A Human Skin Model Recapitulates Systemic Sclerosis Dermal Fibrosis and Identifies COL22A1 as a TGFβ Early Response Gene that Mediates Fibroblast to Myofibroblast Transition
Abstract
1. Introduction
2. Materials and Methods
2.1. Primary Human Skin and Lung Fibroblasts Culture
2.2. Small Interfering RNA (siRNA) Transfection
2.3. Ex Vivo Human Skin Culture
2.4. Quantitative PCR
2.5. Western Blot Analysis
2.6. RNA Expression Profiling
2.7. Bioinformatics and Statistical Analysis
2.8. Statistical Analysis
3. Results
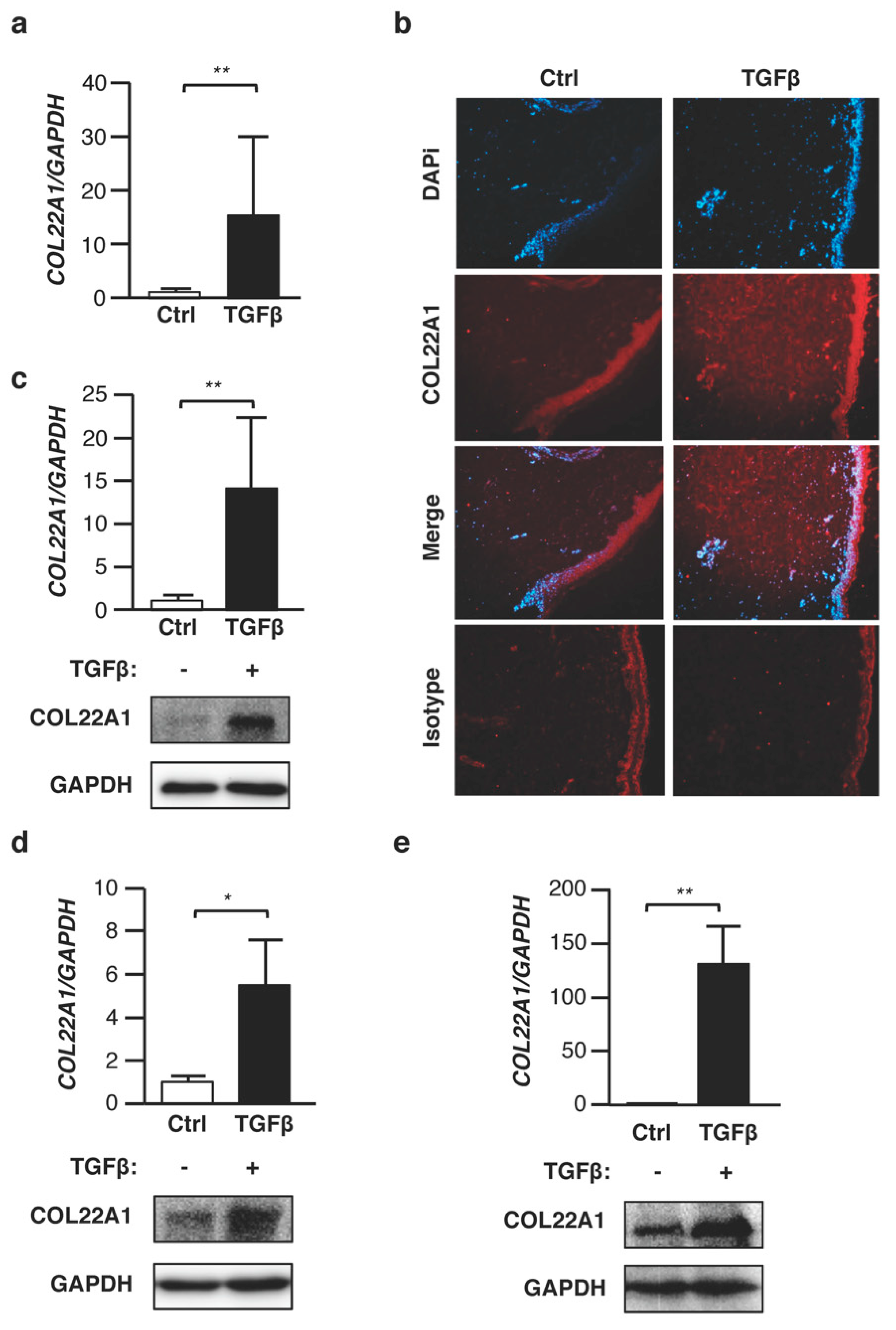
3.1. TGFβ Increases COL22A1 Expression Ex Vivo and In Vitro
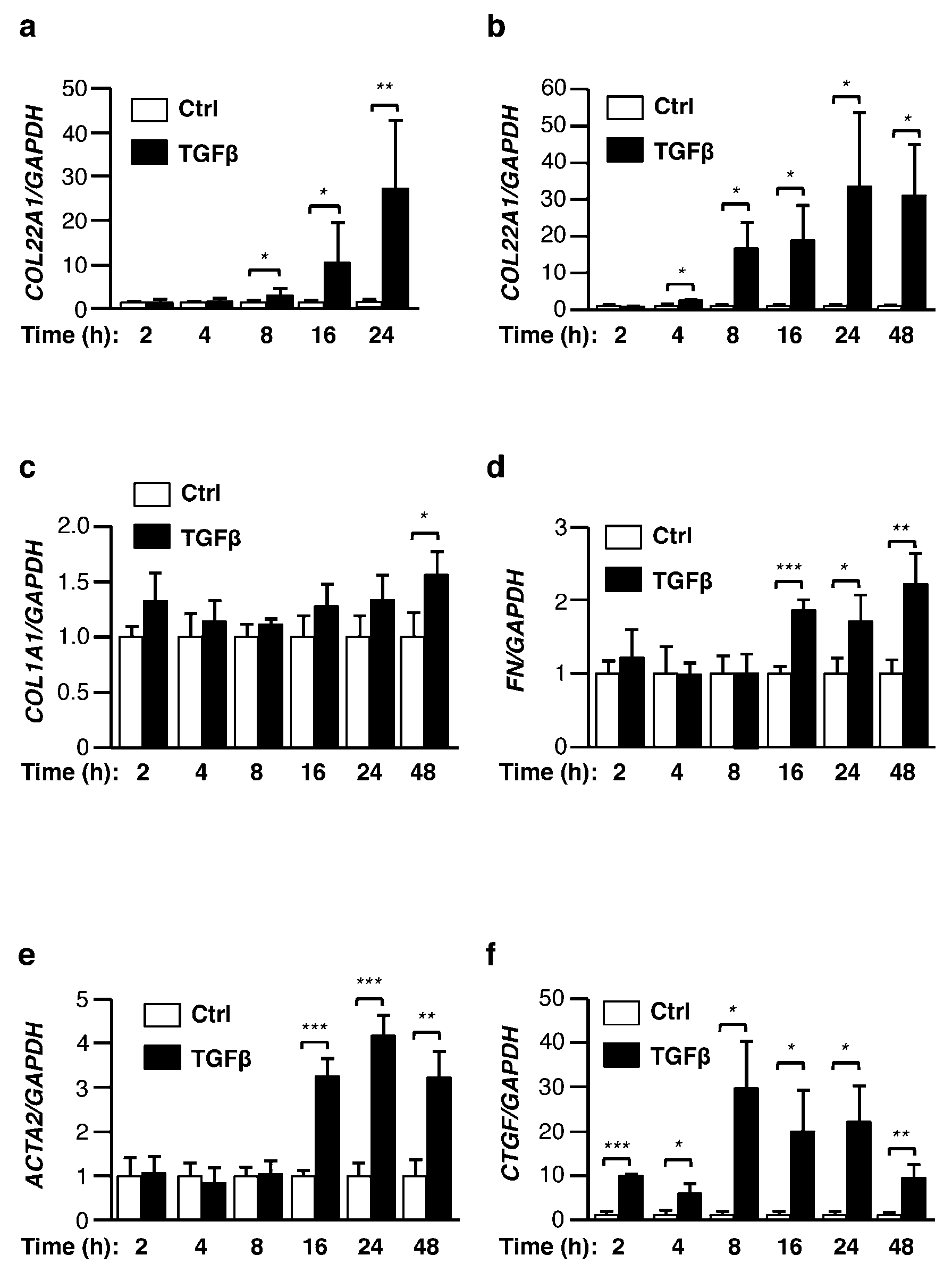
3.2. COL22A1 Is a TGFβ Early Response Gene
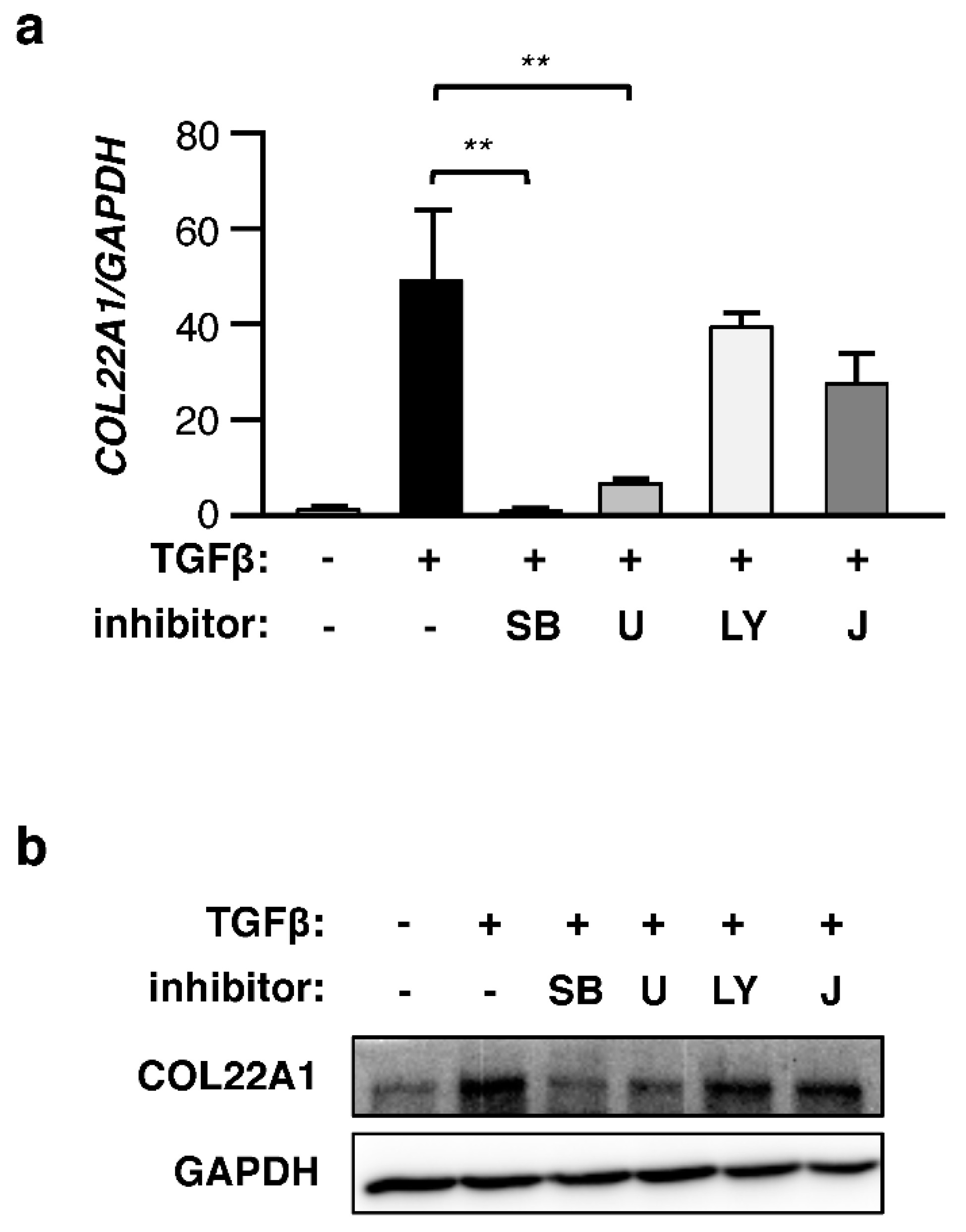
3.3. TGFβ-Induced COL22A1 Expression Depends on ALK5 and MEK Activation
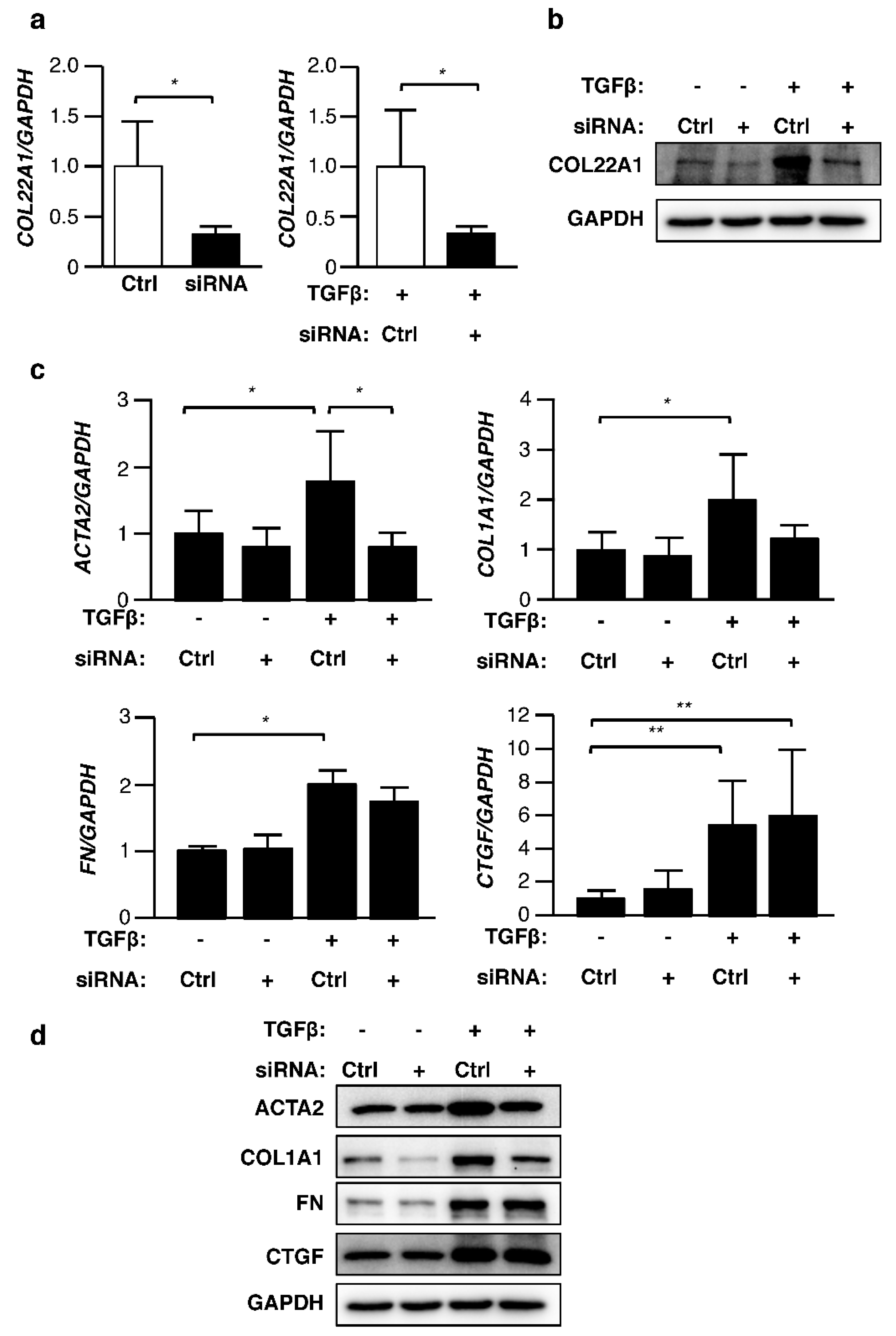
3.4. Silencing COL22A1 Reduces TGFβ-Induced ACTA2 Expression
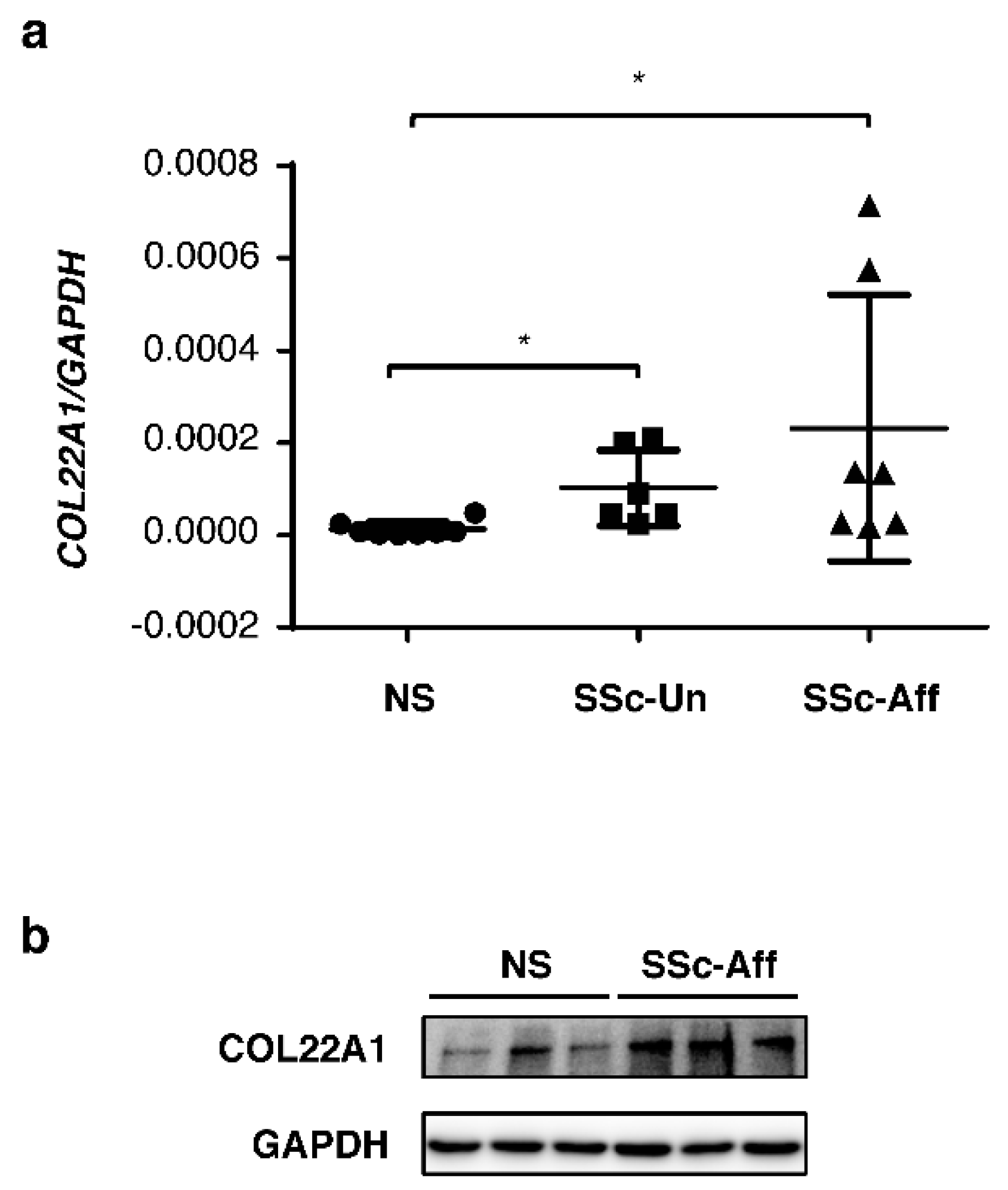
3.5. COL22A1 Expression Is Elevated in SSc Skin Fibroblasts
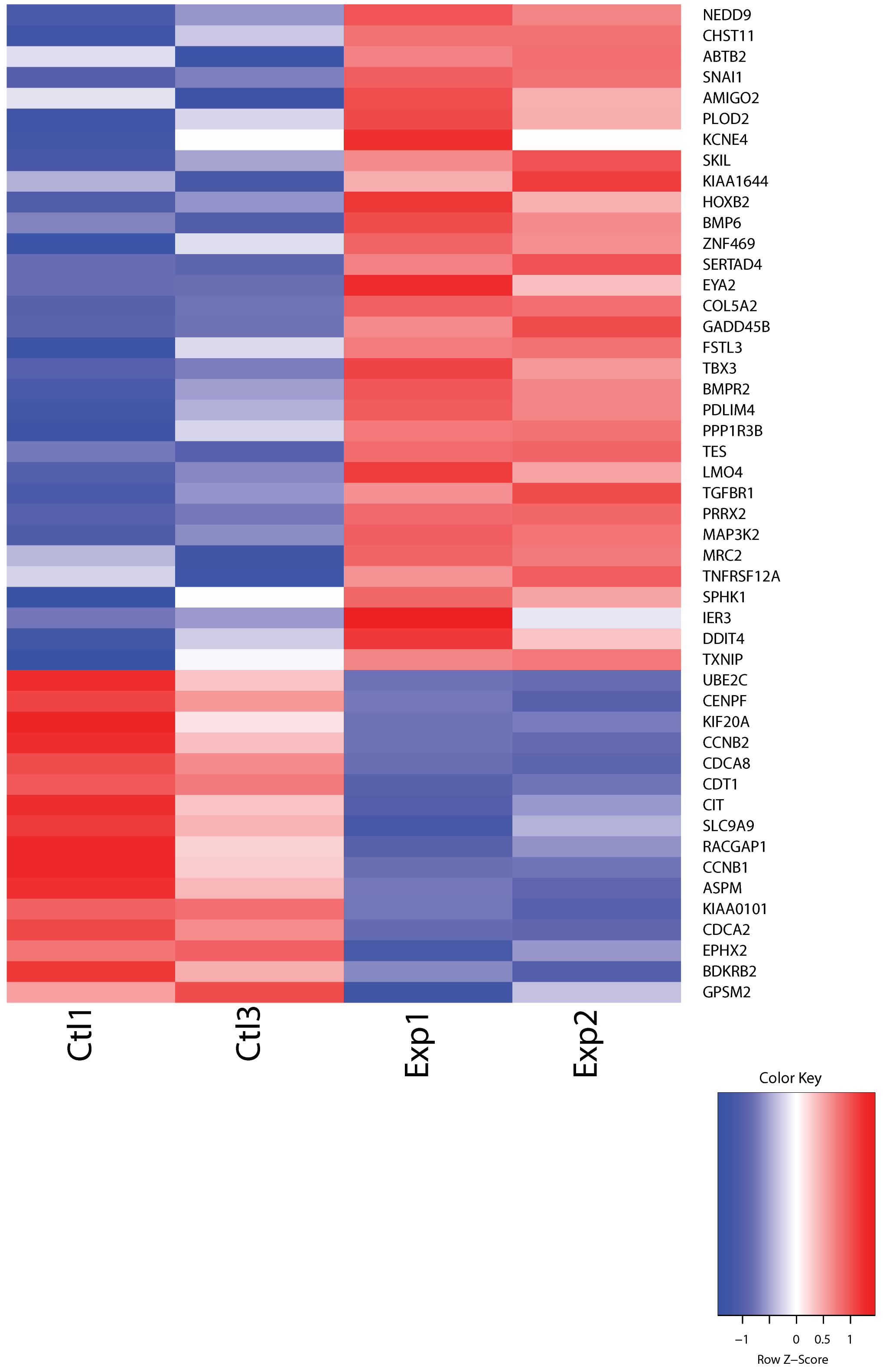
3.6. Genes Identified as Differentially Expressed in TGFβ-Treated Human Skin Overlap with SSc Patient Skin Signatures
4. Discussion
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Almeida, I.; Faria, R.; Vita, P.; Vasconcelos, C. Systemic sclerosis refractory disease: From the skin to the heart. Autoimmun Rev. 2011, 10, 693–701. [Google Scholar] [CrossRef] [PubMed]
- Steen, V.D.; Medsger, T.A., Jr. Epidemiology and natural history of systemic sclerosis. Rheum. Dis. Clin. North Am. 1990, 16, 1–10. [Google Scholar] [PubMed]
- Wynn, T.A. Common and unique mechanisms regulate fibrosis in various fibroproliferative diseases. J. Clin. Investig. 2007, 117, 524–529. [Google Scholar] [CrossRef] [PubMed]
- Koch, M.; Schulze, J.; Hansen, U.; Ashwodt, T.; Keene, D.R.; Brunken, W.J.; Burgeson, R.E.; Bruckner, P.; Bruckner-Tuderman, L. A novel marker of tissue junctions, collagen XXII. J. Biol. Chem. 2004, 279, 22514–22521. [Google Scholar] [CrossRef]
- Ricard-Blum, S.; Ruggiero, F. The collagen superfamily: From the extracellular matrix to the cell membrane. Pathol. Biol. 2005, 53, 430–442. [Google Scholar] [CrossRef] [PubMed]
- Charvet, B.; Guiraud, A.; Malbouyres, M.; Zwolanek, D.; Guillon, E.; Bretaud, S.; Monnot, C.; Schulze, J.; Bader, H.L.; Allard, B.; et al. Knockdown of COL22A1 gene in zebrafish induces a muscular dystrophy by disruption of the myotendinous junction. Development 2013, 140, 4602–4613. [Google Scholar] [CrossRef] [PubMed]
- Misawa, K.; Kanazawa, T.; Imai, A.; Endo, S.; Mochizuki, D.; Fukushima, H.; Misawa, Y.; Mineta, H. Prognostic value of type XXII and XXIV collagen mRNA expression in head and neck cancer patients. Mol. Clin. Oncol. 2014, 2, 285–291. [Google Scholar] [CrossRef] [PubMed]
- Mak, A.C.; Tang, P.L.; Cleveland, C.; Smith, M.H.; Kari Connolly, M.; Katsumoto, T.R.; Wolters, P.J.; Kwok, P.Y.; Criswell, L.A. Brief Report: Whole-Exome Sequencing for Identification of Potential Causal Variants for Diffuse Cutaneous Systemic Sclerosis. Arthritis Rheumatol. 2016, 68, 2257–2262. [Google Scholar] [CrossRef]
- Feghali, C.A.; Wright, T.M. Identification of multiple, differentially expressed messenger RNAs in dermal fibroblasts from patients with systemic sclerosis. Arthritis Rheum. 1999, 42, 1451–1457. [Google Scholar] [CrossRef]
- Hsu, E.; Shi, H.; Jordan, R.M.; Lyons-Weiler, J.; Pilewski, J.M.; Feghali-Bostwick, C.A. Lung tissues in patients with systemic sclerosis have gene expression patterns unique to pulmonary fibrosis and pulmonary hypertension. Arthritis Rheum. 2011, 63, 783–794. [Google Scholar] [CrossRef]
- Pilewski, J.M.; Liu, L.; Henry, A.C.; Knauer, A.V.; Feghali-Bostwick, C.A. Insulin-like growth factor binding proteins 3 and 5 are overexpressed in idiopathic pulmonary fibrosis and contribute to extracellular matrix deposition. Am. J. Pathol. 2005, 166, 399–407. [Google Scholar] [CrossRef]
- Davis-Turak, J.; Courtney, S.M.; Hazard, E.S.; Glen, W.B.; da Silveira, W.A.; Wesselman, T.; Harbin, L.P.; Wolf, B.J.; Chung, D.; Hardiman, G. Genomics pipelines and data integration: Challenges and opportunities in the research setting. Expert Rev. Mol. Diagn. 2017, 17, 225–237. [Google Scholar] [CrossRef] [PubMed]
- Benjamini, Y.; Hochberg, Y. Controlling the False Discovery Rate: A Practical and Powerful Approach to Multiple Testing. J. R. Stat. Soc. Ser. B (Methodol.) 1995, 57, 289–300. [Google Scholar] [CrossRef]
- Draghici, S.; Khatri, P.; Tarca, A.L.; Amin, K.; Done, A.; Voichita, C.; Georgescu, C.; Romero, R. A systems biology approach for pathway level analysis. Genome Res. 2007, 17, 1537–1545. [Google Scholar] [CrossRef]
- Garrett, S.M.; Baker Frost, D.; Feghali-Bostwick, C. The mighty fibroblast and its utility in scleroderma research. J. Scleroderma Relat. Disord. 2017, 2, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Sargent, J.L.; Milano, A.; Bhattacharyya, S.; Varga, J.; Connolly, M.K.; Chang, H.Y.; Whitfield, M.L. A TGFβ-Responsive Gene Signature Is Associated with a Subset of Diffuse Scleroderma with Increased Disease Severity. J. Investig. Dermatol. 2010, 130, 694–705. [Google Scholar] [CrossRef] [PubMed]
- Milano, A.; Pendergrass, S.A.; Sargent, J.L.; George, L.K.; McCalmont, T.H.; Connolly, M.K.; Whitfield, M.L. Molecular Subsets in the Gene Expression Signatures of Scleroderma Skin. PLoS ONE 2008, 3, e2696. [Google Scholar] [CrossRef]
- Yamaguchi, Y.; Takihara, T.; Chambers, R.A.; Veraldi, K.L.; Larregina, A.T.; Feghali-Bostwick, C.A. A peptide derived from endostatin ameliorates organ fibrosis. Sci. Transl. Med. 2012, 4, 136ra71. [Google Scholar] [CrossRef] [PubMed]
- Yasuoka, H.; Larregina, A.T.; Yamaguchi, Y.; Feghali-Bostwick, C.A. Human skin culture as an ex vivo model for assessing the fibrotic effects of insulin-like growth factor binding proteins. Open Rheumatol. J. 2008, 2, 17–22. [Google Scholar]
- Watanabe, T.; Nishimoto, T.; Mlakar, L.; Heywood, J.; Malaab, M.; Hoffman, S.; Feghali-Bostwick, C. Optimization of a murine and human tissue model to recapitulate dermal and pulmonary features of systemic sclerosis. PLoS ONE 2017, 12, e0179917. [Google Scholar] [CrossRef]
- Kawanabe, Y.; Nauli, S.M. Endothelin. Cell. Mol. Life Sci. 2011, 68, 195–203. [Google Scholar] [CrossRef] [PubMed]
- Leask, A.; Holmes, A.; Abraham, D.J. Connective tissue growth factor: A new and important player in the pathogenesis of fibrosis. Curr. Rheumatol. Rep. 2002, 4, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharyya, S.; Wu, M.; Fang, F.; Tourtellotte, W.; Feghali-Bostwick, C.; Varga, J. Early growth response transcription factors: Key mediators of fibrosis and novel targets for anti-fibrotic therapy. Matrix Biol. 2011, 30, 235–242. [Google Scholar] [CrossRef]
- Brigstock, D.R. Connective tissue growth factor (CCN2, CTGF) and organ fibrosis: Lessons from transgenic animals. J. Cell Commun. Signal. 2010, 4, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharyya, S.; Chen, S.J.; Wu, M.; Warner-Blankenship, M.; Ning, H.; Lakos, G.; Mori, Y.; Chang, E.; Nihijima, C.; Takehara, K.; et al. Smad-independent transforming growth factor-β regulation of early growth response-1 and sustained expression in fibrosis: Implications for scleroderma. Am. J. Pathol. 2008, 173, 1085–1099. [Google Scholar] [CrossRef]
- Ibrahim, M.M.; Chen, L.; Bond, J.E.; Medina, M.A.; Ren, L.; Kokosis, G.; Selim, A.M.; Levinson, H. Myofibroblasts contribute to but are not necessary for wound contraction. Lab. Investig. 2015, 95, 1429–1438. [Google Scholar] [CrossRef] [PubMed]
- Tomasek, J.J.; Haaksma, C.J.; Schwartz, R.J.; Howard, E.W. Whole animal knockout of smooth muscle α-actin does not alter excisional wound healing or the fibroblast-to-myofibroblast transition. Wound Repair Regen. 2013, 21, 166–176. [Google Scholar] [CrossRef] [PubMed]
- Conrad, P.A.; Giuliano, K.A.; Fisher, G.; Collins, K.; Matsudaira, P.T.; Taylor, D.L. Relative distribution of actin, myosin I, and myosin II during the wound healing response of fibroblasts. J. Cell Biol. 1993, 120, 1381–1391. [Google Scholar] [CrossRef] [PubMed]
- Boor, P.; Ostendorf, T.; Floege, J. Renal fibrosis: Novel insights into mechanisms and therapeutic targets. Nat. Rev. Nephrol. 2010, 6, 643–656. [Google Scholar] [CrossRef]
- Heinrich, P.C.; Behrmann, I.; Mϋller-Newen, G.; Schaper, F.; Graeve, L. Interleukin-6-type cytokine signalling through the gp130/Jak/STAT pathway. Biochem. J. 1998, 334 Pt 2, 297–314. [Google Scholar] [CrossRef]
- Chung, C.D.; Liao, J.; Liu, B.; Rao, X.; Jay, P.; Berta, P.; Shuai, K. Specific inhibition of Stat3 signal transduction by PIAS3. Science 1997, 278, 1803–1805. [Google Scholar] [CrossRef] [PubMed]
- Thiery, J.P.; Acloque, H.; Huang, R.Y.; Nieto, M.A. Epithelial-mesenchymal transitions in development and disease. Cell 2009, 139, 871–890. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.K.; Kugler, M.C.; Wolters, P.J.; Robillard, L.; Galvez, M.G.; Brumwell, A.N.; Sheppard, D.; Chapman, H.A. Alveolar epithelial cell mesenchymal transition develops in vivo during pulmonary fibrosis and is regulated by the extracellular matrix. Proc. Natl. Acad. Sci. USA 2006, 103, 13180–13185. [Google Scholar] [CrossRef] [PubMed]
- Mistriotis, P.; Andreadis, T. Hair Follicle: A novel source of multipotent stem cells for tissue engineering and regenerative medicine. Tissue Eng. Part B Rev. 2013, 19, 265–278. [Google Scholar] [CrossRef] [PubMed]
| Symbol | GeneID | Description | Padj | Fold Change |
|---|---|---|---|---|
| COL22A1 | 169044 | collagen, type XXII, alpha 1 | 6.40 × 10−36 | 9.19 |
| PMEPA1 | 56937 | prostate transmembrane protein, androgen induced 1 | 6.36 × 10−33 | 3.51 |
| DPT | 1805 | dermatopontin | 2.89 × 10−29 | 4.69 |
| LTBP2 | 4053 | latent transforming growth factor beta binding protein 2 | 6.31 × 10−26 | 3.18 |
| COL1A1 | 1277 | collagen, type I, alpha 1 | 2.49 × 10−23 | 3.11 |
| FN1 | 2335 | fibronectin 1 | 2.78 × 10−20 | 3.39 |
| MMP10 | 4319 | matrix metallopeptidase 10 | 6.47 × 10−13 | 2.76 |
| COL3A1 | 1281 | collagen, type III, alpha 1 | 5.68 × 10−12 | 2.34 |
| DHRS2 | 10202 | dehydrogenase/reductase (SDR family) member 2 | 6.16 × 10−12 | 4.55 |
| COL5A2 | 1290 | collagen, type V, alpha 2 | 8.53 × 10−12 | 2.36 |
| ITGB6 | 3694 | integrin, beta 6 | 1.66 × 10−11 | 2.94 |
| ADAMTS15 | 170689 | ADAM metallopeptidase with thrombospondin type 1 motif, 15 | 1.77 × 10−11 | 3.55 |
| LRRC15 | 131578 | leucine rich repeat containing 15 | 1.77 × 10−11 | 4.17 |
| TGFBI | 7045 | transforming growth factor, beta-induced, 68kDa | 6.21 × 10−11 | 3.12 |
| MKI67 | 4288 | marker of proliferation Ki-67 | 7.29 × 10−11 | −2.56 |
| COL1A2 | 1278 | collagen, type I, alpha 2 | 8.85 × 10−11 | 2.11 |
| ADAM12 | 8038 | ADAM metallopeptidase domain 12 | 3.00 × 10−10 | 2.71 |
| GLS | 2744 | glutaminase | 3.08 × 10−10 | 2.08 |
| MIAT | 440823 | myocardial infarction associated transcript (non-protein coding) | 3.36 × 10−10 | 3.23 |
| C4orf26 | 152816 | chromosome 4 open reading frame 26 | 3.59 × 10−10 | 4.07 |
| WNT5B | 81029 | wingless-type MMTV integration site family, member 5B | 1.01 × 10−9 | 3.58 |
| KRT77 | 374454 | keratin 77, type II | 3.56 × 10−9 | 2.19 |
| CXCL14 | 9547 | chemokine (C-X-C motif) ligand 14 | 7.49 × 10−9 | 2.61 |
| TPST1 | 8460 | tyrosylprotein sulfotransferase 1 | 8.75 × 10−9 | 2.58 |
| COL15A1 | 1306 | collagen, type XV, alpha 1 | 1.03 × 10−8 | 2.75 |
| SNAI1 | 6615 | snail family zinc finger 1 | 1.04 × 10−8 | 2.65 |
| NKD1 | 85407 | naked cuticle homolog 1 (Drosophila) | 2.62 × 10−8 | 3.41 |
| LDLRAD4 | 753 | low density lipoprotein receptor class A domain containing 4 | 1.43 × 10−7 | 3.30 |
| NPR3 | 4883 | natriuretic peptide receptor 3 | 1.46 × 10−7 | 2.96 |
| DHRS9 | 10170 | dehydrogenase/reductase (SDR family) member 9 | 1.64 × 10−7 | −2.44 |
| COL5A1 | 1289 | collagen, type V, alpha 1 | 2.11 × 10−7 | 2.11 |
| ESM1 | 11082 | endothelial cell-specific molecule 1 | 2.11 × 10−7 | 2.83 |
| DIRAS1 | 148252 | DIRAS family, GTP-binding RAS-like 1 | 2.17 × 10−7 | 2.51 |
| DLGAP5 | 9787 | discs, large (Drosophila) homolog-associated protein 5 | 3.77 × 10−7 | −2.66 |
| RRM2 | 6241 | ribonucleotide reductase M2 | 7.85 × 10−7 | −2.46 |
| TPM1 | 7168 | tropomyosin 1 (alpha) | 7.85 × 10−7 | 2.55 |
| VCAN | 1462 | versican | 8.57 × 10−7 | 2.42 |
| CENPF | 1063 | centromere protein F, 350/400kDa | 9.28 × 10−7 | −2.54 |
| CEP55 | 55165 | centrosomal protein 55kDa | 1.84 × 10−6 | −2.49 |
| SOX9 | 6662 | SRY (sex determining region Y)-box 9 | 1.84 × 10−6 | 1.93 |
| HECW2 | 57520 | HECT, C2 and WW domain containing E3 ubiquitin protein ligase 2 | 2.00 × 10−6 | 2.61 |
| PRSS23 | 11098 | protease, serine, 23 | 2.00 × 10−6 | 2.44 |
| SPRR2D | 6703 | small proline-rich protein 2D | 2.42 × 10−6 | −1.78 |
| GADD45B | 4616 | growth arrest and DNA-damage-inducible, beta | 2.70 × 10−6 | 1.98 |
| KIF4A | 24137 | kinesin family member 4A | 2.84 × 10−6 | −2.55 |
| CACNA1C | 775 | calcium channel, voltage-dependent, L type, alpha 1C subunit | 2.87 × 10−6 | 2.69 |
| LARP6 | 55323 | La ribonucleoprotein domain family, member 6 | 3.68 × 10−6 | 2.23 |
| MMP13 | 4322 | matrix metallopeptidase 13 | 3.83 × 10−6 | 3.02 |
| FGFBP2 | 83888 | fibroblast growth factor binding protein 2 | 5.18 × 10−6 | 2.93 |
| TOP2A | 7153 | topoisomerase (DNA) II alpha 170kDa | 6.21 × 10−6 | −2.37 |
| DNAH17 | 8632 | dynein, axonemal, heavy chain 17 | 7.27 × 10−6 | 1.98 |
| IL11 | 3589 | interleukin 11 | 8.58 × 10−6 | 2.68 |
| EREG | 2069 | epiregulin | 9.06 × 10−6 | −2.16 |
| PHLDB1 | 23187 | pleckstrin homology-like domain, family B, member 1 | 9.42 × 10−6 | 1.95 |
| IQGAP3 | 128239 | IQ motif containing GTPase activating protein 3 | 9.76 × 10−6 | −2.42 |
| A2ML1 | 144568 | alpha-2-macroglobulin-like 1 | 9.83 × 10−6 | −1.84 |
| NDC80 | 10403 | NDC80 kinetochore complex component | 1.02 × 10−5 | −2.57 |
| TROAP | 10024 | trophinin associated protein | 1.20 × 10−5 | −2.45 |
| CDCA8 | 55143 | cell division cycle associated 8 | 1.40 × 10−5 | −2.24 |
| TRIP13 | 9319 | thyroid hormone receptor interactor 13 | 1.89 × 10−5 | −2.33 |
| GPRC5A | 9052 | G protein-coupled receptor, class C, group 5, member A | 2.19 × 10−5 | 2.37 |
| ARL15 | 54622 | ADP-ribosylation factor-like 15 | 2.51 × 10−5 | 2.32 |
| CDC20 | 991 | cell division cycle 20 | 2.68 × 10−5 | −2.48 |
| BIRC5 | 332 | baculoviral IAP repeat containing 5 | 2.69 × 10−5 | −2.34 |
| LYPD1 | 116372 | LY6/PLAUR domain containing 1 | 2.81 × 10−5 | 2.77 |
| DCLK3 | 85443 | doublecortin-like kinase 3 | 2.91 × 10−5 | 2.78 |
| AURKB | 9212 | aurora kinase B | 2.91 × 10−5 | −2.28 |
| MYBL2 | 4605 | v-myb avian myeloblastosis viral oncogene homolog-like 2 | 3.49 × 10−5 | −2.09 |
| MFAP2 | 4237 | microfibrillar-associated protein 2 | 3.53 × 10−5 | 1.88 |
| WNT2 | 7472 | wingless-type MMTV integration site family member 2 | 3.53 × 10−5 | 2.76 |
| S100A7A | 338324 | S100 calcium binding protein A7A | 3.77 × 10−5 | −2.12 |
| NREP | 9315 | neuronal regeneration related protein | 3.86 × 10−5 | 1.92 |
| PKMYT1 | 9088 | protein kinase, membrane associated tyrosine/threonine 1 | 4.74 × 10−5 | −2.07 |
| HMCN2 | 256158 | hemicentin 2 | 5.10 × 10−5 | 2.69 |
| CDC45 | 8318 | cell division cycle 45 | 5.23 × 10−5 | −2.05 |
| TICRR | 90381 | TOPBP1-interacting checkpoint and replication regulator | 6.00 × 10−5 | −2.40 |
| SETBP1 | 26040 | SET binding protein 1 | 6.31 × 10−5 | 1.87 |
| TPX2 | 22974 | TPX2, microtubule-associated | 6.31 × 10−5 | −2.25 |
| KIFC1 | 3833 | kinesin family member C1 | 6.49 × 10−5 | −2.27 |
| CDCA5 | 113130 | cell division cycle associated 5 | 6.62 × 10−5 | −2.12 |
| PRICKLE1 | 144165 | prickle homolog 1 (Drosophila) | 7.37 × 10−5 | 2.23 |
| LBH | 81606 | limb bud and heart development | 8.71 × 10−5 | 2.31 |
| CCL28 | 56477 | chemokine (C-C motif) ligand 28 | 8.81 × 10−5 | 2.48 |
| FAM150B | 285016 | family with sequence similarity 150, member B | 8.81 × 10−5 | 2.65 |
| SKA3 | 221150 | spindle and kinetochore associated complex subunit 3 | 9.14 × 10−5 | −2.41 |
| PRC1 | 9055 | protein regulator of cytokinesis 1 | 9.24 × 10−5 | −2.12 |
| TACC3 | 10460 | transforming, acidic coiled-coil containing protein 3 | 9.34 × 10−5 | −1.96 |
| KIF18B | 146909 | kinesin family member 18B | 1.05 × 10−4 | −2.25 |
| CD83 | 9308 | CD83 molecule | 1.09 × 10−4 | 2.07 |
| TMEM86A | 144110 | transmembrane protein 86A | 1.09 × 10−4 | −1.88 |
| RUNX1 | 861 | runt-related transcription factor 1 | 1.18 × 10−4 | 1.99 |
| ATP12A | 479 | ATPase, H+/K+ transporting, nongastric, alpha polypeptide | 1.25 × 10−4 | −2.26 |
| MAP1B | 4131 | microtubule-associated protein 1B | 1.25 × 10−4 | 1.71 |
| BGN | 633 | biglycan | 1.30 × 10−4 | 2.43 |
| PNMAL1 | 55228 | paraneoplastic Ma antigen family-like 1 | 1.31 × 10−4 | 2.25 |
| TK1 | 7083 | thymidine kinase 1, soluble | 1.42 × 10−4 | −2.08 |
| BMP6 | 654 | bone morphogenetic protein 6 | 1.46 × 10−4 | 2.19 |
| HPSE | 10855 | heparanase | 1.61 × 10−4 | −1.77 |
| SEMA7A | 8482 | semaphorin 7A, GPI membrane anchor (John Milton Hagen blood group) | 1.73 × 10−4 | 1.78 |
| CCL8 | 6355 | chemokine (C-C motif) ligand 8 | 1.82 × 10−4 | −2.56 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Watanabe, T.; Baker Frost, D.; Mlakar, L.; Heywood, J.; da Silveira, W.A.; Hardiman, G.; Feghali-Bostwick, C. A Human Skin Model Recapitulates Systemic Sclerosis Dermal Fibrosis and Identifies COL22A1 as a TGFβ Early Response Gene that Mediates Fibroblast to Myofibroblast Transition. Genes 2019, 10, 75. https://doi.org/10.3390/genes10020075
Watanabe T, Baker Frost D, Mlakar L, Heywood J, da Silveira WA, Hardiman G, Feghali-Bostwick C. A Human Skin Model Recapitulates Systemic Sclerosis Dermal Fibrosis and Identifies COL22A1 as a TGFβ Early Response Gene that Mediates Fibroblast to Myofibroblast Transition. Genes. 2019; 10(2):75. https://doi.org/10.3390/genes10020075
Chicago/Turabian StyleWatanabe, Tomoya, DeAnna Baker Frost, Logan Mlakar, Jonathan Heywood, Willian A. da Silveira, Gary Hardiman, and Carol Feghali-Bostwick. 2019. "A Human Skin Model Recapitulates Systemic Sclerosis Dermal Fibrosis and Identifies COL22A1 as a TGFβ Early Response Gene that Mediates Fibroblast to Myofibroblast Transition" Genes 10, no. 2: 75. https://doi.org/10.3390/genes10020075
APA StyleWatanabe, T., Baker Frost, D., Mlakar, L., Heywood, J., da Silveira, W. A., Hardiman, G., & Feghali-Bostwick, C. (2019). A Human Skin Model Recapitulates Systemic Sclerosis Dermal Fibrosis and Identifies COL22A1 as a TGFβ Early Response Gene that Mediates Fibroblast to Myofibroblast Transition. Genes, 10(2), 75. https://doi.org/10.3390/genes10020075






