The n-3 Polyunsaturated Fatty Acids Supplementation Improved the Cognitive Function in the Chinese Elderly with Mild Cognitive Impairment: A Double-Blind Randomized Controlled Trial
Abstract
:1. Introduction
2. Materials and Methods
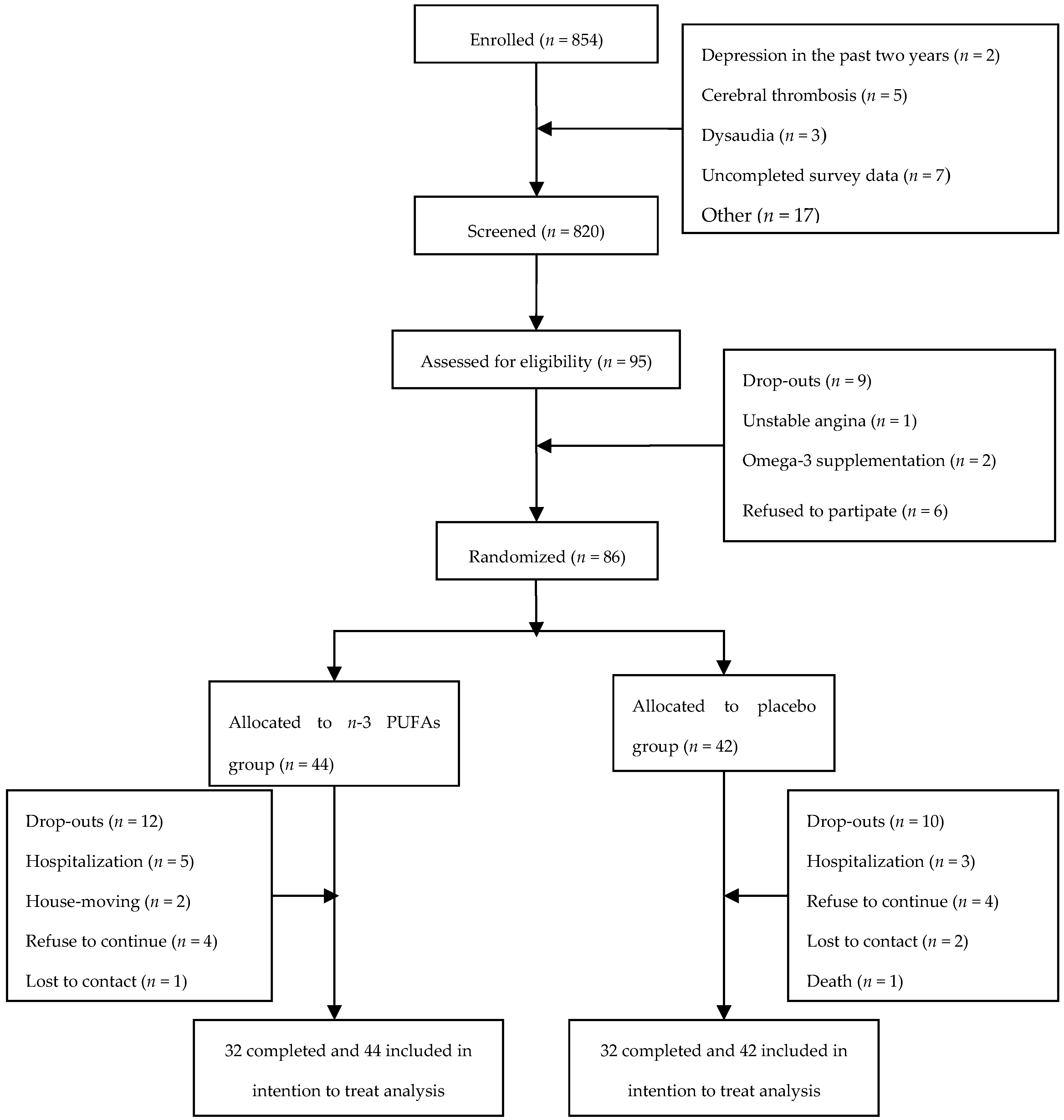
2.1. Participants
2.2. Randomization and Intervention
2.3. Cognitive Function Test
2.4. Blood Collection and Analysis
2.5. Data Analysis
3. Results
3.1. Baseline Characteristics
3.2. Changes in Plasma Fatty Acids Composition
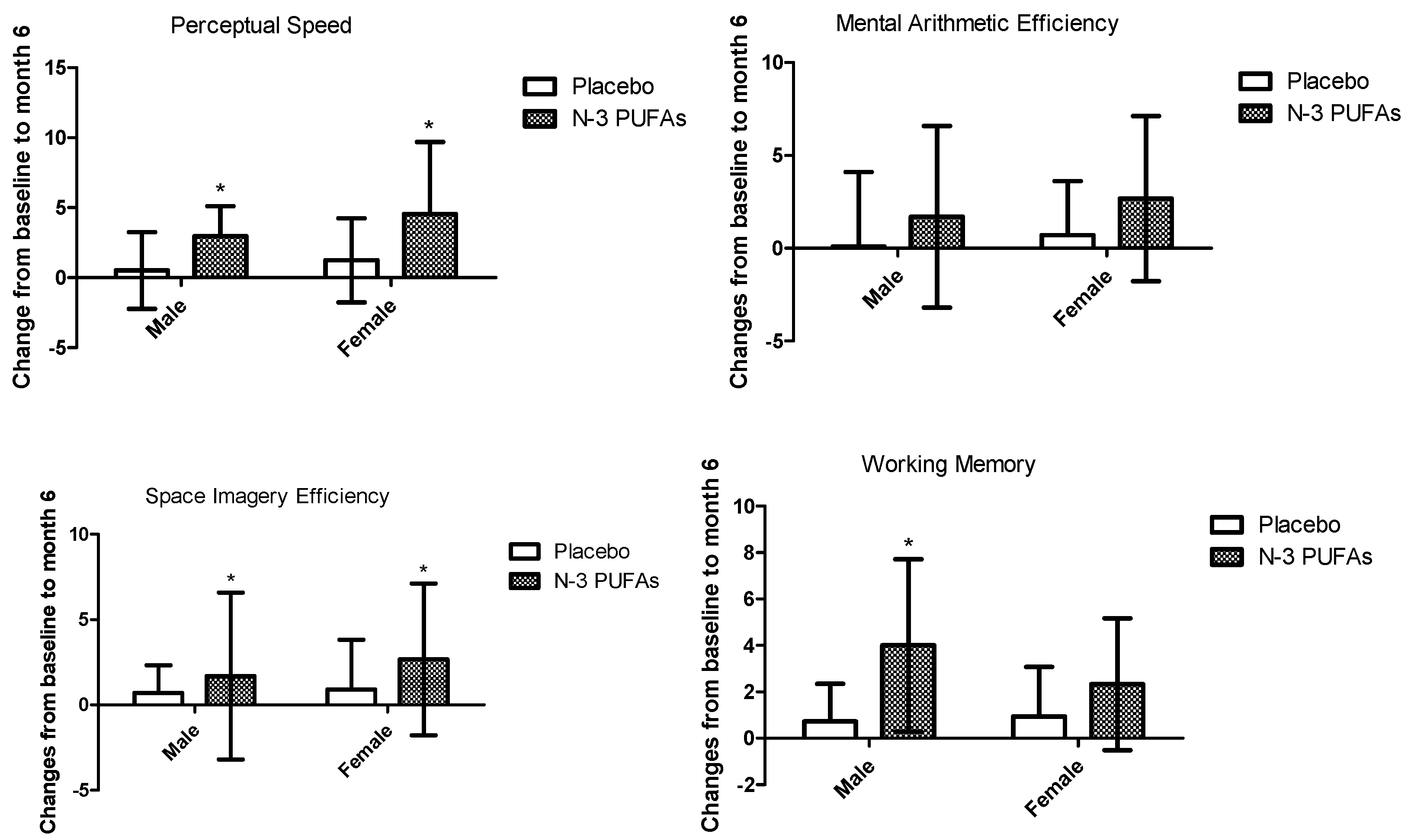
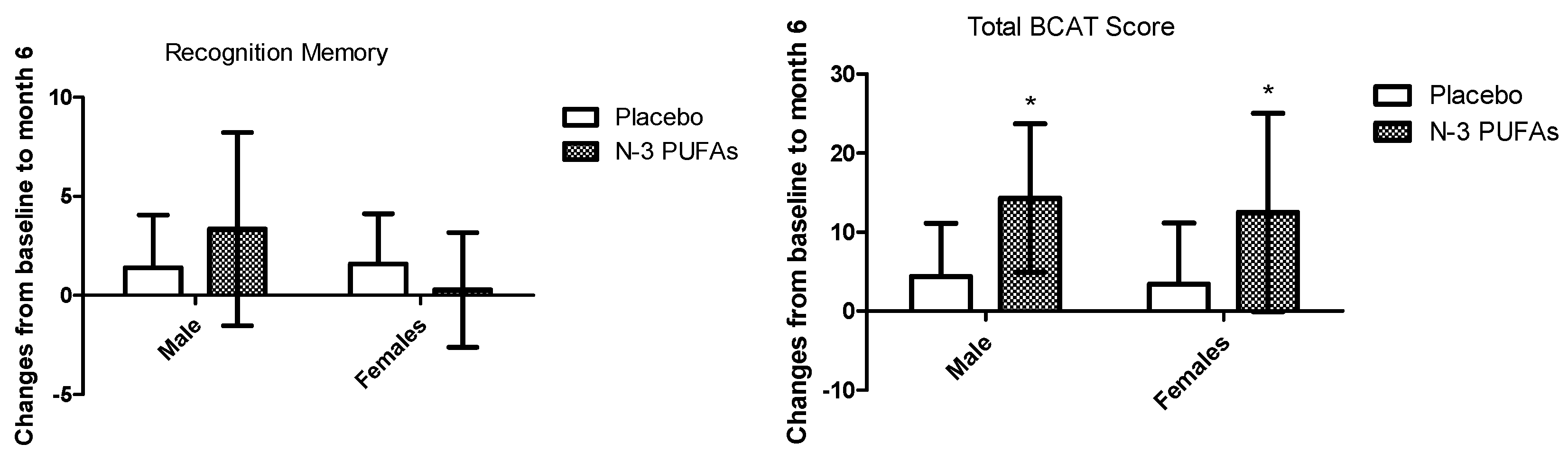
3.3. Cognitive Function Changes
3.4. Changes in the Plasma Indicators Levels
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Eshkoor, S.A.; Hamid, T.A.; Mun, C.Y.; Ng, C.K. Mild cognitive impairment and its management in older people. Clin. Interv. Aging 2015, 10, 687–693. [Google Scholar] [CrossRef] [PubMed]
- Ward, A.; Arrighi, H.M.; Michels, S.; Cedarbaum, J.M. Mild cognitive impairment: Disparity of incidence and prevalence estimates. Alzheimers Dement. 2012, 8, 14–21. [Google Scholar] [CrossRef] [PubMed]
- Nie, H.; Xu, Y.; Liu, B.; Zhang, Y.; Lei, T.; Hui, X.; Zhang, L.; Wu, Y. The prevalence of mild cognitive impairment about elderly population in china: A meta-analysis. Int. J. Geriatr. Psychiatry 2011, 26, 558–563. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.C. Clinical practice. Mild cognitive impairment. N. Engl. J. Med. 2011, 364, 2227–2234. [Google Scholar] [CrossRef] [PubMed]
- Van de Rest, O.; Geleijnse, J.M.; Kok, F.J.; van Staveren, W.A.; Dullemeijer, C.; Olderikkert, M.G.; Beekman, A.T.; de Groot, C.P. Effect of fish oil on cognitive performance in older subjects: A randomized, controlled trial. Neurology 2008, 71, 430–438. [Google Scholar] [CrossRef] [PubMed]
- Dangour, A.D.; Allen, E.; Elbourne, D.; Fasey, N.; Fletcher, A.E.; Hardy, P.; Holder, G.E.; Knight, R.; Letley, L.; Richards, M.; et al. Effect of 2-y n-3 long-chain polyunsaturated fatty acid supplementation on cognitive function in older people: A randomized, double-blind, controlled trial. Am. J. Clin. Nutr. 2010, 91, 1725–1732. [Google Scholar] [CrossRef] [PubMed]
- Witte, A.V.; Kerti, L.; Hermannstaedter, H.M.; Fiebach, J.B.; Schreiber, S.J.; Schuchardt, J.P.; Hahn, A.; Floeel, A. Long-chain omega-3 fatty acids improve brain function and structure in older adults. Cereb. Cortex 2014, 24, 3059–3068. [Google Scholar] [CrossRef] [PubMed]
- Kotani, S.; Sakaguchi, E.; Warashina, S.; Matsukawa, N.; Ishikura, Y.; Kiso, Y.; Sakakibara, M.; Yoshimoto, T.; Guo, J.; Yamashima, T. Dietary supplementation of arachidonic and docosahexaenoic acids improves cognitive dysfunction. Neurosci. Res. 2006, 56, 159–164. [Google Scholar] [CrossRef] [PubMed]
- Sinn, N.; Milte, C.M.; Street, S.J.; Buckley, J.D.; Coates, A.M.; Petkov, J.; Howe, P.R. Effects of n-3 fatty acids, epa v. Dha, on depressive symptoms, quality of life, memory and executive function in older adults with mild cognitive impairment: A 6-month randomised controlled trial. Br. J. Nutr. 2012, 107, 1682–1693. [Google Scholar] [CrossRef] [PubMed]
- Chiu, C.C.; Su, K.P.; Cheng, T.C.; Liu, H.C.; Chang, C.J.; Dewey, M.E.; Stewart, R.; Huang, S.Y. The effects of omega-3 fatty acids monotherapy in alzheimer’s disease and mild cognitive impairment: A preliminary randomized double-blind placebo-controlled study. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2008, 32, 1538–1544. [Google Scholar] [CrossRef] [PubMed]
- Quinn, J.F.; Raman, R.; Thomas, R.G.; Yurko-Mauro, K.; Nelson, E.B.; Van Dyck, C.; Galvin, J.E.; Emond, J.; Jack, C.R., Jr.; Weiner, M.; et al. Docosahexaenoic acid supplementation and cognitive decline in Alzheimer disease: A randomized trial. JAMA 2010, 304, 1903–1911. [Google Scholar] [CrossRef] [PubMed]
- Glass, C.K.; Saijo, K.; Winner, B.; Marchetto, M.C.; Gage, F.H. Mechanisms underlying inflammation in neurodegeneration. Cell 2010, 140, 918–934. [Google Scholar] [CrossRef] [PubMed]
- Trepanier, M.O.; Hopperton, K.E.; Orr, S.K.; Bazinet, R.P. N-3 polyunsaturated fatty acids in animal models with neuroinflammation: An update. Eur. J. Pharmacol. 2015, 785, 187–206. [Google Scholar] [CrossRef] [PubMed]
- Cederholm, T.; Salem, N., Jr.; Palmblad, J. Omega-3 fatty acids in the prevention of cognitive decline in humans. Adv. Nutr. 2013, 4, 672–676. [Google Scholar] [CrossRef] [PubMed]
- Serhan, C.N.; Chiang, N.; Van Dyke, T.E. Resolving inflammation: Dual anti-inflammatory and pro-resolution lipid mediators. Nat. Rev. Immunol. 2008, 8, 349–361. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.C.; Smith, G.E.; Waring, S.C.; Ivnik, R.J.; Tangalos, E.G.; Kokmen, E. Mild cognitive impairment: Clinical characterization and outcome. Arch. Neurol. 1999, 56, 303–308. [Google Scholar] [CrossRef] [PubMed]
- Fisk, H.L.; West, A.L.; Childs, C.E.; Burdge, G.C.; Calder, P.C. The use of gas chromatography to analyze compositional changes of fatty acids in rat liver tissue during pregnancy. J. Vis. Exp. 2014. [Google Scholar] [CrossRef] [PubMed]
- Food and Agriculture Organization. Fat and Fatty Acids in Human Nutrition; FAO: Rome, Italy, 2010. [Google Scholar]
- EFSA. Science opinion on dietary reference values for fats, including saturated fatty acids, polyunsaturated fatty acids, monounsaturated fatty acids, trans fatty acids, and cholesterol. EFSA J. 2010, 8, 1461. [Google Scholar]
- Geleijnse, J.M.; Giltay, E.J.; Kromhout, D. Effects of n-3 fatty acids on cognitive decline: A randomized, double-blind, placebo-controlled trial in stable myocardial infarction patients. Alzheimers Dement. 2012, 8, 278–287. [Google Scholar] [CrossRef] [PubMed]
- Kong, H.Y.; Cheng, D.M.; Pang, W.; Sun, S.D.; Liu, J.; Huang, C.Y.; Jiang, Y.G. Homocysteine levels and cognitive function scores measured with mmse and bcat of middle-aged and elderly subjects in Tianjin city. J. Nutr. Health Aging 2013, 17, 527–532. [Google Scholar] [CrossRef] [PubMed]
- Cheng, D.; Kong, H.; Pang, W.; Yang, H.; Lu, H.; Huang, C.; Jiang, Y. B vitamin supplementation improves cognitive function in the middle aged and elderly with hyperhomocysteinemia. Nutr. Neurosci. 2014, 19, 461–466. [Google Scholar] [CrossRef] [PubMed]
- Lee, L.K.; Shahar, S.; Chin, A.V.; Yusoff, N.A. Docosahexaenoic acid-concentrated fish oil supplementation in subjects with mild cognitive impairment (MCI): A 12-month randomised, double-blind, placebo-controlled trial. Psychopharmacology 2013, 225, 605–612. [Google Scholar] [CrossRef] [PubMed]
- Vakhapova, V.; Cohen, T.; Richter, Y.; Herzog, Y.; Korczyn, A.D. Phosphatidylserine containing omega-3 fatty acids may improve memory abilities in non-demented elderly with memory complaints: A double-blind placebo-controlled trial. Dement. Geriatr. Cogn. Disord 2010, 29, 467–474. [Google Scholar] [CrossRef] [PubMed]
- Otsuka, M. Analysis of dietary factors in Alzheimer’s disease: Clinical use of nutritional intervention for prevention and treatment of dementia. Nihon Ronen Igakkai Zasshi 2000, 37, 970–973. [Google Scholar] [CrossRef] [PubMed]
- Yehuda, S.; Rabinovtz, S.; Carasso, R.L.; Mostofsky, D.I. Essential fatty acids preparation (sr-3) improves alzheimer’s patients quality of life. Int. J. Neurosci. 1996, 87, 141–149. [Google Scholar] [CrossRef] [PubMed]
- Terano, T.; Fujishiro, S.; Ban, T.; Yamamoto, K.; Tanaka, T.; Noguchi, Y.; Tamura, Y.; Yazawa, K.; Hirayama, T. Docosahexaenoic acid supplementation improves the moderately severe dementia from thrombotic cerebrovascular diseases. Lipids 1999, 34, S345–S346. [Google Scholar] [CrossRef] [PubMed]
- Freund-Levi, Y.; Basun, H.; Cederholm, T.; Faxen-Irving, G.; Garlind, A.; Grut, M.; Vedin, I.; Palmblad, J.; Wahlund, L.O.; Eriksdotter-Jonhagen, M. Omega-3 supplementation in mild to moderate Alzheimer’s disease: Effects on neuropsychiatric symptoms. Int. J. Geriatr. Psychiatry 2008, 23, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Boston, P.F.; Bennett, A.; Horrobin, D.F.; Bennett, C.N. Ethyl-epa in Alzheimer’s disease—A pilot study. Prostaglandins Leukot. Essent. Fat. Acids 2004, 71, 341–346. [Google Scholar] [CrossRef] [PubMed]
- Freund-Levi, Y.; Eriksdotter-Jonhagen, M.; Cederholm, T.; Basun, H.; Faxen-Irving, G.; Garlind, A.; Vedin, I.; Vessby, B.; Wahlund, L.O.; Palmblad, J. Omega-3 fatty acid treatment in 174 patients with mild to moderate Alzheimer disease: Omegad study: A randomized double-blind trial. Arch. Neurol. 2006, 63, 1402–1408. [Google Scholar] [CrossRef] [PubMed]
- Grosso, G.; Pajak, A.; Marventano, S.; Castellano, S.; Galvano, F.; Bucolo, C.; Drago, F.; Caraci, F. Role of omega-3 fatty acids in the treatment of depressive disorders: A comprehensive meta-analysis of randomized clinical trials. PLoS ONE 2014, 9, e96905. [Google Scholar] [CrossRef] [PubMed]
- Serhan, C.N. Resolution phase of inflammation: Novel endogenous anti-inflammatory and proresolving lipid mediators and pathways. Annu. Rev. Immunol. 2007, 25, 101–137. [Google Scholar] [CrossRef] [PubMed]
- Serhan, C.N. Novel lipid mediators and resolution mechanisms in acute inflammation: To resolve or not? Am. J. Pathol. 2010, 177, 1576–1591. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Garcia, E.; Schulze, M.B.; Manson, J.E.; Meigs, J.B.; Albert, C.M.; Rifai, N.; Willett, W.C.; Hu, F.B. Consumption of (n-3) fatty acids is related to plasma biomarkers of inflammation and endothelial activation in women. J. Nutr. 2004, 134, 1806–1811. [Google Scholar] [PubMed]
- Hao, W.; Wong, O.Y.; Liu, X.; Lee, P.; Chen, Y.; Wong, K.K. Omega-3 fatty acids suppress inflammatory cytokine production by macrophages and hepatocytes. J. Pediatr. Surg. 2010, 45, 2412–2418. [Google Scholar] [CrossRef] [PubMed]
- Kiecolt-Glaser, J.K.; Belury, M.A.; Andridge, R.; Malarkey, W.B.; Hwang, B.S.; Glaser, R. Omega-3 supplementation lowers inflammation in healthy middle-aged and older adults: A randomized controlled trial. Brain Behav. Immun. 2012, 26, 988–995. [Google Scholar] [CrossRef] [PubMed]
- Sun, G.Y.; Shelat, P.B.; Jensen, M.B.; He, Y.; Sun, A.Y.; Simonyi, A. Phospholipases a2 and inflammatory responses in the central nervous system. Neuromol. Med. 2010, 12, 133–148. [Google Scholar] [CrossRef] [PubMed]
- Li, K.; Huang, T.; Zheng, J.; Wu, K.; Li, D. Effect of marine-derived n-3 polyunsaturated fatty acids on C-reactive protein, interleukin 6 and tumor necrosis factor alpha: A meta-analysis. PLoS ONE 2014, 9, e88103. [Google Scholar]
- Gomez-Pinilla, F. Brain foods: The effects of nutrients on brain function. Nat. Rev. Neurosci. 2008, 9, 568–578. [Google Scholar] [CrossRef] [PubMed]
- Akbar, M.; Calderon, F.; Wen, Z.; Kim, H.Y. Docosahexaenoic acid: A positive modulator of akt signaling in neuronal survival. Proc. Natl. Acad. Sci. USA 2005, 102, 10858–10863. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.; Hu, X.; Khan, N.; Yang, J.; Li, D. Effect of polyunsaturated fatty acids on homocysteine metabolism through regulating the gene expressions involved in methionine metabolism. Sci. World J. 2013, 2013, 931626. [Google Scholar] [CrossRef] [PubMed]
- Jump, D.B. Dietary polyunsaturated fatty acids and regulation of gene transcription. Curr. Opin. Lipidol. 2002, 13, 155–164. [Google Scholar] [CrossRef] [PubMed]
- Hopperton, K.E.; Trepanier, M.O.; Giuliano, V.; Bazinet, R.P. Brain omega-3 polyunsaturated fatty acids modulate microglia cell number and morphology in response to intracerebroventricular amyloid-beta 1-40 in mice. J. Neuroinflamm. 2016, 13, 257. [Google Scholar] [CrossRef] [PubMed]
| Variable | Placebo (n = 42) | n-3 PUFAs (n = 44) | t/X2 | p |
|---|---|---|---|---|
| Age (year) | 70.45 ± 6.82 2 | 71.75 ± 5.68 | 0.961 | 0.339 3 |
| Gender | 0.002 | 0.967 4 | ||
| Male | 25 | 26 | ||
| Female | 17 | 18 | ||
| Education level | 1.038 | 0.595 4 | ||
| Illiterate | 1 | 1 | ||
| Primary school | 11 | 16 | ||
| Junior high school and above | 30 | 27 | ||
| EPA (%) | 0.96 ± 0.59 | 0.80 ± 0.16 | −1.728 | 0.088 3 |
| DHA (%) | 1.62 ± 0.43 | 1.55 ± 0.39 | −0.698 | 0.487 3 |
| AA (%) | 0.14 ± 0.04 | 0.15 ± 0.03 | 0.875 | 0.384 3 |
| ALA (%) | 0.63 ± 0.17 | 0.68 ± 0.19 | −1.286 | 0.202 3 |
| LA (%) | 22.39 ± 3.26 | 22.34 ± 2.86 | −0.075 | 0.940 3 |
| BCAT | 33.17 ± 15.01 | 31.16 ± 15.41 | −0.612 | 0.542 3 |
| MMSE | 25.62 ± 1.68 | 25.11 ± 1.66 | −1.403 | 0.164 3 |
| Baseline | After Treatment | Difference | p | |
|---|---|---|---|---|
| EPA (%) | ||||
| Placebo (n = 42) | 0.96 ± 0.59 | 0.92 ± 0.58 2 | −0.05 ± 0.19 | <0.0001 3 |
| n-3 PUFAs (n = 44) | 0.80 ± 0.16 | 1.16 ± 0.56 | 0.36 ± 0.52 | |
| DHA (%) | ||||
| Placebo (n = 42) | 1.62 ± 0.43 | 1.36 ± 0.42 2 | −0.25 ± 0.43 | <0.0001 3 |
| n-3 PUFAs (n = 44) | 1.55 ± 0.39 | 1.89 ± 0.56 2 | 0.34 ± 0.42 | |
| AA (%) | ||||
| Placebo (n = 42) | 0.14 ± 0.04 | 0.15 ± 0.05 | −0.01 ± 0.05 | 0.066 |
| n-3 PUFAs (n = 44) | 0.15 ± 0.03 | 0.14 ± 0.04 | 0.01 ± 0.04 | |
| ALA (%) | ||||
| Placebo (n = 42) | 0.63 ± 0.17 | 0.65 ± 0.15 | 0.003 ± 0.12 | 0.582 |
| n-3 PUFAs (n = 44) | 0.68 ± 0.19 | 0.68 ± 0.19 | 0.02 ± 0.20 | |
| LA (%) | ||||
| Placebo (n = 42) | 22.39 ± 3.26 | 22.22 ± 3.02 | −0.17 ± 2.48 | 0.333 |
| n-3 PUFAs (n = 44) | 22.34 ± 2.86 | 21.67 ± 2.83 | −0.66 ± 2.15 | |
| Outcome Measure | Overall BCAT Score | p | ||
|---|---|---|---|---|
| Baseline | After Treatment | Difference | ||
| PS | ||||
| Placebo (n = 42) | 5.62 ± 3.84 | 6.43 ± 4.62 | 0.81 ± 2.83 | 0.0002 3 |
| n-3 PUFAs (n = 44) | 5.22 ± 4.40 | 8.84 ± 4.65 2 | 3.61 ± 3.69 | |
| MAE | ||||
| Placebo (n = 42) | 7.90 ± 5.33 | 8.70 ± 6.02 | 0.33 ± 3.58 | 0.055 |
| n-3 PUFAs (n = 44) | 7.09 ± 4.83 | 8.63 ± 4.60 | 2.09 ± 4.68 | |
| SIE | ||||
| Placebo (n = 42) | 6.29 ± 3.38 | 6.28 ± 2.48 | 0.00 ± 3.22 | 0.0002 3 |
| n-3 PUFAs (n = 44) | 4.46 ± 2.34 | 6.81 ± 3.23 2 | 2.45 ± 2.72 | |
| WM | ||||
| Placebo (n = 42) | 5.47 ± 3.80 | 6.85 ± 4.80 | 1.38 ± 2.66 | 0.0047 3 |
| n-3 PUFAs (n = 44) | 5.32 ± 2.92 | 8.63 ± 4.06 2 | 3.32 ± 3.45 | |
| RM | ||||
| Placebo (n = 42) | 7.52 ± 4.85 | 9.50 ± 5.16 | 1.98 ± 3.13 | 0.579 |
| n-3 PUFAs (n = 44) | 9.32 ± 7.69 | 10.86 ± 6.71 | 1.55 ± 3.96 | |
| Total | ||||
| Placebo (n = 42) | 33.17 ± 15.01 | 37.17 ± 16.85 | 4.00 ± 7.07 | <0.0001 3 |
| n-3 PUFAs (n = 44) | 31.16 ± 15.41 | 44.73 ± 13.87 2 | 13.57 ± 10.72 | |
| Baseline | After Treatment | Difference | p | |
|---|---|---|---|---|
| IL-6, pg/mL | ||||
| Placebo (n = 42) | 120.90 ± 41.60 | 109.26 ± 37.21 | −11.64 ± 42.28 | 0.018 3 |
| n-3 PUFAs (n = 44) | 120.60 ± 52.64 | 85.66 ± 53.01 2 | −34.94 ± 46.18 | |
| IL-10, ng/mL | ||||
| Placebo (n = 42) | 166.10 ± 70.54 | 152.43 ± 43.43 | −13.67 ± 67.74 | 0.649 |
| n-3 PUFAs (n = 44) | 136.42 ± 48.96 | 128.69 ± 37.53 | −7.73 ± 71.22 | |
| TNF-α, fmol/mL | ||||
| Placebo (n = 42) | 17.17 ± 7.98 | 15.43 ± 5.01 | −1.74 ± 8.15 | 0.027 3 |
| n-3 PUFAs (n = 44) | 19.00 ± 9.89 | 13.09 ± 7.86 2 | −5.91 ± 9.03 | |
| COX, U/L | ||||
| Placebo (n = 42) | 545.32 ± 146.12 | 539.92 ± 152.23 | −5.40 ± 169.98 | 0.259 |
| n-3 PUFAs (n = 44) | 543.34 ± 146.81 | 579.94 ± 125.21 | 36.59 ± 172.64 | |
| LOX, IU/L | ||||
| Placebo (n = 42) | 128.83 ± 25.95 | 131.87 ± 21.10 | 3.04 ± 23.47 | 0.558 |
| n-3 PUFAs (n = 44) | 118.30 ± 26.14 | 124.61 ± 24.27 | 6.31 ± 27.63 | |
| sPLA2, ng/L | ||||
| Placebo (n = 42) | 944.00 ± 201.36 | 940.47 ± 233.43 | −3.53 ± 267.60 | 0.052 3 |
| n-3 PUFAs (n = 44) | 1002.55 ± 204.43 | 888.97 ± 211.82 2 | −113.58 ± 249.81 | |
© 2017 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bo, Y.; Zhang, X.; Wang, Y.; You, J.; Cui, H.; Zhu, Y.; Pang, W.; Liu, W.; Jiang, Y.; Lu, Q. The n-3 Polyunsaturated Fatty Acids Supplementation Improved the Cognitive Function in the Chinese Elderly with Mild Cognitive Impairment: A Double-Blind Randomized Controlled Trial. Nutrients 2017, 9, 54. https://doi.org/10.3390/nu9010054
Bo Y, Zhang X, Wang Y, You J, Cui H, Zhu Y, Pang W, Liu W, Jiang Y, Lu Q. The n-3 Polyunsaturated Fatty Acids Supplementation Improved the Cognitive Function in the Chinese Elderly with Mild Cognitive Impairment: A Double-Blind Randomized Controlled Trial. Nutrients. 2017; 9(1):54. https://doi.org/10.3390/nu9010054
Chicago/Turabian StyleBo, Yacong, Xueyuan Zhang, Youli Wang, Jie You, Han Cui, Yiwei Zhu, Wei Pang, Wei Liu, Yugang Jiang, and Quanjun Lu. 2017. "The n-3 Polyunsaturated Fatty Acids Supplementation Improved the Cognitive Function in the Chinese Elderly with Mild Cognitive Impairment: A Double-Blind Randomized Controlled Trial" Nutrients 9, no. 1: 54. https://doi.org/10.3390/nu9010054
APA StyleBo, Y., Zhang, X., Wang, Y., You, J., Cui, H., Zhu, Y., Pang, W., Liu, W., Jiang, Y., & Lu, Q. (2017). The n-3 Polyunsaturated Fatty Acids Supplementation Improved the Cognitive Function in the Chinese Elderly with Mild Cognitive Impairment: A Double-Blind Randomized Controlled Trial. Nutrients, 9(1), 54. https://doi.org/10.3390/nu9010054




