progression of Age-Related Macular Disease: A Survey" Diagnostics 11, no. 12: 2313. https://doi.org/10.3390/diagnostics11122313
APA StyleElsharkawy, M., Elrazzaz, M., Ghazal, M., Alhalabi, M., Soliman, A., Mahmoud, A., El-Daydamony, E., Atwan, A., Thanos, A., Sandhu, H. S., Giridharan, G., & El-Baz, A. (2021). Role of Optical Coherence Tomography Imaging in Predicting Progression of Age-Related Macular Disease: A Survey. Diagnostics, 11(12), 2313. https://doi.org/10.3390/diagnostics11122313










