A Comparison by Milk Feeding Method of the Nutrient Intake of a Cohort of Australian Toddlers
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design
2.2. Setting and Recruitment
2.3. Ethical Considerations
2.4. Collection and Handling of Dietary Data
2.5. Statistical Analysis
3. Results
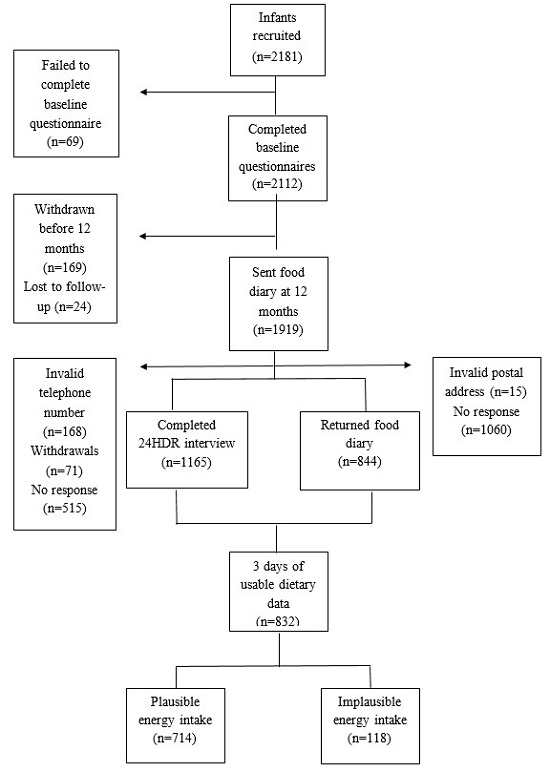
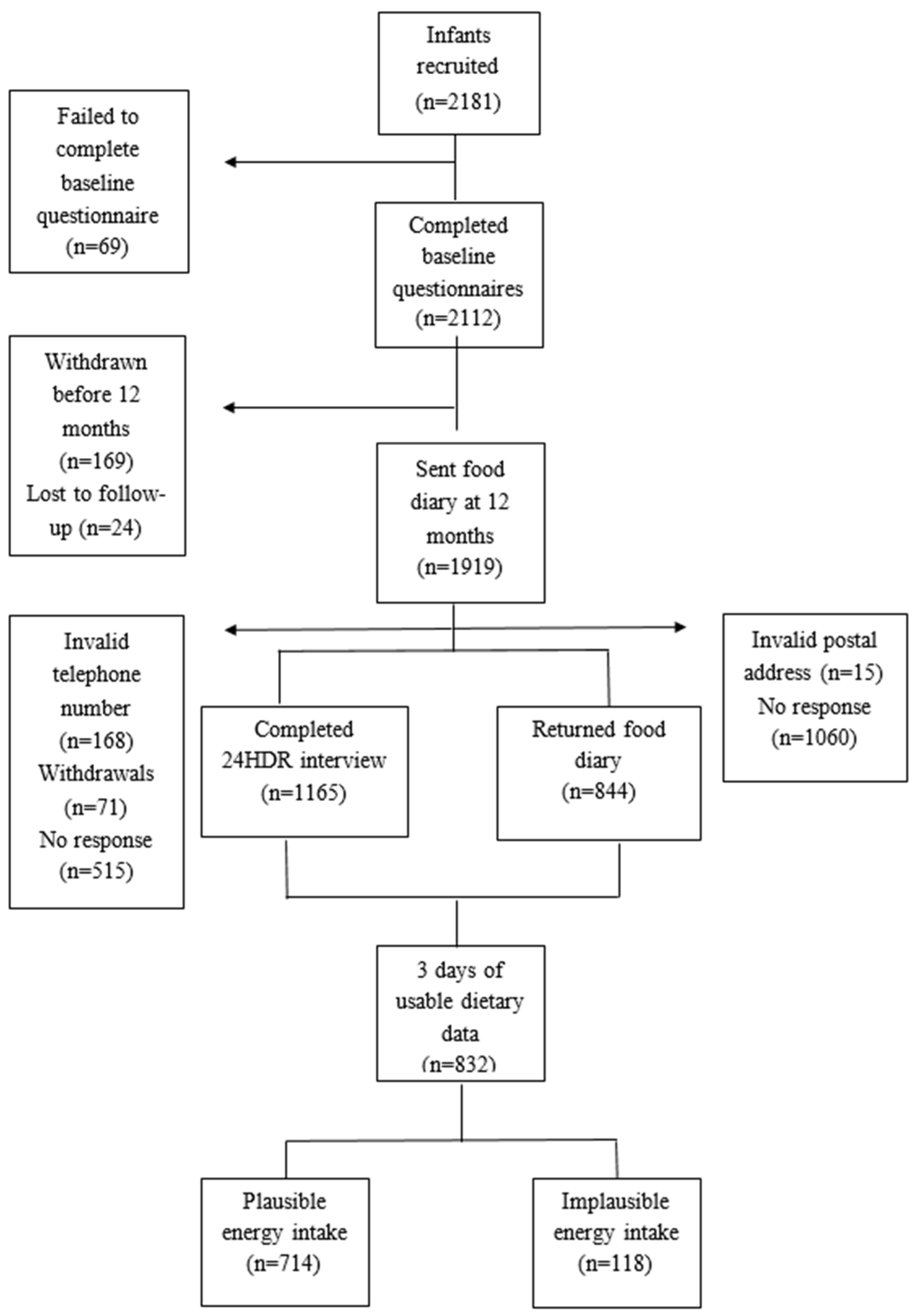
3.1. Participant Characteristics
3.2. Nutrient Intake of Children
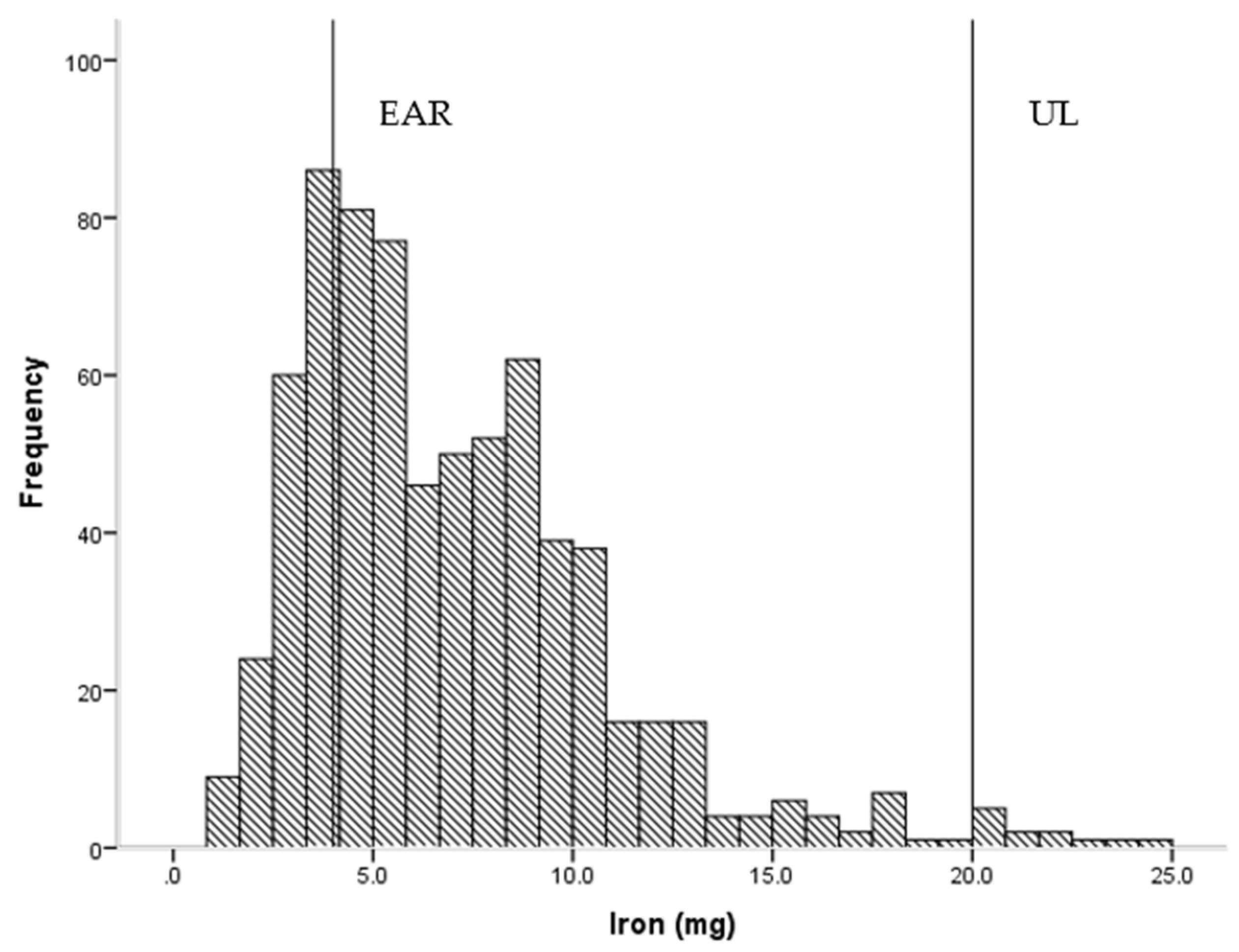
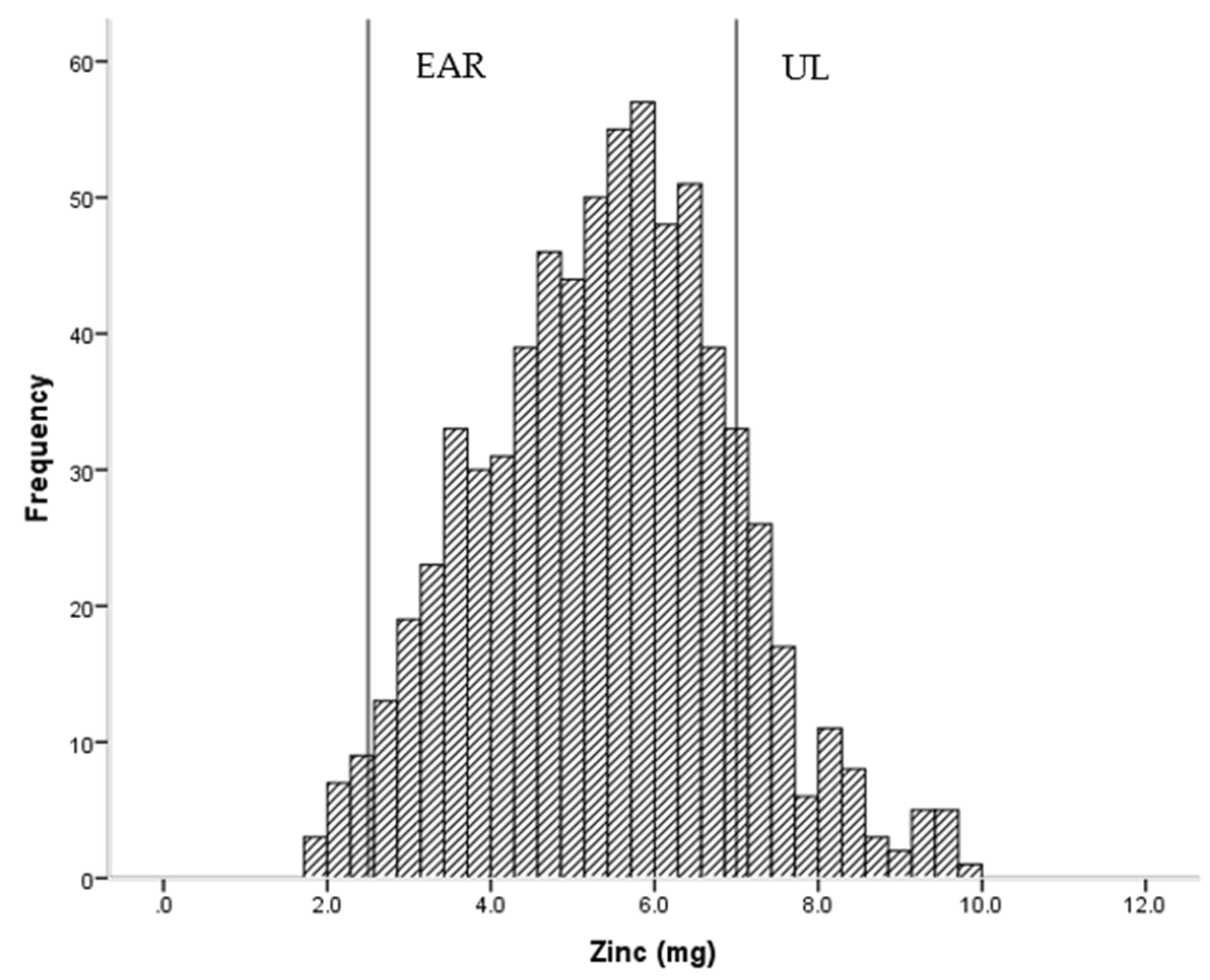
3.2.1. Comparison of Nutrient Intakes with Nutrient Reference Values
3.2.2. Comparison of Nutrient Intakes by Milk Feeding Method
3.3. Relationship of Milk Feeding Method and Adequacy of Selected Nutrients
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| AIFG | Australian Infant Feeding Guidelines |
| CI | Confidence interval |
| EAR | Estimated average requirement |
| IRSAD | Index of Relative Socio-Economic Advantage and Disadvantage |
| NRV | Nutrient reference value |
| OR | Odds ratio |
| RE | Retinol equivalents |
| UL | Upper level of intake |
Appendix A
References
- National Health and Medical Research Council. Infant Feeding Guidelines; National Health and Medical Research Council: Canberra, Australia, 2012.
- WHO/UNICEF. Global Strategy for Infant and Young Child Feeding; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Victora, C.G.; Bahl, R.; Barros, A.J.; França, G.V.; Horton, S.; Krasevec, J.; Murch, S.; Sankar, M.J.; Walker, N.; Rollins, N.C.; et al. Breastfeeding in the 21st century: Epidemiology, mechanisms, and lifelong effect. Lancet 2016, 387, 475–490. [Google Scholar] [CrossRef]
- Australian Institute of Health and Welfare. 2010 Australian National Infant Feeding Survey: Indicator Results; Cat. No. PHE 156; AIHW: Canberra, Australia, 2011.
- Australian Bureau of Statistics and Food Standards Australia and New Zealand. 4364.0.55.008—Australian Health Survey: Usual Nutrient Intakes, 2011–2012; Australian Bureau of Statistics: Canberra, Australia, 2015.
- Commonwealth Scientific Industrial Research Organisation (CSIRO) Preventative Health National Research Flagship and the University of South Australia. 2007 Australian National Children’s Nutrition and Physical Activity Survey: Main Findings; Commonwealth of Australia: Canberra, Australia, 2008.
- Conn, J.A.; Davies, M.J.; Walker, R.B.; Moore, V.M. Food and nutrient intakes of 9-month-old infants in Adelaide, Australia. Public Health Nutr. 2009, 12, 2448–2456. [Google Scholar] [CrossRef] [PubMed]
- Atkins, L.A.; McNaughton, S.A.; Campbell, K.J.; Szymlek-Gay, E.A. Iron intakes of Australian infants and toddlers: Findings from the Melbourne Infant Feeding, Activity and Nutrition Trial (InFANT) Program. Br. J. Nutr. 2016, 115, 285–293. [Google Scholar] [CrossRef] [PubMed]
- Byrne, R.; Magarey, A.; Daniels, L. Food and beverage intake in Australian children aged 12–16 months participating in the NOURISH and SAIDI studies. Aust. N. Z. J. Public Health 2014, 38, 326–331. [Google Scholar] [CrossRef] [PubMed]
- Lioret, S.; Cameron, A.J.; McNaughton, S.A.; Crawford, D.; Spence, A.C.; Hesketh, K.; Campbell, K.J. Association between maternal education and diet of children at 9 months is partially explained by mothers’ diet. Matern. Child Nutr. 2015, 11, 936–947. [Google Scholar] [CrossRef] [PubMed]
- Kavian, F.; Scott, J.; Perry, R.; Byrne, R.; Magarey, A. Assessing dietary intake and growth of infants. Matern. Paediatr. Nutr. J. 2015, 1, 101. [Google Scholar]
- Webb, K.L.; Lahti-Koski, M.; Rutishauser, I.; Hector, D.J.; Knezevic, N.; Gill, T.; Peat, J.K.; Leeder, S.R.; CAPS Team. Consumption of ‘extra’ foods (energy-dense, nutrient-poor) among children aged 16–24 months from western Sydney, Australia. Public Health Nutr. 2007, 9, 1035. [Google Scholar] [CrossRef]
- Butte, N.F.; Fox, M.K.; Briefel, R.R.; Siega-Riz, A.M.; Dwyer, J.T.; Deming, D.M.; Reidy, K.C. Nutrient intakes of US infants, toddlers, and preschoolers meet or exceed dietary reference intakes. J. Am. Diet. Assoc. 2010, 110, S27–S37. [Google Scholar] [CrossRef] [PubMed]
- Lennox, A.; Sommerville, J.; Ong, K.; Henderson, H.; Allen, R. Diet and Nutrition Survey of Infants and Young Children, 2011, 2013. Available online: http://webarchive.nationalarchives.gov.uk/20130402145952/http://transparency.dh.gov.uk/2013/03/13/dnsiyc-2011/ (accessed on 18 March 2016).
- Smithers, L.G.; Brazionis, L.; Golley, R.K.; Mittinty, M.N.; Northstone, K.; Emmett, P.; McNaughton, S.A.; Campbell, K.J.; Lynch, J.W. Associations between dietary patterns at 6 and 15 months of age and sociodemographic factors. Eur. J. Clin. Nutr. 2012, 66, 658–666. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council and Ministry of Health. Nutrient Reference Values for Australia and New Zealand; NHMRC: Canberra, Australia, 2005.
- Do, L.; Scott, J.; Thomson, W.; Stamm, J.W.; Rugg-Gunn, A.J.; Levy, S.M.; Wong, C.; Devenish, G.; Ha, D.H.; Spencer, A.J. Common risk factor approach to address socioeconomic inequality in the oral health of preschool children—A prospective cohort study. BMC Public Health 2014, 14, 429. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. 4363.0.55.001—Australian Health Survey: Users’ Guide, 2011–2013. 24-h Dietary Recall 2014. Available online: http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/0D6B1FE95EAB8FF3CA257CD2001CA113?opendocument (accessed on 18 March 2016).
- Food Standards Australia and New Zealand. Ausnut 2011–2013. Australian Food, Supplement and Nutrient Database 2015. Available online: http://www.foodstandards.gov.au/science/monitoringnutrients/ausnut/pages/default.aspx (accessed on 18 November 2015).
- Kent, J.C.; Mitoulas, L.; Cox, D.B.; Owens, R.A.; Hartmann, P.E. Breast volume and milk production during extended lactation in women. Exp. Physiol. 1999, 84, 435–447. [Google Scholar] [CrossRef] [PubMed]
- Scheil, W.; Jolly, K.; Scott, J.; Catcheside, B.; Sage, L.; Kennare, R. Pregnancy Outcome in South Australia 2013; Pregnancy Outcome Unit SA Health, Ed.; Government of South Australia: Adelaide, Australia, 2015.
- World Health Organization. International Code of Marketing of Breast-Milk Substitutes; WHO: Geneva, Switzerland, 1981. [Google Scholar]
- Berry, N.J.; Jones, S.C.; Iverson, D. Toddler milk advertising in Australia: Infant formula advertising in disguise? Australas. Market. J. 2012, 20, 24–27. [Google Scholar] [CrossRef]
- Cattaneo, A.; Pani, P.; Carletti, C.; Guidetti, M.; Mutti, V.; Guidetti, C.; Knowles, A. Advertisements of follow-on formula and their perception by pregnant women and mothers in Italy. Arch. Dis. Child. 2015, 100, 323–328. [Google Scholar] [CrossRef] [PubMed]
- Department of Health. Dietary Reference Values for Food Energy and Nutrients for the United Kingdom; HMSO: London, UK, 1991.
- Mcmillan, J.A.; Landaw, S.A.; Oski, F.A. Iron sufficiency in breast-fed infants and the availability of iron from human milk. Pediatrics 1976, 58, 686–691. [Google Scholar] [PubMed]
- Male, C.; Persson, L.A.; Freeman, V.; Guerra, A.; van’t Hof, M.A.; Haschke, F.; Euro-Growth Iron Study Group. Prevalence of iron deficiency in 12-mo-old infants from 11 European areas and influence of dietary factors on iron status (Euro-Growth study). Acta Paediatr. 2001, 90, 492–498. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council. Eat for Health Educator Guide. National Health and Medical Research Council: Canberra, Australia, 2013. Available online: https://www.nhmrc.gov.au/_files_nhmrc/publications/attachments/n55b_educator_guide_140321.pdf (accessed on 26 June 2016). [Google Scholar]
- Piernas, C.; Miles, D.R.; Deming, D.M.; Reidy, K.C.; Popkin, B.M. Estimating usual intakes mainly affects the micronutrient distribution among infants, toddlers and pre-schoolers from the 2012 Mexican National Health and Nutrition Survey. Public Health Nutr. 2016, 19, 1017–1026. [Google Scholar] [CrossRef] [PubMed]
| Total | Plausible | Implausible | |||||
|---|---|---|---|---|---|---|---|
| (n = 832) | (n = 714) | (n = 118) | |||||
| Maternal characteristics | n | % | n | % | n | % | p a |
| Maternal age at birth (years) | |||||||
| <25 | 74 | 8.9 | 62 | 8.7 | 12 | 10.3 | 0.583 |
| 25–29 | 259 | 31.2 | 227 | 31.9 | 32 | 27.4 | |
| ≥30 | 496 | 59.8 | 423 | 59.4 | 73 | 62.4 | |
| Maternal education completed | |||||||
| School/vocational | 358 | 43.4 | 310 | 43.7 | 48 | 41.0 | 0.585 |
| Some university and above | 468 | 56.7 | 399 | 56.3 | 69 | 59.0 | |
| IRSAD score b | |||||||
| Deciles 1–2 | 120 | 14.5 | 104 | 14.7 | 16 | 13.7 | 0.941 |
| Deciles 3–4 | 175 | 21.2 | 147 | 20.7 | 28 | 23.9 | |
| Deciles 5–6 | 172 | 20.8 | 147 | 20.7 | 25 | 21.4 | |
| Deciles 7–8 | 161 | 19.5 | 140 | 19.7 | 21 | 17.9 | |
| Deciles 9–10 | 198 | 24.0 | 171 | 24.1 | 27 | 23.1 | |
| Mother’s country of birth | |||||||
| Australia and N. Zealand | 613 | 74.1 | 519 | 73.1 | 94 | 80.3 | 0.061 |
| Asia—other | 57 | 6.9 | 35 | 4.8 | 5 | 1.7 | |
| India | 50 | 6.0 | 47 | 6.6 | 3 | 2.6 | |
| China | 36 | 4.4 | 34 | 3.2 | 2 | 6.8 | |
| UK | 31 | 3.7 | 23 | 7.3 | 8 | 4.3 | |
| Other | 40 | 4.8 | 35 | 4.7 | 5 | 4.3 | |
| Maternal BMI c (kg/m2) | |||||||
| <25 | 476 | 60.6 | 413 | 60.8 | 63 | 58.9 | 0.217 |
| 25–29.99 | 170 | 21.6 | 151 | 22.2 | 19 | 17.8 | |
| >30 | 140 | 17.8 | 115 | 16.9 | 25 | 23.4 | |
| Parity | |||||||
| Primiparous | 388 | 48.2 | 336 | 48.7 | 52 | 45.2 | 0.489 |
| Multiparous | 417 | 51.8 | 354 | 51.3 | 63 | 54.8 | |
| Child characteristics | |||||||
| Child age (mean SD) | 13.1 | 0.8 | 13.1 | 0.8 | 13.0 | 0.7 | 0.660 d |
| Infant sex | |||||||
| Boy | 455 | 54.7 | 395 | 55.3 | 60 | 50.8 | 0.366 |
| Girl | 377 | 45.3 | 319 | 44.7 | 58 | 49.2 | |
| Milk feeding method | |||||||
| Breastmilk | 219 | 26.3 | 201 | 28.3 | 18 | 15.3 | <0.001 |
| Breastmilk and formula | 68 | 8.2 | 59 | 8.3 | 9 | 7.6 | |
| Infant formula | 314 | 37.7 | 275 | 38.5 | 39 | 33.1 | |
| Other | 231 | 27.8 | 179 | 25.1 | 52 | 44.1 | |
| Average Intake/Day | Mean | SD | 25 | 75 | EAR | <EAR% | UL | >UL% |
|---|---|---|---|---|---|---|---|---|
| Total mass (kg) | 1179 | 393 | 993 | 1322 | ||||
| Energy (kJ) | 3803 | 714 | 3297 | 4378 | ||||
| Protein (g) | 36 | 11 | 28 | 44 | 12.0 | 0.0 | ||
| Total carbohydrate (g) | 107 | 23 | 89 | 123 | ||||
| Sugar (g) | 63 | 17 | 51 | 73 | ||||
| Total fat (g) | 36 | 9 | 29 | 42 | ||||
| Saturated fat (g) | 16.5 | 5.1 | 12.8 | 20.1 | ||||
| Polyunsaturated fat (g) | 4.2 | 1.6 | 3.1 | 5.0 | ||||
| Monounsaturated fat (g) | 12.3 | 3.4 | 10.0 | 14.3 | ||||
| Dietary fibre (g) | 9.6 | 4.0 | 6.7 | 11.8 | ||||
| Water (g) | 1013 | 386 | 809 | 1100 | ||||
| Sodium (mg) | 725 | 324 | 487 | 916 | 1000 | 18.2 | ||
| Potassium (mg) | 1467 | 433 | 1171 | 1745 | ||||
| Calcium (mg) | 650 | 235 | 481 | 812 | 360 | 12.6 | 2500 | 0.0 |
| Phosphorous (mg) | 736 | 229 | 573 | 888 | 380 | 6.3 | 3000 | 0.0 |
| Magnesium (mg) | 137 | 38 | 110 | 164 | 65 | 2.0 | ||
| Iron (mg) | 7.1 | 4.0 | 4.2 | 9.0 | 4 | 22.5 | 20 | 1.5 |
| Zinc (mg) | 5.4 | 1.5 | 4.4 | 6.4 | 2.5 | 2.2 | 7 | 14.1 |
| Vitamin A RE b (µg) | 726 | 492 | 487 | 851 | 210 | 0.4 | NA c | |
| Thiamin (mg) | 0.8 | 0.5 | 0.5 | 1.0 | 0.4 | 14.4 | ||
| Riboflavin (mg) | 1.4 | 0.6 | 1.0 | 1.8 | 0.4 | 2.1 | ||
| Niacin equivalents (mg) | 16.6 | 5.5 | 12.8 | 19.8 | 5 | 0.0 | NA d | |
| Folate (µg) | 321 | 130 | 226 | 404 | 120 | 3.1 | NA d | |
| Vitamin C (mg) | 61 | 46 | 36 | 80 | 25 | 14.0 |
| Milk Feeding Method | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Breastmilk (n = 201) | Combination—Breastmilk & Formula § (n = 59) | Formula § (n = 275) | Other (n = 179) | ||||||||||||
| Average intake/day | Mean | SD | % CF | % BM | Mean | SD | % CF | % BM | % F | Mean | SD | % CF | % F | Mean | SD |
| Total mass (g) | 1102 a | 263 | 67 | 33 | 1214 | 1047 | 58 | 21 | 21 | 1186 | 264 | 62 | 38 | 1240 a | 253 |
| Energy (kJ) | 3708 a | 747 | 72 | 28 | 3557 b | 783 | 62 | 20 | 18 | 3723 c | 656 | 66 | 34 | 4111 a,b,c | 646 |
| Protein (g) | 33 a | 10 | 84 | 16 | 30 b,c | 10 | 73 | 12 | 15 | 35 b,d | 9 | 74 | 26 | 45 a,c,d | 9 |
| Total carbohydrate (g) | 100 a,b | 25 | 75 | 25 | 102 | 21 | 65 | 16 | 19 | 110 a | 21 | 66 | 34 | 111 b | 22 |
| Total fat (g) | 38 a | 9 | 60 | 40 | 35 | 12 | 49 | 30 | 21 | 33 a,b | 8 | 58 | 42 | 38 b | 9 |
| Na (mg) | 700 a,b | 393 | 89 | 11 | 546 a,c,d | 183 | 79 | 8 | 13 | 687 c,e | 279 | 78 | 22 | 872 b,d,e | 284 |
| Ca (mg) | 467 a,b | 175 | 72 | 28 | 522 c,d | 191 | 50 | 17 | 33 | 703 a,c,e | 177 | 50 | 50 | 815 b,d,e | 229 |
| Fe (mg) | 5.0 a,b | 3.3 | 97 | 3 | 7.8 a,c,d | 4.3 | 68 | 1 | 31 | 9.3 b,c,e | 3.1 | 50 | 50 | 5.9 d,e | 4.2 |
| Zinc (mg) | 4.2 a,b,c | 1.2 | 84 | 16 | 5.1 a,d,e | 2 | 63 | 10 | 27 | 6.2 b,d,f | 1.2 | 56 | 44 | 5.6 c,e,f | 1.2 |
| Thiamin (mg) | 0.7 a,b | 0.5 | 89 | 11 | 0.7 c | 0.3 | 72 | 6 | 22 | 0.9 a,c | 0.4 | 64 | 36 | 0.9 b | 0.6 |
| Vitamin C (mg) | 52 a,b,c | 21 | 62 | 38 | 69 a,d | 30 | 44 | 20 | 36 | 83 b,e | 58 | 40 | 60 | 36 c,d,e | 30 |
| Total (n = 714) | Breastmilk (n = 201) | Formula (n = 334) | Other (n = 179) | |||||
|---|---|---|---|---|---|---|---|---|
| Calcium | ||||||||
| Number (%) below EAR | 90 | (12.6) | 64 | (31.8) | 19 | (5.7) | 7 | (3.9) |
| Adjusted # odds ratio (95% CI) | Ref | 0.13 | (0.07–0.22) | 0.09 | (0.04–0.19) | |||
| Iron | ||||||||
| Number (%) below EAR | 161 | (22.5) | 98 | (48.8) | 11 | (3.3) | 52 | (29.1) |
| Adjusted # odds ratio (95% CI) | Ref | 0.04 | (0.02–0.07) | 0.42 | (0.27–0.64) | |||
| Thiamin | ||||||||
| Number (%) below EAR | 103 | (14.4) | 62 | (30.8) | 19 | (5.7) | 22 | (12.3) |
| Adjusted # odds ratio (95% CI) | Ref | 0.13 | (0.07–0.23) | 0.30 | (0.17–0.51) | |||
| Vitamin C | ||||||||
| Number (%) below EAR | 100 | (14.0) | 15 | (7.5) | 6 | (1.8) | 79 | (44.1) |
| Adjusted # odds ratio (95% CI) | Ref | 0.23 | (0.09–0.59) | 9.64 | (5.27–17.62) | |||
| Zinc | ||||||||
| Number (%) above UL | 101 | (14.1) | 4 | (2.0) | 75 | (22.5) | 22 | (12.3) |
| Adjusted # odds ratio (95% CI) | Ref | 13.5 | (4.85–37.66) | 6.35 | (2.14–18.85) | |||
| Sodium | ||||||||
| Number (%) above UL | 130 | (18.2) | 33 | (16.4) | 45 | (13.5) | 52 | (29.1) |
| Adjusted # odds ratio (95% CI) | Ref | 0.79 | (0.49–1.29) | 2.10 | (1.28–3.44) | |||
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scott, J.; Davey, K.; Ahwong, E.; Devenish, G.; Ha, D.; Do, L. A Comparison by Milk Feeding Method of the Nutrient Intake of a Cohort of Australian Toddlers. Nutrients 2016, 8, 501. https://doi.org/10.3390/nu8080501
Scott J, Davey K, Ahwong E, Devenish G, Ha D, Do L. A Comparison by Milk Feeding Method of the Nutrient Intake of a Cohort of Australian Toddlers. Nutrients. 2016; 8(8):501. https://doi.org/10.3390/nu8080501
Chicago/Turabian StyleScott, Jane, Kristina Davey, Ellen Ahwong, Gemma Devenish, Diep Ha, and Loc Do. 2016. "A Comparison by Milk Feeding Method of the Nutrient Intake of a Cohort of Australian Toddlers" Nutrients 8, no. 8: 501. https://doi.org/10.3390/nu8080501
APA StyleScott, J., Davey, K., Ahwong, E., Devenish, G., Ha, D., & Do, L. (2016). A Comparison by Milk Feeding Method of the Nutrient Intake of a Cohort of Australian Toddlers. Nutrients, 8(8), 501. https://doi.org/10.3390/nu8080501