Mechanical Stress Induce PG-E2 in Murine Synovial Fibroblasts Originating from the Temporomandibular Joint
Abstract
1. Introduction
2. Materials and Methods
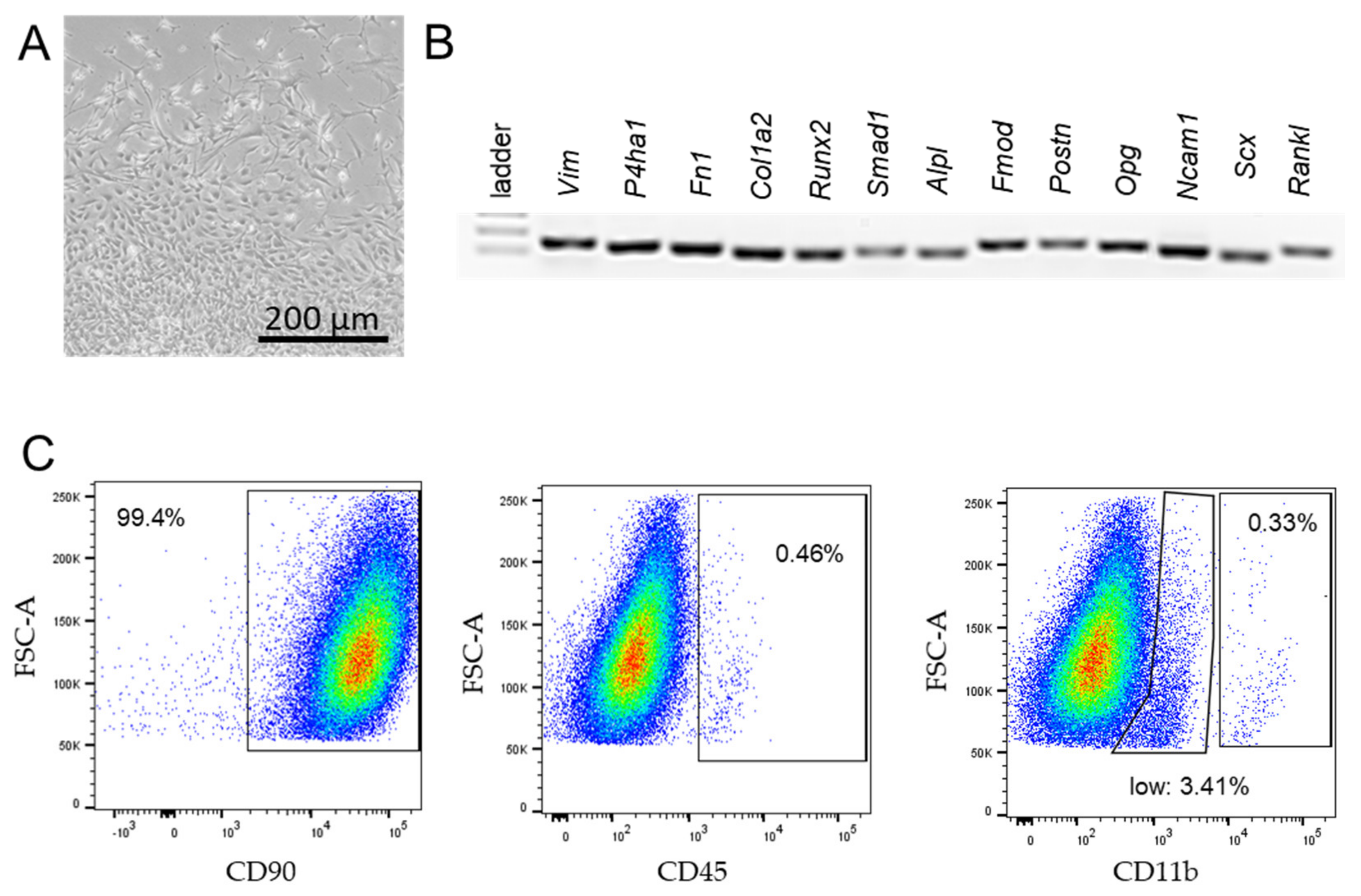
2.1. Tissue Collection, Isolation, and Culture of Murine Synovial Fibroblasts
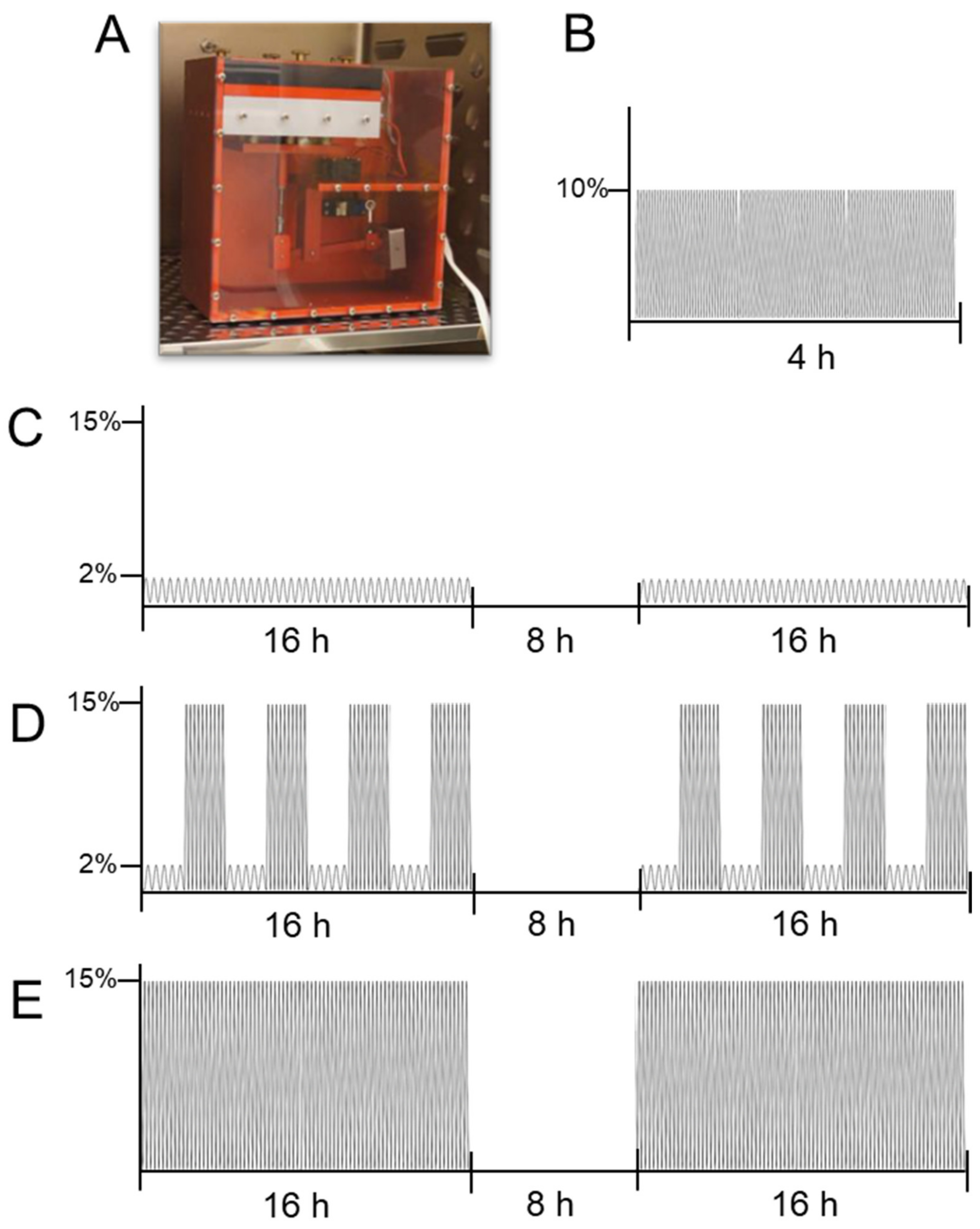
2.2. In Vitro Cell Culture Experiment Setup
2.3. RNA Isolation, cDNA Synthesis, Semiquantitative PCR, and Quantitative RT-PCR
2.4. Protein and Glycosaminoglycan Analysis
2.4.1. Enzyme-Linked Immunosorbent Assays (ELISA)
2.4.2. Total Collagen Content Assessment
2.4.3. Liquid-Chromatography Glycosaminoglycan Analysis
2.5. Statistical Analysis
3. Results
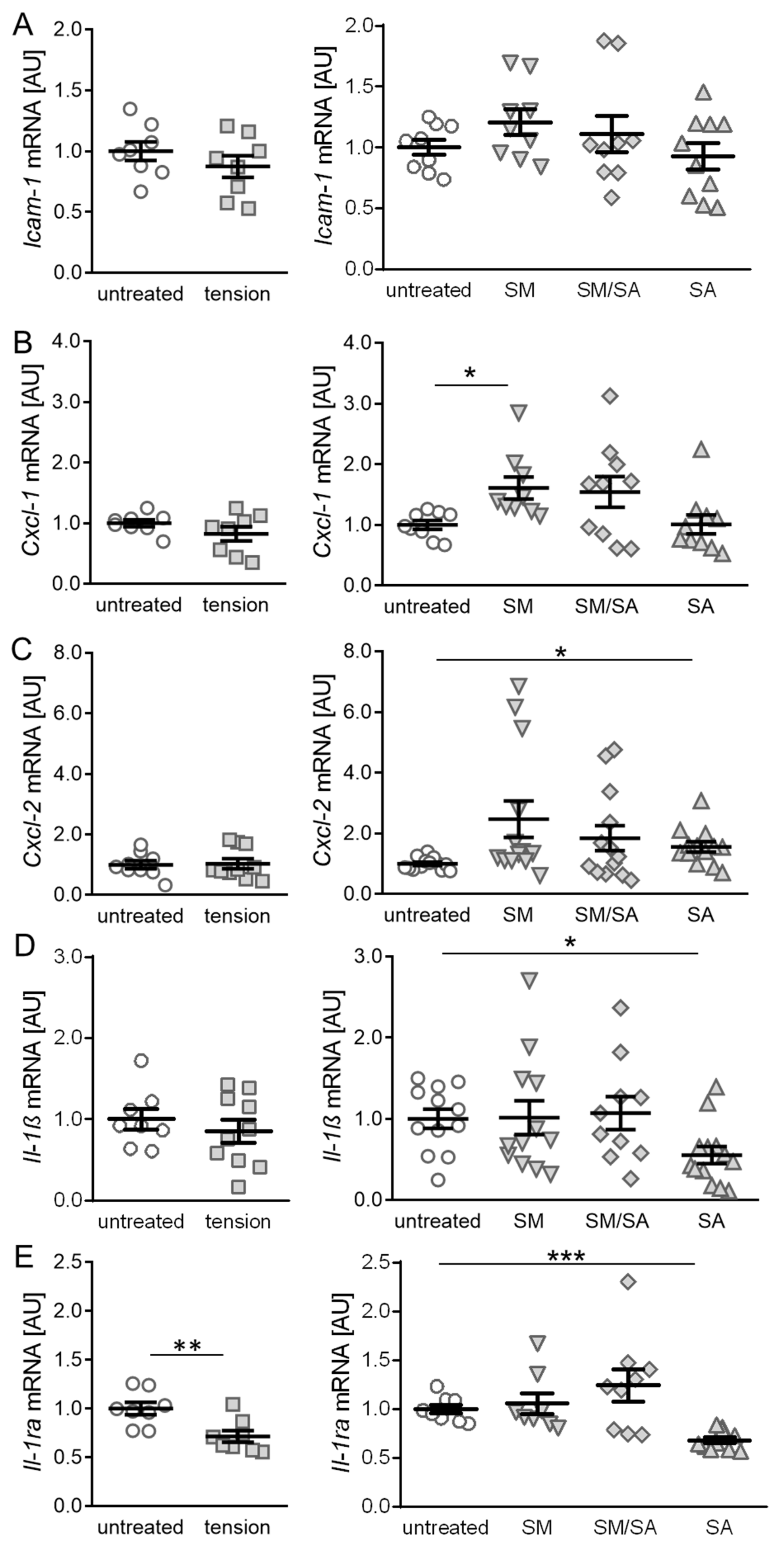
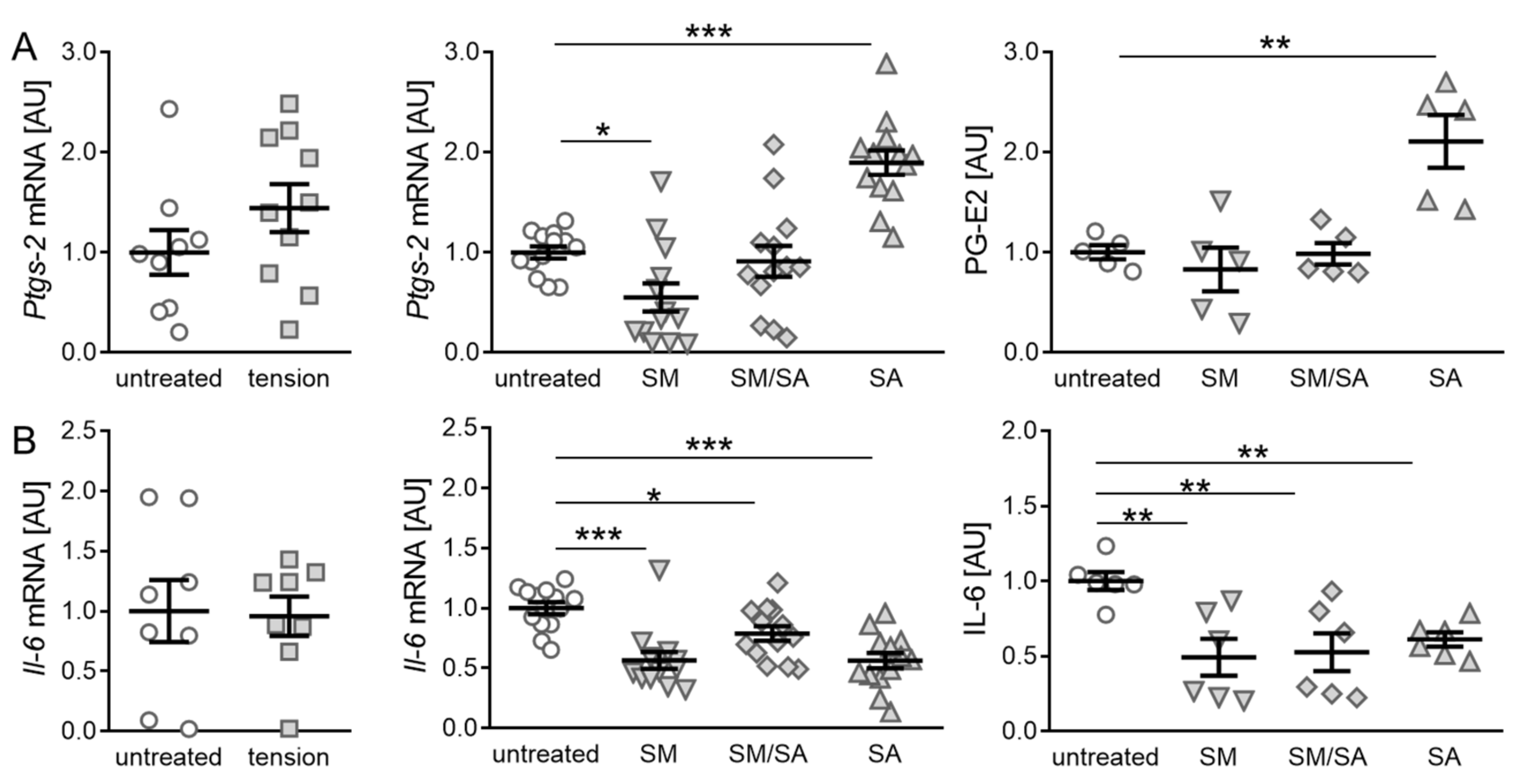
3.1. Effects of Cyclic Tensile Strain on the Expression of Inflammatory Mediators in Synovial Fibroblasts of the Temporomandibular Joint
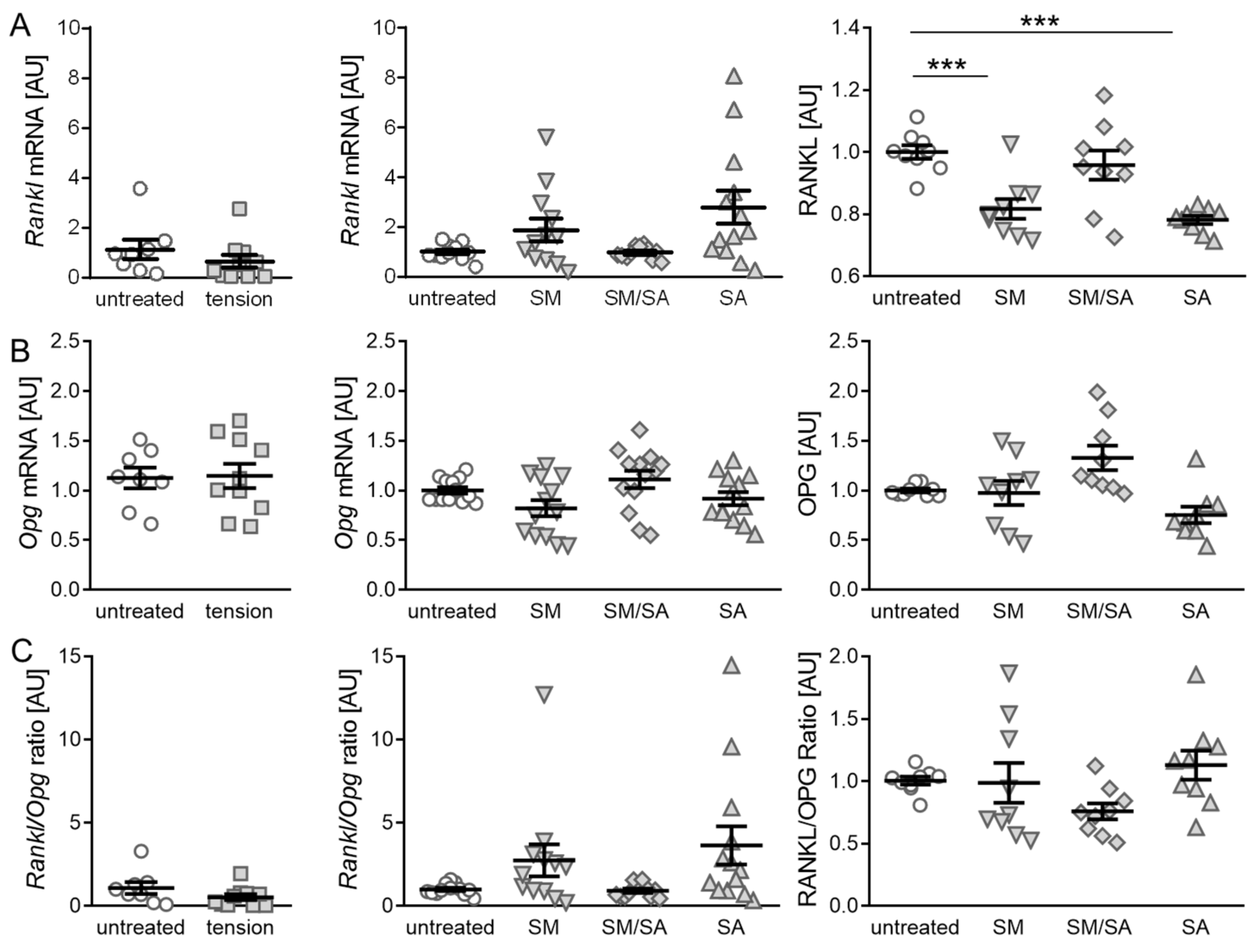
3.2. Effect of Cyclic Tensile Strain on RANKL/OPG-Mediated Osteoclast Activation
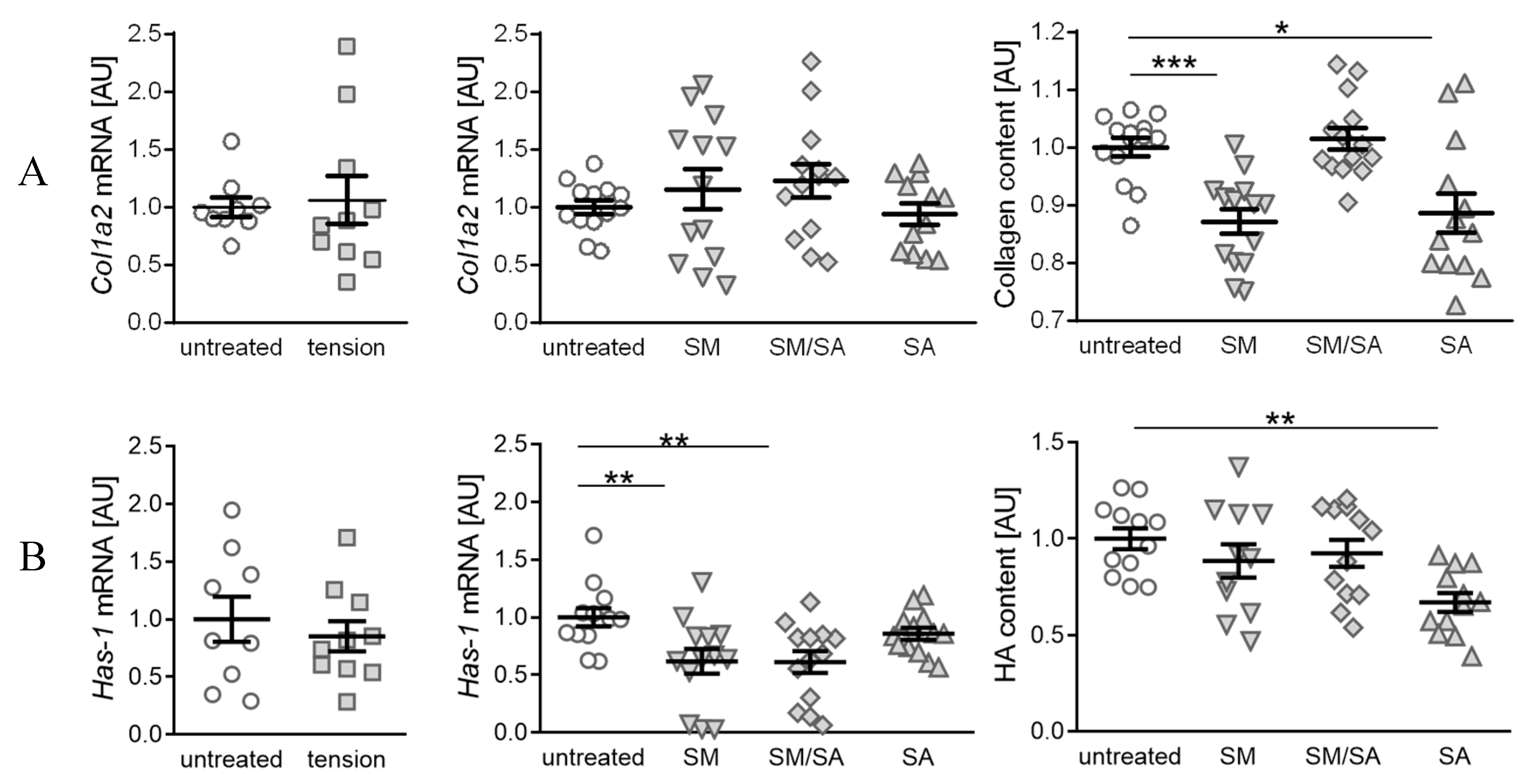
3.3. Diminished Matrix Constituent Deposition by the Prolonged Cyclic Tensile Strain
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stocum, D.L.; Roberts, W.E. Part I: Development and Physiology of the Temporomandibular Joint. Curr. Osteoporos. Rep. 2018, 16, 360–368. [Google Scholar] [CrossRef] [PubMed]
- Kuroki, Y.; Honda, K.; Kijima, N.; Wada, T.; Arai, Y.; Matsumoto, N.; Iwata, K.; Shirakawa, T. In vivo morphometric analysis of inflammatory condylar changes in rat temporomandibular joint. Oral Dis. 2011, 17, 499–507. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.D.; Zhang, J.N.; Gan, Y.H.; Zhou, Y.H. Current understanding of pathogenesis and treatment of TMJ osteoarthritis. J. Dent. Res. 2015, 94, 666–673. [Google Scholar] [CrossRef] [PubMed]
- Bleuel, J.; Zaucke, F.; Brüggemann, G.-P.; Niehoff, A. Effects of cyclic tensile strain on chondrocyte metabolism: A systematic review. PLoS ONE 2015, 10, e0119816. [Google Scholar] [CrossRef] [PubMed]
- Bhattaram, P.; Chandrasekharan, U. The joint synovium: A critical determinant of articular cartilage fate in inflammatory joint diseases. Semin. Cell Dev. Biol. 2017, 62, 86–93. [Google Scholar] [CrossRef]
- Clark, R.B.; Schmidt, T.A.; Sachse, F.B.; Boyle, D.; Firestein, G.S.; Giles, W.R. Cellular electrophysiological principles that modulate secretion from synovial fibroblasts. J. Physiol. 2017, 595, 635–645. [Google Scholar] [CrossRef]
- Hui, A.Y.; McCarty, W.J.; Masuda, K.; Firestein, G.S.; Sah, R.L. A systems biology approach to synovial joint lubrication in health, injury, and disease. Wiley Interdiscip. Rev. Syst. Biol. Med. 2012, 4, 15–37. [Google Scholar] [CrossRef]
- Carrión, M.; Juarranz, Y.; Pérez-García, S.; Jimeno, R.; Pablos, J.L.; Gomariz, R.P.; Gutiérrez-Cañas, I. RNA sensors in human osteoarthritis and rheumatoid arthritis synovial fibroblasts: Immune regulation by vasoactive intestinal peptide. Arthritis Rheum. 2011, 63, 1626–1636. [Google Scholar] [CrossRef]
- Ospelt, C.; Brentano, F.; Rengel, Y.; Stanczyk, J.; Kolling, C.; Tak, P.P.; Gay, R.E.; Gay, S.; Kyburz, D. Overexpression of toll-like receptors 3 and 4 in synovial tissue from patients with early rheumatoid arthritis: Toll-like receptor expression in early and longstanding arthritis. Arthritis Rheum. 2008, 58, 3684–3692. [Google Scholar] [CrossRef]
- Wehmeyer, C.; Pap, T.; Buckley, C.D.; Naylor, A.J. The role of stromal cells in inflammatory bone loss. Clin. Exp. Immunol. 2017, 189, 1–11. [Google Scholar] [CrossRef]
- Boyan, B.D.; Tosi, L.L.; Coutts, R.D.; Enoka, R.M.; Hart, D.A.; Nicolella, D.P.; Berkley, K.J.; Sluka, K.A.; Kwoh, C.K.; O’Connor, M.I.; et al. Addressing the gaps: Sex differences in osteoarthritis of the knee. Biol. Sex Differ. 2013, 4, 4. [Google Scholar] [CrossRef] [PubMed]
- Boyce, M.K.; Trumble, T.N.; Carlson, C.S.; Groschen, D.M.; Merritt, K.A.; Brown, M.P. Non-terminal animal model of post-traumatic osteoarthritis induced by acute joint injury. Osteoarthr. Cartil. 2013, 21, 746–755. [Google Scholar] [CrossRef] [PubMed]
- Buckwalter, J.A.; Mankin, H.J. Articular cartilage: Degeneration and osteoarthritis, repair, regeneration, and transplantation. Instr. Course Lect. 1998, 47, 487–504. [Google Scholar] [PubMed]
- Buckwalter, J.A. The role of mechanical forces in the initiation and progression of osteoarthritis. HSS J. 2012, 8, 37–38. [Google Scholar] [CrossRef]
- Kalladka, M.; Quek, S.; Heir, G.; Eliav, E.; Mupparapu, M.; Viswanath, A. Temporomandibular joint osteoarthritis: Diagnosis and long-term conservative management: A topic review. J. Indian Prosthodont. Soc. 2014, 14, 6–15. [Google Scholar] [CrossRef]
- Ricks, M.L.; Farrell, J.T.; Falk, D.J.; Holt, D.W.; Rees, M.; Carr, J.; Williams, T.; Nichols, B.A.; Bridgewater, L.C.; Reynolds, P.R.; et al. Osteoarthritis in temporomandibular joint of Col2a1 mutant mice. Arch. Oral Biol. 2013, 58, 1092–1099. [Google Scholar] [CrossRef]
- Stoll, M.L.; Sharpe, T.; Beukelman, T.; Good, J.; Young, D.; Cron, R.Q. Risk factors for temporomandibular joint arthritis in children with juvenile idiopathic arthritis. J. Rheumatol. 2012, 39, 1880–1887. [Google Scholar] [CrossRef]
- Felson, D.T.; Niu, J.; Neogi, T.; Goggins, J.; Nevitt, M.C.; Roemer, F.; Torner, J.; Lewis, C.E.; Guermazi, A. Synovitis and the risk of knee osteoarthritis: The MOST Study. Osteoarthr. Cartil. 2016, 24, 458–464. [Google Scholar] [CrossRef]
- Mathiessen, A.; Conaghan, P.G. Synovitis in osteoarthritis: Current understanding with therapeutic implications. Arthritis Res. Ther. 2017, 19, 18. [Google Scholar] [CrossRef]
- Roemer, F.W.; Guermazi, A.; Felson, D.T.; Niu, J.; Nevitt, M.C.; Crema, M.D.; Lynch, J.A.; Lewis, C.E.; Torner, J.; Zhang, Y. Presence of MRI-detected joint effusion and synovitis increases the risk of cartilage loss in knees without osteoarthritis at 30-month follow-up: The MOST study. Ann. Rheum. Dis. 2011, 70, 1804–1809. [Google Scholar] [CrossRef]
- Hou, C.-H.; Tang, C.-H.; Hsu, C.-J.; Hou, S.-M.; Liu, J.-F. CCN4 induces IL-6 production through αvβ5 receptor, PI3K, Akt, and NF-κB singling pathway in human synovial fibroblasts. Arthritis Res. Ther. 2013, 15, R19. [Google Scholar] [CrossRef] [PubMed]
- Hou, S.-M.; Hou, C.-H.; Liu, J.-F. CX3CL1 promotes MMP-3 production via the CX3CR1, c-Raf, MEK, ERK, and NF-κB signaling pathway in osteoarthritis synovial fibroblasts. Arthritis Res. Ther. 2017, 19, 282. [Google Scholar] [CrossRef] [PubMed]
- Mor, A.; Abramson, S.B.; Pillinger, M.H. The fibroblast-like synovial cell in rheumatoid arthritis: A key player in inflammation and joint destruction. Clin. Immunol. 2005, 115, 118–128. [Google Scholar] [CrossRef] [PubMed]
- Scanzello, C.R.; Goldring, S.R. The role of synovitis in osteoarthritis pathogenesis. Bone 2012, 51, 249–257. [Google Scholar] [CrossRef]
- Jiao, K.; Niu, L.-N.; Wang, M.-Q.; Dai, J.; Yu, S.-B.; Liu, X.-D.; Wang, J. Subchondral bone loss following orthodontically induced cartilage degradation in the mandibular condyles of rats. Bone 2011, 48, 362–371. [Google Scholar] [CrossRef]
- Embree, M.; Ono, M.; Kilts, T.; Walker, D.; Langguth, J.; Mao, J.; Bi, Y.; Barth, J.L.; Young, M. Role of subchondral bone during early-stage experimental TMJ osteoarthritis. J. Dent. Res. 2011, 90, 1331–1338. [Google Scholar] [CrossRef]
- Athanasou, N.A. Cellular biology of bone-resorbing cells. J. Bone Jt. Surg. Am. 1996, 78, 1096–1112. [Google Scholar] [CrossRef]
- Minkin, C. Bone acid phosphatase: Tartrate-resistant acid phosphatase as a marker of osteoclast function. Calcif. Tissue Int. 1982, 34, 285–290. [Google Scholar] [CrossRef]
- Kobayashi, Y.; Udagawa, N.; Takahashi, N. Action of RANKL and OPG for osteoclastogenesis. Crit. Rev. Eukaryot. Gene Expr. 2009, 19, 61–72. [Google Scholar] [CrossRef]
- Dickerson, T.J.; Suzuki, E.; Stanecki, C.; Shin, H.-S.; Qui, H.; Adamopoulos, I.E. Rheumatoid and pyrophosphate arthritis synovial fibroblasts induce osteoclastogenesis independently of RANKL, TNF and IL-6. J. Autoimmun. 2012, 39, 369–376. [Google Scholar] [CrossRef]
- Takayanagi, H.; Iizuka, H.; Juji, T.; Nakagawa, T.; Yamamoto, A.; Miyazaki, T.; Koshihara, Y.; Oda, H.; Nakamura, K.; Tanaka, S. Involvement of receptor activator of nuclear factor kappaB ligand/osteoclast differentiation factor in osteoclastogenesis from synoviocytes in rheumatoid arthritis. Arthritis Rheum. 2000, 43, 259–269. [Google Scholar] [CrossRef]
- Jones, A.R.C.; Chen, S.; Chai, D.H.; Stevens, A.L.; Gleghorn, J.P.; Bonassar, L.J.; Grodzinsky, A.J.; Flannery, C.R. Modulation of lubricin biosynthesis and tissue surface properties following cartilage mechanical injury. Arthritis Rheum. 2009, 60, 133–142. [Google Scholar] [CrossRef] [PubMed]
- Miosge, N.; Hartmann, M.; Maelicke, C.; Herken, R. Expression of collagen type I and type II in consecutive stages of human osteoarthritis. Histochem. Cell Biol. 2004, 122, 229–236. [Google Scholar] [CrossRef] [PubMed]
- Siiskonen, H.; Oikari, S.; Pasonen-Seppänen, S.; Rilla, K. Hyaluronan synthase 1: A mysterious enzyme with unexpected functions. Front. Immunol. 2015, 6, 43. [Google Scholar] [CrossRef] [PubMed]
- Zhong, D.; Zhang, M.; Yu, J.; Luo, Z.-P. Local Tensile Stress in the Development of Posttraumatic Osteoarthritis. Biomed Res. Int. 2018, 2018, 4210353. [Google Scholar] [CrossRef] [PubMed]
- Armaka, M.; Gkretsi, V.; Kontoyiannis, D.; Kollias, G. A standardized protocol for the isolation and culture of normal and arthritogenic murine synovial fibroblasts. Nat. Protoc. 2009. PREPRINT (Version 1). [Google Scholar] [CrossRef]
- Ntougkos, E.; Chouvardas, P.; Roumelioti, F.; Ospelt, C.; Frank-Bertoncelj, M.; Filer, A.; Buckley, C.D.; Gay, S.; Nikolaou, C.; Kollias, G. Genomic Responses of Mouse Synovial Fibroblasts During Tumor Necrosis Factor-Driven Arthritogenesis Greatly Mimic Those in Human Rheumatoid Arthritis. Arthritis Rheum. 2017, 69, 1588–1600. [Google Scholar] [CrossRef]
- Muschter, D.; Beiderbeck, A.-S.; Späth, T.; Kirschneck, C.; Schröder, A.; Grässel, S. Sensory Neuropeptides and their Receptors Participate in Mechano-Regulation of Murine Macrophages. Int. J. Mol. Sci. 2019, 20, 503. [Google Scholar] [CrossRef]
- Lohberger, B.; Kaltenegger, H.; Weigl, L.; Mann, A.; Kullich, W.; Stuendl, N.; Leithner, A.; Steinecker-Frohnwieser, B. Mechanical exposure and diacerein treatment modulates integrin-FAK-MAPKs mechanotransduction in human osteoarthritis chondrocytes. Cell. Signal. 2019, 56, 23–30. [Google Scholar] [CrossRef]
- Nazet, U.; Schröder, A.; Grässel, S.; Muschter, D.; Proff, P.; Kirschneck, C. Housekeeping gene validation for RT-qPCR studies on synovial fibroblasts derived from healthy and osteoarthritic patients with focus on mechanical loading. PLoS ONE 2019, 14, e0225790. [Google Scholar] [CrossRef]
- Lyck, R.; Enzmann, G. The physiological roles of ICAM-1 and ICAM-2 in neutrophil migration into tissues. Curr. Opin. Hematol. 2015, 22, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Ohh, M.; Takei, F. New insights into the regulation of ICAM-1 gene expression. Leuk. Lymphoma 1996, 20, 223–228. [Google Scholar] [CrossRef] [PubMed]
- Bernhardt, O.; Biffar, R.; Kocher, T.; Meyer, G. Prevalence and clinical signs of degenerative temporomandibular joint changes validated by magnetic resonance imaging in a non-patient group. Ann. Anat. 2007, 189, 342–346. [Google Scholar] [CrossRef] [PubMed]
- Völzke, H. Study of Health in Pomerania (SHIP). Konzept, Kohortendesign und ausgewählte Ergebnisse. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 2012, 55, 790–794. [Google Scholar] [CrossRef]
- Schmitter, M.; Essig, M.; Seneadza, V.; Balke, Z.; Schröder, J.; Rammelsberg, P. Prevalence of clinical and radiographic signs of osteoarthrosis of the temporomandibular joint in an older persons community. Dentomaxillofac. Radiol. 2010, 39, 231–234. [Google Scholar] [CrossRef]
- Tanne, K.; Okamoto, Y.; Su, S.-C.; Mitsuyoshi, T.; Asakawa-Tanne, Y.; Tanimoto, K. Current status of temporomandibular joint disorders and the therapeutic system derived from a series of biomechanical, histological, and biochemical studies. APOS Trends Orthod. 2015, 5, 4–21. [Google Scholar] [CrossRef]
- Slade, G.D.; Conrad, M.S.; Diatchenko, L.; Rashid, N.U.; Zhong, S.; Smith, S.; Rhodes, J.; Medvedev, A.; Makarov, S.; Maixner, W.; et al. Cytokine biomarkers and chronic pain: Association of genes, transcription, and circulating proteins with temporomandibular disorders and widespread palpation tenderness. Pain 2011, 152, 2802–2812. [Google Scholar] [CrossRef]
- Kaneyama, K.; Segami, N.; Yoshimura, H.; Honjo, M.; Demura, N. Increased levels of soluble cytokine receptors in the synovial fluid of temporomandibular joint disorders in relation to joint effusion on magnetic resonance images. J. Oral Maxillofac. Surg. 2010, 68, 1088–1093. [Google Scholar] [CrossRef]
- Kim, Y.-K.; Kim, S.-G.; Kim, B.-S.; Lee, J.-Y.; Yun, P.-Y.; Bae, J.-H.; Oh, J.-S.; Ahn, J.-M.; Kim, J.-S.; Lee, S.-Y. Analysis of the cytokine profiles of the synovial fluid in a normal temporomandibular joint: Preliminary study. J. Craniomaxillofac. Surg. 2012, 40, e337–e341. [Google Scholar] [CrossRef]
- Wang, X.D.; Kou, X.X.; Mao, J.J.; Gan, Y.H.; Zhou, Y.H. Sustained inflammation induces degeneration of the temporomandibular joint. J. Dent. Res. 2012, 91, 499–505. [Google Scholar] [CrossRef]
- Moreno-Rubio, J.; Herrero-Beaumont, G.; Tardio, L.; Alvarez-Soria, M.A.; Largo, R. Nonsteroidal antiinflammatory drugs and prostaglandin E(2) modulate the synthesis of osteoprotegerin and RANKL in the cartilage of patients with severe knee osteoarthritis. Arthritis Rheum. 2010, 62, 478–488. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Ellman, M.; Muddasani, P.; Wang, J.H.-C.; Cs-Szabo, G.; van Wijnen, A.J.; Im, H.-J. Prostaglandin E2 and its cognate EP receptors control human adult articular cartilage homeostasis and are linked to the pathophysiology of osteoarthritis. Arthritis Rheum. 2009, 60, 513–523. [Google Scholar] [CrossRef] [PubMed]
- Asakawa-Tanne, Y.; Su, S.; Kunimatsu, R.; Hirose, N.; Mitsuyoshi, T.; Okamoto, Y.; Tanaka, E.; Tanne, K.; Tanimoto, K. Effects of enzymatic degradation after loading in temporomandibular joint. J. Dent. Res. 2015, 94, 337–343. [Google Scholar] [CrossRef] [PubMed]
- Kopp, S.; Alstergren, P.; Ernestam, S.; Nordahl, S.; Morin, P.; Bratt, J. Reduction of temporomandibular joint pain after treatment with a combination of methotrexate and infliximab is associated with changes in synovial fluid and plasma cytokines in rheumatoid arthritis. Cells Tissues Organs 2005, 180, 22–30. [Google Scholar] [CrossRef]
- Arend, W.P.; Welgus, H.G.; Thompson, R.C.; Eisenberg, S.P. Biological properties of recombinant human monocyte-derived interleukin 1 receptor antagonist. J. Clin. Investig. 1990, 85, 1694–1697. [Google Scholar] [CrossRef]
- Davis, A.J.; Perkins, M.N. The involvement of bradykinin B1 and B2 receptor mechanisms in cytokine-induced mechanical hyperalgesia in the rat. Br. J. Pharmacol. 1994, 113, 63–68. [Google Scholar] [CrossRef]
- Yang, Y.; Zhou, X.; Li, Y.; Chen, A.; Liang, W.; Liang, G.; Huang, B.; Li, Q.; Jin, D. CXCL2 attenuates osteoblast differentiation by inhibiting the ERK1/2 signaling pathway. J. Cell Sci. 2019, 132, jcs230490. [Google Scholar] [CrossRef]
- De Filippo, K.; Dudeck, A.; Hasenberg, M.; Nye, E.; van Rooijen, N.; Hartmann, K.; Gunzer, M.; Roers, A.; Hogg, N. Mast cell and macrophage chemokines CXCL1/CXCL2 control the early stage of neutrophil recruitment during tissue inflammation. Blood 2013, 121, 4930–4937. [Google Scholar] [CrossRef]
- Vernal, R.; Velásquez, E.; Gamonal, J.; Garcia-Sanz, J.A.; Silva, A.; Sanz, M. Expression of proinflammatory cytokines in osteoarthritis of the temporomandibular joint. Arch. Oral Biol. 2008, 53, 910–915. [Google Scholar] [CrossRef]
- Hou, S.-M.; Chen, P.-C.; Lin, C.-M.; Fang, M.-L.; Chi, M.-C.; Liu, J.-F. CXCL1 contributes to IL-6 expression in osteoarthritis and rheumatoid arthritis synovial fibroblasts by CXCR2, c-Raf, MAPK, and AP-1 pathway. Arthritis Res. Ther. 2020, 22, 251. [Google Scholar] [CrossRef]
- Sanchez, C.; Pesesse, L.; Gabay, O.; Delcour, J.-P.; Msika, P.; Baudouin, C.; Henrotin, Y.E. Regulation of subchondral bone osteoblast metabolism by cyclic compression. Arthritis Rheum. 2012, 64, 1193–1203. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Sorensen, K.P.; Gupta, T.; Kilts, T.; Young, M.; Wadhwa, S. Altered functional loading causes differential effects in the subchondral bone and condylar cartilage in the temporomandibular joint from young mice. Osteoarthr. Cartil. 2009, 17, 354–361. [Google Scholar] [CrossRef] [PubMed]
- Monasterio, G.; Castillo, F.; Rojas, L.; Cafferata, E.A.; Alvarez, C.; Carvajal, P.; Núñez, C.; Flores, G.; Díaz, W.; Vernal, R. Th1/Th17/Th22 immune response and their association with joint pain, imagenological bone loss, RANKL expression and osteoclast activity in temporomandibular joint osteoarthritis: A preliminary report. J. Oral Rehabil. 2018, 45, 589–597. [Google Scholar] [CrossRef] [PubMed]
- McDonald, J.N.; Levick, J.R. Effect of intra-articular hyaluronan on pressure-flow relation across synovium in anaesthetized rabbits. J. Physiol. 1995, 485, 179–193. [Google Scholar] [CrossRef]
- Ogston, A.G.; Stanier, J.E. The physiological function of hyaluronic acid in synovial fluid; viscous, elastic and lubricant properties. J. Physiol. 1953, 119, 244–252. [Google Scholar] [CrossRef]
- Bollet, A.J. The intrinsic viscosity of synovial fluid hyaluronic acid. J. Lab. Clin. Med. 1956, 48, 721–728. [Google Scholar]
- Decker, B.; McGuckin, W.F.; McKenzie, B.F.; Slocumb, C.H. Concentration of hyaluronic acid in synovial fluid. Clin. Chem. 1959, 5, 465–469. [Google Scholar] [CrossRef]
- Gomez, J.E.; Thurston, G.B. Comparisons of the oscillatory shear viscoelasticity and composition of pathological synovial fluids. Biorheology 1993, 30, 409–427. [Google Scholar] [CrossRef]
- Caskey, R.C.; Allukian, M.; Lind, R.C.; Herdrich, B.J.; Xu, J.; Radu, A.; Mitchell, M.E.; Liechty, K.W. Lentiviral-mediated over-expression of hyaluronan synthase-1 (HAS-1) decreases the cellular inflammatory response and results in regenerative wound repair. Cell Tissue Res. 2013, 351, 117–125. [Google Scholar] [CrossRef]
- Stuhlmeier, K.M.; Pollaschek, C. Differential effect of transforming growth factor beta (TGF-beta) on the genes encoding hyaluronan synthases and utilization of the p38 MAPK pathway in TGF-beta-induced hyaluronan synthase 1 activation. J. Biol. Chem. 2004, 279, 8753–8760. [Google Scholar] [CrossRef]
- Yamada, Y.; Itano, N.; Hata, K.-I.; Ueda, M.; Kimata, K. Differential regulation by IL-1beta and EGF of expression of three different hyaluronan synthases in oral mucosal epithelial cells and fibroblasts and dermal fibroblasts: Quantitative analysis using real-time RT-PCR. J. Investig. Dermatol. 2004, 122, 631–639. [Google Scholar] [CrossRef] [PubMed]
- Tammi, R.H.; Passi, A.G.; Rilla, K.; Karousou, E.; Vigetti, D.; Makkonen, K.; Tammi, M.I. Transcriptional and post-translational regulation of hyaluronan synthesis. FEBS J. 2011, 278, 1419–1428. [Google Scholar] [CrossRef] [PubMed]
- Cheng, G.; Swaidani, S.; Sharma, M.; Lauer, M.E.; Hascall, V.C.; Aronica, M.A. Hyaluronan deposition and correlation with inflammation in a murine ovalbumin model of asthma. Matrix Biol. 2011, 30, 126–134. [Google Scholar] [CrossRef] [PubMed]
- Elsaid, K.A.; Jay, G.D.; Warman, M.L.; Rhee, D.K.; Chichester, C.O. Association of articular cartilage degradation and loss of boundary-lubricating ability of synovial fluid following injury and inflammatory arthritis. Arthritis Rheum. 2005, 52, 1746–1755. [Google Scholar] [CrossRef]
- Sato, T.; Konomi, K.; Yamasaki, S.; Aratani, S.; Tsuchimochi, K.; Yokouchi, M.; Masuko-Hongo, K.; Yagishita, N.; Nakamura, H.; Komiya, S.; et al. Comparative analysis of gene expression profiles in intact and damaged regions of human osteoarthritic cartilage. Arthritis Rheum. 2006, 54, 808–817. [Google Scholar] [CrossRef]
- Sanchez, A.; Blanco, M.; Correa, B.; Perez-Martin, R.I.; Sotelo, C.G. Effect of Fish Collagen Hydrolysates on Type I Collagen mRNA Levels of Human Dermal Fibroblast Culture. Mar. Drugs 2018, 16, 144. [Google Scholar] [CrossRef]
- Kubein-Meesenburg, D.; Nägerl, H.; Fialka-Fricke, J.; Hahn, W.; Weber, S.; Hönig, J.; Hansen, C.; Fanghänel, J.; Thieme, K.M.; Ihlow, D. Functional states of mandibular movements and synovial pumps of the temporomandibular joint. Is it possible to provide a biomechanically correct replacement for the TMJ? Ann. Anat. 2012, 194, 200–207. [Google Scholar] [CrossRef]
- Xu, Y.; Zhan, J.; Zheng, Y.; Han, Y.; Zhang, Z.; Xi, Y.; Zhu, P. Synovial fluid dynamics with small disc perforation in temporomandibular joint. J. Oral Rehabil. 2012, 39, 719–726. [Google Scholar] [CrossRef]
| Gene-Symbol | Gene Name | 5′-Forward Primer-3′ | 5′-Reverse Primer-3′ |
|---|---|---|---|
| Alpl | alkaline phosphatase | GGGGTACAAGGCTAGATGGC | AGTTCAGTGCGGTTCCAGAC |
| Col1a2 | collagen, type I, alpha 2 | TGGCCCCAATGGATTTGCTG | CCTTAGGCCCTTTGGTTCCC |
| Cxcl-1 | C-X-C motif chemokine ligand 1 | CTGGGATTCACCTCAAGAACATC | CAGGGTCAAGGCAAGCCTC |
| Cxcl-2 | C-X-C motif chemokine ligand 2 | TTAAAAACCTGGATCGGAACCAA | GCATTAGCTTCAGATTTACGGGT |
| Fmod | fibromodulin | CCTCCTGTCAACACCAACCTGG | TTCCCATCCAGGCGTAGCAC |
| Fn-1 | fibronectin 1 | AGCCAGGAACCGAGTACACC | AGCCAGGAACCGAGTACACC |
| Gapdh | glyceraldehyde-3-phosphate dehydrogenase | GTCATCCCAGAGCTGAACGG | ATGCCTGCTTCACCACCTTC |
| Has-1 | hyaluronan synthase 1 | TGACAGGCACCTCACCAACC | TGGCTCAACCAACGAAGGAAGG |
| Hprt | hypoxanthine guanine phosphoribosyl transferase | AGCTTGCTGGTGAAAAGGAC | AGTCAAGGGCATATCCAACAAC |
| Icam-1 | intercellular adhesion molecule 1 | GTGATGCTCAGGTATCCATCCA | CACAGTTCTCAAAGCACAGCG |
| Il-1β | Interleukin-1 β | GTGTAATGAAAGACGGCACACC | ACCAGTTGGGGAACTCTGC |
| Il1-ra | Interleukin-1 receptor antagonist | GCTCATTGCTGGGTACTTACAA | CCAGACTTGGCACAAGACAGG |
| Il-6 | Interleukin-6 | ACAAAGCCAGAGTCCTTCAGAG | GAGCATTGGAAATTGGGGTAGG |
| Ncam-1 | neural cell adhesion molecule 1 | GTCACTCTGACCTGTGAAGCC | CACCATGTGCCCATCCAGAG |
| Opg | osteoprotegerin | CCTTGCCCTGACCACTCTTAT | CACACACTCGGTTGTGGGT |
| P4ha-1 | prolyl 4-hydroxylase subunit alpha 1 | GTCTGGCTACGAAGACCCTGTG | GGGGCTCATACTGTCCTCCAAC |
| Postn | periostin | TCATTGAAGGTGGCGATGGTC | AACGGCCTTCTCTTGATCGTC |
| Ptgs-2 | prostaglandin-endoperoxide synthase 2 | TCCCTGAAGCCGTACACATC | TCCCCAAAGATAGCATCTGGAC |
| Rankl | tumor necrosis factor superfamily, member 11 | AAACGCAGATTTGCAGGACTC | CCCCACAATGTGTTGCAGTTC |
| Runx-2 | runt related transcription factor 2 | GACGTGCCCAGGCGTATTTC | CACCTGCCTGGCTCTTCTTAC |
| Scx | scleraxis | AGAACACCCAGCCCAAACAG | ATCGCCGTCTTTCTGTCACG |
| Sdha | succinate dehydrogenase complex, subunit A, flavoprotein | AACACTGGAGGAAGCACACC | AGTAGGAGCGGATAGCAGGAG |
| Smad-1 | SMAD family member 1 | CGGGTTCGAGACCGTGTATG | GGGGTGCTGGTAACATCCTG |
| Vim | vimentin | TTCTCTGGCACGTCTTGACC | GCTTGGAAACGTCCACATCG |
| Ywhaz | tyrosine 3-monooxygenase/tryptophan 5-monooxygenase activation protein | AATGCTTCGCAACCAGAAAGC | TGGTATGCTTGCTGTGACTGG |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nazet, U.; Feulner, L.; Muschter, D.; Neubert, P.; Schatz, V.; Grässel, S.; Jantsch, J.; Proff, P.; Schröder, A.; Kirschneck, C. Mechanical Stress Induce PG-E2 in Murine Synovial Fibroblasts Originating from the Temporomandibular Joint. Cells 2021, 10, 298. https://doi.org/10.3390/cells10020298
Nazet U, Feulner L, Muschter D, Neubert P, Schatz V, Grässel S, Jantsch J, Proff P, Schröder A, Kirschneck C. Mechanical Stress Induce PG-E2 in Murine Synovial Fibroblasts Originating from the Temporomandibular Joint. Cells. 2021; 10(2):298. https://doi.org/10.3390/cells10020298
Chicago/Turabian StyleNazet, Ute, Laura Feulner, Dominique Muschter, Patrick Neubert, Valentin Schatz, Susanne Grässel, Jonathan Jantsch, Peter Proff, Agnes Schröder, and Christian Kirschneck. 2021. "Mechanical Stress Induce PG-E2 in Murine Synovial Fibroblasts Originating from the Temporomandibular Joint" Cells 10, no. 2: 298. https://doi.org/10.3390/cells10020298
APA StyleNazet, U., Feulner, L., Muschter, D., Neubert, P., Schatz, V., Grässel, S., Jantsch, J., Proff, P., Schröder, A., & Kirschneck, C. (2021). Mechanical Stress Induce PG-E2 in Murine Synovial Fibroblasts Originating from the Temporomandibular Joint. Cells, 10(2), 298. https://doi.org/10.3390/cells10020298







