Antiosteoporotic Activity of Genistein Aglycone in Postmenopausal Women: Evidence from a Post-Hoc Analysis of a Multicenter Randomized Controlled Trial
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design Overview, Setting, Participants
2.2. Study Population
2.3. Assessment of Fracture Risk
2.4. Statistical Analysis
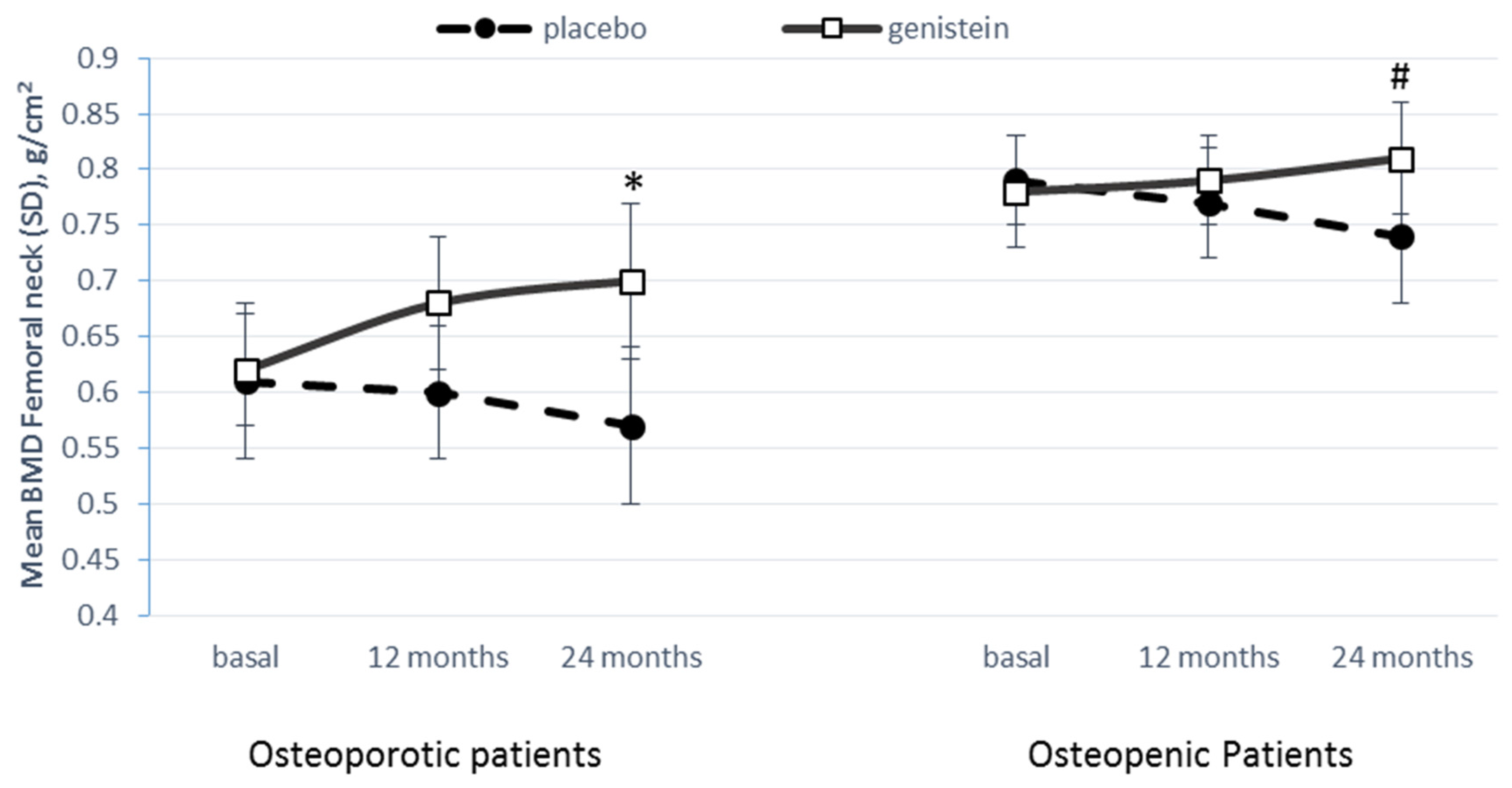
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Writing Group for the Women’s Health Initiative Investigators. Risks and benefits of estrogen plus progestin in healthy postmenopausal women: Principal results from the Women’s Health Initiative randomized controlled trial. JAMA 2002, 288, 321–333. [Google Scholar]
- Collaborative group on Hormonal Factors in Breast Cancer. Breast Cancer and hormone replacement therapy: Collaborative reanalysis of data from 51 epidemiological studies of 52,705 women with breast cancer and 108,411 women without breast cancer. Lancet 1997, 350, 1047–1059. [Google Scholar]
- Beral, V.; Million Women Study Collaborators. Breast cancer and hormone replacement therapy in the Million Women Study. Lancet 2003, 362, 419–427. [Google Scholar] [CrossRef]
- Adlecreutz, H.L.; Mazur, W. Phyto-estrogen and western disease. Ann. Med. 1997, 29, 95–120. [Google Scholar] [CrossRef]
- Horiuchi, T.; Onouchi, T.; Takahashi, M.; Ito, H.; Orimo, H. Effect of soy protein on bone metabolism in postmenopausal Japanese women. Osteoporos. Int. 2000, 11, 721–724. [Google Scholar] [CrossRef] [PubMed]
- Marini, H.; Minutoli, L.; Polito, F.; Bitto, A.; Altavilla, D.; Atteritano, M.; Gaudio, A.; Mazzaferro, S.; Frisina, A.; Frisina, N.; et al. Effects of the phytoestrogen genistein on bone metabolism in osteopenic postmenopausal women: A randomized trial. Ann. Intern. Med. 2007, 146, 839–847. [Google Scholar] [CrossRef] [PubMed]
- Marini, H.; Minutoli, L.; Polito, F.; Bitto, A.; Altavilla, D.; Atteritano, M.; Gaudio, A.; Mazzaferro, S.; Frisina, A.; Frisina, N.; et al. OPG and sRANKL serum concentrations in osteopenic, postmenopausal women after 2-year genistein administration. J. Bone Miner. Res. 2008, 23, 715–720. [Google Scholar] [CrossRef] [PubMed]
- Marini, H.; Bitto, A.; Altavilla, D.; Burnett, B.P.; Polito, F.; Di Stefano, V.; Minutoli, L.; Atteritano, M.; Levy, R.M.; D’Anna, R.; et al. Breast safety and efficacy of genistein aglycone for postmenopausal bone loss: A follow-up study. J. Clin. Endocrinol. Metab. 2008, 93, 4787–4796. [Google Scholar] [CrossRef] [PubMed]
- Bitto, A.; Polito, F.; Squadrito, F.; Marini, H.; D’Anna, R.; Irrera, N.; Minutoli, L.; Granese, R.; Altavilla, D. Genistein Aglycone: A Dual Mode of Action Anti-Osteoporotic Soy Isoflavone Rebalancing Bone Turnover Towards Bone Formation. Curr. Med. Chem. 2010, 27, 3007–3018. [Google Scholar] [CrossRef]
- Atteritano, M.; Mazzaferro, S.; Frisina, A.; Cannata, M.L.; Bitto, A.; D’Anna, R.; Squadrito, F.; Macrì, I.; Frisina, N.; Buemi, M. Genistein effects on quantitative ultrasound parameters and bone mineral density in osteopenic postmenopausal women. Osteoporos. Int. 2009, 20, 1947–1954. [Google Scholar] [CrossRef] [PubMed]
- Atteritano, M.; Mazzaferro, S.; Bitto, A.; Cannata, M.L.; D’Anna, R.; Squadrito, F.; Macrì, I.; Frisina, A.; Frisina, N.; Bagnato, G. Genistein effects on quality of life and depression symptoms in osteopenic postmenopausal women: A 2-year randomized, double-blind, controlled study. Osteoporos. Int. 2014, 25, 1123–1129. [Google Scholar] [CrossRef] [PubMed]
- Atteritano, M.; Pernice, F.; Mazzaferro, S.; Mantuano, S.; Frisina, A.; D’Anna, R.; Cannata, M.L.; Bitto, A.; Squadrito, F.; Frisina, N.; et al. Effects of phytoestrogen genistein on cytogenetic biomarkers in postmenopausal women: 1 year randomized, placebo-controlled study. Eur. J. Pharmacol. 2008, 28, 22–26. [Google Scholar] [CrossRef] [PubMed]
- Harkness, L.S.; Fiedler, K.; Sehgal, A.R.; Oravec, D.; Lerner, E. Decreased bone resorption with soy isoflavone supplementation in postmenopausal women. J. Womens Health 2004, 13, 1000–1007. [Google Scholar] [CrossRef] [PubMed]
- Kreijkamp-Kaspers, S.; Kok, L.; Grobbee, D.E.; de Haan, E.H.; Aleman, A.; Lampe, J.W.; van der Schouw, Y.T. Effect of soy protein containing isoflavones on cognitive function, bone mineral density, and plasma lipids in postmenopausal women: A randomized controlled trial. JAMA 2004, 292, 65–74. [Google Scholar] [CrossRef] [PubMed]
- Lydeking-Olsen, E.; Beck-Jensen, J.E.; Setchell, K.D.; Holm-Jensen, T. Soymilk or progesterone for prevention of bone loss—A 2 years randomized, placebo-controlled trial. Eur. J. Nutr. 2004, 43, 246–257. [Google Scholar] [CrossRef] [PubMed]
- Newton, K.M.; LaCroix, A.Z.; Levy, L.; Li, S.S.; Qu, P.; Potter, J.D.; Lampe, J.W. Soy protein and bone mineral density in older men and women: A randomized trial. Maturitas 2006, 55, 270–277. [Google Scholar] [CrossRef] [PubMed]
- Sehmisch, S.; Uffenorde, J.; Maehlmeyer, S.; Tezval, M.; Jarry, H.; Stuermer, K.M.; Stuermer, E.K. Evaluation of bone quality and quantity in osteoporotic mice—The effects of genistein and equol. Phytomedicine 2010, 17, 424–430. [Google Scholar] [CrossRef] [PubMed]
- Bitto, A.; Burnett, B.P.; Polito, F.; Levy, R.M.; Marini, H.; Di Stefano, V.; Irrera, N.; Armbruster, M.A.; Minutoli, L.; Altavilla, D.; et al. Genistein aglycone reverses glucocorticoid-induced osteoporosis and increases bone breaking strength in rats: A comparative study with alendronate. Br. J. Pharmacol. 2009, 156, 1287–1295. [Google Scholar] [CrossRef] [PubMed]
- FRAX. Fracture Risk Assessment Tool. Available online: http://www.shef.ac.uk/FRAX (accessed on 7–11 March 2016).
- Kanis, J.A.; Johnell, O.; Oden, A.; Johansson, H.; McCloskey, E. FRAX and the assessment of fracture probability in men and women from the UK. Osteoporos. Int. 2008, 19, 385–397. [Google Scholar] [CrossRef] [PubMed]
- Kanis, J.A.; Burlet, N.; Cooper, C. European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos. Int. 2008, 19, 399–428. [Google Scholar] [CrossRef] [PubMed]
- Kanis, J.A.; Johnell, O. Requirements for DXA for the management of osteoporosis in Europe. Osteoporos. Int. 2005, 16, 229–238. [Google Scholar] [CrossRef] [PubMed]
- Palacios, S. Advances in hormone replacement therapy: Making the menopause manageable. BMC Womens Health 2008, 8, 22. [Google Scholar] [CrossRef] [PubMed]
| Variable | Osteoporotic | Osteopenic | ||
|---|---|---|---|---|
| Placebo (59) | Genistein (62) | Placebo (132) | Genistein (136) | |
| Mean age (SD), year | 54.3 (2.4) | 54.5 (2.9) | 54.6 (2.7) | 54.8 (2.2) |
| Mean body mass index (SD), Kg/m2 | 25.2 (3.0) | 25.5 (2.8) | 25.4 (3.9) | 24.8 (3.7) |
| Mean time since menopause (SD), m | 69.4 (44.7) | 68.3 (39.2) | 69.1 (35.9) | 66.4 (38.3) |
| Mean BMD Femoral neck (SD), g/cm2 | 0.61 (0.07) | 0.62 (0.05) | 0.79 (0.04) | 0.78 (0.05) |
| Mean BMD Lumbar Spine (SD), g/cm2 | 0.81 (0.10) | 0.82 (0.08) | 0.85 (0.10 | 0.85 (0.08) |
| Mean BMD Total hip (SD), g/cm2 | 0.72 (0.08) | 0.73 (0.06) | 0.93 (0.04) | 0.92 (0.05) |
| B-ALP (μg/L) | 10.8 (1.79) | 10.0 (2.21) | 10.0 (1.87) | 10.6 (2.09) |
| D-Pyr (pmol/μmol of urinary creatinine) | 22.0 (6.92) | 22.7 (7.86) | 20.6 (5.19) | 21.2 (3.97) |
| FRAX index | ||||
| Major fractures (SD) | 6.5 (2.8) | 6.6 (2.4) | 3.3 (0.5) | 3.4 (0.5) |
| Femur fractures (SD) | 4.1 (1.9) | 4.2 (2.1) | 0.7 (0.1) | 0.7 (0.1) |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arcoraci, V.; Atteritano, M.; Squadrito, F.; D’Anna, R.; Marini, H.; Santoro, D.; Minutoli, L.; Messina, S.; Altavilla, D.; Bitto, A. Antiosteoporotic Activity of Genistein Aglycone in Postmenopausal Women: Evidence from a Post-Hoc Analysis of a Multicenter Randomized Controlled Trial. Nutrients 2017, 9, 179. https://doi.org/10.3390/nu9020179
Arcoraci V, Atteritano M, Squadrito F, D’Anna R, Marini H, Santoro D, Minutoli L, Messina S, Altavilla D, Bitto A. Antiosteoporotic Activity of Genistein Aglycone in Postmenopausal Women: Evidence from a Post-Hoc Analysis of a Multicenter Randomized Controlled Trial. Nutrients. 2017; 9(2):179. https://doi.org/10.3390/nu9020179
Chicago/Turabian StyleArcoraci, Vincenzo, Marco Atteritano, Francesco Squadrito, Rosario D’Anna, Herbert Marini, Domenico Santoro, Letteria Minutoli, Sonia Messina, Domenica Altavilla, and Alessandra Bitto. 2017. "Antiosteoporotic Activity of Genistein Aglycone in Postmenopausal Women: Evidence from a Post-Hoc Analysis of a Multicenter Randomized Controlled Trial" Nutrients 9, no. 2: 179. https://doi.org/10.3390/nu9020179
APA StyleArcoraci, V., Atteritano, M., Squadrito, F., D’Anna, R., Marini, H., Santoro, D., Minutoli, L., Messina, S., Altavilla, D., & Bitto, A. (2017). Antiosteoporotic Activity of Genistein Aglycone in Postmenopausal Women: Evidence from a Post-Hoc Analysis of a Multicenter Randomized Controlled Trial. Nutrients, 9(2), 179. https://doi.org/10.3390/nu9020179








