Embedded Disposable Functionalized Electrochemical Biosensor with a 3D-Printed Flow Cell for Detection of Hepatic Oval Cells (HOCs)
Abstract
1. Introduction
2. Materials and Methods
2.1. 3D-Printing Process of the Flow Cell
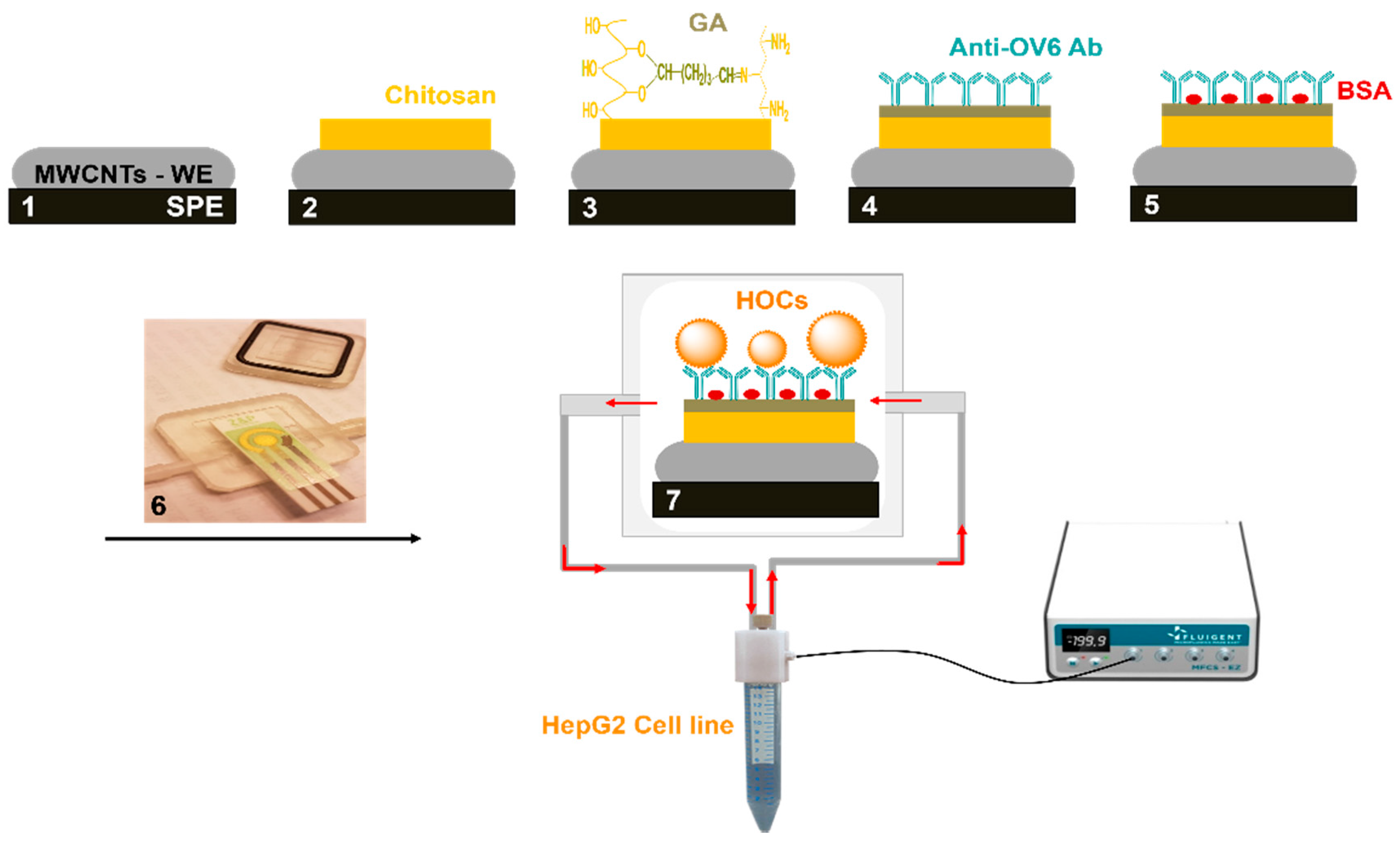
2.2. Preparation of the Functionalized Chitosan Matrix on the Multiwall Carbon Nanotubes Electrode
2.3. Contact Angle Measurements
2.4. Cell Lines and Cell Culture
2.5. Flow Cytometry Analysis
2.6. Electrochemical Measurements
3. Results and Discussion
3.1. Contact Angle Measurements and Surface Sensor Characterization
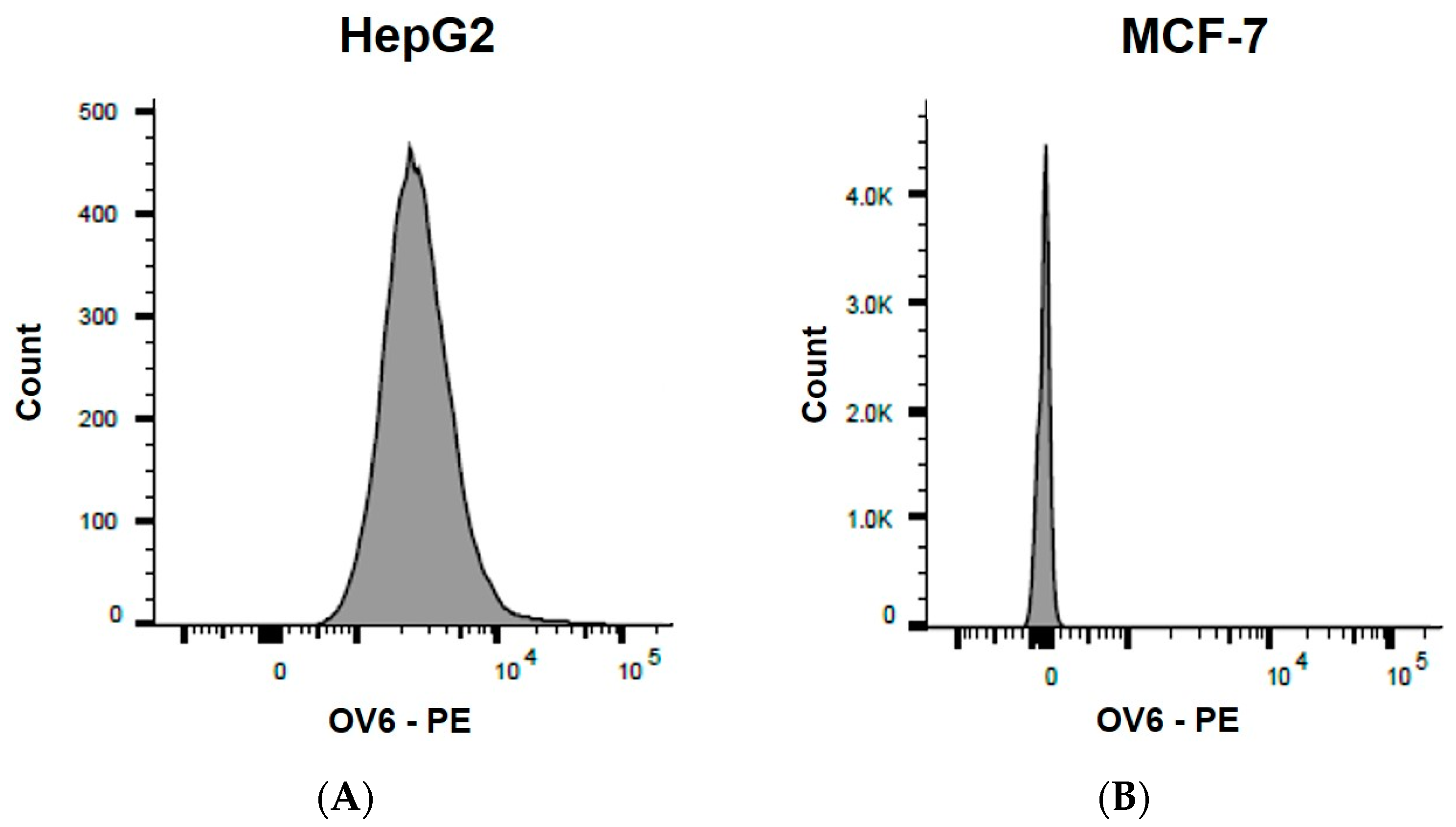
3.2. Detection of the OV6 Marker in Human Cancer Cell Lines via Flow Cytometry
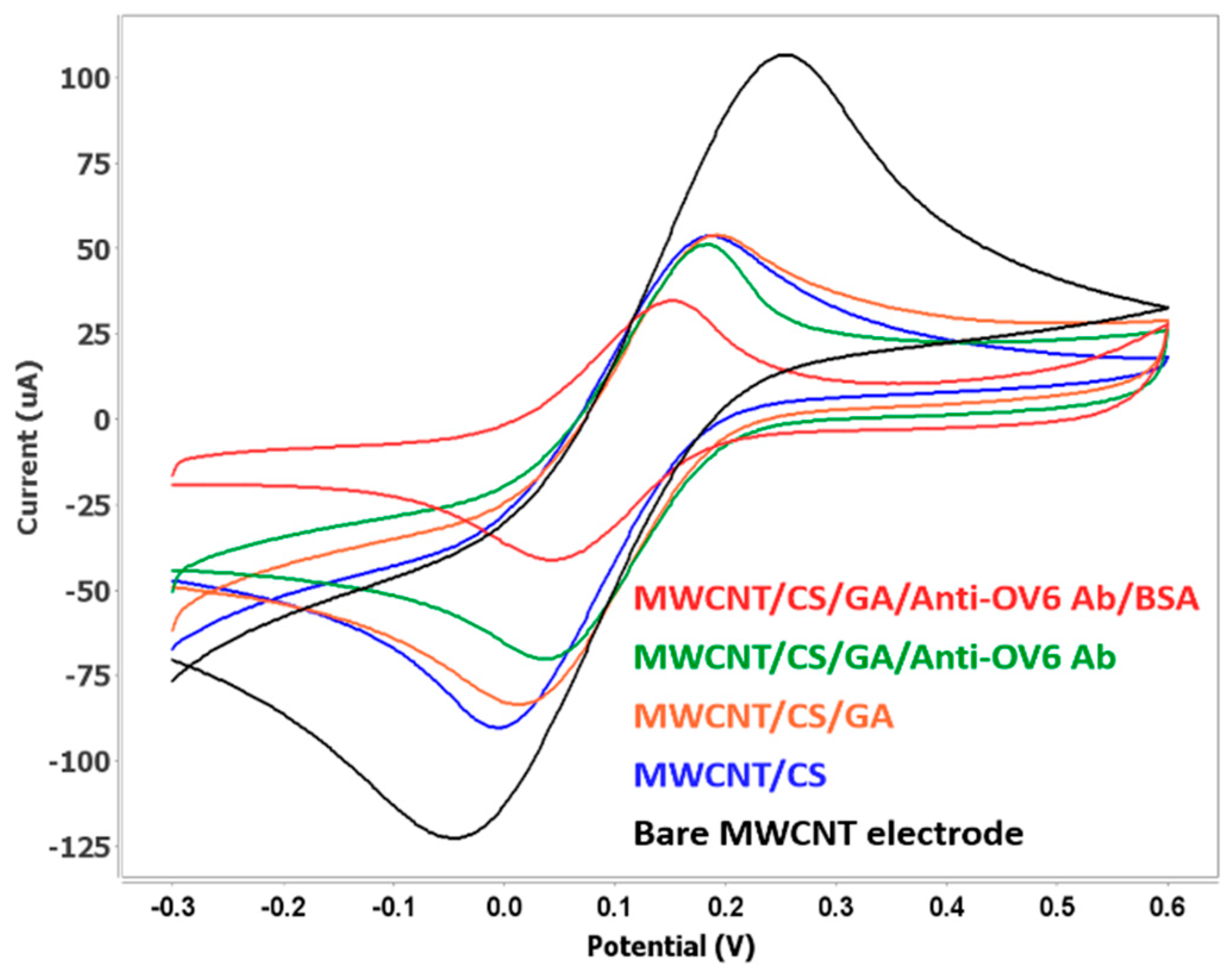
3.3. Electrochemical Behavior of the Fabricated Biosensor
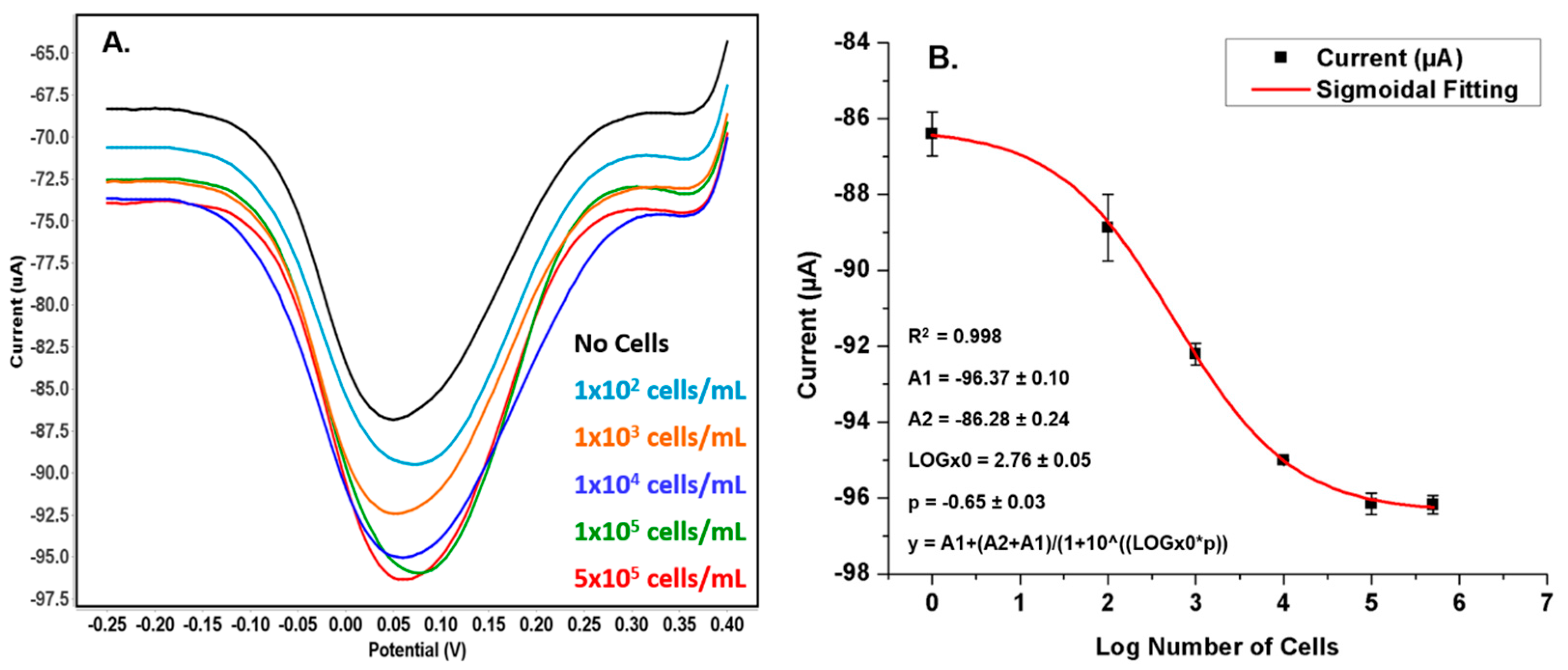
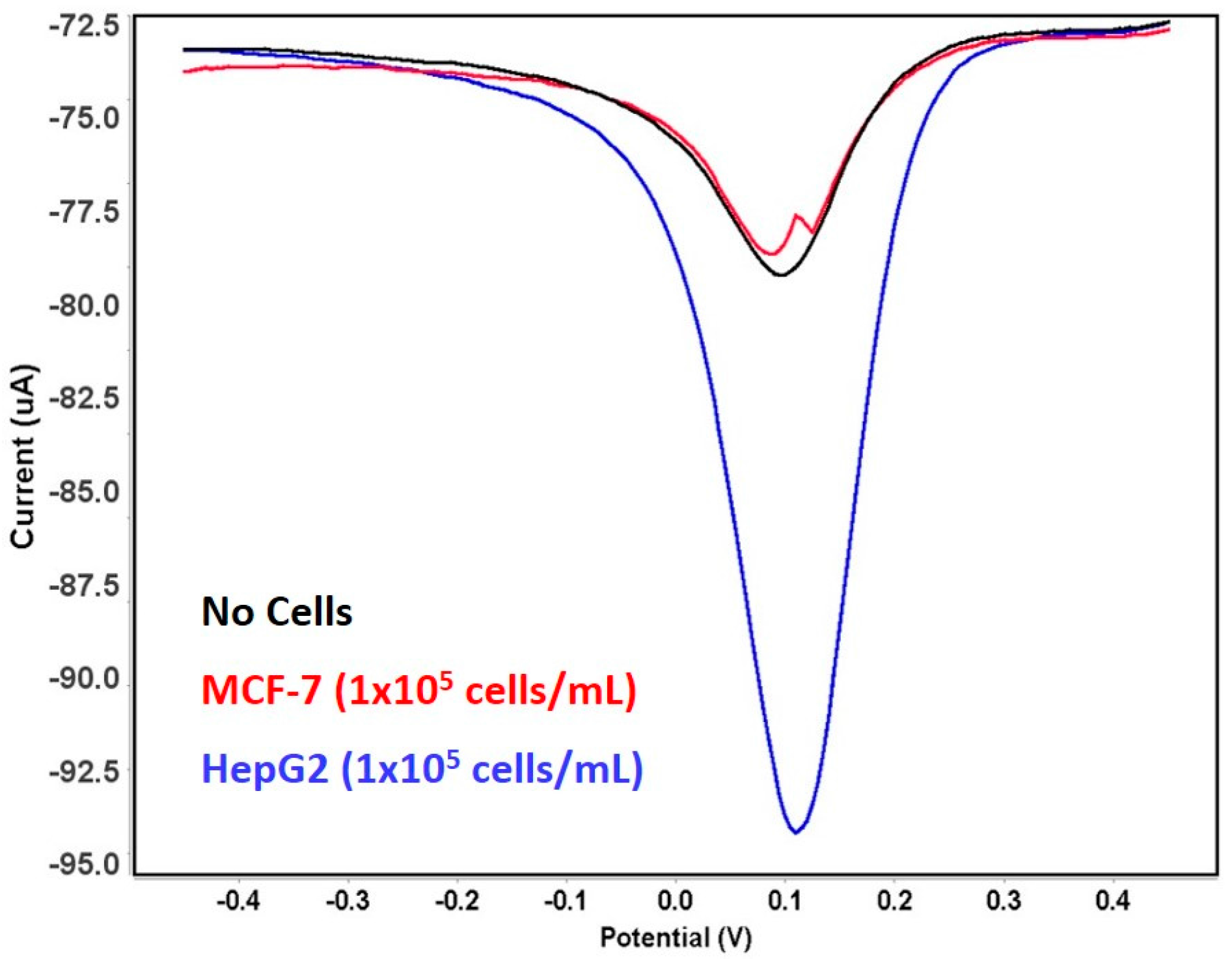
3.4. Detection of Hepatic Oval Cells on the Fabricated Sensor
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ferlay, J.; Soerjomataram, I.; Ervik, M.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, D.M.; Forman, D.; Bray, F. GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 11; International Agency for Research on Cancer: Lyon, France, 2013. [Google Scholar]
- Benson, J.; Jatoi, I. The global breast cancer burden. Future Oncol. 2012, 8, 697–702. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.K.; Hawkins, C.; Clarke, I.D.; Squire, J.A.; Bayani, J.; Hide, T.; Henkelman, R.M.; Cusimano, M.D.; Dirks, P.B. Identification of human brain tumour initiating cells. Nature 2004, 432, 396–401. [Google Scholar] [CrossRef] [PubMed]
- Yin, H.; Zhou, Y.; Chen, C.; Zhu, L.; Ai, S. An electrochemical signal “off-on” sensing platform for microRNA detection. Analyst 2012, 137, 1389–1395. [Google Scholar] [CrossRef] [PubMed]
- Schamhart, D.; Swinnen, J.; Kurth, K.H.; Westerhof, A.; Kuster, R.; Borchers, H.; Sternberg, C. Numeric definition of the clinical performance of the nested reverse transcription-PCR for detection of hematogenous epithelial cells and correction for specific mRNA of non-target cell origin as evaluated for prostate cancer cells. Clin. Chem. 2003, 49, 1458–1466. [Google Scholar] [CrossRef] [PubMed]
- Phillips, J.A.; Xu, Y.; Xia, Z.; Fan, Z.H.; Tan, W.H. Enrichment of cancer cells using aptamers immobilized on a microfluidic channel. Anal. Chem. 2009, 81, 1033–1039. [Google Scholar] [CrossRef] [PubMed]
- Vestergaard, M.; Kerman, K.; Tamiya, E. An overview of label-free electrochemical protein sensors. Sensors 2007, 7, 3442–3458. [Google Scholar] [CrossRef] [PubMed]
- Zamay, G.S.; Zamay, T.N.; Kolovskii, V.A.; Shabanov, A.V.; Glazyrin, Y.E.; Veprintsev, D.V.; Krat, A.V.; Zamay, S.S.; Kolovskaya, O.S.; Gargaun, A.; et al. Electrochemical aptasensor for lung cancer-related protein detection in crude blood plasma samples. Sci. Rep. 2016, 6, 34350. [Google Scholar] [CrossRef] [PubMed]
- Damiati, S.; Küpcü, S.; Peacock, M.; Eilenberger, C.; Zamzami, M.; Qadri, I.; Choudhry, H.; Sleytr, U.; Schuster, B. Acoustic and hybrid 3D-printed electrochemical biosensors for the real-time immunodetection of liver cancer cells (HepG2). Biosens. Bioelectron. 2017, 94, 500–506. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Q.; Kwa, T.; Gao, Y.; Liu, Y.; Rahimian, A.; Revzin, A. On-chip regeneration of aptasensors for monitoring cell secretion. Lab Chip 2014, 14, 276–279. [Google Scholar] [CrossRef] [PubMed]
- Gu, S.; Lu, Y.; Ding, Y.; Li, L.; Song, H.; Wang, J.; Wu, Q. A droplet-based microfluidic electrochemical sensor using platinum-black microelectrode and its application in high sensitive glucose sensing. Biosens. Bioelectron. 2014, 55, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Nagrath, S.; Sequist, L.V.; Maheswaran, S.; Bell, D.W.; Irimia, D.; Ulkus, L.; Smith, M.R.; Kwak, E.L.; Digumarthy, S.; Muzikansky, A.; et al. Isolation of rare circulating tumour cells in cancer patients by microchip technology. Nature 2007, 450, 1235–1240. [Google Scholar] [CrossRef] [PubMed]
- Ortega, F.; Fernández-Baldo, M.; Serrano, M.; Messina, G.; Lorente, J.A.; Raba, J. Epithelial cancer biomarker EpCAM determination in peripheral bloodsamples using a microfluidic immunosensor based in silvernanoparticles as platform. Sens. Actuators B 2015, 221, 248–256. [Google Scholar] [CrossRef]
- Fan, R.; Emery, T.; Zhang, Y.; Xia, Y.; Sun, J.; Wan, J. Circulatory shear flow alters the viability and proliferation of circulating colon cancer cells. Sci. Rep. 2016, 6, 27073. [Google Scholar] [CrossRef] [PubMed]
- Fan, R.; Emery, T.; Zhang, Y.; Xia, Y.; Sun, J.; Wan, J. Therapeutic strategies targeting cancer stem cells. Cancer Biol. Ther. 2013, 14, 295–303. [Google Scholar]
- Riethdorf, S.; Wikman, H.; Pantel, K. Review: Biological relevance of disseminated tumor cells in cancer patients. Int. J. Cancer 2008, 123, 1991–2006. [Google Scholar] [CrossRef] [PubMed]
- King, M.R. Rolling in the deep: Therapeutic targeting of circulating tumor cells. Front. Oncol. 2012, 2, 184. [Google Scholar] [CrossRef] [PubMed]
- Allard, W.J.; Matera, J.; Miller, M.C.; Repollet, M.; Connelly, M.C.; Rao, C.; Tibbe, A.G.; Uhr, J.W.; Terstappen, L.W. Tumor cells circulate in the peripheral blood of all major carcinomas but not in healthy subjects or patients with nonmalignant diseases. Clin. Cancer Res. 2004, 10, 6897–6904. [Google Scholar] [CrossRef] [PubMed]
- Miller, M.C.; Doyle, G.V.; Terstappen, L.W. Significance of circulating tumor cells detected by the cell search system in patients with metastatic breast colorectal and prostate cancer. J. Oncol. 2010, 2010, 617421. [Google Scholar] [CrossRef] [PubMed]
- Rolle, A.; Günzel, R.; Pachmann, U.; Willen, B.; Höffken, K.; Pachmann, K. Increase in number of circulating disseminated epithelial cells after surgery for non-small cell lung cancer monitored by MAINTRAC(R) is a predictor for relapse: A preliminary report. World J. Surg. Oncol. 2005, 3, 18. [Google Scholar] [CrossRef] [PubMed]
- Zieglschmid, V.; Hollmann, C.; Bocher, O. Detection of disseminated tumor cells in peripheral blood. Crit. Rev. Clin. Lab. Sci. 2005, 42, 155–196. [Google Scholar] [CrossRef] [PubMed]
- Bell, D.W.; Haber, D.A. A blood-based test for epidermal growth factor receptor mutations in lung cancer. Clin. Cancer Res. 2006, 12, 3875–3877. [Google Scholar] [CrossRef] [PubMed]
- Krivacic, R.T.; Ladanyi, A.; Curry, D.N.; Hsieh, H.B.; Kuhn, P.; Bergsrud, D.E.; Kepros, J.F.; Barbera, T.; Ho, M.Y.; Chen, L.B.; et al. A rare-cell detector for cancer. Proc. Natl. Acad. Sci. USA 2004, 101, 10501–10504. [Google Scholar] [CrossRef] [PubMed]
- Racila, E.; Euhus, D.; Weiss, A.J.; Uhr, J. Detection and characterization of carcinoma cells in the blood. Proc. Natl. Acad. Sci. USA 1998, 95, 4589–4594. [Google Scholar] [CrossRef] [PubMed]
- Ji, J.; Wang, X. Clinical implications of cancer stem cell biology in hepatocellular carcinoma. Semin. Oncol. 2012, 39, 461–472. [Google Scholar] [CrossRef] [PubMed]
- Ji, J.; Wang, X. Identification of cancer stem cell-related microRNAs in hepatocellular carcinoma. Methods Mol. Biol. 2012, 826, 163–175. [Google Scholar] [PubMed]
- Theise, N.D.; Saxena, R.; Portmann, B.C.; Thung, S.N.; Yee, H.; Chiriboga, L.; Kumar, A.; Crawford, J.M. The canals of Hering and hepatic stem cells in humans. Hepatology 1999, 30, 1425–1433. [Google Scholar] [CrossRef] [PubMed]
- Vessey, C.J.; de la Hall, P.M. Hepatic stem cells: A review. Pathology 2001, 33, 130–141. [Google Scholar] [CrossRef] [PubMed]
- Tîlmaciu, C.M.; Morris, M.C. Carbon nanotube biosensors. Front. Chem. 2015, 3, 59. [Google Scholar] [CrossRef] [PubMed]
- Haslam, C.; Damiati, S.; Whitley, T.; Davey, P.; Ifeachor, E.; Awan, S.A. Label-Free Sensors Based on Graphene Field-Effect Transistors for the detection of human chorionic gonadotropin cancer risk biomarker. Diagnostics 2018, 8, 5. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Lu, X.B.; Li, J.; Yao, X.; Li, J.H. Direct electrochemistry of glucose oxidase and electrochemical biosensing of glucose on quantum dots/carbon nanotubes electrodes. Biosens. Bioelectron. 2007, 22, 3203–3209. [Google Scholar] [CrossRef] [PubMed]
- Meng, L.; Jin, J.; Yang, G.X.; Lu, T.H.; Zhang, H.; Cai, C.X. Nonenzymatic electrochemical detection of glucose based on palladium−single-walled carbon nanotube hybrid nanostructures. Anal. Chem. 2009, 81, 7271–7280. [Google Scholar] [CrossRef] [PubMed]
- Gholivand, M.; Mohammadi-Behzad, L. An electrochemical sensor for warfarin determination based on covalent immobilization of quantum dots onto carboxylated multiwalled carbon nanotubes and chitosan composite film modified electrode. Mater. Sci. Eng. C 2015, 57, 77–87. [Google Scholar] [CrossRef] [PubMed]
- Akanda, R.; Ju, H. A tyrosinase-responsive nonenzymatic redox cycling for amplified electrochemical immunosensing of protein. Anal. Chem. 2016, 88, 9856–9861. [Google Scholar] [CrossRef] [PubMed]
- Ling, S.J.; Yuan, R.; Chai, Y.Q.; Zhang, T.T. Study on immunosensor based on gold nanoparticles/chitosan and MnO2 nanoparticles composites membrane/Prussian blue modified gold electrode. Bioprocess Biosyst. Eng. 2009, 32, 407–414. [Google Scholar] [CrossRef] [PubMed]
- Batra, B.; Pundir, C.S. An amperometric glutamate biosensor based on immobilization of glutamate oxidase onto carboxylated multiwalled carbon nanotubes/gold nanoparticles/chitosan composite film modified Au electrode. Biosens. Bioelectron. 2013, 47, 496–501. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Chen, Y.; Jin, G. Chitosan cushioned phospholipid membrane and its application in imaging ellipsometry based-biosensor. Langmuir 2010, 26, 11140–11144. [Google Scholar] [CrossRef] [PubMed]
- Tsai, H.S.; Wang, Y.Z. Properties of hydrophilic chitosan network membranes by introducing binary crosslink agents. Polym. Bull. 2008, 60, 103–113. [Google Scholar] [CrossRef]
- Lee, Y.M.; Nam, S.Y.; Woo, D.J. Pervaporation of ionically surface crosslinked chitosan composite membranes for water-alcohol mixtures. J. Membr. Sci. 1997, 133, 103–110. [Google Scholar] [CrossRef]
- Hyder, M.N.; Huang, R.; Chen, P. Correlation of physicochemical characteristics with pervaporation performance of poly(vinyl alcohol) membranes. J. Membr. Sci. 2006, 283, 281–290. [Google Scholar] [CrossRef]
- Lee, J.; Dak, P.; Lee, Y.; Park, H.; Choi, W.; Alam, M.; Kim, S. Two-dimensional layered MoS2 biosensors enable highly sensitive detection of biomolecules. Sci. Rep. 2014, 4, 7352. [Google Scholar] [CrossRef] [PubMed]
- Islam, K.; Damiati, S.; Sethi, J.; Suhail, A.; Pan, G. Development of a label-free immunosensor for clusterin detection as an alzheimer’s biomarker. Sensors 2018, 18, 308. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Wang, M.; Cheng, P.; Huang, H.; Dong, W.; Zhang, W.; Li, P.; Lin, C.; Pan, Z.; Wu, M.; et al. Hepatitis B virus X protein promotes the stem-like properties of OV6+ cancer cells in hepatocellular carcinoma. Cell Death Dis. 2017, 8, e2560. [Google Scholar] [CrossRef] [PubMed]
- Strain, A.J.; Crosby, H.A.; Nijjar, S.; Kelly, D.A.; Hubscher, S.G. Human liver-derived stem cells. Semin. Liver Dis. 2003, 23, 373–384. [Google Scholar] [PubMed]
- Lee, T.; Cheung, V.; Ng, I. Liver tumor-initiating cells as a therapeutic target for hepatocellular carcinoma. Cancer Lett. 2013, 338, 101–109. [Google Scholar] [CrossRef] [PubMed]


© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Damiati, S.; Peacock, M.; Leonhardt, S.; Damiati, L.; Baghdadi, M.A.; Becker, H.; Kodzius, R.; Schuster, B. Embedded Disposable Functionalized Electrochemical Biosensor with a 3D-Printed Flow Cell for Detection of Hepatic Oval Cells (HOCs). Genes 2018, 9, 89. https://doi.org/10.3390/genes9020089
Damiati S, Peacock M, Leonhardt S, Damiati L, Baghdadi MA, Becker H, Kodzius R, Schuster B. Embedded Disposable Functionalized Electrochemical Biosensor with a 3D-Printed Flow Cell for Detection of Hepatic Oval Cells (HOCs). Genes. 2018; 9(2):89. https://doi.org/10.3390/genes9020089
Chicago/Turabian StyleDamiati, Samar, Martin Peacock, Stefan Leonhardt, Laila Damiati, Mohammed A. Baghdadi, Holger Becker, Rimantas Kodzius, and Bernhard Schuster. 2018. "Embedded Disposable Functionalized Electrochemical Biosensor with a 3D-Printed Flow Cell for Detection of Hepatic Oval Cells (HOCs)" Genes 9, no. 2: 89. https://doi.org/10.3390/genes9020089
APA StyleDamiati, S., Peacock, M., Leonhardt, S., Damiati, L., Baghdadi, M. A., Becker, H., Kodzius, R., & Schuster, B. (2018). Embedded Disposable Functionalized Electrochemical Biosensor with a 3D-Printed Flow Cell for Detection of Hepatic Oval Cells (HOCs). Genes, 9(2), 89. https://doi.org/10.3390/genes9020089





