Particulate Matter and Its Impact on Mortality among Elderly Residents of Seoul, South Korea
Abstract
1. Introduction
2. Materials and Methods
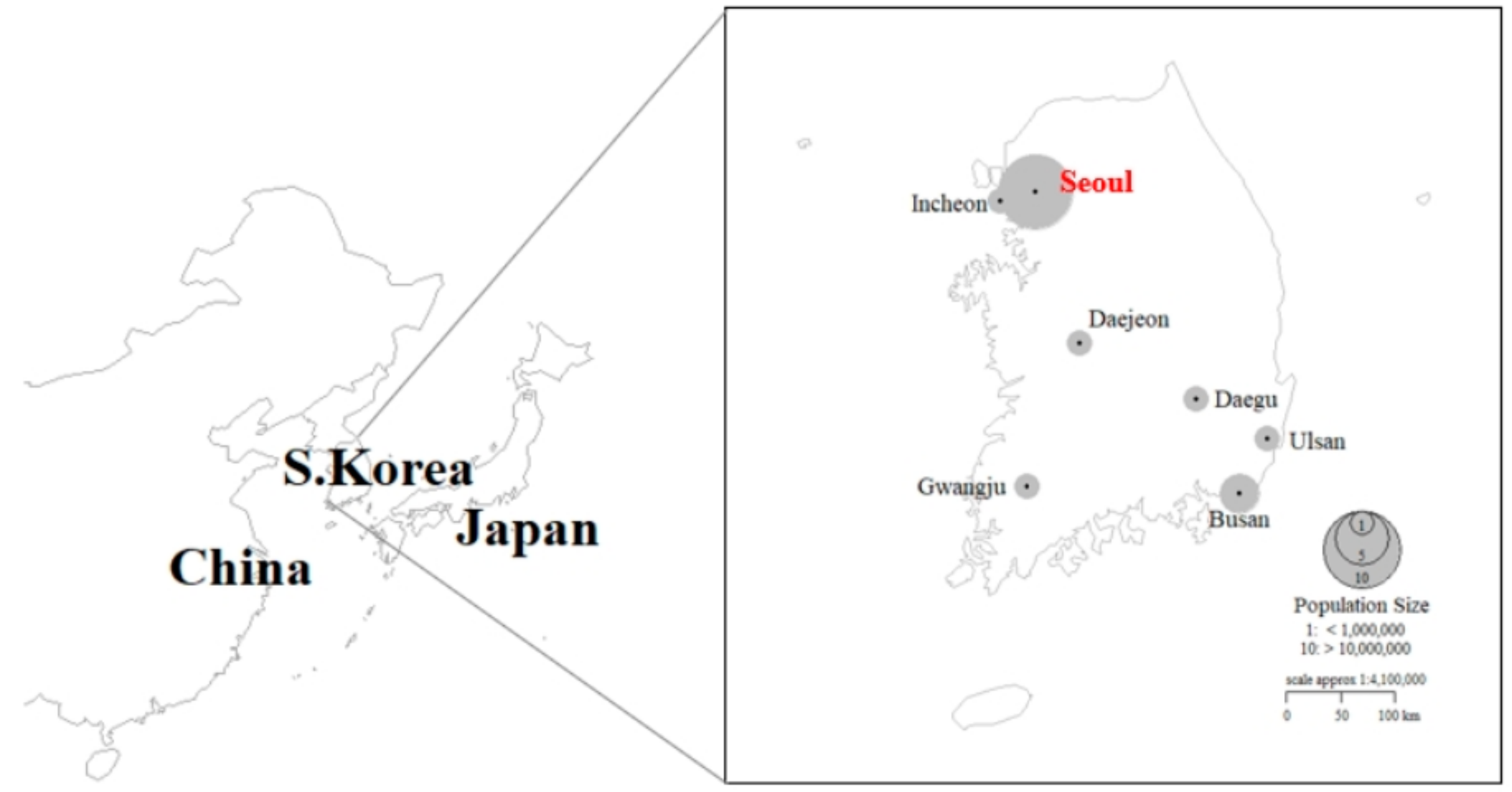
2.1. Study Location
2.2. Data
2.3. Statistical Analyses
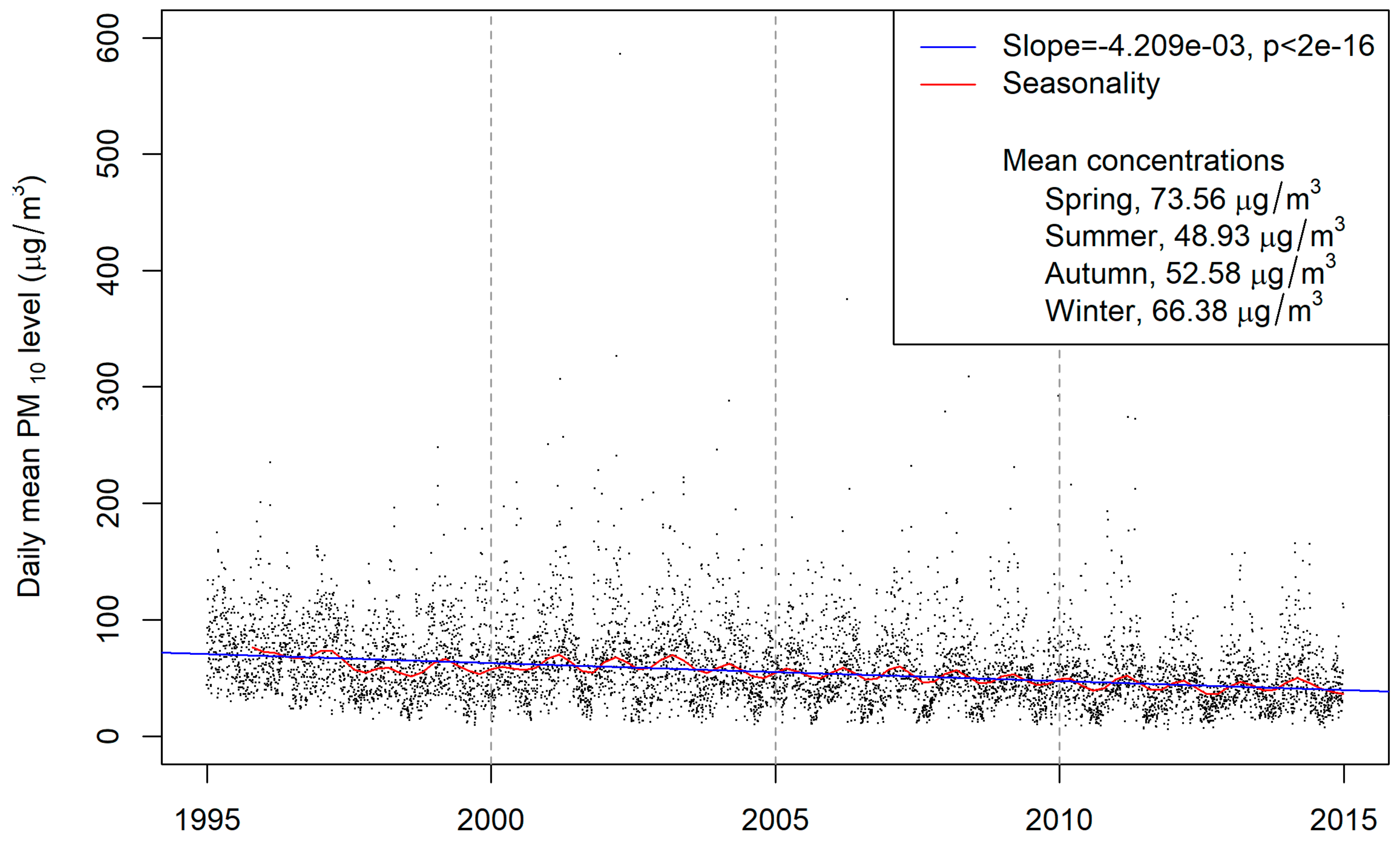
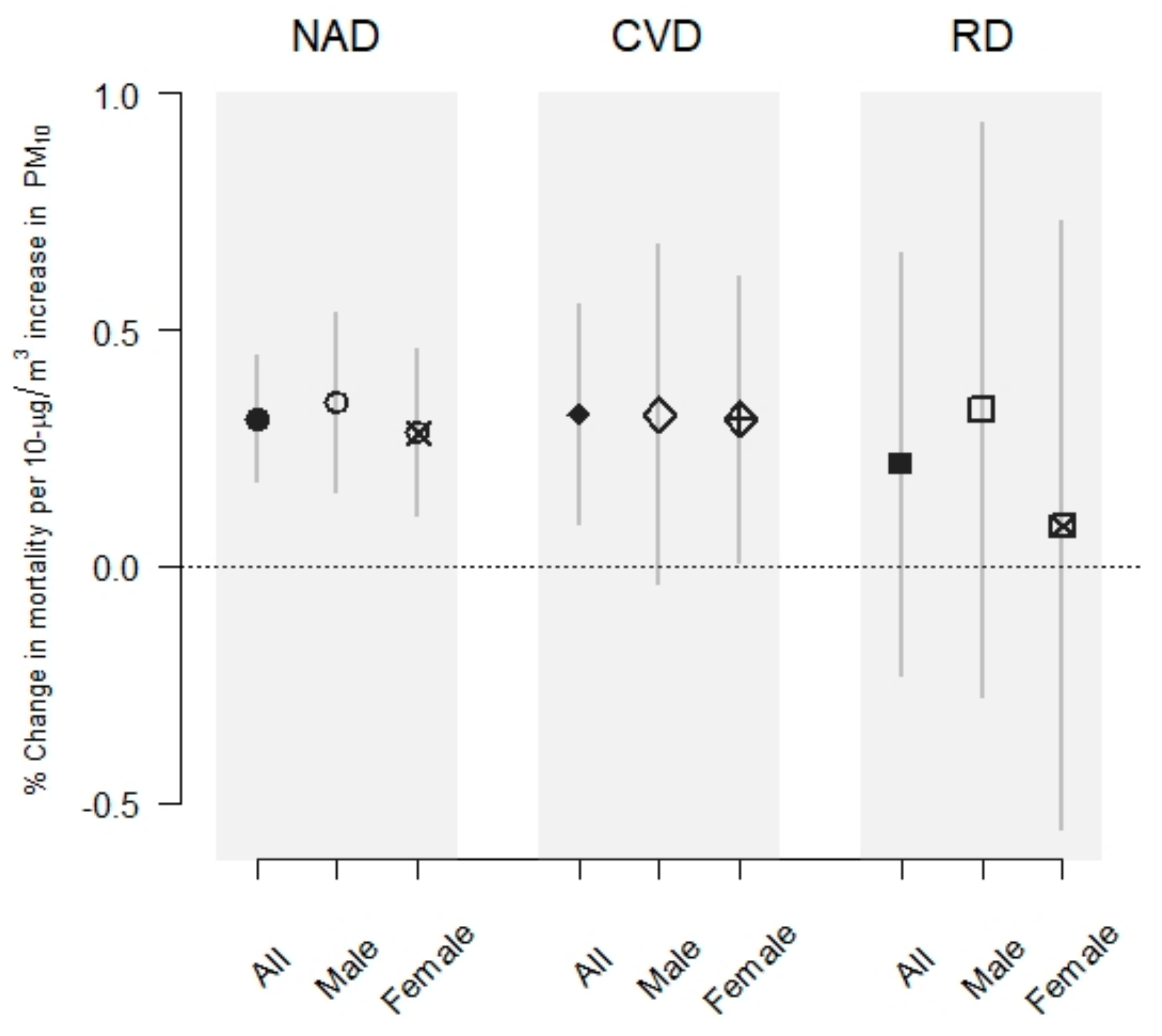
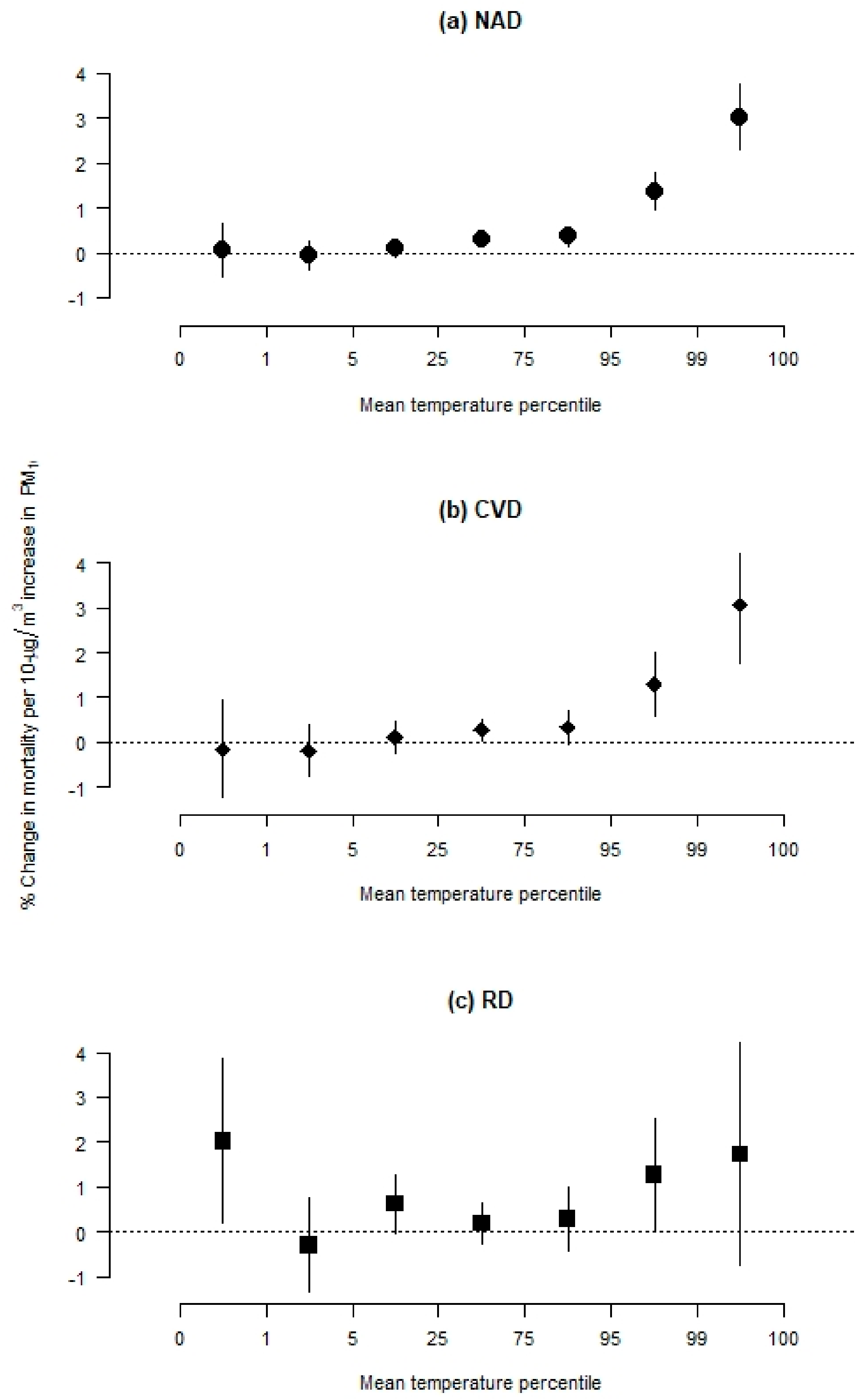
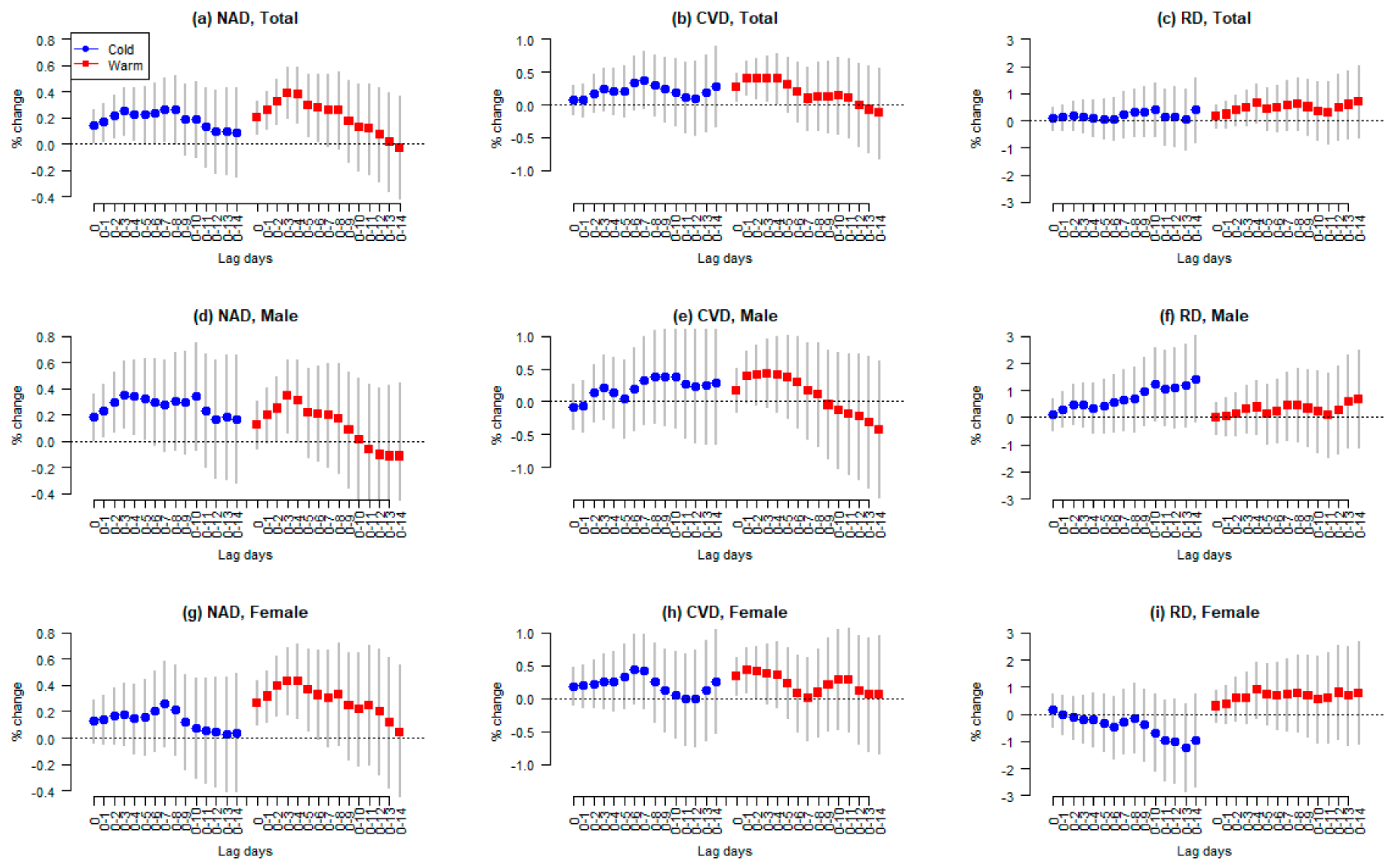
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- James, S.L.; Abate, D.; Abate, K.H.; Abay, S.M.; Abbafati, C.; Abbasi, N.; Abbastabar, H.; Abd-Allah, F.; Abdela, J.; Abdelalim, A.; et al. Global, regional, and national incidence, prevalence, and years lived with disability for 354 Diseases and Injuries for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1789–1858. [Google Scholar] [CrossRef]
- Jung, M.; Cho, D. The Impact of Particulate Matter on Outdoor Activity and Mental Health: A Matching Approach. Int. J. Env. Res. Public Health 2019, 16, 2893. [Google Scholar] [CrossRef]
- Ahmed, C.; Jiang, H.; Chen, J.; Lin, Y.-H. Traffic-Related Particulate Matter and Cardiometabolic Syndrome: A Review. Atmosphere 2018, 9, 336. [Google Scholar] [CrossRef]
- Chen, R.; Kan, H.; Chen, B.; Huang, W.; Bai, Z.; Song, G.; Pan, G. Association of particulate air pollution with daily mortality: The China air pollution and health effects study. Am. J. Epidemiol. 2012, 175, 1173–1181. [Google Scholar] [CrossRef]
- Sunil, V.R.; Patel, K.J.; Mainelis, G.; Turpin, B.J.; Ridgely, S.; Laumbach, R.J.; Kipen, H.M.; Nazarenko, Y.; Veleeparambil, M.; Gow, A.J.; et al. Pulmonary effects of inhaled diesel exhaust in aged mice. Toxicol. Appl. Pharmacol. 2009, 241, 283–293. [Google Scholar] [CrossRef] [PubMed]
- Gomez, C.R.; Nomellini, V.; Faunce, D.E.; Kovacs, E.J. Innate immunity and aging. Exp. Gerontol. 2008, 43, 718–728. [Google Scholar] [CrossRef] [PubMed]
- He, W.; Goodkind, D.; Kowal, P.R. An aging world: 2015-International Population Reports; U.S. Government Publishing Office; United States Census Bureau: Washington, DC, USA, 2016.
- Bae, S.; Kwon, H.J. Current state of research on the risk of morbidity and mortality associated with air pollution in korea. Yonsei Med. J. 2019, 60, 243–256. [Google Scholar] [CrossRef] [PubMed]
- Willers, S.M.; Jonker, M.F.; Klok, L.; Keuken, M.P.; Odink, J.; van den Elshout, S.; Sabel, C.E.; Mackenbach, J.P.; Burdorf, A. High resolution exposure modelling of heat and air pollution and the impact on mortality. Environ. Int. 2016, 89, 102–109. [Google Scholar] [CrossRef] [PubMed]
- Analitis, A.; De’ Donato, F.; Scortichini, M.; Lanki, T.; Basagana, X.; Ballester, F.; Astrom, C.; Paldy, A.; Pascal, M.; Gasparrini, A.; et al. Synergistic Effects of Ambient Temperature and Air Pollution on Health in Europe: Results from the PHASE Project. Int. J. Environ. Res. Public Health 2018, 15, 1856. [Google Scholar] [CrossRef]
- Kim, S.E.S.E.; Lim, Y.H.Y.-H.; Kim, H. Temperature modifies the association between particulate air pollution and mortality: A multi-city study in South Korea. Sci. Total Environ. 2015, 524, 376–383. [Google Scholar] [CrossRef]
- Tian, L.; Liang, F.; Guo, Q.; Chen, S.; Xiao, S.; Wu, Z.; Jin, X.; Pan, X. The effects of interaction between particulate matter and temperature on mortality in Beijing, China. Environ. Sci. Process. Impacts 2018, 20, 395–405. [Google Scholar] [CrossRef] [PubMed]
- Luís Ferreira Braga, A.; Zanobetti, A.; Schwartz, J. The Lag Structure Between Particulate Air Pollution and Respiratory and Cardiovascular Deaths in 10 US Cities. J. Occup. Environ. Med. 2001, 43, 927–933. [Google Scholar] [CrossRef] [PubMed]
- KOSIS Population Density (Population and Housing Census). Available online: http://kosis.kr/statHtml/statHtml.do?orgId=101&tblId=DT_1B08024&vw_cd=MT_ZTITLE&list_id=A1_13&seqNo=&lang_mode=ko&language=kor&obj_var_id=&itm_id=&conn_path=MT_ZTITLE (accessed on 2 October 2019).
- KOSIS Elderly population ratio. Available online: http://kosis.kr/statHtml/statHtml.do?orgId=101&tblId=DT_1YL20631 (accessed on 2 October 2019).
- WHO. WHO Air Quality Guidelines for Particulate Matter, Ozone, Nitrogen Dioxide and Sulfur Dioxide: Summary of Risk Assessment; WHO: Geneva, Switzerland, 2006; ISBN 9289021926. [Google Scholar]
- Wood, S. On confidence intervals for generalized additive models based on penalized regression splines. Aust. New Zealand J. Stat. 2006, 48, 445–464. [Google Scholar] [CrossRef]
- Son, J.Y.; Bell, M.L. The relationships between short-term exposure to particulate matter and mortality in Korea: Impact of particulate matter exposure metrics for sub-daily exposures. Environ. Res. Lett. 2013, 8. [Google Scholar]
- Wong, C.M.; Vichit-Vadakan, N.; Kan, H.; Qian, Z.; Vajanapoom, N.; Ostro, B.; Wong, C.M.; Thach, T.Q.; Chau, P.Y.K.; Chan, K.P.; et al. Public Health and Air Pollution in Asia (PAPA): A multicity study of short-term effects of air pollution on mortality. Environ. Health Perspect. 2008, 116, 1195–1202. [Google Scholar] [CrossRef] [PubMed]
- Ostro, B.; Chestnut, L.; Vichit-Vadakan, N.; Laixuthai, A. The impact of particulate matter on daily mortality in Bangkok, Thailand. J. Air Waste Manag. Assoc. 1999, 49, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Stafoggia, M.; Samoli, E.; Alessandrini, E.; Cadum, E.; Ostro, B.; Berti, G.; Faustini, A.; Jacquemin, B.; Linares, C.; Pascal, M.; et al. Short-term associations between fine and coarse particulate matter and hospitalizations in Southern Europe: Results from the MED-PARTICLES project. Environ. Health Perspect. 2013, 121, 1026–1033. [Google Scholar] [CrossRef]
- Zeka, A.; Zanobetti, A.; Schwartz, J. Short term effects of particulate matter on cause specific mortality: Effects of lags and modification by city characteristics. Occup. Environ. Med. 2005, 62, 718–725. [Google Scholar] [CrossRef]
- Kan, H.; London, S.J.; Chen, G.; Zhang, Y.; Song, G.; Zhao, N.; Jiang, L.; Chen, B. Season, sex, age, and education as modifiers of the effects of outdoor air pollution on daily mortality in Shanghai, China: The Public Health and Air Pollution in Asia (PAPA) study. Environ. Health Perspect. 2008, 116, 1183–1188. [Google Scholar] [CrossRef]
- Yap, J.; Ng, Y.; Yeo, K.K.; Sahlén, A.; Lam, C.S.P.; Lee, V.; Ma, S. Particulate air pollution on cardiovascular mortality in the tropics: Impact on the elderly. Environ. Health A Glob. Access Sci. Source 2019, 18, 1–9. [Google Scholar] [CrossRef]
- Yu, G.-H.; Park, S.-S.; Park, J.S.; Park, S.M.; Song, I.H.; Oh, J.; Shin, H.J.; Lee, M.D.; Lim, H.B.; Kim, H.W.; et al. Pollution Characteristics of PM2.5 Observed during Winter and Summer in Baengryeongdo and Seoul. J. Korean Soc. Atmos. Environ. 2018, 34, 38–55. [Google Scholar] [CrossRef]
- Zanobetti, A.; Schwartz, J.; Samoli, E.; Gryparis, A.; Touloumi, G.; Peacock, J.; Anderson, R.H.; Le Tertre, A.; Bobros, J.; Celko, M.; et al. The temporal pattern of respiratory and heart disease mortality in response to air pollution. Environ. Health Perspect. 2003, 111, 1188–1193. [Google Scholar] [CrossRef] [PubMed]
- Brook, R.D.; Rajagopalan, S.; Pope, C.A.; Brook, J.R.; Bhatnagar, A.; Diez-Roux, A.V.; Holguin, F.; Hong, Y.; Luepker, R.V.; Mittleman, M.A.; et al. Particulate matter air pollution and cardiovascular disease: An update to the scientific statement from the american heart association. Circulation 2010, 121, 2331–2378. [Google Scholar] [CrossRef] [PubMed]
- Ostro, B.; Roth, L.; Malig, B.; Marty, M. The effects of fine particle components on respiratory hospital admissions in children. Environ. Health Perspect. 2009, 117, 475–480. [Google Scholar] [CrossRef]
- Zelikoff, J.T.; Chen, L.C.; Cohen, M.D.; Fang, K.; Gordon, T.; Li, Y.; Nadziejko, C.; Schlesinger, R.B. Effects of inhaled ambient particulate matter on pulmonary antimicrobial immune defense. Inhal. Toxicol. 2003, 15, 131–150. [Google Scholar] [CrossRef]
- Clougherty, J.E. A growing role for gender analysis in air pollution epidemiology. Environ. Health Perspect. 2010, 118, 167–176. [Google Scholar] [CrossRef]
- Sara, H.; Barney, C. Department of Economic and Social Affairs, P.D. Population 2030: Demographic Challenges and Opportunities for Sustainable Development Planning; United Nations: New York, NY, USA, 2015. [Google Scholar]
- Statistics of Korea Population Projections for Korea. Available online: http://kosis.kr/statHtml/statHtml.do?orgId=101&tblId=DT_1BPA401&vw_cd=MT_ZTITLE&list_id=A41_10&seqNo=&lang_mode=ko&language=kor&obj_var_id=&itm_id=&conn_path=MT_ZTITLE (accessed on 2 October 2019).
- Laumbach, R.; Meng, Q.; Kipen, H. What can individuals do to reduce personal health risks from air pollution? J. Thorac. Dis. 2015, 7, 96–107. [Google Scholar]
- Sharma, A.P.; Kim, K.H.; Ahn, J.W.; Shon, Z.H.; Sohn, J.R.; Lee, J.H.; Ma, C.J.; Brown, R.J.C. Ambient particulate matter (PM10) concentrations in major urban areas of Korea during 1996-2010. Atmos. Pollut. Res. 2014, 5, 161–169. [Google Scholar] [CrossRef]
- Zhao, Y.; Cheng, Z.; Lu, Y.; Chang, X.; Chan, C.; Bai, Y.; Zhang, Y.; Cheng, N. PM10 and PM2.5 particles as main air pollutants contributing to rising risks of coronary heart disease: A systematic review. Environ. Technol. Rev. 2017, 6, 174–185. [Google Scholar] [CrossRef]
- Lee, H.; Myung, W.; Kim, D.K.; Kim, S.E.; Kim, C.T.; Kim, H. Short-term air pollution exposure aggravates Parkinson’s disease in a population-based cohort. Sci. Rep. 2017, 7, 44741. [Google Scholar] [CrossRef]
| Category | Sub-Category | Mean | SD | Min | Max |
|---|---|---|---|---|---|
| Cause of Death | NAD | 62.69 | 12.11 | 28 | 114 |
| CVD | 17.68 | 4.7 | 4 | 37 | |
| RD | 5.10 | 2.72 | 0 | 18 | |
| Sex | Male | 28.75 | 7.96 | 7 | 65 |
| Female | 33.94 | 6.98 | 13 | 64 | |
| Season 1 | Warm | 59.36 | 11.06 | 28 | 103 |
| Cold | 66.04 | 12.20 | 32 | 114 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, S.E.; Hijioka, Y.; Nagashima, T.; Kim, H. Particulate Matter and Its Impact on Mortality among Elderly Residents of Seoul, South Korea. Atmosphere 2020, 11, 18. https://doi.org/10.3390/atmos11010018
Kim SE, Hijioka Y, Nagashima T, Kim H. Particulate Matter and Its Impact on Mortality among Elderly Residents of Seoul, South Korea. Atmosphere. 2020; 11(1):18. https://doi.org/10.3390/atmos11010018
Chicago/Turabian StyleKim, Satbyul Estella, Yasuaki Hijioka, Tatsuya Nagashima, and Ho Kim. 2020. "Particulate Matter and Its Impact on Mortality among Elderly Residents of Seoul, South Korea" Atmosphere 11, no. 1: 18. https://doi.org/10.3390/atmos11010018
APA StyleKim, S. E., Hijioka, Y., Nagashima, T., & Kim, H. (2020). Particulate Matter and Its Impact on Mortality among Elderly Residents of Seoul, South Korea. Atmosphere, 11(1), 18. https://doi.org/10.3390/atmos11010018





