Prevalence and Impact of Reported Drug Allergies among Rheumatology Patients
Abstract
1. Introduction
2. Methods
3. Statistical Analysis
4. Results
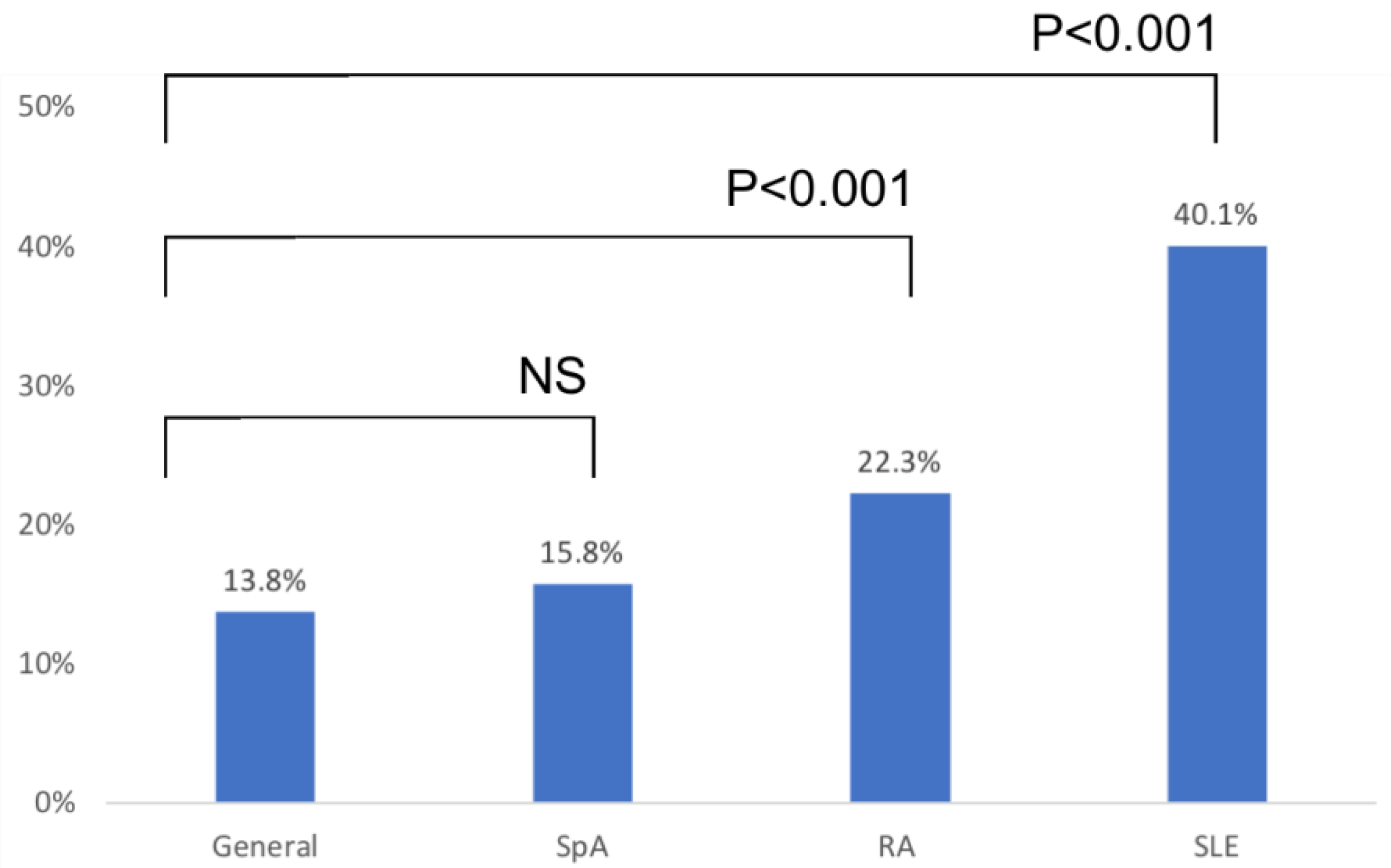
4.1. Prevalence of Reported DA Was Significantly Higher among Rheumatology Patients, Affecting 40.1% of SLE Patients and 22.3% of RA Patients
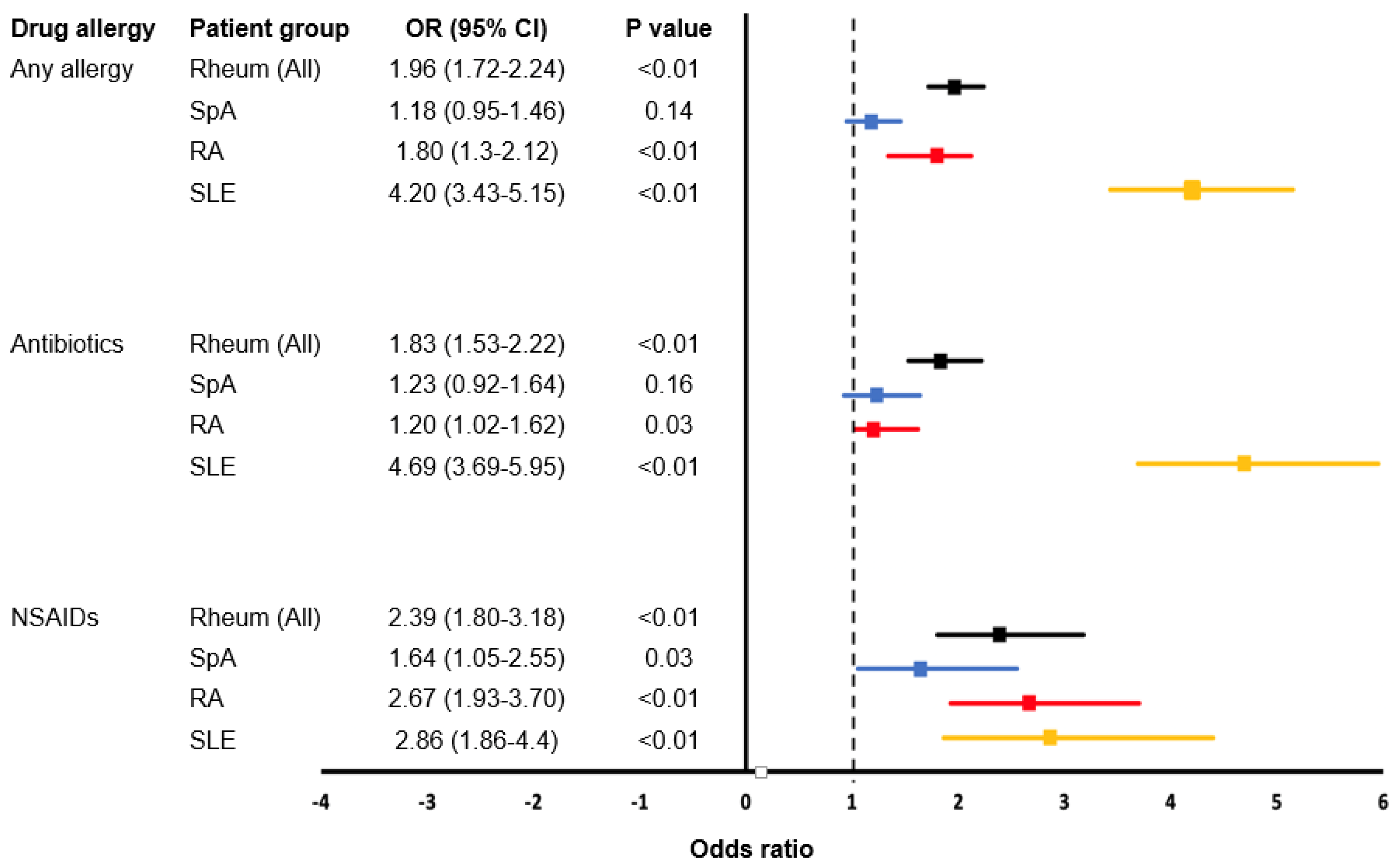
4.2. Antibiotics (Especially Beta-Lactams) and NSAID Were the Most Frequently Reported DA among Rheumatology Patients, and Significantly More Than Controls
4.3. Reported Antibiotic DA Was Independently Associated with Increased Rate of Infection-Related Admissions
4.4. Drug Allergy Testing Was Useful, and Genuine BL Allergy Was Infrequent among Rheumatology Patients
5. Discussion
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Li, P.H.; Yeung, H.H.F.; Lau, C.S.; Au, E.Y.L. Prevalence, Incidence, and Sensitization Profile of beta-lactam Antibiotic Allergy in Hong Kong. JAMA Netw. Open 2020, 3, e204199. [Google Scholar] [CrossRef]
- Mayer, P.; Sivakumar, N.; Pritz, M.; Varga, M.; Mehmann, A.; Lee, S.; Salvatore, A.; Magno, M.; Pharr, M.; Johannssen, H.C.; et al. Flexible and Lightweight Devices for Wireless Multi-Color Optogenetic Experiments Controllable via Commercial Cell Phones. Front. Neurosci. 2019, 13. [Google Scholar] [CrossRef] [PubMed]
- Blumenthal, K.G.; Peter, J.G.; Trubiano, J.A.; Phillips, E.J. Antibiotic allergy. Lancet 2019, 393, 183–198. [Google Scholar] [CrossRef]
- Zhou, L.; Dhopeshwarkar, N.; Blumenthal, K.G.; Goss, F.; Topaz, M.; Slight, S.P.; Bates, D.W. Drug allergies documented in electronic health records of a large healthcare system. Allergy 2016, 71, 1305–1313. [Google Scholar] [CrossRef] [PubMed]
- Macy, E.; Ho, N.J. Multiple drug intolerance syndrome: Prevalence, clinical characteristics, and management. Ann. Allergy Asthma Immunol. 2012, 108, 88–93. [Google Scholar] [CrossRef] [PubMed]
- Gomes, E.; Cardoso, M.F.; Praca, F.; Gomes, L.; Marino, E.; Demoly, P. Self-reported drug allergy in a general adult Portuguese population. Clin. Exp. Allergy 2004, 34, 1597–1601. [Google Scholar] [CrossRef] [PubMed]
- Torres, M.J.; Montanez, M.I.; Ariza, A.; Salas, M.; Fernandez, T.D.; Barbero, N.; Mayorga, C.; Blanca, M. The role of IgE recognition in allergic reactions to amoxicillin and clavulanic acid. Clin. Exp. Allergy 2016, 46, 264–274. [Google Scholar] [CrossRef] [PubMed]
- Leru, P.M.; Leontescu, A.; Stefan, I.; Nedelea, I.; Ceausu, I.; Antoine, E. Drug allergies interpretation based on patient’s history alone may have therapeutic consequences in hospital setting. Rom. J. Mil. Med. 2019, 122, 101–105. [Google Scholar]
- Mattingly, T.J., 2nd; Fulton, A.; Lumish, R.A.; Williams, A.M.C.; Yoon, S.; Yuen, M.; Heil, E.L. The Cost of Self-Reported Penicillin Allergy: A Systematic Review. J. Allergy Clin. Immunol. Pract. 2018, 6, 1649–1654.e4. [Google Scholar] [CrossRef]
- MacFadden, D.R.; LaDelfa, A.; Leen, J.; Gold, W.L.; Daneman, N.; Weber, E.; Al-Busaidi, I.; Petrescu, D.; Saltzman, I.; Devlin, M.; et al. Impact of Reported Beta-Lactam Allergy on Inpatient Outcomes: A Multicenter Prospective Cohort Study. Clin. Infect. Dis. 2016, 63, 904–910. [Google Scholar] [CrossRef]
- Macy, E.; Contreras, R. Health care use and serious infection prevalence associated with penicillin “allergy” in hospitalized patients: A cohort study. J. Allergy Clin. Immunol. 2014, 133, 790–796. [Google Scholar] [CrossRef]
- Macy, E. Addressing the epidemic of antibiotic “allergy” over-diagnosis. Ann. Allergy Asthma Immunol. 2020, 124, 550–557. [Google Scholar] [CrossRef]
- Charneski, L.; Deshpande, G.; Smith, S.W. Impact of an antimicrobial allergy label in the medical record on clinical outcomes in hospitalized patients. Pharmacotherapy 2011, 31, 742–747. [Google Scholar] [CrossRef] [PubMed]
- Siew, L.Q.C.; Li, P.H.; Watts, T.J.; Thomas, I.; Ue, K.L.; Caballero, M.R.; Rutkowski, K.; Till, S.J.; Pillai, P.; Haque, R. Identifying Low-Risk Beta-Lactam Allergy Patients in a UK Tertiary Centre. J. Allergy Clin. Immunol. Pract. 2019, 7, 2173–2181.e1. [Google Scholar] [CrossRef] [PubMed]
- Thong, B.Y.; Tan, T.C. Epidemiology and risk factors for drug allergy. Br. J. Clin Pharmacol. 2011, 71, 684–700. [Google Scholar] [CrossRef]
- Dona, I.; Barrionuevo, E.; Blanca-Lopez, N.; Torres, M.J.; Fernandez, T.D.; Mayorga, C.; Canto, G.; Blanca, M. Trends in hypersensitivity drug reactions: More drugs, more response patterns, more heterogeneity. J. Investig. Allergol. Clin. Immunol. 2014, 24, 143–153, quiz 141 p following 153. [Google Scholar]
- Williams, B.O.; St Onge, R.A.; Young, A.; Nuki, G.; Dick, W.C.; Whaley, K. Penicillin allergy in rheumatoid arthritis. With special reference to Sjogren’s syndrome. Ann. Rheum Dis. 1969, 28, 607–611. [Google Scholar] [CrossRef]
- Littlejohns, D.W. Drug allergy in rheumatology. Rheumatol. Phys. Med. 1972, 11, 435–436. [Google Scholar] [CrossRef]
- Pope, J.; Jerome, D.; Fenlon, D.; Krizova, A.; Ouimet, J. Frequency of adverse drug reactions in patients with systemic lupus erythematosus. J. Rheumatol. 2003, 30, 480–484. [Google Scholar]
- Aceves-Avila, F.J.; Benites-Godinez, V. Drug allergies may be more frequent in systemic lupus erythematosus than in rheumatoid arthritis. J. Clin. Rheumatol. 2008, 14, 261–263. [Google Scholar] [CrossRef]
- Brockow, K.; Garvey, L.H.; Aberer, W.; Atanaskovic-Markovic, M.; Barbaud, A.; Bilo, M.B.; Bircher, A.; Blanca, M.; Bonadonna, B.; Campi, P.; et al. Skin test concentrations for systemically administered drugs—An ENDA/EAACI Drug Allergy Interest Group position paper. Allergy 2013, 68, 702–712. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Safety of Medicines: A Guide to Detecting and Reporting Adverse Drug Reactions; World Health Organization: Geneva, Switzerland, 2002. [Google Scholar]
- Johansson, S.G.; Bieber, T.; Dahl, R.; Friedmann, P.S.; Lanier, B.Q.; Lockey, R.F.; Motala, C.; Ortega Martell, J.A.; Platts-Mills, T.A.; Ring, J.; et al. Revised nomenclature for allergy for global use: Report of the Nomenclature Review Committee of the World Allergy Organization, October 2003. J. Allergy Clin. Immunol. 2004, 113, 832–836. [Google Scholar] [CrossRef]
- Lai, N.S.; Tsai, T.Y.; Koo, M.; Lu, M.C. Association of rheumatoid arthritis with allergic diseases: A nationwide population-based cohort study. Allergy Asthma Proc. 2015, 36, 99–103. [Google Scholar] [CrossRef]
- Chang, W.P.; Kuo, C.N.; Kuo, L.N.; Wang, Y.T.; Perng, W.T.; Kuo, H.C.; Wei, J.C. Increase risk of allergic diseases in patients with ankylosing spondylitis: A 10-year follow-up population-based study in Taiwan. Medicine (Baltimore) 2016, 95, e5172. [Google Scholar] [CrossRef]
- Sequeira, J.F.; Cesic, D.; Keser, G.; Bukelica, M.; Karanagnostis, S.; Khamashta, M.A.; Hughes, G.R. Allergic disorders in systemic lupus erythematosus. Lupus 1993, 2, 187–191. [Google Scholar] [CrossRef]
- Jeong, H.E.; Jung, S.M.; Cho, S.I. Association between Rheumatoid Arthritis and Respiratory Allergic Diseases in Korean Adults: A Propensity Score Matched Case-Control Study. Int. J. Rheumatol. 2018, 2018, 3798124. [Google Scholar] [CrossRef]
- Sin, E.; Anand, P.; Frieri, M. A link: Allergic rhinitis, Asthma & Systemic Lupus Erythematosus. Autoimmun. Rev. 2016, 15, 487–491. [Google Scholar] [CrossRef]
- Khan, D.A.; Solensky, R. Drug allergy. J. Allergy Clin. Immunol. 2010, 125, S126–S137. [Google Scholar] [CrossRef]
- Eaddy Norton, A.; Broyles, A.D. Drug allergy in children and adults: Is it the double X chromosome? Ann. Allergy Asthma Immunol. 2019, 122, 148–155. [Google Scholar] [CrossRef]
- Konstantinou, G.N.; Asero, R.; Ferrer, M.; Knol, E.F.; Maurer, M.; Raap, U.; Schmid-Grendelmeier, P.; Skov, P.S.; Grattan, C.E. EAACI taskforce position paper: Evidence for autoimmune urticaria and proposal for defining diagnostic criteria. Allergy 2013, 68, 27–36. [Google Scholar] [CrossRef]
- Kolkhir, P.; Church, M.K.; Weller, K.; Metz, M.; Schmetzer, O.; Maurer, M. Autoimmune chronic spontaneous urticaria: What we know and what we do not know. J Allergy Clin Immunol 2017, 139, 1772–1781.e1. [Google Scholar] [CrossRef]
- Bracken, S.J.; Abraham, S.; MacLeod, A.S. Autoimmune Theories of Chronic Spontaneous Urticaria. Front. Immunol. 2019, 10, 627. [Google Scholar] [CrossRef]
- Dema, B.; Pellefigues, C.; Hasni, S.; Gault, N.; Jiang, C.; Ricks, T.K.; Bonelli, M.M.; Scheffel, J.; Sacre, K.; Jablonski, M.; et al. Autoreactive IgE is prevalent in systemic lupus erythematosus and is associated with increased disease activity and nephritis. PLoS ONE 2014, 9, e90424. [Google Scholar] [CrossRef] [PubMed]
- Leru, P.M.; Deleanu, D.M. Romanian Allergology in the actual European context. Rom. J. Intern. Med. 2015, 53, 111–117. [Google Scholar] [CrossRef]
- Lee, T.H.; Leung, T.F.; Wong, G.; Ho, M.; Duque, J.R.; Li, P.H.; Lau, C.S.; Lam, W.F.; Wu, A.; Chan, E.; et al. The unmet provision of allergy services in Hong Kong impairs capability for allergy prevention-implications for the Asia Pacific region. Asian Pac. J. Allergy Immunol. 2019, 37, 1–8. [Google Scholar] [CrossRef]
- Li, P.H.; Watts, T.J.; Lui, M.S.; Lau, C.S.; Chung, H.Y. Recall Urticaria in Adalimumab Hypersensitivity. J Allergy Clin. Immunol. Pract. 2018, 6, 1032–1033. [Google Scholar] [CrossRef]
- Li, P.H.; Watts, T.J.; Chung, H.Y.; Lau, C.S. Fixed Drug Eruption to Biologics and Role of Lesional Patch Testing. J. Allergy Clin. Immunol. Pract. 2019, 7, 2398–2399. [Google Scholar] [CrossRef]
| All Patients (N = 6081) | ||||
| Total | No drug allergy | Drug allergy | p value | |
| Number | 6081 | 4988 (82.0%) | 1093 (18.0%) | |
| Age (years) | 64.6 ± 18.0 | 64.7 ± 18.3 | 63.7 ± 16.0 | 0.06 |
| Male | 2393 (39.4%) | 2089 (41.9%) | 304 (27.8%) | <0.01 |
| Controls (N = 3540) | ||||
| Total | No drug allergy | Drug allergy | p value | |
| Number | 3540 | 3053 (86.2%) | 487 (13.8%) | |
| Age (years) | 71.3 ± 17.6 | 71.4 ± 17.7 | 71.0 ± 17.0 | 0.65 |
| Male | 1649 (46.6%) | 1458 (47.8%) | 191 (39.2%) | <0.01 |
| Rheumatology patients (N = 2541) | ||||
| Total | No drug allergy | Drug allergy | p value | |
| Number | 2541 | 1935 (76.2%) | 606 (23.8%) | |
| Age (years) | 55.2 ± 13.8 | 54.3 ± 14.1 | 57.9 ± 12.5 | <0.01 |
| Male | 744 (29.3%) | 631 (32.6%) | 113 (18.6%) | <0.01 |
| Rheumatoid arthritis (N = 1286) | ||||
| Total | No drug allergy | Drug allergy | p value | |
| Number | 1286 | 999 (77.7%) | 287 (22.3%) | |
| Age (years) | 58.9 ± 12.1 | 58.2 ± 12.2 | 61.3 ± 11.8 | <0.01 |
| Male | 228 (17.7%) | 189 (18.9%) | 39 (13.6%) | 0.04 |
| Spondyloarthritis (N = 759) | ||||
| Total | No drug allergy | Drug allergy | p value | |
| Number | 759 | 639 (84.2%) | 120 (15.8%) | |
| Age (years) | 49.5 ± 15.0 | 48.8 ± 15.0 | 53.3 ± 14.2 | <0.01 |
| Male | 473 (62.3%) | 416 (65.1%) | 57 (47.5%) | <0.01 |
| Systemic lupus erythematosus (N = 496) | ||||
| Total | No drug allergy | Drug allergy | p value | |
| Number | 496 | 297 (59.9%) | 199 (40.1%) | |
| Age (years) | 54.1 ± 12.7 | 53.0 ± 13.6 | 55.7 ± 11.1 | 0.01 |
| Male | 43 (8.7%) | 17 (8.5%) | 26 (8.8%) | 0.94 |
| Rheumatology Patients (N = 2541) | Controls (N = 3540) | ||||||
|---|---|---|---|---|---|---|---|
| RA | SLE | SpA | Total | % | Total | % | |
| Any antibiotics | 113 | 129 | 64 | 306 | 12 | 247 | 7 |
| Beta-lactam antibiotics | 69 | 82 | 43 | 194 | 7.6 | 170 | 4.8 |
| Non-steroidal anti-inflammatory drugs | 73 | 30 | 27 | 130 | 5.1 | 78 | 2.2 |
| Disease-modifying antirheumatic drugs/immunosuppressants | 79 | 19 | 15 | 113 | 4.4 | 0 | 0 |
| Cardiovascular drugs | 42 | 19 | 4 | 65 | 2.6 | 59 | 1.7 |
| Intravenous contrast | 14 | 11 | 8 | 33 | 1.3 | 41 | 1.2 |
| Other analgesics | 16 | 6 | 8 | 30 | 1.2 | 12 | 0.3 |
| Allopurinol | 3 | 4 | 1 | 8 | 0.3 | 17 | 0.5 |
| Anti-fungal | 4 | 2 | 2 | 8 | 0.3 | 4 | 0.1 |
| Anti-virals | 3 | 4 | 0 | 7 | 0.3 | 3 | 0.1 |
| Rheumatology Patients (N = 2541) | ||||||
|---|---|---|---|---|---|---|
| Univariate | Multivariate | |||||
| Admission | No Admission | OR (95%CI) | p Value | OR (95%CI) | p Value | |
| Number of patients | 103 (4.1%) | 2438 (95.9%) | ------ | ------ | ------ | ------ |
| Age | 62.0 ± 14.5 | 54.9 ± 13.7 | ------ | <0.01 | 1.04 (1.03–1.06) | <0.01 |
| Male | 33 (32.0%) | 711 (29.2%) | 1.15 (0.75–1.75) | 0.53 | ------ | ------ |
| RA | 52 (50.5%) | 1234 (50.6%) | 1.00 (0.67–1.48) | 0.98 | ------ | ------ |
| SpA | 26 (25.2%) | 733 (30.1%) | 0.79 (0.50–1.24) | 0.30 | ------ | ------ |
| SLE | 25 (24.3%) | 471 (19.3%) | 1.34 (0.84–2.12) | 0.21 | ------ | ------ |
| Reported DA | ||||||
| Antibiotics | 21 (20.4%) | 285 (11.7%) | 1.94 (1.18–3.17) | 0.01 | 1.79 (1.09–2.95) | 0.02 |
| NSAIDs | 9 (8.7%) | 121 (5.0%) | 1.83 (0.90–3.72) | 0.09 | ------ | ------ |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chan, S.C.W.; Yeung, W.W.Y.; Wong, J.C.Y.; Chui, E.S.H.; Lee, M.S.H.; Chung, H.Y.; Cheung, T.T.; Lau, C.S.; Li, P.H. Prevalence and Impact of Reported Drug Allergies among Rheumatology Patients. Diagnostics 2020, 10, 918. https://doi.org/10.3390/diagnostics10110918
Chan SCW, Yeung WWY, Wong JCY, Chui ESH, Lee MSH, Chung HY, Cheung TT, Lau CS, Li PH. Prevalence and Impact of Reported Drug Allergies among Rheumatology Patients. Diagnostics. 2020; 10(11):918. https://doi.org/10.3390/diagnostics10110918
Chicago/Turabian StyleChan, Shirley Chiu Wai, Winnie Wan Yin Yeung, Jane Chi Yan Wong, Ernest Sing Hong Chui, Matthew Shing Him Lee, Ho Yin Chung, Tommy Tsang Cheung, Chak Sing Lau, and Philip Hei Li. 2020. "Prevalence and Impact of Reported Drug Allergies among Rheumatology Patients" Diagnostics 10, no. 11: 918. https://doi.org/10.3390/diagnostics10110918
APA StyleChan, S. C. W., Yeung, W. W. Y., Wong, J. C. Y., Chui, E. S. H., Lee, M. S. H., Chung, H. Y., Cheung, T. T., Lau, C. S., & Li, P. H. (2020). Prevalence and Impact of Reported Drug Allergies among Rheumatology Patients. Diagnostics, 10(11), 918. https://doi.org/10.3390/diagnostics10110918







