Nano-Therapies for Glioblastoma Treatment
Abstract
1. Introduction
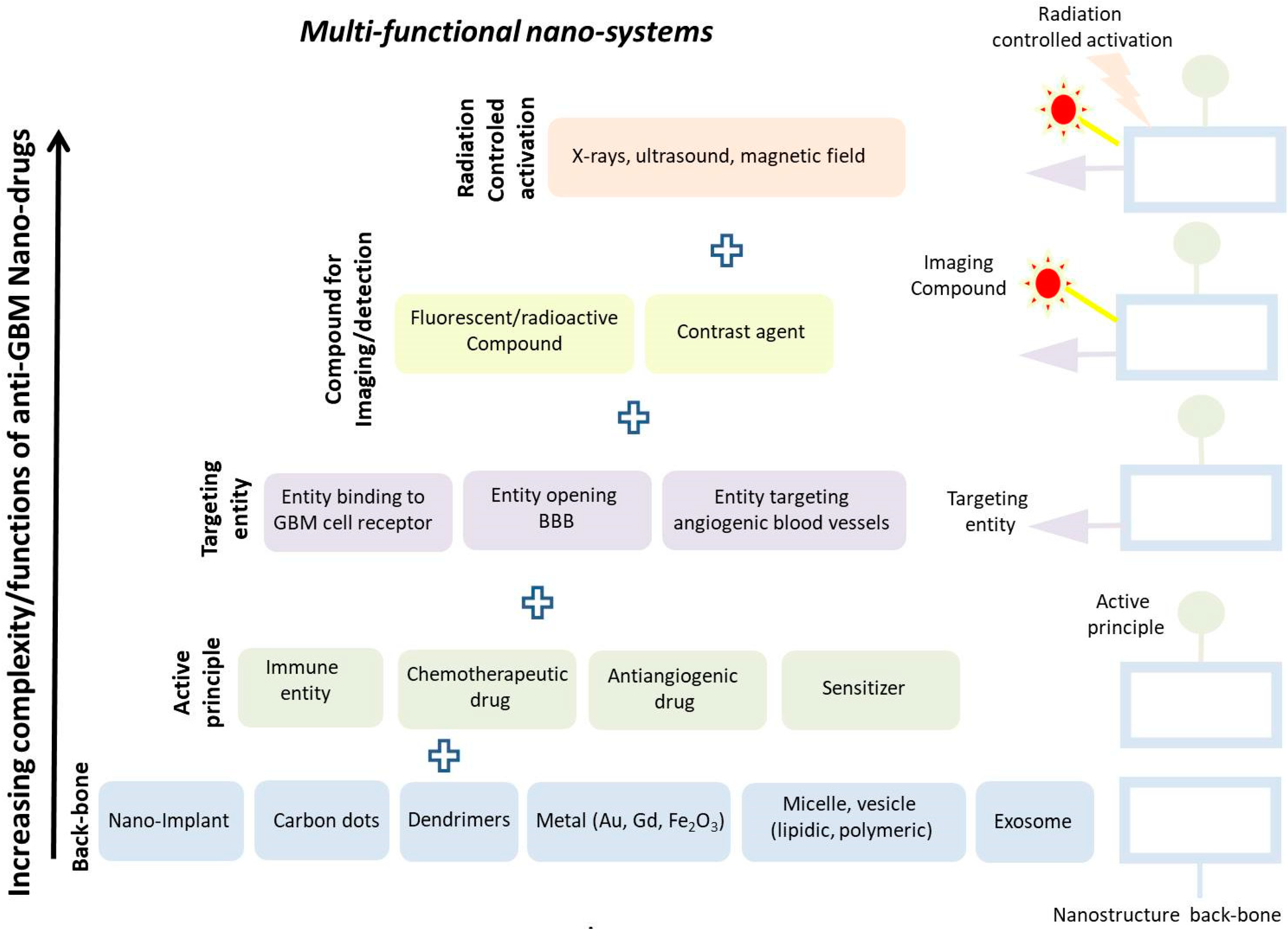
2. Different Types of Nano-Systems for GBM Treatment
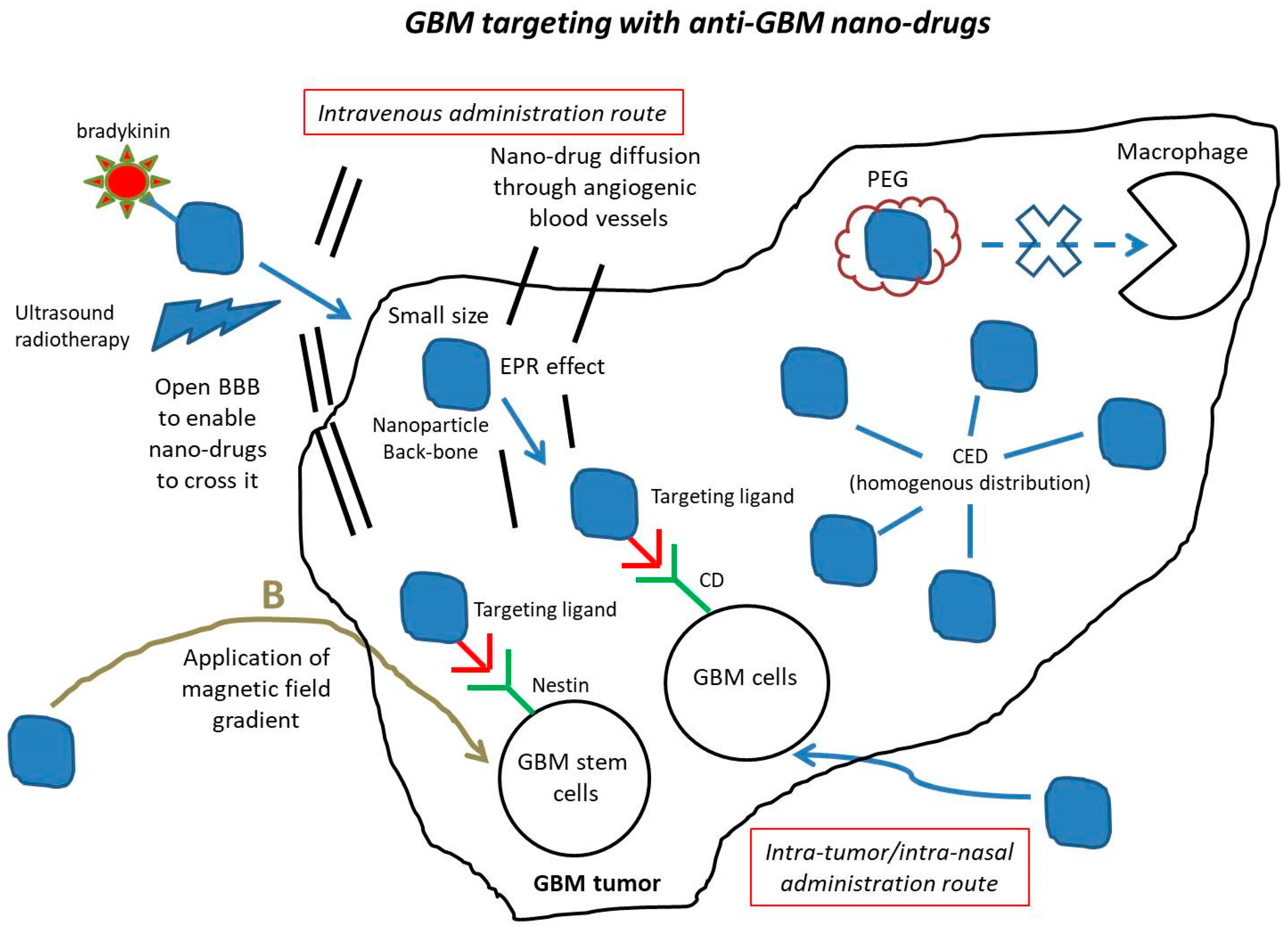
3. Nano-Drugs Improve GBM Drug Delivery
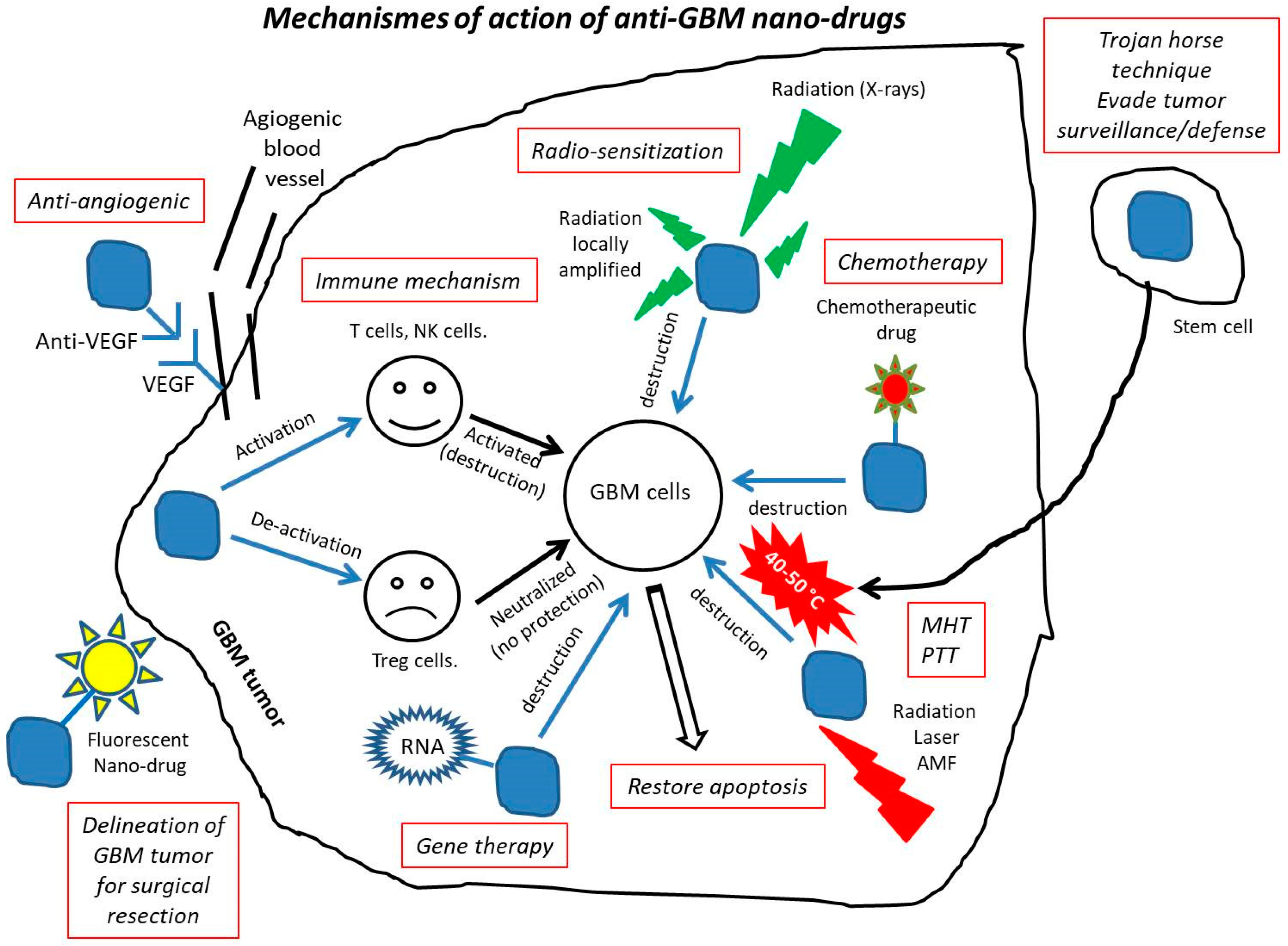
4. Mechanisms of Action of Anti-GBM Nano-Drugs
- Redox variations, which are due to a larger glutathione concentration inside than outside cells, where glutathione is responsible for cleavage of disulfide bonds [95], resulting in selective intracellular release of various chemotherapeutics from nanostructures (e.g., PTX from self-assembled nanoparticles [68] or DOX from polymeric micelles [54]).
- pH, which is usually more acidic inside than outside the tumor, enabling the release of anti-GBM drugs from nanostructures when the linkers between them is acid-sensitive (e.g., DOX could be selectively released in tumors from polymeric micelles using poly(histidine) as linker [96]).
- High intensity focused ultrasound, which can yield a higher accumulation of DOX in tumor tissue than in healthy tissue when applied on a nanostructure consisting of DOX attached to polymer [97].
- Alternating magnetic field, which can trigger TMZ release from a lipid-based magnetic NM, and whose therapeutic activity against U87MG cells is enhanced by mild heating at 43 °C under these conditions of excitation [42].
- Photothermal therapy (PTT), where nanoparticles such as gold or iron oxide are exposed to near infra-red light (e.g., at 808 nm), absorbing this light and transforming it into localized heat through plasmonic effect, leading to the selective photothermal destruction of GBM cells at typical temperatures of 50–60 °C [35,100,101,102,103].
Funding
Conflicts of Interest
Abbreviations
| AMF | Alternating magnetic field |
| ATO | Arsenic trioxide |
| Au | Gold |
| BBB | Blood brain barrier |
| BCNU | Carmustine |
| CED | Convection enhanced delivery |
| CQ | Chloroquine |
| CTX | Chlorotoxin |
| CSC | Cancer stem cells |
| DOX | Doxorubicin |
| EPR | Enhanced permeability and retention effect |
| Gd | Gadolinium |
| GBM | Glioblastoma multiforme |
| GMP | Good manufacturing practice |
| MHT | Magnetic hyperthermia, the application of an alternating magnetic field on magnetic nanoparticles |
| NK | Natural killer |
| PTX | Paclitaxel |
| PAM | Polyacrylamide |
| PAMAM | Poly(amidoamine) |
| PDT | Photodynamic therapy, the application of a laser light on a photosensitizer to produce ROS |
| PLGA | Poly(lactic-co-glycolic acid) |
| PEG | Polyethylene glycol |
| PTT | Photothermal therapy, the application of laser light on nanoparticles, producing heat through plasmonic effects |
| RGD | Arginylglycylaspartic acid peptide |
| RNS | Radical nitrogen species |
| ROS | Radical oxygen species |
| T cells | T lymphocytes |
| TMZ | Temozolomide |
| TME | Tumor microenvironment |
| VEGF | Vascular endothelium growth factor |
References
- Alphandéry, E. Glioblastoma Treatments: An Account of Recent Industrial Developments. Front. Pharmacol. 2018, 9, 879. [Google Scholar] [CrossRef]
- Jahanban-Esfahlan, A.; Seidi, K.; Jaymand, M.; Schmidt, T.L.; Majdi, H.; Javaheri, T.; Jahanban-Esfahlang, M.; Zarei, P. Dynamic DNA nanostructures in biomedicine: Beauty, utility and limits. J. Control. Release 2019, 315, 166–185. [Google Scholar] [CrossRef]
- Patra, J.K.; Das, G.; Fraceto, L.F.; Campos, E.V.R.; del Pilar Rodriguez-Torres, M.; Acosta-Torres, L.S.; Diaz-Torres, L.A.; Grillo, R.; Swamy, M.K.; Sharma, S.; et al. Nano based drug delivery systems: Recent developments and future prospects. J. Nanobiotechnol. 2018, 16, 71. [Google Scholar] [CrossRef]
- Jahanban-Esfahlan, R.; Seidi, K.; Jahanban-Esfahlan, A.; Jaymand, M.; Alizadeh, E.; Majdi, H.; Najjar, R.; Javaheri, T.; Zare, P. Static DNA Nanostructures for Cancer Theranostics: Recent Progress in Design and Applications. Nanotechnol. Sci. Appl. 2019, 12, 25. [Google Scholar] [CrossRef]
- Fakhoury, M. Drug delivery approaches for the treatment of glioblastoma multiforme. Artif. Cells Nanomed. Biotechnol. 2016, 44, 1365–1373. [Google Scholar] [CrossRef]
- Glaser, T.; Han, I.; Wu, L.; Zeng, X. Targeted Nanotechnology in Glioblastoma Multiforme. Front. Pharmacol. 2017, 8, 166. [Google Scholar] [CrossRef]
- Prasad, M.; Lambe, U.P.; Brar, B.; Shah, I.; Manimegalai, J.; Ranjan, K.; Rao, R.; Kumar, S.; Mahant, S.; Khurana, S.K.; et al. Nanotherapeutics: An insight into healthcare and multi-dimensional applications in medical sector of the modern world. Biomed. Pharmacother. 2018, 97, 1521–1537. [Google Scholar] [CrossRef]
- Wadajkar, A.S.; Dancy, J.G.; Hersha, D.S.; Anastasiadis, P.; Tran, N.L.; Woodworth, G.F.; Winkles, J.A.; Kim, A.J. Tumor-targeted Nanotherapeutics: Overcoming Treatment Barriers for Glioblastoma. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnol. 2017, 9, e1439. [Google Scholar] [CrossRef]
- Gonawala1, S.; Ali, M.M. Application of Dendrimer-based Nanoparticles in Glioma Imaging. J. Nanomed Nanotechnol. 2017, 8, 3. [Google Scholar]
- Sneider, A.; VanDyke, D.; Paliwal, S.; Rai, P. Remotely Triggered Nano-Theranostics for Cancer Applications. Nanotheranostics 2017, 1, 1–22. [Google Scholar] [CrossRef]
- Lu, Y.; Han, S.; Zheng, H.; Ma, R.; Ping, Y.; Zou, J.; Tang, H.; Zhang, Y.; Xu, X.; Li, F. A novel RGDyC/PEG co-modified PAMAM dendrimer-loaded arsenic trioxide of glioma targeting delivery system. Int. J. Nanomed. 2018, 13, 5937–5952. [Google Scholar] [CrossRef]
- Yong, S.B.; Chung, J.Y.; Song, Y.; Kim, J.; Ra, S.; Kim, Y.H. Non-viral nano-immunotherapeutics targeting tumor microenvironmental immune cells. Biomaterials 2019, 219, 119401. [Google Scholar] [CrossRef]
- Yang, B.; Chen, Y.; Shi, J. Reactive Oxygen Species (ROS)-Based Nanomedicine. Chem. Rev. 2019, 119, 4881–4985. [Google Scholar] [CrossRef]
- Nel, A.; Ruoslahti, E. New Insights into “Permeability” as in the Enhanced Permeability and Retention Effect of Cancer Nanotherapeutics. ACS Nano 2017, 11, 9567–9569. [Google Scholar] [CrossRef]
- Li, L.; Jiang, W.; Luo, K.; Song, H.; Lan, F.; Wu, Y.; Gu, Z. Superparamagnetic Iron Oxide Nanoparticles as MRI contrast agents for Non-invasive Stem Cell Labeling and Tracking. Theranostics 2013, 3, 595–615. [Google Scholar] [CrossRef]
- Alphandéry, E.; Idbaih, A.; Adam, C.; Delattre, J.-Y.; Schmitt, C.; Guyot, F.; Chebbi, I. Development of non-pyrogenic magnetosome minerals coated with poly-l-lysine leading to full disappearance of intracranial U87-Luc tumors in 100% of treated mice using magnetic hyperthermia. Biomaterials 2019, 141, 210–222. [Google Scholar] [CrossRef]
- Lungarea, S.; Hallam, K.; Badhana, R.K.S. Phytochemical-loaded mesoporous silica nanoparticles for nose-to-brain olfactory drug delivery. Int. J. Pharm. 2016, 513, 280–293. [Google Scholar] [CrossRef]
- Hu, J.; Zhang, X.; Wen, Z.; Tan, Y.; Huang, N.; Cheng, S.; Zheng, H.; Cheng, Y. Asn-Gly-Arg-modified polydopamine-coated nanoparticles for dual-targeting therapy of brain glioma in rats. Oncotarget 2016, 7, 73681–73696. [Google Scholar] [CrossRef]
- Eldridge, B.N.; Bernish, B.W.; Fahrenholtz, C.D.; Singh, R. Photothermal therapy of glioblastoma multiforme using multiwalled carbon nanotubes optimized for diffusion in extracellular space. ACS Biomater. Sci. Eng. 2016, 2, 963–976. [Google Scholar] [CrossRef]
- Qian, M.; Du, Y.; Wang, S.; Li, C.; Jiang, H.; Shi, W.; Chen, J.; Wang, Y.; Wagner, E.; Huang, R. Highly Crystalline Multicolor Carbon Nanodots for Dual-Modal Imaging-Guided Photothermal Therapy of Glioma. ACS Appl. Mater. Interfaces 2018, 10, 4031–4040. [Google Scholar] [CrossRef]
- Hettiarachchi, S.D.; Graham, R.M.; Mintz, K.J.; Zhou, Y.; Vanni, S.; Penga, Z.; Leblanc, R.M. Triple conjugated carbon dots as a nano-drug delivery model for glioblastoma brain tumors. Nanoscale 2019, 11, 6192–6205. [Google Scholar] [CrossRef]
- Sanz, B.; Calatayud, M.P.; Torres, T.E.; Fanarrag, M.L.; Ibarra, M.R.; Goya, G.F. Magnetic hyperthermia enhances cell toxicity with respect to exogenous heating. Biomaterials 2017, 114, 62–70. [Google Scholar] [CrossRef]
- Akiloa, O.D.; Choonara, Y.E.; Strydom, A.M.; du Toita, L.C.; Kumara, P.; Modic, G.; Pillaya, V. An in vitro evaluation of a carmustine-loaded Nano-co-Plex for potential magnetic-targeted intranasal delivery to the brain. Int. J. Pharm. 2016, 500, 196–209. [Google Scholar] [CrossRef]
- Shen, Z.; Liu, T.; Li, Y.; Lau, J.; Yang, Z.; Fan, W.; Zhou, Z.; Shi, C.; Ke, C.; Bregadze, V.E.; et al. Fenton-Reaction-Acceleratable Magnetic Nanoparticles for Ferroptosis Therapy of Orthotopic Brain Tumors. ACS Nano 2018, 12, 11355–11365. [Google Scholar] [CrossRef]
- Shevtsov, M.; Nikolaev, B.; Marchenko, Y.; Yakovleva, L.; Skvortsov, N.; Mazur, A.; Tolstoy, P.; Ryzhov, V.; Multhoff, G. Targeting experimental orthotopic glioblastoma with chitosan-based superparamagnetic iron oxide nanoparticles (CS -DX-SPIONs). Int. J. Nanomed. 2018, 13, 1471–1482. [Google Scholar] [CrossRef]
- Hamdous, Y.; Chebbi, I.; Mandawala, C.; Le Fèvre, R.; Guyot, F.; Seksek, O.; Alphandéry, E. Biocompatible coated magnetosome minerals with various organization and cellular interaction properties induce cytotoxicity towards RG-2 and GL-261 glioma cells in the presence of an alternating magnetic field. J. Nanobiotechnol. 2017, 15, 74. [Google Scholar] [CrossRef]
- Mandawala, C.; Chebbi, I.; Durand-Dubief, M.; Le Fèvre, R.; Hamdous, Y.; Guyot, F.; Alphandéry, E. Biocompatible and stable magnetosome minerals coated with poly-l-lysine, citric acid, oleic acid, and carboxy-methyl-dextran for application in the magnetic hyperthermia treatment of tumors. J. Mater. Chem. B 2017, 5, 7644–7660. [Google Scholar] [CrossRef]
- Hu, Y.; Zhou, Y.; Zhao, N.; Liu, F.; Xu, F.-J. Multifunctional pDNA-Conjugated Polycationic Au Nanorod-Coated Fe 3 O 4 Hierarchical Nanocomposites for Trimodal Imaging and Combined Photothermal/Gene Therapy. Small 2016, 18, 2459–2468. [Google Scholar] [CrossRef]
- Ruan, S.; Hu, C.; Tang, X.; Cun, X.; Xiao, W.; Shi, K.; He, Q.; Gao, H. Increased Gold Nanoparticle Retention in Brain Tumors by in Situ Enzyme-Induced Aggregation. ACS Nano 2016, 10, 10086–10098. [Google Scholar] [CrossRef]
- Lee, C.; Hwang, H.S.; Lee, S.; Kim, B.; Kim, J.O.; Oh, K.T.; Lee, E.S.; Choi, H.-G.; Youn, Y.S. Rabies Virus-Inspired Silica-Coated Gold Nanorods as a Photothermal Therapeutic Platform for Treating Brain Tumors. Adv. Mater. 2017, 29, 1605563. [Google Scholar] [CrossRef]
- Albertini, B.; Mathieu, V.; Iraci, N.; Van Woensel, M.; Schoubben, A.; Donnadio, A.; Greco, S.M.L.; Ricci, M.; Temperini, A.; Blasi, P.; et al. Tumor Targeting by Peptide-Decorated Gold Nanoparticles. Mol. Pharm. 2019, 16, 2430–2444. [Google Scholar] [CrossRef]
- Kunoh, T.; Shimura, T.; Kasai, T.; Matsumoto, S.; Mahmud, H.; Khayrani, A.C.; Seno, M.; Kunoh, H.; Takada, J. Use of DNA-generated gold nanoparticles to radiosensitize and eradicate radioresistant glioma stem cells. Nanotechnology 2019, 30, 055101. [Google Scholar] [CrossRef]
- Lee, C.; Kim, G.R.; Yoon, J.; Kim, S.E.; Yoo, A.S.; Piao, X. In vivo delineation of glioblastoma by targeting tumor-associated macrophages with near-infrared fluorescent silica coated iron oxide nanoparticles in orthotopic xenografts for surgical guidance. Sci. Rep. 2018, 8, 11122. [Google Scholar] [CrossRef]
- Ricciardi, L.; Sancey, L.; Palermo, G.; Termine, R.; De Luca, A.; Szerb, E.I.; Aiello, I. Plasmon-mediated cancer phototherapy: The combined effect of thermal and photodynamic processes. Nanoscale 2017, 9, 19279–19289. [Google Scholar] [CrossRef]
- Seo, B.; Lima, K.; Kim, S.S.; Oh, K.T.; Lee, E.S.; Choi, H.-G.; Shin, B.S.; Youn, Y.S. Small gold nanorods-loaded hybrid albumin nanoparticles with high photothermal efficacy for tumor ablation. Colloids Surf. B Biointerfaces 2019, 179, 340–351. [Google Scholar] [CrossRef]
- Sukumar, U.K.; Bose RJ, C.; Malhotra, M.; Babikir, H.A.; Afjei, R.; Robinson, E.; Zeng, Y.; Chang, E.; Habte, F.; Sinclair, R.; et al. Intranasal delivery of targeted polyfunctional gold–iron oxide nanoparticles loaded with therapeutic microRNAs for combined theranostic multimodality imaging and presensitization of glioblastoma to temozolomide. Biomaterials 2019, 218, 119342. [Google Scholar] [CrossRef]
- Dufort, S.; Appelboom, G.; Verry, C.; Barbier, E.L.; Lux, F.; Bräuer-Krisch, E.; Sancey, L.; Chang, S.D.; Zhang, M.; Roux, S.; et al. Ultrasmall theranostic gadolinium-based nanoparticles improve high-grade rat glioma survival. J. Clin. Neurosci. 2019, 67, 215–219. [Google Scholar] [CrossRef]
- Shaw, T.K.; Dey, D.M.G.; Pal, M.M.; Paul, P.; Chakraborty, S.; Ali, K.A.; Mukherjee, B.; Bandyopadhyay, A.K.; Mandal, M. Successful delivery of docetaxel to rat brain using experimentally developed nanoliposome: A treatment strategy for brain tumor. Drug Deliv. 2017, 24, 346–357. [Google Scholar] [CrossRef]
- Bhunia, S.; Vangala, V.; Bhattacharya, D.; Ravuri, H.G.; Kuncha, M.; Chakravarty, S.; Sistla, R.; Chaudhuri, A. Large Amino Acid Transporter 1 Selective Liposomes of L-DOPA Functionalized Amphiphile for Combating Glioblastoma. Mol. Pharm. 2017, 14, 3834–3847. [Google Scholar] [CrossRef]
- Rehman, M.; Madni, A.; Shi, D.; Ihsan, A.; Tahir, N.; Chang, K.R.; Javed, I.; Webster, T.J. Enhanced blood brain barrier permeability and glioblastoma cell targeting via thermoresponsive lipid nanoparticles. Nanoscale 2017, 9, 15434–15440. [Google Scholar] [CrossRef]
- Erel-Akbaba, G.; Carvalho, L.A.; Tian, T.; Zinter, M.; Akbaba, H.; Obeid, P.J.; Chiocca, E.A.; Weissleder, R.; Kantarci, A.G.; Tannous, B.A. Radiation-Induced Targeted Nanoparticle-Based Gene Delivery for Brain Tumor Therapy. ACS Nano 2019, 13, 4028–4040. [Google Scholar] [CrossRef]
- Tapeinos, C.; Marino, A.; Battaglini, M.; Migliorin, S.; Brescia, R.; Scarpellini, A.; Fernández, C.D.J.; Prato, M.; Dragog, F.; Ciofani, G. Stimuli-responsive lipid-based magnetic nanovectors increase apoptosis in glioblastoma cells through synergic intracellular hyperthermia and chemotherapy. Nanoscale 2019, 11, 1–368. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhai, M.; Chen, Z.; Han, X.; Yu, F.; Li, Z.; Xie, X.; Han, C.; Yu, L.; Yang, Y.; et al. Dual-modified liposome codelivery of doxorubicin and vincristine improve targeting and therapeutic efficacy of glioma. Drug Deliv. 2017, 24, 1045–1055. [Google Scholar] [CrossRef]
- Ying, X.; Wang, Y.; Xu, H.; Li, X.; Yan, H.; Tang, H.; Wen, C.; Li, Y. The construction of the multifunctional targeting ursolic acids liposomes and its apoptosis effects to C6 glioma stem cells. Oncotarget 2017, 8, 64129–64142. [Google Scholar] [CrossRef]
- Nordling-David, M.M.; Yaffe, R.; Guez, D.; Meirow, H.; Last, D.; Grad, A.; Salomon, S.; Sharabi, S.; Levi-Kalisman, Y.; Golomb, G.; et al. Liposomal temozolomide drug delivery using convection enhanced delivery. J. Control. Release 2017, 261, 138–146. [Google Scholar] [CrossRef]
- Bayrac, A.T.; Akca, O.E.; Eyidogan, F.I.; Oktem, H.A. Target-specific delivery of doxorubicin to human glioblastoma cell line via ssDNA aptamer. J. Biosci. 2018, 43, 97–104. [Google Scholar] [CrossRef]
- Gamage, N.H.; Jing, L.; Worsham, M.J.; Ali, M.M. Targeted Theranostic Approach for Glioma Using Dendrimer-Based Curcumin Nanoparticle. J. Nanomed Nanotechnol. 2016, 7, 393. [Google Scholar]
- Agarwal, S.; Muniyandi, P.; Maekawa, T.; Kumar, D.S. Vesicular systems employing natural substances as promising drug candidates for MMP inhibition in glioblastoma: A nanotechnological approach. Int. J. Pharm. 2018, 551, 339–361. [Google Scholar] [CrossRef]
- Kargar, S.; Khoei, S.; Khoee, S.; Shirvalilou, S.; Mahdavi, S.R. Evaluation of the combined effect of NIR laser and ionizing radiation on cellular damages induced by IUdR-loaded PLGA-coated Nano-graphene oxide. Photodiagn. Photodyn. Ther. 2018, 21, 91–97. [Google Scholar] [CrossRef]
- Lin, T.; Zhao, P.; Jiang, Y.; Tang, Y.; Jin, H.; Pan, Z.; He, H.; Yang, V.C.; Huang, Y. Blood−Brain-Barrier-Penetrating Albumin Nanoparticles for Biomimetic Drug Delivery via Albumin-Binding Protein Pathways for Antiglioma Therapy. ACS Nano 2016, 10, 9999–10012. [Google Scholar] [CrossRef]
- Han, L.; Kong, D.K.; Zheng, M.-Q.; Murikinati, S.; Ma, C.; Yuan, P.; Li, L.; Tian, D.; Cai, Q.; Ye, C.; et al. Increased Nanoparticle Delivery to Brain Tumors by Autocatalytic Priming for Improved Treatment and Imaging. ACS Nano 2016, 10, 4209–4218. [Google Scholar] [CrossRef]
- Ramachandran, R.; Junnuthula, V.R.; Gowd, G.S.; Ashokan, A.; Thomas, J.; Peethambaran, R.; Thomas, A.; Unni AK, K.; Panikar, D.; Nair, S.V.; et al. Theranostic 3-Dimensional nano brain-implant for prolonged and localized treatment of recurrent glioma. Sci. Rep. 2017, 7, 43271. [Google Scholar] [CrossRef]
- Castañeda-Gill, J.M.; Ranjan, A.P.; Vishwanatha, J.K. Development and Characterization of Methylene Blue Oleate Salt-Loaded Polymeric Nanoparticles and their Potential Application as a Treatment for Glioblastoma. J. Nanomed Nanotechnol. 2017, 8, 449. [Google Scholar]
- Li, Y.; Baiyang, L.; Leran, B.; Zhen, W.; Yandong, X.; Baixiang, D.; Dandan, Z.; Yufu, Z.; Jun, L.; Rutong, Y.; et al. Reduction-responsive PEtOz-SS-PCL micelle with tailored size to overcome blood–brain barrier and enhance doxorubicin antiglioma effect. Drug Deliv. 2017, 24, 1782–1790. [Google Scholar] [CrossRef]
- Bi, Y.; Liu, L.; Lu, Y.; Sun, T.; Shen, C.; Chen, X.; Chen, Q.; An, S.; He, X.; Ruan, C.; et al. T7 Peptide-Functionalized PEG-PLGA Micelles Loaded with Carmustine for Targeting Therapy of Glioma. ACS Appl. Mater. Interfaces 2016, 8, 27465–27473. [Google Scholar] [CrossRef]
- Ran, D.; Mao, J.; Shen, Q.; Xie, C.; Zhan, C.; Wang, R.; Lu, W. GRP78 enabled micelle-based glioma targeted drug delivery. J. Control. Release 2017, 255, 120–131. [Google Scholar] [CrossRef]
- Singleton, W.G.; Collins, A.M.; Bienemann, A.S.; Killick-Cole, C.L.; Haynes, H.R.; Asby, D.J.; Butts, C.P.; Wyatt, M.J.; Barua, N.U.; Gill, S.S. Convection enhanced delivery of panobinostat (LBH589)-loaded pluronic nano-micelles prolongs survival in the F98 rat glioma model. Int. J. Nanomed. 2017, 12, 1385–1399. [Google Scholar] [CrossRef]
- Wu, C.; Xu, Q.; Chen, X.; Liu, J. Delivery luteolin with folacin-modified nanoparticle for glioma therapy. Int. J. Nanomed. 2019, 14, 7515–7531. [Google Scholar] [CrossRef]
- Zheng, S.; Cheng, Y.; Teng, Y.; Liu, X.; Yu, T.; Wang, Y.; Liu, J.; Hu, Y.; Wu, C.; Wang, X.; et al. Application of luteolin nanomicelles anti-glioma effect with improvement in vitro and in vivo. Oncotarget 2017, 8, 61146–61162. [Google Scholar] [CrossRef]
- Sun, L.; Chen, Y.; Zhou, Y.; Guo, D.; Fan, Y.; Guo, F.; Zheng, Y.; Chen, W. Preparation of 5-fluorouracil-loaded chitosan nanoparticles and study of the sustained release in vitro and in vivo. Asian J. Pharm. Sci. 2017, 12, 418–423. [Google Scholar] [CrossRef]
- Grabowska, M.; Grześkowiak, B.F.; Szutkowski, K.; Wawrzyniak, D.; Głodowicz, P.; Barciszewski, J.; Jurga, S.; Rolle, K.; Mrowczyński, R. Nano-mediated delivery of double-stranded RNA for gene therapy of glioblastoma multiforme. PLoS ONE 2019, 14, e0213852. [Google Scholar] [CrossRef] [PubMed]
- Yu, D.; Khan, O.F.; Suvàc, M.L.; Dong, B.; Panek, W.K.; Xiao, T.; Wu, M.; Han, Y.; Ahmed, A.U.; Balyasnikova, I.V.; et al. Multiplexed RNAi therapy against brain tumorinitiating cells via lipopolymeric nanoparticle infusion delays glioblastoma progression. Proc. Natl. Acad. Sci. USA 2017, 114, E6147–E6156. [Google Scholar] [CrossRef]
- Lopez-Bertoni, H.; Kozielski, K.L.; Rui, Y.; La, R.; Vaughan, H.; Wilson, D.R.; Mihelson, N.; Eberhart, C.G.; Laterra, J.; Green, J.J. Bioreducible Polymeric Nanoparticles Containing Multiplexed Cancer Stem Cell Regulating miRNAs Inhibit Glioblastoma Growth and Prolong Survival. Nano Lett. 2018, 18, 4086–4094. [Google Scholar] [CrossRef]
- Shatsberg, Z.; Zhang, X.; Ofek, P.; Malhotr, S.; Krivitsky, A.; Scomparin, A.; Tiram, G.; Calderón, M.; Haag, R.; Satchi-Fainaro, R. Functionalized nanogels carrying an anticancer microRNA for glioblastoma therapy. J. Control. Release 2016, 239, 159–168. [Google Scholar] [CrossRef]
- Alphandéry, E.; Idbaih, A.; Adam, C.; Delattre, J.-Y.; Schmitt, C.; Guyot, F.; Chebbi, I. Chains of magnetosomes with controlled endotoxin release and partial tumor occupation induce full destruction of intracranial U87-Luc glioma in mice under the application of an alternating magnetic field. J. Control. Release 2017, 262, 259–272. [Google Scholar] [CrossRef]
- Zhang, C.; Nance, E.A.; Mastorakos, P.; Chisholma, P.; Berry, S.; Eberhart, C.; Tyler, B.; Brem, H.; Soo, J.S.; Hanes, J. Convection enhanced delivery of cisplatin-loaded brain penetrating nanoparticles cures malignant glioma in rats. J. Control. Release 2017, 263, 112–119. [Google Scholar] [CrossRef]
- Young, J.S.; Bernal, G.; Polster, S.P.; Nunez, L.; Larsen, G.F.; Mansour, N.; Podell, M.; Yamini, B. Convection Enhanced Delivery of Polymeric Nanoparticles Encapsulating Chemotherapy in Canines with Spontaneous Supratentorial Tumors. World Neurosurg. 2018, 117, e698–e704. [Google Scholar] [CrossRef]
- Arshad, A.; Yang, B.; Bienemann, A.S.; Barua, N.U.; Wyatt, M.J.; Woolley, M.; Johnson, D.E.; Edler, K.J.; Gill, S.S. Convection-Enhanced Delivery of Carboplatin PLGA Nanoparticles for the Treatment of Glioblastoma. PLoS ONE 2015, 10, e0132266. [Google Scholar] [CrossRef]
- Finbloom, J.A.; Aanei, I.L.; Bernard, J.M.; Klass, S.H.; Elledge, S.K.; Han, K.; Ozawa, T.; Nicolaides, T.P.; Berger, M.S.; Francis, M.B. Evaluation of Three Morphologically Distinct Virus-Like Particles as Nanocarriers for Convection-Enhanced Drug Delivery to Glioblastoma. Nanomaterials 2018, 8, 1007. [Google Scholar] [CrossRef]
- Alphandéry, E. Biodistribution and targeting properties of iron oxide nanoparticles for treatments of cancer and iron anemia disease. Nanotoxicology 2019, 13, 573–596. [Google Scholar] [CrossRef]
- Ganipineni, P.L.; Danhier, F.; Préat, V. Drug delivery challenges and future of chemotherapeutic nanomedicine for glioblastoma treatment. J. Control. Release 2018, 281, 42–57. [Google Scholar] [CrossRef] [PubMed]
- Coluccia, D.; Figueiredo, C.A.; Wu, M.Y.; Riemenschneider, A.N.; Diaz Luck, A.; Smith, C.; Das, S.; Ackerley, C.; O’Reilly, M.; Hynynen, K.; et al. Enhancing glioblastoma treatment using cisplatin-gold-nanoparticle conjugates and targeted delivery with magnetic resonance-guided focused ultrasound. Nanomed. Nanotechnol. Biol. Med. 2018, 14, 1137–1148. [Google Scholar] [CrossRef] [PubMed]
- Azad, T.D.; Pan, J.; Connolly, I.D.; Remington, A.; Wilson, C.M.; Grant, G.A. Therapeutic strategies to improve drug delivery across the blood-brain barrier. Neurosurg Focus 2015, 38, E9. [Google Scholar] [CrossRef]
- Parodi, A.; Rudzinska, M.; Deviatkin, A.A.; Soond, S.M.; Baldin, A.V.; Zamyatnin, A.A. Established and Emerging Strategies for Drug Delivery Across the Blood-Brain Barrier in Brain Cancer. Pharmaceutics 2019, 11, 245. [Google Scholar] [CrossRef]
- Yu, S.S.; Lau, C.M.; Thomas, S.N.; Jerome, W.G.; Maron, D.J.; Dickerson, J.H.; Hubbell, J.A.; Giorgio, T.D. Size- and charge-dependent non-specific uptake of PEGylated nanoparticles by macrophages. Int. J. Nanomed. 2012, 7, 799–813. [Google Scholar] [CrossRef]
- Peng, C.; Gao, X.; Xu, J.; Du, B.; Ning, X.; Tang, S.; Bachoo, R.M.; Yu, M.; Ge, W.-P.; Zheng, J. Targeting orthotopic gliomas with renal-clearable luminescent gold nanoparticles. Nano Res. 2017, 10, 1366–1376. [Google Scholar] [CrossRef]
- Jiang, Y.; Wang, X.; Liu, X.; Lv, W.; Zhang, H.; Zhang, M.; Li, X.; Xin, H.; Xu, Q. Enhanced Antiglioma Efficacy of Ultrahigh Loading Capacity Paclitaxel Prodrug Conjugate Self-Assembled Targeted Nanoparticles. ACS Appl. Mater. Interfaces 2017, 9, 211–217. [Google Scholar] [CrossRef]
- Shirvalilou, S.; Khoei, S.; Khoee, S.; Raoufi, N.J.; Karimi, M.R.; Shakeri-Zadeh, A. Development of a magnetic nano-graphene oxide carrier for improved glioma-targeted drug delivery and imaging: In vitro and in vivo evaluations. Chem. Biol. Interact. 2018, 295, 97–108. [Google Scholar] [CrossRef]
- Gonçalves, D.P.N.; Rodriguez, R.D.; Kurth, T.; Bray, L.J.; Binner, M.; Jungnickel, C.; Gür, F.N.; Poser, S.W.; Schmidt, T.L.; Zahn, D.R.T.; et al. Enhanced targeting of invasive glioblastoma cells by peptidefunctionalized gold nanorods in hydrogel-based 3D culture. Acta Biomater. 2017, 58, 12–25. [Google Scholar] [CrossRef]
- Gonçalves, D.P.N.; Park, D.M.; Schmidt, T.L.; Werner, C. Modular peptide-functionalized gold nanorods for effective glioblastoma multicellular tumor spheroid targeting. Biomater. Sci. 2018, 6, 1140–1146. [Google Scholar] [CrossRef]
- Ni, D.; Zhang, J.; Bu, W.; Xing, H.; Han, F.; Xiao, Q.; Yao, Z.; Chen, F.; He, Q.; Liu, J.; et al. Dual-Targeting Upconversion Nanoprobes across the BloodBrain Barrier for Magnetic Resonance/Fluorescence Imaging of Intracranial Glioblastoma. ACS Nano 2014, 8, 1231–1242. [Google Scholar] [CrossRef] [PubMed]
- Patil, R.; Galstyan, A.; Sun, T.; Shatalova, E.S.; Butte, P.; Mamelak, A.N.; Carico, C.; Kittle, D.C.; Grodzinski, Z.B.; Chiechi, A.; et al. Polymalic acid chlorotoxin nanoconjugate for near-infrared fluorescence guided resection of glioblastoma multiforme. Biomaterials 2019, 206, 146–159. [Google Scholar] [CrossRef] [PubMed]
- Karakaş, C.Y.; Şahin, H.T.; İnan, B.; Özçimen, D.; Erginer, Y.Ö. In vitro cytotoxic activity of microalgal extracts loaded nano–micro particles produced via electrospraying and microemulsion methods. Biotechnol. Prog. 2019, 2019, e2876. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Zhang, Z.; Mason, R.P.; Sarkaria, J.N.; Zhao, D. Convertible MRI contrast: Sensing the delivery and release of antiglioma nano-drugs. Sci. Rep. 2015, 5, 09874. [Google Scholar] [CrossRef] [PubMed]
- Mu, Q.; Lin, G.; Patton, V.K.; Wang, K.; Press, O.W.; Zhang, M. Gemcitabine and Chlorotoxin Conjugated Iron Oxide Nanoparticles for Glioblastoma Therapy. J. Mater. Chem. B 2016, 7, 32–36. [Google Scholar] [CrossRef]
- Mirgani, M.T.; Isacchi, B.; Sadeghizadeh, M.; Marra, F.; Bilia, A.R.; Mowla, S.J.; Najafi, F.; Babaei, E. Dendrosomal curcumin nanoformulation downregulates pluripotency genes via miR-145 activation in U87MG glioblastoma cells. Int. J. Nanomed. 2014, 9, 403–417. [Google Scholar]
- Steiniger, S.C.J.; Kreuter, J.; Khalansky, A.S.; Skidan, I.N.; Bobruskin, A.I.; Smirnova, Z.S.; Severin, S.E.; Uhl, R.; Kock, M.; Geiger, K.D.; et al. Chemotherapy of glioblastoma in rats using doxorubicin-loaded nanoparticles. Int. J. Cancer 2004, 109, 759–767. [Google Scholar] [CrossRef]
- Di Mauro, P.P.; Cascante, A.; Vilà, P.B.; Gómez-Vallejo, V.; Llop, J.; Borrós, S. Peptide functionalized and high drug loaded novel nanoparticles as dualtargeting drug delivery system for modulated and controlled release of paclitaxel to brain glioma. Int. J. Pharm. 2018, 553, 169–185. [Google Scholar] [CrossRef]
- Fang, C.; Wang, K.; Stephen, Z.R.; Mu, Q.; Kievit, F.M.; Chiu, D.T.; Press, O.W.; Zhang, M. Temozolomide Nanoparticles for Targeted Glioblastoma Therapy. ACS Appl. Mater. Interfaces 2015, 7, 6674–6682. [Google Scholar] [CrossRef]
- Mi1, Y.; Shao, Z.; Vang, J.; Kaidar-Person, O.; Wang, A.Z. Application of nanotechnology to cancer radiotherapy. Cancer Nano 2016, 7, 11. [Google Scholar]
- Morgenroth1, A.; Vogg AT, J.; Ermert, K.; Zlatopolskiy, B.; Mottaghy, F.M. Hedgehog signaling sensitizes Glioma stem cells to endogenous nano-irradiation. Oncotarget 2014, 5, 5483–5493. [Google Scholar] [CrossRef] [PubMed]
- Chen, N.; Yang, W.; Bao, Y.; Xu, H.; Qin, S.; Tu, Y. BSA capped Au nanoparticle as an efficient sensitizer for glioblastoma tumor radiation therapy. RSC Adv. 2015, 5, 40514–40520. [Google Scholar] [CrossRef]
- Hainfeld, J.F.; Ridwan, S.M.; Stanishevskiy1, Y.; Panchal, R.; Slatkin1, D.N.; Smilowitz, H.M. Iodine nanoparticles enhance radiotherapy of intracerebral human glioma in mice and increase efficacy of chemotherapy. Sci. Rep. 2019, 9, 4505. [Google Scholar] [CrossRef] [PubMed]
- Tamborini, M.; Locatelli, E.; Rasile, M.; Monaco, I.; Rodighiero, S.; Corradini, I.; Franchini, M.C.; Passoni, L.; Matteoli, M. A Combined Approach Employing Chlorotoxin-Nanovectors and Low Dose Radiation To Reach Infiltrating Tumor Niches in Glioblastoma. ACS Nano 2016, 10, 2509–2520. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, C.; Suares, D.; Yergeri, M. Tumor Microenvironment Targeted Nanotherapy. Front. Pharmacol. 2018, 9, 1230. [Google Scholar] [CrossRef] [PubMed]
- Uthaman, S.; Huh, K.M.; Park, I.-K. Tumor microenvironment-responsive nanoparticles for cancer theragnostic applications. Biomater. Res. 2018, 22, 22. [Google Scholar] [CrossRef]
- Yang, F.-Y.; Teng, M.-C.; Lu, M.; Liang, H.-F.; Lee, Y.-R.; Yen, C.-C.; Liang, M.-L.; Wong, T.-T. Treating glioblastoma multiforme with selective high-dose liposomal doxorubicin chemotherapy induced by repeated focused ultrasound. Int. J. Nanomed. 2012, 7, 965–974. [Google Scholar] [CrossRef]
- Chen, L.; Wu, Y.; Wu, H.; Li, J.; Xie, J.; Zang, F.; Maa, M.; Gu, N.; Zhang, Y. Magnetic targeting combined with active targeting of dual-ligand iron oxide nanoprobes to promote the penetration depth in tumors for effective magnetic resonance imaging and hyperthermia. Acta Biomater. 2019, 96, 491–504. [Google Scholar] [CrossRef]
- Gupta, R.; Sharma, D. Biofunctionalization of magnetite nanoparticles with stevioside: Effect on the size and thermal behaviour for use in hyperthermia applications. Int. J. Hyperth. 2019, 36, 302–312. [Google Scholar] [CrossRef]
- Cabada, T.F.; de Pablo, C.S.L.; Serrano, A.M.; del Pozo Guerrero, F.; Olmedo, J.J.S.; Gomez, M.R. Induction of cell death in a glioblastoma line by hyperthermic therapy based on gold nanorods. Int. J. Nanomed. 2012, 7, 1511–1523. [Google Scholar]
- Jang, Y.; Lee, N.; Kim, J.H.; Park, Y.I.; Piao, Y. Shape-Controlled Synthesis of Au Nanostructures Using EDTA Tetrasodium Salt and Their Photothermal Therapy Applications. Nanomaterials 2018, 8, 252. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Zhou, Z.; Zhang, F.; Xu, H.; Chen, W.; Jiang, T. A novel nanocomposite based on fluorescent turn-on gold nanostars for near-infrared photothermal therapy and self-theranostic caspase-3 imaging of glioblastoma tumor cell. Colloids Surf. B Biointerfaces 2018, 170, 303–311. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.-L.; ZhuGe, D.-L.; Chen, P.-P.; Tong, M.-G.; Lin, M.-T.; Jiang, X.; Zheng, Y.-W.; Chen, B.; Li, X.-K.; Zhao, Y.-Z. Silk fibroin nanoparticles dyeing indocyanine green for imaging-guided photo-thermal therapy of glioblastoma. Drug Deliv. 2018, 25, 364–375. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.-H.; Ko, Y.T. Dual-selective photodynamic therapy with a mitochondria-targeted photosensitizer and fiber optic cannula for malignant brain tumors. Biomater. Sci. 2019, 7, 2812–2825. [Google Scholar] [CrossRef]
- Huang, J.-L.; Jiang, G.; Song, Q.-X.; Gu, X.; Hu, M.; Wang, X.-L.; Song, H.-H.; Chen, L.-P.; Lin, Y.-Y.; Jiang, D.; et al. Lipoprotein-biomimetic nanostructure enables efficient targeting delivery of siRNA to Ras-activated glioblastoma cells via macropinocytosis. Nat. Commun. 2017, 8, 15144. [Google Scholar] [CrossRef]
- Liu, N.; Zhang, L.; Wang, Z.; Cheng, Y.; Zhang, P.; Wang, X.; Wen, W.; Yang, H.; Liu, H.; Jin, W.; et al. MicroRNA-101 inhibits proliferation, migration and invasion of human glioblastoma by targeting SOX9. Oncotarget 2017, 8, 19244–19254. [Google Scholar] [CrossRef]
- Galstyan, A.; Markman, J.L.; Shatalova, E.S.; Chiechi1, A.; Korman, A.J.; Patil, R.; Klymyshyn, D.; Tourtellotte, W.G.; Israel1, L.L.; Ljubimov BO, V.A.; et al. Blood–brain barrier permeable nano immunoconjugates induce local immune responses for glioma therapy. Nat. Commun. 2019, 10, 3850. [Google Scholar] [CrossRef]
- Huang, P.; Wang, X.; Liang, X.; Yang, J.; Zhang, C.; Kong, D.; Wang, W. Nano-, micro-, and macroscale drug delivery systems for cancer immunotherapy. Acta Biomater. 2019, 85, 1–26. [Google Scholar] [CrossRef]
- Kadiyala, P.; Li, D.; Nuñez, F.M.; Altshuler, D.; Doherty, R.; Kuai, R.; Yu, M.; Kamran, N.; Edwards, M.; Moon, J.J.; et al. High Density Lipoprotein-Mimicking Nanodiscs for Chemo-Immunotherapy against Glioblastoma Multiforme. ACS Nano 2019, 13, 1365–1384. [Google Scholar] [CrossRef]
- Abdalla AM, E.; Xiao, L.; Ullah, M.W.; Yu, M.; Ouyang, C.; Yang, C. Current Challenges of Cancer Anti-angiogenic Therapy and the Promise of Nanotherapeutics. Theranostics 2018, 8, 533–548. [Google Scholar] [CrossRef]
- Caffo, M.; Cardali, S.M.; Fazzari, E.; Barresi, V.; Caruso, G. Nanoparticles drug-delivery systems and antiangiogenic approaches in the treatment of gliomas. Glioma 2018, 1, 183–188. [Google Scholar] [CrossRef]
- Naletova, I.; Cucci, L.M.; D’Angeli, F.; Anfuso, C.D.; Magrì, A.; La Mendola, D.; Lupo, G.; Satriano, C. A Tunable Nanoplatform of Nanogold Functionalised with Angiogenin Peptides for Anti-Angiogenic Therapy of Brain Tumours. Cancers 2019, 11, 1322. [Google Scholar] [CrossRef] [PubMed]
- Sudha, T.; Bharali, D.J.; Sell, S.; Darwish NH, E.; Davis, P.J.; Mousa, S.A. Nanoparticulate Tetrac Inhibits Growth and Vascularity of Glioblastoma Xenografts. Horm. Canc. 2017, 8, 157–165. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Clavreu, A.; Pourbaghi-Masouleh, M.; Roger, E.; Menei, P. Nanocarriers and nonviral methods for delivering antiangiogenic factors for glioblastoma therapy: The story so far. Int. J. Nanomed. 2019, 14, 2497–2513. [Google Scholar] [CrossRef] [PubMed]
- Wierzbicki, M.; Sawosz, E.; Strojny, B.; Jaworski1, S.; Grodzik, M.; Chwalibog, A. NF-κB-related decrease of glioma angiogenic potential by graphite nanoparticles and graphene oxide nanoplatelets. Sci. Rep. 2018, 8, 14733. [Google Scholar] [CrossRef]
- Miao, L.; Huang, L. Exploring the Tumor Microenvironment with Nanoparticles. Cancer Treat. Res. 2015, 166, 193–226. [Google Scholar]
- Zhu, S.; Gu, Z.; Zhao, Y. Harnessing Tumor Microenvironment for Nanoparticle-Mediated Radiotherapy. Adv. Therap. 2018, 1, 1800050. [Google Scholar] [CrossRef]
- Aldea, M.; Potara, M.; Soritau, O.; Florian, I.S.; Florea, A.; Nagy-Simon, T.; Pileczki, V.; Brie, I.; Maniu, D.; Kacso, G. Chitosan-capped gold nanoparticles impair radioresistant glioblastoma stem-like cells. JBUON 2018, 23, 800–813. [Google Scholar]
- Khan, I.S.; Ehtesham, M. Targeting glioblastoma cancer stem cells: The next great hope? Neurosurg. Focus 2014, 37, E7. [Google Scholar] [CrossRef]
- Lu, L.; Shen, X.; Tao, B.; Lin, C.; Li, K.; Luo, Z.; Cai, K. The nanoparticle-facilitated autophagy inhibition of cancer stem cells for improved chemotherapeutic effects on glioblastomas. J. Mater. Chem. B 2019, 7, 2054–2062. [Google Scholar] [CrossRef]
- Singh, P.K.; Srivastava, A.K.; Dev, A.; Kaunda, B.; Choudhury, S.R.; Karmakar, S. 1, 3β-Glucan anchored, paclitaxel loaded chitosan nanocarrier endows enhanced hemocompatibility with efficient anti-glioblastoma stem cells therapy. Carbohydr. Polym. 2018, 180, 365–375. [Google Scholar] [CrossRef] [PubMed]
- Suryaprakash, S.; Lao, Y.-H.; Cho, H.-Y.; Li, M.; Ji, H.Y.; Shao, D.; Hu, H.; Quek, C.H.; Huang, D.; Mintz, R.L.; et al. Engineered Mesenchymal Stem Cell/Nanomedicine Spheroid as an Active Drug Delivery Platform for Combinational Glioblastoma Therapy. Nano Lett. 2019, 19, 1701–1705. [Google Scholar] [CrossRef] [PubMed]
- Elmore, S. Apoptosis: A Review of Programmed Cell Death. Toxicol. Pathol. 2007, 35, 495–516. [Google Scholar] [CrossRef] [PubMed]
| Nanoparticle Backbone Composition | Size (nm) | Functionalization Coating | Bypass BBB | In Vitro Efficacy | In Vivo Efficacy | Mech. of Action | Admin. | Ref. |
|---|---|---|---|---|---|---|---|---|
| Mesoporous silica | 220 | Curcumin + chrysin | NA | NA | NA | pH dependant release of curcumin/chrysin + cellular internalization | In | [17] |
| Mesoporous Silica | 100–200 | PDA+Asn-Gly-Arg (targ: CD13) | Yes | Cytotoxicity demonstrated on C6 cells | Increased survival in glioma bearing rates treated with NP | Increase accumulation in tumor tissue | Iv | [18] |
| Carbon nanotubes (CNT) | 100–200 | PEG | NA | Demonstrated on several cell lines (U87, U373, D54 NHA) | NA | Heat produced by CNT exposed to lIR aser | It | [19] |
| Carbon dots | 6–8 | NA | NA | Cytotoxicity on U87 cells | Increased survival of mice bearing U87 GBM tumors treated by CD exposed to IR laser | Heat produced by CD exposed to lIR aser | Iv | [20] |
| Carbon dots | 2–4 | transferrin (targeted ligand) + Epirubicin, temozolomide (anti-cancer drugs) | NA | Cytoxicity demonstrated on SJGBM2, CHLA266, CHLA200 and U87 GBM cells | NA | Target specifically GBM cells Enhances the effect of chemotherapy | NA | [21] |
| Iron oxide nanoparticle (IONP) | NA | PEI | NA | More cytotoxicity using MHT than exogenous heating | NA | Heat produced by IONP exposed to AMF | NA | [22] |
| IONP | 30–50 | Polyplex + BCNU | Yes | Cytotoxicity towards GBM cells | NA | Release of BCNU + internalization (intranasal admin) | NA | [23] |
| Fe3O4/Gd2O3 | 7 | Cisplatin + lactoferrin + RGD | Yes | Cytotoxicity towards GBM cells | Increased survival of U87-Luc bearing mice treated with NP | Internalization in cancer cells and release of Fe2+, Fe3+ (Fenton reaction favored by cisplatin) | Iv | [24] |
| IONP | 55 | Chitosan | NA | Cytotoxoicity towards GBM cells (C6 and U87) | NA | Accumulation of NP in tumor following iv adminiistration | Iv | [25] |
| Magnetosome (IONP) | 40 | PEI, chitosan, neridronate | NA | Cytotoxicity demonstrated on GL261 and RG2 cells | NA | Heat produced by magnetosomes exposed to AMF | NA | [26] |
| Magnetosome (IONP) | 40 | Poly-L-lysine, citric acid, oleic acid, CMD | NA | Cytotoxicity demonstrated on GL261 and RG2 cells | NA | Heat produced by magnetosomes exposed to AMF | NA | [27] |
| Nanoparticle backbone composition | Size (nm) | Functionalization Coating | Bypass BBB | In vitro efficacy | In vivo efficacy | Mech. of action | Admin. | Ref. |
| Au NP | 40 | Fe3O4 + DNA | NA | Cytoxicity demonstrated on C6 cells | Decreased tumor growth in mice bearing C6 tumor treated by NP exposed to laser | Heat produced by NP exposed to laser + gene therapy | Iv | [28] |
| Au NP | 20–35 | Ala-Ala-Asn- Cys-Lys or 2-cyano-6-aminobenzothiazole modified AuNPs + DOX | NA | Cytotoxicity on C6 cells | Increased survivavl for mice treated with NP | Nanoparticle aggregation that blocks exocytosis and nanoparticle backflow in blood stream | Iv | [29] |
| Au NP AuNRs@SiO2 | 75 | RVG29; PEG | yes | Cytotoxicity towards N2a cells | Tumor growth delay in mice bearing Na2 tumors | Photothermal therapy (NP mimicking virus) Bypass BBB through interaction between RVG29 and AchR | It | [30] |
| Au | 35 | RGD | NA | NA | Enhanced accumulation in brain due to RGD | NA | Iv | [31] |
| Au | 5 | DNA | NA | Cytotoxicity towards CSC-like U251MG-P1 cells and GBM U251MG cells in the presence of radiation | NA | Radiosensitize GBM stem cells (enhancement of abnormal nuclei) | NA | [32] |
| Au | 37 | Silica coated | yes | In vitro uptake of NP in U87-MG | In vivo delineation of glioblastoma | Endocytosis by tumor associated macrophages. Enables delineation of GBM tumor margin by fluorescence | Iv | [33] |
| Au | 30 | Irridium inserted inside NP | NA | Cytotoxicity towards U87 Luc cells at very low NP concentration (< 0.5 µM) due to combined PTT/PDT | NA | Combination of cell imaging/ PTT/ PDT | NA | [34] |
| Au | 130 | Albumin | NA | NA | Decrease in tumor growth in mice bearing N2a tumor | Combination of: - albumin for biocompatibility - Gold for photothermy (passive targeting) | Iv | [35] |
| Au + IONP | 30 | Chitosan+miRNA + TMZ+PEG-T7 peptide | Yes (in admin) | NA | NP treatment leads to: (i) accumulation of miRNAs in GBM tumor; (ii) increased survival of mice bearing GM tumor | Increased activity of miRNA + TMZ | In | [36] |
| Gd (AGuIX) | 3 | polysiloxane | NA | NA | Improved survivakl of rats bearing 9L GBM treated with AGUIX + RT | Improves delineation of GBM tumor; | iv | [37] |
| Nanoparticle backbone composition | Size (nm) | Functionalization Coating | Bypass BBB | In vitro efficacy | In vivo efficacy | Mech. of action | Admin. | Ref. |
| Liposome (nano) | <50 | Docetaxel | NA | Increased cytotoxicity on C6 glioma cells compared with free drug | NA | Increased DTX accumulation in brain compared with free drug | NA | [38] |
| Liposome (nano) | 100–135 | DOPA + DNA | NA | Cellular uptake in GBM cells via receptor LAT1 | Increaed survival of mice treated with liposomes | Chemotherapy + immunotherapy | Iv | [39] |
| Liposome (thermo-responsive) | < 270 | PCTX | Yes | Cytoxicity towards GBM cells increases between 37 and 39°C | NA | Release of drugs with increasing temperature | NA | [40] |
| Liposome | 50 | cyclic peptide iRGD + siRNA-EGFR + siRNA-PD-L1 | Yes | Cytoxicity towards U87 and GL-261 cells | Increased survival of mice bearing GL-261 glioblastoma tumors. | Increased targeting (radiotherapy + RGD) + chemotherapy + immunotherapy | Iv | [41] |
| Liposome + IONP | 50–100 | Temozolomide | Yes | Cytotoxicity towards U87-Luc cella | NA | Heat under AMF application + drug release | NA | [42] |
| Liposome | 100–150 | RGD + TMZ + Vincristine | NA | Cytotoxicity towards U87 and T98G GBM cells | Tumor growth deay in mice tbearing U87 GBM tumors reated with NP | Specific targerting of GBM cells + drug release | Iv | [43] |
| Liposome | 100–150 | Ursolic acid + EGCG + MAN | Yes | Cytotoxicity towards C6 GBM cells | Inhibition of GBM C6 tumor growth | EGCG induce apoptosis of GBM cells. MAN for targeting. UA, anti-cancer drug. | Iv | [44] |
| Liposome | 121 | TMZ | NA | Cytotoxicity towards CNS-1 GBM cells | Increase survival of GBM bearing rats (lipsomal formulation more efficient than free TMZ) | Increases the anti-tumor efficacy of TMZ | it | [45] |
| Nanoparticle backbone composition | Size (nm) | Functionalization Coating | Bypass BBB | In vitro efficacy | In vivo efficacy | Mech. of action | Admin. | Ref. |
| Aptamer (ssDNA) | NA | DOX | NA | Aptamer causes more inhibition on targeted cells A-172 than non-targeted cells MCF-7. | NA | Selective targeting of GBM cells | NA | [46] |
| Dendrimer (3G3) | NA | Curcumin | NA | NP internalized inside tumor cells selectively within nuclei. | NA | Selective cytotoxicity towards GBM cells | Iv | [47] |
| Dendrimer | NA | Arg-Gly-Asp (RGDyC) + αvβ3 integrin targeting ligand + PEG + ATO | yes | More cytotoxic than free ATO on C6 cell lines | RGDyC-mPEG-PAMAM could enhance the antitumor of ATO to glioma, it provides a desirable strategy for targeted therapy of glioma. | selective release of ATO at acidic pH | Iv | [11] |
| Polymer (PLGA) | NA | Chlorotoxin + Morusin | NA | Cytotoxicity towards GI-1 and U87 cell lines. | NA | Specifically target chloride channels (CIC-3) and matrix metalloproteinase (MMP-2), present in GBM cells/environment. Cytoxicity through ROS production | NA | [48] |
| Polymer (PLGA) | 100 | Nano-graphene + 5-iodo-2-deoxyuridine (IUdR) | NA | NP cause damage towards U87MG cell line in the presence of Xray (6 MV) and NIR laser. | NA | Reduced the plating efficiency of the cells Specific targeting of GBM cells | NA | [49] |
| Polymer (albumin) | 150 | paclitaxel and fenretinide | yes | Cytotoxicity towards U87 cells | Tumor growth delay and increased survival in mice bearing U87 GBM tumors. | Croosing of BBB Release of PTX | Iv | [50] |
| Polymer (poly(amine-co-ester) terpolymer) | NA | BBB modulator Lexiscan, NECA, minoxidil) | yes | NA | Increased survival of mice bearing intracranial GL-261 GBM | Accumulation in brain tumor and trigger gene therapy/chemotherapy | Iv | [51] |
| Polymer (PLGA-PLA-PCL) (nano-implant) | NA | TMZ | NA | NA | Increased survival of rats bearing GBM | Release of TMZ under laser excitation | NA | [52] |
| Polymer (Methylene Blue Oleate Salt-Loaded Polymeric NP) | 170 | Methylene blue | Yes | NPs inhibit U87 and T98G cells | NPs bypass BBB more efficientlt than free drugs. | Drug release in GBM tumor | iv | [53] |
| Nanoparticle composition | Size (nm) | Functionalization Coating | Bypass BBB | In vitro efficacy | In vivo efficacy | Mech. of action | Admin. | Ref. |
| Micelle (PEtOz-SS-PCL) | 100–150 | DOX | yes | Cytotoxicity towards C6 cells | Efficacy shown on orthotopic C6-Luci cells-bearing mice | Overcomes BBB and enhances DOX effect (release of DOX inside cells) | Iv | [54] |
| Micelle | 80 | BCNU + T7 peptide | yes | Cytotoxicity towards U87 GBM cells | Increased survival of mice bearing U87 GBM tumors | Accumulation of NP in tumor Increase in drug efficacy BCNU | Iv | [55] |
| Micelle (polymeric) | 25 | RI-VAP + D-VAP (targeting); paclitaxel (drug) | na | Cytotoxicity towards U87 and HUVEC cells | Delays tumor growth of mice bearing U87 GBM tumors | Targets tumors + release drug | Iv | [56] |
| Micelle | NA | panobinostat | Yes | Cytotoxicity towards F98, MO59K and U87-MG GBM cells | Increased survival of rats bearing GBM tumors | Inhibition of pan-histone deacetylase enhanced by NP | it | [57] |
| Micelle (FA-PEG-PCL) | 20 | luteolin | yes | Enhanced growth inhibition and more apoptosis of GL261 cells with NP | Increases survival of mice bearing GL261 GBM tumor | Increases the effect of luteolin | NA | [58] |
| Micelle (MPEG-PCL) | 50 | luteolin | NA | Luteolin/MPEG-PCL micelles had stronger cytotoxicity and induced a higher percentage of apoptosis in C6 and U87 cells than free luteolin Apotosis induced through mitochondrial pathway | Tumor growth delay in mice bearing C6 GBM tumors. | release of luteolin Luteolin/MPEG-PCL micelles induced more glioma cell apoptosis than free luteolin and inhibited neovascularization in tumor tissues | Iv | [59] |
| Micelle (Au+IONP) | PEG | NA | Increase in cell DNA damage when GBM cells are incubated with NP and irradiated at 4 Gy | Possibility to image tumor border by MRI (T2 contrast) | Radiosensitization: increase in DNA breaks when NP irradiated. | iv | [60] | |
| RNA (+ MNP) | 10 | PEI | NA | No cytotoxicity | NA | Immune response against the tumor | NA | [61] |
| RNA (+ lipoprotein) | 20–40 | none | yes | Cytotoxicity towards C6 cells | Improved survival on mice bearing patient derived GICs glioblastoma | RNA-interfering efficiency, increases glioblastoma cell apoptosis | Iv | [62] |
| miRNAs (+ polymer NP) | 100 | none | NA | Cytotoxicity towards GBM cells | Treated mice bearing GBM have long term survival | Increase the efficacy of radiotherapy | It | [63] |
| miRNA (+ nanogel) | 200 | polyglycerol | NA | Cytotoxicity towards U87-Luc cells | Tumor growth delay observed in mice bearing xenograft U87 GBM tumors. | Gene targeting responsible for tumor cell suppression | It | [64] |
| RNAi (+ liposome) | NA | NA | NA | Reduction of GBM tumor sphere formation by NP | Prolonges survival of mice bearing GBM tumors | Target brain tumor-initiating cells | it | [62] |
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alphandéry, E. Nano-Therapies for Glioblastoma Treatment. Cancers 2020, 12, 242. https://doi.org/10.3390/cancers12010242
Alphandéry E. Nano-Therapies for Glioblastoma Treatment. Cancers. 2020; 12(1):242. https://doi.org/10.3390/cancers12010242
Chicago/Turabian StyleAlphandéry, Edouard. 2020. "Nano-Therapies for Glioblastoma Treatment" Cancers 12, no. 1: 242. https://doi.org/10.3390/cancers12010242
APA StyleAlphandéry, E. (2020). Nano-Therapies for Glioblastoma Treatment. Cancers, 12(1), 242. https://doi.org/10.3390/cancers12010242





