Primary Thromboprophylaxis in Ambulatory Pancreatic Cancer Patients Receiving Chemotherapy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
Abstract
1. Introduction
2. Results
2.1. Search Results and Study Characteristics
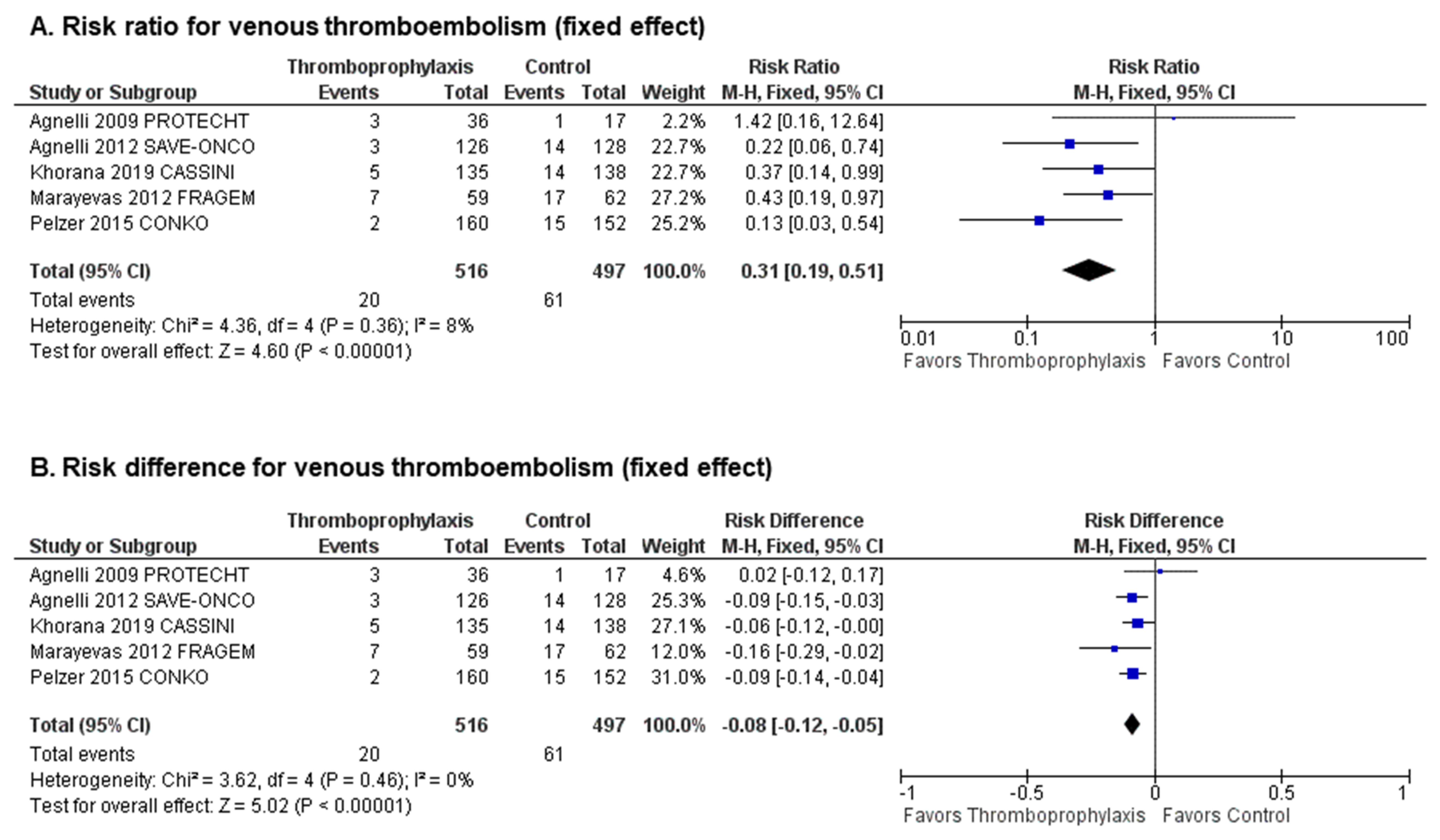
2.2. Efficacy of Primary Thromboprophylaxis with Anticoagulants
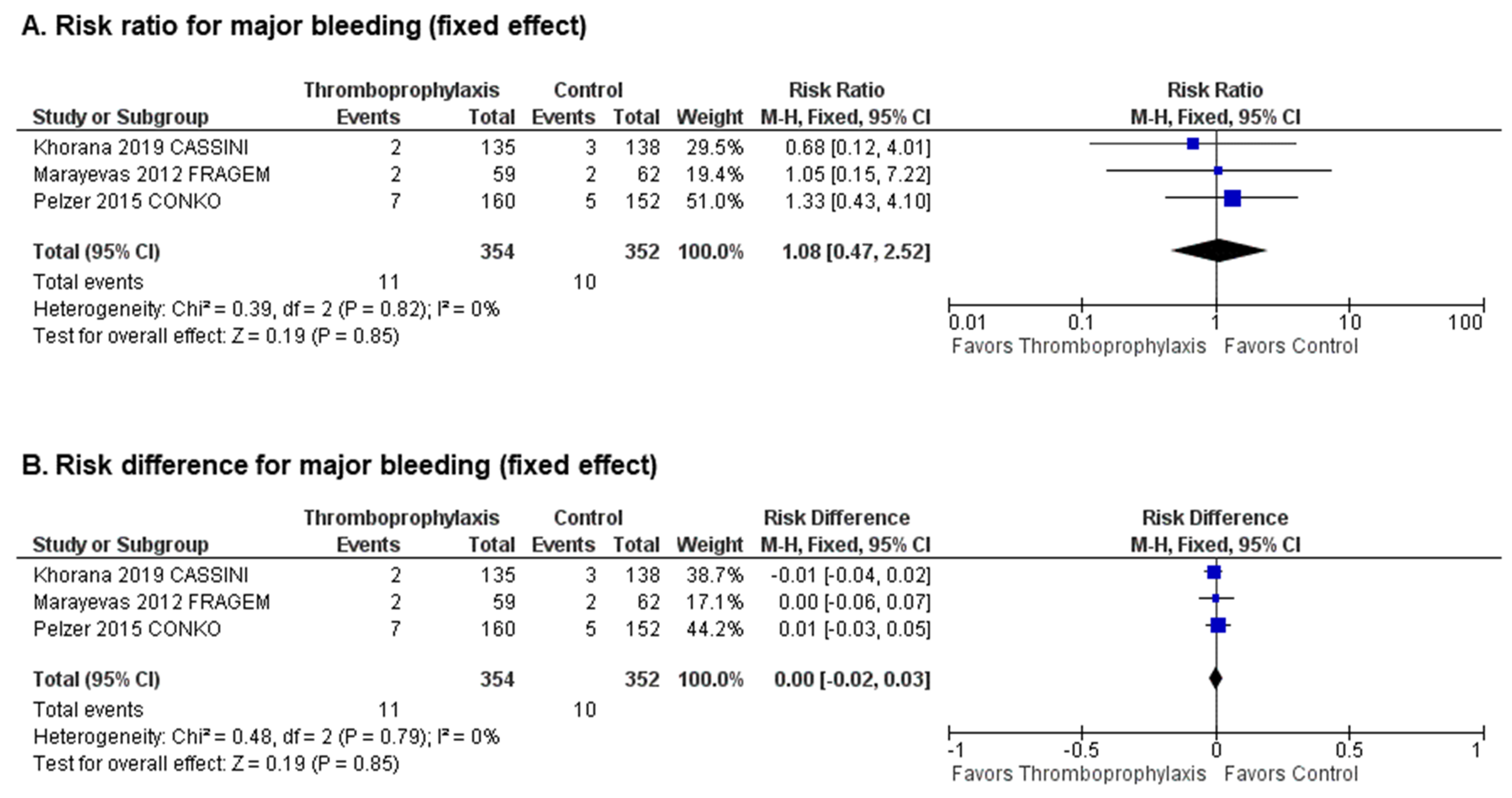
2.3. Safety of Primary Thromboprophylaxis with Anticoagulants
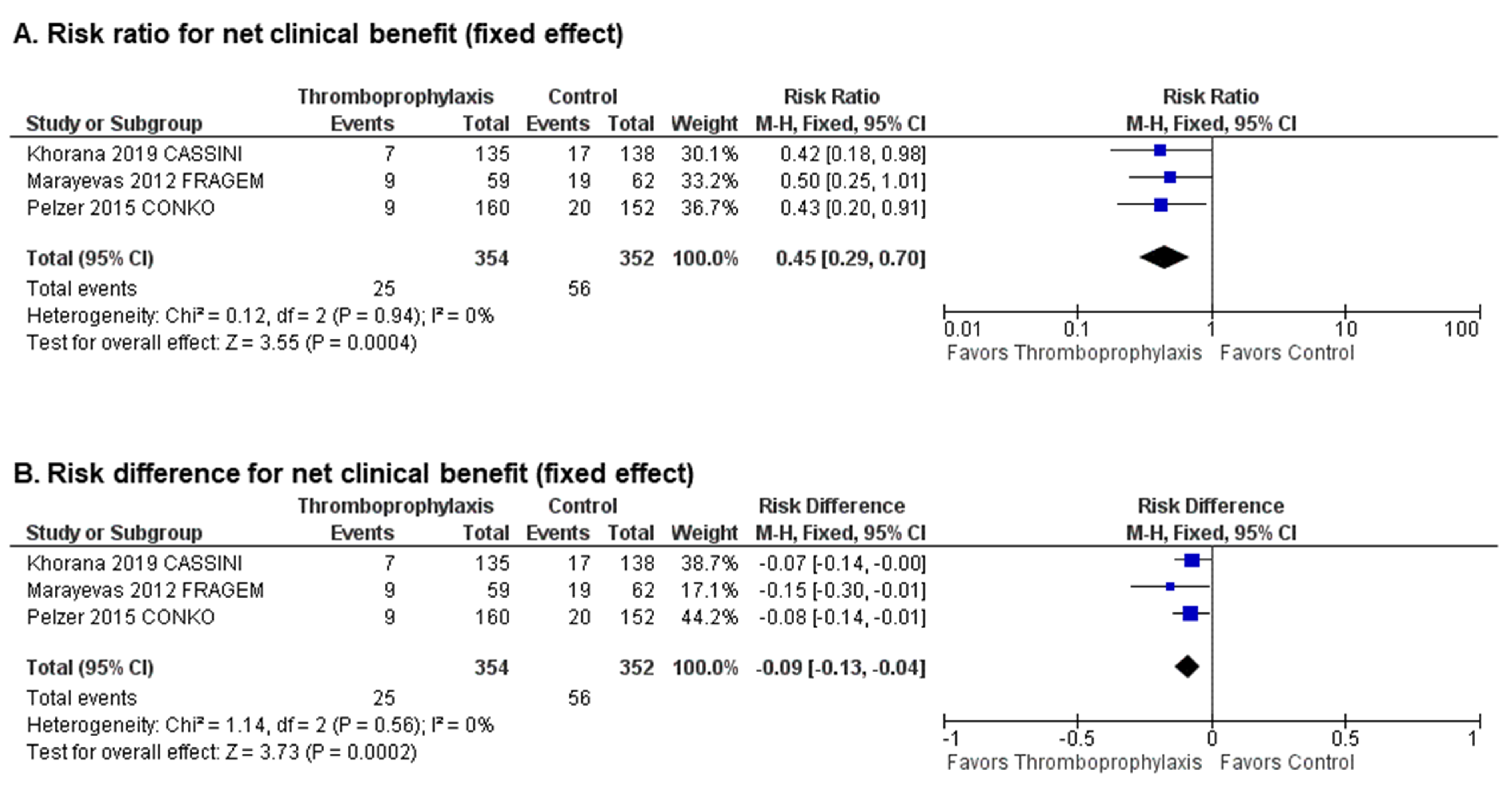
2.4. Net Clinical Benefit of Primary Thromboprophylaxis with Anticoagulants
3. Discussion
4. Materials and Methods
4.1. Study Objectives
4.2. Study Outcomes
4.3. Literature Search
4.4. Study Eligibility
4.5. Data Extraction
4.6. Study Quality and Assessment of Risk of Bias
4.7. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Horsted, F.; West, J.; Grainge, M.J. Risk of venous thromboembolism in patients with cancer: A systematic review and meta-analysis. PLoS Med. 2012, 9, e1001275. [Google Scholar] [CrossRef] [PubMed]
- Timp, J.F.; Braekkan, S.K.; Versteeg, H.H.; Cannegieter, S.C. Epidemiology of cancer-associated venous thrombosis. Blood 2013, 122, 1712–1723. [Google Scholar] [CrossRef] [PubMed]
- Blom, J.W.; Osanto, S.; Rosendaal, F.R. High risk of venous thrombosis in patients with pancreatic cancer: A cohort study of 202 patients. Eur. J. Cancer 2006, 42, 410–414. [Google Scholar] [CrossRef] [PubMed]
- Mandalà, M.; Reni, M.; Cascinu, S.; Barni, S.; Floriani, I.; Cereda, S.; Berardi, R.; Mosconi, S.; Torri, V.; Labianca, R. Venous thromboembolism predicts poor prognosis in irresectable pancreatic cancer patients. Ann. Oncol. 2007, 18, 1660–1665. [Google Scholar] [CrossRef]
- Mitry, E.; Taleb-Fayad, R.; Deschamps, A.; Mansencal, N.; Lepère, C.; Declety, G.; Lièvre, A.; Vaillant, J.-N.; Lesur, G.; Cramer, E.; et al. Risk of venous thrombosis in patients with pancreatic adenocarcinoma. Gastroenterol. Clin. Biol. 2007, 31, 1139–1142. [Google Scholar] [CrossRef]
- Oh, S.Y.; Kim, J.H.; Lee, K.-W.; Bang, S.-M.; Hwang, J.-H.; Oh, D.; Lee, J.S. Venous thromboembolism in patients with pancreatic adenocarcinoma: Lower incidence in Asian ethnicity. Thromb. Res. 2008, 122, 485–490. [Google Scholar] [CrossRef]
- Poruk, K.E.; Firpo, M.A.; Huerter, L.M.; Scaife, C.L.; Emerson, L.L.; Boucher, K.M.; Jones, K.A.; Mulvihill, S.J. Serum platelet factor 4 is an independent predictor of survival and venous thromboembolism in patients with pancreatic adenocarcinoma. Cancer Epidemiol. Biomarkers Prev. 2010, 19, 2605–2610. [Google Scholar] [CrossRef]
- Shaib, W.; Deng, Y.; Zilterman, D.; Lundberg, B.; Saif, M.W. Assessing risk and mortality of venous thromboembolism in pancreatic cancer patients. Anticancer Res. 2010, 30, 4261–4264. [Google Scholar]
- Epstein, A.S.; Soff, G.A.; Capanu, M.; Crosbie, C.; Shah, M.A.; Kelsen, D.P.; Denton, B.; Gardos, S.; O’Reilly, E.M. Analysis of incidence and clinical outcomes in patients with thromboembolic events and invasive exocrine pancreatic cancer. Cancer 2012, 118, 3053–3061. [Google Scholar] [CrossRef]
- Menapace, L.A.; Peterson, D.R.; Berry, A.; Sousou, T.; Khorana, A.A. Symptomatic and incidental thromboembolism are both associated with mortality in pancreatic cancer. Thromb. Haemost. 2011, 106, 371–378. [Google Scholar] [CrossRef]
- Afsar, C.U.; Gunaldi, M.; Kum, P.; Sahin, B.; Erkisi, M.; Kara, I.O.; Paydas, S.; Duman, B.B.; Ercolak, V.; Karaca, F.; et al. Pancreatic carcinoma, thrombosis and mean platelet volume: Single center experience from the southeast region of Turkey. Asian Pac. J. Cancer Prev. 2014, 15, 9143–9146. [Google Scholar] [CrossRef] [PubMed]
- Muñoz Martín, A.J.; García Alfonso, P.; Rupérez Blanco, A.B.; Pérez Ramírez, S.; Blanco Codesido, M.; Martín Jiménez, M. Incidence of venous thromboembolism (VTE) in ambulatory pancreatic cancer patients receiving chemotherapy and analysis of Khorana’s predictive model. Clin. Transl. Oncol. 2014, 16, 927–930. [Google Scholar] [CrossRef]
- Krepline, A.N.; Christians, K.K.; George, B.; Ritch, P.S.; Erickson, B.A.; Tolat, P.; Evans, D.B.; Tsai, S. Venous thromboembolism prophylaxis during neoadjuvant therapy for resectable and borderline resectable pancreatic cancer-Is it indicated? J. Surg. Oncol. 2016, 114, 581–586. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.-C.; Ro, Y.S.; Cho, J.; Park, Y.; Lee, J.H.; Hwang, J.-H.; Choi, H.J.; Lee, S. Characteristics of Venous Thromboembolism in Pancreatic Adenocarcinoma in East Asian Ethnics: A Large Population-Based Observational Study. Medicine 2016, 95, e3472. [Google Scholar] [CrossRef] [PubMed]
- Kruger, S.; Haas, M.; Burkl, C.; Goehring, P.; Kleespies, A.; Roeder, F.; Gallmeier, E.; Ormanns, S.; Westphalen, C.B.; Heinemann, V.; et al. Incidence, outcome and risk stratification tools for venous thromboembolism in advanced pancreatic cancer—A retrospective cohort study. Thromb. Res. 2017, 157, 9–15. [Google Scholar] [CrossRef]
- Van Es, N.; Franke, V.F.; Middeldorp, S.; Wilmink, J.W.; Büller, H.R. The Khorana score for the prediction of venous thromboembolism in patients with pancreatic cancer. Thromb. Res. 2017, 150, 30–32. [Google Scholar] [CrossRef]
- Berger, A.K.; Singh, H.M.; Werft, W.; Muckenhuber, A.; Sprick, M.R.; Trumpp, A.; Weichert, W.; Jäger, D.; Springfeld, C. High prevalence of incidental and symptomatic venous thromboembolic events in patients with advanced pancreatic cancer under palliative chemotherapy: A retrospective cohort study. Pancreatology 2017, 17, 629–634. [Google Scholar] [CrossRef]
- Chen, J.-S.; Hung, C.-Y.; Chang, H.; Liu, C.-T.; Chen, Y.-Y.; Lu, C.-H.; Chang, P.-H.; Hung, Y.-S.; Chou, W.-C. Venous Thromboembolism in Asian Patients with Pancreatic Cancer Following Palliative Chemotherapy: Low Incidence but a Negative Prognosticator for Those with Early Onset. Cancers 2018, 10, 501. [Google Scholar] [CrossRef]
- Kim, J.S.; Kang, E.J.; Kim, D.S.; Choi, Y.J.; Lee, S.Y.; Kim, H.J.; Seo, H.Y.; Kim, J.S. Early venous thromboembolism at the beginning of palliative chemotherapy is a poor prognostic factor in patients with metastatic pancreatic cancer: A retrospective study. BMC Cancer 2018, 18, 1260. [Google Scholar] [CrossRef]
- Ouaissi, M.; Frasconi, C.; Mege, D.; Panicot-Dubois, L.; Boiron, L.; Dahan, L.; Debourdeau, P.; Dubois, C.; Farge, D.; Sielezneff, I. Impact of venous thromboembolism on the natural history of pancreatic adenocarcinoma. Hepatobiliary Pancreat. Dis. Int. 2015, 14, 436–442. [Google Scholar] [CrossRef]
- Mikal, S.; Campbell, A.J.A. Carcinoma of the pancreas; diagnostic and operative criteria based on 100 consecutive autopsies. Surgery 1950, 28, 963–969. [Google Scholar] [PubMed]
- Frere, C.; Bournet, B.; Gourgou, S.; Fraisse, J.; Canivet, C.; Connors, J.M.; Buscail, L.; Farge, D. Incidence of Venous Thromboembolism in Patients with Newly Diagnosed Pancreatic Cancer and Factors Associated With Outcomes. Gastroenterology 2020, 158, 1346–1358.e4. [Google Scholar] [CrossRef] [PubMed]
- Farge, D.; Frere, C.; Connors, J.M.; Ay, C.; Khorana, A.A.; Munoz, A.; Brenner, B.; Kakkar, A.; Rafii, H.; Solymoss, S.; et al. 2019 international clinical practice guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer. Lancet Oncol. 2019, 20, e566–e581. [Google Scholar] [CrossRef]
- Key, N.S.; Khorana, A.A.; Kuderer, N.M.; Bohlke, K.; Lee, A.Y.Y.; Arcelus, J.I.; Wong, S.L.; Balaban, E.P.; Flowers, C.R.; Francis, C.W.; et al. Venous Thromboembolism Prophylaxis and Treatment in Patients With Cancer: ASCO Clinical Practice Guideline Update. J. Clin. Oncol. 2020, 38, 496–520. [Google Scholar] [CrossRef]
- Maraveyas, A.; Waters, J.; Roy, R.; Fyfe, D.; Propper, D.; Lofts, F.; Sgouros, J.; Gardiner, E.; Wedgwood, K.; Ettelaie, C.; et al. Gemcitabine versus gemcitabine plus dalteparin thromboprophylaxis in pancreatic cancer. Eur. J. Cancer 2012, 48, 1283–1292. [Google Scholar] [CrossRef]
- Pelzer, U.; Opitz, B.; Deutschinoff, G.; Stauch, M.; Reitzig, P.C.; Hahnfeld, S.; Müller, L.; Grunewald, M.; Stieler, J.M.; Sinn, M.; et al. Efficacy of Prophylactic Low-Molecular Weight Heparin for Ambulatory Patients With Advanced Pancreatic Cancer: Outcomes From the CONKO-004 Trial. J. Clin. Oncol. 2015, 33, 2028–2034. [Google Scholar] [CrossRef]
- Farge, D.; Debourdeau, P.; Beckers, M.; Baglin, C.; Bauersachs, R.M.; Brenner, B.; Brilhante, D.; Falanga, A.; Gerotzafias, G.T.; Haim, N.; et al. International clinical practice guidelines for the treatment and prophylaxis of venous thromboembolism in patients with cancer. J. Thromb. Haemost. 2013, 11, 56–70. [Google Scholar] [CrossRef]
- Farge, D.; Bounameaux, H.; Brenner, B.; Cajfinger, F.; Debourdeau, P.; Khorana, A.A.; Pabinger, I.; Solymoss, S.; Douketis, J.; Kakkar, A. International clinical practice guidelines including guidance for direct oral anticoagulants in the treatment and prophylaxis of venous thromboembolism in patients with cancer. Lancet Oncol. 2016, 17, e452–e466. [Google Scholar] [CrossRef]
- Khorana, A.A.; Soff, G.A.; Kakkar, A.K.; Vadhan-Raj, S.; Riess, H.; Wun, T.; Streiff, M.B.; Garcia, D.A.; Liebman, H.A.; Belani, C.P.; et al. Rivaroxaban for Thromboprophylaxis in High-Risk Ambulatory Patients with Cancer. N. Engl. J. Med. 2019, 380, 720–728. [Google Scholar] [CrossRef]
- Vadhan-Raj, S.; McNamara, M.G.; Venerito, M.; Riess, H.; O’Reilly, E.M.; Overman, M.J.; Zhou, X.; Vijapurkar, U.; Kaul, S.; Wildgoose, P.; et al. Rivaroxaban thromboprohylaxis in ambulatory patients with pancreatic cancer: Results from a prespecified subgroup analysis of the CASSINI study. Cancer Med. 2020. (Epub ahead of print). [Google Scholar] [CrossRef]
- Agnelli, G.; Gussoni, G.; Bianchini, C.; Verso, M.; Mandalà, M.; Cavanna, L.; Barni, S.; Labianca, R.; Buzzi, F.; Scambia, G.; et al. Nadroparin for the prevention of thromboembolic events in ambulatory patients with metastatic or locally advanced solid cancer receiving chemotherapy: A randomised, placebo-controlled, double-blind study. Lancet Oncol. 2009, 10, 943–949. [Google Scholar] [CrossRef]
- Agnelli, G.; George, D.J.; Kakkar, A.K.; Fisher, W.; Lassen, M.R.; Mismetti, P.; Mouret, P.; Chaudhari, U.; Lawson, F.; Turpie, A.G.G.; et al. Semuloparin for thromboprophylaxis in patients receiving chemotherapy for cancer. N. Engl. J. Med. 2012, 366, 601–609. [Google Scholar] [CrossRef] [PubMed]
- Carrier, M.; Abou-Nassar, K.; Mallick, R.; Tagalakis, V.; Shivakumar, S.; Schattner, A.; Kuruvilla, P.; Hill, D.; Spadafora, S.; Marquis, K.; et al. Apixaban to Prevent Venous Thromboembolism in Patients with Cancer. N. Engl. J. Med. 2019, 380, 711–719. [Google Scholar] [CrossRef] [PubMed]
- Di Nisio, M.; Porreca, E.; Candeloro, M.; De Tursi, M.; Russi, I.; Rutjes, A.W. Primary prophylaxis for venous thromboembolism in ambulatory cancer patients receiving chemotherapy. Cochrane Database Syst. Rev. 2016, 12, CD008500. [Google Scholar] [CrossRef] [PubMed]
- Khorana, A.A.; Kuderer, N.M.; Culakova, E.; Lyman, G.H.; Francis, C.W. Development and validation of a predictive model for chemotherapy-associated thrombosis. Blood 2008, 111, 4902–4907. [Google Scholar] [CrossRef]
- Farge, D.; Bournet, B.; Conroy, T.; Vicaut, E.; Rak, J.; Zogoulous, G.; Barkun, J.; Ouaissi, M.; Buscail, L.; Frere, C. Primary Thromboprophylaxis in Pancreatic Cancer Patients: Why Clinical Practice Guidelines Should Be Implemented. Cancers 2020, 12, 618. [Google Scholar] [CrossRef]
- Tun, N.M.; Guevara, E.; Oo, T.H. Benefit and risk of primary thromboprophylaxis in ambulatory patients with advanced pancreatic cancer receiving chemotherapy: A systematic review and meta-analysis of randomized controlled trials. Blood Coagul. Fibrinolysis 2016, 27, 270–274. [Google Scholar] [CrossRef]
- Rahib, L.; Smith, B.D.; Aizenberg, R.; Rosenzweig, A.B.; Fleshman, J.M.; Matrisian, L.M. Projecting cancer incidence and deaths to 2030: The unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res. 2014, 74, 2913–2921. [Google Scholar] [CrossRef]
- Lambert, A.; Schwarz, L.; Borbath, I.; Henry, A.; Van Laethem, J.-L.; Malka, D.; Ducreux, M.; Conroy, T. An update on treatment options for pancreatic adenocarcinoma. Ther. Adv. Med. Oncol. 2019, 11, 1758835919875568. [Google Scholar] [CrossRef]
- Moffat, G.T.; Epstein, A.S.; O’Reilly, E.M. Pancreatic cancer-A disease in need: Optimizing and integrating supportive care. Cancer 2019, 125, 3927–3935. [Google Scholar] [CrossRef]
- Parpia, S.; Julian, J.A.; Thabane, L.; Lee, A.Y.Y.; Rickles, F.R.; Levine, M.N. Competing events in patients with malignant disease who are at risk for recurrent venous thromboembolism. Contemp. Clin. Trials 2011, 32, 829–833. [Google Scholar] [CrossRef] [PubMed]
- Icli, F.; Akbulut, H.; Utkan, G.; Yalcin, B.; Dincol, D.; Isikdogan, A.; Demirkazik, A.; Onur, H.; Cay, F.; Büyükcelik, A. Low molecular weight heparin (LMWH) increases the efficacy of cisplatinum plus gemcitabine combination in advanced pancreatic cancer. J. Surg. Oncol. 2007, 95, 507–512. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: Explanation and elaboration. BMJ 2009, 339, b2700. [Google Scholar] [CrossRef] [PubMed]
- McGinn, T.; Wyer, P.C.; Newman, T.B.; Keitz, S.; Leipzig, R.; For, G.G. Evidence-Based Medicine Teaching Tips Working Group Tips for learners of evidence-based medicine: 3. Measures of observer variability (kappa statistic). CMAJ 2004, 171, 1369–1373. [Google Scholar] [CrossRef]
- Jadad, A.R.; Moore, R.A.; Carroll, D.; Jenkinson, C.; Reynolds, D.J.; Gavaghan, D.J.; McQuay, H.J. Assessing the quality of reports of randomized clinical trials: Is blinding necessary? Control. Clin. Trials 1996, 17, 1–12. [Google Scholar] [CrossRef]
- Higgins, J.P.T.; Altman, D.G.; Gøtzsche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.C.; et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, d5928. [Google Scholar] [CrossRef]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Wen, L.; Badgett, R.; Cornell, J. Number needed to treat: A descriptor for weighing therapeutic options. Am. J. Health Syst. Pharm. 2005, 62, 2031–2036. [Google Scholar] [CrossRef]
| Study | Study Type | Number of PC Patients (Intervention /Control) | Patient Characteristics | Study Treatments | Duration of Thromboprophylaxis | Primary Endpoint | Efficacy Outcome | Major Bleeding | ||
|---|---|---|---|---|---|---|---|---|---|---|
| Intervention | Control | Intervention | Control | |||||||
| Agnelli 2009 PROTECHT [31] | Randomized, double blind, placebo-controlled multicenter phase III study | 36/17 | Ambulatory patients aged 18 years or older on chemotherapy with metastatic or locally advanced PC, ECOG Performance Status ≤ 2 | Nadroparin (3800 IU o.d.) versus placebo | For the duration of chemotherapy up to a maximum of 4 months | Composite of symptomatic VTE or arterial thromboembolism | 3/36 | 1/17 | - | - |
| Agnelli 2012SAVE ONCO [32] | Randomized, double blind, placebo-controlled multicenter phase III study | 126/128 | Ambulatory patients aged 18 years or older with metastatic or locally advanced PC beginning to receive a course of chemotherapy, ECOG PS < 3 | Semuloparin (20 mg o.d.) versus placebo | For the duration of chemotherapy then discontinued when chemotherapy was stopped, or regimen changed | Any symptomatic DVT in lower or upper limbs, any non-fatal PE, or death related to VTE (fatal PE or unexplained death) | 3/126 | 14/128 | - | - |
| Marayevas 2012FRAGEM [25] | Randomized, open label, controlled Phase IIb study | 59/62 | Patients aged 18 years or older with advanced or metastatic PC, Karnofsky performance status 60–100 | Gemcitabine + Dalteparin (200 IU/kg o.d., for 4 weeks, followed by a step-down regimen to 150 IU/kg) versus Gemcitabine alone | For up to 12 weeks | All type DVT/PE, all arterial events and all visceral thromboembolism | 7/59 | 17/62 | 2/59 | 2/62 |
| Pelzer 2015 CONKO [26] | Prospective, open label, randomized, multicenter and group-sequential phase IIb study | 160/152 | Patients aged 18 years or older with advanced PC receiving ambulant first-line chemotherapy | Enoxaparin 1 mg/kg o.d. versus no enoxaparin | Until disease progression | First symptomatic VTE | 2/160 | 15/152 | 7/160 | 5/152 |
| Khorana 2019 CASSINI [29,30] | Double-blind, randomized, placebo-controlled, parallel-group, multicenter phase III study | 135/138 | Adult ambulatory patients with various cancers initiating a new systemic regimen and at increased risk for VTE (defined as Khorana score ≥ 2). | Rivaroxaban 10 mg o.d. versus placebo | 180 (±3) days | Objectively confirmed symptomatic or asymptomatic lower-extremity proximal DVT, symptomatic upper extremity or distal lower-extremity DVT, symptomatic or incidental PE and VTE–related death | 5/135 | 14/138 | 2/135 | 3/138 |
| Sensitivity Analyses of Efficacy | nStudies, n Patients | RR (95% CI) | p(Test for Overall Effect) | I² (%) |
| Parenteral anticoagulants [25,26,31,32] | 4 studies, 740 patients | 0.30 (0.17–0.53) | <0.0001 | 31 |
| Oral anticoagulants [30] | 1 study, 273 patients | 0.37 (0.14–0.99) | 0.05 | NA |
| Prophylactic doses of anticoagulants [30,31,32] | 3 studies, 580 patients | 0.34 (0.17–0.70) | 0.003 | 7 |
| Supra-prophylactic or therapeutic doses of anticoagulants [25,26] | 2 studies, 433 patients | 0.27 (0.08–0.90) | 0.03 | 55 |
| Sensitivity Analyses of Safety | nStudies,nPatients | RR (95% CI) | p(Test for Overall Effect) | I² (%) |
| Parenteral anticoagulants [25,26] | 2 studies, 433 patients | 1.25 (0.47–3.31) | 0.65 | 0 |
| Oral anticoagulants [30] | 1 study, 273 patients | 0.68 (0.12–4.01) | 0.67 | NA |
| Prophylactic doses of anticoagulants [30] | 1 study, 273 patients | 0.68 (0.12–4.01) | 0.67 | NA |
| Supra-prophylactic or therapeutic doses of anticoagulants [25,26] | 2 studies, 433 patients | 1.25 (0.47–3.31) | 0.65 | 0 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Frere, C.; Crichi, B.; Bournet, B.; Canivet, C.; Abdallah, N.A.; Buscail, L.; Farge, D. Primary Thromboprophylaxis in Ambulatory Pancreatic Cancer Patients Receiving Chemotherapy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Cancers 2020, 12, 2028. https://doi.org/10.3390/cancers12082028
Frere C, Crichi B, Bournet B, Canivet C, Abdallah NA, Buscail L, Farge D. Primary Thromboprophylaxis in Ambulatory Pancreatic Cancer Patients Receiving Chemotherapy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Cancers. 2020; 12(8):2028. https://doi.org/10.3390/cancers12082028
Chicago/Turabian StyleFrere, Corinne, Benjamin Crichi, Barbara Bournet, Cindy Canivet, Nassim Ait Abdallah, Louis Buscail, and Dominique Farge. 2020. "Primary Thromboprophylaxis in Ambulatory Pancreatic Cancer Patients Receiving Chemotherapy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials" Cancers 12, no. 8: 2028. https://doi.org/10.3390/cancers12082028
APA StyleFrere, C., Crichi, B., Bournet, B., Canivet, C., Abdallah, N. A., Buscail, L., & Farge, D. (2020). Primary Thromboprophylaxis in Ambulatory Pancreatic Cancer Patients Receiving Chemotherapy: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Cancers, 12(8), 2028. https://doi.org/10.3390/cancers12082028






