High-Risk Human Papillomavirus and Tobacco Smoke Interactions in Epithelial Carcinogenesis
Abstract
1. Introduction
2. Human Papillomavirus (HPV)
2.1. Structure, Classification and Replication Cycle
2.2. Gene Expression Regulation
2.3. HPV Role in Epithelial Tumors
3. Tobacco Smoke and HPV Interactions
3.1. History and Epidemiology
3.2. Tobacco Smoke Affects HPV Replication
3.3. Tobacco Smoke Promotes HPV E6 and E7 Expression
3.4. Tobacco Smoke Affects Immune Responses Against HPV
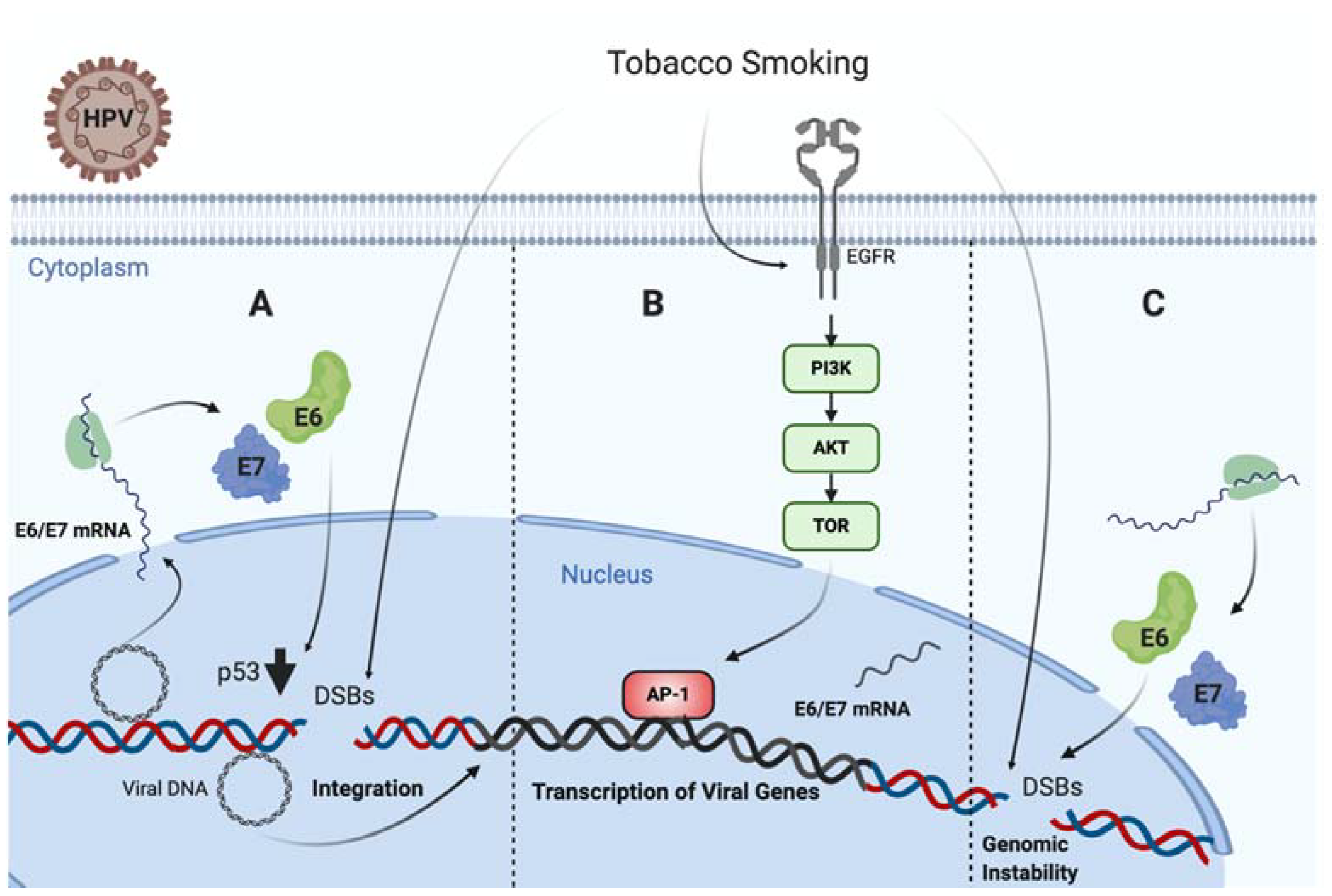
3.5. Tobacco Smoke Promotes DNA Damage Leading to an Increased HPV Oncogenic Role
3.6. Tobacco Smoke Alters Cellular Gene Expression Involved in HPV-Mediated Carcinogenesis
4. Conclusions and Remarks
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bosch, F.X.; De Sanjose, S. The Epidemiology of Human Papillomavirus Infection and Cervical Cancer. Dis. Markers 2007, 23, 213–227. [Google Scholar] [CrossRef]
- Wentz, W.B. Histologic grade and survival in cervical cancer. Obstet. Gynecol. 1961, 18, 412–416. [Google Scholar] [PubMed]
- Arbyn, M.; Weiderpass, E.; Bruni, L.; De Sanjosé, S.; Saraiya, M.; Ferlay, J.; Bray, F. Estimates of incidence and mortality of cervical cancer in 2018: A worldwide analysis. Lancet Glob. Health 2020, 8, e191–e203. [Google Scholar] [CrossRef]
- Ferlay, J.; Soerjomataram, I.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, N.M.; Forman, D.; Bray, F. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int. J. Cancer 2014, 136. [Google Scholar] [CrossRef]
- Ferlay, J.; Colombet, M.; Soerjomataram, I.; Mathers, C.; Parkin, D.M.; Piñeros, M.; Znaor, A.; Bray, F. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int. J. Cancer 2018, 144, 1941–1953. [Google Scholar] [CrossRef] [PubMed]
- De Cecco, L.; Nicolau, M.; Giannoccaro, M.; Daidone, M.G.; Bossi, P.; Locati, L.D.; Licitra, L.; Canevari, S. Head and neck cancer subtypes with biological and clinical relevance: Meta-analysis of gene-expression data. Oncotarget 2015, 6, 9627–9642. [Google Scholar] [CrossRef] [PubMed]
- Maasland, D.H.; Brandt, P.A.V.D.; Kremer, B.; Goldbohm, R.A.; Schouten, L.J. Alcohol consumption, cigarette smoking and the risk of subtypes of head-neck cancer: Results from the Netherlands Cohort Study. BMC Cancer 2014, 14, 187. [Google Scholar] [CrossRef] [PubMed]
- Sabatini, M.E.; Chiocca, S. Human papillomavirus as a driver of head and neck cancers. Br. J. Cancer 2019, 122, 306–314. [Google Scholar] [CrossRef]
- Kreimer, A.R.; Clifford, G.M.; Boyle, P.; Franceschi, S. Human papillomavirus types in head and neck squamous cell carcinomas worldwide: A systematic review. Cancer Epidemiol. Biomark. Prev. 2005, 14, 467–475. [Google Scholar] [CrossRef]
- Gillison, M.L.; Chaturvedi, A.K.; Anderson, W.F.; Fakhry, C. Epidemiology of human papillomavirus–positive head and neck squamous cell carcinoma. J. Clin. Oncol. 2015, 33, 3235–3242. [Google Scholar] [CrossRef]
- Ang, K.K.; Harris, J.; Wheeler, R.; Weber, R.; Rosenthal, D.I.; Nguyen-Tan, P.F.; Westra, W.H.; Chung, C.H.; Jordan, R.C.; Lu, C.; et al. Human papillomavirus and survival of patients with oropharyngeal cancer. N. Engl. J. Med. 2010, 363, 24–35. [Google Scholar] [CrossRef] [PubMed]
- Hausen, H.Z. Papillomaviruses and cancer: From basic studies to clinical application. Nat. Rev. Cancer 2002, 2, 342–350. [Google Scholar] [CrossRef] [PubMed]
- Cid, A.; Auewarakul, P.; Garcia-Carranca, A.; Ovseiovich, R.; Gaissert, H.; Gissmann, L. Cell-type-specific activity of the human papillomavirus type 18 upstream regulatory region in transgenic mice and its modulation by tetradecanoyl phorbol acetate and glucocorticoids. J. Virol. 1993, 67, 6742–6752. [Google Scholar] [CrossRef] [PubMed]
- Cripe, T.P.; Alderborn, A.; Anderson, R.D.; Parkkinen, S.; Bergman, P.; Haugen, T.H.; Pettersson, U.; Turek, L.P. Transcriptional activation of the human papillomavirus-16 P97 promoter by an 88-nucleotide enhancer containing distinct cell-dependent and AP-1-responsive modules. N. Biol. 1990, 2, 450–463. [Google Scholar]
- Bzhalava, D.; Eklund, C.; Dillner, J. International standardization and classification of human papillomavirus types. Virology 2015, 476, 341–344. [Google Scholar] [CrossRef]
- Shafti-Keramat, S.; Handisurya, A.; Kriehuber, E.; Meneguzzi, G.; Slupetzky, K.; Kirnbauer, R. Different heparan sulfate proteoglycans serve as cellular receptors for human papillomaviruses. J. Virol. 2003, 77, 13125–13135. [Google Scholar] [CrossRef]
- Giroglou, T.; Florin, L.; Schäfer, F.; Streeck, R.E.; Sapp, M. Human papillomavirus infection requires cell surface heparan sulfate. J. Virol. 2001, 75, 1565–1570. [Google Scholar] [CrossRef]
- Abban, C.Y.; Meneses, P.I. Usage of heparan sulfate, integrins, and FAK in HPV16 infection. Virology 2010, 403, 1–16. [Google Scholar] [CrossRef]
- Scheffer, K.D.; Gawlitza, A.; Spoden, G.A.; Zhang, X.A.; Lambert, C.; Berditchevski, F.; Florin, L. Tetraspanin cd151 mediates papillomavirus type 16 endocytosis. J. Virol. 2013, 87, 3435–3446. [Google Scholar] [CrossRef]
- Schelhaas, M.; Shah, B.; Holzer, M.; Blattmann, P.; Kühling, L.; Day, P.M.; Schiller, J.T.; Helenius, A. Entry of human papillomavirus type 16 by actin-dependent, clathrin- and lipid raft-independent endocytosis. PLoS Pathog. 2012, 8, e1002657. [Google Scholar] [CrossRef]
- Day, P.M.; Roden, R.B.S.; Lowy, D.R.; Schiller, J.T. The papillomavirus minor capsid protein, L2, induces localization of the major capsid protein, L1, and the viral transcription/replication protein, E2, to pml oncogenic domains. J. Virol. 1998, 72, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Ilves, I.; Kivi, S.; Ustav, M. Long-term episomal maintenance of bovine papillomavirus type 1 plasmids is determined by attachment to host chromosomes, which is mediated by the viral E2 protein and its binding sites. J. Virol. 1999, 73, 4404–4412. [Google Scholar] [CrossRef] [PubMed]
- Bastien, N.; McBride, A.A. Interaction of the papillomavirus E2 protein with mitotic chromosomes. Virology 2000, 270, 124–134. [Google Scholar] [CrossRef] [PubMed]
- Côté-Martin, A.; Moody, C.; Fradet-Turcotte, A.; D’Abramo, C.M.; Lehoux, M.; Joubert, S.; Poirier, G.G.; Coulombe, B.; Laimins, L.A.; Archambault, J. Human papillomavirus e1 helicase interacts with the wd repeat protein p80 to promote maintenance of the viral genome in keratinocytes. J. Virol. 2007, 82, 1271–1283. [Google Scholar] [CrossRef]
- McBride, A.A. The papillomavirus E2 proteins. Virology 2013, 445, 57–79. [Google Scholar] [CrossRef]
- Steger, G.; Corbach, S. Dose-dependent regulation of the early promoter of human papillomavirus type 18 by the viral E2 protein. J. Virol. 1997, 71, 50–58. [Google Scholar] [CrossRef]
- Pim, D.; Banks, L. Interaction of viral oncoproteins with cellular target molecules: Infection with high-risk vs low-risk human papillomaviruses. APMIS 2010, 118, 471–493. [Google Scholar] [CrossRef]
- Scheffner, M.; Werness, B.A.; Huibregtse, J.M.; Levine, A.J.; Howley, P.M. The E6 oncoprotein encoded by human papillomavirus types 16 and 18 promotes the degradation of p53. Cell 1990, 63, 1129–1136. [Google Scholar] [CrossRef]
- Dyson, N.; Howley, P.M.; Munger, K.; Harlow, E. The human papilloma virus-16 E7 oncoprotein is able to bind to the retinoblastoma gene product. Science 1989, 243, 934–937. [Google Scholar] [CrossRef]
- Estêvão, D.; Costa, N.R.; Gil Da Costa, R.M.; Medeiros, R. Hallmarks of HPV carcinogenesis: The role of E6, E7 and E5 oncoproteins in cellular malignancy. Biochim. Biophys. Acta 2019, 1862, 153–162. [Google Scholar] [CrossRef]
- Crusius, K.; Auvinen, E.; Steuer, B.; Gaissert, H.; Alonso, A. The human papillomavirus type 16 E5-protein modulates ligand-dependent activation of the EGF receptor family in the human epithelial cell line HaCaT. Exp. Cell Res. 1998, 241, 76–83. [Google Scholar] [CrossRef]
- DiMaio, D.; Petti, L.M. The E5 proteins. Virology 2013, 445, 99–114. [Google Scholar] [CrossRef]
- Murakami, I.; Egawa, N.; Griffin, H.; Yin, W.; Kranjec, C.; Nakahara, T.; Kiyono, T.; Doorbar, J. Roles for E1-independent replication and E6-mediated p53 degradation during low-risk and high-risk human papillomavirus genome maintenance. PLoS Pathog. 2019, 15, e1007755. [Google Scholar] [CrossRef] [PubMed]
- Longworth, M.S.; Laimins, L.A. Pathogenesis of human papillomaviruses in differentiating epithelia. Microbiol. Mol. Biol. Rev. 2004, 68, 362–372. [Google Scholar] [CrossRef] [PubMed]
- Nasseri, M.; Hirochika, R.; Broker, T.R.; Chow, L.T. A human papilloma virus type 11 transcript encoding an E1^E4 protein. Virology 1987, 159, 433–439. [Google Scholar] [CrossRef]
- Doorbar, J.; Foo, C.; Coleman, N.; Medcalf, L.; Hartley, O.; Prospero, T.; Napthine, S.; Sterling, J.; Winter, G.; Griffin, H. Characterization of events during the late stages of HPV16 infectionin vivousing high-affinity synthetic fabs to E4. Virology 1997, 238, 40–52. [Google Scholar] [CrossRef] [PubMed]
- Doorbar, J.; Campbell, D.; Grand, R.; Gallimore, P.H. Identification of the human papilloma virus-1a E4 gene products. EMBO J. 1986, 5, 355–362. [Google Scholar] [CrossRef]
- Khan, J.; Davy, C.E.; McIntosh, P.B.; Jackson, D.J.; Hinz, S.; Wang, Q.; Doorbar, J. Role of calpain in the formation of human papillomavirus type 16 E1^E4 amyloid fibers and reorganization of the keratin network. J. Virol. 2011, 85, 9984–9997. [Google Scholar] [CrossRef]
- Rösl, F.; Dürst, M.; Hausen, H.Z. Selective suppression of human papillomavirus transcription in non-tumorigenic cells by 5-azacytidine. EMBO J. 1988, 7, 1321–1328. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.; Garner-Hamrick, P.A.; Fisher, C.; Lee, D.; Lambert, P.F. Methylation patterns of papillomavirus dna, its influence on E2 Function, and implications in viral infection. J. Virol. 2003, 77, 12450–12459. [Google Scholar] [CrossRef] [PubMed]
- Graham, S.V.; Faizo, A.A.A. Control of human papillomavirus gene expression by alternative splicing. Virus Res. 2017, 231, 83–95. [Google Scholar] [CrossRef] [PubMed]
- Terhune, S.S.; Milcarek, C.; Laimins, L.A. Regulation of human papillomavirus type 31 polyadenylation during the differentiation-dependent life cycle. J. Virol. 1999, 73, 7185–7192. [Google Scholar] [CrossRef] [PubMed]
- Kanda, T.; Mori, S. Regulation of HPV-gene expression. Tanpakushitsu Kakusan Koso Protein Nucleic Acid Enzym. 2007, 52, 1106–1112. [Google Scholar]
- Sycuro, L.K.; Xi, L.F.; Hughes, J.P.; Feng, Q.; Winer, R.L.; Lee, S.; O’Reilly, S.; Kiviat, N.B.; Koutsky, L.A. Persistence of genital human papillomavirus infection in a long-term follow-up study of female university students. J. Infect. Dis. 2008, 198, 971–978. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Chan, W.K.; Chong, T.; Bernard, H.U.; Kiock, G. Transcription of the transforming genes of the oncogenic human papillomavirus-16 is stimulated by tumor promotors through AP1 binding sites. Nucleic Acids Res. 1990, 18, 763–769. [Google Scholar] [CrossRef]
- Chong, T.; Chan, W.K.; Bernard, H.U. Transcriptional activation of human papillomavirus 16 by nuclear factor I, AP1, steroid receptors and a possibly novel transcription factor, PVF: A model for the composition of genital papillomavirus enhancers. Nucleic Acids Res. 1990, 18, 465–470. [Google Scholar] [CrossRef]
- Bejjani, F.; Evanno, E.; Ghanbari, A.; Piechaczyk, M.; Jariel-Encontre, I.; Fabienne, B.; Emilie, E.; Kazem, Z.; Piechaczyk, M.; Jariel-Encontre, I. The AP-1 transcriptional complex: Local switch or remote command? Biochim. Biophys. Acta 2019, 1872, 11–23. [Google Scholar] [CrossRef]
- Lopez-Bergami, P.; Lau, E.; Ronai, Z.A. Emerging roles of ATF2 and the dynamic AP1 network in cancer. Nat. Rev. Cancer 2010, 10, 65–76. [Google Scholar] [CrossRef]
- Shaulian, E.; Karin, M. AP-1 as a regulator of cell life and death. Nature 2002, 4, E131–E136. [Google Scholar] [CrossRef]
- Hoppe-Seyler, F.; Butz, K.; Hausen, H.Z. Repression of the human papillomavirus type 18 enhancer by the cellular transcription factor Oct-1. J. Virol. 1991, 65, 5613–5618. [Google Scholar] [CrossRef]
- Sibbet, G.J.; Cuthill, S.; Campo, M.S. The enhancer in the long control region of human papillomavirus type 16 is up-regulated by PEF-1 and down-regulated by Oct-1. J. Virol. 1995, 69, 4006–4011. [Google Scholar] [CrossRef] [PubMed]
- Bernard, H.-U.; Apt, D. Transcriptional control and cell type specificity of HPV gene expression. Arch. Dermatol. 1994, 130, 210. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, S. Papillomavirus transcripts and posttranscriptional regulation. Virology 2013, 445, 187–196. [Google Scholar] [CrossRef] [PubMed]
- McBride, A.A.; Romanczuk, H.; Howley, P.M. The papillomavirus E2 regulatory proteins. J. Biol. Chem. 1991, 266, 18411–18414. [Google Scholar]
- Hebner, C.M.; Laimins, L.A. Human papillomaviruses: Basic mechanisms of pathogenesis and oncogenicity. Rev. Med. Virol. 2006, 16, 83–97. [Google Scholar] [CrossRef]
- Li, C.C.; Gilden, R.V.; Showalter, S.D.; Shah, K.V. Identification of the human papillomavirus E2 protein in genital tract tissues. J. Virol. 1988, 62, 606–609. [Google Scholar] [CrossRef]
- Sedman, T.; Sedman, J.; Stenlund, A. Binding of the E1 and E2 proteins to the origin of replication of bovine papillomavirus. J. Virol. 1997, 71, 2887–2896. [Google Scholar] [CrossRef]
- Stubenrauch, F.; Hummel, M.; Iftner, T.; Laimins, L.A. The E8^E2C protein, a negative regulator of viral transcription and replication, is required for extrachromosomal maintenance of human papillomavirus type 31 in keratinocytes. J. Virol. 2000, 74, 1178–1186. [Google Scholar] [CrossRef]
- Lace, M.J.; Anson, J.R.; Thomas, G.S.; Turek, L.P.; Haugen, T.H. The E8∧E2 gene product of human papillomavirus type 16 represses early transcription and replication but is dispensable for viral plasmid persistence in keratinocytes. J. Virol. 2008, 82, 10841–10853. [Google Scholar] [CrossRef]
- Dreer, M.; Fertey, J.; Van De Poel, S.; Straub, E.; Madlung, J.; Macek, B.; Iftner, T.; Stubenrauch, F. interaction of ncor/smrt repressor complexes with papillomavirus E8^E2C proteins inhibits viral replication. PLoS Pathog. 2016, 12, e1005556. [Google Scholar] [CrossRef]
- Cerasuolo, A.; Buonaguro, L.; Buonaguro, F.M.; Tornesello, M.L. The role of RNA splicing factors in cancer: Regulation of viral and human gene expression in human papillomavirus-related cervical cancer. Front. Cell Dev. Biol. 2020, 8. [Google Scholar] [CrossRef]
- Tang, S.; Tao, M.; McCoy, J.P.; Zheng, Z.M. The E7 oncoprotein is translated from spliced E6*I transcripts in high-risk human papillomavirus type 16- or type 18-positive cervical cancer cell lines via translation reinitiation. J. Virol. 2006, 80, 4249–4263. [Google Scholar] [CrossRef] [PubMed]
- Straub, E.; Fertey, J.; Dreer, M.; Iftner, T.; Stubenrauch, F. Characterization of the human papillomavirus 16 E8 promoter. J. Virol. 2015, 89, 7304–7313. [Google Scholar] [CrossRef] [PubMed]
- Johansson, C.; Somberg, M.; Li, X.; Winquist, E.B.; Fay, J.; Ryan, F.; Pim, D.; Banks, L.; Schwartz, S. HPV-16 E2 contributes to induction of HPV-16 late gene expression by inhibiting early polyadenylation. EMBO J. 2012, 31, 3212–3227. [Google Scholar] [CrossRef] [PubMed]
- Prescott, E.L.; Brimacombe, C.L.; Hartley, M.; Bell, I.; Graham, S.; Roberts, S. Human Papillomavirus Type 1 E1^E4 protein is a potent inhibitor of the serine-arginine (sr) protein kinase srpk1 and inhibits phosphorylation of host sr proteins and of the viral transcription and replication regulator E2. J. Virol. 2014, 88, 12599–12611. [Google Scholar] [CrossRef] [PubMed]
- Chan, W.K.; Klock, G.; Bernard, H.U. Progesterone and glucocorticoid response elements occur in the long control regions of several human papillomaviruses involved in anogenital neoplasia. J. Virol. 1989, 63, 3261–3269. [Google Scholar] [CrossRef]
- Yuan, F.; Auborn, K.; James, C. Altered growth and viral gene expression in human papillomavirus type 16-containing cancer cell lines treated with progesterone. Cancer Investig. 1999, 17, 19–29. [Google Scholar] [CrossRef]
- Psyrri, A.; DiMaio, D. Human papillomavirus in cervical and head-and-neck cancer. Nat. Clin. Pr. Oncol. 2008, 5, 24–31. [Google Scholar] [CrossRef]
- Hausen, H. Human papillomavirus & cervical cancer. Indian J. Med. Res. 2009, 130, 209. [Google Scholar]
- Hausen, H.Z. Papillomaviruses in the causation of human cancers—A brief historical account. Virology 2009, 384, 260–265. [Google Scholar] [CrossRef]
- Niedobitek, G.; Pitteroff, S.; Herbst, H.; Shepherd, P.; Finn, T.; Anagnostopoulos, I.; Stein, H. Detection of human papillomavirus type 16 DNA in carcinomas of the palatine tonsil. J. Clin. Pathol. 1990, 43, 918–921. [Google Scholar] [CrossRef] [PubMed]
- Begum, S. Tissue Distribution of human papillomavirus 16 DNA integration in patients with tonsillar carcinoma. Clin. Cancer Res. 2005, 11, 5694–5699. [Google Scholar] [CrossRef] [PubMed]
- Bodelon, C.; Untereiner, M.E.; Machiela, M.J.; Vinokurova, S.; Wentzensen, N. Genomic characterization of viral integration sites in HPV-related cancers. Int. J. Cancer 2016, 139, 2001–2011. [Google Scholar] [CrossRef] [PubMed]
- Brant, A.C.; Menezes, A.N.; Felix, S.P.; De Almeida, L.M.; Sammeth, M.; Moreira, M.; Ângelo, M.; De Almeida, L.M. Characterization of HPV integration, viral gene expression and E6E7 alternative transcripts by RNA-Seq: A descriptive study in invasive cervical cancer. Genomics 2019, 111, 1853–1861. [Google Scholar] [CrossRef] [PubMed]
- Dall, K.L.; Scarpini, C.G.; Roberts, I.; Williamson, D.M.; Stanley, M.A.; Muralidhar, B.; Herdman, M.T.; Pett, M.R.; Coleman, N. Characterization of naturally occurring HPV16 integration sites isolated from cervical keratinocytes under noncompetitive conditions. Cancer Res. 2008, 68, 8249–8259. [Google Scholar] [CrossRef]
- Li, W.; Tian, S.; Wang, P.; Zang, Y.; Chen, X.; Yao, Y.; Li, W. The characteristics of HPV integration in cervical intraepithelial cells. J. Cancer 2019, 10, 2783–2787. [Google Scholar] [CrossRef]
- Cheung, J.L.; Cheung, T.H.; Yu, M.Y.; Chan, P.K. Virological characteristics of cervical cancers carrying pure episomal form of HPV16 genome. Gynecol. Oncol. 2013, 131, 374–379. [Google Scholar] [CrossRef]
- De La Cruz-Hernández, E.; Perez-Cardenas, E.; Contreras-Paredes, A.; Cantú, D.; Mohar-Betancourt, A.; Lizano, M.; Duenas-Gonzalez, A. The effects of DNA methylation and histone deacetylase inhibitors on human papillomavirus early gene expression in cervical cancer, an in vitro and clinical study. Virol. J. 2007, 4, 18. [Google Scholar] [CrossRef]
- Zhang, C.; Deng, Z.; Pan, X.; Uehara, T.; Suzuki, M.; Xie, M. Effects of methylation status of CpG Sites within the HPV16 long control region on HPV16-positive head and neck cancer cells. PLoS ONE 2015, 10, e0141245. [Google Scholar] [CrossRef]
- Bhattacharjee, B.; Sengupta, S. CpG methylation of HPV 16 LCR at E2 binding site proximal to P97 is associated with cervical cancer in presence of intact E2. Virology 2006, 354, 280–285. [Google Scholar] [CrossRef]
- Reuschenbach, M.; Huebbers, C.U.; Prigge, E.-S.; Bermejo, J.L.; Kalteis, M.S.; Preuss, S.F.; Seuthe, I.M.; Kolligs, J.; Speel, E.J.M.; Olthof, N.; et al. Methylation status of HPV16 E2-binding sites classifies subtypes of HPV-associated oropharyngeal cancers. Cancer 2015, 121, 1966–1976. [Google Scholar] [CrossRef] [PubMed]
- Villiers, E.M.; Wagner, D.; Schneider, A.; Wesch, H.; Miklaw, H.; Wahrendorf, J.; Papendick, U.; Hausen, H. Human papillomavirus infections in women with and without abnormal cervical cytology. Lancet 1987, 330, 703–706. [Google Scholar] [CrossRef]
- Rous, P.; Beard, J.W. A virus-induced mammalian growth with the characters of a tumor (the shope rabbit papilloma). J. Exp. Med. 1934, 60, 741–766. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Winkelstein, W. Smoking and cancer of the uterine cerVIX: Hypothesis. Am. J. Epidemiol. 1977, 106, 257–259. [Google Scholar] [CrossRef]
- Kim, M.S.; Shin, K.H.; Baek, J.H.; Cherrick, H.M.; Park, N.H. HPV-16, tobacco-specific N-nitrosamine, and N-methyl-N’-nitro-N-nitrosoguanidine in oral carcinogenesis. Cancer Res. 1993, 53, 4811–4816. [Google Scholar]
- Gunnell, A.S.; Tran, T.N.; Torrång, A.; Dickman, P.W.; Sparén, P.; Palmgren, J.; Ylitalo, N. synergy between cigarette smoking and human papillomavirus type 16 in cervical cancer In situ Development. Cancer Epidemiol. Biomark. Prev. 2006, 15, 2141–2147. [Google Scholar] [CrossRef]
- Al-Zalabani, A.H. Cancer incidence attributable to tobacco smoking in GCC countries in 2018. Tob. Induc. Dis. 2020, 18, 18. [Google Scholar] [CrossRef]
- Louie, K.S.; Castellsagué, X.; De Sanjose, S.; Herrero, R.; Meijer, C.J.; Shah, K.; Muñoz, N.; Bosch, F. For the international agency for research on cancer multicenter cervical cancer study group smoking and passive smoking in cervical cancer risk: Pooled analysis of couples from the IARC multicentric case-control studies. Cancer Epidemiol. Biomark. Prev. 2011, 20, 1379–1390. [Google Scholar] [CrossRef]
- Plummer, M.; Herrero, R.; Franceschi, S.; Meijer, C.J.; Snijders, P.; Bosch, F.; De Sanjosé, S.; Muñoz, N. IARC multi-centre cervical cancer study group smoking and cervical cancer: Pooled analysis of the IARC multi-centric case–control study. Cancer Causes Control. 2003, 14, 805–814. [Google Scholar] [CrossRef]
- IARC. Tobacco Smoking and Tobacco Smoke. IARC Monographs on the Evaluation of the Carcinogenic Risks of Chemicals to Humans; IARCPress: Lyon, France, 2004. [Google Scholar]
- Hang, B. Formation and repair of tobacco carcinogen-derived bulky DNA adducts. J. Nucleic Acids 2010, 2010, 1–29. [Google Scholar] [CrossRef]
- Melikian, A.A.; Sun, P.; Prokopczyk, B.; El-Bayoumy, K.; Hoffmann, D.; Wang, X.; Waggoner, S. Identification of benzo[a]pyrene metabolites in cervical mucus and DNA adducts in cervical tissues in humans by gas chromatography-mass spectrometry. Cancer Lett. 1999, 146, 127–134. [Google Scholar] [CrossRef]
- Prokopczyk, B.; Cox, J.E.; Hoffmann, D.; Steven, E.S.E. Identification of tobacco specific carcinogen in the cervical mucus of smokers and nonsmokers. J. Natl. Cancer Inst. 1997, 89, 868–873. [Google Scholar] [CrossRef]
- Alam, S.; Conway, M.J.; Chen, H.-S.; Meyers, C. The cigarette smoke carcinogen benzo[a]pyrene enhances human papillomavirus synthesis. J. Virol. 2007, 82, 1053–1058. [Google Scholar] [CrossRef] [PubMed]
- Bowser, B.S.; Alam, S.; Meyers, C. Treatment of a human papillomavirus type 31b-positive cell line with benzo[a]pyrene increases viral titer through activation of the Erk1/2 signaling pathway. J. Virol. 2011, 85, 4982–4992. [Google Scholar] [CrossRef] [PubMed]
- Schiffman, M.; Adrianza, E. ALTS group ASCUS-LSIL triage study. Acta Cytol. 2000, 44, 726–742. [Google Scholar] [CrossRef]
- Xi, L.F.; Koutsky, L.A.; Castle, P.E.; Edelstein, Z.R.; Meyers, C.; Ho, J.; Schiffman, M. Relationship between cigarette smoking and human papilloma virus types 16 and 18 DNA load. Cancer Epidemiol. Biomark. Prev. 2009, 18, 3490–3496. [Google Scholar] [CrossRef]
- Castle, E.P.; Meyers, C.; Alam, S.; Conway, M.J. How Does tobacco smoke contribute to cervical carcinogenesis? J. Virol. 2008, 82, 6084–6086. [Google Scholar] [CrossRef]
- Ndisang, D.; Khan, A.; Lorenzato, F.; Sindos, M.; Singer, A.; Latchman, D.S. The cellular transcription factor Brn-3a and the smoking-related substance nicotine interact to regulate the activity of the HPV URR in the cervix. Oncogene 2010, 29, 2701–2711. [Google Scholar] [CrossRef][Green Version]
- Maher, D.M.; Bell, M.C.; O’Donnell, E.A.; Gupta, B.K.; Jaggi, M.; Chauhan, S.C. Curcumin suppresses human papillomavirus oncoproteins, restores p53, rb, and ptpn13 proteins and inhibits benzo[a]pyrene-induced upregulation of HPV E7. Mol. Carcinog. 2010, 50, 47–57. [Google Scholar] [CrossRef]
- Wei, L.; Griego, A.M.; Chu, M.; Ozbun, M.A. Tobacco exposure results in increased E6 and E7 oncogene expression, DNA damage and mutation rates in cells maintaining episomal human papillomavirus 16 genomes. Carcinogenesis 2014, 35, 2373–2381. [Google Scholar] [CrossRef]
- Peña, N.; Carrillo, D.; Muñoz, J.P.; Chnaiderman, J.; Urzúa, U.; Leon, O.; Tornesello, M.L.; Corvalan, A.; Rifo, R.S.; Aguayo, F. Tobacco smoke activates human papillomavirus 16 p97 promoter and cooperates with high-risk E6/E7 for oxidative DNA damage in lung cells. PLoS ONE 2015, 10, e0123029. [Google Scholar] [CrossRef] [PubMed]
- Muñoz, J.P.; Carrillo-Beltrán, D.; Aedo-Aguilera, V.; Calaf, G.M.; León, O.; Maldonado, E.; Tapia, J.C.; Boccardo, E.; Ozbun, M.A.; Aguayo, F. Tobacco exposure enhances human papillomavirus 16 oncogene expression via EGFR/PI3K/Akt/c-Jun signaling pathway in cervical cancer Cells. Front. Microbiol. 2018, 9. [Google Scholar] [CrossRef]
- Li, Y.T.; He, B.; Wang, Y.Z. Exposure to cigarette smoke upregulates AP-1 activity and induces TNF-alpha overexpression in mouse lungs. Inhal. Toxicol. 2009, 21, 641–647. [Google Scholar] [CrossRef] [PubMed]
- Swenson, W.G.; Wuertz, B.R.K.; Ondrey, F.G. Tobacco carcinogen mediated up-regulation of AP-1 dependent pro-angiogenic cytokines in head and neck carcinogenesis. Mol. Carcinog. 2011, 50, 668–679. [Google Scholar] [CrossRef]
- Liu, Y.; Li, J.Z.; Yuan, X.H.; Adler-Storthz, K.; Chen, Z. An AP-1 binding site mutation in HPV-16 LCR enhances E6/E7 promoter activity in human oral epithelial Cells. Virus Genes 2002, 24, 29–37. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Storthz, K.A.; Shillitoe, E.J. Mutations in the long control region of human papillomavirus DNA in oral cancer cells, and their functional consequences. Cancer Res. 1997, 57, 1614–1619. [Google Scholar]
- Geng, H.; Zhao, L.; Liang, Z.; Zhang, Z.; Xie, D.; Bi, L.; Wang, Y.; Zhang, T.; Cheng, L.; Yu, D.; et al. Cigarette smoke extract-induced proliferation of normal human urothelial cells via the MAPK/AP-1 pathway. Oncol. Lett. 2016, 13, 469–475. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Zhong, C.Y.; Zhou, Y.M.; Douglas, G.C.; Witschi, H.; Pinkerton, K.E. MAPK/AP-1 signal pathway in tobacco smoke-induced cell proliferation and squamous metaplasia in the lungs of rats. Carcinogenesis 2005, 26, 2187–2195. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Geng, H.; Zhao, L.; Zhang, Z.; Xie, D.; Zhang, T.; Min, J.; Yu, D.; Zhong, C. Role of AP-1 in the tobacco smoke-induced urocystic abnormal cell differentiation and epithelial-mesenchymal transition in vivo. Int J. Clin. Exp. Pathol 2017, 10, 8243–8252. [Google Scholar]
- Rahman, I.; Antonicelli, F.; MacNee, W. Molecular mechanism of the regulation of glutathione synthesis by tumor necrosis factor-α and dexamethasone in human alveolar epithelial cells. J. Biol. Chem. 1999, 274, 5088–5096. [Google Scholar] [CrossRef]
- Rahman, I.; Smith, C.A.; Antonicelli, F.D.; MacNee, W. Characterisation of γ-glutamylcysteine synthethase-heavy subunit promoter: A critical role for AP-1. FEBS Lett. 1998, 427, 129–133. [Google Scholar] [CrossRef]
- Marwick, J.A.; Kirkham, P.A.; Stevenson, C.S.; Danahay, H.; Giddings, J.; Butler, K.; Donaldson, K.; MacNee, W.; Rahman, I. Cigarette smoke alters chromatin remodeling and induces proinflammatory genes in rat lungs. Am. J. Respir. Cell Mol. Biol. 2004, 31, 633–642. [Google Scholar] [CrossRef] [PubMed]
- Filosto, S.; Becker, C.R.; Goldkorn, T. Cigarette smoke induces aberrant EGF receptor activation that mediates lung cancer development and resistance to tyrosine kinase inhibitors. Mol. Cancer Ther. 2012, 11, 795–804. [Google Scholar] [CrossRef] [PubMed]
- Petecchia, L.; Sabatini, F.; Varesio, L.; Camoirano, A.; Usai, C.; Pezzolo, A.; Rossi, G.A. Bronchial airway epithelial cell damage following exposure to cigarette smoke includes disassembly of tight junction components mediated by the extracellular signal-regulated kinase 1/2 pathway. Chest 2009, 135, 1502–1512. [Google Scholar] [CrossRef]
- Mercer, B.A.; D’Armiento, J.M. Emerging role of MAP kinase pathways as therapeutic targets in COPD. Int. J. Chronic Obstr. Pulm. Dis. 2006, 1, 137–150. [Google Scholar] [CrossRef]
- Sekine, T.; Hirata, T.; Ishikawa, S.; Ito, S.; Ishimori, K.; Matsumura, K.; Muraki, K. Regulation of NRF2, AP-1 and NF-κB by cigarette smoke exposure in three-dimensional human bronchial epithelial cells. J. Appl. Toxicol. 2018, 39, 717–725. [Google Scholar] [CrossRef]
- Zhang, Q.; Adiseshaiah, P.; Reddy, S.P. Matrix metalloproteinase/epidermal growth factor receptor/mitogen-activated protein kinase signaling regulatefra-1induction by cigarette smoke in lung epithelial cells. Am. J. Respir. Cell Mol. Biol. 2005, 32, 72–81. [Google Scholar] [CrossRef]
- Liu, M.; Zhou, C.; Zheng, J. Cigarette smoking impairs the response of EGFR-TKIs therapy in lung adenocarcinoma patients by promoting EGFR signaling and epithelial-mesenchymal transition. Am. J. Transl. Res. 2015, 7, 2026–2035. [Google Scholar]
- Hu, X.; Peng, N.; Qi, F.; Li, J.; Shi, L.; Chen, R. Cigarette smoke upregulates SPRR3 by favoring c-Jun/Fra1 heterodimerization in human bronchial epithelial cells. Future Oncol. 2018, 14, 2599–2613. [Google Scholar] [CrossRef]
- Giuliano, A.R.; Sedjo, R.L.; Roe, D.J.; Harri, R.; Baldwi, S.; Papenfuss, M.R.; Abrahamsen, M.; Inserra, P. Clearance of oncogenic human papillomavirus (HPV) infection: Effect of smoking (United States). Cancer Causes Control 2002, 13, 839–846. [Google Scholar] [CrossRef]
- Koshiol, J.; Schroeder, J.; Jamieson, D.J.; Marshall, S.; Duerr, A.; Heilig, C.M.; Shah, K.V.; Klein, R.S.; Cu-Uvin, S.; Schuman, P.; et al. Smoking and time to clearance of human papillomavirus infection in hiv-seropositive and HIV-seronegative women. Am. J. Epidemiol. 2006, 164, 176–183. [Google Scholar] [CrossRef] [PubMed]
- Qiu, F.; Liang, C.L.; Liu, H.; Zeng, Y.Q.; Hou, S.; Huang, S.; Lai, X.; Dai, Z. Impacts of cigarette smoking on immune responsiveness: Up and down or upside down? Oncotarget 2016, 8, 268–284. [Google Scholar] [CrossRef] [PubMed]
- Ferson, M.; Edwards, A.; Lind, A.; Milton, G.W.; Hersey, P. Low natural killer-cell activity and immunoglobulin levels associated with smoking in human subjects. Int. J. Cancer 1979, 23, 603–609. [Google Scholar] [CrossRef] [PubMed]
- Holt, P.G.; Keast, D. Environmentally induced changes in immunological function: Acute and chronic effects of inhalation of tobacco smoke and other atmospheric contaminants in man and experimental animals. Bacteriol. Rev. 1977, 41, 205–216. [Google Scholar] [CrossRef]
- Poppe, W.A.; Ide, P.S.; Drijkoningen, M.P.; Lauweryns, J.M.; Van Assche, A. Tobacco Smoking Impairs the Local Immunosurveillance in the Uterine Cervix. Gynecol. Obstet. Investig. 1995, 39, 34–38. [Google Scholar] [CrossRef]
- Szarewski, A.; Maddox, P.; Royston, P.; Jarvis, M.; Anderson, M.; Guillebaud, J.; Cuzick, J. The effect of stopping smoking on cervical Langerhans’ cells and lymphocytes. BJOG: Int. J. Obstet. Gynaecol. 2001, 108, 295–303. [Google Scholar]
- Miller, L.G.; Goldstein, G.; Murphy, M.; Ginns, L.C. Reversible alterations in immunoregulatory T cells in smoking. Chest 1982, 82, 526–529. [Google Scholar] [CrossRef]
- Geng, Y.; Savage, S.M.; Razani-Boroujerdi, S.; Sopori, M.L. Effects of nicotine on the immune response. II. Chronic nicotine treatment induces T cell anergy. J. Immunol. 1996, 156, 2384–2390. [Google Scholar]
- Geng, Y.; Savage, S.; Johnson, L.; Seagrave, J.; Sopori, M. Effects of nicotine on the immune response. i. chronic exposure to nicotine impairs antigen receptor-mediated signal transduction in lymphocytes. Toxicol. Appl. Pharmacol. 1995, 135, 268–278. [Google Scholar] [CrossRef]
- Wang, C.; Gu, W.; Zhang, Y.; Ji, Y.; Wen, Y.; Xu, X. Nicotine promotes cervical carcinoma cell line HeLa migration and invasion by activating PI3k/Akt/NF-κB pathway in vitro. Exp. Toxicol. Pathol. 2017, 69, 402–407. [Google Scholar] [CrossRef]
- Lee, W.K.; Ramanathan, M.; Spannhake, E.W.; Lane, A.P. The cigarette smoke component acrolein inhibits expression of the innate immune components IL-8 and human Beta-Defensin 2 by Sinonasal Epithelial cells. Am. J. Rhinol. 2007, 21, 658–663. [Google Scholar] [CrossRef] [PubMed]
- Fueldner, C.; Kohlschmidt, J.; Riemschneider, S.; Schulze, F.; Zoldan, K.; Esser, C.; Hauschildt, S.; Lehmann, J. Benzo(a)pyrene attenuates the pattern-recognition-receptor induced proinflammatory phenotype of murine macrophages by inducing IL-10 expression in an aryl hydrocarbon receptor-dependent manner. Toxicology 2018, 409, 80–90. [Google Scholar] [CrossRef] [PubMed]
- Chu, M.; Guo, J.; Chen, C.Y. Long-term Exposure to nicotine, via ras pathway, induces cyclin D1 to stimulate G1Cell cycle transition. J. Biol. Chem. 2004, 280, 6369–6379. [Google Scholar] [CrossRef] [PubMed]
- Phillips, D.H.; Schoket, B.; Hewer, A.; Grover, P.L. Human DNA adducts due to smoking and other exposures to carcinogens. Prog. Clin. Biol. Res. 1990, 283–292. [Google Scholar]
- Phillips, D.H.; Schoket, B.; Hewer, A.; Bailey, E.; Kostic, S.; Vincze, I. Influence of cigarette smoking on the levels of DNA adducts in human bronchial epithelium and white blood cells. Int. J. Cancer 1990, 46, 569–575. [Google Scholar] [CrossRef]
- Starek, A.; Podolak, I. Carcinogenic effect of tobacco smoke. Roczniki Państwowego Zakładu Higieny 2009, 60, 299–310. [Google Scholar]
- Trushin, N.; Alam, S.; El-Bayoumy, K.; Krzeminski, J.; Amin, S.G.; Gullett, J.; Meyers, C.; Prokopczyk, B. Comparative metabolism of benzo[a]pyrene by human keratinocytes infected with high-risk human papillomavirus types 16 and 18 as episomal or integrated genomes. J. Carcinog. 2012, 11, 1. [Google Scholar] [CrossRef]
- Gupta, R.C.; Moktar, A.; Ravoori, S.; Vadhanam, M.V.; Gairola, C.G. Cigarette smoke-induced DNA damage and repair detected by the comet assay in HPV-transformed cervical cells. Int. J. Oncol. 2009, 35, 1297–1304. [Google Scholar] [CrossRef][Green Version]
- Gupta, R.C.; Moktar, A.; Singh, R.; Vadhanam, M.V.; Ravoori, S.; Lillard, J.W.; Gairola, C.G. Cigarette smoke condensate-induced oxidative DNA damage and its removal in human cervical cancer cells. Int. J. Oncol. 2011, 39, 941–947. [Google Scholar] [CrossRef]
- Chen, B.; Simpson, D.A.; Zhou, Y.; Mitra, A.; Mitchell, D.L.; Cordeiro-Stone, M.; Kaufmann, W.K. Human papilloma virus type16 E6 deregulates CHK1 and sensitizes human fibroblasts to environmental carcinogens independently of its effect on p53. Cell Cycle 2009, 8, 1775–1787. [Google Scholar] [CrossRef]
- Westra, W.H.; Taube, J.M.; Poeta, M.L.; Begum, S.; Sidransky, D.; Koch, W.M. Inverse relationship between human papillomavirus-16 infection and disruptive p53 gene mutations in squamous cell carcinoma of the head and neck. Clin. Cancer Res. 2008, 14, 366–369. [Google Scholar] [CrossRef] [PubMed]
- Busby-Earle, R.M.; Steel, C.M.; Williams, A.R.; Cohen, B.; Bird, C.C. p53 mutations in cervical carcinogenesis–low frequency and lack of correlation with human papillomavirus status. Br. J. Cancer 1994, 69, 732–737. [Google Scholar] [CrossRef] [PubMed]
- Brosh, R.; Rotter, V. When mutants gain new powers: News from the mutant p53 field. Nat. Rev. Cancer 2009, 9, 701–713. [Google Scholar] [CrossRef] [PubMed]
- Jamaly, S.; Khanehkenari, M.R.; Rao, R.; Patil, G.; Thakur, S.; Ramaswamy, P.; Ajaikumar, B.S.; Sahoo, R. Relationship between p53 overexpression, human papillomavirus infection, and lifestyle in Indian patients with head and neck cancers. Tumor Biol. 2012, 33, 543–550. [Google Scholar] [CrossRef]
- Muñoz, J.P.; González, C.; Parra, B.; Corvalan, A.; Tornesello, M.L.; Eizuru, Y.; Aguayo, F. Functional interaction between human papillomavirus type 16 E6 and E7 oncoproteins and cigarette smoke components in lung epithelial cells. PLoS ONE 2012, 7, e38178. [Google Scholar] [CrossRef]
- Chen, D.; Fang, L.; Li, H.; Tang, M.S.; Jin, C. Cigarette smoke component acrolein modulates chromatin assembly by inhibiting histone acetylation*. J. Biol. Chem. 2013, 288, 21678–21687. [Google Scholar] [CrossRef]
- Doorbar, J. Papillomavirus life cycle organization and biomarker selection. Dis. Markers 2007, 23, 297–313. [Google Scholar] [CrossRef]
- Alam, S.; Bowser, B.S.; Conway, M.J.; Israr, M.; Ryndock, E.J.; Xi, L.F.; Meyers, C. Downregulation of Cdc2/CDK1 kinase activity induces the synthesis of noninfectious human papillomavirus type 31b virions in organotypic tissues exposed to benzo[a]pyrene. J. Virol. 2010, 84, 4630–4645. [Google Scholar] [CrossRef]
- Zhang, W.; Liu, Y.; Zhao, N.; Chen, H.; Qiao, L.; Zhao, W.; Chen, J.J. Role of Cdk1 in the p53-independent abrogation of the postmitotic checkpoint by human papillomavirus E6. J. Virol. 2014, 89, 2553–2562. [Google Scholar] [CrossRef]
- Wang, S.; Pang, T.; Gao, M.; Kang, H.; Ding, W.; Sun, X.; Zhao, Y.; Zhu, W.; Tang, X.; Yao, Y.; et al. HPV E6 induces eIF4E transcription to promote the proliferation and migration of cervical cancer. FEBS Lett. 2013, 587, 690–697. [Google Scholar] [CrossRef]
- Pang, T.; Wang, S.; Gao, M.; Kang, H.; Zhao, Y.; Yao, Y.; Hu, X. HPV18 E7 induces the over-transcription of eIF4E gene in cervical cancer. Iran. J. Basic Med. Sci 2015, 18, 684–690. [Google Scholar] [PubMed]
- Chen, L.; Wang, H. eIF4E is a critical regulator of human papillomavirus (HPV)-immortalized cervical epithelial (H8) cell growth induced by nicotine. Toxicology 2019, 419, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Wang, H. Nicotine promotes human papillomavirus (HPV)-immortalized cervical epithelial cells (H8) proliferation by activating RPS27a-Mdm2-P53 pathway in vitro. Toxicol. Sci. 2018, 167, 408–418. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.M.; Cheng, Y.W.; Wang, Y.C.; Wu, T.C.; Chen, C.Y.; Lee, H. Up-regulation of FOXM1 by E6 oncoprotein through the MZF1/NKX2-1 axis is required for human papillomavirus-associated tumorigenesis. Neoplasia 2014, 16, 961–971. [Google Scholar] [CrossRef] [PubMed]
- Lepore, S.; Lettini, G.; Condelli, V.; Sisinni, L.; Piscazzi, A.; Simeon, V.; Zoppoli, P.; Pedicillo, M.C.; Natalicchio, M.I.; Pietrafesa, M.; et al. comparative gene expression profiling of tobacco-associated HPV-positive versus negative oral squamous carcinoma cell lines. Int. J. Med. Sci. 2020, 17, 112–124. [Google Scholar] [CrossRef]
- Gelbman, B.D.; Heguy, A.; O’Connor, T.P.; Zabner, J.; Crystal, R.G. Upregulation of pirin expression by chronic cigarette smoking is associated with bronchial epithelial cell apoptosis. Respir. Res. 2007, 8, 10. [Google Scholar] [CrossRef]
- Carrillo-Beltrán, D.; Muñoz, J.P.; Guerrero-Vásquez, N.; Blanco, R.; León, O.; Lino, V.D.S.; Tapia, J.C.; Maldonado, E.; Dubois-Camacho, K.; Hermoso, M.A.; et al. Human papillomavirus 16 E7 promotes EGFR/PI3K/AKT1/NRF2 signaling pathway contributing to PIR/NF-κB activation in oral cancer cells. Cancers 2020, 12, 1904. [Google Scholar] [CrossRef]
- Rangasamy, T.; Cho, C.Y.; Thimmulappa, R.K.; Zhen, L.; Srisuma, S.S.; Kensler, T.W.; Yamamoto, M.; Petrache, I.; Tuder, R.M.; Biswal, S. Genetic ablation of Nrf2 enhances susceptibility to cigarette smoke-induced emphysema in mice. J. Clin. Investig. 2004, 114, 1248–1259. [Google Scholar] [CrossRef]
- Kontostathi, G.; Zoidakis, J.; Makridakis, M.; Lygirou, V.; Mermelekas, G.; Papadopoulos, T.; Vougas, K.; Vlamis-Gardikas, A.; Drakakis, P.; Loutradis, D.; et al. Cervical cancer cell line secretome highlights the roles of transforming growth factor-beta-induced protein ig-h3, peroxiredoxin-2, and nrf2 on cervical carcinogenesis. BioMed Res. Int. 2017, 2017, 4180703–4180715. [Google Scholar] [CrossRef]
- Cicchini, L.; Westrich, J.A.; Xu, T.; Vermeer, D.W.; Berger, J.N.; Clambey, E.T.; Lee, D.; Song, J.I.; Lambert, P.F.; Greer, R.O.; et al. Suppression of antitumor immune responses by human papillomavirus through epigenetic downregulation of CXCL14. mBio 2016, 7, e00270-16. [Google Scholar] [CrossRef]
- Parsanejad, R.; Fields, W.; Steichen, T.J.; Bombick, B.R.; Doolittle, D.J. Distinct regulatory profiles of interleukins and chemokines in response to cigarette smoke condensate in normal human bronchial epithelial (NHBE) cells. J. Interf. Cytokine Res. 2008, 28, 703–712. [Google Scholar] [CrossRef] [PubMed]
- Martínez-García, E.; Irigoyen, M.; González-Moreno, Ó.; Corrales, L.; Teijeira, A.; Salvo, E.; Rouzaut, A. Repetitive nicotine exposure leads to a more malignant and metastasis-prone phenotype of SCLC: A molecular insight into the importance of quitting smoking during treatment. Toxicol. Sci. 2010, 116, 467–476. [Google Scholar] [CrossRef]
- Meuris, F.; Carthagena, L.; Jaracz-Ros, A.; Gaudin, F.; Cutolo, P.; Deback, C.; Xue, Y.; Thierry, F.; Doorbar, J.; Bachelerie, F. The CXCL12/CXCR4 signaling pathway: A new susceptibility factor in human papillomavirus pathogenesis. PLOS Pathog. 2016, 12, e1006039. [Google Scholar] [CrossRef] [PubMed]
- Hatterschide, J.; Bohidar, A.E.; Grace, M.; Nulton, T.J.; Kim, H.W.; Windle, B.; Morgan, I.M.; Munger, K.; White, E.A. PTPN14 degradation by high-risk human papillomavirus E7 limits keratinocyte differentiation and contributes to HPV-mediated oncogenesis. Proc. Natl. Acad. Sci. USA 2019, 116, 7033–7042. [Google Scholar] [CrossRef] [PubMed]
- Solanki, H.S.; Advani, J.; Khan, A.A.; Radhakrishnan, A.; Sahasrabuddhe, N.A.; Pinto, S.M.; Chang, X.; Prasad, T.S.K.; Mathur, P.P.; Sidransky, D.; et al. Chronic cigarette smoke mediated global changes in lung mucoepidermoid cells: A phosphoproteomic analysis. OMICS J. Integr. Biol. 2017, 21, 474–487. [Google Scholar] [CrossRef] [PubMed]
| Molecule | Effect | Cell Line | Ref. |
|---|---|---|---|
| Tobacco Smoke Affects HPV Replication | |||
| BaP | Increases number of virions and genomes of HPV31 | CIN (CIN-612 9E) | [94] |
| BaP | Increases number of virions of HPV31 by MAPK ERK1/2 pathway | CIN (CIN-612 9E) | [95] |
| Tobacco Smoke Promotes HPV E6/E7 Expression | |||
| Nicotine | Promotes indirectly HPV16 E6 and E7 expression | CIN1, CIN2, CIN3 | [99] |
| and cervical cancer | |||
| BaP | Increases HPV16 E7 expression | Cervical carcinoma (CaSki) | [100] |
| CSE | Increases E6 and E7 expression in cells maintaining episomal HPV16 genomes | CIN1 | [101] |
| (W12 and CIN612) | |||
| CSE | Increases tumor properties in cells expressing HPV16 E6 and E7 | Lung adenocarcinoma (A549) | [146] |
| Lung carcinoma (A549), | |||
| CSE | Induces HPV16 p97 promoter activation | bronquial carcinoma (H-2170), | [102] |
| bronquial (BEAS-2B), alveolar (NL-20), | |||
| cervical carcinoma (CaSki and SiHa) | |||
| CSE | Promotes mutation that favors AP-1 binding to HPV16 LCR, increasing the activity of p97 promoter | Oral keratinocyte | [106] |
| (16BNNK) | |||
| CSE | Increases HPV16 E6 and E7 through p97 promoter activation involving EGFR/PI3K/Akt/C-Jun signaling pathway | Cervical carcinoma | [103] |
| (CaSki and SiHa) | |||
| Tobacco Smoke Promotes DNA Damage | |||
| Nicotine | Generates adducts and actives Ras signaling pathway | Lung epithelial (LA4) | [134] |
| Acrolein | Remodels chromatin leading to oxidative stress responses | Bronchial epithelial (BEAS-2B), | [147] |
| Lung adenocarcinoma (A549) | |||
| CSE | Increases DNA damage in cells maintaining episomal HPV16 genomes | CIN1 | [101] |
| (W12 and CIN612) | |||
| Tobacco Smoke Affects Immune Responses | |||
| Nicotine | Induces T cell anergy | T cells | [129] |
| Nicotine | Promotes migration in HPV18 cells by activating | Cervical carcinoma | [131] |
| the PI3K/Akt/NF-κB pathway | (HeLa) | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aguayo, F.; Muñoz, J.P.; Perez-Dominguez, F.; Carrillo-Beltrán, D.; Oliva, C.; Calaf, G.M.; Blanco, R.; Nuñez-Acurio, D. High-Risk Human Papillomavirus and Tobacco Smoke Interactions in Epithelial Carcinogenesis. Cancers 2020, 12, 2201. https://doi.org/10.3390/cancers12082201
Aguayo F, Muñoz JP, Perez-Dominguez F, Carrillo-Beltrán D, Oliva C, Calaf GM, Blanco R, Nuñez-Acurio D. High-Risk Human Papillomavirus and Tobacco Smoke Interactions in Epithelial Carcinogenesis. Cancers. 2020; 12(8):2201. https://doi.org/10.3390/cancers12082201
Chicago/Turabian StyleAguayo, Francisco, Juan P. Muñoz, Francisco Perez-Dominguez, Diego Carrillo-Beltrán, Carolina Oliva, Gloria M. Calaf, Rances Blanco, and Daniela Nuñez-Acurio. 2020. "High-Risk Human Papillomavirus and Tobacco Smoke Interactions in Epithelial Carcinogenesis" Cancers 12, no. 8: 2201. https://doi.org/10.3390/cancers12082201
APA StyleAguayo, F., Muñoz, J. P., Perez-Dominguez, F., Carrillo-Beltrán, D., Oliva, C., Calaf, G. M., Blanco, R., & Nuñez-Acurio, D. (2020). High-Risk Human Papillomavirus and Tobacco Smoke Interactions in Epithelial Carcinogenesis. Cancers, 12(8), 2201. https://doi.org/10.3390/cancers12082201





