NKG2D Natural Killer Cell Receptor—A Short Description and Potential Clinical Applications
Abstract
1. Introduction
1.1. NK Cells and Their Receptors
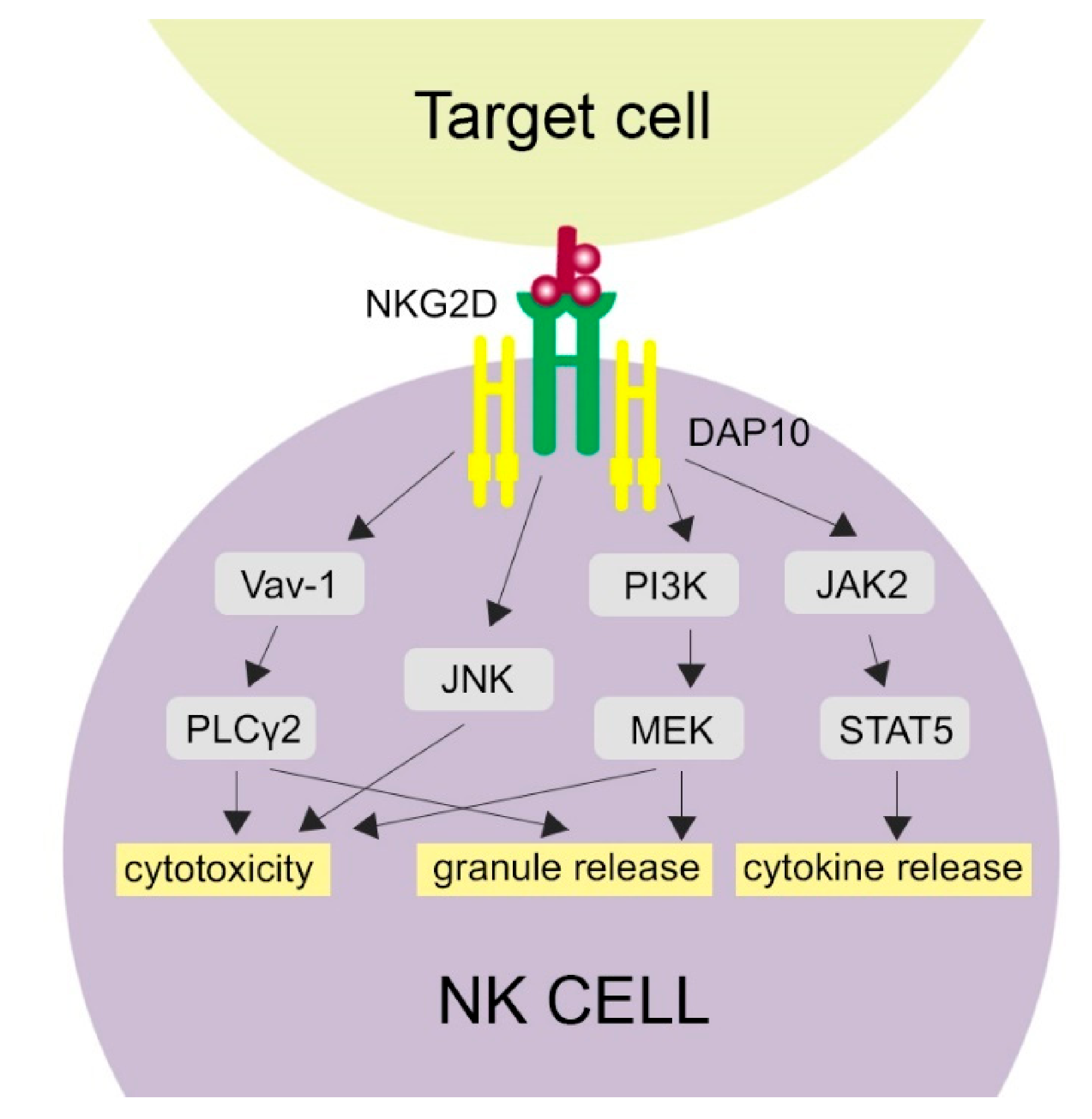
1.2. NKG2D and Its Ligands
2. Variability of the NKG2D Gene—Its Functional Effect and Clinical Associations
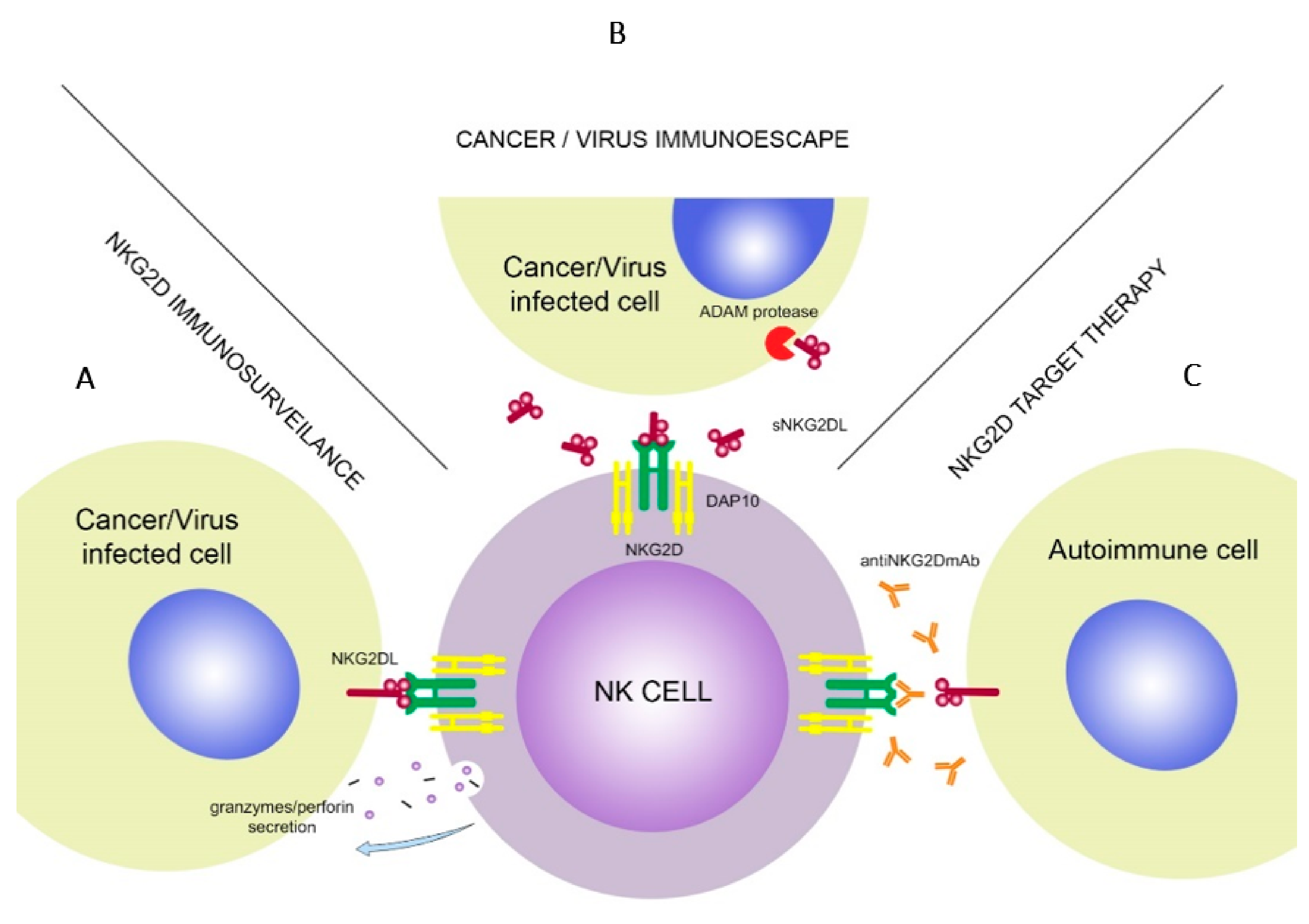
3. Multiple Functions of the Activating NKG2D Receptor—Clinical Implications and Application for Treatment
3.1. Cancers and Cancer Immunotherapy
Hematologic Malignancies
3.2. Transplantation
3.3. Viral Infections
NKG2D and its Role in SARS-CoV-2 Infection
3.4. Inflammatory and Autoimmune Diseases
3.5. Pregnancy Miscarriage
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Caligiuri, M.A. Human Natural Killer Cells. Blood 2008, 112, 461–469. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Wang, S.; Xin, J.; Wang, J.; Yao, C.; Zhang, Z. Role of NKG2D and Its Ligands in Cancer Immunotherapy. Am. J. Cancer Res. 2019, 9, 2064–2078. [Google Scholar] [PubMed]
- Stewart, C.A.; Vivier, E.; Colonna, M. Strategies of Natural Killer Cell Recognition and Signaling. In Immunobiology of Natural Killer Cell Receptors; Vivier, E., Colonna, M., Eds.; Springer: Berlin/Heidelberg, Germany, 2006; Volume 298, pp. 1–21. [Google Scholar]
- Dogra, P.; Rancan, C.; Ma, W.; Toth, M.; Senda, T.; Carpenter, D.J.; Kubota, M.; Matsumoto, R.; Thapa, P.; Szabo, P.A.; et al. Tissue Determinants of Human NK Cell Development, Function, and Residence. Cell 2020, 180, 749–763.e13. [Google Scholar] [CrossRef] [PubMed]
- Vivier, E.; Tomasello, E.; Baratin, M.; Walzer, T.; Ugolini, S. Functions of Natural Killer Cells. Nat. Immunol. 2008, 9, 503–510. [Google Scholar] [CrossRef]
- Ljunggren, H.G.; Karre, K. In Search of the ‘Missing Self’: MHC Molecules and NK Cell Recognition. Immunol. Today 1990, 11, 237–244. [Google Scholar] [CrossRef]
- Cooley, S.; Parham, P.; Miller, J.S. Strategies to Activate NK Cells to Prevent Relapse and Induce Remission Following Hematopoietic Stem Cell Transplantation. Blood 2018, 131, 1053–1062. [Google Scholar] [CrossRef]
- Jelenčić, V.; Lenartić, M.; Wensveen, F.M.; Polić, B. NKG2D: A Versatile Player in the Immune System. Immunol. Lett. 2017, 189, 48–53. [Google Scholar] [CrossRef]
- Oldham, R.K.; Siwarski, D.; McCoy, J.L.; Plata, E.J.; Herberman, R.B. Evaluation of a Cell-Mediated Cytotoxicity Assay Utilizing 125 Iododeoxyuridine-Labeled Tissue-Culture Target Cells. Natl. Cancer Inst. Monogr. 1973, 37, 49–58. [Google Scholar]
- Herberman, R.B.; Nunn, M.E.; Lavrin, D.H. Natural Cytotoxic Reactivity of Mouse Lymphoid Cells against Syngeneic and Allogeneic Tumors. I. Distribution of Reactivity and Specificity. Int. J. Cancer 1975, 16, 216–229. [Google Scholar] [CrossRef]
- Abel, A.M.; Yang, C.; Thakar, M.S.; Malarkannan, S. Natural Killer Cells: Development, Maturation, and Clinical Utilization. Front. Immunol. 2018, 9, 1869. [Google Scholar] [CrossRef]
- Vuletić, A.; Jurišić, V.; Jovanić, I.; Milovanović, Z.; Nikolić, S.; Konjević, G. Distribution of Several Activating and Inhibitory Receptors on CD3−CD56+ NK Cells in Regional Lymph Nodes of Melanoma Patients. J. Surg. Res. 2013, 183, 860–868. [Google Scholar] [CrossRef]
- Cooper, M.A.; Fehniger, T.A.; Caligiuri, M.A. The Biology of Human Natural Killer-Cell Subsets. Trends Immunol. 2001, 22, 633–640. [Google Scholar] [CrossRef]
- Mirjačić Martinović, K.M.; Babović, N.L.; Džodić, R.R.; Jurišić, V.B.; Tanić, N.T.; Konjević, G.M. Decreased Expression of NKG2D, NKp46, DNAM-1 Receptors, and Intracellular Perforin and STAT-1 Effector Molecules in NK Cells and Their Dim and Bright Subsets in Metastatic Melanoma Patients. Melanoma Res. 2014, 24, 295–304. [Google Scholar] [CrossRef]
- Merkt, W.; Salzer, U.; Thiel, J.; Jandova, I.; Bergner, R.; Venhoff, A.C.; Venhoff, N. Blood CD3-(CD56 or 16)+ Natural Killer Cell Distributions Are Heterogeneous in Healthy Adults and Suppressed by Azathioprine in Patients with ANCA-Associated Vasculitides. BMC Immunol. 2021, 22, 26. [Google Scholar] [CrossRef]
- Pende, D.; Falco, M.; Vitale, M.; Cantoni, C.; Vitale, C.; Munari, E.; Bertaina, A.; Moretta, F.; Del Zotto, G.; Pietra, G.; et al. Killer Ig-Like Receptors (KIRs): Their Role in NK Cell Modulation and Developments Leading to Their Clinical Exploitation. Front. Immunol. 2019, 10, 1179. [Google Scholar] [CrossRef]
- Husain, Z.; Alper, C.A.; Yunis, E.J.; Dubey, D.P. Complex Expression of Natural Killer Receptor Genes in Single Natural Killer Cells. Immunology 2002, 106, 373–380. [Google Scholar] [CrossRef]
- Thielens, A.; Vivier, E.; Romagné, F. NK Cell MHC Class I Specific Receptors (KIR): From Biology to Clinical Intervention. Curr. Opin. Immunol. 2012, 24, 239–245. [Google Scholar] [CrossRef]
- Bogunia-Kubik, K.; Łacina, P. Non-KIR NK Cell Receptors: Role in Transplantation of Allogeneic Haematopoietic Stem Cells. Int. J. Immunogenet. 2021, 48, 157–171. [Google Scholar] [CrossRef]
- Biassoni, R.; Malnati, M.S. Human Natural Killer Receptors, Co-Receptors, and Their Ligands. Curr. Protoc. Immunol. 2018, 121. [Google Scholar] [CrossRef]
- Brown, D.P.; Jones, D.C.; Anderson, K.J.; Lapaque, N.; Buerki, R.A.; Trowsdale, J.; Allen, R.L. The Inhibitory Receptor LILRB4 (ILT3) Modulates Antigen Presenting Cell Phenotype and, along with LILRB2 (ILT4), Is Upregulated in Response to Salmonella Infection. BMC Immunol. 2009, 10, 56. [Google Scholar] [CrossRef]
- Becker, P.S.A.; Suck, G.; Nowakowska, P.; Ullrich, E.; Seifried, E.; Bader, P.; Tonn, T.; Seidl, C. Selection and Expansion of Natural Killer Cells for NK Cell-Based Immunotherapy. Cancer Immunol. Immunother. 2016, 65, 477–484. [Google Scholar] [CrossRef]
- Paul, P.; Pedini, P.; Lyonnet, L.; Di Cristofaro, J.; Loundou, A.; Pelardy, M.; Basire, A.; Dignat-George, F.; Chiaroni, J.; Thomas, P.; et al. FCGR3A and FCGR2A Genotypes Differentially Impact Allograft Rejection and Patients’ Survival After Lung Transplant. Front. Immunol. 2019, 10, 1208. [Google Scholar] [CrossRef]
- Carrington, M.; Norman, P. The KIR Gene Cluster; Bethesda (MD): National Center for Biotechnology Information (US). 2003. Available online: https://www.ncbi.nlm.nih.gov/books/NBK10135/ (accessed on 18 January 2021).
- Huang, H.; Wang, X.; Zhang, Y.; Zheng, Z.; Wei, H.; Sun, R. Up-Regulation of NKG2F Receptor, a Functionally Unknown Killer Receptor, of Human Natural Killer Cells by Interleukin-2 and Interleukin-15. Oncol. Rep. 2010, 24, 1043–1048. [Google Scholar] [CrossRef]
- Perez, C.; Prajapati, K.; Burke, B.; Plaza-Rojas, L.; Zeleznik-Le, N.J.; Guevara-Patino, J.A. NKG2D Signaling Certifies Effector CD8 T Cells for Memory Formation. J. Immunother. Cancer 2019, 7, 48. [Google Scholar] [CrossRef]
- Orbelyan, G.A.; Tang, F.; Sally, B.; Solus, J.; Meresse, B.; Ciszewski, C.; Grenier, J.-C.; Barreiro, L.B.; Lanier, L.L.; Jabri, B. Human NKG2E Is Expressed and Forms an Intracytoplasmic Complex with CD94 and DAP12. J. Immunol. 2014, 193, 610–616. [Google Scholar] [CrossRef]
- Barrow, A.D.; Martin, C.J.; Colonna, M. The Natural Cytotoxicity Receptors in Health and Disease. Front. Immunol. 2019, 10, 909. [Google Scholar] [CrossRef]
- Allcock, R.J.N.; Barrow, A.D.; Forbes, S.; Beck, S.; Trowsdale, J. The Human TREM Gene Cluster at 6p21.1 Encodes Both Activating and Inhibitory Single IgV Domain Receptors and Includes NKp44. Eur. J. Immunol. 2003, 33, 567–577. [Google Scholar] [CrossRef]
- Wende, H.; Volz, A.; Ziegler, A. Extensive Gene Duplications and a Large Inversion Characterize the Human Leukocyte Receptor Cluster. Immunogenetics 2000, 51, 703–713. [Google Scholar] [CrossRef]
- Borrego, F.; Masilamani, M.; Marusina, A.I.; Tang, X.; Coligan, J.E. The CD94/NKG2 Family of Receptors: From Molecules and Cells to Clinical Relevance. IR 2006, 35, 263–278. [Google Scholar] [CrossRef]
- Van der Touw, W.; Chen, H.-M.; Pan, P.-Y.; Chen, S.-H. LILRB Receptor-Mediated Regulation of Myeloid Cell Maturation and Function. Cancer Immunol. Immunother. 2017, 66, 1079–1087. [Google Scholar] [CrossRef]
- Hikami, K.; Tsuchiya, N.; Yabe, T.; Tokunaga, K. Variations of Human Killer Cell Lectin-like Receptors: Common Occurrence of NKG2-C Deletion in the General Population. Genes Immun. 2003, 4, 160–167. [Google Scholar] [CrossRef] [PubMed]
- Lieto, L.D.; Maasho, K.; West, D.; Borrego, F.; Coligan, J.E. The Human CD94 Gene Encodes Multiple, Expressible Transcripts Including a New Partner of NKG2A/B. Genes Immun. 2006, 7, 36–43. [Google Scholar] [CrossRef] [PubMed]
- Iwaszko, M.; Bogunia-Kubik, K. Clinical Significance of the HLA-E and CD94/NKG2 Interaction. Arch. Immunol. Ther. Exp. 2011, 59, 353–367. [Google Scholar] [CrossRef] [PubMed]
- Kordelas, L.; Steckel, N.-K.; Horn, P.A.; Beelen, D.W.; Rebmann, V. The Activating NKG2C Receptor Is Significantly Reduced in NK Cells after Allogeneic Stem Cell Transplantation in Patients with Severe Graft-versus-Host Disease. Int. J. Mol. Sci. 2016, 17, 1797. [Google Scholar] [CrossRef]
- Bauer, S.; Groh, V.; Wu, J.; Steinle, A.; Phillips, J.H.; Lanier, L.L.; Spies, T. Activation of NK Cells and T Cells by NKG2D, a Receptor for Stress-Inducible MICA. Science 1999, 285, 727–729. [Google Scholar] [CrossRef]
- Dukovska, D.; Fernández-Soto, D.; Valés-Gómez, M.; Reyburn, H.T. NKG2H-Expressing T Cells Negatively Regulate Immune Responses. Front. Immunol. 2018, 9, 390. [Google Scholar] [CrossRef]
- Spear, P.; Wu, M.-R.; Sentman, M.-L.; Sentman, C.L. NKG2D Ligands as Therapeutic Targets. Cancer Immun. 2013, 13, 8. [Google Scholar]
- Wensveen, F.M.; Jelenčić, V.; Polić, B. NKG2D: A Master Regulator of Immune Cell Responsiveness. Front. Immunol. 2018, 9, 441. [Google Scholar] [CrossRef]
- Lanier, L.L. NKG2D Receptor and Its Ligands in Host Defense. Cancer Immunol. Res. 2015, 3, 575–582. [Google Scholar] [CrossRef]
- González, S.; López-Soto, A.; Suarez-Alvarez, B.; López-Vázquez, A.; López-Larrea, C. NKG2D Ligands: Key Targets of the Immune Response. Trends Immunol. 2008, 29, 397–403. [Google Scholar] [CrossRef]
- Campos-Silva, C.; Kramer, M.K.; Valés-Gómez, M. NKG2D-Ligands: Putting Everything under the Same Umbrella Can Be Misleading. HLA 2018, 91, 489–500. [Google Scholar] [CrossRef]
- Schmiedel, D.; Mandelboim, O. NKG2D Ligands–Critical Targets for Cancer Immune Escape and Therapy. Front. Immunol. 2018, 9, 2040. [Google Scholar] [CrossRef]
- Li, P.; Morris, D.L.; Willcox, B.E.; Steinle, A.; Spies, T.; Strong, R.K. Complex Structure of the Activating Immunoreceptor NKG2D and Its MHC Class I–like Ligand MICA. Nat. Immunol. 2001, 2, 443–451. [Google Scholar] [CrossRef]
- Risti, M.; Bicalho, M.D. MICA and NKG2D: Is There an Impact on Kidney Transplant Outcome? Front. Immunol. 2017, 8. [Google Scholar] [CrossRef]
- Garrity, D.; Call, M.E.; Feng, J.; Wucherpfennig, K.W. The Activating NKG2D Receptor Assembles in the Membrane with Two Signaling Dimers into a Hexameric Structure. Proc. Natl. Acad. Sci. USA 2005, 102, 7641–7646. [Google Scholar] [CrossRef]
- Diefenbach, A.; Tomasello, E.; Lucas, M.; Jamieson, A.M.; Hsia, J.K.; Vivier, E.; Raulet, D.H. Selective Associations with Signaling Proteins Determine Stimulatory versus Costimulatory Activity of NKG2D. Nat. Immunol. 2002, 3, 1142–1149. [Google Scholar] [CrossRef]
- Gilfillan, S.; Ho, E.L.; Cella, M.; Yokoyama, W.M.; Colonna, M. NKG2D Recruits Two Distinct Adapters to Trigger NK Cell Activation and Costimulation. Nat. Immunol. 2002, 3, 1150–1155. [Google Scholar] [CrossRef]
- Rosen, D.B.; Araki, M.; Hamerman, J.A.; Chen, T.; Yamamura, T.; Lanier, L.L. A Structural Basis for the Association of DAP12 with Mouse, but Not Human, NKG2D. J. Immunol. 2004, 173, 2470–2478. [Google Scholar] [CrossRef]
- Xu, H. Expressions of Natural Cytotoxicity Receptor, NKG2D and NKG2D Ligands in Endometriosis. J. Reprod. Immunol. 2019, 136, 102615. [Google Scholar] [CrossRef]
- Diefenbach, A.; Hsia, J.K.; Hsiung, M.-Y.B.; Raulet, D.H. A Novel Ligand for the NKG2D Receptor Activates NK Cells and Macrophages and Induces Tumor Immunity. Eur. J. Immunol. 2003, 33, 381–391. [Google Scholar] [CrossRef]
- Poggi, A.; Prevosto, C.; Massaro, A.-M.; Negrini, S.; Urbani, S.; Pierri, I.; Saccardi, R.; Gobbi, M.; Zocchi, M.R. Interaction between Human NK Cells and Bone Marrow Stromal Cells Induces NK Cell Triggering: Role of NKp30 and NKG2D Receptors. J. Immunol. 2005, 175, 6352–6360. [Google Scholar] [CrossRef]
- Burgess, S.J.; Maasho, K.; Masilamani, M.; Narayanan, S.; Borrego, F.; Coligan, J.E. The NKG2D Receptor: Immunobiology and Clinical Implications. Immunol. Res. 2008, 40, 18–34. [Google Scholar] [CrossRef]
- Groh, V.; Bahram, S.; Bauer, S.; Herman, A.; Beauchamp, M.; Spies, T. Cell Stress-Regulated Human Major Histocompatibility Complex Class I Gene Expressed in Gastrointestinal Epithelium. Proc. Natl. Acad. Sci. USA 1996, 93, 12445–12450. [Google Scholar] [CrossRef]
- Zhao, Y.; Chen, N.; Yu, Y.; Zhou, L.; Niu, C.; Liu, Y.; Tian, H.; Lv, Z.; Han, F.; Cui, J. Prognostic Value of MICA/B in Cancers: A Systematic Review and Meta-Analysis. Oncotarget 2017, 8, 96384–96395. [Google Scholar] [CrossRef] [PubMed]
- Hayashi, T.; Imai, K.; Morishita, Y.; Hayashi, I.; Kusunoki, Y.; Nakachi, K. Identification of the NKG2D Haplotypes Associated with Natural Cytotoxic Activity of Peripheral Blood Lymphocytes and Cancer Immunosurveillance. Cancer Res. 2006, 66, 563–570. [Google Scholar] [CrossRef] [PubMed]
- Sherry, S.T.; Ward, M.H.; Kholodov, M.; Baker, J.; Phan, L.; Smigielski, E.M.; Sirotkin, K. dbSNP: The NCBI database of genetic variation. Nucleic Acids Res. 2001, 29, 308–311. [Google Scholar] [CrossRef]
- Furue, H.; Matsuo, K.; Kumimoto, H.; Hiraki, A.; Suzuki, T.; Yatabe, Y.; Komori, K.; Kanemitsu, Y.; Hirai, T.; Kato, T.; et al. Decreased Risk of Colorectal Cancer with the High Natural Killer Cell Activity NKG2D Genotype in Japanese. Carcinogenesis 2008, 29, 316–320. [Google Scholar] [CrossRef] [PubMed]
- Ghobadzadeh, S.; Shams, A.; Eslami, G.; Mirghanizadeh, A. Investigation of NKG2D Rs1049174G>C Gene Polymorphism in Women with Breast Cancer. JSSU 2013, 21, 291–299. [Google Scholar]
- Zheng, W.; Li, H.; Liu, B.; Wu, C. Association between the SNPs in Trace Element-Related Metabolic Genes and the Risk of Gastric Cancer: A Case-Control Study in Xianyou of China. J. Genet. 2019, 98. [Google Scholar] [CrossRef]
- Hara, R.; Onizuka, M.; Matsusita, E.; Kikkawa, E.; Nakamura, Y.; Matsushita, H.; Ohgiya, D.; Murayama, H.; Machida, S.; Ohmachi, K.; et al. NKG2D Gene Polymorphisms Are Associated with Disease Control of Chronic Myeloid Leukemia by Dasatinib. Int. J. Hematol. 2017, 106, 666–674. [Google Scholar] [CrossRef]
- Fechtenbaum, M.; Desoutter, J.; Delvallez, G.; Brochot, E.; Guillaume, N.; Goëb, V. MICA and NKG2D Variants as Risk Factors in Spondyloarthritis: A Case-Control Study. Genes Immun. 2019, 20, 599–605. [Google Scholar] [CrossRef]
- Iwaszko, M.; Świerkot, J.; Kolossa, K.; Jeka, S.; Wiland, P.; Bogunia-Kubik, K. Influence of NKG2D Genetic Variants on Response to Anti-TNF Agents in Patients with Rheumatoid Arthritis. Genes 2018, 9, 64. [Google Scholar] [CrossRef]
- Wielińska, J.; Tarassi, K.; Iwaszko, M.; Kościńska, K.; Wysoczańska, B.; Mole, E.; Kitsiou, V.; Świerkot, J.; Kolossa, K.; Kouniaki, D.; et al. Shared epitope and polymorphism of MICA and NKG2D encoding genes in Greek and Polish patients with rheumatoid arthritis. Cent. Eur. J. Immunol. 2021, 46. [Google Scholar] [CrossRef]
- Espinoza, J.L.; Nguyen, V.H.; Ichimura, H.; Pham, T.T.T.; Nguyen, C.H.; Pham, T.V.; Elbadry, M.I.; Yoshioka, K.; Tanaka, J.; Trung, L.Q.; et al. A Functional Polymorphism in the NKG2D Gene Modulates NK-Cell Cytotoxicity and Is Associated with Susceptibility to Human Papilloma Virus-Related Cancers. Sci. Rep. 2016, 6, 39231. [Google Scholar] [CrossRef]
- Viet, N.H.; Trung, N.Q.; Dong, L.T.; Trung, L.Q.; Espinoza, J.L. Genetic Variants in NKG2D Axis and Susceptibility to Epstein-Barr Virus-Induced Nasopharyngeal Carcinoma. J. Cancer Res. Clin. Oncol. 2021, 147, 713–723. [Google Scholar] [CrossRef]
- Asadi-Saghandi, A.; Shams, A.; Eslami, G.; Mirghanizadeh, S.A.; Eskandari-Nasab, E. Peginterferon Alfa-2a/Ribavirin Treatment Efficacy in Chronic Hepatitis C Patients Is Related to Natural Killer Group 2D Gene Rs1049174 GC Polymorphism. Virusdisease 2016, 27, 369–374. [Google Scholar] [CrossRef]
- Rohn, H.; Tomoya Michita, R.; Schwich, E.; Dolff, S.; Gäckler, A.; Trilling, M.; Le-Trilling, V.T.K.; Wilde, B.; Korth, J.; Heinemann, F.M.; et al. The Donor Major Histocompatibility Complex Class I Chain-Related Molecule A Allele Rs2596538 G Predicts Cytomegalovirus Viremia in Kidney Transplant Recipients. Front. Immunol. 2018, 9, 917. [Google Scholar] [CrossRef]
- Espinoza, J.L.; Takami, A.; Onizuka, M.; Sao, H.; Akiyama, H.; Miyamura, K.; Okamoto, S.; Inoue, M.; Kanda, Y.; Ohtake, S.; et al. NKG2D Gene Polymorphism Has a Significant Impact on Transplant Outcomes after HLA-Fully-Matched Unrelated Bone Marrow Transplantation for Standard Risk Hematologic Malignancies. Haematologica 2009, 94, 1427–1434. [Google Scholar] [CrossRef]
- Asl, A.A.; Nezamdoust, F.V.; Fesahat, F.; Astani, A.; Barati, M.; Raee, P.; Asadi-Saghandi, A. Association between Rs1049174 NKG2D Gene Polymorphism and Idiopathic Recurrent Spontaneous Abortion in Iranian Women: A Case-Control Study. J. Obstet. Gynaecol. 2020, 1–5. [Google Scholar] [CrossRef]
- Piotrowski, P.; Lianeri, M.; Olesińska, M.; Jagodziński, P.P. Prevalence of the NKG2D Thr72Ala Polymorphism in Patients with Systemic Lupus Erythematosus. Mol. Biol. Rep. 2012, 39, 1343–1347. [Google Scholar] [CrossRef]
- Kabalak, G.; Thomas, R.M.; Martin, J.; Ortego-Centeno, N.; Jimenez-Alonso, J.; de Ramón, E.; Buyny, S.; Hamsen, S.; Gross, W.L.; Schnarr, S.; et al. Association of an NKG2D Gene Variant with Systemic Lupus Erythematosus in Two Populations. Hum. Immunol. 2010, 71, 74–78. [Google Scholar] [CrossRef] [PubMed]
- Park, K.S.; Park, J.H.; Song, Y.W. Inhibitory NKG2A and Activating NKG2D and NKG2C Natural Killer Cell Receptor Genes: Susceptibility for Rheumatoid Arthritis. Tissue Antigens 2008, 72, 342–346. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.-C.; Wu, I.-C.; Chiu, Y.-C.; Tseng, K.-C.; Chen, C.-Y.; Chiu, H.-C.; Cheng, P.-N.; Chang, T.-T. Genotyping of Immune-Related Loci Associated with Delayed HBeAg Seroconversion in Immune-Active Chronic Hepatitis B Patients. Antiviral Res. 2020, 176, 104719. [Google Scholar] [CrossRef] [PubMed]
- Taniguchi, R.; Koyano, S.; Suzutani, T.; Goishi, K.; Ito, Y.; Morioka, I.; Nakamura, H.; Yamada, H.; Oka, A.; Inoue, N. A Thr72Ala Polymorphism in the NKG2D Gene Is Associated with Early Symptomatic Congenital Cytomegalovirus Disease. Infection 2015, 43, 353–359. [Google Scholar] [CrossRef]
- Roszak, A.; Lianeri, M.; Jagodziński, P.P. Prevalence of the NKG2D Thr72Ala Polymorphism in Patients with Cervical Carcinoma. Genet. Test. Mol. Biomark. 2012, 16, 841–845. [Google Scholar] [CrossRef]
- Ma, J.; Guo, X.; Wu, X.; Li, J.; Zhu, X.; Li, Z.; Li, J.; Pan, L.; Li, T.; Li, H.; et al. Association of NKG2D Genetic Polymorphism with Susceptibility to Chronic Hepatitis B in a Han Chinese Population. J. Med. Virol. 2010, 82, 1501–1507. [Google Scholar] [CrossRef]
- Tozatto-Maio, K.; Girot, R.; Ly, I.D.; Silva Pinto, A.C.; Rocha, V.; Fernandes, F.; Diagne, I.; Benzerara, Y.; Dinardo, C.L.; Soler, J.P.; et al. Polymorphisms in Inflammatory Genes Modulate Clinical Complications in Patients With Sickle Cell Disease. Front. Immunol. 2020, 11, 2041. [Google Scholar] [CrossRef]
- Mariaselvam, C.M.; Tamouza, R.; Krishnamoorthy, R.; Charron, D.; Misra, D.P.; Jain, V.K.; Negi, V.S. Association of NKG2D Gene Variants with Susceptibility and Severity of Rheumatoid Arthritis. Clin. Exp. Immunol. 2017, 187, 369–375. [Google Scholar] [CrossRef]
- Hizem, S.; Mtiraoui, N.; Massaoudi, S.; Fortier, C.; Boukouaci, W.; Kahina, A.; Charron, D.; Mahjoub, T.; Tamouza, R. Polymorphisms in Genes Coding for the NK-Cell Receptor NKG2D and Its Ligand MICA in Recurrent Miscarriage. Am. J. Reprod. Immunol. 2014, 72, 577–585. [Google Scholar] [CrossRef]
- Wadsworth, C.A.; Dixon, P.H.; Taylor-Robinson, S.; Kim, J.U.; Zabron, A.A.; Wong, J.H.; Chapman, M.H.; McKay, S.C.; Spalding, D.R.; Wasan, H.S.; et al. Polymorphisms in Natural Killer Cell Receptor Protein 2D (NKG2D) as a Risk Factor for Cholangiocarcinoma. J. Clin. Exp. Hepatol. 2019, 9, 171–175. [Google Scholar] [CrossRef]
- Pu, X.; Hildebrandt, M.A.; Lu, C.; Roth, J.A.; Stewart, D.J.; Zhao, Y.; Heist, R.S.; Ye, Y.; Chang, D.W.; Su, L.; et al. Inflammation-Related Genetic Variations and Survival in Patients with Advanced Non-Small Cell Lung Cancer Receiving First-Line Chemotherapy. Clin. Pharmacol. Ther. 2014, 96, 360–369. [Google Scholar] [CrossRef]
- Pasanen, A.; Karjalainen, M.K.; Kummola, L.; Waage, J.; Bønnelykke, K.; Ruotsalainen, M.; Piippo-Savolainen, E.; Goksör, E.; Nuolivirta, K.; Chawes, B.; et al. NKG2D Gene Variation and Susceptibility to Viral Bronchiolitis in Childhood. Pediatr. Res. 2018, 84, 451–457. [Google Scholar] [CrossRef]
- Melum, E.; Karlsen, T.H.; Schrumpf, E.; Bergquist, A.; Thorsby, E.; Boberg, K.M.; Lie, B.A. Cholangiocarcinoma in Primary Sclerosing Cholangitis Is Associated with NKG2D Polymorphisms. Hepatology 2008, 47, 90–96. [Google Scholar] [CrossRef]
- Sikora, M.; Laayouni, H.; Menendez, C.; Mayor, A.; Bardaji, A.; Sigauque, B.; Netea, M.G.; Casals, F.; Bertranpetit, J. A Targeted Association Study of Immunity Genes and Networks Suggests Novel Associations with Placental Malaria Infection. PLoS ONE 2011, 6, e24996. [Google Scholar] [CrossRef]
- Gimeno, L.; Martínez-Banaclocha, H.; Bernardo, M.V.; Bolarin, J.M.; Marín, L.; López-Hernández, R.; López-Alvarez, M.R.; Moya-Quiles, M.R.; Muro, M.; Frias-Iniesta, J.F.; et al. NKG2D Polymorphism in Melanoma Patients from Southeastern Spain. Cancers 2019, 11, 438. [Google Scholar] [CrossRef]
- Imai, K.; Matsuyama, S.; Miyake, S.; Suga, K.; Nakachi, K. Natural Cytotoxic Activity of Peripheral-Blood Lymphocytes and Cancer Incidence: An 11-Year Follow-up Study of a General Population. Lancet 2000, 356, 1795–1799. [Google Scholar] [CrossRef]
- Imai, K.; Hayashi, T.; Yamaoka, M.; Kajimura, J.; Yoshida, K.; Kusunoki, Y.; Nakachi, K. Effects of NKG2D Haplotypes on the Cell-Surface Expression of NKG2D Protein on Natural Killer and CD8 T Cells of Peripheral Blood among Atomic-Bomb Survivors. Hum. Immunol. 2012, 73, 686–691. [Google Scholar] [CrossRef]
- Espinoza, J.L.; Takami, A.; Yoshioka, K.; Nakata, K.; Sato, T.; Kasahara, Y.; Nakao, S. Human MicroRNA-1245 down-Regulates the NKG2D Receptor in Natural Killer Cells and Impairs NKG2D-Mediated Functions. Haematologica 2012, 97, 1295–1303. [Google Scholar] [CrossRef]
- Peralta-Zaragoza, O.; Bermúdez-Morales, V.; Gutiérrez-Xicotencatl, L.; Alcocer-González, J.; Recillas-Targa, F.; Madrid-Marina, V. E6 and E7 Oncoproteins from Human Papillomavirus Type 16 Induce Activation of Human Transforming Growth Factor Beta1 Promoter throughout Sp1 Recognition Sequence. Viral Immunol. 2006, 19, 468–480. [Google Scholar] [CrossRef]
- Lee, J.-C.; Lee, K.-M.; Kim, D.-W.; Heo, D.S. Elevated TGF-Beta1 Secretion and down-Modulation of NKG2D Underlies Impaired NK Cytotoxicity in Cancer Patients. J. Immunol. 2004, 172, 7335–7340. [Google Scholar] [CrossRef]
- Vazquez-Gonzalez, W.G.; Martinez-Alvarez, J.C.; Arrazola-Garcia, A.; Perez-Rodriguez, M. Haplotype Block 1 Variant (HB-1v) of the NKG2 Family of Receptors. Hum. Immunol. 2019, 80, 842–847. [Google Scholar] [CrossRef] [PubMed]
- Lin, F.; Dai, C.; Ge, X.; Tang, W.; Lin, Y.; Wang, Y.; Li, J. Prognostic Significance and Functional Implication of Immune Activating Receptor NKG2D in Gastric Cancer. Biochem. Biophys. Res. Commun. 2017, 487, 619–624. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Sun, M.; Yu, S.; Liu, K.; Li, X.; Shi, H. Potential Therapeutic Strategy for Gastric Cancer Peritoneal Metastasis by NKG2D Ligands-Specific T Cells. OncoTargets Ther. 2015, 8, 3095–3104. [Google Scholar] [CrossRef]
- Sheppard, S.; Ferry, A.; Guedes, J.; Guerra, N. The Paradoxical Role of NKG2D in Cancer Immunity. Front. Immunol. 2018, 9, 1808. [Google Scholar] [CrossRef]
- Hwang, S.; Han, J.; Baek, J.-S.; Tak, E.; Song, G.-W.; Lee, S.-G.; Jung, D.-H.; Park, G.-C.; Ahn, C.-S.; Kim, N. Cytotoxicity of Human Hepatic Intrasinusoidal CD56bright Natural Killer Cells against Hepatocellular Carcinoma Cells. IJMS 2019, 20, 1564. [Google Scholar] [CrossRef]
- Wang, J.; Li, C.-D.; Sun, L. Recent Advances in Molecular Mechanisms of the NKG2D Pathway in Hepatocellular Carcinoma. Biomolecules 2020, 10, 301. [Google Scholar] [CrossRef]
- Sheppard, S.; Guedes, J.; Mroz, A.; Zavitsanou, A.-M.; Kudo, H.; Rothery, S.M.; Angelopoulos, P.; Goldin, R.; Guerra, N. The Immunoreceptor NKG2D Promotes Tumour Growth in a Model of Hepatocellular Carcinoma. Nat. Commun. 2017, 8, 13930. [Google Scholar] [CrossRef]
- Huergo-Zapico, L.; Acebes-Huerta, A.; López-Soto, A.; Villa-Álvarez, M.; Gonzalez-Rodriguez, A.P.; Gonzalez, S. Molecular Bases for the Regulation of NKG2D Ligands in Cancer. Front. Immunol. 2014, 5, 106. [Google Scholar] [CrossRef]
- Salih, H.R.; Antropius, H.; Gieseke, F.; Lutz, S.Z.; Kanz, L.; Rammensee, H.-G.; Steinle, A. Functional Expression and Release of Ligands for the Activating Immunoreceptor NKG2D in Leukemia. Blood 2003, 102, 1389–1396. [Google Scholar] [CrossRef]
- Groh, V.; Rhinehart, R.; Secrist, H.; Bauer, S.; Grabstein, K.H.; Spies, T. Broad Tumor-Associated Expression and Recognition by Tumor-Derived Gamma Delta T Cells of MICA and MICB. Proc. Natl. Acad. Sci. USA 1999, 96, 6879–6884. [Google Scholar] [CrossRef]
- Weber, K.J.; Rao, G.; Quiros, R.; Bajnrauh, R.; Xu, X.; Prinz, R.A. Increased Expression of MICA in Serum of Pancreatic Cancer Patients. J. Am. Coll. Surg. 2004, 199, 89. [Google Scholar] [CrossRef]
- Madjd, Z.; Spendlove, I.; Moss, R.; Bevin, S.; Pinder, S.E.; Watson, N.F.; Ellis, I.; Durrant, L.G. Upregulation of MICA on highgrade invasive operable breast carcinoma. Cancer Immun. 2007, 7, 17. [Google Scholar]
- Chen, Y.; Lin, W.; Zhu, W.; Lin, J.; Zhou, Z.; Huang, C.; Chen, G.; Shi, Y.; Guo, Z.; Ye, Y. Tumor MICA Status Predicts the Efficacy of Immunotherapy with Cytokine-Induced Killer Cells for Patients with Gastric Cancer. Immunol. Res. 2016, 64, 251–259. [Google Scholar] [CrossRef]
- Deng, W.; Gowen, B.G.; Zhang, L.; Wang, L.; Lau, S.; Iannello, A.; Xu, J.; Rovis, T.L.; Xiong, N.; Raulet, D.H. A Shed NKG2D Ligand That Promotes Natural Killer Cell Activation and Tumor Rejection. Science 2015, 348, 136–139. [Google Scholar] [CrossRef]
- Steigerwald, J.; Raum, T.; Pflanz, S.; Cierpka, R.; Mangold, S.; Rau, D.; Hoffmann, P.; Kvesic, M.; Zube, C.; Linnerbauer, S.; et al. Human IgG1 Antibodies Antagonizing Activating Receptor NKG2D on Natural Killer Cells. mAbs 2009, 1, 115–127. [Google Scholar] [CrossRef]
- Groh, V.; Wu, J.; Yee, C.; Spies, T. Tumour-Derived Soluble MIC Ligands Impair Expression of NKG2D and T-Cell Activation. Nature 2002, 419, 734–738. [Google Scholar] [CrossRef]
- Liu, C.-J.; Lui, M.-T.; Chen, H.-L.; Lin, S.-C.; Chang, K.-W. MICA and MICB Overexpression in Oral Squamous Cell Carcinoma: MICA and MICB Overexpression in OSCC. J. Oral Pathol. Med. 2006, 36, 43–47. [Google Scholar] [CrossRef]
- Yamaguchi, K.; Chikumi, H.; Shimizu, A.; Takata, M.; Kinoshita, N.; Hashimoto, K.; Nakamoto, M.; Matsunaga, S.; Kurai, J.; Miyake, N.; et al. Diagnostic and Prognostic Impact of Serum-Soluble UL16-Binding Protein 2 in Lung Cancer Patients. Cancer Sci. 2012, 103, 1405–1413. [Google Scholar] [CrossRef]
- Paschen, A.; Sucker, A.; Hill, B.; Moll, I.; Zapatka, M.; Nguyen, X.D.; Sim, G.C.; Gutmann, I.; Hassel, J.; Becker, J.C.; et al. Differential Clinical Significance of Individual NKG2D Ligands in Melanoma: Soluble ULBP2 as an Indicator of Poor Prognosis Superior to S100B. Clin. Cancer Res. 2009, 15, 5208–5215. [Google Scholar] [CrossRef]
- Nückel, H.; Switala, M.; Sellmann, L.; Horn, P.A.; Dürig, J.; Dührsen, U.; Küppers, R.; Grosse-Wilde, H.; Rebmann, V. The Prognostic Significance of Soluble NKG2D Ligands in B-Cell Chronic Lymphocytic Leukemia. Leukemia 2010, 24, 1152–1159. [Google Scholar] [CrossRef]
- Zocchi, M.R.; Camodeca, C.; Nuti, E.; Rossello, A.; Venè, R.; Tosetti, F.; Dapino, I.; Costa, D.; Musso, A.; Poggi, A. ADAM10 New Selective Inhibitors Reduce NKG2D Ligand Release Sensitizing Hodgkin Lymphoma Cells to NKG2D-Mediated Killing. OncoImmunology 2016, 5, e1123367. [Google Scholar] [CrossRef]
- Pham, D.H.; Kim, J.S.; Kim, S.K.; Shin, D.J.; Hyun, H.; Yoon, M.S.; Kang, S.J.; Ryu, Y.J.; Cho, J.S.; Yoon, J.H.; et al. Effects of ADAM10 and ADAM17 Inhibitors on Natural Killer Cell Expansion and Antibody-Dependent Cellular Cytotoxicity Against Breast Cancer Cells In Vitro. Anticancer Res. 2017, 37. [Google Scholar] [CrossRef]
- Wu, J.; Mishra, H.K.; Walcheck, B. Role of ADAM17 as a Regulatory Checkpoint of CD16A in NK Cells and as a Potential Target for Cancer Immunotherapy. J. Leukoc. Biol. 2019, 105, 1297–1303. [Google Scholar] [CrossRef]
- Basar, R.; Daher, M.; Rezvani, K. Next-Generation Cell Therapies: The Emerging Role of CAR-NK Cells. Blood Adv. 2020, 4, 5868–5876. [Google Scholar] [CrossRef]
- Eyquem, J.; Mansilla-Soto, J.; Giavridis, T.; van der Stegen, S.J.C.; Hamieh, M.; Cunanan, K.M.; Odak, A.; Gönen, M.; Sadelain, M. Targeting a CAR to the TRAC Locus with CRISPR/Cas9 Enhances Tumour Rejection. Nature 2017, 543, 113–117. [Google Scholar] [CrossRef]
- Klingemann, H. Are Natural Killer Cells Superior CAR Drivers? OncoImmunology 2014, 3, e28147. [Google Scholar] [CrossRef]
- Xie, G.; Dong, H.; Liang, Y.; Ham, J.D.; Rizwan, R.; Chen, J. CAR-NK Cells: A Promising Cellular Immunotherapy for Cancer. EBioMedicine 2020, 59, 102975. [Google Scholar] [CrossRef]
- Ruggeri, L.; Capanni, M.; Urbani, E. Effectiveness of Donor Natural Killer Cell Alloreactivity in Mismatched Hematopoietic Transplants. Science 2002, 295, 2097–2100. [Google Scholar] [CrossRef]
- Stadtmauer, E.A.; Fraietta, J.A.; Davis, M.M.; Cohen, A.D.; Weber, K.L.; Lancaster, E.; Mangan, P.A.; Kulikovskaya, I.; Gupta, M.; Chen, F.; et al. CRISPR-Engineered T Cells in Patients with Refractory Cancer. Science 2020, 367, eaba7365. [Google Scholar] [CrossRef]
- Han, Y.; Xie, W.; Song, D.-G.; Powell, D.J. Control of Triple-Negative Breast Cancer Using Ex Vivo Self-Enriched, Costimulated NKG2D CAR T Cells. J. Hematol. Oncol. 2018, 11, 92. [Google Scholar] [CrossRef]
- Duan, S.; Guo, W.; Xu, Z.; He, Y.; Liang, C.; Mo, Y.; Wang, Y.; Xiong, F.; Guo, C.; Li, Y.; et al. Natural Killer Group 2D Receptor and Its Ligands in Cancer Immune Escape. Mol. Cancer 2019, 18, 29. [Google Scholar] [CrossRef] [PubMed]
- Montagner, I.M.; Penna, A.; Fracasso, G.; Carpanese, D.; Dalla Pietà, A.; Barbieri, V.; Zuccolotto, G.; Rosato, A. Anti-PSMA CAR-Engineered NK-92 Cells: An Off-the-Shelf Cell Therapy for Prostate Cancer. Cells 2020, 9, 1382. [Google Scholar] [CrossRef] [PubMed]
- Huergo-Zapico, L.; Acebes-Huerta, A.; Gonzalez-Rodriguez, A.P.; Contesti, J.; Gonzalez-García, E.; Payer, A.R.; Villa-Alvarez, M.; Fernández-Guizán, A.; López-Soto, A.; Gonzalez, S. Expansion of NK Cells and Reduction of NKG2D Expression in Chronic Lymphocytic Leukemia. Correlation with Progressive Disease. PLoS ONE 2014, 9, e108326. [Google Scholar] [CrossRef] [PubMed]
- Jurisic, V.; Colovic, N.; Konjevic, G.; Minic, I.; Colovic, M. An Aggressive Extramedullary Cutaneous Plasmacytoma Associated with Extreme Alterations in the Innate Immune System. Onkologie 2010, 33, 113–115. [Google Scholar] [CrossRef]
- Jurisic, V.; Srdic, T.; Konjevic, G.; Markovic, O.; Colovic, M. Clinical Stage-Depending Decrease of NK Cell Activity in Multiple Myeloma Patients. Med. Oncol. 2007, 24, 312–317. [Google Scholar] [CrossRef]
- Holthof, L.C.; Stikvoort, A.; van der Horst, H.J.; Gelderloos, A.T.; Poels, R.; Li, F.; Groen, R.W.J.; Zweegman, S.; van de Donk, N.W.C.J.; O’Dwyer, M.; et al. Bone Marrow Mesenchymal Stromal Cell-Mediated Resistance in Multiple Myeloma Against NK Cells Can Be Overcome by Introduction of CD38-CAR or TRAIL-Variant. HemaSphere 2021, 5, e561. [Google Scholar] [CrossRef]
- Sallman, D.A.; Brayer, J.; Sagatys, E.M.; Lonez, C.; Breman, E.; Agaugué, S.; Verma, B.; Gilham, D.E.; Lehmann, F.F.; Davila, M.L. NKG2D-Based Chimeric Antigen Receptor Therapy Induced Remission in a Relapsed/Refractory Acute Myeloid Leukemia Patient. Haematologica 2018, 103, e424–e426. [Google Scholar] [CrossRef]
- Wang, W.; Gao, L.; Ma, Y.-G. [Effect of NKG2D in eliminating hematological malignant cell lines by natural killer cells]. Zhongguo Shi Yan Xue Ye Xue Za Zhi 2012, 20, 296–299. [Google Scholar]
- Sandoval-Borrego, D.; Moreno-Lafont, M.C.; Vazquez-Sanchez, E.A.; Gutierrez-Hoya, A.; López-Santiago, R.; Montiel-Cervantes, L.A.; Ramírez-Saldaña, M.; Vela-Ojeda, J. Overexpression of CD158 and NKG2A Inhibitory Receptors and Underexpression of NKG2D and NKp46 Activating Receptors on NK Cells in Acute Myeloid Leukemia. Arch. Med. Res. 2016, 47, 55–64. [Google Scholar] [CrossRef]
- Ashiru, O.; Boutet, P.; Fernández-Messina, L.; Agüera-González, S.; Skepper, J.N.; Valés-Gómez, M.; Reyburn, H.T. Natural Killer Cell Cytotoxicity Is Suppressed by Exposure to the Human NKG2D Ligand MICA*008 That Is Shed by Tumor Cells in Exosomes. Cancer Res. 2010, 70, 481–489. [Google Scholar] [CrossRef]
- Lapidot, T.; Sirard, C.; Vormoor, J.; Murdoch, B.; Hoang, T.; Caceres-Cortes, J.; Minden, M.; Paterson, B.; Caligiuri, M.A.; Dick, J.E. A Cell Initiating Human Acute Myeloid Leukaemia after Transplantation into SCID Mice. Nature 1994, 367, 645–648. [Google Scholar] [CrossRef]
- Paczulla, A.M.; Rothfelder, K.; Raffel, S.; Konantz, M.; Steinbacher, J.; Wang, H.; Tandler, C.; Mbarga, M.; Schaefer, T.; Falcone, M.; et al. Absence of NKG2D Ligands Defines Leukaemia Stem Cells and Mediates Their Immune Evasion. Nature 2019, 572, 254–259. [Google Scholar] [CrossRef]
- Baragaño Raneros, A.; Martín-Palanco, V.; Fernandez, A.F.; Rodriguez, R.M.; Fraga, M.F.; Lopez-Larrea, C.; Suarez-Alvarez, B. Methylation of NKG2D Ligands Contributes to Immune System Evasion in Acute Myeloid Leukemia. Genes Immun. 2015, 16, 71–82. [Google Scholar] [CrossRef]
- Suárez-Alvarez, B.; López-Vázquez, A.; Baltar, J.M.; Ortega, F.; López-Larrea, C. Potential Role of NKG2D and Its Ligands in Organ Transplantation: New Target for Immunointervention. Am. J. Transplant. 2009, 9, 251–257. [Google Scholar] [CrossRef]
- Kim, J.; Chang, C.K.; Hayden, T.; Liu, F.-C.; Benjamin, J.; Hamerman, J.A.; Lanier, L.L.; Kang, S.-M. The Activating Immunoreceptor NKG2D and Its Ligands Are Involved in Allograft Transplant Rejection. J. Immunol. 2007, 179, 6416–6420. [Google Scholar] [CrossRef]
- Ogasawara, K.; Hamerman, J.A.; Ehrlich, L.R.; Bour-Jordan, H.; Santamaria, P.; Bluestone, J.A.; Lanier, L.L. NKG2D Blockade Prevents Autoimmune Diabetes in NOD Mice. Immunity 2004, 20, 757–767. [Google Scholar] [CrossRef]
- Yu, R.; Xu, S.; Wang, Y.; Cai, H.; Xu, P. Role of MICA Expression, Anti-MICA Antibodies and Serum MICA during Acute Rejection in a Rat-to-Mouse Cardiac Transplantation Model. Int. J. Clin. Exp. Pathol. 2015, 8, 14514–14520. [Google Scholar]
- Fabritius, C.; Ritschl, P.V.; Resch, T.; Roth, M.; Ebner, S.; Günther, J.; Mellitzer, V.; Nguyen, A.-V.; Pratschke, J.; Sauter, M.; et al. Deletion of the Activating NK Cell Receptor NKG2D Accelerates Rejection of Cardiac Allografts. Am. J. Transplant. 2017, 17, 3199–3209. [Google Scholar] [CrossRef]
- Suárez-Álvarez, B.; Fernández-Sánchez, A.; López-Vázquez, A.; Coto, E.; Ortega, F.; López-Larrea, C. NKG2D and Its Ligands: Active Factors in the Outcome of Solid Organ Transplantation? Kidney Int. Suppl. 2011, 1, 52–57. [Google Scholar] [CrossRef][Green Version]
- Thompson, T.W.; Kim, A.B.; Li, P.J.; Wang, J.; Jackson, B.T.; Huang, K.T.H.; Zhang, L.; Raulet, D.H. Endothelial Cells Express NKG2D Ligands and Desensitize Antitumor NK Responses. eLife 2017, 6. [Google Scholar] [CrossRef]
- Karimi, M.A.; Bryson, J.L.; Richman, L.P.; Fesnak, A.D.; Leichner, T.M.; Satake, A.; Vonderheide, R.H.; Raulet, D.H.; Reshef, R.; Kambayashi, T. NKG2D Expression by CD8+ T Cells Contributes to GVHD and GVT Effects in a Murine Model of Allogeneic HSCT. Blood 2015, 125, 3655–3663. [Google Scholar] [CrossRef] [PubMed]
- Ogasawara, K.; Benjamin, J.; Takaki, R.; Phillips, J.H.; Lanier, L.L. Function of NKG2D in Natural Killer Cell-Mediated Rejection of Mouse Bone Marrow Grafts. Nat. Immunol. 2005, 6, 938–945. [Google Scholar] [CrossRef] [PubMed]
- Picardi, A.; Mengarelli, A.; Marino, M.; Gallo, E.; Benevolo, M.; Pescarmona, E.; Cocco, R.; Fraioli, R.; Tremante, E.; Petti, M.C.; et al. Up-Regulation of Activating and Inhibitory NKG2 Receptors in Allogeneic and Autologous Hematopoietic Stem Cell Grafts. J. Exp. Clin. Cancer Res. 2015, 34, 98. [Google Scholar] [CrossRef] [PubMed]
- Hu, B.; Bao, G.; Zhang, Y.; Lin, D.; Wu, Y.; Wu, D.; Liu, H. Donor NK Cells and IL-15 Promoted Engraftment in Nonmyeloablative Allogeneic Bone Marrow Transplantation. J. Immunol. 2012, 189, 1661–1670. [Google Scholar] [CrossRef] [PubMed]
- Koike, J.; Wakao, H.; Ishizuka, Y.; Sato, T.; Hamaoki, M.; Seino, K.; Koseki, H.; Nakayama, T.; Taniguchi, M. Bone Marrow Allograft Rejection Mediated by a Novel Murine NK Receptor, NKG2I. J. Exp. Med. 2004, 199, 137–144. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sheng, L.; Mu, Q.; Wu, X.; Yang, S.; Zhu, H.; Wang, J.; Lai, Y.; Wu, H.; Sun, Y.; Hu, Y.; et al. Cytotoxicity of Donor Natural Killer Cells to apithyFollowing Allogeneic Stem Cell Transplantation. Front. Immunol. 2020, 11, 1534. [Google Scholar] [CrossRef] [PubMed]
- Weiss, T.; Schneider, H.; Silginer, M.; Steinle, A.; Pruschy, M.; Polić, B.; Weller, M.; Roth, P. NKG2D-Dependent Antitumor Effects of Chemotherapy and Radiotherapy against Glioblastoma. Clin. Cancer Res. 2018, 24, 882–895. [Google Scholar] [CrossRef]
- Apithy, M.-J.; Charbonnier, A.; Desoutter, J.; Diouf, M.; Morel, P.; Garçon, L.; Marolleau, J.-P.; Guillaume, N. Impact of MICA and NKG2D Polymorphisms in HLA-Fully Matched Related and Unrelated Hematopoietic Stem Cell Transplantation. Bone Marrow Transplant. 2018, 53, 918–922. [Google Scholar] [CrossRef]
- Moretta, L.; Biassoni, R.; Bottino, C.; Cantoni, C.; Pende, D.; Mingari, M.C.; Moretta, A. Human NK Cells and Their Receptors. Microbes Infect. 2002, 4, 1539–1544. [Google Scholar] [CrossRef]
- Schmiedel, D.; Mandelboim, O. Disarming Cellular Alarm Systems-Manipulation of Stress-Induced NKG2D Ligands by Human Herpesviruses. Front. Immunol. 2017, 8, 390. [Google Scholar] [CrossRef]
- Stern-Ginossar, N.; Elefant, N.; Zimmermann, A.; Wolf, D.G.; Saleh, N.; Biton, M.; Horwitz, E.; Prokocimer, Z.; Prichard, M.; Hahn, G.; et al. Host Immune System Gene Targeting by a Viral MiRNA. Science 2007, 317, 376–381. [Google Scholar] [CrossRef]
- Cosman, D.; Müllberg, J.; Sutherland, C.L.; Chin, W.; Armitage, R.; Fanslow, W.; Kubin, M.; Chalupny, N.J. ULBPs, Novel MHC Class I–Related Molecules, Bind to CMV Glycoprotein UL16 and Stimulate NK Cytotoxicity through the NKG2D Receptor. Immunity 2001, 14, 123–133. [Google Scholar] [CrossRef]
- Eagle, R.A.; Traherne, J.A.; Hair, J.R.; Jafferji, I.; Trowsdale, J. ULBP6/RAET1L Is an Additional Human NKG2D Ligand. Eur. J. Immunol. 2009, 39, 3207–3216. [Google Scholar] [CrossRef]
- Fielding, C.A.; Aicheler, R.; Stanton, R.J.; Wang, E.C.Y.; Han, S.; Seirafian, S.; Davies, J.; McSharry, B.P.; Weekes, M.P.; Antrobus, P.R.; et al. Two Novel Human Cytomegalovirus NK Cell Evasion Functions Target MICA for Lysosomal Degradation. PLoS Pathog. 2014, 10, e1004058. [Google Scholar] [CrossRef]
- Sutherland, C.L.; Chalupny, N.J.; Cosman, D. The UL16-Binding Proteins, a Novel Family of MHC Class I-Related Ligands for NKG2D, Activate Natural Killer Cell Functions: ULBPs Activate Human NK Cells. Immunol. Rev. 2001, 181, 185–192. [Google Scholar] [CrossRef]
- Rölle, A.; Mousavi-Jazi, M.; Eriksson, M.; Odeberg, J.; Söderberg-Nauclér, C.; Cosman, D.; Kärre, K.; Cerboni, C. Effects of Human Cytomegalovirus Infection on Ligands for the Activating NKG2D Receptor of NK Cells: Up-Regulation of UL16-Binding Protein (ULBP)1 and ULBP2 Is Counteracted by the Viral UL16 Protein. J. Immunol. 2003, 171, 902–908. [Google Scholar] [CrossRef]
- Zdrenghea, M.T.; Telcian, A.G.; Laza-Stanca, V.; Bellettato, C.M.; Edwards, M.R.; Nikonova, A.; Khaitov, M.R.; Azimi, N.; Groh, V.; Mallia, P.; et al. RSV Infection Modulates IL-15 Production and MICA Levels in Respiratory Epithelial Cells. Eur. Respir. J. 2012, 39, 712–720. [Google Scholar] [CrossRef]
- Song, H.; Park, H.; Kim, J.; Park, G.; Kim, Y.-S.; Kim, S.M.; Kim, D.; Seo, S.K.; Lee, H.-K.; Cho, D.; et al. IDO Metabolite Produced by EBV-Transformed B Cells Inhibits Surface Expression of NKG2D in NK Cells via the c-Jun N-Terminal Kinase (JNK) Pathway. Immunol. Lett. 2011, 136, 187–193. [Google Scholar] [CrossRef]
- Velapasamy, S.; Dawson, C.W.; Young, L.S.; Paterson, I.C.; Yap, L.F. The Dynamic Roles of TGF-β Signalling in EBV-Associated Cancers. Cancers 2018, 10, 247. [Google Scholar] [CrossRef]
- Rivellese, F.; Prediletto, E. ACE2 at the Centre of COVID-19 from Paucisymptomatic Infections to Severe Pneumonia. Autoimmun. Rev. 2020, 19, 102536. [Google Scholar] [CrossRef]
- Zhu, Y.; Jiang, M.; Gao, L.; Huang, X. Single Cell Analysis of ACE2 Expression Reveals the Potential Targets for 2019-nCoV. Preprints 2020, 2020020221. [Google Scholar] [CrossRef]
- Van Eeden, C.; Khan, L.; Osman, M.S.; Cohen Tervaert, J.W. Natural Killer Cell Dysfunction and Its Role in COVID-19. Int. J. Mol. Sci. 2020, 21, 6351. [Google Scholar] [CrossRef]
- Bozzano, F.; Dentone, C.; Perrone, C.; Di Biagio, A.; Fenoglio, D.; Parodi, A.; Mikulska, M.; Bruzzone, B.; Giacobbe, D.R.; Vena, A.; et al. Extensive Activation, Tissue Trafficking, Turnover and Functional Impairment of NK Cells in COVID-19 Patients at Disease Onset Associates with Subsequent Disease Severity. PLoS Pathog. 2021, 17, e1009448. [Google Scholar] [CrossRef]
- Leisman, D.E.; Ronner, L.; Pinotti, R.; Taylor, M.D.; Sinha, P.; Calfee, C.S.; Hirayama, A.V.; Mastroiani, F.; Turtle, C.J.; Harhay, M.O.; et al. Cytokine Elevation in Severe and Critical COVID-19: A Rapid Systematic Review, Meta-Analysis, and Comparison with Other Inflammatory Syndromes. Lancet Respir. Med. 2020, 8, 1233–1244. [Google Scholar] [CrossRef]
- Cifaldi, L.; Prencipe, G.; Caiello, I.; Bracaglia, C.; Locatelli, F.; De Benedetti, F.; Strippoli, R. Inhibition of Natural Killer Cell Cytotoxicity by Interleukin-6: Implications for the Pathogenesis of Macrophage Activation Syndrome: INHIBITION OF NK CELL CYTOTOXICITY BY IL-6. Arthritis Rheumatol. 2015, 67, 3037–3046. [Google Scholar] [CrossRef]
- Ge, X.; Li, C.-R.; Yang, J.; Wang, G.-B. Aberrantly Decreased Levels of NKG2D Expression in Children with Kawasaki Disease. Scand. J. Immunol. 2013, 77, 389–397. [Google Scholar] [CrossRef]
- Gupta, M.; Noel, G.J.; Schaefer, M.; Friedman, D.; Bussel, J.; Johann-Liang, R. Cytokine modulation with immune gamma-globulin in peripheral blood of normal children and its implications in Kawasaki disease treatment. J. Clin. Immunol. 2001, 21, 193–199. [Google Scholar] [CrossRef]
- A Phase I/II Study of Universal Off-The-Shelf NKG2D-ACE2 CAR-NK Cells for Therapy of COVID-19. Available online: https://clinicaltrials.gov/ct2/show/NCT04324996 (accessed on 19 January 2021).
- Ma, M.; Badeti, S.; Geng, K.; Liu, D. Efficacy of Targeting SARS-CoV-2 by CAR-NK Cells. Immunology 2020, preprint. [Google Scholar] [CrossRef]
- Sharma, A.; Bhatt, N.S.; Martin, A.S.; Abid, M.B.; Bloomquist, J.; Chemaly, R.F.; Dandoy, C.; Gauthier, J.; Gowda, L.; Perales, M.-A.; et al. Clinical Characteristics and Outcomes of COVID-19 in Haematopoietic Stem-Cell Transplantation Recipients: An Observational Cohort Study. Lancet Haematol. 2021, 8, e185–e193. [Google Scholar] [CrossRef]
- Goronzy, J.J.; Weyand, C.M. T-Cell Regulation in Rheumatoid Arthritis. Curr. Opin. Rheumatol. 2004, 16, 212–217. [Google Scholar] [CrossRef]
- Vadstrup, K.; Bendtsen, F. Anti-NKG2D MAb: A New Treatment for Crohn’s Disease? Int. J. Mol. Sci. 2017, 18, 1997. [Google Scholar] [CrossRef] [PubMed]
- Allez, M.; Petryka, R.; Skolnick, B.E.; Wisniewska-Jarosinska, M.A. Mo1213 Efficacy and Safety of NNC0142-0002, a Novel Human Monoclonal Antibody Targeting NKG2D: A Randomized, Double-Blind, Single-Dose Phase 2 Trial in Patients with Crohn’s Disease. Gastroenterology 2014, 146 (Suppl. S1), S-587. [Google Scholar] [CrossRef]
- Mei, B.; Zhang, S.-R.; Chen, Y.-L.; Wang, C.-F. Defects in NKG2D Ligand Expression Result in Failed Tolerance Induction at the Maternal–Fetal Interface: A Possible Cause for Recurrent Miscarriage. Med. Hypotheses 2012, 79, 465–467. [Google Scholar] [CrossRef] [PubMed]
- Ferretti, C.; Bruni, L.; Dangles-Marie, V.; Pecking, A.P.; Bellet, D. Molecular Circuits Shared by Placental and Cancer Cells, and Their Implications in the Proliferative, Invasive and Migratory Capacities of Trophoblasts. Hum. Reprod. Update 2006, 13, 121–141. [Google Scholar] [CrossRef] [PubMed]
- Hedlund, M.; Stenqvist, A.-C.; Nagaeva, O.; Kjellberg, L.; Wulff, M.; Baranov, V.; Mincheva-Nilsson, L. Human Placenta Expresses and Secretes NKG2D Ligands via Exosomes That Down-Modulate the Cognate Receptor Expression: Evidence for Immunosuppressive Function. J. Immunol. 2009, 183, 340–351. [Google Scholar] [CrossRef] [PubMed]
- Mincheva-Nilsson, L.; Nagaeva, O.; Chen, T.; Stendahl, U.; Antsiferova, J.; Mogren, I.; Hernestål, J.; Baranov, V. Placenta-Derived Soluble MHC Class I Chain-Related Molecules Down-Regulate NKG2D Receptor on Peripheral Blood Mononuclear Cells during Human Pregnancy: A Possible Novel Immune Escape Mechanism for Fetal Survival. J. Immunol. 2006, 176, 3585–3592. [Google Scholar] [CrossRef] [PubMed]
- Hanna, J.; Goldman-Wohl, D.; Hamani, Y.; Avraham, I.; Greenfield, C.; Natanson-Yaron, S.; Prus, D.; Cohen-Daniel, L.; Arnon, T.I.; Manaster, I.; et al. Decidual NK Cells Regulate Key Developmental Processes at the Human Fetal-Maternal Interface. Nat. Med. 2006, 12, 1065–1074. [Google Scholar] [CrossRef] [PubMed]
- Beaman, K.D.; Ntrivalas, E.; Mallers, T.M.; Jaiswal, M.K.; Kwak-Kim, J.; Gilman-Sachs, A. Immune Etiology of Recurrent Pregnancy Loss and Its Diagnosis. Am. J. Reprod. Immunol. 2012, 67, 319–325. [Google Scholar] [CrossRef]
- Yamada, H.; Morikawa, M.; Kato, E.H.; Shimada, S.; Kobashi, G.; Minakami, H. Pre-Conceptional Natural Killer Cell Activity and Percentage as Predictors of Biochemical Pregnancy and Spontaneous Abortion with Normal Chromosome Karyotype: NK CELL ACTIVITY AND PERCENTAGE IN INFERTILITY. Am. J. Reprod. Immunol. 2003, 50, 351–354. [Google Scholar] [CrossRef]
- Perricone, R.; Muzio, G.D.; Perricone, C.; Giacomelli, R.; Nardo, D.D.; Fontana, L.; Carolis, C.D. High Levels of Peripheral Blood NK Cells in Women Suffering from Recurrent Spontaneous Abortion Are Reverted from High-Dose Intravenous Immunoglobulins. Am. J. Reprod. Immunol. 2006, 55, 232–239. [Google Scholar] [CrossRef]
- Morikawa, M.; Yamada, H.; Kato, E.H.; Shimada, S.; Ebina, Y.; Yamada, T.; Sagawa, T.; Kobashi, G.; Fujimoto, S. NK Cell Activity and Subsets in Women with a History of Spontaneous Abortion. Gynecol. Obstet. Investig. 2001, 52, 163–167. [Google Scholar] [CrossRef]
- Zhu, L.; Aly, M.; Wang, H.; Karakizlis, H.; Weimer, R.; Morath, C.; Kuon, R.J.; Toth, B.; Ekpoom, N.; Opelz, G.; et al. Increased Natural Killer Cell Subsets with Inhibitory Cytokines and Inhibitory Surface Receptors in Patients with Recurrent Miscarriage and Decreased or Normal Subsets in Kidney Transplant Recipients Late Post-Transplant: Inhibitory NK Cells in RM Patients. Clin. Exp. Immunol. 2018, 193, 241–254. [Google Scholar] [CrossRef]
- Zhang, Y.; Huang, C.; Lian, R.; Xu, J.; Fu, Y.; Zeng, Y.; Tu, W. The Low Cytotoxic Activity of Peripheral Blood NK Cells May Relate to Unexplained Recurrent Miscarriage. Am. J. Reprod. Immunol. 2021, 85. [Google Scholar] [CrossRef]
- Toth, B.; Jeschke, U.; Rogenhofer, N.; Scholz, C.; Würfel, W.; Thaler, C.J.; Makrigiannakis, A. Recurrent miscarriage: Current concepts in diagnosis and treatment. J. Reprod. Immunol. 2010, 85, 25–32. [Google Scholar] [CrossRef]
- Wallace, A.E.; Goulwara, S.S.; Whitley, G.S.; Cartwright, J.E. Oxygen modulates human decidual natural killer cell surface receptor expression and interactions with trophoblasts. Biol. Reprod. 2014, 91, 134. [Google Scholar] [CrossRef]
- Egerup, P.; Lindschou, J.; Gluud, C.; Christiansen, O.B.; ImmuReM IPD Study Group. The Effects of Intravenous Immunoglobulins in Women with Recurrent Miscarriages: A Systematic Review of Randomised Trials with Meta-Analyses and Trial Sequential Analyses Including Individual Patient Data. PLoS ONE 2015, 10, e0141588. [Google Scholar] [CrossRef]
- Ng, Y.Y.; Tay, J.C.K.; Wang, S. CXCR1 Expression to Improve Anti-Cancer Efficacy of Intravenously Injected CAR-NK Cells in Mice with Peritoneal Xenografts. Mol. Ther. Oncolytics 2020, 16, 75–85. [Google Scholar] [CrossRef]
- Wang, J.; Lupo, K.B.; Chambers, A.M.; Matosevic, S. Purinergic Targeting Enhances Immunotherapy of CD73+ Solid Tumors with PiggyBac-Engineered Chimeric Antigen Receptor Natural Killer Cells. J. Immunother. Cancer 2018, 6, 136. [Google Scholar] [CrossRef]
- Li, Y.; Hermanson, D.L.; Moriarity, B.S.; Kaufman, D.S. Human IPSC-Derived Natural Killer Cells Engineered with Chimeric Antigen Receptors Enhance Anti-Tumor Activity. Cell Stem Cell 2018, 23, 181–192.e5. [Google Scholar] [CrossRef]
- Oberschmidt, O.; Morgan, M.; Huppert, V.; Kessler, J.; Gardlowski, T.; Matthies, N.; Aleksandrova, K.; Arseniev, L.; Schambach, A.; Koehl, U.; et al. Development of Automated Separation, Expansion, and Quality Control Protocols for Clinical-Scale Manufacturing of Primary Human NK Cells and Alpharetroviral Chimeric Antigen Receptor Engineering. Hum. Gene Ther. Methods 2019, 30, 102–120. [Google Scholar] [CrossRef]
| NK Cells Receptors | |||||
|---|---|---|---|---|---|
| Type | Receptor | Ligands | Gene | Chromosome | Ref. |
| Activating | CD16 | IgG 1, 3, 4 | FCGR3A | 1q23.3 | [23] |
| KIR2DS1 | HLA-C | KIR2DS1 | 19q13.4 | [24] | |
| KIR2DS4 | HLA-A, HLA-C | KIR2DS4 | 19q13.4 | [24] | |
| KIR2DL4 | HLA-G, HS | KIR3DL4 | 19q13.4 | [24] | |
| NKG2C | HLA-E | KLRC2 | 12p13.2 | [25,26] | |
| NKG2D | MICA/MICB, ULBP1-6 | KLRK1 | 12p13.2 | [8,26] | |
| NKG2E | HLA-E | KLRC1 | 12p13.2 | [27] | |
| NKp30 | B7-H6, BAT3, pp65 | NCR3 | 6p21.33 | [28] | |
| NKp44 | viral hemagglutinins | NCR2 | 6p21.1 | [29] | |
| NKp46 | viral hemagglutinins | NCR1 | 19q13.42 | [30] | |
| Inhibiting | KIR2DL1-3 | HLA-C | KIR2DL1 | 19q13.4 | [24,30] |
| KIR3DL1 | HLA-B | KIR3DL1 | 19q13.4 | [24] | |
| KIR3DL2 | HLA-A | KIR3DL2 | 19q13.4 | [24] | |
| KIR3DL3 | unknown | KIR3DL3 | 19q13.4 | [24] | |
| KIR2DL4 | HLA-G | KIR2DL4 | 19q13.4 | [24] | |
| KIR2DL5 | HLA class I | KIR2DL5 | 19q13.4 | [24,31] | |
| LIR-1 | HLA class I | LILRB1 | 19q13.4 | [32] | |
| NKG2A/B | HLA-E | KLRC1 | 12p13.2 | [33,34] | |
| SNP ID | Localization [58] | Main Findings/Associations | Ref. |
|---|---|---|---|
| rs1049174 (G > C) | KLRK1 exon 8 (3’UTR) | G allele associated with reduced risk of colorectal carcinoma (colon, rectal, both) in Japanese patients | [57] |
| G allele associated with reduced risk of aerodigestive cancer (head, neck, esophageal) among Japanese never smokers and never drinkers | [59] | ||
| CC genotype associated with higher breast cancer risk in Iranian women | [60] | ||
| GG and GC genotypes associated with increased risk of gastric cancer in Chinese patients | [61] | ||
| GG homozygosity in chronic myeloid leukemia Japanese patients associated with better response to dasatinib treatment, compared to other CML patients’ genotypes; G allele affected the incidence of skin rash after Das treatment | [62] | ||
| CC homozygosity in Caucasians protected against spondyloarthritis | [63] | ||
| CC polymorphism associated with inefficient anti-TNF therapy in Polish rheumatoid arthritis patients; presence of C allele correlated with worse EULAR response | [64] | ||
| G allele associated with rheumatoid arthritis lower disease activity scores among Greek patients | [65] | ||
| C allele associated with increased HPV+ cervical, anal and vaginal cancers risk in Vietnamese patients | [66] | ||
| CC homozygosity associated with higher risk of EBV-infected nasopharyngeal carcinoma in Vietnamese patients | [67] | ||
| GG genotype in chronic hepatitis C Iranian patients demonstrated higher response to Peginterferon Alfa-2a/Ribavirin therapy against HCV infection | [68] | ||
| No association between Caucasian alleles and CMV infection in the first year after kidney transplantation | [69] | ||
| Donor GG genotype associated with improved overall survival and transplant related mortality in Japanese patients with standard risk disease after HLA-fully matched unrelated BM transplantation; no impact on disease relapse or development of aGvHD, cGvHD | [70] | ||
| C allele associated with decreased risk of recurrent miscarriages among Iranian women | [71] | ||
| rs2255336 (A, C > G, T) | KLRK1 exon 4 (region encoding transmembrane part of receptor) | A allele in Caucasian patients associated with lower incidence of systemic lupus erythematosus | [72] |
| GG genotype associated with systemic lupus erythematosus risk in Caucasian patients; reduced stimulatory effect of CD4+ NKG2D+ T cells carrying the GG variant | [73] | ||
| AA genotype associated with susceptibility to rheumatoid arthritis in Korean patients | [74] | ||
| GG genotype associated with inefficient anti-TNF therapy in rheumatoid arthritis Caucasian patients | [64] | ||
| TT genotype in Taiwanese chronic hepatitis B patients associated with a decreased risk of delayed spontaneous HBeAg seroconversion | [75] | ||
| Higher A allele frequency in Japanese congenital CMV infection cases symptomatic at birth than in asymptomatic cases | [76] | ||
| AA and GA genotypes associated with reduced HPV-related cancer risk; protective effect of A allele against the progression to advanced stages of cancer | [77] | ||
| rs2617160 (A > T) | Intergenic KLRC4-KLRK1 | TT genotype associated with increased risk of chronic hepatitis B in Chinese patients | [78] |
| A allele associated with lower frequency of retinopathy—vascular complication in sickle cell disease in Sub-Saharan African and French West Indian patients | [79] | ||
| rs2246809 (A > G) | Intergenic KLRC4-KLRK1 | A allele frequency higher in South Indian rheumatoid arthritis patients with deformities—marker of severe disease | [80] |
| A allele associated with lower frequency of retinopathy—vascular complication in sickle cell disease in Sub-Saharan African and French West Indian patients | [79] | ||
| rs2617169 (A > T) | KLRC4 intron 3 | T allele frequency higher in South Indian rheumatoid arthritis patients with deformities—marker of severe disease | [80] |
| A allele associated with lower frequency of retinopathy—vascular complication in sickle cell disease in Sub-Saharan African and French West Indian patients | [79] | ||
| rs2617170 (T > C) | KLRC4 exon 3 | TT homozygosity associated with lower risk of recurrent miscarriage among North African women | [81] |
| rs7397310 (T > C) | 3’ flanking region of KLRK1 | No association between alleles frequency and cholangiocarcinoma risk in Caucasian individuals | [82] |
| rs2900420 (G > A) | 3’ flanking region of KLRK1 | A allele associated with better survival time in advanced-stage non-small cell lung cancer Non-Hispanic Whites patients treated with first-line chemotherapy | [83] |
| rs10772271 (G > A) | 3’ flanking region of KLRK1 | A allele associated with decreased NKG2D expression on NK cells in Finnish infants, and increased viral bronchiolitis susceptibility | [84] |
| rs11053781 (G > A) | KLRK1 intron 3 | Higher G allele frequency in PSC Scandinavian patients with cholangiocarcinoma | [85] |
| rs7972757 (A > G) | Intergenic KLRC4-KLRK1 | Higher A allele frequency in placental malaria affected African patients | [86] |
| rs728010 (G > A) | Intergenic KLRC4-KLRK1 | Higher GG genotype frequency in placental malaria affected African patients | [86] |
| rs12821887 (T > C) | Intergenic KLRC4-KLRK1 | Higher TT genotype frequency in placental malaria affected African patients | [86] |
| rs2617167 (G > A) | Intergenic KLRC4-KLRK1 | Higher A allele frequency in PSC Scandinavian patients with cholangiocarcinoma | [85] |
| rs1154831 (A > C) | Intergenic KLRC4-KLRK1 | CC genotype associated with lower disease activity scores in rheumatoid arthritis Greek patients | [65] |
| CCGGGCA > CCAGGCG (rs1049174, rs2255336, rs11053781, rs12819494, rs728010, rs2617165, rs2617167) | Haplotypes associated with increasing/decreasing cholangiocarcinoma risk in PSC Scandinavian patients | [85] | |
| GAT (rs2255336, rs224809, rs2617169) | Haplotype associated with higher risk for cutaneous melanoma in Caucasian patients | [87] | |
| GCAGATCC (rs1049174, rs2255336, rs2617160, rs2246809, rs2617169, rs2617170, rs2617171, rs1983526) | Higher haplotype frequency in rheumatoid arthritis among South Indian patients | [80] | |
| CAT > GGA (rs1049174, rs2255336, rs2617160) | Haplotypes associated with higher recurrent miscarriage risk among North African women | [81] | |
| CAA (rs1049174, rs2255336, rs2617160) | Haplotypes associated with higher recurrent miscarriage risk among North African women | [81] | |
| GTTG > ATTC (rs2246809, rs2617169, rs2617170, rs2617171) | Haplotypes associated with increasing/decreasing recurrent miscarriage risk among North African women | [81] | |
| (ATG, TTC) > (TTC, TTG) (rs1746123, rs10431294, rs1049174) | KLRK1 haplotypes associated with decreasing/increasing gastric cancer risk in Chinese patients | [61] | |
| CAR-T Cells | CAR-NK Cells |
|---|---|
| CAR—Specific mechanism | Spontaneous cytotoxic activity [118] |
| Target cell killing dependent on target antigen | Target cell killing not restricted to specific antigen (various receptors) [119] |
| Proinflammatory cytokines (TNF-α, IL-6, IL-15) | Cytokines (IFN-γ, GM-CSF) [119] |
| Suicide genes to control t cells life span | No need for suicide genes; short life span [118] |
| May induce cytokine storm and | One cell can kill multiple targets |
| cytokine-release syndrome | (“serial killers”) [118] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Siemaszko, J.; Marzec-Przyszlak, A.; Bogunia-Kubik, K. NKG2D Natural Killer Cell Receptor—A Short Description and Potential Clinical Applications. Cells 2021, 10, 1420. https://doi.org/10.3390/cells10061420
Siemaszko J, Marzec-Przyszlak A, Bogunia-Kubik K. NKG2D Natural Killer Cell Receptor—A Short Description and Potential Clinical Applications. Cells. 2021; 10(6):1420. https://doi.org/10.3390/cells10061420
Chicago/Turabian StyleSiemaszko, Jagoda, Aleksandra Marzec-Przyszlak, and Katarzyna Bogunia-Kubik. 2021. "NKG2D Natural Killer Cell Receptor—A Short Description and Potential Clinical Applications" Cells 10, no. 6: 1420. https://doi.org/10.3390/cells10061420
APA StyleSiemaszko, J., Marzec-Przyszlak, A., & Bogunia-Kubik, K. (2021). NKG2D Natural Killer Cell Receptor—A Short Description and Potential Clinical Applications. Cells, 10(6), 1420. https://doi.org/10.3390/cells10061420






