Multi-Lens Arrays (MLA)-Assisted Photothermal Effects for Enhanced Fractional Cancer Treatment: Computational and Experimental Validations
Abstract
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
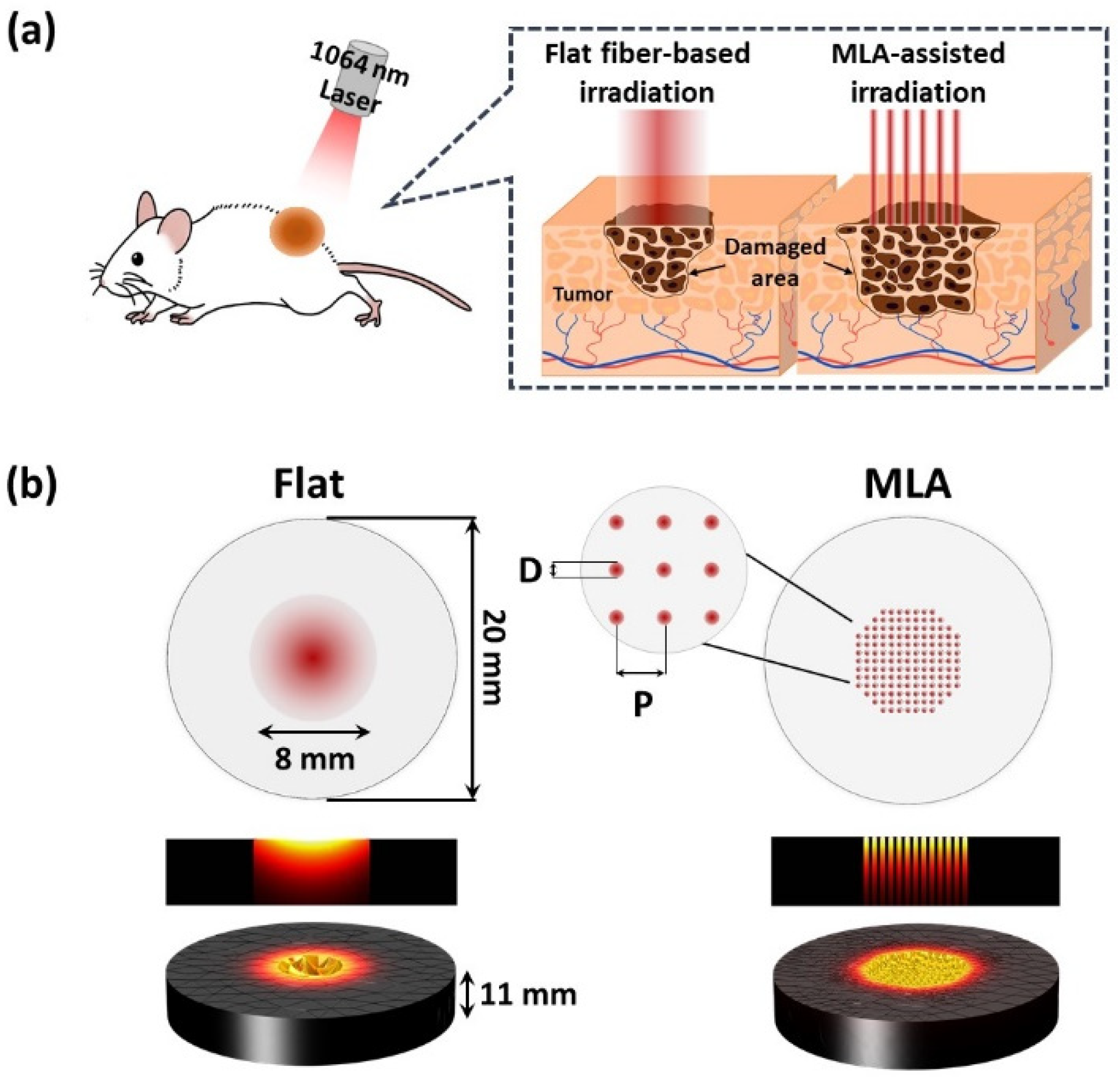
2.1. Light Source
2.2. Temperature Assessments
2.2.1. Numerical Simulation
2.2.2. Phantom Evaluations
2.3. Aqueous Solution Experiments
2.4. In Vivo Validations
2.5. Histological Analysis
2.6. Statistical Analysis
3. Results
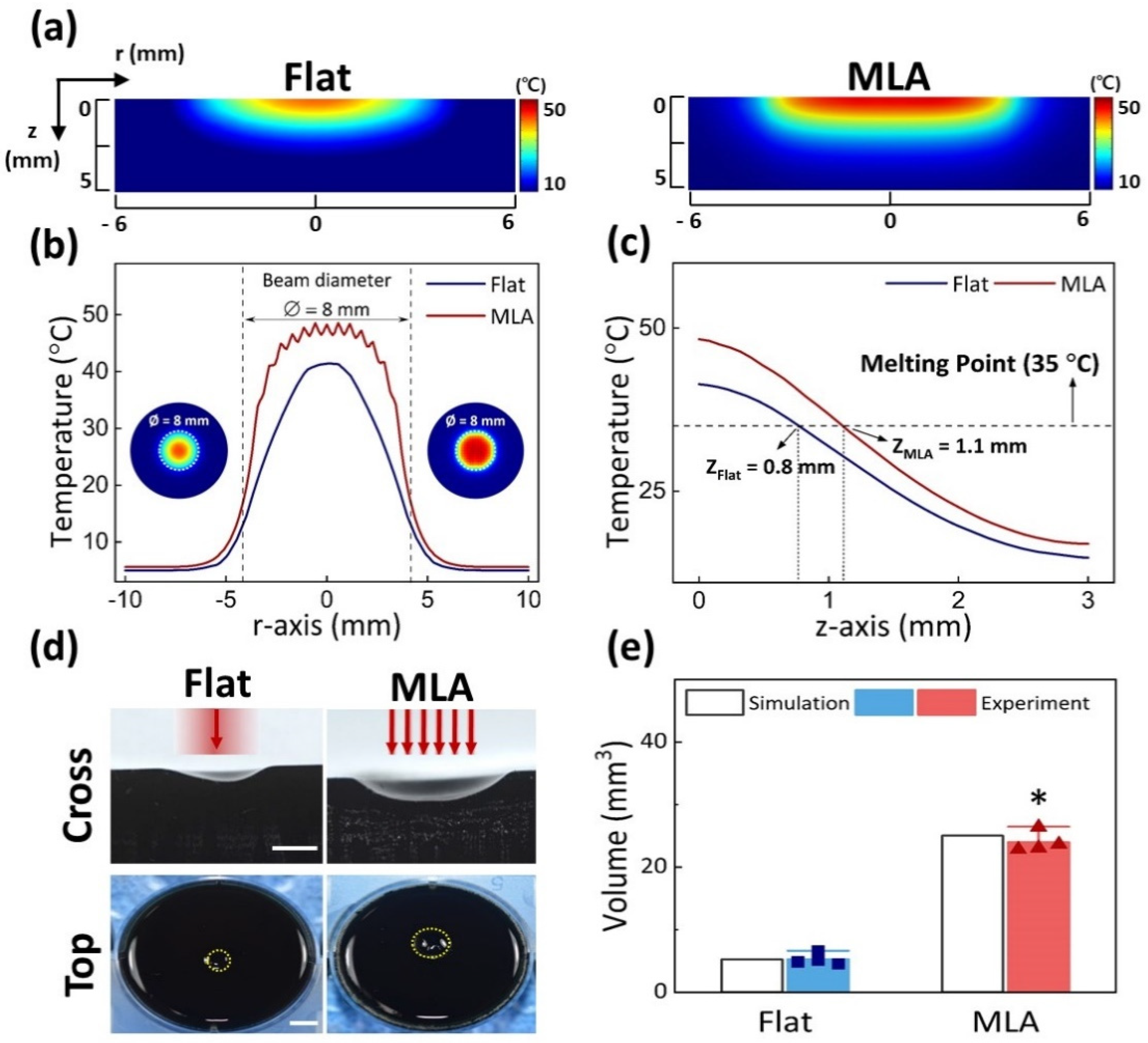
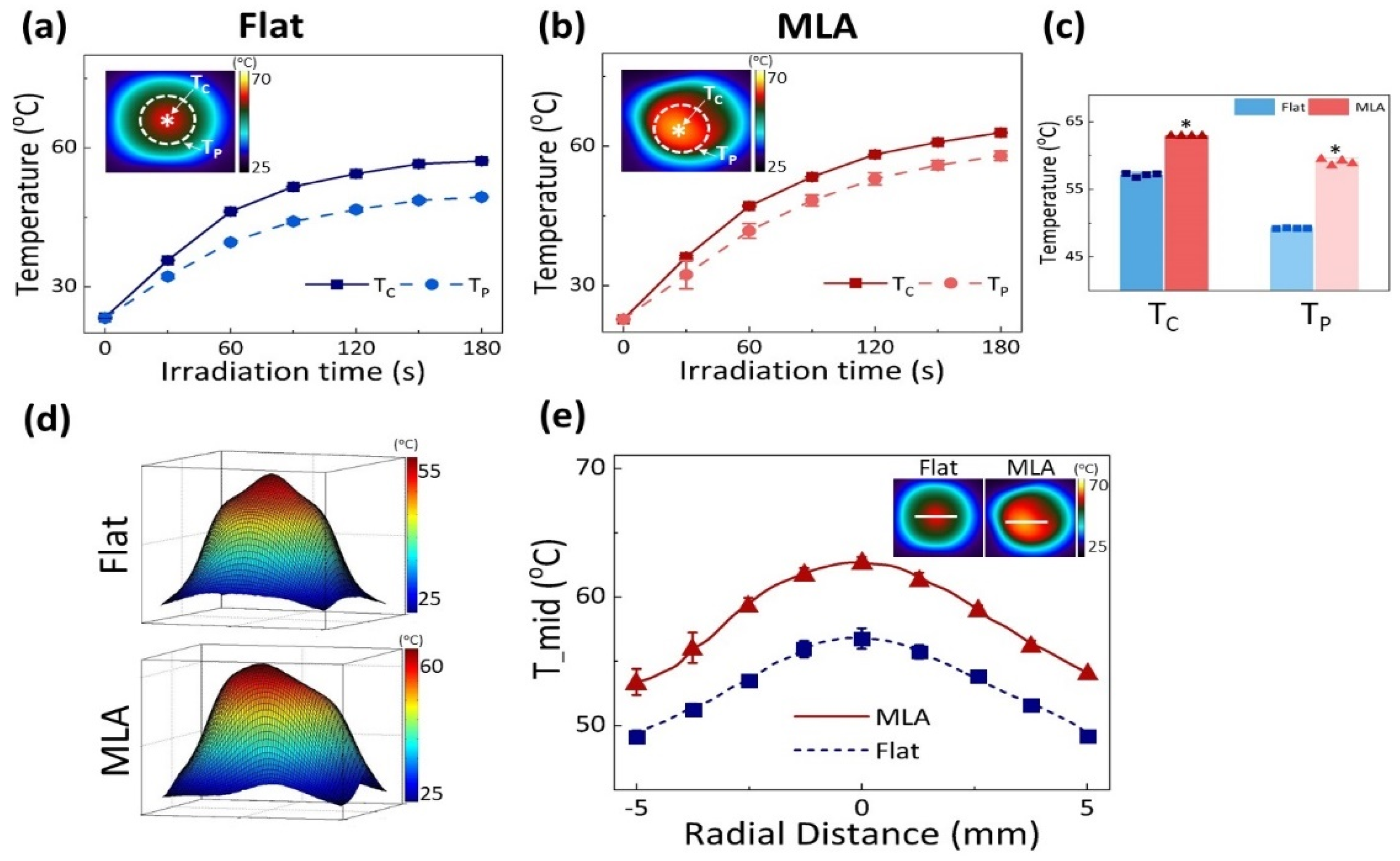
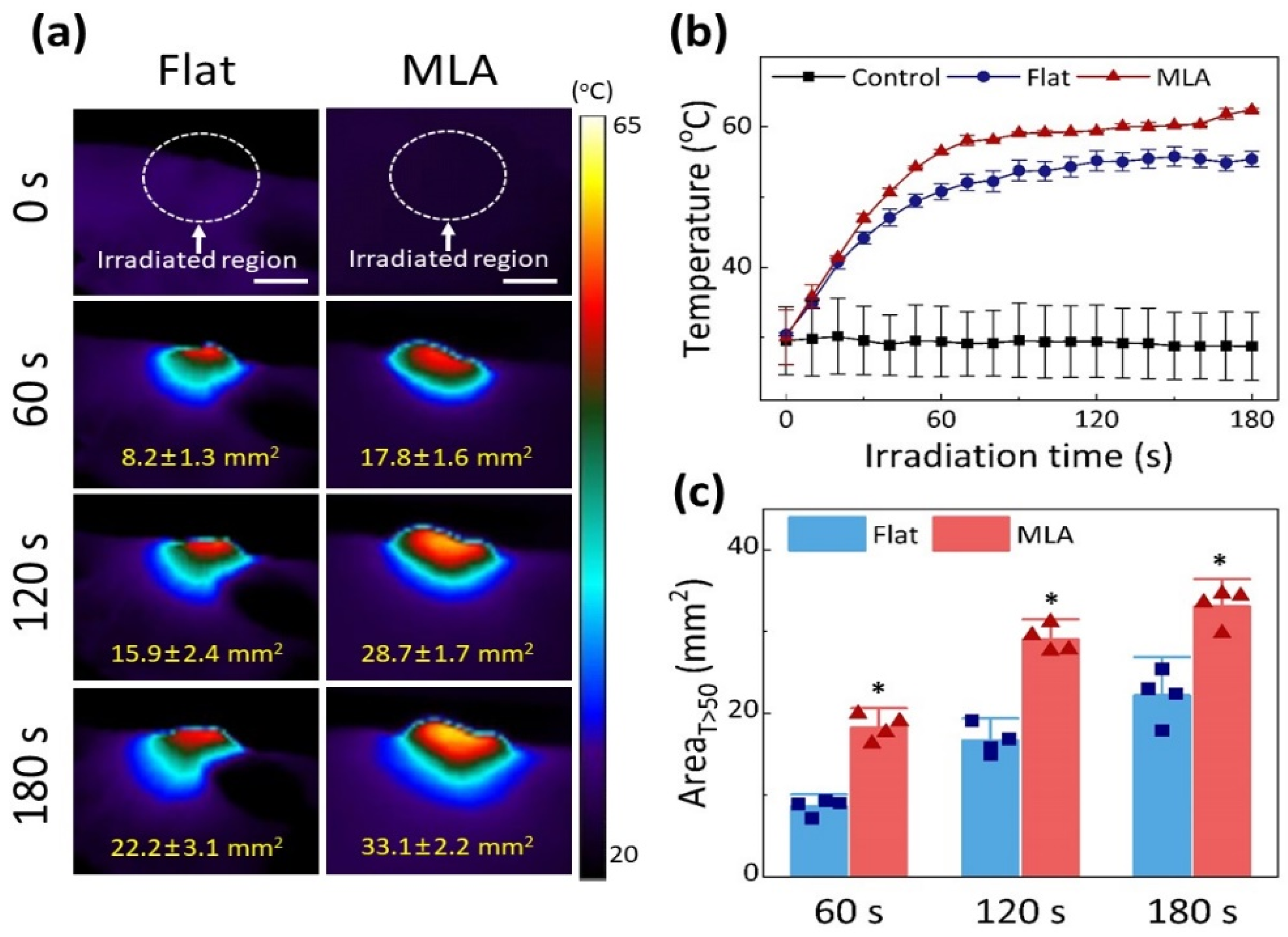
3.1. Temperature Assessments
3.2. Dosimetry Tests
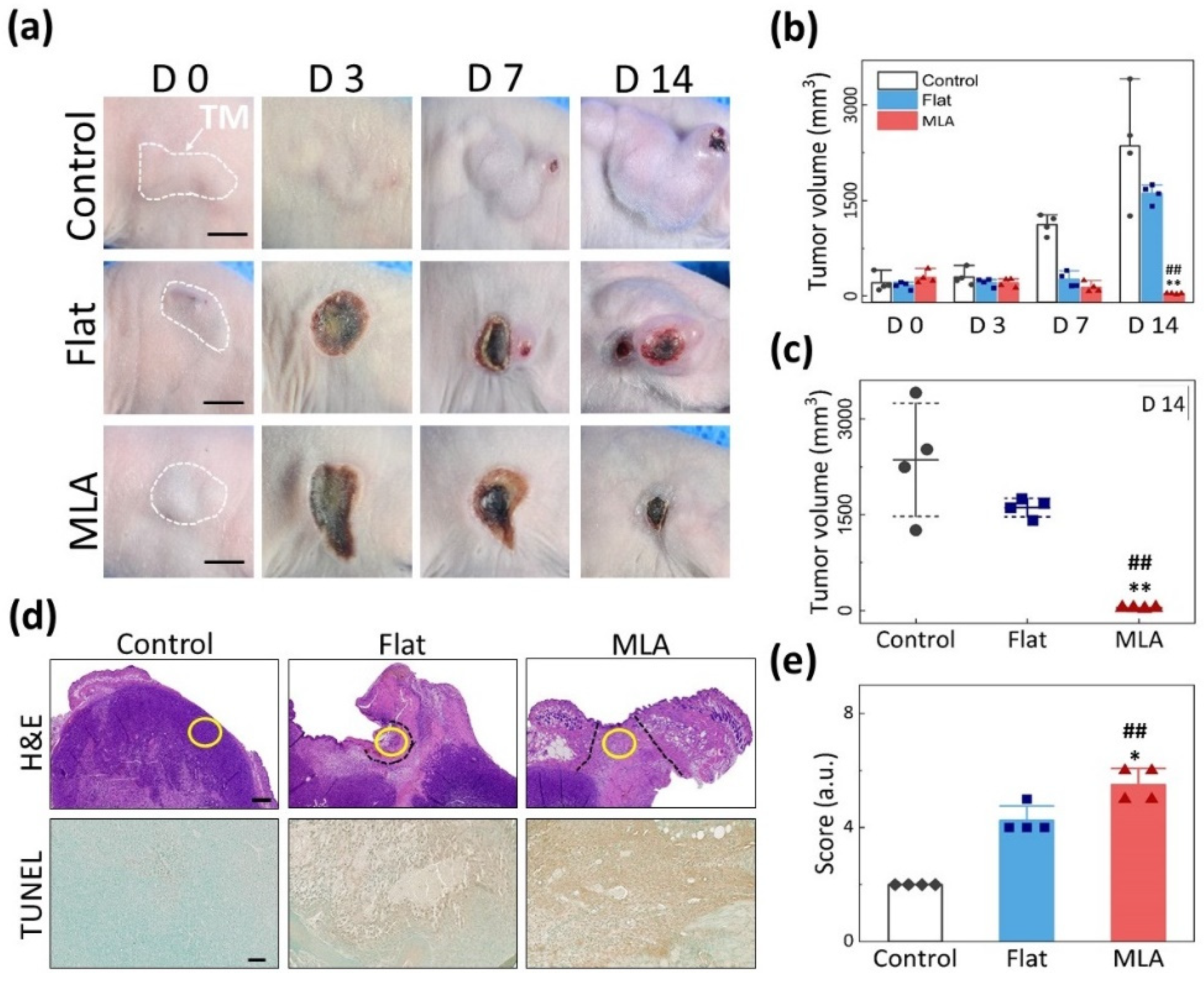
3.3. In vivo Treatment
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Siegel, R.L.; Miller, K.D.; Goding Sauer, A.; Fedewa, S.A.; Butterly, L.F.; Anderson, J.C.; Cercek, A.; Smith, R.A.; Jemal, A. Colorectal cancer statistics, 2020. CA Cancer J. Clin. 2020, 70, 145–164. [Google Scholar] [CrossRef]
- Wild, C.P.; Stewart, B.W.; Wild, C. World Cancer Report 2014; World Health Organization Geneva: Genève, Switzerland, 2014. [Google Scholar]
- Kawczyk-Krupka, A.; Bugaj, A.M.; Latos, W.; Zaremba, K.; Wawrzyniec, K.; Sieroń, A. Photodynamic therapy in colorectal cancer treatment: The state of the art in clinical trials. Photodiagnosis Photodyn. Ther. 2015, 12, 545–553. [Google Scholar] [CrossRef]
- Chen, C.; Neumann, J.; Kühn, F.; Lee, S.M.; Drefs, M.; Andrassy, J.; Werner, J.; Bazhin, A.V.; Schiergens, T.S. Establishment of an Endoscopy-Guided Minimally Invasive Orthotopic Mouse Model of Colorectal Cancer. Cancers 2020, 12, 3007. [Google Scholar] [CrossRef] [PubMed]
- Khot, M.I.; Andrew, H.; Svavarsdottir, H.S.; Armstrong, G.; Quyn, A.J.; Jayne, D.G. A review on the scope of photothermal therapy–based nanomedicines in preclinical models of colorectal cancer. Clin. Colorectal Cancer 2019, 18, e200–e209. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.; Van Phuc Nguyen, P.M.; Jung, M.J.; Kim, S.W.; Oh, J.; Kang, H.W. Doxorubicin-fucoidan-gold nanoparticles composite for dual-chemo-photothermal treatment on eye tumors. Oncotarget 2017, 8, 113719. [Google Scholar] [CrossRef] [PubMed]
- Salem, D.S.; Sliem, M.A.; El-Sesy, M.; Shouman, S.A.; Badr, Y. Improved chemo-photothermal therapy of hepatocellular carcinoma using chitosan-coated gold nanoparticles. J. Photochem. Photobiol. B Biol. 2018, 182, 92–99. [Google Scholar] [CrossRef]
- Mirrahimi, M.; Abed, Z.; Beik, J.; Shiri, I.; Dezfuli, A.S.; Mahabadi, V.P.; Kamrava, S.K.; Ghaznavi, H.; Shakeri-Zadeh, A. A thermo-responsive alginate nanogel platform co-loaded with gold nanoparticles and cisplatin for combined cancer chemo-photothermal therapy. Pharmacol. Res. 2019, 143, 178–185. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.-J.; Lin, C.-W.; Yang, H.-W.; Lin, K.-J.; Wey, S.-P.; Sun, C.-L.; Wei, K.-C.; Yen, T.-C.; Lin, C.-I.; Ma, C.-C.M. Biodistribution of PEGylated graphene oxide nanoribbons and their application in cancer chemo-photothermal therapy. Carbon 2014, 74, 83–95. [Google Scholar] [CrossRef]
- Hong, G.; Diao, S.; Antaris, A.L.; Dai, H. Carbon nanomaterials for biological imaging and nanomedicinal therapy. Chem. Rev. 2015, 115, 10816–10906. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, N.; Rodrigues, C.F.; Moreira, A.F.; Correia, I.J. Overview of the application of inorganic nanomaterials in cancer photothermal therapy. Biomater. Sci. 2020, 8, 2990–3020. [Google Scholar] [CrossRef]
- Nguyen, T.H.; Rhee, Y.-h.; Ahn, J.-c.; Kang, H.W. Circumferential irradiation for interstitial coagulation of urethral stricture. Opt. Express 2015, 23, 20829–20840. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.C.; Childs, J.; Chung, H.J.; Park, J.; Hong, J.; Cho, S.B. Pattern analysis of 532-and 1,064-nm picosecond-domain laser-induced immediate tissue reactions in ex vivo pigmented micropig skin. Sci. Rep. 2019, 9, 1–10. [Google Scholar]
- Hwang, C.Y.; Chen, C.C. Serial change in laser-induced optical breakdown by 1064-nm Nd:YAG picosecond laser. Photodermatol. Photoimmunol. Photomed. 2020, 36, 63–64. [Google Scholar] [CrossRef] [PubMed]
- Yoo, S.W.; Park, H.-J.; Oh, G.; Hwang, S.; Yun, M.; Wang, T.; Seo, Y.-S.; Min, J.-J.; Kim, K.H.; Kim, E.-S. Non-ablative fractional thulium laser irradiation suppresses early tumor growth. Curr. Opt. Photonics 2017, 1, 51–59. [Google Scholar] [CrossRef]
- Al-Jawad, S.M.; Taha, A.A.; Al-Halbosiy, M.M.; Al-Barram, L.F. Synthesis and characterization of small-sized gold nanoparticles coated by bovine serum albumin (BSA) for cancer photothermal therapy. Photodiagnosis Photodyn. Ther. 2018, 21, 201–210. [Google Scholar] [CrossRef] [PubMed]
- Welch, A.J.; Van Gemert, M.J. Optical-Thermal Response of Laser-Irradiated Tissue; Springer: Berlin/Heidelberg, Germany, 2011; Volume 2. [Google Scholar]
- Gnyawali, S.C.; Chen, Y.; Wu, F.; Bartels, K.E.; Wicksted, J.P.; Liu, H.; Sen, C.K.; Chen, W.R. Temperature measurement on tissue surface during laser irradiation. Med Biol. Eng. Comput. 2008, 46, 159–168. [Google Scholar] [CrossRef]
- Mahesh, S.; Joshi, S.C. Thermal conductivity variations with composition of gelatin-silica aerogel-sodium dodecyl sulfate with functionalized multi-walled carbon nanotube doping in their composites. Int. J. Heat Mass Transf. 2015, 87, 606–615. [Google Scholar] [CrossRef]
- Kalmar, M.; Hoffmann, T.; Sauerhering, J.; Klink, F. Manufacturing process for hydrogel vessel phantoms. Curr. Dir. Biomed. Eng. 2019, 5, 537–540. [Google Scholar] [CrossRef]
- Kim, H.; Kim, S.W.; Seok, K.H.; Hwang, C.W.; Ahn, J.-C.; Jin, J.-O.; Kang, H.W. Hypericin-assisted photodynamic therapy against anaplastic thyroid cancer. Photodiagnosis Photodyn. Ther. 2018, 24, 15–21. [Google Scholar] [CrossRef]
- Takahashi, M.; Yasui, H.; Ogura, A.; Asanuma, T.; Kubota, N.; Tsujitani, M.; Kuwabara, M.; Inanami, O. X Irradiation Combined with TNF α-related Apoptosis-inducing Ligand (TRAIL) Reduces Hypoxic Regions of Human Gastric Adenocarcinoma Xenografts in SCID Mice. J. Radiat. Res. 2008, 49, 153–161. [Google Scholar] [CrossRef][Green Version]
- Mocan, L.; Tabaran, F.A.; Mocan, T.; Bele, C.; Orza, A.I.; Lucan, C.; Stiufiuc, R.; Manaila, I.; Iulia, F.; Dana, I. Selective ex-vivo photothermal ablation of human pancreatic cancer with albumin functionalized multiwalled carbon nanotubes. Int. J. Nanomed. 2011, 6, 915. [Google Scholar]
- Laubach, H.J.; Tannous, Z.; Anderson, R.R.; Manstein, D. Skin responses to fractional photothermolysis. Lasers Surg. Med. Off. J. Am. Soc. Laser Med. Surg. 2006, 38, 142–149. [Google Scholar] [CrossRef]
- Lipozenčić, J.; Bukvić Mokoš, Z. Dermatologic lasers in the treatment of aging skin. Acta Dermatovenerol. Croat. 2010, 18, 176–180. [Google Scholar] [PubMed]
- Anderson, R.R. Lasers for dermatology and skin biology. J. Investig. Derm. 2013, 133, E21–E23. [Google Scholar] [CrossRef] [PubMed]
- Gye, J.; Ahn, S.K.; Kwon, J.-E.; Hong, S.-P. Use of fractional CO2 laser decreases the risk of skin cancer development during ultraviolet exposure in hairless mice. Dermatol. Surg. 2015, 41, 378–386. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Ma, X.; Hong, X.; Cheng, Y.; Tian, Y.; Zhao, S.; Liu, W.; Tang, Y.; Zhao, R.; Song, L. Adjuvant photothermal therapy inhibits local recurrences after breast-conserving surgery with little skin damage. ACS Nano 2018, 12, 662–670. [Google Scholar] [CrossRef] [PubMed]
- Revazova, E.; Bryzgalov, I.; Sorokina, I.; Ivanov, A.; Sebastian, J.; Keller, G.; Watson, J. Stimulation of the growth of human tumor by low-power laser irradiation. Bull. Exp. Biol. Med. 2001, 132, 778–779. [Google Scholar] [CrossRef] [PubMed]
- Kara, C.; Selamet, H.; Gökmenoğlu, C.; Kara, N. Low level laser therapy induces increased viability and proliferation in isolated cancer cells. Cell Prolif. 2018, 51, e12417. [Google Scholar] [CrossRef]
- Bamps, M.; Dok, R.; Nuyts, S. Low-level laser therapy stimulates proliferation in head and neck squamous cell carcinoma cells. Front. Oncol. 2018, 8, 343. [Google Scholar] [CrossRef]
- De Castro, J.L.F.; Pinheiro, A.L.B.; Werneck, C.E.; Soares, C.P. The effect of laser therapy on the proliferation of oral KB carcinoma cells: An in vitro study. Photomed. Laser Surg. 2005, 23, 586–589. [Google Scholar] [CrossRef]
- Zhang, J.; Xing, D.; Gao, X. Low-power laser irradiation activates Src tyrosine kinase through reactive oxygen species-mediated signaling pathway. J. Cell. Physiol. 2008, 217, 518–528. [Google Scholar] [CrossRef] [PubMed]
- Rhee, Y.-H.; Moon, J.-H.; Choi, S.-H.; Ahn, J.-C. Low-level laser therapy promoted aggressive proliferation and angiogenesis through decreasing of transforming growth factor-β1 and increasing of Akt/Hypoxia inducible factor-1α in anaplastic thyroid cancer. Photomed. Laser Surg. 2016, 34, 229–235. [Google Scholar] [CrossRef]
- Jing, X.; Yang, F.; Shao, C.; Wei, K.; Xie, M.; Shen, H.; Shu, Y. Role of hypoxia in cancer therapy by regulating the tumor microenvironment. Mol. Cancer 2019, 18, 1–15. [Google Scholar] [CrossRef]
- Bredholt, G.; Mannelqvist, M.; Stefansson, I.M.; Birkeland, E.; Bø, T.H.; Øyan, A.M.; Trovik, J.; Kalland, K.-H.; Jonassen, I.; Salvesen, H.B. Tumor necrosis is an important hallmark of aggressive endometrial cancer and associates with hypoxia, angiogenesis and inflammation responses. Oncotarget 2015, 6, 39676. [Google Scholar] [CrossRef] [PubMed]
- Kopp, C.; Ravel, L.; Meyrueis, P. Efficient beamshaper homogenizer design combining diffractive optical elements, microlens array and random phase plate. J. Opt. A Pure Appl. Opt. 1999, 1, 398. [Google Scholar] [CrossRef]
- Przybyszewska, M.; Miłoszewska, J.; Kotlarz, A.; Swoboda, P.; Pyśniak, K.; Szczepek, W.; Kaczmarek, Ł.; Markowicz, S. Imatinib inhibits the renewal and tumorigenicity of CT-26 colon cancer cells after cytoreductive treatment with doxorubicin. Arch. Immunol. Ther. Exp. 2017, 65, 51–67. [Google Scholar] [CrossRef] [PubMed]
- Lai, P.; Xu, X.; Wang, L.V. Dependence of optical scattering from Intralipid in gelatin-gel based tissue-mimicking phantoms on mixing temperature and time. J. Biomed. Opt. 2014, 19, 035002. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Value |
|---|---|
| Absorption coefficient (μa, mm-1) | 1 |
| Density (ρ, kg·mm-1) | 1060 |
| Thermal conductivity (k, W/m·K) | 0.303 |
| Specific heat (Cp, J/kg·K) | 3600 |
| Beam radius (r0, mm) | 8 |
| Convective heat coefficient (h, W/m2·K) | 10 |
| Air temperature (Tair, K) | 293.15 |
| Laser power (P, W) | 1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, H.; Pyo, H.; Kim, H.; Kang, H.W. Multi-Lens Arrays (MLA)-Assisted Photothermal Effects for Enhanced Fractional Cancer Treatment: Computational and Experimental Validations. Cancers 2021, 13, 1146. https://doi.org/10.3390/cancers13051146
Kim H, Pyo H, Kim H, Kang HW. Multi-Lens Arrays (MLA)-Assisted Photothermal Effects for Enhanced Fractional Cancer Treatment: Computational and Experimental Validations. Cancers. 2021; 13(5):1146. https://doi.org/10.3390/cancers13051146
Chicago/Turabian StyleKim, Hyejin, Hanjae Pyo, Hyeonsoo Kim, and Hyun Wook Kang. 2021. "Multi-Lens Arrays (MLA)-Assisted Photothermal Effects for Enhanced Fractional Cancer Treatment: Computational and Experimental Validations" Cancers 13, no. 5: 1146. https://doi.org/10.3390/cancers13051146
APA StyleKim, H., Pyo, H., Kim, H., & Kang, H. W. (2021). Multi-Lens Arrays (MLA)-Assisted Photothermal Effects for Enhanced Fractional Cancer Treatment: Computational and Experimental Validations. Cancers, 13(5), 1146. https://doi.org/10.3390/cancers13051146






