Influence of Vitamin D in Advanced Non-Small Cell Lung Cancer Patients Treated with Nivolumab
Abstract
:1. Introduction
2. Results
2.1. Patient Characteristics
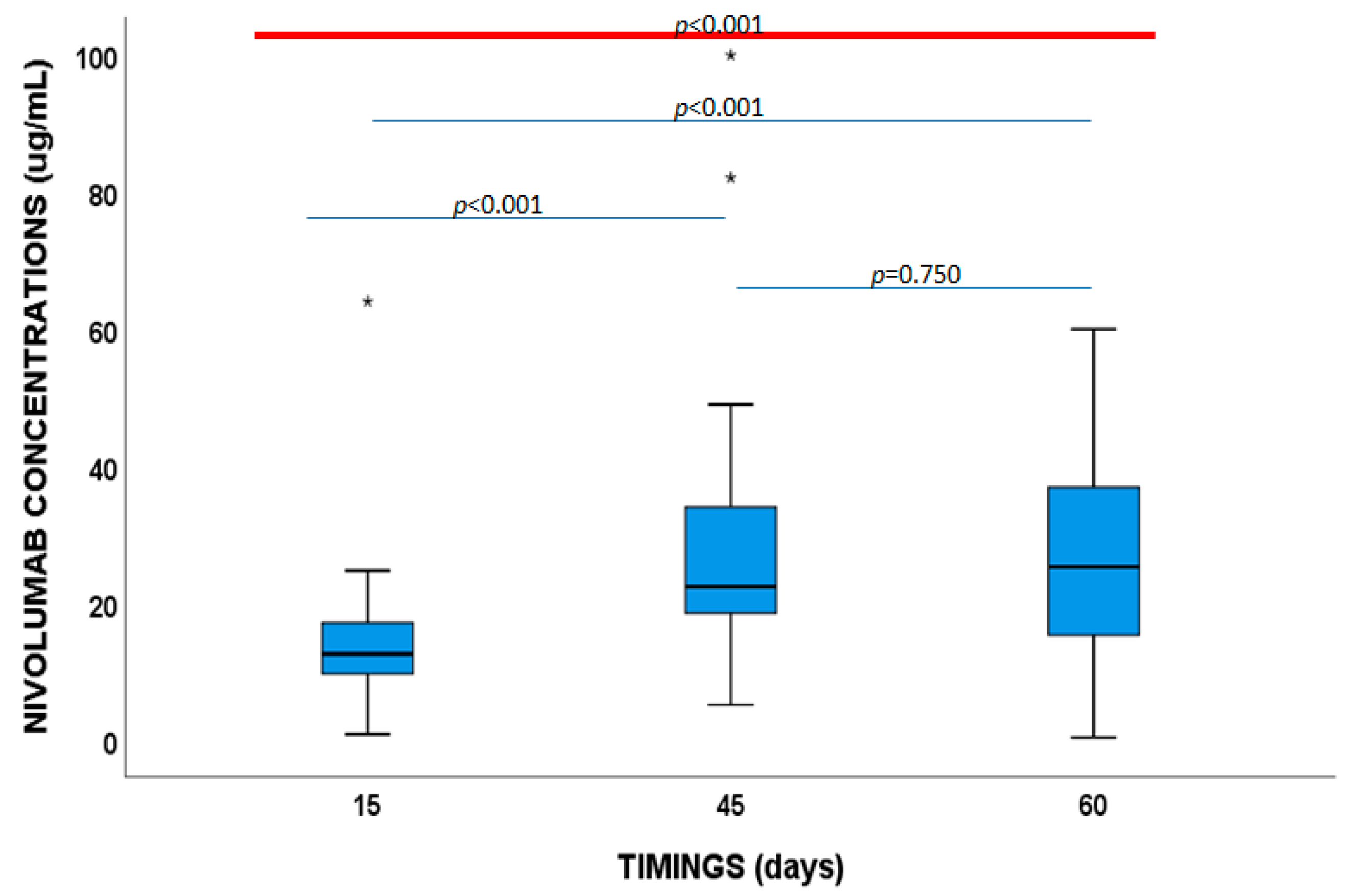
2.2. Nivolumab and Vitamin D Concentrations
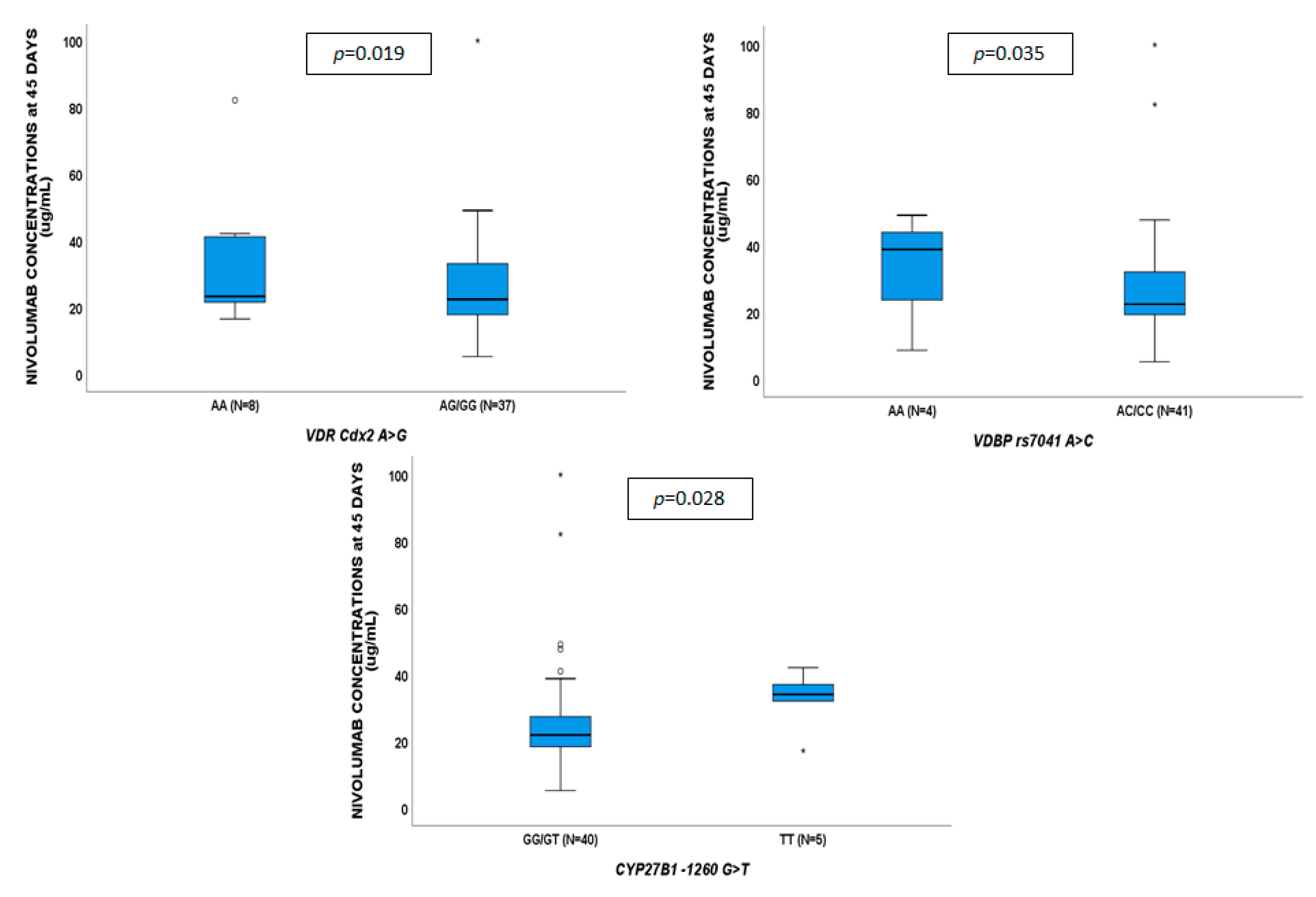
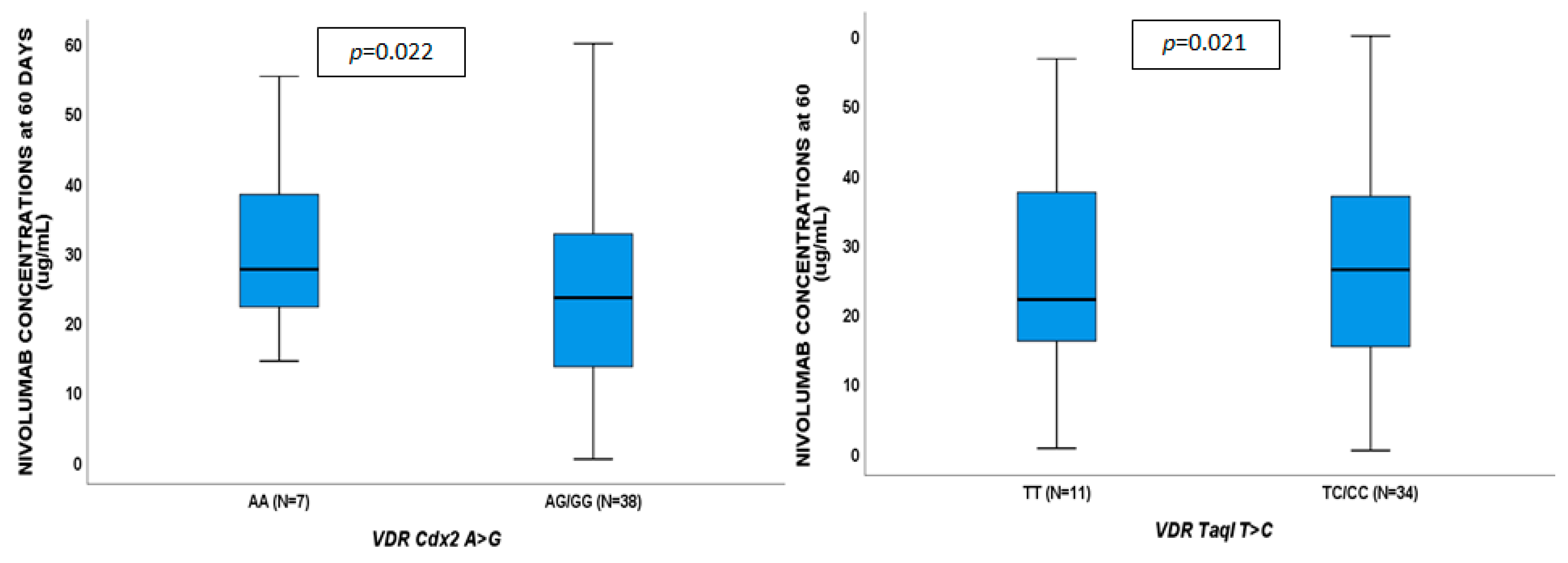
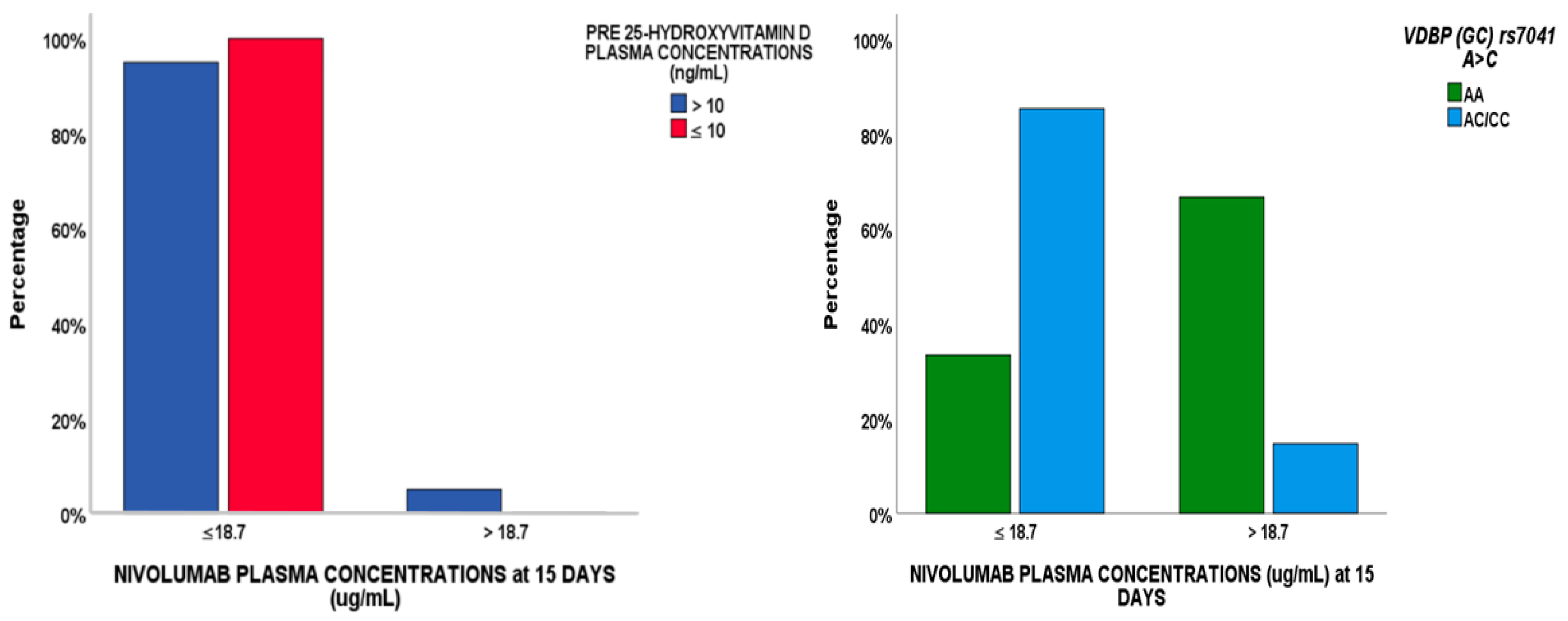
2.3. Pharmacogenetics
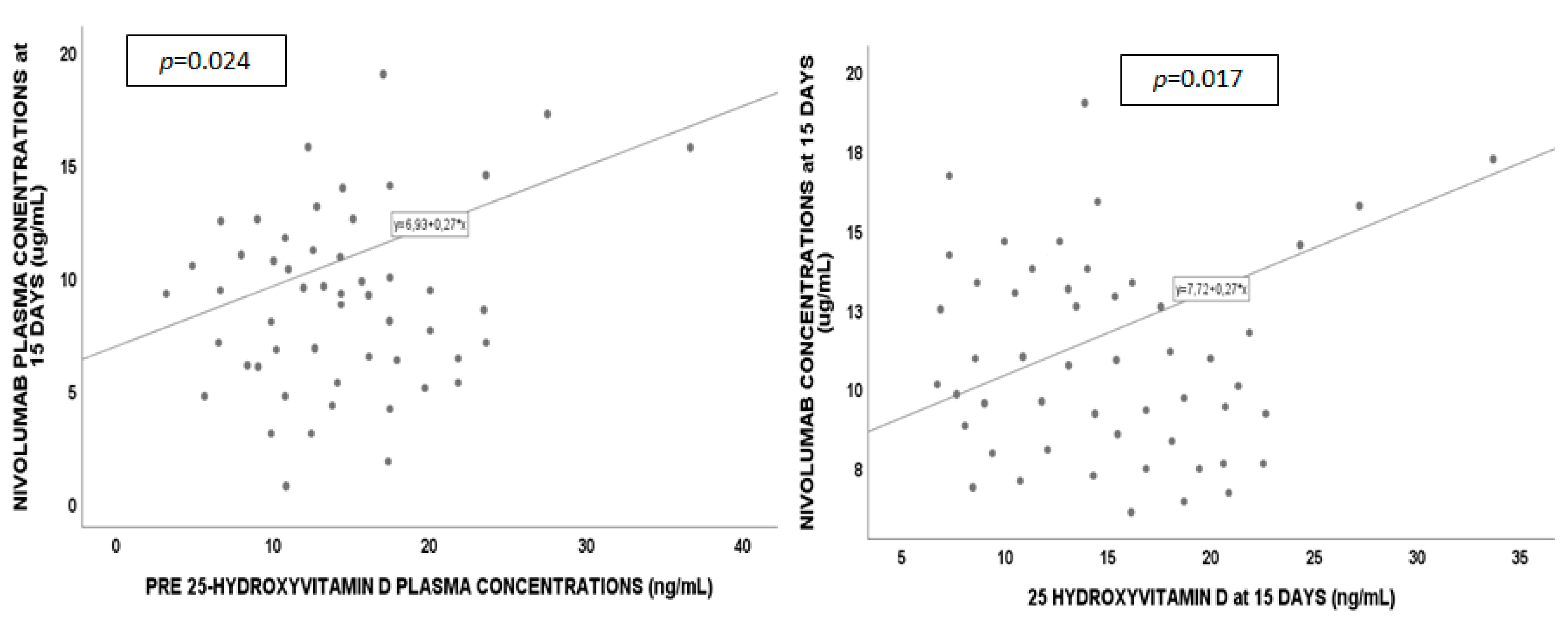
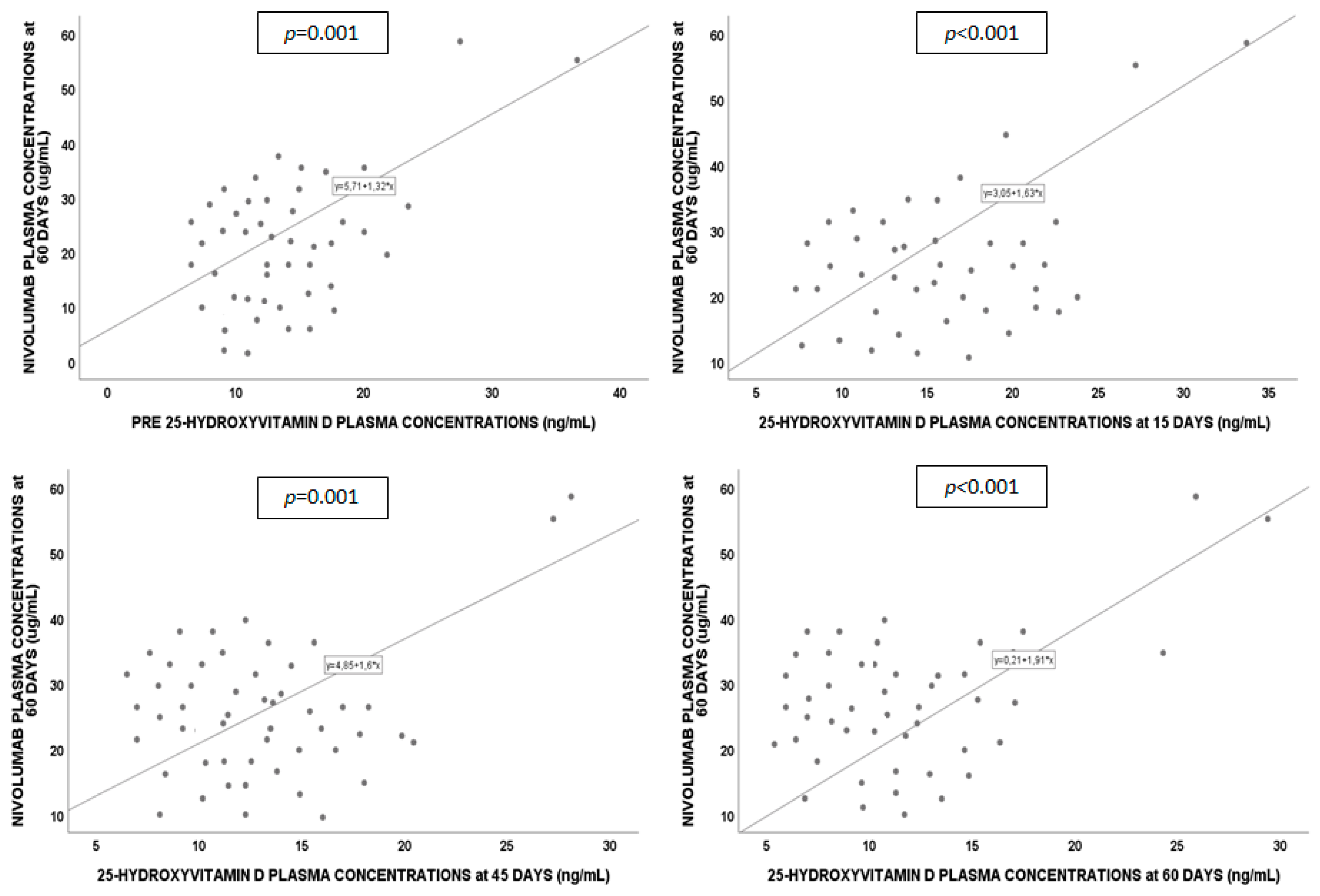
2.4. Regression Analysis
3. Discussion
4. Materials and Methods
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Couzin-Frankel, J. Breakthrough of the year 2013. Cancer immunotherapy. Science 2013, 342, 1432–1433. [Google Scholar] [CrossRef] [PubMed]
- Alsaab, H.O.; Sau, S.; Alzhrani, R.; Tatiparti, K.; Bhise, K.; Kashaw, S.K.; Iyer, A.K. PD-1 and PD-L1 checkpoint signaling inhibition for cancer immunotherapy: Mechanism, combinations, and clinical outcome. Front. Pharm. 2017, 8, 561. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.; Lin, J.; Liao, G.; Tian, Y.; Liang, Y.; Li, R.; Liu, M.; Yuan, Y. Comparative analysis of immune checkpoint inhibitors and chemotherapy in the treatment of advanced non-small cell lung cancer: A meta-analysis of randomized controlled trials. Medicine (Baltimore) 2018, 97, e11936. [Google Scholar] [CrossRef] [PubMed]
- Tykodi, S.S.; Schadendorf, D.; Cella, D.; Reck, M.; Harrington, K.; Wagner, S.; Shaw, J.W. Patient-reported outcomes with nivolumab in advanced solid cancers. Cancer Treat. Rev. 2018, 70, 75–87. [Google Scholar] [CrossRef] [PubMed]
- (FDA) FaDA. FDA Grants Nivolumab Accelerated Approval for Third-Line Treatment of Metastatic Small Cell Lung Cancer; Food and Drug Administration: Silver Spring, MD, USA, 2015.
- Koolen, S.L.W.; Basak, E.A.; Hurkmans, D.; Schreurs, M.W.J.; Bins, S.; Oomen De Hoop, E.; Wijkhuis, A.J.M.; Den Besten, I.; Sleijfer, S.; Debets, R.; et al. Correlation between nivolumab exposure and treatment outcome in NSCLC. In Proceedings of the 2018 ASCO Annual Meeting, Chicago, IL, USA, 1–5 June 2018. [Google Scholar]
- Michot, J.M.; Bigenwald, C.; Champiat, S.; Collins, M.; Carbonnel, F.; Postel-Vinay, S.; Berdelou, A.; Varga, A.; Bahleda, R.; Hollebecque, A.; et al. Immune-related adverse events with immune checkpoint blockade: A comprehensive review. Eur. J. Cancer 2016, 54, 139–148. [Google Scholar] [CrossRef] [PubMed]
- Agrawal, S.; Statkevich, P.; Bajaj, G.; Feng, Y.; Saeger, S.; Desai, D.D.; Park, J.S.; Waxman, I.M.; Roy, A.; Gupta, M. Evaluation of immunogenicity of nivolumab monotherapy and its clinical relevance in patients with metastatic solid tumors. J. Clin. Pharmacol. 2017, 57, 394–400. [Google Scholar] [CrossRef] [PubMed]
- Bersanelli, M.; Leonetti, A.; Buti, S. The link between calcitriol and anticancer immunotherapy: vitamin D as the possible balance between inflammation and autoimmunity in the immune-checkpoint blockade. Immunotherapy 2017, 9, 1127–1131. [Google Scholar] [CrossRef] [Green Version]
- Wang, T.J.; Zhang, F.; Richards, J.B.; Kestenbaum, B.; Van Meurs, J.B.; Berry, D.; Kiel, D.P.; Streeten, E.A.; Ohlsson, C.; Koller, D.L.; et al. Common genetic determinants of vitamin D insufficiency: A genome-wide association study. Lancet 2010, 376, 180–188. [Google Scholar] [CrossRef]
- Ma, K.; Xu, W.; Wang, C.; Li, B.; Su, K.; Li, W. Vitamin D deficiency is associated with a poor prognosis in advanced non-small cell lung cancer patients treated with platinum-based first-line chemotherapy. Cancer Biomark. 2017, 18, 297–303. [Google Scholar] [CrossRef]
- Horn, L.; Spigel, D.R.; Vokes, E.E.; Holgado, E.; Ready, N.; Steins, M.; Poddubskaya, E.; Borghaei, H.; Felip, E.; Paz-Ares, L.; et al. Nivolumab versus docetaxel in previously treated patients with advanced non-small-cell lung cancer: Two-year outcomes from two randomized, open-label, phase III trials (CheckMate 017 and CheckMate 057). J. Clin. Oncol. 2017, 35, 3924–3933. [Google Scholar] [CrossRef]
- Aguiar, P.N., Jr.; Perry, L.A.; Penny-Dimri, J.; Babiker, H.; Tadokoro, H.; De Mello, R.A.; Lopes, G.L., Jr. The effect of PD-L1 testing on the cost-effectiveness and economic impact of immune checkpoint inhibitors for the second-line treatment of NSCLC. Ann. Oncol. 2017, 28, 2256–2263. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Matter-Walstra, K.; Schwenkglenks, M.; Aebi, S.; Dedes, K.; Diebold, J.; Pietrini, M.; Klingbiel, D.; Von Moos, R.; Gautschi, O. A cost-effectiveness analysis of nivolumab versus docetaxel for advanced nonsquamous NSCLC including PD-L1 testing. J. Thorac. Oncol. 2016, 11, 1846–1855. [Google Scholar] [CrossRef] [PubMed]
- Bochen, F.; Balensiefer, B.; Korner, S.; Bittenbring, J.T.; Neumann, F.; Koch, A.; Bumm, K.; Marx, A.; Wemmert, S.; Papaspyrou, G.; et al. Vitamin D deficiency in head and neck cancer patients-prevalence, prognostic value and impact on immune function. Oncoimmunology 2018, 7, e1476817. [Google Scholar] [CrossRef]
- Feng, Q.; Zhang, H.; Dong, Z.; Zhou, Y.; Ma, J. Circulating 25-hydroxyvitamin D and lung cancer risk and survival: A dose-response meta-analysis of prospective cohort studies. Medicine (Baltimore) 2017, 96, e8613. [Google Scholar] [CrossRef] [PubMed]
- Smolders, J.; Menheere, P.; Thewissen, M.; Peelen, E.; Tervaert, J.W.; Hupperts, R.; Damoiseaux, J. Regulatory T cell function correlates with serum 25-hydroxyvitamin D, but not with 1,25-dihydroxyvitamin D, parathyroid hormone and calcium levels in patients with relapsing remitting multiple sclerosis. J. Steroid Biochem. Mol. Biol. 2010, 121, 243–246. [Google Scholar] [CrossRef] [PubMed]
- Malik, S.; Fu, L.; Juras, D.J.; Karmali, M.; Wong, B.Y.; Gozdzik, A.; Cole, D.E. Common variants of the vitamin D binding protein gene and adverse health outcomes. Crit. Rev. Clin. Lab. Sci. 2013, 50, 1–22. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, T.O.; Zhang, J.H.; Parra, E.; Ellis, B.K.; Simpson, C.; Lee, W.M.; Balko, J.; Fu, L.; Wong, B.Y.; Cole, D.E. Vitamin D binding protein is a key determinant of 25-hydroxyvitamin D levels in infants and toddlers. J. Bone Miner. Res. 2013, 28, 213–221. [Google Scholar] [CrossRef] [PubMed]
- Anderson, L.N.; Cotterchio, M.; Cole, D.E.; Knight, J.A. Vitamin D-related genetic variants, interactions with vitamin D exposure, and breast cancer risk among Caucasian women in Ontario. Cancer Epidemiol. Biomark. Prev. 2011, 20, 1708–1717. [Google Scholar] [CrossRef]
- Lafi, Z.M.; Irshaid, Y.M.; El-Khateeb, M.; Ajlouni, K.M.; Hyassat, D. Association of rs7041 and rs4588 polymorphisms of the vitamin D binding protein and the rs10741657 polymorphism of CYP2R1 with vitamin D status among Jordanian patients. Genet. Test Mol. Biomar. 2015, 19, 629–636. [Google Scholar] [CrossRef]
- Daffara, V.; Verdoia, M.; Rolla, R.; Nardin, M.; Marino, P.; Bellomo, G.; Carriero, A.; De Luca, G. Impact of polymorphism rs7041 and rs4588 of Vitamin D Binding Protein on the extent of coronary artery disease. Nutr. Metab. Cardiovasc. Dis. 2017, 27, 775–783. [Google Scholar] [CrossRef]
- Schmid, S.; Diem, S.; Li, Q.; Krapf, M.; Flatz, L.; Leschka, S.; Desbiolles, L.; Klingbiel, D.; Jochum, W.; Fruh, M. Organ-specific response to nivolumab in patients with non-small cell lung cancer (NSCLC). Cancer Immunol. Immunother. 2018, 67, 1825–1832. [Google Scholar] [CrossRef] [PubMed]
- Du Prel, J.B.; Rohrig, B.; Hommel, G.; Blettner, M. Choosing statistical tests: Part 12 of a series on evaluation of scientific publications. Dtsch. Arztebl. Int. 2010, 107, 343–348. [Google Scholar] [PubMed]

| Characteristics | n (%), Median (IQR) | |
|---|---|---|
| n | 45 | |
| Age (years) | 73 (65–79.5) | |
| Male sex | 31 (69) | |
| BMI (Kg/m2) | 23.4 (20.1–26.4) | |
| Caucasian | 45 (100) | |
| NSCLC type | Adenocarcinoma | 34 (52.3) |
| Squamous cell carcinoma | 9 (13.8) | |
| Poorly differentiated carcinoma | 1 (1.5) | |
| Large-cell neuroendocrine carcinoma | 1 (1.5) | |
| Concomitant drugs | Cardiovascular | 24 (36.9) |
| Diabetes | 4 (6.2) | |
| Opioids | 9 (13.8) | |
| Protease inhibitors | 20 (30.8) | |
| Corticosteroid | 12 (18.5) | |
| Vitamin D | 2 (3.1) | |
| Pre-treatment drugs | Cisplatine | 24 (53.3) |
| Docetaxel | 10 (22.2) | |
| Carboplatine | 24 (53.3) | |
| Gemcitabine | 12 (26.7) | |
| Gefitinib | 2 (4.4) | |
| Pemetrexed | 30 (66.7) | |
| Afatinib | 1 (2.2) | |
| Osimertinib | 1 (2.2) | |
| Erlotinib | 20 (44.4) | |
| Vinorelbine | 10 (22.2) | |
| Paclitaxel | 3 (6.7) | |
| Bevacizumab | 3 (6.7) | |
| Etoposide | 4 (8.9) | |
| Zoledronic acid | 1 (2.2) | |
| Bavicizumab | 1 (2.2) | |
| Farletuzumab | 1 (2.2) | |
| Radiotherapy | 1 (2.2) | |
| Single Nucleotide Polymorphism (SNP) | % Homozigous Wild Type | % Heterozygous | % Homozygous Mutant |
|---|---|---|---|
| CYP27B1 +2838 C > T | 20 CC | 2.2 CT | 77.8 TT |
| CYP27B1 −1260 G > T | 73.3 CC | 15.6 CT | 11.1 TT |
| CYP24A1 rs2248359 T > C | 42.2 TT | 40 TC | 17.8 CC |
| CYP24A1 rs927650 C > T | 33.3 CC | 22.2 CT | 44.5 TT |
| CYP24A1 rs2585428 A > G | 31.1 AA | 28.9 AC | 40 CC |
| VDR Cdx2 A > G | 17.8 AA | 13.3 AG | 68.9 GG |
| VDR TaqI T > C | 33.3 TT | 26.7 TC | 40 CC |
| VDR FokI T > C | 11.1 TT | 42.2 TC | 46.7 CC |
| VDR BsmI G > A | 42.2 GG | 57.8 GA | - |
| VDR ApaI C > A | 26.7 CC | 28.9 CA | 44.4 AA |
| VDBP rs7041 T > G | 6.7 TT | 62.2 TG | 31.1 GG |
| Variables | Nivolumab Concentrations ≤ 18.7 μg/mL | |||
|---|---|---|---|---|
| Univariate | Multivariate | |||
| p-Value | OR (95% IC) | p-Value | OR (95% IC) | |
| BMI < 25 Kg/m2 | 0.766 | 1.270 (0.392–6.112) | ||
| Age > 60 years | 0.939 | 0.970 (0.091–9.145) | ||
| Gender (male) | 0.213 | 2.260 (0.692–12.419) | ||
| Drug dosage < 200 mg | 0.945 | 1.056 (0.099–4.867) | ||
| VDBP (GC) AC/CC | 0.059 | 11.667 (0.909–149.700) | 0.049 | 10.667 (0.830–137.145) |
| CYP24A1 3999 CC | NC | |||
| VDR TaqI TC/CC | 0.164 | 3.077 (0.632–14.976) | ||
| CYP27B1 -1260 GG | 0.148 | 3.250 (0.658–16.040) | ||
| Pre 25-hydroxyvitamin D levels | NC | NC | ||
| Pre 1,25-hydroxyvitamin D levels | 0.124 | 3.840 (0.692–21.312) | ||
| Adenocarcinoma NSCLC type | NC | |||
| Squamous cell carcinoma | NC | |||
| Cisplatine pre-treatment | 0.093 | 4.442 (0.852–24.853) | ||
| Carboplatine pre-treatment | 0.190 | 0.300 (0.051–1.854) | ||
| Pemetrexed pre-treatment | NC | |||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cusato, J.; Genova, C.; Tomasello, C.; Carrega, P.; Ottonello, S.; Pietra, G.; Mingari, M.C.; Cossu, I.; Rijavec, E.; Leggieri, A.; et al. Influence of Vitamin D in Advanced Non-Small Cell Lung Cancer Patients Treated with Nivolumab. Cancers 2019, 11, 125. https://doi.org/10.3390/cancers11010125
Cusato J, Genova C, Tomasello C, Carrega P, Ottonello S, Pietra G, Mingari MC, Cossu I, Rijavec E, Leggieri A, et al. Influence of Vitamin D in Advanced Non-Small Cell Lung Cancer Patients Treated with Nivolumab. Cancers. 2019; 11(1):125. https://doi.org/10.3390/cancers11010125
Chicago/Turabian StyleCusato, Jessica, Carlo Genova, Cristina Tomasello, Paolo Carrega, Selene Ottonello, Gabriella Pietra, Maria Cristina Mingari, Irene Cossu, Erika Rijavec, Anna Leggieri, and et al. 2019. "Influence of Vitamin D in Advanced Non-Small Cell Lung Cancer Patients Treated with Nivolumab" Cancers 11, no. 1: 125. https://doi.org/10.3390/cancers11010125
APA StyleCusato, J., Genova, C., Tomasello, C., Carrega, P., Ottonello, S., Pietra, G., Mingari, M. C., Cossu, I., Rijavec, E., Leggieri, A., Di Perri, G., Dal Bello, M. G., Coco, S., Boccardo, S., Ferlazzo, G., Grossi, F., & D’Avolio, A. (2019). Influence of Vitamin D in Advanced Non-Small Cell Lung Cancer Patients Treated with Nivolumab. Cancers, 11(1), 125. https://doi.org/10.3390/cancers11010125







