Effectiveness of CPR in Hypogravity Conditions—A Systematic Review
Abstract
:1. Introduction
2. Materials and Methods
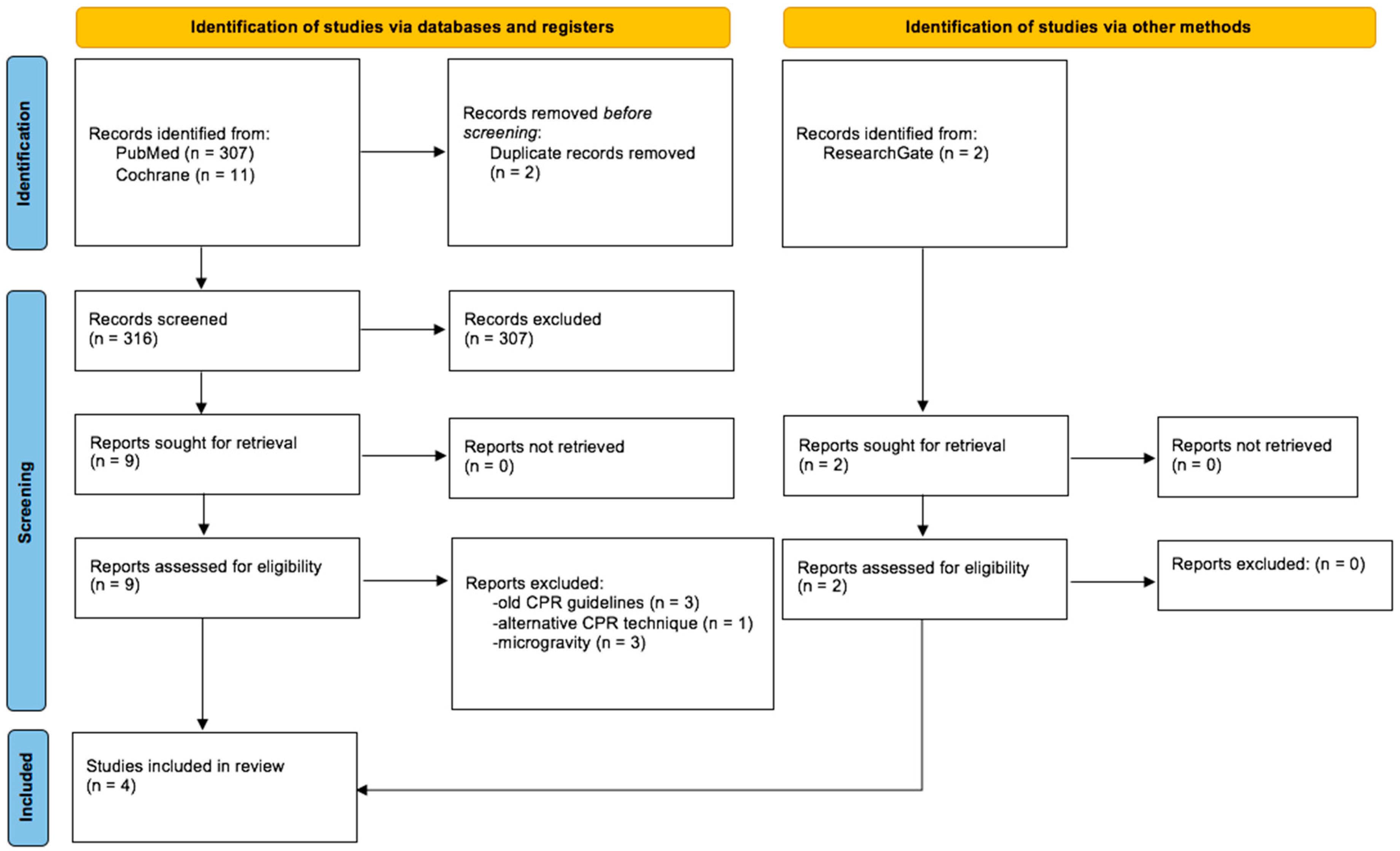
2.1. Search Strategy
2.2. Eligibility Criteria and Data Collection
3. Results
3.1. Study Characteristics
3.2. Risk of Bias
- (1)
- Selection Bias: Do participants represent possible astronauts concerning variability of for example gender, age, or weight?
- (2)
- Order Bias: Is the order of gravity conditions randomized to eliminate influence of fatigue or learning effect?
- (3)
- Intervention Bias: Do setting and surroundings of intervention adequately resemble an emergency in hypogravity?
- (4)
- Reporting Bias: Is there any selective reporting or missing data?
3.3. CPR Quality
3.4. Physical Effort
| Publication | 1 G | Post-Heart Rate 0.38 G | 0.17 G/0.16 G |
|---|---|---|---|
| Baptista | 107.43 (17.12) | 121.29 (27.03) | ----- |
| Mackaill | 130 (11.4) | 127 (13.9) | 130 (20.3) |
| Russomano | 117 (21) | 140 (21) | ------ |
| Sriharan * | 106.18 (14.71) | 108.97 (20.53) | 108.54 (19.34) |
| Publication | 1 G | VO2peak 0.38 G | 0.17 G/0.16 G | 1 G | Ve 0.38 G | 0.17 G/0.16 G |
|---|---|---|---|---|---|---|
| Russomano | 16.4 (4.5) | 21.8 (8.1) | ----- | 27.5 (7.9) | 40.6 (10.2) | ----- |
| Sriharan * | 14.4 (7.8) | 16.8 (7.2) | 15.9 (6.2) | 20.6 (11.7) | 23.7 (10.6) | 22.9 (8.8) |
| Publication | 1 G | BORG 0.38 G | 0.17 G/0.16 G |
|---|---|---|---|
| Baptista | 9.33 (2.29) | 12.42 (1.78) | --- |
| Russomano * | 10.2 | 13.2 | |
| Sriharan ** | 10.5 (2.7) | 11.4 (2.4) | 11.9 (2.8) |
3.5. Elbow Flexion
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CPR | Cardiopulmonary Resuscitation |
| AHA | American Heart Association |
| NASA | National Aeronautics and Space Administration |
| VO2peak | Peak Oxygen Consumption |
| Ve | Minute Ventilation |
| BLS | Basic Life Support |
| ALS | Advanced Life Support |
| SeAL | Seated-Arm-Lock |
| MR | Mackaill–Russomano |
| ROSC | Return of Spontaneous Circulation |
| EVA | Extravehicular Activity |
| EMG | Electromyography |
| CD | Compression Depth |
| CR | Compression Rate |
| BSD | Body-Suspension Device |
References
- Sasson, C.; Rogers, M.F.; Dahl, J.; Kellermann, A.L. Predictors of survival from out-of-hospital cardiac arrest: A systematic review and meta-analysis. Circ. Cardiovasc. Qual. Outcomes 2010, 3, 63–81. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Merchant, R.M.; Panchal, A.R.; Cheng, A.; Aziz, K.; Berg, K.M.; Lavonas, E.J.; Magid, D.J. Part 1: Executive Summary: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2020, 142, S337–S357. [Google Scholar] [CrossRef]
- Komorowski, M.; Fleming, S.; Mawkin, M.; Hinkelbein, J. Anaesthesia in austere environments: Literature review and considerations for future space exploration missions. NPJ Microgravity 2018, 4, 5. [Google Scholar] [CrossRef] [PubMed]
- Hinkelbein, J.; Russomano, T.; Hinkelbein, F.; Komorowski, M. Cardiac arrest during space missions: Specificities and challenges. Trends Anaesth. Crit. Care 2018, 19, 6–12. [Google Scholar] [CrossRef] [Green Version]
- Boerma, M.; Nelson, G.A.; Sridharan, V.; Mao, X.W.; Koturbash, I.; Hauer-Jensen, M. Space radiation and cardiovascular disease risk. World J. Cardiol. 2015, 7, 882–888. [Google Scholar] [CrossRef]
- Hodkinson, P.D.; Anderton, R.A.; Posselt, B.N.; Fong, K.J. An overview of space medicine. Br. J. Anaesth. 2017, 119, i143–i153. [Google Scholar] [CrossRef] [Green Version]
- Antonsen, E.A.-O.; Myers, J.A.-O.; Boley, L.; Arellano, J.; Kerstman, E.; Kadwa, B.; Buckland, D.M.; Van Baalen, M. Estimating medical risk in human spaceflight. NPJ Microgravity 2022, 8, 8. [Google Scholar] [CrossRef]
- Summers, R.L.; Johnston, S.L.; Marshburn, T.H.; Williams, D.R. Emergencies in Space. Ann. Emerg. Med. 2005, 46, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Criley, J.M.; Niemann, J.T.; Rosborough, J.P. Cardiopulmonary resuscitation research 1960–1984: Discoveries and advances. Ann. Emerg. Med. 1984, 13, 756–758. [Google Scholar] [CrossRef]
- Braunecker, S.; Douglas, B.; Hinkelbein, J. Comparison of different techniques for in microgravity—A simple mathematic estimation of cardiopulmonary resuscitation quality for space environment. Am. J. Emerg. Med. 2015, 33, 920–924. [Google Scholar] [CrossRef]
- Schmitz, J.; Ahlbäck, A.; DuCanto, J.; Kerkhoff, S.; Komorowski, M.; Löw, V.; Russomano, T.; Starck, C.; Thierry, S.; Warnecke, T.; et al. Randomized Comparison of Two New Methods for Chest Compressions during CPR in Microgravity-A Manikin Study. J. Clin. Med. 2022, 11, 646. [Google Scholar] [CrossRef] [PubMed]
- Evetts, S.N.; Evetts, L.M.; Russomano, T.; Castro, J.C.; Ernsting, J. Basic life support in microgravity: Evaluation of a novel method during parabolic flight. Aviat. Space Environ. Med. 2005, 76, 506–510. [Google Scholar]
- Jay, G.D.; Lee, P.; Goldsmith, H.; Battat, J.; Maurer, J.; Suner, S. CPR effectiveness in microgravity: Comparison of three positions and a mechanical device. Aviat. Space Environ. Med. 2003, 74, 1183–1189. [Google Scholar]
- Hinkelbein, J.; Kerkhoff, S.; Adler, C.; Ahlbäck, A.; Braunecker, S.; Burgard, D.; Cirillo, F.; De Robertis, E.; Glaser, E.; Haidl, T.M.; et al. Cardiopulmonary resuscitation (CPR) during spaceflight—A guideline for CPR in microgravity from the German Society of Aerospace Medicine (DGLRM) and the European Society of Aerospace Medicine Space Medicine Group (ESAM-SMG). Scand. J. Trauma Resusc. Emerg. Med. 2020, 28, 108. [Google Scholar] [CrossRef] [PubMed]
- Borg, G. Perceived exertion as an indicator of somatic stress. Scand J. Rehabil. Med. 1970, 2, 92–98. [Google Scholar]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Syst. Rev. 2021, 10, 89. [Google Scholar] [CrossRef]
- Mackaill, C.; Sponchiado, G.; Leite, A.K.; Dias, P.; Da Rosa, M.; Brown, E.J.; de Lima, J.C.M.; Rehnberg, L.; Russomano, T. A new method for the performance of external chest compressions during hypogravity simulation. Life Sci. Space Res. 2018, 18, 72–79. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Russomano, T.; Baers, J.H.; Velho, R.; Cardoso, R.B.; Ashcroft, A.; Rehnberg, L.; Gehrke, R.D.; Dias, M.K.P.; Baptista, R.R. A comparison between the 2010 and 2005 basic life support guidelines during simulated hypogravity and microgravity. Extrem. Physiol. Med. 2013, 2, 11. [Google Scholar] [CrossRef] [Green Version]
- Baptista, R.; Susin, T.; Dias, M.; Corria, N.; Cardoso, R.; Russomano, T. Muscle Activity during the Performance of CPR in Simulated Microgravity and Hypogravity. Am. J. Med. Biol. Res. 2015, 3, 82–87. [Google Scholar]
- Sriharan, S.; Kay, G.; Lee, J.C.Y.; Pollock, R.D.; Russomano, T. Cardiopulmonary Resuscitation in Hypogravity Simulation. Aerosp. Med. Hum. Perform. 2021, 92, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Russomano, T.; Rehnberg, L. Extraterrestrial CPR and Its Applications in Terrestrial Medicine. In Resuscitation Aspects, [Internet]; Aslanidis, T., Ed.; IntechOpen: London, UK, 2017; Available online: https://www.intechopen.com/chapters/56577 (accessed on 1 August 2022).
- Higgins, J.P.T.; Chandler, J.; Cumpston, M.; Li, T.; Page, M.J.; Welch, V.A. Cochrane Handbook for Systematic Reviews of Interventions, version 6.2 (updated February 2021); Cochrane, London, UK. 2021. Available online: http://www.training.cochrane.org/handbook (accessed on 1 August 2021).
- Sides, M.B.; Vernikos, J.; Convertino, V.A.; Stepanek, J.; Tripp, L.D.; Draeger, J.; Hargens, A.R.; Kourtidou-Papadeli, C.; Pavy-LeTraon, A.; Russomano, T.; et al. The Bellagio Report: Cardiovascular risks of spaceflight: Implications for the future of space travel. Aviat. Space Environ. Med. 2005, 76, 877–895. [Google Scholar]
- West, J.B. Physiology in microgravity. J. Appl. Physiol. 2000, 89, 379–384. [Google Scholar] [CrossRef]
- Tanaka, K.; Nishimura, N.; Kawai, Y. Adaptation to microgravity, deconditioning, and countermeasures. J. Physiol. Sci. 2017, 67, 271–281. [Google Scholar] [CrossRef] [PubMed]
- Vernice, N.A.-O.; Meydan, C.; Afshinnekoo, E.; Mason, C.E. Long-term spaceflight and the cardiovascular system. Precis Clin. Med. 2020, 3, 284–291. [Google Scholar] [CrossRef]
- Meck, J.V.; Reyes, C.J.; Perez, S.A.; Goldberger, A.L.; Ziegler, M.G. Marked exacerbation of orthostatic intolerance after long- vs. short-duration spaceflight in veteran astronauts. Psychosom. Med. 2001, 63, 865–873. [Google Scholar] [CrossRef] [PubMed]
- Dalmarco, G.; Calder, A.; Falcão, F.; de Azevedo, D.F.; Sarkar, S.; Evetts, S.; Moniz, S.; Russomano, T. Evaluation of external cardiac massage performance during hypogravity simulation. Conf. Proc. Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. 2006, 2006, 2904–2907. [Google Scholar]
- Panchal, A.R.; Bartos, J.A.; Cabañas, J.G.; Donnino, M.W.; Drennan, I.R.; Hirsch, K.G.; Kudenchuk, P.J.; Kurz, M.C.; Lavonas, E.J.; Morley, P.T.; et al. Part 3: Adult Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2020, 142, S366–S468. [Google Scholar] [CrossRef] [PubMed]
- Kordi, M.; Kluge, N.; Kloeckner, M.; Russomano, T. Gender influence on the performance of chest compressions in simulated hypogravity and microgravity. Aviat. Space Environ. Med. 2012, 83, 643–648. [Google Scholar] [CrossRef]
- Krygiel, R.G.; Waye, A.B.; Baptista, R.R.; Heidner, G.S.; Rehnberg, L.; Russomano, T. The evaluation of upper body muscle activity during the performance of external chest compressions in simulated hypogravity. Life Sci. Space Res. 2014, 1, 60–66. [Google Scholar] [CrossRef]
- Kaminska, H.; Wieczorek, W.; Matusik, P.; Czyzewski, L.; Ladny, J.R.; Smereka, J.; Filipiak, K.J.; Szarpak, L. Factors influencing high-quality chest compressions during cardiopulmonary resuscitation scenario, according to 2015 American Heart Association Guidelines. Kardiol. Pol. 2018, 76, 642–647. [Google Scholar] [CrossRef] [Green Version]
- Miller, A.E.; Tarnopolsky, M.A.; Sale, D.G. Gender differences in strength and muscle fiber characteristics. Eur. J. Appl. Physiol. Occup. Physiol. 1993, 66, 254–262. [Google Scholar] [CrossRef] [PubMed]
- Harm, D.L.; Jennings, R.T.; Meck, J.V.; Powell, M.R.; Putcha, L.; Sams, C.P.; Schneider, S.M.; Shackelford, L.C.; Smith, S.M.; Whitson, P.A. Genome and Hormones: Gender Differences in Physiology Invited Review: Gender issues related to spaceflight: A NASA perspective. J. Appl. Physiol. 2001, 91, 2374–2383. [Google Scholar] [CrossRef] [PubMed]
- Lurie, K.G.; Nemergut, E.C.; Yannopoulos, D.; Sweeney, M. The Physiology of Cardiopulmonary Resuscitation. Anesth. Analg. 2016, 122, 767–783. [Google Scholar] [CrossRef] [PubMed]
- Sugerman, N.T.; Edelson, D.P.; Leary, M.; Weidman, E.K.; Herzberg, D.L.; Vanden Hoek, T.L.; Becker, L.B.; Abella, B.S. Rescuer fatigue during actual in-hospital cardiopulmonary resuscitation with audiovisual feedback: A prospective multicenter study. Resuscitation 2009, 80, 981–984. [Google Scholar] [CrossRef] [Green Version]
- Benyoucef, Y.; Keady, T.; Marwaha, N. The Seated Arm-Lock Method: A New Concept of Basic Life Support in Simulated Hypogravity of the Moon and Mars. J. Space Saf. Eng. 2014, 1, 28–31. [Google Scholar] [CrossRef]
- Supatanakij, P.; Yuksen, C.; Chantawong, T.; Sawangwong, P.; Jenpanitpong, C.; Patchkrua, J.; Kanchayawong, P. Straddle versus Conventional Chest Compressions in a Confined Space; a Comparative Study. Arch. Acad. Emerg. Med. 2020, 9, e4. [Google Scholar]
- Demontis, G.C.; Germani, M.M.; Caiani, E.G.; Barravecchia, I.; Passino, C.; Angeloni, D. Human Pathophysiological Adaptations to the Space Environment. Front. Physiol. 2017, 8, 547. [Google Scholar] [CrossRef]
- Norcross, J.R.; Clark, T.; Harvill, L.; Morency, R.M.; Stroud, L.C.; Desantis, L.; Vos, J.R.; Gernhardt, M.L. Metabolic Costs and Biomechanics of Level Ambulation in a Planetary Suit; National Aeronautics and Space Administration, Johnson Space Center, NASA Technical Publication: Houston, TX, USA, 2010. [Google Scholar]
- Bonnes, J.L.; Brouwer, M.A.; Navarese, E.P.; Verhaert, D.V.; Verheugt, F.W.; Smeets, J.L.; de Boer, M.-J. Manual Cardiopulmonary Resuscitation Versus CPR Including a Mechanical Chest Compression Device in Out-of-Hospital Cardiac Arrest: A Comprehensive Meta-analysis from Randomized and Observational Studies. Ann. Emerg. Med. 2016, 67, 349–360.e3. [Google Scholar] [CrossRef]

| Publication | Participants | % Males/Females | Age (Years) | Weight (kg) |
|---|---|---|---|---|
| Baptista | 30 | 100/0 | 22 (3.0) | 78.9 (10.6) |
| Mackaill | 10 | --- | 24.5 (2,8) | 74.2 (11.1) |
| Russomano | 30 | 100/0 | 22.5 (3.5) | 78.2 (13.1) |
| Sriharan | 21 | 52.3/47.7 | 28.7 (5.7) | 72.9 (16) |
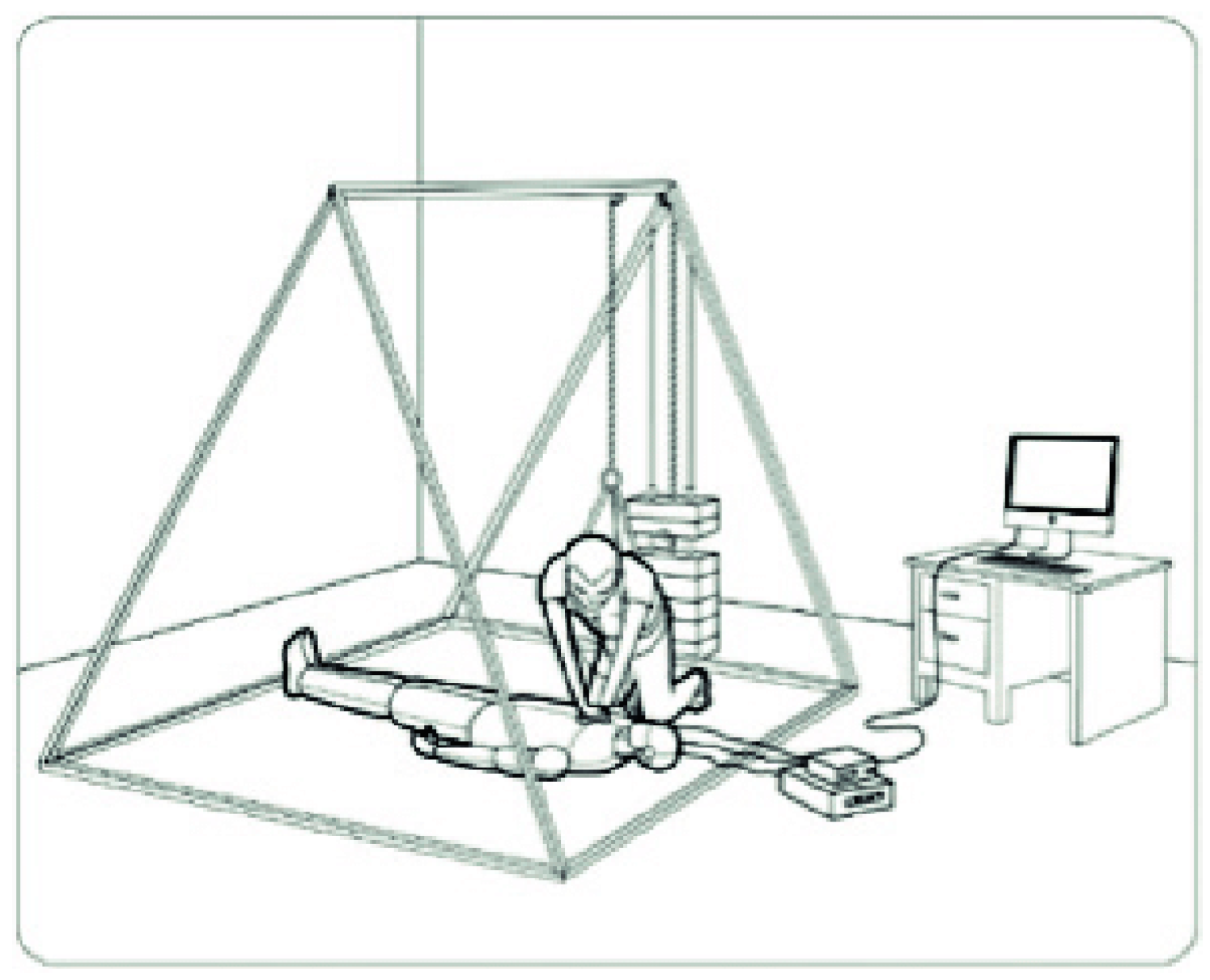
| Publication | Guideline | Simulation | Protocol | Feedback CD | Feedback CR | Hypogravity |
|---|---|---|---|---|---|---|
| Baptista | AHA 2010 | Body-Suspension Device | 3 × 30c | Visual * | Verbal | 0.38 G |
| Mackaill | ERC 2015 | Body-Suspension Device | 3 × 30c | Visual * | Metronome ** | 0.38 G + 0.17 G |
| Russomano | ERC 2010 | Body-Suspension Device | 4 × 30c | Visual * | Metronome ** | 0.38 G |
| Sriharan | ERC 2015 | Body-Suspension Device | 5 min | Verbal initial 20 s | Verbal initial 20 s | 0.38 G + 0.16 G |
| Publication | Selection Bias | Order Bias | Intervention Bias | Reporting Bias |
|---|---|---|---|---|
| Baptista | x | -- | -- | -- |
| Mackaill | x | -- | -- | + |
| Russomano | x | + | -- | + |
| Sriharan | -- | + | + | + |
| Publication | 1 G | Compression Depth 0.38 G | 0.17 G/0.16 G | 1 G | Compression Rate 0.38 G | 0.17 G/0.16 G |
|---|---|---|---|---|---|---|
| Baptista | 48.09 (2.61) | 45.92 (2.84) | ------ | # | # | ----- |
| Mackaill ** | 56.6 (2.0) | 49.4 (3.4) | 44.0 (3.5) | 101.7 | 106.4 | 106.4 |
| Russomano | 57.0 (2.3) | 55.1 (3.7) | ------ | 104.25 (3.5) | 103 (5.3) | ------ |
| Sriharan * | 52.94 (10.48) | 44.23 (9.98) | 43.09 (9.55) | 107.39 (6.59) | 107.75 (6.75) | 108.14 (7.41) |
| Publication | 1 G | Elbow Flexion 0.38 G | 0.17 G/0.16 G |
|---|---|---|---|
| Mackaill | 3.8 (1.5) | 6.5 (1.6) | 8.6 (3.1) |
| Russomano | 4.3 (2.8) | 14.0 (8.1) | ------ |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Overbeek, R.; Schmitz, J.; Rehnberg, L.; Benyoucef, Y.; Dusse, F.; Russomano, T.; Hinkelbein, J. Effectiveness of CPR in Hypogravity Conditions—A Systematic Review. Life 2022, 12, 1958. https://doi.org/10.3390/life12121958
Overbeek R, Schmitz J, Rehnberg L, Benyoucef Y, Dusse F, Russomano T, Hinkelbein J. Effectiveness of CPR in Hypogravity Conditions—A Systematic Review. Life. 2022; 12(12):1958. https://doi.org/10.3390/life12121958
Chicago/Turabian StyleOverbeek, Remco, Jan Schmitz, Lucas Rehnberg, Yacine Benyoucef, Fabian Dusse, Thais Russomano, and Jochen Hinkelbein. 2022. "Effectiveness of CPR in Hypogravity Conditions—A Systematic Review" Life 12, no. 12: 1958. https://doi.org/10.3390/life12121958
APA StyleOverbeek, R., Schmitz, J., Rehnberg, L., Benyoucef, Y., Dusse, F., Russomano, T., & Hinkelbein, J. (2022). Effectiveness of CPR in Hypogravity Conditions—A Systematic Review. Life, 12(12), 1958. https://doi.org/10.3390/life12121958







