Cannabis Use among Cancer Survivors amid the COVID-19 Pandemic: Results from the COVID-19 Cannabis Health Study
Abstract
:Simple Summary
Abstract
1. Introduction
2. Materials and Methods
2.1. COVID-19 Cannabis Health Study
2.2. Measures
2.3. Data Analysis
3. Results
3.1. Demographics
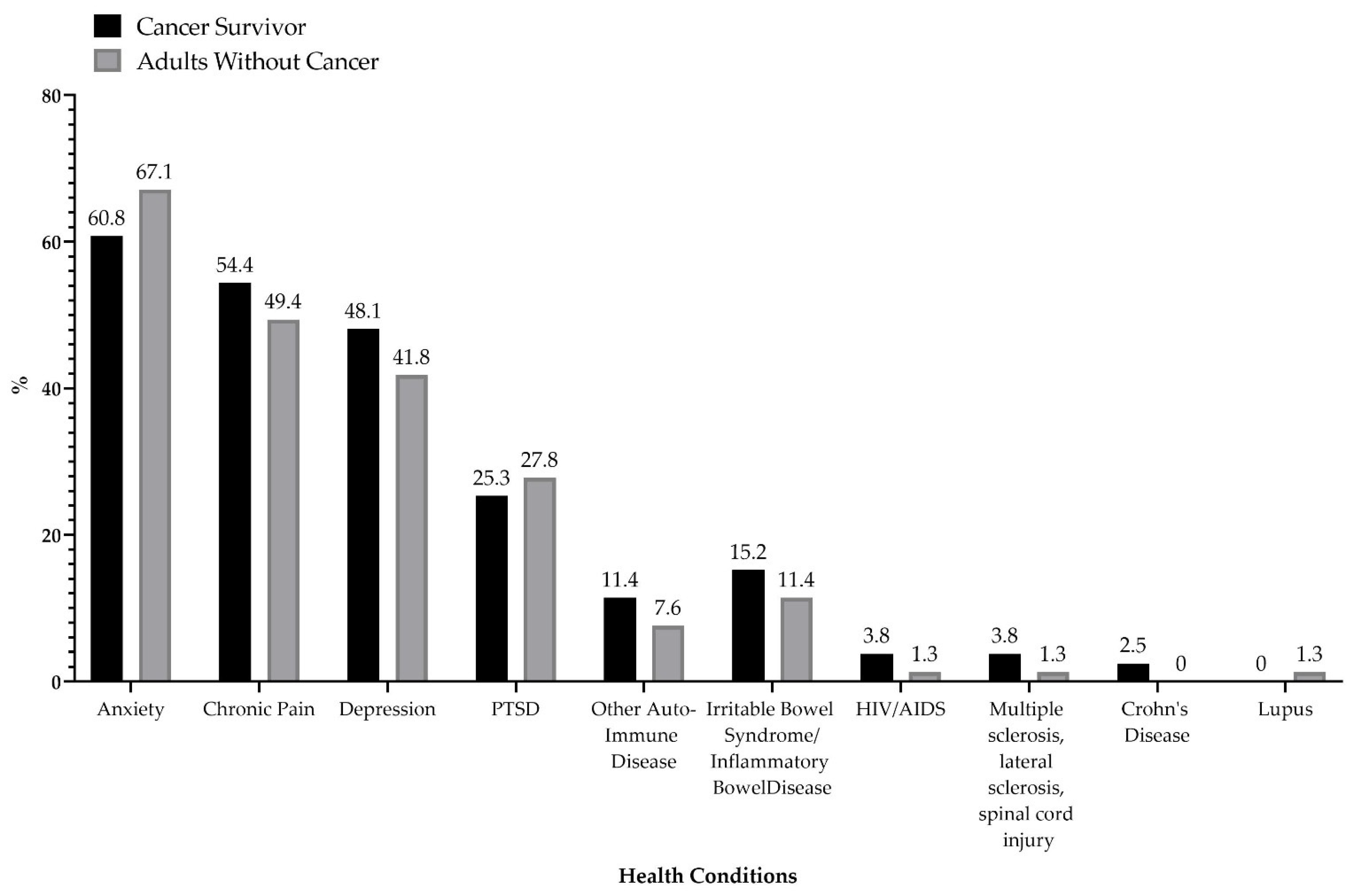
3.2. Health Conditions and Symptoms Managed by Cannabis Users
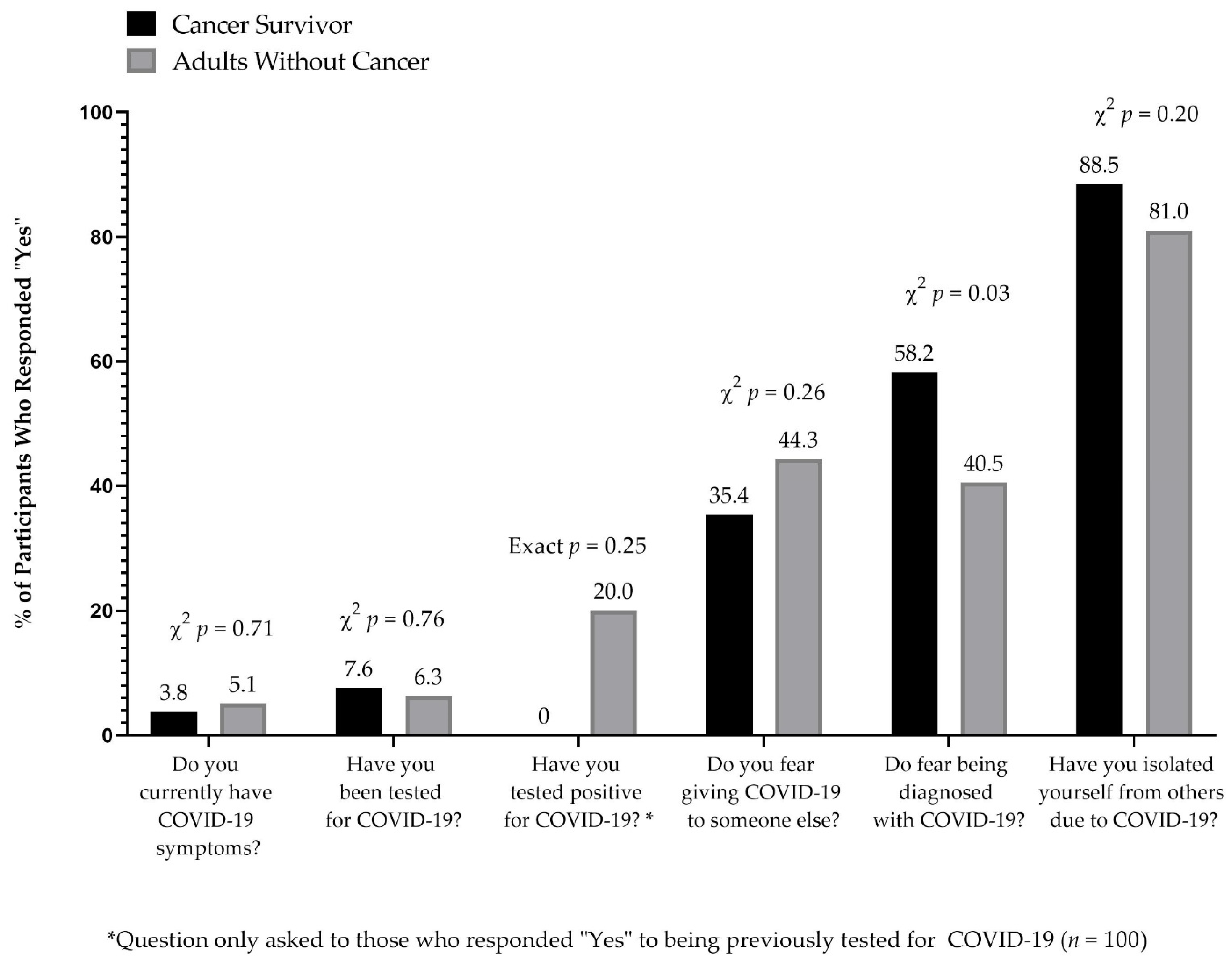
3.3. Cannabis Use Behaviors and COVID-19-Related Concerns
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Sohrabi, C.; Alsafi, Z.; O’Neill, N.; Khan, M.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, R. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int. J. Surg. 2020, 76, 71–76. [Google Scholar] [CrossRef] [PubMed]
- Killerby, M.E.; Link-Gelles, R.; Haight, S.C.; Schrodt, C.A.; England, L.; Gomes, D.J.; Shamout, M.; Pettrone, K.; O’Laughlin, K.; Kimball, A.; et al. CDC COVID-19 Response Clinical Team Characteristics Associated with Hospitalization Among Patients with COVID-19—Metropolitan Atlanta, Georgia, March–April 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 790–794. [Google Scholar] [CrossRef]
- Azcarate, P.M.; Zhang, A.J.; Keyhani, S.; Steigerwald, S.; Ishida, J.H.; Cohen, B.E. Medical reasons for marijuana use, forms of use, and patient perception of physician attitudes among the US population. J. Gen. Intern. Med. 2020, 35, 1979–1986. [Google Scholar] [CrossRef]
- Islam, J.Y.; Camacho-Rivera, M.; Vidot, D.C. Examining COVID-19 Preventive Behaviors among Cancer Survivors in the United States: An Analysis of the COVID-19 Impact Survey. Cancer Epidemiol. Biomarkers Prev. 2020, 29, 2583–2590. [Google Scholar] [CrossRef] [PubMed]
- Nekhlyudov, L.; Duijts, S.; Hudson, S.V.; Jones, J.M.; Keogh, J.; Love, B.; Lustberg, M.; Smith, K.C.; Tevaarwerk, A.; Yu, X.; et al. Addressing the needs of cancer survivors during the COVID-19 pandemic. J. Cancer Surviv. 2020, 14, 601–606. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kutikov, A.; Weinberg, D.S.; Edelman, M.J.; Horwitz, E.M.; Uzzo, R.G.; Fisher, R.I. A War on Two Fronts: Cancer Care in the Time of COVID-19. Ann. Intern. Med. 2020, 172, 756–758. [Google Scholar] [CrossRef] [Green Version]
- Camacho-Rivera, M.; Islam, J.Y.; Vidot, D.C. Associations between Chronic Health Conditions and COVID-19 Preventive Behaviors Among a Nationally Representative Sample of U.S. Adults: An Analysis of the COVID Impact Survey. Health Equity 2020, 4, 336–344. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Duan, Z.; Ma, Z.; Mao, Y.; Li, X.; Wilson, A.; Qin, H.; Ou, J.; Peng, K.; Zhou, F.; et al. Epidemiology of mental health problems among patients with cancer during COVID-19 pandemic. Transl. Psychiatry 2020, 10, 263. [Google Scholar] [CrossRef]
- Solomou, I.; Constantinidou, F. Prevalence and Predictors of Anxiety and Depression Symptoms during the COVID-19 Pandemic and Compliance with Precautionary Measures: Age and Sex Matter. Int. J. Environ. Res. Public Health 2020, 17, 4924. [Google Scholar] [CrossRef] [PubMed]
- Twenge, J.M.; Joiner, T.E.U.S. Census Bureau-assessed prevalence of anxiety and depressive symptoms in 2019 and during the 2020 COVID-19 pandemic. Depress. Anxiety 2020, 37, 954–956. [Google Scholar] [CrossRef]
- Vidot, D.C.; Islam, J.Y.; Camacho-Rivera, M.; Harrell, M.B.; Rao, D.R.; Chavez, J.V.; Ochoa, L.G.; Hlaing, W.M.; Weiner, M.; Messiah, S.E. The COVID-19 cannabis health study: Results from an epidemiologic assessment of adults who use cannabis for medicinal reasons in the United States. J. Addict. Dis. 2021, 39, 26–36. [Google Scholar] [CrossRef] [PubMed]
- National Conference of State Legislatures State Medical Marijuana Laws. Available online: https://www.ncsl.org/research/health/state-medical-marijuana-laws.aspx (accessed on 30 June 2021).
- National Academies of Sciences, Engineering, and Medicine; Board on Population Health and Public Health Practice; Health and Medicine Division. Committee on the Health Effects of Marijuana: An Evidence Review and Research Agenda. The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research; National Academies Press: Washington, DC, USA, 2017. [Google Scholar]
- Dariš, B.; Tancer Verboten, M.; Knez, Ž.; Ferk, P. Cannabinoids in cancer treatment: Therapeutic potential and legislation. Bosn. J. Basic Med. Sci. 2019, 19, 14–23. [Google Scholar] [CrossRef] [PubMed]
- Pergam, S.A.; Woodfield, M.C.; Lee, C.M.; Cheng, G.-S.; Baker, K.K.; Marquis, S.R.; Fann, J.R. Cannabis use among patients at a comprehensive cancer center in a state with legalized medicinal and recreational use. Cancer 2017, 123, 4488–4497. [Google Scholar] [CrossRef] [Green Version]
- Hardy, J.; Haywood, A.; Gogna, G.; Martin, J.; Yates, P.; Greer, R.; Good, P. Oral medicinal cannabinoids to relieve symptom burden in the palliative care of patients with advanced cancer: A double-blind, placebo-controlled, randomised clinical trial of efficacy and safety of 1:1 delta-9-tetrahydrocannabinol (THC) and cannabidiol (CBD). Trials 2020, 21, 611. [Google Scholar] [CrossRef]
- Likar, R.; Köstenberger, M.; Nahler, G. Cannabidiol in cancer treatment. Schmerz 2020, 34, 117–122. [Google Scholar] [CrossRef]
- Kleckner, A.S.; Kleckner, I.R.; Kamen, C.S.; Tejani, M.A.; Janelsins, M.C.; Morrow, G.R.; Peppone, L.J. Opportunities for cannabis in supportive care in cancer. Ther. Adv. Med. Oncol. 2019, 11, 1758835919866362. [Google Scholar] [CrossRef] [Green Version]
- Aviram, J.; Lewitus, G.M.; Vysotski, Y.; Uribayev, A.; Procaccia, S.; Cohen, I.; Leibovici, A.; Abo-Amna, M.; Akria, L.; Goncharov, D.; et al. Short-Term Medical Cannabis Treatment Regimens Produced Beneficial Effects among Palliative Cancer Patients. Pharmaceuticals 2020, 13, 435. [Google Scholar] [CrossRef]
- COVID-19 Cannabis Health Questionnaire (CCHQ). Available online: https://elcentro.sonhs.miami.edu/research/measures-library/cchq/index.html (accessed on 14 November 2020).
- Pratt, M.; Stevens, A.; Thuku, M.; Butler, C.; Skidmore, B.; Wieland, L.S.; Clemons, M.; Kanji, S.; Hutton, B. Benefits and harms of medical cannabis: A scoping review of systematic reviews. Syst. Rev. 2019, 8, 320. [Google Scholar] [CrossRef] [Green Version]
- Black, N.; Stockings, E.; Campbell, G.; Tran, L.T.; Zagic, D.; Hall, W.D.; Farrell, M.; Degenhardt, L. Cannabinoids for the treatment of mental disorders and symptoms of mental disorders: A systematic review and meta-analysis. Lancet Psychiatry 2019, 6, 995–1010. [Google Scholar] [CrossRef]
- Häuser, W.; Welsch, P.; Klose, P.; Radbruch, L.; Fitzcharles, M.-A. Efficacy, tolerability and safety of cannabis-based medicines for cancer pain: A systematic review with meta-analysis of randomised controlled trials. Schmerz 2019, 33, 424–436. [Google Scholar] [CrossRef] [PubMed]
- McTaggart-Cowan, H.; Bentley, C.; Raymakers, A.; Metcalfe, R.; Hawley, P.; Peacock, S. Understanding cancer survivors’ reasons to medicate with cannabis: A qualitative study based on the theory of planned behavior. Cancer Med. 2021, 10, 396–404. [Google Scholar] [CrossRef]
- Donovan, K.A.; Portman, D.G. Effect of COVID-19 Pandemic on Cannabis Use in Cancer Patients. Am. J. Hosp. Palliat. Care 2021, 38, 850–853. [Google Scholar] [CrossRef]
- Braun, I.M.; Nayak, M.M.; Revette, A.; Wright, A.A.; Chai, P.R.; Yusufov, M.; Pirl, W.F.; Tulsky, J.A. Cancer patients’ experiences with medicinal cannabis-related care. Cancer 2020, 127, 67–73. [Google Scholar] [CrossRef]
- Zhou, E.S.; Nayak, M.M.; Chai, P.R.; Braun, I.M. Cancer patient’s attitudes of using medicinal cannabis for sleep. J. Psychosoc. Oncol. 2021, 1–7. [Google Scholar] [CrossRef]
- Birdsall, S.M.; Birdsall, T.C.; Tims, L.A. The use of medical marijuana in cancer. Curr. Oncol. Rep. 2016, 18, 40. [Google Scholar] [CrossRef]
- Howie, L.; Peppercorn, J. Early palliative care in cancer treatment: Rationale, evidence and clinical implications. Ther. Adv. Med. Oncol. 2013, 5, 318–323. [Google Scholar] [CrossRef] [Green Version]
- Cyr, C.; Arboleda, M.F.; Aggarwal, S.K.; Balneaves, L.G.; Daeninck, P.; Néron, A.; Prosk, E.; Vigano, A. Cannabis in palliative care: Current challenges and practical recommendations. Ann. Palliat. Med. 2018, 7, 463–477. [Google Scholar] [CrossRef] [PubMed]
- Niedzwiedz, C.L.; Knifton, L.; Robb, K.A.; Katikireddi, S.V.; Smith, D.J. Depression and anxiety among people living with and beyond cancer: A growing clinical and research priority. BMC Cancer 2019, 19, 943. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Campos, A.C.; Ortega, Z.; Palazuelos, J.; Fogaça, M.V.; Aguiar, D.C.; Díaz-Alonso, J.; Ortega-Gutiérrez, S.; Vázquez-Villa, H.; Moreira, F.A.; Guzmán, M.; et al. The anxiolytic effect of cannabidiol on chronically stressed mice depends on hippocampal neurogenesis: Involvement of the endocannabinoid system. Int. J. Neuropsychopharmacol. 2013, 16, 1407–1419. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fogaça, M.V.; Campos, A.C.; Coelho, L.D.; Duman, R.S.; Guimarães, F.S. The anxiolytic effects of cannabidiol in chronically stressed mice are mediated by the endocannabinoid system: Role of neurogenesis and dendritic remodeling. Neuropharmacology 2018, 135, 22–33. [Google Scholar] [CrossRef] [PubMed]
- Yang, K.-H.; Galadari, S.; Isaev, D.; Petroianu, G.; Shippenberg, T.S.; Oz, M. The nonpsychoactive cannabinoid cannabidiol inhibits 5-hydroxytryptamine3A receptor-mediated currents in Xenopus laevis oocytes. J. Pharmacol. Exp. Ther. 2010, 333, 547–554. [Google Scholar] [CrossRef] [Green Version]
- Islam, J.Y.; Vidot, D.C.; Camacho-Rivera, M. Evaluating Mental Health-Related Symptoms Among Cancer Survivors During the COVID-19 Pandemic: An Analysis of the COVID Impact Survey. JCO Oncol. Pract. 2021, OP2000752. [Google Scholar] [CrossRef]
- Rahman, M.A.; Hoque, N.; Alif, S.M.; Salehin, M.; Islam, S.M.S.; Banik, B.; Sharif, A.; Nazim, N.B.; Sultana, F.; Cross, W. Factors associated with psychological distress, fear and coping strategies during the COVID-19 pandemic in Australia. Global Health 2020, 16, 95. [Google Scholar] [CrossRef] [PubMed]
- Parlapani, E.; Holeva, V.; Voitsidis, P.; Blekas, A.; Gliatas, I.; Porfyri, G.N.; Golemis, A.; Papadopoulou, K.; Dimitriadou, A.; Chatzigeorgiou, A.F.; et al. Psychological and Behavioral Responses to the COVID-19 Pandemic in Greece. Front. Psychiatry 2020, 11, 821. [Google Scholar] [CrossRef] [PubMed]
- Richardson, S.; Hirsch, J.S.; Narasimhan, M.; Crawford, J.M.; McGinn, T.; Davidson, K.W.; Barnaby, D.P.; Becker, L.B.; Chelico, J.D.; Cohen, S.L.; et al. Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area. JAMA 2020, 323, 2052–2059. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.; Xiao, W.; Shi, L.; Wang, Y.; Yang, H. Is cancer an independent risk factor for fatal outcomes of coronavirus disease 2019 patients? Arch. Med. Res. 2021, 2670. [Google Scholar] [CrossRef]
- Beckman, M.F.; Mougeot, F.B.; Mougeot, J.-L.C. Comorbidities and Susceptibility to COVID-19: A Generalized Gene Set Data Mining Approach. J. Clin. Med. 2021, 10, 1666. [Google Scholar] [CrossRef]
- Kuderer, N.M.; Choueiri, T.K.; Shah, D.P.; Shyr, Y.; Rubinstein, S.M.; Rivera, D.R.; Shete, S.; Hsu, C.-Y.; Desai, A.; de Lima Lopes, G.; et al. COVID-19 and Cancer Consortium Clinical impact of COVID-19 on patients with cancer (CCC19): A cohort study. Lancet 2020, 395, 1907–1918. [Google Scholar] [CrossRef]
- Yang, F.; Shi, S.; Zhu, J.; Shi, J.; Dai, K.; Chen, X. Clinbical characteristics and outcomes of cancer patients with COVID-19. J. Med. Virol. 2020, 92, 2067–2073. [Google Scholar] [CrossRef]
- Mehta, V.; Goel, S.; Kabarriti, R.; Cole, D.; Goldfinger, M.; Acuna-Villaorduna, A.; Pradhan, K.; Thota, R.; Reissman, S.; Sparano, J.A.; et al. Case Fatality Rate of Cancer Patients with COVID-19 in a New York Hospital System. Cancer Discov. 2020, 10, 935–941. [Google Scholar] [CrossRef]
- Frey, M.K.; Chapman-Davis, E.; Glynn, S.M.; Lin, J.; Ellis, A.E.; Tomita, S.; Fowlkes, R.K.; Thomas, C.; Christos, P.J.; Cantillo, E.; et al. Adapting and avoiding coping strategies for women with ovarian cancer during the COVID-19 pandemic. Gynecol. Oncol. 2021, 160, 492–498. [Google Scholar] [CrossRef] [PubMed]
- Galica, J.; Liu, Z.; Kain, D.; Merchant, S.; Booth, C.; Koven, R.; Brundage, M.; Haase, K.R. Coping during COVID-19: A mixed methods study of older cancer survivors. Support. Care Cancer 2021, 29, 3389–3398. [Google Scholar] [CrossRef] [PubMed]
- Purcell, J.B.; Orihuela, C.A.; Elliott, M.N.; Tortolero Emery, S.; Schuster, M.A.; Mrug, S. Examining Sex and Racial/Ethnic Differences in Co-use of Alcohol, Cannabis, and Cigarettes in a Community Sample of Adolescents. Subst. Use Misuse 2021, 56, 101–110. [Google Scholar] [CrossRef]
- Kim, J.H.; Weinberger, A.H.; Zhu, J.; Barrington-Trimis, J.; Wyka, K.; Goodwin, R.D. Impact of state-level cannabis legalization on poly use of alcohol and cannabis in the United States, 2004–2017. Drug Alcohol Depend. 2021, 218, 108364. [Google Scholar] [CrossRef] [PubMed]
| Total | Adults Without Cancer | Cancer Survivors | p-Value | ||||
|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | ||
| What is your gender? | 0.109 | ||||||
| Female | 68 | 43.3 | 28 | 35.4 | 40 | 51.3 | |
| Male | 87 | 55.4 | 50 | 63.3 | 37 | 47.4 | |
| Other | 1 | 0.6 | 0 | 0 | 1 | 1.3 | |
| Transgender | 1 | 0.6 | 1 | 1.3 | 0 | 0 | |
| Do you live in the United States? | 0.043 | ||||||
| No | 13 | 8.2 | 3 | 3.8 | 10 | 12.7 | |
| Yes | 145 | 91.8 | 76 | 96.2 | 69 | 87.3 | |
| Race/Ethnicity | 0.427 | ||||||
| Non-Hispanic White | 132 | 85.2 | 69 | 88.5 | 63 | 81.8 | |
| Non-Hispanic Black or African American | 6 | 3.9 | 2 | 2.6 | 4 | 5.2 | |
| Hispanic | 9 | 5.8 | 2 | 2.6 | 7 | 9.1 | |
| Non-Hispanic Asian | 2 | 1.3 | 1 | 1.3 | 1 | 1.3 | |
| Native Hawaiian or Other Pacific Islander | 1 | 0.6 | 1 | 1.3 | 0 | 0 | |
| American Indian or Alaska Native | 5 | 3.2 | 3 | 3.8 | 2 | 2.6 | |
| Education Level | 0.983 | ||||||
| High school or less | 18 | 11.4 | 9 | 11.4 | 9 | 11.4 | |
| Bachelor’s degree or some college | 99 | 62.7 | 50 | 63.3 | 49 | 62 | |
| Masters degree or higher | 41 | 25.9 | 20 | 25.3 | 21 | 26.6 | |
| Household Income | 0.876 | ||||||
| Less than $30,000 | 38 | 32.2 | 19 | 31.1 | 19 | 33.3 | |
| Between $30,000 and $50,000 | 29 | 24.6 | 16 | 26.2 | 13 | 22.8 | |
| Between $50,000 and $100,000 | 26 | 22 | 12 | 19.7 | 14 | 24.6 | |
| More than $100,000 | 25 | 21.2 | 14 | 23 | 11 | 19.3 | |
| Medical Cannabis User | 0.000 | ||||||
| No | 24 | 15.2 | 21 | 26.6 | 3 | 3.8 | |
| Yes | 134 | 84.8 | 58 | 73.4 | 76 | 96.2 | |
| Employed for Wages | 0.714 | ||||||
| No | 118 | 74.7 | 58 | 73.4 | 60 | 75.9 | |
| Yes | 40 | 25.3 | 21 | 26.6 | 19 | 24.1 | |
| Self-Employed | 0.428 | ||||||
| No | 126 | 79.7 | 65 | 82.3 | 61 | 77.2 | |
| Yes | 32 | 20.3 | 14 | 17.7 | 18 | 22.8 | |
| Unemployed Due to COVID | 0.118 | ||||||
| No | 147 | 93 | 71 | 89.9 | 76 | 96.2 | |
| Yes | 11 | 7 | 8 | 10.1 | 3 | 3.8 | |
| Unemployed Prior to COVID | 0.119 | ||||||
| No | 141 | 89.2 | 73 | 92.4 | 68 | 86.1 | |
| Yes | 17 | 10.8 | 6 | 7.6 | 11 | 13.9 | |
| Respiratory Comorbidities | 0.198 | ||||||
| No | 132 | 83.5 | 63 | 79.7 | 69 | 87.3 | |
| Yes | 26 | 16.5 | 16 | 20.3 | 10 | 12.7 | |
| Cardiometabolic Comorbidities | 0.478 | ||||||
| No | 114 | 72.2 | 59 | 74.7 | 55 | 69.6 | |
| Yes | 44 | 27.8 | 20 | 25.3 | 24 | 30.4 | |
| Mental Health Comorbidities | 0.749 | ||||||
| No | 86 | 54.4 | 42 | 53.2 | 44 | 55.7 | |
| Yes | 72 | 45.6 | 37 | 46.8 | 35 | 44.3 | |
| Pain | 0.749 | ||||||
| No | 88 | 55.7 | 45 | 57 | 43 | 54.4 | |
| Yes | 70 | 44.3 | 34 | 43 | 36 | 45.6 | |
| Total | Adults Without Cancer | Cancer Survivors | p-Value | ||||
|---|---|---|---|---|---|---|---|
| Symptoms | n | % | n | % | n | % | |
| Acute Pain | 59 | 37.3 | 29 | 36.7 | 30 | 38 | 0.869 |
| Chronic non-cancer pain | 74 | 46.8 | 34 | 43 | 40 | 50.6 | 0.339 |
| Cancer pain | 33 | 20.9 | 0 | 0 | 33 | 41.8 | < 0.001 |
| Nausea/vomiting | 48 | 30.4 | 16 | 20.3 | 32 | 40.5 | 0.006 |
| Appetite Stimulant | 45 | 28.5 | 14 | 17.7 | 31 | 39.2 | 0.003 |
| Headaches/migraines | 43 | 27.2 | 15 | 19 | 28 | 35.4 | 0.02 |
| Muscle spams | 44 | 27.8 | 22 | 27.8 | 22 | 27.8 | 1 |
| Seizures | 8 | 5.1 | 1 | 1.3 | 7 | 8.9 | 0.029 |
| Sleep problems | 99 | 62.7 | 43 | 54.4 | 56 | 70.9 | 0.033 |
| Alcohol withdrawal symptoms | 7 | 4.4 | 3 | 3.8 | 4 | 5.1 | 0.69 |
| Opioid withdrawal symptoms | 8 | 5.1 | 2 | 2.5 | 6 | 7.6 | 0.147 |
| Palliative care | 8 | 5.1 | 2 | 2.5 | 6 | 7.6 | 0.147 |
| Other | 20 | 12.7 | 9 | 11.4 | 11 | 13.9 | 0.632 |
| Total | Adults Without Cancer | Cancer Survivors | p-Value | ||||
|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | ||
| Have you had any pain in your throat, chest, or lungs after using cannabis? | 0.344 | ||||||
| No | 133 | 84.2 | 65 | 82.3 | 68 | 86.1 | |
| Yes | 25 | 15.8 | 14 | 17.7 | 11 | 13.9 | |
| Since COVID-19 has been declared a pandemic, are you (or were you) worried about not being able to pay for your cannabis? | 0.012 | ||||||
| No | 88 | 58.7 | 51 | 68.9 | 37 | 48.7 | |
| Yes | 62 | 41.3 | 23 | 31.1 | 39 | 51.3 | |
| Since COVID-19 has been declared a pandemic, did a health professional recommend you use cannabis to manage COVID-19 or the coronavirus? | 0.311 | ||||||
| No | 154 | 97.5 | 78 | 98.7 | 76 | 96.2 | |
| Yes | 4 | 2.5 | 1 | 1.3 | 3 | 3.8 | |
| Since COVID-19 has been declared a pandemic, did a health professional recommend you to get an advance supply of your cannabis? | 0.039 | ||||||
| No | 106 | 89.1 | 48 | 96 | 58 | 84.1 | |
| Yes | 13 | 10.9 | 2 | 4 | 11 | 15.9 | |
| Since COVID-19 has been declared a pandemic, how has the dose of your cannabis use changed? | 0.483 | ||||||
| The amount used has increased | 43 | 28.7 | 19 | 25.7 | 24 | 31.6 | |
| The amount used has decreased | 18 | 12 | 11 | 14.9 | 7 | 9.2 | |
| The amount used has stayed the same | 89 | 59.3 | 44 | 59.5 | 45 | 59.2 | |
| Since COVID-19 has been declared a pandemic, do you share joints, blunts, or spliffs? | 0.999 | ||||||
| Yes, more than usual | 2 | 1.3 | 1 | 1.4 | 1 | 1.3 | |
| Yes, the same as usual | 16 | 10.7 | 8 | 10.8 | 8 | 10.5 | |
| Yes, less than usual | 4 | 2.7 | 2 | 2.7 | 2 | 2.6 | |
| No, I did not share before COVID-19 | 88 | 58.7 | 44 | 59.5 | 44 | 57.9 | |
| No, I stopped | 40 | 26.7 | 19 | 25.7 | 21 | 27.6 | |
| Since COVID-19 has been declared a pandemic, do you share electronic vaporizing devices? | 0.573 | ||||||
| Yes devices containing cannabis | 11 | 7 | 4 | 5.1 | 7 | 8.9 | |
| Yes devices containing nicotine | |||||||
| Yes devices containing both cannabis and nicotine | |||||||
| No I do/did not share devices | 91 | 57.6 | 45 | 57 | 46 | 58.2 | |
| No I do/did not use devices | 56 | 35.4 | 30 | 38 | 26 | 32.9 | |
| What is the dominant cannabinoid (i.e., THC, CBD, CBN) within your medical cannabis? | 0.257 | ||||||
| CBD dominant | 7 | 5 | 2 | 2.9 | 5 | 6.8 | |
| CBN dominant | 3 | 2.1 | 0 | 0 | 3 | 4.1 | |
| THC dominant | 87 | 61.7 | 45 | 66.2 | 42 | 57.5 | |
| CBD and THC ratio | 38 | 27 | 17 | 25 | 21 | 28.8 | |
| Other cannabinoid dominant | |||||||
| Unsure | 6 | 4.3 | 4 | 5.9 | 2 | 2.7 | |
| How often were you under the influence of psychoactive cannabis for 6 or more hours? | 0.587 | ||||||
| Never | 16 | 10.3 | 8 | 10.3 | 8 | 10.4 | |
| Less than Monthly | 11 | 7.1 | 4 | 5.1 | 7 | 9.1 | |
| Monthly | 4 | 2.6 | 3 | 3.8 | 1 | 1.3 | |
| Weekly | 27 | 17.4 | 16 | 20.5 | 11 | 14.3 | |
| Daily/Almost Daily | 97 | 62.6 | 47 | 60.3 | 50 | 64.9 | |
| Does your health insurance cover the cost of your medical cannabis? | 0.563 | ||||||
| Yes | |||||||
| No | 111 | 92.5 | 48 | 94.1 | 63 | 91.3 | |
| I do not have health insurance | 9 | 7.5 | 3 | 5.9 | 6 | 8.7 | |
| How long will the advance supply of cannabis last you? | 0.001 | ||||||
| 1 week | 3 | 4.2 | 3 | 8.3 | 0 | 0 | |
| 2 weeks | 18 | 25.4 | 5 | 13.9 | 13 | 37.1 | |
| 3 weeks | 8 | 11.3 | 4 | 11.1 | 4 | 11.4 | |
| 1 month | 15 | 21.1 | 5 | 13.9 | 10 | 28.6 | |
| 2 months | 10 | 14.1 | 10 | 27.8 | 0 | 0 | |
| 3 months | 3 | 4.2 | 3 | 8.3 | 0 | 0 | |
| More than 3 months | 14 | 19.7 | 6 | 16.7 | 8 | 22.9 | |
| Before COVID-19 has been declared a pandemic, which method of cannabis delivery did you use most? | 0.18 | ||||||
| Smoked it in a pipe/bowl | 6 | 30 | 2 | 25 | 4 | 33.3 | |
| Smoked it in a blunt | 3 | 15 | 1 | 12.5 | 2 | 16.7 | |
| Smoked it in a joint | 3 | 15 | 0 | 0 | 3 | 25 | |
| Edible (in food or drink) | 3 | 15 | 3 | 37.5 | 0 | 0 | |
| Vaporizer | 3 | 15 | 2 | 25 | 1 | 8.3 | |
| Ointment, cream, patch | |||||||
| Tincture | 1 | 5 | 0 | 0 | 1 | 8.3 | |
| Pill | 1 | 5 | 0 | 0 | 1 | 8.3 | |
| Since COVID-19 has been declared a pandemic, which method of delivery do you use? | 0.67 | ||||||
| Smoked it in a pipe/bowl | 5 | 25 | 2 | 25 | 3 | 25 | |
| Smoked it in a blunt | |||||||
| Smoked it in a joint | 3 | 15 | 1 | 12.5 | 2 | 16.7 | |
| Edible (in food or drink) | 4 | 20 | 1 | 12.5 | 3 | 25 | |
| Vaporizer | 4 | 20 | 3 | 37.5 | 1 | 8.3 | |
| Ointment, cream, patch | |||||||
| Tincture | 3 | 15 | 1 | 12.5 | 2 | 16.7 | |
| Pill | 1 | 5 | 0 | 0 | 1 | 8.3 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Camacho-Rivera, M.; Islam, J.Y.; Rodriguez, D.L.; Vidot, D.C. Cannabis Use among Cancer Survivors amid the COVID-19 Pandemic: Results from the COVID-19 Cannabis Health Study. Cancers 2021, 13, 3495. https://doi.org/10.3390/cancers13143495
Camacho-Rivera M, Islam JY, Rodriguez DL, Vidot DC. Cannabis Use among Cancer Survivors amid the COVID-19 Pandemic: Results from the COVID-19 Cannabis Health Study. Cancers. 2021; 13(14):3495. https://doi.org/10.3390/cancers13143495
Chicago/Turabian StyleCamacho-Rivera, Marlene, Jessica Y. Islam, Diane L. Rodriguez, and Denise C. Vidot. 2021. "Cannabis Use among Cancer Survivors amid the COVID-19 Pandemic: Results from the COVID-19 Cannabis Health Study" Cancers 13, no. 14: 3495. https://doi.org/10.3390/cancers13143495
APA StyleCamacho-Rivera, M., Islam, J. Y., Rodriguez, D. L., & Vidot, D. C. (2021). Cannabis Use among Cancer Survivors amid the COVID-19 Pandemic: Results from the COVID-19 Cannabis Health Study. Cancers, 13(14), 3495. https://doi.org/10.3390/cancers13143495








