Water and Beverage Consumption: Analysis of the Australian 2011–2012 National Nutrition and Physical Activity Survey
Abstract
:1. Introduction
2. Materials and Methods
2.1. Respondents and Water Intake Data Collection
2.2. Water, Moisture, and Food Sources
2.3. Anthropometry, Demographic, and Other Characters
2.4. Dietary Factors
2.5. Misreporting
2.6. Statistical Analysis
3. Results
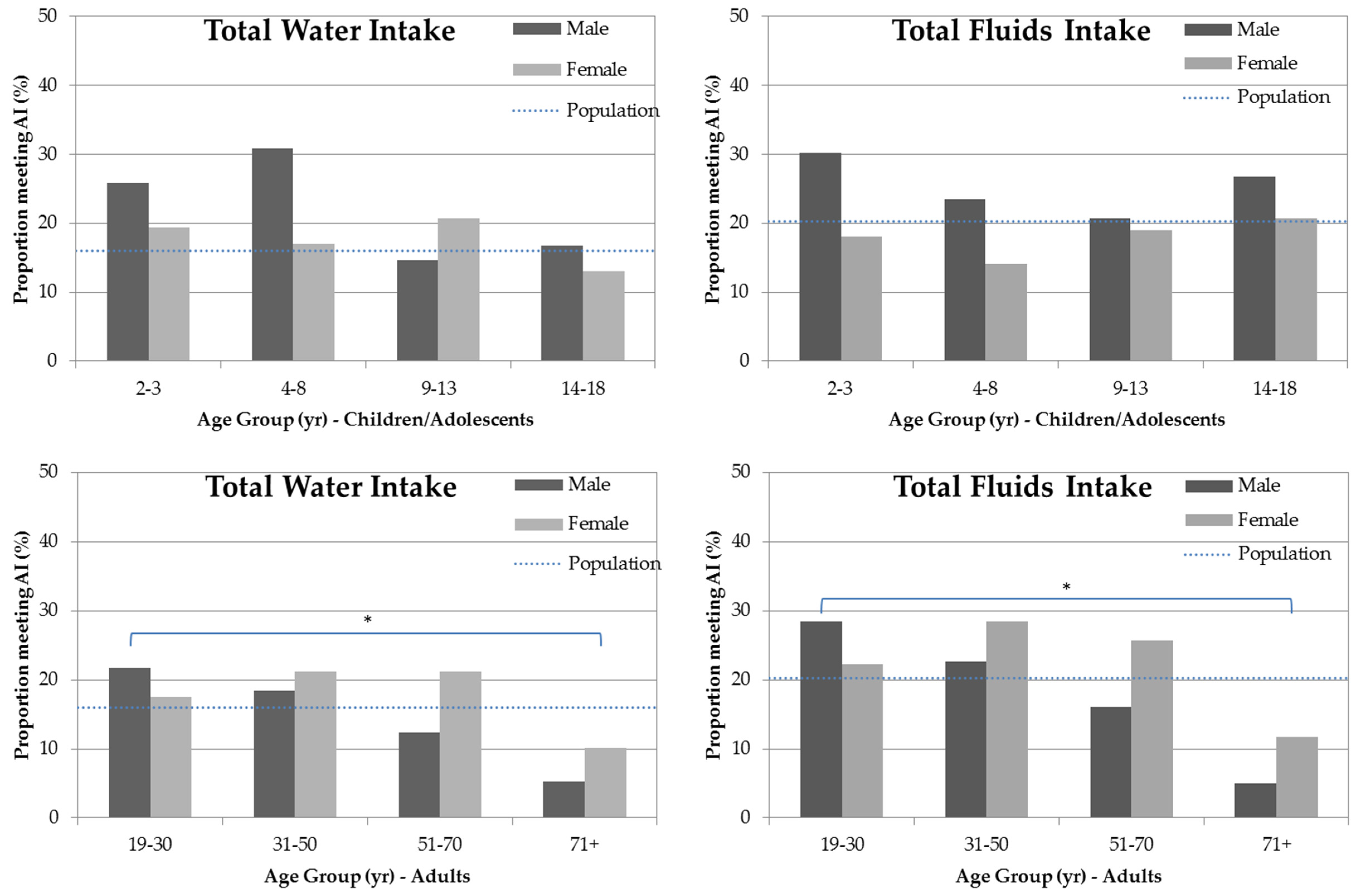
3.1. Total Water Intake
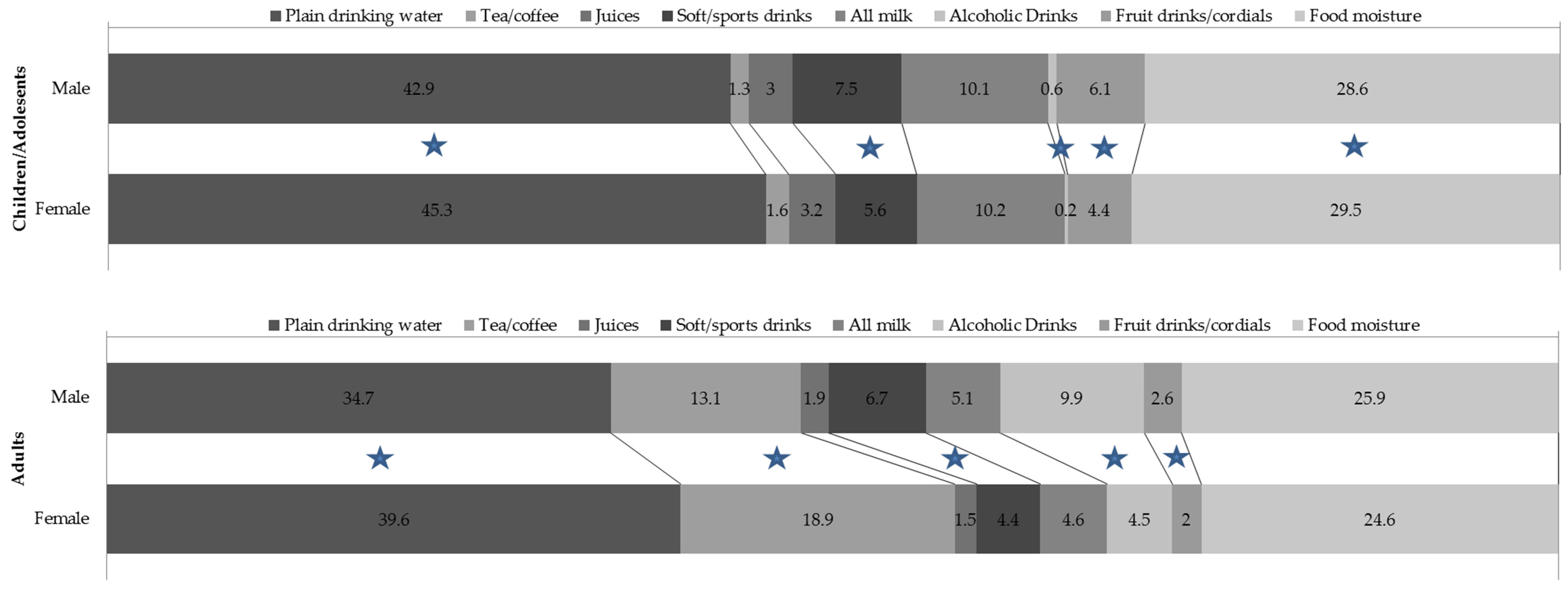
3.2. Sources of Water
3.3. Plain Drinking Water
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Institute of Medicine. DRI, Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate; National Academy Press: Washington, DC, USA, 2005. [Google Scholar]
- National Health and Medical Research Council. Nutrients-Water. Available online: https://www.nrv.gov.au/nutrients/water (accessed on 17 July 2016).
- Jequier, E.; Constant, F. Water as an essential nutrient: The physiological basis of hydration. Eur. J. Clin. Nutr. 2010, 64, 115–123. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, L.E. Challenges of linking chronic dehydration and fluid consumption to health outcomes. Nutr. Rev. 2012, 70, S121–S127. [Google Scholar] [CrossRef] [PubMed]
- Masento, N.A.; Golightly, M.; Field, D.T.; Butler, L.T.; van Reekum, C.M. Effects of hydration status on cognitive performance and mood. Br. J. Nutr. 2014, 111, 1841–1852. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Water for Health-Who Guidelines for Drinking-Water Quality. Available online: http://www.who.int/water_sanitation_health/WHS_WWD2010_guidelines_2010_6_en.pdf?ua=1 (accessed on 18 July 2016).
- Drewnowski, A.; Rehm, C.D.; Constant, F. Water and beverage consumption among adults in the United States: Cross-sectional study using data from NHANES 2005–2010. BMC Public Health 2013, 13. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Rehm, C.D.; Constant, F. Water and beverage consumption among children age 4–13 years in the United States: Analyses of 2005–2010 NHANES data. Nutr. J. 2013, 12. [Google Scholar] [CrossRef] [PubMed]
- Kant, A.K.; Graubard, B.I.; Atchison, E.A. Intakes of plain water, moisture in foods and beverages, and total water in the adult us population—Nutritional, meal pattern, and body weight correlates: National health and nutrition examination surveys 1999–2006. Am. J. Clin. Nutr. 2009, 90, 655–663. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, L.; Walton, J.; Flynn, A. Water intakes and dietary sources of a nationally representative sample of Irish adults. J. Hum. Nutr. Diet. 2014, 27, 550–556. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council. Eat for Health-Educator Guide; National health and Medical Research Council: Canberra, Australia, 2013.
- An, R.; McCaffrey, J. Plain water consumption in relation to energy intake and diet quality among us adults, 2005–2012. J. Hum. Nutr. Diet. 2016, 29, 624–632. [Google Scholar] [CrossRef] [PubMed]
- Zheng, M.B.; Rangan, A.; Olsen, N.J.; Andersen, L.B.; Wedderkopp, N.; Kristensen, P.; Grontved, A.; Ried-Larsen, M.; Lempert, S.M.; Allman-Farinelli, M.; et al. Substituting sugar-sweetened beverages with water or milk is inversely associated with body fatness development from childhood to adolescence. Nutrition 2015, 31, 38–44. [Google Scholar] [CrossRef] [PubMed]
- Stookey, J.D.; Constant, F.; Gardner, C.D.; Popkin, B.M. Replacing sweetened caloric beverages with drinking water is associated with lower energy intake. Obesity (Silver Spring) 2007, 15, 3013–3022. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. Australian Health Survey: User’s Guide, 2011–2013; Australian Government Publishing Service; Australian Bureau of Statistics: Canberra, Australia, 2013.
- Bornhorst, C.; Bel-Serrat, S.; Pigeot, I.; Huybrechts, I.; Ottavaere, C.; Sioen, I.; de Henauw, S.; Mouratidou, T.; Mesana, M.I.; Westerterp, K.; et al. Validity of 24-h recalls in (pre-)school aged children: Comparison of proxy-reported energy intakes with measured energy expenditure. Clin. Nutr. 2014, 33, 79–84. [Google Scholar] [CrossRef] [PubMed]
- Food Standards Australia New Zealand. Australian Food, Supplement and Nutrient Database (Ausnut); Food Standards Australia New Zealand: Canberra, Australia, 2014.
- World Health Organization. Length/Height-for-Age, Weight-for-Age, Weight-for-Length, Weight-for-Height and Body Mass Index-for-Age: Methods and Development; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- Australian Bureau of Statistics. Australian Health Survey: Nutrition First Results-Foods and Nutrients, 2011–2012; Australian Bureau of Statistics: Canberra, Australia, 2014.
- National Health and Medical Research Council. Australian Guide to Healthy Eating; National Health and Medical Research Council: Canberra, Australia, 2013.
- Rangan, A.; Allman-Farinelli, M.; Donohoe, E.; Gill, T. Misreporting of energy intake in the 2007 Australian children’s survey: Differences in the reporting of food types between plausible, under- and over-reporters of energy intake. J. Hum. Nutr. Diet. 2014, 27, 450–458. [Google Scholar] [CrossRef] [PubMed]
- Gemming, L.; Jiang, Y.; Swinburn, B.; Utter, J.; Mhurchu, C.N. Under-reporting remains a key limitation of self-reported dietary intake: An analysis of the 2008/2009 New Zealand adult nutrition survey. Eur. J. Clin. Nutr. 2014, 68, 259–264. [Google Scholar] [CrossRef] [PubMed]
- Vanrullen, I.B.; Volatier, J.L.; Bertaut, A.; Dufour, A.; Dallongeville, J. Characteristics of energy intake under-reporting in french adults. Br. J. Nutr. 2014, 111, 1292–1302. [Google Scholar] [CrossRef] [PubMed]
- Black, A.E. The sensitivity and specificity of the goldberg cut-off for EI:BMR for identifying diet reports of poor validity. Eur. J. Clin. Nutr. 2000, 54, 395–404. [Google Scholar] [CrossRef] [PubMed]
- Rennie, K.L.; Coward, A.; Jebb, S.A. Estimating under-reporting of energy intake in dietary surveys using an individualised method. Br. J. Nutr. 2007, 97, 1169–1176. [Google Scholar] [CrossRef] [PubMed]
- Harttig, U.; Haubrock, J.; Knuppel, S.; Boeing, H.; Consortium, E. The MSM program: Web-based statistics package for estimating usual dietary intake using the multiple source method. Eur. J. Clin. Nutr. 2011, 65 (Suppl. 1), S87–S91. [Google Scholar] [CrossRef] [PubMed]
- Vieux, F.; Maillot, M.; Constant, F.; Drewnowski, A. Water and beverage consumption among children aged 4–13 years in France: Analyses of INCA 2 (etude individuelle nationale des consommations alimentaires 2006–2007) data. Public Health Nutr. 2016, 19, 2305–2314. [Google Scholar] [CrossRef] [PubMed]
- National Health and Medical Research Council. Nutrient Reference Values for Australia and New Zealand. Available online: https://www.nrv.gov.au/ (accessed on 15 June 2016).
- Frangeskou, M.; Lopez-Valcarcel, B.; Serra-Majem, L. Dehydration in the elderly: A review focused on economic burden. J. Nutr. Health Aging 2015, 19, 619–627. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Luben, R.; Khaw, K.T.; Bingham, S.; Wareham, N.J.; Forouhi, N.G. Dietary energy density predicts the risk of incident type 2 diabetes: The European prospective investigation of cancer (EPIC)-NORFOLK study. Diabetes Care 2008, 31, 2120–2125. [Google Scholar] [CrossRef] [PubMed]
- Mendoza, J.A.; Drewnowski, A.; Christakis, D.A. Dietary energy density is associated with obesity and the metabolic syndrome in US Adults. Diabetes Care 2007, 30, 974–979. [Google Scholar] [CrossRef] [PubMed]
- Millar, L.; Rowland, B.; Nichols, M.; Swinburn, B.; Bennett, C.; Skouteris, H.; Allender, S. Relationship between raised BMI and sugar sweetened beverage and high fat food consumption among children. Obesity (Silver Spring) 2014, 22, E96–E103. [Google Scholar] [CrossRef] [PubMed]
- Jayalath, V.H.; de Souza, R.J.; Ha, V.; Mirrahimi, A.; Blanco-Mejia, S.; di Buono, M.; Jenkins, A.L.; Leiter, L.A.; Wolever, T.M.; Beyene, J.; et al. Sugar-sweetened beverage consumption and incident hypertension: A systematic review and meta-analysis of prospective cohorts. Am. J. Clin. Nutr. 2015, 102, 914–921. [Google Scholar] [CrossRef] [PubMed]
- Keller, A.; Bucher, D.T.S. Sugar-sweetened beverages and obesity among children and adolescents: A review of systematic literature reviews. Child. Obes. 2015, 11, 338–346. [Google Scholar] [CrossRef] [PubMed]
- An, R. Plain water and sugar-sweetened beverage consumption in relation to energy and nutrient intake at full-service restaurants. Nutrients 2016, 8. [Google Scholar] [CrossRef] [PubMed]
- Zheng, M.; Rangan, A.; Allman-Farinelli, M.; Rohde, J.F.; Olsen, N.J.; Heitmann, B.L. Replacing sugary drinks with milk is inversely associated with weight gain among young obesity-predisposed children. Br. J. Nutr. 2015, 114, 1448–1455. [Google Scholar] [CrossRef] [PubMed]
- Ali, A.; O’Donnell, J.M.; Starck, C.; Rutherfurd-Markwick, K.J. The effect of caffeine ingestion during evening exercise on subsequent sleep quality in females. Int. J. Sports Med. 2015, 36, 433–439. [Google Scholar] [CrossRef] [PubMed]
- Owens, J.A.; Mindell, J.; Baylor, A. Effect of energy drink and caffeinated beverage consumption on sleep, mood, and performance in children and adolescents. Nutr. Rev. 2014, 72 (Suppl. 1), 65–71. [Google Scholar] [CrossRef] [PubMed]
- Perrier, E.; Vergne, S.; Klein, A.; Poupin, M.; Rondeau, P.; le Bellego, L.; Armstrong, L.E.; Lang, F.; Stookey, J.; Tack, I. Hydration biomarkers in free-living adults with different levels of habitual fluid consumption. Br. J. Nutr. 2013, 109, 1678–1687. [Google Scholar] [CrossRef] [PubMed]
- Perrier, E.; Rondeau, P.; Poupin, M.; le Bellego, L.; Armstrong, L.E.; Lang, F.; Stookey, J.; Tack, I.; Vergne, S.; Klein, A. Relation between urinary hydration biomarkers and total fluid intake in healthy adults. Eur. J. Clin. Nutr. 2013, 67, 939–943. [Google Scholar] [CrossRef] [PubMed]
- Tooze, J.A.; Midthune, D.; Dodd, K.W.; Freedman, L.S.; Krebs-Smith, S.M.; Subar, A.F.; Guenther, P.M.; Carroll, R.J.; Kipnis, V. A new statistical method for estimating the usual intake of episodically consumed foods with application to their distribution. J. Am. Diet. Assoc. 2006, 106, 1575–1587. [Google Scholar] [CrossRef] [PubMed]
| Children/Adolescents | Age (Years) | 2–18 | 2–3 | 4–8 | 9–13 | 14–18 | p-Value * | |
| Males | n | 1017 | 159 | 295 | 294 | 269 | ||
| Total water | AI | 1.4 | 1.6 | 2.2 | 2.7 | |||
| Mean (SD) | 1.7 (0.6) | 1.2 (0.4) | 1.5 (0.4) | 1.7 (0.5) | 2.1 (0.6) | <0.001 | ||
| Median (IQR) | 1.6 (1.3–2.0) | 1.2 (1.0–1.4) | 1.4 (1.2–1.7) | 1.7 (1.4–2.0) | 2.0 (1.6–2.5) | <0.001 | ||
| Total fluids | AI | 1.0 | 1.2 | 1.6 | 1.9 | |||
| Mean (SD) | 1.2 (0.5) | 0.9 (0.3) | 1.0 (0.4) | 1.3 (0.4) | 1.6 (0.6) | <0.001 | ||
| Median (IQR) | 1.1 (0.9–1.5) | 0.8 (0.6–1.1) | 1.0 (0.8–1.2) | 1.2 (1–1.5) | 1.5 (1.1–1.9) | <0.001 | ||
| Food moisture | Mean (SD) | 0.4 (0.2) | 0.4 (0.1) | 0.4 (0.1) | 0.5 (0.1) | 0.5 (0.2) | <0.001 | |
| Median (IQR) | 0.4 (0.3–0.5) | 0.3 (0.3–0.4) | 0.4 (0.3–0.5) | 0.4 (0.4–0.6) | 0.5 (0.4–0.6) | <0.001 | ||
| Females | n | 953 | 160 | 276 | 295 | 222 | ||
| Total water | AI | 1.4 | 1.6 | 1.9 | 2.2 | |||
| Mean (SD) | 1.5 (0.4) | 1.1 (0.3) | 1.3 (0.3) | 1.3 (0.3) | 1.7 (0.5) | <0.001 | ||
| Median (IQR) | 1.4 (1.1–1.7) | 1.1 (0.9–1.3) | 1.2 (1.1–1.5) | 1.6 (1.3–1.8) | 1.7 (1.4–2) | <0.001 | ||
| Total fluids | AI | 1.0 | 1.2 | 1.4 | 1.6 | |||
| Mean (SD) | 1.0 (0.4) | 0.8 (0.3) | 0.9 (0.3) | 1.1 (0.4) | 1.3 (0.4) | <0.001 | ||
| Median (IQR) | 1.0 (0.8–1.3) | 0.7 (0.6–0.9) | 0.8 (0.7–1.1) | 1.1 (0.9–1.3) | 1.2 (1.0–1.5) | <0.001 | ||
| Food moisture | Mean (SD) | 0.4 (0.1) | 0.4 (0.1) | 0.4 (0.1) | 0.5 (0.1) | 0.5 (0.2) | <0.001 | |
| Median (IQR) | 0.4 (0.3–0.5) | 0.4 (0.3–0.4) | 0.4 (0.3–0.5) | 0.4 (0.4–0.5) | 0.4 (0.3–0.5) | <0.001 | ||
| Adults | Age (Years) | 19+ | 19–30 | 31–50 | 51–70 | 71+ | p-Value | |
| Males | n | 2999 | 553 | 1160 | 925 | 361 | ||
| Total water | AI | 3.4 | 3.4 | 3.4 | 3.4 | 3.4 | ||
| Mean (SD) | 2.6 (0.9) | 2.8 (1.0) | 2.7 (0.9) | 2.5 (0.8) | 2.2 (0.6) | <0.001 | ||
| Median (IQR) | 2.4 (2.0–3.0) | 2.6 (2.1–3.3) | 2.5 (2.1–3.1) | 2.4 (2–2.9) | 2.1 (1.8–2.5) | <0.001 | ||
| Total fluids | AI | 2.6 | 2.6 | 2.6 | 2.6 | 2.6 | ||
| Mean (SD) | 2.0 (0.8) | 2.2 (0.9) | 2.1 (0.8) | 1.9 (0.7) | 1.6 (0.5) | <0.001 | ||
| Median (IQR) | 1.8 (1.4–2.4) | 2.0 (1.6–2.7) | 2.0 (1.6–2.5) | 1.8 (1.4–2.3) | 1.5 (1.2–1.8) | <0.001 | ||
| Food moisture | Mean (SD) | 0.6 (0.2) | 0.6 (0.2) | 0.6 (0.2) | 0.6 (0.2) | 0.6 (0.2) | ns | |
| Median (IQR) | 0.6 (0.4–0.7) | 0.5 (0.5–0.7) | 0.5 (0.4–0.7) | 0.6 (0.5–0.7) | 0.6 (0.5–0.7) | ns | ||
| Females | n | 3233 | 548 | 1189 | 1024 | 472 | ||
| Total water | AI | 2.8 | 2.8 | 2.8 | 2.8 | 2.8 | ||
| Mean (SD) | 2.3 (0.7) | 2.2 (0.7) | 2.4 (0.7) | 2.3 (0.7) | 2.0 (0.6) | <0.001 | ||
| Median (IQR) | 2.2 (1.8–2.7) | 2.1 (1.8–2.6) | 2.3 (1.9–2.7) | 2.2 (1.8–2.7) | 2.0 (1.6–2.3) | <0.001 | ||
| Total fluids | AI | 2.1 | 2.1 | 2.1 | 2.1 | 2.1 | ||
| Mean (SD) | 1.8 (0.6) | 1.7 (0.6) | 1.9 (0.7) | 1.8 (0.6) | 1.5 (0.5) | <0.001 | ||
| Median (IQR) | 1.7 (1.3–2.1) | 1.6 (1.3–2.1) | 1.8 (1.4–2.2) | 1.7 (1.3–2.1) | 1.4 (1.1–1.8) | <0.001 | ||
| Food moisture | Mean (SD) | 0.5 (0.2) | 0.5 (0.2) | 0.5 (0.2) | 0.5 (0.2) | 0.5 (0.2) | ns | |
| Median (IQR) | 0.5 (0.4–0.6) | 0.5 (0.4–0.6) | 0.5 (0.4–0.6) | 0.5 (0.4–0.6) | 0.5 (0.4–0.6) | ns | ||
| Quartiles | Children/Adolescents | Adults | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Q1 (<1.2) | Q2 (1.2–1.5) | Q3 (1.5–1.8) | Q4 (>1.8) | p-Value * | Q1 (<1.9) | Q2 (1.9–2.3) | Q3 (2.3–2.8) | Q4 (>2.8) | p-Value * | |
| Mean total water intake (L) | 1.0 (0.1) | 1.3 (0.1) | 1.7 (0.1) | 2.3 (0.4) | <0.001 | 1.6 (0.2) | 2.1 (0.1) | 2.5 (0.1) | 3.5 (0.7) | <0.001 |
| Demographic | ||||||||||
| Age (year) | 5.7 (3.9) | 8.4 (4.5) | 10.3 (4.4) | 12.9 (3.4) | <0.001 | 52.1 (19.4) | 49.8 (17.5) | 48.3 (16.6) | 44.9 (15.3) | <0.001 |
| Male (%) | 39.1 | 50.2 | 51.7 | 65.4 | <0.001 | 37.0 | 44.0 | 50.4 | 61.0 | <0.001 |
| Interviewed in summer (%) | 25.4 | 24.6 | 26.8 | 32.7 | <0.001 | 25.0 | 28.7 | 28.8 | 29.3 | <0.001 |
| Born in NE countries (%) + | 5.3 | 5.5 | 6.5 | 6.3 | ns | 19.8 | 17.1 | 16.0 | 13.2 | <0.001 |
| Lowest SES quintile (%) | 16.6 | 17.3 | 16.6 | 14.8 | ns | 21.0 | 16.6 | 16.8 | 16.5 | 0.01 |
| Highest SES quintile (%) | 24.1 | 25.8 | 28 | 26 | ns | 22.7 | 24.6 | 25.2 | 24.0 | ns |
| Anthropometric ^ | ||||||||||
| BMI (z-score for children, kg/m2 for adults) | 0.5 (1.2) | 0.4 (1.2) | 0.5 (1.1) | 0.7 (1.1) | ns | 27.1 (0.4) | 27.7 (0.4) | 27.3 (0.4) | 27.5 (0.4) | ns |
| Waist circumference (cm) | 63.9 (0.8) | 64.7 (0.8) | 64.8 (0.7) | 67.3 (0.8) | <0.001 | 99.9 (4.2) | 100.8 (4.2) | 97.9 (4.1) | 100.3 (4.2) | ns |
| Lifestyle ^ | ||||||||||
| Physical activity in last week (min) | 104.2 (26.3) | 213.1 (20.1) | 260.2 (11.5) | 252.3 (14.1) | ns | 199.7 (18) | 231.5 (17.9) | 251.3 (17.8) | 290.1 (18.2) | <0.001 |
| Sleep duration (min) | 581.4 (10.8) | 593.2 (8.3) | 590.4 (7.5) | 583.6 (7.6) | ns | 479.1 (4.8) | 477.2 (4.8) | 473.3 (4.8) | 465.9 (4.9) | 0.001 |
| Currently smoking (%) | - | - | - | - | - | 14.3 | 14.4 | 14.1 | 14.3 | ns |
| Nutrients ^ | ||||||||||
| Water density (L/Mj) | 0.15 (0.1) | 0.19 (0.1) | 0.22 (0.1) | 0.27 (0.1) | <0.001 | 0.20 (0.1) | 0.25 (0.04) | 0.29 (0.1) | 0.36 (0.2) | 0.001 |
| Energy (Mj) | 7.2 (0.2) | 7.8 (0.2) | 8.3 (0.2) | 9.2 (0.2) | <0.001 | 8.5 (0.1) | 9.2 (0.1) | 9.6 (0.1) | 10.4 (0.1) | <0.001 |
| Protein (%E) | 15.9 (0.4) | 15.7 (0.4) | 16.6 (0.4) | 16.7 (0.4) | 0.001 | 17.6 (0.3) | 17.7 (0.3) | 17.9 (0.3) | 18.0 (0.3) | ns |
| Total fat (%E) | 32.4 (0.7) | 31.5 (0.6) | 31.1 (0.6) | 30.3 (0.7) | 0.002 | 32.7 (0.4) | 31.8 (0.4) | 31.2 (0.4) | 29.9 (0.4) | <0.001 |
| Saturated fat (%E) | 14.1 (0.4) | 14.1 (0.4) | 13.7 (0.4) | 13.4 (0.4) | 0.03 | 13.3 (0.2) | 12.7 (0.2) | 12.2 (0.2) | 11.7 (0.2) | <0.001 |
| Total carbohydrates (%E) | 49.1 (0.8) | 50.2 (0.7) | 49.5 (0.7) | 49.8 (0.8) | ns | 43.8 (0.5) | 43.4 (0.5) | 42.7 (0.5) | 41.4 (0.5) | <0.001 |
| Free sugar (%E) | 11.9 (2.3) | 11.4 (1.8) | 10.4 (1.5) | 10.3 (1.3) | <0.001 | 9.5 (1.0) | 9.0 (0.9) | 8.5 (0.9) | 8.2 (0.7) | <0.001 |
| Dietary fibre (%E) | 1.9 (0.1) | 2.0 (0.1) | 2.1 (0.1) | 2.2 (0.1) | <0.001 | 2.0 (0.1) | 2.2 (0.1) | 2.2 (0.1) | 2.3 (0.1) | <0.001 |
| Sodium (mg/Mj) | 298.4 (10.3) | 285.6 (9.4) | 279.4 (9.4) | 292 (10.3) | 0.04 | 286.2 (6) | 279.1 (6) | 276.7 (6) | 268.4 (6.1) | 0.001 |
| Caffeine (mg/Mj) | 2.2 (0.4) | 1.9 (0.4) | 2.0 (0.4) | 2.3 (0.4) | ns | 17.0 (1.0) | 19.6 (1) | 22.0 (1) | 23.1 (1.0) | <0.001 |
| Food groups ^ | ||||||||||
| Grains (g/Mj) | 22.8 (0.9) | 21.7 (0.8) | 22.4 (0.8) | 22.6 (0.9) | ns | 20.8 (0.5) | 20.4 (0.4) | 20.4 (0.4) | 19.7 (0.5) | 0.02 |
| Vegetable (g/Mj) | 16.4 (0.8) | 15.3 (0.7) | 16.2 (0.7) | 16.4 (0.8) | ns | 20.8 (0.5) | 21.2 (0.5) | 21.9 (0.5) | 21.9 (0.5) | 0.005 |
| Fruits (g/Mj) | 21.8 (1.4) | 24 (1.3) | 24 (1.3) | 24.9 (1.4) | 0.03 | 17.7 (0.7) | 19.2 (0.7) | 19.4 (0.7) | 20.2 (0.7) | <0.001 |
| Dairy products (g/Mj) | 30.4 (2.0) | 31 (1.8) | 32.9 (1.8) | 34.7 (2.0) | 0.02 | 25.3 (0.8) | 26.4 (0.8) | 26.9 (0.8) | 26.7 (0.8) | 0.048 |
| Meat and alternatives (g/Mj) | 12.4 (0.6) | 11.6 (0.5) | 12.1 (0.5) | 12.3 (0.6) | ns | 15.1 (0.3) | 14.8 (0.3) | 14.9 (0.3) | 15 (0.3) | ns |
| Discretionary foods (g/Mj) | 23.2 (0.9) | 21.7 (0.8) | 19.8 (0.8) | 20.4 (0.9) | <0.001 | 18.4 (0.4) | 17.3 (0.4) | 16.3 (0.4) | 16.1 (0.4) | <0.001 |
| Discretionary beverages (g/Mj) | 26.7 (2.2) | 26.5 (2) | 24.1 (2) | 25.8 (2.2) | ns | 21.7 (0.9) | 20.6 (0.9) | 19.4 (0.9) | 18.1 (1.0) | <0.001 |
| Alcoholic drinks (g/Mj) | - | - | - | - | - | 14.7 (1.7) | 18.7 (1.7) | 22.3 (1.7) | 34.3 (1.7) | <0.001 |
| Children/Adolescents | 2–18 | 2–3 | 4–8 | 9–13 | 14–18 | p-Value * | Adults | 19+ | 19–30 | 31–50 | 51–70 | 71+ | p-Value |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Plain drinking water | 44.1 | 39.1 | 45.1 | 44.2 | 44.4 | ns | Plain drinking water | 37.4 | 43.9 | 38.7 | 32.0 | 29.5 | <0.001 |
| Tap water | 42.0 | 38.1 | 42.7 | 42.0 | 42.3 | ns | Tap water | 33.7 | 39.4 | 34.7 | 28.9 | 28.1 | <0.001 |
| Bottled water | 2.1 | 1.0 | 2.4 | 2.2 | 2.1 | ns | Bottled water | 3.8 | 4.5 | 4.0 | 3.1 | 1.3 | <0.001 |
| Tea/coffee | 1.4 | 0.2 | 0.4 | 0.7 | 3.3 | <0.001 | Tea/coffee | 16.2 | 8.1 | 16.0 | 21.2 | 24.2 | <0.001 |
| Tea | 0.9 | 0.2 | 0.4 | 0.6 | 1.6 | <0.001 | Tea | 8.2 | 4.3 | 7.2 | 11.2 | 14.7 | <0.001 |
| Coffee | 0.5 | <0.1 | <0.1 | 0.1 | 1.6 | <0.001 | Coffee | 7.9 | 3.8 | 8.8 | 10.1 | 9.5 | <0.001 |
| Juices | 3.1 | 3.6 | 3.4 | 2.9 | 2.9 | <0.001 | Juices | 1.7 | 2.0 | 1.6 | 1.5 | 1.6 | <0.001 |
| Fruit Juice | 3.1 | 3.5 | 3.4 | 2.9 | 2.9 | <0.001 | Fruit Juice | 1.6 | 2.0 | 1.5 | 1.4 | 1.4 | <0.001 |
| Vegetable Juice | <0.1 | <0.1 | <0.1 | <0.1 | <0.1 | ns | Vegetable Juice | 0.1 | <0.1 | <0.1 | 0.1 | 0.2 | ns |
| Milk | 10.1 | 17.4 | 10.0 | 9.9 | 8.5 | <0.001 | Milk | 4.8 | 5.0 | 4.5 | 4.8 | 6.4 | <0.001 |
| Plain Milk (Full Fat) | 6.3 | 14.1 | 6.7 | 5.8 | 4.4 | <0.001 | Plain Milk (Full Fat) | 2.1 | 2.5 | 1.9 | 1.9 | 2.4 | ns |
| Plain Milk (Reduced Milk) | 1.7 | 2.3 | 1.8 | 1.8 | 1.4 | ns | Plain Milk (Reduced Milk) | 1.5 | 1.1 | 1.4 | 1.7 | 2.5 | <0.001 |
| Plain Milk (Skim) | 0.4 | 0.4 | 0.4 | 0.5 | 0.2 | ns | Plain Milk (Skim) | 0.6 | 0.4 | 0.5 | 0.7 | 1.0 | <0.001 |
| Flavoured Milk | 1.7 | 0.5 | 1.2 | 1.7 | 2.5 | <0.001 | Flavoured Milk | 0.7 | 1.0 | 0.8 | 0.5 | 0.4 | <0.001 |
| Milk substitute | <0.1 | <0.1 | <0.1 | <0.1 | <0.1 | ns | Milk substitute | <0.1 | <0.1 | <0.1 | <0.1 | <0.1 | <0.001 |
| Soft/sports drinks | 6.6 | 0.9 | 3.1 | 6.8 | 10.6 | <0.001 | Soft/sports drinks | 5.5 | 7.8 | 5.8 | 4.0 | 1.9 | <0.001 |
| Regular Soft Drinks | 5.4 | 0.9 | 2.9 | 5.4 | 8.4 | <0.001 | Regular Soft Drinks | 3.2 | 5.1 | 3.2 | 2.1 | 1.2 | <0.001 |
| Diet Soft Drinks | 0.8 | <0.1 | 0.2 | 1.0 | 1.4 | <0.001 | Diet Soft Drinks | 1.8 | 1.7 | 2.1 | 1.9 | 0.6 | <0.001 |
| Energy & Sports Drinks | 0.4 | <0.1 | <0.1 | 0.3 | 0.9 | <0.001 | Energy & Sports Drinks | 0.4 | 1.0 | 0.5 | 0.1 | <0.1 | <0.001 |
| Fruit drinks/cordials | 5.3 | 6.7 | 5.8 | 5.8 | 3.9 | ns | Fruit drinks/cordials | 2.3 | 4.1 | 2.1 | 1.6 | 1.9 | <0.001 |
| Fruit Drinks | 2.4 | 3.2 | 2.7 | 2.4 | 2 | ns | Fruit Drinks | 1.0 | 1.8 | 0.8 | 0.6 | 1.1 | <0.001 |
| Regular Cordial | 2.1 | 2.3 | 2.4 | 2.5 | 1.5 | ns | Regular Cordial | 0.9 | 1.8 | 1.0 | 0.6 | 0.6 | <0.001 |
| Diet Cordial | 0.3 | 0.8 | 0.3 | 0.2 | 0.1 | ns | Diet Cordial | 0.2 | 0.2 | 0.2 | 0.2 | <0.1 | ns |
| Others | 0.5 | 0.3 | 0.3 | 0.8 | 0.4 | ns | Others | 0.2 | 0.3 | 0.1 | 0.1 | 0.1 | ns |
| Alcoholic Drinks | 0.4 | <0.1 | <0.1 | <0.1 | 1.2 | <0.001 | Alcoholic Drinks | 7.0 | 6.1 | 7.1 | 8.3 | 5.1 | <0.001 |
| Food moisture | 29.0 | 32.1 | 32.1 | 29.8 | 25.1 | ns | Food moisture | 25.2 | 23.8 | 24.2 | 26.6 | 29.4 | 0.02 |
| Plain Drinking Water Intake (mL) | Children/Adolescents | Adults | |||||
|---|---|---|---|---|---|---|---|
| β | SE | p-Value | β | SE | p-Value | ||
| Gender (Ref. Male) | −63.3 | 19.1 | <0.001 | −10.2 | 16.5 | 0.01 | |
| Age (year) | 37.3 | 3.7 | <0.001 | −8.9 | 0.4 | <0.001 | |
| BMI * | 2.6 | 0.7 | ns | 3.3 | 0.9 | ns | |
| SEIFA (Ref. 1st quintile) | 2nd quintile | −0.7 | 30.0 | ns | 44.3 | 22.5 | 0.04 |
| 3rd quintile | 62.7 | 29.4 | ns | 49.5 | 22.5 | 0.03 | |
| 4th quintile | 38.9 | 30.0 | ns | 92.9 | 23.4 | <0.001 | |
| 5th quintile | 32.1 | 28.1 | ns | 69.2 | 21.8 | 0.002 | |
| Grain (100 g) | −11.0 | 3.8 | ns | −34.3 | 9.1 | <0.001 | |
| Vegetables (100 g) | −10.0 | 20.0 | ns | −11.7 | 9.4 | ns | |
| Fruit (100 g) | −6.1 | 3.9 | ns | 27.1 | 6.3 | <0.001 | |
| Dairy products (100 g) | −30.8 | 9.8 | 0.002 | −31.2 | 4.9 | <0.001 | |
| Meat and alternatives (100 g) | 19.1 | 5.4 | ns | 13.6 | 13.7 | ns | |
| Discretionary beverages (100 g) | −74.8 | 9.0 | <0.001 | −34.7 | 4.1 | <0.001 | |
| Discretionary foods (100 g) | −46.4 | 14.2 | 0.001 | −64.3 | 10.5 | <0.001 | |
| Alcoholic drinks (100 g) | −4.0 | 2.1 | ns | ||||
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sui, Z.; Zheng, M.; Zhang, M.; Rangan, A. Water and Beverage Consumption: Analysis of the Australian 2011–2012 National Nutrition and Physical Activity Survey. Nutrients 2016, 8, 678. https://doi.org/10.3390/nu8110678
Sui Z, Zheng M, Zhang M, Rangan A. Water and Beverage Consumption: Analysis of the Australian 2011–2012 National Nutrition and Physical Activity Survey. Nutrients. 2016; 8(11):678. https://doi.org/10.3390/nu8110678
Chicago/Turabian StyleSui, Zhixian, Miaobing Zheng, Man Zhang, and Anna Rangan. 2016. "Water and Beverage Consumption: Analysis of the Australian 2011–2012 National Nutrition and Physical Activity Survey" Nutrients 8, no. 11: 678. https://doi.org/10.3390/nu8110678
APA StyleSui, Z., Zheng, M., Zhang, M., & Rangan, A. (2016). Water and Beverage Consumption: Analysis of the Australian 2011–2012 National Nutrition and Physical Activity Survey. Nutrients, 8(11), 678. https://doi.org/10.3390/nu8110678





