Application of Artificial Intelligence Technology in Oncology: Towards the Establishment of Precision Medicine
Abstract
Simple Summary
Abstract
1. Introduction
2. History of Artificial Intelligence and Its Application in Medicine
2.1. From the 18th Century to the 19th Century: Bayes’ Theorem and Pierre-Simon Laplace
2.2. The Birth of AI, First AI Boom, and First Phase of the AI Winter
2.3. The Second AI Boom and Second Phase of the AI Winter
2.4. The Third AI Boom and Era of Deep Learning
3. Introducing AI Technology in Oncology
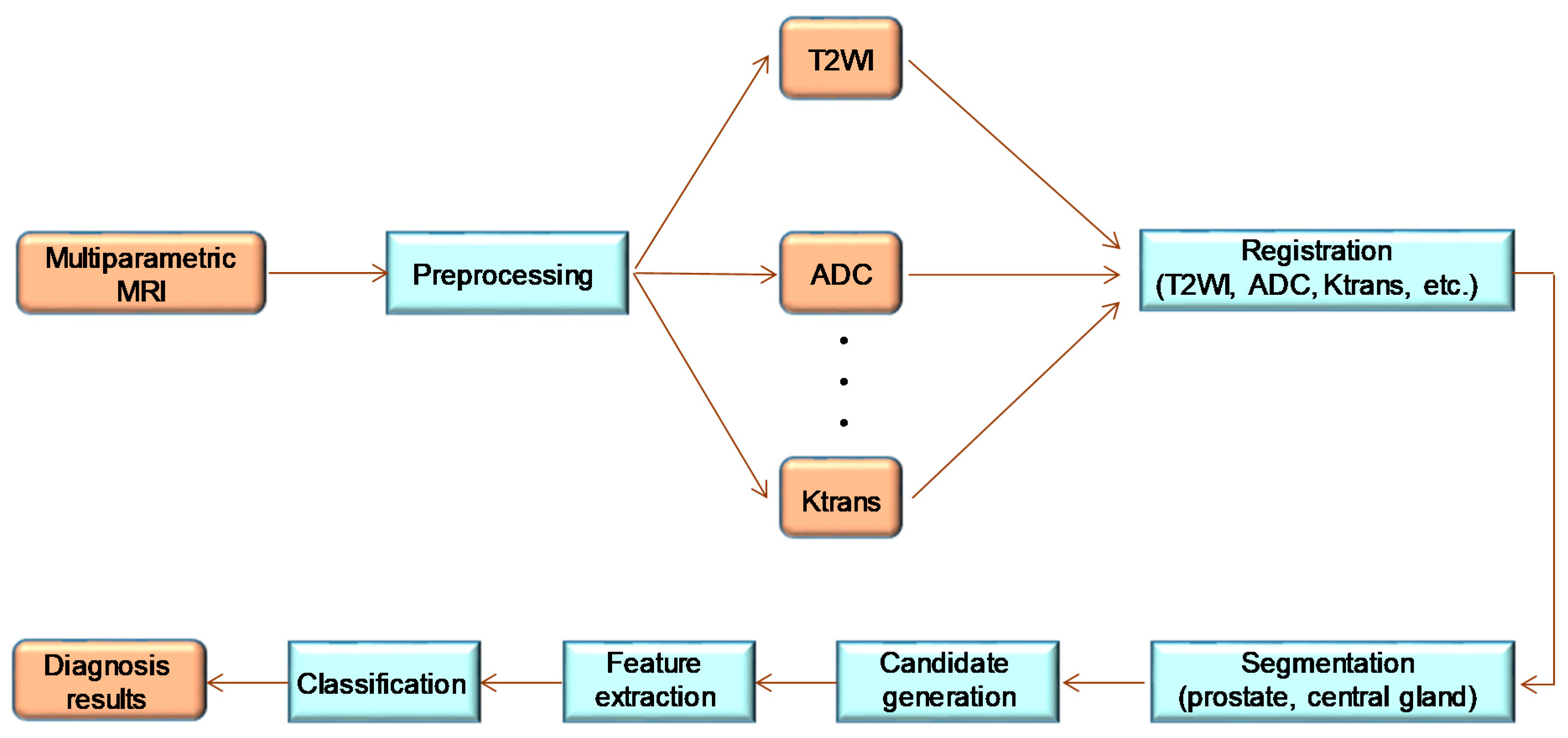
3.1. Radiology
3.2. Endoscopy
3.3. Pathological Images
3.4. Skin Images
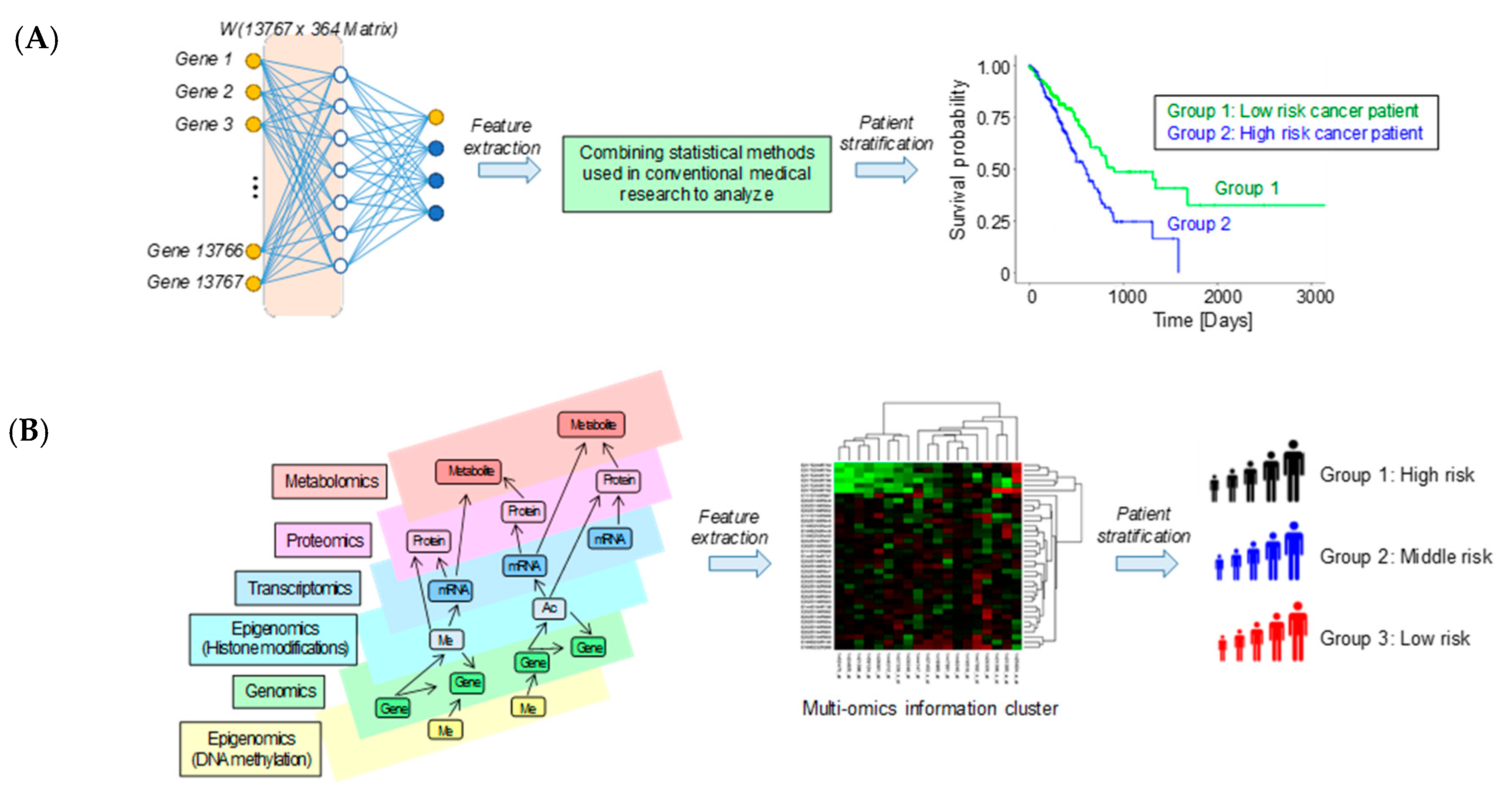
4. Application of Machine Learning and Deep Learning Techniques to Omics Analysis
- Multimodal learning: different types of medical data (e.g., genomic, epigenomic, and proteomic data) can be integrated and treated as inputs;
- Multitasking learning: multiple different tasks can be learned simultaneously by sharing parts of the model;
- Representational and semi-supervised learning: acquire a way to represent data from large amounts of unlabeled data, making it possible to learn from small amounts of labeled data;
- It is possible to capture higher order correlations of inputs.
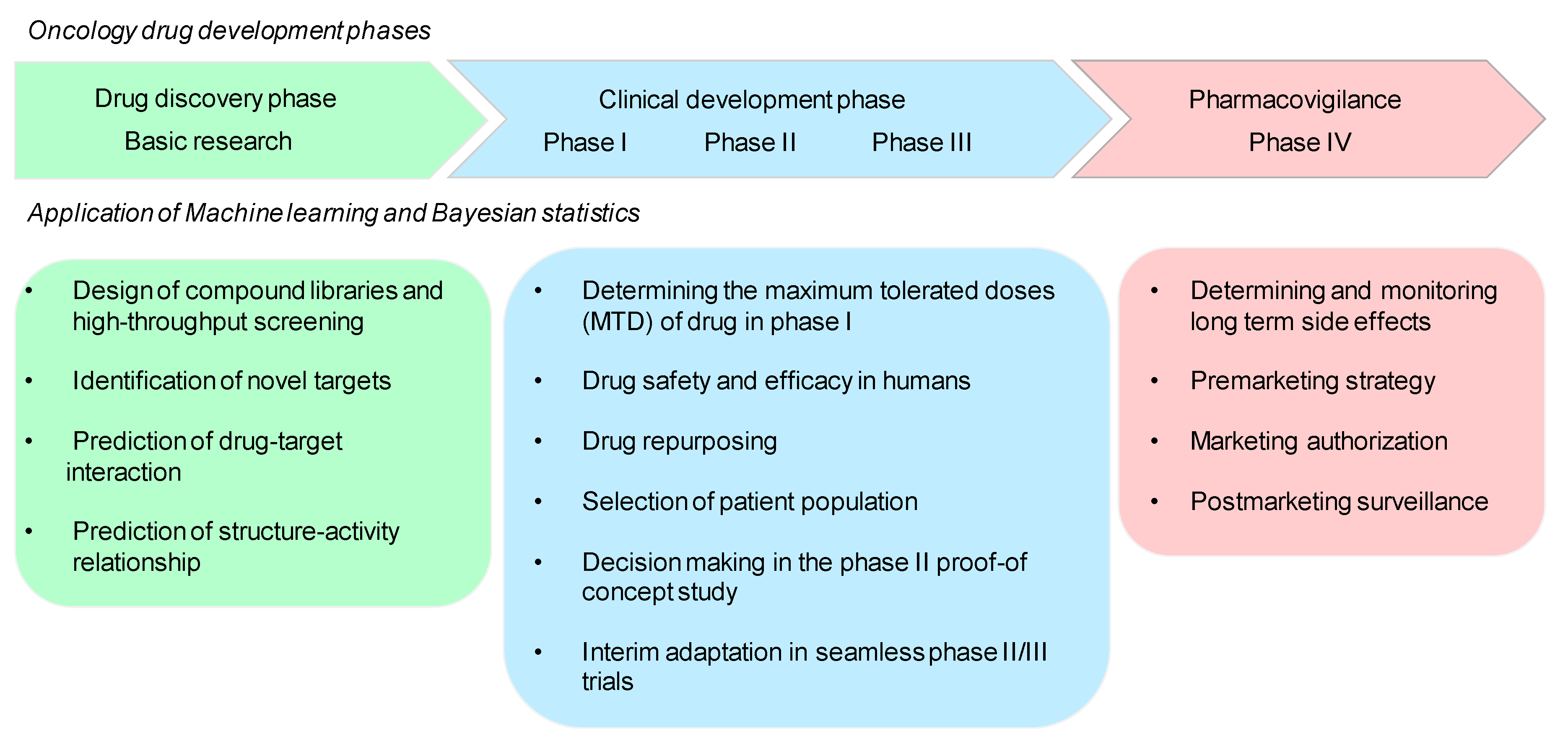
5. Drug Development Using Machine Learning and Bayesian Statistics in Oncology
6. Issues to Be Overcome in the Application of AI to Oncology
6.1. Overfitting
6.2. Black Box Problem
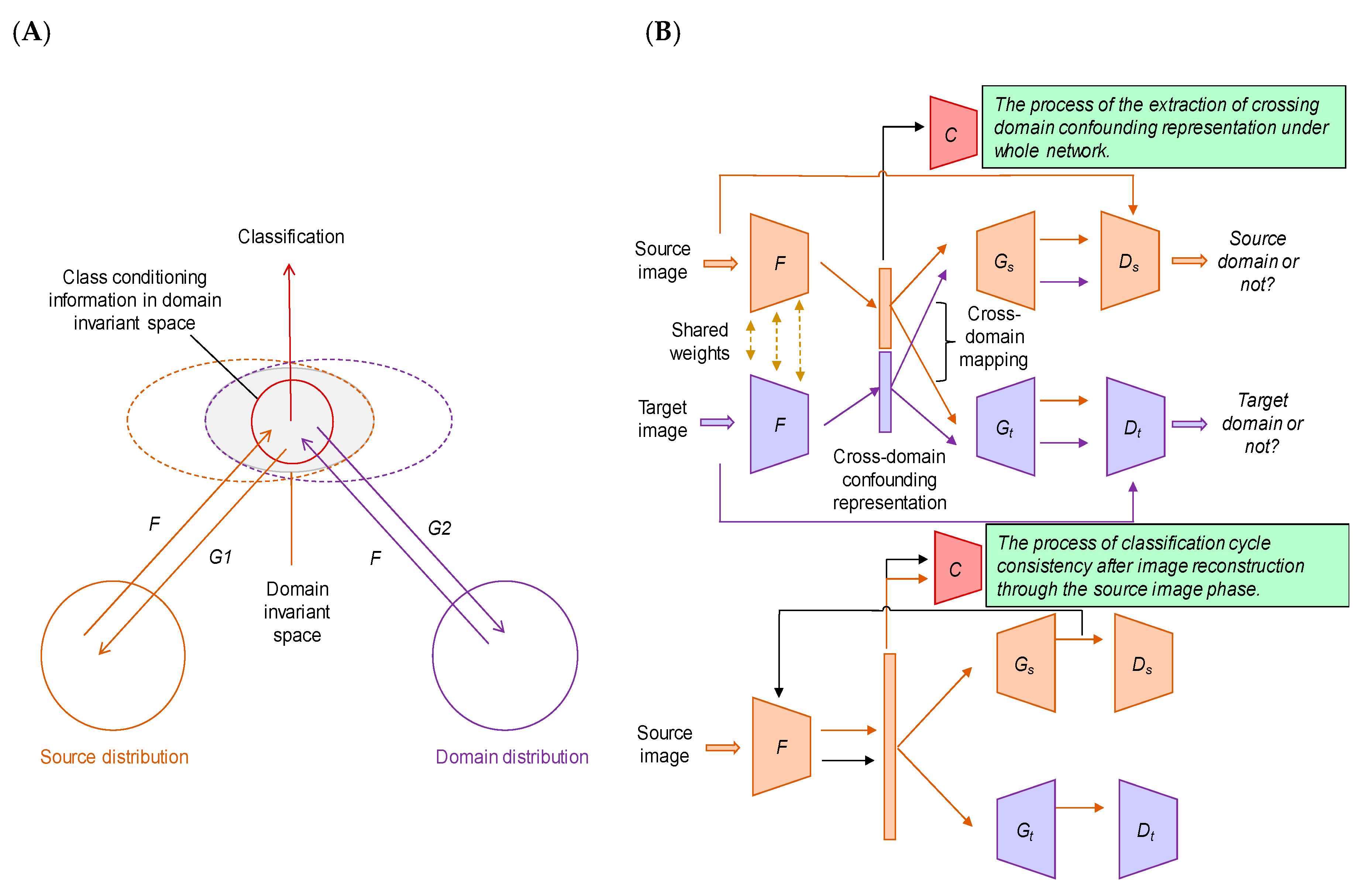
6.3. Discrepancies among Facilities, especially in Medical Imaging (Domain Shift and Domain Adaptation)
7. Concluding Remarks and Future Perspectives
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Hamamoto, R.; Komatsu, M.; Takasawa, K.; Asada, K.; Kaneko, S. Epigenetics Analysis and Integrated Analysis of Multiomics Data, Including Epigenetic Data, Using Artificial Intelligence in the Era of Precision Medicine. Biomolecules 2020, 10, 62. [Google Scholar] [CrossRef] [PubMed]
- Moor, J. The Dartmouth College Artificial Intelligence Conference: The Next Fifty years. AI Mag. 2006, 27, 87–89. [Google Scholar]
- Fujita, H. AI-based computer-aided diagnosis (AI-CAD): The latest review to read first. Radiol. Phys. Technol. 2020, 13, 6–19. [Google Scholar] [CrossRef] [PubMed]
- Nakaura, T.; Higaki, T.; Awai, K.; Ikeda, O.; Yamashita, Y. A primer for understanding radiology articles about machine learning and deep learning. Diagn. Interv. Imaging 2020. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.W.; Gao, J.X. Big Data Bioinformatics. Methods 2016, 111, 1–2. [Google Scholar] [CrossRef]
- Kumar, A.; Kim, J.; Lyndon, D.; Fulham, M.; Feng, D. An Ensemble of Fine-Tuned Convolutional Neural Networks for Medical Image Classification. IEEE J. Biomed. Health Inform. 2017, 21, 31–40. [Google Scholar] [CrossRef] [PubMed]
- Monshi, M.M.A.; Poon, J.; Chung, V. Deep learning in generating radiology reports: A survey. Artif. Intell. Med. 2020, 106, 101878. [Google Scholar] [CrossRef]
- Falk, T.; Mai, D.; Bensch, R.; Cicek, O.; Abdulkadir, A.; Marrakchi, Y.; Bohm, A.; Deubner, J.; Jackel, Z.; Seiwald, K.; et al. U-Net: Deep learning for cell counting, detection, and morphometry. Nat. Methods 2019, 16, 67–70. [Google Scholar] [CrossRef]
- Prasad, V.; Fojo, T.; Brada, M. Precision oncology: Origins, optimism, and potential. Lancet Oncol. 2016, 17, e81–e86. [Google Scholar] [CrossRef]
- Senft, D.; Leiserson, M.D.M.; Ruppin, E.; Ronai, Z.A. Precision Oncology: The Road Ahead. Trends Mol. Med. 2017, 23, 874–898. [Google Scholar] [CrossRef]
- Ku, S.Y.; Gleave, M.E.; Beltran, H. Towards precision oncology in advanced prostate cancer. Nat. Rev. Urol. 2019, 16, 645–654. [Google Scholar] [CrossRef] [PubMed]
- Markman, M. Precision Cancer Medicine. MD Advis. 2018, 11, 4–6. [Google Scholar] [PubMed]
- Rodon, J.; Soria, J.C.; Berger, R.; Miller, W.H.; Rubin, E.; Kugel, A.; Tsimberidou, A.; Saintigny, P.; Ackerstein, A.; Brana, I.; et al. Genomic and transcriptomic profiling expands precision cancer medicine: The WINTHER trial. Nat. Med. 2019, 25, 751–758. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Yang, H.; Zhang, R. Challenges and future of precision medicine strategies for breast cancer based on a database on drug reactions. Biosci. Rep. 2019, 39. [Google Scholar] [CrossRef]
- Prasad, V. Perspective: The precision-oncology illusion. Nature 2016, 537, S63. [Google Scholar] [CrossRef]
- Meric-Bernstam, F.; Brusco, L.; Shaw, K.; Horombe, C.; Kopetz, S.; Davies, M.A.; Routbort, M.; Piha-Paul, S.A.; Janku, F.; Ueno, N.; et al. Feasibility of Large-Scale Genomic Testing to Facilitate Enrollment Onto Genomically Matched Clinical Trials. J. Clin. Oncol. 2015, 33, 2753–2762. [Google Scholar] [CrossRef]
- Bayes, T. An Essay towards solving a Problem in the Doctrine of Chance. Philos. Trans. R. Soc. Lond. 1763, 53, 370–418. [Google Scholar] [CrossRef]
- Gelman, A.; Stern, H.S.; Carlin, J.B.; Dunson, D.B.; Vehtari, A.; Rubin, D.B. Bayesian Data Analysis; Chapman and Hall/CRC: Boca Raton, FL, USA, 2013. [Google Scholar]
- Fienberg, S.E. When did Bayesian inference become “Bayesian”? Bayesian Anal. 2006, 1, 1–40. [Google Scholar] [CrossRef]
- Solomonoff, R.J. The Time Scale of Artificial Intelligence; Reflections on Social Effects. Hum. Syst. Manag. 1985, 5, 149–153. [Google Scholar] [CrossRef]
- Russell, S.; Norvig, P. Artificial Intelligence: A Modern Approach; Prentice Hall: Upper Saddle River, NJ, USA, 1995. [Google Scholar]
- Luger, G.; Stubblefield, W. Artificial Intelligence: Structures and Strategies for Complex Problem Solving; Benjamin/Cummings: San Francisco, CA, USA, 2004. [Google Scholar]
- Nillson, M. Artificial Intelligence: A New Synthesis; Morgan Kaufmann: Burlington, MA, USA, 1998. [Google Scholar]
- Lindsay, R.; Buchanan, B.; Feigenbaum, E.; Lederberg, J. Applications of Artificial Intelligence for Organic Chemistry: The DENDRAL Project; McGraw-Hill: New York, NY, USA, 1980. [Google Scholar]
- Shortliffe, E.H. Computer-Based Medical Consultations: MYCIN; Elsevier: North Holland, NY, USA, 1976. [Google Scholar]
- Feigenbaum, E.A. Knowledge Engineering: The Applied Side of Artificial Intelligence. Ann. N. Y. Acad. Sci. 1984, 1, 91–107. [Google Scholar] [CrossRef]
- Karimi, A.M.; Çelebi, F.V.; Mohammed, A.S. Software Development for Blood Disease Expert System. Lect. Notes Softw. Eng. 2016, 4, 179–183. [Google Scholar]
- Heckerman, D.; Shortliffe, E. From Certainty Factors to Belief Networks. Artif. Intell. Med. 1992, 4, 35–52. [Google Scholar] [CrossRef]
- Hinton, G.E.; Salakhutdinov, R.R. Reducing the Dimensionality of Data with Neural Networks. Science 2006, 313, 504–507. [Google Scholar] [CrossRef] [PubMed]
- Krizhevsky, A.; Sutskever, I.; Hinton, G.E. ImageNet classification with deep convolutional neural networks. Adv. Neural Inf. Process. Syst. 2012, 1097–1105. [Google Scholar] [CrossRef]
- Markoff, J. How Many Computers to Identify a Cat? 16,000. The New York Times, 25 June 2012. [Google Scholar]
- Asada, K.; Kobayashi, K.; Joutard, S.; Tubaki, M.; Takahashi, S.; Takasawa, K.; Komatsu, M.; Kaneko, S.; Sese, J.; Hamamoto, R. Uncovering Prognosis-Related Genes and Pathways by Multi-Omics Analysis in Lung Cancer. Biomolecules 2020, 10, 524. [Google Scholar] [CrossRef]
- Jinnai, S.; Yamazaki, N.; Hirano, Y.; Sugawara, Y.; Ohe, Y.; Hamamoto, R. The Development of a Skin Cancer Classification System for Pigmented Skin Lesions Using Deep Learning. Biomolecules 2020, 10, 1123. [Google Scholar] [CrossRef]
- Kobayashi, K.; Bolatkan, A.; Shiina, S.; Hamamoto, R. Fully-Connected Neural Networks with Reduced Parameterization for Predicting Histological Types of Lung Cancer from Somatic Mutations. Biomolecules 2020, 10, 1249. [Google Scholar] [CrossRef]
- Kobayashi, K.; Hataya, R.; Kurose, Y.; Bolatkan, A.; Miyake, M.; Watanabe, H.; Takahashi, M.; Mihara, N.; Itami, J.; Harada, T.; et al. Unsupervised Brain Abnormality Detection Using High Fidelity Image Reconstruction Networks. arXiv 2020, arXiv:2005.12573. [Google Scholar]
- Yamada, M.; Saito, Y.; Imaoka, H.; Saiko, M.; Yamada, S.; Kondo, H.; Takamaru, H.; Sakamoto, T.; Sese, J.; Kuchiba, A.; et al. Development of a real-time endoscopic image diagnosis support system using deep learning technology in colonoscopy. Sci. Rep. 2019, 9, 14465. [Google Scholar] [CrossRef]
- Yasutomi, S.; Arakaki, T.; Hamamoto, R. Shadow Detection for Ultrasound Images Using Unlabeled Data and Synthetic Shadows. arXiv 2019, arXiv:1908.01439. [Google Scholar]
- Weisberg, E.M.; Chu, L.C.; Park, S.; Yuille, A.L.; Kinzler, K.W.; Vogelstein, B.; Fishman, E.K. Deep lessons learned: Radiology, oncology, pathology, and computer science experts unite around artificial intelligence to strive for earlier pancreatic cancer diagnosis. Diagn. Interv. Imaging 2020, 101, 111–115. [Google Scholar] [CrossRef] [PubMed]
- Dong, J.; Geng, Y.; Lu, D.; Li, B.; Tian, L.; Lin, D.; Zhang, Y. Clinical Trials for Artificial Intelligence in Cancer Diagnosis: A Cross-Sectional Study of Registered Trials in ClinicalTrials.gov. Front. Oncol. 2020, 10, 1629. [Google Scholar] [CrossRef] [PubMed]
- Blanc, D.; Racine, V.; Khalil, A.; Deloche, M.; Broyelle, J.A.; Hammouamri, I.; Sinitambirivoutin, E.; Fiammante, M.; Verdier, E.; Besson, T.; et al. Artificial intelligence solution to classify pulmonary nodules on CT. Diagn. Interv. Imaging 2020. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Y.; Edwards, A.V.; Newstead, G.M. Artificial Intelligence Applied to Breast MRI for Improved Diagnosis. Radiology 2020, 200292. [Google Scholar] [CrossRef]
- European Society of Radiology. What the radiologist should know about artificial intelligence—An ESR white paper. Insights Imaging 2019, 10, 44. [Google Scholar] [CrossRef]
- Qin, C.; Yao, D.; Shi, Y.; Song, Z. Computer-aided detection in chest radiography based on artificial intelligence: A survey. Biomed. Eng. Online 2018, 17, 113. [Google Scholar] [CrossRef]
- Wang, S.; Burtt, K.; Turkbey, B.; Choyke, P.; Summers, R.M. Computer aided-diagnosis of prostate cancer on multiparametric MRI: A technical review of current research. Biomed. Res. Int. 2014, 2014, 789561. [Google Scholar] [CrossRef]
- Transin, S.; Souchon, R.; Gonindard-Melodelima, C.; de Rozario, R.; Walker, P.; de la Vega, M.F.; Loffroy, R.; Cormier, L.; Rouviere, O. Computer-aided diagnosis system for characterizing ISUP grade>/=2 prostate cancers at multiparametric MRI: A cross-vendor evaluation. Diagn. Interv. Imaging 2019, 100, 801–811. [Google Scholar] [CrossRef]
- Hizukuri, A.; Nakayama, R.; Nara, M.; Suzuki, M.; Namba, K. Computer-Aided Diagnosis Scheme for Distinguishing Between Benign and Malignant Masses on Breast DCE-MRI Images Using Deep Convolutional Neural Network with Bayesian Optimization. J. Digit. Imaging 2020. [Google Scholar] [CrossRef]
- Huang, F.; Zhang, Z.; Wang, N.; Li, N.; Du, M.; Hao, T.; Zhan, J. A new direction to promote the implementation of artificial intelligence in natural clinical settings. arXiv 2019, arXiv:1905.02940. [Google Scholar]
- Ha, E.J.; Baek, J.H. Application of machine learning and deep learning to thyroid imaging: Where do we stand? Ultrasonography 2020. [Google Scholar] [CrossRef] [PubMed]
- Dlamini, Z.; Francies, F.Z.; Hull, R.; Marima, R. Artificial intelligence (AI) and big data in cancer and precision oncology. Comput. Struct. Biotechnol. J. 2020, 18, 2300–2311. [Google Scholar] [CrossRef] [PubMed]
- Hwang, T.J.; Kesselheim, A.S.; Vokinger, K.N. Lifecycle Regulation of Artificial Intelligence- and Machine Learning-Based Software Devices in Medicine. JAMA 2019. [Google Scholar] [CrossRef] [PubMed]
- Tanenbaum, L.N. Artificial Intelligence and Medical Imaging: Image Acquisition and Reconstruction. Appl. Radiol. 2020, 49, 34–35. [Google Scholar]
- Bryant, M. The Potential and Reality of AI in Clinical Application. Appl. Radiol. 2020, 49, 10–11. [Google Scholar]
- Hsieh, J.; Liu, E.; Nett, B.; Tang, J.; Thibault, J.B.; Sahney, S. A New Era of Image Reconstruction: TrueFidelity™. Technical White Paper on Deep Learning Image Reconstruction; GE Healthcare: Chicago, IL, USA, 2019. [Google Scholar]
- Bryant, M.; Massat, M.B. The Ubiquity of AI at RSNA 2019. Appl. Radiol. 2020, 49, 32–38. [Google Scholar]
- Ministry of Economy, Trade and Industry. The Medical Device Industry in Japan. Report from the Medical and Assistive Device Industries Office, 2018. Available online: https://www.meti.go.jp/committee/kenkyukai/iryou_innovation/pdf/002_05_00.pdf (accessed on 8 February 2018).
- Kudo, S.E.; Misawa, M.; Mori, Y.; Hotta, K.; Ohtsuka, K.; Ikematsu, H.; Saito, Y.; Takeda, K.; Nakamura, H.; Ichimasa, K.; et al. Artificial Intelligence-assisted System Improves Endoscopic Identification of Colorectal Neoplasms. Clin. Gastroenterol. Hepatol. 2020, 18, 1874–1881.e2. [Google Scholar] [CrossRef]
- Hori, M.; Matsuda, T.; Shibata, A.; Katanoda, K.; Sobue, T.; Nishimoto, H.; Japan Cancer Surveillance Research Group. Cancer incidence and incidence rates in Japan in 2009: A study of 32 population-based cancer registries for the Monitoring of Cancer Incidence in Japan (MCIJ) project. Jpn. J. Clin. Oncol. 2015, 45, 884–891. [Google Scholar] [CrossRef]
- Winawer, S.J.; Zauber, A.G.; Ho, M.N.; O’Brien, M.J.; Gottlieb, L.S.; Sternberg, S.S.; Waye, J.D.; Schapiro, M.; Bond, J.H.; Panish, J.F.; et al. Prevention of colorectal cancer by colonoscopic polypectomy. The National Polyp Study Workgroup. N. Engl. J. Med. 1993, 329, 1977–1981. [Google Scholar] [CrossRef]
- Zauber, A.G.; Winawer, S.J.; O’Brien, M.J.; Lansdorp-Vogelaar, I.; van Ballegooijen, M.; Hankey, B.F.; Shi, W.; Bond, J.H.; Schapiro, M.; Panish, J.F.; et al. Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. N. Engl. J. Med. 2012, 366, 687–696. [Google Scholar] [CrossRef]
- Metter, D.M.; Colgan, T.J.; Leung, S.T.; Timmons, C.F.; Park, J.Y. Trends in the US and Canadian Pathologist Workforces From 2007 to 2017. JAMA Netw. Open 2019, 2, e194337. [Google Scholar] [CrossRef] [PubMed]
- Yoshizawa, A. A trial of integrated telepathology (iTP) in Nagano prefecture. Rinsho. Byori. 2013, 61, 65–73. [Google Scholar] [PubMed]
- Coudray, N.; Ocampo, P.S.; Sakellaropoulos, T.; Narula, N.; Snuderl, M.; Fenyo, D.; Moreira, A.L.; Razavian, N.; Tsirigos, A. Classification and mutation prediction from non-small cell lung cancer histopathology images using deep learning. Nat. Med. 2018, 24, 1559–1567. [Google Scholar] [CrossRef] [PubMed]
- Schadendorf, D.; van Akkooi, A.C.J.; Berking, C.; Griewank, K.G.; Gutzmer, R.; Hauschild, A.; Stang, A.; Roesch, A.; Ugurel, S. Melanoma. Lancet 2018, 392, 971–984. [Google Scholar] [CrossRef]
- Melanoma of the Skin 2019 . In Cancer Stat Facts; National Cancer Institute: Bethesda, MD, USA, 2019.
- Esteva, A.; Kuprel, B.; Novoa, R.A.; Ko, J.; Swetter, S.M.; Blau, H.M.; Thrun, S. Dermatologist-level classification of skin cancer with deep neural networks. Nature 2017, 542, 115–118. [Google Scholar] [CrossRef]
- Collins, F.S.; Morgan, M.; Patrinos, A. The Human Genome Project: Lessons from large-scale biology. Science 2003, 300, 286–290. [Google Scholar] [CrossRef]
- Auffray, C.; Caulfield, T.; Khoury, M.J.; Lupski, J.R.; Schwab, M.; Veenstra, T. Genome Medicine: Past, present and future. Genome Med. 2011, 3, 6. [Google Scholar] [CrossRef]
- Ashley, E.A. The precision medicine initiative: A new national effort. JAMA 2015, 313, 2119–2120. [Google Scholar] [CrossRef]
- Oki, S.; Sone, K.; Oda, K.; Hamamoto, R.; Ikemura, M.; Maeda, D.; Takeuchi, M.; Tanikawa, M.; Mori-Uchino, M.; Nagasaka, K.; et al. Oncogenic histone methyltransferase EZH2: A novel prognostic marker with therapeutic potential in endometrial cancer. Oncotarget 2017, 8, 40402–40411. [Google Scholar] [CrossRef]
- Saloura, V.; Vougiouklakis, T.; Zewde, M.; Deng, X.; Kiyotani, K.; Park, J.H.; Matsuo, Y.; Lingen, M.; Suzuki, T.; Dohmae, N.; et al. WHSC1L1-mediated EGFR mono-methylation enhances the cytoplasmic and nuclear oncogenic activity of EGFR in head and neck cancer. Sci. Rep. 2017, 7, 40664. [Google Scholar] [CrossRef]
- Yoshioka, Y.; Suzuki, T.; Matsuo, Y.; Nakakido, M.; Tsurita, G.; Simone, C.; Watanabe, T.; Dohmae, N.; Nakamura, Y.; Hamamoto, R. SMYD3-mediated lysine methylation in the PH domain is critical for activation of AKT1. Oncotarget 2016, 7, 75023–75037. [Google Scholar] [CrossRef] [PubMed]
- Saloura, V.; Vougiouklakis, T.; Zewde, M.; Kiyotani, K.; Park, J.H.; Gao, G.; Karrison, T.; Lingen, M.; Nakamura, Y.; Hamamoto, R. WHSC1L1 drives cell cycle progression through transcriptional regulation of CDC6 and CDK2 in squamous cell carcinoma of the head and neck. Oncotarget 2016, 7, 42527–42538. [Google Scholar] [CrossRef] [PubMed]
- Shigekawa, Y.; Hayami, S.; Ueno, M.; Miyamoto, A.; Suzaki, N.; Kawai, M.; Hirono, S.; Okada, K.I.; Hamamoto, R.; Yamaue, H. Overexpression of KDM5B/JARID1B is associated with poor prognosis in hepatocellular carcinoma. Oncotarget 2018, 9, 34320–34335. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.K.; Kim, K.; Ryu, J.W.; Ryu, T.Y.; Lim, J.H.; Oh, J.H.; Min, J.K.; Jung, C.R.; Hamamoto, R.; Son, M.Y.; et al. The novel prognostic marker, EHMT2, is involved in cell proliferation via HSPD1 regulation in breast cancer. Int. J. Oncol. 2019, 54, 65–76. [Google Scholar] [CrossRef]
- Toyokawa, G.; Takada, K.; Tagawa, T.; Hamamoto, R.; Yamada, Y.; Shimokawa, M.; Oda, Y.; Maehara, Y. A Positive Correlation Between the EZH2 and PD-L1 Expression in Resected Lung Adenocarcinomas. Ann. Thorac. Surg. 2019, 107, 393–400. [Google Scholar] [CrossRef]
- Toyokawa, G.; Takada, K.; Tagawa, T.; Kinoshita, F.; Kozuma, Y.; Matsubara, T.; Haratake, N.; Takamori, S.; Akamine, T.; Hirai, F.; et al. Prevalence of Enhancer of Zeste Homolog 2 in Patients with Resected Small Cell Lung Cancer. Anticancer Res. 2018, 38, 3707–3711. [Google Scholar] [CrossRef]
- Ryu, J.W.; Kim, S.K.; Son, M.Y.; Jeon, S.J.; Oh, J.H.; Lim, J.H.; Cho, S.; Jung, C.R.; Hamamoto, R.; Kim, D.S.; et al. Novel prognostic marker PRMT1 regulates cell growth via downregulation of CDKN1A in HCC. Oncotarget 2017, 8, 115444–115455. [Google Scholar] [CrossRef]
- Kim, S.; Bolatkan, A.; Kaneko, S.; Ikawa, N.; Asada, K.; Komatsu, M.; Hayami, S.; Ojima, H.; Abe, N.; Yamaue, H.; et al. Deregulation of the Histone Lysine-Specific Demethylase 1 Is Involved in Human Hepatocellular Carcinoma. Biomolecules 2019, 9, 810. [Google Scholar] [CrossRef]
- Saloura, V.; Vougiouklakis, T.; Bao, R.; Kim, S.; Baek, S.; Zewde, M.; Bernard, B.; Burkitt, K.; Nigam, N.; Izumchenko, E.; et al. WHSC1 monomethylates histone H1 and induces stem-cell like features in squamous cell carcinoma of the head and neck. Neoplasia 2020, 22, 283–293. [Google Scholar] [CrossRef]
- Asada, K.; Bolatkan, A.; Takasawa, K.; Komatsu, M.; Kaneko, S.; Hamamoto, R. Critical Roles of N(6)-Methyladenosine (m(6)A) in Cancer and Virus Infection. Biomolecules 2020, 10, 1071. [Google Scholar] [CrossRef]
- Kojima, M.; Sone, K.; Oda, K.; Hamamoto, R.; Kaneko, S.; Oki, S.; Kukita, A.; Kawata, A.; Honjoh, H.; Kawata, Y.; et al. The histone methyltransferase SMYD2 is a novel therapeutic target for the induction of apoptosis in ovarian clear cell carcinoma cells. Oncol. Lett. 2020, 20, 153. [Google Scholar] [CrossRef] [PubMed]
- Sone, K.; Piao, L.; Nakakido, M.; Ueda, K.; Jenuwein, T.; Nakamura, Y.; Hamamoto, R. Critical role of lysine 134 methylation on histone H2AX for gamma-H2AX production and DNA repair. Nat. Commun. 2014, 5, 5691. [Google Scholar] [CrossRef] [PubMed]
- Cho, H.S.; Kelly, J.D.; Hayami, S.; Toyokawa, G.; Takawa, M.; Yoshimatsu, M.; Tsunoda, T.; Field, H.I.; Neal, D.E.; Ponder, B.A.; et al. Enhanced expression of EHMT2 is involved in the proliferation of cancer cells through negative regulation of SIAH1. Neoplasia 2011, 13, 676–684. [Google Scholar] [CrossRef] [PubMed]
- Cho, H.S.; Toyokawa, G.; Daigo, Y.; Hayami, S.; Masuda, K.; Ikawa, N.; Yamane, Y.; Maejima, K.; Tsunoda, T.; Field, H.I.; et al. The JmjC domain-containing histone demethylase KDM3A is a positive regulator of the G1/S transition in cancer cells via transcriptional regulation of the HOXA1 gene. Int. J. Cancer 2012, 131, E179–E189. [Google Scholar] [CrossRef] [PubMed]
- Hamamoto, R.; Furukawa, Y.; Morita, M.; Iimura, Y.; Silva, F.P.; Li, M.; Yagyu, R.; Nakamura, Y. SMYD3 encodes a histone methyltransferase involved in the proliferation of cancer cells. Nat. Cell Biol. 2004, 6, 731–740. [Google Scholar] [CrossRef]
- Hamamoto, R.; Silva, F.P.; Tsuge, M.; Nishidate, T.; Katagiri, T.; Nakamura, Y.; Furukawa, Y. Enhanced SMYD3 expression is essential for the growth of breast cancer cells. Cancer Sci. 2006, 97, 113–118. [Google Scholar] [CrossRef]
- Hayami, S.; Kelly, J.D.; Cho, H.S.; Yoshimatsu, M.; Unoki, M.; Tsunoda, T.; Field, H.I.; Neal, D.E.; Yamaue, H.; Ponder, B.A.; et al. Overexpression of LSD1 contributes to human carcinogenesis through chromatin regulation in various cancers. Int. J. Cancer 2011, 128, 574–586. [Google Scholar] [CrossRef]
- Hayami, S.; Yoshimatsu, M.; Veerakumarasivam, A.; Unoki, M.; Iwai, Y.; Tsunoda, T.; Field, H.I.; Kelly, J.D.; Neal, D.E.; Yamaue, H.; et al. Overexpression of the JmjC histone demethylase KDM5B in human carcinogenesis: Involvement in the proliferation of cancer cells through the E2F/RB pathway. Mol. Cancer 2010, 9, 59. [Google Scholar] [CrossRef]
- Kang, D.; Cho, H.S.; Toyokawa, G.; Kogure, M.; Yamane, Y.; Iwai, Y.; Hayami, S.; Tsunoda, T.; Field, H.I.; Matsuda, K.; et al. The histone methyltransferase Wolf-Hirschhorn syndrome candidate 1-like 1 (WHSC1L1) is involved in human carcinogenesis. Genes Chromosomes Cancer 2013, 52, 126–139. [Google Scholar] [CrossRef]
- Mutonga, M.; Tamura, K.; Malnassy, G.; Fulton, N.; de Albuquerque, A.; Hamamoto, R.; Stock, W.; Nakamura, Y.; Alachkar, H. Targeting Suppressor of Variegation 3-9 Homologue 2 (SUV39H2) in Acute Lymphoblastic Leukemia (ALL). Transl. Oncol. 2015, 8, 368–375. [Google Scholar] [CrossRef]
- Saloura, V.; Cho, H.S.; Kyiotani, K.; Alachkar, H.; Zuo, Z.; Nakakido, M.; Tsunoda, T.; Seiwert, T.; Lingen, M.; Licht, J.; et al. WHSC1 Promotes Oncogenesis through Regulation of NIMA-related-kinase-7 in Squamous Cell Carcinoma of the Head and Neck. Mol. Cancer Res. 2015, 13, 293–304. [Google Scholar] [CrossRef] [PubMed]
- Silva, F.P.; Hamamoto, R.; Kunizaki, M.; Tsuge, M.; Nakamura, Y.; Furukawa, Y. Enhanced methyltransferase activity of SMYD3 by the cleavage of its N-terminal region in human cancer cells. Oncogene 2008, 27, 2686–2692. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Toyokawa, G.; Cho, H.S.; Iwai, Y.; Yoshimatsu, M.; Takawa, M.; Hayami, S.; Maejima, K.; Shimizu, N.; Tanaka, H.; Tsunoda, T.; et al. The histone demethylase JMJD2B plays an essential role in human carcinogenesis through positive regulation of cyclin-dependent kinase 6. Cancer Prev. Res. 2011, 4, 2051–2061. [Google Scholar] [CrossRef] [PubMed]
- Toyokawa, G.; Cho, H.S.; Masuda, K.; Yamane, Y.; Yoshimatsu, M.; Hayami, S.; Takawa, M.; Iwai, Y.; Daigo, Y.; Tsuchiya, E.; et al. Histone Lysine Methyltransferase Wolf-Hirschhorn Syndrome Candidate 1 Is Involved in Human Carcinogenesis through Regulation of the Wnt Pathway. Neoplasia 2011, 13, 887–898. [Google Scholar] [CrossRef]
- Takawa, M.; Masuda, K.; Kunizaki, M.; Daigo, Y.; Takagi, K.; Iwai, Y.; Cho, H.S.; Toyokawa, G.; Yamane, Y.; Maejima, K.; et al. Validation of the histone methyltransferase EZH2 as a therapeutic target for various types of human cancer and as a prognostic marker. Cancer Sci. 2011, 102, 1298–1305. [Google Scholar] [CrossRef] [PubMed]
- Tsuge, M.; Hamamoto, R.; Silva, F.P.; Ohnishi, Y.; Chayama, K.; Kamatani, N.; Furukawa, Y.; Nakamura, Y. A variable number of tandem repeats polymorphism in an E2F-1 binding element in the 5′ flanking region of SMYD3 is a risk factor for human cancers. Nat. Genet. 2005, 37, 1104–1107. [Google Scholar] [CrossRef]
- Miles, W.O.; Lepesant, J.M.; Bourdeaux, J.; Texier, M.; Kerenyi, M.A.; Nakakido, M.; Hamamoto, R.; Orkin, S.H.; Dyson, N.J.; Di Stefano, L. The LSD1 Family of Histone Demethylases and the Pumilio Posttranscriptional Repressor Function in a Complex Regulatory Feedback Loop. Mol. Cell. Biol. 2015, 35, 4199–4211. [Google Scholar] [CrossRef]
- Yoshimatsu, M.; Toyokawa, G.; Hayami, S.; Unoki, M.; Tsunoda, T.; Field, H.I.; Kelly, J.D.; Neal, D.E.; Maehara, Y.; Ponder, B.A.; et al. Dysregulation of PRMT1 and PRMT6, Type I arginine methyltransferases, is involved in various types of human cancers. Int. J. Cancer 2011, 128, 562–573. [Google Scholar] [CrossRef]
- Toyokawa, G.; Taguchi, K.; Edagawa, M.; Shimamatsu, S.; Toyozawa, R.; Nosaki, K.; Hirai, F.; Yamaguchi, M.; Shimokawa, M.; Seto, T.; et al. The Prognostic Impact of Jumonji Domain-containing 2B in Patients with Resected Lung Adenocarcinoma. Anticancer Res. 2016, 36, 4841–4846. [Google Scholar] [CrossRef]
- Hamamoto, R.; Saloura, V.; Nakamura, Y. Critical roles of non-histone protein lysine methylation in human tumorigenesis. Nat. Rev. Cancer 2015, 15, 110–124. [Google Scholar] [CrossRef]
- Hamamoto, R.; Nakamura, Y. Dysregulation of protein methyltransferases in human cancer: An emerging target class for anticancer therapy. Cancer Sci. 2016, 107, 377–384. [Google Scholar] [CrossRef] [PubMed]
- Vougiouklakis, T.; Hamamoto, R.; Nakamura, Y.; Saloura, V. The NSD family of protein methyltransferases in human cancer. Epigenomics 2015, 7, 863–874. [Google Scholar] [CrossRef] [PubMed]
- Berdasco, M.; Esteller, M. Clinical epigenetics: Seizing opportunities for translation. Nat. Rev. Genet. 2019, 20, 109–127. [Google Scholar] [CrossRef] [PubMed]
- Kukita, A.; Sone, K.; Oda, K.; Hamamoto, R.; Kaneko, S.; Komatsu, M.; Wada, M.; Honjoh, H.; Kawata, Y.; Kojima, M.; et al. Histone methyltransferase SMYD2 selective inhibitor LLY-507 in combination with poly ADP ribose polymerase inhibitor has therapeutic potential against high-grade serous ovarian carcinomas. Biochem. Biophys. Res. Commun. 2019, 513, 340–346. [Google Scholar] [CrossRef]
- Chaudhary, K.; Poirion, O.B.; Lu, L.; Garmire, L.X. Deep Learning-Based Multi-Omics Integration Robustly Predicts Survival in Liver Cancer. Clin. Cancer Res. 2018, 24, 1248–1259. [Google Scholar] [CrossRef]
- Takahashi, S.; Asada, K.; Takasawa, K.; Shimoyama, R.; Sakai, A.; Bolatkan, A.; Shinkai, N.; Kobayashi, K.; Komatsu, M.; Kaneko, S.; et al. Predicting Deep Learning Based Multi-Omics Parallel Integration Survival Subtypes in Lung Cancer Using Reverse Phase Protein Array Data. Biomolecules 2020, 10, 1460. [Google Scholar] [CrossRef]
- Diao, G.; Vidyashankar, A.N. Assessing genome-wide statistical significance for large p small n problems. Genetics 2013, 194, 781–783. [Google Scholar] [CrossRef]
- Romero, A.; Carrier, P.L.; Erraqabi, A.; Sylvain, T.; Auvolat, A.; Dejoie, E.; Legault, M.A.; Dubé, M.P.; Hussin, J.G.; Bengio, Y. Diet Networks: Thin Parameters for Fat Genomics. arXiv 2016, arXiv:1611.09340. [Google Scholar]
- Clayton, E.A.; Pujol, T.A.; McDonald, J.F.; Qiu, P. Leveraging TCGA gene expression data to build predictive models for cancer drug response. BMC Bioinform. 2020, 21, 364. [Google Scholar] [CrossRef]
- Naulaerts, S.; Menden, M.P.; Ballester, P.J. Concise Polygenic Models for Cancer-Specific Identification of Drug-Sensitive Tumors from Their Multi-Omics Profiles. Biomolecules 2020, 10, 963. [Google Scholar] [CrossRef]
- Tolios, A.; De Las Rivas, J.; Hovig, E.; Trouillas, P.; Scorilas, A.; Mohr, T. Computational approaches in cancer multidrug resistance research: Identification of potential biomarkers, drug targets and drug-target interactions. Drug Resist. Updat. 2020, 48, 100662. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Muglia, L.J.; Huang, L.F. Network as a Biomarker: A Novel Network-Based Sparse Bayesian Machine for Pathway-Driven Drug Response Prediction. Genes 2019, 10, 602. [Google Scholar] [CrossRef] [PubMed]
- Song, P.; Cui, X.; Bai, L.; Zhou, X.; Zhu, X.; Zhang, J.; Jin, F.; Zhao, J.; Zhou, C.; Zhou, Y.; et al. Molecular characterization of clinical responses to PD-1/PD-L1 inhibitors in non-small cell lung cancer: Predictive value of multidimensional immunomarker detection for the efficacy of PD-1 inhibitors in Chinese patients. Thorac. Cancer 2019, 10, 1303–1309. [Google Scholar] [CrossRef] [PubMed]
- Ali, M.; Aittokallio, T. Machine learning and feature selection for drug response prediction in precision oncology applications. Biophys. Rev. 2019, 11, 31–39. [Google Scholar] [CrossRef]
- Shukla, A.; Nguyen, T.H.M.; Moka, S.B.; Ellis, J.J.; Grady, J.P.; Oey, H.; Cristino, A.S.; Khanna, K.K.; Kroese, D.P.; Krause, L.; et al. Chromosome arm aneuploidies shape tumour evolution and drug response. Nat. Commun. 2020, 11, 449. [Google Scholar] [CrossRef]
- Rendeiro, A.F.; Krausgruber, T.; Fortelny, N.; Zhao, F.; Penz, T.; Farlik, M.; Schuster, L.C.; Nemc, A.; Tasnady, S.; Reti, M.; et al. Chromatin mapping and single-cell immune profiling define the temporal dynamics of ibrutinib response in CLL. Nat. Commun. 2020, 11, 577. [Google Scholar] [CrossRef]
- Sever, R.; Brugge, J.S. Signal transduction in cancer. Cold Spring Harb. Perspect. Med. 2015, 5, a006098. [Google Scholar] [CrossRef]
- Chiyoda, T.; Hart, P.C.; Eckert, M.A.; McGregor, S.M.; Lastra, R.R.; Hamamoto, R.; Nakamura, Y.; Yamada, S.D.; Olopade, O.I.; Lengyel, E.; et al. Loss of BRCA1 in the Cells of Origin of Ovarian Cancer Induces Glycolysis: A Window of Opportunity for Ovarian Cancer Chemoprevention. Cancer Prev. Res. 2017, 10, 255–266. [Google Scholar] [CrossRef]
- Cho, H.S.; Hayami, S.; Toyokawa, G.; Maejima, K.; Yamane, Y.; Suzuki, T.; Dohmae, N.; Kogure, M.; Kang, D.; Neal, D.E.; et al. RB1 methylation by SMYD2 enhances cell cycle progression through an increase of RB1 phosphorylation. Neoplasia 2012, 14, 476–486. [Google Scholar] [CrossRef]
- Cho, H.S.; Shimazu, T.; Toyokawa, G.; Daigo, Y.; Maehara, Y.; Hayami, S.; Ito, A.; Masuda, K.; Ikawa, N.; Field, H.I.; et al. Enhanced HSP70 lysine methylation promotes proliferation of cancer cells through activation of Aurora kinase B. Nat. Commun. 2012, 3, 1072. [Google Scholar] [CrossRef]
- Cho, H.S.; Suzuki, T.; Dohmae, N.; Hayami, S.; Unoki, M.; Yoshimatsu, M.; Toyokawa, G.; Takawa, M.; Chen, T.; Kurash, J.K.; et al. Demethylation of RB regulator MYPT1 by histone demethylase LSD1 promotes cell cycle progression in cancer cells. Cancer Res. 2011, 71, 655–660. [Google Scholar] [CrossRef] [PubMed]
- Deng, X.; Hamamoto, R.; Vougiouklakis, T.; Wang, R.; Yoshioka, Y.; Suzuki, T.; Dohmae, N.; Matsuo, Y.; Park, J.H.; Nakamura, Y. Critical roles of SMYD2-mediated beta-catenin methylation for nuclear translocation and activation of Wnt signaling. Oncotarget 2017, 8, 55837–55847. [Google Scholar] [CrossRef] [PubMed]
- Deng, X.; Von Keudell, G.; Suzuki, T.; Dohmae, N.; Nakakido, M.; Piao, L.; Yoshioka, Y.; Nakamura, Y.; Hamamoto, R. PRMT1 promotes mitosis of cancer cells through arginine methylation of INCENP. Oncotarget 2015. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Deng, Z.; Matsuda, K.; Tanikawa, C.; Lin, J.; Furukawa, Y.; Hamamoto, R.; Nakamura, Y. Late Cornified Envelope Group I, a novel target of p53, regulates PRMT5 activity. Neoplasia 2014, 16, 656–664. [Google Scholar] [CrossRef]
- Hamamoto, R.; Toyokawa, G.; Nakakido, M.; Ueda, K.; Nakamura, Y. SMYD2-dependent HSP90 methylation promotes cancer cell proliferation by regulating the chaperone complex formation. Cancer Lett. 2014, 351, 126–133. [Google Scholar] [CrossRef]
- Kunizaki, M.; Hamamoto, R.; Silva, F.P.; Yamaguchi, K.; Nagayasu, T.; Shibuya, M.; Nakamura, Y.; Furukawa, Y. The lysine 831 of vascular endothelial growth factor receptor 1 is a novel target of methylation by SMYD3. Cancer Res. 2007, 67, 10759–10765. [Google Scholar] [CrossRef]
- Matsuno, Y.; Atsumi, Y.; Shimizu, A.; Katayama, K.; Fujimori, H.; Hyodo, M.; Minakawa, Y.; Nakatsu, Y.; Kaneko, S.; Hamamoto, R.; et al. Replication stress triggers microsatellite destabilization and hypermutation leading to clonal expansion in vitro. Nat. Commun. 2019, 10, 3925. [Google Scholar] [CrossRef]
- Nakakido, M.; Deng, Z.; Suzuki, T.; Dohmae, N.; Nakamura, Y.; Hamamoto, R. Dysregulation of AKT Pathway by SMYD2-Mediated Lysine Methylation on PTEN. Neoplasia 2015, 17, 367–373. [Google Scholar] [CrossRef]
- Nakakido, M.; Deng, Z.; Suzuki, T.; Dohmae, N.; Nakamura, Y.; Hamamoto, R. PRMT6 increases cytoplasmic localization of p21CDKN1A in cancer cells through arginine methylation and makes more resistant to cytotoxic agents. Oncotarget 2015, 6, 30957–30967. [Google Scholar] [CrossRef]
- Obama, K.; Satoh, S.; Hamamoto, R.; Sakai, Y.; Nakamura, Y.; Furukawa, Y. Enhanced expression of RAD51 associating protein-1 is involved in the growth of intrahepatic cholangiocarcinoma cells. Clin. Cancer Res. 2008, 14, 1333–1339. [Google Scholar] [CrossRef]
- Piao, L.; Fujioka, K.; Nakakido, M.; Hamamoto, R. Regulation of poly(ADP-Ribose) polymerase 1 functions by post-translational modifications. Front. Biosci. 2018, 23, 13–26. [Google Scholar]
- Piao, L.; Kang, D.; Suzuki, T.; Masuda, A.; Dohmae, N.; Nakamura, Y.; Hamamoto, R. The histone methyltransferase SMYD2 methylates PARP1 and promotes poly(ADP-ribosyl)ation activity in cancer cells. Neoplasia 2014, 16, 257–264. [Google Scholar] [CrossRef] [PubMed]
- Piao, L.; Suzuki, T.; Dohmae, N.; Nakamura, Y.; Hamamoto, R. SUV39H2 methylates and stabilizes LSD1 by inhibiting polyubiquitination in human cancer cells. Oncotarget 2015, 6, 16939–16950. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, M.; Fujita, M.; Furukawa, Y.; Hamamoto, R.; Shimokawa, T.; Miwa, N.; Ogawa, M.; Nakamura, Y. Isolation of a novel human gene, APCDD1, as a direct target of the beta-Catenin/T-cell factor 4 complex with probable involvement in colorectal carcinogenesis. Cancer Res. 2002, 62, 5651–5656. [Google Scholar] [PubMed]
- Takawa, M.; Cho, H.S.; Hayami, S.; Toyokawa, G.; Kogure, M.; Yamane, Y.; Iwai, Y.; Maejima, K.; Ueda, K.; Masuda, A.; et al. Histone Lysine Methyltransferase SETD8 Promotes Carcinogenesis by Deregulating PCNA Expression. Cancer Res. 2012, 72, 3217–3227. [Google Scholar] [CrossRef] [PubMed]
- Toyokawa, G.; Masuda, K.; Daigo, Y.; Cho, H.S.; Yoshimatsu, M.; Takawa, M.; Hayami, S.; Maejima, K.; Chino, M.; Field, H.I.; et al. Minichromosome Maintenance Protein 7 is a potential therapeutic target in human cancer and a novel prognostic marker of non-small cell lung cancer. Mol. Cancer 2011, 10, 65. [Google Scholar] [CrossRef] [PubMed]
- Yagyu, R.; Hamamoto, R.; Furukawa, Y.; Okabe, H.; Yamamura, T.; Nakamura, Y.; Osada, H.; Hamamoto, R.; Simizu, S. Isolation and characterization of a novel human gene, VANGL1, as a therapeutic target for hepatocellular carcinoma. Int. J. Oncol. 2002, 20, 1173–1178. [Google Scholar] [CrossRef]
- Yoshioka, Y.; Suzuki, T.; Matsuo, Y.; Tsurita, G.; Watanabe, T.; Dohmae, N.; Nakamura, Y.; Hamamoto, R. Protein lysine methyltransferase SMYD3 is involved in tumorigenesis through regulation of HER2 homodimerization. Cancer Med. 2017, 6, 1665–1672. [Google Scholar] [CrossRef]
- Kim, S.; Bae, W.J.; Ahn, J.M.; Heo, J.H.; Kim, K.M.; Choi, K.W.; Sung, C.O.; Lee, D. MicroRNA signatures associated with lymph node metastasis in intramucosal gastric cancer. Mod. Pathol. 2020. [Google Scholar] [CrossRef]
- Kouznetsova, V.L.; Li, J.; Romm, E.; Tsigelny, I.F. Finding distinctions between oral cancer and periodontitis using saliva metabolites and machine learning. Oral Dis. 2020. [Google Scholar] [CrossRef]
- Eicher, T.; Kinnebrew, G.; Patt, A.; Spencer, K.; Ying, K.; Ma, Q.; Machiraju, R.; Mathe, A.E.A. Metabolomics and Multi-Omics Integration: A Survey of Computational Methods and Resources. Metabolites 2020, 10, 202. [Google Scholar] [CrossRef] [PubMed]
- Milanez-Almeida, P.; Martins, A.J.; Germain, R.N.; Tsang, J.S. Cancer prognosis with shallow tumor RNA sequencing. Nat. Med. 2020, 26, 188–192. [Google Scholar] [CrossRef] [PubMed]
- Sanchez, R.; Mackenzie, S.A. Integrative Network Analysis of Differentially Methylated and Expressed Genes for Biomarker Identification in Leukemia. Sci. Rep. 2020, 10, 2123. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Bismeijer, T.; Zwart, W.; Wessels, L.F.A.; Vis, D.J. Genomic data integration by WON-PARAFAC identifies interpretable factors for predicting drug-sensitivity in vivo. Nat. Commun. 2019, 10, 5034. [Google Scholar] [CrossRef]
- Keshava, N.; Toh, T.S.; Yuan, H.; Yang, B.; Menden, M.P.; Wang, D. Defining subpopulations of differential drug response to reveal novel target populations. NPJ Syst. Biol. Appl. 2019, 5, 36. [Google Scholar] [CrossRef]
- Norman, T.M.; Horlbeck, M.A.; Replogle, J.M.; Ge, A.Y.; Xu, A.; Jost, M.; Gilbert, L.A.; Weissman, J.S. Exploring genetic interaction manifolds constructed from rich single-cell phenotypes. Science 2019, 365, 786–793. [Google Scholar] [CrossRef]
- Nelson, C.A.; Butte, A.J.; Baranzini, S.E. Integrating biomedical research and electronic health records to create knowledge-based biologically meaningful machine-readable embeddings. Nat. Commun. 2019, 10, 3045. [Google Scholar] [CrossRef]
- Wang, Y.; Wang, Z.; Xu, J.; Li, J.; Li, S.; Zhang, M.; Yang, D. Systematic identification of non-coding pharmacogenomic landscape in cancer. Nat. Commun. 2018, 9, 3192. [Google Scholar] [CrossRef]
- Zhang, W.; Chien, J.; Yong, J.; Kuang, R. Network-based machine learning and graph theory algorithms for precision oncology. NPJ Precis. Oncol. 2017, 1, 25. [Google Scholar] [CrossRef]
- Madubata, C.J.; Roshan-Ghias, A.; Chu, T.; Resnick, S.; Zhao, J.; Arnes, L.; Wang, J.; Rabadan, R. Identification of potentially oncogenic alterations from tumor-only samples reveals Fanconi anemia pathway mutations in bladder carcinomas. NPJ Genom. Med. 2017, 2, 29. [Google Scholar] [CrossRef]
- Réda, C.; Kaufmann, E.; Delahaye-Duriez, A. Machine learning applications in drug development. Comput. Struct. Biotechnol. J. 2020, 18, 241–252. [Google Scholar] [CrossRef]
- Ekins, S.; Puhl, A.C.; Zorn, K.M.; Lane, T.R.; Russo, D.P.; Klein, J.J.; Hickey, A.J.; Clark, A.M. Exploiting machine learning for end-to-end drug discovery and development. Nat. Mater. 2019, 18, 435–441. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharjee, A. Application of Bayesian Approach in Cancer Clinical Trial. World J. Oncol. 2014, 5, 109–112. [Google Scholar] [CrossRef] [PubMed]
- Madhukar, N.S.; Khade, P.K.; Huang, L.; Gayvert, K.; Galletti, G.; Stogniew, M.; Allen, J.E.; Giannakakou, P.; Elemento, O. A Bayesian machine learning approach for drug target identification using diverse data types. Nat. Commun. 2019, 10, 5221. [Google Scholar] [CrossRef] [PubMed]
- Lyu, J.; Curran, E.; Ji, Y. Bayesian Adaptive Design for Finding the Maximum Tolerated Sequence of Doses in Multicycle Dose-Finding Clinical Trials. JCO Precis. Oncol. 2018, 2018, 1–19. [Google Scholar] [CrossRef]
- Cook, N.; Basu, B.; Smith, D.M.; Gopinathan, A.; Evans, J.; Steward, W.P.; Palmer, D.; Propper, D.; Venugopal, B.; Hategan, M.; et al. A phase I trial of the gamma-secretase inhibitor MK-0752 in combination with gemcitabine in patients with pancreatic ductal adenocarcinoma. Br. J. Cancer 2018, 118, 793–801. [Google Scholar] [CrossRef]
- Yan, F.; Mandrekar, S.J.; Yuan, Y. Keyboard: A Novel Bayesian Toxicity Probability Interval Design for Phase I Clinical Trials. Clin. Cancer Res. 2017, 23, 3994–4003. [Google Scholar] [CrossRef]
- Jin, J.; Liu, Q.; Zheng, W.; Shun, Z.; Lin, T.T.; Gao, L.; Dong, Y. A Bayesian Method for the Detection of Proof of Concept in Early Phase Oncology Studies with a Basket Design. Stat. Biosci. Vol. 2020, 12, 167–179. [Google Scholar] [CrossRef]
- Tang, R.; Shen, J.; Yuan, Y. ComPAS: A Bayesian drug combination platform trial design with adaptive shrinkage. Stat. Med. 2019, 38, 1120–1134. [Google Scholar] [CrossRef]
- da Silveira Nogueira Lima, J.P.; Georgieva, M.; Haaland, B.; de Lima Lopes, G. A systematic review and network meta-analysis of immunotherapy and targeted therapy for advanced melanoma. Cancer Med. 2017, 6, 1143–1153. [Google Scholar] [CrossRef]
- Gupta, S.K. Use of Bayesian statistics in drug development: Advantages and challenges. Int. J. Appl. Basic Med. Res. 2012, 2, 3–6. [Google Scholar] [CrossRef] [PubMed]
- Rudin, C. Stop explaining black box machine learning models for high stakes decisions and use interpretable models instead. Nat. Mach. Intell. 2019, 1, 206–215. [Google Scholar] [CrossRef]
- Samek, W.; Montavon, G.; Lapuschkin, S.; Anders, C.J.; Müller, K.R. Toward Interpretable Machine Learning: Transparent Deep Neural Networks and Beyond. arXiv 2020, arXiv:2003.07631. [Google Scholar]
- Montavon, G.; Samek, W.; Müller, K.R. Methods for interpreting and understanding deep neural networks. Digit. Signal Process. 2018, 73, 1–15. [Google Scholar] [CrossRef]
- Wang, N.; Chen, M.; Subbalakshmi, K.P. Explainable CNN-attention Networks (C-Attention Network) for Automated Detection of Alzheimer’s Disease. arXiv 2020, arXiv:2006.14135. [Google Scholar]
- Yang, J.H.; Wright, S.N.; Hamblin, M.; McCloskey, D.; Alcantar, M.A.; Schrubbers, L.; Lopatkin, A.J.; Satish, S.; Nili, A.; Palsson, B.O.; et al. A White-Box Machine Learning Approach for Revealing Antibiotic Mechanisms of Action. Cell 2019, 177, 1649–1661.e9. [Google Scholar] [CrossRef]
- Wu, M.; Zhong, X.; Peng, Q.; Xu, M.; Huang, S.; Yuan, J.; Ma, J.; Tan, T. Prediction of molecular subtypes of breast cancer using BI-RADS features based on a “white box” machine learning approach in a multi-modal imaging setting. Eur. J. Radiol. 2019, 114, 175–184. [Google Scholar] [CrossRef]
- Gunning, D. Explainable Artificial Intelligence (xAI); Technical Report; Defense Advanced Research Projects Agency (DARPA): Arlington County, FL, USA, 2017; Available online: http://www.darpa.mil/program/explainable-artificial-intelligence (accessed on 9 September 2017).
- Kuhn, D.R.; Kacker, R.N.; Lei, Y.; Simos, D.E. Combinatorial Methods for Explainable AI. In Proceedings of the 2020 IEEE International Conference on Software Testing, Verification and Validation Workshops (ICSTW), Porto, Portugal, 24–28 October 2020. [Google Scholar]
- Shakerin, F.; Gupta, G. Induction of Non-Monotonic Logic Programs to Explain Boosted Tree Models Using LIME. arXiv 2018, arXiv:1808.00629. [Google Scholar] [CrossRef]
- Stacke, K.; Eilertsen, G.; Unger, J.; Lundstrom, C. Measuring Domain Shift for Deep Learning in Histopathology. IEEE J. Biomed. Health Inform. 2020. [Google Scholar] [CrossRef]
- Pandey, P.; Ap, P.; Kyatham, V.; Mishra, D.; Dastidar, T.R. Target-Independent Domain Adaptation for WBC Classification using Generative Latent Search. IEEE Trans. Med. Imaging 2020. [Google Scholar] [CrossRef]
- Bian, C.; Yuan, C.; Wang, J.; Li, M.; Yang, X.; Yu, S.; Ma, K.; Yuan, J.; Zheng, Y. Uncertainty-aware domain alignment for anatomical structure segmentation. Med. Image Anal. 2020, 64, 101732. [Google Scholar] [CrossRef] [PubMed]
- Gu, Y.; Ge, Z.; Bonnington, C.P.; Zhou, J. Progressive Transfer Learning and Adversarial Domain Adaptation for Cross-Domain Skin Disease Classification. IEEE J. Biomed. Health Inform. 2020, 24, 1379–1393. [Google Scholar] [CrossRef] [PubMed]
- Pooch, E.H.P.; Ballester, P.L.; Barros, R.C. Can we trust deep learning models diagnosis? The impact of domain shift in chest radiograph classification. arXiv 2020, arXiv:1909.01940. [Google Scholar]
- Jiang, J.; Hu, Y.C.; Tyagi, N.; Wang, C.; Lee, N.; Deasy, J.O.; Sean, B.; Veeraraghavan, H. Self-derived organ attention for unpaired CT-MRI deep domain adaptation based MRI segmentation. Phys. Med. Biol. 2020, 65, 205001. [Google Scholar] [CrossRef] [PubMed]
- Choudhary, A.; Tong, L.; Zhu, Y.; Wang, M.D. Advancing Medical Imaging Informatics by Deep Learning-Based Domain Adaptation. Yearb. Med. Inform. 2020, 29, 129–138. [Google Scholar] [CrossRef]
- Li, X.; Gu, Y.; Dvornek, N.; Staib, L.H.; Ventola, P.; Duncan, J.S. Multi-site fMRI analysis using privacy-preserving federated learning and domain adaptation: ABIDE results. Med. Image Anal. 2020, 65, 101765. [Google Scholar] [CrossRef]
- Xia, Y.; Yang, D.; Yu, Z.; Liu, F.; Cai, J.; Yu, L.; Zhu, Z.; Xu, D.; Yuille, A.; Roth, H. Uncertainty-aware multi-view co-training for semi-supervised medical image segmentation and domain adaptation. Med. Image Anal. 2020, 65, 101766. [Google Scholar] [CrossRef]
- Chen, C.; Dou, Q.; Chen, H.; Qin, J.; Heng, P.A. Unsupervised Bidirectional Cross-Modality Adaptation via Deeply Synergistic Image and Feature Alignment for Medical Image Segmentation. IEEE Trans. Med. Imaging 2020, 39, 2494–2505. [Google Scholar] [CrossRef]
- Yan, Z.; Yang, X.; Cheng, K.T. Enabling a Single Deep Learning Model for Accurate Gland Instance Segmentation: A Shape-Aware Adversarial Learning Framework. IEEE Trans. Med. Imaging 2020, 39, 2176–2189. [Google Scholar] [CrossRef]
- Xing, F.; Bennett, T.; Ghosh, D. Adversarial Domain Adaptation and Pseudo-Labeling for Cross-Modality Microscopy Image Quantification. Med. Image Comput. Comput. Assist. Interv. 2019, 11764, 740–749. [Google Scholar]
- Hamed Mozaffari, M.; Lee, W.S. Domain adaptation for ultrasound tongue contour extraction using transfer learning: A deep learning approach. J. Acoust. Soc. Am. 2019, 146, EL431. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Q.; Du, B.; Yan, P. Boundary-Weighted Domain Adaptive Neural Network for Prostate MR Image Segmentation. IEEE Trans. Med. Imaging 2020, 39, 753–763. [Google Scholar] [CrossRef] [PubMed]
- Perone, C.S.; Ballester, P.; Barros, R.C.; Cohen-Adad, J. Unsupervised domain adaptation for medical imaging segmentation with self-ensembling. Neuroimage 2019, 194, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Jiang, J.; Hu, Y.C.; Tyagi, N.; Zhang, P.; Rimner, A.; Mageras, G.S.; Deasy, J.O.; Veeraraghavan, H. Tumor-aware, Adversarial Domain Adaptation from CT to MRI for Lung Cancer Segmentation. Med. Image Comput. Comput. Assist. Interv. 2018, 11071, 777–785. [Google Scholar]
- Mahmood, F.; Chen, R.; Durr, N.J. Unsupervised Reverse Domain Adaptation for Synthetic Medical Images via Adversarial Training. IEEE Trans. Med. Imaging 2018, 37, 2572–2581. [Google Scholar] [CrossRef] [PubMed]
- Qin, R.; Zhang, H.; Jiang, L.; Qiao, K.; Hai, J.; Chen, J.; Xu, J.; Shi, D.; Yan, B. Multicenter Computer-Aided Diagnosis for Lymph Nodes Using Unsupervised Domain-Adaptation Networks Based on Cross-Domain Confounding Representations. Comput. Math Methods Med. 2020, 2020, 3709873. [Google Scholar] [CrossRef]
- Ganin, Y.; Ustinova, E.; Ajakan, H. Domain-adversarial training of neural networks. J. Mach. Learn. Res. 2017, 17, 2096-2030. [Google Scholar]
- Borgwardt, K.M.; Gretton, A.; Rasch, M.J.; Kriegel, H.P.; Scholkopf, B.; Smola, A.J. Integrating structured biological data by Kernel Maximum Mean Discrepancy. Bioinformatics 2006, 22, e49–e57. [Google Scholar] [CrossRef]
- Sankaranarayanan, S.; Balaji, Y.; Castillo, C.D.; Chellappa, R. Generate To Adapt: Aligning Domains using Generative Adversarial Networks. arXiv 2017, arXiv:1704.01705. [Google Scholar]
| No. | FDA Approval Number | Product Name (Company) | Description | Regulation Medical Specialty | Decision Date | Regulatory Class (Submission Type) |
|---|---|---|---|---|---|---|
| 1 | K140933 | AliveCor Heart Monitor (AliveCor) | An ECG recording device using machine learning techniques to detect abnormal heart rhythms. | Cardiovascular | 08/15/2014 | Class II (510(k)) |
| 2 | K143468 | QbCheck (Qbtech) | A non-invasive test using AI for diagnosis and treatment of ADHD in children. | Neurology | 03/22/2016 | Unclassified (510(k)) |
| 3 | K160016 | Steth IO (StratoScientific) | An acoustic device using AI to aid in the identification of abnormal heart and lung sounds. | Cardiovascular | 07/15/2016 | Class II (510(k)) |
| 4 | K163253 | Arterys Cardio DL (Arterys) | A software using deep learning to visualize and quantify cardiovascular MR images. | Radiology | 01/05/2017 | Class II (510(k)) |
| 5 | K161328 | CANTAB Mobile (Cambridge Cognition) | An iPad-based memory-assessment tool for older adults. | Neurology | 01/13/2017 | Class II (510(k)) |
| 6 | K162627 | EnsoSleep (EnsoData) | An AI sleep scoring and analysis solution that automates event detection during sleep. | Neurology | 03/31/2017 | Class II (510(k)) |
| 7 * | K162574 | AmCAD-US (AmCad BioMed Corporation) | A software to visualize and quantify ultrasound image data with backscattered signals. | Radiology | 05/30/2017 | Class II (510(k)) |
| 8 * | DEN170022 | QuantX (Quantitative Insights) | An AI-equipped diagnosis system to aid in accurate diagnosis of breast cancer. | Radiology | 07/19/2017 | Class II (De Novo) |
| 9 | K172311 | BioFlux Device (Biotricity) | A remote patient monitoring platform with AI. | Cardiovascular | 12/15/2017 | Class II (510(k)) |
| 10 | K171056 | WAVE Clinical Platform (Excel Medical Electronics) | A patient surveillance and predictive algorithm platform using AI. | Cardiovascular | 01/04/2018 | Class II (510(k)) |
| 11 * | K173542 | Arterys Oncology DL (Arterys) | An AI-based, cloud-based medical imaging software that automatically measures and tracks lesions and nodules in MRI and CT scans. | Radiology | 01/25/2018 | Class II (510(k)) |
| 12 | DEN170073 | ContaCT (Viz.AI) | An AI algorithm to analyze CT scans and detect signs of stroke. | Radiology | 02/13/2018 | Class II (De Novo) |
| 13 | K170540 | DM-Density (Densitas) | A machine learning application that provides on demand automated breast density assessments at point-of-care. | Radiology | 02/23/2018 | Class II (510(k)) |
| 14 | P160007 | Guardian Connect System (Medtronic MiniMed) | A continuous glucose monitor with AI assistance. | Clinical Chemistry | 03/08/2018 | PMA |
| 15 | DEN180001 | IDx-DR (IDx) | A software program that uses an AI algorithm to analyze retinal images. | Ophthalmic | 04/11/2018 | Class II (De Novo) |
| 16 | K173931 | MindMotion GO (MindMaze) | A gamified neurorehabilitation therapy platform using AI. | Physical Medicine | 05/17/2018 | Class II (510(k)) |
| 17 | K180455 | NeuralBot (Neural Analytics) | A lucid robotic ultrasound system for brain blood flow assessment. | Radiology | 05/22/2018 | Class II (510(k)) |
| 18 | DEN180005 | OsteoDetect (Imagen Technologies) | A computer-aided detection and diagnostic software that uses an AI algorithm to analyze two-dimensional X-ray images for signs of distal radius fracture. | Radiology | 05/24/2018 | Class II (De Novo) |
| 19 | K173821 | LungQ (Thirona Corporation) | A lung quantification software to analyze chest CT scans. | Radiology | 06/05/2018 | Class II (510(k)) |
| 20 | DEN170043 | DreaMed Advisor Pro (DreaMed Diabetes) | An AI-powered technology to seamlessly treat patients remotely with its virtual diabetes management service. | Clinical Chemistry | 06/12/2018 | Class II (De Novo) |
| 21 | K172983 | HealthCCS (Zebra Medical Vision) | An AI-powered software that can be used to evaluate calcified plaques in the coronary arteries. | Radiology | 06/13/2018 | Class II (510(k)) |
| 22 | K173780 | EchoMD Automated Ejection Fraction Software (Bay Labs) | A system that enables fully automated AI echocardiogram analysis. | Radiology | 06/14/2018 | Class II (510(k)) |
| 23 | K180647 | BriefCase (Aidoc Medical) | An AI algorithm to detect and triage abnormal findings in non-enhanced head CT images. | Radiology | 08/01/2018 | Class II (510(k)) |
| 24 | DEN180042 | Irregular Rhythm Notification Feature (Apple) | An application to detect irregular heart rhythms in pulse rate data collected by the Apple Watch photoplethysmograph sensors. | Cardiovascular | 09/11/2018 | Class II (De Novo) |
| 25 | DEN180044 | ECG App (Apple) | Applications to detect atrial fibrillations and sinus rhythms in ECG data from an Apple Watch and display the results on an iPhone. | Cardiovascular | 09/11/2018 | Class II (De Novo) |
| 26 | K173872 | FibriCheck (Qompium) | A smartphone application for the detection of heart rhythm disorders such as atrial fibrillation. | Cardiovascular | 09/28/2018 | Class II (510(k)) |
| 27 | K181771 | RightEye Vision System (RightEye) | A cloud-based system that uses objective eye movement measurements to aid in the evaluation of Parkinson’s disease. | Neurology | 09/28/2018 | Class II (510(k)) |
| 28 * | K182034 | Arterys MICA (Arterys) | An AI-based platform for analyzing medical images such as MRI and CT. | Radiology | 10/17/2018 | Class II (510(k)) |
| 29 | K182177 | Accipio Ix (MaxQ-AI) | An AI-enabled software workflow tool that aids in identifying acute intracranial hemorrhage and prioritizing the treatment of strokes or head trauma. | Radiology | 10/26/2018 | Class II (510(k)) |
| 30 | K181939 | icobrain (icometrix) | A software that extracts clinically meaningful information from brain CT or MRI scans of patients with multiple sclerosis, dementia or brain injury. | Radiology | 11/06/2018 | Class II (510(k)) |
| 31 | K180432 | AI-ECG Platform (Shenzhen Carewell Electronics) | A software package which is a distributed ECG auto analysis system designed to assist in measuring and interpreting 12-lead resting ECG with an AI algorithm. | Cardiovascular | 11/19/2018 | Class II (510(k)) |
| 32 | K182218 | FerriSmart Analysis System (Resonance Health Analysis Service) | An automated system for measuring liver iron concentration. | Radiology | 11/30/2018 | Class II (510(k)) |
| 33 * | K182336 | SubtlePET (Subtle Medical) | An AI-powered technology that enables centers to deliver a faster and safer patient scanning experience, while enhancing exam throughput and provider profitability. | Radiology | 11/30/2018 | Class II (510(k)) |
| 34 | K173681 | reSET-O (Pear Therapeutics) | A Prescription Digital Therapeutic (PDT) platform for the treatment of Opioid Use Disorder. | Neurology | 12/10/2018 | Class II (510(k)) |
| 35 | K181861 | Embrace (Empatica) | An epilepsy smartband that detects patterns in motion and physiological signals that may be associated with generalized tonic-clonic seizures, and immediately alerts caregivers. | Neurology | 12/20/2018 | Class II (510(k)) |
| 36 | K182130 | iSchemaView RAPID (iSchemaView) | An AI-enhanced advanced medical imaging for stroke. | Radiology | 12/27/2018 | Class II (510(k)) |
| 37 | K182564 | Quantib ND (Quantib) | An AI solution that helps radiologists read MRI brain scans. | Radiology | 12/27/2018 | Class II (510(k)) |
| 38 | K182456 | Study Watch (Verily Life Sciences) | A wearable device to record, store, transfer, and display ECG rhythms. | Cardiovascular | 01/17/2019 | Class II (510(k)) |
| 39 | K182344 | RhythmAnalytics (Biofourmis Singapore) | An AI-powered software to detect irregular heart rhythms when ECG data are uploaded. | Cardiovascular | 03/07/2019 | Class II (510(k)) |
| 40 * | K183285 | cmTriage (CureMetrix) | An AI-based triage software for mammography. | Radiology | 03/08/2019 | Class II (510(k)) |
| 41 | K181823 | KardiaAI (AliveCor) | An AI-based software analysis library to assess ambulatory ECG rhythms from adult subjects. | Cardiovascular | 03/11/2019 | Class II (510(k)) |
| 42 | K181352 | Loop System (Spry Health) | A tool to collect and transfer physiological data of patients in the home environment. | Cardiovascular | 03/29/2019 | Class II (510(k)) |
| 43 * | K183202 | Deep Learning Image Reconstruction (GE Medical Systems) | A deep learning-based CT image reconstruction technology. | Radiology | 04/12/2019 | Class II (510(k)) |
| 44 | K181988 | eMurmur ID (CSD Labs) | A software screening device that uses a smartphone, electronic stethoscope and machine learning to automate the detection of heart murmurs. | Cardiovascular | 04/17/2019 | Class II (510(k)) |
| 45 | K190362 | HealthPNX (Zebra Medical Vision) | A radiological computer-assisted triage and notification software system. | Radiology | 05/06/2019 | Class II (510(k)) |
| 46 * | K183046 | Aquilion ONE (TSX-305A/6) V8.9 with AiCE (Canon Medical Systems Corporation) | A device to acquire and display cross-sectional volumes of the whole body, including the head, with the capability of imaging whole organs in a single rotation. | Radiology | 06/12/2019 | Class II (510(k)) |
| 47 * | K191384 | RayCare 2.3 (RaySearch Laboratories) | An oncology information system used to support workflows, scheduling and clinical information management for oncology care and follow-up. | Radiology | 07/08/2019 | Class II (510(k)) |
| 48 | K183322 | physIQ Heart Rhythm and Respiratory Module (physIQ) | A device for the calculation of heart rate and heart rate variability, the detection of atrial fibrillation and the determination of respiration rate using ambulatory ECG and triaxial accelerometer data. | Cardiovascular | 07/10/2019 | Class II (510(k)) |
| 49 | K191272 | Current Wearable Health Monitoring System (Current Health) | A device for reusable bedside, mobile and central multi-parameter, physiologic patient monitoring of adult patients in professional healthcare facilities. | Cardiovascular | 07/12/2019 | Class II (510(k)) |
| 50 | K182384 | ACR | LAB Urine Analysis Test System (Healthy.io) | A device for the semi-quantitative detection of albumin and creatinine in urine, using a smartphone application, a proprietary Color-Board, and ACR Reagent Strips. | Clinical Chemistry | 07/26/2019 | Class II (510(k)) |
| 51 | K183271 | AI-Rad Companion (Pulmonary) (Siemens Medical Solutions USA) | An image processing software that provides a quantitative and qualitative analysis from previously acquired CT DICOM images to support radiologists and physicians in the evaluation and assessment of lung disease. | Radiology | 07/26/2019 | Class II (510(k)) |
| 52 | K183282 | Biovitals Analytics Engine (Biofourmis Singapore) | An AI-based software engine used with continuous biometric data from already cleared sensors measuring heart rate, respiratory rate, and activity in ambulatory patients being monitored in a healthcare facility or at home, during periods of minimal activity. | Cardiovascular | 08/15/2019 | Class II (510(k)) |
| 53 | K183268 | AI-Rad Companion (Cardiovascular) (Siemens Medical Solutions USA) | An image processing software that provides quantitative and qualitative analysis from previously acquired CT DICOM images to support radiologists and physicians in the evaluation and assessment of cardiovascular diseases. | Radiology | 09/10/2019 | Class II (510(k)) |
| 54 | K190815 | BrainScope TBI (BrainScope Company) | A portable, non-invasive, non-radiation emitting, point of care device intended to provide results and measures to support clinical assessments and aid in the diagnosis of concussion/mild traumatic brain injury (mTBI). | Neurology | 09/11/2019 | Class II (510(k)) |
| 55 | K191688 | SubtleMR (Subtle Medical) | An image processing software that can be used for image enhancement in MRI images. | Radiology | 09/16/2019 | Class II (510(k)) |
| 56 * | K191994 | ProFound AI Software V2.1 (iCAD) | A CAD software device intended to be used concurrently by interpreting physicians while reading digital breast tomosynthesis (DBT) exams from compatible DBT systems. | Radiology | 10/04/2019 | Class II (510(k)) |
| 57 | K191713 | CS-series-FP Radiographic/Fluoroscopic Systems with Optional CA-100S/FluoroShield (Omega Medical Imaging) | A modification device to provide an automated region of interest that reduces exposure to the patient and operator. | Radiology | 10/04/2019 | Class II (510(k)) |
| 58 | K191171 | EchoGo Core (Ultromics) | A software for use in quantification and reporting of results of cardiovascular function to support physician diagnosis. | Radiology | 11/13/2019 | Class II (510(k)) |
| 59 * | K192287 | Transpara (ScreenPoint Medical) | A device for use as a concurrent reading aid for physicians interpreting screening mammograms from compatible FFDM systems to identify regions suspicious for breast cancer and assess their likelihood of malignancy. | Radiology | 12/10/2019 | Class II (510(k)) |
| 60 | K192004 | Eko Analysis Software (Eko Devices) | A software to provide support to the physician in the evaluation of patients’ heart sounds and ECG’s. | Cardiovascular | 01/15/2020 | Class II (510(k)) |
| 61 | DEN190040 | Caption Guidance (Caption Health) | A software to assist in the acquisition of cardiac ultrasound images. | Radiology | 02/07/2020 | Class II (De Novo) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hamamoto, R.; Suvarna, K.; Yamada, M.; Kobayashi, K.; Shinkai, N.; Miyake, M.; Takahashi, M.; Jinnai, S.; Shimoyama, R.; Sakai, A.; et al. Application of Artificial Intelligence Technology in Oncology: Towards the Establishment of Precision Medicine. Cancers 2020, 12, 3532. https://doi.org/10.3390/cancers12123532
Hamamoto R, Suvarna K, Yamada M, Kobayashi K, Shinkai N, Miyake M, Takahashi M, Jinnai S, Shimoyama R, Sakai A, et al. Application of Artificial Intelligence Technology in Oncology: Towards the Establishment of Precision Medicine. Cancers. 2020; 12(12):3532. https://doi.org/10.3390/cancers12123532
Chicago/Turabian StyleHamamoto, Ryuji, Kruthi Suvarna, Masayoshi Yamada, Kazuma Kobayashi, Norio Shinkai, Mototaka Miyake, Masamichi Takahashi, Shunichi Jinnai, Ryo Shimoyama, Akira Sakai, and et al. 2020. "Application of Artificial Intelligence Technology in Oncology: Towards the Establishment of Precision Medicine" Cancers 12, no. 12: 3532. https://doi.org/10.3390/cancers12123532
APA StyleHamamoto, R., Suvarna, K., Yamada, M., Kobayashi, K., Shinkai, N., Miyake, M., Takahashi, M., Jinnai, S., Shimoyama, R., Sakai, A., Takasawa, K., Bolatkan, A., Shozu, K., Dozen, A., Machino, H., Takahashi, S., Asada, K., Komatsu, M., Sese, J., & Kaneko, S. (2020). Application of Artificial Intelligence Technology in Oncology: Towards the Establishment of Precision Medicine. Cancers, 12(12), 3532. https://doi.org/10.3390/cancers12123532








