Choice of Antiplatelet vs. Anticoagulant for Blunt Cerebrovascular Injury
Abstract
1. Introduction
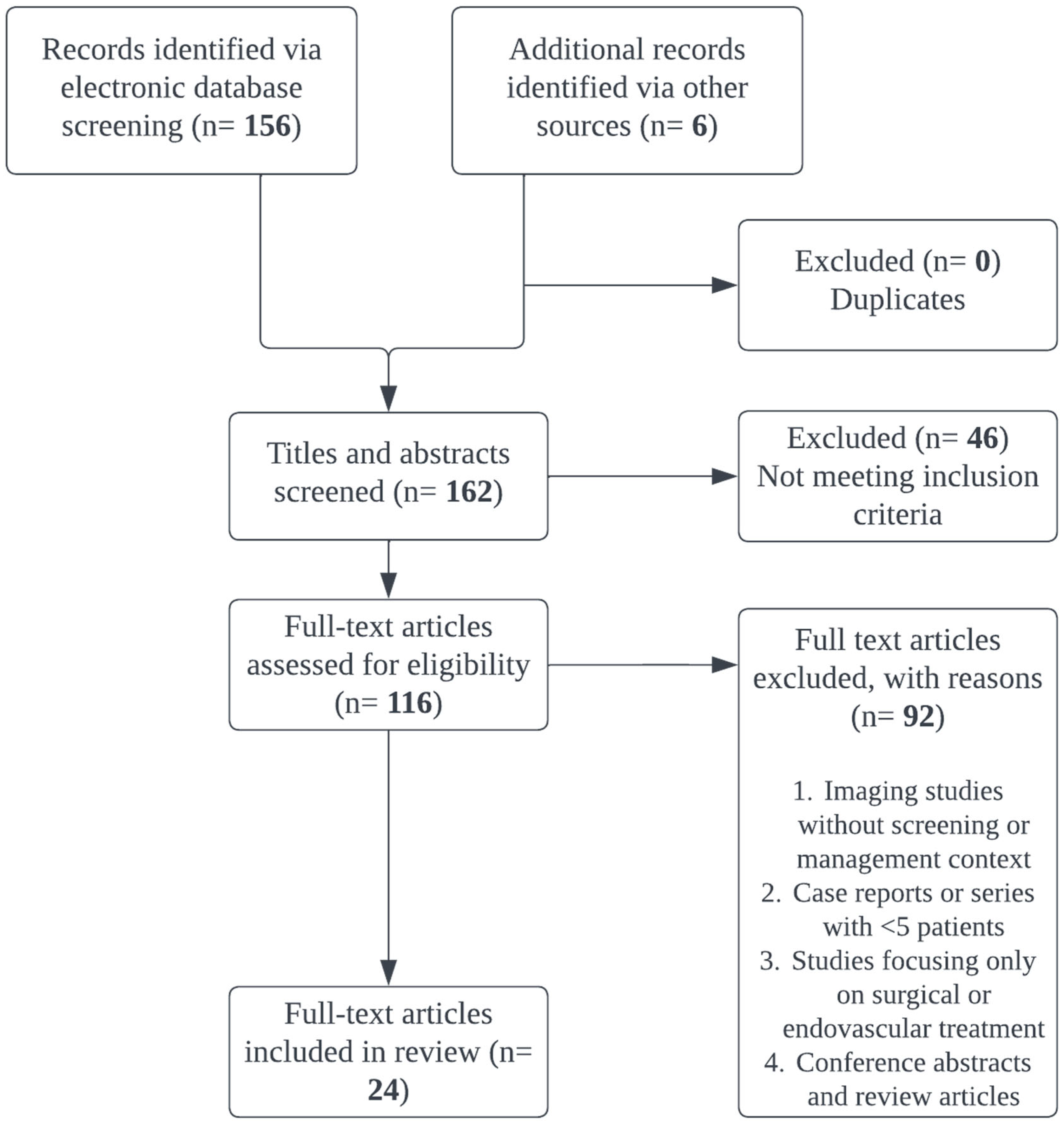
2. Materials and Methods
3. Discussion
3.1. Overview of BCVI
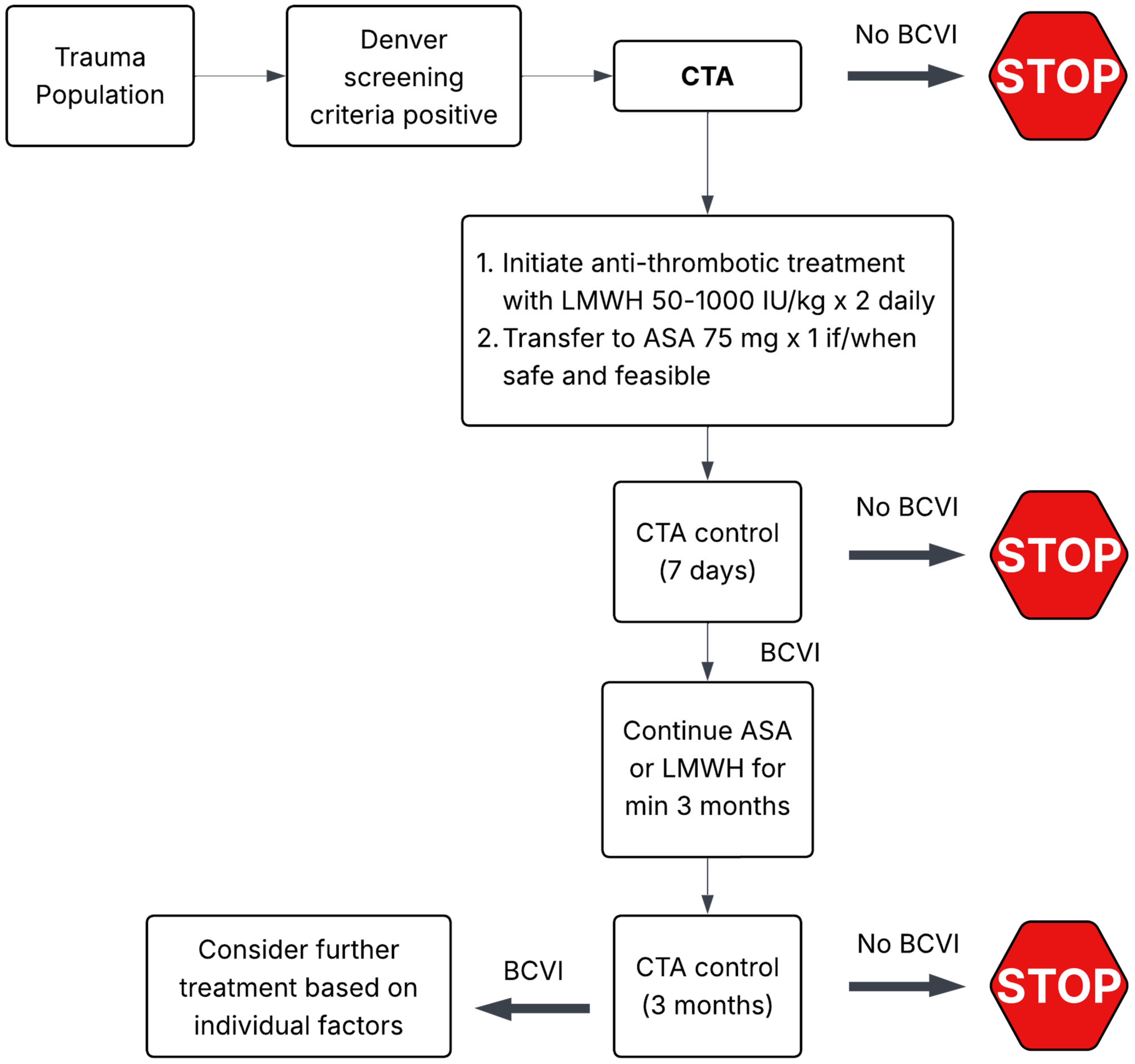
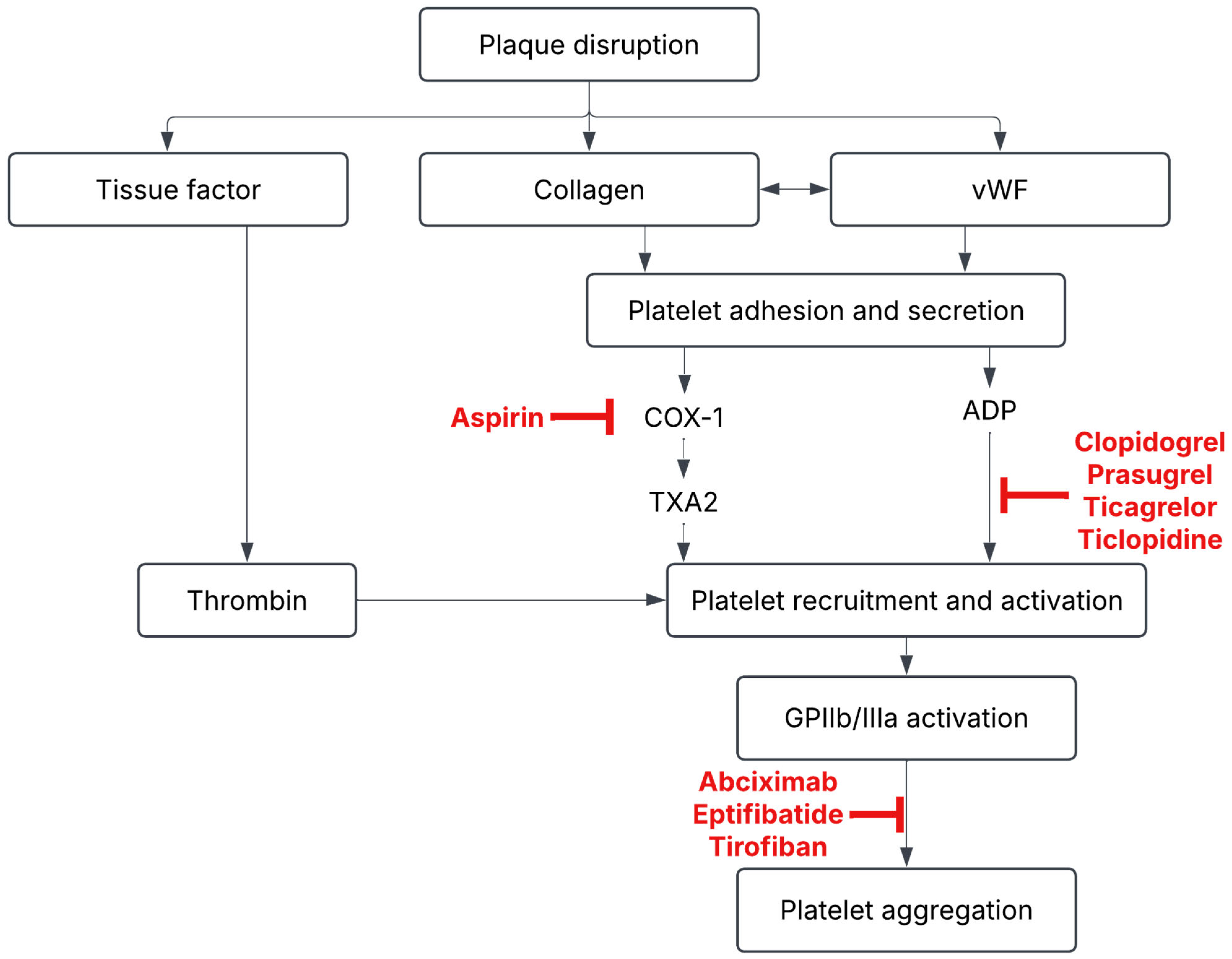
3.2. Medical Management of BCVI
3.3. Comparison of Anticoagulation and Antiplatelet
3.4. Pediatric BCVI Treatment
3.5. Elderly BCVI Treatment
3.6. Polytrauma BCVI Treatment
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| BCVI | Blunt Cerebrovascular Injury |
| DOAC | Dual Oral Anticoagulants |
| ICA | Internal Carotid Artery |
| TBI | Traumatic Brain Injury |
| CCF | Carotid-Cavernous Fistulas |
| WTA | Western Trauma Association |
| EAST | Eastern Association for the Surgery of Trauma |
| CTA | Computed Tomography Angiography |
| MRA | Magnetic Resonance Angiography |
| DSA | Digital Subtraction Angiography |
| ASA | Aspirin |
| COX | Cyclooxygenase |
| UFH | Unfractionated Heparin |
| LMWH | Low Molecular Weight Heparin |
| AHA/ASA | American Heart Association/American Stroke Association |
| CVA | Cerebrovascular Accident |
References
- Bonow, R.H.; Witt, C.E.; Mosher, B.P.; Mossa-Basha, M.; Vavilala, M.S.; Rivara, F.P.; Cuschieri, J.; Arbabi, S.; Chesnut, R.M. Transcranial Doppler Microemboli Monitoring for Stroke Risk Stratification in Blunt Cerebrovascular Injury. Crit. Care Med. 2017, 45, e1011–e1017. [Google Scholar] [CrossRef] [PubMed]
- Stein, D.M.; Boswell, S.; Sliker, C.W.; Lui, F.Y.; Scalea, T.M. Blunt cerebrovascular injuries: Does treatment always matter? J. Trauma 2009, 66, 132–144. [Google Scholar] [CrossRef]
- Cothren, C.C.; Biffl, W.L.; Moore, E.E.; Kashuk, J.L.; Johnson, J.L. Treatment for blunt cerebrovascular injuries: Equivalence of anticoagulation and antiplatelet agents. Arch. Surg. 2009, 144, 685–690. [Google Scholar] [CrossRef]
- Burlew, C.C.; Sumislawski, J.J.; Behnfield, C.D.; McNutt, M.K.; McCarthy, J.; Sharpe, J.P.; Croce, M.A.; Bala, M.; Kashuk, J.; Spalding, M.C.; et al. Time to stroke: A Western Trauma Association multicenter study of blunt cerebrovascular injuries. J. Trauma Acute Care Surg. 2018, 85, 858–866. [Google Scholar] [CrossRef]
- Hundersmarck, D.; Slooff, W.-B.M.; Homans, J.F.; van der Vliet, Q.M.J.; Moayeri, N.; Hietbrink, F.; de Borst, G.J.; Öner, F.C.; Muijs, S.P.J.; Leenen, L.P.H. Blunt cerebrovascular injury: Incidence and long-term follow-up. Eur. J. Trauma Emerg. Surg. 2019, 47, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Berne, J.D.; Norwood, S.H.; E McAuley, C.; Vallina, V.L.; Creath, R.G.; McLarty, J. The high morbidity of blunt cerebrovascular injury in an unscreened population: More evidence of the need for mandatory screening protocols. J. Am. Coll. Surg. 2001, 192, 314–321. [Google Scholar] [CrossRef] [PubMed]
- Rutman, A.M.; Vranic, J.E.; Mossa-Basha, M. Imaging and Management of Blunt Cerebrovascular Injury. RadioGraphics 2018, 38, 542–563. [Google Scholar] [CrossRef]
- Harrigan, M.R.; A Weinberg, J.; Peaks, Y.-S.; Taylor, S.M.; Cava, L.P.; Richman, J.; Walters, B.C. Management of blunt extracranial traumatic cerebrovascular injury: A multidisciplinary survey of current practice. World J. Emerg. Surg. 2011, 6, 11. [Google Scholar] [CrossRef]
- Barrera, D.; Sercy, E.; Orlando, A.; Mains, C.W.; Madayag, R.; Carrick, M.M.; Tanner, A.; Lieser, M.; Acuna, D.; Yon, J.; et al. Associations of antithrombotic timing and regimen with ischemic stroke and bleeding complications in blunt cerebrovascular injury. J. Stroke Cerebrovasc. Dis. 2020, 29, 104804. [Google Scholar] [CrossRef]
- Brommeland, T.; Helseth, E.; Aarhus, M.; Moen, K.G.; Dyrskog, S.; Bergholt, B.; Olivecrona, Z.; Jeppesen, E. Best practice guidelines for blunt cerebrovascular injury (BCVI). Scand. J. Trauma Resusc. Emerg. Med. 2018, 26, 90. [Google Scholar] [CrossRef]
- Bonow, R.H.; Witt, C.E.; Mossa-Basha, M.; Cuschieri, J.; Arbabi, S.; Vavilala, M.S.; Rivara, F.P.; Chesnut, R.M. Aspirin versus anticoagulation for stroke prophylaxis in blunt cerebrovascular injury: A propensity-matched retrospective cohort study. J. Neurosurg. 2021, 135, 1413–1420. [Google Scholar] [CrossRef] [PubMed]
- Covino, M.; Manno, A.; Della Pepa, G.M.; Piccioni, A.; Tullo, G.; Petrucci, M.; Navarra, S.; Sardeo, F.; Torelli, E.; Nicolo, R.; et al. Delayed intracranial hemorrhage after mild traumatic brain injury in patients on oral anticoagulants: Is the juice worth the squeeze? Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 3066–3073. [Google Scholar] [CrossRef] [PubMed]
- Coyle, M.; Lynch, A.; Higgins, M.; Costello, M.; Judge, C.; O’dOnnell, M.; Reddin, C. Risk of Intracranial Hemorrhage Associated With Direct Oral Anticoagulation vs Antiplatelet Therapy: A Systematic Review and Meta-Analysis. JAMA Netw. Open 2024, 7, e2449017. [Google Scholar] [CrossRef]
- Esnault, P.; Cardinale, M.; Boret, H.; D’ARanda, E.; Montcriol, A.; Bordes, J.; Prunet, B.; Joubert, C.; Dagain, A.; Goutorbe, P.; et al. Blunt cerebrovascular injuries in severe traumatic brain injury: Incidence, risk factors, and evolution. J. Neurosurg. 2017, 127, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Figueroa, J.M.; Berry, K.; Boddu, J.; Kader, M.; Silva, M.; Luther, E.; Ayala, V.; Starke, R.M.; Jagid, J.; Benveniste, R. Treatment strategies for patients with concurrent blunt cerebrovascular and traumatic brain injury. J. Clin. Neurosci. 2021, 88, 243–250. [Google Scholar] [CrossRef]
- Hanna, K.; Douglas, M.; Asmar, S.; Khurrum, M.; Bible, L.; Castanon, L.; Ditillo, M.D.; Kulvatunyou, N.; Joseph, B. Treatment of blunt cerebrovascular injuries: Anticoagulants or antiplatelet agents? J. Trauma Acute Care Surg. 2020, 89, 74–79. [Google Scholar] [CrossRef]
- Hiatt, K.D.; Agarwal, R.; Oravec, C.S.; Johnson, E.C.; Patel, N.P.; Geer, C.P.; Wolfe, S.Q.; Zapadka, M.E. Blunt Cerebrovascular Injury: Are We Overscreening Low-Mechanism Trauma? Am. J. Neuroradiol. 2023, 44, 1296–1301. [Google Scholar] [CrossRef]
- Kim, D.Y.; Biffl, W.; Bokhari, F.; Brackenridge, S.; Chao, E.; Claridge, J.A.; Fraser, D.; Jawa, R.; Kasotakis, G.; Kerwin, A.; et al. Evaluation and management of blunt cerebrovascular injury: A practice management guideline from the Eastern Association for the Surgery of Trauma. J. Trauma Acute Care Surg. 2020, 88, 875–887. [Google Scholar] [CrossRef]
- Ku, J.C.; Priola, S.M.; Mathieu, F.; Taslimi, S.; Pasarikovski, C.R.; Zeiler, F.A.; Machnowska, M.; Nathens, A.; Yang, V.X.; da Costa, L. Antithrombotic choice in blunt cerebrovascular injuries: Experience at a tertiary trauma center, systematic review, and meta-analysis. J. Trauma Acute Care Surg. 2021, 91, e1–e12. [Google Scholar] [CrossRef]
- Lau, K.-W.; Chen, C.-T.; Chen, C.-C.; Lin, T.-C.; Yeap, M.-C.; Hsieh, P.-C.; Chuang, C.-C.; Wang, Y.-C.; Yang, S.-T.; Liu, Z.-H. Clinical outcomes among patients with concurrent blunt cerebrovascular injury and traumatic intracranial hemorrhage. J. Neurol. Sci. 2024, 466, 123216. [Google Scholar] [CrossRef]
- Lauerman, M.H.; Feeney, T.; Sliker, C.W.; Saksobhavivat, N.; Bruns, B.R.; Laser, A.; Tesoriero, R.; Brenner, M.; Scalea, T.M.; Stein, D.M. Lethal now or lethal later: The natural history of Grade 4 blunt cerebrovascular injury. J. Trauma Acute Care Surg. 2015, 78, 1071–1075. [Google Scholar] [CrossRef]
- Leverich, M.; Afifi, A.M.; Rejent, K.; Ren, G.; Nazzal, M.; Osman, M.F. Mortality and morbidity following initiation of anticoagulant or antiplatelet treatment for blunt cerebrovascular injury. J. Vasc. Surg. 2023, 78, e152–e158. [Google Scholar] [CrossRef] [PubMed]
- Matsushima, K.; Leichtle, S.W.; Wild, J.; Young, K.; Chang, G.; Demetriades, D.; Lomangino, C.D.; Massetti, J.; Glass, N.E.; Livingston, D.H.; et al. Anticoagulation therapy in patients with traumatic brain injury: An Eastern Association for the Surgery of Trauma multicenter prospective study. Surgery 2021, 169, 470–476. [Google Scholar] [CrossRef]
- Momic, J.; Yassin, N.; Kim, M.Y.; Walser, E.; Smith, S.; Ball, I.; Moffat, B.; Parry, N.; Vogt, K. Antiplatelets versus anticoagulants in the treatment of blunt cerebrovascular injury (BCVI)—A systematic review and meta-analysis. Injury 2024, 55, 111485. [Google Scholar] [CrossRef] [PubMed]
- Probst, M.A.; Gupta, M.; Hendey, G.W.; Rodriguez, R.M.; Winkel, G.; Loo, G.T.; Mower, W.R. Prevalence of intracranial injury in adult patients with blunt head trauma with and without anticoagulant or antiplatelet use. Ann. Emerg. Med. 2020, 75, 354–364. [Google Scholar] [CrossRef]
- Ravindra, V.M.; Bollo, R.J.; Dewan, M.C.; Riva-Cambrin, J.K.; Tonetti, D.; Awad, A.-W.; Akbari, S.H.; Gannon, S.; Shannon, C.; Birkas, Y.; et al. Comparison of anticoagulation and antiplatelet therapy for treatment of blunt cerebrovascular injury in children <10 years of age: A multicenter retrospective cohort study. Child’s Nerv. Syst. 2021, 37, 47–54. [Google Scholar] [CrossRef]
- Russo, R.M.; Davidson, A.J.; Alam, H.B.; DuBose, J.J.; Galante, J.M.; Fabian, T.C.; Savage, S.; Holcomb, J.B.; Scalea, T.M.; AAST PROOVIT Study Group; et al. Blunt cerebrovascular injuries: Outcomes from the American Association for the Surgery of Trauma PROspective Observational Vascular Injury Treatment (PROOVIT) multicenter registry. J. Trauma Acute Care Surg. 2021, 90, 987–995. [Google Scholar] [CrossRef] [PubMed]
- Shafafy, R.; Suresh, S.; Afolayan, J.O.; Vaccaro, A.R.; Panchmatia, J.R. Blunt vertebral vascular injury in trauma patients: ATLS® recommendations and review of current evidence. J. Spine Surg. 2017, 3, 217–225. [Google Scholar] [CrossRef]
- Shahan, C.P.; Magnotti, L.J.; McBeth, P.B.; Weinberg, J.A.; Croce, M.A.; Fabian, T.C. Early antithrombotic therapy is safe and effective in patients with blunt cerebrovascular injury and solid organ injury or traumatic brain injury. J. Trauma Acute Care Surg. 2016, 81, 173–177. [Google Scholar] [CrossRef]
- Tso, M.K.; Lee, M.M.; Ball, C.G.; Morrish, W.F.; Mitha, A.P.; Kirkpatrick, A.W.; Wong, J.H. Clinical utility of a screening protocol for blunt cerebrovascular injury using computed tomography angiography. J. Neurosurg. 2017, 126, 1033–1041. [Google Scholar] [CrossRef]
- Biffl, W.L.; Moore, E.E.; Ryu, R.K.; Offner, P.J.; Novak, Z.; Coldwell, D.M.; Franciose, R.J.; Burch, J.M. The unrecognized epidemic of blunt carotid arterial injuries: Early diagnosis improves neurologic outcome. Ann. Surg. 1998, 228, 462–470. [Google Scholar] [CrossRef]
- Alsheik, N.; Gentry, L.R.; Smoker, W.R.K. Comprehensive Diagnostic Evaluation of Traumatic Vascular Injury in Head Trauma; RSNA: Chicago, IL, USA, 2007. [Google Scholar]
- Nagpal, P.; Policeni, B.; Bathla, G.; Khandelwal, A.; Derdeyn, C.; Skeete, D. Blunt Cerebrovascular Injuries: Advances in Screening, Imaging, and Management Trends. Am. J. Neuroradiol. 2017, 39, 406–414. [Google Scholar] [CrossRef] [PubMed]
- Arthurs, Z.M.; Starnes, B.W. Blunt carotid and vertebral artery injuries. Injury 2008, 39, 1232–1241. [Google Scholar] [CrossRef] [PubMed]
- Mueller, C.-A.; Peters, I.; Podlogar, M.; Kovacs, A.; Urbach, H.; Schaller, K.; Schramm, J.; Kral, T. Vertebral artery injuries following cervical spine trauma: A prospective observational study. Eur. Spine J. 2011, 20, 2202–2209. [Google Scholar] [CrossRef] [PubMed]
- Harrigan, M.R. Ischemic Stroke due to Blunt Traumatic Cerebrovascular Injury. Stroke 2020, 51, 353–360. [Google Scholar] [CrossRef]
- So, T.Y.; Sawhney, A.; Wang, L.; Wang, Y.X.J. Current Concepts in Imaging Diagnosis and Screening of Blunt Cerebrovascular Injuries. Tomography 2022, 8, 402–413. [Google Scholar] [CrossRef]
- Fitzgerald, D.J.; FitzGerald, G.A. Historical lessons in translational medicine: Cyclooxygenase inhibition and P2Y12 antagonism. Circ. Res. 2013, 112, 174–194. [Google Scholar] [CrossRef]
- Eastern Association for the Surgery of Trauma (EAST). Blunt Cerebrovascular Injury: Evaluation and Management. Published July 2010. Available online: https://www.east.org/education-resources/practice-management-guidelines/details/blunt-cerebrovascular-injury-evaluation-and-management-of (accessed on 17 May 2025).
- Weber, C.D.; Lefering, R.; Kobbe, P.; Horst, K.; Pishnamaz, M.; Sellei, R.M.; Hildebrand, F.; Pape, H.; Dgu, T. Blunt Cerebrovascular Artery Injury and Stroke in Severely Injured Patients: An International Multicenter Analysis. World J. Surg. 2018, 42, 2043–2053. [Google Scholar] [CrossRef]
- McNutt, M.K.; Kale, A.C.; Kitagawa, R.S.; Turkmani, A.H.; Fields, D.W.; Baraniuk, S.; Gill, B.S.; Cotton, B.A.; Moore, L.J.; Wade, C.E.; et al. Management of blunt cerebrovascular injury (BCVI) in the multisystem injury patient with contraindications to immediate anti-thrombotic therapy. Injury 2018, 49, 67–74. [Google Scholar] [CrossRef]
- Biffl, W.L.; Ray, C.E.; Moore, E.E.; Franciose, R.J.; Aly, S.; Heyrosa, M.G.; Johnson, J.L.; Burch, J.M. Treatment-Related Outcomes From Blunt Cerebrovascular Injuries: Importance of routine follow-up arteriography. Ann. Surg. 2002, 235, 699–706; discussion 706–707. [Google Scholar] [CrossRef]
- Callcut, R.A.; Hanseman, D.J.; Solan, P.D.; Kadon, K.S.; Ingalls, N.K.; Fortuna, G.R.; Tsuei, B.J.; Robinson, B.R.H. Early treatment of blunt cerebrovascular injury with concomitant hemorrhagic neurologic injury is safe and effective. J. Trauma. Acute Care Surg. 2012, 72, 338–346; discussion 345–346. [Google Scholar] [CrossRef] [PubMed]
- Berne, J.D.; Norwood, S.H.; McAuley, C.E.; Villareal, D.H. Helical computed tomographic angiography: An excellent screening test for blunt cerebrovascular injury. J. Trauma 2004, 57, 11–17; discussion 17–19. [Google Scholar] [CrossRef] [PubMed]
- Kanoto, M.; Hosoya, T. Diagnosis of Intracranial Artery Dissection. Neurol. Med.-Chir. 2016, 56, 524–533. [Google Scholar] [CrossRef] [PubMed]
- Miller, P.R.; Fabian, T.C.; Croce, M.A.; Cagiannos, C.; Williams, J.S.; Vang, M.; Qaisi, W.G.; Felker, R.E.; Timmons, S.D. Prospective screening for blunt cerebrovascular injuries: Analysis of diagnostic modalities and outcomes. Ann. Surg. 2002, 236, 386–395. [Google Scholar] [CrossRef]
- Cothren, C.C.; Moore, E.E.; Ray, C.E.; Johnson, J.L.; Moore, J.B.; Burch, J.M. Cervical spine fracture patterns mandating screening to rule out blunt cerebrovascular injury. Surgery 2007, 141, 76–82. [Google Scholar] [CrossRef]
- Warner, T.D.; Nylander, S.; Whatling, C. Anti-platelet therapy: Cyclo-oxygenase inhibition and the use of aspirin with particular regard to dual anti-platelet therapy. Br. J. Clin. Pharmacol. 2011, 72, 619–633. [Google Scholar] [CrossRef]
- Biffl, W.L.; Moore, E.E.; Kansagra, A.P.; Flores, B.C.; Weiss, J.S. Diagnosis and management of blunt cerebrovascular injuries: What you need to know. J. Trauma Acute Care Surg. 2025, 98, 1–10. [Google Scholar] [CrossRef]
- Umerah, C.O.; Momodu, I.I. Anticoagulation. In StatPearls; StatPearls Publishing LLC.: Treasure Island, FL, USA, 2025. [Google Scholar]
- Iqbal, A.M.; Lopez, R.A.; Hai, O. Antiplatelet Medications. In StatPearls; StatPearls Publishing LLC.: Treasure Island, FL, USA, 2025. [Google Scholar]
- Moore, E.E.; Moore, H.B.; Kornblith, L.Z.; Neal, M.D.; Hoffman, M.; Mutch, N.J.; Schöchl, H.; Hunt, B.J.; Sauaia, A. Trauma-induced coagulopathy. Nat. Rev. Dis. Primers 2021, 7, 30. [Google Scholar] [CrossRef]
- Hung, K.-C.; Chang, L.-C.; Chen, I.-W. Antiplatelet versus anticoagulant therapy in blunt cerebrovascular injury: More evidence needed before changing clinical practice. Injury 2024, 56, 111799. [Google Scholar] [CrossRef]
- Arahata, M.; Asakura, H. Antithrombotic therapies for elderly patients: Handling problems originating from their comorbidities. Clin. Interv. Aging 2018, 13, 1675–1690. [Google Scholar] [CrossRef]
- Bromberg, W.J.; Collier, B.C.D.; Diebel, L.N.; Dwyer, K.M.; Holevar, M.R.; Jacobs, D.G.; Kurek, S.J.D.; Schreiber, M.A.; Shapiro, M.L.; Vogel, T.R. Blunt cerebrovascular injury practice management guidelines: The eastern association for the surgery of trauma. J. Trauma 2010, 68, 471–477. [Google Scholar] [CrossRef] [PubMed]
- Melkonian, M.; Jarzebowski, W.; Pautas, E.; Siguret, V.; Belmin, J.; Lafuente-Lafuente, C. Bleeding risk of antiplatelet drugs compared with oral anticoagulants in older patients with atrial fibrillation: A systematic review and meta-analysis. J. Thromb. Haemost. 2017, 15, 1500–1510. [Google Scholar] [CrossRef] [PubMed]
- Lui, F.; Suheb, M.Z.K.; Patti, L. Ischemic Stroke. In StatPearls; StatPearls Publishing LLC.: Treasure Island, FL, USA, 2025. [Google Scholar]
- Murphy, P.B.; Severance, S.; Holler, E.; Menard, L.; Savage, S.; Zarzaur, B.L. Treatment of asymptomatic blunt cerebrovascular injury (BCVI): A systematic review. Trauma Surg. Acute Care Open 2021, 6, e000668. [Google Scholar] [CrossRef] [PubMed]
- Beavers, C.J.; Patel, P.; Naqvi, I.A. Clopidogrel. In StatPearls; StatPearls Publishing LLC.: Treasure Island, FL, USA, 2025. [Google Scholar]
- DiCocco, J.M.; Fabian, T.C.; Emmett, K.P.; Magnotti, L.J.; Zarzaur, B.L.; Bate, B.G.; Muhlbauer, M.S.; Khan, N.; Kelly, J.M.; Williams, J.S.; et al. Optimal outcomes for patients with blunt cerebrovascular injury (BCVI): Tailoring treatment to the lesion. J. Am. Coll. Surg. 2011, 212, 549–557. [Google Scholar] [CrossRef]
- Findlay, M.C.; Sarriera-Valentin, G.; Earl, E.R.; Cole, K.L.; Hamrick, F.A.; Baradaran, H.; Cortez, J.; Lombardo, S.; Nunez, J.; Kilburg, C.; et al. Management patterns and outcomes after traumatic brain injury with associated blunt cerebrovascular injury. Neurosurgery 2024, 94, 340–349. [Google Scholar] [CrossRef]
- Miller, P.R.; Fabian, T.C.; Bee, T.K.; Timmons, S.; Chamsuddin, A.; Finkle, R.; Croce, M.A. Blunt cerebrovascular injuries: Diagnosis and treatment. J. Trauma 2001, 51, 279–286. [Google Scholar] [CrossRef]

| Reference | Sample Size | Anticoagulation Use | Outcomes Evaluated | Morbidity | Mortality | Mean Follow-Up |
|---|---|---|---|---|---|---|
| Barrera et al. 2020 [9] | 189 cases | Yes | Ischemic stroke, blood transfusion | VAI stroke rate: 55.3% CAI stroke rate: 30.9% Stroke rate of both: 13.8% | 5.80% | N/A |
| Brommeland et al. 2018 [10] | 78 studies | Yes | Radiological investigation, vessel injury, stroke, morbidity, mortality | N/A | N/A | N/A |
| Bonow et al. 2021 [11] | 677 cases | Yes | Stroke after admission | Overall stroke rate: 8.11% | Overall: 10.2% | N/A |
| Burlew et al. 2018 [4] | 492 cases | Yes | Time to stroke | N/A–cohort is stroke-focused | Overall: 32% | N/A |
| Covino et al. 2021 [12] | 685 cases | Yes | Delayed intracranial hemorrhage | N/A | N/A | N/A |
| Coyle et al. 2024 [13] | 8 studies | Yes | Intracranial bleeding | N/A | N/A | N/A |
| Esnault et al. 2017 [14] | 228 cases | Yes | Neurologic outcomes | Overall stroke rate: 16% | Overall: 33% | 95.2% of patients had clinical follow-up at 3 months |
| Figueroa et al. 2021 [15] | 30 cases | Yes | Recovery, short-term outcomes (hospitalization), long-term outcomes (speech and language deficits) | Overall stroke rate: 23.7% | Overall: 7.9% | 68% patients had clinical f/u of which 8 patients had f/u arteriography |
| Hanna et al. 2020 [16] | 725 cases | Yes | Rate of cerebrovascular accident post-discharge | On anticoagulants: 1.8% On antiplatelets: 5.72% | On anticoagulants: 4.2% On antiplatelets: 3.9% | N/A |
| Hiatt et al. 2023 [17] | 77 cases | Yes | Neurologic deficits on follow-up, emboli on transcranial Doppler ultrasound, new or worsening intracranial hemorrhage, extracranial bleeding complications, ischemic stroke, death | Overall stroke rate: 3.5% | Overall: 20.9% | 76.02% patients had at least one f/u arteriography |
| Kim et al. 2020 [18] | 10 studies | Yes | Stroke incidence, hemorrhagic deterioration | N/A | N/A | N/A |
| Ku et al. 2021 [19] | 2044 cases | Yes | Ischemic stroke rate, hemorrhagic complications | N/A | N/A | N/A |
| Lau et al. 2024 [20] | 11 cases | Yes | Stroke, mortality | Overall stroke rate: 31.6% | Overall: 29.8% | N/A |
| Lauerman et al. 2015 [21] | 82 cases | Yes | Stroke after admission | CAI GIV stroke rate: 70% VAI GIV stroke rate: 2.9% | CAI: 38.5% VAI: 5.8% | N/A |
| Leverich et al. 2023 [22] | 1091 cases | Yes | Morbidity, mortality, readmission rate | Overall (ischemic) stroke rate: 2.9% Overall (hemorrhagic) stroke rate: 2.4% | Overall: 2.1% | N/A |
| Matsushima et al. 2020 [23] | 168 cases | Yes | Traumatic brain injury progression | N/A | N/A | N/A |
| Momic et al. 2024 [24] | 7643 cases | Yes | Stroke risk, bleeding complications | N/A | N/A | N/A |
| Probst et al. 2019 [25] | 9070 cases | Yes | Intracranial bleeding | N/A | N/A | N/A |
| Ravindra et al. 2020 [26] | 18 cases | Yes | Hemorrhagic complications, healing | Overall stroke rate: 47.05% | Overall: 5.8% | 82.5% patients had f/u arteriography |
| Russo et al. 2021 [27] | 971 cases | Yes | Stroke, mortality | Overall stroke rate: 7% | Overall: 12% | N/A |
| Shafafy et al. 2017 [28] | 258 BCVI cases, 23 asymptomatic | Yes | Neurological outcomes, grade of injury, death | N/A | N/A | N/A |
| Shahan et al. 2016 [29] | 119 cases | Yes | Morbidity, mortality | Overall stroke rate: 9% | Overall: 9.7% | N/A |
| Hundersmarck et al. 2021 [5] | 71 cases | No, antiplatelet only | In-hospital stroke | Overall stroke rate: 28% | Overall: 23% | 83% patients had f/u arteriography |
| Tso et al. 2017 [30] | 3049 cases | No, antiplatelet only | Ischemic complications | Overall stroke rate: 29.1% | Overall: 8% | N/A |
| Grade Injury | Angiographic Characteristics |
|---|---|
| Grade I | Non-hemodynamically significant intramural irregularity with 25% luminal narrowing |
| Grade II | Potentially hemodynamically significant dissections and hematomas with 50% luminal narrowing presence of intraluminal thrombus, or a dissection with a visible raised intimal flap |
| Grade III | Pseudoaneurysms |
| Grade IV | Occlusions |
| Grade V | Vessel transections with active extravasation |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baloi, D.; Al-Nuaimy, Y.; Saloum, A.; Rahmanipour, E.; Ghorbani, M.; Karsy, M.; Lucke-Wold, B.; Pahlevani, M. Choice of Antiplatelet vs. Anticoagulant for Blunt Cerebrovascular Injury. Life 2025, 15, 1364. https://doi.org/10.3390/life15091364
Baloi D, Al-Nuaimy Y, Saloum A, Rahmanipour E, Ghorbani M, Karsy M, Lucke-Wold B, Pahlevani M. Choice of Antiplatelet vs. Anticoagulant for Blunt Cerebrovascular Injury. Life. 2025; 15(9):1364. https://doi.org/10.3390/life15091364
Chicago/Turabian StyleBaloi, Denise, Yusor Al-Nuaimy, Ammar Saloum, Elham Rahmanipour, Mohammad Ghorbani, Michael Karsy, Brandon Lucke-Wold, and Mehrdad Pahlevani. 2025. "Choice of Antiplatelet vs. Anticoagulant for Blunt Cerebrovascular Injury" Life 15, no. 9: 1364. https://doi.org/10.3390/life15091364
APA StyleBaloi, D., Al-Nuaimy, Y., Saloum, A., Rahmanipour, E., Ghorbani, M., Karsy, M., Lucke-Wold, B., & Pahlevani, M. (2025). Choice of Antiplatelet vs. Anticoagulant for Blunt Cerebrovascular Injury. Life, 15(9), 1364. https://doi.org/10.3390/life15091364







