Simple Summary
As the treatment for breast cancer continues to improve and more women survive their initial diagnosis, there is an increasingly large number of women who are at risk of a second new breast cancer in their lifetimes. However, the hereditary causes of these second breast cancers are not well understood. In this study, we used the latest genetic sequencing technologies to investigate hereditary causes for the second breast cancer in individuals who are known not to have alterations in one of the three main breast cancer genes (BRCA1, BRCA2 and PALB2). We analyzed the genetic profiles of selected participants from the WECARE study, one of the largest studies looking at second breast cancers in women. By comparing the genetic profiles of women who have had one breast cancer to similarly matched women who went on to have a second breast cancer, we found that younger women (under 50) with second breast cancers had a higher number of inherited gene alterations compared with those women with one breast cancer. We did not see the same effect in the older women. The results from this study improve our understanding of the hereditary contribution to second breast cancers.
Abstract
Background: Contralateral breast cancer (CBC) is associated with younger age at first diagnosis, family history and pathogenic germline variants (PGVs) in genes such as BRCA1, BRCA2 and PALB2. However, data regarding genetic factors predisposing to CBC among younger women who are BRCA1/2/PALB2-negative remain limited. Methods: In this nested case-control study, participants negative for BRCA1/2/PALB2 PGVs were selected from the WECARE Study. The burden of PGVs in established breast cancer risk genes was compared in 357 cases with CBC and 366 matched controls with unilateral breast cancer (UBC). The samples were sequenced in two phases. Whole exome sequencing was used in Group 1, 162 CBC and 172 UBC (mean age at diagnosis: 42 years). A targeted panel of genes was used in Group 2, 195 CBC and 194 UBC (mean age at diagnosis: 50 years). Comparisons of PGVs burdens between CBC and UBC were made in these groups, and additional stratified sub-analysis was performed within each group according to the age at diagnosis and the time from first breast cancer (BC). Results: The PGVs burden in Group 1 was significantly higher in CBC than in UBC (p = 0.002, OR = 2.5, 95CI: 1.2–5.6), driven mainly by variants in CHEK2 and ATM. The proportions of PGVs carriers in CBC and UBC in this group were 14.8% and 5.8%, respectively. There was no significant difference in PGVs burden between CBC and UBC in Group 2 (p = 0.4, OR = 1.4, 95CI: 0.7–2.8), with proportions of carriers being 8.7% and 8.2%, respectively. There was a significant association of PGVs in CBC with younger age. Metanalysis combining both groups confirmed the significant association between the burden of PGVs and the risk of CBC (p = 0.006) with the significance driven by the younger cases (Group 1). Conclusion: In younger BRCA1/BRCA2/PALB2-negative women, the aggregated burden of PGVs in breast cancer risk genes was associated with the increased risk of CBC and was inversely proportional to the age at onset.
1. Introduction
Advances in the treatment of breast cancer (BC) over recent decades have substantially improved the survival rates of women with BC, thereby increasing the population of women at risk of a second primary BC. The risk of developing asynchronous contralateral BC (CBC) is higher than the risk of a first BC in the population [1,2,3], equating to at least 4% at ten years after the first BC [3,4]. The development of CBC is associated with a worse prognosis and other morbidities [5,6]. However, there is no clinical consensus for managing the individual risk of developing CBC, with rates of prophylactic bilateral mastectomies varying significantly across U.S. clinics [7,8,9]. A number of informatic tools estimating individual CBC risk have been deployed to address this challenge [10,11,12,13], but given the lack of data available, their utility and generalizability for accurate clinical decision-making have been limited [13,14].
Risk factors for CBC include young age at the first BC and family history [1,15], indicating that hereditary factors play a role [16]. Treatment for the first BC is also known to modify subsequent CBC risk and has been studied in combination with specific genetic risk factors; examples include the use of tamoxifen in carriers of pathogenic germline variants (PGVs) in BRCA1 and BRCA2 [17,18,19] and the effects of radiation exposure in combination with pathogenic variants in ATM [20]. Overall, the use of chemotherapy and hormone therapy has been linked to a decrease in CBC risk by 42% [6,21,22].
Pathogenic germline variants (PGVs) in BRCA1 and BRCA2 have been associated with an increased risk of CBC [23,24,25]. Carriers of PGVs in BRCA1 and BRCA2 are highly susceptible to CBC development with a risk of 2.5% per year after diagnosis of the first BC [24], which is at least five times higher than in non-carriers [2,3]. A number of studies have attempted to identify further PGVs associated with CBC risks, including previous WECARE (for Women’s Environment, Cancer and Radiation Epidemiology) Study publications that analyzed CHEK2*1100delC and variants in ATM and PALB2 [20,26,27,28]. However, the role of PGVs beyond these genes is not yet known.
The WECARE Study is a population-based case-control study that collected phenotype data and blood DNA samples from women with CBC (cases) and individually matched controls with unilateral BC (UBC) [29]. The rich phenotypic data available from the WECARE Study, including demographic, epidemiologic and clinical information, provide the opportunity to study predisposition to CBC, while adjusting for known general risk factors of CBC. A number of previous publications based on the WECARE Study participants examined the joint roles of environmental risk factors, common variants and rare variants in individual genes, primarily focusing on BRCA1 and BRCA2 [18,25,27,30,31,32,33,34]. The present study investigated the aggregated burden of PGVs in established BC genes beyond BRCA1/2 and PALB2, focusing on BRCA1/2/PALB2-negative participants in the WECARE Study.
2. Materials and Methods
2.1. Study Population, Library Preparation and Sequencing of Samples
The participants with CBC (“cases”) and UBC (“controls”) were recruited to WECARE Study as described earlier [29]. Briefly, all cases and controls were diagnosed before age 55 years from 1985 to 2000 with a first primary invasive breast cancer that had not spread beyond regional lymph nodes. Cases were diagnosed with a second primary invasive or in situ CBC at least one year after a first primary diagnosis in 1986 to 2001. Controls were individually matched to each case on birth year, year of first primary diagnosis, cancer registry and race/ethnicity and were required to have an intact contralateral breast. Controls were assigned a reference date reflecting a cancer-free at-risk period following the first BC equivalent to the interval between first and second diagnoses of the matched cases (latency). Cases and controls were required to have had no other prior or intervening cancers, to have resided in a cancer registry catchment area at both diagnoses/reference date, and to have provided a blood sample. Informed consent was obtained from participants. For this study, one control was matched to each case and known carriers of PGVs in BRCA1/2/PALB2 were excluded.
For the current study, participants selected were of European ancestry from the U.S., identified through population-based cancer registries covering Iowa, California (Los Angeles and Orange Counties ) and Washington State associated with the Surveillance, Epidemiology and End Results (SEER) registry system. This study was conducted in two phases using different sequencing techniques (termed “Group 1” and “Group 2”): whole exome sequencing (WES) was conducted in Group 1 while targeted panel sequencing was used for Group 2 using a custom Ampliseq panel that included 106 genes related to BC and DNA repair (Supplementary Table S1). Across both groups, participants were over-selected for family history of breast cancer in a first-degree relative, and further matched on the dates of diagnosis and follow-up (latency), race and reporting region. Participants with an early age of onset were prioritized during the 1st group selection. Cases and controls were initially individually matched 1:1; however, as some samples failed sequencing, and some of the individual case-control matching was broken, matching factors were adjusted for the analyses along with cytotoxic chemotherapy, hormonal therapy, breast irradiation, the number of pregnancies and the top PCs, as described below. The models were not adjusted for family history of BC because this could be a proxy for carrying pathogenic germline variants. The age distribution between the two groups was different because the earlier onset cases were selected for Group 1 (Group 1: mean age 42; Group 2: mean age 50).
For both groups, DNA was extracted from blood using QIAGEN columns (QIAGEN LLC, USA, Germantown). For Group 1, the WES libraries (125xPE, 24x multiplexed) were prepared using Illumina Nextera Rapid Exome kits (Illumina, Great Abington, Cambridge, UK; FC−140–9001) following the manufacturer’s recommendations. Sequencing of WES libraries was performed using Illumina HiSeq−2500 machines (Illumina, Great Abington, Cambridge, UK) and SBS v3 or v4 kits (in CRUK Cambridge Institute Genetic core). Each library was sequenced on 4–6 lanes to reach required depth on targets (68 ± 20, mean ± SD). For Group 2, the Ampliseq libraries were prepared and sequenced in SMCL genomics core (Department of Medical Genetics, Cambridge University). The custom library was designed using Thermo Fisher Ampliseq Designer tool (Thermo Fisher Scientific, Waltham, USA). Libraries (150PE, 2 pools) were prepared using a protocol adapted from Konig et al., 2015 [35]. Ampliseq samples were sequenced on 2 lanes of HiSeq 4000 Illumina machines (Illumina, Great Abington, Cambridge, UK) to a mean depth on targets of 442 ± 196 (mean ± SD).
A deidentified study dataset used for the analysis in this publication, which complies with regulatory data sharing restrictions, will be made available upon qualified request to WECARE Study Collaborative Data Repository,
2.2. Alignment, Variant Calling and Annotation
The study flowchart is presented in Supplementary Figure S1. An ethnically close subset of samples (non-Finnish female Europeans, NFFE) from One Thousand Genomes project [36] was used for the joint variant calling with WECARE samples. In addition, these NFFE samples were used for a supplementary supportive analysis to verify that burden of observed PGVs in UBC or CBC was higher than in an unselected population. FASTQ files were demultiplexed and passed through standard QC checks (including FastQC v.0.11.3 and multi-genome alignment [37]). Adaptors and low-quality bases were trimmed using Cutadapt [38]. Alignment and variant calling were performed following GATK Best Practices recommended by the Broad institute at the time of analysis. Reads were aligned to GRCh37 reference genome using BWA MEM (v. 0.7.12) [39]. BAM files from multiple lanes were merged and sorted using samtools (v.1.2) [40]. PCR duplicates were removed in WES, but not in Ampliseq data; diverse QC metrics for alignment and enrichment were then calculated by Picard (https://github.com/broadinstitute/picard accessed on 30 November 2022). FASTQ files for 196 NFFE samples of good quality were selected from One Thousand Genomes project (1KGP) dataset [36]. NFFE FASTQ files were processed by the same pipeline as the WECARE WES data.
Variant calling was performed using GATK (v. 3.4–46 and 3.6–0) [41], and g.vcf files were generated using Haplotype Caller after base quality recalibration and local realignment around indels. Individual g.vcf files were combined into batches of ~100 samples; then, the combined g.vcf-s were used to perform the joint genotyping. Variant calling was performed within the targeted areas only (with 10 bp padding). Variants were filtered by a combination of GATK VQSR and bespoke hard filters, and multiallelic variants were then split to separate lines. GATK down-sampling was suppressed for Ampliseq variant calling and filtering. Variant annotations were added to VCF file using VEP (v.101) [42] and ClinVar (v.20200905) [43]. Along with the standard predicted consequences, the VaP annotations included SIFT (v.5.2.2) [44], PolyPhen (v.2.2.2) [45] and CADD (v.1.6) [46].
Calculations were performed using CRUK CI and Cambridge University high-performance computing clusters. The source data may be requested from the WECARE consortium. The scripts for key steps of the pipeline are available upon request to the WECARE Study Collaborative Data Repository.
2.3. Selecting Genes and Pathogenic Variants
The list of BC susceptibility genes was compiled from the studies of Easton et al. (2015), Hu et al. (2021) and Dorling et al. (2021) [47,48,49]. It included BRCA1/2, PALB2, ATM, CHEK2, CDH1, TP53, PTEN, STK11, NF1, NBN, RAD51C, BARD1 and RAD51D. Carriers of PGVs in BRCA1/2 and PALB2 were excluded from this analysis. Variants in the remaining 11 genes were analyzed in the WES dataset. BARD1 and RAD51D were not available in the Ampliseq multigene panel, leaving nine BC susceptibility genes for the analysis in the Ampliseq dataset. As the focus of this study was on potentially actionable rare variants with high effect size, rather than on polygenic risks or gene interactions, we used relatively strict criteria in our definition of PGVs:
- Variants annotated as Pathogenic/Likely pathogenic by ClinVar or
- Loss of Function variants as predicted by VEP (stop/start gain/loss, frameshift, essential splice sites) or
- Missense variants that were simultaneously called Deleterious by PolyPhen, Probably Damaging by SIFT and had CADD Phred score > 25.
Of those variants that fulfilled the above criteria, only rare variants (AF < 0.01) with a call rate >0.85 were kept in the analysis. Variants annotated as Benign/Likely benign in ClinVar were excluded.
2.4. Statistical Analysis
The burden of PGVs aggregated across the preselected genes taken together was compared in CBC and UBC. Visual assessment of PGVs burden was performed using bar-plots showing aggregated allelic frequencies (AF) and proportions of carriers in the compared groups. The aggregated AF was defined as the total count of ALT alleles (AC) over the mean allele number (AN) across the aggregated variants. The statistical significance of differences between CBC and UBC was evaluated by the Burden test as implemented in the SKAT R library (v.2.0.1) [50]. Specifically, p-values for dichotomous outcome were calculated using efficient resampling, default (linear weighted) kernel and default settings for imputation and weighting. After excluding variants with call rates <0.85, only a small proportion of genotypes required imputation, where the default SKAT-binary imputation method assigned the most likely values observed in the data (0,1,2) to the missing genotypes. The default weighting implemented in SKAT assigns higher weight to rare variants: numerically the weights are calculated using beta-distribution as dbeta(MAF,1,25). As noted above, covariates added into the model included age at the first CBC, latency, number of pregnancies, use of chemo- and hormonal therapies, and breast irradiation for the first BC. Principal components (PCs) for ancestry were calculated using bigsnpr R library (v.1.6.1) [51] based on common variants not in linkage disequilibrium across all genes available in WES/panel data. European ancestry of participants was confirmed by projecting WECARE Study samples to PC space of the major 1KGP populations (Supplementary Figures S2A and S3A). Visual assessment of the Scree plots suggested adding the two top PCs as covariates for both Group 1 and Group 2 regression models to account for potential confounding due to residual population stratification (Supplementary Figures S2B and S3B). Three top PCs were added to the POLR model in the additional joined analysis of WES + NFFE after evaluation of the Scree plot for the joined WES + NFFE dataset (Supplementary Figure S4). PCA outliers (if any) were excluded.
Additional subgroup analyses were performed to compare burdens of PGVs in CBC and UBC depending on age or latency (time to CBC) within Group 1 and Group 2 separately. For the age subgroup analysis, study participants were split by median age in each group; the latency threshold for the sub-analysis was set to 5 years. The burden of PGVs within the subgroups was compared using the Fisher test for crude counts and visualized using bar-plots.
Because NFFE controls were unselected for BC, the PGVs prevalence in BC genes is expected to be lower in NFFE than in any WECARE Study sample group (UBC or CBC). Therefore, an additional supportive data check was performed to assess the PGVs burdens between NFFE, UBC and CBC samples. Only variants that had at least 0.85 call rate in both WECARE and NFFE samples were used for this analysis. The NFFE-UBC-CBC trend was visualized by bar-plots for crude counts. Proportional Odds Logit Regression (POLR), as implemented in the MASS R package [52], was used for the trend significance assessment (including top PCs into the model).
Metanalysis of summary statistics (p-values for PGVs burdens in Group 1 and Group 2) was performed using the METAL package (v.2011–03−25) [53] employing a weighted Z-score to obtain a summary test statistic and p-value (i.e., Stouffer’s approach).
3. Results
Of the total of 748 samples used for this analysis, 25 samples failed sequencing (15 samples failed WES and 10 samples failed the panel sequencing); 723 samples were successfully sequenced: 334 (172 UBC and 162 CBC) in Group 1 and 389 (194 UBC and 195 CBC) in Group 2.
Table 1 summarizes characteristics of women included in the statistical analysis. The limited sample size precluded analysis of individual variants. At the individual gene level, no genes reached statistical significance after multiple testing correction. In the analysis of PGVs burden over all predefined BC susceptibility genes taken together, the aggregated burden of PGVs in CBC was significantly higher than in UBC in Group 1 (Figure 1A, SKAT Burden test p = 0.002). The proportions of PGVs carriers in CBC and UBC in this group were 14.8% and 5.8%, respectively. This was driven mainly by variants in CHEK2 and ATM (Table 2). The full details of PGVs detected in the younger cohort (Group 1, mean age at first breast cancer = 42 years) are given in Supplementary Table S2. There was no significant difference in the burden of PGVs between CBC and UBC in Group 2 (mean age at diagnosis of the first BC = 50 years), with proportions of carriers being 8.7% and 8.2%, respectively (Figure 1B, SKAT Burden test p = 0.42; details of PGVs detected in Group 2 are given in Supplementary Tables S3 and S4).

Table 1.
Participant characteristics.
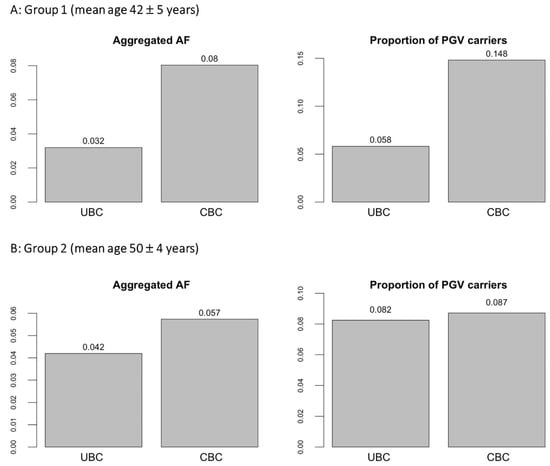
Figure 1.
Burden of PGVs in Group 1 and Group 2. Figure notes: In Group 1, the PGVs burden in CBC is significantly higher than in UBC (Burden SKAT test p = 0.002). Differences between CBC and UBC in Group 2 are not statistically significant (Burden SKAT test p = 0.42). Aggregated ALT allele frequency (aggregated AF) was calculated as the total count of ALT alleles (aggregated AC) over the mean allele number (mean AN) across the aggregated variants. The proportion of PGVs carriers was calculated as the fraction of participants carrying at least one variant in question (homo- or heterozygous). PGV: pathogenic germline variant.

Table 2.
PGVs burden per gene in Group 1.
3.1. Subgroup Analyses by Age and Latency
To further investigate the suggested association with age, we performed a stratified subgroup analysis within each of the studied groups separately, splitting them by the median age at the first BC: 43 years in the younger cohort (Group 1) and 51 years in the older cohort (Group 2). The stratified analysis confirmed higher PGVs burdens in CBC compared with UBC in the younger subgroups of participants (Figure 2).
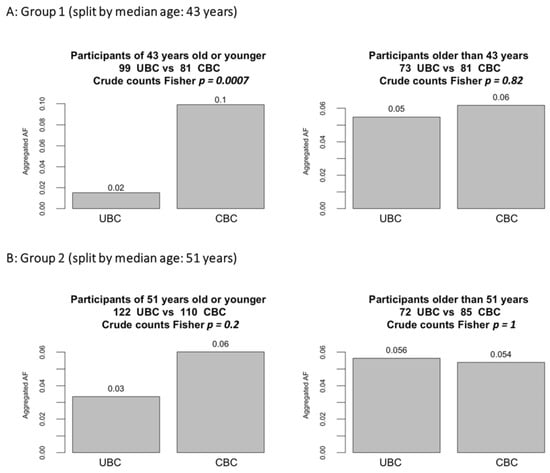
Figure 2.
Burden of PGVs stratified by age. Figure note: Each group was split by median age; then, PGVs burdens were evaluated in the subgroups.
Additionally, we performed a similar stratified subgroup analysis by latency (time between the first and second BCs). No significant difference was observed between participants who developed the second tumor before and after 5 years from the first tumor (Supplementary Figure S5).
3.2. Metanalysis and Comparison of PGVs Burdens with NFFE
As expected, the burden of observed PGVs in NFFE was lower than in either UBC or CBC (Supplementary Figure S6), consistent with the fact that 1KGP NFFE represents a population not selected for BC.
Metanalysis combining data from both Groups 1 and 2 confirmed the higher burden of PGVs in CBC compared with UBC (p = 0.006, driven by the participants with younger ages at diagnosis). No significant heterogeneity between the groups was detected in the metanalysis (p = 0.08).
4. Discussion
As BC survival rates improve, there is an increasing need to better understand the risk factors for CBC development. This study measured the aggregated burden of PGVs in established BC genes in BRCA1/2/PALB2-negative CBC patients who were part of the WECARE Study. We observed that 14.8% of participants with a younger age at CBC diagnosis (Group 1) carried a PGV in at least one of the studied genes, which was significantly higher than in participants with UBC (5.8%) or in the general population. This excess in the aggregated burden of PGVs was mainly driven by variants in CHEK2 and ATM (Table 2). The absence of similar findings in the older group (Group 2) may be explained by the different biology of BC in women of reproductive age (Group 1: 42 ± 5 years old) and in peri-/postmenopausal age (Group 2: 50 ± 4 years old).
Data on the prevalence of PGVs in CBC beyond BRCA1/2 and PALB2 genes are scarce. Yao et al. [54] reported on ~4000 CBC individuals of different ethnicities tested in a single laboratory by panels containing various BC genes. The prevalence of PGVs carriers amongst women with CBC was 3.3% for CHEK2, 1.64% for ATM, 0.38% for TP53 and 0.36% for NBN. The proportion of CHEK2 carriers was higher in women with CBC than in women with UBC (p < 0.001, driven by individuals of Caucasian origin). However, the study did not have clinical and phenotype data to adjust for treatment, number of pregnancies, and for the fact that some of the first primary BCs, which were used for comparison with CBC, still could develop a second BC later. Fanale et al. (2020) [55] reported results of a panel sequencing for a series of 139 bilateral BCs collected in a single hospital. The study reported 7.9% carriers of PGVs beyond BRCA1/2 and PALB2 genes (five CHEK2, three ATM, two RAD51C and one PTEN variant(s)), which is comparable to the results observed in our study. Of note, the series reported by Fanale et al. [55] included a large proportion of synchronous CBCs (33.1%), and they did not compare the prevalence of PGVs between CBC and UBC or by age at diagnosis.
Our study has several strengths. First, we leveraged a well-characterized study population that allowed the comparison of CBC and UBC, while controlling for multiple known confounding factors. Further, the participants were recruited through population-based cancer registries, rather than in a single hospital series, which enhances generalizability of results. Only early-stage BCs (stages 1 and 2) were included in both UBC and CBC groups, which allowed for longer latency. Including CBC with at least one year between the first and the second cancers ensures that the results predominately apply to the risk of metachronous primary BC. The unique design of the WECARE Study, where UBC controls were individually matched to the CBC cases, as well as the comprehensive phenotype annotations, allowed adjustment for the most important confounding factors influencing the CBC and UBC comparison, such as age at the first BC diagnosis, time to the second BC, treatment, and number of full-term pregnancies.
In spite of these strengths, we were limited by the relatively small sample size: 357 CBC cases and 366 UBC controls altogether, which precluded or limited detailed subgroup analyses or investigation of individual PGVs or genes. This reflects the practical challenges in collecting the dataset where CBC and UBC are matched by age and latency. The limited sample size meant that we had to aggregate variants across multiple genes. Larger BC cohorts will be necessary to assess the individual effects of genes. Two different sequencing techniques were applied to participants with younger and older ages of diagnosis of BC in our study, and while the bioinformatics pipelines were kept as similar as possible, they were not identical.
5. Conclusions
In conclusion, we have estimated the burden of PGVs in established BC risk genes in BRCA1/BRCA2/PALB2-negative CBC cases compared with UBC controls, and found an increased aggregated burden of PGVs in established BC-risk genes, which was modified by age. These findings provide further evidence of a strong genetic component of breast cancer etiology, beyond the known high penetrance genes among young women, and demonstrate the importance of screening for PGVs in women diagnosed with BC to identify those who are at increased risk of developing CBC.
Supplementary Materials
The following supporting information can be downloaded at https://www.mdpi.com/article/10.3390/cancers15020415/s1: Supplementary Figure S1: Study flowchart; Figure S2: PCA for Group 1; Figure S3: PCA for Group 2; Figure S4: WECARE-Group1 + NFFE PCA Scree plot; Figure S5: Burden of PGVs stratified by latency; Figure S6: WECARE-Group1 + NFFE PGVs burden; Table S1: PGVs detected in Group 2 samples summarized per gene; Table S2: PGVs detected in Group 1 samples; Table S3: PGVs detected in Group 2 samples; Table S4: PGVs detected in Group 2 samples summarized per gene.
Author Contributions
Conceptualization, A.L., J.B. (John Boice), J.B. (Jonine Bernstein), D.V.C., P.C. and M.T.; Methodology, A.L., J.B., D.V.C. and M.T.; Formal analysis, E.F, J.R., M.G. and A.L.; Investigation, E.F, J.R., G.C., M.G. and A.L.; Resources, WECARE Study Collaborative Group; Data curation, E.F., J.R, M.G. and A.L.; Writing—original draft, A.L., E.F. and M.T.; Writing—review and editing, all authors and WECARE Study Collaborative Group; Funding acquisition, M.T. All authors have read and agreed to the published version of the manuscript.
Funding
This work was funded by the European Union Seventh Framework Program (2007e2013)/European Research Council (310018) and the UK Medical Research Council PhD pro-gramme. MT was supported by the NIHR Cambridge Biomedical Research Centre (BRC, 1215−20014). The WECARE Study was generously funded through US National Institutes of Health grant numbers (U01CA083178, R01CA097397, R01CA114236, R01CA129639, P30CA008748).
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and the study was approved by the local ethics committees and by the WECARE Study Collaborative Group. The WECARE Study biospecimens were collected at multicenter sites between 1999–2004, with Mt Sinai School of Medicine (New York) serving as the coordinating center for the overall study during that time. This manuscript represents scientific work done as an ancillary Whole Exome Study (WECARE WES: Investigating Hereditary Cancer Predisposition, IHCAP) utilizing the ‘secondary use of the biospecimens’ for a subset of the WECARE Study population. This scientific work obtained institutional regulatory approval at Memorial Sloan Kettering Cancer Center (#17-495 biospecimen research protocol, approved Oct2017), which currently serves as the coordinating center for the overall WECARE Study, and the University of Cambridge (12/EE/0478), where the laboratory work was conducted to generate the WES results.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
A deidentified study dataset used for the analysis in this publication, which complies with regulatory data sharing restrictions, will be made available upon qualified request to the corresponding author (mdt33@medschl.cam.ac.uk).
Acknowledgments
The Women’s Environmental, Cancer and Epidemiology (WECARE) Study Collaborative Group: Memorial Sloan Kettering Cancer Center (New York, NY): Jonine L. Bernstein (WECARE Study P.I.), Marinela Capanu, Xiaolin Liang M.S., Irene Or, Anne S. Reiner, Mark Robson, Meghan Woods; Beckman Research Institute, City of Hope Comprehensive Cancer Center (Duarte, CA): Leslie Bernstein; Cedars-Sinai Medical Center (Los Angeles, CA): Robert W. Haile; Fred Hutchinson Cancer Research Center (Seattle, WA): Kathleen E. Malone; Translational Genomics Research Institute (TGen) (Phoenix, AZ): David Duggan; University of Cambridge (Cambridge, England): Marc Tischkowitz; Genetics Institute, University of Florida (Gainesville, FL): Patrick Concannon; University of Iowa (Iowa City, IA): Charles F. Lynch; University of Southern California (Los Angeles, CA): Daniel O. Stram, Duncan C. Thomas, Dave V. Conti.
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
BC: breast cancer; CBC: contralateral breast cancer; UBC: unilateral breast cancer; PGVs: pathogenic germline variants; 1KGP: One Thousand Genomes Project; NFFE: non-Finnish female Europeans; SKAT: Sequence Kernel Association Test; POLR: Proportional Odds Logit Regression.
References
- Bernstein, J.L.; Thompson, W.D.; Risch, N.; Holford, T.R. Risk factors predicting the incidence of second primary breast cancer among women diagnosed with a first primary breast cancer. Am. J. Epidemiol. 1992, 136, 925–936. [Google Scholar] [CrossRef] [PubMed]
- Narod, S.A. Bilateral breast cancers. Nat. Rev. Clin. Oncol. 2014, 11, 157–166. [Google Scholar] [CrossRef] [PubMed]
- Giannakeas, V.; Lim, D.W.; Narod, S.A. The risk of contralateral breast cancer: A SEER-based analysis. Br. J. Cancer 2021, 125, 601–610. [Google Scholar] [CrossRef]
- Reiner, A.S.; John, E.M.; Brooks, J.D.; Lynch, C.F.; Bernstein, L.; Mellemkjaer, L.; Malone, K.E.; Knight, J.A.; Capanu, M.; Teraoka, S.N.; et al. Risk of asynchronous contralateral breast cancer in noncarriers of BRCA1 and BRCA2 mutations with a family history of breast cancer: A report from the Women’s Environmental Cancer and Radiation Epidemiology Study. J. Clin. Oncol. 2013, 31, 433–439. [Google Scholar] [CrossRef]
- Hartman, M.; Czene, K.; Reilly, M.; Adolfsson, J.; Bergh, J.; Adami, H.O.; Dickman, P.W.; Hall, P. Incidence and prognosis of synchronous and metachronous bilateral breast cancer. J. Clin. Oncol. 2007, 25, 4210–4216. [Google Scholar] [CrossRef] [PubMed]
- Schaapveld, M.; Visser, O.; Louwman, W.J.; Willemse, P.H.; de Vries, E.G.; van der Graaf, W.T.; Otter, R.; Coebergh, J.W.; van Leeuwen, F.E. The impact of adjuvant therapy on contralateral breast cancer risk and the prognostic significance of contralateral breast cancer: A population based study in the Netherlands. Breast Cancer Res. Treat. 2008, 110, 189–197. [Google Scholar] [CrossRef]
- Nash, R.; Goodman, M.; Lin, C.C.; Freedman, R.A.; Dominici, L.S.; Ward, K.; Jemal, A. State Variation in the Receipt of a Contralateral Prophylactic Mastectomy Among Women Who Received a Diagnosis of Invasive Unilateral Early-Stage Breast Cancer in the United States, 2004–2012. JAMA Surg. 2017, 152, 648–657. [Google Scholar] [CrossRef]
- Chiesa, F.; Sacchini, V.S. Risk-reducing mastectomy. Minerva Ginecol. 2016, 68, 544–547. [Google Scholar]
- Liede, A.; Cai, M.; Crouter, T.F.; Niepel, D.; Callaghan, F.; Evans, D.G. Risk-reducing mastectomy rates in the US: A closer examination of the Angelina Jolie effect. Breast Cancer Res. Treat. 2018, 171, 435–442. [Google Scholar] [CrossRef]
- Basu, N.N.; Ross, G.L.; Evans, D.G.; Barr, L. The Manchester guidelines for contralateral risk-reducing mastectomy. World J. Surg. Oncol. 2015, 13, 237. [Google Scholar] [CrossRef]
- Chowdhury, M.; Euhus, D.; Onega, T.; Biswas, S.; Choudhary, P.K. A model for individualized risk prediction of contralateral breast cancer. Breast Cancer Res. Treat. 2017, 161, 153–160. [Google Scholar] [CrossRef]
- O’Donnell, M. Estimating contralateral breast cancer risk. Curr. Breast Cancer Rep. 2018, 10, 91–97. [Google Scholar] [CrossRef]
- Giardiello, D.; Hooning, M.J.; Hauptmann, M.; Keeman, R.; Heemskerk-Gerritsen, B.A.M.; Becher, H.; Blomqvist, C.; Bojesen, S.E.; Bolla, M.K.; Camp, N.J.; et al. PredictCBC-2.0: A contralateral breast cancer risk prediction model developed and validated in ~200,000 patients. Breast Cancer Res. 2022, 24, 69. [Google Scholar] [CrossRef]
- Giardiello, D.; Hauptmann, M.; Steyerberg, E.W.; Adank, M.A.; Akdeniz, D.; Blom, J.C.; Blomqvist, C.; Bojesen, S.E.; Bolla, M.K.; Brinkhuis, M.; et al. Prediction of contralateral breast cancer: External validation of risk calculators in 20 international cohorts. Breast Cancer Res. Treat. 2020, 181, 423–434. [Google Scholar] [CrossRef]
- Reiner, A.S.; Sisti, J.; John, E.M.; Lynch, C.F.; Brooks, J.D.; Mellemkjaer, L.; Boice, J.D.; Knight, J.A.; Concannon, P.; Capanu, M.; et al. Breast Cancer Family History and Contralateral Breast Cancer Risk in Young Women: An Update From the Women’s Environmental Cancer and Radiation Epidemiology Study. J. Clin. Oncol. 2018, 36, 1513–1520. [Google Scholar] [CrossRef] [PubMed]
- Kramer, I.; Hooning, M.J.; Mavaddat, N.; Hauptmann, M.; Keeman, R.; Steyerberg, E.W.; Giardiello, D.; Antoniou, A.C.; Pharoah, P.D.P.; Canisius, S.; et al. Breast Cancer Polygenic Risk Score and Contralateral Breast Cancer Risk. Am. J. Hum. Genet. 2020, 107, 837–848. [Google Scholar] [CrossRef]
- Gronwald, J.; Tung, N.; Foulkes, W.D.; Offit, K.; Gershoni, R.; Daly, M.; Kim-Sing, C.; Olsson, H.; Ainsworth, P.; Eisen, A.; et al. Tamoxifen and contralateral breast cancer in BRCA1 and BRCA2 carriers: An update. Int. J. Cancer 2006, 118, 2281–2284. [Google Scholar] [CrossRef]
- Reding, K.W.; Bernstein, J.L.; Langholz, B.M.; Bernstein, L.; Haile, R.W.; Begg, C.B.; Lynch, C.F.; Concannon, P.; Borg, A.; Teraoka, S.N.; et al. Adjuvant systemic therapy for breast cancer in BRCA1/BRCA2 mutation carriers in a population-based study of risk of contralateral breast cancer. Breast Cancer Res. Treat. 2010, 123, 491–498. [Google Scholar] [CrossRef] [PubMed]
- Brooks, J.D.; Teraoka, S.N.; Malone, K.E.; Haile, R.W.; Bernstein, L.; Lynch, C.F.; Mellemkjaer, L.; Duggan, D.J.; Reiner, A.S.; Concannon, P.; et al. Variants in tamoxifen metabolizing genes: A case-control study of contralateral breast cancer risk in the WECARE study. Int. J. Mol. Epidemiol. Genet. 2013, 4, 35–48. [Google Scholar]
- Bernstein, J.L.; Haile, R.W.; Stovall, M.; Boice, J.D., Jr.; Shore, R.E.; Langholz, B.; Thomas, D.C.; Bernstein, L.; Lynch, C.F.; Olsen, J.H.; et al. Radiation exposure, the ATM Gene, and contralateral breast cancer in the women’s environmental cancer and radiation epidemiology study. J. Natl. Cancer Inst. 2010, 102, 475–483. [Google Scholar] [CrossRef]
- Bertelsen, L.; Bernstein, L.; Olsen, J.H.; Mellemkjaer, L.; Haile, R.W.; Lynch, C.F.; Malone, K.E.; Anton-Culver, H.; Christensen, J.; Langholz, B.; et al. Effect of systemic adjuvant treatment on risk for contralateral breast cancer in the Women’s Environment, Cancer and Radiation Epidemiology Study. J. Natl. Cancer Inst. 2008, 100, 32–40. [Google Scholar] [CrossRef]
- Langballe, R.; Mellemkjaer, L.; Malone, K.E.; Lynch, C.F.; John, E.M.; Knight, J.A.; Bernstein, L.; Brooks, J.; Andersson, M.; Reiner, A.S.; et al. Systemic therapy for breast cancer and risk of subsequent contralateral breast cancer in the WECARE Study. Breast Cancer Res. 2016, 18, 65. [Google Scholar] [CrossRef] [PubMed]
- Fletcher, O.; Johnson, N.; Dos Santos Silva, I.; Kilpivaara, O.; Aittomaki, K.; Blomqvist, C.; Nevanlinna, H.; Wasielewski, M.; Meijers-Heijerboer, H.; Broeks, A.; et al. Family history, genetic testing, and clinical risk prediction: Pooled analysis of CHEK2 1100delC in 1,828 bilateral breast cancers and 7030 controls. Cancer Epidemiol. Biomarkers Prev. 2009, 18, 230–234. [Google Scholar] [CrossRef] [PubMed]
- Metcalfe, K.; Gershman, S.; Lynch, H.T.; Ghadirian, P.; Tung, N.; Kim-Sing, C.; Olopade, O.I.; Domchek, S.; McLennan, J.; Eisen, A.; et al. Predictors of contralateral breast cancer in BRCA1 and BRCA2 mutation carriers. Br. J. Cancer 2011, 104, 1384–1392. [Google Scholar] [CrossRef]
- Malone, K.E.; Begg, C.B.; Haile, R.W.; Borg, A.; Concannon, P.; Tellhed, L.; Xue, S.; Teraoka, S.; Bernstein, L.; Capanu, M.; et al. Population-based study of the risk of second primary contralateral breast cancer associated with carrying a mutation in BRCA1 or BRCA2. J. Clin. Oncol. 2010, 28, 2404–2410. [Google Scholar] [CrossRef] [PubMed]
- Tischkowitz, M.; Capanu, M.; Sabbaghian, N.; Li, L.; Liang, X.; Vallee, M.P.; Tavtigian, S.V.; Concannon, P.; Foulkes, W.D.; Bernstein, L.; et al. Rare germline mutations in PALB2 and breast cancer risk: A population-based study. Hum. Mutat. 2012, 33, 674–680. [Google Scholar] [CrossRef]
- Reiner, A.S.; Robson, M.E.; Mellemkjaer, L.; Tischkowitz, M.; John, E.M.; Lynch, C.F.; Brooks, J.D.; Boice, J.D.; Knight, J.A.; Teraoka, S.N.; et al. Radiation Treatment, ATM, BRCA1/2, and CHEK2*1100delC Pathogenic Variants and Risk of Contralateral Breast Cancer. J. Natl. Cancer Inst. 2020, 112, 1275–1279. [Google Scholar] [CrossRef]
- Mellemkjaer, L.; Dahl, C.; Olsen, J.H.; Bertelsen, L.; Guldberg, P.; Christensen, J.; Borresen-Dale, A.L.; Stovall, M.; Langholz, B.; Bernstein, L.; et al. Risk for contralateral breast cancer among carriers of the CHEK2*1100delC mutation in the WECARE Study. Br. J. Cancer 2008, 98, 728–733. [Google Scholar] [CrossRef]
- Bernstein, J.L.; Langholz, B.; Haile, R.W.; Bernstein, L.; Thomas, D.C.; Stovall, M.; Malone, K.E.; Lynch, C.F.; Olsen, J.H.; Anton-Culver, H.; et al. Study design: Evaluating gene-environment interactions in the etiology of breast cancer—The WECARE study. Breast Cancer Res. 2004, 6, R199–R214. [Google Scholar] [CrossRef]
- Borg, A.; Haile, R.W.; Malone, K.E.; Capanu, M.; Diep, A.; Torngren, T.; Teraoka, S.; Begg, C.B.; Thomas, D.C.; Concannon, P.; et al. Characterization of BRCA1 and BRCA2 deleterious mutations and variants of unknown clinical significance in unilateral and bilateral breast cancer: The WECARE study. Hum. Mutat. 2010, 31, E1200–E1240. [Google Scholar] [CrossRef]
- Robson, M.E.; Reiner, A.S.; Brooks, J.D.; Concannon, P.J.; John, E.M.; Mellemkjaer, L.; Bernstein, L.; Malone, K.E.; Knight, J.A.; Lynch, C.F.; et al. Association of Common Genetic Variants With Contralateral Breast Cancer Risk in the WECARE Study. J. Natl. Cancer Inst. 2017, 109, djx051. [Google Scholar] [CrossRef] [PubMed]
- Sisti, J.S.; Bernstein, J.L.; Lynch, C.F.; Reiner, A.S.; Mellemkjaer, L.; Brooks, J.D.; Knight, J.A.; Bernstein, L.; Malone, K.E.; Woods, M.; et al. Reproductive factors, tumor estrogen receptor status and contralateral breast cancer risk: Results from the WECARE study. Springerplus 2015, 4, 825. [Google Scholar] [CrossRef] [PubMed]
- Figueiredo, J.C.; Brooks, J.D.; Conti, D.V.; Poynter, J.N.; Teraoka, S.N.; Malone, K.E.; Bernstein, L.; Lee, W.D.; Duggan, D.J.; Siniard, A.; et al. Risk of contralateral breast cancer associated with common variants in BRCA1 and BRCA2: Potential modifying effect of BRCA1/BRCA2 mutation carrier status. Breast Cancer Res. Treat. 2011, 127, 819–829. [Google Scholar] [CrossRef]
- Poynter, J.N.; Langholz, B.; Largent, J.; Mellemkjaer, L.; Bernstein, L.; Malone, K.E.; Lynch, C.F.; Borg, A.; Concannon, P.; Teraoka, S.N.; et al. Reproductive factors and risk of contralateral breast cancer by BRCA1 and BRCA2 mutation status: Results from the WECARE study. Cancer Causes Control 2010, 21, 839–846. [Google Scholar] [CrossRef] [PubMed]
- Konig, K.; Peifer, M.; Fassunke, J.; Ihle, M.A.; Kunstlinger, H.; Heydt, C.; Stamm, K.; Ueckeroth, F.; Vollbrecht, C.; Bos, M.; et al. Implementation of Amplicon Parallel Sequencing Leads to Improvement of Diagnosis and Therapy of Lung Cancer Patients. J. Thorac. Oncol. 2015, 10, 1049–1057. [Google Scholar] [CrossRef]
- Clarke, L.; Fairley, S.; Zheng-Bradley, X.; Streeter, I.; Perry, E.; Lowy, E.; Tasse, A.M.; Flicek, P. The international Genome sample resource (IGSR): A worldwide collection of genome variation incorporating the 1000 Genomes Project data. Nucleic Acids Res. 2017, 45, D854–D859. [Google Scholar] [CrossRef]
- Hadfield, J.; Eldridge, M.D. Multi-genome alignment for quality control and contamination screening of next-generation sequencing data. Front. Genet. 2014, 5, 31. [Google Scholar] [CrossRef]
- Martin, M. Cutadapt removes adapter sequences from high-throughput sequencing reads. EMBnet J. 2011, 17, 10–12. [Google Scholar] [CrossRef]
- Li, H. Aligning sequence reads, clone sequences and assembly contigs with BWA-MEM. arXiv 2013, arXiv:1303.3997v1302. [Google Scholar]
- Danecek, P.; Bonfield, J.K.; Liddle, J.; Marshall, J.; Ohan, V.; Pollard, M.O.; Whitwham, A.; Keane, T.; McCarthy, S.A.; Davies, R.M.; et al. Twelve years of SAMtools and BCFtools. Gigascience 2021, 10, giab008. [Google Scholar] [CrossRef]
- Van der Auwera, G.A.; Carneiro, M.O.; Hartl, C.; Poplin, R.; Del Angel, G.; Levy-Moonshine, A.; Jordan, T.; Shakir, K.; Roazen, D.; Thibault, J.; et al. From FastQ data to high confidence variant calls: The Genome Analysis Toolkit best practices pipeline. Curr. Protoc. Bioinform. 2013, 43, 11.10.1–11.10.33. [Google Scholar] [CrossRef] [PubMed]
- McLaren, W.; Gil, L.; Hunt, S.E.; Riat, H.S.; Ritchie, G.R.; Thormann, A.; Flicek, P.; Cunningham, F. The Ensembl Variant Effect Predictor. Genome Biol. 2016, 17, 122. [Google Scholar] [CrossRef] [PubMed]
- Landrum, M.J.; Chitipiralla, S.; Brown, G.R.; Chen, C.; Gu, B.; Hart, J.; Hoffman, D.; Jang, W.; Kaur, K.; Liu, C.; et al. ClinVar: Improvements to accessing data. Nucleic Acids Res. 2020, 48, D835–D844. [Google Scholar] [CrossRef]
- Ng, P.C.; Henikoff, S. SIFT: Predicting amino acid changes that affect protein function. Nucleic Acids Res. 2003, 31, 3812–3814. [Google Scholar] [CrossRef]
- Adzhubei, I.A.; Schmidt, S.; Peshkin, L.; Ramensky, V.E.; Gerasimova, A.; Bork, P.; Kondrashov, A.S.; Sunyaev, S.R. A method and server for predicting damaging missense mutations. Nat. Methods 2010, 7, 248–249. [Google Scholar] [CrossRef]
- Rentzsch, P.; Witten, D.; Cooper, G.M.; Shendure, J.; Kircher, M. CADD: Predicting the deleteriousness of variants throughout the human genome. Nucleic Acids Res. 2019, 47, D886–D894. [Google Scholar] [CrossRef]
- Easton, D.F.; Pharoah, P.D.; Antoniou, A.C.; Tischkowitz, M.; Tavtigian, S.V.; Nathanson, K.L.; Devilee, P.; Meindl, A.; Couch, F.J.; Southey, M.; et al. Gene-panel sequencing and the prediction of breast-cancer risk. N. Engl. J. Med. 2015, 372, 2243–2257. [Google Scholar] [CrossRef] [PubMed]
- Hu, C.; Hart, S.N.; Gnanaolivu, R.; Huang, H.; Lee, K.Y.; Na, J.; Gao, C.; Lilyquist, J.; Yadav, S.; Boddicker, N.J.; et al. A Population-Based Study of Genes Previously Implicated in Breast Cancer. N. Engl. J. Med. 2021, 384, 440–451. [Google Scholar] [CrossRef]
- Breast Cancer Association, C.; Dorling, L.; Carvalho, S.; Allen, J.; Gonzalez-Neira, A.; Luccarini, C.; Wahlstrom, C.; Pooley, K.A.; Parsons, M.T.; Fortuno, C.; et al. Breast Cancer Risk Genes - Association Analysis in More than 113,000 Women. N. Engl. J. Med. 2021, 384, 428–439. [Google Scholar] [CrossRef]
- Wu, M.C.; Lee, S.; Cai, T.; Li, Y.; Boehnke, M.; Lin, X. Rare-variant association testing for sequencing data with the sequence kernel association test. Am. J. Hum. Genet. 2011, 89, 82–93. [Google Scholar] [CrossRef] [PubMed]
- Prive, F.; Luu, K.; Blum, M.G.B.; McGrath, J.J.; Vilhjalmsson, B.J. Efficient toolkit implementing best practices for principal component analysis of population genetic data. Bioinformatics 2020, 36, 4449–4457. [Google Scholar] [CrossRef] [PubMed]
- Venables, W.N.; Ripley, B.D. Modern applied statistics with S-PLUS, 4th ed.; Springer: Berlin/Heidelberg, Germany, 2002. [Google Scholar]
- Willer, C.J.; Li, Y.; Abecasis, G.R. METAL: Fast and efficient meta-analysis of genomewide association scans. Bioinformatics 2010, 26, 2190–2191. [Google Scholar] [CrossRef] [PubMed]
- Yao, K.K.; Clifford, J.; Li, S.; LaDuca, H.; Hulick, P.; Gutierrez, S.; Black, M.H. Prevalence of Germline Pathogenic and Likely Pathogenic Variants in Patients With Second Breast Cancers. JNCI Cancer Spectr. 2020, 4, pkaa094. [Google Scholar] [CrossRef]
- Fanale, D.; Incorvaia, L.; Filorizzo, C.; Bono, M.; Fiorino, A.; Calo, V.; Brando, C.; Corsini, L.R.; Barraco, N.; Badalamenti, G.; et al. Detection of Germline Mutations in a Cohort of 139 Patients with Bilateral Breast Cancer by Multi-Gene Panel Testing: Impact of Pathogenic Variants in Other Genes beyond BRCA1/2. Cancers 2020, 12, 2415. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).