Factors Associated with Health-Related Quality of Life in Women with Breast Cancer in the Middle East: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Sources and Search Strategy
2.2. Eligibility Criteria
- Population: women diagnosed with BC only;
- Setting: studies conducted in one or more Middle East countries;
- Outcome: HRQoL assessed using any valid and reliable instrument that measures quality of life, such as EORTC QLQ-C30: European Organization for Research and treatment of Cancer—Quality of Life Questionnaire; BR23: Breast cancer specific module; FACT-B: The Functional Assessment of Cancer Therapy—Breast Cancer; FACT-G: The Functional Assessment of Cancer Therapy—General Questionnaire; NMCBRI-Q: the national medical center and Beckman research institute questionnaire; LQI: Life quality inventory; QOL-BC: The American quality of life BC; QoLS: The Quality of Life Scale; SF-36: Short-Form Health Survey Questionnaire; WHOQOL-BREF: WHO questionnaire of quality of life;
- Experimental or observational study investigating any associated factors with HRQoL;
- English language articles.
- Narrative or systematic reviews;
- Editorials, expert opinions, comments (commentary), methodological article, or conference abstracts and proceedings;
- Assessment of the effect of specific interventions on HRQoL, such as sport, exercise, yoga, or focus groups.
2.3. Data Extraction and Synthesis
2.4. Methodological Quality Assessment
3. Results
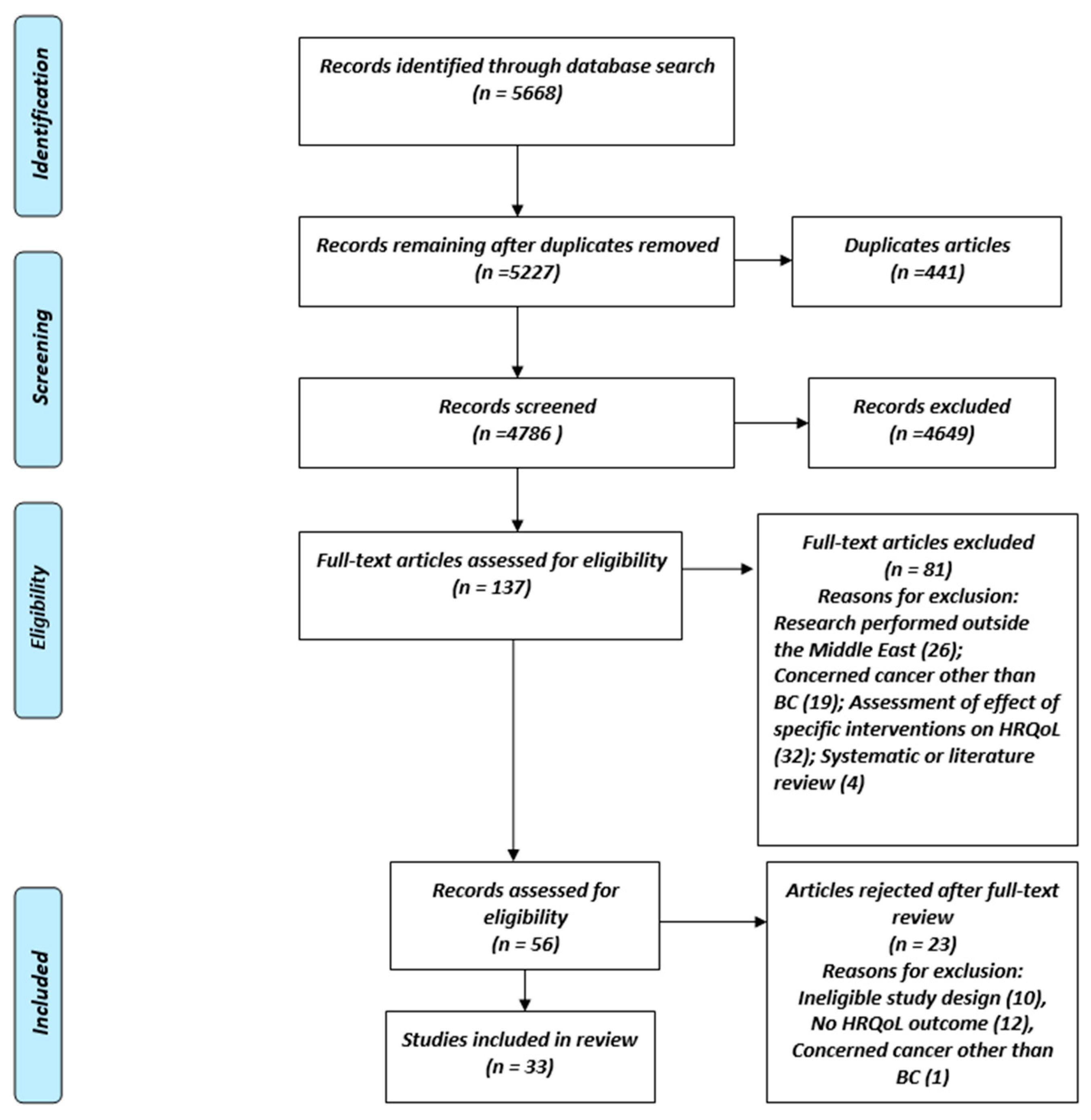
3.1. Study Selection
3.2. Characteristics of the Included Studies
3.3. Description of the Selected Atudies
3.3.1. Characteristics of the Cross-Sectional Studies
3.3.2. Characteristics of the Case-Control Studies
3.3.3. Characteristics of the Longitudinal Studies
3.4. Quality Assessment
3.5. Factors Associated with HRQoL in Women with BC in the Middle East
3.5.1. Socio-Demographic Factors
3.5.2. Clinical Factors
3.5.3. Treatment-Related Factors
3.5.4. Behavioral Factors
3.5.5. Psychosocial Factors
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: Globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424. [Google Scholar] [CrossRef] [PubMed]
- Hirko, K.A.; Soliman, A.S.; Hablas, A.; Seifeldin, I.A.; Ramadan, M.; Banerjee, M.; Harford, J.B.; Chamberlain, R.M.; Merajver, S.D. Trends in Breast Cancer Incidence Rates by Age and Stage at Diagnosis in Gharbiah, Egypt, over 10 Years (1999–2008). J. Cancer Epidemiol. 2013, 2013, 916394. [Google Scholar] [CrossRef] [PubMed]
- Elobaid, Y.; Aw, T.-C.; Lim, J.N.W.; Hamid, S.; Grivna, M. Breast cancer presentation delays among Arab and national women in the UAE: A qualitative study. SSM Popul. Health 2016, 2, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Osoba, D. Lessons learned from measuring health-related quality of life in oncology. J. Clin. Oncol. 1994, 12, 608–616. [Google Scholar] [CrossRef] [PubMed]
- Keegan, T.H.M.; DeRouen, M.C.; Press, D.J.; Kurian, A.W.; Clarke, C.A. Occurrence of breast cancer subtypes in adolescent and young adult women. Breast Cancer Res. 2012, 14, R55. [Google Scholar] [CrossRef] [PubMed]
- Collins, L.C.; Marotti, J.D.; Gelber, S.; Cole, K.; Ruddy, K.; Kereakoglow, S.; Brachtel, E.F.; Schapira, L.; Come, S.E.; Winer, E.P.; et al. Pathologic features and molecular phenotype by patient age in a large cohort of young women with breast cancer. Breast Cancer Res. Treat. 2012, 131, 1061–1066. [Google Scholar] [CrossRef] [PubMed]
- Hirai, K.; Motooka, H.; Ito, N.; Wada, N.; Yoshizaki, A.; Shiozaki, M.; Momino, K.; Okuyama, T.; Akechi, T. Problem-solving therapy for psychological distress in Japanese early-stage breast cancer patients. Jpn. J. Clin. Oncol. 2012, 42, 1168–1174. [Google Scholar] [CrossRef] [PubMed]
- Paraskevi, T. Quality of life outcomes in patients with breast cancer. Oncol. Rev. 2012, 6, e2. [Google Scholar] [CrossRef]
- Schou, I.; Ekeberg, Ø.; Sandvik, L.; Hjermstad, M.J.; Ruland, C.M. Multiple predictors of health-related quality of life in early stage breast cancer. Data from a year follow-up study compared with the general population. Qual. Life Res. 2005, 14, 1813–1823. [Google Scholar] [CrossRef] [PubMed]
- Ekwueme, D.U.; Trogdon, J.G. The Economics of Breast Cancer in Younger Women in the U.S. Am. J. Prev. Med. 2016, 50, 249–254. [Google Scholar] [CrossRef] [PubMed]
- Keim-Malpass, J.; Levine, B.; Danhauer, S.C.; Avis, N.E. Work-related perceptions and quality of life among breast cancer survivors. Psychooncology 2016, 25, 873–876. [Google Scholar] [CrossRef] [PubMed]
- Kwan, M.L.; Ergas, I.J.; Somkin, C.P.; Quesenberry, C.P.; Neugut, A.I.; Hershman, D.L.; Mandelblatt, J.; Pelayo, M.P.; Timperi, A.W.; Miles, S.Q.; et al. Quality of life among women recently diagnosed with invasive breast cancer: The pathways study. Breast Cancer Res. Treat. 2010, 123, 507–524. [Google Scholar] [CrossRef] [PubMed]
- Kreitler, S.; Peleg, D.; Ehrenfeld, M. Stress, self-efficacy and quality of life in cancer patients. Psychooncology 2007, 16, 329–341. [Google Scholar] [CrossRef] [PubMed]
- Hutter, N.; Vogel, B.; Alexander, T.; Baumeister, H.; Helmes, A.; Bengel, J. Are depression and anxiety determinants or indicators of quality of life in breast cancer patients? Psychol. Health Med. 2013, 18, 412–419. [Google Scholar] [CrossRef] [PubMed]
- Leung, J.; Pachana, N.A.; McLaughlin, D. Social support and health-related quality of life in women with breast cancer: A longitudinal study. Psychooncology 2014, 23, 1014–1020. [Google Scholar] [CrossRef] [PubMed]
- Papadopoulou, C.; Kotronoulas, G.; Schneider, A.; Miller, M.I.; McBride, J.; Polly, Z.; Bettles, S.; Whitehouse, A.; McCann, L.; Kearney, N.; et al. Patient-reported self-efficacy, anxiety, and health-related quality of life during chemotherapy: Results from a longitudinal study. Oncol. Nurs. Forum. 2017, 44, 127–136. [Google Scholar] [CrossRef]
- Herschbach, P.; Berg, P.; Waadt, S.; Duran, G.; Engst-Hastreiter, U.; Henrich, G.; Book, K.; Dinkel, A. Group psychotherapy of dysfunctional fear of progression in patients with chronic arthritis or cancer. Psychother. Psychosom. 2010, 79, 31–38. [Google Scholar] [CrossRef]
- Hashemi, S.-M.; Balouchi, A.; Al-Mawali, A.; Rafiemanesh, H.; Rezaie-Keikhaie, K.; Bouya, S.; Dehghan, B.; Farahani, M.A. Health-related quality of life of breast cancer patients in the Eastern Mediterranean region: A systematic review and meta-analysis. Breast Cancer Res. Treat. 2019, 174, 585–596. [Google Scholar] [CrossRef]
- Hutton, B.; Salanti, G.; Caldwell, D.M.; Chaimani, A.; Schmid, C.H.; Cameron, C.; Ioannidis, J.P.A.; Straus, S.; Thorlund, K.; Jansen, J.P.; et al. The prisma extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: Checklist and explanations. Ann. Intern. Med. 2015, 162, 777–784. [Google Scholar] [CrossRef]
- Stang, A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur. J. Epidemiol. 2010, 25, 603–605. [Google Scholar] [CrossRef]
- Ahmed, A.E.; Alharbi, A.G.; Alsadhan, M.A.; Almuzaini, A.S.; Almuzaini, H.S.; Ali, Y.Z.; Jazieh, A.-R. The predictors of poor quality of life in a sample of Saudi women with breast cancer. Breast Cancer 2017, 9, 51–58. [Google Scholar] [CrossRef] [PubMed]
- Ahrafizadeh, H.; Fayazi, S.; Kord, Z.; Farokhpayam, M.; Farokhpayam, H.; Kiyani, B. The survey quality of life and its related factors among patients with breast cancer who referred to golestan & amp, Shefa hospitals in ahvaz 2014. Indo Am. J. Pharm. Sci. 2017, 4, 1072–1078. [Google Scholar]
- Akel, R.; El Darsa, H.; Anouti, B.; Mukherji, D.; Temraz, S.; Raslan, R.; Tfayli, A.; Assi, H. Anxiety, depression and quality of life in breast cancer patients in the levant. Asian Pac. J. Cancer Prev. 2017, 18, 2809–2816. [Google Scholar] [PubMed]
- Akin, S.; Can, G.; Durna, Z.; Aydiner, A. The quality of life and self-efficacy of Turkish breast cancer patients undergoing chemotherapy. Eur. J. Oncol. Nurs. 2008, 12, 449–456. [Google Scholar] [CrossRef] [PubMed]
- Alawadi, S.A.; Ohaeri, J.U. Health—related quality of life of Kuwaiti women with breast cancer: A comparative study using the eortc quality of life questionnaire. BMC Cancer 2009, 9, 222. [Google Scholar] [CrossRef] [PubMed]
- Albabtain, H.; Alwhaibi, M.; Alburaikan, K.; Asiri, Y. Quality of life and complementary and alternative medicine use among women with breast cancer. Saudi Pharm. J. 2018, 26, 416–421. [Google Scholar] [CrossRef] [PubMed]
- Almutairi, K.M.; Mansour, E.A.; Vinluan, J.M. A cross-sectional assessment of quality of life of breast cancer patients in Saudi Arabia. Public Health 2016, 136, 117–125. [Google Scholar] [CrossRef]
- Al-Naggar, R.A.; Nagi, N.M.S.; Ali, M.M.S.; Almuasli, M. Quality of life among breast cancer patients in Yemen. Asian Pac. J. Cancer Prev. 2011, 12, 2335–2341. [Google Scholar]
- Al-Natour, A.; Al Momani, S.M.; Qandil, A.M.A. The relationship between spirituality and quality of life of jordanian women diagnosed with breast cancer. J. Relig. Health 2017, 56, 2096–2108. [Google Scholar] [CrossRef]
- Bagheri, M.; Mazaheri, M. Body image and quality of life in female patients with breast cancer and healthy women. J. Midwifery Reprod. Health 2015, 3, 285–292. [Google Scholar]
- Bayram, Z.; Durna, Z.; Akin, S. Quality of life during chemotherapy and satisfaction with nursing care in Turkish breast cancer patients. Eur. J. Cancer Care 2014, 23, 675–684. [Google Scholar] [CrossRef] [PubMed]
- Filazoglu, G.; Griva, K. Coping and social support and health related quality of life in women with breast cancer in Turkey. Psychol. Health Med. 2008, 13, 559–573. [Google Scholar] [CrossRef] [PubMed]
- Abu-Saad Huijer, H.; Abboud, S. Health-related quality of life among breast cancer patients in Lebanon. Eur. J. Oncol. Nurs. 2012, 16, 491–497. [Google Scholar] [CrossRef] [PubMed]
- Jafari, N.; Farajzadegan, Z.; Zamani, A.; Bahrami, F.; Emami, H.; Loghmani, A. Spiritual well-being and quality of life in Iranian women with breast cancer undergoing radiation therapy. Support Care Cancer 2013, 21, 1219–1225. [Google Scholar] [CrossRef] [PubMed]
- Jassim, G.A.; Whitford, D.L. Quality of life of Bahraini women with breast cancer: A cross sectional study. BMC Cancer 2013, 13, 212. [Google Scholar] [CrossRef] [PubMed]
- Khalili, N.; Farajzadegan, Z.; Mokarian, F.; Bahrami, F. Coping strategies, quality of life and pain in women with breast cancer. Iran. J. Nurs. Midwifery Res. 2013, 18, 105–111. [Google Scholar]
- Ahmad Kiadaliri, A.; Bastani, P.; Ibrahimipour, H. Health-related quality of life of breast cancer patients in Iran: Pooled analysis using generalized estimating equations. Asian Pac. J. Cancer Prev. 2012, 13, 941–944. [Google Scholar] [CrossRef][Green Version]
- Mohammadi, S.; Sulaiman, S.; Koon, P.B.; Amani, R.; Hosseini, S.M. Association of nutritional status with quality of life in breast cancer survivors. Asian Pac. J. Cancer Prev. 2013, 14, 7749–7755. [Google Scholar] [CrossRef]
- Moradi, R.; Roudi, M.A.; Kiani, M.M.; Mousavi Rigi, S.A.; Mohammadi, M.; Keshvari, M.; Hosseini, M. Investigating the relationship between self-efficacy and quality of life in breast cancer Patients receiving chemical therapy. Bali Med. J. 2017, 6, 6. [Google Scholar] [CrossRef]
- Musarezaie, A.; Zargham-Boroujeni, A. Quality of life and related factors among the women undergoing mastectomy. Iran. J. Nurs. Midwifery Res. 2015, 20, 287–291. [Google Scholar]
- Najafi, F.; Nedjat, S.; Zendehdel, K.; Mirzania, M.; Montazeri, A. Self-reported versus proxy reported quality of life for breast cancer patients in the islamic Republic of Iran. East. Mediterr. Health J. 2017, 22, 786–793. [Google Scholar] [CrossRef] [PubMed]
- Nikmanesh, Z.; Shirazi, M.; Farazinezhad, F. Examining the predictive role of emotional self-regulation in quality of life and perception of suffering among patients with breast cancer. Middle East J. Cancer 2017, 8, 93–101. [Google Scholar]
- Pehlivan, S.; Kuzhan, A.; Yildirim, Y.; Fadiloglu, C. Comfort and quality of life in patients with breast cancer undergoing radiation therapy. J. BUON 2016, 21, 549–555. [Google Scholar] [PubMed]
- Rohani, C.; Abedi, H.-A.; Omranipour, R.; Langius-Eklöf, A. Health-related quality of life and the predictive role of sense of coherence, spirituality and religious coping in a sample of Iranian women with breast cancer: A prospective study with comparative design. Health Qual. Life Outcomes 2015, 13, 40. [Google Scholar] [CrossRef] [PubMed]
- Safa, A.; Rahemi, Z.; Aghajani, M. Quality of life in patients with breast cancer in Kashan: A cross-sectional study. Life Sci. J. 2014, 11, 141–145. [Google Scholar]
- Shakeri, J.; Golshani, S.; Jalilian, E.; Farnia, V.; Nooripour, R.; Alikhani, M.; Yaghoobi, K. Studying the amount of depression and its role in predicting the quality of life of women with breast cancer. Asian Pac. J. Cancer Prev. 2016, 17, 643–646. [Google Scholar] [CrossRef]
- Saatci, E.; Akin, S.; Akpinar, E. Do the unmet needs affect the quality of life in breast cancer patients? West Indian Med. J. 2007, 56, 253–257. [Google Scholar] [CrossRef]
- Safaee, A.; Moghimi-Dehkordi, B.; Zeighami, B.; Tabatabaee, H.; Pourhoseingholi, M. Predictors of quality of life in breast cancer patients under chemotherapy. Indian J. Cancer 2008, 45, 107–111. [Google Scholar] [CrossRef]
- Homaee Shandiz, F.; Karimi, F.Z.; Khosravi Anbaran, Z.; Abdollahi, M.; Rahimi, N.; Ghasemi, M. Investigating the quality of life and the related factors in iranian women with breast cancer. Asian Pac. J. Cancer Prev. 2017, 18, 2089–2092. [Google Scholar]
- Sinaei, F.; Zendehdel, K.; Adili, M.; Ardestani, A.; Montazeri, A.; Mohagheghi, M.A. Association Between Breast Reconstruction Surgery and Quality of Life in Iranian Breast Cancer Patients. Acta Med. Iran. 2017, 55, 35–41. [Google Scholar]
- Uzun, O.; Aslan, F.E.; Selimen, D.; Koç, M. Quality of life in women with breast cancer in Turkey. J. Nurs. Scholarsh. 2004, 36, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Zamanian, H.; Eftekhar-Ardebili, H.; Eftekhar-Ardebili, M.; Shojaeizadeh, D.; Nedjat, S.; Taheri-Kharameh, Z.; Daryaafzoon, M. Religious coping and quality of life in women with breast cancer. Asian Pac. J. Cancer Prev. 2015, 16, 7721–7725. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Zargani, A.; Nasiri, M.; Hekmat, K.; Abbaspour, Z.; Vahabi, S. A survey on the relationship between religiosity and quality of life in patients with breast cancer: A study in iranian muslims. Asia Pac. J. Oncol. Nurs. 2018, 5, 217–222. [Google Scholar] [PubMed]
- Yan, B.; Yang, L.-M.; Hao, L.-P.; Yang, C.; Quan, L.; Wang, L.-H.; Wu, Z.; Li, X.-P.; Gao, Y.-T.; Sun, Q.; et al. Determinants of Quality of Life for Breast Cancer Patients in Shanghai, China. PLoS ONE 2016, 11, e0153714. [Google Scholar] [CrossRef] [PubMed]
- Broeckel, J.A.; Jacobsen, P.B.; Balducci, L.; Horton, J.; Lyman, G.H. Quality of life after adjuvant chemotherapy for breast cancer. Breast Cancer Res. Treat. 2000, 62, 141–150. [Google Scholar] [CrossRef] [PubMed]
- Broeckel, J.A.; Jacobsen, P.B.; Horton, J.; Balducci, L.; Lyman, G.H. Characteristics and correlates of fatigue after adjuvant chemotherapy for breast cancer. J. Clin. Oncol. 1998, 16, 1689–1696. [Google Scholar] [CrossRef]
- Wildes, K.A.; Miller, A.R.; de Majors, S.S.M.; Ramirez, A.G. The religiosity/spirituality of Latina breast cancer survivors and influence on health-related quality of life. Psychooncology 2009, 18, 831–840. [Google Scholar] [CrossRef]
- Poleshuck, E.L.; Katz, J.; Andrus, C.H.; Hogan, L.A.; Jung, B.F.; Kulick, D.I.; Dworkin, R.H. Risk factors for chronic pain following breast cancer surgery: A prospective study. J. Pain 2006, 7, 626–634. [Google Scholar] [CrossRef]
- Shelby, R.A.; Taylor, K.L.; Kerner, J.F.; Coleman, E.; Blum, D. The role of community-based and philanthropic organizations in meeting cancer patient and caregiver needs. CA Cancer J. Clin. 2002, 52, 229–246. [Google Scholar] [CrossRef][Green Version]
| MeSH Terms for HRQoL | MeSH Terms for Breast Cancer | MeSH Terms for ME Countries |
|---|---|---|
| quality of life OR health related quality of life OR life style OR well-being OR health status | Breast Neoplasms OR Breast Neoplasm OR Breast Cancer OR Breast Carcinoma OR Breast OR mammary carcinoma OR cancer OR mammary cancer OR carcinoma mammae | Middle East OR Bahrain OR Egypt OR Iran OR Iraq OR Jordan OR Kuwait OR Lebanon OR Oman OR Palestine OR Qatar OR Saudi Arabia OR Syria OR Turkey OR United Arab Emirates OR Yemen |
| Characteristic | Number | Percentage |
|---|---|---|
| Country | ||
| Iran | 15 | 45 |
| Turkey | 9 | 27 |
| Saudi Arabia | 3 | 9 |
| Jordan | 2 | 6 |
| Lebanon | 1 | 3 |
| Kuwait | 1 | 3 |
| Bahrain | 1 | 3 |
| Yemen | 1 | 3 |
| Location of study | ||
| Cancer center | 17 | 52 |
| Hospital | 16 | 48 |
| Main location of first author | ||
| University | 27 | 82 |
| Hospital | 3 | 9 |
| Research center | 2 | 6 |
| Medical center | 1 | 3 |
| Type of journal | ||
| Medical | 14 | 42 |
| Medical oncology | 6 | 18 |
| Multidisciplinary | 4 | 12 |
| Clinical | 4 | 12 |
| Academic | 4 | 12 |
| Clinical psychology | 1 | 3 |
| Type of data collection | ||
| Self-reported | 12 | 36 |
| Interview | 21 | 64 |
| Study design | ||
| Cross-sectional | 28 | 85 |
| Case-control | 3 | 9 |
| Longitudinal | 2 | 6 |
| Author Name, Country—Year of Publication | Type of Study | Sample Size | Age of BC Patients | Stage | Treatment | Time of Assessment | Questionnaires |
|---|---|---|---|---|---|---|---|
| Mean (SD) | % | % | |||||
| Ahmad A [21], Saudi Arabia—2017 | Cross-sectional | 145 | 50.3 (13.5) | I and II: 61.2 III and IV: 38.8 | Cancer surgery: 64.8 Chemotherapy: 73.1 Radiotherapy: 57.9 Immunotherapy: 49 | First year after cancer % Yes: 52.4 No: 47.6 | SF-36 |
| Ahrafizadeh H [22], Iran—2017 | Cross-sectional | 100 | 46.8 (11.5) | - | Mastectomy: 58 Breast conservative surgery: 31 Chemotherapy: 100 | During chemotherapy | WHOQOL-BREF |
| Akel R [23], Lebanon—2017 | Cross-sectional | 150 (121 Lebanese, 26 Iraqi, 6 other) | 53.5 (10.4) | I: 29.3 II: 38.7 III: 23.3 IV: 8.7 | Chemotherapy: 79.3 Radiotherapy: 80.7 Surgery: 97.3 Hormone therapy: 86 | 0.5 to ≤ 2 years: 13.3 3 to ≤ 5 years: 68.7 ≥ 5 years: 18 | FACT-B |
| Akin S [24], Turkey—2008 | Longitudinal | 141 | 46.9 (10.1) | I: 6.4 II: 47.5 III: 31.2 IV: 14.29 | Chemotherapy: 100 Surgery: 76.6 | Pre and Post chemotherapy | FACT-B |
| Alawadi S [25], Kuwait—2009 | Cross-sectional | 348 | 48.3 (10.3) | I: 7 II: 34.3 III: 36 IV: 22.7 | Chemotherapy: 98.3 Radiotherapy: 21 Surgery: 58.6 | During chemotherapy | EORTC-QLQ-C30 plus QLQ-BR23 |
| Albabtain H [26], Saudi Arabia—2018 | Cross-sectional | 95 | 25–39 years: 26.3 40–59 years: 47.4 > 60 years: 26.3 | - | 89.5 undergoing cancer treatment | During cancer treatment | EORTC-QLQ-C30 plus QLQ-BR23 |
| Almutairi K [27], Saudi Arabia—2016 | Cross-sectional | 145 | 26–35 years: 13.1 36–45 years: 30.3 | I: 21.4 II: 57.9 III and IV: 20 Distant metastasis: 0.7 | Chemotherapy: 3.4 Radiotherapy: 2.1 Surgery: 31.7 Hormone therapy: 0.7 Combination modalities: 62.1 | During the visit of outpatient clinics | EORTC-QLQ-C30 plus QLQ-BR23 |
| >46 years: 56.6 | |||||||
| Al-Naggar R [28], Yemen—2011 | Cross-sectional | 106 | < 55 years: 67.9 | III: 35.8 | Chemotherapy: 94.3 Radiotherapy: 63.2 Surgery: 85.8 | unspecified | FACT-B |
| Al-Natour A [29], Jordan—2017 | Cross-sectional | 150 | 47.9 (9.7) | I: 25.5 II: 48.9 III: 19 IV: 6.6 | - | During cancer treatment | FACT-G |
| Bagheri M [30], Iran—2015 | Case- Control | 50 cases 50 Healthy control | Cases: 32 (0.5) Controls: 33.7 (4.2) | - | - | unspecified | SF-36 |
| Bayram Z [31], Turkey—2014 | Cross-sectional | 105 | 50.1 (11.8) | I: 40 II: 37.1 III: 19.0 IV: 3.8 | Chemotherapy: 100 | Newly diagnosed and undergoing chemotherapy | FACT-G |
| Filazoglu G [32], Turkey—2008 | Cross-sectional | 188 | 45.1 (5.6) | I: 23.4 II: 55.9 III: 18.6 IV: 2.1 | Chemotherapy: 17.6 Radiotherapy: 38.8 Chemotherapy + Radiotherapy: 14.4 No treatment: 29.3 Surgery: 100 | After breast surgery for a minimum of 3 months before the study. | SF-36 |
| Hujeir H [33], Lebanon—2012 | Cross-sectional | 89 | 49.2 (11.1) | Metastasis: 37.1 | Chemotherapy: 47.2 Radiotherapy: 31.4 Surgery: 70.7 Hormone therapy: 15.7 | 30.6 (39.06) months | EORTC-QLQ-C30 |
| Jafari N [34], Iran—2013 | Cross-sectional | 68 | 48 (10.3) | - | Radiotherapy: 100 | During Radiotherapy | EORTC-QLQ-C30 plus QLQ-BR23 |
| Jassim G [35], Bahrain—2013 | Cross-sectional | 239 | 50.2 (11.1) | I: 29.9 II: 44.8 III and IV: 25.3 | Chemotherapy: 80.5 Radiotherapy: 83.9 Lumpectomy: 51.3 Mastectomy: 50 Lymph node dissection: 85.1 Hormone therapy: 69.8 | Early diagnosed: 14.6 Transitional period: 53.6 Long-term survivors: 31.8 | EORTC-QLQ-C30 plus QLQ-BR23 |
| Khalili N [36], Iran—2013 | Cross-sectional | 62 | 45.8 (6.7) | IA: 1.6 IB: 6.4 IIA: 22.5 IIB: 25.8 IIIA: 16.1 IIIB: 14.5 IIIC: 8.1 | - | Diagnosis with BC in a recent year | EORTC-QLQ-C30 |
| Kiadaliri A [37], Iran—2012 | Longitudinal | 100 | TAC: 46.7 (8.2) FAC: 49.3 (11.5) | - | - | Before and after chemotherapy and 4 months later | EORTC-QLQ-C30 |
| Mohammadi S [38], Iran—2013 | Cross-sectional | 100 | 47.8(6.7) | I: 8 II: 41 III: 51.3 | All patients completed 3 phases of BC treatment, which included mastectomy, chemotherapy, radiation therapy. | Duration of survivorship: 2 years: 25 3 years: 44 4 years: 25 5 years: 6 | EORTC-QLQ-C30 |
| Moradi R [39], Iran—2017 | Cross-sectional | 87 | 48.25 (11.9) | - | Chemotherapy: 100 | After chemotherapy | WHOQOL-BREF |
| Musarezaei A [40], Iran—2015 | Cross-sectional | 105 | 45.3 (4.6) | II: 50 | Mastectomy: 100 | Underwent mastectomy (at least 1 year and a maximum of 5 years previously) | NMCBRI-Q |
| Najafi F [41], Iran—2016 | Cross-sectional | 148 | 47.6 (10.1) | In situ: 7.1 Local: 45.7 Loco/regional: 40 Advanced: 7.1 | Patients completed at least 2 chemotherapy sessions (only those with very small tumors did not undergo chemotherapy). | Time since diagnosis: 17.2 (1.4) months | EORTC-QLQ-C30 |
| Nikamenesh Z [42], Iran—2017 | Cross-sectional | 42 | 30-50 years: 69% | - | - | Diagnosis for at least 6 months and under treatment | EORTC-QLQ-C30 |
| Pehlivan S [43], Turkey—2016 | Cross-sectional | 61 | 50.37 (11.8) | I: 9.8 II: 59 III: 23 IV: 8.2 | Chemotherapy: 19.7 Chemotherapy + Radiotherapy: 80.3 | During Radiotherapy | EORTC QLQ-BR23 |
| Rohani C [44], Iran—2015 | Case-control | Cases (BC patients): 162 Controls: 210 | Cases: 46.1 (9.8) Control: 46.6 (8.4) | 0: 2.5 I: 22.8 II:49.4 III: 24.1 IV: 1.2 | Chemotherapy: 79 Radiotherapy: 75.3 Hormone therapy: 68.5 | Baseline pre-diagnosis phase of BC (T1) and 6 months post pre-diagnosis (T2). | EORTC-QLQ-C30 |
| Safa A [45], Iran—2014 | Cross-sectional | 92 | 42.9 (8.7) | - | - | At least 3 months since treatment | QOL-BC |
| Shakeri J [46], Iran—2016 | Cross-sectional | 98 | 47.6 (14) | - | - | Unspecified | LQI |
| Saatci E [47], Turkey—2007 | Cross-sectional | 100 | 48.64 (10.6) | I: 49 II: 51 | Chemotherapy: 59 Radiotherapy: 10 Chemotherapy + Radiotherapy: 31 | 22.6 (24.3) months | FACT-G |
| Safaee A [48], Iran—2008 | Cross-sectional | 119 | 48.27 (11.4) | Well differentiated: 33.6 Moderately differentiated: 42 Poorly differentiated: 24.4 | Chemotherapy: 100 | Time since diagnosis: < 4 months: 39.5 4-12 months: 34.4 >12 months: 26.1 | EORTC-QLQ-C30 |
| Shandiz,F H [49], Iran—2008 | Cross-sectional | 94 | 45.20(8.6) | - | Chemotherapy: 100 Radiotherapy: 69.1 Surgery: 100 Hormone therapy: 52.1 | During chemotherapy | EORTC-QLQ-C30 |
| Sinaei F [50], Iran—2017 | Case-control | Mastectomy group: 45 Reconstruction group: 61 | Mastectomy: 50.2 (8.5) Reconstruction: 46.7 (8.1) | - | Surgery: 100 Chemo radiation: Mastectomy: 86.7 Reconstruction: 90 | unspecified | EORTC-QLQ-C30 plus QLQ-BR23 |
| Uzun Ö [51], Turkey—2004 | Cross-sectional | 72 | 50.1 (9.3) | I: 24 II: 58.3 III: 16.7 | Chemotherapy: 100 Radiotherapy: 52.8 Surgery: 100 | unspecified | QoLS |
| Zamanian H [52], Iran—2015 | Cross-sectional | 224 | 47.1 (9.0) | - | Chemotherapy: 61.6 Radiotherapy: 40 Surgery: 26.8 | Time since diagnosis: 43.8 (37.6) months | FACT-B |
| Zargani A [53], Iran—2018 | Cross-sectional | 84 | 54.7 (10.4) | - | All patients undergoing cancer treatment (surgery, radiotherapy or chemotherapy). | Diagnosis at least 1 year prior | SF-36 |
| Author | Study Design | Selection of Participants | Comparability Based on Design or Analysis | Assessment of Outcome/Exposure | Total |
|---|---|---|---|---|---|
| (a) | |||||
| Ahmed et al. [21] | Cross-sectional | ** | ** | * | 5(/6) |
| Ahrafizadeh et al. [22] | Cross-sectional | ** | * | 3(/6) | |
| Akel et al. [23] | Cross-sectional | ** | * | 3(/6) | |
| Akin et al. [24] | longitudinal | *** | ** | 5(/9) | |
| Alawadi et al. [25] | Cross-sectional | ** | ** | * | 5(/6) |
| Albabtain et al. [26] | Cross-sectional | ** | * | 3(/6) | |
| Almutairi et al. [27] | Cross-sectional | ** | ** | * | 5(/6) |
| Al Naggar et al. [28] | Cross-sectional | ** | ** | * | 5(/6) |
| Al Natour et al. [29] | Cross-sectional | ** | * | 3(/6) | |
| Bayram et al. [31] | Cross-sectional | ** | * | 3(/6) | |
| Filazoglu et al. [32] | Cross-sectional | ** | ** | * | 5(/6) |
| Hujeir et al. [33] | Cross-sectional | ** | * | 3(/6) | |
| Jafari et al. [34] | Cross-sectional | ** | * | * | 4(/6) |
| Jassim et al. [35] | Cross-sectional | ** | ** | * | 5(/6) |
| Khalili et al. [36] | Cross-sectional | ** | * | 3(/6) | |
| Kiadaliri et al. [37] | longitudinal | *** | ** | 5(/9) | |
| Mohammadi et al. [38] | Cross-sectional | ** | * | 3(/6) | |
| Moradi et al. [39] | Cross-sectional | *** | * | 4(/6) | |
| Musarezaei et al. [40] | Cross-sectional | ** | * | 3(/6) | |
| Najafi et al. [41] | Cross-sectional | *** | ** | * | 6(/6) |
| Nikmanesh et al. [42] | Cross-sectional | ** | * | 3(/6) | |
| Pehlivan et al. [43] | Cross-sectional | ** | * | 3(/6) | |
| Saatci et al. [47] | Cross-sectional | ** | * | 3(/6) | |
| Safa et al. [45] | Cross-sectional | *** | * | 4(/6) | |
| Safaee et al. [48] | Cross-sectional | ** | ** | * | 5(/6) |
| Shakeri et al. [46] | Cross-sectional | ** | * | 3(/6) | |
| Shandiz et al. [49] | Cross-sectional | ** | ** | * | 5(/6) |
| Uzun et al. [51] | Cross-sectional | ** | * | 3(/6) | |
| Zamanian et al. [52] | Cross-sectional | ** | ** | * | 5(/6) |
| Zargani et al. [53] | Cross-sectional | ** | * | 3(/6) | |
| (b) | |||||
| Bagheri et al. [30] | Case-control | * | * | ** | 4(/9) |
| Rohani et al. [44] | Case-control | *** | ** | ** | 7(/9) |
| Sinaei et al. [50] | Case-control | *** | ** | ** | 7(/9) |
| Author Name | Global HRQoL Mean (SD) | Determinants of HRQoL | Signs of Association |
|---|---|---|---|
| Ahmed A et al. [21] | 50.7 (19.2) | Regular exercise | + |
| Multiple tumors | − | ||
| Metastasis | − | ||
| Fever | − | ||
| Age | − | ||
| Ahrafizadeh H [22] | 87.9 (2.15) | Higher level of education | + |
| Higher income | + | ||
| Type of surgery (breast conserving surgery versus mastectomy) | + | ||
| Duration of the disease/diagnosis | + | ||
| Akel R [23] | 108.7 (18.7) | Iraqi | − |
| Stage IV | − | ||
| Monthly income below 1000 USD | − | ||
| Chemotherapy | − | ||
| Anxiety and depression | − | ||
| Akin S [24] | Before chemotherapy: 69.2 (21.6) chemotherapy: 53.3 (20.5) | Age (40–50 years) | − |
| Married | − | ||
| Employed women | − | ||
| Low income | − | ||
| Obesity | − | ||
| Stage I, II, III, | − | ||
| FAC/FEC and Docetaxel/Paclitaxel AC/EC | − | ||
| Diagnosis since 2–6 months | − | ||
| Breast-sparing surgical procedure | − | ||
| Alawadi S [25] | 45.3 (15.3) | Social functioning | − |
| Sexual enjoyment | − | ||
| Pain | − | ||
| Financial difficulty | + | ||
| Albabtain H [26] | CAM = 73.1 (20.2) No CAM = 64.8 (32.7) | Complementary alternative medicine | + |
| Almutairi K [27] | 31.2 (20.5) | Pathological staging | − |
| Al-Naggar R [28] | < 55 years = 83.2 (22.8) ≥ 55 years = 77 (21.6) | Lower income | − |
| >2 years after diagnosis | − | ||
| Under radiotherapy | + | ||
| Al-Natour A [29] | 79.9 (18. 1) | Spiritual wellbeing | + |
| Bagheri M [30] | 73.3 (11.2) | Body image, Appearance evaluative, Appearance orientation, Fitness evaluative, Fitness orientation, Subjective weight, Body satisfaction | + |
| Bayram Z [31] | 63.8 (16.4) | Literate, Homemakers, ECOG2, Stage IV, Chemotherapy agents (gemcitabine+cisplatin). | − |
| Filazoglu G [32] | - | Physical component score: | PCS: |
| Stage of Cancer | − | ||
| Time since operation | + | ||
| Time since diagnosis | + | ||
| Social support | + | ||
| Problem solving coping | + | ||
| Mental component score: | MCS: | ||
| Type of treatment | − | ||
| Stage of Cancer | − | ||
| Time since operation | + | ||
| Social support | + | ||
| Problem solving coping | + | ||
| Helplessness coping | − | ||
| Hujeir H [33] | 59.6 (29.0) | Psychological symptoms | − |
| Physical symptoms | − | ||
| Total memorial symptom assessment scale | − | ||
| Jafari N [34] | 41.4 (18.0) | Social functioning | + |
| Pain | − | ||
| Arm symptoms | − | ||
| Spiritual well-being | + | ||
| Jassim G [35] | 63.9 (21.3) | Advanced stage | − |
| Menopause | − | ||
| Khalili N [36] | 60.3 (21.10) | Emotion focused coping strategy | + |
| Affective interference of pain | − | ||
| Kiadaliri A [37] | Baseline: TAC: 69.3 (0.9) FAC: 69.4 (1.5) | Having children | + |
| Being married | − | ||
| TAC treatment | − | ||
| Mohammadi S [38] | 68.1 (17.7) | Nutritional status (well-nourished) | + |
| Moradi R [39] | 75.9 (15.2) | Economic status | + |
| Self-efficacy | + | ||
| Musarezaei A [40] | Weak HRQoL 16.36% Moderate HRQoL 58.48% Good HRQoL 25.15% | Higher level of education | + |
| Fatigue | − | ||
| Najafi F [41] | 43.86 (23.5) | Older Age | + |
| Nikamenesh Z [42] | 10.78 (2.4) | Self-regulation | + |
| Pehlivan S [43] | 55.1 (10.8) | Age, RTCS, Functional, Symptom | + |
| Rohani C [44] | Baseline: | Sense of coherence | + |
| BC group: 58.1 (20.1) | |||
| Control group: 70.1(21.6) | |||
| 6 months post pre-diagnosis: | Education | + | |
| BC group: 68.7 (18.5) | |||
| Control group: 72.4 (18) | |||
| Safa A [45] | Average QoL: 87% High QoL: 13% | Age | + |
| Disease duration | + | ||
| Fatigue | + | ||
| Interval between diagnosis and treatment | − | ||
| Shakeri J [46] | 70.02 (14.4) | Depression | − |
| Saatci E [47] | 76.1 (14.8) | Unmet needs | + |
| Working women | + | ||
| Safaee A [48] | 64.9 (11.4) | Grade of tumor | − |
| Occupation | + | ||
| Post menopause | + | ||
| Financial difficulties | − | ||
| Dyspnea | − | ||
| Shandiz,F H [49] | 71.4 (22.3) | Older age | − |
| High social status | + | ||
| No radiotherapy | + | ||
| Receiving hormone therapy | + | ||
| Fatigue | − | ||
| Dyspnea | − | ||
| Sinaei F [50] | Mastectomy group: 57.1 Reconstruction group: 72.5 | Breast reconstruction surgery more positive effect on QoL than Mastectomy | + |
| Uzun Ö [51] | 147.6 (24.0) | Education | + |
| Employed women | + | ||
| Zamanian H [52] | 105.0 (22.7) | Positive religious coping | + |
| Zargani A [53] | 73.1 (9.2) | Religiosity | + |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
El Haidari, R.; Abbas, L.A.; Nerich, V.; Anota, A. Factors Associated with Health-Related Quality of Life in Women with Breast Cancer in the Middle East: A Systematic Review. Cancers 2020, 12, 696. https://doi.org/10.3390/cancers12030696
El Haidari R, Abbas LA, Nerich V, Anota A. Factors Associated with Health-Related Quality of Life in Women with Breast Cancer in the Middle East: A Systematic Review. Cancers. 2020; 12(3):696. https://doi.org/10.3390/cancers12030696
Chicago/Turabian StyleEl Haidari, Rana, Linda Abou Abbas, Virginie Nerich, and Amélie Anota. 2020. "Factors Associated with Health-Related Quality of Life in Women with Breast Cancer in the Middle East: A Systematic Review" Cancers 12, no. 3: 696. https://doi.org/10.3390/cancers12030696
APA StyleEl Haidari, R., Abbas, L. A., Nerich, V., & Anota, A. (2020). Factors Associated with Health-Related Quality of Life in Women with Breast Cancer in the Middle East: A Systematic Review. Cancers, 12(3), 696. https://doi.org/10.3390/cancers12030696






