Neoadjuvant and Adjuvant Chemotherapy for Pancreatic Adenocarcinoma: Literature Review and Our Experience of NAC-GS
Abstract
Simple Summary
Abstract
1. Introduction
2. Evidence of the Benefits of Adjuvant/Neoadjuvant Chemotherapy for Pancreatic Adenocarcinoma
3. Association between the Responses to Neoadjuvant and Adjuvant Therapies
4. Experience at Dokkyo Medical University
4.1. Results of Neoadjuvant Chemotherapy Using Gemcitabine Plus S-1
4.2. Factors Predictive of the Response to NAC-GS
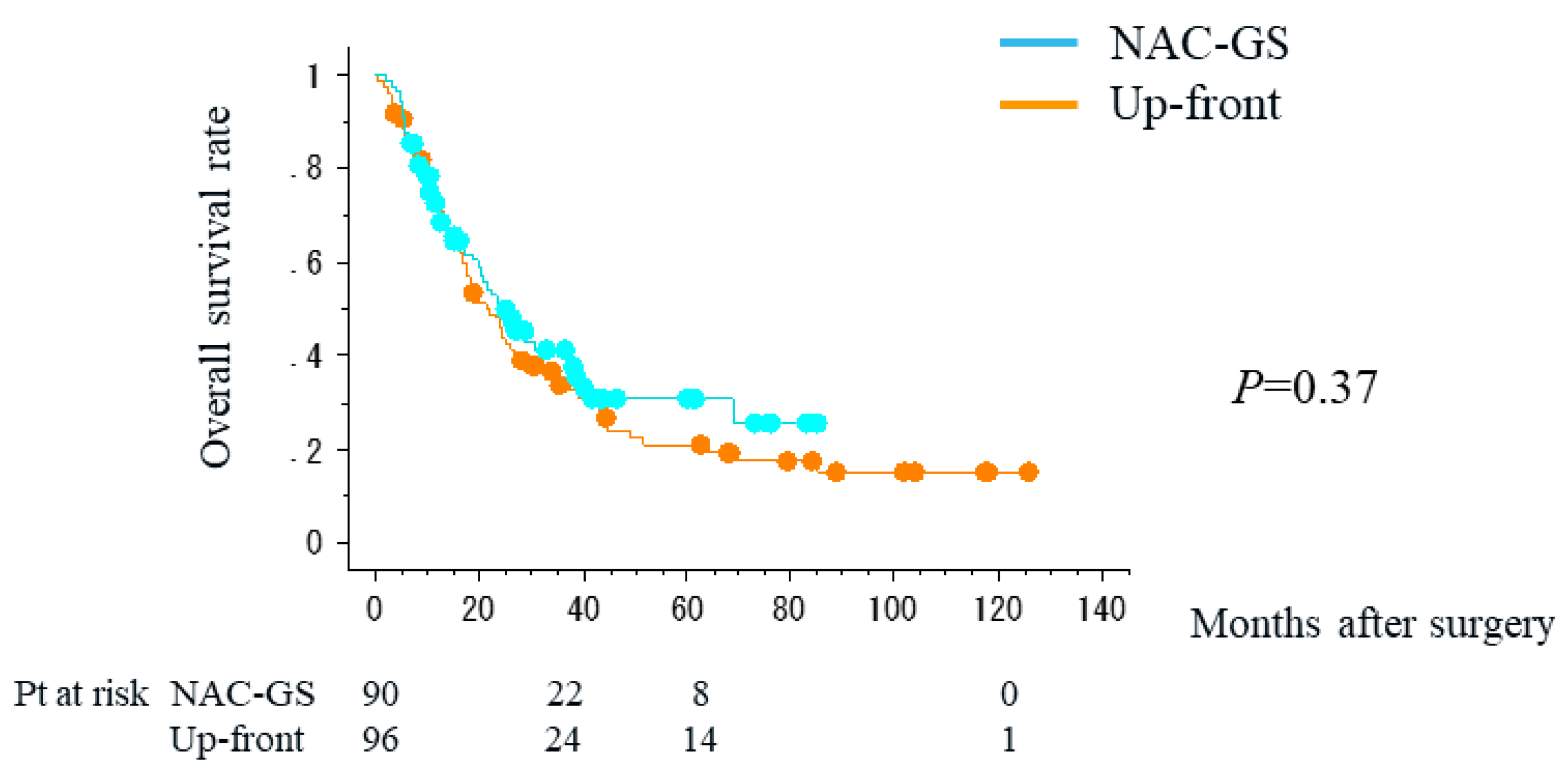
4.3. Impact of NAC-GS on the Outcomes of Adjuvant Chemotherapy
5. Discussion
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
References
- Lippi, G.; Mattiuzzi, C. The global burden of pancreatic cancer. Arch. Med. Sci 2020, 16, 820–824. [Google Scholar] [CrossRef] [PubMed]
- American Cancer Society: Cancer Facts and Figures 2023. Available online: https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2023/2023-cancer-facts-and-figures.pdf (accessed on 16 January 2024).
- Japan, N.C.C. Cancer Statistics in Japan. Available online: https://ganjoho.jp/public/qa_links/report/statistics/pdf/cancer_statistics_2023.pdf (accessed on 30 December 2023).
- Li, D.; Xie, K.; Wolff, R.; Abbruzzese, J.L. Pancreatic cancer. Lancet 2004, 363, 1049–1057. [Google Scholar] [CrossRef] [PubMed]
- National Cancer Institute. SEER Stat Fact Sheets: Pancreas Cancer. Available online: https://seer.cancer.gov/statfacts/html/pancreas.html (accessed on 23 December 2023).
- Khorana, A.A.; McKernin, S.E.; Berlin, J.; Hong, T.S.; Maitra, A.; Moravek, C.; Mumber, M.; Schulick, R.; Zeh, H.J.; Katz, M.H.G. Potentially curative pancreatic adenocarcinoma: ASCO Clinical Practice Guideline update. J. Clin. Oncol. 2019, 37, 2082–2088. [Google Scholar] [CrossRef] [PubMed]
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology. Pancreatic Adenocarcinoma. Version 1, 2024. Available online: https://www.nccn.org/professionals/physician_gls/pdf/pancreatic.pdf (accessed on 3 January 2024).
- Smaglo, B.G. Role for Neoadjuvant Systemic Therapy for Potentially Resectable Pancreatic Cancer. Cancers 2023, 15, 2377. [Google Scholar] [CrossRef]
- Xu, Y.; Chen, Y.; Han, F.; Wu, J.; Zhang, Y. Neoadjuvant therapy vs. upfront surgery for resectable pancreatic cancer: An update on a systematic review and meta-analysis. Biosci. Trends 2022, 15, 365–373. [Google Scholar] [CrossRef] [PubMed]
- Kwaśniewska, D.; Fudalej, M.; Nurzyński, P.; Badwska-Kozakiewicz, A.; Czerw, A.; Cipora, E.; Sygit, K.; Bandurska, E.; Deptala, A. How A Patient with Borderline Resectable Pancreatic Cancer should Be Treated—A Comprehensive Review. Cancers 2023, 15, 4275. [Google Scholar] [CrossRef]
- Roesel, R.; Deantonio, L.; Bernardi, L.; Garo, M.L.; Majno-Hurst, P.; Vannelli, A.; Cefalì, M.; Palmarocchi, M.C.; Valli, M.C.; Pesola, G.; et al. Neo-Adjuvant Treatment in Primary Resectable Pancreatic Cancer: A Systematic Review—Compliant Updated Metanalysis of Oncological Outcomes. Cancers 2023, 15, 4627. [Google Scholar] [CrossRef]
- Oettle, H.; Neuhaus, P.; Hochhaus, A.; Hartmann, J.T.; Gellert, K.; Ridwelski, K.; Niedergethmann, M.; Zülke, C.; Fahike, J.; Arning, M.B.; et al. Adjuvant chemotherapy with gemcitabine and long-term outcomes among patients with resected pancreatic cancer: The CONKO-001 randomized trial. JAMA 2013, 310, 1473–1481. [Google Scholar] [CrossRef]
- Uesaka, K.; Boku, N.; Fukutomi, A.; Okamura, Y.; Konishi, M.; Matsumoto, I.; Kaneoka, Y.; Shimizu, Y.; Nakamori, S.; Sakamoto, H.; et al. Adjuvant chemotherapy of S-1 versus gemcitabine for resected pancreatic cancer: A phase 3, open-label, randomised, non-inferiority trial (JASPAC 01). Lancet 2016, 388, 248–257. [Google Scholar] [CrossRef]
- Neoptolemos, J.P.; Palmer, D.H.; Ghaneh, P.; Psarelli, E.E.; Valle, J.W.; Halloran, C.M.; Faluyi, O.; O’Reilly, D.A.; Cunningham, D.; Wadsley, J.; et al. Comparison of adjuvant gemcitabine and capecitabine with gemcitabine monotherapy in patients with resected pancreatic cancer (ESPAC-4): A multicentre, open-label, randomised, phase 3 trial. Lancet 2017, 389, 1011–1024. [Google Scholar] [CrossRef]
- Conroy, T.; Hammel, P.; Hebbar, M.; Ben Abdelghani, M.; Wei, A.C.; Raoul, J.L.; Choné, L.; Francois, E.; Artru, P.; Biagi, J.J.; et al. FOLFIRINOX or Gemcitabine as Adjuvant Therapy for Pancreatic Cancer. N. Engl. J. Med. 2018, 379, 2395–2406. [Google Scholar] [CrossRef]
- Sohal, D.P.S.; Duong, M.; Ahmad, S.A.; Gandhi, N.S.; Beg, M.S.; Wang-Gilliam, A.; Wade, J.L., 3rd; Chiorean, E.G.; Guthrie, K.A.; Lowy, A.M.; et al. Efficacy of Perioperative Chemotherapy for Resectable Pancreatic Adenocarcinoma: A Phase 2 Randomized Clinical Trial. JAMA Oncol. 2021, 7, 421–427. [Google Scholar] [CrossRef]
- ESMO. Clinical Practice Guidelines: Gastrointestinal Cancers, Pancreatic Cancer. Available online: https://interactiveguidelines.esmo.org/esmo-web-app/gl_toc/index.php?GL_id=8 (accessed on 3 January 2024).
- Smeenk, H.G.; van Eijck, C.H.; Hop, W.C.; Erdmann, J.; Tran, K.C.; Debois, M.; van Cutsem, E.; van Dekken, H.; Klinkenbijl, J.H.; Jeelel, J. Long-term survival and metastatic pattern of pancreatic and periampullary cancer after adjuvant chemoradiation or observation: Long-term results of EORTIC trial 40891. Ann. Surg. 2007, 246, 734–740. [Google Scholar] [CrossRef] [PubMed]
- Shi, X.; Peng, J.; Jiang, H.; Gao, Y.; Wang, W.; Zhou, F. Impact of adjuvant chemoradiotherapy on survival of resected pancreatic adenocarcinoma cancer: A Surveillance, Epidemiology and End Results (SEER) analysis. Front. Oncol. 2021, 13, 36. [Google Scholar] [CrossRef] [PubMed]
- Janssen, Q.P.; Buettner, S.; Suker, M.; Beumer, B.R.; Addeo, P.; Bachellier, P.; Bahary, N.; Bekkai-Saab, T.; Bali, M.A.; Besselink, M.G.; et al. Neoadjuvant FOLFIRINOX in patients with borderline resectable pancreatic cancer: A systematic review and patient-level meta-analysis. J. Natl. Cancer Inst. 2019, 111, 782–794. [Google Scholar] [CrossRef]
- Van Dam, J.L.; Janssen, Q.P.; Besselink, M.G.; Homs, M.Y.V.; van Santvoort, H.C.; van Tienhoven, G.; de Wilde, R.F.; Wilmink, J.W.; van Eijck, C.H.J.; Groot Koerkamp, B. Neoadjuvant therapy or upfront surgery for resectable and borderline resectable pancreatic cancer: A meta-analysis of randomized controlled trials. Eur. J. Cancer 2022, 160, 140–149. [Google Scholar] [CrossRef]
- Nagakawa, Y.; Sahara, Y.; Hosokawa, Y.; Murakami, Y.; Yamaue, H.; Satoi, S.; Unno, M.; Isaji, S.; Endo, I.; Sho, M.; et al. Clinical impact of neoadjuvant chemotherapy and chemoradiotherapy in borderline resectable pancreatic cancer: Analysis of 884 patients at facilities specializing in pancreatic surgery. Ann. Surg. Oncol. 2019, 26, 1629–1636. [Google Scholar] [CrossRef]
- Nassour, I.; Parrish, A.; Baptist, L.; Voskamp, S.; Handoo, K.; Rogers, S.; Fabregas, J.; George, T.; Hitchcock, K.; Paniccia, A.; et al. National adoption of neoadjuvant chemotherapy: Paradigm shift in the treatment of pancreatic cancer. HPB 2023, 25, 1323–1328. [Google Scholar] [CrossRef] [PubMed]
- Unno, M.; Motoi, F.; Matsuyama, Y.; Satoi, S.; Matsumoto, I.; Aosasa, S.; Shirakawa, H.; Wada, K.; Fujii, T.; Yoshitomi, H.; et al. Randomized phase II/III trial of neoadjuvant chemotherapy with gemcitabine and S-1 versus upfront surgery for resectable pancreatic cancer (Prep-02/JSAP-05). J. Clin. Oncol. 2020, 37 (Suppl. 4), 189. [Google Scholar] [CrossRef]
- Versteijne, E.; Suker, M.; Groothuis, K.; Akkermans-Vogelaar, J.M.; Besselink, M.G.; Bonsing, B.A.; Buijsen, J.; Busch, O.R.; Creemers, G.M.; van Dam, R.M.; et al. Preoperative chemoradiotherapy versus immediate surgery for resectable and borderline resectable pancreatic cancer: Results of the Dutch Randomized Phase III PREOPANC Trial. J. Clin. Oncol. 2020, 38, 1763–1773. [Google Scholar] [CrossRef]
- Schwartz, L.; Vernerey, D.; Bachet, J.B.; Tuech, J.J.; Portales, F.; Michel, P.; Cunha, A.S. Correction to: Resectable pancreatic adenocarcinoma neo-adjuvant FOLF(IRIN)OX-based chemotherapy—A multicenter, non-comparative, randomized, phase II trial (PANACHE01-PRODIGE48 study). BMC Cancer 2020, 20, 168. [Google Scholar] [CrossRef] [PubMed]
- Tzeng, C.W.D.; Balachandran, A.; Ahmad, M.; Lee, J.E.; Krishnan, S.; Wang, H.; Crane, C.H.; Wolff, R.A.; Varadhachary, G.R.; Pisters, P.W.T.; et al. Serum carbohydrate antigen 19-9 represents a marker of response to neoadjuvant therapy in patients with borderline resectable pancreatic cancer. HBP 2014, 16, 430–438. [Google Scholar] [CrossRef] [PubMed]
- Isaji, S.; Mizuno, S.; Windsor, J.A.; Bassi, C.; Fernández-Del Castillo, C.; Hacket, T.; Hayasaki, A.; Katz, M.H.G.; Kim, S.W.; KIshiwada, H.; et al. International consensus on definition and criteria of borderline resectable pancreatic ductal adenocaecinoma 2017. Pancreatology 2018, 18, 2–11. [Google Scholar] [CrossRef] [PubMed]
- Van Roessel, S.; van Veldhuisen, E.; Klompmaker, S.; Janssen, Q.P.; Abu Hilal, M.; Alseidi, A.; Balduzzi, A.; Balzano, G.; Bassi, C.; Berrevoetr, F.; et al. Evaluation of adjuvant chemotherapy in patients with resected pancreatic cancer after neoadjuvant FOLFIRINOX treatment. JAMA Oncol. 2020, 6, 1733–1740. [Google Scholar] [CrossRef] [PubMed]
- Maggino, L.; Malleo, G.; Crippa, S.; Belfiori, G.; Bannone, E.; Lionetto, G.; Gasparini, G.; Nobile, S.; Luchini, C.; Mattiolo, P.; et al. Pathological staging in psotneoadjuvant pancreatectomy for pancreatic cancer: Implications for adjuvant surgery. Br. J. Surg. 2023, 110, 973–982. [Google Scholar] [CrossRef] [PubMed]
- Motoi, F.; Ishida, K.; Fujishima, F.; Ottomo, S.; Oikawa, M.; Okada, T.; Shimamura, H.; Takemura, S.; Ono, F.; Akada, M.; et al. Naoadjuvant chemotherapy with gemcitabine and S-1 for resectable and borderline pancreatic ductal adenocarcinoma: Results from a prospective multi-institutional phase 2 trial. Ann. Surg. Oncol. 2013, 20, 3794–3801. [Google Scholar] [CrossRef]
- Mori, S.; Aoki, T.; Sakuraoka, Y.; Shimizu, T.; Yamaguchi, T.; Park, K.H.; Matsumoto, T.; Shiraki, T.; Iso, Y.; Kubota, K. Efficacy of adjuvant chemotherapy according to the pathological response to neoadjuvant chemotherapy among patients with pancreatic ductal adenocarcinoma. Anticancer Res 2021, 41, 1629–1639. [Google Scholar] [CrossRef]
- The Japan Pancreas Society. Classification of Pancreatic Carcinoma, 4th ed.; Kanehara & Co., Ltd.: Tokyo, Japan, 2017. [Google Scholar]
- Luo, G.; Liu, C.; Guo, M.; Cheng, H.; Lu, Y.; Jin, K.; Liu, L.; Long, J.; Xu, J.; Lu, R.; et al. Potential Biomarkers in Lewis Negative Patients With Pancreatic Cancer. Ann. Surg. 2017, 265, 800–805. [Google Scholar] [CrossRef]
- Omiya, K.; Oba, A.; Inoue, Y.; Kobayashi, K.; Wu, Y.H.A.; Ono, Y.; Sato, T.; Sasaki, T.; Ozaka, M.; Sasahira, N.; et al. Serum DUPAN-2 could be an Alternative Biological Marker for Ca19-9 Nonsecretors with Pancreatic Cancer. Ann. Surg. 2023, 277, e1278–e1283. [Google Scholar] [CrossRef]
- Shimizu, T.; Asakuma, M.; Tomioka, A.; Inoue, Y.; Hirokawa, F.; Hayashi, M.; Uchiyama, K. Span-1 and CA19-9 as Predictors of Early Recurrence and Lymph Node Metastasis for Patients with Invasive Pancreatic Cancer after Pancreatectomy. Am. Surg. 2018, 84, 109–113. [Google Scholar] [CrossRef]
- Hamano, H.; Hayakawa, T.; Kondo, T. Serum immunoreactive elastase in diagnosis of pancreatic diseases. A sensitive marker for pancreatic cancer. Dig. Dis. Sci. 1987, 32, 50–56. [Google Scholar] [CrossRef]
- Mori, S.; Aoki, T.; Sakuraoka, Y.; Shimizu, T.; Yamaguchi, T.; Park, K.H.; Matsumoto, T.; Shiraki, T.; Iso, Y.; Kubota, K. Predictors of poor pathological response to neoadjuvant gemcitabine plus S-1 chemotherapy in patients with pancreatic ductal adenocarcinoma. Pancreas 2021, 50, 744–750. [Google Scholar] [CrossRef]
- Mori, S.; Aoki, T.; Sakuraoka, Y.; Shimizu, T.; Yamaguchi, T.; Park, K.H.; Matsumoto, T.; Shiraki, T.; Iso, Y.; Kubota, K. Impact of adverse events of adjuvant and neoadjuvant chemotherapies on outcomes of patients with pancreatic ductal adenocarcinoma. Cancer Chemother. Pharmacol. 2021, 88, 109–120. [Google Scholar] [CrossRef]
- Casadei, R.; Di Marco, M.; Ricci, C.; Santini, D.; Serra, C.; Calculli, L.; D’Ambra, M.; Guido, A.; Morselli-Labate, A.M.; Minni, F. Neoadjuvant Chemoradiotherapy and Surgery Versus Surgery Alone in Resectable Pancreatic Cancer: A Single-Center Prospective, Randomized, Controlled Trial Which Failed to Achieve Accrual Targets. J. Gastrointest. Surg. 2015, 19, 1802–1812. [Google Scholar] [CrossRef]
- Golcher, H.; Brunner, T.B.; Witzigmann, H.; Marti, L.; Bechstein, W.O.; Bruns, C.; Jungnickel, H.; Schreiber, S.; Grabenbauer, G.G.; Meyer, T.; et al. Neoadjuvant chemoradiation therapy with gemcitabine/cisplatin and surgery versus immediate surgery in resectable pancreatic cancer: Results of the first prospective randomized phase II trial. Strahlenther. Onkol. 2015, 191, 7–16. [Google Scholar] [CrossRef]
- Reni, M.; Balzano, G.; Zanon, S.; Zerbi, A.; Rimassa, L.; Castoldi, R.; Pinelli, D.; Mosconi, S.; Doglioni, C.; Chiaravalli, M.; et al. Safety and efficacy of preoperative or postoperative chemotherapy for resectable pancreatic adenocarcinoma (PACT-15): A randomised, open-label, phase 2-3 trial. Lancet Gastroenterol. Hepatol. 2018, 3, 413–423. [Google Scholar] [CrossRef] [PubMed]
- Versteijne, E.; van Dam, J.L.; Suker, M.; Janssen, Q.P.; Groothuis, K.; Akkermans-Vogelaar, J.M.; Besselink, M.G.; Bonsing, B.A.; Buijsen, J.; Busch, O.R.; et al. Neoadjuvant Chemoradiotherapy Versus Upfront Surgery for Resectable and Borderline Resectable Pancreatic Cancer: Long-Term Results of the Dutch Randomized PREOPANC Trial. J. Clin. Oncol. 2022, 40, 1220–1230. [Google Scholar] [CrossRef] [PubMed]
- Seufferlein, T.; Uhl, W.; Kornmann, M.; Algül, H.; Friess, H.; König, A.; Ghadimi, M.; Gallmeier, E.; Bartsch, D.K.; Lutz, M.P.; et al. Perioperative or only adjuvant gemcitabine plus nab-paclitaxel for resectable pancreatic cancer (NEONAX)-a randomized phase II trial of the AIO pancreatic cancer group. Ann. Oncol. 2023, 34, 91–100. [Google Scholar] [CrossRef] [PubMed]
- Hilmi, M.; Delaye, M.; Muzzolini, M.; Nicolle, R.; Cros, J.; Hammel, P.; Cardot-Ruffino, V.; Neuzillet, C. The immunological landscape in pancreatic ductal adenocarcinoma and overcoming resistance to immunotherapy. Lancet Gastroenterol. Hepatol. 2023, 8, 1129–1142. [Google Scholar] [CrossRef] [PubMed]
- Katz, M.H.G.; Petroni, G.R.; Bauer, T.; Reilly, M.J.; Wolpin, B.M.; Stucky, C.C.; Bekaii-Saab, T.S.; Elias, R.; Merchant, N.; Dias Costa, A.; et al. Multicenter randomized controlled trial of neoadjuvant chemoradiotherapy alone or in combination with pembrolizumab in patients with resectable or borderline resectable pancreatic adenocarcinoma. J. Immunother. Cancer 2023, 11, e007586. [Google Scholar] [CrossRef] [PubMed]
- Heumann, T.; Judkins, C.; Li, K.; Lim, S.J.; Hoare, J.; Parkinson, R.; Cao, H.; Zhang, T.; Gai, J.; Celiker, B.; et al. A platform trial of neoadjuvant and adjuvant antitumor vaccination alone or in combination with PD-1 antagonist and CD137 agonist antibodies in patients with resectable pancreatic adenocarcinoma. Nat. Commun. 2023, 14, 3650. [Google Scholar] [CrossRef] [PubMed]

| Variable | Pre-NAC-GS (n = 95) | Post-NAC-GS (n = 95) | p Value | Post/Pre Ratio |
|---|---|---|---|---|
| Tumor size (mm) | 24.6 (2.4–70.0) | 18.2 (1.4–64.0) | <0.0001 | 0.82 (0.40–1.90) |
| CEA (ng/mL) | 3.0 (0.8–163.0) | 3.4 (0.7–97.5) | 0.72 | 1.02 (0.25–4.92) |
| CA19-9 (U/mL) | 203.0 (2–12,000) | 84.5 (2–12,000) | <0.0001 | 0.63 (0.01–55.0) |
| DUPAN-2 (U/mL) | 220.0 (25–14,000) | 97.0 (4–3400) | <0.0001 | 0.66 (0.03–10.8) |
| Span-1 (U/mL) | 52.0 (1–1600) | 25.0 (1–1100) | <0.0001 | 0.68 (0.01–9.57) |
| Elastase-1 (ng/dL) | 218.0 (25–8620) | 150.0 (40–3613) | <0.0001 | 0.61 (0.01–8.17) |
| R Up-Front (n = 77) | R NAC-GS (n = 65) | p Value | BR-PV Up-Front (n = 20) | BR-PV NAC-GS (n = 16) | p Value | BR-A Up-Front (n = 7) | BR-A NAC-GS (n = 14) | p Value | |
|---|---|---|---|---|---|---|---|---|---|
| Resection | 0.14 | 0.16 | 0.99 | ||||||
| (+) | 72 | 64 | 18 | 15 | 5 | 10 | |||
| (−) | 5 | 1 | 2 | 1 | 2 | 4 | |||
| R0 resection | 0.60 | 0.03 | 0.67 | ||||||
| Yes | 60 | 48 | 13 | 14 | 2 | 5 | |||
| No | 7 | 4 | 5 | 0 | 2 | 3 | |||
| Adjuvant chemotherapy | 0.01 | 0.34 | 0.69 | ||||||
| (+) | 49 | 55 | 15 | 13 | 3 | 7 | |||
| (−) | 22 | 9 | 4 | 2 | 2 | 3 |
| Author | Country | Period | Study Design | Number of Patients | NAT Regimen | Duration | Pathological Response | Median OS (Months) |
|---|---|---|---|---|---|---|---|---|
| Motoi et al. (2013) [31] | Japan | 2008–2010 | Prospective phase 2 | 35 | Gemcitabine plus S-1 | 2 cycles (6 weeks) | Evans Grade I: 23%; Grade IIa: 57%; Garde IIb: 20% | 19.7 |
| Casadei et al. (2015) [40] | Italy | 2007–2014 | RCT | 38 | Gemcitaine plus radiation | 12 weeks | Rebekah Grade Minimal: 11.1%; Small: 16.7%; Moderate: 27.8%; Large: 5.6% | 22.4 |
| Golcher et al. (2015) [41] | Germany | 2003–2009 | RCT | 33 | Gemcitabine plus cisplatin plus radiatioon | 30 days | NR | 17.4 |
| Reni et al. (2018) [42] | Italy | 2010–2015 | RCT | 29 | Cisplatin plus epirubicin plus gemcitabine | 3 months | Marked: 36%; Moderate: 32%; Poor: 32% | 38.2 |
| Versteijne et al. (2022) [43] | Netherlands | 2013–2017 | RCT | 91 | Gemcitabine plus radiation | 10 weeks | NR | 15.7 |
| Seufferlein et al. (2023) [44] | Germany | 2015–2019 | RCT | 59 | Gemcitabine plus nab-paclitaxel | 2 cycles (8 weeks) | Complete: 6.2%; Moderate: 3.1%; Minimal: 40.6%; Poor: 50.0% | 25.5 |
| Our series [32] | Japan | 2013–2019 | Retrospective | 95 | Gemcitabine plus S-1 | 2 cycles | Evans Grade I: 23.5%, Grade IIa: 60.5%; Grade IIb: 13.6%; Grade III: 2.4%. | 22.0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aoki, T.; Mori, S.; Kubota, K. Neoadjuvant and Adjuvant Chemotherapy for Pancreatic Adenocarcinoma: Literature Review and Our Experience of NAC-GS. Cancers 2024, 16, 910. https://doi.org/10.3390/cancers16050910
Aoki T, Mori S, Kubota K. Neoadjuvant and Adjuvant Chemotherapy for Pancreatic Adenocarcinoma: Literature Review and Our Experience of NAC-GS. Cancers. 2024; 16(5):910. https://doi.org/10.3390/cancers16050910
Chicago/Turabian StyleAoki, Taku, Shozo Mori, and Keiichi Kubota. 2024. "Neoadjuvant and Adjuvant Chemotherapy for Pancreatic Adenocarcinoma: Literature Review and Our Experience of NAC-GS" Cancers 16, no. 5: 910. https://doi.org/10.3390/cancers16050910
APA StyleAoki, T., Mori, S., & Kubota, K. (2024). Neoadjuvant and Adjuvant Chemotherapy for Pancreatic Adenocarcinoma: Literature Review and Our Experience of NAC-GS. Cancers, 16(5), 910. https://doi.org/10.3390/cancers16050910







