Assessing the Association between Biomarkers and COVID-19 Mortality Using the Joint Modelling Approach
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Patients
2.2. Statistical Analyses
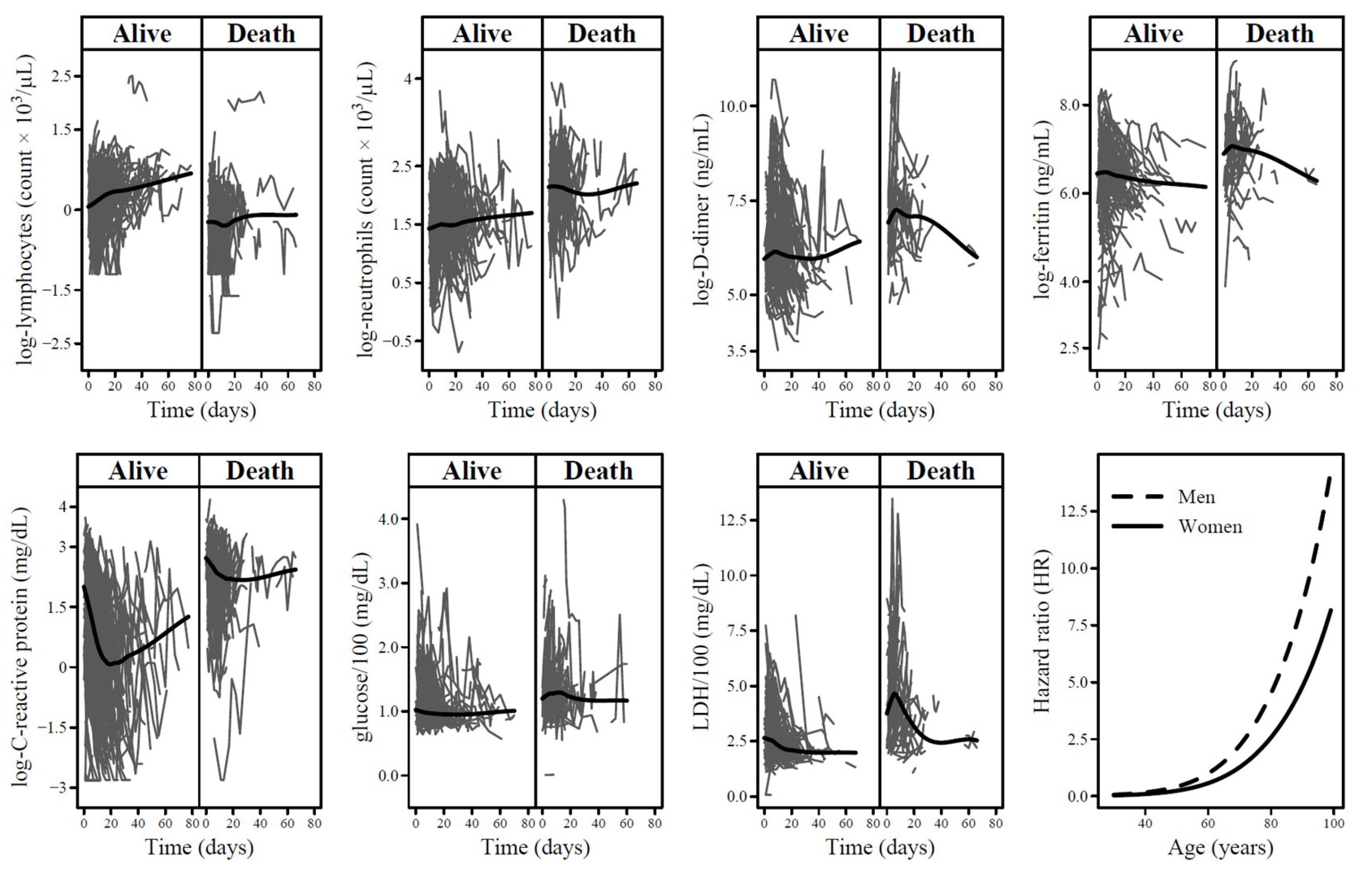
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization (WHO). Coronavirus Disease (COVID-19) Weekly Epidemiological Update. Available online: https://www.who.int/publications/m/item/covid-19-epidemiological-update---22-december-2023 (accessed on 8 January 2024).
- Gao, Y.D.; Ding, M.; Dong, X.; Zhang, J.J.; Kursat Azkur, A.; Azkur, D.; Gan, H.; Sun, Y.L.; Fu, W.; Li, W.; et al. Risk factors for severe and critically ill COVID-19 patients: A review. Allergy 2021, 76, 428–455. [Google Scholar] [CrossRef]
- Zhang, J.J.; Dong, X.; Liu, G.H.; Gao, Y.D. Risk and Protective Factors for COVID-19 Morbidity, Severity, and Mortality. Clin. Rev. Allergy Immunol. 2022, 64, 90–107. [Google Scholar] [CrossRef]
- Pijls, B.G.; Jolani, S.; Atherley, A.; Derckx, R.T.; Dijkstra, J.I.R.; Franssen, G.H.L.; Hendriks, S.; Richters, A.; Venemans-Jellema, A.; Zalpuri, S.; et al. Demographic risk factors for COVID-19 infection, severity, ICU admission and death: A meta-analysis of 59 studies. BMJ Open 2021, 11, e044640. [Google Scholar] [CrossRef]
- Lighter, J.; Phillips, M.; Hochman, S.; Sterling, S.; Johnson, D.; Francois, F.; Stachel, A. Obesity in Patients Younger Than 60 Years Is a Risk Factor for COVID-19 Hospital Admission. Clin. Infect. Dis. 2020, 71, 896–897. [Google Scholar] [CrossRef]
- Fresan, U.; Guevara, M.; Elia, F.; Albeniz, E.; Burgui, C.; Castilla, J. For the Working Group for the Study of COVID-19 in Navarra Independent Role of Severe Obesity as a Risk Factor for COVID-19 Hospitalization: A Spanish Population-Based Cohort Study. Obesity 2021, 29, 29–37. [Google Scholar] [CrossRef]
- Gao, F.; Zheng, K.I.; Wang, X.B.; Sun, Q.F.; Pan, K.H.; Wang, T.Y.; Chen, Y.P.; Targher, G.; Byrne, C.D.; George, J.; et al. Obesity Is a Risk Factor for Greater COVID-19 Severity. Diabetes Care 2020, 43, e72–e74. [Google Scholar] [CrossRef]
- Cai, Q.; Chen, F.; Wang, T.; Luo, F.; Liu, X.; Wu, Q.; He, Q.; Wang, Z.; Liu, Y.; Liu, L.; et al. Obesity and COVID-19 Severity in a Designated Hospital in Shenzhen, China. Diabetes Care 2020, 43, 1392–1398. [Google Scholar] [CrossRef]
- Klang, E.; Kassim, G.; Soffer, S.; Freeman, R.; Levin, M.A.; Reich, D.L. Severe Obesity as an Independent Risk Factor for COVID-19 Mortality in Hospitalized Patients Younger than 50. Obesity 2020, 28, 1595–1599. [Google Scholar] [CrossRef] [PubMed]
- Cai, Q.; Huang, D.; Ou, P.; Yu, H.; Zhu, Z.; Xia, Z.; Su, Y.; Ma, Z.; Zhang, Y.; Li, Z.; et al. COVID-19 in a designated infectious diseases hospital outside Hubei Province, China. Allergy 2020, 75, 1742–1752. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA 2020, 323, 1061–1069. [Google Scholar] [CrossRef] [PubMed]
- Wan, S.; Xiang, Y.; Fang, W.; Zheng, Y.; Li, B.; Hu, Y.; Lang, C.; Huang, D.; Sun, Q.; Xiong, Y.; et al. Clinical features and treatment of COVID-19 patients in northeast Chongqing. J. Med. Virol. 2020, 92, 797–806. [Google Scholar] [CrossRef]
- Bae, S.; Kim, S.R.; Kim, M.N.; Shim, W.J.; Park, S.M. Impact of cardiovascular disease and risk factors on fatal outcomes in patients with COVID-19 according to age: A systematic review and meta-analysis. Heart 2021, 107, 373–380. [Google Scholar] [CrossRef]
- Liang, W.; Guan, W.; Chen, R.; Wang, W.; Li, J.; Xu, K.; Li, C.; Ai, Q.; Lu, W.; Liang, H.; et al. Cancer patients in SARS-CoV-2 infection: A nationwide analysis in China. Lancet Oncol. 2020, 21, 335–337. [Google Scholar] [CrossRef]
- Li, X.; Xu, S.; Yu, M.; Wang, K.; Tao, Y.; Zhou, Y.; Shi, J.; Zhou, M.; Wu, B.; Yang, Z.; et al. Risk factors for severity and mortality in adult COVID-19 inpatients in Wuhan. J. Allergy Clin. Immunol. 2020, 146, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Li, R.; Tian, J.; Yang, F.; Lv, L.; Yu, J.; Sun, G.; Ma, Y.; Yang, X.; Ding, J. Clinical characteristics of 225 patients with COVID-19 in a tertiary Hospital near Wuhan, China. J. Clin. Virol. 2020, 127, 104363. [Google Scholar] [CrossRef] [PubMed]
- Ou, M.; Zhu, J.; Ji, P.; Li, H.; Zhong, Z.; Li, B.; Pang, J.; Zhang, J.; Zheng, X. Risk factors of severe cases with COVID-19: A meta-analysis. Epidemiol. Infect. 2020, 148, e175. [Google Scholar] [CrossRef]
- Guo, W.; Li, M.; Dong, Y.; Zhou, H.; Zhang, Z.; Tian, C.; Qin, R.; Wang, H.; Shen, Y.; Du, K.; et al. Diabetes is a risk factor for the progression and prognosis of COVID-19. Diabetes Metab. Res. Rev. 2020, 36, e3319. [Google Scholar] [CrossRef]
- Shi, Q.; Zhang, X.; Jiang, F.; Zhang, X.; Hu, N.; Bimu, C.; Feng, J.; Yan, S.; Guan, Y.; Xu, D.; et al. Clinical Characteristics and Risk Factors for Mortality of COVID-19 Patients with Diabetes in Wuhan, China: A Two-Center, Retrospective Study. Diabetes Care 2020, 43, 1382–1391. [Google Scholar] [CrossRef] [PubMed]
- Huang, I.; Lim, M.A.; Pranata, R. Diabetes mellitus is associated with increased mortality and severity of disease in COVID-19 pneumonia—A systematic review, meta-analysis, and meta-regression. Diabetes Metab. Syndr. 2020, 14, 395–403. [Google Scholar] [CrossRef]
- Feng, Y.; Ling, Y.; Bai, T.; Xie, Y.; Huang, J.; Li, J.; Xiong, W.; Yang, D.; Chen, R.; Lu, F.; et al. COVID-19 with Different Severities: A Multicenter Study of Clinical Features. Am. J. Respir. Crit. Care Med. 2020, 201, 1380–1388. [Google Scholar] [CrossRef]
- Tian, J.; Yuan, X.; Xiao, J.; Zhong, Q.; Yang, C.; Liu, B.; Cai, Y.; Lu, Z.; Wang, J.; Wang, Y.; et al. Clinical characteristics and risk factors associated with COVID-19 disease severity in patients with cancer in Wuhan, China: A multicentre, retrospective, cohort study. Lancet Oncol. 2020, 21, 893–903. [Google Scholar] [CrossRef]
- Williamson, E.J.; Walker, A.J.; Bhaskaran, K.; Bacon, S.; Bates, C.; Morton, C.E.; Curtis, H.J.; Mehrkar, A.; Evans, D.; Inglesby, P.; et al. Factors associated with COVID-19-related death using OpenSAFELY. Nature 2020, 584, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Ng, J.H.; Hirsch, J.S.; Wanchoo, R.; Sachdeva, M.; Sakhiya, V.; Hong, S.; Jhaveri, K.D.; Fishbane, S. On behalf of the Northwell COVID-19 Research Consortium and the Northwell Nephrology COVID-19 Research Consortium Outcomes of patients with end-stage kidney disease hospitalized with COVID-19. Kidney Int. 2020, 98, 1530–1539. [Google Scholar] [CrossRef] [PubMed]
- Samprathi, M.; Jayashree, M. Biomarkers in COVID-19: An Up-To-Date Review. Front. Pediatr. 2020, 8, 607647. [Google Scholar] [CrossRef] [PubMed]
- Li, B.B.; Huang, S.J.; Fu, Y.L.; Li, Z.L.; Wang, J.; Wang, J.L. Laboratory Biomarkers for the Diagnosis and Management of Patients with COVID-19: An Updated Review. Discov. Med. 2021, 31, 61–68. [Google Scholar] [PubMed]
- Loomba, R.S.; Villarreal, E.G.; Farias, J.S.; Aggarwal, G.; Aggarwal, S.; Flores, S. Serum biomarkers for prediction of mortality in patients with COVID-19. Ann. Clin. Biochem. 2022, 59, 15–22. [Google Scholar] [CrossRef] [PubMed]
- Rizopoulos, D. Joint Models for Longitudinal and Time-to-Event Data with Applications in R; CRC Press, Taylor & Francis: Boca Raton, FL, USA, 2012. [Google Scholar]
- Cox, D.R. Regression Models and Life-Tables. J. R. Stat. Soc. B 1972, 34, 187. [Google Scholar] [CrossRef]
- Breslow, N.E. Analysis of Survival Data under Proportional Hazards Model. Int. Stat. Rev. 1975, 43, 45–58. [Google Scholar] [CrossRef]
- Therneau, T.M.; Grambsch, P.M. Modeling Survival Data: Extending the Cox Model, 1st ed.; Springer: New York, NY, USA, 2000. [Google Scholar]
- Rizopoulos, D. The R Package JMbayes for Fitting Joint Models for Longitudinal and Time-to-Event Data Using MCMC. J. Stat. Softw. 2016, 72, 1–46. [Google Scholar] [CrossRef]
- Liu, J.; Li, S.; Liu, J.; Liang, B.; Wang, X.; Wang, H.; Li, W.; Tong, Q.; Yi, J.; Zhao, L.; et al. Longitudinal characteristics of lymphocyte responses and cytokine profiles in the peripheral blood of SARS-CoV-2 infected patients. EBioMedicine 2020, 55, 102763. [Google Scholar] [CrossRef]
- Huang, G.; Kovalic, A.J.; Graber, C.J. Prognostic Value of Leukocytosis and Lymphopenia for Coronavirus Disease Severity. Emerg. Infect. Dis. 2020, 26, 1839–1841. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Du, X.; Chen, J.; Jin, Y.; Peng, L.; Wang, H.H.X.; Luo, M.; Chen, L.; Zhao, Y. Neutrophil-to-lymphocyte ratio as an independent risk factor for mortality in hospitalized patients with COVID-19. J. Infect. 2020, 81, e6–e12. [Google Scholar] [CrossRef] [PubMed]
- Qin, C.; Zhou, L.; Hu, Z.; Zhang, S.; Yang, S.; Tao, Y.; Xie, C.; Ma, K.; Shang, K.; Wang, W.; et al. Dysregulation of Immune Response in Patients with Coronavirus 2019 (COVID-19) in Wuhan, China. Clin. Infect. Dis. 2020, 71, 762–768. [Google Scholar] [CrossRef] [PubMed]
- Mo, P.; Xing, Y.; Xiao, Y.; Deng, L.; Zhao, Q.; Wang, H.; Xiong, Y.; Cheng, Z.; Gao, S.; Liang, K.; et al. Clinical Characteristics of Refractory Coronavirus Disease 2019 in Wuhan, China. Clin. Infect. Dis. 2021, 73, e4208–e4213. [Google Scholar] [CrossRef] [PubMed]
- Chen, R.; Sang, L.; Jiang, M.; Yang, Z.; Jia, N.; Fu, W.; Xie, J.; Guan, W.; Liang, W.; Ni, Z.; et al. Longitudinal hematologic and immunologic variations associated with the progression of COVID-19 patients in China. J. Allergy Clin. Immunol. 2020, 146, 89–100. [Google Scholar] [CrossRef]
- Huang, I.; Pranata, R. Lymphopenia in severe coronavirus disease-2019 (COVID-19): Systematic review and meta-analysis. J. Intensive Care 2020, 8, 36. [Google Scholar] [CrossRef] [PubMed]
- Ye, W.; Chen, G.; Li, X.; Lan, X.; Ji, C.; Hou, M.; Zhang, D.; Zeng, G.; Wang, Y.; Xu, C.; et al. Dynamic changes of D-dimer and neutrophil-lymphocyte count ratio as prognostic biomarkers in COVID-19. Respir. Res. 2020, 21, 169. [Google Scholar] [CrossRef]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.C.; et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef]
- Bompard, F.; Monnier, H.; Saab, I.; Tordjman, M.; Abdoul, H.; Fournier, L.; Sanchez, O.; Lorut, C.; Chassagnon, G.; Revel, M.P. Pulmonary embolism in patients with COVID-19 pneumonia. Eur. Respir. J. 2020, 56, 2001365. [Google Scholar] [CrossRef]
- Zhang, K.; Liu, X.; Shen, J.; Li, Z.; Sang, Y.; Wu, X.; Zha, Y.; Liang, W.; Wang, C.; Wang, K.; et al. Clinically Applicable AI System for Accurate Diagnosis, Quantitative Measurements, and Prognosis of COVID-19 Pneumonia Using Computed Tomography. Cell 2020, 182, 1360. [Google Scholar] [CrossRef]
- Yu, H.H.; Qin, C.; Chen, M.; Wang, W.; Tian, D.S. D-dimer level is associated with the severity of COVID-19. Thromb. Res. 2020, 195, 219–225. [Google Scholar] [CrossRef] [PubMed]
- Danwang, C.; Endomba, F.T.; Nkeck, J.R.; Wouna, D.L.A.; Robert, A.; Noubiap, J.J. A meta-analysis of potential biomarkers associated with severity of coronavirus disease 2019 (COVID-19). Biomark. Res. 2020, 8, 37. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Liu, L.; Jiao, J.; Yang, L.; Zhu, B.; Li, X. Characterisation of clinical, laboratory and imaging factors related to mild vs. severe covid-19 infection: A systematic review and meta-analysis. Ann. Med. 2020, 52, 334–344. [Google Scholar] [CrossRef] [PubMed]
- Zhu, J.; Pang, J.; Ji, P.; Zhong, Z.; Li, H.; Li, B.; Zhang, J.; Lu, J. Coagulation dysfunction is associated with severity of COVID-19: A meta-analysis. J. Med. Virol. 2021, 93, 962–972. [Google Scholar] [CrossRef]
- Lin, J.; Yan, H.; Chen, H.; He, C.; Lin, C.; He, H.; Zhang, S.; Shi, S.; Lin, K. COVID-19 and coagulation dysfunction in adults: A systematic review and meta-analysis. J. Med. Virol. 2021, 93, 934–944. [Google Scholar] [CrossRef] [PubMed]
- Tian, W.; Jiang, W.; Yao, J.; Nicholson, C.J.; Li, R.H.; Sigurslid, H.H.; Wooster, L.; Rotter, J.I.; Guo, X.; Malhotra, R. Predictors of mortality in hospitalized COVID-19 patients: A systematic review and meta-analysis. J. Med. Virol. 2020, 92, 1875–1883. [Google Scholar] [CrossRef] [PubMed]
- Figliozzi, S.; Masci, P.G.; Ahmadi, N.; Tondi, L.; Koutli, E.; Aimo, A.; Stamatelopoulos, K.; Dimopoulos, M.A.; Caforio, A.L.P.; Georgiopoulos, G. Predictors of adverse prognosis in COVID-19: A systematic review and meta-analysis. Eur. J. Clin. Investig. 2020, 50, e13362. [Google Scholar] [CrossRef] [PubMed]
- Ghahramani, S.; Tabrizi, R.; Lankarani, K.B.; Kashani, S.M.A.; Rezaei, S.; Zeidi, N.; Akbari, M.; Heydari, S.T.; Akbari, H.; Nowrouzi-Sohrabi, P.; et al. Laboratory features of severe vs. non-severe COVID-19 patients in Asian populations: A systematic review and meta-analysis. Eur. J. Med. Res. 2020, 25, 30. [Google Scholar] [CrossRef]
- Di Minno, M.N.D.; Calcaterra, I.; Lupoli, R.; Storino, A.; Spedicato, G.A.; Maniscalco, M.; Di Minno, A.; Ambrosino, P. Hemostatic Changes in Patients with COVID-19: A Meta-Analysis with Meta-Regressions. J. Clin. Med. 2020, 9, 2244. [Google Scholar] [CrossRef]
- Soraya, G.V.; Ulhaq, Z.S. Crucial laboratory parameters in COVID-19 diagnosis and prognosis: An updated meta-analysis. Med. Clin. 2020, 155, 143–151. [Google Scholar] [CrossRef]
- Huang, I.; Pranata, R.; Lim, M.A.; Oehadian, A.; Alisjahbana, B. C-reactive protein, procalcitonin, D-dimer, and ferritin in severe coronavirus disease-2019: A meta-analysis. Ther. Adv. Respir. Dis. 2020, 14, 1753466620937175. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Yan, X.; Fan, Q.; Liu, H.; Liu, X.; Liu, Z.; Zhang, Z. D-dimer levels on admission to predict in-hospital mortality in patients with COVID-19. J. Thromb. Haemost. 2020, 18, 1324–1329. [Google Scholar] [CrossRef] [PubMed]
- Yao, Y.; Cao, J.; Wang, Q.; Shi, Q.; Liu, K.; Luo, Z.; Chen, X.; Chen, S.; Yu, K.; Huang, Z.; et al. D-dimer as a biomarker for disease severity and mortality in COVID-19 patients: A case control study. J. Intensive Care 2020, 8, 49. [Google Scholar] [CrossRef] [PubMed]
- Zeng, F.; Huang, Y.; Guo, Y.; Yin, M.; Chen, X.; Xiao, L.; Deng, G. Association of inflammatory markers with the severity of COVID-19: A meta-analysis. Int. J. Infect. Dis. 2020, 96, 467–474. [Google Scholar] [CrossRef]
- Henry, B.M.; de Oliveira, M.H.S.; Benoit, S.; Plebani, M.; Lippi, G. Hematologic, biochemical and immune biomarker abnormalities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): A meta-analysis. Clin. Chem. Lab. Med. 2020, 58, 1021–1028. [Google Scholar] [CrossRef] [PubMed]
- Tural Onur, S.; Altin, S.; Sokucu, S.N.; Fikri, B.I.; Barca, T.; Bolat, E.; Toptas, M. Could ferritin level be an indicator of COVID-19 disease mortality? J. Med. Virol. 2021, 93, 1672–1677. [Google Scholar] [CrossRef]
- Taneri, P.E.; Gomez-Ochoa, S.A.; Llanaj, E.; Raguindin, P.F.; Rojas, L.Z.; Roa-Diaz, Z.M.; Salvador, D.J.; Groothof, D.; Minder, B.; Kopp-Heim, D.; et al. Anemia and iron metabolism in COVID-19: A systematic review and meta-analysis. Eur. J. Epidemiol. 2020, 35, 763–773. [Google Scholar] [CrossRef]
- Malik, P.; Patel, U.; Mehta, D.; Patel, N.; Kelkar, R.; Akrmah, M.; Gabrilove, J.L.; Sacks, H. Biomarkers and outcomes of COVID-19 hospitalisations: Systematic review and meta-analysis. BMJ Evid. Based Med. 2021, 26, 107–108. [Google Scholar] [CrossRef]
- Mori, S.; Ai, T.; Otomo, Y. Characteristics, laboratories, and prognosis of severe COVID-19 in the Tokyo metropolitan area: A retrospective case series. PLoS ONE 2020, 15, e0239644. [Google Scholar] [CrossRef]
- Bao, J.; Li, C.; Zhang, K.; Kang, H.; Chen, W.; Gu, B. Comparative analysis of laboratory indexes of severe and non-severe patients infected with COVID-19. Clin. Chim. Acta 2020, 509, 180–194. [Google Scholar] [CrossRef]
- Wu, C.; Chen, X.; Cai, Y.; Xia, J.; Zhou, X.; Xu, S.; Huang, H.; Zhang, L.; Zhou, X.; Du, C.; et al. Risk Factors Associated with Acute Respiratory Distress Syndrome and Death in Patients With Coronavirus Disease 2019 Pneumonia in Wuhan, China. JAMA Intern. Med. 2020, 180, 934–943. [Google Scholar] [CrossRef] [PubMed]
- Paces, J.; Strizova, Z.; Smrz, D.; Cerny, J. COVID-19 and the immune system. Physiol. Res. 2020, 69, 379–388. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zhao, J.; Yang, L.; Hu, J.; Yao, Y. Value of the Neutrophil-Lymphocyte Ratio in Predicting COVID-19 Severity: A Meta-analysis. Dis. Markers 2021, 2021, 2571912. [Google Scholar] [CrossRef] [PubMed]
- Palladino, M. Complete blood count alterations in COVID-19 patients: A narrative review. Biochem. Med. 2021, 31, 030501. [Google Scholar] [CrossRef]
- Kernan, K.F.; Carcillo, J.A. Hyperferritinemia and inflammation. Int. Immunol. 2017, 29, 401–409. [Google Scholar] [CrossRef]
- Kermali, M.; Khalsa, R.K.; Pillai, K.; Ismail, Z.; Harky, A. The role of biomarkers in diagnosis of COVID-19—A systematic review. Life Sci. 2020, 254, 117788. [Google Scholar] [CrossRef]
- Zhu, X.; Gebo, K.A.; Abraham, A.G.; Habtehyimer, F.; Patel, U.E.; Laeyendecker, O.; Gniadek, T.J.; Fernandez, R.E.; Baker, O.R.; Ram, M.; et al. Dynamics of inflammatory response after SARS-CoV-2 infection by vaccination status in the USA: A prospective cohort study. Lancet Microbe 2023, 4, e692–e703. [Google Scholar] [CrossRef]
- Korishettar, G.; Chikkahonnaiah, P.; Tulimilli, S.V.; Dallavalasa, S.; Byrappa, S.H.; Madhunapantula, S.V.; Veeranna, R.P. Assessment of Clinical Profile and Treatment Outcome in Vaccinated and Unvaccinated SARS-CoV-2 Infected Patients. Vaccines 2022, 10, 1125. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Li, Y.; Pan, Y.; Zhou, L.; Zhang, X.; Wei, Y.; Guo, F.; Shu, Y.; Gao, J. Clinical and immune response characteristics among vaccinated persons infected with SARS-CoV-2 delta variant: A retrospective study. J. Zhejiang Univ. Sci. B 2022, 23, 899–914. [Google Scholar] [CrossRef] [PubMed]
| Age (Years) | Men (n = 235; 58.3%) | Women (n = 168; 41.7%) | ||||||
|---|---|---|---|---|---|---|---|---|
| At Risk | Mortality Rate a | HR (95% CI) b | At Risk | Mortality Rate a | HR (95% CI) b | |||
| <40 | 14 | 0.00 | 3.18 c | Ref | 6 | 0.00 | 2.27 c | Ref |
| 40–49 | 26 | 0.00 | 6 | 0.00 | ||||
| 50–59 | 29 | 7.59 | 17 | 3.32 | ||||
| 60–69 | 41 | 10.85 | 3.55 (1.07, 11.81) | 15 | 4.37 | 1.84 (0.11, 29.41) | ||
| 70–79 | 50 | 26.72 | 8.34 (2.86, 24.32) | 26 | 28.44 | 12.12 (1.58, 93.30) | ||
| 80–89 | 62 | 30.55 | 9.27 (3.27, 26.32) | 71 | 23.67 | 10.29 (1.40, 75.49) | ||
| ≥90 | 13 | 88.71 | 26.88 (8.52, 84.81) | 27 | 43.86 | 18.74 (2.51, 139.91) | ||
| Variables | Univariable JM | Multivariable JM | ||
|---|---|---|---|---|
| Estimate (95% CI) | P | Estimate (95% CI) | P | |
| Hematological biomarkers | ||||
| Longitudinal submodel: log-lymphocytes (count × 103/µL) | ||||
| Intercept | 0.68 (0.29, 1.05) | P < 0.01 | 0.64 (0.38, 0.90) | P < 0.01 |
| ns(time at measurement in days) 1 | 1.11 (0.95, 1.27) | P < 0.01 | 1.23 (0.98, 1.49) | P < 0.01 |
| ns(time at measurement in days) 2 | 0.52 (0.40, 0.65) | P < 0.01 | 0.93 (0.47, 1.43) | P < 0.01 |
| ns(age in years) 1 | −1.47 (−2.20, −0.72) | P < 0.01 | −1.32 (−1.81, −0.82) | P < 0.01 |
| ns(age in years) 2 | −0.69 (−0.97, −0.39) | P < 0.01 | −0.53 (−0.74, −0.30) | P < 0.01 |
| Sex (Ref: women) | −0.11 (−0.25, 0.03) | P = 0.14 | −0.13 (−0.23, −0.04) | P < 0.01 |
| Longitudinal sub-model: log-neutrophils (count × 103/µL) | ||||
| Intercept | 0.90 (0.57, 1.22) | P < 0.01 | 1.09 (0.79, 1.41) | P < 0.01 |
| ns(time at measurement in days) 1 | −1.10 (−1.40, −0.78) | P < 0.01 | −0.81 (−1.21, 0.41) | P < 0.01 |
| ns(time at measurement in days) 2 | −2.89 (−3.55, −2.15) | P < 0.01 | −2.15 (−2.98, −1.36) | P < 0.01 |
| ns(age in years) 1 | 1.24 (0.65, 1.85) | P < 0.01 | 0.94 (0.32, 1.54) | P < 0.01 |
| ns(age in years) 2 | 0.89 (0.64, 1.15) | P < 0.01 | 0.62 (0.35, 0.89) | P < 0.01 |
| Sex (Ref: women) | 0.25 (0.13, 0.37) | P < 0.01 | 0.23 (0.12, 0.34) | P < 0.01 |
| Coagulation biomarkers | ||||
| Longitudinal sub-model: log-D-dimer (ng/mL) | ||||
| Intercept | 4.34 (3.62, 5.01) | P < 0.01 | Excluded due to the high number of missing values | |
| ns(time at measurement in days) 1 | −1.72 (−2.02, −1.39) | P < 0.01 | ||
| ns(time at measurement in days) 2 | −2.99 (−3.47, −2.57) | P < 0.01 | ||
| ns(age in years) 1 | 4.18 (2.93, 5.52) | P < 0.01 | ||
| ns(age in years) 2 | 1.57 (1.01, 2.09) | P < 0.01 | ||
| Sex (Ref: women) | 0.35 (0.10, 0.61) | P = 0.01 | ||
| Biochemical biomarkers | ||||
| Longitudinal sub-model: log-ferritin (ng/mL) | ||||
| Intercept | 5.18 (4.67, 5.67) | P < 0.01 | 5.27 (4.74, 5.82) | P < 0.01 |
| ns(time at measurement in days) 1 | −1.05 (−1.32, −0.77) | P < 0.01 | −1.16 (−1.66, −0.71) | P < 0.01 |
| ns(time at measurement in days) 2 | −1.69 (−2.23, −1.08) | P < 0.01 | −2.07 (−3.25, −1.05) | P = 0.01 |
| ns(age in years) 1 | 2.13 (1.15, 3.06) | P < 0.01 | 1.93 (0.82, 2.97) | P < 0.01 |
| ns(age in years) 2 | 0.20 (−0.18, 0.59) | P = 0.31 | 0.16 (−0.29, 0.63) | P = 0.52 |
| Sex (Ref: women) | 0.53 (0.34, 0.70) | P < 0.01 | 0.56 (0.35, 0.76) | P < 0.01 |
| Longitudinal sub-model: log-C-reactive protein (mg/L) | ||||
| Intercept | −0.19 (−0.71, 0.34) | P = 0.47 | 0.29 (−0.32, 0.91) | P = 0.36 |
| ns(time at measurement in days) 1 | −4.23 (−5.09, −3.35) | P < 0.01 | −5.16 (−6.47, −3.90) | P < 0.01 |
| ns(time at measurement in days) 2 | 1.03 (−0.65, 2.64) | P = 0.23 | −0.84 (−3.67, 1.79) | P = 0.51 |
| ns(age in years) 1 | 4.31 (3.30, 5.32) | P < 0.01 | 3.67 (2.51, 4.83) | P < 0.01 |
| ns(age in years) 2 | 0.98 (0.57, 1.40) | P < 0.01 | 0.70 (0.20, 1.24) | P < 0.04 |
| Sex (Ref: women) | 0.50 (0.31, 0.68) | P < 0.01 | 0.38 (0.13, 0.61) | P < 0.01 |
| Longitudinal sub-model: glucose/100 (mg/dL) | ||||
| Intercept | 0.94 (0.45, 1.44) | P < 0.01 | 0.99 (0.75, 1.25) | P < 0.01 |
| ns(time at measurement in days) 1 | −0.33 (−0.45, −0.20) | P < 0.01 | −0.40 (−0.64, −0.17) | P < 0.01 |
| ns(time at measurement in days) 2 | −0.35 (−0.52, −0.20) | P < 0.01 | −0.61 (−1.23, −0.04) | P = 0.04 |
| ns(age in years) 1 | 0.57 (−0.42, 1.49) | P = 0.25 | 0.41 (−0.08, 0.88) | P = 0.11 |
| ns(age in years) 2 | 0.08 (−0.30, 0.46) | P = 0.66 | 0.05 (−0.15, 0.24) | P = 0.64 |
| Sex (Ref: women) | 0.02 (−0.16, 0.21) | P = 0.80 | 0.04 (−0.04, 0.14) | P = 0.33 |
| Longitudinal sub-model: LDH/100 (U/L) | ||||
| Intercept | 2.09 (1.56, 2.63) | P < 0.01 | 2.65 (1.76, 3.49) | P < 0.01 |
| ns(time at measurement in days) 1 | −2.45 (−2.70, −2.19) | P < 0.01 | −2.45 (−3.21, 1.69) | P < 0.01 |
| ns(time at measurement in days) 2 | −3.74 (−4.77, −2.80) | P < 0.01 | −3.32 (−5.36, −1.35) | P < 0.01 |
| ns(age in years) 1 | 2.39 (1.36, 3.40) | P < 0.01 | 1.16 (−0.47, 2.91) | P = 0.16 |
| ns(age in years) 2 | 0.86 (0.46, 1.25) | P < 0.01 | 0.44 (−0.33, 1.21) | P = 0.23 |
| Sex (Ref: women) | 0.27 (0.07, 0.47) | P = 0.01 | 0.29 (−0.01, 0.61) | P = 0.05 |
| Variables | log-hazard ratio (95% CI) | P | log-hazard ratio (95% CI) | P |
| Survival sub-model | ||||
| Baseline characteristics | ||||
| ns(age in years) 1 | - | - | 9.12 (2.17, 16.30) | P < 0.01 |
| ns(age in years) 2 | - | - | 3.96 (2.53, 5.38) | P < 0.01 |
| Sex (Ref: women) | - | - | 0.56 (0.07, 1.03) | P = 0.03 |
| Hematological biomarkers | - | |||
| log-lymphocytes (count × 103/µL) | −0.78 (−1.11, −0.44) | P < 0.01 | 0.02 (−0.43, 0.52) | P = 0.96 |
| log-neutrophils (count × 103/µL) | 1.56 (1.21, 1.91) | P < 0.01 | 0.83 (0.18, 1.52) | P = 0.02 |
| Coagulation biomarkers | ||||
| log-D-dimer (ng/mL) | 0.48 (0.31, 0.64) | P < 0.01 | Excluded due to the high number of missing values | |
| Biochemical biomarkers | ||||
| log-ferritin (ng/mL) | 0.55 (0.33, 0.79) | P < 0.01 | −0.12 (−0.45, 0.22) | P = 0.46 |
| log-C-reactive protein (mg/L) | 1.34 (1.05, 1.67) | P < 0.01 | 0.58 (0.25, 0.96) | P < 0.01 |
| glucose/100 (mg/dL) | 1.15 (0.78, 1.51) | P < 0.01 | 0.98 (0.37, 1.60) | P < 0.01 |
| LDH/100 (U/L) | 0.59 (0.49, 0.69) | P < 0.01 | 0.27 (0.11, 0.44) | P < 0.01 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Di Maso, M.; Delbue, S.; Sampietro, M.; Ferraroni, M.; Modenese, A.; Dolci, M.; Ambrogi, F.; Ferrante, P. Assessing the Association between Biomarkers and COVID-19 Mortality Using the Joint Modelling Approach. Life 2024, 14, 343. https://doi.org/10.3390/life14030343
Di Maso M, Delbue S, Sampietro M, Ferraroni M, Modenese A, Dolci M, Ambrogi F, Ferrante P. Assessing the Association between Biomarkers and COVID-19 Mortality Using the Joint Modelling Approach. Life. 2024; 14(3):343. https://doi.org/10.3390/life14030343
Chicago/Turabian StyleDi Maso, Matteo, Serena Delbue, Maurizio Sampietro, Monica Ferraroni, Annalisa Modenese, Maria Dolci, Federico Ambrogi, and Pasquale Ferrante. 2024. "Assessing the Association between Biomarkers and COVID-19 Mortality Using the Joint Modelling Approach" Life 14, no. 3: 343. https://doi.org/10.3390/life14030343
APA StyleDi Maso, M., Delbue, S., Sampietro, M., Ferraroni, M., Modenese, A., Dolci, M., Ambrogi, F., & Ferrante, P. (2024). Assessing the Association between Biomarkers and COVID-19 Mortality Using the Joint Modelling Approach. Life, 14(3), 343. https://doi.org/10.3390/life14030343







