Ultrasound-Guided Injection of Botulinum Toxin Type A for Piriformis Muscle Syndrome: A Case Report and Review of the Literature
Abstract
:1. Introduction
2. Methods
| First author and year of publication | Study design | Number of patients with PMS | Doses (U) and number of injections | Injection guide | Outcome measures | Adjunctive therapy | Clinical results/adverse effects |
|---|---|---|---|---|---|---|---|
| Fanucci et al., 2001 [4] | Prospective | 30 | OnabotulinumtoxinA 100 U: 26 received one injections 4 received two injections | CT | Not specific pain score | Not indicated | Reduction of pain intensity after 5–7 days for 26 subjects; other 4 subjects reported a complete pain reduction in the following week/No adverse effects |
| Fishman et al., 2002 [17] | RCT double-blind, parallel | 21 | AbobotulinumtoxinA 200 U | EMG | VAS | Twice-weekly physical therapy program | 65% of the patients reported a 50% of pain reduction/No adverse effects |
| Childers et al., 2002 [3] | RCT double-blind, crossover | 9 | OnabotulinumtoxinA 100 U | FL EMG | VAS | Not indicated | Reduction of pain intensity, distress, spasm and interference with activities respect to baseline/No adverse effects |
| Fishman et al., 2004 [20] | Prospective | 27 | BoNT-B 12,500 U | EMG | VAS | Physical therapy twice weekly for 3 months | A total of 24 of 27 study patients had a pain relief of 50%. The most severe adverse effects were dry mouth and dysphagia, approaching 50% of patients at 2 and 4 weeks |
| Lang et al., 2004 [21] | Prospective | 20 | BoNT-B 5,000 U | EMG | VAS | Dry mouth was reported in 6 of 20 patients | Reduction of myofascial buttock and hip pain associated with PMS/No adverse effects |
| Yoon et al., 2006 [6] | Prospective | 20 | AbobotulinumtoxinA 150 U: One injection | CT | NRS at 4, 8, 12 weeks Korean SF-36 | Stretching exercise 20 times/day for 12 week | Pain reduction respect to baseline(p < 0.0001) Improvement of physical functioning, role physical, bodily pain, general health, vitality and social functioning/Mild and transient adverse events (one case of flu-like syndrome lasting 2 days, five cases of worsening muscular pain lasting 2–3 days, one patient had ecchymosis in the lower limb for 2 days, two patients had atrophy of the piriformis muscle, one case of transient numbness lasting no longer than 72 h |
| Michel et al., 2013 [16] | Prospective | 122 | OnabotulinumtoxinA Ranged between 50 and 100 U: 51 received one Injection; 43 received two injections; 18 received three injections; 9 received four injections; 1 received five injections | EMG | VAS | Not indicated | “Very good’ or ‘Good” in 77% of the cases “Average” in 7.4% of the cases “Poor” in 15.6% of the cases/No adverse effects |
| Fabregat et al., 2014 [18] | Feasibility study | 10 | OnabotulinumtoxinA 100 U | US | Not indicated | Not indicated | No adverse effects during the BoNT-A injections |
| Al-Al-Shaikh et al., 2015 [19] | Retrospective | 12 | OnabotulinumtoxinA 100 U | US CT | VAS | Not indicated | Buttock and sciatic pain reduction respect to baseline (p < 0.001)/No adverse effects |
3. Botulinum Toxin in Piriformis Muscle Syndrome
4. Case Report
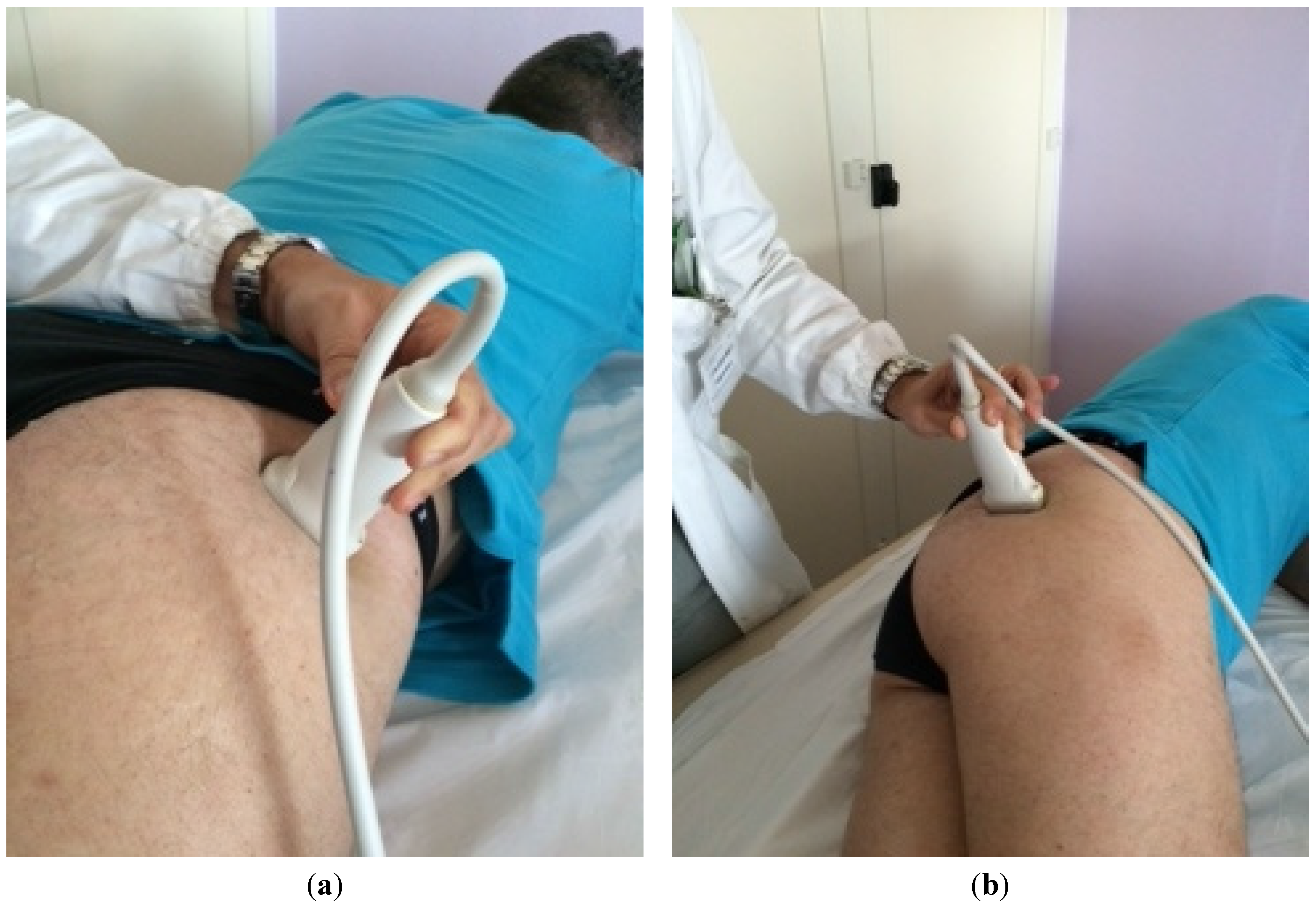
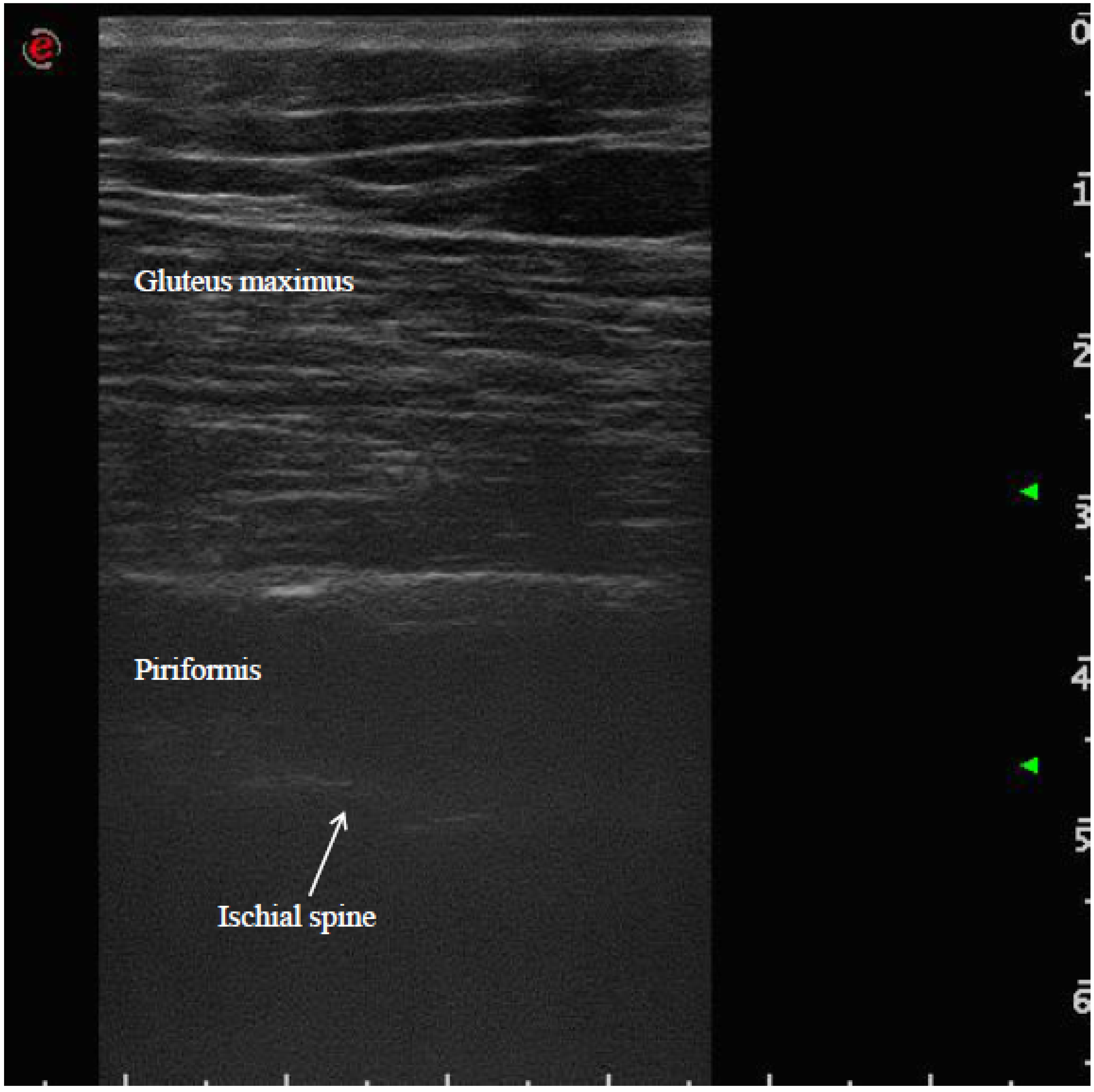
5. Discussion
Author Contributions
Conflicts of Interest
References
- Foster, M.R. Piriformis syndrome. Orthopedics 2002, 25, 821–825. [Google Scholar]
- Kirschner, J.S.; Foye, P.M.; Cole, J.L. Piriformis syndrome, diagnosis and treatment. Muscle Nerve 2009, 40, 10–18. [Google Scholar] [PubMed]
- Childers, M.K.; Wilson, D.J.; Gnatz, S.M.; Conway, R.R.; Sherman, A.K. Botulinum toxin type A use in piriformis muscle syndrome: A pilot study. Am. J. Phys. Med. Rehabil. 2002, 81, 751–759. [Google Scholar] [PubMed]
- Fanucci, E.; Masala, S.; Sodani, G.; Varrucciu, V.; Romagnoli, A.; Squillaci, E.; Simonetti, G. CT-guided injection of botulinic toxin for percutaneous therapy of piriformis muscle syndrome with pre-liminary MRI results about denervative process. Eur. Radiol. 2001, 11, 2543–2548. [Google Scholar] [PubMed]
- Wu, Z.; Yang, Y.; Lee, C.; Cheng, Y. Sciatic perineural edema treated by Botulinum toxin injection on piriformis muscle. Spine J. 2015, 15, 1680–1681. [Google Scholar] [PubMed]
- Yoon, S.J.; Ho, J.; Kang, H.Y.; Lee, S.H.; Kim, K.I.; Shin, W.G.; Oh, J.M. Low-dose botulinum toxin type A for the treatment of refractory piriformis syndrome. Pharmacotherapy 2007, 27, 657–665. [Google Scholar] [PubMed]
- Wissel, J.; Ward, A.B.; Erztgaard, P.; Bensmail, D.; Hecht, M.J.; Lejeune, T.M.; Schnider, P.; Altavista, M.C.; Cavazza, S.; Deltombe, T.; et al. European consensus table on the use of botulinum toxin type A in adult spasticity. J. Rehabil. Med. 2009, 41, 13–25. [Google Scholar] [PubMed]
- Hallett, M.; Benecke, R.; Blitzer, A.; Comella, C.L. Treatment of focal dystonias with botulinum neurotoxin. Toxicon 2009, 54, 628–633. [Google Scholar] [PubMed]
- Naumann, M.; So, Y.; Argoff, C.E.; Childers, M.K.; Dykstra, D.D.; Gronseth, G.S.; Jabbari, B.; Kaufmann, H.C.; Schurch, B.; Silberstein, S.D.; et al. Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Assessment: Botulinum neurotoxin in the treatment of autonomic disorders and pain (an evidence-based review): Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 2008, 70, 1707–1714. [Google Scholar] [PubMed]
- Jabbari, B. Evidence based medicine in the use of botulinum toxin for back pain. J. Neural. Transm. 2008, 115, 637–640. [Google Scholar] [PubMed]
- Soares, A.; Andriolo, R.B.; Atallah, A.N.; da Silva, E.M. Botulinum toxin for myofascial pain syndromes in adults. Cochrane Database Syst. Rev. 2014, 25, 1–37. [Google Scholar]
- Santamato, A.; Ranieri, M.; Panza, F.; Solfrizzi, V.; Frisardi, V.; Lapenna, L.M.; Moretti, B.; Fiore, P. Botulinum toxin type A in the treatment of painful adductor muscle contracture after total hip arthroplasty. Orthopedics 2009, 32. [Google Scholar] [CrossRef]
- Arezzo, J.C. Possible mechanisms for the effects of botulinum toxin on pain. Clin. J. Pain 2002, 18, S125–S132. [Google Scholar] [PubMed]
- Aoki, K.R. Review of a proposed mechanism for the antinociceptive action of botulinum toxin type A. Neurotoxicology 2005, 26, 785–793. [Google Scholar] [CrossRef] [PubMed]
- Welch, M.J.; Purkiss, J.R.; Foster, K.A. Sensitivity of embryonic rat dorsal root ganglia neurons to Clostridium botulinum neurotoxins. Toxicon 2000, 38, 245–258. [Google Scholar] [CrossRef]
- Michel, F.; Decavel, P.; Toussirot, E.; Tatu, L.; Aleton, E.; Monnier, G.; Garbuio, P.; Parratte, B. Piriformis muscle syndrome: diagnostic criteria and treatment of a monocentric series of 250 patients. Ann. Phys. Rehabil. Med. 2013, 56, 371–383. [Google Scholar] [CrossRef] [PubMed]
- Fishman, L.M.; Anderson, C.; Rosner, B. BOTOX and physical therapy in the treatment of piriformis syndrome. Am. J. Phys. Med. Rehabil. 2002, 81, 936–942. [Google Scholar] [CrossRef] [PubMed]
- Fabregat, G.; Roselló, M.; Asensio-Samper, J.M.; Villaneuva-Pérez, V.L.; Martínez-Sanjuan, V.; De Andrés, J.; Eichenberger, U. Computer-tomographic verification of ultrasound-guided piriformis muscle injection: a feasibility study. Pain Physician 2014, 17, 507–513. [Google Scholar] [PubMed]
- Al-Al-Shaikh, M.; Michel, F.; Parratte, B.; Kastler, B.; Vidal, C.; Aubry, S. An MRI evaluation of changes in piriformis muscle morphology induced by botulinum toxin injections in the treatment of piriformis syndrome. Diagn. Interv. Imaging 2015, 96, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Fishman, L.M.; Konnoth, C.; Rozner, B. Botulinum neurotoxin type B and physical therapy in the treatment of piriformis syndrome: A dose-finding study. Am. J. Phys. Med. Rehabil. 2004, 83, 42–50. [Google Scholar] [CrossRef] [PubMed]
- Lang, A.M. Botulinum toxin type B in piriformis syndrome. Am. J. Phys. Med. Rehabil. 2004, 83, 198–202. [Google Scholar] [CrossRef] [PubMed]
- Fishman, L.M.; Dombi, G.W.; Michaelsen, C.; Ringel, S.; Rozbruch, J.; Rosner, B.; Weber, C. Piriformis syndrome: Diagnosis, treatment, and outcome—A 10-year study. Arch. Phys. Med. Rehabil. 2002, 83, 295–301. [Google Scholar] [CrossRef] [PubMed]
- Freiberg, A.H.; Vinke, T.H. Sciatica and the sacroiliac joint. J. Bone Joint Surg. Am. 1934, 16, 126–136. [Google Scholar]
- Pace, J.B.; Nagle, D. Piriformis syndrome. West J. Med. 1976, 124, 435–439. [Google Scholar] [PubMed]
- Niu, C.C.; Lai, P.L.; Fu, T.S.; Chen, L.H.; Chen, W.J. Ruling out piriformis syndrome before diagnosing lumbar radiculopathy. Chang Gung Med. J. 2009, 32, 182–187. [Google Scholar] [PubMed]
- Price, D.D.; Bush, F.M.; Long, S.; Harkins, S.W. A comparison of pain measurement characteristics of mechanical visual analogue and simple numerical rating scales. Pain 1994, 56, 217–226. [Google Scholar] [CrossRef]
- Smith, J.; Hurdle, M.F.; Locketz, A.J.; Wisniewski, S.J. Ultrasound-guided piriformis injection: Technique description and verification. Arch. Phys. Med. Rehabil. 2006, 87, 1664–1667. [Google Scholar] [CrossRef] [PubMed]
- Stewart, J.D. The piriformis syndrome is overdiagnosed. Muscle Nerve 2003, 28, 644–649. [Google Scholar] [CrossRef] [PubMed]
- Porta, M. A comparative trial of botulinum toxin type A and methylprednisolone for the treatment of myofascial pain syndrome and pain from chronic muscle spasm. Pain 2000, 85, 101–105. [Google Scholar] [CrossRef]
- Hanania, M. New technique for piriformis muscle injection using nerve stimulator. Reg. Anesth. 1997, 22, 200–202. [Google Scholar] [CrossRef]
- Hanania, M.; Kitain, E. Perisciatic injection of steroid for the treatment of sciatica due to piriformis syndrome. Region. Anesth. Pain Med. 1998, 23, 223–228. [Google Scholar] [CrossRef]
- Fishman, S.M.; Caneris, O.A.; Bandman, T.B.; Audette, J.F.; Borsook, D. Injection of the piriformis muscle by fluoroscopic and electromyographic guidance. Reg. Anesth. Pain Med. 1998, 23, 554–559. [Google Scholar] [PubMed]
- Betts, A. Combined fluoroscopic and nerve stimulator technique for injection of the piriformis muscle. Pain Physician 2004, 7, 279–281. [Google Scholar] [PubMed]
- Gonzalez, P.; Pepper, M.; Sullivan, W.; Akuthota, V. Confirmation of needle placement within the piriformis muscle of a cadaveric specimen using anatomic landmarks and fluoroscopic guidance. Pain Physician 2008, 11, 327–331. [Google Scholar] [PubMed]
- Bradley, M.; O’Donnell, P. Atlas of Musculoskeletal Ultrasound Anatomy; Cambridge University Press: Cambridge, UK, 2002. [Google Scholar]
- Waseem, Z.; Boulias, C.; Gordon, A.; Ismail, F.; Sheean, G.; Furlan, A.D. Botulinum toxin injections for low-back pain and sciatica. Cochrane Database Syst. Rev. 2010, 30, 419–437. [Google Scholar]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Santamato, A.; Micello, M.F.; Valeno, G.; Beatrice, R.; Cinone, N.; Baricich, A.; Picelli, A.; Panza, F.; Logroscino, G.; Fiore, P.; et al. Ultrasound-Guided Injection of Botulinum Toxin Type A for Piriformis Muscle Syndrome: A Case Report and Review of the Literature. Toxins 2015, 7, 3045-3056. https://doi.org/10.3390/toxins7083045
Santamato A, Micello MF, Valeno G, Beatrice R, Cinone N, Baricich A, Picelli A, Panza F, Logroscino G, Fiore P, et al. Ultrasound-Guided Injection of Botulinum Toxin Type A for Piriformis Muscle Syndrome: A Case Report and Review of the Literature. Toxins. 2015; 7(8):3045-3056. https://doi.org/10.3390/toxins7083045
Chicago/Turabian StyleSantamato, Andrea, Maria Francesca Micello, Giovanni Valeno, Raffaele Beatrice, Nicoletta Cinone, Alessio Baricich, Alessandro Picelli, Francesco Panza, Giancarlo Logroscino, Pietro Fiore, and et al. 2015. "Ultrasound-Guided Injection of Botulinum Toxin Type A for Piriformis Muscle Syndrome: A Case Report and Review of the Literature" Toxins 7, no. 8: 3045-3056. https://doi.org/10.3390/toxins7083045
APA StyleSantamato, A., Micello, M. F., Valeno, G., Beatrice, R., Cinone, N., Baricich, A., Picelli, A., Panza, F., Logroscino, G., Fiore, P., & Ranieri, M. (2015). Ultrasound-Guided Injection of Botulinum Toxin Type A for Piriformis Muscle Syndrome: A Case Report and Review of the Literature. Toxins, 7(8), 3045-3056. https://doi.org/10.3390/toxins7083045








