A Novel Transdermal Power Transfer Device for the Application of Implantable Microsystems
Abstract
:1. Introduction
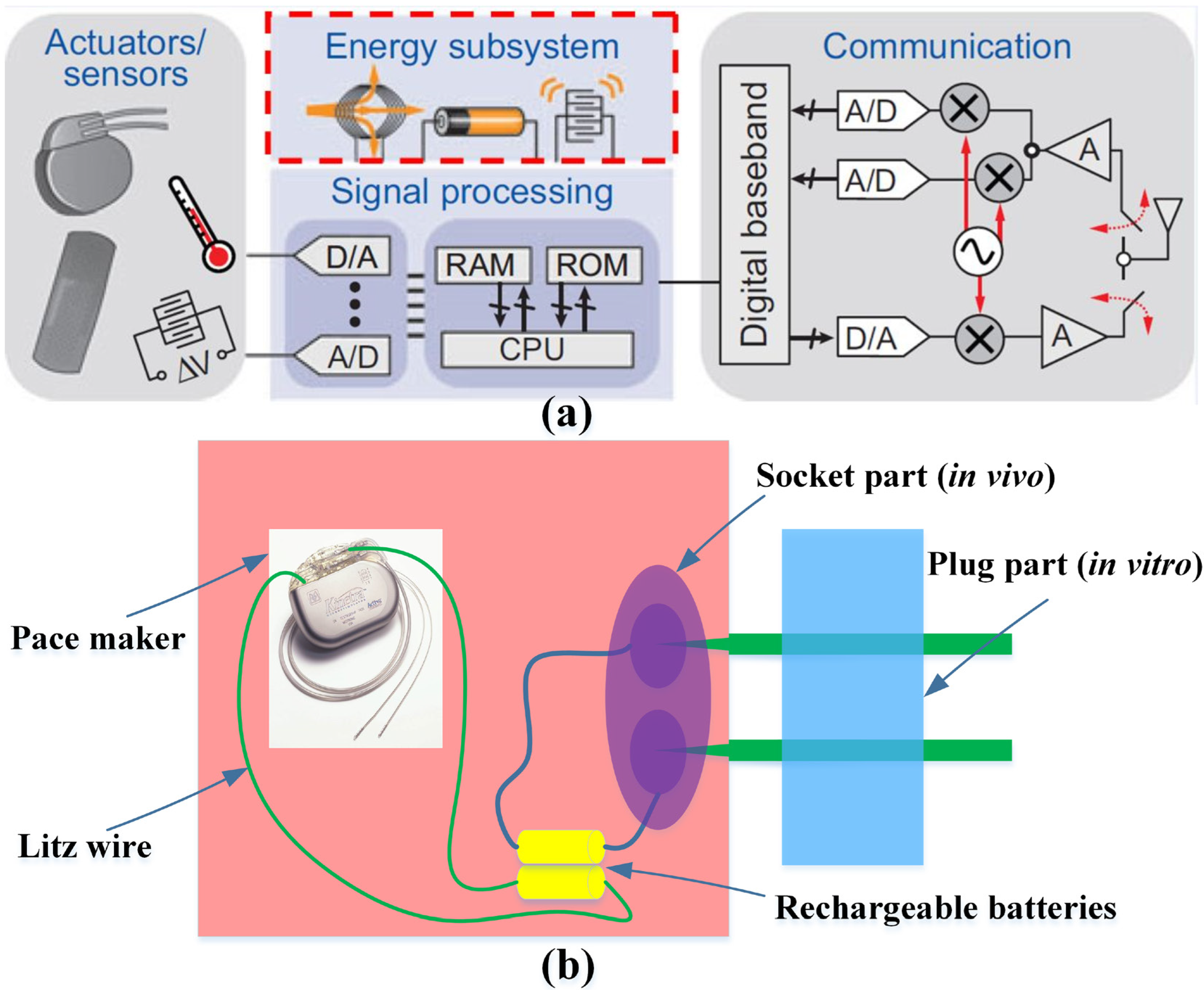
2. Experimental Section
2.1. Design
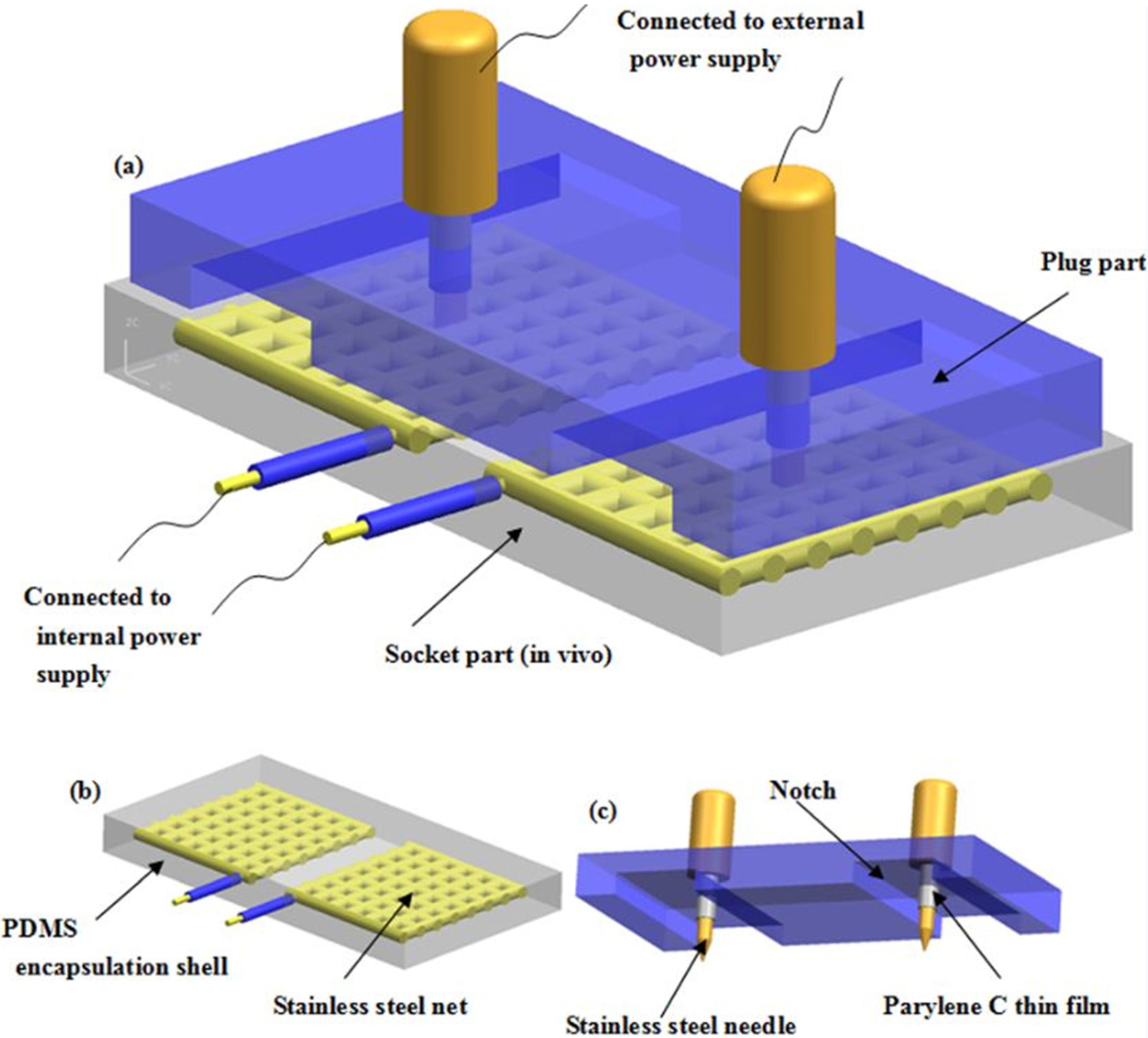
2.2. Fabrication
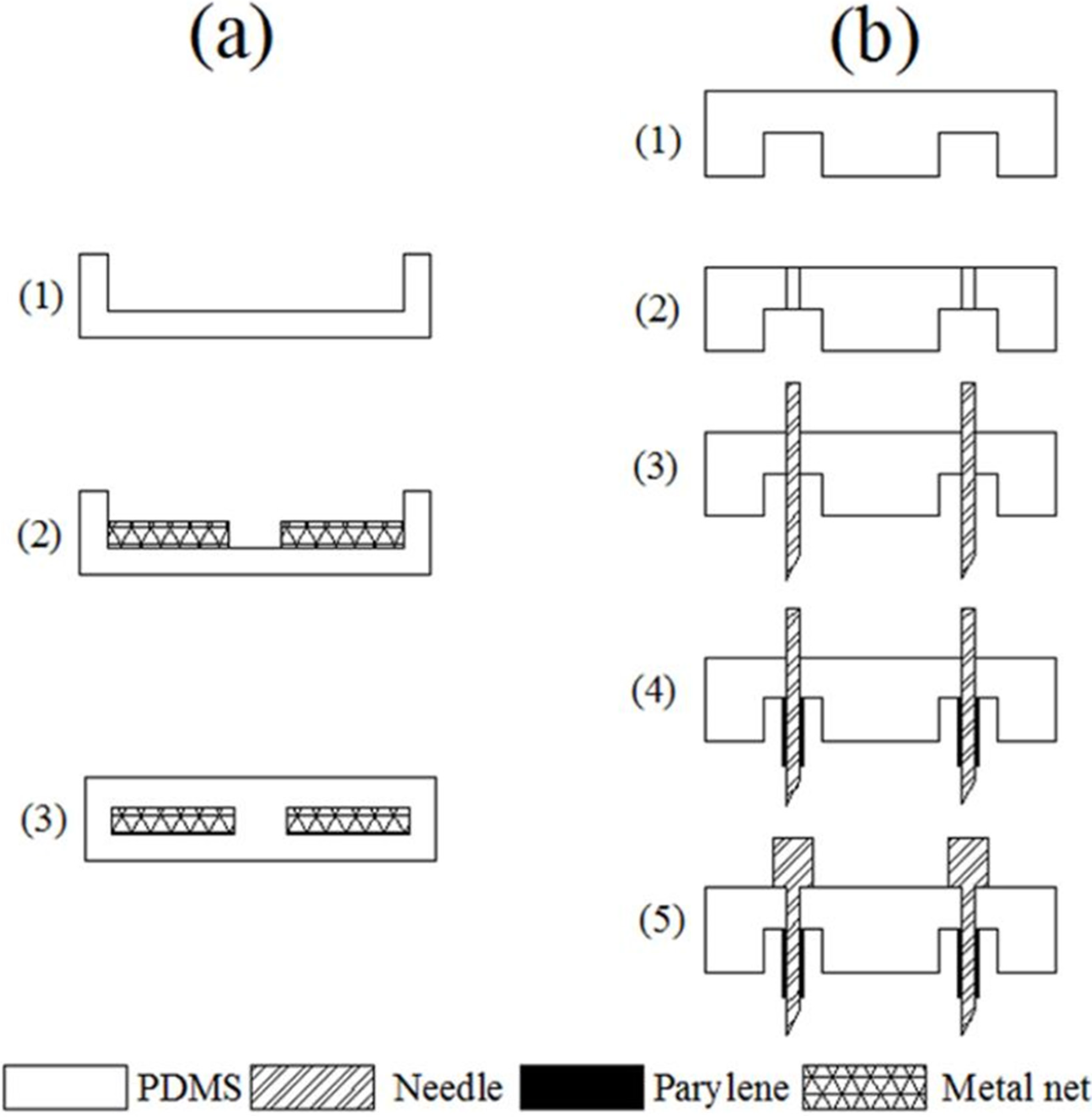

3. Results and Discussion
3.1. Electrical Connection
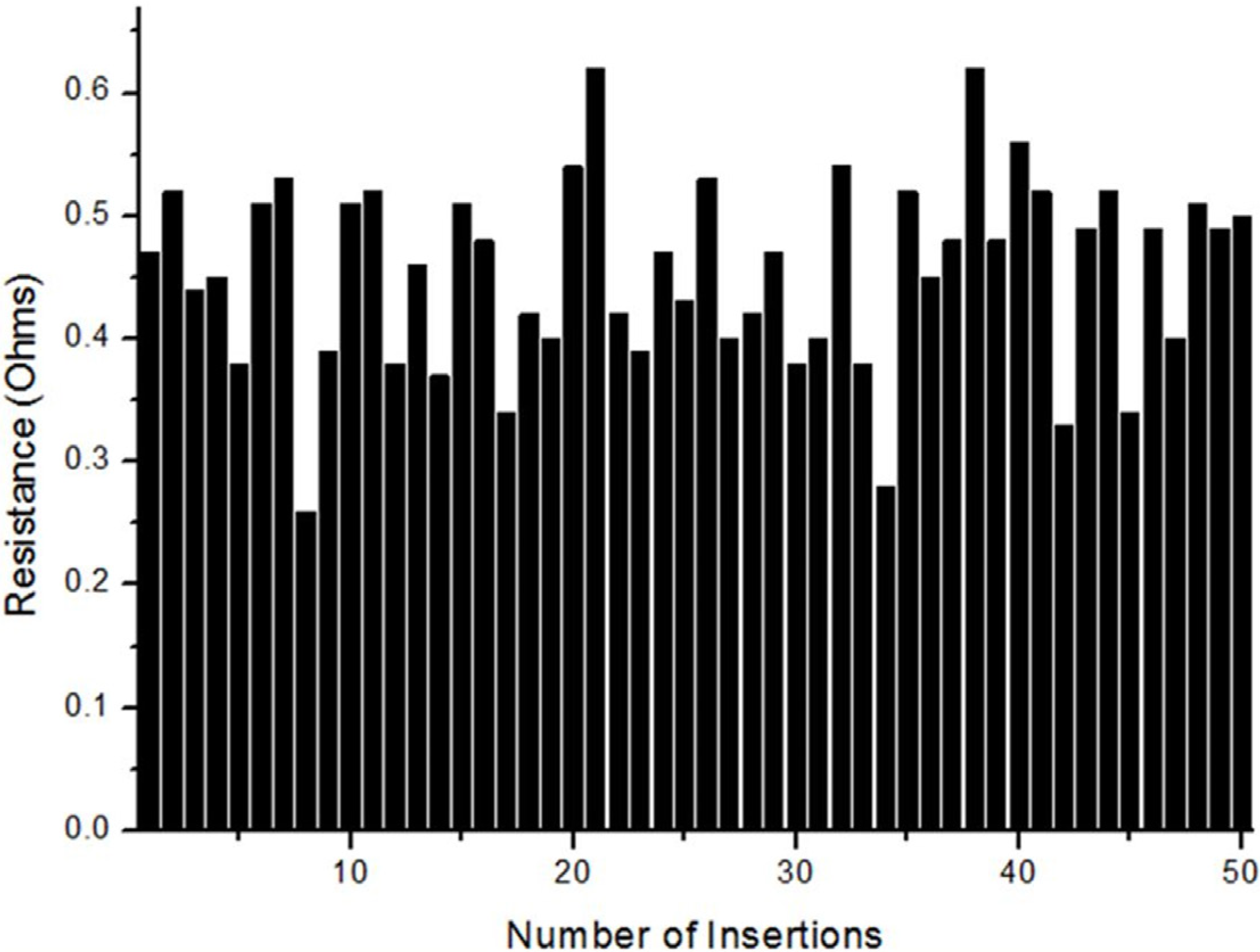

3.2. Waterproofness

3.3. Penetrating Force
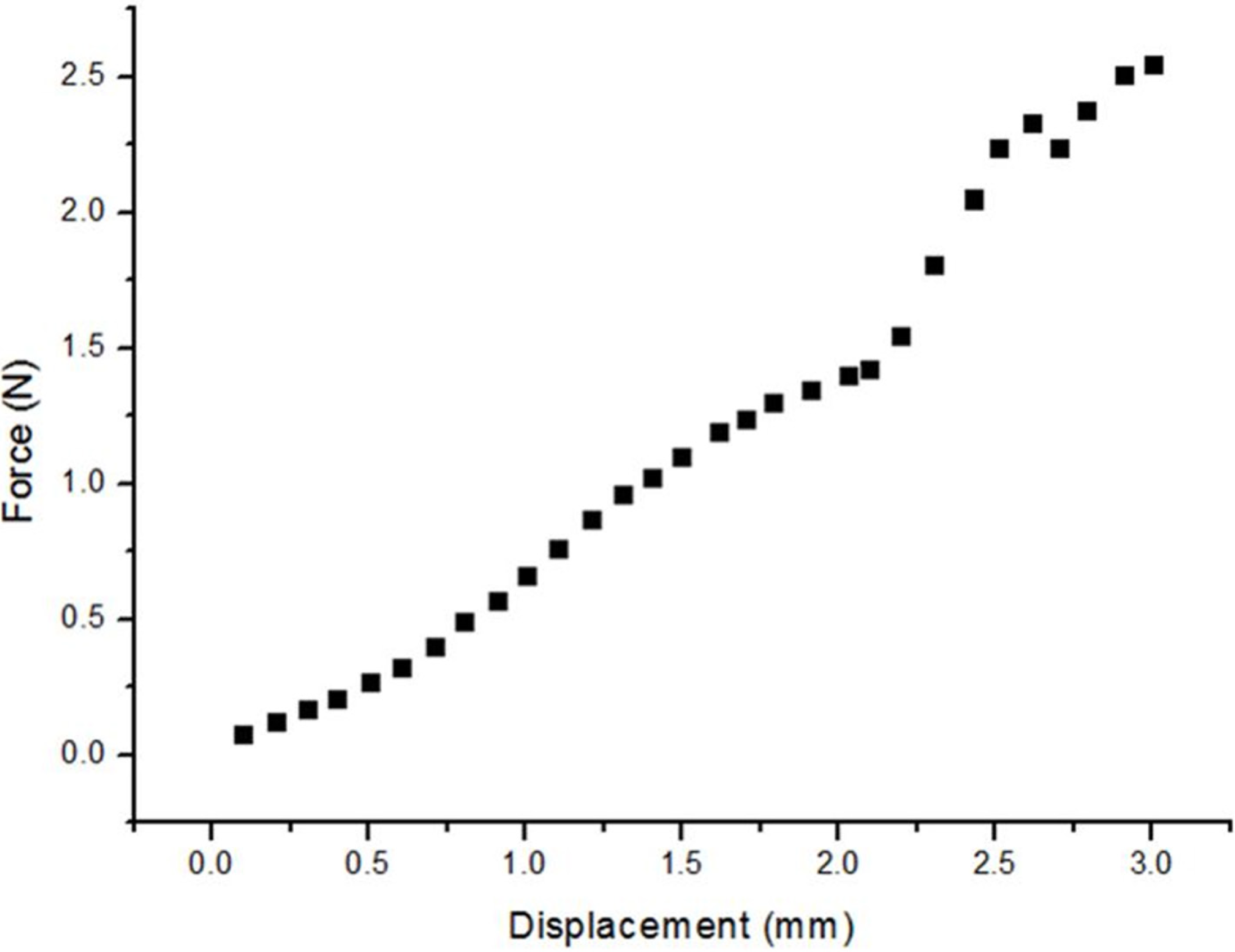
3.4. Charging Temperature
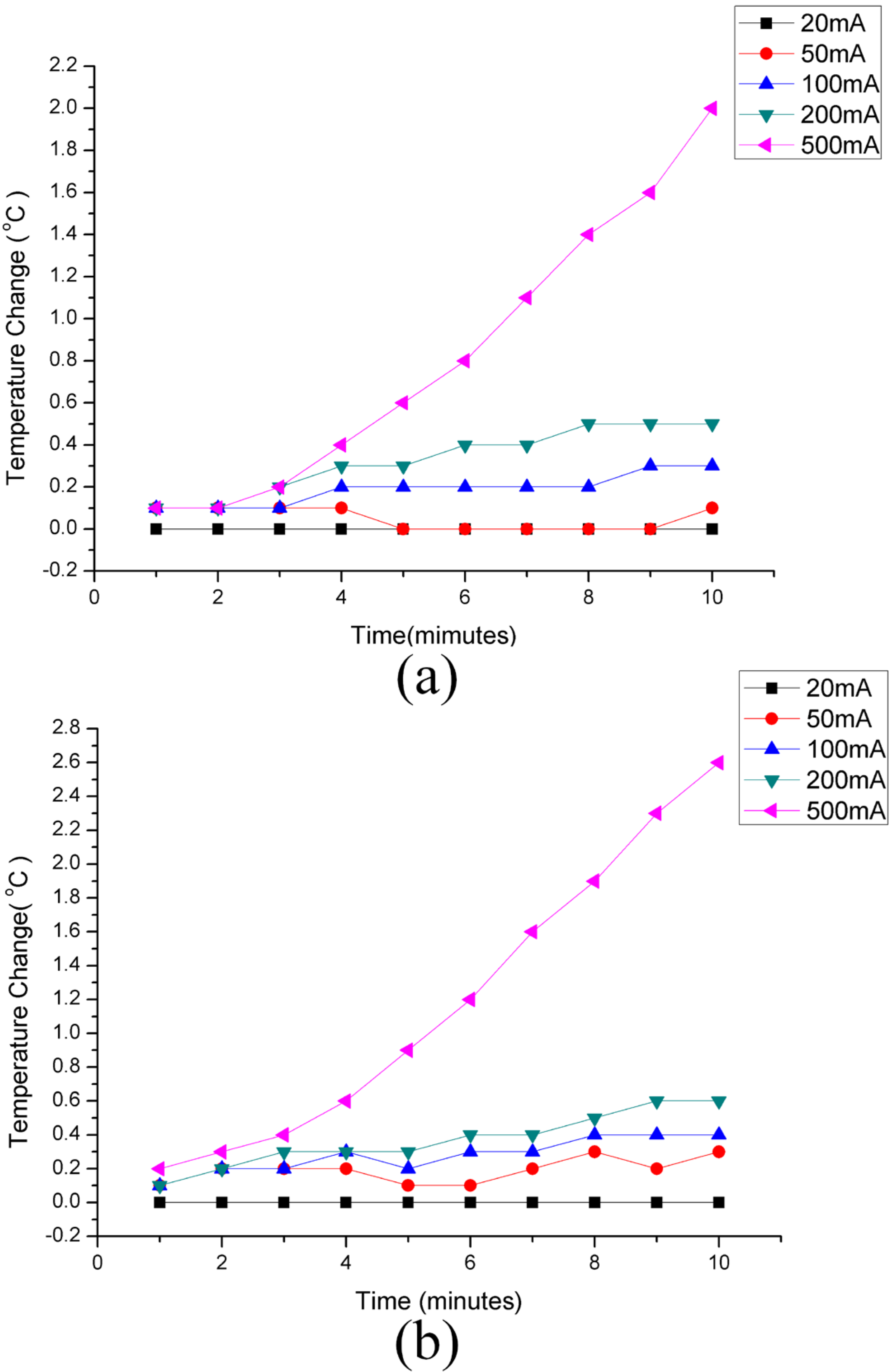
3.5. Implantation of Device

4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Gamini, D.S.; Shastry, P.N. Design and measurements of implantable chip radiator and external receptor for wireless blood pressure monitoring system. In Proceedings of IEEE 2009 MTT-S International Microwave Symposium Digest, Boston, MA, USA, 7–12 June 2009; pp. 1681–1684.
- Hao, S.Y.; Taylor, J.; Miles, A.W.; Bowen, C.R. An implantable electronic system for in-vivo stability evaluation of prosthesis in total hip and knee arthroplasty. In Proceedings of IEEE 2009 Instrumentation and Measurement Technology Conference, Singapore, 5–7 May 2009; pp. 167–172.
- Ko, W.H.; Guo, J.; Ye, X.S.; Zhang, R.; Young, D.J.; Megerian, C.A. Mems acoustic sensors for totally implantable hearing aid systems. In Proceedings of IEEE 2008 International Symposium on Circuits and Systems (ISCAS 2008), Seattle, WA, USA, 18–21 May 2008; pp. 1812–1817.
- Rahimi, S.; Sarraf, E.H.; Wong, G.K.; Takahata, K. Implantable drug delivery device using frequency-controlled wireless hydrogel microvalves. Biomed. Microdevices 2011, 13, 267–277. [Google Scholar] [CrossRef] [PubMed]
- Winzenburg, G.; Schmidt, C.; Fuchs, S.; Kissel, T. Biodegradable polymers and their potential use in parenteral veterinary drug delivery systems. Adv. Drug Deliv. Rev. 2004, 56, 1453–1466. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Chu, M.; Koulajian, K.; Wu, X.Y.; Giacca, A.; Sun, Y. A monolithic polymeric microdevice for pH-responsive drug delivery. Biomed. Microdevices 2009, 11, 1251–1257. [Google Scholar] [CrossRef] [PubMed]
- Grider, J.S.; Brown, R.E.; Colclough, G.W. Perioperative management of patients with an intrathecal drug delivery system for chronic pain. Anesth. Analg. 2008, 107, 1393–1396. [Google Scholar] [CrossRef] [PubMed]
- Meacham, K.W.; Giuly, R.J.; Guo, L.; Hochman, S.; DeWeerth, S.P. A lithographically-patterned, elastic multi-electrode array for surface stimulation of the spinal cord. Biomed. Microdevices 2008, 10, 259–269. [Google Scholar] [CrossRef] [PubMed]
- McCreery, D.B. Cochlear nucleus auditory prostheses. Hear. Res. 2008, 242, 64–73. [Google Scholar] [CrossRef] [PubMed]
- Fayad, J.N.; Otto, S.R.; Shannon, R.V.; Brackmann, D.E. Cochlear and brainstern auditory prostheses “neural interface for hearing restoration: Cochlear and brain stem implants”. Proc. IEEE 2008, 96, 1085–1095. [Google Scholar] [CrossRef]
- Koo, K.I.; Lee, S.; Bae, S.H.; Seo, J.M.; Chung, H.; Cho, D.I. Arrowhead-shaped microelectrodes fabricated on a flexible substrate for enhancing the spherical conformity of retinal prostheses. J. Microelectromech. Syst. 2011, 20, 251–259. [Google Scholar] [CrossRef]
- Chandrakasan, A.P.; Verma, N.; Daly, D.C. Ultralow-power electronics for biomedical applications. Annu. Rev. Biomed. Eng. 2008, 10, 247–274. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Suo, Y.M.; Mitra, S.; Chin, S.; Hsiao, S.; Yazicioglu, R.F.; Tran, T.D.; Etienne-Cummings, R. An efficient and compact compressed sensing microsystem for implantable neural recordings. IEEE Trans. Biomed. Circuits Syst. 2014, 8, 485–496. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Borton, D.A.; Kang, M.Y.; Nurmikko, A.V.; Song, Y.K. An implantable neural sensing microsystem with fiber-optic data transmission and power delivery. Sensors 2013, 13, 6014–6031. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.W.; Chiou, J.C. A wireless and batteryless microsystem with implantable grid electrode/3-dimensional probe array for ecog and extracellular neural recording in rats. Sensors 2013, 13, 4624–4639. [Google Scholar] [CrossRef] [PubMed]
- Cheong, J.H.; Ng, S.S.Y.; Liu, X.; Xue, R.F.; Lim, H.J.; Khannur, P.B.; Chan, K.L.; Lee, A.A.; Kang, K.; Lim, L.S.; et al. An inductively powered implantable blood flow sensor microsystem for vascular grafts. IEEE Trans. BioMed. Eng. 2012, 59, 2466–2475. [Google Scholar] [CrossRef]
- Mallela, V.S.; Ilankumaran, V.; Rao, N.S. Trends in cardiac pacemaker batteries. Indian Pacing Electrophysiol. J. 2004, 4, 201–212. [Google Scholar] [PubMed]
- Cong, P.; Suster, M.A.; Chaimanonart, N.; Young, D.J. Wireless power recharging for implantable bladder pressure sensor. In Proceedings of 2009 IEEE Sensors, Christchurch, New Zealand, 25–28 October 2009; pp. 1670–1673.
- Gaddam, V.R.; Yernagula, J.; Anantha, R.R.; Kona, S.; Kopparthi, S.; Chamakura, A.; Ajmera, P.K.; Srivastava, A. Remote power delivery for hybrid integrated bio-implantable electrical stimulation system. Proc. SPIE 2005, 5763, 20–31. [Google Scholar]
- Li, P.F.; Bashirullah, R.; Principe, J.C. A low power battery management system for rechargeable wireless implantable electronics. In Proceedings of 2006 IEEE International Symposium on Circuits and Systems, 2006, ISCAS 2006, Island of Kos, Greece, 21–24 May 2006; pp. 1139–1142.
- Evans, A.T.; Chiravuri, S.; Gianchandani, Y.B. Transdermal power transfer for recharging implanted drug delivery devices via the refill port. Biomed. Microdevices 2010, 12, 179–185. [Google Scholar] [CrossRef] [PubMed]
- Cong, P.; Chaimanonart, N.; Ko, W.H.; Young, D.J. A wireless and batteryless 10-bit implantable blood pressure sensing microsystem with adaptive RF powering for real-time laboratory mice monitoring. IEEE J. Solid-State Circuits 2009, 44, 3631–3644. [Google Scholar] [CrossRef]
- Cong, P.; Ko, W.H.; Young, D.J. Wireless implantable blood pressure sensing microsystem design for monitoring of small laboratory animals. Sens. Mater. 2008, 20, 327–340. [Google Scholar]
- Cong, P.; Ko, W.H.; Young, D.J. Integrated electronic system design for an implantable wireless batteryless blood pressure sensing microsystem. IEEE Commun. Mag. 2010, 48, 98–104. [Google Scholar] [CrossRef]
- Cong, P.; Ko, W.H.; Young, D.J. Wireless batteryless implantable blood pressure monitoring microsystem for small laboratory animals. IEEE Sens. J. 2010, 10, 243–254. [Google Scholar] [CrossRef]
- Gosselin, B.; Simard, V.; Sawan, M. Low-power implantable microsystem intended to multichannel cortical recording. IEEE Int. Symp. Circuits Syst. 2004, 4, 5–8. [Google Scholar] [CrossRef]
- Martelli, D.; Silvani, A.; McAllen, R.M.; May, C.N.; Ramchandra, R. The low frequency power of heart rate variability is neither a measure of cardiac sympathetic tone nor of baroreflex sensitivity. Am. J. Physiol. Heart. Circ. Physiol. 2014, 307. [Google Scholar] [CrossRef]
- Huang, S.C.; Wong, M.K.; Lin, P.J.; Tsai, F.C.; Fu, T.C.; Wen, M.S.; Kuo, C.T.; Wang, J.S. Modified high-intensity interval training increases peak cardiac power output in patients with heart failure. Eur. J. Appl. Physiol. 2014, 114, 1853–1862. [Google Scholar] [CrossRef] [PubMed]
- Grodin, J.L.; Dupont, M.; Mullens, W.; Taylor, D.O.; Starling, R.C.; Tang, W. The prognostic role of cardiac power indices in advanced chronic heart failure. J. Heart Lung Transpl. 2014, 33. [Google Scholar] [CrossRef]
- Mun, J.Y.; Seo, M.G.; Kang, W.G.; Jun, H.Y.; Park, Y.H.; Pack, J.K. Study on the human effect of a wireless power transfer device at low frequency. In Proceedings of 2012 Progress in Electromagnetics Research Symposium (PIERS 2012), Moscow, Russia, 19–23 August 2012; pp. 322–324.
- Leung, H.Y.; Budgett, D.M.; Taberner, A.; Hu, P. Power loss measurement of implantable wireless power transfer components using a peltier device balance calorimeter. Meas. Sci. Technol. 2014, 25. [Google Scholar] [CrossRef]
- Shmilovitz, D.; Ozeri, S.; Wang, C.C.; Spivak, B. Noninvasive control of the power transferred to an implanted device by an ultrasonic transcutaneous energy transfer link. IEEE Trans. BioMed. Eng. 2014, 61, 995–1004. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.X.; Wang, X.P.; Ma, Y.J.; Liu, N.; Yang, Z.Y. Analysis of heat transfer in power split device for hybrid electric vehicle using thermal network method. Adv. Mech. Eng. 2014, 2014, 210170. [Google Scholar] [CrossRef]
- Jonah, O.; Georgakopoulos, S.V.; Tentzeris, M.M. Wireless power transfer to mobile wearable device via resonance magnetic. In Proceedings of IEEE 14th Annual Wireless and Microwave Technology Conference (WAMICON), Orlando, FL, USA, 7–9 April 2013; pp. 1–3.
- Krop, D.C.J.; Jansen, J.W.; Lomonova, E.A. Decoupled modeling in a multifrequency domain: Integration of actuation and power transfer in one device. IEEE Trans. Magn. 2013, 49, 3009–3019. [Google Scholar] [CrossRef]
- Van Mastrigt, R.; de Zeeuw, S.; Boeve, E.R.; Groen, J. Diagnostic power of the noninvasive condom catheter method in patients eligible for transurethral resection of the prostate. Neurourol. Urodynam. 2014, 33, 408–413. [Google Scholar]
- Myers, K.A.; Leung, M.T.; Potts, M.T.; Potts, J.E.; Sandor, G.G.S. Noninvasive assessment of vascular function and hydraulic power and efficiency in pediatric fontan patients. J. Am. Soc. Echocardiog. 2013, 26, 1221–1227. [Google Scholar] [CrossRef]
- Suzuki, S.; Ishihara, M.; Kobayashi, Y. The improvement of the noninvasive power-supply system using magnetic coupling for medical implants. IEEE Trans. Magn. 2011, 47, 2811–2814. [Google Scholar] [CrossRef]
- Li, Q.B.; Liu, J.Q.; Zhang, G.J. Research on continuum power regression in noninvasive measurement of human blood glucose. Spectrosc. Spect. Anal. 2011, 31, 1481–1485. [Google Scholar]
- Rodger, D.C.; Fong, A.J.; Wen, L.; Ameri, H.; Ahuja, A.K.; Gutierrez, C.; Lavrov, I.; Hui, Z.; Menon, P.R.; Meng, E.; et al. Flexible parylene-based multielectrode array technology for high-density neural stimulation and recording. Sens. Actuat. B Chem. 2008, 132, 449–460. [Google Scholar] [CrossRef]
- Wei, P.; Taylor, R.; Ding, Z.; Chung, C.; Abilez, O.J.; Higgs, G.; Pruitt, B.L.; Ziaie, B. Stretchable microelectrode array using room-temperature liquid alloy interconnects. J. Micromech. Microeng. 2011, 21. [Google Scholar] [CrossRef]
- Rui, Y.F.; Liu, J.Q.; Yang, B.; Li, K.Y.; Yang, C.S. Parylene-based implantable platinum-black coated wire microelectrode for orbicularis oculi muscle electrical stimulation. Biomed. Microdevices 2012, 14, 367–373. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, J.-Q.; Rui, Y.-F.; Kang, X.-Y.; Yang, B.; Chen, X.; Yang, C.-S. A Novel Transdermal Power Transfer Device for the Application of Implantable Microsystems. Micromachines 2015, 6, 396-408. https://doi.org/10.3390/mi6030396
Liu J-Q, Rui Y-F, Kang X-Y, Yang B, Chen X, Yang C-S. A Novel Transdermal Power Transfer Device for the Application of Implantable Microsystems. Micromachines. 2015; 6(3):396-408. https://doi.org/10.3390/mi6030396
Chicago/Turabian StyleLiu, Jing-Quan, Yue-Feng Rui, Xiao-Yang Kang, Bin Yang, Xiang Chen, and Chun-Sheng Yang. 2015. "A Novel Transdermal Power Transfer Device for the Application of Implantable Microsystems" Micromachines 6, no. 3: 396-408. https://doi.org/10.3390/mi6030396
APA StyleLiu, J.-Q., Rui, Y.-F., Kang, X.-Y., Yang, B., Chen, X., & Yang, C.-S. (2015). A Novel Transdermal Power Transfer Device for the Application of Implantable Microsystems. Micromachines, 6(3), 396-408. https://doi.org/10.3390/mi6030396





