Effects of Cinnamon Consumption on Glycemic Indicators, Advanced Glycation End Products, and Antioxidant Status in Type 2 Diabetic Patients
Abstract
:1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Ethical Issues
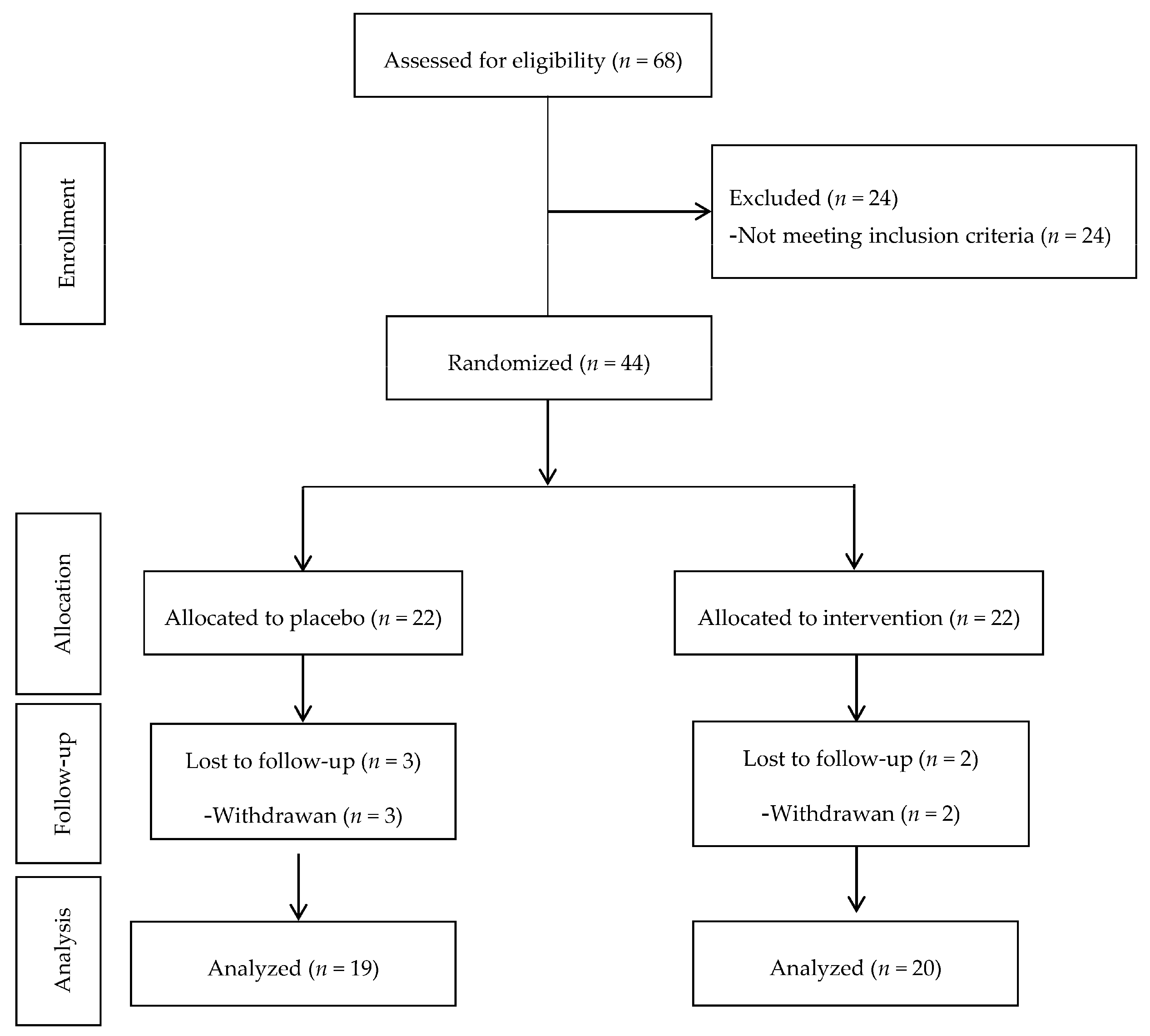
2.3. Study Design
2.4. Lifestyle and Anthropometric Assessment
2.5. Clinical and Biological Measurements
2.6. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Guariguata, L.; Whiting, D.R.; Hambleton, I.; Beagley, J.; Linnenkamp, U.; Shaw, J.E. Global estimates of diabetes prevalence for 2013 and projections for 2035. Diabetes Res. Clin. Pract. 2014, 103, 137–149. [Google Scholar] [CrossRef] [PubMed]
- Shaw, J.E.; Sicree, R.A.; Zimmet, P.Z. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res. Clin. Pract. 2010, 87, 4–14. [Google Scholar] [CrossRef] [PubMed]
- Hossain, P.; Kawar, B.; El Nahas, M. Obesity and diabetes in the developing world—A growing challenge. N. Engl. J. Med. 2007, 356, 213–215. [Google Scholar] [CrossRef] [PubMed]
- Esteghamati, A.; Gouya, M.M.; Abbasi, M.; Delavari, A.; Alikhani, S.; Alaedini, F.; Safaie, A.; Forouzanfar, M.; Gregg, E.W. Prevalence of diabetes and impaired fasting glucose in the adult population of Iran: National survey of risk factors for non-communicable diseases of Iran. Diabetes Care 2008, 31, 96–98. [Google Scholar] [CrossRef] [PubMed]
- Lillioja, S.; Mott, D.M.; Spraul, M.; Ferraro, R.; Foley, J.E.; Ravussin, E.; Knowler, W.C.; Bennett, P.H.; Bogardus, C. Insulin resistance and insulin secretory dysfunction as precursors of non-insulin-dependent diabetes mellitus. Prospective studies of pima Indians. N. Engl. J. Med. 1993, 329, 1988–1992. [Google Scholar] [CrossRef] [PubMed]
- Bohl, M.; Bjornshave, A.; Larsen, M.K.; Gregersen, S.; Hermansen, K. The effects of proteins and medium-chain fatty acids from milk on body composition, insulin sensitivity and blood pressure in abdominally obese adults. Eur. J. Clin. Nutr. 2017, 71, 76–82. [Google Scholar] [CrossRef] [PubMed]
- Pastors, J.G.; Warshaw, H.; Daly, A.; Franz, M.; Kulkarni, K. The evidence for the effectiveness of medical nutrition therapy in diabetes management. Diabetes Care 2002, 25, 608–613. [Google Scholar] [CrossRef] [PubMed]
- Pastors, J.G. Medications or lifestyle change with medical nutrition therapy. Curr. Diabetes Rep. 2003, 3, 386–391. [Google Scholar] [CrossRef]
- Yeh, G.Y.; Eisenberg, D.M.; Kaptchuk, T.J.; Phillips, R.S. Systematic review of herbs and dietary supplements for glycemic control in diabetes. Diabetes Care 2003, 26, 1277–1294. [Google Scholar] [CrossRef] [PubMed]
- Anderson, R.A.; Broadhurst, C.L.; Polansky, M.M.; Schmidt, W.F.; Khan, A.; Flanagan, V.P.; Schoene, N.W.; Graves, D.J. Isolation and characterization of polyphenol type-a polymers from cinnamon with insulin-like biological activity. J. Agric. Food Chem. 2004, 52, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Ebadi, M. Pharmacodynamic Basis of Herbal Medicine, 1st ed.; CRC Press: Boca Raton, FL, USA, 2006. [Google Scholar]
- Cao, H.; Polansky, M.M.; Anderson, R.A. Cinnamon extract and polyphenols affect the expression of tristetraprolin, insulin receptor, and glucose transporter 4 in mouse 3t3-l1 adipocytes. Arch. Biochem. Biophys. 2007, 459, 214–222. [Google Scholar] [CrossRef] [PubMed]
- Allen, R.W.; Schwartzman, E.; Baker, W.L.; Coleman, C.I.; Phung, O.J. Cinnamon use in type 2 diabetes: An updated systematic review and meta-analysis. Ann. Fam. Med. 2013, 11, 452–459. [Google Scholar] [CrossRef] [PubMed]
- Crawford, P. Effectiveness of cinnamon for lowering hemoglobin a1c in patients with type 2 diabetes: A randomized, controlled trial. J. Am. Board Fam. Med. 2009, 22, 507–512. [Google Scholar] [CrossRef] [PubMed]
- Blevins, S.M.; Leyva, M.J.; Brown, J.; Wright, J.; Scofield, R.H.; Aston, C.E. Effect of cinnamon on glucose and lipid levels in non insulin-dependent type 2 diabetes. Diabetes Care 2007, 30, 2236–2237. [Google Scholar] [CrossRef] [PubMed]
- Mang, B.; Wolters, M.; Schmitt, B.; Kelb, K.; Lichtinghagen, R.; Stichtenoth, D.O.; Hahn, A. Effects of a cinnamon extract on plasma glucose, HbA1c, and serum lipids in diabetes mellitus type 2. Eur. J. Clin. Investig. 2006, 36, 340–344. [Google Scholar] [CrossRef] [PubMed]
- Vanschoonbeek, K.; Thomassen, B.J.; Senden, J.M.; Wodzig, W.K.; van Loon, L.J. Cinnamon supplementation does not improve glycemic control in postmenopausal type 2 diabetes patients. J. Nutr. 2006, 136, 977–980. [Google Scholar] [PubMed]
- Vafa, M.; Mohammadi, F.; Shidfar, F.; Sormaghi, M.S.; Heidari, I.; Golestan, B.; Amiri, F. Effects of cinnamon consumption on glycemic status, lipid profile and body composition in type 2 diabetic patients. Int. J. Prev. Med. 2012, 3, 531–536. [Google Scholar] [PubMed]
- Yamagishi, S.; Maeda, S.; Matsui, T.; Ueda, S.; Fukami, K.; Okuda, S. Role of advanced glycation end products (ages) and oxidative stress in vascular complications in diabetes. Biochim. Biophys. Acta 2012, 1820, 663–671. [Google Scholar] [CrossRef] [PubMed]
- Pourvali, K.; Abbasi, M.; Mottaghi, A. Role of superoxide dismutase 2 gene ala16val polymorphism and total antioxidant capacity in diabetes and its complications. Avic. J. Med. Biotechnol. 2016, 8, 48–56. [Google Scholar]
- Amin, K.A.; Abd El-Twab, T.M. Oxidative markers, nitric oxide and homocysteine alteration in hypercholesterolimic rats: Role of atorvastatine and cinnamon. Int. J. Clin. Exp. Med. 2009, 2, 254–265. [Google Scholar] [PubMed]
- Moselhy, S.S.; Ali, H.K. Hepatoprotective effect of cinnamon extracts against carbon tetrachloride induced oxidative stress and liver injury in rats. Biol. Res. 2009, 42, 93–98. [Google Scholar] [CrossRef] [PubMed]
- Peng, X.; Cheng, K.W.; Ma, J.; Chen, B.; Ho, C.T.; Lo, C.; Chen, F.; Wang, M. Cinnamon bark proanthocyanidins as reactive carbonyl scavengers to prevent the formation of advanced glycation endproducts. J. Agric. Food Chem. 2008, 56, 1907–1911. [Google Scholar] [CrossRef] [PubMed]
- Mashhadi, N.S.; Ghiasvand, R.; Hariri, M.; Askari, G.; Feizi, A.; Darvishi, L.; Hajishafiee, M.; Barani, A. Effect of ginger and cinnamon intake on oxidative stress and exercise performance and body composition in Iranian female athletes. Int. J. Prev. Med. 2013, 4, S31–S35. [Google Scholar] [PubMed]
- Pisprasert, V.; Ingram, K.H.; Lopez-Davila, M.F.; Munoz, A.J.; Garvey, W.T. Limitations in the use of indices using glucose and insulin levels to predict insulin sensitivity: Impact of race and gender and superiority of the indices derived from oral glucose tolerance test in African Americans. Diabetes Care 2013, 36, 845–853. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.; Safdar, M.; Ali Khan, M.M.; Khattak, K.N.; Anderson, R.A. Cinnamon improves glucose and lipids of people with type 2 diabetes. Diabetes Care 2003, 26, 3215–3218. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | Total (n = 39) | Case Group (n = 20) | Control Group (n = 19) | p-Value |
|---|---|---|---|---|
| Age (years) | 57.61 ± 8.70 | 58.90 ± 7.93 | 56.26 ± 9.46 | 0.43 |
| Male (%) | 38.5 | 40.0 | 36.8 | 0.83 |
| Weight (kg) | 75.41 ± 13.28 | 73.75 ± 10.74 | 77.15 ± 15.63 | 0.43 |
| Height (cm) | 164.89 ± 8.67 | 167.15 ± 7.38 | 162.52 ± 9.47 | 0.09 |
| Body mass index (kg/m2) | 27.70 ± 4.52 | 26.41 ± 3.06 | 29.02 ± 5.53 | 0.18 |
| Characteristics | Case Group (n = 20) | Control Group (n = 19) | p-Value * | |
|---|---|---|---|---|
| Fasting blood glucose (mg/dL) | Before | 183.85 ± 36.16 | 190.57 ± 70.58 | 0.71 |
| After | 172.20 ± 44.86 | 199.15 ± 49.86 | 0.53 | |
| Differences | −11.65 ± 29.34 | 8.57 ± 35.10 | 0.06 | |
| p ** | 0.09 | 0.30 | - | |
| Fasting insulin (mU/L) | Before | 9.85 (7.92–19.22) | 10.60 (8.80–17.30) | 0.86 |
| After | 12.10 (10.65–18.45) | 12.20 (9.30–14.20) | 0.73 | |
| Differences | 2.05 (−1.62–5.45) | 1.20 (−2.40–4.70) | 0.86 | |
| p | 0.24 | 0.46 | - | |
| Homeostasis model assessment for insulin resistance (HOMA-IR) | Before | 5.35 (2.97–9.22) | 5.39 (2.64–6.98) | 0.86 |
| After | 6.00 (3.34–9.00) | 6.16 (3.48–8.49) | 0.83 | |
| Differences | −0.03 (−1.50–1.97) | 0.68 (−0.73–1.50) | 0.42 | |
| p | 1.00 | 0.39 | - | |
| HemoglobinA1c | Before | 10.04 ± 1.30 | 10.31 ± 1.86 | 0.59 |
| After | 10.11 ± 1.49 | 10.30 ± 1.70 | 0.86 | |
| Differences | 0.075 ± 1.51 | −0.15 ± 1.93 | 0.87 | |
| p | 0.83 | 0.97 | - | |
| Carboxymethyl lysine | Before | 185.00 (178.50–188.75) | 183.00 (178.00–189.00) | 0.65 |
| After | 187.00 (181.25–191.00) | 185.00 (182.00–189.00) | 0.39 | |
| Differences | (−2.00–6.00) | 2.00 (−5.00–8.00) | 0.63 | |
| p | 0.44 | 0.44 | - | |
| Total antioxidant capacity (mmol) | Before | 0.708 ± 0.12 | 0.710 ± 0.13 | 0.96 |
| After | 0.706 ± 0.18 | 0.716 ± 0.13 | 0.80 | |
| Differences | 0.002 ± 0.11 | 0.006 ± 0.10 | 0.81 | |
| P | 0.93 | 0.78 | - | |
| Malondialdehyde | Before | 5.73 (4.16–9.11) | 5.21 (3.64–7.81) | 0.47 |
| After | 6.25 (4.29–7.29) | 6.25 (4.69–7.81) | 0.14 | |
| Differences | 0.00 (−3.12–0.52) | 1.05 (−1.57–2.96) | 0.08 | |
| p | 0.37 | 0.53 | - |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Talaei, B.; Amouzegar, A.; Sahranavard, S.; Hedayati, M.; Mirmiran, P.; Azizi, F. Effects of Cinnamon Consumption on Glycemic Indicators, Advanced Glycation End Products, and Antioxidant Status in Type 2 Diabetic Patients. Nutrients 2017, 9, 991. https://doi.org/10.3390/nu9090991
Talaei B, Amouzegar A, Sahranavard S, Hedayati M, Mirmiran P, Azizi F. Effects of Cinnamon Consumption on Glycemic Indicators, Advanced Glycation End Products, and Antioxidant Status in Type 2 Diabetic Patients. Nutrients. 2017; 9(9):991. https://doi.org/10.3390/nu9090991
Chicago/Turabian StyleTalaei, Behrouz, Atieh Amouzegar, Shamim Sahranavard, Mehdi Hedayati, Parvin Mirmiran, and Fereidoun Azizi. 2017. "Effects of Cinnamon Consumption on Glycemic Indicators, Advanced Glycation End Products, and Antioxidant Status in Type 2 Diabetic Patients" Nutrients 9, no. 9: 991. https://doi.org/10.3390/nu9090991
APA StyleTalaei, B., Amouzegar, A., Sahranavard, S., Hedayati, M., Mirmiran, P., & Azizi, F. (2017). Effects of Cinnamon Consumption on Glycemic Indicators, Advanced Glycation End Products, and Antioxidant Status in Type 2 Diabetic Patients. Nutrients, 9(9), 991. https://doi.org/10.3390/nu9090991




