Role of Circulating Tumor Cells (CTC), Androgen Receptor Full Length (AR-FL) and Androgen Receptor Splice Variant 7 (AR-V7) in a Prospective Cohort of Castration-Resistant Metastatic Prostate Cancer Patients
Abstract
:1. Introduction
2. Materials and Methods
2.1. Patient Selection
2.2. CTC Capture and AR-FL/AR-V7 Analysis
2.3. Statistical Analysis
3. Results
3.1. Patients Cohort
3.2. CTC Isolation and AR-FL/AR-V7 Prevalence
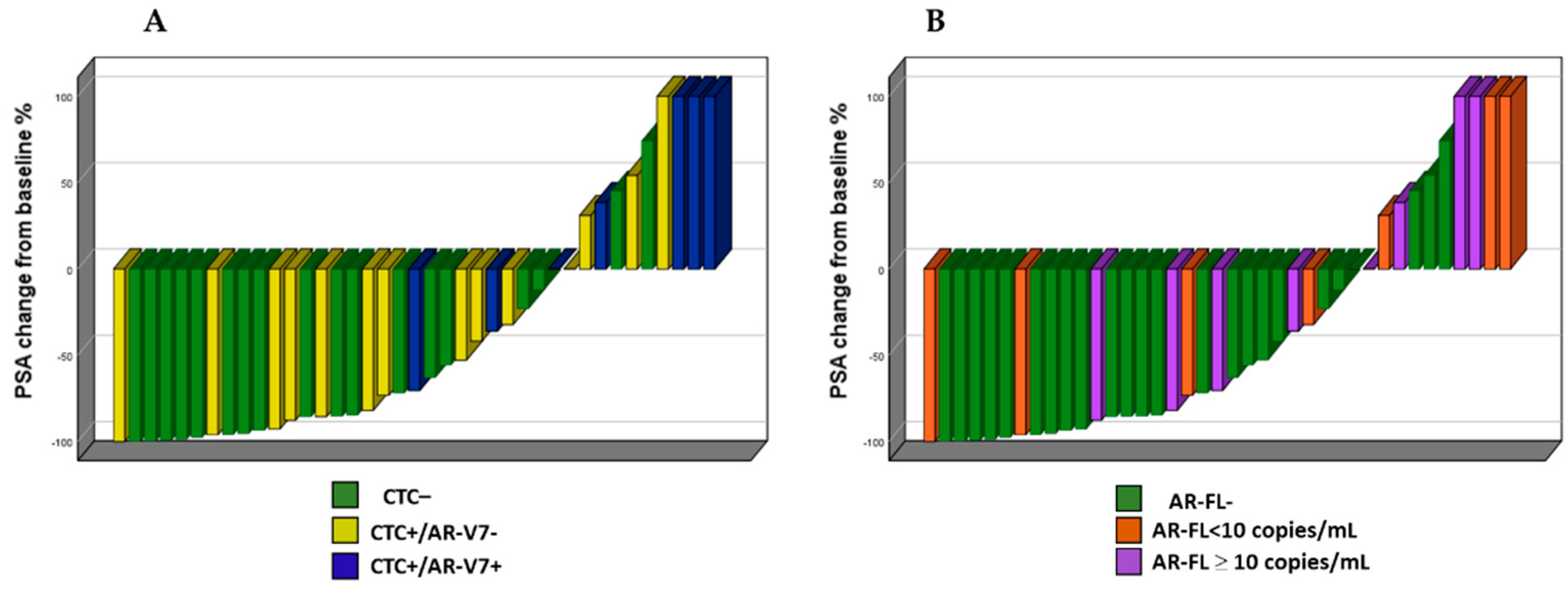
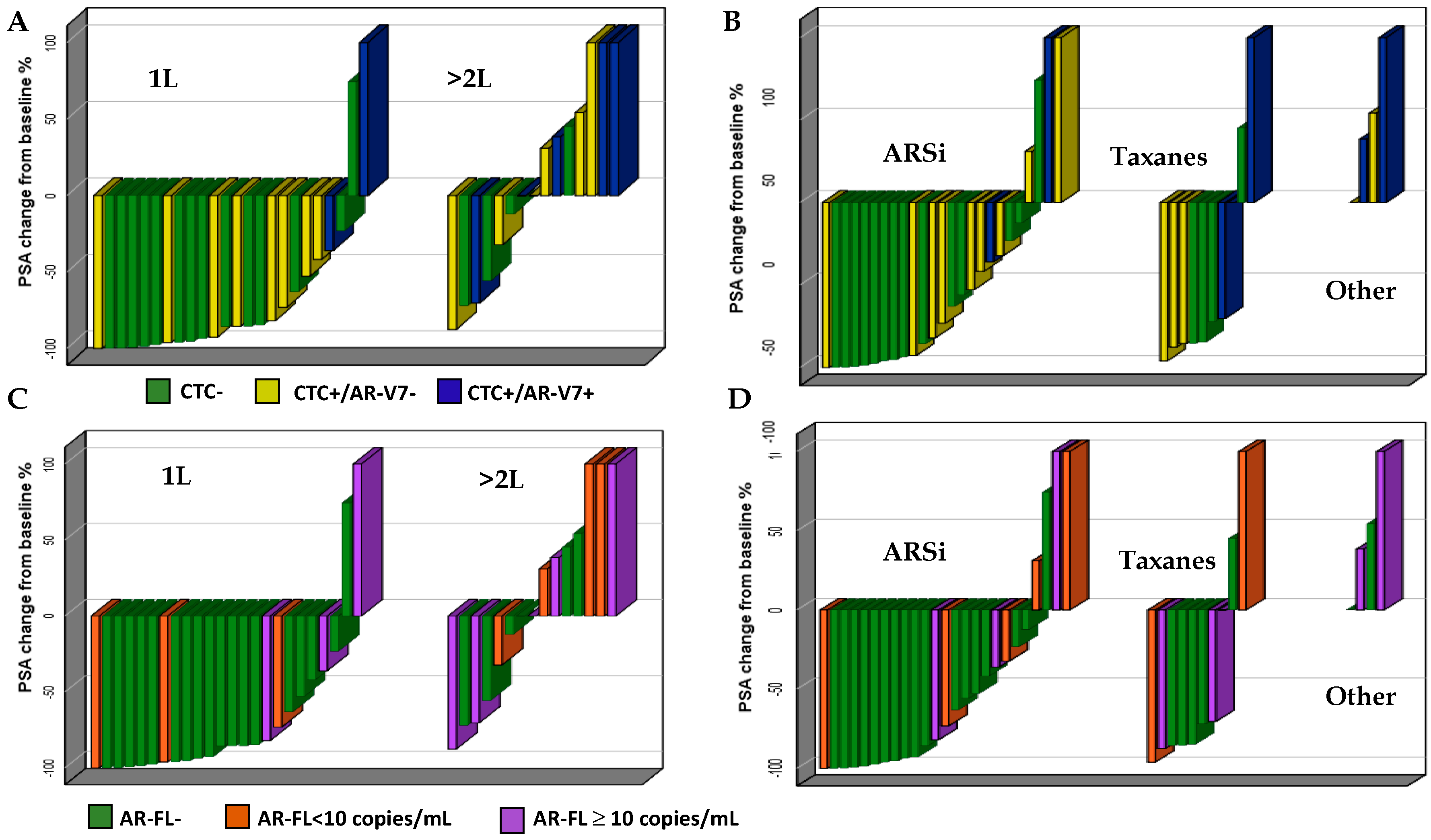
3.3. Association of CTC, AR-FL, and AR-V7 with PSA50 Response
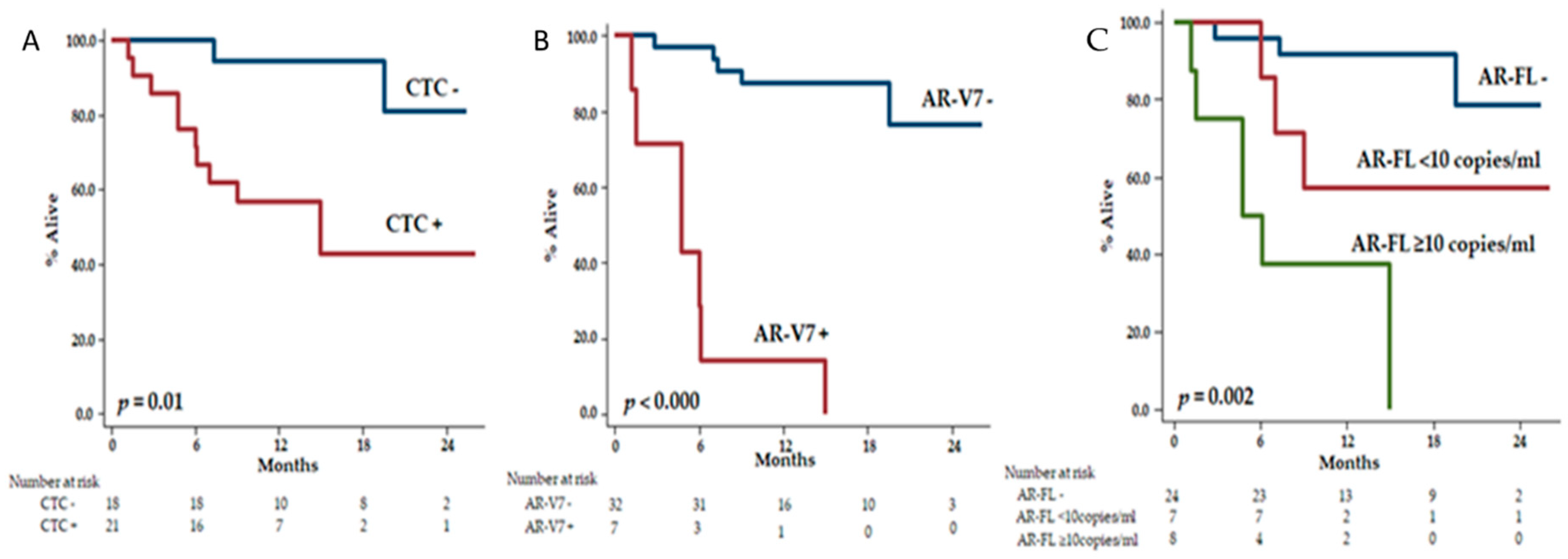
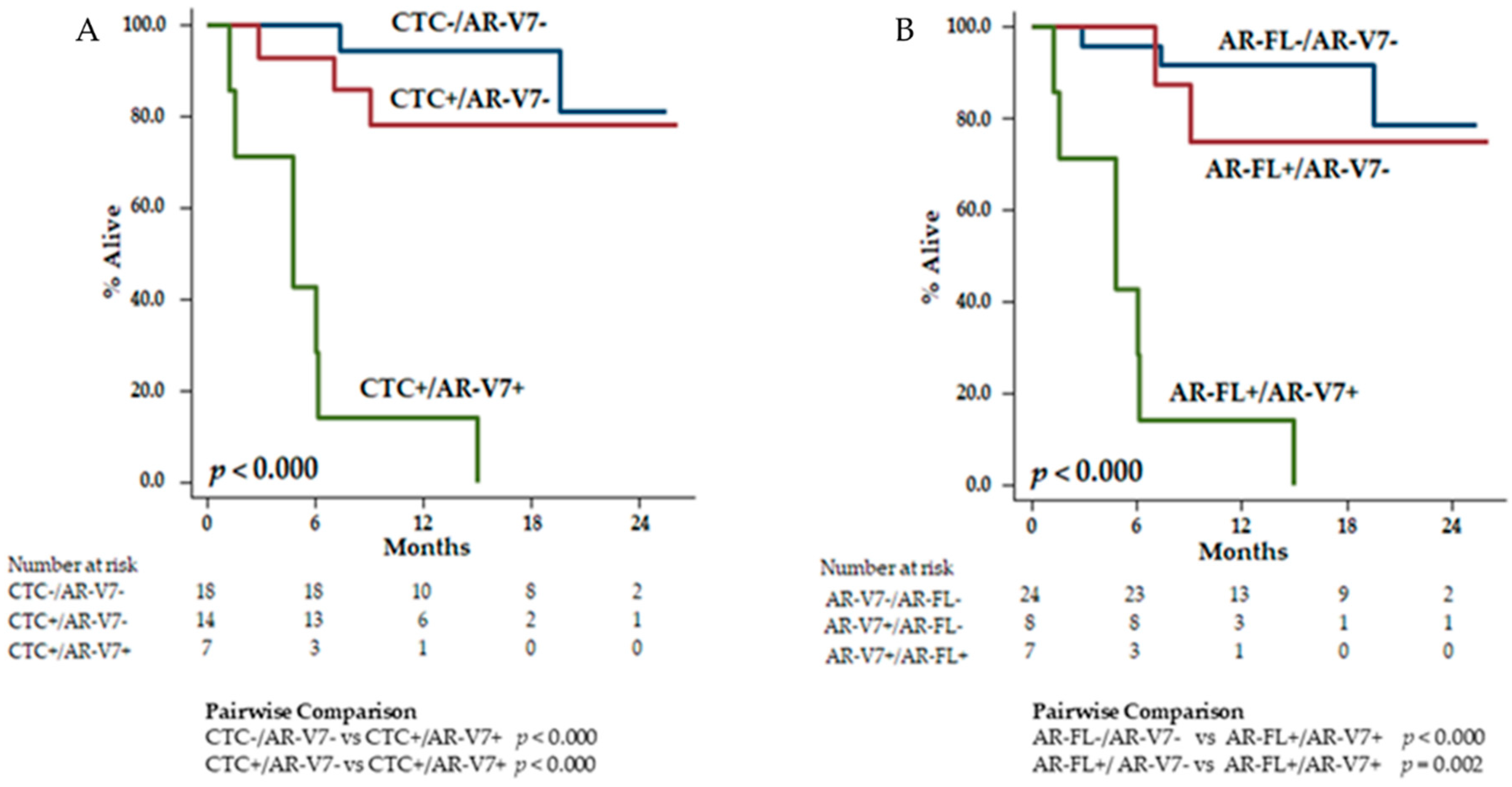
3.4. Association of CTC, AR-FL, and AR-V7 with OS
3.5. Exploratory Prognostic Nomograms for OS
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Sartor, O.; de Bono, J.S. Metastatic Prostate Cancer. N. Engl. J. Med. 2018, 378, 645–657. [Google Scholar] [CrossRef] [PubMed]
- Snow, O.; Lallous, N.; Singh, K.; Lack, N.; Rennie, P.; Cherkasov, A. Androgen receptor plasticity and its implications for prostate cancer therapy. Cancer Treat. Rev. 2019. Articles in Press. [Google Scholar] [CrossRef]
- Antonarakis, E.S.; Lu, C.; Wang, H.; Luber, B.; Nakazawa, M.; Roeser, J.C.; Chen, Y.; Mohammad, T.A.; Chen, Y.; Fedor, H.L.; et al. AR-V7 and resistance to enzalutamide and abiraterone in prostate cancer. N. Engl. J. Med. 2014, 371, 1028–1038. [Google Scholar] [CrossRef] [PubMed]
- Antonarakis, E.S.; Lu, C.; Luber, B.; Wang, H.; Chen, Y.; Nakazawa, M.; Nadal, R.; Paller, C.J.; Denmeade, S.R.; Carducci, M.A.; et al. Androgen Receptor Splice Variant 7 and Efficacy of Taxane Chemotherapy in Patients with Metastatic Castration-Resistant Prostate Cancer. JAMA Oncol. 2015, 1, 582–591. [Google Scholar] [CrossRef] [PubMed]
- Antonarakis, E.S.; Lu, C.; Luber, B.; Wang, H.; Chen, Y.; Zhu, Y.; Silberstein, J.L.; Taylor, M.N.; Maughan, B.L.; Denmeade, S.R.; et al. Clinical Significance of Androgen Receptor Splice Variant-7 mRNA Detection in Circulating Tumor Cells of Men with Metastatic Castration-Resistant Prostate Cancer Treated With First- and Second-Line Abiraterone and Enzalutamide. J. Clin. Oncol. 2017, 35, 2149–2156. [Google Scholar] [CrossRef] [PubMed]
- Scher, H.I.; Lu, D.; Schreiber, N.A.; Louw, J.; Graf, R.P.; Vargas, H.A.; Johnson, A.; Jendrisak, A.; Bambury, R.; Danila, D.; et al. Association of AR-V7 on Circulating Tumor Cells as a Treatment-Specific Biomarker with Outcomes and Survival in Castration-Resistant Prostate Cancer. JAMA Oncol. 2016, 2, 1441–1449. [Google Scholar] [CrossRef] [PubMed]
- Scher, H.I.; Graf, R.P.; Schreiber, N.A.; Jayaram, A.; Winquist, E.; McLaughlin, B.; Lu, D.; Fleisher, M.; Orr, S.; Lowes, L.; et al. Assessment of the Validity of Nuclear-Localized Androgen Receptor Splice Variant 7 in Circulating Tumor Cells as a Predictive Biomarker for Castration-Resistant Prostate Cancer. JAMA Oncol. 2018, 4, 1179–1186. [Google Scholar] [CrossRef]
- Armstrong, A.J.; Halabi, S.; Luo, J.; Nanus, D.M.; Giannakakou, P.; Szmulewitz, R.Z.; Danila, D.C.; Healy, P.; Anand, M.; Rothwell, C.J.; et al. Prospective Multicenter Validation of Androgen Receptor Splice Variant 7 and Hormone Therapy Resistance in High-Risk Castration-Resistant Prostate Cancer: The PROPHECY Study. J. Clin. Oncol. 2019, Jco1801731. [Google Scholar] [CrossRef]
- Qu, F.; Xie, W.; Nakabayashi, M.; Zhang, H.; Jeong, S.H.; Wang, X.; Komura, K.; Sweeney, C.J.; Sartor, O.; Lee, G.M.; et al. Association of AR-V7 and Prostate-Specific Antigen RNA Levels in Blood with Efficacy of Abiraterone Acetate and Enzalutamide Treatment in Men with Prostate Cancer. Clin. Cancer Res. 2017, 23, 726–734. [Google Scholar] [CrossRef]
- Todenhofer, T.; Azad, A.; Stewart, C.; Gao, J.; Eigl, B.J.; Gleave, M.E.; Joshua, A.M.; Black, P.C.; Chi, K.N. AR-V7 Transcripts in Whole Blood RNA of Patients with Metastatic Castration Resistant Prostate Cancer Correlate with Response to Abiraterone Acetate. J. Urol. 2017, 197, 135–142. [Google Scholar] [CrossRef]
- Scher, H.I.; Graf, R.P.; Schreiber, N.A.; McLaughlin, B.; Lu, D.; Louw, J.; Danila, D.C.; Dugan, L.; Johnson, A.; Heller, G.; et al. Nuclear-specific AR-V7 Protein Localization is Necessary to Guide Treatment Selection in Metastatic Castration-resistant Prostate Cancer. Eur. Urol. 2017, 71, 874–882. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.; Sharp, A.; Anderson, C.M.; Silberstein, J.L.; Taylor, M.; Lu, C.; Zhao, P.; De Marzo, A.M.; Antonarakis, E.S.; Wang, M.; et al. Novel Junction-specific and Quantifiable in Situ Detection of AR-V7 and its Clinical Correlates in Metastatic Castration-resistant Prostate Cancer. Eur. Urol. 2018, 73, 727–735. [Google Scholar] [CrossRef] [PubMed]
- Sharp, A.; Welti, J.C.; Lambros, M.B.K.; Dolling, D.; Rodrigues, D.N.; Pope, L.; Aversa, C.; Figueiredo, I.; Fraser, J.; Ahmad, Z.; et al. Clinical Utility of Circulating Tumour Cell Androgen Receptor Splice Variant-7 Status in Metastatic Castration-resistant Prostate Cancer. Eur. Urol. 2019. In Press, Corrected Proof. [Google Scholar] [CrossRef] [PubMed]
- Sharp, A.; Coleman, I.; Yuan, W.; Sprenger, C.; Dolling, D.; Rodrigues, D.N.; Russo, J.W.; Figueiredo, I.; Bertan, C.; Seed, G.; et al. Androgen receptor splice variant-7 expression emerges with castration resistance in prostate cancer. J. Clin. Investig. 2019, 129, 192–208. [Google Scholar] [CrossRef] [PubMed]
- Luo, J.; Attard, G.; Balk, S.P.; Bevan, C.; Burnstein, K.; Cato, L.; Cherkasov, A.; De Bono, J.S.; Dong, Y.; Gao, A.C.; et al. Role of Androgen Receptor Variants in Prostate Cancer: Report from the 2017 Mission Androgen Receptor Variants Meeting. Eur. Urol. 2018, 73, 715–723. [Google Scholar] [CrossRef] [PubMed]
- Salvi, S.; Casadio, V.; Conteduca, V.; Burgio, S.L.; Menna, C.; Bianchi, E.; Rossi, L.; Carretta, E.; Masini, C.; Amadori, D.; et al. Circulating cell-free AR and CYP17A1 copy number variations may associate with outcome of metastatic castration-resistant prostate cancer patients treated with abiraterone. Br. J. Cancer. 2015, 112, 1717–1724. [Google Scholar] [CrossRef] [PubMed]
- Salvi, S.; Casadio, V.; Conteduca, V.; Lolli, C.; Gurioli, G.; Martignano, F.; Schepisi, G.; Testoni, S.; Scarpi, E.; Amadori, D.; et al. Circulating AR copy number and outcome to enzalutamide in docetaxel-treated metastatic castration-resistant prostate cancer. Oncotarget 2016, 7, 37839–37845. [Google Scholar] [CrossRef]
- Conteduca, V.; Wetterskog, D.; Sharabiani, M.T.A.; Grande, E.; Fernandez-Perez, M.P.; Jayaram, A.; Salvi, S.; Castellano, D.; Romanel, A.; Lolli, C.; et al. Androgen receptor gene status in plasma DNA associates with worse outcome on enzalutamide or abiraterone for castration-resistant prostate cancer: A multi-institution correlative biomarker study. Ann. Oncol. 2017, 28, 1508–1516. [Google Scholar] [CrossRef]
- Conteduca, V.; Jayaram, A.; Romero-Laorden, N.; Wetterskog, D.; Salvi, S.; Gurioli, G.; Scarpi, E.; Castro, E.; Marin-Aguilera, M.; Lolli, C.; et al. Plasma Androgen Receptor and Docetaxel for Metastatic Castration-resistant Prostate Cancer. Eur. Urol. 2019, 75, 368–373. [Google Scholar] [CrossRef]
- Silberstein, J.; Luber, B.; Wang, H.; Lu, C.; Chen, Y.; Zhu, Y.; Taylor, M.N.; Carducci, M.A.; Eisenberger, M.A.; Luo, J.; et al. Clinical significance of AR mRNA quantification from circulating tumor cells (CTCs) in men with metastatic castration-resistant prostate cancer (mCRPC) treated with abiraterone (Abi) or enzalutamide (Enza). J. Clin. Oncol. 2017, 35, 132. [Google Scholar] [CrossRef]
- Del Re, M.; Crucitta, S.; Sbrana, A.; Rofi, E.; Paolieri, F.; Gianfilippo, G.; Galli, L.; Falcone, A.; Morganti, R.; Porta, C.; et al. AR-V7 and AR-FL expression is associated with clinical outcome: A translational study in patients with castrate resistant prostate cancer. BJU Int. 2019. [Google Scholar] [CrossRef] [PubMed]
- Tommasi, S.; Pilato, B.; Carella, C.; Lasorella, A.; Danza, K.; Vallini, I.; De Summa, S.; Naglieri, E. Standardization of CTC AR-V7 PCR assay and evaluation of its role in castration resistant prostate cancer progression. Prostate 2019, 79, 54–61. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, E.L.; Meier, P. Nonparametric estimation from incomplete observations. J. Am. Stat. Assoc. 1958, 53, 457–481. [Google Scholar] [CrossRef]
- Harrell, F.E., Jr.; Lee, K.L.; Mark, D.B. Multivariable prognostic models: Issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat. Med 1996, 15, 361–387. [Google Scholar] [CrossRef]
- EAU–ESTRO–ESUR–SIOG Guidelines on Prostate Cancer. Available online: https://uroweb.org/guideline/prostate-cancer (accessed on 3 September 2019).
- Paschalis, A.; Sharp, A.; Welti, J.C.; Neeb, A.; Raj, G.V.; Luo, J.; Plymate, S.R.; de Bono, J.S. Alternative splicing in prostate cancer. Nat. Rev. Clin. Oncol. 2018, 15, 663–675. [Google Scholar] [CrossRef] [PubMed]
| Variable | CTC−/AR-V7− | CTC+/AR-V7− | CTC+/AR-V7+ | All |
|---|---|---|---|---|
| n = 18 | n = 14 | n = 7 | n = 39 | |
| Age | ||||
| Median (range), years | 74 (56–84) | 72 (58–84) | 70 (66–84) | 72 (56–84) |
| PSA | ||||
| Median (range), ng/mL | 11.8 (2.93–516.9) | 63.9 (0.33–564.9) | 514.0 (35.22–4688) | 35.2 (0.33–4688) |
| LDH | ||||
| Median (range), U/L | 216 (138–301) | 234 (152–339) | 452 (121–1616) | 228 (121–1616) |
| Planned treatment line at study entry * | ||||
| 1L | 14 (77.8%) | 8 (57.1%) | 2 (28.6%) | 24 (61.5%) |
| >2L | 4 (22.2%) | 6 (42.9%) | 5 (71.4%) | 15 (38.5%) |
| Treatment at AR-V7 sample Δ | ||||
| ARSi Therapy | 14 (77.8%) | 9 (64.3%) | 2 (28.6%) | 25 (64.1%) |
| Cabazitaxel/Docetaxel | 4 (22.2%) | 3 (21.4%) | 3 (42.8%) | 10 (25.6%) |
| Other | - | 2 (14.3%) | 2 (28.6%) | 4 (10.3%) |
| Bone metastases | ||||
| Absent | 6 (33.3%) | 2 (14.3%) | - | 8 (20.5%) |
| Present | 12 (66.7%) | 12 (85.7%) | 7 (100.0%) | 31 (79.5%) |
| Visceral metastases | ||||
| Absent | 16 (88.9%) | 10 (71.4%) | 6 (85.7%) | 32 (82.1%) |
| Present | 2 (11.1%) | 4 (28.6%) | 1 (14.3%) | 7 (17.9%) |
| Number of metastatic sites | ||||
| =1 site | 12 (66.7%) | 7 (50.0%) | 2 (28.6%) | 21 (53.8%) |
| >1 sites | 6 (33.3%) | 7 (50.0%) | 5 (71.4%) | 18 (46.2%) |
| Variable | 1° Model | 2° Model | 3° Model | 4° Model | ||||
|---|---|---|---|---|---|---|---|---|
| HR (95% CI) | p≤ | HR (95% CI) | p≤ | HR (95% CI) | p≤ | HR (95% CI) | p≤ | |
| PSA (ng/mL) | ||||||||
| <35 ng/mL | 1 | 1 | 1 | 1 | ||||
| ≥35 ng/mL | 6.63 (0.52–84.11) | 0.1 | 7.31 (0.54–98.24) | 0.1 | 6.47 (0.49–85.59) | 0.1 | 5.47 (0.38–78.17) | 0.2 |
| Treatment line * | ||||||||
| 1L | 1 | 1 | 1 | 1 | ||||
| >2L | 2.54 (0.53–12.08) | 0.2 | 4.03 (0.95–17.14) | 0.06 | 3.17 (0.70–14.35) | 0.1 | 2.21 (0.44–11.19) | 0.3 |
| Metastatic sites | ||||||||
| =1 site | 1 | 1 | 1 | 1 | ||||
| >1 sites | 1.56 (0.36–6.93) | 0.5 | 1.66 (0.38–7.21) | 0.5 | 1.93 (0.45–8.33) | 0.4 | 2.15 (0.39–12.20) | 0.4 |
| AR-V7 | ||||||||
| Negative | 1 | 1 | ||||||
| Positive | 6.09 (1.53–24.31) | 0.01 | − | − | − | − | 8.96 (0.94–85.38) | 0.057 |
| CTC | ||||||||
| Negative | 1 | 1 | ||||||
| Positive | − | − | 2.85 (0.42–19.18) | 0.3 | − | − | 1.08 (0.07–16.94) | 0.9 |
| AR-FL | ||||||||
| Negative | 1 | 0.2 | 1 | 0.6 | ||||
| <10 copies/mL | − | − | − | − | 2.80 (0.48–16.36) | 0.2 | 1.91 (0.15–23.76) | 0.6 |
| ≥10 copies/mL | 4.16 (0.83–20.89) | 0.08 | 0.73 (0.04–14.33) | 0.8 | ||||
| C-Index | 0.92 (0.86–0.98) | 0.86 (0.77–0.94) | 0.87 (0.78–0.95) | 0.91 (0.85–0.98) | ||||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cattrini, C.; Rubagotti, A.; Zinoli, L.; Cerbone, L.; Zanardi, E.; Capaia, M.; Barboro, P.; Boccardo, F. Role of Circulating Tumor Cells (CTC), Androgen Receptor Full Length (AR-FL) and Androgen Receptor Splice Variant 7 (AR-V7) in a Prospective Cohort of Castration-Resistant Metastatic Prostate Cancer Patients. Cancers 2019, 11, 1365. https://doi.org/10.3390/cancers11091365
Cattrini C, Rubagotti A, Zinoli L, Cerbone L, Zanardi E, Capaia M, Barboro P, Boccardo F. Role of Circulating Tumor Cells (CTC), Androgen Receptor Full Length (AR-FL) and Androgen Receptor Splice Variant 7 (AR-V7) in a Prospective Cohort of Castration-Resistant Metastatic Prostate Cancer Patients. Cancers. 2019; 11(9):1365. https://doi.org/10.3390/cancers11091365
Chicago/Turabian StyleCattrini, Carlo, Alessandra Rubagotti, Linda Zinoli, Luigi Cerbone, Elisa Zanardi, Matteo Capaia, Paola Barboro, and Francesco Boccardo. 2019. "Role of Circulating Tumor Cells (CTC), Androgen Receptor Full Length (AR-FL) and Androgen Receptor Splice Variant 7 (AR-V7) in a Prospective Cohort of Castration-Resistant Metastatic Prostate Cancer Patients" Cancers 11, no. 9: 1365. https://doi.org/10.3390/cancers11091365
APA StyleCattrini, C., Rubagotti, A., Zinoli, L., Cerbone, L., Zanardi, E., Capaia, M., Barboro, P., & Boccardo, F. (2019). Role of Circulating Tumor Cells (CTC), Androgen Receptor Full Length (AR-FL) and Androgen Receptor Splice Variant 7 (AR-V7) in a Prospective Cohort of Castration-Resistant Metastatic Prostate Cancer Patients. Cancers, 11(9), 1365. https://doi.org/10.3390/cancers11091365







