In Vitro and In Vivo Comparison Study of Electrospun PLA and PLA/PVA/SA Fiber Membranes for Wound Healing
Abstract
1. Introduction
2. Methods
2.1. Materials
2.2. Preparation and Characterization of the Materials
2.3. In Vitro Cytocompatibility
2.4. Animal Experiments
2.5. Histology
2.6. Immunohistochemistry
2.7. Western Blot Analysis
2.8. qRT-PCR Analysis
3. Results and Discussion
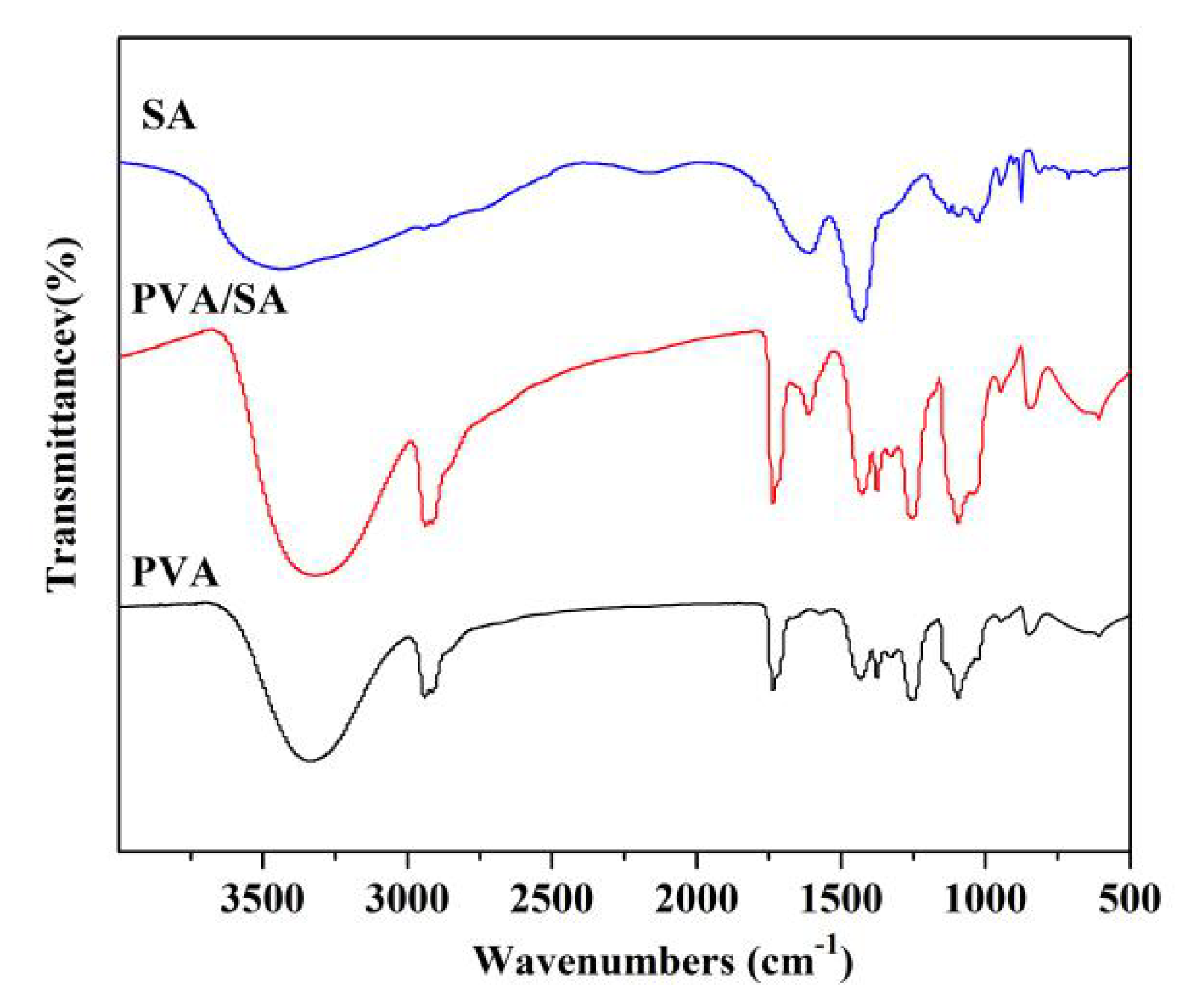
3.1. Morphology and Performance of Material
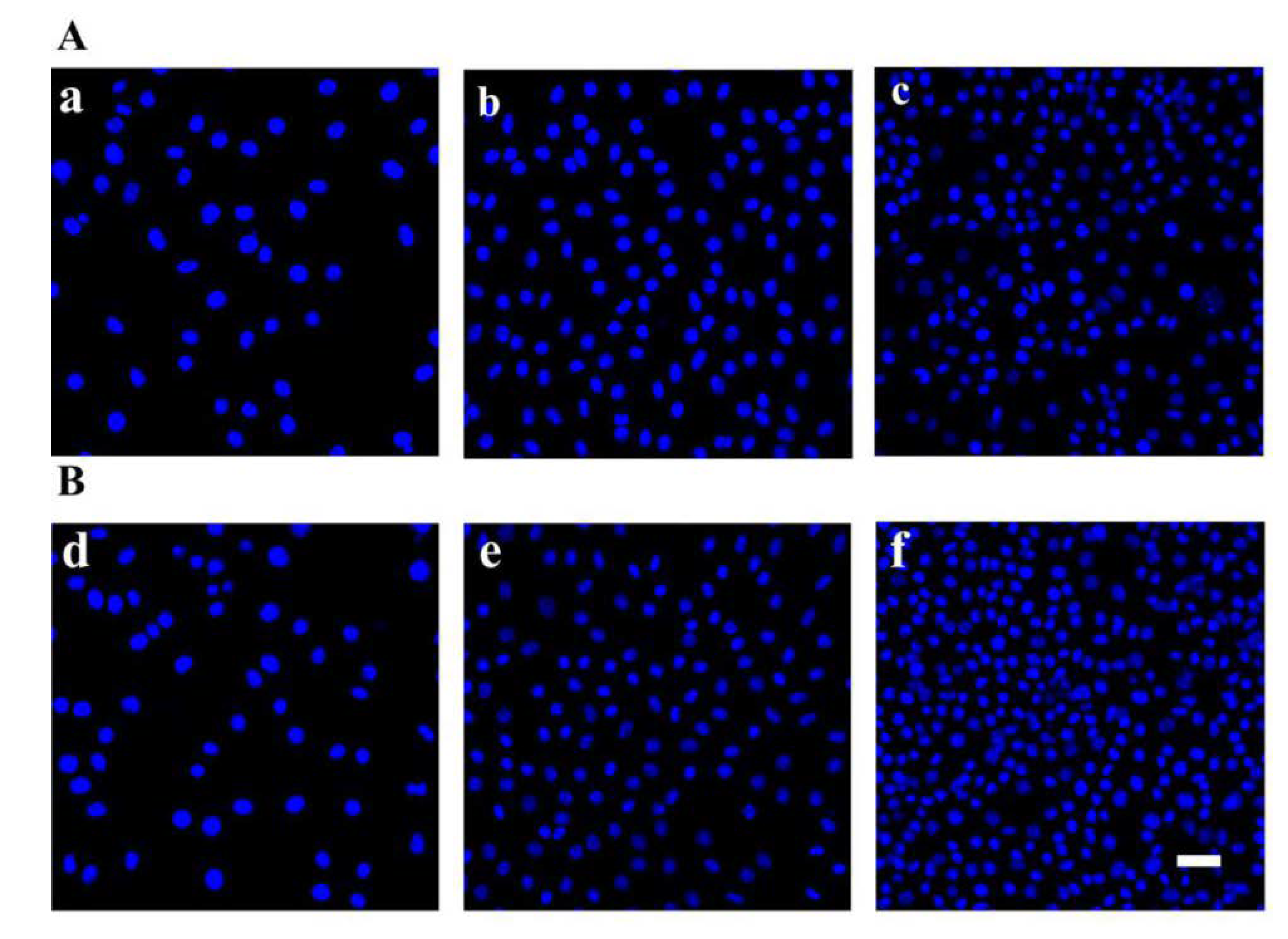
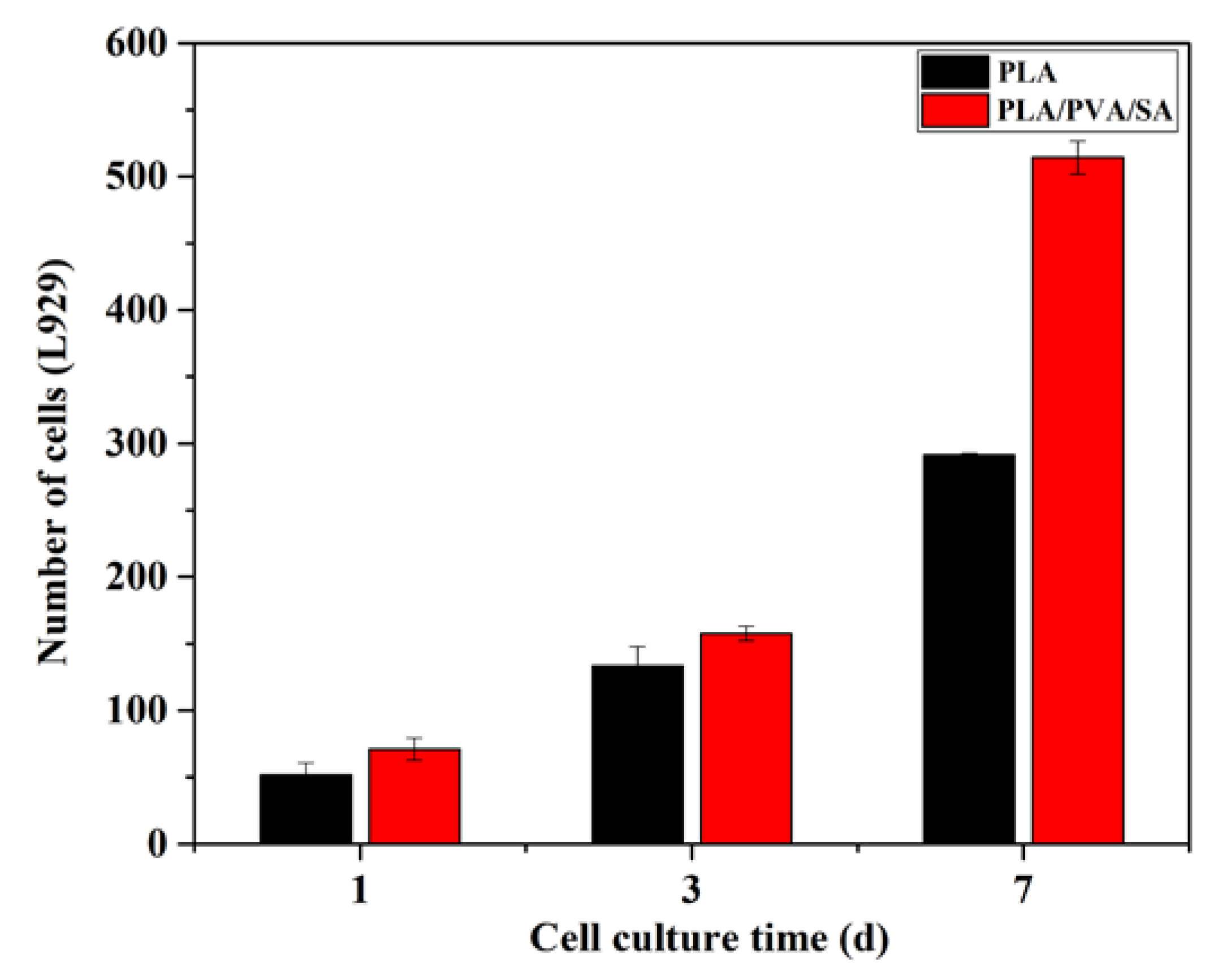
3.2. In Vitro Compatibility
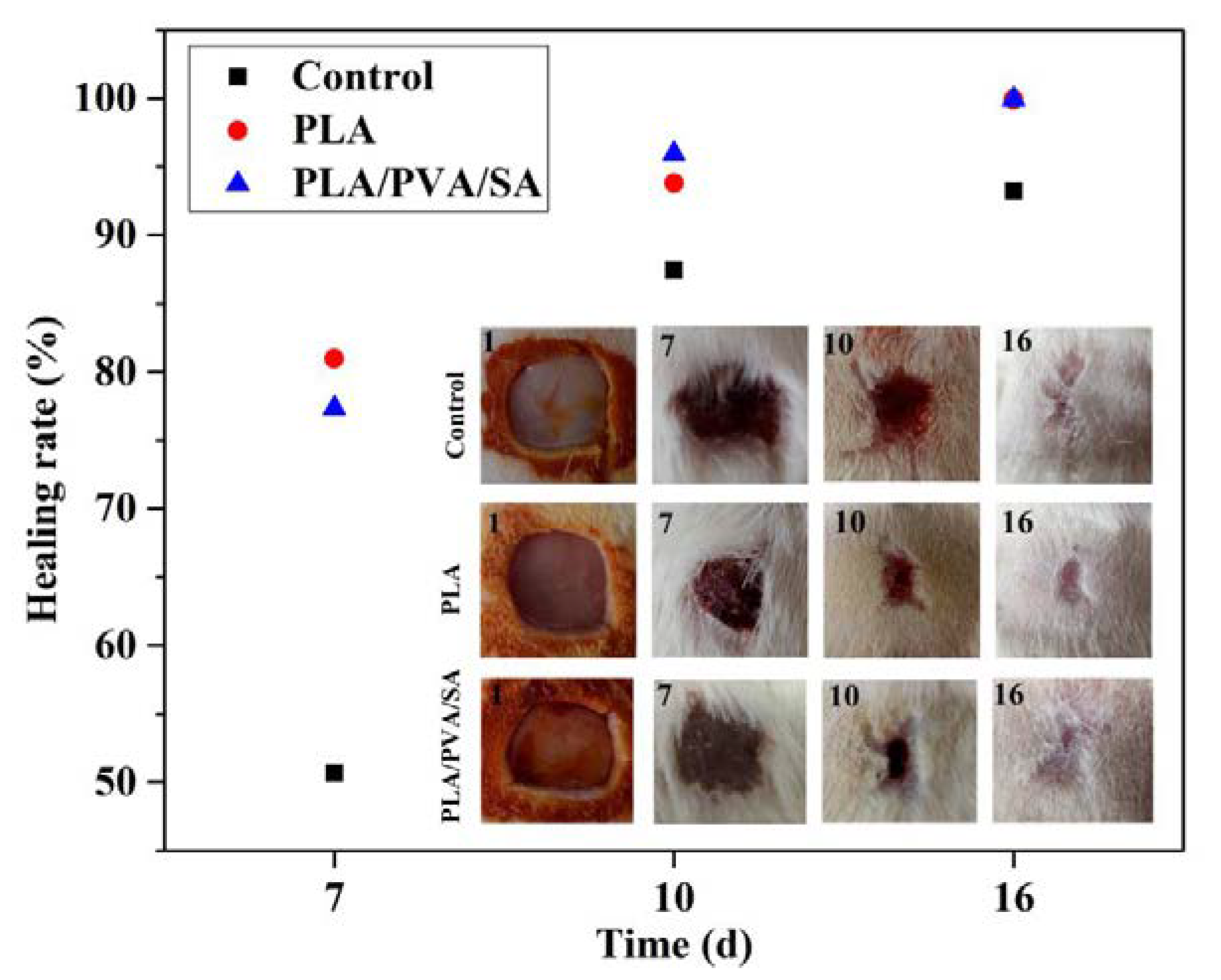
3.3. In Vivo Assessments
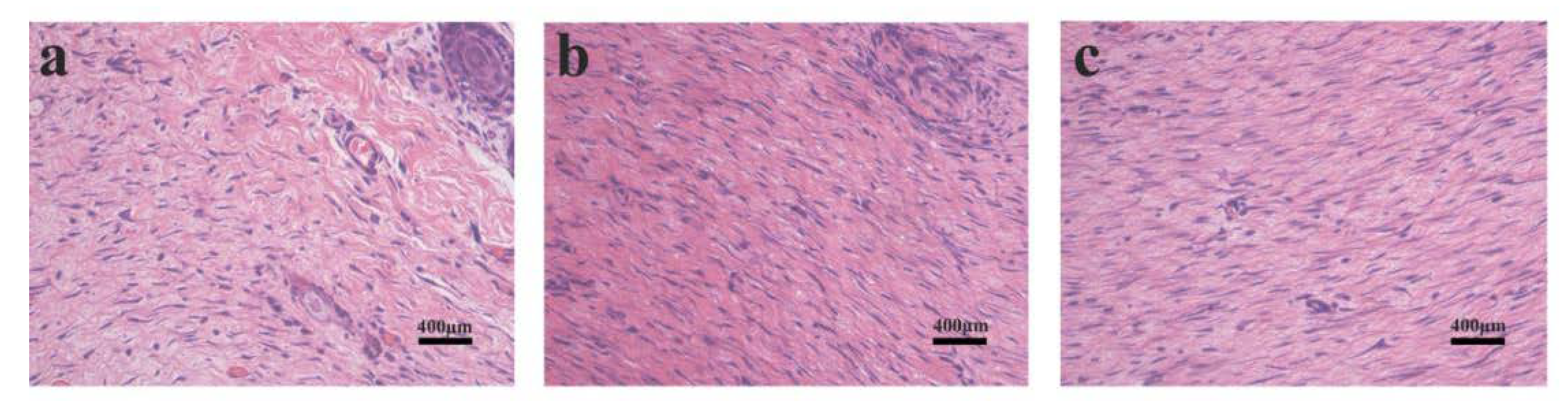
3.4. Histological Assessments
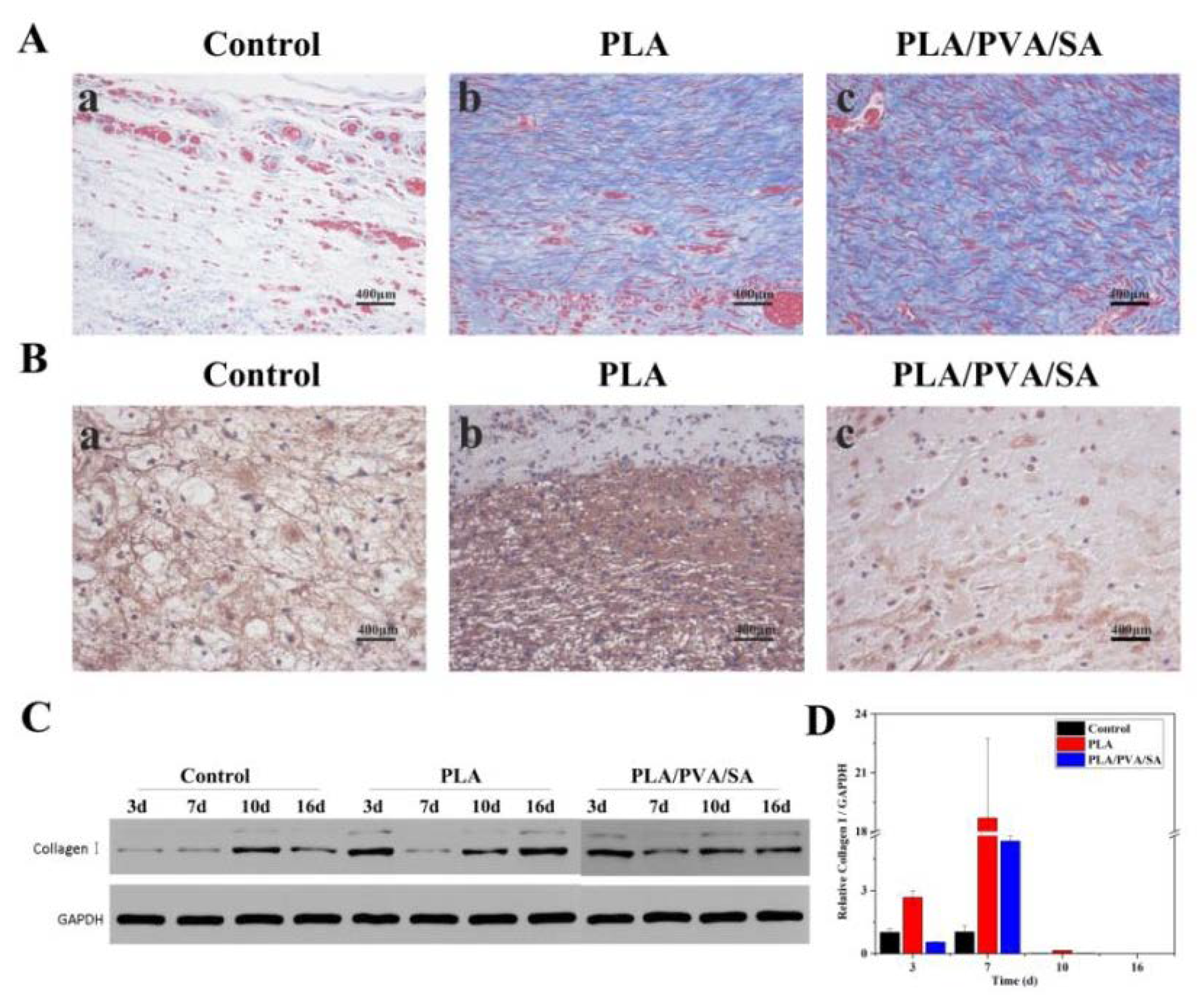
3.5. Collagen Deposition
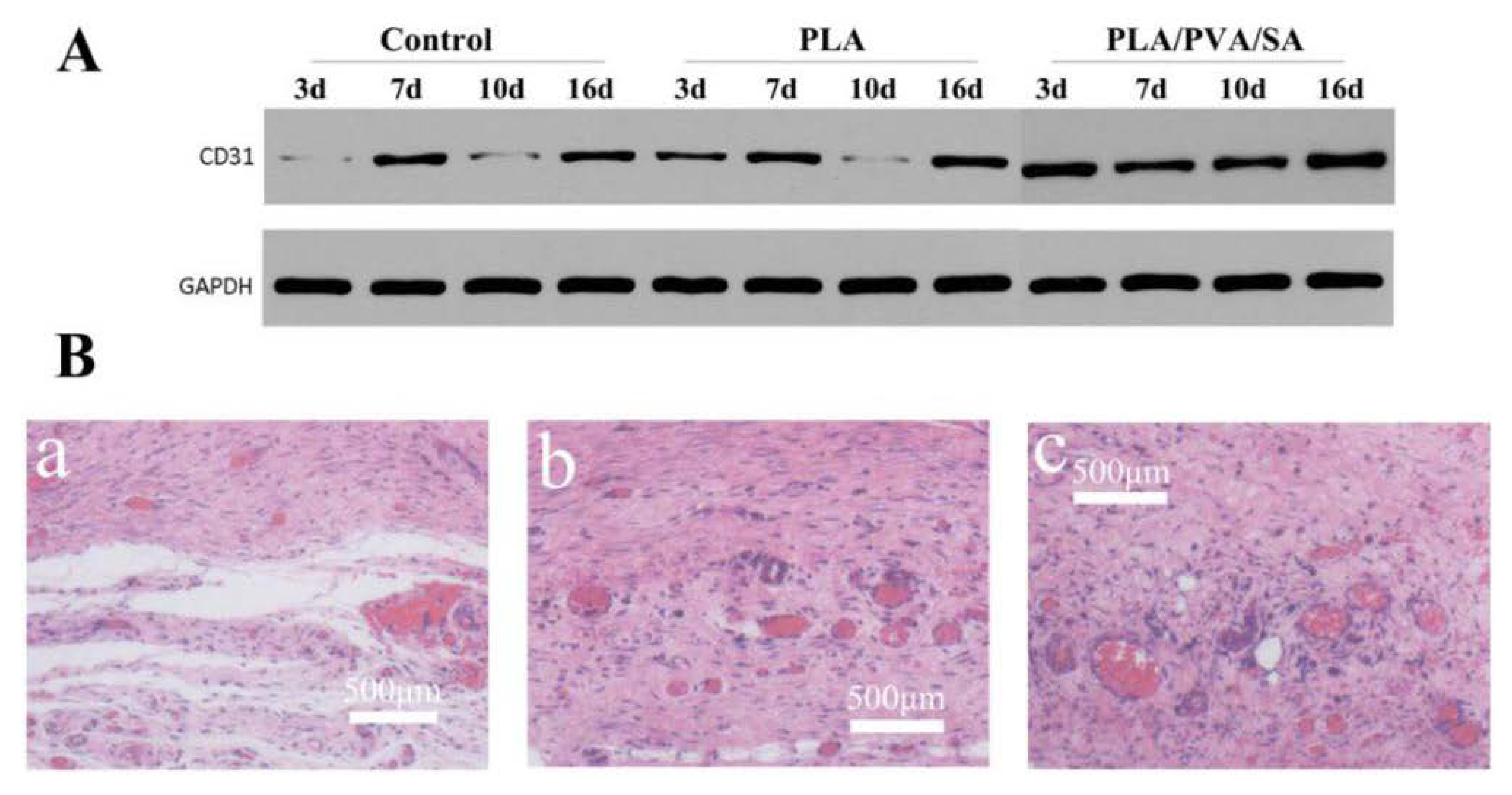
3.6. Effects of PLA and PLA/PVA/SA Fiber Membranes on Wound Angiogenesis
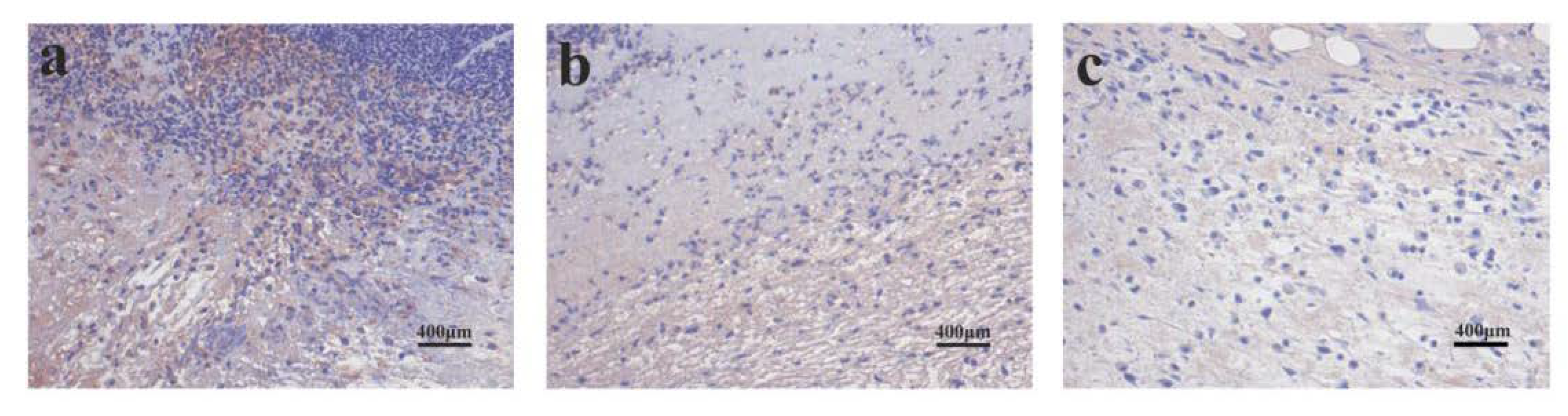
3.7. PLA and PLA/PVA/SA Membranes Prevent Inflammation
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Brown, A.L.; Tonelli, A.E.; Hudson, S.M.; Gupta, B.S. A hybrid bioabsorbable wound dressing. Acs Symp. 2001, 792, 90–114. [Google Scholar]
- Gurtner, G.C.; Werner, S.; Barrandon, Y.; Longaker, M.T. Wound repair and regeneration. Wound Repair Regen. 2010, 11, 5A–8A. [Google Scholar] [CrossRef] [PubMed]
- Tomoko, I.; Naoki, O.; Kentaro, M.; Masazumi, E.; Yoshiyuki, K. Bioadhesive and biodissolvable hydrogels consisting of water-swellable poly(acrylic acid)/poly(vinylpyrrolidone) complexes. J. Biomed. Mater. Res. Part B Appl. Biomater. 2019, 108, 1–10. [Google Scholar]
- Qu, J.; Zhao, X.; Liang, Y.P.; Xu, Y.M.; Ma, P.X.; Guo, B.L. Degradable conductive injectable hydrogels as novel antibacterial, anti-oxidant wound dressings for wound healing. Chem. Eng. J. 2019, 362, 548–560. [Google Scholar] [CrossRef]
- Cheng, H.; Li, C.; Jiang, Y.; Wang, B.; Mao, F.; Xu, H.; Sui, X. Facile preparation of polysaccharide-based sponges and its potential application in wound dressing. J. Mater. Chem. B 2018, 6, 634–640. [Google Scholar] [CrossRef]
- Zhang, K.X.; Bai, X.F.; Yuan, Z.P.; Cao, X.T.; Jiao, X.Y.; Li, Y.S.; Qin, Y. Layered nanofiber sponge with an improved capacity for promoting blood coagulation and wound healing. Biomaterials 2019, 204, 70–79. [Google Scholar] [CrossRef]
- Ni, P.L.; Bi, H.Y.; Zhao, G.; Han, Y.C.; Wickramaratne, M.N.; Dai, H.L.; Wang, X.Y. Electrospun preparation and biological properties in vitro of poly(vinyl alcohol)/sodium alginate/nano-hydroxyapatite composite fiber membrane. Colloids Surf. B Biointerfaces 2019, 173, 171–177. [Google Scholar] [CrossRef]
- Bhattarai, S.R.; Bhattarai, N.; Yi, H.K.; Hwang, P.H.; Cha, D.I.; Kim, H.Y. Novel biodegradable electrospun membrane: Scaffold for tissue engineering. Biomaterials 2014, 25, 2595–2602. [Google Scholar] [CrossRef]
- Zahedi, P.; Rezaeian, I.; Ranaei-Siadat, S.O.; Jafari, S.H.; Supaphol, P. A review on wound dressing with an emphasis on electrospun nanofibrous polymeric bandages. Polym. Adv. Technol. 2009, 21, 77–95. [Google Scholar] [CrossRef]
- Cheng, J.; Jun, Y.; Qin, J.; Lee, S.H. Electrospinning versus microfluidic spinning of functional fibers for biomedical applications. Biomaterials 2016, 114, 121. [Google Scholar] [CrossRef]
- Dias, J.R.; Granja, P.L.; Bártolo, P.J. Advances in electrospun skin substitutes. Prog. Mater. Sci. 2016, 84, 314–334. [Google Scholar] [CrossRef]
- Li, H.; Williams, G.R.; Wu, J.; Wang, H.; Sun, X.; Zhu, L. Poly(n-isopropylacrylamide)/poly(l-lactic acid-co-ε-caprolactone) fibers loaded with ciprofloxacin as wound dressing materials. Mater. Sci. Eng. C 2017, 79, 245–254. [Google Scholar] [CrossRef] [PubMed]
- Rezvani, Z.; Venugopal, J.R.; Urbanska, A.M.; Mills, D.K.; Ramakrishna, S.; Mozafari, M. A bird’s eye view on the use of electrospun nanofibrous scaffolds for bone tissue engineering: Current state-of-the-art, emerging directions and future trends. Nanomed. Nanotechnol. Biol. Med. 2016, 12, 2181–2200. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.L.; Hai, T.; Feng, Z.B.; Yu, D.G.; Yang, Y.Y.; Annie Bligh, S.W. The relationships between the working fluids, process characteristics and products from the modifified coaxial electrospinning of zein. Polymers 2019, 11, 1287. [Google Scholar] [CrossRef]
- Zhao, K.; Wang, W.; Yang, Y.Y.; Wang, K.; Yu, D.G. From Taylor cone to solid nanofifiber in tri-axial electrospinning: Size relationships. Results Phys. 2019, 15, 102770. [Google Scholar] [CrossRef]
- Wang, M.G.; Wang, K.; Yang, Y.Y.; Liu, Y.G.; Yu, D.G. Electrospun environment remediation nanofifibers using unspinnable liquids as the sheath fluids: A review. Polymers 2020, 12, 103. [Google Scholar] [CrossRef]
- Yu, D.G.; Wang, M.L.; Li, X.Y.; Liu, X.K.; Zhu, L.M.; Annie Bligh, S.W. Multifluid electrospinning for the generation of complex nanostructures. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnol. 2019. [Google Scholar] [CrossRef]
- Yang, Y.Y.; Zhu, T.H.; Liu, Z.P.; Luo, M.Y.; Yu, D.G.; Annie Bligh, S.W. The key role of straight flfluid jet in predicting the drug dissolution from electrospun nanofifibers. Int. J. Pharm. 2019, 569, 118634. [Google Scholar] [CrossRef]
- Heydari, Z.; Mohebbi-Kalhori, D.; Afarani, M.S. Engineered electrospun poly(caprolactone) (pcl)/octacalcium phosphate (ocp) scaffold for bone tissue engineering. Mater. Sci. Eng. C 2017, 81, 127. [Google Scholar] [CrossRef]
- Drumright, R.E.; Gruber, P.R.; Henton, D.E. Poly(lactic acid)technology. Adv. Mater. 2000, 12, 1841–1846. [Google Scholar] [CrossRef]
- Hamad, K.; Kaseem, M.; Yang, H.W.; Deri, F.; Ko, Y.G. Properties and medical applications of poly(lactic acid): A review. Express Polym. Lett. 2015, 9, 435–455. [Google Scholar] [CrossRef]
- Tyler, B.; Gullotti, D.; Mangraviti, A.; Utsuki, T.; Brem, H. Poly(lactic acid) (pla) controlled delivery carriers for biomedical applications. Adv. Drug Deliv. Rev. 2016, 107, 163–175. [Google Scholar] [CrossRef] [PubMed]
- Saini, P.; Arora, M.; Kumar, M.N.V.R. Poly(lactic acid) blends in biomedical applications. Adv. Drug Deliv. Rev. 2016, 107, 47–59. [Google Scholar] [CrossRef]
- Taemeh, M.K.; Shiravandi, A.; Korayem, M.A.; Daemi, H. Fabrication challenges and trends in biomedical applications of alginate electrospun nanofibers. Carbohydr. Polym. 2019, 228, 115419. [Google Scholar] [CrossRef]
- Naghshineh, N.; Tahvildari, K.; Nozari, M. Preparation of chitosan, sodium alginate, gelatin and collagen biodegradable sponge composites and their application in wound healing and curcumin delivery. J. Polym. Environ. 2019, 27, 2819–2830. [Google Scholar] [CrossRef]
- Pan, H.; Fan, D.D.; Zhu, C.H.; Duan, Z.G.; Fu, R.Z.; Li, X. Preparation of physically crosslinked PVA/HLC/SA hydrogel and exploration of its effects on full-thickness skin defects. Int. J. Polym. Mater. 2019, 1–10. [Google Scholar] [CrossRef]
- Niranjan, R.; Kaushik, M.; Selvi, R.T.; Prakash, J.; Venkataprasanna, K.S.; Prema, D.; Pannerselvam, B. PVA/SA/TiO2-CUR patch for enhanced wound healing application: In vitro and in vivo analysis. Int. J. Boil. Macromol. 2019, 138, 704–717. [Google Scholar] [CrossRef]
- Sharma, K.; Bullock, A.; Ralsto, N.D.; Macneil, S. Development of a one-step approach for the reconstruction of full thickness skin defects using minced split thickness skin grafts and biodegradable synthetic scaffolds as a dermal substitute. Burns 2014, 40, 957–965. [Google Scholar] [CrossRef]
- Nguyen, T.T.T.; Ghosh, C.; Hwang, S.G.; Tran, L.D.; Park, J.S. Characteristics of curcumin-loaded poly(lactic acid) nanofibers for wound healing. J. Mater. Sci. 2013, 48, 7125–7133. [Google Scholar] [CrossRef]
- Chen, K.; Wang, F.Y.; Liu, S.Y.; Wu, X.F.; Xu, L.M.; Zhang, D.K. In situ reduction of silver nanoparticles by sodium alginate to obtain silver-loaded composite wound dressing with enhanced mechanical and antimicrobial property. Biol. Macromol. 2020, 1, 156. [Google Scholar] [CrossRef] [PubMed]
- Tang, Y.D.; Lan, X.Z.; Liang, C.F.; Zhong, Z.X.; Xie, R.T.; Zhou, Y.; Miao, X.M. Honey loaded alginate/PVA nanofibrous membrane as potential bioactive wound dressing. Carbohydr. Polym. 2019, 219, 113–120. [Google Scholar] [CrossRef] [PubMed]
- Lv, F.; Wang, J.; Xu, P.; Han, Y.; Ma, H.; Xu, H. A conducive bioceramic/polymer composite biomaterial for diabetic wound healing. Acta Biomater. 2017, 60, 128–143. [Google Scholar] [CrossRef] [PubMed]
- Martins, A.; Araújo, J.V.; Reis, R.L.; Neves, N.M. Electrospun nanostructured scaffolds for tissue engineering applications. Nanomedicine 2007, 2, 929–942. [Google Scholar] [CrossRef] [PubMed]
- Abrigo, M.; Mcarthur, S.L.; Kingshott, P. Electrospun nanofibers as dressings for chronic wound care: Advances, challenges, and future prospects. Macromol. Biosci. 2014, 14, 772–792. [Google Scholar] [CrossRef] [PubMed]
- Bhattarai, N.; Edmondson, D.; Veiseh, O.; Matsen, F.A.; Zhang, M. Electrospun chitosan-based nanofibers and their cellular compatibility. Biomaterials 2005, 26, 6176–6184. [Google Scholar] [CrossRef]
- García-Orue, I.; Gainza, G.; Gutierrez, F.B.; Aguirre, J.J.; Evora, C.; Pedraz, J.L.; Hernandez, R.M.; Delgado, A.; Lgartua, M. Novel nanofibrous dressings containing rhegf and aloe vera for wound healing applications. Int. J. Pharm. 2016, 523, 556–566. [Google Scholar] [CrossRef]
- Kanani, A.G.; Bahrami, S.H.; Taftei, H.A.; Rabbani, S.; Sotoudeh, M. Effect of chitosan-poly(vinyl alcohol) blend nanofibrous web on the healing of excision and incision full thickness wounds. IET Nanobiotechnology 2010, 4, 109–117. [Google Scholar] [CrossRef]




© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bi, H.; Feng, T.; Li, B.; Han, Y. In Vitro and In Vivo Comparison Study of Electrospun PLA and PLA/PVA/SA Fiber Membranes for Wound Healing. Polymers 2020, 12, 839. https://doi.org/10.3390/polym12040839
Bi H, Feng T, Li B, Han Y. In Vitro and In Vivo Comparison Study of Electrospun PLA and PLA/PVA/SA Fiber Membranes for Wound Healing. Polymers. 2020; 12(4):839. https://doi.org/10.3390/polym12040839
Chicago/Turabian StyleBi, Hongyan, Tianyi Feng, Binbin Li, and Yingchao Han. 2020. "In Vitro and In Vivo Comparison Study of Electrospun PLA and PLA/PVA/SA Fiber Membranes for Wound Healing" Polymers 12, no. 4: 839. https://doi.org/10.3390/polym12040839
APA StyleBi, H., Feng, T., Li, B., & Han, Y. (2020). In Vitro and In Vivo Comparison Study of Electrospun PLA and PLA/PVA/SA Fiber Membranes for Wound Healing. Polymers, 12(4), 839. https://doi.org/10.3390/polym12040839




