Epidemiology and Management of Cerebral Venous Thrombosis during the COVID-19 Pandemic
Abstract
:1. Introduction
- Increased intracranial pressure with newly onset headache in 70 to 90% of patients [2], and less frequently papilledema and palsy of the abducent nerve;
- Seizures, which may affect as much as 34% of patients [3];
- Focal neurological deficits [4];
- Encephalopathy or coma, usually in the context of multiple sinus or deep venous occlusions;
- Specific regional syndromes, including periorbital pain, ocular chemosis, palsies of oculomotor cranial nerves and the ophthalmic division of the fifth cranial nerve (in the case of cavernous sinus thrombosis).
2. Materials and Methods
3. Results
4. Discussion
4.1. CVT Related to COVID-19 Infection: A Literature Review
4.2. CVT Associated with COVID-19 Vaccines
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stam, J. Thrombosis of the cerebral veins and sinuses. N. Engl. J. Med. 2005, 352, 1791–1798. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wasay, M.; Kojan, S.; Dai, A.I.; Bobustuc, G.; Sheikh, Z. Headache in Cerebral Venous Thrombosis: Incidence, pattern and location in 200 consecutive patients. J. Headache Pain. 2010, 11, 137–139. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lindgren, E.; Silvis, S.M.; Hiltunen, S.; Heldner, M.R.; Serrano, F.; de Scisco, M.; Zelano, J.; Zuurbier, S.M.; van Kammen, M.S.; Mansour, M.; et al. Acute symptomatic seizures in cerebral venous thrombosis. Neurology 2020, 95, e1706–e1715. [Google Scholar] [CrossRef]
- Ropper, A.H.; Klein, J.P. Cerebral Venous Thrombosis. N. Engl. J. Med. 2021, 385, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Coutinho, J.M.; Ferro, J.M.; Canhão, P.; Barinagarrementeria, F.; Cantú, C.; Bousser, M.G.; Stam, J. Cerebral venous and sinus thrombosis in women. Stroke 2009, 40, 2356–2361. [Google Scholar] [CrossRef] [Green Version]
- WHO Coronavirus (COVID-19) Dashboard. 2022. Available online: https://covid19.who.int (accessed on 26 May 2022).
- Dakay, K.; Cooper, J.; Bloomfield, J.; Overby, P.; Mayer, S.A.; Nuoman, R.; Sahni, R.; Gulko, E.; Kaur, G.; Santarelli, J.; et al. Cerebral Venous Sinus Thrombosis in COVID-19 Infection: A Case Series and Review of The Literature. J. Stroke Cereb. Dis. 2021, 30, 105434. [Google Scholar] [CrossRef] [PubMed]
- Al-Mufti, F.; Amuluru, K.; Sahni, R.; Bekelis, K.; Karimi, R.; Ogulnick, J.; Cooper, J.; Overby, P.; Nuoman, R.; Tiwari, A.; et al. Cerebral Venous Thrombosis in COVID-19: A New York Metropolitan Cohort Study. AJNR Am. J. Neuroradiol. 2021, 42, 1196–1200. [Google Scholar] [CrossRef]
- Devasagayam, S.; Wyatt, B.; Leyden, J.; Kleinig, T. Cerebral Venous Sinus Thrombosis Incidence Is Higher Than Previously Thought: A Retrospective Population-Based Study. Stroke 2016, 47, 2180–2182. [Google Scholar] [CrossRef]
- Coutinho, J.M.; Zuurbier, S.M.; Aramideh, M.; Stam, J. The incidence of cerebral venous thrombosis: A cross-sectional study. Stroke 2012, 43, 3375–3377. [Google Scholar] [CrossRef] [Green Version]
- Siegler, J.E.; Cardona, P.; Arenillas, J.F.; Talavera, B.; Guillen, A.N.; Chavarría-Miranda, A.; de Lera, M.; Khandelwal, P.; Bach, I.; Patel, P.; et al. Cerebrovascular events and outcomes in hospitalized patients with COVID-19: The SVIN COVID-19 Multinational Registry. Int. J. Stroke 2021, 16, 437–447. [Google Scholar] [CrossRef]
- Taquet, M.; Husain, M.; Geddes, J.R.; Luciano, S.; Harrison, P.J. Cerebral venous thrombosis and portal vein thrombosis: A retrospective cohort study of 537,913 COVID-19 cases. EClinicalMedicine 2021, 39, 101061. [Google Scholar] [CrossRef] [PubMed]
- Tu, T.M.; Goh, C.; Tan, Y.K.; Leow, A.S.; Pang, Y.Z.; Chien, J.; Shafi, H.; Pl Chan, B.; Hui, A.; Koh, J.; et al. Cerebral Venous Thrombosis in Patients with COVID-19 Infection: A Case Series and Systematic Review. J. Stroke Cereb. Dis. 2020, 29, 105379. [Google Scholar] [CrossRef] [PubMed]
- Silvis, S.M.; Middeldorp, S.; Zuurbier, S.M.; Cannegieter, S.C.; Coutinho, J.M. Risk Factors for Cerebral Venous Thrombosis. Semin. Thromb. Hemost. 2016, 42, 622–631. [Google Scholar] [CrossRef] [PubMed]
- Yaghi, S.; Shu, L.; Bakradze, E.; Salehi Omran, S.; Giles, J.A.; Amar, J.Y.; Henninger, N.; Elnazeir, M.; Liberman, A.; Moncrieffe, K.; et al. Direct Oral Anticoagulants Versus Warfarin in the Treatment of Cerebral Venous Thrombosis (ACTION-CVT): A Multicenter International Study. Stroke 2022, 53, 728–738. [Google Scholar] [CrossRef] [PubMed]
- Male, C.; Lensing, A.W.A.; Palumbo, J.S.; Kumar, R.; Nurmeev, I.; Hege, K.; Bonnet, D.; Connor, P.; Hooimeijer, H.; Torres, M.; et al. Rivaroxaban compared with standard anticoagulants for the treatment of acute venous thromboembolism in children: A randomised, controlled, phase 3 trial. Lancet Haematol. 2020, 7, e18–e27. [Google Scholar] [CrossRef]
- Saposnik, G.; Barinagarrementeria, F.; Brown, R.D.; Bushnell, C.D.; Cucchiara, B.; Cushman, M.; deVeber, G.; Ferro, J.M.; Tsai, F.Y. Diagnosis and management of cerebral venous thrombosis: A statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2011, 42, 1158–1192. [Google Scholar] [CrossRef] [Green Version]
- Siddiqui, F.M.; Dandapat, S.; Banerjee, C.; Zuurbier, S.M.; Johnson, M.; Stam, J.; Coutinho, J. Mechanical thrombectomy in cerebral venous thrombosis: Systematic review of 185 cases. Stroke 2015, 46, 1263–1268. [Google Scholar] [CrossRef]
- Ilyas, A.; Chen, C.J.; Raper, D.M.; Ding, D.; Buell, T.; Mastorakos, P.; Liu, K. Endovascular mechanical thrombectomy for cerebral venous sinus thrombosis: A systematic review. J. Neurointerv. Surg. 2017, 9, 1086–1092. [Google Scholar] [CrossRef]
- Medhi, G.; Parida, S.; Nicholson, P.; Senapati, S.B.; Padhy, B.P.; Pereira, V.M. Mechanical Thrombectomy for Cerebral Venous Sinus Thrombosis: A Case Series and Technical Note. World Neurosurg. 2020, 140, 148–161. [Google Scholar] [CrossRef]
- Liao, C.H.; Liao, N.C.; Chen, W.H.; Chen, H.C.; Shen, C.C.; Yang, S.F.; Tsuei, Y.S. Endovascular Mechanical Thrombectomy and On-Site Chemical Thrombolysis for Severe Cerebral Venous Sinus Thrombosis. Sci. Rep. 2020, 10, 4937. [Google Scholar] [CrossRef] [Green Version]
- Coutinho, J.M.; Zuurbier, S.M.; Bousser, M.G.; Ji, X.; Canhão, P.; Roos, Y.B.; Crassard, I.; Paiva Nunes, A.; Uyttenboogaart, M.; Chen, J.; et al. Effect of Endovascular Treatment With Medical Management vs Standard Care on Severe Cerebral Venous Thrombosis: The TO-ACT Randomized Clinical Trial. JAMA Neurol. 2020, 77, 966–973. [Google Scholar] [CrossRef] [PubMed]
- Baharvahdat, H.; Ahmadi, S.; Ganjeifar, B.; Etemadrezaie, H.; Zabyhian, S.; Sasannejad, P.; Bahadorkhan, G.; Mowla, A. Malignant Cerebral Venous Infarction: Decompressive Craniectomy versus Medical Treatment. World Neurosurg. 2019, 128, e918–e922. [Google Scholar] [CrossRef] [PubMed]
- Ferro, J.M.; Crassard, I.; Coutinho, J.M.; Canhão, P.; Barinagarrementeria, F.; Cucchiara, B.; Derex, L.; Lichy, C.; Masjuan, J.; Massaro, A.; et al. Decompressive surgery in cerebrovenous thrombosis: A multicenter registry and a systematic review of individual patient data. Stroke 2011, 42, 2825–2831. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zuurbier, S.M.; Coutinho, J.M.; Majoie, C.B.; Coert, B.A.; van den Munckhof, P.; Stam, J. Decompressive hemicraniectomy in severe cerebral venous thrombosis: A prospective case series. J. Neurol. 2012, 259, 1099–1105. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rizk, J.G.; Gupta, A.; Sardar, P.; Henry, B.M.; Lewin, J.C.; Lippi, G.; Lavie, C. Clinical Characteristics and Pharmacological Management of COVID-19 Vaccine-Induced Immune Thrombotic Thrombocytopenia With Cerebral Venous Sinus Thrombosis: A Review. JAMA Cardiol. 2021, 6, 1451–1460. [Google Scholar] [CrossRef]
- Abdalkader, M.; Shaikh, S.P.; Siegler, J.E.; Cervantes-Arslanian, A.M.; Tiu, C.; Radu, R.A.; Tiu, V.; Jillella, D.; Mansour, O.; Vera, V.; et al. Cerebral Venous Sinus Thrombosis in COVID-19 Patients: A Multicenter Study and Review of Literature. J. Stroke Cereb. Dis. 2021, 30, 105733. [Google Scholar] [CrossRef]
- Medicherla, C.B.; Pauley, R.A.; de Havenon, A.; Yaghi, S.; Ishida, K.; Torres, J.L. Cerebral Venous Sinus Thrombosis in the COVID-19 Pandemic. J. Neuroophthalmol. 2020, 40, 457–462. [Google Scholar] [CrossRef]
- Wang, W.; Sun, Q.; Bao, Y.; Liang, M.; Meng, Q.; Chen, H.; Li, J.; Wang, H.; Li, H.; Shi, Y.; et al. Analysis of Risk Factors for Thromboembolic Events in 88 Patients with COVID-19 Pneumonia in Wuhan, China: A Retrospective Descriptive Report. Med. Sci. Monit. 2021, 27, e929708. [Google Scholar] [CrossRef]
- Han, H.; Yang, L.; Liu, R.; Liu, F.; Wu, K.L.; Li, J.; Liu, X.H.; Zhu, C.L. Prominent changes in blood coagulation of patients with SARS-CoV-2 infection. Clin. Chem. Lab. Med. 2020, 58, 1116–1120. [Google Scholar] [CrossRef] [Green Version]
- Zhang, Y.; Xiao, M.; Zhang, S.; Xia, P.; Cao, W.; Jiang, W.; Chen, H.; Ding, X.; Zhao, H.; Zhang, H.; et al. Coagulopathy and Antiphospholipid Antibodies in Patients with Covid-19. N. Engl. J. Med. 2020, 382, e38. [Google Scholar] [CrossRef]
- Acanfora, D.; Acanfora, C.; Ciccone, M.M.; Scicchitano, P.; Bortone, A.S.; Uguccioni, M.; Casucci, G. The Cross-Talk between Thrombosis and Inflammatory Storm in Acute and Long-COVID-19: Therapeutic Targets and Clinical Cases. Viruses 2021, 13, 1904. [Google Scholar] [CrossRef] [PubMed]
- Cavalcanti, D.D.; Raz, E.; Shapiro, M.; Dehkharghani, S.; Yaghi, S.; Lillemoe, K.; Nossek, E.; Torres, J.; Jain, R.; Riin, H.A.; et al. Cerebral Venous Thrombosis Associated with COVID-19. AJNR Am. J. Neuroradiol. 2020, 41, 1370–1376. [Google Scholar] [CrossRef] [PubMed]
- Girot, M.; Ferro, J.M.; Canhão, P.; Stam, J.; Bousser, M.G.; Barinagarrementeria, F.; Leys, D. Predictors of outcome in patients with cerebral venous thrombosis and intracerebral hemorrhage. Stroke 2007, 38, 337–342. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ghosh, R.; Roy, D.; Mandal, A.; Pal, S.K.; Chandra Swaika, B.; Naga, D.; Pandit, A.; Ray, B.K.; Benito-Léon, J. Cerebral venous thrombosis in COVID-19. Diabetes. Metab. Syndr. 2021, 15, 1039–1045. [Google Scholar] [CrossRef] [PubMed]
- Goeijenbier, M.; van Wissen, M.; van de Weg, C.; Jong, E.; Gerdes, V.E.; Meijers, J.C.; Brandjes, D.P.M.; van Gorp, E.C.M. Review: Viral infections and mechanisms of thrombosis and bleeding. J. Med. Virol. 2012, 84, 1680–1696. [Google Scholar] [CrossRef]
- Becker, R.C. COVID-19 update: Covid-19-associated coagulopathy. J. Thromb. Thrombolysis 2020, 50, 54–67. [Google Scholar] [CrossRef]
- Eskey, C.J.; Meyers, P.M.; Nguyen, T.N.; Ansari, S.A.; Jayaraman, M.; McDougall, C.G.; DeMarco, J.K.; Gray, W.A.; Hess, D.C.; Higashida, R.T.; et al. Indications for the Performance of Intracranial Endovascular Neurointerventional Procedures: A Scientific Statement From the American Heart Association. Circulation 2018, 137, e661–e689. [Google Scholar] [CrossRef]
- Bousser, M.G.; Ferro, J.M. Cerebral venous thrombosis: An update. Lancet Neurol. 2007, 6, 162–170. [Google Scholar] [CrossRef]
- Sharifian-Dorche, M.; Bahmanyar, M.; Sharifian-Dorche, A.; Mohammadi, P.; Nomovi, M.; Mowla, A. Vaccine-induced immune thrombotic thrombocytopenia and cerebral venous sinus thrombosis post COVID-19 vaccination, a systematic review. J. Neurol. Sci. 2021, 428, 117607. [Google Scholar] [CrossRef]
- Sangli, S.; Virani, A.; Cheronis, N.; Vannatter, B.; Minich, C.; Noronha, S.; Bhagavatula, R.; Speredelozzi, D.; Sareen, M.; Kaplan, R.B. Thrombosis With Thrombocytopenia After the Messenger RNA-1273 Vaccine. Ann. Intern. Med. 2021, 174, 1480–1482. [Google Scholar] [CrossRef]
- Smadja, D.M.; Yue, Q.Y.; Chocron, R.; Sanchez, O.; Lillo-Le Louet, A. Vaccination against COVID-19: Insight from arterial and venous thrombosis occurrence using data from VigiBase. Eur. Respir. J. 2021, 58. [Google Scholar] [CrossRef] [PubMed]
- Schulz, J.B.; Berlit, P.; Diener, H.C.; Gerloff, C.; Greinacher, A.; Klein, C.; Petzold, G.C.; Piccininni, M.; Poli, S.; Röhrig, R.; et al. COVID-19 Vaccine-Associated Cerebral Venous Thrombosis in Germany. Ann. Neurol. 2021, 90, 627–639. [Google Scholar] [CrossRef] [PubMed]
- Franchini, M.; Liumbruno, G.M.; Pezzo, M. COVID-19 vaccine-associated immune thrombosis and thrombocytopenia (VITT): Diagnostic and therapeutic recommendations for a new syndrome. Eur. J. Haematol. 2021, 107, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Palaiodimou, L.; Stefanou, M.I.; Katsanos, A.H.; Aguiar de Sousa, D.; Coutinho, J.M.; Lagiou, P.; Michopoulos, I.; Naska, A.; Giannopoulos, S.; Vadikolias, K.; et al. Cerebral Venous Sinus Thrombosis and Thrombotic Events After Vector-Based COVID-19 Vaccines: A Systematic Review and Meta-analysis. Neurology 2021, 97, e2136–e2147. [Google Scholar] [CrossRef]
- See, I.; Su, J.R.; Lale, A.; Woo, E.J.; Guh, A.Y.; Shimabukuro, T.T.; Streiff, M.B.; Rao, A.K.; Wheeler, A.P.; Beavers, S.F.; et al. US Case Reports of Cerebral Venous Sinus Thrombosis With Thrombocytopenia After Ad26.COV2.S Vaccination, March 2 to April 21, 2021. JAMA 2021, 325, 2448–2456. [Google Scholar] [CrossRef]
- Gupta, A.; Sardar, P.; Cash, M.E.; Milani, R.V.; Lavie, C.J. Covid-19 vaccine- induced thrombosis and thrombocytopenia-a commentary on an important and practical clinical dilemma. Prog. Cardiovasc. Dis. 2021, 67, 105–107. [Google Scholar] [CrossRef]
- Perry, R.J.; Tamborska, A.; Singh, B.; Craven, B.; Marigold, R.; Arthur-Farraj, P.; Yeo, J.M.; Zhang, L.; Hassan-Smith, G.; Jones, M.; et al. Cerebral venous thrombosis after vaccination against COVID-19 in the UK: A multicentre cohort study. Lancet 2021, 398, 1147–1156. [Google Scholar] [CrossRef]
- Dias, L.; Soares-Dos-Reis, R.; Meira, J.; Ferrão, D.; Soares, P.R.; Pastor, A.; Gama, G.; Fonseca, L.; Fagundes, V.; Carvalho, M. Cerebral Venous Thrombosis after BNT162b2 mRNA SARS-CoV-2 vaccine. J. Stroke Cerebrovasc. Dis. 2021, 30, 105906. [Google Scholar] [CrossRef]
- Warkentin, T.E. High-dose intravenous immunoglobulin for the treatment and prevention of heparin-induced thrombocytopenia: A review. Expert Rev Hematol. 2019, 12, 685–698. [Google Scholar] [CrossRef]
- Scully, M.; Singh, D.; Lown, R.; Poles, A.; Solomon, T.; Levi, M.; Goldblatt, D.; Kotoucek, P.; Thomas, W.; Lester, W. Pathologic Antibodies to Platelet Factor 4 after ChAdOx1 nCoV-19 Vaccination. N. Engl. J. Med. 2021, 384, 2202–2211. [Google Scholar] [CrossRef]
- Goel, R.; Ness, P.M.; Takemoto, C.M.; Krishnamurti, L.; King, K.E.; Tobian, A.A. Platelet transfusions in platelet consumptive disorders are associated with arterial thrombosis and in-hospital mortality. Blood 2015, 125, 1470–1476. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schell, A.M.; Petras, M.; Szczepiorkowski, Z.M.; Ornstein, D.L. Refractory heparin induced thrombocytopenia with thrombosis (HITT) treated with therapeutic plasma exchange and rituximab as adjuvant therapy. Transfus. Apher. Sci. 2013, 49, 185–188. [Google Scholar] [CrossRef] [PubMed]
- Tiede, A.; Sachs, U.J.; Czwalinna, A.; Werwitzke, S.; Bikker, R.; Krauss, J.K.; Donnerstag, F.; WeiBenborn, K.; Hölinger, G.; Maasoumy, B.; et al. Prothrombotic immune thrombocytopenia after COVID-19 vaccination. Blood 2021, 138, 350–353. [Google Scholar] [CrossRef] [PubMed]
- Thakur, K.T.; Tamborska, A.; Wood, G.K.; McNeill, E.; Roh, D.; Akpan, I.J.; Miller, E.; Bautista, A.; Classeen, J.; Kim, C.Y.; et al. Clinical review of cerebral venous thrombosis in the context of COVID-19 vaccinations: Evaluation, management, and scientific questions. J. Neurol. Sci. 2021, 427, 117532. [Google Scholar] [CrossRef] [PubMed]

| Gender | Age | Vaccination | Risk Factors | Time from COVID to CVT (Days) | Neuroimage | Treatment | Complications | Disclosure |
|---|---|---|---|---|---|---|---|---|
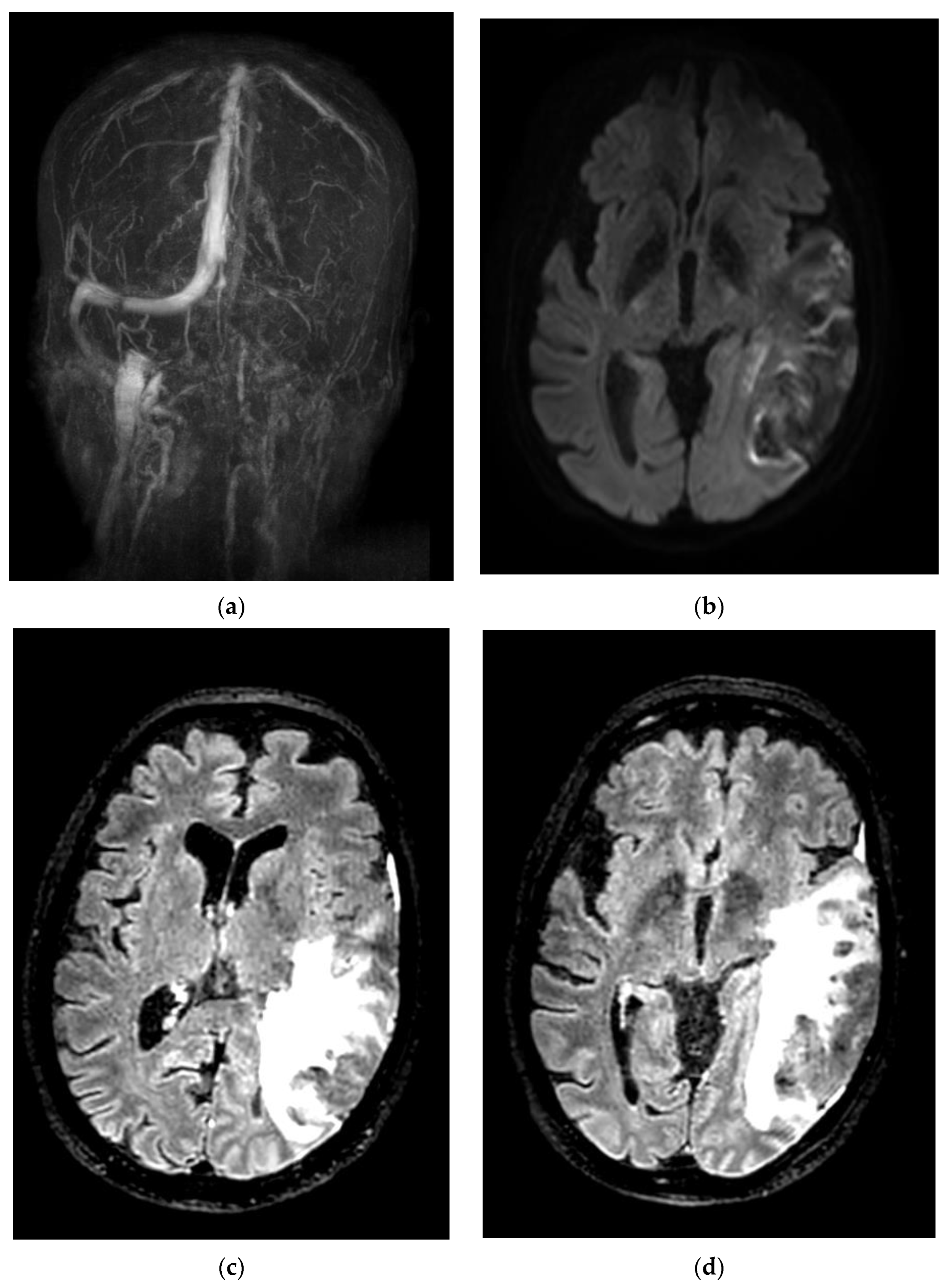
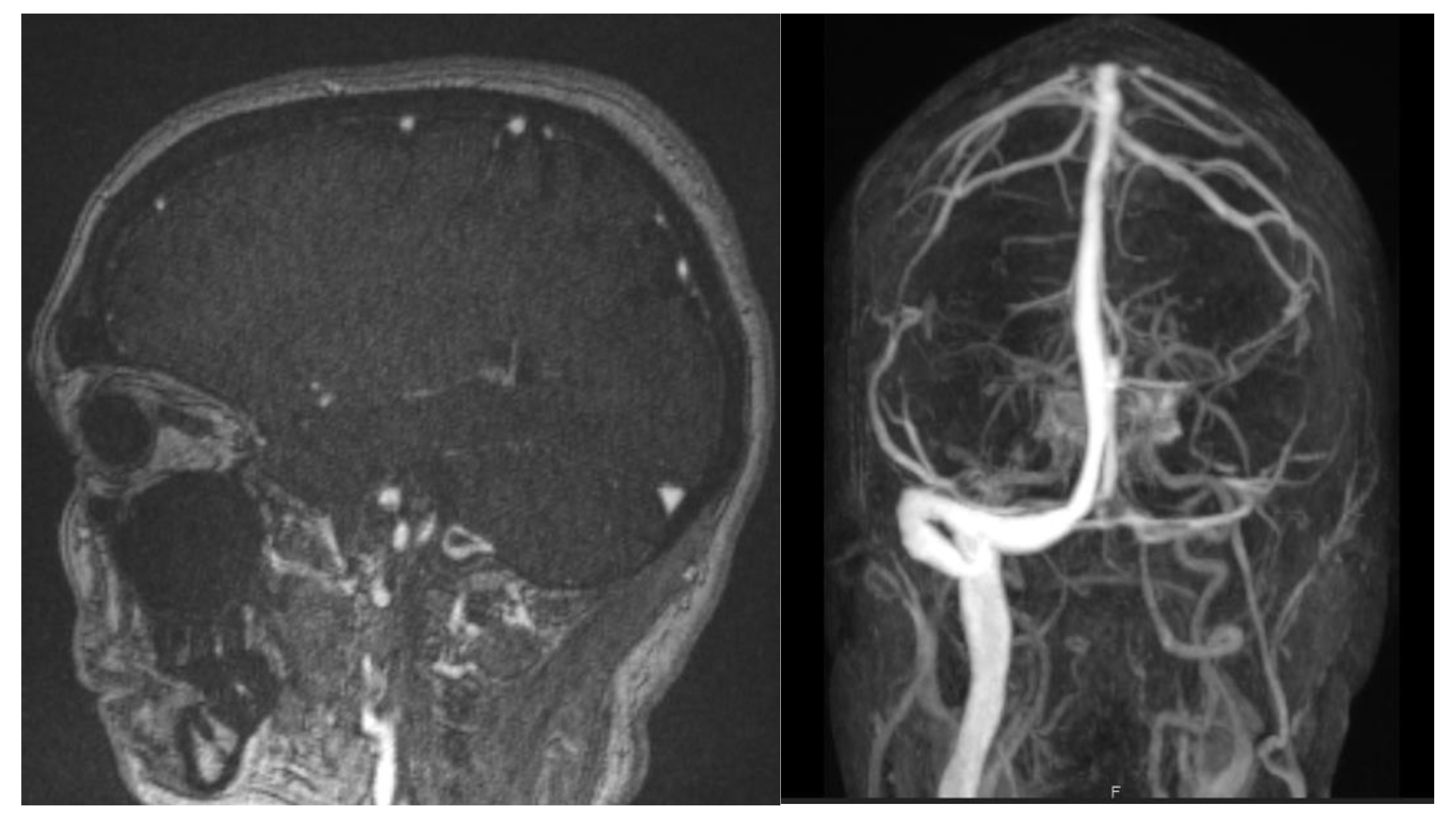
| F | 61 | No | No | 15 | Thrombosis in multiple sinuses (internal cerebral vein, Galen vein, right sinus, torcula, left lateral sinus) | LMWH, craniectomy, thrombectomy | Epilepsy | Death |
| F | 54 | No | Previous cancer, under Tamoxifen | 0 | Left transverse and sigmoid sinus thrombosis, with left temporal and parietal hemorrhagic infarct | LMWH | Neuropsychiatric alterations | Transferred to Psychiatry, not fully recovered. Persistence of cognitive disorders. |
| F | 52 | Yes (Astra Zeneca) | 5 miscarriages, SAPL-negative | 18 | Right lateral and sigmoid sinus thrombosis | LMWH then apixaban | None | Discharged with no complications |
| F | 31 | No | No | 30 | Right lateral sinus and superior sagittal sinus thrombosis | LMWH | None | Discharged with no complications |
| F | 31 | No | Oral contraceptive, anemia Hb 7 g/dL | 30 | Right lateral and sigmoid sinus thrombosis | LMWH followed by Dabigatran | None | Discharged with no complications |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Novaes, N.; Sadik, R.; Sadik, J.-C.; Obadia, M. Epidemiology and Management of Cerebral Venous Thrombosis during the COVID-19 Pandemic. Life 2022, 12, 1105. https://doi.org/10.3390/life12081105
Novaes N, Sadik R, Sadik J-C, Obadia M. Epidemiology and Management of Cerebral Venous Thrombosis during the COVID-19 Pandemic. Life. 2022; 12(8):1105. https://doi.org/10.3390/life12081105
Chicago/Turabian StyleNovaes, Natalia, Raphaël Sadik, Jean-Claude Sadik, and Michaël Obadia. 2022. "Epidemiology and Management of Cerebral Venous Thrombosis during the COVID-19 Pandemic" Life 12, no. 8: 1105. https://doi.org/10.3390/life12081105
APA StyleNovaes, N., Sadik, R., Sadik, J.-C., & Obadia, M. (2022). Epidemiology and Management of Cerebral Venous Thrombosis during the COVID-19 Pandemic. Life, 12(8), 1105. https://doi.org/10.3390/life12081105







