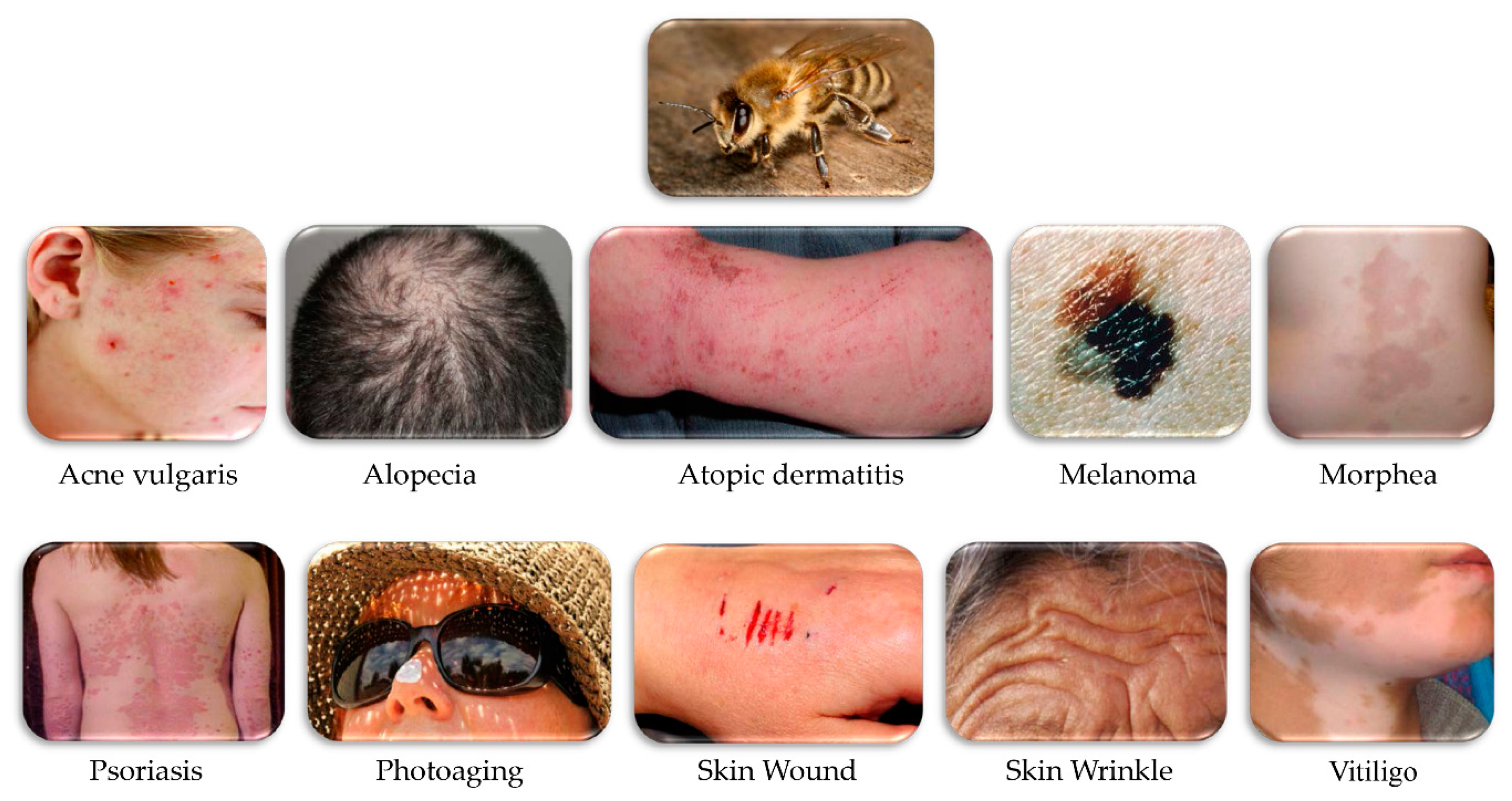
Potential Therapeutic Applications of Bee Venom on Skin Disease and Its Mechanisms: A Literature Review
Abstract
1. Introduction
2. Therapeutic Effects of BV in Skin Diseases
2.1. Acne
2.1.1. Clinical Studies
2.1.2. In Vivo Studies
2.1.3. In Vitro Studies
2.2. Alopecia
2.2.1. In Vivo Studies
2.2.2. In Vitro Studies
2.3. Atopic Dermatitis (AD)
2.3.1. Clinical Studies
2.3.2. In Vivo Studies
2.3.3. In Vitro Studies
2.4. Melanoma
2.4.1. In Vivo Studies
2.4.2. In Vitro Studies
2.5. Morphea
Clinical Studies (Case Report)
2.6. Photoaging
In Vitro Studies
2.7. Psoriasis
Clinical Studies
2.8. Skin Wounds
In Vivo Studies
2.9. Skin Wrinkling
Clinical Studies
2.10. Vitiligo
In Vitro Studies
3. Inhibitory Effects of BV against Pathogenic Agent which is Related to Skin Disease
3.1. Bacteria
3.1.1. Propionibacterium Acnes, Clindamycin-Resistant P. acnes, Staphylococcus epidermidis, and Streptococcus pyogenes
3.1.2. Staphylococcus aureus and Methicillin-Resistant Staphylococcus aureus (MRSA)
3.2. Fungi
3.2.1. Dermatophytes, Trichophyton mentagrophytes, and Trichophyton rubrum
3.2.2. Candida Albicans
3.2.3. Malassezia furfur
3.3. Viruses
Herpes Simplex Virus
4. Therapeutic Mechanisms of BV on Skin Diseases
5. Discussion
Funding
Conflicts of Interest
References
- Son, D.J.; Lee, J.W.; Lee, Y.H.; Song, H.S.; Lee, C.K.; Hong, J.T. Therapeutic application of anti-arthritis, pain-releasing, and anti-cancer effects of bee venom and its constituent compounds. Pharmacol. Ther. 2007, 115, 246–270. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.S.; Pittler, M.H.; Shin, B.C.; Kong, J.C.; Ernst, E. Bee venom acupuncture for musculoskeletal pain: A review. J. Pain 2008, 9, 289–297. [Google Scholar] [CrossRef] [PubMed]
- Han, C.H.; Lee, Y.S.; Sung, S.H.; Lee, B.H.; Shin, H.Y.; Lee, Y.J. Trend analysis of the research on bee venom acupuncture in south korea, based on published articles. J. Korean Med. 2015, 36, 80–103. [Google Scholar] [CrossRef]
- Lee, J.A.; Son, M.J.; Choi, J.; Jun, J.H.; Kim, J.I.; Lee, M.S. Bee venom acupuncture for rheumatoid arthritis: A systematic review of randomised clinical trials. BMJ Open 2014, 4, e006140. [Google Scholar] [CrossRef] [PubMed]
- Seo, B.K.; Lee, J.H.; Sung, W.S.; Song, E.M.; Jo, D.J. Bee venom acupuncture for the treatment of chronic low back pain: Study protocol for a randomized, double-blinded, sham-controlled trial. Trials 2013, 14, 16. [Google Scholar] [CrossRef] [PubMed]
- Nitecka-Buchta, A.; Buchta, P.; Tabenska-Bosakowska, E.; Walczynska-Dragon, K.; Baron, S. Myorelaxant effect of bee venom topical skin application in patients with rdc/tmd ia and rdc/tmd ib: A randomized, double blinded study. Biomed. Res. Int. 2014, 2014, 296053. [Google Scholar] [CrossRef] [PubMed]
- Hwang, D.S.; Kim, S.K.; Bae, H. Therapeutic effects of bee venom on immunological and neurological diseases. Toxins 2015, 7, 2413–2421. [Google Scholar] [CrossRef]
- Yang, E.J.; Jiang, J.H.; Lee, S.M.; Yang, S.C.; Hwang, H.S.; Lee, M.S.; Choi, S.M. Bee venom attenuates neuroinflammatory events and extends survival in amyotrophic lateral sclerosis models. J. Neuroinflamm. 2010, 7, 69. [Google Scholar] [CrossRef]
- Gu, H.; An, H.J.; Kim, J.Y.; Kim, W.H.; Gwon, M.G.; Kim, H.J.; Han, S.M.; Park, I.; Park, S.C.; Leem, J.; et al. Bee venom attenuates porphyromonas gingivalis and rankl-induced bone resorption with osteoclastogenic differentiation. Food Chem. Toxicol. 2019, 129, 344–353. [Google Scholar] [CrossRef]
- Zhang, S.; Liu, Y.; Ye, Y.; Wang, X.R.; Lin, L.T.; Xiao, L.Y.; Zhou, P.; Shi, G.X.; Liu, C.Z. Bee venom therapy: Potential mechanisms and therapeutic applications. Toxicon 2018, 148, 64–73. [Google Scholar] [CrossRef]
- Zolfagharian, H.; Mohajeri, M.; Babaie, M. Bee venom (apis mellifera) an effective potential alternative to gentamicin for specific bacteria strains: Bee venom an effective potential for bacteria. J. Pharmacopunct. 2016, 19, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Uddin, M.B.; Lee, B.H.; Nikapitiya, C.; Kim, J.H.; Kim, T.H.; Lee, H.C.; Kim, C.G.; Lee, J.S.; Kim, C.J. Inhibitory effects of bee venom and its components against viruses in vitro and in vivo. J. Microbiol. 2016, 54, 853–866. [Google Scholar] [CrossRef] [PubMed]
- Han, S.M.; Kim, J.M.; Hong, I.P.; Woo, S.O.; Kim, S.G.; Jang, H.R.; Pak, S.C. Antibacterial activity and antibiotic-enhancing effects of honeybee venom against methicillin-resistant staphylococcus aureus. Molecules 2016, 21, 79. [Google Scholar] [CrossRef] [PubMed]
- Socarras, K.M.; Theophilus, P.A.S.; Torres, J.P.; Gupta, K.; Sapi, E. Antimicrobial activity of bee venom and melittin against borrelia burgdorferi. Antibiotics 2017, 6, 31. [Google Scholar] [CrossRef] [PubMed]
- Lyu, C.; Fang, F.; Li, B. Anti-tumor effects of melittin and its potential applications in clinic. Curr. Protein Pept. Sci. 2019, 20, 240–250. [Google Scholar] [CrossRef] [PubMed]
- Rady, I.; Siddiqui, I.A.; Rady, M.; Mukhtar, H. Melittin, a major peptide component of bee venom, and its conjugates in cancer therapy. Cancer Lett. 2017, 402, 16–31. [Google Scholar] [CrossRef]
- Memariani, H.; Memariani, M.; Shahidi-Dadras, M.; Nasiri, S.; Akhavan, M.M.; Moravvej, H. Melittin: From honeybees to superbugs. Appl. Microbiol. Biotechnol. 2019, 103, 3265–3276. [Google Scholar] [CrossRef] [PubMed]
- Jappe, U. Pathological mechanisms of acne with special emphasis on propionibacterium acnes and related therapy. Acta Derm. Venereol. 2003, 83, 241–248. [Google Scholar] [CrossRef]
- Toyoda, M.; Morohashi, M. Pathogenesis of acne. Med. Electron Microsc. 2001, 34, 29–40. [Google Scholar] [CrossRef]
- Ochsendorf, F. Systemic antibiotic therapy of acne vulgaris. J. Dtsch. Dermatol. Ges. 2006, 4, 828–841. [Google Scholar] [CrossRef]
- Eady, E.A. Bacterial resistance in acne. Dermatology 1998, 196, 59–66. [Google Scholar] [CrossRef] [PubMed]
- Eady, E.A.; Cove, J.H.; Holland, K.T.; Cunliffe, W.J. Erythromycin resistant propionibacteria in antibiotic treated acne patients: Association with therapeutic failure. Br. J. Dermatol. 1989, 121, 51–57. [Google Scholar] [CrossRef]
- Tan, H.H. Antibacterial therapy for acne: A guide to selection and use of systemic agents. Am. J. Clin. Dermatol. 2003, 4, 307–314. [Google Scholar] [CrossRef]
- Han, S.M.; Lee, K.G.; Pak, S.C. Effects of cosmetics containing purified honeybee (apis mellifera l.) venom on acne vulgaris. J. Integr. Med. 2013, 11, 320–326. [Google Scholar] [CrossRef] [PubMed]
- Han, S.M.; Pak, S.C.; Nicholls, Y.M.; Macfarlane, N. Evaluation of anti-acne property of purified bee venom serum in humans. J. Cosmet. Dermatol. 2016, 15, 324–329. [Google Scholar] [CrossRef] [PubMed]
- Leyden, J.J.; McGinley, K.J.; Mills, O.H.; Kligman, A.M. Propionibacterium levels in patients with and without acne vulgaris. J. Investig. Dermatol. 1975, 65, 382–384. [Google Scholar] [CrossRef] [PubMed]
- Vowels, B.R.; Yang, S.; Leyden, J.J. Induction of proinflammatory cytokines by a soluble factor of propionibacterium acnes: Implications for chronic inflammatory acne. Infect. Immun. 1995, 63, 3158–3165. [Google Scholar] [PubMed]
- An, H.J.; Lee, W.R.; Kim, K.H.; Kim, J.Y.; Lee, S.J.; Han, S.M.; Lee, K.G.; Lee, C.K.; Park, K.K. Inhibitory effects of bee venom on propionibacterium acnes-induced inflammatory skin disease in an animal model. Int. J. Mol. Med. 2014, 34, 1341–1348. [Google Scholar] [CrossRef] [PubMed]
- Raghuraman, H.; Chattopadhyay, A. Melittin: A membrane-active peptide with diverse functions. Biosci. Rep. 2007, 27, 189–223. [Google Scholar] [CrossRef]
- Lee, G.; Bae, H. Anti-inflammatory applications of melittin, a major component of bee venom: Detailed mechanism of action and adverse effects. Molecules 2016, 21, 616. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.R.; Kim, K.H.; An, H.J.; Kim, J.Y.; Chang, Y.C.; Chung, H.; Park, Y.Y.; Lee, M.L.; Park, K.K. The protective effects of melittin on propionibacterium acnes-induced inflammatory responses in vitro and in vivo. J. Investig. Dermatol. 2014, 134, 1922–1930. [Google Scholar] [CrossRef] [PubMed]
- Hari, A.; Flach, T.L.; Shi, Y.; Mydlarski, P.R. Toll-like receptors: Role in dermatological disease. Mediat. Inflamm. 2010, 2010, 16. [Google Scholar] [CrossRef] [PubMed]
- Han, S.; Lee, K.; Yeo, J.; Baek, H.; Park, K. Antibacterial and anti-inflammatory effects of honeybee (apis mellifera) venom against acne-inducing bacteria. J. Med. Plants Res. 2010, 4, 459–464. [Google Scholar]
- Huang, K.P.; Mullangi, S.; Guo, Y.; Qureshi, A.A. Autoimmune, atopic, and mental health comorbid conditions associated with alopecia areata in the united states. JAMA Dermatol. 2013, 149, 789–794. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Erdogan, S.; Hwang, D.; Hwang, S.; Han, E.H.; Lim, Y.H. Bee venom promotes hair growth in association with inhibiting 5alpha-reductase expression. Biol. Pharm. Bull. 2016, 39, 1060–1068. [Google Scholar] [CrossRef] [PubMed]
- Yim, E.; Nole, K.L.; Tosti, A. 5alpha-reductase inhibitors in androgenetic alopecia. Curr. Opin. Endocrinol. Diabetes Obes. 2014, 21, 493–498. [Google Scholar] [CrossRef]
- Amory, J.K.; Wang, C.; Swerdloff, R.S.; Anawalt, B.D.; Matsumoto, A.M.; Bremner, W.J.; Walker, S.E.; Haberer, L.J.; Clark, R.V. The effect of 5alpha-reductase inhibition with dutasteride and finasteride on semen parameters and serum hormones in healthy men. J. Clin. Endocrinol. Metab. 2007, 92, 1659–1665. [Google Scholar] [CrossRef] [PubMed]
- Traish, A.M.; Hassani, J.; Guay, A.T.; Zitzmann, M.; Hansen, M.L. Adverse side effects of 5alpha-reductase inhibitors therapy: Persistent diminished libido and erectile dysfunction and depression in a subset of patients. J. Sex. Med. 2011, 8, 872–884. [Google Scholar] [CrossRef]
- Cotsarelis, G.; Millar, S.E. Towards a molecular understanding of hair loss and its treatment. Trends Mol. Med. 2001, 7, 293–301. [Google Scholar] [CrossRef]
- Stough, D.; Stenn, K.; Haber, R.; Parsley, W.M.; Vogel, J.E.; Whiting, D.A.; Washenik, K. Psychological effect, pathophysiology, and management of androgenetic alopecia in men. Mayo Clin. Proc. 2005, 80, 1316–1322. [Google Scholar] [CrossRef]
- Lee, H.J.; Lee, S.H. Epidermal permeability barrier defects and barrier repair therapy in atopic dermatitis. Allergy Asthma Immunol. Res. 2014, 6, 276–287. [Google Scholar] [CrossRef] [PubMed]
- Leung, D.Y. Atopic dermatitis: New insights and opportunities for therapeutic intervention. J. Allergy Clin. Immunol. 2000, 105, 860–876. [Google Scholar] [CrossRef] [PubMed]
- Friedman, E.S.; LaNatra, N.; Stiller, M.J. Nsaids in dermatologic therapy: Review and preview. J. Cutan. Med. Surg. 2002, 6, 449–459. [Google Scholar] [CrossRef] [PubMed]
- Belvisi, M.G.; Hele, D.J. Soft steroids: A new approach to the treatment of inflammatory airways diseases. Pulm. Pharmacol. Ther. 2003, 16, 321–325. [Google Scholar] [CrossRef]
- Simons, F.E. The antiallergic effects of antihistamines (h1-receptor antagonists). J. Allergy Clin. Immunol. 1992, 90, 705–715. [Google Scholar] [CrossRef]
- Schafer-Korting, M.; Schmid, M.H.; Korting, H.C. Topical glucocorticoids with improved risk-benefit ratio. Rationale of a new concept. Drug Saf. 1996, 14, 375–385. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.H.; Lee, W.R.; An, H.J.; Kim, J.Y.; Chung, H.; Han, S.M.; Lee, M.L.; Lee, K.G.; Pak, S.C.; Park, K.K. Bee venom ameliorates compound 48/80-induced atopic dermatitis-related symptoms. Int. J. Clin. Exp. Pathol. 2013, 6, 2896–2903. [Google Scholar] [PubMed]
- Wakao, S.; Kuroda, Y.; Ogura, F.; Shigemoto, T.; Dezawa, M. Regenerative effects of mesenchymal stem cells: Contribution of muse cells, a novel pluripotent stem cell type that resides in mesenchymal cells. Cells 2012, 1, 1045–1060. [Google Scholar] [CrossRef]
- You, C.E.; Moon, S.H.; Lee, K.H.; Kim, K.H.; Park, C.W.; Seo, S.J.; Cho, S.H. Effects of emollient containing bee venom on atopic dermatitis: A double-blinded, randomized, base-controlled, multicenter study of 136 patients. Ann. Dermatol. 2016, 28, 593–599. [Google Scholar] [CrossRef]
- Gu, H.; Kim, W.H.; An, H.J.; Kim, J.Y.; Gwon, M.G.; Han, S.M.; Leem, J.; Park, K.K. Therapeutic effects of bee venom on experimental atopic dermatitis. Mol. Med. Rep. 2018, 18, 3711–3718. [Google Scholar] [CrossRef]
- Kim, Y.; Lee, Y.-W.; Kim, H.; Chung, D.K. Bee venom alleviates atopic dermatitis symptoms through the upregulation of decay-accelerating factor (daf/cd55). Toxins 2019, 11, 239. [Google Scholar] [CrossRef]
- Leung, D.Y.; Hanifin, J.M.; Charlesworth, E.N.; Li, J.T.; Bernstein, I.L.; Berger, W.E.; Blessing-Moore, J.; Fineman, S.; Lee, F.E.; Nicklas, R.A.; et al. Disease management of atopic dermatitis: A practice parameter. Ann. Allergy Asthma Immunol. 1997, 79, 197–211. [Google Scholar]
- Sur, B.; Lee, B.; Yeom, M.; Hong, J.H.; Kwon, S.; Kim, S.T.; Lee, H.S.; Park, H.J.; Lee, H.; Hahm, D.H. Bee venom acupuncture alleviates trimellitic anhydride-induced atopic dermatitis-like skin lesions in mice. BMC Complement. Altern. Med. 2016, 16, 38. [Google Scholar] [CrossRef]
- An, H.J.; Kim, J.Y.; Kim, W.H.; Gwon, M.G.; Gu, H.M.; Jeon, M.J.; Han, S.M.; Pak, S.C.; Lee, C.K.; Park, I.S.; et al. Therapeutic effects of bee venom and its major component, melittin, on atopic dermatitis in vivo and in vitro. Br. J. Pharmacol. 2018, 175, 4310–4324. [Google Scholar] [CrossRef]
- Kim, W.H.; An, H.J.; Kim, J.Y.; Gwon, M.G.; Gu, H.; Jeon, M.; Sung, W.J.; Han, S.M.; Pak, S.C.; Kim, M.K.; et al. Beneficial effects of melittin on ovalbumin-induced atopic dermatitis in mouse. Sci. Rep. 2017, 7, 17679. [Google Scholar] [CrossRef]
- Dennis, E.A.; Rhee, S.G.; Billah, M.M.; Hannun, Y.A. Role of phospholipase in generating lipid second messengers in signal transduction. FASEB J. 1991, 5, 2068–2077. [Google Scholar] [CrossRef]
- Mukherjee, A.B.; Miele, L.; Pattabiraman, N. Phospholipase A2 enzymes: Regulation and physiological role. Biochem. Pharmacol. 1994, 48, 1–10. [Google Scholar] [CrossRef]
- Jung, K.H.; Baek, H.; Kang, M.; Kim, N.; Lee, S.Y.; Bae, H. Bee venom phospholipase a2 ameliorates house dust mite extract induced atopic dermatitis like skin lesions in mice. Toxins 2017, 9, 68. [Google Scholar] [CrossRef]
- Amano, W.; Nakajima, S.; Kunugi, H.; Numata, Y.; Kitoh, A.; Egawa, G.; Dainichi, T.; Honda, T.; Otsuka, A.; Kimoto, Y.; et al. The janus kinase inhibitor jte-052 improves skin barrier function through suppressing signal transducer and activator of transcription 3 signaling. J. Allergy Clin. Immunol. 2015, 136, 667–677. [Google Scholar] [CrossRef]
- Tu, W.C.; Wu, C.C.; Hsieh, H.L.; Chen, C.Y.; Hsu, S.L. Honeybee venom induces calcium-dependent but caspase-independent apoptotic cell death in human melanoma a2058 cells. Toxicon 2008, 52, 318–329. [Google Scholar] [CrossRef]
- Soman, N.R.; Baldwin, S.L.; Hu, G.; Marsh, J.N.; Lanza, G.M.; Heuser, J.E.; Arbeit, J.M.; Wickline, S.A.; Schlesinger, P.H. Molecularly targeted nanocarriers deliver the cytolytic peptide melittin specifically to tumor cells in mice, reducing tumor growth. J. Clin. Investig. 2009, 119, 2830–2842. [Google Scholar] [CrossRef]
- Shai, Y. Mechanism of the binding, insertion and destabilization of phospholipid bilayer membranes by alpha-helical antimicrobial and cell non-selective membrane-lytic peptides. Biochim. Biophys. Acta 1999, 1462, 55–70. [Google Scholar] [CrossRef]
- Fett, N.M. Morphea (localized scleroderma). JAMA Dermatol. 2013, 149, 1124. [Google Scholar] [CrossRef]
- Hwang, J.H.; Kim, K.H. Bee venom acupuncture for circumscribed morphea in a patient with systemic sclerosis: A case report. Medicine 2018, 97, e13404. [Google Scholar] [CrossRef]
- Jones, S.A.; McArdle, F.; Jack, C.I.; Jackson, M.J. Effect of antioxidant supplementation on the adaptive response of human skin fibroblasts to uv-induced oxidative stress. Redox Rep. 1999, 4, 291–299. [Google Scholar] [CrossRef]
- Katiyar, S.K.; Bergamo, B.M.; Vyalil, P.K.; Elmets, C.A. Green tea polyphenols: DNA photodamage and photoimmunology. J. Photochem. Photobiol. B 2001, 65, 109–114. [Google Scholar] [CrossRef]
- Han, S.; Lee, K.; Yeo, J.; Kweon, H.; Woo, S.; Lee, M.; Baek, H.; Park, K. Inhibitory effect of bee venom against ultraviolet b induced mmp-11 and mmp-3 in human dermal fibroblasts. J. Apic. Res. 2007, 46, 94–98. [Google Scholar] [CrossRef]
- Lee, H.; Bae, S.K.; Pyo, M.; Heo, Y.; Kim, C.G.; Kang, C.; Kim, E. Anti-wrinkle effect of pla2-free bee venom against uvb-irradiated human skin cells. J. Agric. Life Sci. 2015, 49, 125–135. [Google Scholar]
- Makrantonaki, E.; Zouboulis, C.C. Molecular mechanisms of skin aging: State of the art. Ann. N. Y. Acad. Sci. 2007, 1119, 40–50. [Google Scholar] [CrossRef]
- Schon, M.P.; Boehncke, W.H. Psoriasis. N. Engl. J. Med. 2005, 352, 1899–1912. [Google Scholar] [CrossRef]
- Hegazi, A.G.; Raboh, F.A.A.; Ramzy, N.E.; Shaaban, D.M.; Khader, D.Y. Bee venom and propolis as new treatment modality in patients with localized plaque psoriases. Int. Res. J. Med. Med. Sci. 2013, 1, 27–33. [Google Scholar]
- Mizutani, H.; Ohmoto, Y.; Mizutani, T.; Murata, M.; Shimizu, M. Role of increased production of monocytes TNF-α, IL-1β and IL-6 in psoriasis: Relation to focal infection, disease activity and responses to treatments. J. Dermatol. Sci. 1997, 14, 145–153. [Google Scholar] [CrossRef]
- Feldman, S. Advances in psoriasis treatment. Dermatol. Online J. 2000, 6, 4. [Google Scholar]
- Williams, I.R.; Kupper, T.S. Immunity at the surface: Homeostatic mechanisms of the skin immune system. Life Sci. 1996, 58, 1485–1507. [Google Scholar] [CrossRef]
- Eltaher, S.; Mohammed, G.F.; Younes, S.; Elakhras, A. Efficacy of the apitherapy in the treatment of recalcitrant localized plaque psoriasis and evaluation of tumor necrosis factor-alpha (tnf-alpha) serum level: A double-blind randomized clinical trial. J. Dermatol. Treat. 2015, 26, 335–339. [Google Scholar] [CrossRef]
- Coenen, J. Late results of a triple-layer artificial skin. In Proceedings of the European Burn Association 5th Congres, Brighton, UK, 20–23 September 1993. [Google Scholar]
- Rothe, M.; Falanga, V. Growth factors: Their biology and promise in dermatologic diseases and tissue repair. JAMA Dermatol. 1989, 125, 1390–1398. [Google Scholar] [CrossRef]
- Singer, A.J.; Clark, R.A. Cutaneous wound healing. N. Engl. J. Med. 1999, 341, 738–746. [Google Scholar] [CrossRef]
- Han, S.; Lee, K.; Yeo, J.; Kim, W.; Park, K. Biological effects of treatment of an animal skin wound with honeybee (apis mellifera. L) venom. J. Plast. Reconstr. Aesthet. Surg. 2011, 64, e67–e72. [Google Scholar] [CrossRef]
- Galkowska, H.; Wojewodzka, U.; Olszewski, W.L. Chemokines, cytokines, and growth factors in keratinocytes and dermal endothelial cells in the margin of chronic diabetic foot ulcers. Wound Repair Regen 2006, 14, 558–565. [Google Scholar] [CrossRef]
- Goren, I.; Muller, E.; Pfeilschifter, J.; Frank, S. Severely impaired insulin signaling in chronic wounds of diabetic ob/ob mice: A potential role of tumor necrosis factor-alpha. Am. J. Pathol. 2006, 168, 765–777. [Google Scholar] [CrossRef]
- Hozzein, W.N.; Badr, G.; Badr, B.M.; Allam, A.; Ghamdi, A.A.; Al-Wadaan, M.A.; Al-Waili, N.S. Bee venom improves diabetic wound healing by protecting functional macrophages from apoptosis and enhancing nrf2, ang-1 and tie-2 signaling. Mol. Immunol. 2018, 103, 322–335. [Google Scholar] [CrossRef]
- Han, S.M.; Lee, K.G.; Park, K.K.; Pak, S.C. Skin sensitization study of bee venom (Apis mellifera L.) in guinea pigs and rats. Cutan. Ocul. Toxicol. 2013, 32, 27–30. [Google Scholar] [CrossRef]
- Han, S.M.; Hong, I.P.; Woo, S.O.; Chun, S.N.; Park, K.K.; Nicholls, Y.M.; Pak, S.C. The beneficial effects of honeybee-venom serum on facial wrinkles in humans. Clin. Interv. Aging 2015, 10, 1587–1592. [Google Scholar] [CrossRef]
- Lan, C.C.; Chen, G.S.; Chiou, M.H.; Wu, C.S.; Chang, C.H.; Yu, H.S. Fk506 promotes melanocyte and melanoblast growth and creates a favourable milieu for cell migration via keratinocytes: Possible mechanisms of how tacrolimus ointment induces repigmentation in patients with vitiligo. Br. J. Dermatol. 2005, 153, 498–505. [Google Scholar] [CrossRef]
- Scott, G.A.; Jacobs, S.E.; Pentland, A.P. Spla2-x stimulates cutaneous melanocyte dendricity and pigmentation through a lysophosphatidylcholine-dependent mechanism. J. Investig. Dermatol. 2006, 126, 855–861. [Google Scholar] [CrossRef]
- Maeda, K.; Tomita, Y.; Naganuma, M.; Tagami, H. Phospholipases induce melanogenesis in organ-cultured skin. Photochem. Photobiol. 1996, 64, 220–223. [Google Scholar] [CrossRef]
- Maeda, K.; Naganuma, M. Melanocyte-stimulating properties of secretory phospholipase A2. Photochem. Photobiol. 1997, 65, 145–149. [Google Scholar] [CrossRef]
- Jeon, S.; Kim, N.H.; Koo, B.S.; Lee, H.J.; Lee, A.Y. Bee venom stimulates human melanocyte proliferation, melanogenesis, dendricity and migration. Exp. Mol. Med. 2007, 39, 603–613. [Google Scholar] [CrossRef]
- Chomnawang, M.T.; Surassmo, S.; Nukoolkarn, V.S.; Gritsanapan, W. Antimicrobial effects of thai medicinal plants against acne-inducing bacteria. J. Ethnopharmacol. 2005, 101, 330–333. [Google Scholar] [CrossRef]
- Nakatsuji, T.; Kao, M.C.; Fang, J.Y.; Zouboulis, C.C.; Zhang, L.; Gallo, R.L.; Huang, C.M. Antimicrobial property of lauric acid against propionibacterium acnes: Its therapeutic potential for inflammatory acne vulgaris. J. Investig. Dermatol. 2009, 129, 2480–2488. [Google Scholar] [CrossRef]
- Leyden, J.J.; Del Rosso, J.Q.; Webster, G.F. Clinical considerations in the treatment of acne vulgaris and other inflammatory skin disorders: A status report. Dermatol. Clin. 2009, 27, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Bojar, R.A.; Holland, K.T. Acne and propionibacterium acnes. Clin. Dermatol. 2004, 22, 375–379. [Google Scholar] [CrossRef] [PubMed]
- Lebwohl, M.G.; Heymann, W.R.; Berth-Jones, J.; Coulson, I. Impetigo. In Treatment of Skin Disease E-Book: Comprehensive Therapeutic Strategies, 4th ed.; Elsevier Health Sciences: Amsterdam, The Netherlands, 2013; p. 332. [Google Scholar]
- Lebwohl, M.G.; Heymann, W.R.; Berth-Jones, J.; Coulson, I. Paronychia. In Treatment of Skin Disease E-Book: Comprehensive Therapeutic Strategies, 4th ed.; Elsevier Health Sciences: Amsterdam, The Netherlands, 2013; p. 542. [Google Scholar]
- Lebwohl, M.G.; Heymann, W.R.; Berth-Jones, J.; Coulson, I. Staphylococcal Scalded Skin Syndrome. In Treatment of Skin Disease E-Book: Comprehensive Therapeutic Strategies, 4th ed.; Elsevier Health Sciences: Amsterdam, The Netherlands, 2013; p. 723. [Google Scholar]
- Taylor, A.R. Methicillin-resistant staphylococcus aureus infections. Prim. Care Clin. Off. Pract. 2013, 40, 637–654. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.H.; Jang, A.Y.; Lin, S.; Lim, S.; Kim, D.; Park, K.; Han, S.-M.; Yeo, J.-H.; Seo, H.S. Melittin, a honeybee venom-derived antimicrobial peptide, may target methicillin-resistant staphylococcus aureus. Mol. Med. Rep. 2015, 12, 6483–6490. [Google Scholar] [CrossRef] [PubMed]
- Lebwohl, M.G.; Heymann, W.R.; Berth-Jones, J.; Coulson, I. Tinea Pedis and Skin Dermatophytosis. In Treatment of Skin Disease E-Book: Comprehensive Therapeutic Strategies, 4th ed.; Elsevier Health Sciences: Amsterdam, The Netherlands, 2013; p. 756. [Google Scholar]
- Yu, A.R.; Kim, J.J.; Park, G.S.; Oh, S.M.; Han, C.S.; Lee, M.Y. Biochemistry: The antifungal activity of bee venom against dermatophytes. J. Appl. Biol. Chem. 2012, 55, 7–11. [Google Scholar] [CrossRef]
- Park, J.; Kwon, O.; An, H.J.; Park, K.K. Antifungal effects of bee venom components on trichophyton rubrum: A novel approach of bee venom study for possible emerging antifungal agent. Ann. Dermatol. 2018, 30, 202–210. [Google Scholar] [CrossRef] [PubMed]
- Lebwohl, M.G.; Heymann, W.R.; Berth-Jones, J.; Coulson, I. Cutaneous Candidiasis and Chronic Mucocutaneous Candidasis. In Treatment of Skin Disease E-Book: Comprehensive Therapeutic Strategies, 4th ed.; Elsevier Health Sciences: Amsterdam, The Netherlands, 2013; p. 157. [Google Scholar]
- Lee, S.B. Antifungal activity of bee venom and sweet bee venom against clinically isolated candida albicans. J. Pharmacopunct. 2016, 19, 45–50. [Google Scholar] [CrossRef]
- Park, C.; Lee, D.G. Melittin induces apoptotic features in candida albicans. Biochem. Biophys. Res. Commun. 2010, 394, 170–172. [Google Scholar] [CrossRef]
- Prakash, S.; Bhargava, H. Apis cerana bee venom: It’s antidiabetic and anti-dandruff activity against malassezia furfur. World Appl. Sci. J. 2014, 32, 343–348. [Google Scholar]
- Lebwohl, M.G.; Heymann, W.R.; Berth-Jones, J.; Coulson, I. Herpes Labialis. In Treatment of Skin Disease E-Book: Comprehensive Therapeutic Strategies, 4th ed.; Elsevier Health Sciences: Amsterdam, The Netherlands, 2013; p. 308. [Google Scholar]
- Kim, J.-Y.; Lee, W.-R.; Kim, K.-H.; An, H.-J.; Chang, Y.-C.; Han, S.-M.; Park, Y.-Y.; Pak, S.C.; Park, K.-K. Effects of bee venom against propionibacterium acnes-induced inflammation in human keratinocytes and monocytes. Int. J. Mol. Med. 2015, 35, 1651–1656. [Google Scholar] [CrossRef]
- Park, J.H.; Yim, B.K.; Lee, J.H.; Lee, S.; Kim, T.H. Risk associated with bee venom therapy: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0126971. [Google Scholar] [CrossRef] [PubMed]
- Cavallucci, E.; Ramondo, S.; Renzetti, A.; Turi, M.C.; Di Claudio, F.; Braga, M.; Incorvaia, C.; Schiavone, C.; Ballone, E.; Di Gioacchino, M. Maintenance venom immunotherapy administered at a 3-month interval preserves safety and efficacy and improves adherence. J. Investig. Allergol. Clin. Immunol. 2010, 20, 63–68. [Google Scholar] [PubMed]
- Kim, J.-H.; Kim, M.-S.; Lee, J.-Y.; Yeom, S.-R.; Kwon, Y.-D.; Kim, D.-W. The case report of anaphylaxis after treated with bee-venom acupuncture. J. Korean Med. Rehabil. 2015, 25, 175–182. [Google Scholar] [CrossRef]
- Lee, S.-K.; Ye, Y.-M.; Park, H.-S.; Jang, G.C.; Jee, Y.-K.; Park, H.-K.; Koh, Y.-I.; Kim, J.-H.; Kim, C.-W.; Hur, G.-Y. Hymenoptera venom anaphylaxis in adult korean: A multicenter retrospective case study. Allergy Asthma Respir. Dis. 2014, 2, 344–351. [Google Scholar]
- Alam, M.; Ratner, D. Cutaneous squamous-cell carcinoma. N. Engl. J. Med. 2001, 344, 975–983. [Google Scholar] [CrossRef] [PubMed]
- Lomas, A.; Leonardi-Bee, J.; Bath-Hextall, F. A systematic review of worldwide incidence of nonmelanoma skin cancer. Br. J. Dermatol. 2012, 166, 1069–1080. [Google Scholar] [CrossRef]
- Grossman, D.; Leffell, D.J. The molecular basis of nonmelanoma skin cancer: New understanding. Arch. Dermatol. 1997, 133, 1263–1270. [Google Scholar] [CrossRef]
- Do, N.; Weindl, G.; Grohmann, L.; Salwiczek, M.; Koksch, B.; Korting, H.C.; Schafer-Korting, M. Cationic membrane-active peptides - anticancer and antifungal activity as well as penetration into human skin. Exp. Dermatol. 2014, 23, 326–331. [Google Scholar] [CrossRef]
| Disease | Model | Venom/Compound/(Bee Species) | Dose (Administration Method) | Results | Mechanism/Molecular Response | Reference |
|---|---|---|---|---|---|---|
| Acne | Human DB, RCT (n = 12) | Cosmetic containing BV (Apis melifera) | 0.06 mg/mL, Cosmetic 4 mL twice daily for 2 weeks (Applied to whole face) | Significant improvement of KAGS score (p < 0.01), 57.5% decrease of ATP level which indicate MO level (p < 0.01) | Not reported | [24] |
| Acne | Human (n = 30) | Serum containing BV (Apis melifera) | Not reported, Serum 0.7–0.9 g twice daily for 6 weeks (Applied to whole face) | Significant improvement (52.3%) of MCAGS score after 6 weeks (p < 0.001) Open and closed comedones were significantly decreased (p < 0.001). Significant decrease in papules (p < 0.05) | Not reported | [25] |
| Atopic dermatitis | Human DB, RCT (n = 114) | Emollient containing BV (Apis melifera) | Not reported, twice daily for 4 weeks (Applied to entire body) | Remarkable reduction of EASI score in comparison to control (p < 0.05). VAS score for pruritus was notably declined compared with control (p < 0.05). TEWL value were not notably different between two groups. | Not reported | [49] |
| Psoriasis | Human RLPP patients DB, RCT (n = 50) | BV (Apis melifera) | 0.05 mL/cm2 (intradermal injection around psoriatic lesion) | BV treatment group showed significant lower PGA scores against placebo group (p < 0.001). During the follow-up period of 6 months, psoriasis did not recur. | TNF-α was notably decreased compared to control (p < 0.05). | [75] |
| Psoriasis | Human patients with localized plaque psoriasis (n = 48) | BV (Apis melifera) | Starting with 0.01 µL, increasing 0.01 µL every injection untill arriving 1 µL (Intradermal, twice weekly) TP: topical propolis twice daily OP: oral propolis 1 g/day by capsule | PASI score was significantly decreased decreased after treatment (p < 0.01). Much more reduction than TP and OP. The highest reduction in (TP + OP + BV) group. | Serum IL-1β was significantly decreased after treatment (p < 0.05). Much more decrease than TP and OP.The highest decrease in (TP + OP + BV) group. | [71] |
| Scleroderma | A case report: 64-year-old Korean woman, White circular lesion on the right lateral iliac crest | BV (Apis melifera) | Dried BV 1 g dissolved in 10000cc water. Total volume under 0.2 mL. twice weekly (subcutaneous, along the margins of the lesion) | On a 11-point numeric scale (NRS 11), average score of itch declined from 8 to 4 and sleep disturbance from 6 to 2, respectively. On the fifth visit, patient stated that she no longer felt an itch and had no sleep disturbance due to itching. Three months later, the follow-up evaluation showed that the condition of the skin was close to normal skin. | Not reported | [64] |
| Wrinkle | Human, Double blind (n = 22) | Serum containing BV (Apis melifera) | BV 0.006% serum 4 mL twice daily for 12 weeks (Applied to whole face) | The average visual grade (SKWGS) of all patients with BV serum significantly improved (11.83% decrement) (p < 0.001). Total area, count and average depth of wrinkle were significantly decreased (p < 0.05). | Not reported | [84] |
| Disease | Model | Venom/Compound/(Bee Species)/ | Dose (Administration Method)/Control | Results | Mechanism/Molecular Response | Reference |
|---|---|---|---|---|---|---|
| Acne | 8-week ICR mice, P. acnes intradermally injected into both ears. (n = 30) | BV (Apis melifera) | 1 µg blended with 0.05 g Vaseline (topical, on the right ear) NC: P.acnes only PC: vaseline applied to left ear | Ear thickness was reduced three-fold after 24 h compared to NC (p < 0.05). Swelling, erythema and inflammatory reactions were reduced. | TLR2 and CD14 expression is significantly inhibited. DNA-binding activity of NF-κB and AP-1 is remarkably inhibited compared to NC and PC (p < 0.05). Inhibiting the NF- κB signaling pathways. | [28] |
| Acne | 8-week ICR mice, P. acnes intradermally injected into both ear. (n = 30) | Melittin (Apis melifera) | 100 µg blended with 0.05 g Vaseline (topical, on the right ear) NC: P.acnes only PC: vaseline applied to left ear | Ear thickness was reduced 1.3-fold after 24 h compared with NC (p < 0.05). Swelling and granulomatous response were markedly reduced. | Significant reduction of TNF-α, IL-1β, IL-8, IFN-γ compared with NC and PC (p < 0.05). DNA-binding activity of NF-κB and AP-1 is remarkably inhibited compared to NC and PC (p < 0.05). Melittin significantly reduced the phosphorylation of IKK, IκB and NF- κB. Inhibiting the NF- κB and MAPK signaling pathways. | [31] |
| Alopecia | 6-week female C57BL/6 mice, catagen phase induced on dorsal skin by dexamethasone. | BV (Apis melifera) | Three CONC: 0.001% 0.005% 0.01% 100 µL each Once daily for 19 day (Applied to dorsal skin) NC:dexamethasone only PC: minoxidil 2% 100 µL | Hair growth promoted notably in a dose-dependent manner at all doses. 0.01% BV resulted in the greatest increase in hair growth compared to PC (p < 0.05). | KGF expression is significantly increased compared with NC (p < 0.05). 5α-reductase significantly decreased compared with NC (p < 0.05). | [35] |
| Atopic dermatitis | DNCB induced atopic dermatitis in 7-week male Balb/c mice (n = 8) | BV (Apis melifera) | 0.3 mg/kg (subcutaneous) PBS | Dryness, hemorrhage, excoriation, edema and redness were almost completely restored. | Serum C3C and MAC were significantly decreased after BV injection compared to PBS injection (p < 0.001). Serum-secreted CD55 were significantly elevated compared with PBS injection (p < 0.001). BV increased CD55 production in THP-1 cells | [51] |
| Atopic dermatitis | OVA-induced atopic dermatitis in 6-week female Balb/c mice (n = 25) | BV (Apis melifera) | Three doses: 1 µg/Kg, 10 µg/Kg, 100 µg/Kg twice a week for 2 weeks (intraperitoneal) NC: untreated PC: OVA only | Bleeding, erythema, eczema, and dryness were significantly reduced. Dorsal skin thickness was remarkably reduced in a dose-dependent manner compared to PC (p < 0.05), the greatest decrease in BV 100 group. | Significant reduction of mast cell infiltration in BV 10 and 100 group compared with PC (p < 0.05). Serum IgE levels were reduced, the greatest decrease in BV 100 group. Significant reduction of TNF-α in BV 10 and 100 and TSLP in BV 100 group compared with PC (p < 0.05). | [50] |
| Atopic dermatitis | DNCB induced atopic dermatitis in 6-week female Balb/c mice (n = 45) | Melittin (Apis melifera) | Three doses: 100 µg, 200 µg, 500 µg blended with placebo (topical, to dorsal skin) Placebo only | Dorsal skin thickness was notably decreased in comparison to placebo group (p < 0.05) | Mast cell infiltration was significantly decreased compared with control (p < 0.05). Serum IFN-γ, IL-4, IgE and TSLP were markedly decreased in melittin 200 and 500 group compared to placebo group (p < 0.05). CD4+ and CD3+ were significantly decreased in melittin 500 (p < 0.05). | [54] |
| Atopic dermatitis | Chicken OVA-induced atopic dermatitis in 6-week female Balb/c mice (n = 25) | Melittin (Apis melifera) | Three CONC: 1 µg/Kg, 10 µg/Kg, 100 µg/Kg (intraperitoneal) NC: untreated PC: OVA only | Dorsal skin thickness was significantly reduced in comparison to PC (p < 0.05), the greatest decrease in BV 100 group. Edema, erythema and excoriation were improved in melittin group. | Melittin significantly improved OVA-induced filaggrin deficiency (p < 0.05). CD14 and CD11b were significantly decreased in melittin 100 group compared to PC (p < 0.05). Mast cell infiltration was remarkably decreased in melittin 10 and 100 group compared to PC (p < 0.05). Serum IL-1β, TNF-α was notably decreased in all dose compared to PC (p < 0.05). Serum TSLP was remarkably decreased in melittin 100 compared to PC (p < 0.05). Skin IL-13 mRNA was significantly declined in melittin 100 compared with PC (p < 0.05). | [55] |
| Atopic dermatitis | DFE/DNCB-induced atopic dermatitis in 7–8-week female Balb/c mice (n = 25) | PLA2 (Apis melifera) | Two doses: 16 ng/ear, 80 ng/ear (Applied to ear skin) NC: DFE/DNCB only PC :dexamethasone 50 µg /ear | Ear thickness was notably decreased in all doses compared to NC (p < 0.001), not more than PC. AD-like skin lesions were significantly suppressed by PLA2. | Th1 cytokines (TNF- α, IL-6 and IFN-) and Th2 cytokines (IL-4 and IL-13) were remarkably decreased in comparison to NC (p < 0.05), no more effective than PC. Epidermal hyperplasia and lymphocyte infiltration were significantly attenuated by PLA2 in a dose-dependent manner compared with control (p < 0.01–p < 0.05), no more effective than PC. PLA2 has the potential to counteract AD-like skin lesion-associated inflammation responses via the induction of Tregs. | [58] |
| Atopic dermatitis | Compound 48/80-induced atopic dermatitis in 6-week Balb/c mice (n = 32). | BV (Apis melifera) | Two doses: 0.01 mg/Kg 0.1 mg/Kg (intraperitoneal) PC: Compound 48/80 only | Scratching behavior caused by compound 48/80 was decreased by 75% and 87% compared with PC in BV 0.01 and 0.1 respectively. (p < 0.05) Vascular permeability of the skin was decreased by 33.3% and 70.7% compared with PC in BV 0.01 and 0.1 respectively. (p < 0.05) | Mast cell degranulation was remarkably decreased in a dose-dependent manner compared to PC (p < 0.05). TNF-α and IL-1β were significantly suppressed in skin tissue by BV treatment. BV inhibited activation of NF- κB, which was induced by compound 48/80. | [47] |
| Atopic dermatitis | Trimellitic anhydride -induced atopic dermatitis on ear skin in 10-week male Balb/c mice (n = 50). | BV (Apis melifera) | 0.3 mg/Kg, Once daily for 14 day (subcutaneous, acupuncture bilateral point BL40) NC: TMA treated PC: prednisone BVNA: BV at non acupoint; base of tail | BV at BL40 acupoint significantly relieved the AD symptoms. Thickness of ear and weight of lymph node were remarkably decreased compared to NC (p < 0.001). All results not better than PC but similar to BVNA indicated no healing effect on AD-like symptoms. | Serum IL-4 and IgE was notably declined compared to NC (p < 0.001). Number of CD4 and CD8 positive cells was notably declined in comparison to NC (p < 0.01). TNF-α, IFN-γ, IL-2, IL-4, IL-10 and IL-12 concentration in auricular lymph node were remarkably decreased compared to NC (p < 0.001–p < 0.05). | [53] |
| Melanoma | B16F10 murine melanoma was implanted subcutaneously in C57BL/6 mice (n = 15) | Melittin (Apis melifera) | 8.5 mg/Kg, 4 injections every other day starting at day 5 (intravenous, Melittin is loaded on molecularly targeted nanoparticles.) S: saline only N: nanoparticle only | Tumor weight was significantly decreased on day 14 compared with S (~88% reduction) and N (~87% reduction) (p < 0.01). Decrease in the number of blood vessels in proliferating cells, and significant areas of necrosis in melittin-treated-tumor. | Melittin-loaded nanoparticles cause apoptosis of cancer cell via release of cytochrome c from mitochondria. | [61] |
| Wound (Diabetic wound) | Diabetic 12-week male Balb/c mice wounded on back (n = 45) | BV (Apis melifera) | 200 µg/kg for 15 day (subcutaneous, on wound area) NC: wound on non-diabetic mice PC: diabetic mice without BV treatment | Degree of wound closure was similar to NC, markedly higher than PC (p < 0.05). | Type I collagen expression was significantly recovered in BV-treated diabetic mice compared with PC (p < 0.05), lower than NC. Ang-1, Nrf2, p-Tyr, p-eNOS, p-AKT, p-ERK, CD31, CCL2, CCL3, CXCL2 and β-Defensin-2 expression were significantly recovered in BV-treated diabetic mice compared with PC (p < 0.05). | [82] |
| Wound | 7-week male HR-1 mice wounded on back (n = 30) | BV (Apis melifera) | 1 µg/gauze (Wound was covered with an equal size of gauze treated with BV for 7 day) NC: untreatedPC: treated with Vaseline | Dramatic decrease of wound size was observed in BV group compared to NC and PC (p < 0.05). | Type 1 collagen was remarkably elevated in BV group in comparison to NC and Vaseline. TGF-b1 and fibronectin were significantly decreased in BV group in comparison to control and Vaseline. VEGF was remarkably declined in BV and PC compared to NC (p < 0.05). | [79] |
| Disease | Model | Venom/Compound/(Bee Species) | Dose | Results | Mechanism/Molecular Response | Reference |
|---|---|---|---|---|---|---|
| Acne | THP-1 cell dealt with heat-killed P. acnes | BV (Apis melifera) | Three CONC: 0.1 µg/mL, 1 µg/mL, 5 µg/mL for 48 h | Significant reduction of TNF-α, IL-8 in a concentration-dependent manner (p < 0.05). Lowest TNF-α at 5 µg/mL Lowest IL-8 at 1 µg/mL | Not reported | [32] |
| Acne | THP-1 cell dealt with heat-killed P. acnes | BV (Apis melifera) | Three CONC: 1 ng/mL, 10 ng/mL, 100 ng/mL for 8 h | Significant reduction of TNF-α, IL-8, IFN-γ at all doses compared to control (p < 0.05). Reduced in dose dependent manner. | TLR2 expression significantly suppressed | [107] |
| Acne | THP-1 cell treated with heat-killed P. acnes | Melittin (Apis melifera) | Three CONC: 0.1 ng/mL, 0.5 ng/mL, 1 ng/mL. for 8 h | Significant reduction of TNF-α, IL-8 at all doses compared to control (p < 0.05). Reduced in dose-dependent manner. | Melittin significantly reduced the phosphorylation of IKK, IκB and NF- κB. Inhibiting the NF- κB signaling pathways. | [107] |
| Acne | HaCat cell treated with heat-killed P. acnes | BV (Apis melifera) | Three CONC: 1 ng/mL, 10 ng/mL, 100 ng/mL for 8 h | Significant reduction of TNF-α, IL-8, IFN-γ at 10, 100 ng/mL in comparison to control (p < 0.05). Reduced in dose-dependent manner. | TLR2 expression significantly suppressed | [107] |
| Acne | HaCat cell dealt with heat-killed P. acnes | Melittin (Apis melifera) | 1 µg/mL | Significant reduction of TNF-α, IL-1β, IL-8, IFN-γ compared with control (p < 0.05). | TLR2 and 4 expression significantly decreased. Melittin significantly reduced the phosphorylation of IKK, IκB, NF- κB and p-38. Inhibiting the NF-κB and MAPK signaling pathways. | [31] |
| Alopecia | hDPC treated with 0.1% dexamethasone | BV (Apis melifera) | Three CONC: 100 ng/mL, 200 ng/mL, 500 ng/mL for 24 h | Significant increase of FGF-2, FGF-7, IGF-1R and VEGF compared with DEX only. (p < 0.001–p < 0.05). Protein-level of VEGF is increased 1.95-, 2.95-, 2.08 and 1.47-fold with 100, 200, 500 ng/mL BV and 2% minoxidil respectively. | Not reported | [35] |
| Atopic dermatitis | Hacat cell treated with TNF-α and IFN-γ | Melittin (Apis melifera) | Three CONC: 0.1 µg/mL, 0.5 µg/mL, 1 µg/mL. | IL-1β, IL-6 and IFN-γ were decreased in a dose-dependent manner. mRNA of CCL17 and CCL22 were significantly decreased in a dose-dependent manner in melitin 0.5 and 1 in comparison to control (p < 0.05). pJAK2, pSTAT1 and pSTAT3 expression was decreased in melittin 1 µg/mL | NF- κB DNA-binding activity was markedly reduced. | [54] |
| Atopic dermatitis | Hacat cell treated by 50 ng/mL of IL-4 and IL-13 | Melittin (Apis melifera) | Three CONC: 0.1 µg/mL, 0.5 µg/mL, 1 µg/mL. for 24 h | Filaggrin expression was remarkably elevated in a dose-dependent manner in all doses compared to control (p < 0.05) pSTAT3 expression was significantly decreased in melittin 1 µg/mL | Not reported | [55] |
| Melanoma | Human melanoma A2058 cells | BV (Apis melifera) | 4 µg/mL | Application of 4 mg/mL BV for 2 h resulted in the death of approximately 80% of A2058 cells. | BV generated reactive oxygen species (ROS) and altered mitochondrial membrane potential transition. BV causes apoptosis in AIF/EndoG-dependent but caspase-independent manner. BV interfered with AKT and MAPK family kinase activation. BV treatment significantly reduced phosphorylated AKT and p38 BV made ER and extracellular Ca2+ drift to the cytosol. | [60] |
| Photoaging | HDF cell irradiated by UVB (312 nm) | PLA2-free BV(PBV) and BV (Apis melifera) | PBV: 1.5 µg/mL, 3.0 µg/mL, BV 1.5 µg/mL, 3.0 µg/mL | Both PBV and BV significantly restored Type 1 procollagen synthesis in UVB-irradiated HDF cells except for BV 3 μg/mL (p < 0.05). Type 1 collagen significantly increased in both BV, PBV compared with control (p < 0.05). (Degree: 3.0 BV > 1.5 BV > 3.0 PBV > 1.5 PBV) | PBV and BV treatments significantly attenuated the MMP-1, 2 and 3 expressions (p < 0.05). Both PBV and BV significantly inhibited the UVB-stimulated phosphorylations of ERK1/2 and p38 (p < 0.05). | [68] |
| Photoaging | Hacat cell irradiated by UVB (312 nm) | PLA2-free BV(PBV) and BV (Apis melifera) | PBV: 1.5 µg/mL, 3.0 µg/mL, BV: 1.5 µg/mL, 3.0 µg/mL. | PBV and BV treatments significantly attenuated the MMP-1, 13 expressions (p < 0.05). Both PBV and BV significantly inhibited the UVB-stimulated phosphorylations of ERK1/2 and p38 (p < 0.05). | [68] | |
| Photoaging | HDF cell irradiated by UVB (280–350 nm) | BV (Apis melifera) | Three CONC: 0.01 µg/mL, 0.1 µg/mL, 1 µg/mL for 24 h | BV significantly decreased MMP-1 expressions by 50–80% while MMP-3 expression by 50–85% compared to controls (p < 0.05). The biggest MMP-1 and MMP-3 inhibitions were observed at a 0.1 µg/mL. | Not reported | [67] |
| Vitiligo | Human epidermal melanocyte | BV (Apis melifera) | 10 µg/mL | Melanocyte proliferation and melanin content were remarkably increased compared to control (p < 0.05), similar to melanocyte treated with 10 µM forskolin but no more than. | Forskolin increased the cAMP level 40-fold, but BV only tripled. Based on this, the cAMP level does not appear to be the deciding factor | [89] |
| Disease | Type of Study | Venom/Compound/(Bee Species) | Adverse Effect (Severity) | Reference |
|---|---|---|---|---|
| Atopic dermatitis | Clinical | Emollient containing BV (Apis melifera) | Irritation, pruritus, erythema, urticaria and disease exacerbation (mild). No significant differences in the incidence compared with control. | [49] |
| Psoriasis | Clinical | BV (Apis melifera) | Mild pain, redness and swelling at the site of apitheraphy injection | [75] |
| Psoriasis | Clinical | BV (Apis melifera) | 4patients experienced itching but not significant. No systemic adverse effect. | [71] |
| Scleroderma | Clinical | BV (Apis melifera) | Slight itchiness at the location of inoculation for 1 half-day. | [64] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, H.; Park, S.-Y.; Lee, G. Potential Therapeutic Applications of Bee Venom on Skin Disease and Its Mechanisms: A Literature Review. Toxins 2019, 11, 374. https://doi.org/10.3390/toxins11070374
Kim H, Park S-Y, Lee G. Potential Therapeutic Applications of Bee Venom on Skin Disease and Its Mechanisms: A Literature Review. Toxins. 2019; 11(7):374. https://doi.org/10.3390/toxins11070374
Chicago/Turabian StyleKim, Haejoong, Soo-Yeon Park, and Gihyun Lee. 2019. "Potential Therapeutic Applications of Bee Venom on Skin Disease and Its Mechanisms: A Literature Review" Toxins 11, no. 7: 374. https://doi.org/10.3390/toxins11070374
APA StyleKim, H., Park, S.-Y., & Lee, G. (2019). Potential Therapeutic Applications of Bee Venom on Skin Disease and Its Mechanisms: A Literature Review. Toxins, 11(7), 374. https://doi.org/10.3390/toxins11070374





