Performance of In Silico Prediction Tools for the Detection of Germline Copy Number Variations in Cancer Predisposition Genes in 4208 Female Index Patients with Familial Breast and Ovarian Cancer
Abstract
Simple Summary
Abstract
1. Introduction
2. Results
2.1. CNV Predictions Using the Sophia Genetics DDM
2.2. CNV Predictions Using ExomeDepth, GATK gCNV, and panelcn.MOPS
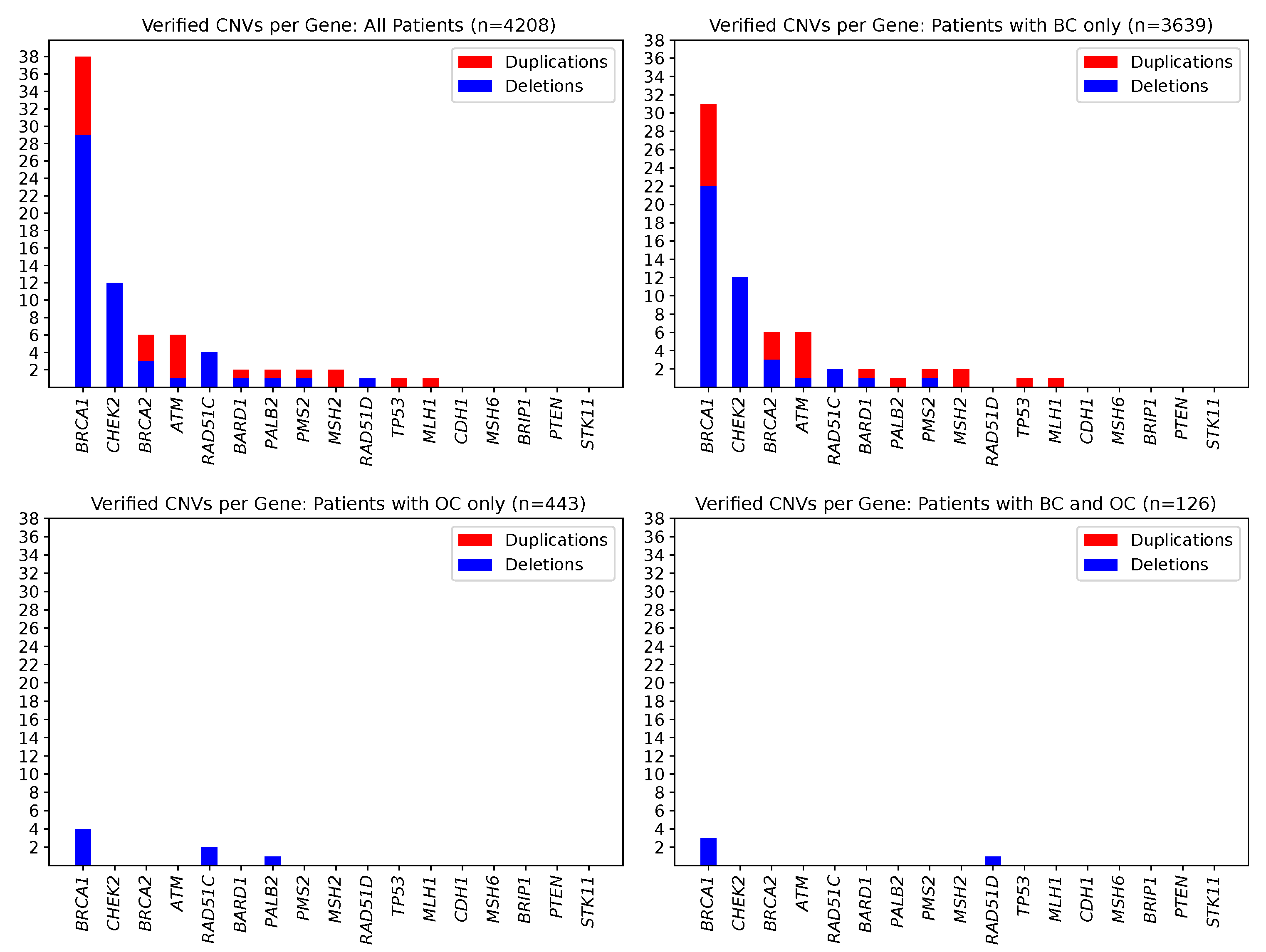
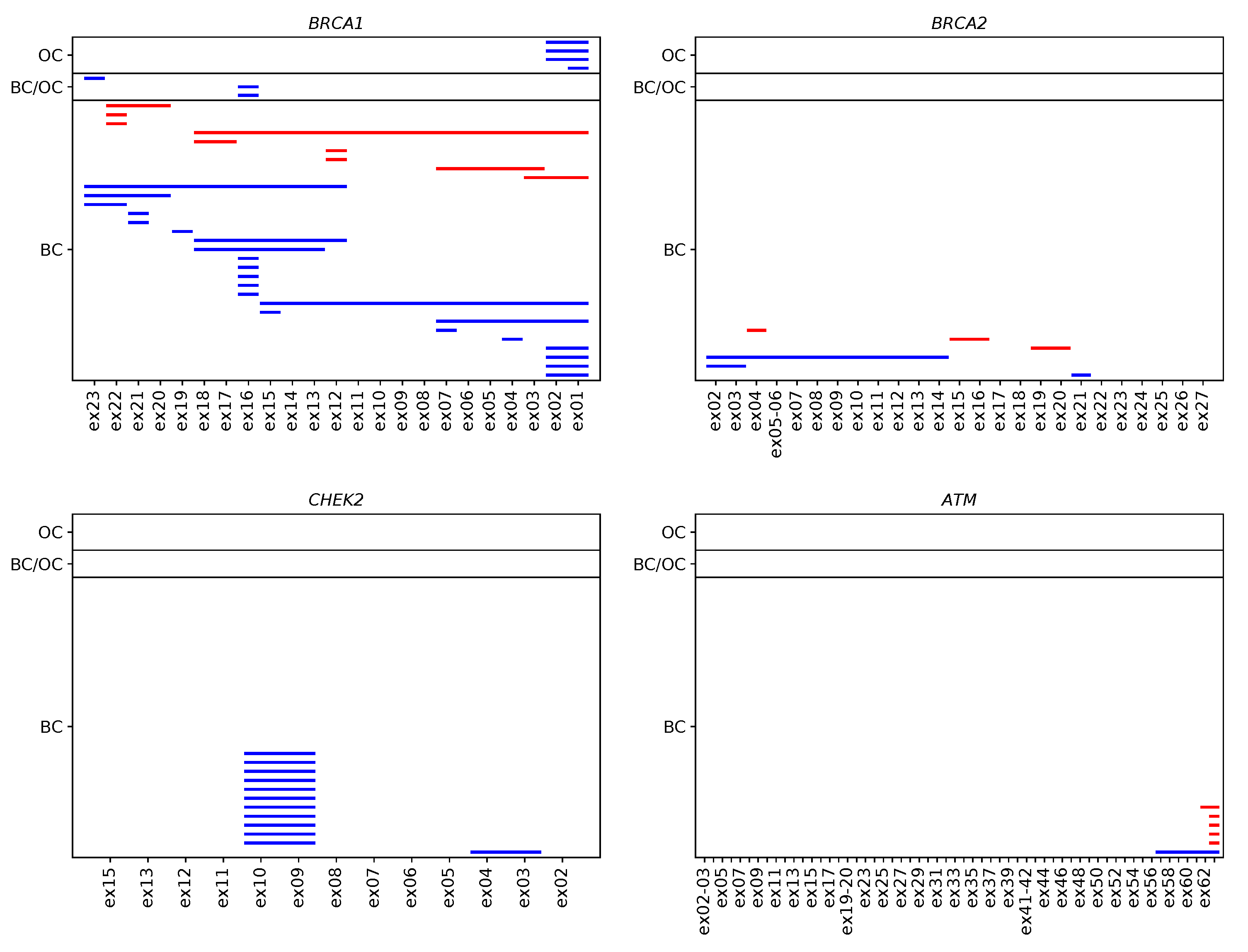
2.3. CNV Landscape in the Study Sample
2.4. Determinants of Sophia Genetics DDM Predictions with Reduced Confidence
3. Discussion
4. Materials and Methods
4.1. Study Sample
4.2. Targeted Next-Generation Sequencing
4.3. Selection of Target Regions
4.4. In silico Prediction of Germline Copy Number Variations in Cancer Predisposition Genes
4.5. Multiplex Ligation-Dependent Probe Amplification Analyses
4.6. Extraction of Sequencing Target Characteristics
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| aCGH | Array comparative genomic hybridization |
| BC | Breast cancer |
| CNV | Copy number variation |
| GC-HBOC | German Consortium for Hereditary Breast and Ovarian Cancer |
| MLPA | Multiplex ligation-dependent probe amplification |
| NGS | Next-generation sequencing |
| OC | Ovarian cancer |
| PPV | Positive predictive value |
| SNV | Single nucleotide variant |
References
- Schouten, J.P.; McElgunn, C.J.; Waaijer, R.; Zwijnenburg, D.; Diepvens, F.; Pals, G. Relative quantification of 40 nucleic acid sequences by multiplex ligation-dependent probe amplification. Nucleic Acids Res. 2002, 30, e57. [Google Scholar] [CrossRef] [PubMed]
- Hackmann, K.; Kuhlee, F.; Betcheva-Krajcir, E.; Kahlert, A.K.; Mackenroth, L.; Klink, B.; Di Donato, N.; Tzschach, A.; Kast, K.; Wimberger, P.; et al. Ready to clone: CNV detection and breakpoint fine-mapping in breast and ovarian cancer susceptibility genes by high-resolution array CGH. Breast Cancer Res. Treat. 2016, 159, 585–590. [Google Scholar] [CrossRef] [PubMed]
- Oostlander, A.E.; Meijer, G.; Ylstra, B. Microarray-based comparative genomic hybridization and its applications in human genetics. Clin. Genet. 2004, 66, 488–495. [Google Scholar] [CrossRef] [PubMed]
- Kerkhof, J.; Schenkel, L.C.; Reilly, J.; McRobbie, S.; Aref-Eshghi, E.; Stuart, A.; Rupar, C.A.; Adams, P.; Hegele, R.A.; Lin, H.; et al. Clinical validation of copy number variant detection from targeted next-generation sequencing panels. J. Mol. Diagn. 2017, 19, 905–920. [Google Scholar] [CrossRef] [PubMed]
- Concolino, P.; Capoluongo, E. Detection of BRCA1/2 large genomic rearrangements in breast and ovarian cancer patients: An overview of the current methods. Expert Rev. Mol. Diagn. 2019, 19, 795–802. [Google Scholar] [CrossRef] [PubMed]
- Ruderfer, D.M.; Hamamsy, T.; Lek, M.; Karczewski, K.J.; Kavanagh, D.; Samocha, K.E.; Daly, M.J.; MacArthur, D.G.; Fromer, M.; Purcell, S.M. Patterns of genic intolerance of rare copy number variation in 59,898 human exomes. Nat. Genet. 2016, 48, 1107–1111. [Google Scholar] [CrossRef]
- Hong, C.S.; Singh, L.N.; Mullikin, J.C.; Biesecker, L.G. Assessing the reproducibility of exome copy number variations predictions. Genome Med. 2016, 8, 82. [Google Scholar] [CrossRef]
- Roca, I.; González-Castro, L.; Fernández, H.; Couce, M.L.; Fernández-Marmiesse, A. Free-access copy-number variant detection tools for targeted next-generation sequencing data. Mutat. Res. Mutat. Res. 2019, 779, 114–125. [Google Scholar] [CrossRef]
- Moreno-Cabrera, J.M.; Del Valle, J.; Castellanos, E.; Feliubadaló, L.; Pineda, M.; Brunet, J.; Serra, E.; Capellà, G.; Lázaro, C.; Gel, B. Evaluation of CNV detection tools for NGS panel data in genetic diagnostics. Eur. J. Hum. Genet. 2020, 28, 1645–1655. [Google Scholar] [CrossRef]
- Mason-Suares, H.; Landry, L.; Lebo, M.S. Detecting copy number variation via next generation technology. Curr. Genet. Med. Rep. 2016, 4, 74–85. [Google Scholar] [CrossRef]
- Plagnol, V.; Curtis, J.; Epstein, M.; Mok, K.Y.; Stebbings, E.; Grigoriadou, S.; Wood, N.W.; Hambleton, S.; Burns, S.O.; Thrasher, A.J.; et al. A robust model for read count data in exome sequencing experiments and implications for copy number variant calling. Bioinformatics 2012, 28, 2747–2754. [Google Scholar] [CrossRef] [PubMed]
- Babadi, M.; Lee, S.K.; Smirnov, A.; Lichtenstein, L.; Gauthier, L.D.; Howrigan, D.P.; Poterba, T. Precise common and rare germline CNV calling with GATK [abstract]. Cancer Res. 2018, 38 (Suppl. 13), 78. [Google Scholar]
- Povysil, G.; Tzika, A.; Vogt, J.; Haunschmid, V.; Messiaen, L.; Zschocke, J.; Klambauer, G.; Hochreiter, S.; Wimmer, K. panelcn.MOPS: Copy-number detection in targeted NGS panel data for clinical diagnostics. Hum. Mutat. 2017, 38, 889–897. [Google Scholar] [CrossRef] [PubMed]
- Cacheiro, P.; Ordóñez-Ugalde, A.; Quintáns, B.; Piñeiro-Hermida, S.; Amigo, J.; García-Murias, M.; Pascual-Pascual, S.; Grandas, F.; Arpa, J.; Carracedo, A.; et al. Evaluating the calling performance of a rare disease NGS panel for single nucleotide and copy number variants. Mol. Diagn. Ther. 2017, 21, 303–313. [Google Scholar] [CrossRef]
- Ellingford, J.M.; Horn, B.; Campbell, C.; Arno, G.; Barton, S.; Tate, C.; Bhaskar, S.; Sergouniotis, P.I.; Taylor, R.L.; Carss, K.J.; et al. Assessment of the incorporation of CNV surveillance into gene panel next-generation sequencing testing for inherited retinal diseases. J. Med. Genet. 2018, 55, 114–121. [Google Scholar] [CrossRef] [PubMed]
- Judkins, T.; Rosenthal, E.; Arnell, C.; Burbidge, L.A.; Geary, W.; Barrus, T.; Schoenberger, J.; Trost, J.; Wenstrup, R.J.; Roa, B.B. Clinical significance of large rearrangements in BRCA1 and BRCA2. Cancer 2012, 118, 5210–5216. [Google Scholar] [CrossRef]
- Ewald, I.P.; Ribeiro, P.L.I.; Palmero, E.I.; Cossio, S.L.; Giugliani, R.; Ashton-Prolla, P. Genomic rearrangements in BRCA1 and BRCA2: A literature review. Genet. Mol. Biol. 2009, 32, 437–446. [Google Scholar] [CrossRef]
- Schmidt, A.Y.; vO Hansen, T.; Ahlborn, L.B.; Jønson, L.; Yde, C.W.; Nielsen, F.C. Next-Generation Sequencing–Based Detection of Germline Copy Number Variations in BRCA1/BRCA2: Validation of a One-Step Diagnostic Workflow. J. Mol. Diagn. 2017, 19, 809–816. [Google Scholar] [CrossRef]
- Concolino, P.; Rizza, R.; Mignone, F.; Costella, A.; Guarino, D.; Carboni, I.; Capoluongo, E.; Santonocito, C.; Urbani, A.; Minucci, A. A comprehensive BRCA1/2 NGS pipeline for an immediate Copy Number Variation (CNV) detection in breast and ovarian cancer molecular diagnosis. Clin. Chim. Acta 2018, 480, 173–179. [Google Scholar] [CrossRef]
- Cybulski, C.; Wokołorczyk, D.; Huzarski, T.; Byrski, T.; Gronwald, J.; Górski, B.; Dębniak, T.; Masojć, B.; Jakubowska, A.; van de Wetering, T.; et al. A deletion in CHEK2 of 5,395 bp predisposes to breast cancer in Poland. Breast Cancer Res. Treat. 2007, 102, 119–122. [Google Scholar] [CrossRef]
- Schnurbein, G.; Hauke, J.; Wappenschmidt, B.; Weber-Lassalle, N.; Engert, S.; Hellebrand, H.; Garbes, L.; Becker, A.; Neidhardt, G.; Rhiem, K.; et al. RAD51C deletion screening identifies a recurrent gross deletion in breast cancer and ovarian cancer families. Breast Cancer Res. 2013, 15, R120. [Google Scholar] [CrossRef]
- Yang, X.; Song, H.; Leslie, G.; Engel, C.; Hahnen, E.; Auber, B.; Horváth, J.; Kast, K.; Niederacher, D.; Turnbull, C.; et al. Ovarian and breast cancer risks associated with pathogenic variants in RAD51C and RAD51D. J. Natl. Cancer Inst. 2020, 112, 1242–1250. [Google Scholar] [CrossRef] [PubMed]
- Landrum, M.J.; Lee, J.M.; Benson, M.; Brown, G.R.; Chao, C.; Chitipiralla, S.; Gu, B.; Hart, J.; Hoffman, D.; Jang, W.; et al. ClinVar: Improving access to variant interpretations and supporting evidence. Nucleic Acids Res. 2018, 46, D1062–D1067. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Y.; Wang, R.; Urrutia, E.; Anastopoulos, I.N.; Nathanson, K.L.; Zhang, N.R. CODEX2: Full-spectrum copy number variation detection by high-throughput DNA sequencing. Genome Biol. 2018, 19, 202. [Google Scholar] [CrossRef] [PubMed]
- Kast, K.; Rhiem, K.; Wappenschmidt, B.; Hahnen, E.; Hauke, J.; Bluemcke, B.; Zarghooni, V.; Herold, N.; Ditsch, N.; Kiechle, M.; et al. Prevalence of BRCA1/2 germline mutations in 21 401 families with breast and ovarian cancer. J. Med. Genet. 2016, 53, 465–471. [Google Scholar] [CrossRef]
- Alkan, C.; Coe, B.P.; Eichler, E.E. Genome structural variation discovery and genotyping. Nat. Rev. Genet. 2011, 12, 363–376. [Google Scholar] [CrossRef]
- Li, H.; Durbin, R. Fast and accurate short read alignment with Burrows–Wheeler transform. Bioinformatics 2009, 25, 1754–1760. [Google Scholar] [CrossRef]
- Li, H. Aligning sequence reads, clone sequences and assembly contigs with BWA-MEM. arXiv 2013, arXiv:1303.3997. [Google Scholar]
- McKenna, A.; Hanna, M.; Banks, E.; Sivachenko, A.; Cibulskis, K.; Kernytsky, A.; Garimella, K.; Altshuler, D.; Gabriel, S.; Daly, M.; et al. The Genome Analysis Toolkit: A MapReduce framework for analyzing next-generation DNA sequencing data. Genome Res. 2010, 20, 1297–1303. [Google Scholar] [CrossRef]
- DePristo, M.A.; Banks, E.; Poplin, R.; Garimella, K.V.; Maguire, J.R.; Hartl, C.; Philippakis, A.A.; Del Angel, G.; Rivas, M.A.; Hanna, M.; et al. A framework for variation discovery and genotyping using next-generation DNA sequencing data. Nat. Genet. 2011, 43, 491. [Google Scholar] [CrossRef]
- Quinlan, A.R.; Hall, I.M. BEDTools: A flexible suite of utilities for comparing genomic features. Bioinformatics 2010, 26, 841–842. [Google Scholar] [CrossRef] [PubMed]
- Klonowska, K.; Ratajska, M.; Czubak, K.; Kuzniacka, A.; Brozek, I.; Koczkowska, M.; Sniadecki, M.; Debniak, J.; Wydra, D.; Balut, M.; et al. Analysis of large mutations in BARD1 in patients with breast and/or ovarian cancer: The Polish population as an example. Sci. Rep. 2015, 5, 10424. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Y.; Oldridge, D.A.; Diskin, S.J.; Zhang, N.R. CODEX: A normalization and copy number variation detection method for whole exome sequencing. Nucleic Acids Res. 2015, 43, e39. [Google Scholar] [CrossRef] [PubMed]
- Huddleston, J.; Chaisson, M.J.; Steinberg, K.M.; Warren, W.; Hoekzema, K.; Gordon, D.; Graves-Lindsay, T.A.; Munson, K.M.; Kronenberg, Z.N.; Vives, L.; et al. Discovery and genotyping of structural variation from long-read haploid genome sequence data. Genome Res. 2017, 27, 677–685. [Google Scholar] [CrossRef] [PubMed]

| Predicted CNVs | True Positive CNVs | PPV (%) | |
|---|---|---|---|
| Overall | 134 | 77 | 57.46 |
| High confidence | 103 | 75 | 72.82 |
| Medium confidence | 31 | 2 | 6.45 |
| Deletions | 63 | 53 | 84.13 |
| Duplications | 71 | 24 | 33.80 |
| 1 target region | 70 | 25 | 35.71 |
| >1 target region | 64 | 52 | 81.25 |
| Sample | CNV Type | Start | Stop | Target Regions | ED | GATK | pcnMOPS |
|---|---|---|---|---|---|---|---|
| 44–22 | deletion | BARD1_ex04 | BARD1_ex01 | 4 | yes | no | yes |
| 14–15 | duplication | BRCA1_ex22 | BRCA1 ex22 | 1 | no | no | no |
| 89–01 | duplication | BRCA2_ex04 | BRCA2_ex04 | 1 | no | no | no |
| 9–25 | duplication | BRCA2_ex19 | BRCA2_ex20 | 2 | no | yes | yes |
| 49–28 | deletion | BRCA2_ex02 | BRCA2_ex14 | 12 | yes | yes | no |
| 29–19 | duplication | PALB2_ex11 | PALB2_ex11 | 1 | no | no | no |
| 16–27 | duplication | TP53_ex08-09 | TP53_ex02-04 | 5 | no | no | yes |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lepkes, L.; Kayali, M.; Blümcke, B.; Weber, J.; Suszynska, M.; Schmidt, S.; Borde, J.; Klonowska, K.; Wappenschmidt, B.; Hauke, J.; et al. Performance of In Silico Prediction Tools for the Detection of Germline Copy Number Variations in Cancer Predisposition Genes in 4208 Female Index Patients with Familial Breast and Ovarian Cancer. Cancers 2021, 13, 118. https://doi.org/10.3390/cancers13010118
Lepkes L, Kayali M, Blümcke B, Weber J, Suszynska M, Schmidt S, Borde J, Klonowska K, Wappenschmidt B, Hauke J, et al. Performance of In Silico Prediction Tools for the Detection of Germline Copy Number Variations in Cancer Predisposition Genes in 4208 Female Index Patients with Familial Breast and Ovarian Cancer. Cancers. 2021; 13(1):118. https://doi.org/10.3390/cancers13010118
Chicago/Turabian StyleLepkes, Louisa, Mohamad Kayali, Britta Blümcke, Jonas Weber, Malwina Suszynska, Sandra Schmidt, Julika Borde, Katarzyna Klonowska, Barbara Wappenschmidt, Jan Hauke, and et al. 2021. "Performance of In Silico Prediction Tools for the Detection of Germline Copy Number Variations in Cancer Predisposition Genes in 4208 Female Index Patients with Familial Breast and Ovarian Cancer" Cancers 13, no. 1: 118. https://doi.org/10.3390/cancers13010118
APA StyleLepkes, L., Kayali, M., Blümcke, B., Weber, J., Suszynska, M., Schmidt, S., Borde, J., Klonowska, K., Wappenschmidt, B., Hauke, J., Kozlowski, P., Schmutzler, R. K., Hahnen, E., & Ernst, C. (2021). Performance of In Silico Prediction Tools for the Detection of Germline Copy Number Variations in Cancer Predisposition Genes in 4208 Female Index Patients with Familial Breast and Ovarian Cancer. Cancers, 13(1), 118. https://doi.org/10.3390/cancers13010118






