A Western Dietary Pattern Increases Prostate Cancer Risk: A Systematic Review and Meta-Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Literature Search Strategy and Selection Criteria
2.2. Data Abstraction and Quality Assessment
2.3. Statistical Analysis
3. Results
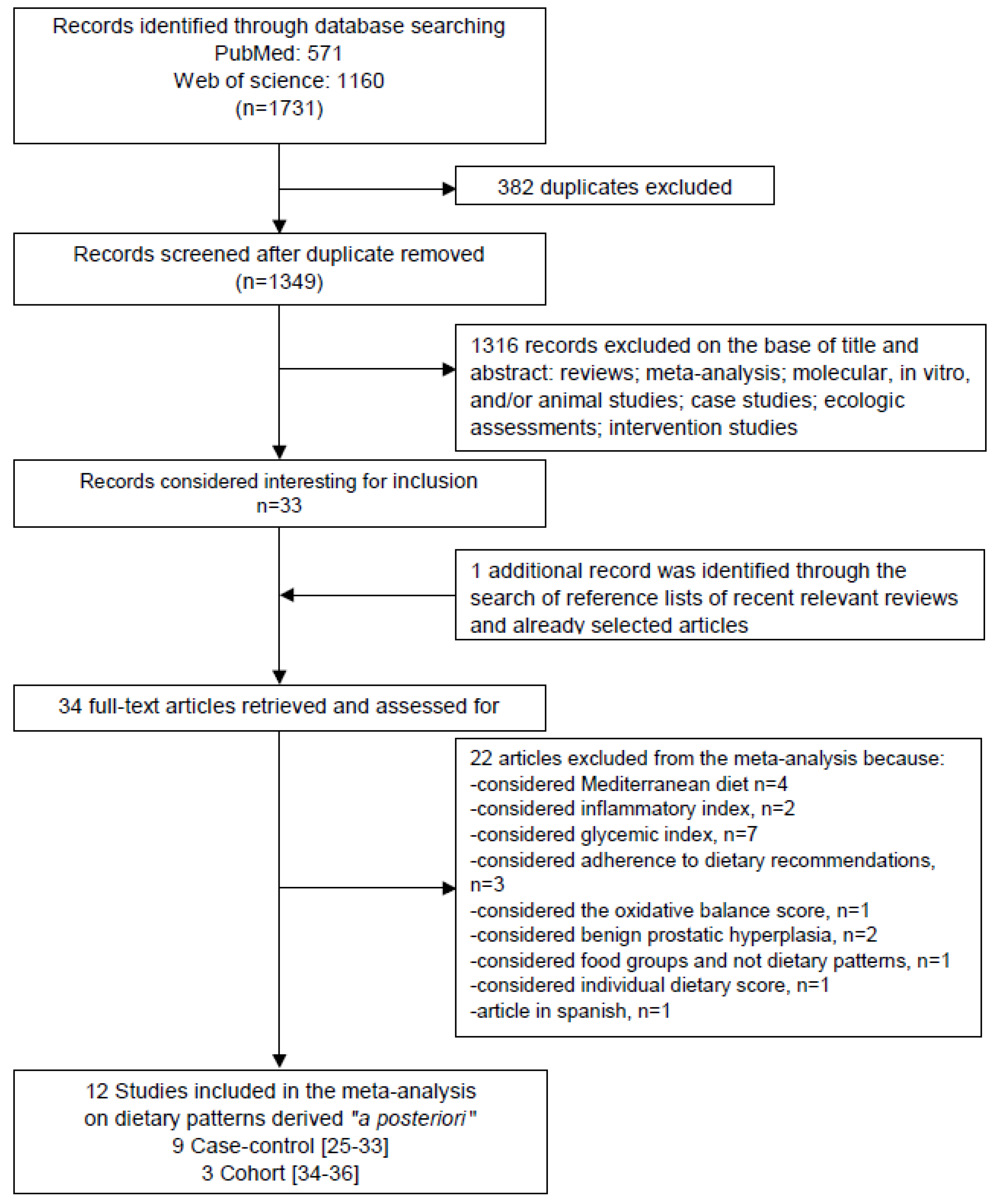
3.1. Study Selection
3.2. Study Characteristics and Quality Assessment
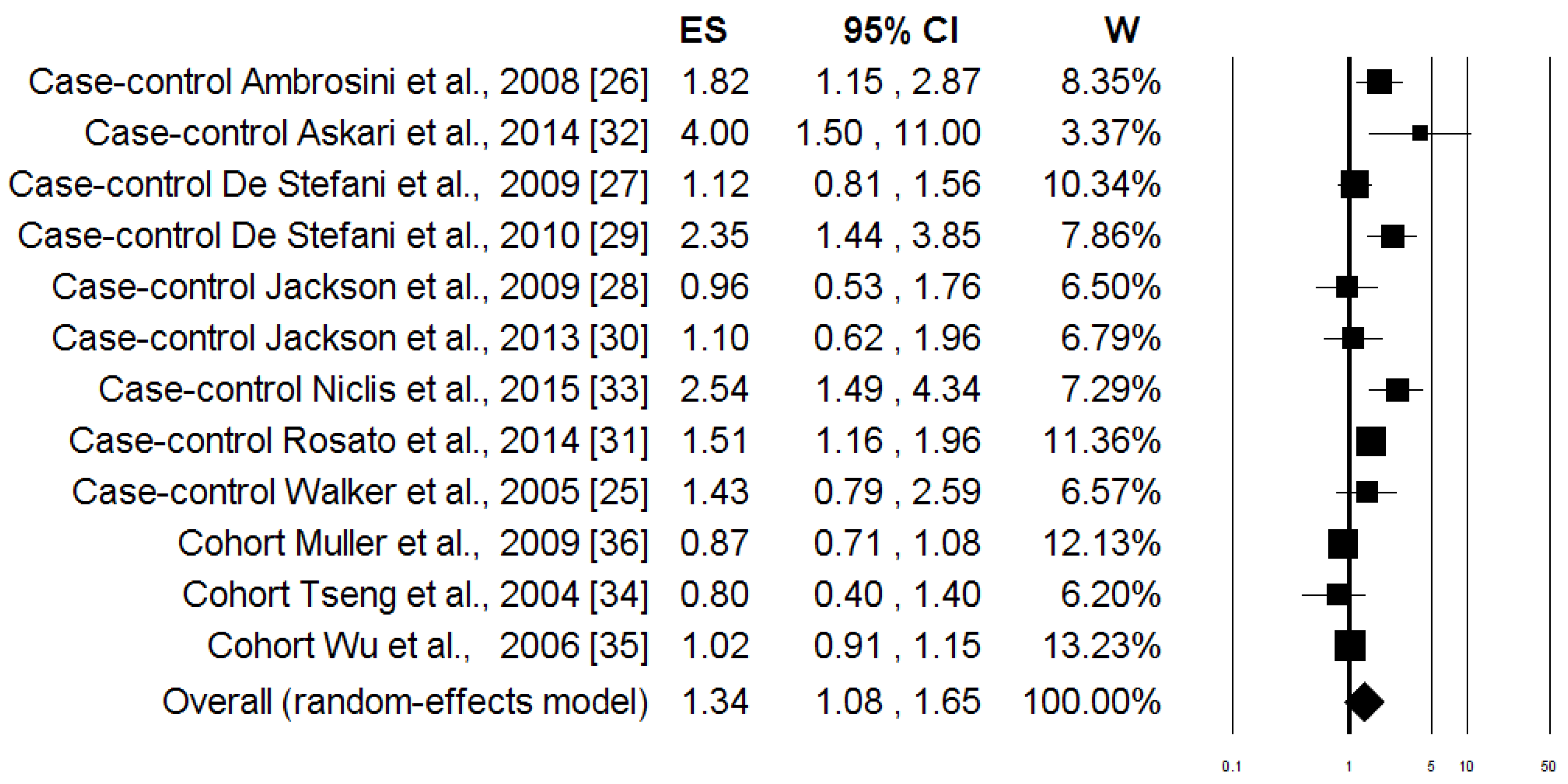
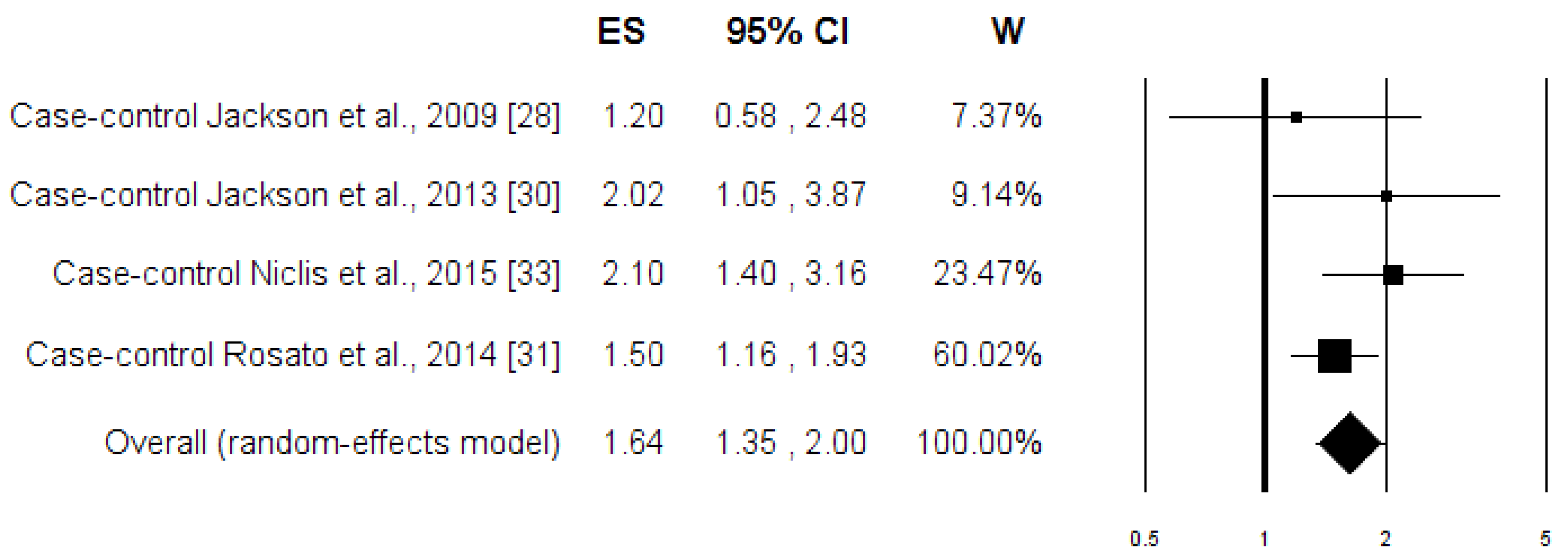
3.3. Meta-Analysis
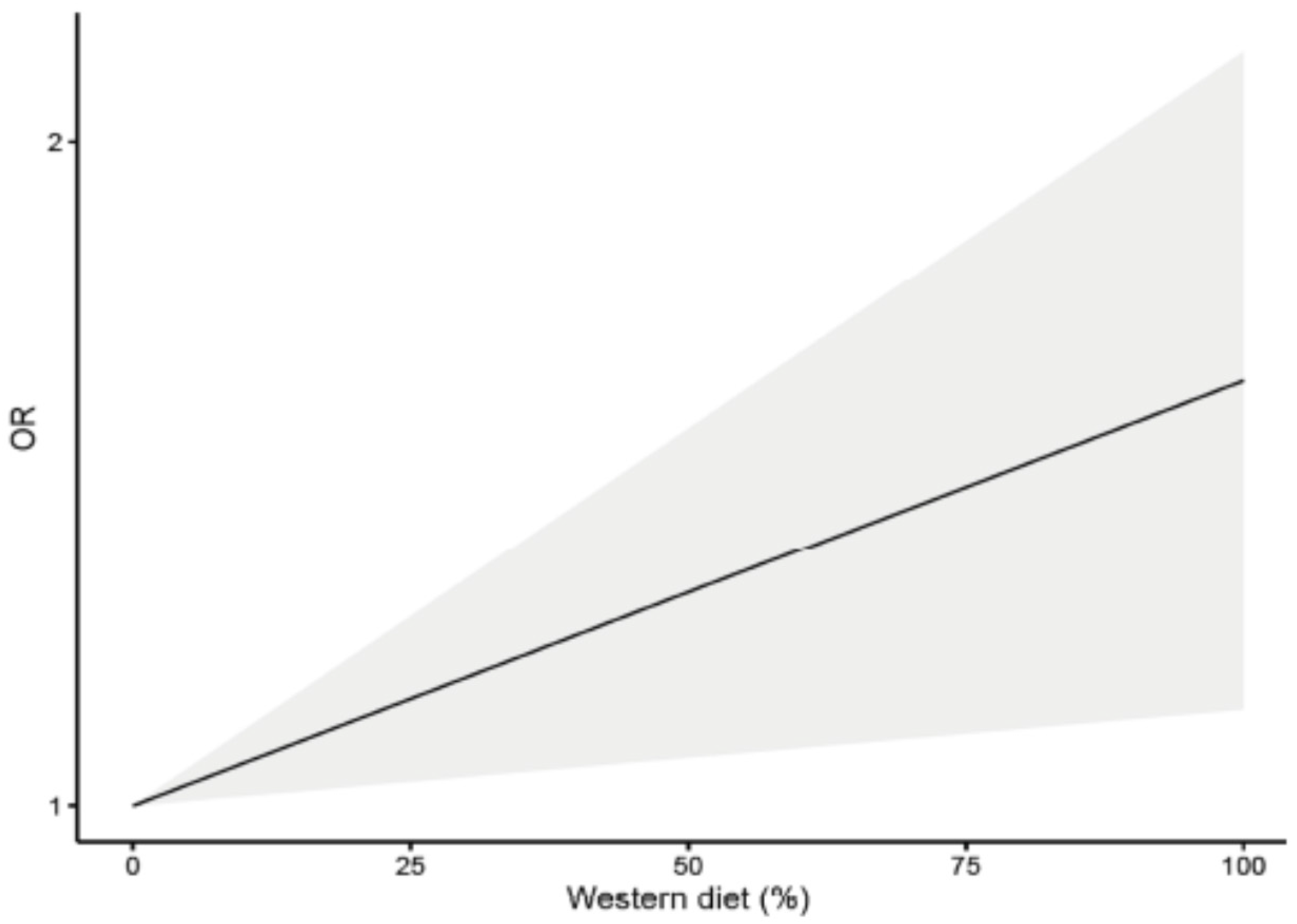
3.4. Dose-Response Analysis
3.5. Publication Bias
3.6. Sensitivity Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ferlay, J.; Soerjomataram, I.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, D.M.; Forman, D.; Bray, F. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int. J. Cancer 2015, 136, E359–E386. [Google Scholar] [CrossRef] [PubMed]
- Cuzick, J.; Thorat, M.A.; Andriole, G.; Brawley, O.W.; Brown, P.H.; Culig, Z.; Eeles, R.A.; Ford, L.G.; Hamdy, F.C.; Holmberg, L.; et al. Prevention and early detection of prostate cancer. Lancet Oncol. 2014, 15, e484–e492. [Google Scholar] [CrossRef]
- Leitzmann, M.F.; Rohrmann, S. Risk factors for the onset of prostatic cancer: Age, location, and behavioral correlates. Clin. Epidemiol. 2012, 4, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Zhou, X.F.; Ding, Z.S.; Liu, N.B. Allium vegetables and risk of prostate cancer: Evidence from 132,192 subjects. Asian Pac. J. Cancer Prev. 2013, 14, 4131–4134. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Cheng, Y.; Li, S.; Zhu, Y.; Xu, X.; Zheng, X.; Mao, Q.; Xie, L. Dietary carrot consumption and the risk of prostate cancer. Eur. J. Nutr. 2014, 53, 1615–1623. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.; Zhai, L.; Zeng, J.; Peng, Q.; Wang, J.; Deng, Y.; Xie, L.; Mo, C.; Yang, S.; Li, S.; et al. Coffee consumption and prostate cancer risk: An updated meta-analysis. Cancer Causes Control 2014, 25, 591–604. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.; Zhang, W.; Wang, X.; Zhao, K.; Negi, D.S.; Zhuo, L.; Qi, M.; Wang, X.; Zhang, X. Lycopene and risk of prostate cancer: A systematic review and meta-analysis. Medicine 2015, 94, e1260. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Song, Y.; Zhang, L. Lycopene/tomato consumption and the risk of prostate cancer: A systematic review and meta-analysis of prospective studies. J. Nutr. Sci. Vitaminol. 2013, 59, 213–223. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.W.; Hu, Z.H.; Wang, X.; Mao, Q.Q.; Qin, J.; Zheng, X.Y.; Xie, L.P. Tea consumption and prostate cancer: An updated meta-analysis. World J. Surg. Oncol. 2014, 12, 38. [Google Scholar] [CrossRef] [PubMed]
- Meng, H.; Hu, W.; Chen, Z.; Shen, Y. Fruit and vegetable intake and prostate cancer risk: A meta-analysis. Asia Pac. J. Clin. Oncol. 2014, 10, 133–140. [Google Scholar] [CrossRef] [PubMed]
- Sheng, T.; Shen, R.L.; Shao, H.; Ma, T.H. No association between fiber intake and prostate cancer risk: A meta-analysis of epidemiological studies. World J. Surg. Oncol. 2015, 13, 264. [Google Scholar] [CrossRef] [PubMed]
- Xu, C.; Han, F.F.; Zeng, X.T.; Liu, T.Z.; Li, S.; Gao, Z.Y. Fat intake is not linked to prostate cancer: A systematic review and dose-response meta-analysis. PLoS ONE 2015, 10, e0131747. [Google Scholar] [CrossRef] [PubMed]
- Wu, K.; Spiegelman, D.; Hou, T.; Albanes, D.; Allen, N.E.; Berndt, S.I.; van den Brandt, P.A.; Giles, G.G.; Giovannucci, E.; Alexandra Goldbohm, R.; et al. Associations between unprocessed red and processed meat, poultry, seafood and egg intake and the risk of prostate cancer: A pooled analysis of 15 prospective cohort studies. Int. J. Cancer 2015, 138, 2368–2382. [Google Scholar] [CrossRef] [PubMed]
- Aune, D.; Navarro Rosenblatt, D.A.; Chan, D.S.; Vieira, A.R.; Vieira, R.; Greenwood, D.C.; Vatten, L.J.; Norat, T. Dairy products, calcium, and prostate cancer risk: A systematic review and meta-analysis of cohort studies. Am. J. Clin. Nutr. 2015, 101, 87–117. [Google Scholar] [CrossRef] [PubMed]
- World Cancer Research Fund International/American Institute for Cancer Research. Continuous Update Project Report: Diet, Nutrition, Physical Activity, and Prostate Cancer. 2014. Available online: http://www.wcrf.org/sites/default/files/Prostate-Cancer-2014-Report.pdf (accessed on 14 March 2016).
- Hu, F.B. Dietary pattern analysis: A new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Michels, K.B.; Schulze, M.B. Can dietary patterns help us detect diet-disease associations? Nutr. Res. Rev. 2005, 18, 241–248. [Google Scholar] [CrossRef] [PubMed]
- Reedy, J.; Wirfält, E.; Flood, A.; Mitrou, P.N.; Krebs-Smith, S.M.; Kipnis, V.; Midthune, D.; Leitzmann, M.; Hollenbeck, A.; Schatzkin, A.; et al. Comparing 3 dietary pattern methods—Cluster analysis, factor analysis, and index analysis with colorectal cancer risk: The NIH-AARP Diet and Health Study. Am. J. Epidemiol. 2010, 171, 479–487. [Google Scholar] [CrossRef] [PubMed]
- Turati, F.; Galeone, C.; Gandini, S.; Augustin, L.S.; Jenkins, D.J.; Pelucchi, C.; La Vecchia, C. High glycemic index and glycemic load are associated with moderately increased cancer risk. Mol. Nutr. Food Res. 2015, 59, 1384–1394. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Hoffmann, G. Adherence to Mediterranean diet and risk of cancer: A systematic review and meta-analysis of observational studies. Int. J. Cancer 2014, 135, 1884–1897. [Google Scholar] [CrossRef] [PubMed]
- Stroup, D.F.; Berlin, J.A.; Morton, S.C.; Olkin, I.; Williamson, G.D.; Rennie, D.; Moher, D.; Becker, B.J.; Sipe, T.A.; Thacker, S.B. Meta-analysis of observational studies in epidemiology: A proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 2000, 283, 2008–2012. [Google Scholar] [CrossRef] [PubMed]
- Wells, G.A.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Non-Randomised Studies in Meta-Analyses. 2015. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 14 March 2016).
- Greenland, S.; Longnecker, M.P. Methods for trend estimation from summarized dose-response data, with applications to meta-analysis. Am. J. Epidemiol. 1992, 135, 1301–1309. [Google Scholar] [PubMed]
- Liu, Q.; Cook, N.R.; Bergström, A.; Hsiehd, C.C. A two-stage hierarchical regression model for meta-analysis of epidemiologic nonlinear dose–response data. Comput. Stat. Data Anal. 2009, 53, 4157–4167. [Google Scholar] [CrossRef]
- Walker, M.; Aronson, K.J.; King, W.; Wilson, J.W.; Fan, W.; Heaton, J.P.; MacNeily, A.; Nickel, J.C.; Morales, A. Dietary patterns and risk of prostate cancer in Ontario, Canada. Int. J. Cancer 2005, 116, 592–598. [Google Scholar] [CrossRef] [PubMed]
- Ambrosini, G.L.; Fritschi, L.; de Klerk, N.H.; Mackerras, D.; Leavy, J. Dietary patterns identified using factor analysis and prostate cancer risk: A case control study in Western Australia. Ann. Epidemiol. 2008, 18, 364–370. [Google Scholar] [CrossRef] [PubMed]
- De Stefani, E.; Deneo-Pellegrini, H.; Boffetta, P.; Ronco, A.L.; Aune, D.; Acosta, G.; Mendilaharsu, M.; Brennan, P.; Ferro, G. Dietary patterns and risk of cancer: A factor analysis in Uruguay. Int. J. Cancer 2009, 124, 1391–1397. [Google Scholar] [CrossRef] [PubMed]
- Jackson, M.; Walker, S.; Simpson, C.; McFarlane-Anderson, N.; Bennett, F. Are food patterns associated with prostate cancer in Jamaican men: A preliminary report. Infect. Agents Cancer 2009, 4. [Google Scholar] [CrossRef] [PubMed]
- De Stefani, E.; Ronco, A.L.; Deneo-Pellegrini, H.; Boffetta, P.; Aune, D.; Acosta, G.; Brennan, P.; Ferro, G.; Mendilaharsu, M. Dietary patterns and risk of advanced prostate cancer: A principal component analysis in Uruguay. Cancer Causes Control 2010, 21, 1009–1016. [Google Scholar] [CrossRef] [PubMed]
- Jackson, M.; Tulloch-Reid, M.; Walker, S.; McFarlane-Anderson, N.; Bennett, F.; Francis, D.; Coard, K. Dietary patterns as predictors of prostate cancer in Jamaican men. Nutr. Cancer 2013, 65, 367–674. [Google Scholar] [CrossRef] [PubMed]
- Rosato, V.; Edefonti, V.; Bravi, F.; Bosetti, C.; Bertuccio, P.; Talamini, R.; Dal Maso, L.; Montella, M.; Ferraroni, M.; La Vecchia, C.; et al. Nutrient-based dietary patterns and prostate cancer risk: A case-control study from Italy. Cancer Causes Control 2014, 25, 525–532. [Google Scholar] [CrossRef] [PubMed]
- Askari, F.; Parizi, M.K.; Jessri, M.; Rashidkhani, B. Dietary patterns in relation to prostate cancer in Iranian men: A case-control study. Asian Pac. J. Cancer Prev. 2014, 15, 2159–2163. [Google Scholar] [CrossRef] [PubMed]
- Niclis, C.; Román, M.D.; Osella, A.R.; Eynard, A.R.; Díaz Mdel, P. Traditional dietary pattern increases risk of prostate cancer in Argentina: Results of a multilevel modeling and bias analysis from a case-control study. J. Cancer Epidemiol. 2015, 2015, 179562. [Google Scholar] [CrossRef] [PubMed]
- Tseng, M.; Breslow, R.A.; DeVellis, R.F.; Ziegler, R.G. Dietary patterns and prostate cancer risk in the national health and nutrition examination survey epidemiological follow-up study cohort. Cancer Epidemiol. Biomark. Prev. 2014, 13, 71–77. [Google Scholar] [CrossRef]
- Wu, K.; Hu, F.B.; Willett, W.C.; Giovannucci, E. Dietary patterns and risk of prostate cancer in U.S. men. Cancer Epidemiol. Biomark. Prev. 2006, 15, 167–171. [Google Scholar] [CrossRef] [PubMed]
- Muller, D.C.; Severi, G.; Baglietto, L.; Krishnan, K.; English, D.R.; Hopper, J.L.; Giles, G.G. Dietary patterns and prostate cancer risk. Cancer Epidemiol. Biomark. Prev. 2009, 18, 3126–3129. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.; Thompson, S.G. Quantifying heterogeneity in a meta-analysis. Stat. Med. 2002, 21, 1539–1558. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.; Thompson, S.G.; Deeks, J.J.; Altman, D.G. Measuring inconsistency in meta-analyses. BMJ 2003, 327, 557–560. [Google Scholar] [CrossRef] [PubMed]
- Begg, C.B.; Mazumdar, M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994, 50, 1088–1101. [Google Scholar] [CrossRef] [PubMed]
- Egger, M.; Davey Smith, G.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2014; Available online: http://www.R-project.org/ (accessed on 14 March 2016).
- Brennan, S.F.; Cantwell, M.M.; Cardwell, C.R.; Velentzis, L.S.; Woodside, J.V. Dietary patterns and breast cancer risk: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2010, 91, 1294–1302. [Google Scholar] [CrossRef] [PubMed]
- Magalhães, B.; Peleteiro, B.; Lunet, N. Dietary patterns and colorectal cancer: Systematic review and meta-analysis. Eur. J. Cancer Prev. 2012, 21, 15–23. [Google Scholar] [CrossRef] [PubMed]
- Feng, Y.L.; Shu, L.; Zheng, P.F.; Zhang, X.Y.; Si, C.J.; Yu, X.L.; Gao, W.; Zhang, L. Dietary patterns and colorectal cancer risk: A meta-analysis. Eur. J. Cancer Prev. 2016, in press. [Google Scholar] [CrossRef] [PubMed]
- Bertuccio, P.; Rosato, V.; Andreano, A.; Ferraroni, M.; Decarli, A.; Edefonti, V.; La Vecchia, C. Dietary patterns and gastric cancer risk: A systematic review and meta-analysis. Ann. Oncol. 2013, 24, 1450–1458. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Wang, X.; Lin, S.; Yuan, J.; Yu, I.T. Dietary patterns and oesophageal squamous cell carcinoma: A systematic review and meta-analysis. Br. J. Cancer 2014, 110, 2785–2795. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Li, Z.; Li, J.; Li, Z.; Han, J. A healthy dietary pattern reduces lung cancer risk: A systematic review and meta-analysis. Nutrients 2016, 8, 134. [Google Scholar] [CrossRef] [PubMed]
- Bouvard, V.; Loomis, D.; Guyton, K.Z.; Grosse, Y.; Ghissassi, F.E.; Benbrahim-Tallaa, L.; Guha, N.; Mattock, H.; Straif, K. International Agency for Research on Cancer Monograph Working Group. Carcinogenicity of consumption of red and processed meat. Lancet Oncol. 2015, 16, 1599–1600. [Google Scholar] [CrossRef]
- Bylsma, L.C.; Alexander, D.D. A review and meta-analysis of prospective studies of red and processed meat, meat cooking methods, heme iron, heterocyclic amines and prostate cancer. Nutr. J. 2015, 14, 125. [Google Scholar] [CrossRef] [PubMed]
- Wang, R.J.; Tang, J.E.; Chen, Y.; Gao, J.G. Dietary fiber, whole grains, carbohydrate, glycemic index, and glycemic load in relation to risk of prostate cancer. OncoTargets Ther. 2015, 8, 2415–2426. [Google Scholar]

| Author, Year Location | Case/Control Age Period | Dietary Pattern Assessment and Identification Method | Dietary Pattern Type and Characteristics | Pattern Score | OR (95% CI) | p for Trend | Confounding Factor Adjusted |
|---|---|---|---|---|---|---|---|
| Walker, 2005 [25] Canada | 80/334 HB 1 50–80 years (mean: 65.0 years cases; 63.6 years controls) (1997–1999) | 67-item FFQ 2 (2 years before), SA 3 34 food groups PCA 4 (in controls) Varimax rotation, EIG 5 > 1.5 Loading > 0.25 4 factors, VE 6 10.51% | 1. Healthy living: vegetables, fruits, whole grains, fish, and poultry | Tertile 1 | 1.00 (Ref.) | 0.45 | Age, physical activity as a teen, current smoking and alcohol intake |
| Tertile 2 | 0.99 (0.55–1.78) | ||||||
| Tertile 3 | 0.78 (0.42–1.45) | ||||||
| 2. Traditional Western: red meats, processed meats, milk, sweets, and hard liquor | Tertile 1 | 1.00 (Ref.) | 0.22 | ||||
| Tertile 2 | 1.00 (0.53–1.88) | ||||||
| Tertile 3 | 1.43 (0.79–2.59) | ||||||
| 3. Processed diet: processed meats, red meats, organ meats, refined grains, onions and tomatoes, vegetable oils and juices, bottled water, and soft drinks | Tertile 1 | 1.00 (Ref.) | 0.003 | ||||
| Tertile 2 | 2.11 (1.06–4.22) | ||||||
| Tertile 3 | 2.75 (1.40–5.39) | ||||||
| 4. Beverages: tap water, “other” beverages including soft drinks and fruit juices, potatoes, poultry and margarine/inversely associated with beer, liquor, wine, and cream for coffee | Tertile 1 | 1.00 (Ref.) | 0.54 | ||||
| Tertile 2 | 0.68 (0.37–1.25) | ||||||
| Tertile 3 | 0.84 (0.47–1.51) | ||||||
| Ambrosini, 2008 [26] Australia | 546/447 PB 7 40–75 years | 101-item FFQ (10 years before), SA PCA (in controls) Varimax rotation, EIG > 1, scree plots Loading > 0.3 3 factors, VE 29.2% | 1. Vegetable: all vegetables listed in the FFQ (including fresh and tinned tomatoes) plus jam, honey, and apples | Quartile 1 | 1.00 (Ref.) | 0.46 | Age, BMI 8, energy intake, and paternal history of prostate cancer |
| Quartile 2 | 1.03 (0.71–1.50) | ||||||
| Quartile 3 | 1.26 (0.85–1.89) | ||||||
| Quartile 4 | 1.13 (0.72–1.78) | ||||||
| 2. Western: full cream milk, white bread, cakes, potato crisps, French fries (chips), eggs, red and processed meats, hamburgers, fried or takeaway fish, and full alcohol beer | Quartile 1 | 1.00 (Ref.) | 0.02 | ||||
| Quartile 2 | 1.42 (0.98–2.06) | ||||||
| Quartile 3 | 1.32 (0.89–1.97) | ||||||
| Quartile 4 | 1.82 (1.15–2.87) | ||||||
| 3. Health-conscious: steamed and grilled fish, tinned fish, chicken, rice, pasta, legumes, and tofu; bean sprouts, nuts, yogurt, ricotta cheese, red wine, and white wine | Quartile 1 | 1.00 (Ref.) | 0.97 | ||||
| Quartile 2 | 1.24 (0.86–1.80) | ||||||
| Quartile 3 | 1.02 (0.70–1.48) | ||||||
| Quartile 4 | 1.06 (0.72–1.58) | ||||||
| De Stefani, 2009 [27] Uruguay | 345/2532 HB (1996–2004) | 64-item FFQ, IA 9 17 food groups PCA (in controls) Varimax rotation, Loading > 0.39 4 factors, VE 36.6% | 1. Prudent: poultry, fish, fresh vegetables, cooked vegetables, and total fruits | Tertile 1 | 1.00 (Ref.) | 0.76 | Age, residence, urban/rural status, education, BMI, smoking status, years since stopping, number of cigarettes/dayamong current smokers, total energy intake and all the dietary patterns |
| Tertile 2 | 1.01 (0.75–1.37) | ||||||
| Tertile 3 | 1.05 (0.77–1.43) | ||||||
| 2. Traditional: total grains, all tubers, desserts, and dairy foods | Tertile 1 | 1.00 (Ref.) | 0.37 | ||||
| Tertile 2 | 1.12 (0.80–1.55) | ||||||
| Tertile 3 | 1.20 (0.81–1.78) | ||||||
| 3. Western: fried red meat, barbecue meat, processed meat, and eggs | Tertile 1 | 1.00 (Ref.) | 0.42 | ||||
| Tertile 2 | 1.36 (1.01–1.81) | ||||||
| Tertile 3 | 1.12 (0.81–1.56) | ||||||
| 4. Drinker: alcoholic beverages such as beer, wine, and hard liquor | Tertile 1 | 1.00 (Ref.) | 0.29 | ||||
| Tertile 2 | 0.69 (0.51–0.92) | ||||||
| Tertile 3 | 0.86 (0.64–1.17) | ||||||
| Jackson, 2009 [28] Jamaica | 204/204 HB (2004–2007) | FFQ, IA 33 food groups PCFA Varimax rotation, EIG > 1 Loading > 0.4 4 factors, VE 24.5% | 1. Healthy: vegetables, fruits, peas and beans | Tertile 1 | 1.00 (Ref.) | Not reported | Age, family history of prostate cancer, education, BMI, smoking, alcohol and total energy intake |
| Tertile 2 | 0.72 (0.39–1.32) | ||||||
| Tertile 3 | 0.84 (0.44–1.59) | ||||||
| 2. Carbohydrate: white bread and refined cereals, poultry, rice/pasta, starchy roots, and tubers | Tertile 1 | 1.00 (Ref.) | |||||
| Tertile 2 | 1.28 (0.70–2.43) | ||||||
| Tertile 3 | 1.20 (0.58–2.48) | ||||||
| 3. Sugary foods: sweet baked products and non-diet drink | Tertile 1 | 1.00 (Ref.) | |||||
| Tertile 2 | 0.88 (0.49–1.62) | ||||||
| Tertile 3 | 0.75 (0.40–1.38) | ||||||
| 4. Organ meat and fast food: high-fat dessert, organ meat, fast food, and salty snacks | Tertile 1 | 1.00 (Ref.) | |||||
| Tertile 2 | 1.31 (0.73–2.33) | ||||||
| Tertile 3 | 0.96 (0.53–1.76) | ||||||
| De Stefani, 2010 [29] Uruguay | 345/690 HB 45–89 years (1996–2004) | 64-item FFQ, IA 21 food groups PCA Quartimax orthogonal Scree plot 5 factors, VE 38.4% | 1. Prudent: raw vegetables, citrus fruits, other fruits, and tea | Quartile 1 | 1.00 (Ref.) | 0.40 | Education, occupation, family history of prostate cancer among first-degree relatives, BMI, tobacco smoking, total energy intake and each pattern for the others |
| Quartile 2 | 0.96 (0.66–1.41) | ||||||
| Quartile 3 | 0.96 (0.66–1.42) | ||||||
| Quartile 4 | 0.82 (0.55–1.23) | ||||||
| 2. Traditional: lamb, dairy foods, cooked vegetables, and all tubers | Quartile 1 | 1.00 (Ref.) | 0.01 | ||||
| Quartile 2 | 1.62 (1.07–2.45) | ||||||
| Quartile 3 | 1.87 (1.22–2.87) | ||||||
| Quartile 4 | 1.85 (1.16–2.94) | ||||||
| 3. Substituter: poultry and fish and a negative loading for lamb consumption | Quartile 1 | 1.00 (Ref.) | 0.58 | ||||
| Quartile 2 | 1.38 (0.94–2.02) | ||||||
| Quartile 3 | 1.35 (0.91–2.01) | ||||||
| Quartile 4 | 1.07 (0.70–1.65) | ||||||
| 4. Drinker: mate, beer, wine, and hard liquor | Quartile 1 | 1.00 (Ref.) | 0.42 | ||||
| Quartile 2 | 0.79 (0.54–1.16) | ||||||
| Quartile 3 | 0.89 (0.61–1.32) | ||||||
| Quartile 4 | 1.18 (0.78–1.78) | ||||||
| 5. Western: beef, processed meat, boiled eggs, fried eggs, and total grains | Quartile 1 | 1.00 (Ref.) | <0.0001 | ||||
| Quartile 2 | 1.41 (0.92–2.17) | ||||||
| Quartile 3 | 2.10 (1.35–3.25) | ||||||
| Quartile 4 | 2.35 (1.44–3.85) | ||||||
| Jackson, 2013 [30] Jamaica | 243/275 HB 40–80 years (2005–2007) | FFQ 33 food groups PCA Varimax rotation EIG > 1, scree plot 4 factors, VE 27.8% | 1.Vegetables & legumes (Healthy): Dark green leafy, yellow vegetable, nuts and seeds, other vegetables, peas and beans, ready-to-eat cereals, fruits | Tertile 1 | 1.00 (Ref.) | 0.766 | Age, family history of prostate cancer, education, BMI, smoking, physical activity, total energy intake |
| Tertile 2 | 0.87 (0.49–1.55) | ||||||
| Tertile 3 | 0.91 (0.50–1.67) | ||||||
| 2. Fast food: fast foods, alcoholic beverages, meal replacements, dairy dessert, fruit juice | Tertile 1 | 1.00 (Ref.) | 0.162 | ||||
| Tertile 2 | 1.12 (0.63–1.96) | ||||||
| Tertile 3 | 0.66 (0.34–1.16) | ||||||
| 3. Meat: processed meat, eggs, poultry, and starchy fruits, roots, and tubers | Tertile 1 | 1.00 (Ref.) | 0.735 | ||||
| Tertile 2 | 0.88 (0.50–1.57) | ||||||
| Tertile 3 | 1.10 (0.62–1.96) | ||||||
| 4. Refined Carbohydrate: rice and pasta, sugar sweetened beverages, sweet baked foods (refined carbohydrates), and poultry | Tertile 1 | 1.00 (Ref.) | 0.029 | ||||
| Tertile 2 | 1.65 (0.94–2.90) | ||||||
| Tertile 3 | 2.02 (1.05–3.87) | ||||||
| Rosato, 2014 [31] Italy | 1294/1451 HB 46–74 years (median: 66 years cases; 63 years controls) (1991–2002) | 78-items FFQ (2 years before), IA 28 selected nutrients/29 food groups PCFA Varimax rotation EIG ≥ 1, scree plot Loading ≥ 0.63 5 factors, VE 78.26% | 1. Animal Products: calcium, phosphorus, riboflavin, animal protein, saturated fatty acids, zinc, and cholesterol Milk and dairy products, eggs, red meat, cheese | Quintile 1 | 1.00 (Ref.) | 0.02 | Age, study center, education, BMI, tobacco, alcohol drinkingand family history of prostatecancer in first-degree relatives |
| Quintile 3 | 1.35 (1.04–1.76) | ||||||
| Quintile 5 | 1.51 (1.16–1.96) | ||||||
| 2. Vitamins and Fiber: vitamin C, total fiber, beta-carotene equivalents, total folate, and soluble carbohydrates Fruits, vegetables, legumes, and olive oil | Quintile 1 | 1.00 (Ref.) | 0.23 | ||||
| Quintile 3 | 1.15 (0.90–1.48) | ||||||
| Quintile 5 | 0.93 (0.72–1.21) | ||||||
| 3. Starch-rich: starch, vegetable protein, and sodium Bread, pasta and rice | Quintile 1 | 1.00 (Ref.) | <0.001 | ||||
| Quintile 3 | 1.16 (0.89–1.49) | ||||||
| Quintile 5 | 1.50 (1.16–1.93) | ||||||
| 4. VUFA 10: linoleic acid, vitamin E, and linolenic acid Specified and unspecified seed oils, leafy vegetables, and olive oil | Quintile 1 | 1.00 (Ref.) | 0.41 | ||||
| Quintile 3 | 1.21 (0.94–1.55) | ||||||
| Quintile 5 | 1.16 (0.89–1.51) | ||||||
| 5. AUFA 11: polyunsaturated fatty acids and vitamin D Fish and offals | Quintile 1 | 1.00 (Ref.) | 0.02 | ||||
| Quintile 3 | 1.05 (0.81–1.36) | ||||||
| Quintile 5 | 1.32 (1.02–1.70) | ||||||
| Askari, 2014 [32] Iran | 50/100 HB 40–78 years (cases) 43–71 years (controls) | 125-item FFQ, IA PCA Varimax rotation Interpretability and scree plot EIG > 1.9 2 factors | 1. Western diet: sweets and desserts, organ meat, snacks, tea and coffee, French fries, salt, carbonated drinks, red or processed meat | Two categories (high 2nd median vs. low 1st median) | 4.00 (1.50–11.00) | Smoking, diabetes, energy intake | |
| 2. Healthy diet: legumes, fish, dairy products, fruits and fruit juice, vegetables, boiled potatoes, whole cereal, and egg | 0.40 (0.20–1.00) | ||||||
| Niclis, 2015 [33] Argentina | 147/300 PB 48–89 years (cases) 46–89 years (controls) | 125-item FFQ, IA 24 food groups PCA Varimax rotation Interpretability and scree plot EIG > 1.0 Loading ≥ 0.40 4 factors, VE 31.52% | 1. Traditional: fatty red meats, offal, processed meat, starchy vegetables, added sugars and sweets, candies, fats, and vegetable oils | Quartile 1 | 1.00 (Ref.) | 0.048 | Age, BMI, energy intake, occupational exposure, family history of cancer |
| Quartile 2 | 1.60 (0.97–2.66) | ||||||
| Quartile 3 | 1.73 (1.17–2.57) | ||||||
| Quartile 4 | 2.54 (1.49–4.34) | ||||||
| 2. Prudent: nonstarchy vegetables, whole grains, and low loading for alcoholic drinks | Quartile 1 | 1.00 (Ref.) | 0.926 | ||||
| Quartile 2 | 0.70 (0.39–1.26) | ||||||
| Quartile 3 | 0.84 (0.54–1.31) | ||||||
| Quartile 4 | 1.31 (0.49–3.51) | ||||||
| 3. Carbohydrate: sodas/juices and bakery products | Quartile 1 | 1.00 (Ref.) | 0.069 | ||||
| Quartile 2 | 1.76 (1.25–2.48) | ||||||
| Quartile 3 | 2.67 (0.98–7.35) | ||||||
| Quartile 4 | 2.10 (1.40–3.16) | ||||||
| 4. Cheese: cheese and low loading for fish | Quartile 1 | 1.00 (Ref.) | 0.720 | ||||
| Quartile 2 | 1.48 (0.69–3.20) | ||||||
| Quartile 3 | 1.34 (0.84–2.16) | ||||||
| Quartile 4 | 1.02 (0.54–1.93) |
| Author, Year Location | Subjects Cohort Age Incident Cases Follow-up (Period) | Dietary Pattern Assessment and Identification Method | Dietary Pattern Type and Characteristics | Pattern Score | RR (95% CI) | p for Trend | Confounding Factor Adjusted |
|---|---|---|---|---|---|---|---|
| Tseng, 2004 [34] USA | 3779 25–74 years (mean 58 year) 136 cases mean follow-up 7.6 years (1982–1992) | 105-item FFQ 1 PCA 2 (Varimax rotation, interpretability, EIG 3 > 1.0, Scree plots) Loading > 0.2 3 factors, VE 4 10.8% | 1. Vegetable-fruit: vegetables, fruits, fish, and shellfish | Tertile 1 | 1.00 (Ref.) | 0.64 | Age, race, poverty census enumeration district, family income, region, residence, education, sun exposure, physical activity, smoking, alcohol, energy intake |
| Tertile 2 | 1.50 (0.9–2.3) | ||||||
| Tertile 3 | 1.20 (0.7–2.0) | ||||||
| 2. Red meat-starch: red meats, potatoes, salty snacks, cheese, sweets, and desserts | Tertile 1 | 1.00 (Ref.) | 0.37 | ||||
| Tertile 2 | 0.70 (0.5–1.2) | ||||||
| Tertile 3 | 0.80 (0.4–1.4) | ||||||
| 3. Southern: beans, rice, and such traditionally Southern United States foods as cornbread, grits, sweet potatoes, and okra | Tertile 1 | 1.00 (Ref.) | 0.08 | ||||
| Tertile 2 | 0.90 (0.6–1.4) | ||||||
| Tertile 3 | 0.60 (0.4–1.1) | ||||||
| Wu, 2006 [35] USA | 47,725 40–75 years 3002 cases follow-up 15 years (1986–2000) | 131-item FFQ 40 food groups, FA 5 (Varimax rotation, interpretability, EIG > 1.0, Scree test) Loading > 0.3 2 factors, VE 17.4% | 1. Prudent: fruits, vegetables, legumes, whole grains, fish, and poultry | Quintile 1 | 1.00 (Ref.) | 0.37 | Age, height, smoking, family history of prostate cancer, race, history of vasectomy, vigorous exercise, BMI 6, alcohol intake, total energy intake |
| Quintile 3 | 1.10 (0.98–1.24) | ||||||
| Quintile 5 | 0.95(0.84–1.07) | ||||||
| 2. Western: red meat, processed meat, butter, eggs, refined grains and high-fat dairy | Quintile 1 | 1.00 (Ref.) | 0.62 | ||||
| Quintile 3 | 1.03 (0.92–1.16) | ||||||
| Quintile 5 | 1.02 (0.91–1.15) | ||||||
| Muller, 2009 [36] Australia | 14,627 34–75 years 1018 cases Mean follow-up 13.6 years (1990–2007) | 121-item FFQ FA (Varimax rotation, interpretability, EIG > 2) Loading > 0.3 4 factor, VE 67% | 1. Mediterranean: some meats, vegetables, and fruits, and avoidance of cakes and sweet biscuits | Quartile 1 | 1.00 (Ref.) | 0.9 | Age, total energy intake and ethnicity. Further adjustment for BMI, physical activity, smoking, alcohol intake, and education did not change estimated HRs or 95% CIs materially. |
| Quartile 2 | 0.93 (0.79–1.11) | ||||||
| Quartile 3 | 1.14 (0.95–1.37) | ||||||
| Quartile 4 | 0.93 (0.74–1.18) | ||||||
| 2. Vegetable: high intake of vegetables | Quartile 1 | 1.00 (Ref.) | 0.5 | ||||
| Quartile 2 | 1.11 (0.90–1.36) | ||||||
| Quartile 3 | 1.02 (0.83–1.27) | ||||||
| Quartile 4 | 1.12 (0.90–1.40) | ||||||
| 3. Meat & Potatoes: high intake of meats and potato cooked in fat | Quartile 1 | 1.00 (Ref.) | 0.2 | ||||
| Quartile 2 | 1.00 (0.84–1.20) | ||||||
| Quartile 3 | 1.04 (0.87–1.24) | ||||||
| Quartile 4 | 0.87 (0.71–1.08) | ||||||
| 4. Fruit & Salad: high intake of salad greens and fruit | Quartile 1 | 1.00 (Ref.) | 0.6 | ||||
| Quartile 2 | 1.14 (0.96–1.36) | ||||||
| Quartile 3 | 1.10 (0.92–1.32) | ||||||
| Quartile 4 | 1.00 (0.81–1.23) |
| Combined Risk Estimate | Test of Heterogeneity | Publication Bias | |||||
|---|---|---|---|---|---|---|---|
| Value (95% CI) | p | Q | I2 % | p | p (Egger Test) | p (Begg Test) | |
| Healthy pattern | |||||||
| Case-control (n = 9) 3 | 0.92 (0.80–1.07) | 0.294 | 6.77 | 0.00 | 0.562 | 0.343 | 0.404 |
| Cohort (n = 3) | 0.97 (0.88–1.08) | 0.567 | 0.83 | 0.00 | 0.661 | 0.003 | 0.117 |
| Pooled 4 (n = 12) | 0.96 (0.88–1.04) | 0.284 | 7.88 | 0.00 | 0.724 | 0.538 | 0.583 |
| Western pattern | |||||||
| Case-control (n = 9) | 1.58 (1.25–2.01) | 0.0001 | 17.62 | 54.61 | 0.024 | 0.349 | 0.677 |
| Cohort (n = 3) | 0.97 (0.87–1.08) | 0.623 | 2.09 | 4.14 | 0.352 | 0.414 | 0.602 |
| Pooled 4 (n = 12) | 1.34 (1.08–1.65) | 0.007 | 43.36 | 74.63 | 0.0001 | 0.045 | 0.583 |
| Carbohydrate pattern | |||||||
| Case-control (n = 4) | 1.64 (1.35–2.00) | 0.0001 | 2.99 | 0.00 | 0.393 | 0.799 | 1.000 |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fabiani, R.; Minelli, L.; Bertarelli, G.; Bacci, S. A Western Dietary Pattern Increases Prostate Cancer Risk: A Systematic Review and Meta-Analysis. Nutrients 2016, 8, 626. https://doi.org/10.3390/nu8100626
Fabiani R, Minelli L, Bertarelli G, Bacci S. A Western Dietary Pattern Increases Prostate Cancer Risk: A Systematic Review and Meta-Analysis. Nutrients. 2016; 8(10):626. https://doi.org/10.3390/nu8100626
Chicago/Turabian StyleFabiani, Roberto, Liliana Minelli, Gaia Bertarelli, and Silvia Bacci. 2016. "A Western Dietary Pattern Increases Prostate Cancer Risk: A Systematic Review and Meta-Analysis" Nutrients 8, no. 10: 626. https://doi.org/10.3390/nu8100626
APA StyleFabiani, R., Minelli, L., Bertarelli, G., & Bacci, S. (2016). A Western Dietary Pattern Increases Prostate Cancer Risk: A Systematic Review and Meta-Analysis. Nutrients, 8(10), 626. https://doi.org/10.3390/nu8100626






