Characterizing HIV-1 Genetic Subtypes and Drug Resistance Mutations among Children, Adolescents and Pregnant Women in Sierra Leone
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design, Populations, and Context
2.2. Ethical Considerations
2.3. Biosample Collection and Molecular Analysis
2.4. Statistical Analyses
3. Results
3.1. Characteristics of the Study Population
3.2. HIV Sequence Distributions by Demographic Groups
3.3. HIV Genotypic Subtypes
3.4. Prevalence of RAMS among Children and Adolescents
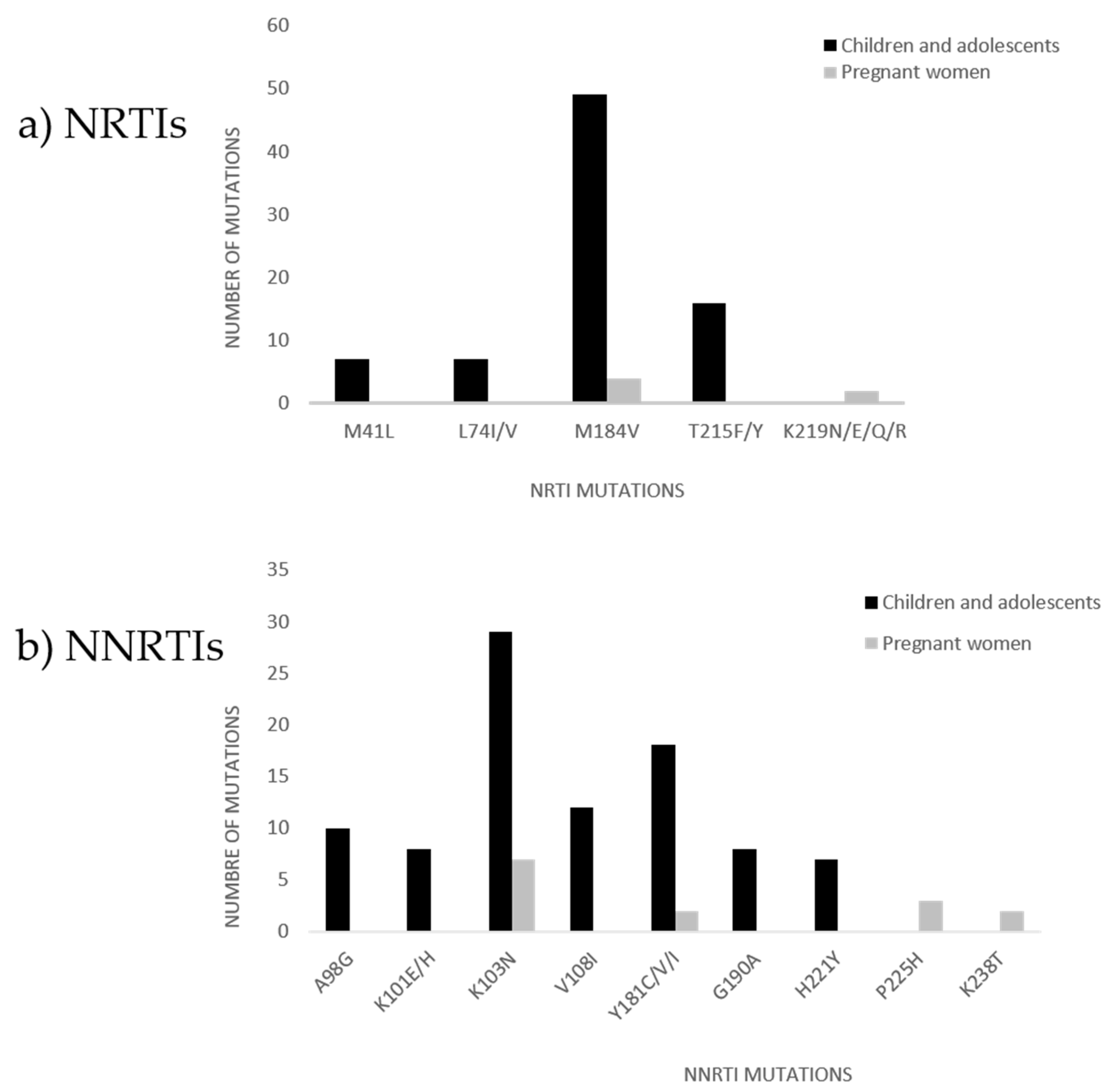
3.4.1. NRTIs and NNRTIs
3.4.2. PIs and INSTIs
3.4.3. Genotypic Susceptibility Scores
3.5. Prevalence of RAMS among Pregnant Women
3.5.1. NRTIs and NNRTIs
3.5.2. PIs and INSTIs
3.5.3. Genotypic Susceptibility Scores
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. HIV Drug Resistance Report 2019. 2019. Available online: https://www.who.int/hiv/pub/drugresistance/hivdr-report-2019/en/ (accessed on 22 June 2021).
- WHO. Global Action Plan on HIV Drug Resistance (2017–2021). 2017. Available online: https://apps.who.int/iris/bitstream/handle/10665/255883/9789241512848-eng.pdf?sequence=1 (accessed on 22 June 2021).
- UNAIDS. UNAIDS Data 2019. 2019. Available online: https://www.unaids.org/en/resources/documents/2019/2019-UNAIDS-data (accessed on 22 June 2021).
- Yendewa, G.A.; Poveda, E.; Yendewa, S.A.; Sahr, F.; Quiñones-Mateu, M.E.; Salata, R.A. HIV/AIDS in Sierra Leone: Characterizing the Hidden Epidemic. AIDS Rev. 2018, 20, 104–113. [Google Scholar] [CrossRef] [PubMed]
- Nagel, E.; Blackowicz, M.J.; Sahr, F.; Jarrett, O.D. Impact of the Ebola epidemic on clinical outcomes of HIV-infected soldiers and their dependents in Sierra Leone. Int. J. STD AIDS 2019, 30, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Gamanga, A.H.; Owiti, P.; Bhat, P.; Harries, A.D.; Kargbo-Labour, I.; Koroma, M. The Ebola outbreak: Effects on HIV reporting, testing and care in Bonthe district, rural Sierra Leone. Public Health Action 2017, 7, S10–S15. [Google Scholar] [CrossRef] [PubMed]
- Parpia, A.S.; Ndeffo-Mbah, M.L.; Wenzel, N.S.; Galvani, A.P. Effects of Response to 2014–2015 Ebola Outbreak on Deaths from Malaria, HIV/AIDS, and Tuberculosis, West Africa. Emerg. Infect. Dis. 2016, 22, 433–441. [Google Scholar] [CrossRef]
- National HIV/AIDS Secretariat 2016. National Strategic Plan 2016–2020. Available online: https://www.nas.gov.sl/images/stories/publications/Sierra%20Leone%20National%20Strategic%20Plan%202016%20-%202020.pdf (accessed on 22 June 2021).
- Yendewa, G.A.; Poveda, E.; Lakoh, S.; Yendewa, S.A.; Jiba, D.F.; Salgado-Barreira, A.; Sahr, F.; Salata, R.A. High prevalence of late-stage disease in newly diagnosed HIV patients in Sierra Leone. Open Forum Infect. Dis. 2018, 5, ofy208. [Google Scholar] [CrossRef] [PubMed]
- Lakoh, S.; Jiba, D.F.; Kanu, J.E.; Poveda, E.; Salgado-Barreira, A.; Sahr, F.; Sesay, M.; Deen, G.F.; Sesay, T.; Gashau, W.; et al. Causes of hospitalization and predictors of HIV-associated in-hospital mortality in Sierra Leone: A Prospective Study. BMC Public Health 2019, 19, 1320. [Google Scholar] [CrossRef] [PubMed]
- Yendewa, G.A.; Sahr, F.; Aguilera, A.; Lakoh, S.; Sesay, M.; Deen, G.F.; Patiño, L.; Poveda, E.; Salata, R.A. Seroprevalence of hepatitis B, hepatitis C and human T-cell lymphotropic virus infections in human immunodeficiency virus-infected patients in Sierra Leone. Am. J. Trop. Med. Hyg. 2019, 100, 1521–1524. [Google Scholar] [CrossRef] [PubMed]
- Yendewa, G.A.; Lakoh, S.; Yendewa, S.A.; Bangura, K.; Lawrence, H.; Patiño, L.; Jiba, D.F.; Vandy, A.O.; Murray, M.J.S.; Massaquoi, S.P.; et al. Prevalence of Hepatitis B Surface Antigen and Serological Markers of Other Endemic Infections in HIV-infected Children, Adolescents and Pregnant Women in Sierra Leone: A Cross-sectional Study. Int. J. Infect. Dis. 2020, 102, 45–52. [Google Scholar] [CrossRef]
- Yendewa, G.A.; Sahr, F.; Lakoh, S.; Ruiz, M.; Patiño, L.; Tabernilla, A.; Deen, G.F.; Sesay, M.; Salata, R.A.; Poveda, E. Prevalence of Drug Resistance Mutations among ART-naïve and experienced HIV-infected patients in Sierra Leone. J. Antimicrob. Chemother. 2019, 74, 2024–2029. [Google Scholar] [CrossRef]
- Villabona-Arenas, C.J.; Vidal, N.; Guichet, E.; Serrano, L.; Delaporte, E.; Gascuel, O.; Peeters, M. In-depth analysis of HIV-1 drug resistance mutations in HIV-infected individuals failing first-line regimens in West and Central Africa. AIDS 2016, 30, 2577–2589. [Google Scholar] [CrossRef]
- Deletsu, S.D.; Maina, E.K.; Quaye, O.; Ampofo, W.K.; Awandare, G.A.; Bonney, E.Y. High resistance to reverse transcriptase inhibitors among persons infected with human immunodeficiency virus type 1 subtype circulating recombinant form 02_AG in Ghana and on antiretroviral therapy. Medicine 2020, 99, e18777. [Google Scholar] [CrossRef]
- Mikasi, S.G.; Gichana, J.O.; Van der Walt, C.; Brado, D.; Obasa, A.E.; Njenda, D.; Messembe, M.; Lyonga, E.; Assoumou, O.; Cloete, R.; et al. HIV-1 Integrase Diversity and Resistance-Associated Mutations and Polymorphisms Among Integrase Strand Transfer Inhibitor-Naive HIV-1 Patients from Cameroon. AIDS Res. Hum. Retrovir. 2020. 36, 450–455. [CrossRef]
- Chaplin, B.; Akanmu, A.S.; Inzaule, S.C.; Samuels, J.O.; Okonkwo, P.; Ilesanmi, O.; Adewole, I.F.A.; Asadu, C.; Khamofu, H.; Mpazanje, R.; et al. Association between HIV-1 subtype and drug resistance in Nigerian infants. J. Antimicrob. Chemother. 2019, 74, 172–176. [Google Scholar] [CrossRef]
- Cissé, A.M.; Laborde-Balen, G.; Kébé-Fall, K.; Dramé, A.; Diop, H.; Diop, K.; FatouNiasse-Traoré; Coulibaly, M.; Have, N.N.; Vidal, N.; et al. High level of treatment failure and drug resistance to first-line antiretroviral therapies among HIV-infected children receiving decentralized care in Senegal. BMC Pediatr. 2019, 19, 47. [Google Scholar] [CrossRef]
- Department of Health and Human Services. Adult and Adolescent Guidelines for the Use of Antiretroviral Agents in Adults and Adolescents with HIV. Available online: http://aidsinfo.nih.gov/contentfiles/lvguidelines/AdultandAdolescentGL.pdf (accessed on 22 June 2021).
- European AIDS Clinical Society. Guidelines Version 10.0. 2019. Available online: https://www.eacsociety.org/files/2019_guidelines-10.0_final.pdf (accessed on 22 June 2021).
- GESIDA. Documento de Consenso de Gesida/Plan Nacional sobre el SIDA Respecto al Tratamiento Antiretroviral en Adultos Infectados por el Virus de la Inmunodeficiencia Humana. Updated January 2018. 2018. Available online: http://gesidaseimc.org/wcontent/uploads/2018/01/gesida_TAR_Gesida_y_PNS_2018.pdf (accessed on 22 June 2021).
- Han, Y.S.; Mesplede, T.; Wainberg, M.A. Differences among HIV-1 subtypes in drug resistance against integrase inhibitors. Infect. Genet. Evol. 2016, 46, 286–291. [Google Scholar] [CrossRef]
- Hurt, C.B.; Sebastian, J.; Hicks, C.B.; Eron, J.J. Resistance to HIV integrase strand transfer inhibitors among clinical specimens in the United States, 2009–2012. Clin. Infect. Dis. 2014, 58, 423–431. [Google Scholar] [CrossRef] [PubMed]
- Koullias, Y.; Sax, P.E.; Fields, N.F.; Walensky, R.P.; Hyle, E.P. Should We Be Testing for Baseline Integrase Resistance in Patients Newly Diagnosed With Human Immunodeficiency Virus? Clin. Infect. Dis. 2017, 65, 1274–1281. [Google Scholar] [CrossRef] [PubMed]
- Zash, R.; Makhema, J.; Shapiro, R.L. Neural-Tube Defects with Dolutegravir Treatment from the Time of Conception. N. Engl. J. Med. 2018, 379, 979–981. [Google Scholar] [CrossRef] [PubMed]
- Zash, R.; Holmes, L.; Diseko, M.; Jacobson, D.L.; Brummel, S.; Mayondi, G.; Isaacson, A.; Davey, S.; Mabuta, J.; Mmalane, M.; et al. Neural-Tube Defects and Antiretroviral Treatment Regimens in Botswana. N. Engl. J. Med. 2019, 381, 827–840. [Google Scholar] [CrossRef]
- Reefhuis, J.; FitzHarris, L.F.; Gray, K.M.; Nesheim, S.; Tinker, S.C.; Isenburg, J.; Laffoon, B.T.; Lowry, J.; Poschman, K.; Cragan, J.D.; et al. Neural Tube Defects in Pregnancies Among Women With Diagnosed HIV Infection—15 Jurisdictions, 2013–2017. Morb. Mortal. Wkly. Rep. 2020, 69, 1–5. [Google Scholar] [CrossRef]
- Garrido, C.; Geretti, A.M.; Zahonero, N.; Booth, C.; Strang, A.; Soriano, V.; De Mendoza, C. Integrase variability and susceptibility to HIV integrase inhibitors: Impact of subtypes, antiretroviral experience and duration of HIV infection. J. Antimicrob. Chemother. 2010, 65, 320–326. [Google Scholar] [CrossRef]
- Lataillade, M.; Chiarella, J.; Kozal, M.J. Natural polymorphism of the HIV-1 integrase gene and mutations associated with integrase inhibitor resistance. Antivir. Ther. 2007, 12, 563–570. [Google Scholar]
- El Bouzidi, K.; Kemp, S.A.; Datir, R.P.; Murtala-Ibrahim, F.; Aliyu, A.; Kwaghe, V.; Frampton, D.; Roy, S.; Breuer, J.; Sabin, C.A.; et al. High prevalence of integrase mutation L74I in West African HIV-1 subtypes prior to integrase inhibitor treatment. J. Antimicrob. Chemother. 2020. published online ahead of print 27 February 2020. [Google Scholar] [CrossRef]
- Tzou, P.L.; Rhee, S.Y.; Descamps, D.; Clutter, D.S.; Hare, B.; Mor, O.; Grude, M.; Parkin, N.; Jordan, M.R.; Bertagnolio, S.; et al. Integrase strand transfer inhibitor (INSTI)-resistance mutations for the surveillance of transmitted HIV-1 drug resistance. J. Antimicrob. Chemother. 2020, 75, 170–182. [Google Scholar] [CrossRef] [PubMed]
- Cahn, P.; Pozniak, A.L.; Mingrone, H.; Shuldyakov, A.; Brites, C.; Andrade-Villanueva, J.F.; Richmond, G.; Buendia, C.B.; Fourie, J.; Ramgopal, M.; et al. Dolutegravir versus raltegravir in antiretroviral-experienced, integrase-inhibitor-naive adults with HIV: Week 48 results from the randomised, double-blind, non-inferiority SAILING study. Lancet 2013, 382, 700–708. [Google Scholar] [CrossRef]
- Walmsley, S.L.; Antela, A.; Clumeck, N.; Duiculescu, D.; Eberhard, A.; Gutiérrez, F.; Hocqueloux, L.; Maggiolo, F.; Sandkovsky, U.; Granier, C.; et al. Dolutegravir plus abacavir-lamivudine for the treatment of HIV-1 infection. N. Engl. J. Med. 2013, 369, 1807–1818. [Google Scholar] [CrossRef] [PubMed]
- Venter, W.D.F.; Moorhouse, M.; Sokhela, S.; Fairlie, L.; Mashabane, N.; Masenya, M.; Serenata, C.; Akpomiemie, G.; Qavi, A.; Chandiwana, N.; et al. Dolutegravir plus Two Different Prodrugs of Tenofovir to Treat HIV. N. Engl. J. Med. 2019, 381, 803–815. [Google Scholar] [CrossRef] [PubMed]
- The NAMSAL ANRS 12313 Study Group; Mpoudi-Etame, M.; Omgba Bassega, P.; Eymard-Duvernay, S.; Leroy, S.; Boyer, S.; Peeters, M.; Calmy, A.; Delaporte, E. Dolutegravir-Based or Low-Dose Efavirenz-Based Regimen for the Treatment of HIV-1. N. Engl. J. Med. 2019, 381, 816–826. [Google Scholar] [CrossRef] [PubMed]
- Miller, V.; Stürmer, M.; Staszewski, S.; Gröschel, B.; Hertogs, K.; de Béthune, M.P.; Pauwels, R.; Harrigan, P.R.; Bloor, S.; Kemp, S.D.; et al. The M184V mutation in HIV-1 reverse transcriptase (RT) conferring lamivudine resistance does not result in broad cross-resistance to nucleoside analogue RT inhibitors. AIDS 1998, 12, 705–712. [Google Scholar] [CrossRef] [PubMed]
- Harrigan, P.R.; Stone, C.; Griffin, P.; Nájera, I.; Bloor, S.; Kemp, S.; Tisdale, M.; Larder, B.; CNA2001 Investigative Group. Resistance profile of the human immunodeficiency virus type 1 reverse transcriptase inhibitor abacavir (1592U89) after monotherapy and combination therapy. J. Infect. Dis. 2000, 181, 912–920. [Google Scholar] [CrossRef]
- Brenner, B.G.; Turner, D.; Wainberg, M.A. HIV-1 drug resistance: Can we overcome? Expert Opin. Biol. Ther. 2002, 2, 751–761. [Google Scholar] [CrossRef]
- Rhee, S.Y.; Taylor, J.; Wadhera, G.; Ben-Hur, A.; Brutlag, D.L.; Shafer, R.W. Genotypic predictors of human immunodeficiency virus type 1 drug resistance. Proc. Natl. Acad. Sci. USA 2006, 103, 17355–17360. [Google Scholar] [CrossRef] [PubMed]
- Whitcomb, J.M.; Parkin, N.T.; Chappey, C.; Hellmann, N.S.; Petropoulos, C.J. Broad nucleoside reverse-transcriptase inhibitor cross-resistance in human immunodeficiency virus type 1 clinical isolates. J. Infect. Dis. 2003, 188, 992–1000. [Google Scholar] [CrossRef]
- Kuritzkes, D.R.; Quinn, J.B.; Benoit, S.L.; Shugarts, D.L.; Griffin, A.; Bakhtiari, M.; Poticha, D.; Eron, J.J.; Fallon, M.A.; Rubin, M. Drug resistance and virologic response in NUCA 3001, a randomized trial of lamivudine (3TC) versus zidovudine (ZDV) versus ZDV plus 3TC in previously untreated patients. AIDS 1996, 10, 975–981. [Google Scholar] [CrossRef] [PubMed]
- Frost, S.D.; Nijhuis, M.; Schuurman, R.; Boucher, C.A.; Brown, A.J. Evolution of lamivudine resistance in human immunodeficiency virus type 1-infected individuals: The relative roles of drift and selection. J. Virol. 2000, 74, 6262–6268. [Google Scholar] [CrossRef]
- Descamps, D.; Flandre, P.; Calvez, V. Mechanism of virologic failure in previously untreated HIV-infect-ed patients from a trial of induction-maintenance therapy. JAMA 2000, 283, 205–211. [Google Scholar] [CrossRef]
- Wei, X.; Liang, C.; Gotte, M.; Wainberg, M.A. The M184V mutation in HIV-1 reverse transcriptase reduces the restoration of wild-type replication by attenuated viruses. AIDS 2002, 16, 2391–2398. [Google Scholar] [CrossRef] [PubMed]
- National AIDS Secretariat 2016. National HIV/AIDS Monitoring and Evaluation Plan 2016–2020. Available online: https://www.nas.gov.sl/images/stories/publications/2016%20-%202020%20HIV%20M&E-Plan.pdf (accessed on 22 June 2021).
| Characteristics | Children N = 96 | Adolescents N = 47 | Pregnant Women N = 54 |
|---|---|---|---|
| Gender | |||
| Male | 49 (51.0) | 25 (53.2) | - |
| Female | 47 (49.0) | 22 (46.8) | 54 (100) |
| Age, years | |||
| Median (IQR) | 5 (4–7) | 13 (10–15) | 26 (23–31) |
| 2–5 | 50 (52.1) | - | - |
| 6–9 | 46 (47.9) | - | - |
| 10–18 | - | 47 (100) | - |
| 18–30 | - | - | 36 (75.0) |
| 31–40 | - | - | 12 (25.0) |
| Mode of HIV acquisition | |||
| Mother to child transmission | 96 (100) | 44 (93.6) | - |
| Sexually transmitted | - | 3 (6.4) | - |
| Median duration of pregnancy (IQR), weeks | - | - | 22 (16–29) |
| Trimester of newly diagnosed N = 15 (100%) | |||
| First (1–13 weeks) | - | - | 4 (26.7) |
| Second (14–26 weeks) | - | - | 8 (53.3) |
| Third (27+ weeks) | - | - | 3 (20.0) |
| CD4 count, median (IQR), cells/mm3 | 985 (596–1407) | 544 (260–849) | 526 (459–698) |
| Current ART regimens | |||
| TDF+ 3TC+ EFV | - | 7 (14.9) | 39 (72.2) |
| AZT+ 3TC+ EFV | 7 (7.3) | 4 (8.5) | - |
| AZT+ 3TC+ NVP | 25 (26.0) | 20 (42.6) | - |
| AZT+ 3TC+ LPV/r | 6 (6.3) | - | - |
| ABC+ 3TC+ EFV | 27 (28.1) | 9 (19.1) | - |
| ABC+ 3TC+ NVP | 15 (15.6) | 2 (4.3) | - |
| ABC+ 3TC+ LPV/r | 16 (16.7) | 5 (10.6) | - |
| Not on ART | - | - | 15 (27.8) |
| Type of ART | |||
| First-line * | 78 (81.3) | 25 (53.2) | 39 (72.2) |
| Second-line ** | 18 (18.8) | 22 (46.8) | - |
| Duration of ART exposure, months | |||
| Median (IQR) | 36 (12–60) | 84 (60–108) | 3 (1–9) |
| ≤24 | 42 (43.8) | 8 (17.0) | 39 (72.2) |
| 25–48 | 23 (24.0) | 2 (4.3) | - |
| 49–60 | 23 (24.0) | 12 (25.5) | - |
| >60 | 6 (8.4) | 25 53.2) | - |
| Population | Preferred WHO First-Line Regimens | GSS < 3 n (%) | Preferred or Alternative WHO Second-Line Regimens | GSS < 3 n (%) |
|---|---|---|---|---|
| Children | AZT + 3TC + DTG | 29 (76.3) | AZT + 3TC + LPV/r (or ATV/r) | 24 (68.6) |
| ABC + 3TC + DTG | 29 (76.3) | AZT + 3TC + DRV/r | 24 (68.6) | |
| ABC + 3TC + LPV/r (or ATV/r) | 24 (68.6) | |||
| ABC + 3TC + DRV/r | 6 (66.6) | |||
| ABC + 3TC + RAL | 7 (70.0) | |||
| Adolescents | AZT + 3TC + DTG | 14 (87.5) | AZT + 3TC + LPV/r (or ATZ/r) | 13 (92.8) |
| ABC + 3TC + DTG | 14 (87.5) | AZT + 3TC + DRV/r | 13 (92.8) | |
| TDF + 3TC + DTG | 14 (87.5) | ABC + 3TC + LPV/r (or ATZ/r) | 24 (68.6) | |
| ABC + 3TC + DRV/r | 6 (100) | |||
| Pregnant women | TDF + 3TC (or FTC) + DTG | 3 (13.6) | TDF + 3TC (or FTC) + ATV/r | 3 (17.6) |
| ABC + 3TC + DTG | 3 (13.6) | TDF + 3TC (or FTC) + LPV/r | 3 (17.6) | |
| AZT + 3TC + DTG | 3 (13.6) | TDF + 3TC (or FTC) + DRV/r | 3 (17.6) | |
| AZT + 3TC + ATV/r | 3 (17.6) | |||
| AZT + 3TC + LPV/r | 3 (17.6) | |||
| AZT + 3TC + DRV/r | 3 (17.6) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yendewa, G.A.; Lakoh, S.; Yendewa, S.A.; Bangura, K.; Tabernilla, A.; Patiño, L.; Jiba, D.F.; Vandy, A.O.; Massaquoi, S.P.; Osório, N.S.; et al. Characterizing HIV-1 Genetic Subtypes and Drug Resistance Mutations among Children, Adolescents and Pregnant Women in Sierra Leone. Genes 2021, 12, 1314. https://doi.org/10.3390/genes12091314
Yendewa GA, Lakoh S, Yendewa SA, Bangura K, Tabernilla A, Patiño L, Jiba DF, Vandy AO, Massaquoi SP, Osório NS, et al. Characterizing HIV-1 Genetic Subtypes and Drug Resistance Mutations among Children, Adolescents and Pregnant Women in Sierra Leone. Genes. 2021; 12(9):1314. https://doi.org/10.3390/genes12091314
Chicago/Turabian StyleYendewa, George A., Sulaiman Lakoh, Sahr A. Yendewa, Khadijah Bangura, Andrés Tabernilla, Lucia Patiño, Darlinda F. Jiba, Alren O. Vandy, Samuel P. Massaquoi, Nuno S. Osório, and et al. 2021. "Characterizing HIV-1 Genetic Subtypes and Drug Resistance Mutations among Children, Adolescents and Pregnant Women in Sierra Leone" Genes 12, no. 9: 1314. https://doi.org/10.3390/genes12091314
APA StyleYendewa, G. A., Lakoh, S., Yendewa, S. A., Bangura, K., Tabernilla, A., Patiño, L., Jiba, D. F., Vandy, A. O., Massaquoi, S. P., Osório, N. S., Deen, G. F., Sahr, F., Salata, R. A., & Poveda, E. (2021). Characterizing HIV-1 Genetic Subtypes and Drug Resistance Mutations among Children, Adolescents and Pregnant Women in Sierra Leone. Genes, 12(9), 1314. https://doi.org/10.3390/genes12091314









