The Development of a Chinese Healthy Eating Index and Its Application in the General Population
Abstract
:1. Introduction
2. Materials and Methods
2.1. The DGC-2016 and the Standard Portion (SP) Size
2.2. Participants and Dietary Assessment
2.3. Relevant Variables and Statistical Analysis
3. Results
3.1. Development of the Chinese Healthy Eating Index
3.1.1. Components
3.1.2. Weighting
3.1.3. Scoring
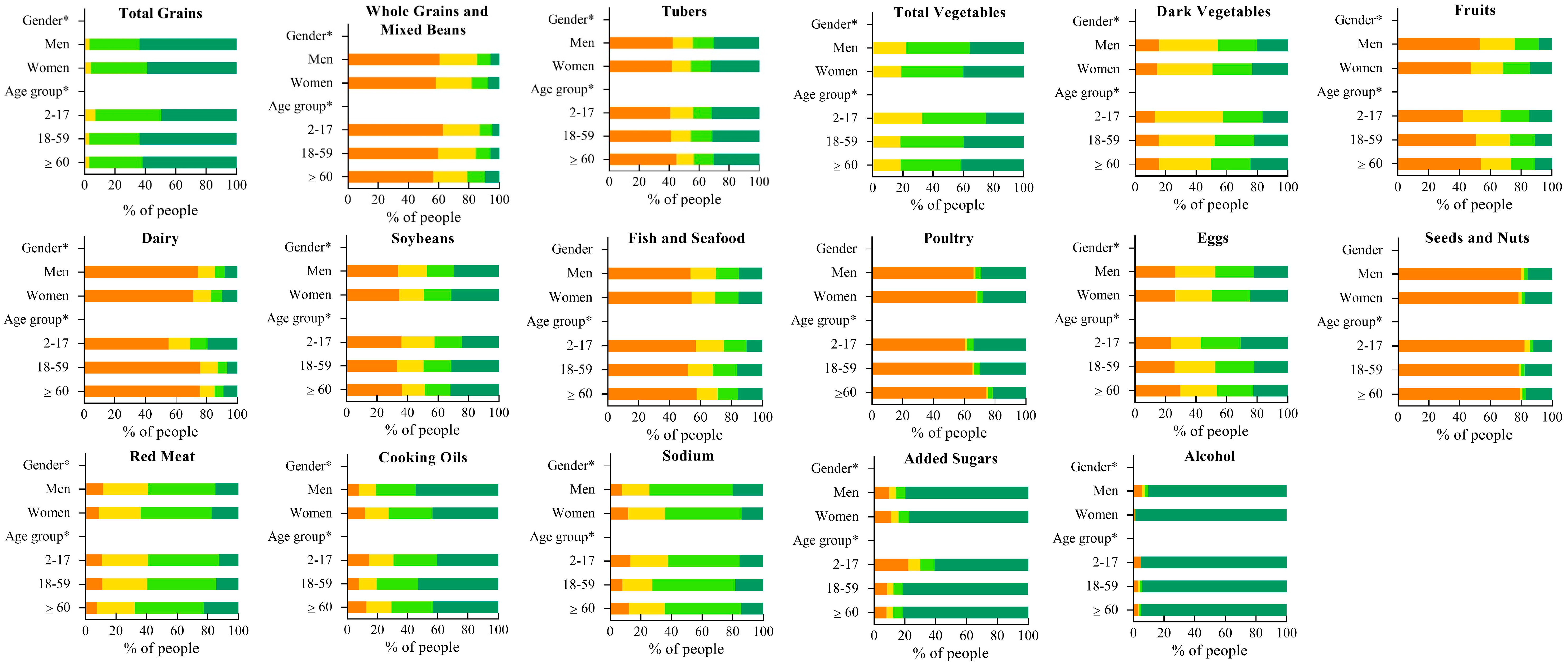
3.2. Application of the Chinese Healthy Eating Index
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Liese, A.D.; Krebs-Smith, S.M.; Subar, A.F.; George, S.M.; Harmon, B.E.; Neuhouser, M.L.; Boushey, C.J.; Schap, T.E.; Reedy, J. The dietary patterns methods project: Synthesis of findings across cohorts and relevance to dietary guidance. J. Nutr. 2015, 145, 393–402. [Google Scholar] [CrossRef] [PubMed]
- Solbak, N.M.; Xu, J.Y.; Vena, J.E.; Csizmadi, I.; Whelan, H.K.; Robson, P.J. Diet quality is associated with reduced incidence of cancer and self-reported chronic disease: Observations from Alberta’s tomorrow project. Prev. Med. 2017, 101, 178–187. [Google Scholar] [CrossRef] [PubMed]
- Glanz, K.; Hersey, J.; Cates, S.; Muth, M.; Creel, D.; Nicholls, J.; Rd, F.V.; Zaripheh, S. Effect of a nutrient rich foods consumer education program: Results from the nutrition advice study. J. Acad. Nutr. Diet. 2012, 112, 56. [Google Scholar] [CrossRef] [PubMed]
- Harmon, B.E.; Boushey, C.J.; Shvetsov, Y.B.; Ettienne, R.; Reedy, J.; Wilkens, L.R.; Le Marchand, L.; Henderson, B.E.; Kolonel, L.N. Associations of key diet-quality indexes with mortality in the multiethnic cohort: The dietary patterns methods project. Am. J. Clin. Nutr. 2015, 101, 587–597. [Google Scholar] [CrossRef] [PubMed]
- Hiza, H.A.B.; Casavale, K.O.; Guenther, P.M.; Davis, C.A. Diet quality of americans differs by age, sex, race/ethnicity, income, and education level. J. Acad. Nutr. Diet. 2013, 113, 297–306. [Google Scholar] [CrossRef] [PubMed]
- Reedy, J.; Krebs-Smith, S.M.; Bosire, C. Evaluating the food environment: Application of the Healthy Eating Index-2005. Am. J. Prev. Med. 2010, 38, 465. [Google Scholar] [CrossRef] [PubMed]
- Sotos-Prieto, M.; Bhupathiraju, S.N.; Mattei, J.; Fung, T.T.; Li, Y.; Pan, A.; Willett, W.C.; Rimm, E.B.; Hu, F.B. Changes in diet quality scores and risk of cardiovascular disease among US men and women. Circulation 2015, 132, 2212–2219. [Google Scholar] [CrossRef] [PubMed]
- Panagiotakos, D.B. healthy indexes in public health practice and research: A review. Crit. Rev. Food Sci. Nutr. 2008, 48, 317. [Google Scholar]
- Guenther, P.M.; Reedy, J.; Krebs Smith, S.M. Development of the Healthy Eating Index-2005. J. Am. Diet. Assoc. 2008, 108, 1896–1901. [Google Scholar] [CrossRef] [PubMed]
- Guenther, P.M.; Casavale, K.O.; Reedy, J.; Kirkpatrick, S.I.; Hiza, H.A.B.; Kuczynski, K.J.; Kahle, L.L.; Krebs-Smith, S.M. Update of the Healthy Eating Index: HEI-2010. J. Acad. Nutr. Diet. 2013, 113, 569–580. [Google Scholar] [CrossRef] [PubMed]
- Guenther, P.M.; Kirkpatrick, S.I.; Reedy, J.; Krebs-Smith, S.M.; Buckman, D.W.; Dodd, K.W.; Casavale, K.O.; Carroll, R.J. The Healthy Eating Index-2010 is a valid and reliable measure of diet quality according to the 2010 Dietary Guidelines for Americans. J. Nutr. 2014, 144, 399–407. [Google Scholar] [CrossRef] [PubMed]
- Previdelli, A.N.; Andrade, S.C.; Pires, M.M.; Ferreira, S.R.; Fisberg, R.M.; Marchioni, D.M. A revised version of the Healthy Eating Index for the Brazilian population. Revista De Saúde Pública 2011, 45, 794–798. [Google Scholar] [CrossRef] [PubMed]
- Roy, R.; Hebden, L.; Rangan, A.; Allmanfarinelli, M. The development, application, and validation of a Healthy Eating Index for Australian Adults (HEIFA-2013). Nutrition 2015, 32, 432–440. [Google Scholar] [CrossRef] [PubMed]
- Taechangam, S.; Pinitchun, U.; Pachotikarn, C. Development of nutrition education tool: Healthy Eating Index in Thailand. Asia Pac. J. Clin. Nutr. 2008, 17, 365–367. [Google Scholar] [PubMed]
- Woodruff, S.J.; Hanning, R.M. Development and implications of a revised Canadian Healthy Eating Index (HEIC-2009). Public Health Nutr. 2010, 13, 820–825. [Google Scholar] [CrossRef] [PubMed]
- He, Y.N.; Zhai, F.Y.; Ge, K.Y. Approaching Chinese diet balance index. J. Hyg. Res. 2005, 34, 208–211. [Google Scholar]
- Stookey, J.D.; Wang, Y.; Ge, K.; Lin, H.; Popkin, B.M. Measuring diet quality in China: The INFH-UNC-CH diet quality index. Eur. J. Clin. Nutr. 2000, 54, 811. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Hall, J.; Byles, J.; Shi, Z. Do older Chinese people’s diets meet the Chinese food pagoda guidelines? Results from the china health and nutrition survey 2009. Public Health Nutr. 2015, 18, 3020–3030. [Google Scholar] [CrossRef] [PubMed]
- Liu, R.; Zhao, Y.; Yan, H.; Dang, S.; Pang, S.; Wang, X.; Wang, F. Using the revised Chinese diet balance index quality of diet to evaluate the quality of diet among rural residents in Hanzhong, Shaanxi province and relative influencing factors. Zhonghua Liuxingbingxue Zazhi 2014, 35, 1087–1090. [Google Scholar] [PubMed]
- Chang, J.L.; Wang, Y.; Liang, X.F.; Wu, L.Y.; Ding, G.Q.; Yu, W.T.; Yu, D.M.; Ma, G.S.; Wang, X.; Wang, J.; et al. Report on Monitoring of Nutrition and Health of Chinese (2010–2013); Peking University Medical Press: Beijing, China, 2016; ISBN 978-7-5659-1460-7. [Google Scholar]
- Bragg, F.; Holmes, M.V.; Iona, A.; Guo, Y.; Du, H.; Chen, Y.; Bian, Z.; Yang, L.; Herrington, W.; Bennett, D. Association between diabetes and cause-specific mortality in rural and urban areas of China. JAMA 2017, 317, 280. [Google Scholar] [CrossRef] [PubMed]
- Du, H.; Li, L.; Bennett, D.; Yang, L.; Guo, Y.; Key, T.J.; Bian, Z.; Chen, Y.; Walters, R.G.; Millwood, I.Y. Fresh fruit consumption and all-cause and cause-specific mortality: Findings from the China Kadoorie Biobank. Int. J. Epidemiol. 2017. [Google Scholar] [CrossRef] [PubMed]
- Zhang, B.; Zhai, F.Y.; Du, S.F.; Popkin, B.M. The China health and nutrition survey, 1989–2011. Obes. Rev. Off. J. Int. Assoc. Stud. Obes. 2014, 15 (Suppl. S1), 2. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Hall, J.; Byles, J.; Shi, Z. Dietary pattern is associated with obesity in older people in China: Data from China health and nutrition survey (CHNS). Nutrients 2015, 7, 8170–8188. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.X.; Ma, A.G.; Sun, C.H.; Ma, G.S.; Wang, D.Y.; Wang, P.Y.; Liu, L.G.; Sun, J.Q.; Sun, G.J.; Zhang, D.; et al. Food and Health Evidence Based Review; People’s Medical Publishing House: Beijing, China, 2014; ISBN 978-7-117-21547-3. [Google Scholar]
- Holden, J. Usda Database for the Added Sugars Content of Selected Foods; USDA: Washington, DC, USA, 2015.
- Lin, P.H.; Aickin, M.; Champagne, C.; Craddick, S.; Sacks, F.M.; McCarron, P.; Most-Windhauser, M.M.; Rukenbrod, F.; Haworth, L. Food group sources of nutrients in the dietary patterns of the dash-sodium trial. J. Am. Diet. Assoc. 2003, 103, 488–496. [Google Scholar] [PubMed]
- Cheng, Y.Y.; Yang, Y.Y.; Yang, X.G.; Su, Y.X.; Guo, J.S.; Wang, Z.X.; Zhai, F.Y.; Ma, G.S.; Pu, J.H.; Huang, C.Y.; et al. Chinese Dietary Reference Intakes, 2013rd ed.; Science Press: Beijing, China, 2014; pp. 192–195. ISBN 978-7-03-041401-4. [Google Scholar]
- Waijers, P.M.; Feskens, E.J.; Ocké, M.C. A critical review of predefined diet quality scores. Br. J. Nutr. 2007, 97, 219–231. [Google Scholar] [CrossRef] [PubMed]
- Van Lee, L.; Geelen, A.; van Huysduynen, E.J.; de Vries, J.H.; van’t Veer, P.; Feskens, E.J. The Dutch Healthy Diet Index (DHD-index): An instrument to measure adherence to the Dutch guidelines for a healthy diet. Nutr. J. 2012, 11, 49. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Hall, J.; Byles, J.; Shi, Z. Assessing dietary quality of older Chinese people using the Chinese diet balance index (DBI). PLoS ONE 2015, 10, e0121618. [Google Scholar] [CrossRef] [PubMed]
- Tang, B.M.; Eslick, G.D.; Nowson, C.; Smith, C.; Bensoussan, A. Use of calcium or calcium in combination with vitamin D supplementation to prevent fractures and bone loss in people aged 50 years and older: A meta-analysis. Lancet 2007, 370, 657–666. [Google Scholar] [CrossRef]
- Wang, Y.; Li, S. Worldwide trends in dairy production and consumption and calcium intake: Is promoting consumption of dairy products a sustainable solution for inadequate calcium intake? Food Nutr. Bull. 2008, 29, 172–185. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; He, M.; Cui, H.; Bian, L.; Wang, Z. The prevalence of lactase deficiency and lactose intolerance in Chinese children of different ages. Chin. Med. J. 2000, 113, 1129–1132. [Google Scholar] [PubMed]
- Wang, Y.G.; Yan, Y.S.; Xu, J.J.; Du, R.F.; Flatz, S.D.; Kuhnau, W.; Flatz, G. Prevalence of primary adult lactose malabsorption in three populations of northern China. Hum. Genet. 1984, 67, 103–106. [Google Scholar] [PubMed]
- Cheng, G.; Xue, H.; Luo, J.; Jia, H.; Zhang, L.; Dai, J.; Buyken, A.E. Relevance of the dietary glycemic index, glycemic load and genetic predisposition for the glucose homeostasis of Chinese adults without diabetes. Sci. Rep. 2017, 7, 400. [Google Scholar] [CrossRef] [PubMed]
- Aune, D.; Norat, T. Dietary fibre, whole grains, and risk of colorectal cancer: Systematic review and dose-response meta-analysis of prospective studies. BMJ Br. Med. J. 2011, 343, d6617. [Google Scholar] [CrossRef] [PubMed]
- Astrup, A.; Dyerberg, J.; Selleck, M.; Stender, S. Nutrition transition and its relationship to the development of obesity and related chronic diseases. Obes. Rev. 2008, 9, 48–52. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Effect of Reduced Sodium Intake on Blood Pressure, and Potential Adverse Effects in Children; WHO: Geneva, Switzerland, 2012. [Google Scholar]
- World Health Organization (WHO). Effect of Reduced Sodium Intake on Cardiovascular Disease, Coronary Heart Disease and Stroke; WHO: Geneva, Switzerland, 2012. [Google Scholar]
- Li, X.Y.; Cai, X.L.; Bian, P.D.; Hu, L.R. High salt intake and stroke: Meta-analysis of the epidemiologic evidence. CNS Neurosci. Ther. 2012, 18, 691–701. [Google Scholar] [CrossRef] [PubMed]
- Graudal, N.; Jürgens, G.; Bo, B.; Alderman, M.H. Compared with usual sodium intake, low- and excessive-sodium diets are associated with increased mortality: A meta-analysis. Am. J. Hypertens. 2014, 27, 1129–1137. [Google Scholar] [CrossRef] [PubMed]
- Moore, L.L.; Singer, M.R.; Bradlee, M.L. Low sodium intakes are not associated with lower blood pressure levels among framingham offspring study adults. FASEB J. 2017, 31, 1. [Google Scholar]
- Liu, S.; Yu, D.; Guo, Q.; Wang, X.; Xu, X.; Jia, F.; Li, J.; Zhao, L. Consumption status and trend of added sugar containing food among Chinese from 2002 to 2012. J. Hyg. Res. 2016, 45, 398–401. [Google Scholar]
- Darmon, N.; Drewnowski, A. Does social class predict diet quality? Am. J. Clin. Nutr. 2008, 87, 1107. [Google Scholar] [PubMed]
- Turrell, G.; Hewitt, B.; Patterson, C.; Oldenburg, B. Measuring socio-economic position in dietary research: Is choice of socio-economic indicator important? Public Health Nutr. 2003, 6, 191–200. [Google Scholar] [CrossRef] [PubMed]
- Harrington, J.; Fitzgerald, A.P.; Layte, R.; Lutomski, J.; Molcho, M.; Perry, I.J. Sociodemographic, health and lifestyle predictors of poor diets. Public Health Nutr. 2011, 14, 2166–2175. [Google Scholar] [CrossRef] [PubMed]
- Vinther, J.L.; Conklin, A.I.; Wareham, N.J.; Monsivais, P. Marital transitions and associated changes in fruit and vegetable intake: Findings from the population-based prospective epic-norfolk cohort, UK. Soc. Sci. Med. 2016, 157, 120–126. [Google Scholar] [CrossRef] [PubMed]
- Umberson, D. Family status and health behaviors: Social control as a dimension of social integration. J. Health Soc. Behav. 1987, 28, 306–319. [Google Scholar] [CrossRef] [PubMed]
- Galobardes, B.; Morabia, A.; Bernstein, M.S. Diet and socioeconomic position: Does the use of different indicators matter? Int. J. Epidemiol. 2001, 30, 334–340. [Google Scholar] [CrossRef] [PubMed]
- Alkerwi, A.; Baydarlioglu, B.; Sauvageot, N.; Stranges, S.; Lemmens, P.; Shivappa, N.; Hebert, J.R. Smoking status is inversely associated with overall diet quality: Findings from the oriscav-lux study. Clin. Nutr. 2017, 36, 1275–1282. [Google Scholar] [CrossRef] [PubMed]
| Components | Weighting | Key Recommendations | Comments | Key Evidence |
|---|---|---|---|---|
| Total Grains Whole Grains and Mixed Beans Tubers | 5 5 5 | Eat a variety of foods, cereal-based. Consume cereal at every meal. Increase intake of whole grains and mixed beans. Cook tubers in various forms to increase consumption. | Whole grains prevalent in China are coarse rice, whole wheat, corn, millet, buckwheat and oats. Mixed beans are rich in carbohydrates, including mung bean, red bean and kidney bean, etc. Tubers, such as potatoes, sweet potatoes and cassava, are also recommended as staple food for their high content of carbohydrates. | Consumption of whole grain reduces the risk of colorectal cancer, type 2 diabetes, cardiovascular disease and weight gain (B). Increased tuber intake reduces the risk of constipation (C). |
| Total Vegetables Dark Vegetables Fruits Dairy Soybeans | 5 5 10 5 5 | Eat plenty of vegetables, fruits, dairy products, and soybeans. Eat vegetables every meal, and half should be dark vegetables. Every day consume fresh fruits rather than processed forms. Consume a variety of dairy. Consume soybeans regularly. Seeds and nuts are beneficial, but should not be consumed excessively. | Dark vegetables include deep green, orange, red and fuchsia vegetables, such as spinach, tomatoes, carrots, and purple cabbage. Cooked, canned, frozen, and dried fruits cannot replace fresh fruits. Yogurt or low-lactose dairy products should be the first choice for individuals with lactose intolerance. Although seeds and nuts are beneficial for health, excessive intake can lead to an excess of energy. | Total vegetable consumption reduces all causes of mortality and the risk of cardiovascular diseases (CVDs) and cancers of the digestive tract; intake of dark green vegetables lowers risks of type 2 diabetes and lung cancer (B). Increased fruit intake lowers the risk of CVDs, cancers of the digestive tract and adult weight gain (B). Low-fat milk consumption decreases the risk of breast cancer, and higher dairy intake is linked to higher bone mineral density (B). Soybean intake lowers the risks of breast cancer, osteoporosis, type 2 diabetes, hyperlipidemia and hypertension (B). Moderate intake of seeds and nuts decreases all causes of mortality and the risk of CVDs, hypertension, and colorectal cancer in women (B). |
| Fish and Seafood Red Meat Poultry Eggs | 5 5 5 5 | Eat moderate amounts of fish, poultry, eggs, and lean meats. Choose fish, seafood and poultry. Decrease intake of fat meat and smoked meat products. | Adverse effects of excessively consuming red meat have been demonstrated. Eat egg with yolk. | Consumption of fish lowers risk of CVDs, stroke (B), cognitive decline and macular degeneration (C). Excessive intake of meat increases all-cause mortality in men and risk of type 2 diabetes, colorectal cancer (B), and obesity (C). Higher meat intake lowers risk of iron deficiency anemia (C). |
| Cooking Oils Sodium Added Sugars Alcohol | 10 10 5 5 | Limit salt, cooking oil, added sugar, and alcohol. Limit cooking oils intake to 25–30g/day. Consume salt less than 6 g/day, and consume sodium less than 1500 mg/day. Limit intake of added sugars to less than 50 g/day. Children, adolescents, pregnant and lactating women should not consume alcohol; men (women) should limit alcohol intake to less than 25 g (15 g). | Cooking oils include plant oil and animal fat. The sodium component of the CHEI also includes sodium in sodium-rich foods (sodium content more than 500 mg/100 g). | Excessive consumption of any kind of fat increases energy intake and the risk of obesity (A). High consumption of sodium increases risk of hypertension (A), CVDs (C), stroke (B), gastric cancer (B). Overconsumption of added sugar increases risk of dental caries (B), weight gain (C), and hyperlipidemia (C). Excessive intake of alcohol rises risk of liver injury (A), gout (A), colorectal cancer (B), breast cancer (B), CVDs (B), and fetal alcohol syndrome (A). |
| Food Group | Standard Portion per 1000 kcal | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Calorie Level (kcal) | 1000 | 1200 | 1400 | 1600 | 1800 | 2000 | 2200 | 2400 | 2600 | 2800 | 3000 |
| Total Grains | 1.7 | 1.7 | 2.1 | 2.5 | 2.5 | 2.5 | 2.5 | 2.5 | 2.7 | 2.7 | 2.7 |
| Whole Grains and Mix Beans | 0.6 | 0.8 | 1.0 | 1.1 | 1.3 | ||||||
| Tubers | 0.3 | 0.3 | 0.4 | 0.3 | 0.4 | 0.5 | 0.4 | 0.4 | |||
| Total Vegetables | 2.0 | 2.1 | 2.1 | 1.9 | 2.2 | 2.3 | 2.0 | 2.1 | 1.9 | 1.8 | 2.0 |
| Dark Vegetables | 1.0 | 1.0 | 1.1 | 0.9 | 1.1 | 1.1 | 1.0 | 1.0 | 1.0 | 0.9 | 1.0 |
| Fruits | 1.5 | 1.3 | 1.1 | 1.3 | 1.1 | 1.5 | 1.4 | 1.5 | 1.3 | 1.4 | 1.3 |
| Dairy | 2.0 | 1.7 | 1.0 | 0.8 | 0.7 | 0.6 | 0.5 | 0.5 | 0.5 | 0.4 | 0.4 |
| Soybeans | 0.3 | 0.6 | 0.5 | 0.5 | 0.4 | 0.4 | 0.6 | 0.5 | 0.5 | 0.4 | 0.4 |
| Seeds and Nuts | 0.6 | 0.6 | 0.5 | 0.5 | 0.4 | 0.4 | 0.4 | 0.3 | |||
| Fish and Seafood | 0.3 | 0.4 | 0.6 | 0.6 | 0.6 | 0.6 | 0.8 | 0.7 | 0.6 | 0.8 | 0.9 |
| Meat and Poultry | 0.3 | 0.5 | 0.6 | 0.6 | 0.6 | 0.6 | 0.8 | 0.7 | 0.6 | 0.8 | 0.7 |
| Eggs | 0.4 | 0.5 | 0.4 | 0.6 | 0.5 | 0.6 | 0.5 | 0.5 | 0.4 | 0.4 | 0.4 |
| Cooking Oils (g/1000 kcal) | 15.0 | 16.7 | 14.3 | 15.6 | 13.9 | 12.5 | 11.4 | 12.5 | 11.5 | 10.7 | 11.7 |
| Component | Score | ||
|---|---|---|---|
| 0 | 5 | 10 | |
| Adequacy | |||
| Total Grains | 0  | ≥2.5 SP/1000 kcal | |
| Whole Grains and Mixed Beans | 0  | ≥0.6 SP/1000 kcal | |
| Tubers | 0  | ≥0.3 SP/1000 kcal | |
| Total Vegetables | 0  | ≥1.9 SP/1000 kcal | |
| Dark Vegetables | 0  | ≥0.9 SP/1000 kcal | |
| Fruits | 0  | ≥1.1 SP/1000 kcal | |
| Dairy | 0  | ≥0.5 SP/1000 kcal | |
| Soybeans | 0  | ≥0.4 SP/1000 kcal | |
| Fish and Seafood | 0  | ≥0.6 SP/1000 kcal | |
| Poultry | 0  | ≥0.3 SP/1000 kcal | |
| Eggs | 0  | ≥0.5 SP/1000 kcal | |
| Seeds and Nuts | 0  | ≥0.4 SP/1000 kcal | |
| Limitation | |||
| Red Meat | ≥3.5  | ≤0.4 SP//1000 kcal | |
| Cooking Oils | ≥32.6  | ≤15.6 g/1000 kcal | |
| Sodium | ≥3608  | ≤1000 mg/1000 kcal | |
| Added Sugars | ≥20%  | ≤10% of energy | |
| Alcohol | ≥25 g (men)/15 g (women)  | ≤60 g (men)/40 g (women) | |
| Characteristics | CHEI Tertiles | ||||
|---|---|---|---|---|---|
| Total (n = 14,584) | Low (n = 4861) | Intermediate (n = 4862) | High (n = 4861) | p for Trend | |
| CHEI Score | 52.4 ± 10.9 | 40.6 ± 5.6 | 52.2 ± 2.7 | 64.3 ± 6.0 | |
| Age group in years (%) | 0.114 | ||||
| 2–17 | 14.5 | 17.4 | 13.4 | 12.7 | |
| 18–59 | 61.0 | 53.9 | 63.8 | 65.3 | |
| ≥60 | 24.5 | 28.7 | 22.8 | 22.0 | |
| Female sex (%) | 52.0 | 52.7 | 49.6 | 53.7 | 0.330 |
| Current smoking(%) | 17.9 | 19.2 | 17.5 | 16.9 | 0.029 |
| Living alone (%) | 14.1 | 15.9 | 13.6 | 12.9 | <0.001 |
| Urbanization (%) | <0.001 | ||||
| Urban | 24.3 | 13.6 | 18.5 | 40.7 | |
| Suburban | 33.2 | 33.3 | 33.8 | 32.4 | |
| Rural | 42.5 | 53.1 | 47.7 | 26.9 | |
| Education level (%) | |||||
| Low | 42.2 | 55.3 | 42.6 | 28.8 | <0.001 |
| Medium | 47.3 | 39.4 | 49.0 | 53.4 | |
| High | 10.5 | 5.3 | 8.4 | 17.8 | |
| Occupation (employed %) | 49.4 | 45.1 | 52.9 | 50.2 | <0.001 |
| BMI | <0.001 | ||||
| Under weight | 14.0 | 17.5 | 13.5 | 11.1 | |
| Normal | 47.5 | 46.1 | 48.5 | 47.9 | |
| Over weight | 28.8 | 26.8 | 28.0 | 31.4 | |
| Obesity | 9.7 | 9.6 | 10.0 | 9.6 | |
| Percentile | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| CHEI Score | Mean | 1st | 5th | 10th | 25th | 50th | 75th | 90th | 95th | 99th |
| Total | 52.4 | 27.6 | 34.6 | 38.7 | 45.0 | 52.2 | 59.6 | 66.5 | 70.9 | 78.3 |
| Men | 52.2 | 27.9 | 35.2 | 39.1 | 45.2 | 52.1 | 59.2 | 65.6 | 69.8 | 76.6 |
| Women | 52.5 | 27.5 | 34.1 | 38.2 | 44.7 | 52.3 | 60.0 | 67.5 | 71.6 | 78.9 |
| 2–17 | 50.4 | 22.9 | 31.1 | 35.2 | 42.3 | 50.9 | 58.5 | 65.2 | 69.4 | 76.9 |
| 18–59 | 53.2 | 29.1 | 36.2 | 39.8 | 46.3 | 53.1 | 60.1 | 67.0 | 70.9 | 77.8 |
| 60+ | 51.4 | 27.6 | 33.8 | 37.9 | 43.6 | 50.6 | 58.6 | 66.1 | 71.5 | 79.8 |
| Variables | CHEI Score | Univariate Model | Final Multivariate Model a | ||
|---|---|---|---|---|---|
| Mean (SD) | Coefficient (95%CI) | p-Value | Coefficient (95%CI) | p-Value | |
| Sex | |||||
| Men | 52.2 (10.4) | Reference | Reference | ||
| Women | 52.5 (11.3) | 0.27 (−0.08, 0.63) | 0.130 | 0.36 (−0.02, 0.73) | 0.070 |
| Age groups | |||||
| 18–59 | 53.2 (10.5) | Reference | Reference | ||
| 2–17 | 50.4 (11.6) | −2.88 (−3.40, −2.37) | <0.001 | −0.32 (−2.09, 1.44) | 0.719 |
| ≥60 | 51.4 (10.9) | −1.86 (−2.28, −1.44) | <0.001 | −0.93 (−1.44, −0.43) | <0.001 |
| Education level | |||||
| Low | 49.3 (10.3) | Reference | Reference | ||
| Medium | 53.8 (10.5) | 4.50 (4.14, 4.86) | <0.001 | 2.66 (2.25,3.06) | <0.001 |
| High | 58.4 (11.1) | 9.06 (8.47, 9.65) | <0.001 | 5.13 (4.47, 5.78) | <0.001 |
| Smoking | |||||
| Non-smoker | 52.5 (10.9) | Reference | Reference | ||
| Former smoker | 54.4 (11.1) | 1.96 (0.76, 3.16) | 0.001 | 0.30 (−0.85, 1.44) | 0.609 |
| Current smoker | 51.8 (10.5) | −0.72 (−1.19, −0.26) | 0.002 | −1.29(−1.78, −0.80) | <0.001 |
| Living alone | |||||
| Yes | 51.3 (10.9) | Reference | Reference | ||
| No | 52.6 (10.9) | 1.28 (0.78, 1.79) | <0.001 | 1.75 (1.24, 2.24) | <0.001 |
| Urbanization | |||||
| Rural | 49.3 (9.5) | Reference | Reference | ||
| Suburban | 52.1 (10.5) | 2.79 (2.40, 3.18) | <0.001 | 1.95 (1.55,2.35) | <0.001 |
| Urban | 58.1 (11.4) | 8.77 (8.34, 9.19) | <0.001 | 6.83 (6.35, 7.31) | <0.001 |
| Occupation | |||||
| Employed | 52.9 (10.2) | Reference | Reference | ||
| Unemployed | 50.1 (10.4) | −2.77 (−3.24, −2.29) | <0.001 | −1.69 (−2.17, −1.22) | <0.001 |
| Retired | 55.0 (11.7) | 2.14 (1.65, 2.62) | <0.001 | 0.96 (0.38, 1.55) | 0.001 |
| At school | 52.1 (11.1) | −0.72 (−1.30, −0.14) | 0.015 | 0.69 (−1.02, 2.40) | 0.428 |
| Dropouts | 46.5 (12.2) | −6.38 (−7.27, −5.48) | <0.001 | −3.73 (−5.67, −1.79) | <0.001 |
| BMI | |||||
| Normal | 52.6 (10.6) | Reference | Reference | ||
| Underweight | 49.9 (11.3) | −2.73 (−3.27, −2.20) | <0.001 | −0.73 (−1.36, −0.09) | 0.024 |
| Overweight | 53.2 (10.9) | 0.59 (0.18, 1.01) | 0.005 | 0.27 (−0.12, 0.66) | 0.176 |
| Obesity | 52.4 (10.9) | −0.12 (−0.74, 0.49) | 0.693 | 0.05 (−0.53, 0.62) | 0.875 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yuan, Y.-Q.; Li, F.; Dong, R.-H.; Chen, J.-S.; He, G.-S.; Li, S.-G.; Chen, B. The Development of a Chinese Healthy Eating Index and Its Application in the General Population. Nutrients 2017, 9, 977. https://doi.org/10.3390/nu9090977
Yuan Y-Q, Li F, Dong R-H, Chen J-S, He G-S, Li S-G, Chen B. The Development of a Chinese Healthy Eating Index and Its Application in the General Population. Nutrients. 2017; 9(9):977. https://doi.org/10.3390/nu9090977
Chicago/Turabian StyleYuan, Ya-Qun, Fan Li, Rui-Hua Dong, Jing-Si Chen, Geng-Sheng He, Shu-Guang Li, and Bo Chen. 2017. "The Development of a Chinese Healthy Eating Index and Its Application in the General Population" Nutrients 9, no. 9: 977. https://doi.org/10.3390/nu9090977






