Responses to SARS-CoV-2 Vaccination in Patients with Cancer (ReCOVer Study): A Prospective Cohort Study of the Hellenic Cooperative Oncology Group
Abstract
:Simple Summary
Abstract
1. Introduction
2. Results
2.1. Participants’ Characteristics
2.2. Serological Outcomes
2.3. Seronegative Volunteers and Cancer Patients
2.4. Adverse Events Post Vaccination
3. Discussion
Limitations
4. Methods
4.1. Patients
4.2. Study Design
4.3. Sample Collection and Detection of Neutralizing Antibodies to SARS-Cov-2 Spike Protein
4.4. Data Recording
4.5. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rüthrich, M.M.; Giessen-Jung, C.; Borgmann, S.; Classen, A.Y.; Dolff, S.; Grüner, B.; Hanses, F.; Isberner, N.; Köh-ler, P.; Lanznaster, J.; et al. LEOSS Study Group. COVID-19 in cancer patients: Clinical characteristics and out-come-an analysis of the LEOSS registry. Ann. Hematol. 2021, 100, 383–393. [Google Scholar] [CrossRef] [PubMed]
- Bhaskaran, K.; Bacon, S.; Evans, S.J.; Bates, C.J.; Rentsch, C.T.; MacKenna, B.; Tomlinson, L.; Walker, A.J.; Schultze, A.; Morton, E.C.; et al. Factors associated with deaths due to COVID-19 versus other causes: Population-based cohort analysis of UK primary care data and linked national death registrations within the OpenSAFELY platform. Lancet Reg. Health Eur. 2021, 6, 100109. [Google Scholar] [CrossRef] [PubMed]
- Kuderer, N.M.; Choueiri, T.K.; Shah, D.P.; Shyr, Y.; Rubinstein, S.M.; Rivera, D.R.; Shete, S.; Hsu, C.Y.; Desai, A.; de Lima Lopes, G., Jr.; et al. Clinical impact of COVID-19 on patients with cancer (CCC19): A cohort study. Lancet 2020, 395, 1907–1918. [Google Scholar] [CrossRef]
- Saini, K.S.; Tagliamento, M.; Lambertini, M.; McNally, R.; Romano, M.; Leone, M.; Curigliano, G.; de Azambuja, E. Mortality in patients with cancer and coronavirus disease 2019: A systematic review and pooled analysis of 52 studies. Eur. J. Cancer 2020, 139, 43–50. [Google Scholar] [CrossRef]
- Vijenthira, A.; Gong, I.Y.; Fox, T.A.; Booth, S.; Cook, G.; Fattizzo, B.; Martín-Moro, F.; Razanamahery, J.; Riches, J.C.; Zwicker, J.; et al. Outcomes of patients with hematologic malignancies and COVID-19: A systematic re-view and meta-analysis of 3377 patients. Blood 2020, 136, 2881–2892. [Google Scholar] [CrossRef]
- Yang, E.A.L.; Chai, P.; Yu, J.; Fan, X. Effects of cancer on patients with COVID-19: A systematic review and meta-analysis of 63,019 participants. Cancer Biol. Med. 2021, 18, 298–307. [Google Scholar] [CrossRef]
- Lei, H.; Yang, Y.; Zhou, W.; Zhang, M.; Shen, Y.; Tao, D.; Wang, L.; Lei, Q.; Wang, Y.; Wu, Y. Higher mortality in lung cancer patients with COVID-19? A systematic review and meta-analysis. Lung Cancer 2021, 157, 60–65. [Google Scholar] [CrossRef]
- Berglund, Å.; Willén, L.; Grödeberg, L.; Skattum, L.; Hagberg, H.; Pauksens, K. The response to vaccination against influenza A(H1N1) 2009, seasonal influenza and Streptococcus pneumoniae in adult outpatients with ongoing treatment for cancer with and without rituximab. Acta Oncol. 2014, 53, 1212–1220. [Google Scholar] [CrossRef]
- Rousseau, B.; Loulergue, P.; Mir, O.; Krivine, A.; Kotti, S.; Viel, E.; Simon, T.; de Gramont, A.; Goldwasser, F.; Launay, O.; et al. Immunogenicity and safety of the influenza A H1N1v 2009 vaccine in cancer patients treated with cytotoxic chemotherapy and/or targeted therapy: The VACANCE study. Ann. Oncol. 2012, 23, 450–457. [Google Scholar] [CrossRef]
- Brydak, L.; Guzy, J.; Starzyk, J.; Machała, M.; Góźdź, S. Humoral immune response after vaccination against influenza in patients with breast cancer. Support. Care Cancer 2001, 9, 65–68. [Google Scholar] [CrossRef]
- Eliakim-Raz, N.; Vinograd, I.; Trestioreanu, A.Z.; Leibovici, L.; Paul, M. Influenza vaccines in immunosuppressed adults with cancer. Cochrane Database Syst. Rev. 2013, 2, CD008983. [Google Scholar] [CrossRef]
- Blanchette, P.S.; Chung, H.; Pritchard, K.I.; Earle, C.C.; Campitelli, M.A.; Buchan, S.A.; Schwartz, K.L.; Crowcroft, N.S.; Gubbay, J.B.; Karnauchow, T.; et al. Influenza Vaccine Effectiveness Among Patients With Cancer: A Population-Based Study Using Health Administrative and La-boratory Testing Data From Ontario, Canada. J. Clin. Oncol. 2019, 37, 2795–2804. [Google Scholar] [CrossRef]
- Nordøy, T.; Aaberge, I.S.; Husebekk, A.; Samdal, H.H.; Steinert, S.; Melby, H.; Kolstad, A. Cancer patients un-dergoing chemotherapy show adequate serological response to vaccinations against influenza virus and Streptococcus pneumoniae. Med. Oncol. 2002, 19, 71–78. [Google Scholar] [CrossRef]
- Polack, F.P.; Thomas, S.J.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Marc, G.P.; Moreira, E.D.; Zerbini, C.; et al. Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine. N. Engl. J. Med. 2020, 383, 2603–2615. [Google Scholar] [CrossRef]
- Jackson, L.A.; Anderson, E.J.; Rouphael, N.G.; Roberts, P.C.; Makhene, M.; Coler, R.N.; McCullough, M.P.; Chappell, J.D.; Denison, M.R.; Stevens, L.J.; et al. An mRNA Vaccine against SARS-CoV-2—Preliminary Report. N. Engl. J. Med. 2020, 383, 1920–1931. [Google Scholar] [CrossRef] [PubMed]
- Voysey, M.; Clemens, S.A.C.; Madhi, S.A.; Weckx, L.Y.; Folegatti, P.M.; Aley, P.K.; Angus, B.; Baillie, V.L.; Barnabas, S.L.; Bhorat, Q.E.; et al. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: An interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. Lancet 2021, 397, 99–111. [Google Scholar] [CrossRef]
- Rotondo, J.C.; Martini, F.; Maritati, M.; Mazziotta, C.; Di Mauro, G.; Lanzillotti, C.; Barp, N.; Gallerani, A.; Tognon, M.; Contini, C. SARS-CoV-2 Infection: New Molecular, Phylogenetic, and Pathogenetic Insights. Efficacy of Current Vaccines and the Potential Risk of Variants. Viruses 2021, 13, 1687. [Google Scholar] [CrossRef]
- Orchard, K.; Dignan, F.L.; Lee, J.; Pearce, R.; Desai, M.; McFarlane, E.; Parkin, A.; Shearn, P.; Snowden, J.A. The NICE COVID-19 rapid guide-line on haematopoietic stem cell transplantation: Development, implementation and impact. Br. J. Haematol. 2021, 192, 467–473. [Google Scholar] [CrossRef]
- Tzarfati, K.H.; Gutwein, O.; Apel, A.; Rahimi-Levene, N.; Sadovnik, M.; Harel, L.; Benveniste-Levkovitz, P.; Bar Chaim, A.; Koren-Michowitz, M. BNT162b2 COVID -19 vaccine is significantly less effective in patients with hematologic malignancies. Am. J. Hematol. 2021, 96, 1195–1203. [Google Scholar] [CrossRef]
- Marra, A.; Generali, D.; Zagami, P.; Cervoni, V.; Gandini, S.; Venturini, S.; Morganti, S.; Passerini, R.; Orecchia, R.; Curigliano, G. Seroconversion in patients with cancer and oncology health care workers infected by SARS-CoV-2. Ann. Oncol. 2021, 32, 113–119. [Google Scholar] [CrossRef] [PubMed]
- Solodky, M.; Galvez, C.; Russias, B.; Detourbet, P.; N’Guyen-Bonin, V.; Herr, A.-L.; Zrounba, P.; Blay, J.-Y. Lower detection rates of SARS-COV2 antibodies in cancer patients versus health care workers after symptomatic COVID-19. Ann. Oncol. 2020, 31, 1087–1088. [Google Scholar] [CrossRef]
- Massarweh, A.; Eliakim-Raz, N.; Stemmer, A.; Levy-Barda, A.; Yust-Katz, S.; Zer, A.; Benouaich-Amiel, A.; Ben-Zvi, H.; Moskovits, N.; Brenner, B.; et al. Evaluation of Seropositivity Following BNT162b2 Messenger RNA Vaccination for SARS-CoV-2 in Patients Undergoing Treatment for Cancer. JAMA Oncol. 2021, 7, 1133. [Google Scholar] [CrossRef]
- Monin, L.; Laing, A.G.; Muñoz-Ruiz, M.; McKenzie, D.R.; Barrio, I.D.M.D.; Alaguthurai, T.; Domingo-Vila, C.; Hayday, T.S.; Graham, C.; Seow, J.; et al. Safety and immunogenicity of one versus two doses of the COVID-19 vaccine BNT162b2 for patients with cancer: Interim analysis of a prospective observational study. Lancet Oncol. 2021, 22, 765–778. [Google Scholar] [CrossRef]
- Jérôme, B.; Emmanuel, C.; Zoubir, A.; Olivier, C.; Abakar, M.; Sabine, M.; Emmanuel, P.; Axel, L.; Vincent, R.; Michel, C. Impaired immunogen-icity of BNT162b2 anti-SARS-CoV-2 vaccine in patients treated for solid tumors. Ann. Oncol. 2021, 32, 1053–1055. [Google Scholar]
- Palich, R.; Veyri, M.; Vozy, A.; Marot, S.; Gligorov, J.; Benderra, M.-A.; Maingon, P.; Morand-Joubert, L.; Adjoutah, Z.; Marcelin, A.-G.; et al. High seroconversion rate but low antibody titers after two injections of BNT162b2 (Pfizer-BioNTech) vaccine in patients treated by chemotherapy for solid cancers. Ann. Oncol. 2021. [Google Scholar] [CrossRef] [PubMed]
- Goshen-Lago, T.; Waldhorn, I.; Holland, R.; Szwarcwort-Cohen, M.; Reiner-Benaim, A.; Shachor-Meyouhas, Y.; Hussein, K.; Fahoum, L.; Baruch, M.; Peer, A.; et al. Serologic Status and Toxic Effects of the SARS-CoV-2 BNT162b2 Vaccine in Patients Undergoing Treatment for Cancer. JAMA Oncol. 2021. [Google Scholar] [CrossRef]
- Addeo, A.; Shah, P.K.; Bordry, N.; Hudson, R.D.; Albracht, B.; Di Marco, M.; Kaklamani, V.; Dietrich, P.Y.; Taylor, B.S.; Simand, P.F.; et al. Immunogenicity of SARS-CoV-2 messenger RNA vaccines in patients with cancer. Cancer Cell 2021, 39, 1091–1098.e2. [Google Scholar] [CrossRef] [PubMed]
- Chamilos, G.; Lionakis, M.S.; Kontoyiannis, D.P. Are All Patients with Cancer at Heightened Risk for Severe Coronavirus Disease 2019 (COVID-19)? Clin. Infect Dis. 2021, 72, 351–356. [Google Scholar] [CrossRef]
- Sinha, S.; Kundu, C.N. Cancer and COVID-19: Why are cancer patients more susceptible to COVID-19? Med. Oncol. 2021, 38, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Garassino, M.C.; Vyas, M.; De Vries, E.G.E.; Kanesvaran, R.; Giuliani, R.; Peters, S. The ESMO Call to Ac-tion on COVID-19 vaccinations and patients with cancer: Vaccinate. Monitor. Educate. Ann. Oncol. 2021, 32, 579–581. [Google Scholar] [CrossRef] [PubMed]
- Lumley, S.F.; O’Donnell, D.; Stoesser, N.E.; Matthews, P.C.; Howarth, A.; Hatch, S.B.; Marsden, B.D.; Cox, S.; James, T.; Warren, F.; et al. Antibody Status and Incidence of SARS-CoV-2 Infection in Health Care Workers. N. Engl. J. Med. 2021, 384, 533–540. [Google Scholar] [CrossRef] [PubMed]
- Wajnberg, A.; Amanat, F.; Firpo, A.; Altman, D.R.; Bailey, M.J.; Mansour, M.; McMahon, M.; Meade, P.; Mendu, D.R.; Muellers, K.; et al. Robust neutralizing anti-bodies to SARS-CoV-2 infection persist for months. Science 2020, 370, 1227–1230. [Google Scholar] [CrossRef] [PubMed]
- Earle, K.A.; Ambrosino, D.M.; Fiore-Gartland, A.; Goldblatt, D.; Gilbert, P.B.; Siber, G.R.; Dull, P.; Plotkin, S.A. Evidence for an-tibody as a protective correlate for COVID-19 vaccines. Vaccine 2021, 39, 4423–4428. [Google Scholar] [CrossRef]
- Jin, P.; Li, J.; Pan, H.; Wu, Y.; Zhu, F. Immunological surrogate endpoints of COVID-2019 vaccines: The evi-dence we have versus the evidence we need. Signal. Transduct Target Ther. 2021, 6, 48. [Google Scholar] [CrossRef]
- Sahin, U.; Muik, A.; Derhovanessian, E.; Vogler, I.; Kranz, L.M.; Vormehr, M.; Baum, A.; Pascal, K.; Quandt, J.; Maurus, D.; et al. COVID-19 vaccine BNT162b1 elicits human antibody and TH1 T-cell responses. Nature 2020, 586, 594–599. [Google Scholar] [CrossRef]
- Giefing-Kröll, C.; Berger, P.; Lepperdinger, G.; Grubeck-Loebenstein, B. How sex and age affect immune responses, susceptibility to infections, and response to vaccination. Aging Cell 2015, 14, 309–321. [Google Scholar] [CrossRef] [PubMed]
- Gebhard, C.; Regitz-Zagrosek, V.; Neuhauser, H.K.; Morgan, R.; Klein, S.L. Impact of sex and gender on COVID-19 outcomes in Europe. Biol. Sex Differ. 2020, 11, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, S.B.; Dumanski, S.M. Sex, gender and COVID-19: A call to action. Can. J. Public Health 2020, 111, 980–983. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, S.; Pahan, K. Is COVID-19 Gender-sensitive? J. Neuroimmune Pharmacol. 2021, 16, 38–47. [Google Scholar] [CrossRef]
- Garassino, M.C.; Whisenant, J.G.; Huang, L.-C.; Trama, A.; Torri, V.; Agustoni, F.; Baena, J.; Banna, G.; Berardi, R.; Bettini, A.C.; et al. COVID-19 in patients with thoracic malignancies (TERAVOLT): First results of an international, registry-based, cohort study. Lancet Oncol. 2020, 21, 914–922. [Google Scholar] [CrossRef]
- Sopori, M.L. Effects of cigarette smoke on the immune system. Nat. Rev. Immunol. 2002, 2, 372–377. [Google Scholar] [CrossRef]
- Hernandez, C.P.; Morrow, K.; Velasco, C.; Wyczechowska, D.D.; Naura, A.S.; Rodriguez, P.C. Effects of ciga-rette smoke extract on primary activated T cells. Cell Immunol. 2013, 282, 38–43. [Google Scholar] [CrossRef] [Green Version]
- Piaggeschi, G.; Rolla, S.; Rossi, N.; Brusa, D.; Naccarati, A.; Couvreur, S.; Spector, T.D.; Roederer, M.; Mangino, M.; Cordero, F.; et al. Immune Trait Shifts in Associa-tion With Tobacco Smoking: A Study in Healthy Women. Front. Immunol. 2021, 12, 637974. [Google Scholar] [CrossRef] [PubMed]
- Nouri-Shirazi, M.; Guinet, E. Exposure to Nicotine Adversely Affects the Dendritic Cell System and Compromises Host Response to Vaccination. J. Immunol. 2012, 188, 2359–2370. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Watanabe, M.; Balena, A.; Tuccinardi, D.; Tozzi, R.; Risi, R.; Masi, D.; Caputi, A.; Rossetti, R.; Spoltore, M.E.; Filippi, V.; et al. Central obesity, smoking habit, and hypertension are associated with lower antibody titres in response to COVID-19 mRNA vaccine. Diabetes/Metabolism Res. Rev. 2021, e3465. [Google Scholar] [CrossRef] [PubMed]
- Dobaño, C.; Ramírez-Morros, A.; Alonso, S.; Vidal-Alaball, J.; Ruiz-Olalla, G.; Vidal, M.; Rubio, R.; Cascant, E.; Parras, D.; Melero, N.R.; et al. Persistence and baseline determinants of seropositivity and reinfection rates in health care workers up to 12.5 months after COVID-19. BMC Med. 2021, 19, 1–6. [Google Scholar] [CrossRef]
- Jonsdottir, H.R.; Bielecki, M.; Siegrist, D.; Buehrer, T.W.; Zust, R.; Deuel, J.W. Titers of Neutralizing Antibodies against SARS-CoV-2 Are Independent of Symptoms of Non-Severe COVID-19 in Young Adults. Viruses 2021, 13, 284. [Google Scholar] [CrossRef] [PubMed]
- Schaffner, A.; Risch, L.; Aeschbacher, S.; Risch, C.; Weber, M.C.; Thiel, S.L.; Jüngert, K.; Pichler, M.; Grossmann, K.; Wohlwend, N.; et al. Characterization of a Pan-Immunoglobulin Assay Quantifying Antibodies Directed against the Receptor Binding Domain of the SARS-CoV-2 S1-Subunit of the Spike Protein: A Population-Based Study. J. Clin. Med. 2020, 9, 3989. [Google Scholar] [CrossRef]
- Bonelli, F.; Blocki, F.A.; Bunnell, T.; Chu, E.; De La, O.A.; Grenache, D.G.; Marzucchi, G.; Montomoli, E.; Okoye, L.; Pallavicini, L.; et al. Evaluation of the automated LIAISON((R)) SARS-CoV-2 TrimericS IgG assay for the detection of circulating antibodies. Clin. Chem. Lab. Med. 2021, 59, 1463–1467. [Google Scholar] [CrossRef]

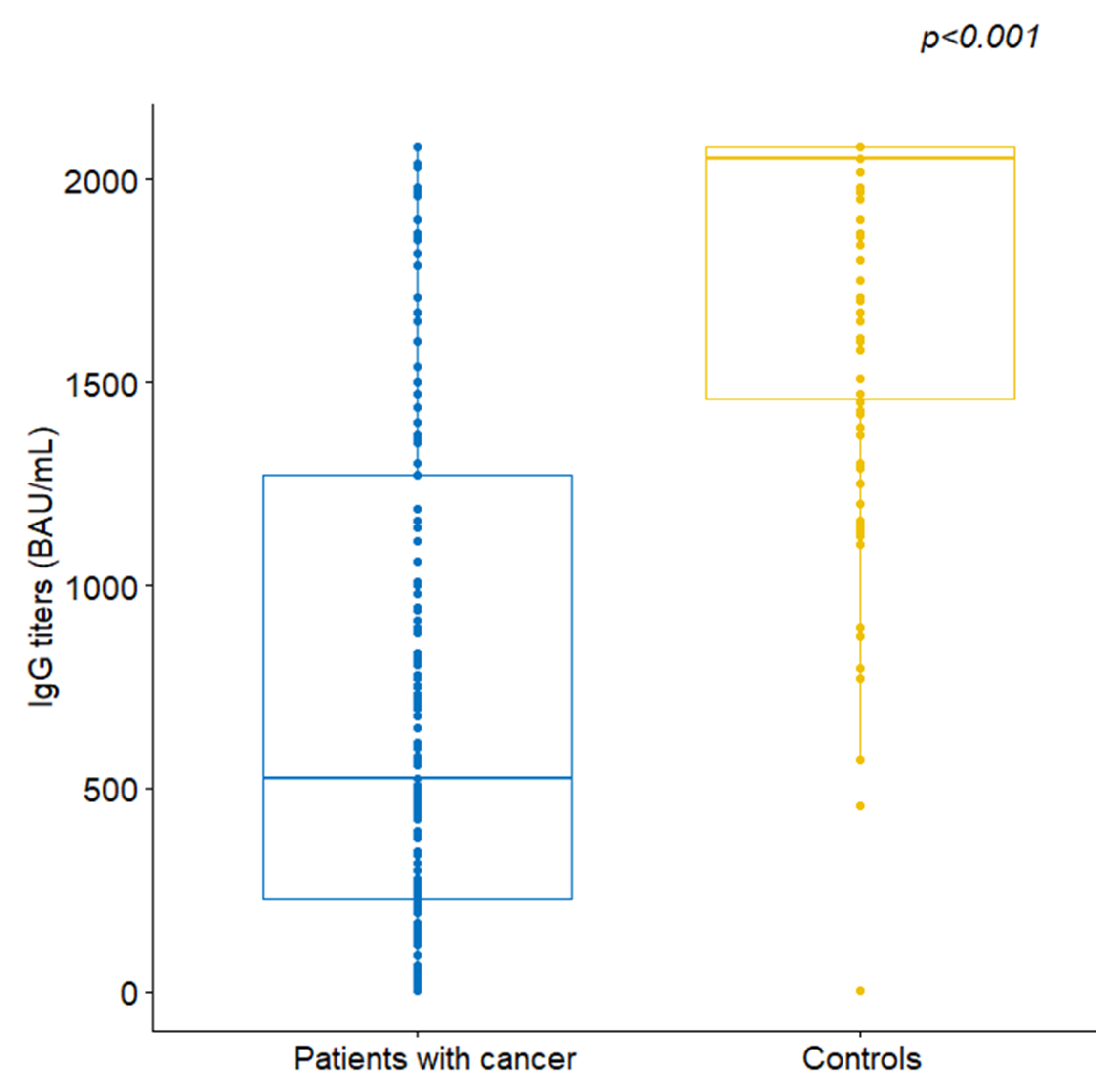
| Parameter | Total (n = 288) | Patients (n = 189) | Controls (n = 99) |
|---|---|---|---|
| BMI, Median (min, max) | 25.2 (17.6, 51.3) | 24.9 (17.6, 51.3) | 25.4 (17.9, 45.7) |
| N of comorbidities, Median (min, max) | 0.00 (0.00, 4.0) | 1.00 (0.00, 4.0) | 0.00 (0.00, 2.0) |
| n (%) | n (%) | n (%) | |
| Gender | |||
| Male | 124 (43.1) | 87 (46.0) | 37 (37.4) |
| Female | 164 (56.9) | 102 (54.0) | 62 (62.6) |
| Age | |||
| 18–29 | 5 (1.7) | 1 (0.53) | 4 (4.0) |
| 30–39 | 28 (9.7) | 3 (1.6) | 25 (25.3) |
| 40–49 | 57 (19.8) | 25 (13.2) | 32 (32.3) |
| 50–59 | 64 (22.2) | 39 (20.6) | 25 (25.3) |
| 60–69 | 60 (20.8) | 51 (27.0) | 9 (9.1) |
| 70–79 | 56 (19.4) | 52 (27.5) | 4 (4.0) |
| 80–85 | 15 (5.2) | 15 (7.9) | 0 (0.0) |
| >85 | 3 (1.0) | 3 (1.6) | 0 (0.0) |
| BMI | |||
| Underweight | 7 (2.4) | 5 (2.6) | 2 (2.0) |
| Normal | 134 (46.5) | 91 (48.1) | 43 (43.4) |
| Obese | 53 (18.4) | 38 (20.1) | 15 (15.2) |
| Overweight | 94 (32.6) | 55 (29.1) | 39 (39.4) |
| Smoking Status | |||
| Never smoker | 124 (43.1) | 82 (43.4) | 42 (42.4) |
| Current smoker | 88 (30.6) | 50 (26.5) | 38 (38.4) |
| Previous smoker—stopped within the last 10 years | 71 (24.7) | 53 (28.0) | 18 (18.2) |
| Not Reported | 5 (1.7) | 4 (2.1) | 1 (1.0) |
| Comorbidities | |||
| No | 168 (58.3) | 91 (48.1) | 77 (77.8) |
| Yes | 120 (41.7) | 98 (51.9) | 22 (22.2) |
| Vaccine administered | |||
| BNT162b2 (Pfizer) | 262 (91.0) | 163 (86.2) | 99 (100.0) |
| mRNA-1273 (Moderna) | 19 (6.6) | 19 (10.1) | 0 (0.0) |
| AZD1222 (Astra Zeneca) | 7 (2.4) | 7 (3.7) | 0 (0.0) |
| Autoimmune disease | |||
| No | 266 (92.4) | 184 (97.4) | 82 (82.8) |
| Active autoimmune disease | 17 (5.9) | 3 (1.6) | 14 (14.1) |
| Inactive autoimmune disease | 4 (1.4) | 1 (0.53) | 3 (3.0) |
| Not Reported | 1 (0.35) | 1 (0.53) | 0 (0.0) |
| Cancer type (primary cancer diagnosis) | |||
| Breast cancer | 51 (27.0) | 51 (27.0) | ---- |
| NSCLC | 37 (19.6) | 37 (19.6) | ---- |
| SCLC | 20 (10.6) | 20 (10.6) | ---- |
| Mesothelioma | 1 (0.53) | 1 (0.53) | ---- |
| Head and Neck cancer | 1 (0.53) | 1 (0.53) | ---- |
| Stomach cancer | 6 (3.2) | 6 (3.2) | ---- |
| Pancreatic cancer | 11 (5.8) | 11 (5.8) | ---- |
| Colorectal cancer | 27 (14.3) | 27 (14.3) | ---- |
| Ovarian cancer | 11 (5.8) | 11 (5.8) | ---- |
| Other Gynecological cancer | 1 (0.53) | 1 (0.53) | ---- |
| Bladder cancer | 4 (2.1) | 4 (2.1) | ---- |
| Prostate cancer | 4 (2.1) | 4 (2.1) | ---- |
| Kidney cancer | 4 (2.1) | 4 (2.1) | ---- |
| Testicular cancer | 1 (0.53) | 1 (0.53) | ---- |
| Melanoma | 3 (1.6) | 3 (1.6) | ---- |
| Other * | 7 (3.7) | 7 (3.7) | ---- |
| Performance Status | |||
| 0 | 157 (83.1) | 157 (83.1) | ---- |
| 1 | 32 (16.9) | 32 (16.9) | ---- |
| Concomitant Corticosteroid use | |||
| No | 179 (94.7) | 179 (94.7) | ---- |
| Yes | 10 (5.3) | 10 (5.3) | ---- |
| Active antineoplastic treatment | |||
| No | 27 (14.3) | 27 (14.3) | ---- |
| Yes | 162 (85.7) | 162 (85.7) | ---- |
| Type of antineoplastic treatment | |||
| Chemotherapy | 89 (54.9) | 89 (54.9) | ---- |
| Immunotherapy only | 32 (19.8) | 32 (19.8) | ---- |
| Chemo-immunotherapy combination | 12 (7.4) | 12 (7.4) | ---- |
| Targeted agent, TKI only | 4 (2.5) | 4 (2.5) | ---- |
| Other biologic therapy only | 21 (13.0) | 21 (13.0) | ---- |
| Endocrine therapy only | 2 (1.2) | 2 (1.2) | ---- |
| Radiotherapy only | 2 (1.2) | 2 (1.2) | ---- |
| Cancer status at vaccination | |||
| Primary recently operated | 45 (23.8) | 45 (23.8) | ---- |
| Recurrent | 49 (25.9) | 49 (25.9) | ---- |
| Metastatic | 89 (47.1) | 89 (47.1) | ---- |
| Other | 6 (3.2) | 6 (3.2) | ---- |
| Patients (n = 189) | Controls (n = 99) | |||||
|---|---|---|---|---|---|---|
| Parameter | n | IgG Median (Min, Max) | p-Value | n | IgG Median (Min, Max) | |
| Cancer Type (Primary Diagnosis) | 0.041 * | |||||
| Breast cancer | 51 | 698 (7.15–2080) | ||||
| Lung cancer NSCLC | 37 | 580 (10.50–2080) | ||||
| Lung cancer SCLC | 20 | 343.5 (18–2080) | ||||
| Mesothelioma | 1 | 2080 (----) | ||||
| Head and Neck cancer | 1 | 735 (----) | ||||
| Stomach cancer | 6 | 340.50 (18.30–2080) | ||||
| Pancreatic cancer | 11 | 238 (8.39–2080) | ||||
| Colorectal cancer | 27 | 491.50 (35.70–2080) | ||||
| Ovarian cancer | 11 | 939 (25.10–2080) | ||||
| Other Gynecological cancer | 1 | 509 (----) | ||||
| Bladder cancer | 4 | 447 (23.6–509) | ||||
| Prostate cancer | 4 | 671.5 (4.81–883) | ||||
| Kidney cancer | 4 | 330 (66.3–897) | ||||
| Testicular cancer | 1 | 1980 (----) | ||||
| Melanoma | 3 | 482 (164.00–730) | ||||
| Other | 7 | 476 (4.81–2080) | ||||
| Cancer status at vaccination | 0.27 | |||||
| Primary recently operated | 45 | 650 (4.81–2080) | ||||
| Recurrent | 49 | 556 (4.81–2080) | ||||
| Metastatic | 89 | 482 (8.07–2080) | ||||
| Other | 6 | 729.50 (193.00–1870) | ||||
| Active antineoplastic treatment | 0.28 | |||||
| No | 27 | 696.00 (18–2080) | ||||
| Yes | 162 | 492.50 (4.81–2080) | ||||
| Type of antineoplastic treatment | ---- | |||||
| Chemotherapy | 89 | 478 (4.81–2080) | ||||
| Immunotherapy only | 32 | 469 (25.10–2080) | ||||
| Chemo-immunotherapy combination | 12 | 536.50 (20.90–1500) | ||||
| Targeted agent, TKI only | 4 | 378.50 (168.00–2080) | ||||
| Other biologic therapy only | 21 | 698 (4.81–2080) | ||||
| Endocrine therapy only | 2 | 1425.50 (771–2080) | ||||
| Radiotherapy only | 2 | 1185 (1000–1370) | ||||
| Concomitant corticosteroid use | 0.83 | |||||
| No | 179 | 509 (4.81–2080) | ||||
| Yes | 10 | 817 (4.81–2080) | ||||
| PS at vaccination | 0.029 | |||||
| 0 | 157 | 560 (4.81–2080) | ||||
| 1 | 32 | 253.5 (4.81–2080) | ||||
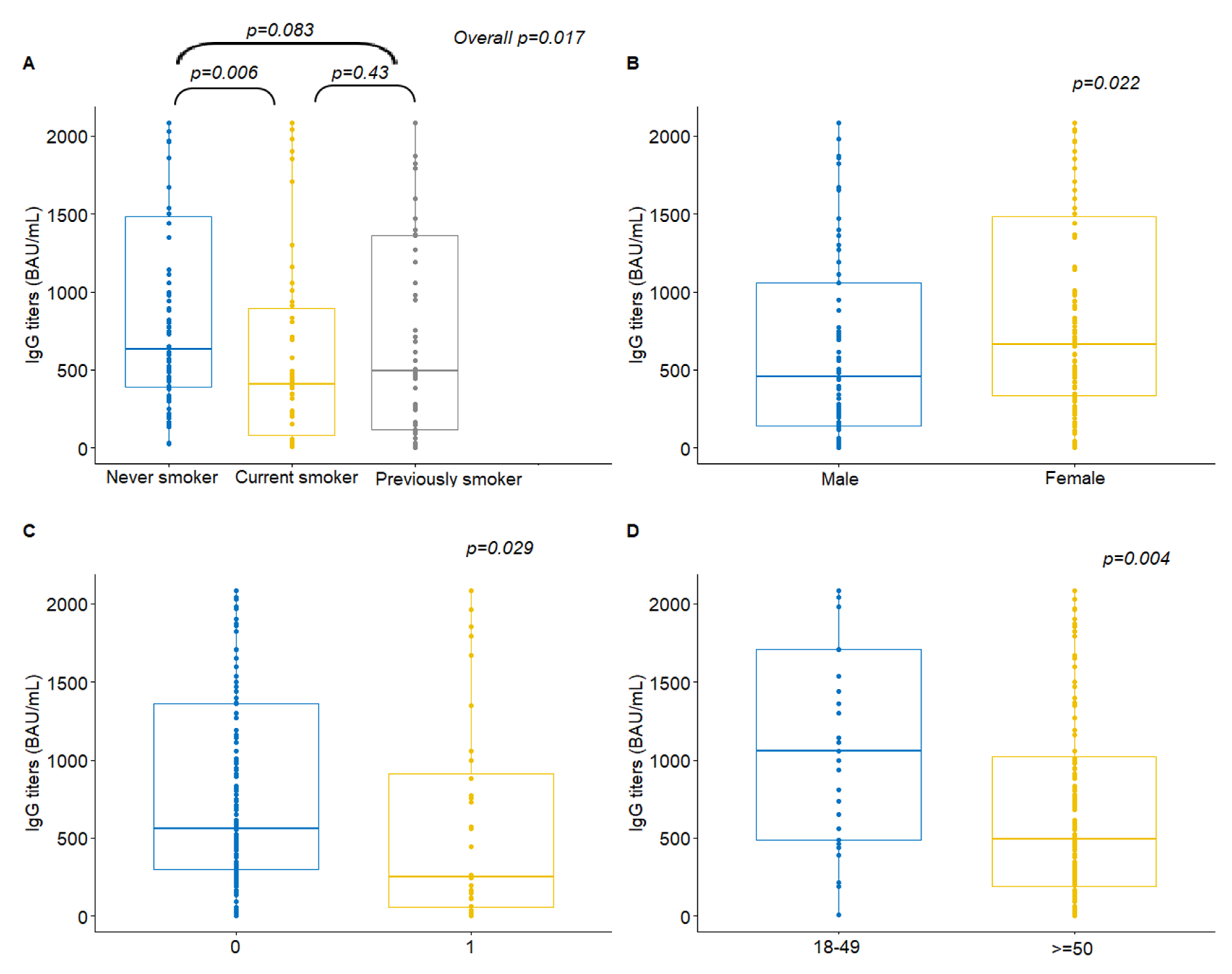
| Smoking status | 0.017 | 0.81 | ||||
| Never smoker | 82 | 632 (25.00–2080) | 42 | 1885 (4.81-2080) | ||
| Current smoker | 50 | 409.50 (8.07–2080) | 38 | 2065 (770-2080) | ||
| Previous smoker—stopped within the last 10 years | 53 | 491 (4.81–2080) | 18 | 1970 (4.81–2080) | ||
| Gender | 0.022 | 0.30 | ||||
| Male | 87 | 456 (4.81–2080) | 37 | 1800 (4.81–2080) | ||
| Female | 102 | 665 (4.81–2080) | 62 | 2065 (770–2080) | ||
| Age | ---- | ---- | ||||
| 18–29 | 1 | 1110 (----) | 4 | 2025 (1700–2080) | ||
| 30–39 | 3 | 563 (215–2080) | 25 | 2080 (770–2080) | ||
| 40–49 | 25 | 1060 (7.15–2080) | 32 | 1905 (1100–2080) | ||
| 50–59 | 39 | 604 (20.90–2080) | 25 | 2080 (4.81–2080) | ||
| 60–69 | 51 | 452 (4.81–2080) | 9 | 1370 (4.81–2080) | ||
| 70–79 | 52 | 491.5 (4.81–2080) | 4 | 1325 (4.81–2080) | ||
| 80–85 | 15 | 347 (8.07–2080) | 0 | ---- | ||
| >85 | 3 | 730 (509–771) | 0 | ---- | ||
| 18–49 | 29 | 1060 (7.15–2080) | 0.004 | 61 | 2080 (770–2080) | 0.26 |
| ≥50 | 160 | 491.5 (4.81–2080) | 38 | 1885 (4.81–2080) | ||
| Comorbidities | 0.051 | 0.72 | ||||
| No | 91 | 650 (4.81–2080) | 77 | 2020 (457–2080) | ||
| Yes | 98 | 491.5 (4.81–2080) | 22 | 2080 (4.81–2080) | ||
| Hypertension | 0.76 | 0.077 | ||||
| No | 120 | 543 (4.81–2080) | 88 | 2080 (4.81–2080) | ||
| Yes | 69 | 509 (8.39–2080) | 11 | 1510 (4.81–2080) | ||
| BMI | 0.80 | ---- | ||||
| Underweight | 5 | 680 (10.5–1500) | 2 | 1835 (1700–1970) | ||
| Normal weight | 91 | 509 (7.15–2080) | 43 | 1950 (570–2080) | ||
| Obese | 38 | 606 (4.81–2080) | 15 | 2080 (4.81–2080) | ||
| Overweight | 55 | 509 (4.81–2080) | 39 | 1860 (4.81–2080) | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Linardou, H.; Spanakis, N.; Koliou, G.-A.; Christopoulou, A.; Karageorgopoulou, S.; Alevra, N.; Vagionas, A.; Tsoukalas, N.; Sgourou, S.; Fountzilas, E.; et al. Responses to SARS-CoV-2 Vaccination in Patients with Cancer (ReCOVer Study): A Prospective Cohort Study of the Hellenic Cooperative Oncology Group. Cancers 2021, 13, 4621. https://doi.org/10.3390/cancers13184621
Linardou H, Spanakis N, Koliou G-A, Christopoulou A, Karageorgopoulou S, Alevra N, Vagionas A, Tsoukalas N, Sgourou S, Fountzilas E, et al. Responses to SARS-CoV-2 Vaccination in Patients with Cancer (ReCOVer Study): A Prospective Cohort Study of the Hellenic Cooperative Oncology Group. Cancers. 2021; 13(18):4621. https://doi.org/10.3390/cancers13184621
Chicago/Turabian StyleLinardou, Helena, Nikolaos Spanakis, Georgia-Angeliki Koliou, Athina Christopoulou, Sofia Karageorgopoulou, Nephely Alevra, Anastasios Vagionas, Nikolaos Tsoukalas, Stavroula Sgourou, Elena Fountzilas, and et al. 2021. "Responses to SARS-CoV-2 Vaccination in Patients with Cancer (ReCOVer Study): A Prospective Cohort Study of the Hellenic Cooperative Oncology Group" Cancers 13, no. 18: 4621. https://doi.org/10.3390/cancers13184621
APA StyleLinardou, H., Spanakis, N., Koliou, G.-A., Christopoulou, A., Karageorgopoulou, S., Alevra, N., Vagionas, A., Tsoukalas, N., Sgourou, S., Fountzilas, E., Sgouros, J., Razis, E., Chatzokou, D., Lampaki, S., Res, E., Saridaki, Z., Mountzios, G., Saroglou, G., & Fountzilas, G. (2021). Responses to SARS-CoV-2 Vaccination in Patients with Cancer (ReCOVer Study): A Prospective Cohort Study of the Hellenic Cooperative Oncology Group. Cancers, 13(18), 4621. https://doi.org/10.3390/cancers13184621










