An Advanced Risk Modeling Method to Estimate Legionellosis Risks Within a Diverse Population
Abstract
1. Introduction
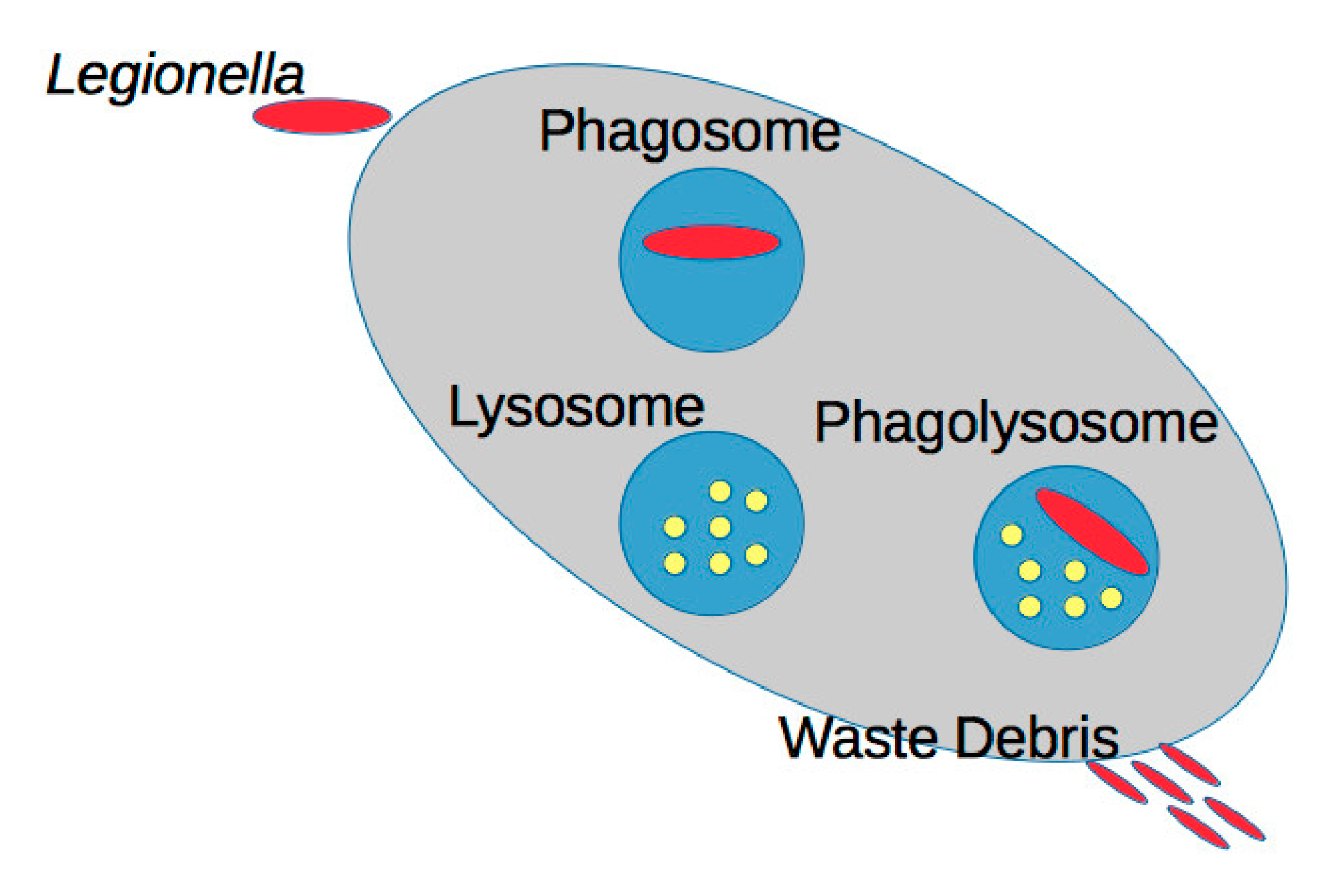
1.1. Fundamental Background of L. pneumophila and Disease Endpoints
1.2. The Evolution of L. pneumophila Causes Water Systems Control Challenges and Drives Pathogenesis
1.3. Health Effects Within Diverse Populations Are Not Equal
1.4. QMRA Can Optimize L. pneumophila Interventions
1.5. Current QMRA Modeling Methods Are Inadequate for L. pneumophila
- The host is exposed to an average dose in the environment (d), modeled as a random discrete Poisson dose (red in Equation (1)).
- From this d, there are j pathogens that are delivered to a susceptible location within the host, for example, alveoli for L. pneumophila.
- From those j organisms, k survive to initiate an infection, which is a Boolean outcome and, thus, the binomial distribution (blue in Equation (1)). These likelihoods are coupled to develop the joint probability that d will result in an infection, which is then simplified to the exponential dose-response function at the far right (green in Equation (1)).
1.6. Scope and Purpose of Research
2. Modeling Methods
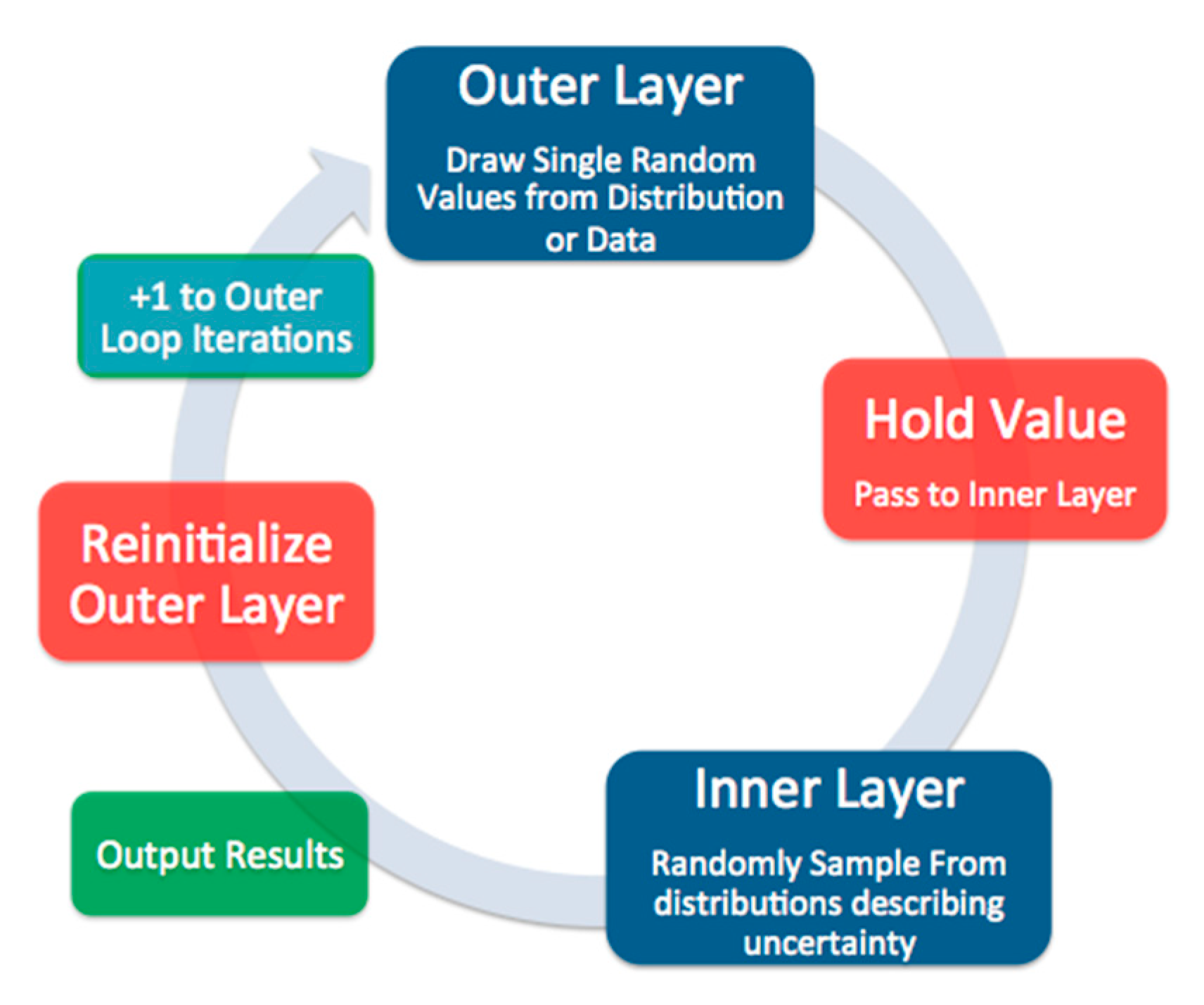
2.1. Two-Dimensional Simulation for Risk Modeling
2.2. Exposure Model and Probability of Infection
- Concentration of L. pneumophila in the premise plumbing water;
- Concentration of L. pneumophila in the air during showering, within a shower duration;
- Generation of aerosols sized ≤5 µm;
- Delivered dose to alveoli of human lungs, accounting for intermediate losses in the previous two regions of the respiratory system.
2.3. Risk Characterization: Probability of Illness and DALYs
2.4. Method to Estimate Morbidity Ratio Proxies and Dynamic Health Effect QMRA Models
3. Results
3.1. Effects of Flow Rate
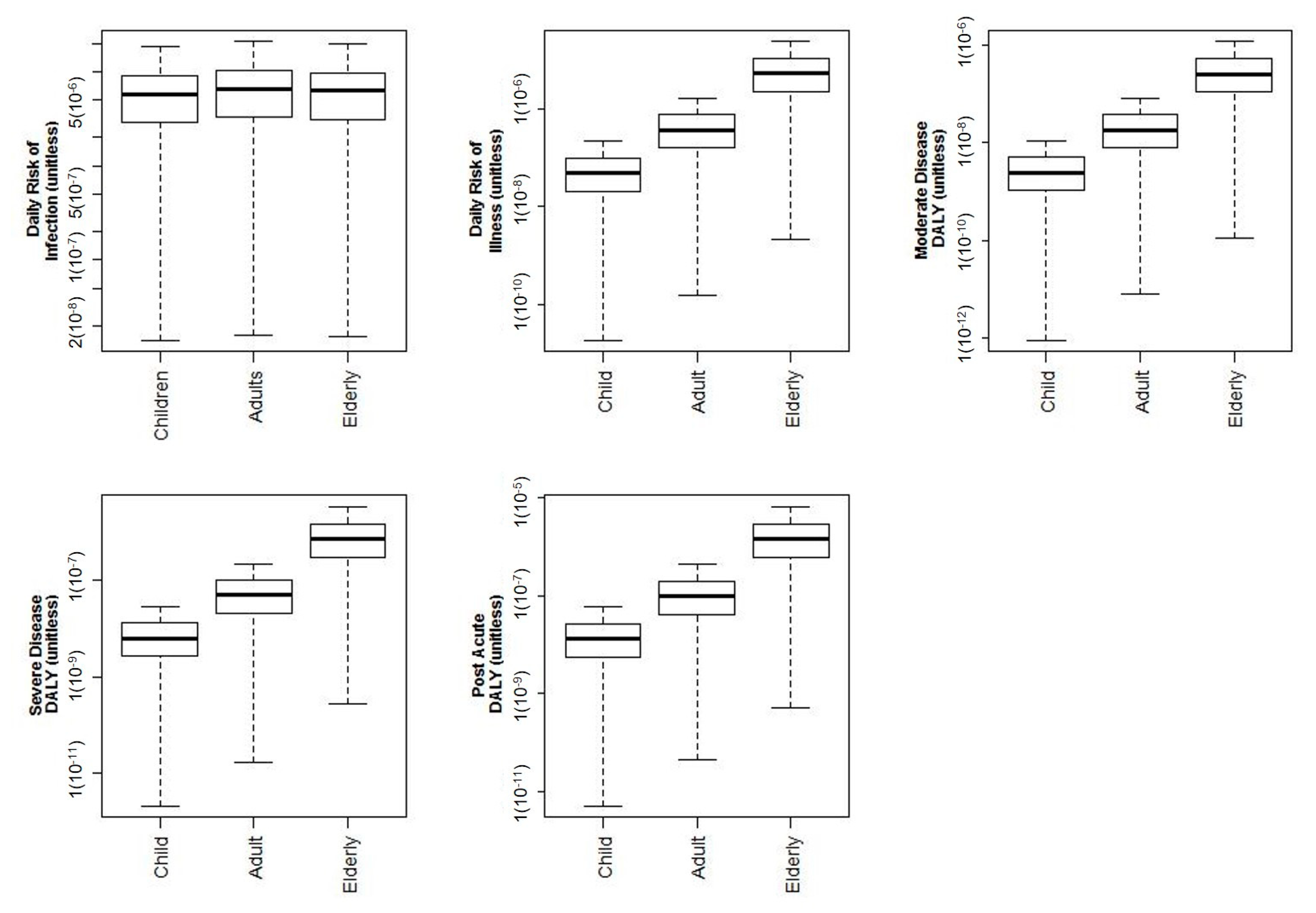
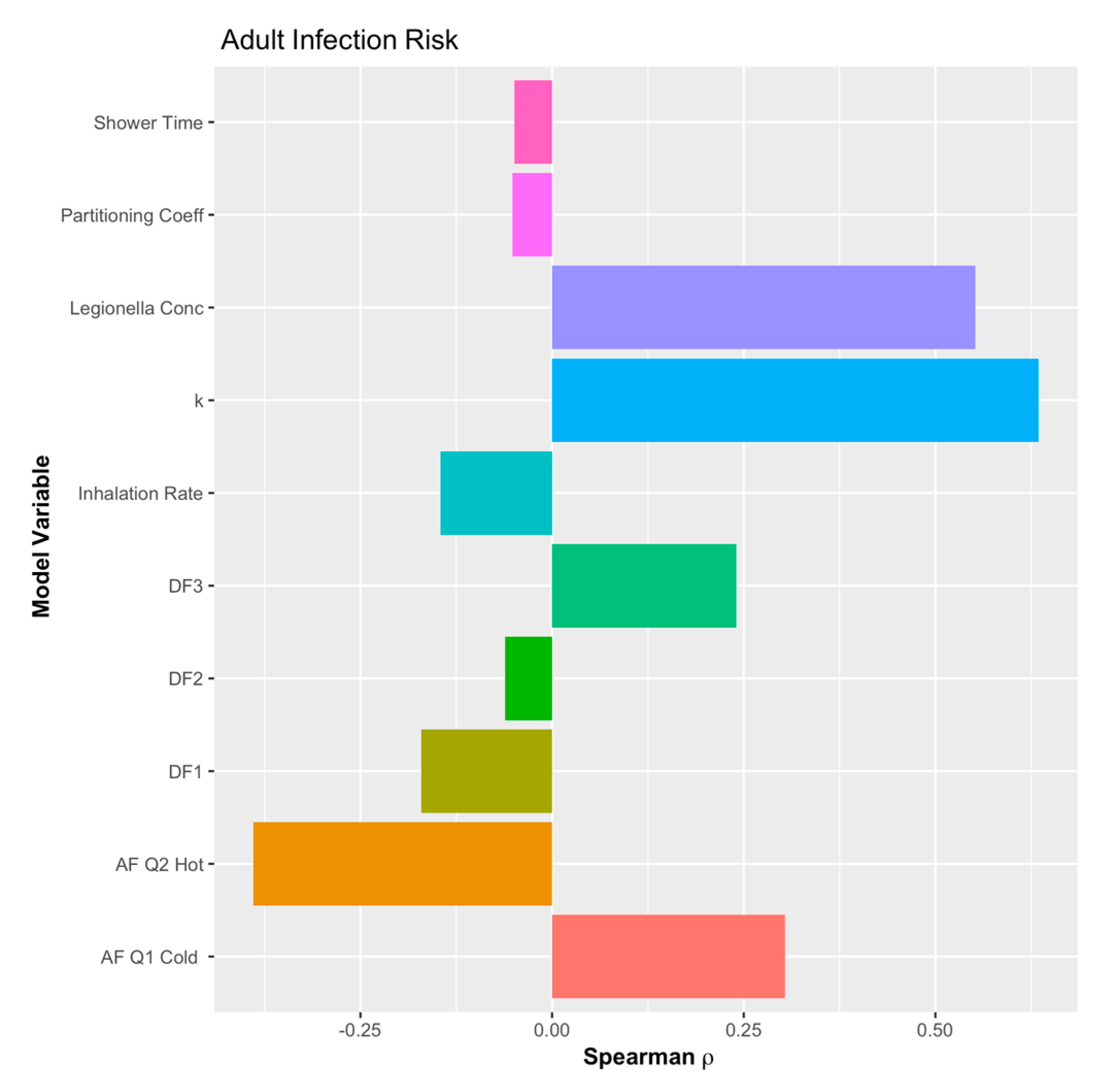
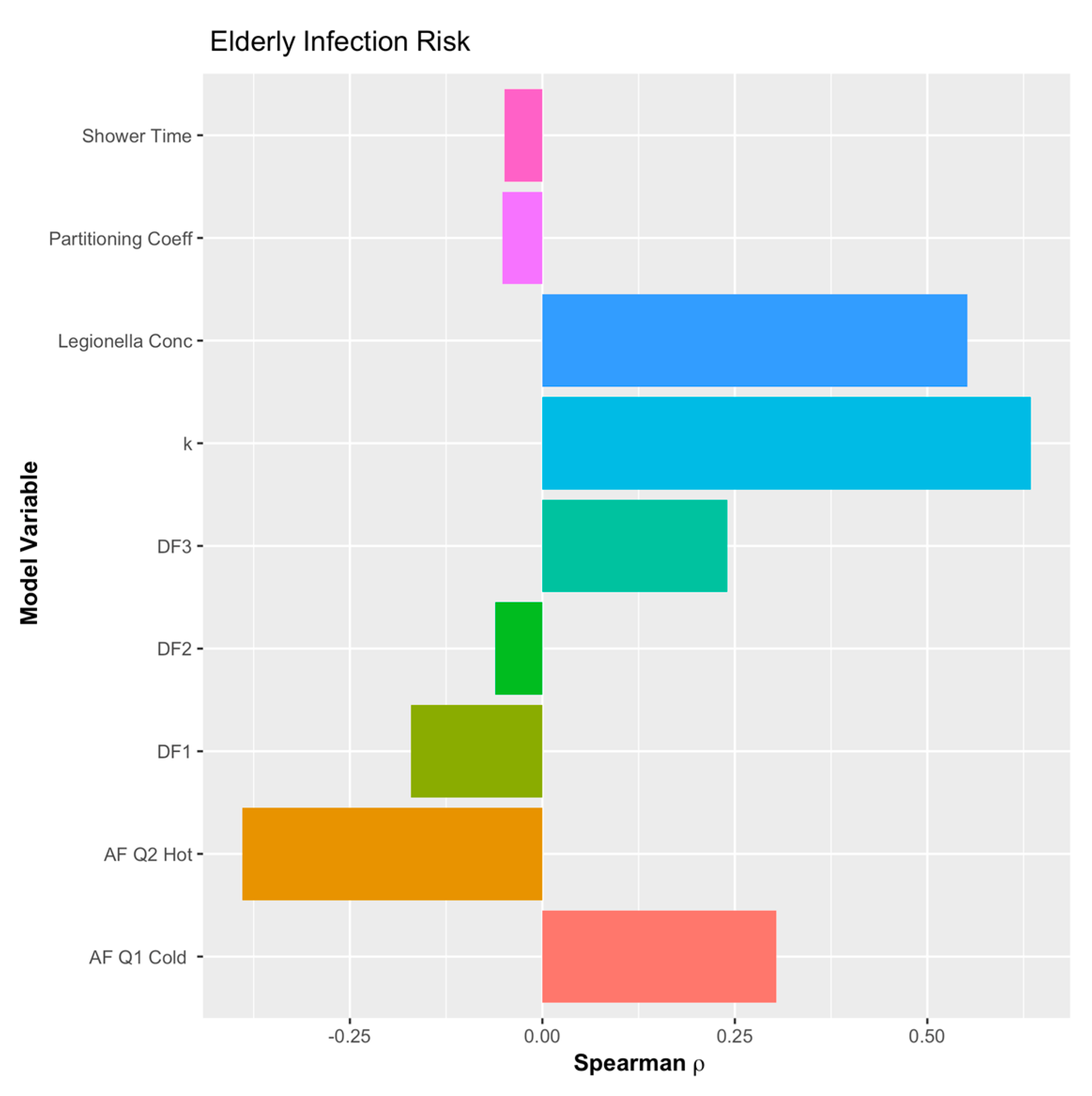
3.2. Age Demographic Risks
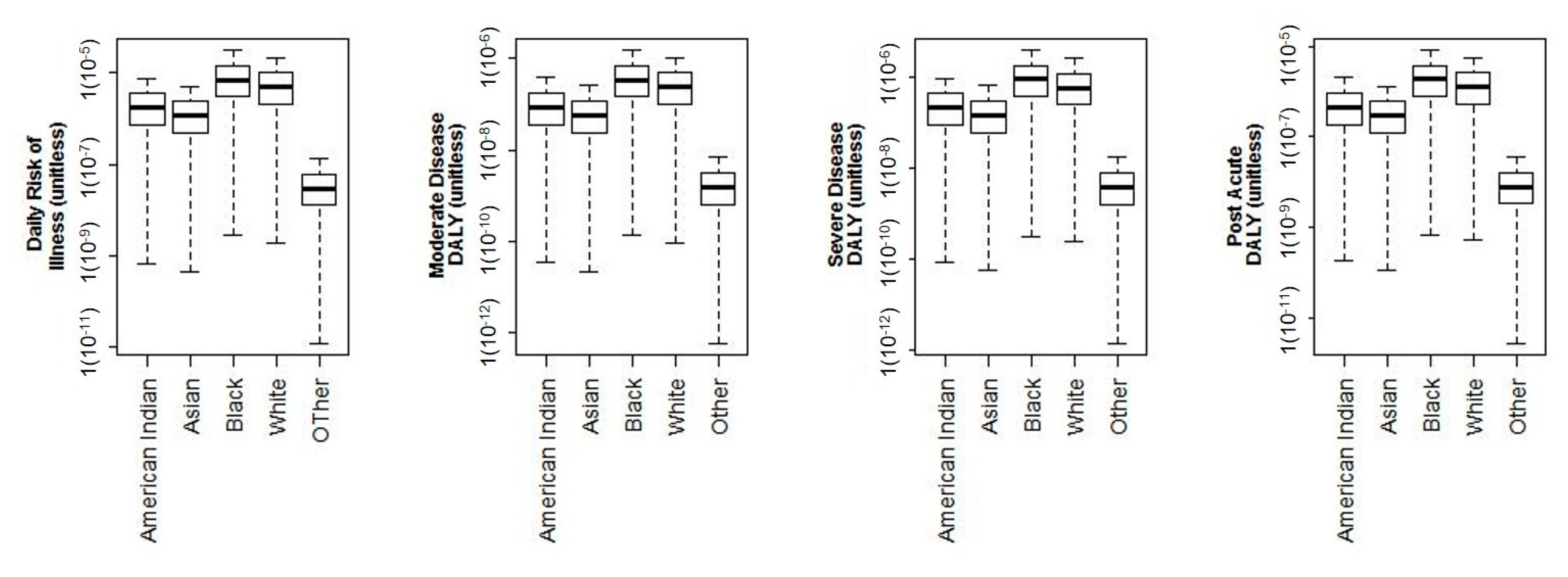
3.3. Race Demographic Risks
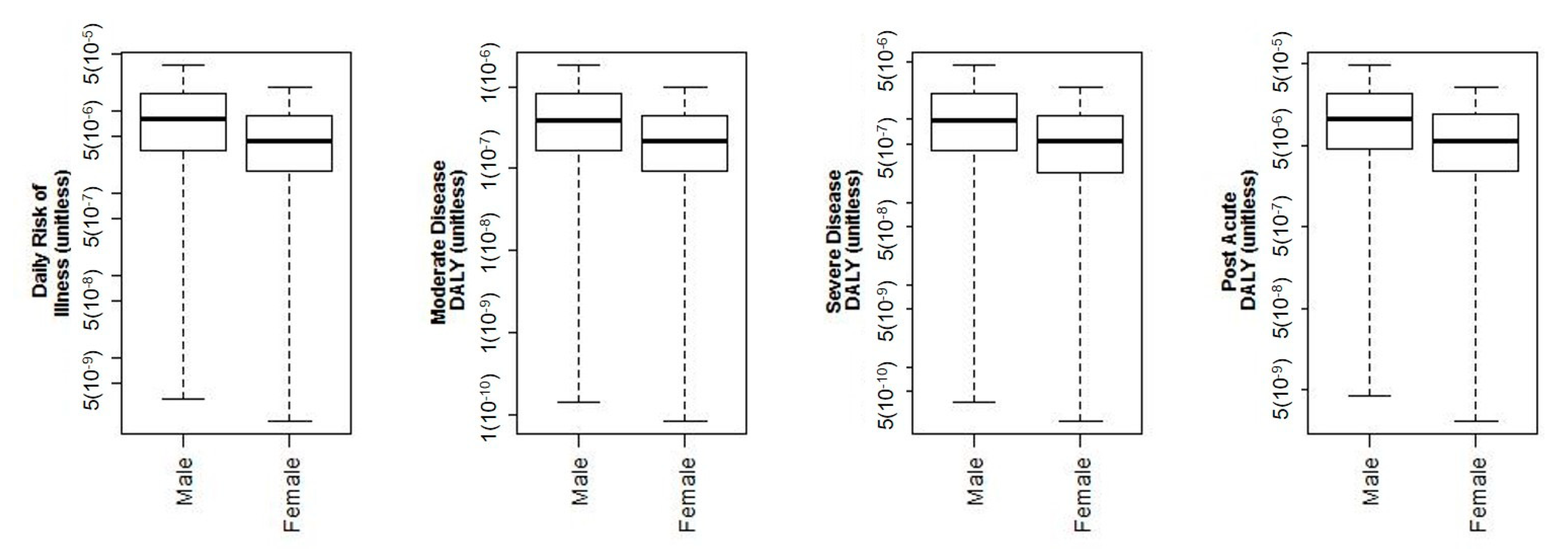
3.4. Sex Demographic Risks
4. Discussion
4.1. Interpretation of Results
4.2. Model Limitations
4.3. Other Potential Methods for Future Research
4.4. Broader Impacts of This Research
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Stout, J.E.; Rihs, J.D.; Yu, V.L. Legionella; Cianciotto, N.P., Hacker, J., Lück, P.C., Fields, B.S., Marre, R., Frosch, M., Abu Kwaik, Y., Bartlett, C., Eds.; American Society of Microbiology: Washington, DC, USA, 2002; ISBN 978-1-55581-230-0. [Google Scholar]
- CDC. Legionella (Legionnaires’ Disease and Pontiac Fever)—History, Burden and Trends. Available online: https://www.cdc.gov/legionella/about/history.html (accessed on 10 March 2019).
- Stout, J.E.; Yu, V.L.; Muraca, P.; Joly, J.; Troup, N.; Tompkins, L.S. Potable Water as a Cause of Sporadic Cases of Community-Acquired Legionnaires’ Disease. N. Engl. J. Med. 1992, 326, 151–155. [Google Scholar] [CrossRef] [PubMed]
- Mandel, A.S.; Sprauer, M.A.; Sniadack, D.H.; Ostroff, S.M. State Regulation of Hospital Water Temperature. Infect. Control Hosp. Epidemiol. 1993, 14, 642–645. [Google Scholar] [CrossRef] [PubMed]
- Yaslianifard, S.; Mobarez, A.M.; Fatolahzadeh, B.; Feizabadi, M.M. Colonization of hospital water systems by Legionella pneumophila, Pseudomonas aeroginosa, and Acinetobacter in ICU wards of Tehran hospitals. Indian J. Pathol. Microbiol. 2012, 55, 352–356. [Google Scholar] [PubMed]
- Tobin, J.O.; Beare, J.; Dunnill, M.S.; Fisher-Hoch, S.; French, M.; Mitchell, R.G.; Morris, P.J.; Muers, M.F. Legionnaires’ disease in a transplant unit: Isolation of the causative agent from shower baths. Lancet 1980, 2, 118–121. [Google Scholar] [CrossRef]
- Falkinham, J.O.; Pruden, A.; Edwards, M. Opportunistic Premise Plumbing Pathogens: Increasingly Important Pathogens in Drinking Water. Pathogens 2015, 4, 373–386. [Google Scholar] [CrossRef]
- Falkinham, J.O.; Hilborn, E.D.; Arduino, M.J.; Pruden, A.; Edwards, M.A. Epidemiology and Ecology of Opportunistic Premise Plumbing Pathogens: Legionella pneumophila, Mycobacterium avium, and Pseudomonas aeruginosa. Environ. Health Perspect. Online Res. Triangle Park 2015, 123, 749. [Google Scholar] [CrossRef]
- Lechevallier, M.W.; Cawthon, C.D.; Lee, R.G. Factors promoting survival of bacteria in chlorinated water supplies. Appl. Environ. Microbiol. 1988, 54, 649–654. [Google Scholar]
- Berry, D.; Xi, C.; Raskin, L. Microbial ecology of drinking water distribution systems. Curr. Opin. Biotechnol. 2006, 17, 297–302. [Google Scholar] [CrossRef]
- Pinto, A.J.; Schroeder, J.; Lunn, M.; Sloan, W.; Raskin, L. Spatial-temporal survey and occupancy-abundance modeling to predict bacterial community dynamics in the drinking water microbiome. MBio 2014, 5, e01135-14. [Google Scholar] [CrossRef]
- Shen, Y.; Monroy, G.L.; Derlon, N.; Janjaroen, D.; Huang, C.; Morgenroth, E.; Boppart, S.A.; Ashbolt, N.J.; Liu, W.-T.; Nguyen, T.H. Role of Biofilm Roughness and Hydrodynamic Conditions in Legionella pneumophila Adhesion to and Detachment from Simulated Drinking Water Biofilms. Environ. Sci. Technol. 2015, 49, 4274–4282. [Google Scholar] [CrossRef]
- Beer, K.D.; Gargano, J.W.; Roberts, V.A.; Hill, V.R.; Garrison, L.E.; Kutty, P.K.; Hilborn, E.D.; Wade, T.J.; Fullerton, K.E.; Yoder, J.S. Surveillance for Waterborne Disease Outbreaks Associated with Drinking Water—United States, 2011–2012. Morb. Mortal. Wkly. Rep. 2015, 64, 842–848. [Google Scholar] [CrossRef] [PubMed]
- Beer, K.D.; Gargano, J.W.; Roberts, V.A.; Reses, H.E.; Hill, V.R.; Garrison, L.E.; Kutty, P.K.; Hillborn, E.D.; Wade, T.J.; Fullerton, K.E.; et al. Outbreaks Associated with Environmental and Undetermined Water Exposures—United States, 2011–2012. Morb. Mortal. Wkly. Rep. 2015, 64, 849–851. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Whiley, H. Legionella Risk Management and Control in Potable Water Systems: Argument for the Abolishment of Routine Testing. Int. J. Environ. Res. Public Health 2017, 14, 12. [Google Scholar] [CrossRef] [PubMed]
- National Academies of Sciences. Management of Legionella in Water Systems; National Academies of Sciences: Washington, DC, USA, 2019; ISBN 978-0-309-49379-6. [Google Scholar]
- Molofsky, A.B.; Shetron-Rama, L.M.; Swanson, M.S. Components of the Legionella pneumophila flagellar regulon contribute to multiple virulence traits, including lysosome avoidance and macrophage death. Infect. Immun. 2005, 73, 5720–5734. [Google Scholar] [CrossRef] [PubMed]
- Abu Khweek, A.; Fernández Dávila, N.S.; Caution, K.; Akhter, A.; Abdulrahman, B.A.; Tazi, M.; Hassan, H.; Novotny, L.A.; Bakaletz, L.O.; Amer, A.O. Biofilm-derived Legionella pneumophila evades the innate immune response in macrophages. Front. Cell. Infect. Microbiol. 2013, 3, 18. [Google Scholar] [CrossRef] [PubMed]
- Mraz, A.L.; Weir, M.H. Knowledge to Predict Pathogens: Legionella pneumophila Lifecycle Critical Review Part I Uptake into Host Cells. Water 2018, 10, 132. [Google Scholar] [CrossRef]
- Brüggemann, H.; Hagman, A.; Jules, M.; Sismeiro, O.; Dillies, M.-A.; Gouyette, C.; Kunst, F.; Steinert, M.; Heuner, K.; Coppée, J.-Y.; et al. Virulence strategies for infecting phagocytes deduced from the in vivo transcriptional program of Legionella pneumophila. Cell. Microbiol. 2006, 8, 1228–1240. [Google Scholar] [CrossRef]
- Amer, A.; Franchi, L.; Kanneganti, T.-D.; Body-Malapel, M.; Özören, N.; Brady, G.; Meshinchi, S.; Jagirdar, R.; Gewirtz, A.; Akira, S.; et al. Regulation of Legionella Phagosome Maturation and Infection through Flagellin and Host Ipaf. J. Biol. Chem. 2006, 281, 35217–35223. [Google Scholar] [CrossRef]
- Khweek, A.A.; Amer, A. Replication of Legionella Pneumophila in Human Cells: Why are We Susceptible? Front. Microbiol. 2010, 1, 133. [Google Scholar] [CrossRef]
- Abdelaziz, D.H.A.; Gavrilin, M.A.; Akhter, A.; Caution, K.; Kotrange, S.; Khweek, A.A.; Abdulrahman, B.A.; Hassan, Z.A.; El-Sharkawi, F.Z.; Bedi, S.S.; et al. Asc-Dependent and Independent Mechanisms Contribute to Restriction of Legionella Pneumophila Infection in Murine Macrophages. Front. Microbiol. 2011, 2, 18. [Google Scholar] [CrossRef]
- Winn, W.C. Legionnaires disease: Historical perspective. Clin. Microbiol. Rev. 1988, 1, 60–81. [Google Scholar] [CrossRef] [PubMed]
- Fields, B.S.; Benson, R.F.; Besser, R.E. Legionella and Legionnaires’ Disease: 25 Years of Investigation. Clin. Microbiol. Rev. 2002, 15, 506–526. [Google Scholar] [CrossRef] [PubMed]
- Haas, C.N.; Rose, J.B.; Gerba, C.P. Quantitative Microbial Risk Assessment, 2nd ed.; John Wiley and Sons: Hoboken, NJ, USA, 2014. [Google Scholar]
- Rose, J.B.; Haas, C.N.; Regli, S. Risk Assessment and Control of Waterborne Giardiasis. Am. J. Public Health 1991, 81, 709–712. [Google Scholar] [CrossRef] [PubMed]
- Ashbolt, N.J.; Schoen, M.E.; Soller, J.A.; Roser, D.J. Predicting pathogen risks to aid beach management: The real value of quantitative microbial risk assessment (QMRA). Water Res. 2010, 44, 4692–4703. [Google Scholar] [CrossRef]
- Schoen, M.E.; Ashbolt, N.J. An in-premise model for Legionella exposure during showering events. Water Res. 2011, 45, 5826–5836. [Google Scholar] [CrossRef] [PubMed]
- Weir, M.H.; Shibata, T.; Masago, Y.; Cologgi, D.L.; Rose, J.B. Effect of Surface Sampling and Recovery of Viruses and Non-Spore-Forming Bacteria on a Quantitative Microbial Risk Assessment Model for Fomites. Environ. Sci. Technol. 2016, 50, 5945–5952. [Google Scholar] [CrossRef]
- Hamilton, K.A.; Hamilton, M.T.; Johnson, W.; Jjemba, P.; Bukhari, Z.; LeChevallier, M.; Haas, C.N.; Gurian, P.L. Risk-Based Critical Concentrations of Legionella pneumophila for Indoor Residential Water Uses. Environ. Sci. Technol. 2019, 53, 4528–4541. [Google Scholar] [CrossRef]
- Schets, F.M.; Engels, G.B.; Evers, E.G. Cryptosporidium and Giardia in swimming pools in the Netherlands. J. Water Health 2004, 2, 191–200. [Google Scholar] [CrossRef][Green Version]
- Pintar, K.D.M.; Fazil, A.; Pollari, F.; Charron, D.F.; Waltner-Toews, D.; McEwen, S.A. A Risk Assessment Model to Evaluate the Role of Fecal Contamination in Recreational Water on the Incidence of Cryptosporidiosis at the Community Level in Ontario. Risk Anal. 2010, 30, 49–64. [Google Scholar] [CrossRef]
- Vergara, G.G.R.V.; Rose, J.B.; Gin, K.Y.H. Risk assessment of noroviruses and human adenoviruses in recreational surface waters. Water Res. 2016, 103, 276–282. [Google Scholar] [CrossRef]
- U.S. EPA. Exposure Factors Handbook 2011 Edition (Final); U.S. Environmental Protection Agency: Washington, DC, USA, 2011.
- Smeets, P.; Medema, G.J.; Van Dijk, J.C. The Dutch secret: How to provide safe drinking water without chlorine in the Netherlands. Drink. Water Eng. Sci. 2009, 2, 1–14. [Google Scholar] [CrossRef]
- Bentham, R.; Whiley, H. Quantitative Microbial Risk Assessment and Opportunist Waterborne Infections–Are There Too Many Gaps to Fill? Int. J. Environ. Res. Public Health 2018, 15, 1150. [Google Scholar] [CrossRef] [PubMed]
- Weir, M.H. Dose-Response Modeling and Use: Challenges and Uncertainties in Environmental Exposure. In Manual of Environmental Microbiology; ASM Press: Sterling, VA, USA, 2016; pp. 1–17. [Google Scholar]
- Haas, C.N. Estimation of risk due to low doses of microorganisms: A comparison of alternative methodologies. Am. J. Epidemiol. 1983, 118, 573–582. [Google Scholar] [CrossRef] [PubMed]
- Weir, M.H.; Haas, C.N. Quantification of the Effects of Age on the Dose Response of Variola major in Suckling Mice. Hum. Ecol. Risk Assess. Int. J. 2009, 15, 1245–1256. [Google Scholar] [CrossRef]
- Weir, M.H.; Haas, C.N. A Model for In-vivo Delivered Dose Estimation for Inhaled Bacillus anthracis Spores in Humans with Interspecies Extrapolation. Environ. Sci. Technol. 2011, 45, 5828–5833. [Google Scholar] [CrossRef] [PubMed]
- Haas, C.N. Microbial Dose Response Modeling: Past, Present, and Future. Environ. Sci. Technol. 2015, 49, 1245–1259. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, T.W.; Haas, C.N. A Quantitative Microbial Risk Assessment Model for Legionnaires’ Disease: Animal Model Selection and Dose-Response Modeling. Risk Anal. 2007, 27, 1581–1596. [Google Scholar] [CrossRef]
- Ross, S.M. Introduction to Probability Models; Academic Press: Burlington, MA, USA, 2007. [Google Scholar]
- Frey, C.H. Separating Variability and Uncertainty in Exposure Assessment: Motivation and Method. In Proceedings of the 86th Annual Meeting of the Air and Waste Management Association, Denver, CO, USA, 13–18 June 1993; pp. 13–18. [Google Scholar]
- Zhou, Y.; Benson, J.M.; Irvin, C.; Irshad, H.; Cheng, Y.-S. Particle Size Distribution and Inhalation Dose of Shower Water Under Selected Operating Conditions. Inhal. Toxicol. 2007, 19, 333–342. [Google Scholar] [CrossRef]
- Borella, P.; Guerrieri, E.; Marchesi, I.; Bondi, M.; Messi, P. Water ecology of Legionella and protozoan: Environmental and public health perspectives. Biotechnol. Annu. Rev. 2005, 11, 355–380. [Google Scholar]
- Völker, S.; Schreiber, C.; Kistemann, T. Drinking water quality in household supply infrastructure—A survey of the current situation in Germany. Int. J. Hyg. Environ. Health 2010, 213, 204–209. [Google Scholar] [CrossRef]
- McClellan, R.O.; Henderson, R.F. Concepts in Inhalation Toxicology; Hemisphere Publishing Corporation: New York, NY, USA, 1989. [Google Scholar]
- Dooling, K.L.; Toews, K.A.; Hicks, L.A.; Garrison, L.E.; Bachaus, B.; Zansky, S.; Carpenter, L.R.; Schaffner, B.; Parker, E.; Petit, S.; et al. Active bacterial core surveillance for legionellosis—United States, 2011–2013. Morb. Mortal. Wkly. Rep. MMWR 2015, 64, 1190–1193. [Google Scholar] [CrossRef] [PubMed]
- Haagsma, J.A.; Maertens de Noordhout, C.; Polinder, S.; Vos, T.; Havelaar, A.H.; Cassini, A.; Devleesschauwer, B.; Kretzschmar, M.E.; Speybroeck, N.; Salomon, J.A. Assessing disability weights based on the responses of 30,660 people from four European countries. Popul. Health Metr. 2015, 13, 10. [Google Scholar] [CrossRef] [PubMed]
- Rizzo, M.L. Statistical Computing with R; Taylor and Francis: Boca Raton, FL, USA, 2008. [Google Scholar]
- Baskerville, A.; Fitzgeorge, R.B.; Broster, M.; Hambleton, P.; Dennis, P.J. Experimental transmission of legionnaires’ disease by exposure to aerosols of Legionella pneumophila. Lancet 1981, 2, 1389–1390. [Google Scholar] [CrossRef]
- Moritz, A.R.; Henriques, F.C. Studies of Thermal Injury. Am. J. Pathol. 1947, 23, 695–720. [Google Scholar]
- Maruyama, W.; Hirano, S.; Kobayashi, T.; Aoki, Y. Quantitative Risk Analysis of Particulate Matter in Air Interspecies Extrapolation with Bioassay and Mathematical Models. Inhal. Toxicol. 2006, 18, 1013–1023. [Google Scholar] [CrossRef]
- Weir, M.H.; Pepe Razzolini, M.T.; Rose, J.B.; Masago, Y. Water reclamation redesign for reducing Cryptosporidium risks at a recreational spray park using stochastic models. Water Res. 2011, 45, 6505–6514. [Google Scholar] [CrossRef]
- Fujioka, R.S.; Solo-Gabriele, H.M.; Byappanahalli, M.N.; Kirs, M. US recreational water quality criteria: A vision for the future. Int. J. Environ. Res. Public Health 2015, 12, 7752–7776. [Google Scholar] [CrossRef]
- OSHA Technical Manual (OTM) | Section III: Chapter 7—Legionnaires’ Disease|Occupational Safety and Health Administration. Available online: https://www.osha.gov/dts/osta/otm/otm_iii/otm_iii_7.html (accessed on 20 September 2017).
- Centers for Disease Control and Prevention (CDC) Legionellosis—United States, 2000–2009. Morb. Mortal. Wkly. Rep. MMWR 2011, 60, 1083–1086.
- Hamilton, K.; Haas, C. Critical review of mathematical approaches for quantitative microbial risk assessment (QMRA) of Legionella in engineered water systems: Research gaps and a new framework. Environ. Sci. Water Res. Technol. 2016, 2, 599–613. [Google Scholar] [CrossRef]
- Weir, M.H.; Mraz, A.L.; Nappier, S.P.; Haas, C.N. Dose-Response Models for Eastern US, Western US and Venezuelan Equine Encephalitis Viruses in Mice—Part II: Quantification of the Effects of Host Age on the Dose Response. Microb. Risk Anal. 2018, 9, 38–54. [Google Scholar] [CrossRef]
- Bartrand, T.A.; Weir, M.H.; Haas, C.N. Dose-Response Models for Inhalation of Bacillus anthracis Spores: Interspecies Comparisons. Risk Anal. 2008, 28, 1115–1124. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, K.A.; Weir, M.H.; Haas, C.N. Dose response models and a quantitative microbial risk assessment framework for the Mycobacterium avium complex that account for recent developments in molecular biology, taxonomy, and epidemiology. Water Res. 2017, 109, 310–326. [Google Scholar] [CrossRef]
- Huang, Y.; Bartrand, T.A.; Haas, C.N.; Weir, M.H. Incorporating TIme Postinoculation into a Dose-Response Model of Yersinia Pestis in Mice. J. Appl. Microbiol. 2009, 107, 727–735. [Google Scholar] [CrossRef] [PubMed]
- Brouwer, A.F.; Weir, M.H.; Eisenberg, M.C.; Meza, R.; Eisenberg, J.N.S. Dose-response relationships for environmentally mediated infectious disease transmission models. PLoS Comput. Biol. 2017, 13, e1005481. [Google Scholar] [CrossRef] [PubMed]

| Model Parameter | Distribution Variability or Uncertainty a; AICw | Value(s) | Units | Citation |
|---|---|---|---|---|
| Hmix | Truncated Normal b—V AICw = 0.350 | µ c = 0.5778; σ d = 0.0399 UB e = 0.5094; LB f = 0.6472 | Unitless | Estimated in this research |
| Cmix | Cauchy—V AICw = 0.65 | Location = 0.363; Scale = 0.0217 | ||
| AFQ1H | Triangular—V AICw = NA h | Min = 0.0097; Median = 0.0013 Max = 0.0069 | Distribution optimized in this research, data used for optimization from [46] | |
| AFQ2H | Triangular—V AICw = NA h | Min = 0.0014; Median = 0.0027 Max = 0.0128 | ||
| AFQ3H | Triangular—V AICw = NA h | Min = 0.0010; Median = 0.0015 Max = 0.0061 | ||
| AFQ1C | Truncated Weibull—V AICw = 0.349 | Scale = 2.754; shape = 0.0308 UB = 0.0478; LB = 1(10−15) | ||
| AFQ2C | Truncated Weibull—V AICw = 0.460 | Scale = 4.125; shape = 0.0373 UB = 0.0473; LB = 1(10−15) | ||
| AFQ3C | Triangular—V AICw = NA h | Min = 0.0097; Median = 0.0128 Max = 0.0173 | ||
| Cw | Uniform—U AICw = NA h | Min = 1; Max = 1(106) | CFU L−1 | Min [47], Max [48] |
| PC | Uniform—V AICw = NA h | Min = 0.25; Max = 0.65 | Unitless | Value from [29] |
| ts | Uniform—V AICw = NA h | Min = 0.0333; Max = 0.25 | Hours | Estimated in this research |
| RI,Child | Triangular—V AICw = NA h | Min = 0.0076; Median = 0.0111 Max = 0.013 | m3 h−1 | Distributions chosen in this research, data from US EPA exposure factors handbook [35] |
| RI,Adult | Triangular—V AICw = NA h | Min = 0.012; Median = 0.0124 Max = 0.013 | ||
| RI,Elderly | Point value—V AICw = NA h | 0.012 | ||
| DF1 | Truncated Logistic b—U AICw = 0.525 | Location = 0.06777; Scale = 0.04305 UB = 0.01; LB = 0.195 | Unitless | Distributions from this research, data from [49] |
| DF2 | Truncated Weibull b—U AICw = 0.658 | Scale = 0.4134; shape = 0.2102 UB = 0.00; LB = 0.41 | ||
| DF3 | Truncated lognormal b—U AICw = 0.429 | µ = –1.052; σ = 0.4350 UB = 0.159; LB = 0.62 | ||
| k | Triangular—U AICw = NA h | Median = 0.00599; Min = 0.00326; Max = 0.131 | Distribution from this research. Values from [43] | |
| ;;g | Point values AICw = NA h | 0.0077; 0.097; 0.75 for Child Adult and Elderly respectively | Calculated in this research Data from [50] | |
| ;;;;g | Point values AICw = NA h | 0.0025; 0.010; 0.15; 0.61; 1.4 (10−5) for American Indian; Asian; Black; White and Other races respectively | ||
| ;g | Point Values AICw = NA h | 0.64; 0.36 for male and female respectively | ||
| DWM | Triangular—U AICw = NA h | Min = 0.039; median = 0.051; max = 0.06 | Distributions from this research data from [51] | |
| DWP | Triangular—U AICw = NA h | Min = 0.104; median = 0.125; max = 0.152 | ||
| DWS | Triangular—U AICw = NA h | Min = 0.179; median = 0.217; max = 0.251 |
| Demographic Group | Statistic | Pinf a | Pill b | MDALY c | SDALY d | PDALY e |
|---|---|---|---|---|---|---|
| Child | U95 f | 7.29 (10−6) | 2.39 (10−7) | 1.20 (10−8) | 3.03 (10−8) | 6.36 (10−8) |
| M g | 2.61 (10−6) | 4.98 (10−8) | 2.48 (10−9) | 6.28 (10−9) | 1.32 (10−8) | |
| L95 h | 2.69 (10−7) | 4.19 (10−9) | 2.08 (10−10) | 5.28 (10−10) | 1.11 (10−9) | |
| Adult | U95 | 7.93 (10−6) | 1.84 (10−6) | 9.30 (10−8) | 2.36 (10−6) | 4.88 (10−7) |
| M | 2.84 (10−6) | 3.85 (10−7) | 1.91 (10−8) | 4.87 (10−8) | 1.02 (10−7) | |
| L95 | 2.93 (10−7) | 3.24 (10−8) | 1.60 (10−9) | 4.09 (10−9) | 8.53 (10−9) | |
| Elderly | U95 | 7.57 (10−6) | 2.64 (10−5) | 1.33 (10−6) | 3.37 (10−6) | 7.00 (10−6) |
| M | 2.71 (10−6) | 5.54 (10−6) | 2.75 (10−7) | 7.03 (10−7) | 1.47 (10−6) | |
| L95 | 2.79 (10−7) | 4.65 (10−7) | 2.30 (10−8) | 5.88 (10−8) | 1.23 (10−7) | |
| Combined Ages | U95 | 5.95 (10−5) | Not Modeled j | |||
| M | 1.25 (10−5) | |||||
| L95 | 1.05 (10−6) | |||||
| American Indian | U95 | NA i | 8.34 (10−6) | 4.20 (10−7) | 1.07 (10−6) | 2.21 (10−6) |
| M | 1.75 (10−6) | 8.70 (10−8) | 2.21 (10−7) | 4.65 (10−7) | ||
| L95 | 1.47 (10−7) | 7.27 (10−9) | 1.86 (10−8) | 3.91 (10−8) | ||
| Asian | U95 | 5.56 (10−6) | 2.80 (10−7) | 7.05 (10−7) | 1.48 (10−6) | |
| M | 1.16 (10−6) | 5.78 (10−8) | 1.48 (10−7) | 3.09 (10−7) | ||
| L95 | 9.80 (10−8) | 4.86 (10−9) | 1.24 (10−8) | 2.60 (10−8) | ||
| Black | U95 | 3.45 (10−5) | 1.74 (10−6) | 4.9 (10−6) | 9.19 (10−6) | |
| M | 7.24 (10−6) | 3.63 (10−7) | 9.15 (10−7) | 1.92 (10−6) | ||
| L95 | 6.09 (10−7) | 3.04 (10−8) | 7.68 (10−8) | 1.62 (10−7) | ||
| White | U95 | 2.34 (10−5) | 1.71 (10−6) | 2.97 (10−6) | 6.20 (10−6) | |
| M | 4.91 (10−6) | 2.45 (10−7) | 6.21 (10−7) | 1.30 (10−6) | ||
| L95 | 4.13 (10−7) | 2.04 (10−8) | 5.21 (10−8) | 1.10 (10−7) | ||
| Other | U95 | 1.48 (10−7) | 7.38 (10−9) | 1.87 (10−8) | 3.93 (10−8) | |
| M | 3.10 (10−8) | 1.55 (10−9) | 3.91 (10−9) | 8.22 (10−9) | ||
| L95 | 2.61 (10−9) | 1.30 (10−10) | 3.29 (10−10) | 6.90 (10−10) | ||
| Female | U95 | 2.10 (10−5) | 1.06 (10−6) | 2.69 (10−6) | 5.61 (10−6) | |
| M | 4.41 (10−6) | 2.19 (10−7) | 5.59 (10−7) | 1.17 (10−6) | ||
| L95 | 3.71 (10−7) | 1.84 (10−8) | 4.69 (10−8) | 9.80 (10−8) | ||
| Male | U95 | 3.85 (10−5) | 1.92 (10−6) | 4.93 (10−6) | 1.02 (10−5) | |
| M | 8.07 (10−6) | 4.03 (10−7) | 1.02 (10−6) | 2.14 (10−6) | ||
| L95 | 6.79 (10−7) | 3.37 (10−8) | 8.56 (10−8) | 1.79 (10−7) | ||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Weir, M.H.; Mraz, A.L.; Mitchell, J. An Advanced Risk Modeling Method to Estimate Legionellosis Risks Within a Diverse Population. Water 2020, 12, 43. https://doi.org/10.3390/w12010043
Weir MH, Mraz AL, Mitchell J. An Advanced Risk Modeling Method to Estimate Legionellosis Risks Within a Diverse Population. Water. 2020; 12(1):43. https://doi.org/10.3390/w12010043
Chicago/Turabian StyleWeir, Mark H., Alexis L. Mraz, and Jade Mitchell. 2020. "An Advanced Risk Modeling Method to Estimate Legionellosis Risks Within a Diverse Population" Water 12, no. 1: 43. https://doi.org/10.3390/w12010043
APA StyleWeir, M. H., Mraz, A. L., & Mitchell, J. (2020). An Advanced Risk Modeling Method to Estimate Legionellosis Risks Within a Diverse Population. Water, 12(1), 43. https://doi.org/10.3390/w12010043






