Caregivers’ Perspectives on Human–Robot Collaboration in Inpatient Elderly Care Settings
Abstract
1. Introduction
1.1. Robotics in Healthcare and Caregivers’ Perspective
1.2. Objectives
2. Materials and Methods
2.1. Recruitment
2.2. Participants
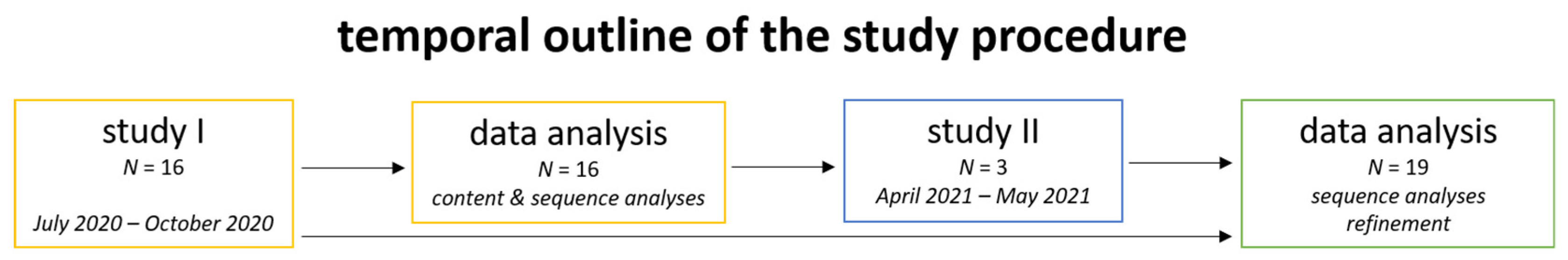
2.3. Procedure
2.4. Addressed Topics of the Semi-Structured Interviews
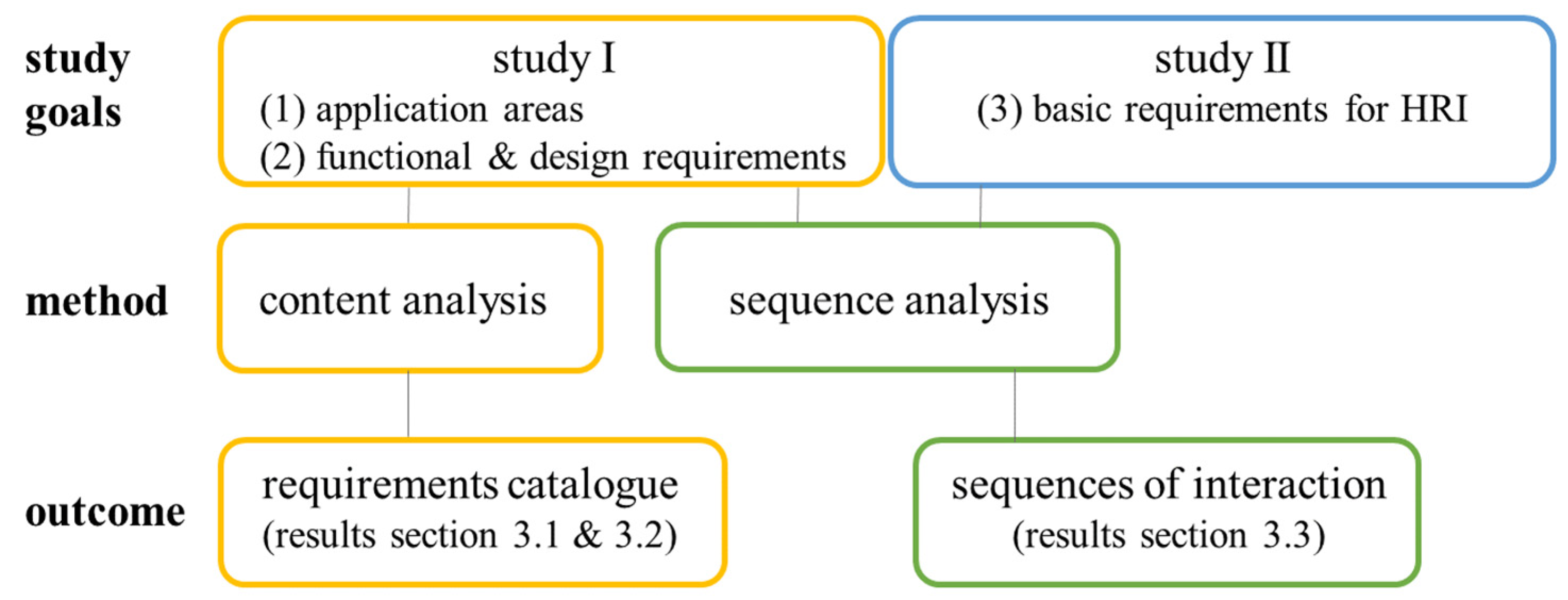
2.5. Data Analysis
2.5.1. Content Analysis
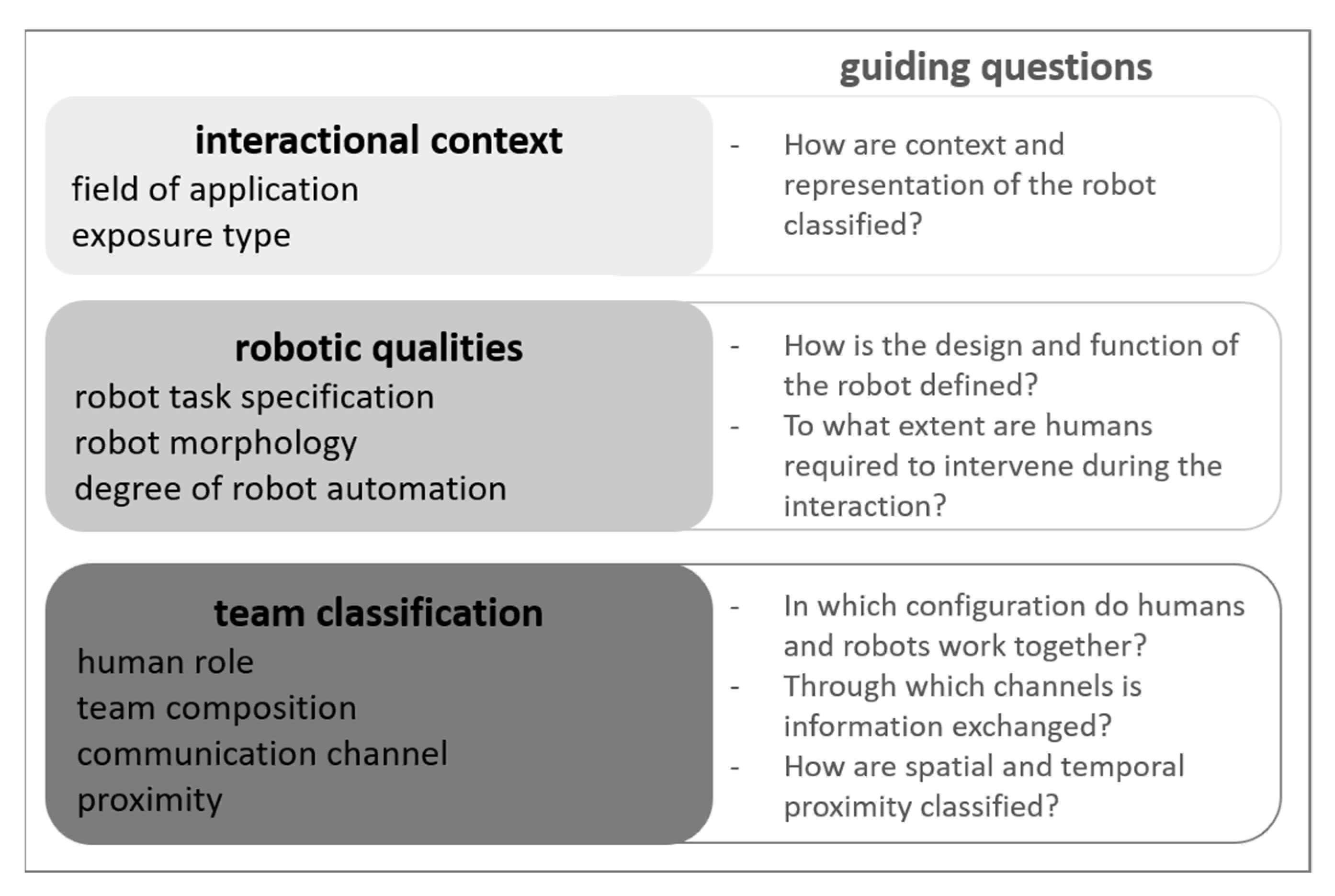
2.5.2. Sequence Analysis
3. Results
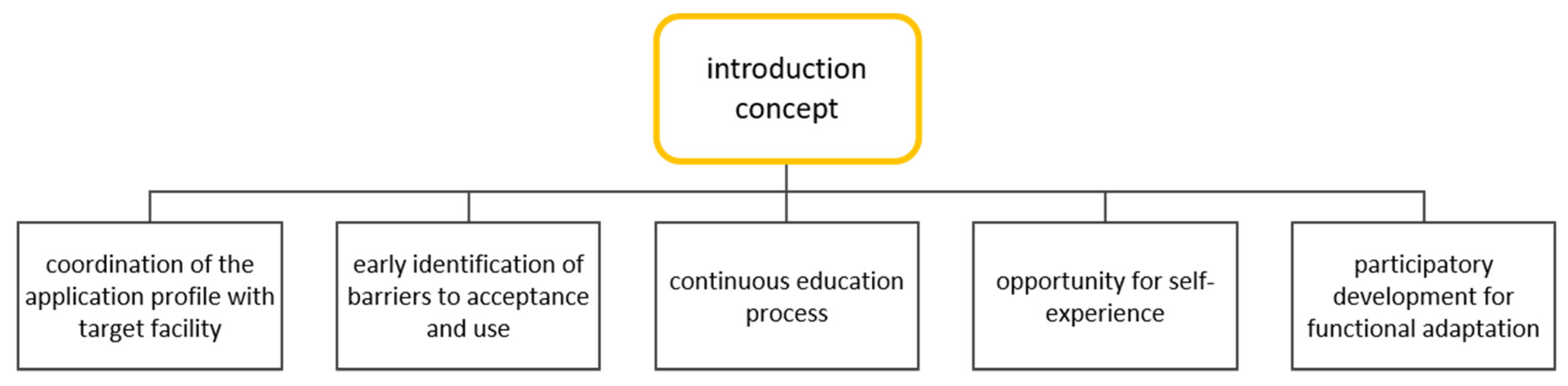
3.1. Prerequisites for Robotic Implementation and Use
3.2. Areas of Application and Ethical Considerations
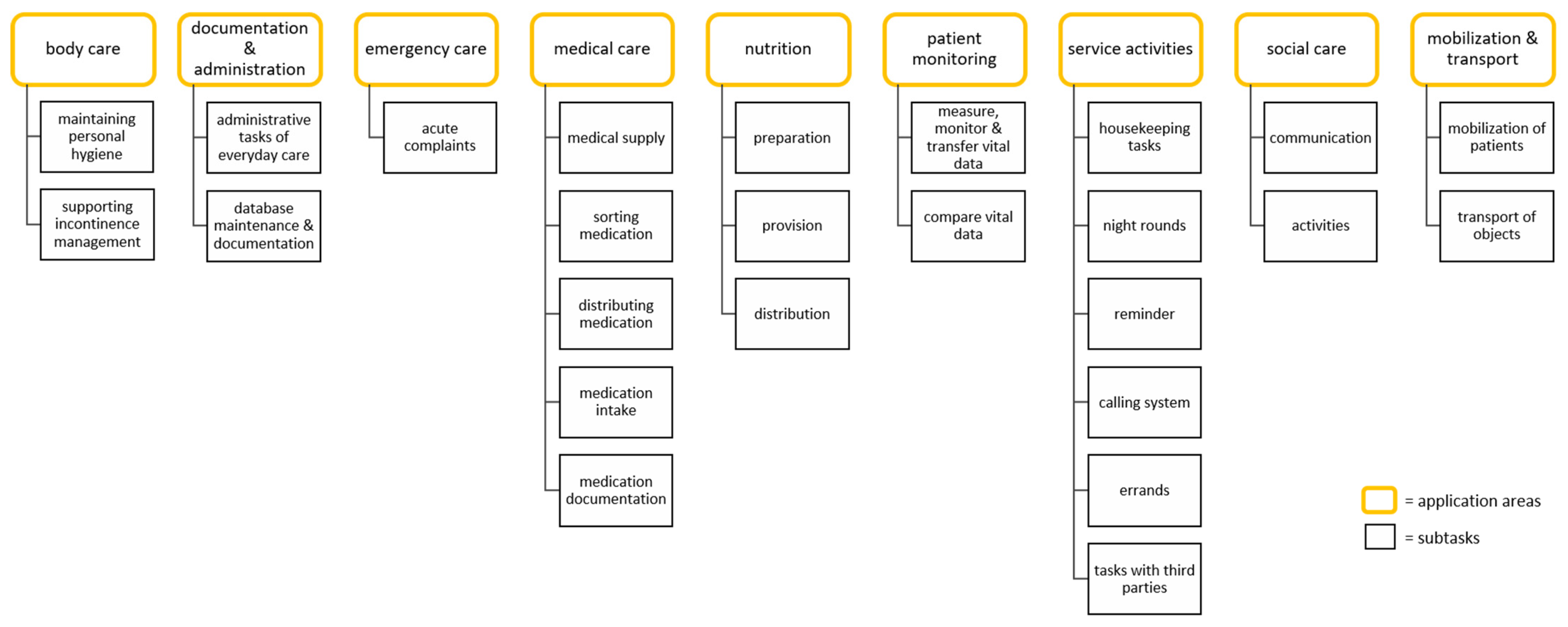
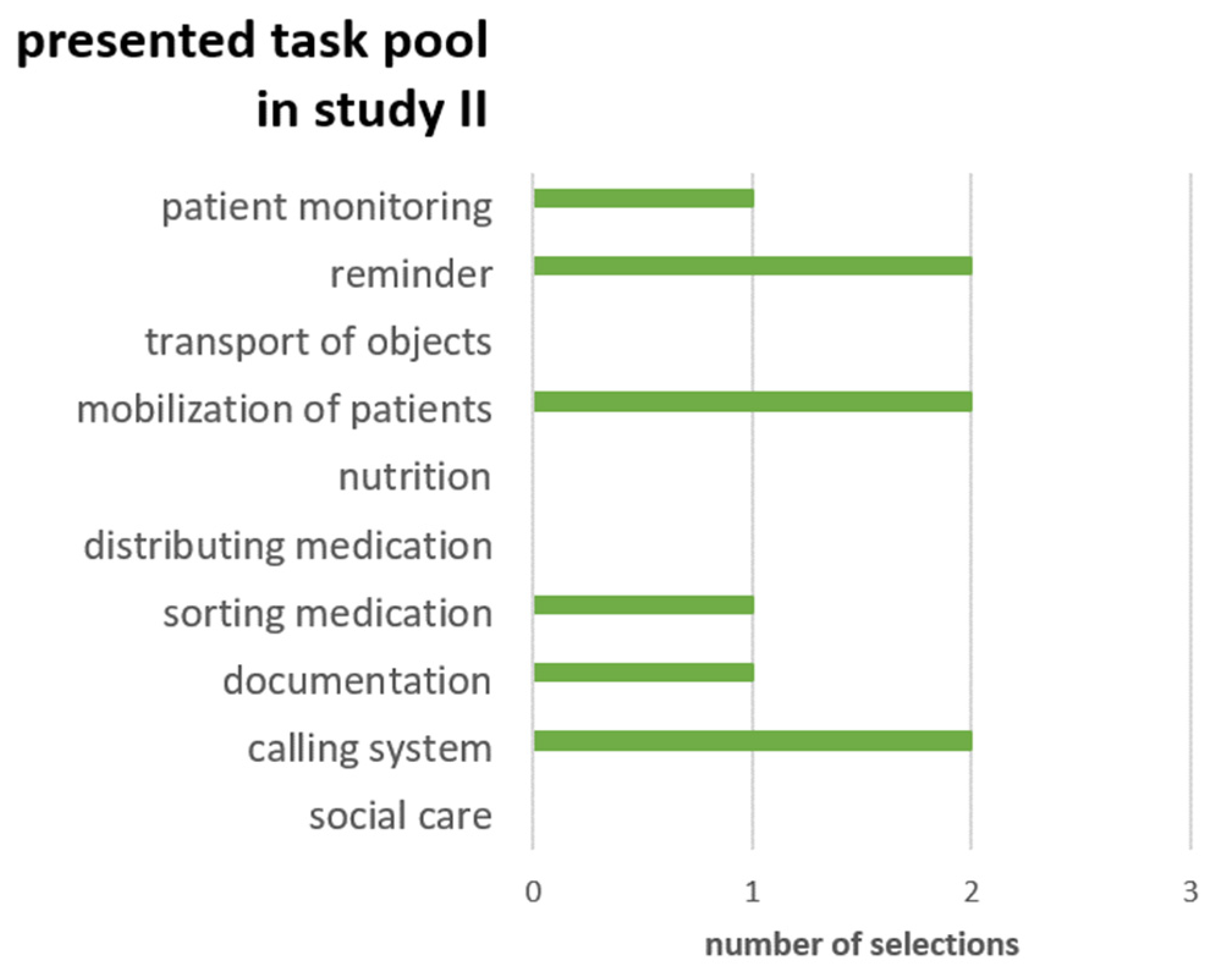
3.2.1. Potential Areas of Application and Collaboration Requirements
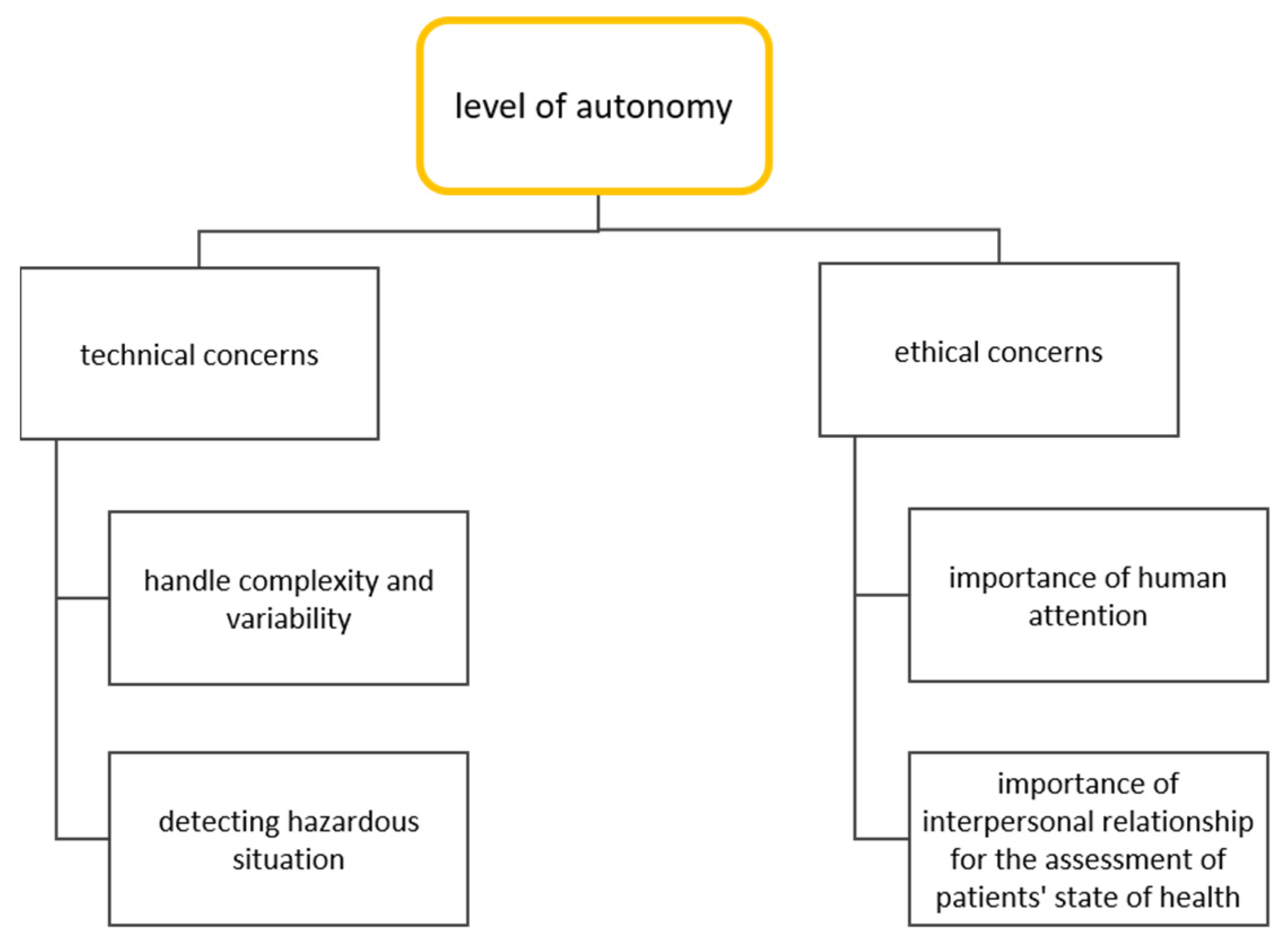
3.2.2. Ethical Considerations towards the Automation of Care Activities
3.3. Requirements for Human-Robot Interaction and Collaboration in Selected Scenarios
3.3.1. General Requirements for the Design of HRI
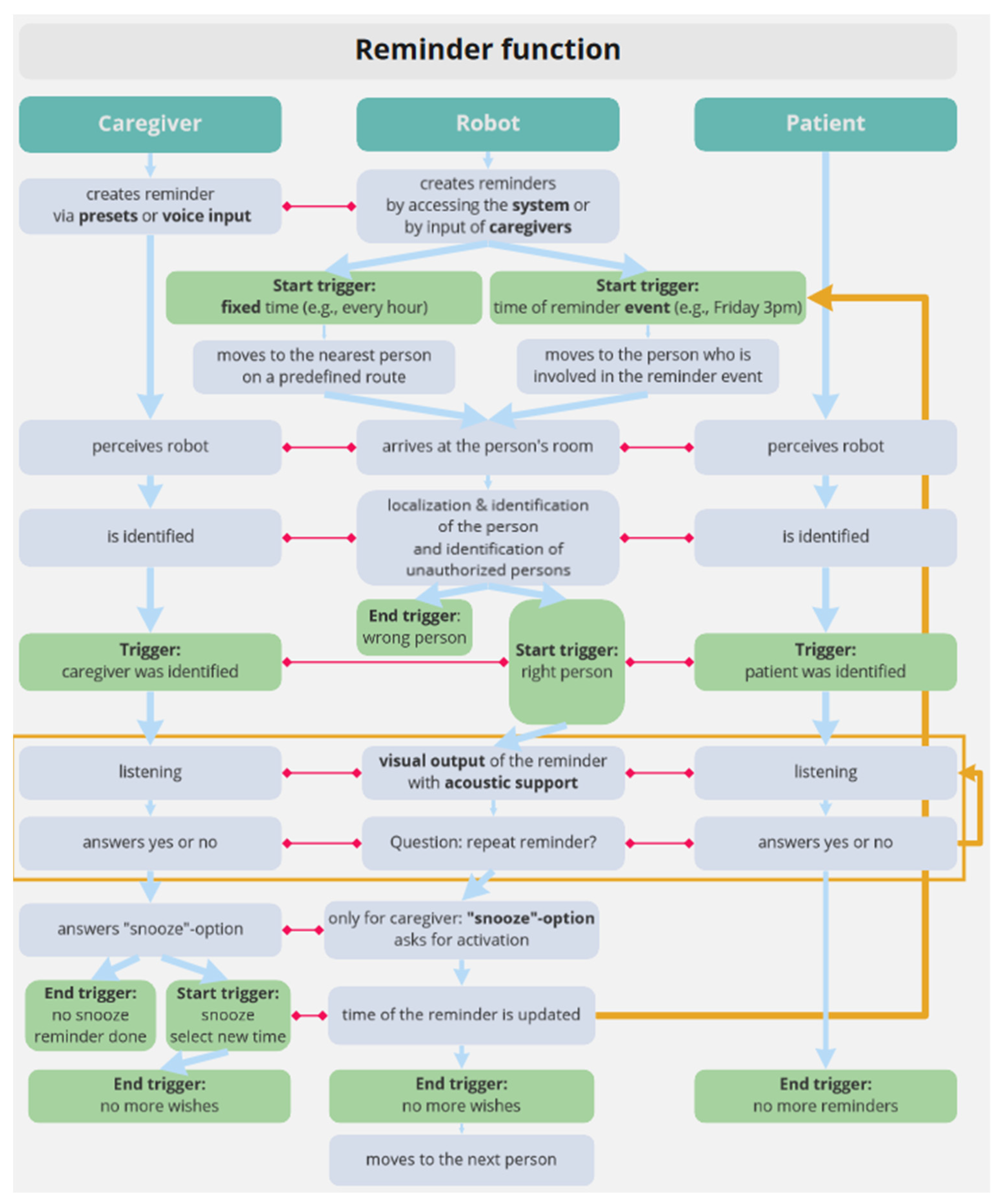
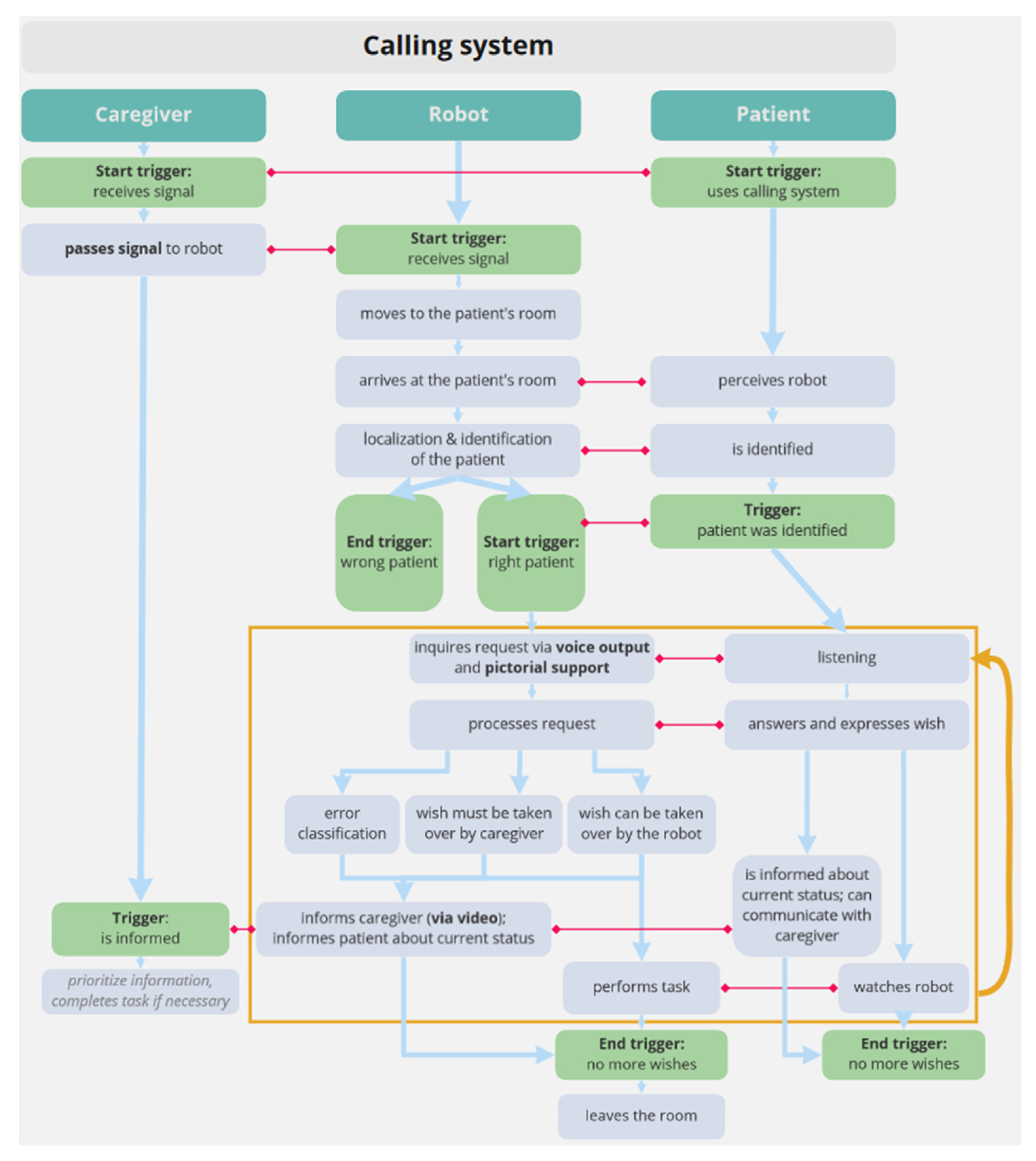
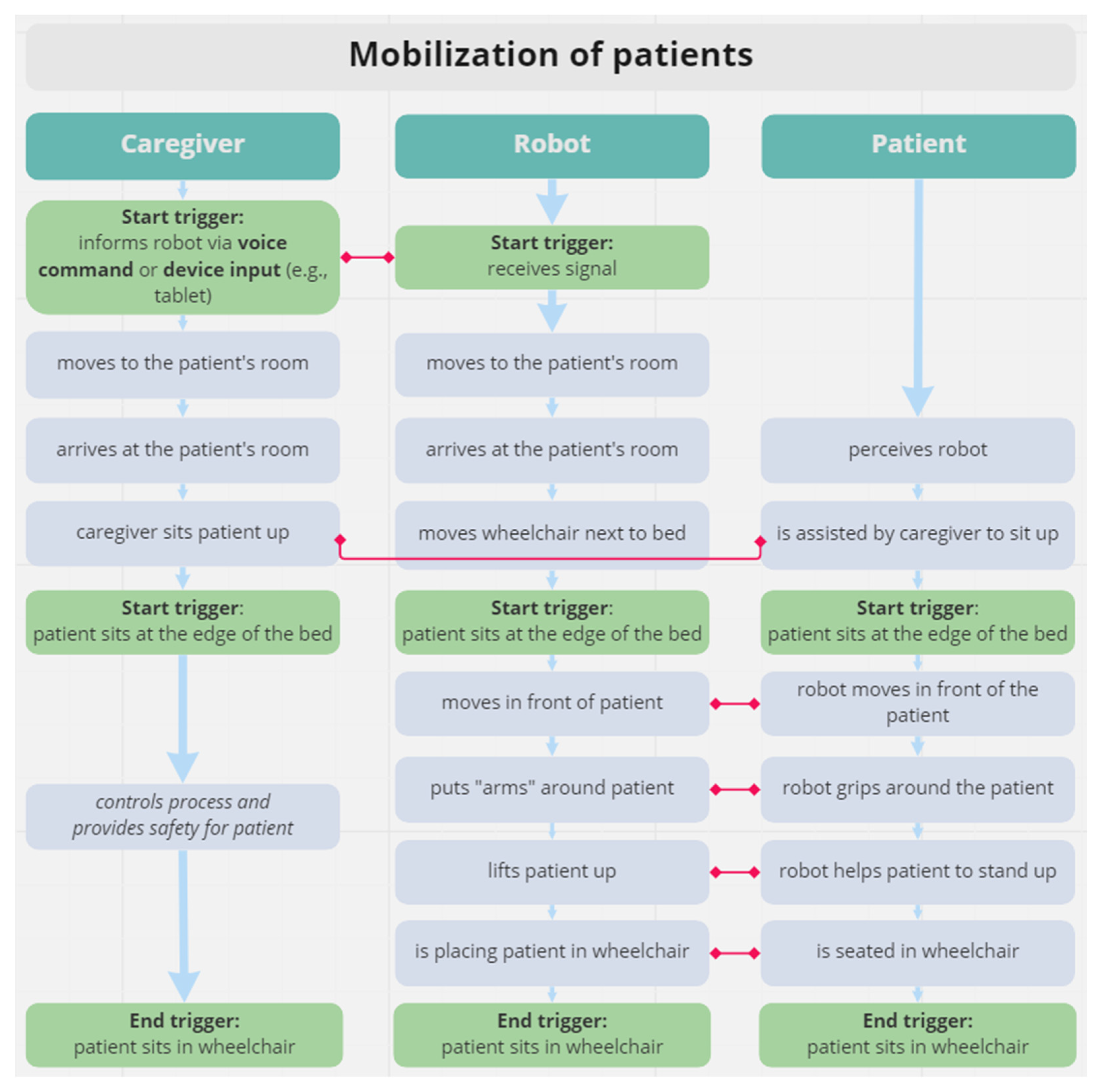
3.3.2. Requirements for Human Robot Collaboration in Selected Scenarios
4. Discussion
4.1. Co-Creation Process as Necessary Prerequisite
4.2. Key Factors for Potential Areas of Application and the Level of Automation
4.3. Key Factors for HRI and Design Guidelines from the Current Study
4.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organisation. State of the World’s Nursing 2020: Investing in Education, Jobs and Leadership; World Health Organization: Geneva, Switzerland, 2020.
- Buchan, J.; Catton, H.; Shaffer, F.A. Ageing Well? Policies to Support Older Nurses at Work. International Centre on Nurse Migration; International Centre on Nurse Migration: Philadelphia, PA, USA, 2020. [Google Scholar]
- Jacobs, K.; Kuhlmey, A.; Greß, S.; Klauber, J.; Schwinger, A. Pflege-Report 2019: Mehr Personal in der Langzeitpflege- aber woher? Springer: Berlin, Heidelberg, 2020; ISBN 978-3-662-58934-2. [Google Scholar]
- Hasselhorn, H.-M.; Müller, B.H.; Tackenberg, P.; Kümmerling, A.; Simone, M. Berufsausstieg bei Pflegepersonal: Arbeitsbedingungen und Beabsichtigter Berufsausstieg bei Pflegepersonal in Deutschland und Europa; Schriftenreihe der Bundesanstalt für Arbeitsschutz und Arbeitsmedizin Ü, Übersetzung; Wirtschaftsverl. NW, Verl. für Neue Wiss GmbH: Bremerhaven, Germany, 2005; ISBN 978-3-86509-247-2. [Google Scholar]
- Statistik der Bundesagentur für Arbeit. Berichte: Blickpunkt Arbeitsmarkt—Arbeitsmarktsituation im Pflegebereich; Blickpunkt Arbeitsmarkt: Nürnberg, Germany, 2021; p. 22. [Google Scholar]
- Institut DGB-Index Gute Arbeit. Arbeitsbedingungen in der Alten- und Krankenpflege—So beurteilen die Beschäftigten die Lage; Institut DGB-Index Gute Arbeit: Berlin, Germany, 2018; p. 24. [Google Scholar]
- Engelberger, J.F. Robotics in Service; Springer: Dordrecht, The Netherlands, 1989; ISBN 978-94-010-6985-4. [Google Scholar]
- Frazier, R.M.; Carter-Templeton, H.; Wyatt, T.H.; Wu, L. Current Trends in Robotics in Nursing Patents—A Glimpse Into Emerging Innovations. CIN Comput. Inform. Nurs. 2019, 37, 290–297. [Google Scholar] [CrossRef]
- Graf, B. Assistenzroboter für die Pflege. Z. Für Gerontol. Geriatr. 2020, 53, 608–614. [Google Scholar] [CrossRef]
- Kehl, C. Robotik und Assistive Neurotechnologien in der Pflege—Gesellschaftliche Herausforderungen; 177. TAB-Arbeitsbericht. Büro für Technikfolgen-Abschätzung beim Deutschen Bundestag (TAB): Berlin, Germany, 2018; p. 240. [Google Scholar]
- Robotik in Betreuung und Gesundheitsversorgung; Becker, H., Ed.; TA-SWISS; vdf Hochschulverl: Zürich, Switzerland, 2013; ISBN 978-3-7281-3520-9. [Google Scholar]
- Bardaro, G.; Antonini, A.; Motta, E. Robots for Elderly Care in the Home: A Landscape Analysis and Co-Design Toolkit. Int. J. Soc. Robot. 2021, 14, 657–681. [Google Scholar] [CrossRef]
- Bedaf, S.; Gelderblom, G.J.; de Witte, L. Overview and Categorization of Robots Supporting Independent Living of Elderly People: What Activities Do They Support and How Far Have They Developed. Assist. Technol. 2015, 27, 88–100. [Google Scholar] [CrossRef]
- Persson, M.; Redmalm, D.; Iversen, C. Caregivers’ Use of Robots and Their Effect on Work Environment—A Scoping Review. J. Technol. Hum. Serv. 2022, 40, 251–277. [Google Scholar] [CrossRef]
- Wright, J. Tactile Care, Mechanical Hugs: Japanese Caregivers and Robotic Lifting Devices. Asian Anthropol. 2018, 17, 24–39. [Google Scholar] [CrossRef]
- Papadopoulos, I.; Koulouglioti, C.; Ali, S. Views of Nurses and Other Health and Social Care Workers on the Use of Assistive Humanoid and Animal-like Robots in Health and Social Care: A Scoping Review. Contemp. Nurse 2018, 54, 425–442. [Google Scholar] [CrossRef]
- Beedholm, K.; Frederiksen, K.; Lomborg, K. What Was (Also) at Stake When a Robot Bathtub Was Implemented in a Danish Elder Center: A Constructivist Secondary Qualitative Analysis. Qual. Health Res. 2016, 26, 1424–1433. [Google Scholar] [CrossRef]
- Mossfeldt Nickelsen, N.C. Imagining and Tinkering with Assistive Robotics in Care for the Disabled. Paladyn J. Behav. Robot. 2019, 10, 128–139. [Google Scholar] [CrossRef]
- Johansson-Pajala, R.-M.; Thommes, K.; Hoppe, J.A.; Tuisku, O.; Hennala, L.; Pekkarinen, S.; Melkas, H.; Gustafsson, C. Care Robot Orientation: What, Who and How? Potential Users’ Percept. Int. J. Soc. Robot. 2020, 12, 1103–1117. [Google Scholar] [CrossRef]
- Moyle, W.; Bramble, M.; Jones, C.; Murfield, J. Care Staff Perceptions of a Social Robot Called Paro and a Look-Alike Plush Toy: A Descriptive Qualitative Approach. Aging Ment. Health 2018, 22, 330–335. [Google Scholar] [CrossRef]
- Nilsen, E.R.; Dugstad, J.; Eide, H.; Gullslett, M.K.; Eide, T. Exploring Resistance to Implementation of Welfare Technology in Municipal Healthcare Services—A Longitudinal Case Study. BMC Health Serv. Res. 2016, 16, 657. [Google Scholar] [CrossRef]
- Parviainen, J.; Turja, T.; Van Aerschot, L. Robots and Human Touch in Care: Desirable and Non-Desirable Robot Assistance. In Social Robotics; Ge, S.S., Cabibihan, J.-J., Salichs, M.A., Broadbent, E., He, H., Wagner, A.R., Castro-González, Á., Eds.; Lecture Notes in Computer Science; Springer International Publishing: Cham, Switzerland, 2018; Volume 11357, pp. 533–540. ISBN 978-3-030-05203-4. [Google Scholar]
- Beane, M.; Orlikowski, W.J. What Difference Does a Robot Make? The Material Enactment of Distributed Coordination. Organ. Sci. 2015, 26, 1553–1573. [Google Scholar] [CrossRef]
- Chen, S.-C.; Jones, C.; Moyle, W. Health Professional and Workers Attitudes towards the Use of Social Robots for Older Adults in Long-Term Care. Int. J. Soc. Robot. 2020, 12, 1135–1147. [Google Scholar] [CrossRef]
- Rantanen, T.; Lehto, P.; Vuorinen, P.; Coco, K. Attitudes towards Care Robots among Finnish Home Care Personnel—A Comparison of Two Approaches. Scand. J. Caring Sci. 2018, 32, 772–782. [Google Scholar] [CrossRef]
- Flandorfer, P. Population Ageing and Socially Assistive Robots for Elderly Persons: The Importance of Sociodemographic Factors for User Acceptance. Int. J. Popul. Res. 2012, 2012, 829835. [Google Scholar] [CrossRef]
- Turja, T.; Van Aerschot, L.; Särkikoski, T.; Oksanen, A. Finnish Healthcare Professionals’ Attitudes towards Robots: Reflections on a Population Sample. Nurs. Open 2018, 5, 300–309. [Google Scholar] [CrossRef]
- van Wynsberghe, A. Designing Robots for Care: Care Centered Value-Sensitive Design. Sci. Eng. Ethics 2013, 19, 407–433. [Google Scholar] [CrossRef]
- Gläser, J.; Laudel, G. Experteninterviews und Qualitative Inhaltsanalyse als Instrumente Rekonstruierender Untersuchungen, 4th ed.; Lehrbuch; VS Verl. für Sozialwiss: Wiesbaden, Germany, 2010; ISBN 978-3-531-17238-5. [Google Scholar]
- Mayring, P. Qualitative Inhaltsanalyse: Grundlagen und Techniken, 12th ed.; Beltz Verlag: Basel, Switzerland, 2015; ISBN 978-3-407-25730-7. [Google Scholar]
- Beyer, H.; Holtzblatt, K. Contextual Design: Defining Customer-Centered Systems; Morgan Kaufmann: San Francisco, CA, USA, 1997; ISBN 978-1-55860-411-7. [Google Scholar]
- Melkas, H.; Hennala, L.; Pekkarinen, S.; Kyrki, V. Impacts of Robot Implementation on Care Personnel and Clients in Elderly-Care Institutions. Int. J. Med. Inf. 2020, 134, 104041. [Google Scholar] [CrossRef]
- Sharts-Hopko, N.C. The Coming Revolution in Personal Care Robotics: What Does It Mean for Nurses? Nurs. Adm. Q. 2014, 38, 5–12. [Google Scholar] [CrossRef]
- Coco, K.; Kangasniemi, M.; Rantanen, T. Care Personnel’s Attitudes and Fears toward Care Robots in Elderly Care: A Comparison of Data from the Care Personnel in Finland and Japan. J. Nurs. Scholarsh. 2018, 50, 634–644. [Google Scholar] [CrossRef] [PubMed]
- Kristoffersson, A.; Coradeschi, S.; Loutfi, A.; Severinson-Eklundh, K. An Exploratory Study of Health Professionals’ Attitudes about Robotic Telepresence Technology. J. Technol. Hum. Serv. 2011, 29, 263–283. [Google Scholar] [CrossRef]
- Pigini, L.; Facal, D.; Blasi, L.; Andrich, R. Service Robots in Elderly Care at Home: Users’ Needs and Perceptions as a Basis for Concept Development. Technol. Disabil. 2012, 24, 303–311. [Google Scholar] [CrossRef]
- Fiorini, L.; De Mul, M.; Fabbricotti, I.; Limosani, R.; Vitanza, A.; D’Onofrio, G.; Tsui, M.; Sancarlo, D.; Giuliani, F.; Greco, A.; et al. Assistive Robots to Improve the Independent Living of Older Persons: Results from a Needs Study. Disabil. Rehabil. Assist. Technol. 2021, 16, 92–102. [Google Scholar] [CrossRef] [PubMed]
- Olatunji, S.; Potenza, A.; Kiselev, A.; Oron-Gilad, T.; Loutfi, A.; Edan, Y. Levels of Automation for a Mobile Robot Teleoperated by a Caregiver. ACM Trans. Hum. -Robot. Interact. 2021, 11, 1–21. [Google Scholar] [CrossRef]
- Christoforou, E.G.; Avgousti, S.; Ramdani, N.; Novales, C.; Panayides, A.S. The Upcoming Role for Nursing and Assistive Robotics: Opportunities and Challenges Ahead. Front. Digit. Health 2020, 2, 585656. [Google Scholar] [CrossRef]
- Chatterji, N.; Allen, C.; Chernova, S. Effectiveness of Robot Communication Level on Likeability, Understandability and Comfortability. In Proceedings of the 2019 28th IEEE International Conference on Robot and Human Interactive Communication (RO-MAN), New Delhi, India, 14–18 October 2019; pp. 1–7. [Google Scholar]
- Klüber, K.; Onnasch, L. Appearance Is Not Everything—Preferred Feature Combinations for Care Robots. Comput. Hum. Behav. 2022, 128, 107128. [Google Scholar] [CrossRef]
- Eyssel, F.; Kuchenbrandt, D.; Bobinger, S.; de Ruiter, L.; Hegel, F. “If You Sound like Me, You Must Be More Human”: On the Interplay of Robot and User Features on Human-Robot Acceptance and Anthropomorphism. In Proceedings of the Seventh Annual ACM/IEEE International Conference on Human-Robot Interaction—HRI ’12, Boston, MA, USA, 5–8 March 2012; p. 125. [Google Scholar]
- Tamagawa, R.; Watson, C.I.; Kuo, I.H.; MacDonald, B.A.; Broadbent, E. The Effects of Synthesized Voice Accents on User Perceptions of Robots. Int. J. Soc. Robot. 2011, 3, 253–262. [Google Scholar] [CrossRef]
- Onnasch, L.; Roesler, E. A Taxonomy to Structure and Analyze Human–Robot Interaction. Int. J. Soc. Robot. 2021, 13, 833–849. [Google Scholar] [CrossRef]
- Pineau, J.; Montemerlo, M.; Pollack, M.; Roy, N.; Thrun, S. towards Robotic Assistants in Nursing Homes: Challenges and Results. Robot. Auton. Syst. 2003, 42, 271–281. [Google Scholar] [CrossRef]
- Leite, I.; Martinho, C.; Paiva, A. Social Robots for Long-Term Interaction: A Survey. Int. J. Soc. Robot. 2013, 5, 291–308. [Google Scholar] [CrossRef]
- Winkle, K.; Caleb-Solly, P.; Turton, A.; Bremner, P. Social Robots for Engagement in Rehabilitative Therapies: Design Implications from a Study with Therapists. In Proceedings of the 2018 ACM/IEEE International Conference on Human-Robot Interaction, Chicago, IL, USA, 26 February 2018; pp. 289–297. [Google Scholar]
- Epley, N.; Waytz, A.; Cacioppo, J.T. On Seeing Human: A Three-Factor Theory of Anthropomorphism. Psychol. Rev. 2007, 114, 864–886. [Google Scholar] [CrossRef] [PubMed]
- Zhang, T.; Zhu, B.; David, B. Kaber Anthropomorphism in Robots and Human Etiquette Expectations for Interaction. In Human–Computer Etiquette. Cultural Expectations and the Design Implications They Place on Computers and Technology; Hayes, C.C., Miller, C.A., Eds.; Taylor & Francis: London, UK, 2010; pp. 231–259. ISBN 978-0-429-24946-4. [Google Scholar]
- Rosenthal-von der Pütten, A.M.; Krämer, N.C. How Design Characteristics of Robots Determine Evaluation and Uncanny Valley Related Responses. Comput. Hum. Behav. 2014, 36, 422–439. [Google Scholar] [CrossRef]
- Kontogiorgos, D.; Pereira, A.; Andersson, O.; Koivisto, M.; Gonzalez Rabal, E.; Vartiainen, V.; Gustafson, J. The Effects of Anthropomorphism and Non-Verbal Social Behaviour in Virtual Assistants. In Proceedings of the 19th ACM International Conference on Intelligent Virtual Agents, Paris, France, 2–5 July 2019; pp. 133–140. [Google Scholar]
- Fong, T.; Nourbakhsh, I.; Dautenhahn, K. A Survey of Socially Interactive Robots. Robot. Auton. Syst. 2003, 42, 143–166. [Google Scholar] [CrossRef]
- Nass, C.; Moon, Y. Machines and Mindlessness: Social Responses to Computers. J. Soc. Issues 2000, 56, 81–103. [Google Scholar] [CrossRef]
- Duffy, B.R. Anthropomorphism and the Social Robot. Robot. Auton. Syst. 2003, 42, 177–190. [Google Scholar] [CrossRef]
- Mori, M.; MacDorman, K.; Kageki, N. The Uncanny Valley [From the Field]. IEEE Robot. Autom. Mag. 2012, 19, 98–100. [Google Scholar] [CrossRef]
- Rossi, S.; Ferland, F.; Tapus, A. User Profiling and Behavioral Adaptation for HRI: A Survey. Pattern Recognit. Lett. 2017, 99, 3–12. [Google Scholar] [CrossRef]
- Nof, S.Y. Automation: What It Means to Us around the World. In Springer Handbook of Automation; Nof, S.Y., Ed.; Springer: Berlin/Heidelberg, Germany, 2009; pp. 13–52. ISBN 978-3-540-78830-0. [Google Scholar]
- Calo, C.; Hunt-Bull, N.; Lewis, L.; Metzler, T. Ethical Implications of Using the Paro Robot, with a Focus on Dementia Patient Care. In Proceedings of the Human-Robot Interaction in Elder Care; Papers from the 2011 AAAI Workshop; AAAI: San Francisco, CA, USA, 2011; pp. 20–24. [Google Scholar]
- Darling, K. Extending Legal Protection to Social Robots: The Effects of Anthropomorphism, Empathy, and Violent Behavior towards Robotic Objects. SSRN Electron. J. 2012. [Google Scholar] [CrossRef]
- Friedman, B.; Kahn, P.H.; Hagman, J. Hardware Companions?: What Online AIBO Discussion Forums Reveal about the Human-Robotic Relationship. In Proceedings of the conference on Human factors in computing systems—CHI ’03, Ft. Lauderdale, FL, USA, 5–10 April 2003; p. 273. [Google Scholar]

| Study | Nursing Home | Robotic Experience | |
|---|---|---|---|
| Without | With | ||
| I | A | 7 | - |
| B | - | 2 | |
| C | - | 2 | |
| D | - | 3 | |
| E | - | 1 | |
| F | 1 | - | |
| D | - | 1 | |
| II | G | 1 | - |
| H | 1 | - | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Klebbe, R.; Klüber, K.; Dahms, R.; Onnasch, L. Caregivers’ Perspectives on Human–Robot Collaboration in Inpatient Elderly Care Settings. Machines 2023, 11, 34. https://doi.org/10.3390/machines11010034
Klebbe R, Klüber K, Dahms R, Onnasch L. Caregivers’ Perspectives on Human–Robot Collaboration in Inpatient Elderly Care Settings. Machines. 2023; 11(1):34. https://doi.org/10.3390/machines11010034
Chicago/Turabian StyleKlebbe, Robert, Kim Klüber, Rebecca Dahms, and Linda Onnasch. 2023. "Caregivers’ Perspectives on Human–Robot Collaboration in Inpatient Elderly Care Settings" Machines 11, no. 1: 34. https://doi.org/10.3390/machines11010034
APA StyleKlebbe, R., Klüber, K., Dahms, R., & Onnasch, L. (2023). Caregivers’ Perspectives on Human–Robot Collaboration in Inpatient Elderly Care Settings. Machines, 11(1), 34. https://doi.org/10.3390/machines11010034







