Health Risks to the Russian Population from Temperature Extremes at the Beginning of the XXI Century
Abstract
1. Introduction
1.1. Definition of Heat and Colds Waves
1.2. Temperature Waves and Human Health
1.3. Russia and Temperature Extremes
2. Materials and Methods
3. Results
3.1. Moscow and Saint Petersburg
3.2. Arctic Macro-Region
3.3. Southern Cities of the European Russia
3.4. Siberia, Continental Climate
3.5. Cities with Monsoon Climate at the Russian Far East: Vladivostok and Khabarovsk
3.6. Ambulance Calls during Periods with Extreme Air Temperature
3.7. Combined Effects of a Heat Wave, Urban and Wildfire Air Pollution
4. Concluding Comments
4.1. Combined Effects of Temperature Waves and COVID-19 on Human Health
4.2. Urban Heat Island Effect
4.3. Mitigation Policy and Prevention Plans
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- AghaKouchak, A.; Chiang, F.; Huning, L.S.; Love, C.A.; Mallakpour, I.; Mazdiyasni, O.; Moftakhari, H.; Papalexiou, S.M.; Ragno, E.; Sadegh, M. Climate Extremes and Compound Hazards in a Warming World. Annu. Rev. Earth Planet. Sci. 2020, 48, 519–548. [Google Scholar] [CrossRef]
- Baldwin, J.W.; Dessy, J.B.; Vecchi, G.A.; Oppenheimer, M. Temporally Compound Heat Wave Events and Global Warming: An Emerging Hazard. Earths Future 2019, 7, 411–427. [Google Scholar] [CrossRef]
- Ciavarella, A.; Cotterill, D.; Stott, P.; Kew, S.; Philip, S.; van Oldenborgh, G.J.; Skålevåg, A.; Lorenz, P.; Robin, Y.; Otto, F.; et al. Prolonged Siberian heat of 2020 almost impossible without human influence. Clim. Chang. 2021, 166, 1–18. [Google Scholar] [CrossRef]
- Clarke, B.J.; Otto, F.E.L.; Jones, R.G. Inventories of extreme weather events and impacts: Implications for loss and damage from and adaptation to climate extremes. Clim. Risk Manag. 2021, 32, 100285. [Google Scholar] [CrossRef]
- Coumou, D.; Rahmstorf, S. A decade of weather extremes. Nat. Clim. Chang. 2012, 2, 491–496. [Google Scholar] [CrossRef]
- Cutter, S.L. Compound, Cascading, or Complex Disasters: What’s in a Name? Environ. Sci. Policy Sustain. Dev. 2018, 60, 16–25. [Google Scholar] [CrossRef]
- Diffenbaugh, N.S.; Singh, D.; Mankin, J.S.; Horton, D.E.; Swain, D.L.; Touma, D.; Charland, A.; Liu, Y.; Haugen, M.; Tsiang, M.; et al. Quantifying the influence of global warming on unprecedented extreme climate events. Proc. Natl. Acad. Sci. USA 2017, 114, 4881–4886. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.L.; Vanos, J.; Baldwin, J.W.; Bell, J.E.; Hondula, D.M.; Errett, N.A.; Hayes, K.; Reid, C.E.; Saha, S.; Spector, J.; et al. Extreme Weather and Climate Change: Population Health and Health System Implications. Annu. Rev. Public Health 2021, 42, 293–315. [Google Scholar] [CrossRef]
- Fischer, E.M.; Sippel, S.; Knutti, R. Increasing probability of record-shattering climate extremes. Nat. Clim. Chang. 2021, 11, 689–695. [Google Scholar] [CrossRef]
- Gessner, C.; Fischer, E.M.; Beyerle, U.; Knutti, R. Very Rare Heat Extremes: Quantifying and Understanding Using Ensemble Reinitialization. J. Clim. 2021, 34, 6619–6634. [Google Scholar] [CrossRef]
- Gruza, G.V.; Rankova, E.Y. Observed and Expected Climate Changes in Russia: Air Temperature; VNIIGMI-MCD; Federal State Institution: Obninsk, Russia, 2012; 194p. (In Russian) [Google Scholar]
- Groisman, P.; Shugart, H.; Kicklighter, D.; Henebry, G.; Tchebakova, N.; Maksyutov, S.; Monier, E.; Gutman, G.; Gulev, S.; Qi, J.; et al. Northern Eurasia Future Initiative (NEFI): Facing the challenges and pathways of global change in the twenty-first century. Prog. Earth Planet. Sci. 2017, 4, 41. [Google Scholar] [CrossRef]
- Hao, Z.; Singh, V.P.; Hao, F. Compound Extremes in Hydroclimatology: A Review. Water 2018, 10, 718. [Google Scholar] [CrossRef]
- Hoag, H. Russian summer tops ’universal’ heatwave index. Nature 2014, 16. [Google Scholar] [CrossRef]
- Ionita, M.; Caldarescu, D.E.; Nagavciuc, V. Compound Hot and Dry Events in Europe: Variability and Large-Scale Drivers. Front. Clim. 2021, 3, 58. [Google Scholar] [CrossRef]
- IPCC, Intergovernmental Panel on Climate Change. Sixth Assessment Report Fact Sheet. 2021. Available online: https://www.ipcc.ch/site/assets/uploads/2021/06/Fact_sheet_AR6.pdf (accessed on 30 August 2021).
- Kharuk, V.I.; Ponomarev, E.I.; Ivanova, G.A.; Dvinskaya, M.L.; Coogan, S.C.P.; Flannigan, M.D. Wildfires in the Siberian taiga. Ambio 2021, 50, 1953–1974. [Google Scholar] [CrossRef] [PubMed]
- Kuznetsova, V.P. Analyzing extreme weather phenomena in northern regions in the context of modern climate change. IOP Conf. Ser. Earth Environ. Sci. 2020, 611, 012050. [Google Scholar] [CrossRef]
- La Sorte, F.A.; Johnston, A.; Ault, T.R. Global trends in the frequency and duration of temperature extremes. Clim. Chang. 2021, 166, 1–14. [Google Scholar] [CrossRef]
- Lau, W.K.M.; Kim, K.-M. The 2010 Pakistan Flood and Russian Heat Wave: Teleconnection of Hydrometeorological Extremes. J. Hydrometeorol. 2012, 13, 392–403. [Google Scholar] [CrossRef]
- Mokhov, I.I.; Semenov, V.A. Weather and Climate Anomalies In Russian Regions Related to Global Climate Change. Russ. Meteorol. Hydrol. 2016, 41, 84–92. [Google Scholar] [CrossRef]
- Mukherjee, S.; Mishra, A.K. Increase in Compound Drought and Heatwaves in a Warming World. Geophys. Res. Lett. 2021, 48, e2020GL090617. [Google Scholar] [CrossRef]
- Otto, F.E.L.; Massey, N.; van Oldenborgh, G.J.; Jones, R.G.; Allen, M.R. Reconciling two approaches to attribution of the 2010 Russian heat wave. Geophys. Res. Lett. 2012, 39, L04702. [Google Scholar] [CrossRef]
- Patz, J.A. Climate Variability and Change: Food, Water, and Societal Impacts. In Climate Change and Global Public Health. Respiratory Medicine; Pinkerton, K.E., Rom, W.N., Eds.; Humana: Cham, Switzerland, 2021; pp. 311–338. [Google Scholar] [CrossRef]
- Perevedentsev, Y.P.; Shumikhina, A.V.; Shantalinskii, K.M.; Guryanov, V.V. Hydrometeorological Hazards in the Volga Federal District. Russ. Meteorol. Hydrol. 2019, 44, 802–809. [Google Scholar] [CrossRef]
- Perkins-Kirkpatrick, S.E.; Lewis, S.C. Increasing trends in regional heatwaves. Nat. Commun. 2020, 11, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Prodhomme, C.; Materia, S.; Ardilouze, C.; White, R.H.; Batté, L.; Guemas, V.; Fragkoulidis, G.; García-Serrano, J. Seasonal prediction of European summer heatwaves. Clim. Dyn. 2021, 1–18. [Google Scholar] [CrossRef]
- Russo, S.; Sillmann, J.; Fischer, E.M. Top ten European heatwaves since 1950 and their occurrence in the coming decades. Environ. Res. Lett. 2015, 10, 124003. [Google Scholar] [CrossRef]
- Schiermeier, Q. Droughts, heatwaves and floods: How to tell when climate change is to blame. Nature 2018, 560, 20–22. [Google Scholar] [CrossRef]
- Sena, A.; Ebi, K. When Land Is Under Pressure Health Is Under Stress. Int. J. Environ. Res. Public Health 2020, 18, 136. [Google Scholar] [CrossRef]
- Shukla, P.R.; Skea, J.; Calvo Buendia, E.; Masson-Delmotte, V.; Pörtner, H.O.; Roberts, D.C.; Zhai, P.; Slade, R.; Connors, S.; Van Diemen, R.; et al. IPCC, 2019: Climate Change and Land: An IPCC Special Report on Climate Change, Desertification, Land Degradation, Sustainable land Management, Food Security, and Greenhouse Gas Fluxes in Terrestrial Ecosystems; IPCC: Geneva, Switzerland, 2019. [Google Scholar]
- Shvidenko, A.Z.; Shchepashchenko, D.G.; Vaganov, E.A.; Sukhinin, A.I.; Maksyutov, S.S.; McCallum, I.; Lakyda, I.P. Impact of wildfire in Russia between 1998–2010 on ecosystems and the global carbon budget. Dokl. Earth Sci. 2011, 441, 1678–1682. [Google Scholar] [CrossRef]
- Smith, E.T.; Sheridan, S. Projections of Cold Air Outbreaks. In CMIP6 Earth System Models; Research Square: Durham, NC, USA, 2021. [Google Scholar] [CrossRef]
- Tedim, F.; Leone, V.; Amraoui, M.; Bouillon, C.; Coughlan, M.R.; Delogu, G.M.; Fernandes, P.M.; Ferreira, C.; McCaffrey, S.; McGee, T.K.; et al. Defining Extreme Wildfire Events: Difficulties, Challenges, and Impacts. Fire 2018, 1, 9. [Google Scholar] [CrossRef]
- Trenberth, K.E.; Fasullo, J. Climate extremes and climate change: The Russian heat wave and other climate extremes of 2010. J. Geophys. Res. 2012, 117, D17103. [Google Scholar] [CrossRef]
- Twardosz, R.; Kossowska-Cezak, U. Large-area thermal anomalies in Europe (1951–2018). Temporal and spatial patterns. Atmospheric Res. 2021, 251, 105434. [Google Scholar] [CrossRef]
- Ummenhofer, C.C.; Meehl, G.A. Extreme weather and climate events with ecological relevance: A review. Philos. Trans. R. Soc. B Biol. Sci. 2017, 372, 20160135. [Google Scholar] [CrossRef]
- Vinogradova, V.V. Thermal impact on the territory of Russia in the middle of the XXI century according to model data. Izv. Ross. Akad. Nauk. Ser. Geogr. 2020, 3, 404–413. (In Russian) [Google Scholar] [CrossRef]
- Zhang, M.; Chen, Y.; Shen, Y.; Li, B. Tracking climate change in Central Asia through temperature and precipitation extremes. J. Geogr. Sci. 2019, 29, 3–28. [Google Scholar] [CrossRef]
- Zhang, P.; Ren, G.; Xu, Y.; Wang, X.L.; Qin, Y.; Sun, X.; Ren, Y. Observed Changes in Extreme Temperature over the Global Land Based on a Newly Developed Station Daily Dataset. J. Clim. 2019, 32, 8489–8509. [Google Scholar] [CrossRef]
- Zscheischler, J.; Martius, O.; Westra, S.; Bevacqua, E.; Raymond, C.; Horton, R.M.; Hurk, B.V.D.; AghaKouchak, A.; Jézéquel, A.; Mahecha, M.D.; et al. A typology of compound weather and climate events. Nat. Rev. Earth Environ. 2020, 1, 333–347. [Google Scholar] [CrossRef]
- Ageev, F.T.; Smirnova, M.D.; Galaninsky, P.V. Assessment of the immediate and delayed impact of the abnormally hot summer of 2010 on the cardiovascular diseases in outpatient practice. Ther. Arch. 2012, 8, 45–51. (In Russian) [Google Scholar]
- Ageev, F.T.; Smirnova, M.D.; Svirida, O.N.; Fofanova, T.V.; Vitsenya, M.V.; Blankova, Z.N.; Mikhailov, G.V.; Lankin, V.Z.; Konovalova, G.G.; Tikhaze, A.K.; et al. Impact of a cold wave on disease course, hemodynamics, carbohydrate metabolism, and blood rheological properties in cardiac patents. Ter. Arkhiv 2015, 87, 11–16. [Google Scholar] [CrossRef] [PubMed]
- Analitis, A.; Michelozzi, P.; D’Ippoliti, D.; De’Donato, F.; Menne, B.; Matthies, F.; Atkinson, R.W.; Iñiguez, C.; Basagaña, X.; Schneider, A.; et al. Effects of Heat Waves on Mortality. Epidemiology 2014, 25, 15–22. [Google Scholar] [CrossRef]
- Anderko, L.; Chalupka, S.; Du, M.; Hauptman, M. Climate changes reproductive and children’s health: A review of risks, exposures, and impacts. Pediatr. Res. 2020, 87, 414–419. [Google Scholar] [CrossRef]
- Baccini, M.; Kosatsky, T.; Biggeri, A. Impact of Summer Heat on Urban Population Mortality in Europe during the 1990s: An Evaluation of Years of Life Lost Adjusted for Harvesting. PLoS ONE 2013, 8, e69638. [Google Scholar] [CrossRef]
- Barriopedro, D.; Fischer, E.M.; Luterbacher, J.; Trigo, R.M.; García-Herrera, R. The Hot Summer of 2010: Redrawing the Temperature Record Map of Europe. Science 2011, 332, 220–224. [Google Scholar] [CrossRef]
- Basarin, B.; Lukić, T.; Matzarakis, A. Quantification and assessment of heat and cold waves in Novi Sad, Northern Serbia. Int. J. Biometeorol. 2015, 60, 139–150. [Google Scholar] [CrossRef]
- Boytsov, S.A.; Lukyanov, M.M.; Deev, A.D.; Klyashtorny, V.G.; Ivanenko, A.V.; Volkova, N.S.; Kuznetsov, A.S.; Skvortsov, A.S.; Solovyev, D.V. The influence of environmental factors on the mortality of the population of Moscow: The possibilities of risks and forecasting. Russ. J. Cardiol. 2016, 6, 34–40. (In Russian) [Google Scholar] [CrossRef][Green Version]
- Brázdil, R.; Chromá, K.; Dolák, L.; Řehoř, J.; Řezníčková, L.; Zahradníček, P.; Dobrovolný, P. Fatalities associated with the severe weather conditions in the Czech Republic, 2000–2019. Nat. Hazards Earth Syst. Sci. 2021, 21, 1355–1382. [Google Scholar] [CrossRef]
- Brennenstuhl, H.; Will, M.; Ries, E.; Mechler, K.; Garbade, S.; Ries, M. Patterns of extreme temperature-related catastrophic events in Europe including the Russian Federation: A cross-sectional analysis of the Emergency Events Database. BMJ Open 2021, 11, e046359. [Google Scholar] [CrossRef]
- Carder, M.; McNamee, R.; Beverland, I.; Elton, R.; Cohen, J.; Boyd, J.; Agius, R. The lagged effect of cold temperature and wind chill on cardiorespiratory mortality in Scotland. Occup. Environ. Med. 2005, 62, 702–710. [Google Scholar] [CrossRef] [PubMed]
- Cheng, W.; Li, D.; Liu, Z.; Brown, R.D. Approaches for identifying heat-vulnerable populations and locations: A systematic review. Sci. Total. Environ. 2021, 799, 149417. [Google Scholar] [CrossRef]
- Chereshnev, V.A.; Gamburtsev, A.G.; Sigachev, A.V. Dynamics of ambulance calls in Moscow (2006–2011). Space Time 2013, 2, 220–228. (In Russian) [Google Scholar]
- Chernykh, D.A.; Taseiko, O.V. Assessment of the Risk Mortality from Thermal Waves in Krasnoyarsk City. Hum. Ecol. 2018, 2, 3–8. (In Russian) [Google Scholar] [CrossRef][Green Version]
- Christidis, N.; Mitchell, D.; Stott, P.A. Anthropogenic climate change and heat effects on health. Int. J. Climatol. 2019, 39, 4751–4768. [Google Scholar] [CrossRef]
- Curtis, S.; Fair, A.; Wistow, J.; Val, D.V.; Oven, K. Impact of extreme weather events and climate change for health and social care systems. Environ. Health 2017, 16, 128. [Google Scholar] [CrossRef]
- De Sario, M.; Katsouyanni, K.; Michelozzi, P. Climate change, extreme weather events, air pollution and respiratory health in Europe. Eur. Respir. J. 2013, 42, 826–843. [Google Scholar] [CrossRef]
- Díaz, J.; Carmona, R.; Miron, I.; Ortiz, C.; Linares, C. Comparison of the effects of extreme temperatures on daily mortality in Madrid (Spain), by age group: The need for a cold wave prevention plan. Environ. Res. 2015, 143, 186–191. [Google Scholar] [CrossRef]
- Dimitriadou, L.; Nastos, P.; Zerefos, C. Defining Heatwaves with Respect to Human Biometeorology. The Case of Attica Region, Greece. Atmosphere 2021, 12, 1100. [Google Scholar] [CrossRef]
- Dole, R.; Hoerling, M.; Perlwitz, J.; Eischeid, J.; Pegion, P.; Zhang, T.; Quan, X.-W.; Xu, T.; Murray, D. Was there a basis for anticipating the 2010 Russian heat wave? Geophys. Res. Lett. 2011, 38, L06702. [Google Scholar] [CrossRef]
- Dong, J.; Peng, J.; He, X.; Corcoran, J.; Qiu, S.; Wang, X. Heatwave-induced human health risk assessment in megacities based on heat stress-social vulnerability-human exposure framework. Landsc. Urban Plan. 2020, 203, 103907. [Google Scholar] [CrossRef]
- Ebi, K.L.; Capon, A.; Berry, P.; Broderick, C.; de Dear, R.; Havenith, G.; Honda, Y.; Kovats, R.S.; Ma, W.; Malik, A.; et al. Hot weather and heat extremes: Health risks. Lancet 2021, 398, 698–708. [Google Scholar] [CrossRef]
- Eckstein, D.; Künzel, V.; Schäfer, L. Global Climate Risk Index. Who Suffers Most from Extreme Weather Events? Weather-Related Loss Events in 2019 and 2000–2019; Germanwatch: Bonn, Germany, 2021. [Google Scholar]
- Evstafeva, E.V.; Lapchenko, V.A.; Macarova, A.S.; Abibullaeva, N.K.; Evstafeva, I.A. Air Temperature and Ozone Concentration as Risk Factors for Life-Threatening Cardiovascular Conditions in Southern Russia. Hum. Ecol. 2020, 5, 50–56. [Google Scholar] [CrossRef]
- Forzieri, G.; Cescatti, A.; e Silva, F.B.; Feyen, L. Increasing risk over time of weather-related hazards to the European population: A data-driven prognostic study. Lancet Planet. Health 2017, 1, e200–e208. [Google Scholar] [CrossRef]
- Garganeeva, A.A.; Kuzheleva, E.A.; Gorbatenko, V.P.; Okrugin, S.A.; Kuzhevskaya, I.V. Specifics of development and course of acute coronary insufficiency during extreme heat weather conditions. Cardiovasc. Ther. Prev. 2017, 16, 52–56. [Google Scholar] [CrossRef]
- Gasparrini, A.; Guo, Y.; Hashizume, M.; Lavigne, E.; Zanobetti, A.; Schwartz, J.; Tobías, A.; Tong, S.; Rocklöv, J.; Forsberg, B.; et al. Mortality risk attributable to high and low ambient temperature: A multicountry observational study. Lancet 2015, 386, 369–375. [Google Scholar] [CrossRef]
- Grigorieva, E.A. Heat waves in Khabarovsk—Approaches to the definition. Reg. Probl. 2014, 17, 43–48. (In Russian) [Google Scholar]
- Grigorieva, E.A. Heat waves in the South of the Far East and human health. Newsl. Public Health Habitat 2017, 2, 11–14. (In Russian) [Google Scholar]
- Grigorieva, E. Cold waves: Approaches to definition and examples for Khabarovsk. Reg. Probl. 2019, 22, 24–37. [Google Scholar] [CrossRef]
- Grigorieva, E.A. Heat and cold waves in the South of the Russian Far East in 2000–2017. IOP Conf. Ser. Earth Environ. Sci. 2020, 606, 012016. [Google Scholar] [CrossRef]
- Grigorieva, E.; Lukyanets, A. Combined Effect of Heat Waves and Outdoor Air Pollution on Respiratory Health: Literature Review. Atmosphere 2021, 12, 790. [Google Scholar] [CrossRef]
- Guo, Y.; Gasparrini, A.; Armstrong, B.G.; Tawatsupa, B.; Tobías, A.; Lavigne, E.; Coelho, M.D.S.Z.S.; Pan, X.; Kim, H.; Hashizume, M.; et al. Heat Wave and Mortality: A Multicountry, Multicommunity Study. Environ. Health Perspect. 2017, 125, 087006. [Google Scholar] [CrossRef]
- Hajat, S.; Kovats, R.S.; Lachowycz, K. Heat-related and cold-related deaths in England and Wales: Who is at risk? Occup. Environ. Med. 2007, 64(2), 93–100. [Google Scholar] [CrossRef] [PubMed]
- Javadinejad, S.; Dara, R.; Jafary, F. Health impacts of extreme events. Saf. Extreme Environ. 2020, 2, 171–181. [Google Scholar] [CrossRef]
- Kendrovski, V.; Baccini, M.; Martinez, G.S.; Wolf, T.; Paunovic, E.; Menne, B. Quantifying Projected Heat Mortality Impacts under 21st-Century Warming Conditions for Selected European Countries. Int. J. Environ. Res. Public Health 2017, 14, 729. [Google Scholar] [CrossRef]
- Liu, J.C.; Pereira, G.; Uhl, S.A.; Bravo, M.A.; Bell, M.L. A systematic review of the physical health impacts from non-occupational exposure to wildfire smoke. Environ. Res. 2015, 136, 120–132. [Google Scholar] [CrossRef] [PubMed]
- Ma, F.; Yuan, X. Impact of climate and population changes on the increasing exposure to summertime compound hot extremes. Sci. Total. Environ. 2021, 772, 145004. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.; Zhou, J.; Yang, S.; Yu, Z.; Wang, F.; Zhou, J. Effects of extreme temperatures on hospital emergency room visits for respiratory diseases in Beijing, China. Environ. Sci. Pollut. Res. 2018, 26, 3055–3064. [Google Scholar] [CrossRef]
- Margolis, H.G. Heat Waves and Rising Temperatures: Human Health Impacts and the Determinants of Vulnerability. In Climate Change and Global Public Health. Respiratory Medicine; Pinkerton, K.E., Rom, W.N., Eds.; Humana: Cham, Switzerland, 2021; pp. 123–161. [Google Scholar] [CrossRef]
- McElroy, S.; Schwarz, L.; Green, H.; Corcos, I.; Guirguis, K.; Gershunov, A.; Benmarhnia, T. Defining heat waves and extreme heat events using sub-regional meteorological data to maximize benefits of early warning systems to population health. Sci. Total. Environ. 2020, 721, 137678. [Google Scholar] [CrossRef]
- McGregor, G.R.; Bessemoulin, R.; Ebi, K.; Menne, B. Heatwaves and Health: Guidance on Warning-System Development; World Meteorological Organization and World Health Organization: Geneva, Switzerland, 2015; p. 1142. Available online: http://bit.ly/2NbDx4S (accessed on 20 August 2021).
- Meierrieks, D. Weather shocks, climate change and human health. World Dev. 2021, 138, 105228. [Google Scholar] [CrossRef]
- Mücke, H.-G.; Litvinovitch, J.M. Heat Extremes, Public Health Impacts, and Adaptation Policy in Germany. Int. J. Environ. Res. Public Health 2020, 17, 7862. [Google Scholar] [CrossRef]
- Oppermann, E.; Kjellstrom, T.; Lemke, B.; Otto, M.; Lee, J.K.W. Establishing intensifying chronic exposure to extreme heat as a slow onset event with implications for health, wellbeing, productivity, society and economy. Curr. Opin. Environ. Sustain. 2021, 50, 225–235. [Google Scholar] [CrossRef]
- Otrachshenko, V.; Popova, O.; Solomin, P. Misfortunes never come singly: Consecutive weather shocks and mortality in Russia. Econ. Hum. Biol. 2018, 31, 249–258. [Google Scholar] [CrossRef]
- Otrachshenko, V.; Popova, O.; Tavares, J. Extreme Temperature and Extreme Violence: Evidence from Russia. Econ. Inq. 2021, 59, 243–262. [Google Scholar] [CrossRef]
- Patz, J.A.; Thomson, M.C. Climate change and health: Moving from theory to practice. PLoS Med. 2018, 15, e1002628. [Google Scholar] [CrossRef]
- Perkins, S.E.; Alexander, L. On the Measurement of Heat Waves. J. Clim. 2013, 26, 4500–4517. [Google Scholar] [CrossRef]
- Peters, A.; Schneider, A. Cardiovascular risks of climate change. Nat. Rev. Cardiol. 2021, 18, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Qiu, H.; Tian, L.; Ho, K.-F.; Yu, I.T.S.; Thach, T.-Q.; Wong, C.-M. Who is more vulnerable to death from extremely cold temperatures? A case-only approach in Hong Kong with a temperate climate. Int. J. Biometeorol. 2016, 60, 711–717. [Google Scholar] [CrossRef]
- Revich, B.A. Heat waves, atmospheric air quality and mortality in the European part of Russia in the summer of 2010: Results of a preliminary assessment. Hum. Ecol. 2011, 7, 3–9. (In Russian) [Google Scholar]
- Revich, B.A. Climatic risks to the health of residents of megacities of different climatic zones. In A Man in a Megalopolis. Experience of Interdisciplinary Research; Revich, B.A., Kuznetsova, O.V., Eds.; LENAND: Moscow, Russia, 2018; pp. 340–375. (In Russian) [Google Scholar]
- Revich, B.A.; Grigorieva, E.A. Health Risks to the Russian Population from Weather Extremes in the Beginning of the XXI Century. Part 1. Heat and Cold Waves. Issues Risk Anal. 2021, 18, 12–33. [Google Scholar] [CrossRef]
- Revich, B.A.; Shaposhnikov, D.A.; Pershagen, Y. A new epidemiological model for assessing the impact of abnormal heat and polluted atmospheric air on the mortality of the population (on the example of Moscow in 2010). Prev. Med. 2015, 5, 5–19. (In Russian) [Google Scholar]
- Revich, B.A.; Shaposhnikov, D.V.; Podolnaya, M.A.; Kharkova, T.L.; Kvasha, E.A. Heat waves in southern cities of the European part of Russia as a risk factor for premature mortality of the population. Stud. Russ. Econ. Dev. 2015, 2, 55–67. (In Russian) [Google Scholar]
- Revich, B.; Shaposhnikov, D. Influence features of cold and heat waves to the population mortality - the city with sharply continental climate. Sib. Med Rev. 2017, 2, 84–90. [Google Scholar] [CrossRef]
- Revich, B.A.; Shaposhnikov, D.A.; Anisimov, O.A.; Belolutskaya, M.A. Heat and cold waves in cities located in the Arctic and Subarctic zones as risk factors for increasing population mortality on the example of Arkhangelsk, Murmansk and Yakutsk. Hyg. Sanit. 2018, 9, 791–799. [Google Scholar] [CrossRef]
- Revich, B.A.; Shaposhnikov, D.A.; Anisimov, O.A.; Belolutskaya, M.A. Impact of Temperature Waves on the Health of Residents in Cities of the Northwestern Region of Russia. Stud. Russ. Econ. Dev. 2019, 30, 327–333. [Google Scholar] [CrossRef]
- Revich, B.A.; Shaposhnikov, D.A.; Shkolnik, I.M. Projections of temperature-dependent mortality In Russian subarctic under climate change scenarios: A longitudinal study across several climate zones. IOP Conf. Ser. Earth Environ. Sci. 2020, 606, 012050. [Google Scholar] [CrossRef]
- Robinson, P.J. On the definition of a heat wave. J. Appl. Meteorol. 2001, 40, 762–775. [Google Scholar] [CrossRef]
- Rom, W.N.; Pinkerton, K.E. Introduction: Consequences of Global Warming to Planetary and Human Health. In Climate Change and Global Public Health; Pinkerton, K.E., Rom, W.N., Eds.; Respiratory Medicine; Humana: Cham, Switzerland, 2021; pp. 1–33. [Google Scholar] [CrossRef]
- Rorie, A.; Poole, J.A. The Role of Extreme Weather and Climate-Related Events on Asthma Outcomes. Immunol. Allergy Clin. North Am. 2021, 41, 73–84. [Google Scholar] [CrossRef] [PubMed]
- Ryti, N.; Guo, Y.; Jaakkola, J.J. Global Association of Cold Spells and Adverse Health Effects: A Systematic Review and Meta-Analysis. Environ. Health Perspect. 2016, 124, 12–22. [Google Scholar] [CrossRef] [PubMed]
- Seltenrich, N. Between Extremes: Health Effects of Heat and Cold. Environ. Health Perspect. 2015, 123, A275–A280. [Google Scholar] [CrossRef] [PubMed]
- Shaposhnikov, D.; Revich, B. Towards meta-analysis of impacts of heat and cold waves on mortality In Russian North. Urban Clim. 2016, 15, 16–24. [Google Scholar] [CrossRef]
- Shaposhnikov, D.; Revich, B.; Bellander, T.; Bedada, G.B.; Bottai, M.; Kharkova, T.; Kvasha, E.; Lezina, E.; Lind, T.; Semutnikova, E.; et al. Mortality Related to Air Pollution with the Moscow Heat Wave and Wildfire of 2010. Epidemiology 2014, 25, 359–364. [Google Scholar] [CrossRef]
- Shartova, N.; Shaposhnikov, D.; Konstantinov, P.; Revich, B. Cardiovascular mortality during heat waves in temperate climate: An association with bioclimatic indices. Int. J. Environ. Health Res. 2018, 28, 522–534. [Google Scholar] [CrossRef]
- Shartova, N.V.; Shaposhnikov, D.A.; Konstantinov, P.I.; Revich, B.A. Bioclimatic approach to the assessment of population mortality during the heat wave on the example of the South of Russia. Bull. Mosc. Univ. Ser. 5 Geogr. 2018, 6, 47–55. (In Russian) [Google Scholar]
- Shartova, N.V.; Shaposhnikov, D.A.; Konstantinov, P.I.; Revich, B.A. Universal Thermal Climate Index (UTCI) applied to determine thresholds for temperature-related mortality. Health Risk Anal. 2019, 3, 83–93. [Google Scholar] [CrossRef]
- Sheridan, S.C.; Allen, M.J. Changes in the Frequency and Intensity of Extreme Temperature Events and Human Health Concerns. Curr. Clim. Chang. Rep. 2015, 1, 155–162. [Google Scholar] [CrossRef]
- Smirnova, M.; Gorbunov, V.; Andreeva, G. The influence of seasonal meteorological factors on the morbidity and mortality of the population from cardiovascular and bronchopulmonary diseases. Prev. Med. 2012, 15, 76–86. (In Russian) [Google Scholar]
- Smirnova, M.D.; Ageev, F.T.; Svirida, O.N.; Konovalova, G.G.; Tikhaze, A.K.; Lankin, V.Z. Influence of summer heat on the health status of patients with moderate and high risk of cardiovascular complications. Cardiovasc. Ther. Prev. 2013, 12, 56–61. [Google Scholar] [CrossRef][Green Version]
- Smirnova, M.D.; Fofanova, T.V.; Yarovaya, E.B.; Ageev, F.T. Prognostic factors of cardiovascular complications during the 2010 heat wave (cohort observational study). Cardiol. Bull. 2016, 1, 43–51. (In Russian) [Google Scholar]
- Smith, E.T.; Sheridan, S.C. The influence of extreme cold events on mortality in the United States. Sci. Total. Environ. 2019, 647, 342–351. [Google Scholar] [CrossRef]
- Song, J.; Pan, R.; Yi, W.; Wei, Q.; Qin, W.; Song, S.; Tang, C.; He, Y.; Liu, X.; Cheng, J.; et al. Ambient high temperature exposure and global disease burden during 1990–2019: An analysis of the Global Burden of Disease Study 2019. Sci. Total. Environ. 2021, 787, 147540. [Google Scholar] [CrossRef] [PubMed]
- Tong, S.L.; Olsen, J.; Kinney, P.L. Climate Change and Temperature-related Mortality: Implications for Health-related Climate Policy. Biomed. Environ. Sci. 2021, 34, 379–386. [Google Scholar]
- Toulemon, L.; Barbieri, M. The mortality impact of the August 2003 heat wave in France: Investigating the ‘harvesting’ effect and other long-term consequences. Popul. Stud. 2008, 62, 39–53. [Google Scholar] [CrossRef]
- Vanos, J.K.; Baldwin, J.W.; Jay, O.; Ebi, K.L. Simplicity lacks robustness when projecting heat-health outcomes in a changing climate. Nat. Commun. 2020, 11, 6079. [Google Scholar] [CrossRef]
- Vanos, J.; Moyce, S.; Lemke, B.; Kjellstrom, T. Extreme Heat Exposure and Occupational Health in a Changing Climate. In Extreme Events and Climate Change; Castillo, F., Wehner, M., Stone, D.A., Eds.; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2021. [Google Scholar] [CrossRef]
- Vicedo-Cabrera, A.M.; Scovronick, N.; Sera, F.; Royé, D.; Schneider, R.; Tobias, A.; Astrom, C.; Guo, Y.; Honda, Y.; Hondula, D.M.; et al. The burden of heat-related mortality attributable to recent human-induced climate change. Nat. Clim. Chang. 2021, 11, 492–500. [Google Scholar] [CrossRef]
- Wang, Y.; Shi, L.; Zanobetti, A.; Schwartz, J.D. Estimating and projecting the effect of cold waves on mortality in 209 US cities. Environ. Int. 2016, 94, 141–149. [Google Scholar] [CrossRef] [PubMed]
- Watts, N.; Amann, M.; Arnell, N.; Ayeb-Karlsson, S.; Beagley, J.; Belesova, K.; Boykoff, M.; Byass, P.; Cai, W.; Campbell-Lendrum, D.; et al. The 2020 report of The Lancet Countdown on health and climate change: Responding to converging crises. Lancet 2021, 397, 129–170. [Google Scholar] [CrossRef]
- Weilnhammer, V.; Schmid, J.; Mittermeier, I.; Schreiber, F.; Jiang, L.; Pastuhovic, V.; Herr, C.; Heinze, S. Extreme weather events in europe and their health consequences—A systematic review. Int. J. Hyg. Environ. Health 2021, 233, 113688. [Google Scholar] [CrossRef]
- Young, J.; Arthur, R.; Spruce, M.; Williams, H. Social Sensing of Heatwaves. Sensors 2021, 21, 3717. [Google Scholar] [CrossRef]
- Zemtsov, S.P.; Shartova, N.V.; Konstantinov, P.I.; Varentsov, M.I.; Kidyaeva, V.M. Vulnerability of the population of Moscow districts to natural hazards. Vestn. Mosk. Univ. Ser. 5 Geogr. 2020, 4, 3–13. (In Russian) [Google Scholar]
- Zemtsov, S.; Shartova, N.; Varentsov, M.; Konstantinov, P.; Kidyaeva, V.; Shchur, A.; Timonin, S.; Grischchenko, M. Intraurban social risk and mortality patterns during extreme heat events: A case study of Moscow, 2010-2017. Health Place 2020, 66, 102429. [Google Scholar] [CrossRef]
- Berry, H.L.; Bowen, K.; Kjellstrom, T. Climate change and mental health: A causal pathways framework. Int. J. Public Health 2010, 55, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Doherty, T.J.; Clayton, S. The psychological impacts of global climate change. Am. Psychol. 2011, 66, 265–276. [Google Scholar] [CrossRef]
- Ioannou, L.; Mantzios, K.; Tsoutsoubi, L.; Panagiotaki, Z.; Kapnia, A.; Ciuha, U.; Nybo, L.; Flouris, A.; Mekjavic, I. Effect of a Simulated Heat Wave on Physiological Strain and Labour Productivity. Int. J. Environ. Res. Public Health 2021, 18, 3011. [Google Scholar] [CrossRef]
- Liu, J.; Varghese, B.M.; Hansen, A.; Xiang, J.; Zhang, Y.; Dear, K.; Gourley, M.; Driscoll, T.; Morgan, G.; Capon, A.; et al. Is there an association between hot weather and poor mental health outcomes? A systematic review and meta-analysis. Environ. Int. 2021, 153, 106533. [Google Scholar] [CrossRef]
- Page, L.A.; Hajat, S.; Kovats, R.S.; Howard, L.M. Temperature-related deaths in people with psychosis, dementia and substance misuse. Br. J. Psychiatry 2012, 200, 485–490. [Google Scholar] [CrossRef] [PubMed]
- Thompson, R.; Hornigold, R.; Page, L.; Waite, T. Associations between high ambient temperatures and heat waves with mental health outcomes: A systematic review. Public Health 2018, 161, 171–191. [Google Scholar] [CrossRef] [PubMed]
- Yoo, E.-H.; Eum, Y.; Roberts, J.E.; Gao, Q.; Chen, K. Association between extreme temperatures and emergency room visits related to mental disorders: A multi-region time-series study in New York, USA. Sci. Total. Environ. 2021, 792, 148246. [Google Scholar] [CrossRef] [PubMed]
- Yoo, E.-H.; Eum, Y.; Gao, Q.; Chen, K. Effect of extreme temperatures on daily emergency room visits for mental disorders. Environ. Sci. Pollut. Res. 2021, 28, 39243–39256. [Google Scholar] [CrossRef] [PubMed]
- Rameshshanker, V.; Wyngaarden, S.; Lau, L.L.; Dodd, W. Health system resilience to extreme weather events in Asia-Pacific: A scoping review. Clim. Dev. 2021, 1–15. [Google Scholar] [CrossRef]
- Matsueda, M. Predictability of Euro-Russian blocking in summer of 2010. Geophys. Res. Lett. 2011, 38, L06801. [Google Scholar] [CrossRef]
- Friedman, L.S.; Abasilim, C.; Fitts, R.; Wueste, M. Clinical outcomes of temperature related injuries treated in the hospital setting, 2011–2018. Environ. Res. 2020, 189, 109882. [Google Scholar] [CrossRef]
- Sera, F.; Armstrong, B.; Tobias, A.; Cabrera, A.M.V.; Åström, C.; Bell, M.L.; Chen, B.-Y.; Coelho, M.D.S.Z.S.; Correa, P.M.; Cruz, J.C.; et al. How urban characteristics affect vulnerability to heat and cold: A multi-country analysis. Int. J. Epidemiol. 2019, 48, 1101–1112. [Google Scholar] [CrossRef]
- Zheng, S.; Zhu, W.; Shi, Q.; Wang, M.; Nie, Y.; Zhang, D.; Cheng, Z.; Yin, C.; Miao, Q.; Luo, Y.; et al. Effects of cold and hot temperature on metabolic indicators in adults from a prospective cohort study. Sci. Total. Environ. 2021, 772, 145046. [Google Scholar] [CrossRef]
- Bedritsky, A.I. (Ed.) Russian Hydrometeorological Encyclopedia; Letnii Sad SPB: Moscow, Russia, 2008; Volume 1, 336p. (In Russian) [Google Scholar]
- Kleshchenko, L.K. Heat and cold waves on the territory of Russia. Trudy GU VNIIGMI MTsD 2010, 175, 76–79. (In Russian) [Google Scholar]
- Vinogradova, V.V. Winter cold waves on the territory of Russia since the second half of the twentieth century. Izv. Ross. Akad. Nauk. Ser. Geogr. 2018, 3, 37–46. (In Russian) [Google Scholar] [CrossRef]
- Shaposhnikov, D.A.; Revich, B.A. On some approaches to calculating the health risks of temperature waves. Health Risk Anal. 2018, 1, 22–31. [Google Scholar] [CrossRef]
- Roshydromet. RD 52.88699-2008. Regulation on the Procedure of Actions of Institutions and Organizations in the Event of a Threat of Dangerous Natural Processes; Roshydromet: Moscow, Russia, 2008. (In Russian) [Google Scholar]
- Radinović, D.; Ćurić, M. Criteria for heat and cold wave duration indexes. Theor. Appl. Climatol. 2011, 107, 505–510. [Google Scholar] [CrossRef]
- Rocklov, J.; Barnett, A.G.; Woodward, A. On the estimation of heat-intensity and heat-duration effects in time series models of temperature-related mortality in Stockholm, Sweden. Environ. Health 2012, 11, 23. [Google Scholar] [CrossRef] [PubMed]
- De Freitas, C.R.; Grigorieva, E.A. The impact of acclimatization on thermophysiological strain for contrasting regional climates. Int. J. Biometeorol. 2014, 58, 2129–2137. [Google Scholar] [CrossRef] [PubMed]
- De Freitas, C.R.; Grigorieva, E.A. Role of Acclimatization in Weather-Related Human Mortality During the Transition Seasons of Autumn and Spring in a Thermally Extreme Mid-Latitude Continental Climate. Int. J. Environ. Res. Public Health 2015, 12, 14974–14987. [Google Scholar] [CrossRef] [PubMed]
- Fatima, S.H.; Rothmore, P.; Giles, L.C.; Varghese, B.M.; Bi, P. Extreme heat and occupational injuries in different climate zones: A systematic review and meta-analysis of epidemiological evidence. Environ. Int. 2021, 148, 106384. [Google Scholar] [CrossRef]
- Foster, J.; Hodder, S.G.; Lloyd, A.B.; Havenith, G. Individual Responses to Heat Stress: Implications for Hyperthermia and Physical Work Capacity. Front. Physiol. 2020, 11, 541483. [Google Scholar] [CrossRef]
- Jay, O.; Capon, A.; Berry, P.; Broderick, C.; de Dear, R.; Havenith, G.; Honda, Y.; Kovats, R.S.; Ma, W.; Malik, A.; et al. Reducing the health effects of hot weather and heat extremes: From personal cooling strategies to green cities. Lancet 2021, 398, 709–724. [Google Scholar] [CrossRef]
- Mücke, H.-G.; Matzarakis, A. Climate Change and Health. Tips on Coping with Hot Weather and Heat Waves; Umweltbundesamt: Vienna, Austria, 2020; 20p, Available online: https://www.umweltbundesamt.de/en/publikationen/climate-change-health-tips-on-coping-hot-weather (accessed on 20 August 2021).
- Taylor, N.A.S.; Notley, S.R.; Lindinger, M.I. Heat adaptation in humans: Extrapolating from basic to applied science. Eur. J. Appl. Physiol. 2021, 121, 1237–1238. [Google Scholar] [CrossRef]
- Zafeiratou, S.; Samoli, E.; Dimakopoulou, K.; Rodopoulou, S.; Analitis, A.; Gasparrini, A.; Stafoggia, M.; Donato, F.D.; Rao, S.; Monteiro, A.; et al. A systematic review on the association between total and cardiopulmonary mortality/morbidity or cardiovascular risk factors with long-term exposure to increased or decreased ambient temperature. Sci. Total. Environ. 2021, 772, 145383. [Google Scholar] [CrossRef]
- Marselle, M.R.; Hartig, T.; Cox, D.T.; de Bell, S.; Knapp, S.; Lindley, S.; Triguero-Mas, M.; Böhning-Gaese, K.; Braubach, M.; Cook, P.A.; et al. Pathways linking biodiversity to human health: A conceptual framework. Environ. Int. 2021, 150, 106420. [Google Scholar] [CrossRef]
- Wang, Q.; Zhang, Y.; Ban, J.; Zhu, H.; Xu, H.; Li, T. The relationship between population heat vulnerability and urbanization levels: A county-level modeling study across China. Environ. Int. 2021, 156, 106742. [Google Scholar] [CrossRef]
- Bocharov, M.I. Physiological Problems of Protection From Cold; SSU: Syktyvkar, Russia, 2004; 40p. (In Russian) [Google Scholar]
- Coccarelli, A.; Hasan, H.M.; Carson, J.; Parthimos, D.; Nithiarasu, P. Influence of ageing on human body blood flow and heat transfer: A detailed computational modelling study. Int. J. Numer. Methods Biomed. Eng. 2018, 34, e3120. [Google Scholar] [CrossRef] [PubMed]
- Grishin, O.V.; Ustyuzhaninova, N.V. Breath in the North. Function. Structure. Reserves. Pathology; Artavenyu: Novosibirsk, Russia, 2006; 253p. (In Russian) [Google Scholar]
- Kozyreva, T.V. Adaptation to cold of homeothermic organism: Changes in afferent and efferent links of the thermoregulatory system. J. Exp. Integr. Med. 2013, 3, 255–265. [Google Scholar] [CrossRef]
- Nagornev, S.N.; Khudov, V.V.; Bobrovnitsky, I.P. Epidemiology of non-communicable diseases associated with adverse environmental impact and human activity in the Arctic. Russ. J. Restor. Med. 2019, 4, 3–37. (In Russian) [Google Scholar]
- Rakhmanov, R.S.; Kolesov, S.A.; Alikberov, M.K.; Potekhina, N.N.; Belousko, N.I.; Tarasov, A.V.; Nepryakhin, D.V.; Zhargalov, S.I. On the issue of health risk under the influence of weather and climatic conditions in the cold period of the year for workers. Health Risk Anal. 2018, 2, 70–77. [Google Scholar] [CrossRef][Green Version]
- Wu, J.; Hu, Z.; Han, Z.; Gu, Y.; Yang, L.; Sun, B. Human physiological responses of exposure to extremely cold environments. J. Therm. Biol. 2021, 98, 102933. [Google Scholar] [CrossRef]
- Kuzmin, S.B. Natural disasters in the Russian Federation. Issues Risk Anal. 2019, 16, 10–35. [Google Scholar] [CrossRef]
- Zolotokrylin, A.N.; Vinogradova, V.V.; Glezer, O.B. (Eds.) Natural and Climatic Conditions and Sociogeographical Space of Russia; Institute of Geography RAS: Moscow, Russia, 2018; 154p. (In Russian) [Google Scholar]
- The Global Risks Report 2020, 15th Edition. Available online: http://www3.weforum.org/docs/WEF%20Global%20Risk%20Report%202020.pdf (accessed on 20 August 2021).
- Roshydromet. Report on the Peculiarities of the Climate on the Territory of the Russian Federation for 2018; Roshydromet: Moscow, Russia, 2019; 79p. [Google Scholar]
- Roshydromet. The Second Assessment Report of Roshydromet on Climate Change and its Consequences on the Territory of the Russian Federation; Roshydromet: Moscow, Russia, 2014. (In Russian) [Google Scholar]
- Overland, J.E.; Wang, M. The 2020 Siberian heat wave. Int. J. Climatol. 2021, 41 (Suppl. 1), E2341–E2346. [Google Scholar] [CrossRef]
- COPERNICUS Wildfires. 2020. Available online: https://atmosphere.copernicus.eu/another-active-year-arctic-wildfires (accessed on 20 August 2021).
- Grishkin, D. Russia’s Record-Breaking Heatwave to Continue Into July—Weather Service. Moscow Times, 24 June 2021. Available online: https://www.themoscowtimes.com/2021/06/24/russias-record-breaking-heatwave-to-continue-into-july-weather-service-a74319 (accessed on 20 August 2021).
- Hayes, K. Wildfire smoke Reaches North Pole for 1st Time in Recorded History. FOX TV Digital Team, 13 August 2021. Available online: https://www.fox35orlando.com/news/wildfire-smoke-reaches-north-pole-for-1st-time-in-recorded-history (accessed on 31 August 2021).
- Titkova, T.B.; Cherenkova, E.A.; Semenov, V.A. Regional features of changes in winter extreme temperatures and precipitation in Russia in 1970–2015. Ice Snow 2018, 58, 486–497. [Google Scholar] [CrossRef]
- Bardin, M.Y.; Platova, T.V. Changes in seasonal indicators of air temperature extremes in Moscow and the central regions of the European part of Russia. Meteorol. Hydrol. 2020, 7, 20–35. (In Russian) [Google Scholar]
- Shaposhnikov, D.A.; Revich, B.A.; Shkolnik, I.M. Scenario estimates of climate warming and mortality In Russian Arctic cities in the XXI century. Health Risk Anal. 2019, 4, 37–49. [Google Scholar] [CrossRef]
- Federal Center for Hygiene and Epidemiology of Rospotrebnadzor. Assessment of the Risk and Damage from Climate Change Affecting the Increase in Morbidity and Mortality in High-Risk Populations: Methodological Recommendations MR 2.1.10.0057-12; Federal Center for Hygiene and Epidemiology of Rospotrebnadzor: Moscow, Russia, 2012; 48p. (In Russian) [Google Scholar]
- De Freitas, C.R.; Grigorieva, E.A. A comprehensive catalogue and classification of human thermal climate indices. Int. J. Biometeorol. 2015, 59, 109–120. [Google Scholar] [CrossRef] [PubMed]
- De Freitas, C.R.; Grigorieva, E.A. A comparison and appraisal of a comprehensive range of human thermal climate indices. Int. J. Biometeorol. 2017, 61, 487–512. [Google Scholar] [CrossRef]
- Osczevski, R.J. The Basis of Wind Chill. Arctic 1995, 48, 372–382. [Google Scholar] [CrossRef]
- Masterson, J.; Richardson, F.A. Humidex, a Method of Quantifying Human Discomfort Due to Excessive Heat and Humidity; Environment Canada: Downsview, ON, Canada, 1979; 45p. [Google Scholar]
- Steadman, R.G. A universal scale of apparent temperature. J. Clim. Appl. Meteorol. 1984, 23, 1674–1687. [Google Scholar] [CrossRef]
- Matzarakis, A.; Mayer, H.; Iziomon, M. Applications of a universal thermal index: Physiological equivalent temperature. Int. J. Biometeorol. 1999, 43, 76–84. [Google Scholar] [CrossRef] [PubMed]
- Broede, P.; Fiala, D.; Blazejczyk, K.; Holmér, I.; Jendritzky, G.; Kampmann, B.; Tinz, B.; Havenith, G. Deriving the operational procedure for the Universal Thermal Climate Index (UTCI). Int. J. Biometeorol. 2012, 56, 481–494. [Google Scholar] [CrossRef]
- Peel, M.C.; Finlayson, B.L.; McMahon, T.A. Updated world map of the Köppen–Geiger climate classification. Hydrol. Earth Syst. Sci. 2007, 11, 1633–1644. [Google Scholar] [CrossRef]
- Sedov, V.E. On climate fluctuations and climate trends in modern Moscow. Meteorol. Hydrol. 2012, 8, 47–58. (In Russian) [Google Scholar] [CrossRef]
- Isaev, A.A. Ecological Climatology: Monograph; Nauch. Mir: Moscow, Russia, 2003; 470p. (In Russian) [Google Scholar]
- Kislov, A.V.; Konstantinov, P.I. Detailed spatial modeling of the temperature of the Moscow megapolis. Meteorol. Hydrol. 2011, 5, 25–32. (In Russian) [Google Scholar]
- Porfiriev, B.N. Economic assessment of human losses as a result of emergency situations. Econ. Iss. 2013, 1, 46–68. (In Russian) [Google Scholar]
- Climate Strategy of St. Petersburg. Project. 2016. Available online: http://www.gov.spb.ru/static/writable/ckeditor/01_klim_str_roject.doc (accessed on 20 August 2021).
- Grigorieva, E.A.; Khristoforova, N.K. Climate and Human Health at the Russian Far East. Ekol. Cheloveka 2019, 5, 4–10. [Google Scholar] [CrossRef]
- Gilbert, N. Russia Counts Environmental Cost of Wildfires. Nat. News. 12 August 2010. Available online: https://www.nature.com/articles/news.2010.404 (accessed on 20 August 2021).
- Konovalov, I.B.; Beekmann, M.; Kuznetsova, I.N.; Yurova, A.; Zvyagintsev, A.M. Atmospheric impacts of the 2010 Russian wildfires: Integrating modelling and measurements of an extreme air pollution episode in the Moscow region. Atmospheric Chem. Phys. Discuss. 2011, 11, 10031–10056. [Google Scholar] [CrossRef]
- Jalava, P.I.; Salonen, R.O.; Hälinen, A.I.; Penttinen, P.; Pennanen, A.; Sillanpää, M.; Sandell, E.; Hillamo, R.; Hirvonen, M.-R. In vitro inflammatory and cytotoxic effects of size-segregated particulate samples collected during long-range transport of wildfire smoke to Helsinki. Toxicol. Appl. Pharmacol. 2006, 215, 341–353. [Google Scholar] [CrossRef]
- Finlay, S.E.; Moffat, A.; Gazzard, R.; Baker, D.; Murray, V. Health Impacts of Wildfires. PLoS Curr. 2012, 4, e4f959951cce2c. [Google Scholar] [CrossRef]
- McClymont, H.; Hu, W. Weather Variability and COVID-19 Transmission: A Review of Recent Research. Int. J. Environ. Res. Public Health 2021, 18, 396. [Google Scholar] [CrossRef]
- Bose-O’Reilly, S.; Daanen, H.; Deering, K.; Gerrett, N.; Huynen, M.M.T.E.; Lee, J.; Karrasch, S.; Matthies-Wiesler, F.; Mertes, H.; Schoierer, J.; et al. COVID-19 and heat waves: New challenges for healthcare systems. Environ. Res. 2021, 198, 111153. [Google Scholar] [CrossRef]
- Martinez, G.; Linares, C.; De’Donato, F.; Diaz, J. Protect the vulnerable from extreme heat during the COVID-19 pandemic. Environ. Res. 2020, 187, 109684. [Google Scholar] [CrossRef]
- Wilhelmi, O.V.; Howe, P.D.; Hayden, M.H.; O’Lenick, C.R. Compounding hazards and intersecting vulnerabilities: Experiences and responses to extreme heat during COVID-19. Environ. Res. Lett. 2021, 16, 084060. [Google Scholar] [CrossRef]
- Revich, B.A.; Shaposhnikov, D.A. The COVID-19 Pandemic: New Knowledge on the Impact of Air Quality on the Spread of Coronavirus Infection in Cities. Stud. Russ. Econ. Dev. 2021, 32, 357–363. [Google Scholar] [CrossRef]
- Oke, T.R. The energetic basis of the urban heat island. Q. J. R. Meteorol. Soc. 1982, 108, 1–24. [Google Scholar] [CrossRef]
- Wimalasena, N.; Chang-Richards, A.; Wang, K.; Dirks, K. Housing Risk Factors Associated with Respiratory Disease: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 2815. [Google Scholar] [CrossRef]
- Ehsan, S.; Abbas, F.; Ibrahim, M.; Ahmad, B.; Farooque, A. Thermal Discomfort Levels, Building Design Concepts, and Some Heat Mitigation Strategies in Low-Income Communities of a South Asian City. Int. J. Environ. Res. Public Health 2021, 18, 2535. [Google Scholar] [CrossRef]
- Grigorieva, E. Bioclimate and urban design for sustainable development. In Water Management and Water Protection, Soil Consumption, Natural Capital Defense and Urban Growth; Proceedings of the Lugano HLRT Symposium 2019 by Water Academy SRD; Water Academy SRD: Lugano, Switzerland, 2020; pp. 99–107. [Google Scholar]
- Ermolaeva, P.; Ermolaeva, Y.; Basheva, O.; Kuznetsova, I.; Korunova, V. The Russian Urban Sustainability Puzzle: How Can Russian Cities Be Green? (Emerald Points); Emerald Group Publishing Ltd.: Bingley, UK, 2021. [Google Scholar] [CrossRef]
- Casanueva, A.; Burgstall, A.; Kotlarski, S.; Messeri, A.; Morabito, M.; Flouris, A.D.; Nybo, L.; Spirig, C.; Schwierz, C. Overview of Existing Heat-Health Warning Systems in Europe. Int. J. Environ. Res. Public Health 2019, 16, 2657. [Google Scholar] [CrossRef]
- Pascal, M.; Laaidi, K.; Ledrans, M.; Baffert, E.; Caserio-Schönemann, C.; Le Tertre, A.; Manach, J.; Medina, S.; Rudant, J.; Empereur-Bissonnet, P. France’s heat health watch warning system. Int. J. Biometeorol. 2005, 50, 144–153. [Google Scholar] [CrossRef]
- Rivin, G.S.; Rozinkina, I.A.; Vil’fand, R.M.; Kiktev, D.B.; Tudrii, K.O.; Blinov, D.V.; Artamonov, A.Y. Development of the High-resolution Operational System for Numerical Prediction of Weather and Severe Weather Events for the Moscow Region. Russ. Meteorol. Hydrol. 2020, 45, 455–465. [Google Scholar] [CrossRef]
- Toloo, G.; Fitzgerald, G.; Aitken, P.; Verrall, K.; Tong, S. Evaluating the effectiveness of heat warning systems: Systematic review of epidemiological evidence. Int. J. Public Health 2013, 58, 667–681. [Google Scholar] [CrossRef] [PubMed]
- Chalabi, Z.; Hajat, S.; Wilkinson, P.; Erens, B.; Jones, L.; Mays, N. Evaluation of the cold weather plan for England: Modelling of cost-effectiveness. Public Health 2016, 137, 13–19. [Google Scholar] [CrossRef] [PubMed]
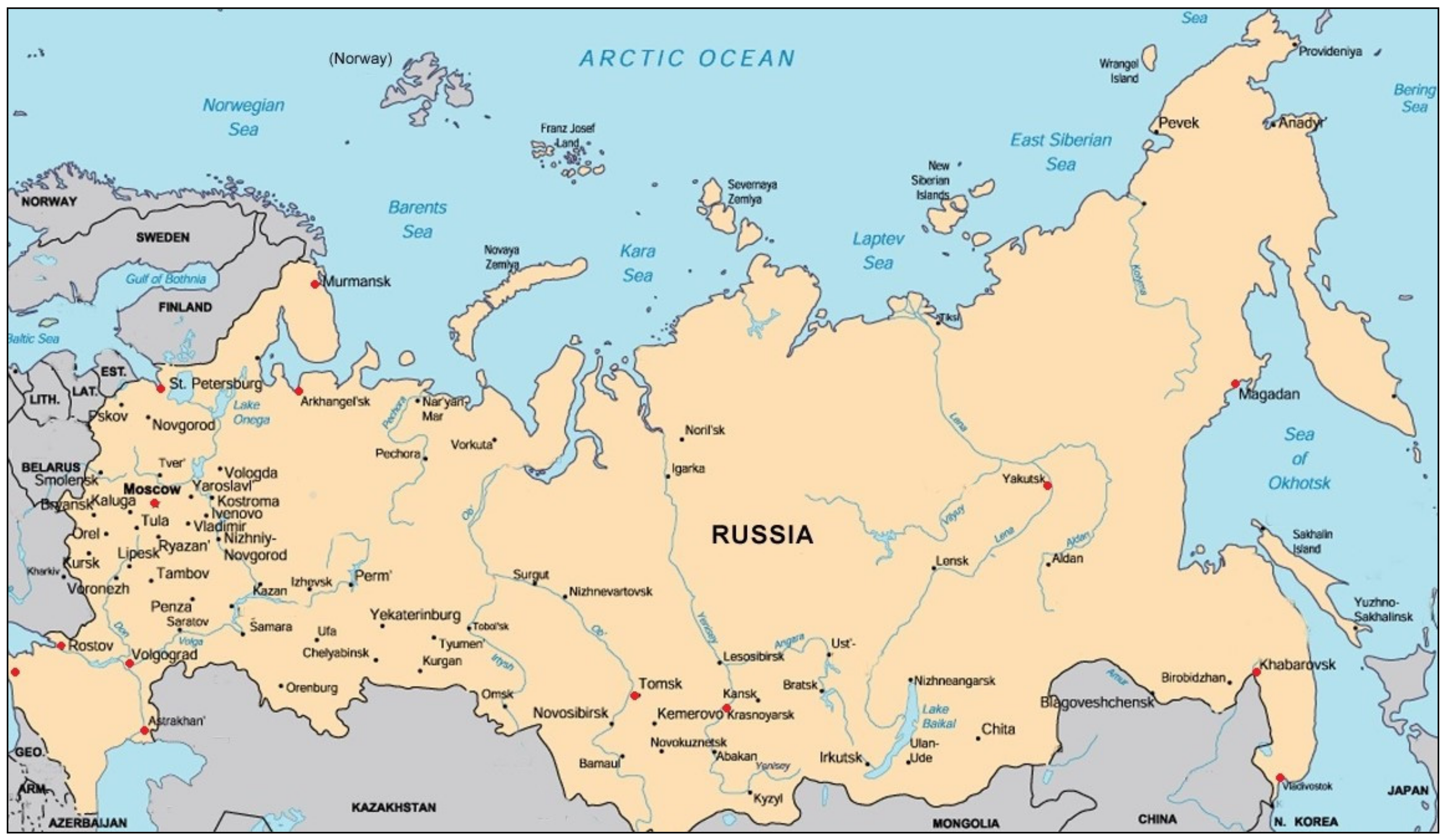
| Weather Station Name | WMO Station Number | Latitude, °N | Longitude, °E | Altitude, m above Sea Level | Climate Classification [186] | |
|---|---|---|---|---|---|---|
| 1. | Murmansk | 22,113 | 68°58′ | 33°03′ | 57 | Dfc (Continental Subarctic) |
| 2. | Arkhangelsk | 22,550 | 64°30′ | 40°44′ | 8 | Dfc (Continental Subarctic) |
| 3. | Yakutsk | 24,959 | 62°01′ | 129°43′ | 98 | Dfd (Extremely cold Continental Subarctic) |
| 4. | Magadan | 25,913 | 59°33′ | 150°47′ | 115 | Dfc (Continental Subarctic) |
| 5. | Saint Petersburg | 26,063 | 59°58′ | 30°18′ | 3 | Dfb (Warm Summer Humid Continental) |
| 6. | Moscow | 27,612 | 55°50′ | 37°37′ | 147 | Dfb (Warm Summer Continental) |
| 7. | Tomsk | 29,430 | 56°30′ | 84°55′ | 141 | Dfb (Warm Summer Continental) |
| 8. | Krasnoyarsk | 29,570 | 56°02′ | 92°45′ | 277 | Dfc (Continental Subarctic) |
| 9. | Khabarovsk | 31,735 | 48°31′ | 135°10′ | 75 | Dwb/Dwa (Monsoon-influenced warm/hot summer humid Continental) |
| 10. | Vladivostok | 31,960 | 43°48′ | 131°56′ | 187 | Dwb (Monsoon-influenced warm summer humid Continental) |
| 11. | Volgograd | 34,561 | 48°40′ | 44°27′ | 118 | Dfa (Hot Summer Continental) |
| 12. | Rostov-on-Don | 34,730 | 47°15′ | 39°49′ | 88 | Dfa (Hot Summer Continental) |
| 13. | Astrakhan | 34,880 | 46°17′ | 47°59′ | 22 | BSk (Cold semi-arid Steppe) |
| 14. | Krasnodar | 34,929 | 45°03′ | 39°02′ | 28 | Cfa (Humid Subtropical) |
| Study | Study Area | Study Period | Threshold Temperature 1 | Hot Weather Description 2 | Results 3 |
|---|---|---|---|---|---|
| Heat waves | |||||
| Boytsov et al. [49] | Moscow | 2007–2014 | Daily T, Tmax | HW: Tmax ≥ 28 °C, duration 4 days and more | Increase in all-cause mortality: RR = 1.43% (95% CI: 1.41–1.45); CVD = 1.65% (95% CI: 1.62–1.67) |
| Chereshnev et al. [54] | Moscow | 2006–2011 | Daily T | HW in 2010 | Increase in ambulance calls during HW in 2010 compared to summer 2009: for stroke, hypotension, angina—up to 2.5 times, for pneumonia—up to 5 times |
| Chernykh, Taseiko [55] | Krasnoyarsk | 2000–2004, 2010–2014 | Daily T | HW: T > 97th percentile of the year-round distribution during the study period, duration >5 days | Absolute risk of increase mortality: CVD (elderly) = 4.4 * 10−3; RD (30–64 year old) = 3.1 * 10−4; ED (30–64) = 1.63 * 10−3 |
| Garganeeva et al. [67] | Tomsk | Summer of 2010 and 2012 | Daily T | HW: T ≥ μ + 1.25σ (reference period 1990–2015), duration 5 days and more | Increase in total mortality among patients with AMI; increase in percentage of women and elderly in structure of AMI patients during the heat wave of 2012 compared to summer 2010 |
| Grigorieva [70] | Khabarovsk | 2000–2015 | Daily T | HW: T > 95th percentile of the year-round distribution during the study period, duration >3 days | Increase in all-cause mortality by 36% with one day lag |
| Revich [94] | Moscow | 2000–2012 | Daily T | HW: T > 97th percentile of the year-round distribution during the study period, duration >5 days | 30–64 years old: CVD RR = 1.20 (95% CI: 1.13–1.27), ED = 1.13% (95% CI: 1.09–1.19), NA = 1.02% (95% CI: 1.00–1.04);≥ 65 years old: IHD = 1.12 (95% CI: 1.10–1.14), CVD = 1.28 (95% CI: 1.24–1.31), RD = 1.19 (95% CI: 1.09–1.31), NA = 1.15% (95% CI: 1.13–1.16) |
| Revich [94] | Vladivostok | 2000–2015 | Daily T, AT | HW: T > 97th percentile of the year-round distribution during the study period, duration >5 days | IHD (30–64 years old) RR = 1.17% (95% CI: 1.00–1.37), RD (30–64) = 1.57% (95% CI: 1.18– 2.08), ED (30–64) = 1.22 % (95% CI: 1.02–1.47), NA (≥65) = 1.08% (95% CI: 1.01–1.16) |
| Revich et all. [97] | Astrakhan, Volgograd, Krasnodar, Rostov–on–Don | 2000–2010 | Daily T | HW: T > μ + 2σ (reference period 1961–2010), duration >5 days | Increase in all-cause mortality: Astrakhan RR = 10.8% (95% CI: 9.3–12.2); Krasnodar = 8.5% (95% CI: 7.5–9.6); Rostov–on–Don = 8.1% (95% CI: 7.2–8.9); Volgograd = 7.6% (95% CI: 6.7–8.5) |
| Revich, Shaposhnikov [98] | Krasnoyarsk | 1999–2015 | Daily T, AT | HW: T > 97th percentile of the year-round distribution during the study period, duration >5 days | Increase in NA (30–64 year old) RR = 1.095, (elderly) = 1.22; hypertension (elderly) = 1.84, strokes (elderly) = 1.44 |
| Revich et al. [99] | Northern cities Arkhangelsk, Murmansk, Yakutsk | 1999–2016 | Daily T, AT | HW: T (AT) > 97th percentile of the year-round distribution during the study period, duration >5 days | Increase in mortality, Arkhangelsk, T as predictor, IHD RR = 1.14% (95% CI: 1.01–1.29), CVD = 1.27% (95% CI: 1.11–1.43) Murmansk, T as predictor, IHD = 1.01% (95% CI: 0.79–1.28), AT as predictor CVD = 1.31% (95% CI: 1.05–1.64) Yakutsk, AT as predictor, IHD = 1.12% (95% CI: 0.92–1.36); T as predictor, CVD = 1.61% (95% CI: 1.27–2.03) |
| Revich et al. [100] | St-Petersburg | 1999–2016 | Daily T, AT | HW: T (AT) > 97th percentile of the year-round distribution during period from 1961 to 2017, duration >5 days | T as predictor: RD (≥65) RR = 1.19% (95% CI: 1.01–1.40) |
| Revich et al. [100] | St-Petersburg | Summer 2010 | Daily T, AT | HW: T (AT) > 97th percentile of the year-round distribution for the period from 1961 to 2017; duration >5 days | AT as predictor: RD (≥65 years old) RR = 1.34% (95% CI: 1.08–1.68); NA (≥65) = 1.26% (95% CI: 1.22–1.30) Increase in all-cause mortality in 2010 by 30.2% compared to the summer of 2009 |
| Shaposhnikov, Revich [107] | Northern cities Arkhangelsk, Magadan, Murmansk, Yakutsk | 1999–2007 | Daily T | HW: T > 97th percentile of the year-round distribution during the study period, duration >5 days | Arkhangelsk (30–64 years old) RR = 1.02, (elderly) = 1.13 Magadan (30–64) = 1.32, (elderly)=1.12 Murmansk (30–64) = 1.05, (elderly) = 1.01 Yakutsk (30–64) = 1.04, (elderly) = 1.03 |
| Shaposhnikov et al. [108] | Moscow | 6 June–18 August 2010 | Daily T, AT | HW: T > 97th percentile of the year-round distribution for the period from 1980 to 2010, duration >5 days | Added deaths due to interaction between HW and air pollution, elevated risks for NA (elderly) RR = 2.14% (95% CI: 2.06–2.23); nervous system = 3.07% (95% CI: 2.52–3.92), genitourinary = 2.54% (95% CI: 2.14–3.12), CVD = 2.37% (95% CI: 2.24–2.52), IHD = 2.29 (95% CI: 2.18–2.40), RD = 2.05% (95% CI: 1.80–2.39) |
| Shartova et al. [110] | Rostov–on–Don | 1999–2011(excluding 2010) | Daily T, HUM, AT, PET | HW: T (HUM, AT, PET) > 97th percentile of the year-round distribution during the study period, duration >5 days | T as predictor for the mortality from CHD (30–64 years old) RR = 1.19% (95% CI: 0.09–2.21); PET for mortality from CVD (30–64) = 1.64% (95% CI: 0.18–4.43), 2 day lag; PET as predictor (elderly): CHD = 1.51% (95% CI: 0.09–7.03) 3 day lag, CVD = 1.72% (95% CI: 0.05–18.63), 1 day lag |
| Shartova et al [111] | Arkhangelsk | 1999–2016 | Daily T, UTCI | HW: T (UTCI) > 97th percentile of the year-round distribution during the study period, duration >5 days | Increase in mortality using: maximum daily T for women all-cause (30–64) = 1.80; RD (elderly) = 0.66; maximum UTCI for men with CVD (30–64) = 0.67, (elderly) = 2.83 |
| Smirnova et al. [115] | Moscow | Summer 2010 | Daily T | HW | Increase in hypertensive crises, unscheduled visits to the doctor, cardiac arrhythmias |
| Cold Waves | |||||
| Ageev [43] | Moscow | 2012–2013 | Daily T | CW: T < 3rd percentile of the year-round distribution during the study period, duration >5 days | Increase in cardiovascular exacerbations in some patients with CVD: hypertensive crisis, ambulance calls |
| Chernykh, Taseiko [55] | Krasnoyarsk | 2000–2004, 2010–2014 | Daily T | CW: T < 3rd percentile of the year-round distribution during the study period, duration >5 days | Absolute risk of mortality increase: for CVD (elderly) = 4.81 * 10−3; ED (30–64 years old) = 1.45 * 10−3 |
| Revich [94] | Moscow | 2000–2012 | Daily T | CW: T < 3rd percentile of the year-round distribution during the study period, duration >5 days | ≥65 years old: IHD = 1.05 (95% CI: 1.03–1.07), CVD = 1.08 (95% CI: 1.05–1.10), NA = 1.05% (95% CI: 1.04–1.06) |
| Revich [94] | Vladivostok | 2000–2016 | Daily T | CW: T (WCI) < 3rd percentile of the year-round distribution during the study period, duration >5 days | IHD (30–64 years old) RR = 1.30% (95% CI: 1.12–1.51), RD (30–64) = 1.39% (95% CI: 1.03–1.87), ED (30–64) = 1.27 % (95% CI: 1.04–1.54). No significant results for the elderly |
| Revich, Shaposhnikov [98] | Krasnoyarsk | 1999–2015 | Daily T, WCI | CW: T (WCI) < 3rd percentile of the year-round distribution during the study period, duration >5 days | Increase in all-cause mortality (30–64 years old) RR = 7.3% (95%, CI: 1.1–13.8), (elderly) = 6.3% (95%, CI: 1.7–11.2) |
| Revich et al. [99] | Northern cities Arkhangelsk, Murmansk, Yakutsk | 1999–2016 | Daily T, WCI | CW: T (WCI) < 3rd percentile of the year-round distribution during the study period, duration >5 days | Increase in mortality, T as predictor: Arkhangelsk, IHD RR = 1.16% (95% CI: 1.037–1.31), CVD = 1.30% (95% CI: 1.15–1.46) Murmansk IHD = 1.24% (95% CI: 1.07–1.42), CVD = 1.10% (95% CI: 0.94–1.29) Yakutsk IHD = 1.26% (95% CI: 1.03–1.53), CVD = 1.36% (95% CI: 1.05–1.76) |
| Revich et al. [101] | St-Petersburg | 1999–2016 | Daily T, WCI | CW: T (WCI) < 3rd percentile of the year-round distribution during period from 1961 to 2017, duration >5 days | T as predictor: RD (≥65) RR = 1.19% (95% CI: 1.01–1.40) |
| Shaposhnikov, Revich [107] | Northern cities Arkhangelsk, Magadan, Murmansk, Yakutsk | 1999–2007 | Daily T | CW: T (WCI) < 3rd percentile of the year-round distribution during study period, duration >5 days | Arkhangelsk: IHD (30–64 years) RR = 1.18, (≥65) = 1.22; CVD (30–64) = 1.13, (≥65) = 1.19; RD (30–64 years) = 1.31; NA (30–64) = 1.12, NA (≥65) = 1.18; Murmansk: IHD (30–64) = 1.18; Magadan: IHD (≥65) = 1.39; CVD (≥65) = 1.66; Yakutsk: IHD (30–64) = 1.38, (≥65) = 1.41; CVD (≥65) = 1.69; RD (≥65) = 1.97, NA (≥65) = 1.24 |
| Shartova et al. [111] | Arkhangelsk | 1999–2016 | Daily T, UTCI | CW: T (UTCI) < 3rd percentile of the year-round distribution during study period, duration >5 days | Increase in mortality: mean daily T for women (30–64 years old) CHD = 0.74, RD (≥65) = 0.58; minimum daily UTCI for men CV (30–64) = 3.67, RD (≥65) = 0.87 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Grigorieva, E.A.; Revich, B.A. Health Risks to the Russian Population from Temperature Extremes at the Beginning of the XXI Century. Atmosphere 2021, 12, 1331. https://doi.org/10.3390/atmos12101331
Grigorieva EA, Revich BA. Health Risks to the Russian Population from Temperature Extremes at the Beginning of the XXI Century. Atmosphere. 2021; 12(10):1331. https://doi.org/10.3390/atmos12101331
Chicago/Turabian StyleGrigorieva, Elena A., and Boris A. Revich. 2021. "Health Risks to the Russian Population from Temperature Extremes at the Beginning of the XXI Century" Atmosphere 12, no. 10: 1331. https://doi.org/10.3390/atmos12101331
APA StyleGrigorieva, E. A., & Revich, B. A. (2021). Health Risks to the Russian Population from Temperature Extremes at the Beginning of the XXI Century. Atmosphere, 12(10), 1331. https://doi.org/10.3390/atmos12101331







