Clinical Effectiveness and Adverse Events of Bee Venom Therapy: A Systematic Review of Randomized Controlled Trials
Abstract
1. Introduction
2. Methods
2.1. Study Registration
2.2. Search Method for Identifying the Studies
2.3. Inclusion Criteria for This Review
2.3.1. Types of Studies
2.3.2. Types of Participants
2.3.3. Types of Interventions
2.3.4. Type of Outcome Measures
2.4. Data Collection, Extraction and Assessment
2.4.1. Selection of Studies
2.4.2. Data Extraction
2.4.3. Assessment of Risk of Bias
3. Results
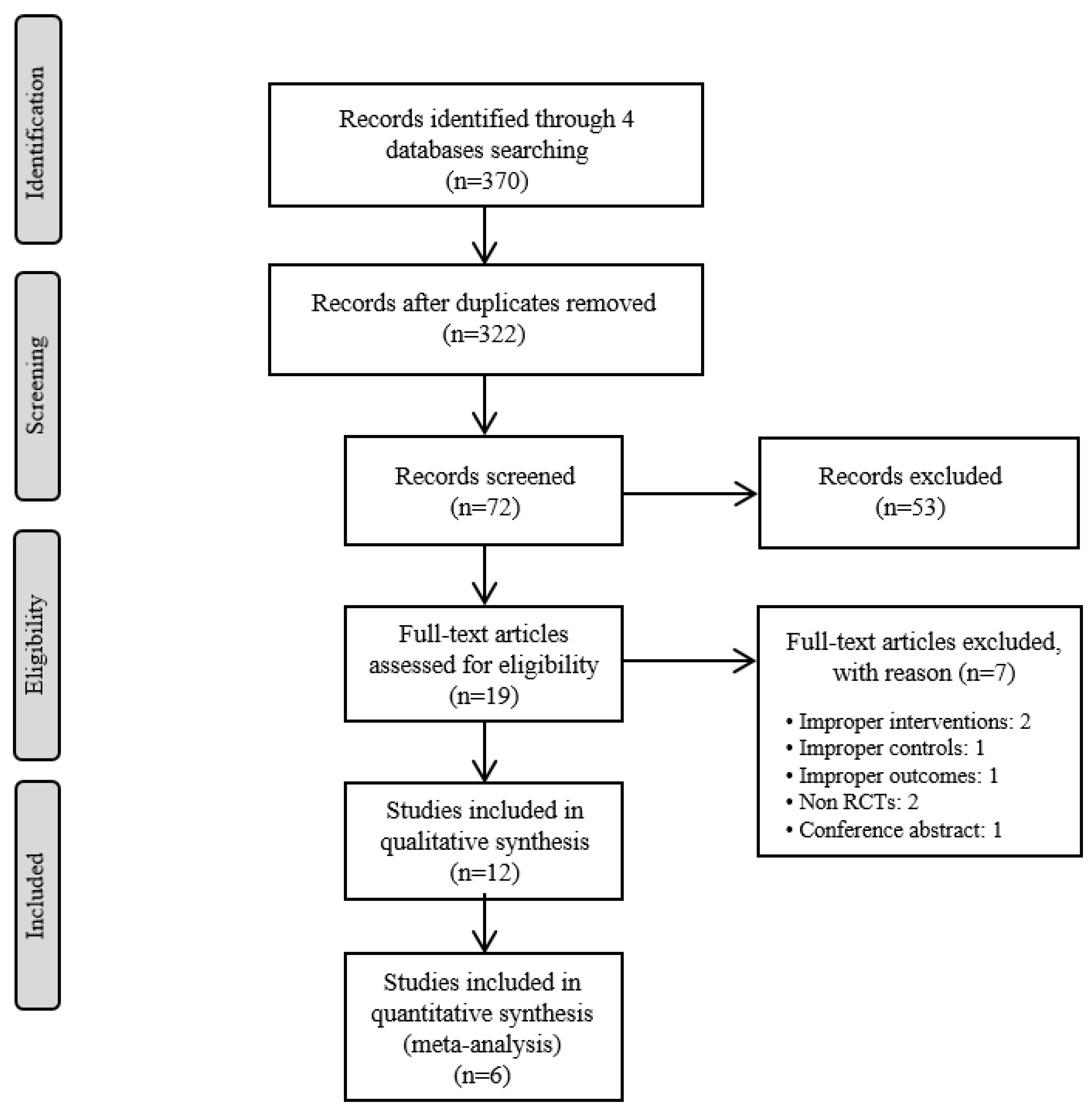
3.1. Description of Included Trials
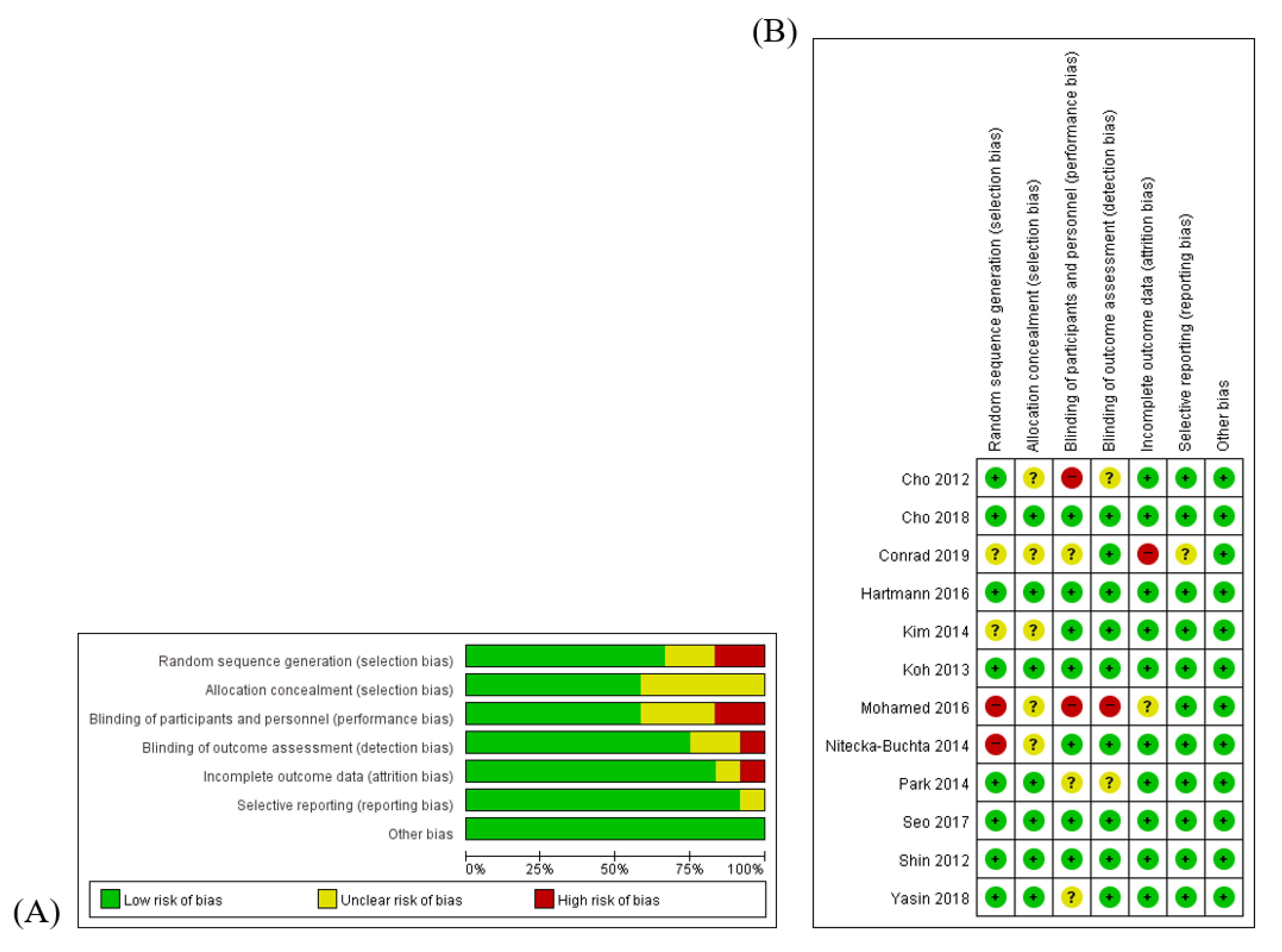
3.2. Risk of Bias of Included Studies
3.3. Effectiveness of the Interventions
3.3.1. Parkinson’s Disease
3.3.2. Arthritis
3.3.3. Musculoskeletal Disorder
3.3.4. Polycystic Ovary Syndrome
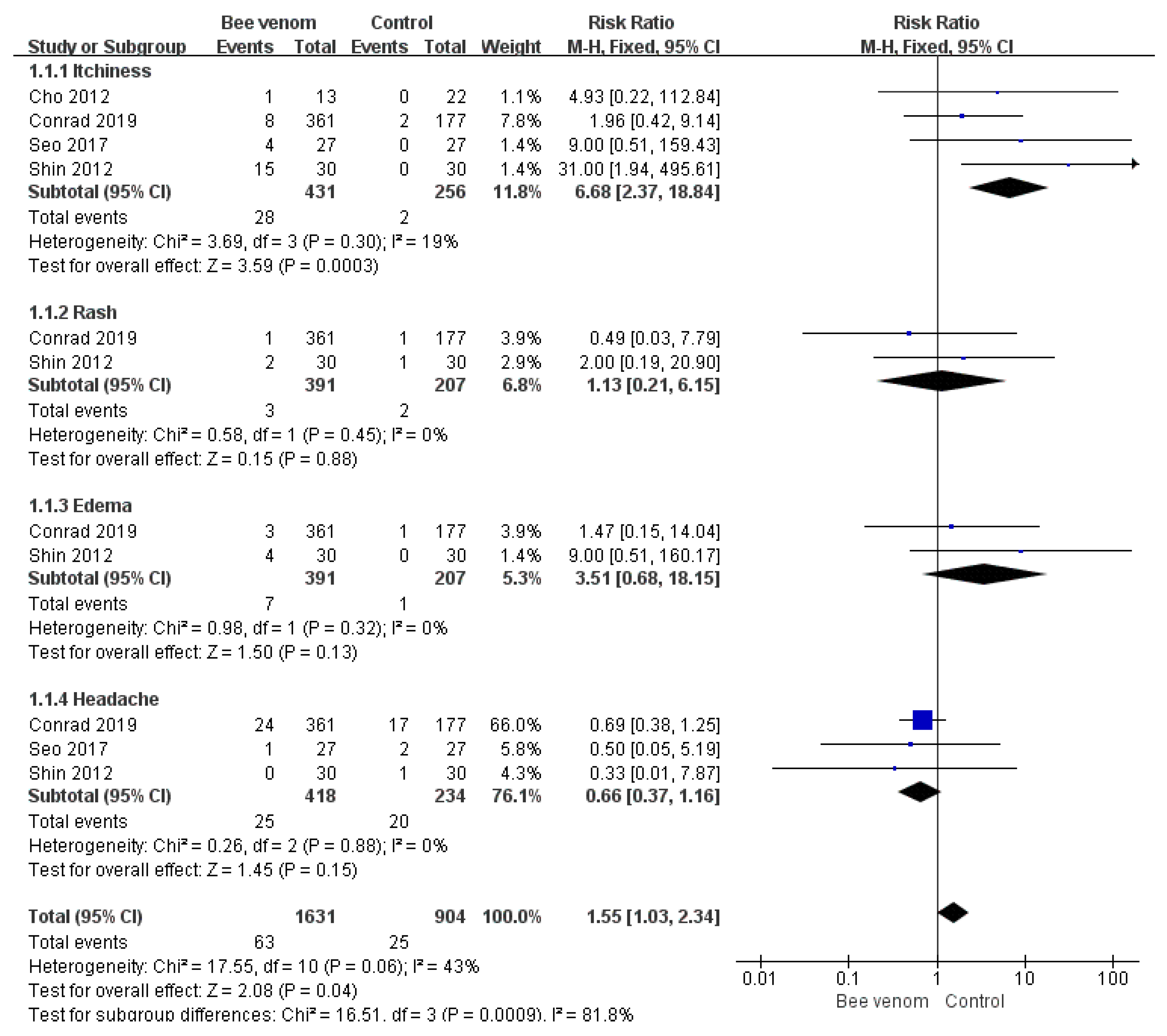
3.4. Adverse Events
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Availability of Data and Materials
References
- Son, D.J.; Lee, J.W.; Lee, Y.H.; Song, H.S.; Lee, C.K.; Hong, J.T. Therapeutic application of anti-arthritis, pain-releasing, and anti-cancer effects of bee venom and its constituent compounds. Pharmacol. Ther. 2007, 115, 246–270. [Google Scholar] [CrossRef]
- Korean Pharmacopuncutre Institute. Pharmacopuncturology, 3rd ed.; Hanmi Medical Publishing Co.: Seoul, Korea, 2019. [Google Scholar]
- Park, J.S.; Lee, M.J.; Chung, K.H.; Ko, D.K.; Chung, H. Live bee acupuncture (Bong-Chim) dermatitis: Dermatitis due to live bee acupuncture therapy in Korea. Int. J. Dermatol. 2013, 52, 1519–1524. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Lariviere, W.R. The nociceptive and anti-nociceptive effects of bee venom injection and therapy: A double-edged sword. Prog. Neurobiol. 2010, 92, 151–183. [Google Scholar] [CrossRef] [PubMed]
- Lee, G.; Bae, H. Bee Venom Phospholipase A2: Yesterday’s Enemy Becomes Today’s Friend. Toxins 2016, 8, 48. [Google Scholar] [CrossRef]
- Zhang, S.; Liu, Y.; Ye, Y.; Wang, X.-R.; Lin, L.-T.; Xiao, L.-Y.; Zhou, P.; Shi, G.-X.; Liu, C.-Z. Bee venom therapy: Potential mechanisms and therapeutic applications. Toxicon 2018, 148, 64–73. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.S.; Pittler, M.H.; Shin, B.C.; Kong, J.C.; Ernst, E. Bee venom acupuncture for musculoskeletal pain: A review. J. Pain. 2008, 9, 289–297. [Google Scholar] [CrossRef] [PubMed]
- Choi, M.S.; Park, S.; Choi, T.; Lee, G.; Haam, K.K.; Hong, M.C.; Min, B.I.; Bae, H. Bee venom ameliorates ovalbumin induced allergic asthma via modulating CD4+CD25+ regulatory T cells in mice. Cytokine 2013, 61, 256–265. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.Y.; Kang, S.S.; Kim, J.-H.; Bae, C.S.; Choi, S.H. Inhibitory effect of whole bee venom in adjuvant-induced arthritis. Vivo 2005, 19, 801–805. [Google Scholar]
- Baek, Y.H.; Huh, J.E.; Lee, J.D.; Choi, D.Y.; Park, D.S. Antinociceptive effect and the mechanism of bee venom acupuncture (Apipuncture) on inflammatory pain in the rat model of collagen-induced arthritis: Mediation by alpha2-Adrenoceptors. Brain Res. 2006, 1073–1074, 305–310. [Google Scholar] [CrossRef]
- Chen, H.-S.; Qu, F.; He, X.; Liao, D.; Kang, S.M.; Lu, S.J. The anti-nociceptive effect and the possible mechanism of acupoint stimulation caused by chemical irritants in the bee venom pain model. Brain Res. 2010, 1355, 61–69. [Google Scholar] [CrossRef]
- Park, J.H.; Yim, B.K.; Lee, J.-H.; Lee, S.; Kim, T.-H. Risk associated with bee venom therapy: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0126971. [Google Scholar] [CrossRef] [PubMed]
- Shamseer, L.; Moher, D.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A.; PRISMA-P Group. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: Elaboration and explanation. BMJ 2015, 2015, g7647. [Google Scholar] [CrossRef] [PubMed]
- Cumpston, M.; Li, T.; Page, M.J.; Chandler, J.; Welch, V.A.; Higgins, J.P.; Thomas, J. Updated guidance for trusted systematic reviews: A new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst. Rev. 2019, 10, ED000142. [Google Scholar] [CrossRef]
- Cho, S.-Y.; Shim, S.-R.; Rhee, H.Y.; Park, H.-J.; Jung, W.-S.; Moon, S.-K.; Park, J.-M.; Ko, C.-N.; Cho, K.-H.; Park, S.-U. Effectiveness of acupuncture and bee venom acupuncture in idiopathic Parkinson’s disease. Parkinsonism. Relat. Disord. 2012, 18, 948–952. [Google Scholar] [CrossRef]
- Hartmann, A.; Mullner, J.; Meier, N.; Hesekamp, H.; van Meerbeeck, P.; Habert, M.-O.; Kas, A.; Tanguy, M.-L.; Mazmanian, M.; Oya, H.; et al. Bee Venom for the Treatment of Parkinson Disease-A Randomized Controlled Clinical Trial. PLoS ONE 2016, 11, e0158235. [Google Scholar] [CrossRef]
- Cho, S.-Y.; Lee, Y.-E.; Doo, K.-H.; Lee, J.-H.; Jung, W.-S.; Moon, S.-K.; Park, J.-M.; Ko, C.-N.; Kim, H.; Rhee, H.Y.; et al. Efficacy of Combined Treatment with Acupuncture and Bee Venom Acupuncture as an Adjunctive Treatment for Parkinson’s Disease. J. Altern. Complem. Med. 2018, 24, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Koh, P.S.; Seo, B.K.; Cho, N.S.; Park, H.S.; Park, D.S.; Baek, Y.H. Clinical effectiveness of bee venom acupuncture and physiotherapy in the treatment of adhesive capsulitis: A randomized controlled trial. J. Shoulder. Elb. Surg. 2013, 22, 1053–1062. [Google Scholar] [CrossRef]
- Park, Y.C.; Koh, P.S.; Seo, B.K.; Lee, J.W.; Cho, N.S.; Park, H.S.; Park, D.S.; Baek, Y.H. Long-term effectiveness of bee venom acupuncture and physiotherapy in the treatment of adhesive capsulitis: A one-year follow-up analysis of a previous randomized controlled trial. J. Altern. Complement. Med. 2014, 20, 919–924. [Google Scholar] [CrossRef]
- Mohamed, E.A.; Ewida, M.M. Efficacy of bee venom phonphoresis in treatment of chronic pelvic inflammatory diseases. Int. J. PharmTech Res. 2016, 9, 66–71. [Google Scholar]
- Conrad, V.J.; Hazan, L.L.; Latorre, A.J.; Jakubowska, A.; Kim, C.M.H. Efficacy and Safety of Honey Bee Venom (Apis mellifera) Dermal Injections to Treat Osteoarthritis Knee Pain and Physical Disability: A Randomized Controlled Trial. J. Altern. Complement. Med. 2019, 25, 845–855. [Google Scholar] [CrossRef]
- Shin, B.-C.; Kong, J.C.; Park, T.-Y.; Yang, C.-Y.; Kang, K.-W.; Choi, S.-M. Bee venom acupuncture for chronic low back pain: A randomised, sham-controlled, triple-blind clinical trial. Eur. J. Integr. Med. 2012, 4, E271–E280. [Google Scholar] [CrossRef]
- Seo, B.-K.; Han, K.; Kwon, O.; Jo, D.-J.; Lee, J.-H. Efficacy of Bee Venom Acupuncture for Chronic Low Back Pain: A Randomized, Double-Blinded, Sham-Controlled Trial. Toxins 2017, 9, 361. [Google Scholar] [CrossRef] [PubMed]
- Nitecka-Buchta, A.; Buchta, P.; Tabenska-Bosakowska, E.; Walczynska-Dragon, K.; Baron, S. Myorelaxant effect of bee venom topical skin application in patients with RDC/TMD Ia and RDC/TMD Ib: A randomized, double blinded study. Biomed. Res. Int. 2014, 2014, 296053. [Google Scholar] [CrossRef]
- Kim, S.K.; Kim, M.C. The affect on delayed onset muscle soreness recovery for ultrasound with bee venom. J. Phys. Ther. Sci. 2014, 26, 1419–1421. [Google Scholar] [CrossRef] [PubMed]
- Yasin, M.M.; Elhosary, E.A.; Hamada, H.A.; Yousef, A.M.; Shahin, M.; Mosaad, D. Effect of bee venom phonophoresis in obese polycystic ovarian women: A Single Blind Randomized Controlled Trial. J. Appl. Pharm. Sci. 2018, 8, 159–164. [Google Scholar] [CrossRef]
- Ahn, C.B.; Youn, H.M.; Cho, E.J. An Investigation of Directions of Research on Bee Venom in the Sphere of Oriental Medicine in Korea in Last Decade. J. Dong-Eui Orient. Med. 2001, 5, 23–42. [Google Scholar]
- World Health Organization Regional Office for the Western Pacific (WPRO). WHO International Standard Terminologies on Traditional Medicine in the Western Pacific Region; WPRO: Manila, Philippines, 2007; Available online: https://apps.who.int/iris/bitstream/handle/10665/206952/9789290612487_eng.pdf?sequence=1&isAllowed=y (accessed on 20 June 2020).
- Castro, H.J.; Mendez-Inocencio, J.I.; Omidvar, B.; Omidvar, J.; Santilli, J.; Nielsen, H.S.; Pavot, A.P.; Richert, J.R.; Bellanti, J.A. A phase I study of the safety of honeybee venom extract as a possible treatment for patients with progressive forms of multiple sclerosis. Allergy. Asthma Proc. 2005, 26, 470–476. [Google Scholar]
- Park, W.; Kim, J.K.; Kim, J.-I.; Choi, D.-Y.; Koh, H.-K. Neuroprotective and Anti-inflammatory Effects of Bee Venom Acupuncture on MPTP-induced Mouse. J. Acupunct. Res. 2010, 27, 105–116. [Google Scholar]
- You, D.-S.; Kwon, Y.-D. The Effect of Bee Venom Pharmacopuncture Therapy on the Condition of Different Concentration in Rheumatoid Arthritis Rat Model. J. Orient. Rehab. Med. 2011, 21, 101–123. [Google Scholar] [CrossRef]
- Aufschnaiter, A.; Kohler, V.; Khalifa, S.; El-Wahed, A.A.; Du, M.; El-Seedi, H.; Buttner, S. Apitoxin and Its Components against Cancer, Neurodegeneration and Rheumatoid Arthritis: Limitations and Possibilities. Toxins 2020, 12, 66. [Google Scholar] [CrossRef]
- Lim, J.A.; Kim, S.C.; Kim, S.N.; Lee, S.Y.; Moon, H.C.; Shin, M.S.; Kim, H.J.; Koo, S.T.; Choi, S.M. The Clinical Study on Bee Venom Acupuncture Treatment on Osteoarthritis of Knee Joint. J. Pharmacopunct. 2005, 20, 73–81. [Google Scholar] [CrossRef]
- Heo, D.S.; Keum, D.H. Effect of Intra-articular Bee Venom Injection on Acute Traumatic Arthritis of Elbow Joint: Two Cases Report. J. Orient. Rehab. Med. 2005, 15, 171–180. [Google Scholar]
- Kim, T.-H.; Kang, K.-S.; Kwon, G.-R. Three cases of affections of the hip treated with Korean Bee-Venom therapy. J. Pharmacopunct. 2001, 4, 127–134. [Google Scholar] [CrossRef]
- Surh, Y.-J.; Chun, K.-S.; Cha, H.-H.; Han, S.S.; Keum, Y.-S.; Park, K.-K.; Lee, S.S. Molecular mechanisms underlying chemopreventive activities of anti-inflammatory phytochemicals: Down-regulation of COX-2 and iNOS through suppression of NF-kappa B activation. Mutat. Res. 2001, 480–481, 243–268. [Google Scholar] [CrossRef]
- Chen, S.-H.; Fahmi, H.; Shi, Q.; Benderdour, M. Regulation of microsomal prostaglandin E2 synthase-1 and 5-lipoxygenase-activating protein/5-lipoxygenase by 4-hydroxynonenal in human osteoarthritic chondrocytes. Arthritis Res. Ther. 2010, 12, R21. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.-H.; Kim, B.-Y.; Kim, W.-B.; Kim, K.-S.; Liu, J.; Kim, D.-H. Bee-venom acupuncture treatment of hip osteoarthritis in a dog. J. Vet. Clin. 2006, 23, 190–193. [Google Scholar]
- Cagnie, B.; Vinck, E.; Rimbaut, S.; Vanderstraeten, G. Phonophoresis versus topical application of ketoprofen: Comparison between tissue and plasma levels. Phys. Ther. 2003, 83, 707–712. [Google Scholar] [CrossRef]
- Kwon, Y.B.; Lee, H.J.; Han, H.J.; Mar, W.C.; Kang, S.K.; Yoon, O.B.; Beitz, A.J.; Lee, J.H. The water-soluble fraction of bee venom produces antinociceptive and anti-inflammatory effects on rheumatoid arthritis in rats. Life Sci. 2002, 71, 191–204. [Google Scholar] [CrossRef]
- Park, J.E.; Kim, K.-H.; Kang, S.; Lee, E.K.; Kim, J.-C.; Jang, B.-H.; Shin, Y.-C.; Ko, S.-G. Usage status and satisfaction with pharmacopuncture in Korea: A survey among Korean medicine doctors. Eur. J. Integr. Med. 2019, 27, 121–130. [Google Scholar] [CrossRef]
- Yang, M.-S.; Lee, S.-H.; Kim, T.-W.; Kwon, J.-W.; Lee, S.-M.; Kim, S.-H.; Kwon, H.-S.; Park, C.-H.; Park, H.-W.; Kim, S.-S.; et al. Epidemiologic and clinical features of anaphylaxis in Korea. Ann. Allerg. Asthma. Im. 2008, 100, 31–36. [Google Scholar] [CrossRef]
- Shim, W.-H.; Park, H.-J.; Kim, H.-S.; Chin, H.-W.; Kim, S.-H.; Ko, H.-C.; Kim, B.-S.; Kim, M.-B.; Kwon, K.-S. Mybacterium chelonae Infection Occurring at the Site of Bee Sting Therapy. Korean J. Dermatol. 2011, 49, 374–378. [Google Scholar]
| Condition | Author [Ref] Year | Conducting Country | Age [Mean] | Sex [M/F] | Study Period | Type of Bee Venom | Intervention | Control | Outcome | Results (p Value between Two Groups) |
|---|---|---|---|---|---|---|---|---|---|---|
| Parkinson’s disease | Cho et al. [15] 2012 | South Korea | (A) 57.0 (B) 55.0 (C) 57.0 | (A) 5/8 (B) 5/8 (C) 3/6 | 8 weeks | Acupuncture (Injection) | (A) - BVA at bilateral GB20, LI11, GB 34, ST36, and LR3, - BV 0.1 mL diluted on 1:20,000 distilled water - twice a week | (B) - Acupuncture at same points with group A - twice a week (C) No treatment | (1) UPDRS (2) PDQL (3) BDI (4) BBS (5) time of steps required to walk 30 m (6) number of steps required to walk 30 m | [A-B, A-C] (1) NS, p < 0.05 (2) NS, NS (3) NS, NS (4) NS, NS (5) NS, NS (6) NS, NS |
| Hartmann et al. [16] 2016 | France | (A) 60.3 (median) (B) 63.3 (median) | (A) 8/12 (B) 12/8 | 11 months | Injection | (A) - BV 0.1mg diluted in 1 mL of NaCl 0.9% - once a month | (B) - Placebo (normal saline 1 mL) - once a month | (1) UPDRS (2) Hoenh and Yahr stages (3) ADL (4) BREF (5) MMS (6) PDQ-39 (7) [123I]-FP-CIT binding potential | (1) NS (2) NS (3) NS (4) NS (5) NS (6) NS (7) NS | |
| Cho et al. [17] 2018 | South Korea | (A) 64.4 (B) 61.3 (C) 64.1 | (A) 14/10 (B) 8/16 (C) 10/5 | 12 weeks + 8 weeks (follow-up) | Acupuncture (Injection) | (A) - BVA at bilateral GB20, LI11, GB 34, ST36, and LR3 - dried BV 1 mg diluted in 20 mL of normal saline - twice a week | (B) - Placebo (normal saline injection at same points with group A - twice a week (C) Antiparkinsonian drugs | (1) UPDRS (2) PDQL (3) BDI (4) PIGD (5) Gait speed (6) Gait number (7) MXE (8) DCL | [A-B, A-C] (1) NS, p = 0.001 (2) NS, p = 0.968 (3) NS, NS (4) NS, p = 0.001 (5) NS, NS (6) NS, p = 0.115 (7) NS, NS (8) NS, NS | |
| Adhesive capsulitis | Koh et al. [18] 2013 | South Korea | (A) 55.0 (B) 56.1 (C) 55.1 | (A) 6/16 (B) 8/15 (C) 6/17 | 12 weeks | Acupuncture (Injection) | (A) - BVA 100 cc (1:10,000 of saline) at LI15, LI16, TE14, GB21, C7, SI11, and additional 5 points around the shoulder - Physiotherapy (B) - BVA 300 cc (1:30,000 of saline) at same points with group A - Physiotherapy | (C) - Placebo (normal saline injection) - Physiotherapy | (1) SPADI (2) VAS—at rest, at night, motion (3) ROM—abduction, forward flexion, extension, external rotation | [Among 3 groups] (1) p = 0.017 (2) p = 0.110 (at rest), p = 0.160 (at night), p = 0.029 (motion) (3) NS |
| Park et al. [19] 2014, follow-up of [18] | (A) 55.4 (B) 52.8 (C) 56.4 | (A) 6/16 (B) 8/15 (C) 6/17 | 1 year | 91) SPADI (2) VAS—at rest, at night, motion (3) Recurrence of symptoms | [Among 3 groups](1) p = 0.043(2) NS(3) A-1, B-3, C-4 | |||||
| Pelvic inflammatory disease | Mohamed et al. [20] 2016 | Egypt | (A) 32.1 (B) 32.5 | (A) 0/15 (B) 0/15 | 4 weeks | Ultrasound gel | (A) - BV gel topical application with phonophoresis - BV 20 μg/gel 1 g - 20 min/time, 3 times per week - doxycycline 100 mg, orally bid for 7 days | (B) Doxycycline 100 mg, orally bid for 7 days | (1) C-reactive protein (2) Pain intensity | (1) p < 0.0001 (2) p < 0.0001 |
| Knee osteoarthritis | Conrad et al. [21] 2019 | South Korea | (A) 56.9 (B) 55.8 | (A) 91/143 (B) 64/69 | 12 weeks | Injection | (A) - BV injection at 2–15 sites escalating over study period (0.1 mL at each site), 10 points at bilateral knees, BL19, BL21, BL23, BL25, and BL27 - dried HV 1.0 mg/1.0 mL 0.5% preservative-free lidocaine | (B) Histamine phosphate injection at same sites with group A | (1-1) WOMAC pain (1-2) WOMAC physical function (2-1) WOMAC VAS resting (2-2) WOMAC VAS walking (3) PGA | (1-1) p = 0.001 (1-2) p = 0.001 (2-1) p = 0.1051 (2-2) p = 0.001 (3) p = 0.0001 |
| Low back pain | Shin et al. [22] 2012 | South Korea | (A) 42.9 (B) 40.0 | (A) 13/17 (B) 14/16 | 4 weeks | Acupuncture (Injection) | (A) - BVA at bilateral BL23, BL24, and BL25 - BV 0.1 mL diluted on 1:2000 distilled water - twice a week | (B) - Placebo (normal saline injection at same points with group A) - twice a week | (1) Pain intensity (VAS) (2) ODQ (3) SF-36 | (1) p = 0.012 (2) NS (3) NS |
| Seo et al. [23] 2017 | South Korea | (A) 49.9 (B) 50.1 | (A) 9/18 (B) 4/23 | 3 weeks | Acupuncture (Injection) | (A) - BVA at bilateral BL23, BL24, BL26, and GB30, GV3, GV4, and GV5 - dried BV diluted on 1:20000 normal saline (0.9% NaCl) - Loxonin 60 mg, orally tid for 3 weeks | (B) - Placebo (normal saline injection at same points with group A) - Loxonin 60 mg, orally tid for 3 weeks | (1) Bothersomeness (VAS) (2) Pain intensity (VAS) (3) ODI (4) BDI (5) EQ-5D | (1) p = 0.016 (2) p = 0.049 (3) p = 0.009 (4) p = 0.043 (5) p = 0.051 | |
| Temporomandibular disorder (RDC/TMD Ia and RDC/TMD Ib) | Nitecka-Buchta et al. [24] 2014 | Poland | 23 (22-34) | (A) 6/28 (B) 4/30 | 2 weeks | Ointment | (A) - BV ointment (0.012 mg liquid BV) for topical skin application in region of both masseter muscles - Massage | (B) - Vaseline at same region with group A - Massage | (1) Muscle tonus (2) Muscle contraction (3) VAS | (1) NR (2) NR (3) NR |
| Delayed onset muscle soreness | Kim et al. [25] 2014 | South Korea | (A) 27.4 (B) 28.9 | (A) 0/10 (B) 0/10 | 3 days | Ultrasound gel | (A) - Ultrasound gel and diluted bee venom (0.001%) mixed at a ratio of 9:1 - Ultrasound at the belly of the biceps brachii muscle, - 1 MHz, 1.0 W/cm2, 2.5 cm/s, 10 min | (B) - Ultrasound in the same way as group A, with pure ultrasound gel without BV | (1) VAS (2) CK (3) ROM—flexion, extension | (1) p < 0.05 (2) NS (3) p < 0.05 |
| Polycystic ovary syndrome | Yasin et al. [26] 2019 | Egypt | (A) 26.0 (B) 26.3 | (A) 0/23 (B) 0/23 | 14 weeks | Ultrasound gel | (A) - BV gel topical application with phonophoresis at BL23 and Zigong - 0.6–1.0 mg of BV each session, 1 MHz - twice a week - low calorie diet (1200–1400 kcal/day) | (B) - Ultrasound in the same way as group A, with pure ultrasound gel without BV - low calorie diet (1200–1400 kcal/day) | (1) LH (2) FSH (3) LH/FSH (4) Progesterone | (1) p = 0.683 (2) p = 0.449 (3) p = 0.456 (4) p = 0.183 |
| Author [Ref] Year | Condition | Type of Bee Venom | Adverse Events [Number of Patients] | |
|---|---|---|---|---|
| Bee Venom Group | Control Group | |||
| Cho et al. [15] 2012 | Parkinson’s disease | Acupuncture | itchiness 1 (drop-out) | - |
| Hartmann et al. [16] 2016 | Parkinson’s disease | Injection | redness/itchiness 165 cases, insomnia 1 case, nausea 3 cases, fatigue 2 cases, dyskinesia 1 case BV specific IgE 18 patients (90%) BV specific IgG4 12 patients (60%) | redness/itchiness 6 cases, insomnia 1, nausea 9 cases, fatigue 10 cases, dyskinesia 1 case, bradycardia 2 cases |
| Shin et al. [22] 2012 | Low back pain | Acupuncture | itchiness 15, skin flare 5, edema 4, rash 2 | rash 1, headache 1, hand-foot tingling 1 |
| Seo et al. [23] 2017 | Low back pain | Acupuncture | minimal itching sensation (recovered completely without any treatment) 4, headache 1, generalized myalgia 1 | headache 2, dizziness 2 |
| Koh et al. [18] 2013 | Adhesive capsulitis | Acupuncture | Muller Grade 0 reactions 30, Muller Grade 1 reactions 1 | slight redness and pruritus 3 |
| Conrad et al. [21] 2019 | Knee osteoarthritis | Injection | swelling 15, discoloration 10, pruritus 8, erythema 7, urticaria 5, hypersensitivity 3, edema 3, injection site pain 3, vesicles 3, rash 1, hematoma 1, paresthesia 1, headache 24, back pain 13, nasopharyngitis 11, upper respiratory tract infection 11, pain in extremity 10, arthralgia 8, diarrhea 10 | itchiness 2, erythema 1, urticaria 1, rash 1, headache 17, back pain 9, nasopharyngitis 7, upper respiratory tract infection 4, pain in extremity 4, arthralgia 4, diarrhea 1 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jang, S.; Kim, K.H. Clinical Effectiveness and Adverse Events of Bee Venom Therapy: A Systematic Review of Randomized Controlled Trials. Toxins 2020, 12, 558. https://doi.org/10.3390/toxins12090558
Jang S, Kim KH. Clinical Effectiveness and Adverse Events of Bee Venom Therapy: A Systematic Review of Randomized Controlled Trials. Toxins. 2020; 12(9):558. https://doi.org/10.3390/toxins12090558
Chicago/Turabian StyleJang, Soobin, and Kyeong Han Kim. 2020. "Clinical Effectiveness and Adverse Events of Bee Venom Therapy: A Systematic Review of Randomized Controlled Trials" Toxins 12, no. 9: 558. https://doi.org/10.3390/toxins12090558
APA StyleJang, S., & Kim, K. H. (2020). Clinical Effectiveness and Adverse Events of Bee Venom Therapy: A Systematic Review of Randomized Controlled Trials. Toxins, 12(9), 558. https://doi.org/10.3390/toxins12090558





