Food Reformulation, Responsive Regulation, and “Regulatory Scaffolding”: Strengthening Performance of Salt Reduction Programs in Australia and the United Kingdom
Abstract
:1. Introduction
2. Salt Consumption, High Blood Pressure, and Cardiovascular Disease
3. Evaluating Australia’s Food and Health Dialogue
4. Evaluating Salt Reduction Initiatives in the UK
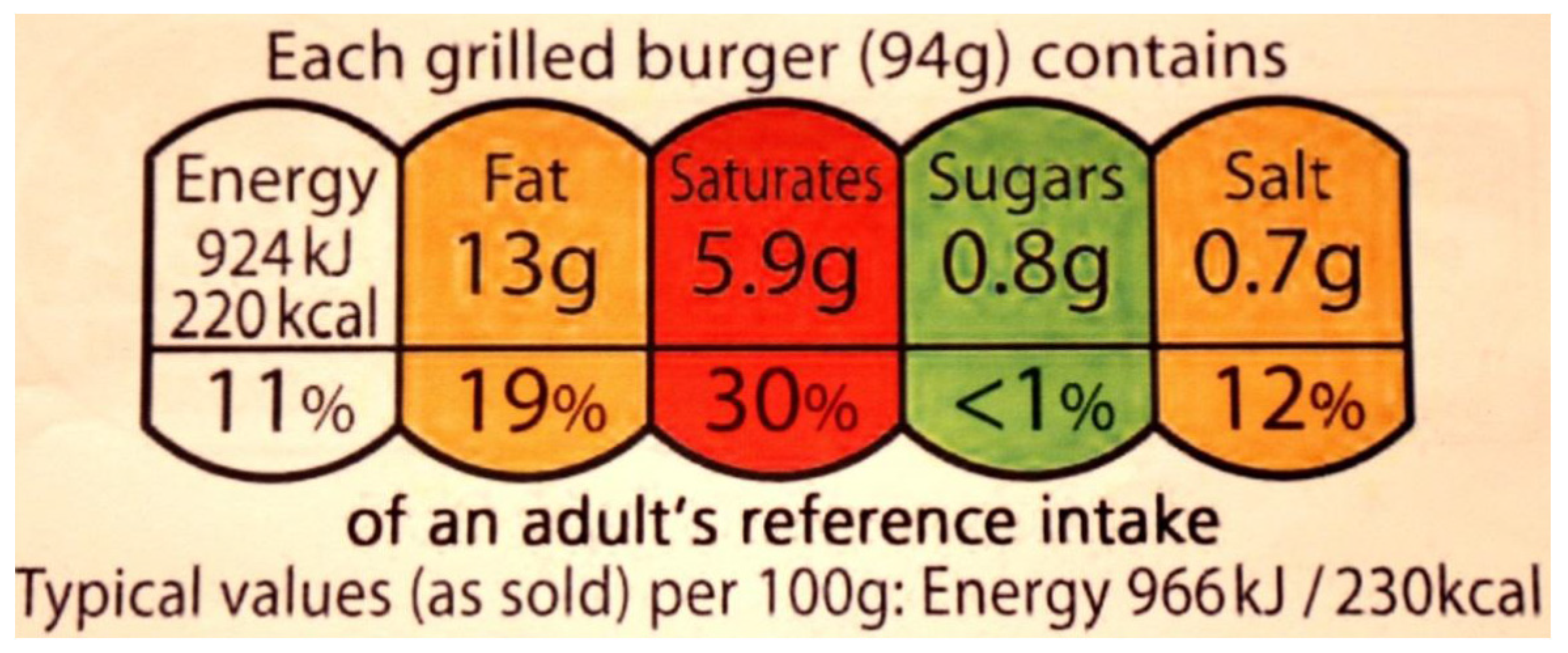

5. Accelerating Progress of Salt Reduction Initiatives: Insights from the Field of Regulatory Studies
| Regulatory Component | Actions to Be Taken |
|---|---|
| Regulatory Category or Dimension | |
| Substantive content | |
| The goals of industry codes | Clearly identify the goals the initiative is intended to achieve; include measurable targets for evaluating overall performance across a defined timeframe. |
| Terms, definitions and exceptions in industry codes | Define key terms and definitions used in initiatives; specifically identify any exceptions. |
| Regulatory processes | |
| Administration | Grant administration of the scheme to an independent, accountable body, e.g., a committee with equal representation from government, industry, and public health organisations, with each member’s roles and responsibilities clearly identified in writing. |
| Monitoring | Conduct independent, transparent and comprehensive monitoring of the scheme, using baseline data and a set of measurable, time-bound process and outcome indicators, and accompanied by public reporting of the results. |
| Review | Undertake regular, independent, external reviews, using baseline data and performance indicators that can be used to measure the initiative’s success in achieving its objectives; publicly report the results of any reviews. |
| Enforcement | |
| Incentives for compliance | Provide incentives that motivate participants to comply, e.g., positive publicity, subsidies for research and development, or a promotional labeling scheme. |
| Deterrents for non-compliance | Provide for a wide range of sanctions that deter non-compliance by participants and free-riding by non-participants, e.g., “naming and shaming”, fines, and expulsion from the scheme; threaten escalation to more coercive regulatory options if voluntary initiatives fail to produce significant improvements in companies’ performance. |
6. Strengthening the Food and Health Dialogue
6.1. Phase 1
| Pre-Requisites to an Effective Product Reformulation Program | |||
Government should:
| |||
| Substantive Content of Participants Obligations | Regulatory Processes | Participation and Enforcement | |
| Phase 1 | Wide-ranging, aggressive reformulation targets are created, which if achieved, will enable food manufacturers and retailers to meet their share of the national target.Maximum salt caps are introduced, particularly for product categories that contribute significantly to excess salt intake, and potentially for new products introduced into the market. Compliance with reformulation targets and salt caps remains voluntary. However, participating companies are required to report on specific actions taken to meet targets and commitments. | Governance structures for the salt reduction scheme are strengthened by increasing the level of representation by government, consumer and public health groups. | Food manufacturers, retailers and caterers that contribute the greatest amount of salt to the food supply are identified and asked to join the scheme. Government and/or scheme administration engages in a targeted recruitment drive. Department of Health threatens industry with mandatory participation in Phase 2 if there is insufficient compliance/low levels of participation. Companies that fail to meet targets and commitments are “named and shamed”; high achievers are praised. Government sets out a timetable for legislative action if progress falls behind minimum-stated level of achievement within a given timeframe. |
| Phase 2 | Average salt reduction targets and salt caps apply specifically to each manufacturer’s product portfolio (rather than collectively to all participants).Reformulation targets and caps remain voluntary, but mandatory high-salt warning labels apply to non- complying products (e.g., mandatory traffic light labeling). | Administration of the scheme is transferred to an independent government agency, which is given a statutory mandate to implement and enforce the program. | Companies that fail to prepare action plans and submit annual reports in a timely fashion are penalized (e.g., fines). |
| Phase 3 | The independent regulator could set mandatory targets for particular product categories where participants fail to make adequate progress.Dept. of Health (or independent regulator) requires under-performing companies to enter into enforceable agreements to implement reformulation plans, with company-specific targets for product lines, interim targets, and sanctions for non-compliance.Complying companies would remain under Phase 2. | ||
| Phase 4 | Government introduces mandatory salt limits for sales-weighted averages and maximum salt caps for a wide range of processed and restaurant food categories. | ||
6.2. Phase 2
6.3. Phase 3
7. Improving the UK’s Salt Reduction Program under the Responsibility Deal
7.1. Phase 1
7.2. Phase 2
7.3. Phase 3
7.4. Phase 4
8. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organisation. Global Status Report on Noncommunicable Diseases; World Health Organisation: Geneva, Switzerland, 2014. [Google Scholar]
- Graudal, N.; Jürgens, G.; Baslund, B.; Alderman, M.H. Compared with usual sodium intake, low-and excessive-sodium diets are associated with increased mortality: A meta-analysis. Am. J. Hypertens. 2014, 27, 1129–1137. [Google Scholar] [CrossRef] [PubMed]
- O’Donnell, M.J.; Yusuf, S.; Mente, A.; Gao, P.; Mann, J.F.; Teo, K.; McQueen, M.; Sleight, P.; Sharma, A.M.; Dans, A.; et al. Urinary sodium and potassium excretion and risk of cardiovascular events. J. Am. Med. Assoc. 2011, 306, 2229–2238. [Google Scholar] [CrossRef] [PubMed]
- He, F.J.; Burnier, M.; MacGregor, G.A. Nutrition in cardiovascular disease: Salt in hypertension and heart failure. Eur. Heart J. 2011, 32, 3073–3080. [Google Scholar] [CrossRef] [PubMed]
- Strazzullo, P.; D’Elia, L.; Kandala, N.B.; Cappuccio, F.P. Salt intake, stroke, and cardiovascular disease: Meta-analysis of prospective studies. Br. Med. J. 2009, 339. [Google Scholar] [CrossRef] [PubMed]
- Aburto, N.J.; Ziolkovska, A.; Hooper, L.; Elliott, P.; Cappuccio, F.P.; Meerpohl, J.J. Effect of lower sodium intake on health: Systematic review and meta-analyses. Br. Med. J. 2013, 346. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lim, S.S.; Vos, T.; Flaxman, A.D.; Danaei, G.; Shibuya, K.; Adair-Rohani, H.; Amann, M.; Anderson, R.; Andrews, K.G.; Aryee, M.; et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2224–2260. [Google Scholar] [CrossRef]
- Webster, J.; Trieu, K.; Dunford, E.; Hawkes, C. Target salt 2025: A global overview of national programs to encourage the food industry to reduce salt in foods. Nutrients 2014, 6, 3274–3287. [Google Scholar] [CrossRef] [PubMed]
- Webster, J.L.; Dunford, E.K.; Hawkes, C.; Neal, B.C. Salt reduction initiatives around the world. J. Hypertens. 2011, 29, 1043–1050. [Google Scholar] [CrossRef] [PubMed]
- Australian Government. Food and Health Dialogue. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/Home (accessed on 25 June 2015).
- Department of Health (UK). Public Health Responsibility Deal. Available online: https://responsibilitydeal.dh.gov.uk/ (accessed on 25 June 2015).
- Trevena, H.; Neal, B.; Dunford, E.; Wu, J.H. An evaluation of the effects of the Australian Food and Health Dialogue targets on the sodium content of bread, breakfast cereals and processed meats. Nutrients 2014, 6, 3802–3817. [Google Scholar] [CrossRef] [PubMed]
- He, F.; Brinsden, H.; Macgregor, G. Salt reduction in the United Kingdom: A successful experiment in public health. J. Hum. Hypertens. 2014, 28, 345–352. [Google Scholar] [CrossRef] [PubMed]
- Sadler, K.; Nicholson, S.; Steer, T.; Gill, V.; Bates, B.; Tipping, S.; Cox, L.; Lennox, A.; Prentice, A. National Diet and Nutrition Survey: Assessment of Dietary Sodium in Adults (Aged 19 to 64 Years) in England. 2011. Available online: https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/213420/Sodium-Survey-England-2011_Text_to-DH_FINAL1.pdf (accessed on 25 June 2015).
- Magnusson, R.; Reeve, B. “Steering” private regulation? A new strategy for reducing population salt intake in Australia. Syd. Law Rev. 2014, 36, 255–289. [Google Scholar]
- Reeve, B.; Magnusson, R. Food reformulation and the neo-liberal state: New strategies for strengthening voluntary salt reduction programs in the UK and USA. Public Health 2015, 129, 351–363. [Google Scholar] [CrossRef] [PubMed]
- Reeve, B.; Magnusson, R. Legislative scaffolding: A new approach to prevention. Aust. N. Z. J. Public Health 2013, 37, 494–496. [Google Scholar] [CrossRef] [PubMed]
- Australian Institute of Health and Welfare. Australia’s Health 2014; Australian Institute of Health and Welfare: Canberra, Australia, 2014; p. 161. [Google Scholar]
- Begg, S.J.; Vos, T.; Barker, B.; Stanley, L.; Lopez, A.D. Burden of disease and injury in Australia in the new millennium: Measuring health loss from diseases, injuries and risk factors. Med. J. Aust. 2008, 188, 36–40. [Google Scholar] [PubMed]
- Australian Institute of Health and Welfare. Cardiovascular Disease: Australian Facts, 2011; Australian Institute of Health and Welfare: Canberra, Australia, 2011; p. 48. [Google Scholar]
- Keogh, J.; Clifton, P.M. Salt Intake and Health in the Australian Population; Australasian Medical Publishing Company: Sydney, Australia, 2008. [Google Scholar]
- National Health and Medical Research Council. Nutrient Reference Values for Australia and New Zealand. Available online: http://www.nhmrc.gov.au/_files_nhmrc/publications/attachments/n35.pdf (accessed on 25 June 2015).
- Goodall, S.; Gallego, G.; Norman, R. Scenario Modelling of Potential Health Benefits Subsequent to the Introduction of the Proposed Standard for Nutrition, Health and Related Claims; Centre for Health Economics Research and Evaluation, University of Technology Sydney: Sydney, Australia, 2008; pp. 26–31. [Google Scholar]
- Health and Social Care Information Centre. Health Survey for England—2011: Chapter 3, Hypertension. Available online: http://www.hscic.gov.uk/catalogue/PUB09300/HSE2011-Ch3-Hypertension.pdf (accessed on 25 June 2015).
- Health and Social Care Information Centre. Health survey for England—2011, Health, Social Care and Lifestyle: Chapter 2, CVD. Available online: http://www.hscic.gov.uk/catalogue/PUB09300/HSE2011-Ch2-CVD.pdf (accessed on 25 June 2015).
- He, F.J.; Pombo-Rodrigues, S.; MacGregor, G.A. Salt reduction in England from 2003 to 2011: Its relationship to blood pressure, stroke and ischaemic heart disease mortality. BMJ Open 2014, 4. [Google Scholar] [CrossRef] [PubMed]
- Bates, B.; Lennox, A.; Prentice, A.; Bates, C.; Page, P.; Nicholson, S.; Swan, G. National Diet and Nutrition Survey: Results from Years 1, 2, 3 and 4 (Combined) of the Rolling Programme (2008/2009–2011/2012); Public Health England: London, UK, 2014. [Google Scholar]
- Mattes, R.; Donnelly, D. Relative contributions of dietary sodium sources. J. Am. Coll. Nutr. 1991, 10, 383–393. [Google Scholar] [CrossRef] [PubMed]
- Farley, T. The Public Health Crisis Hiding in Our Food. The New York Times. 20 April 2014. Available online: http://www.nytimes.com/2014/04/21/opinion/the-public-health-crisis-hiding-in-our-food.html?_r=0 (accessed on 25 June 2015).
- Kenten, C.; Rowe, G. UK consumers’ perceptions and consumption patterns. Appetite 2013, 70, 104–111. [Google Scholar] [CrossRef] [PubMed]
- Taylor, C.L.; Henry, J.E. Strategies to Reduce Sodium Intake in the United States; National Academies Press: Washington, DC, USA, 2010. [Google Scholar]
- Webster, J.L.; Dunford, E.K.; Neal, B.C. A systematic survey of the sodium contents of processed foods. Am. J. Clin. Nutr. 2010, 91, 413–420. [Google Scholar] [CrossRef] [PubMed]
- Dunford, E.; Webster, J.; Woodward, M.; Czernichow, S.; Yuan, W.L.; Jenner, K.; ni Mhurchu, C.; Jacobson, M.; Campbell, N.; Neal, B.; et al. The variability of reported salt levels in fast foods across six countries: Opportunities for salt reduction. Can. Med. Assoc. J. 2012, 184, 1023–1028. [Google Scholar] [CrossRef] [PubMed]
- Girgis, S.; Neal, B.; Prescott, J.; Prendergast, J.; Dumbrell, S.; Turner, C.; Woodward, M. A one-quarter reduction in the salt content of bread can be made without detection. Eur. J. Clin. Nutr. 2003, 57, 616–620. [Google Scholar] [CrossRef] [PubMed]
- Australian Government Department of Health. Principles for Collaboration. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/industry-engagement (accessed on 25 June 2015).
- Elliott, T.; Trevena, H.; Sacks, G.; Dunford, E.; Martin, J.; Webster, J.; Swinburn, B.; Moodie, A.R.; Neal, B.C. A systematic interim assessment of the Australian Government’s Food and Health Dialogue. Med. J. Aust. 2014, 200, 92–95. [Google Scholar] [CrossRef] [PubMed]
- Australian Government Department of Health. Summary of Food Categories Engaged under the Food and Health Dialogue to Date. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/summary_food_categories (accessed on 25 June 2015).
- Australian Government Department of Health. Food Category Action Plans. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/food-category-action-plans (accessed on 25 June 2015).
- Australian Government Department of Health. Breads. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/breads (accessed on 25 June 2015).
- Australian Government Department of Health. Ready-To-Eat Breakfast Cereals. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/ready-to-eat-breakfast-cereals (accessed on 25 June 2015).
- Australian Government Department of Health. Food and Health Dialogue Newsletter, 5th ed. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/newsletter-5 (accessed on 25 June 2015).
- Australian Government Department of Health. Legislative and Governance Forum on Food Regulation Final Communiqué. 13 December 2013; Available online: http://www.health.gov.au/internet/main/publishing.nsf/Content/foodsecretariat-communiques.htm (accessed on 25 June 2015).
- Australian Government Department. Health Star Rating System. Available online: http://www.healthstarrating.gov.au/internet/healthstarrating/publishing.nsf/Content/home (accessed on 25 June 2015).
- Australian Government Department. Health Star Rating System Style Guide. Available online: http://www.healthstarrating.gov.au/internet/healthstarrating/publishing.nsf/AttachmentsByTitle/style-guide/$FILE/HSR+Style+Guide-30June2014.pdf (accessed on 25 June 2015).
- Food Standards Authority Australia New Zealand (FSANZ). Standard 1.2.7—Nutrition, Health and Related Claims, Schedule 1 (Conditions for Nutrition Content Claims). Available online: http://www.comlaw.gov.au/Series/F2013L00054 (accessed on 25 June 2015).
- Kaldor, J.; Magnusson, R.; Colagiuri, S. Diabetes, prevention, and law: Time to try something new. Med. J. Aust. 2015, 202, 578–581. [Google Scholar] [CrossRef] [PubMed]
- Christoforou, A.K.; Dunford, E.K.; Neal, B.C. Changes in the sodium content of Australian ready meals between 2008 and 2011. Asia Pac. J. Clin. Nutr. 2013, 22, 138–143. [Google Scholar] [PubMed]
- Trevena, H.; Dunford, E.; Neal, B.; Webster, J. The Australian Food and Health Dialogue—The implications of the sodium recommendation for pasta sauces. Public Health Nutr. 2014, 17, 1647–1653. [Google Scholar] [CrossRef] [PubMed]
- Food Standards Agency. Agency Publishes Revised 2012 Targets. Available online: http://tna.europarchive.org/20120209120540/http://www.food.gov.uk/news/newsarchive/2009/may/salttargets (accessed on 25 June 2015).
- Australian Government Department of Health. Simmer Sauces. Available online: http://www.foodhealthdialogue.gov.au/internet/foodandhealth/publishing.nsf/Content/simmer-sauces (accessed on 25 June 2015).
- Wyness, L.A.; Butriss, J.L.; Stanner, S.A. Reducing the population’s sodium intake: The UK Food Standards Agency’s salt reduction programme. Public Health Nutr. 2012, 15, 254–261. [Google Scholar] [CrossRef] [PubMed]
- Webster, J. Signalling Change—Working with the Private Food Sector to Improve Nutrition: A Comparative Analysis of National Strategies in the UK and the Netherlands; World Health Organisation: Geneva, Switzerland, 2006. [Google Scholar]
- Hawkes, C.; Webster, J. National approaches to monitoring population salt intake: A trade-off between accuracy and practicality? PLoS ONE 2012, 7, e46727. [Google Scholar] [CrossRef] [PubMed]
- European Commission. Collated Information on Salt Reduction in the EU. Available online: http://ec.europa.eu/health/nutrition_physical_activity/high_level_group/nutrition_salt_en.htm (accessed on 25 June 2015).
- Sutherland, J.; Edwards, P.; Shankar, B.; Dangour, A.D. Fewer adults add salt at the table after initiation of a national salt campaign in the UK: A repeated cross-sectional analysis. Br. J. Nutr. 2013, 110, 552–558. [Google Scholar] [CrossRef] [PubMed]
- MacGregor, G.A.; He, F.J.; Pombo-Rodrigues, S. Food and the responsibility deal: How the salt reduction strategy was derailed. Br. Med. J. 2015, 350. [Google Scholar] [CrossRef] [PubMed]
- Jebb, S. The Public Health Responsibility Deal Food Network. Nutr. Bull. 2012, 37, 355–358. [Google Scholar] [CrossRef]
- Petticrew, M.; Eastmure, E.; Mays, N.; Knai, C.; Durand, M.A.; Nolte, E. The Public Health Responsibility Deal: How should such a complex public health policy be evaluated? J. Public Health 2013, 35, 495–501. [Google Scholar] [CrossRef] [PubMed]
- Department of Health Public Health Responsibility Deal. How Progress Is Reported. Available online: https://responsibilitydeal.dh.gov.uk/monitoring-progress/ (accessed on 25 June 2015).
- Food Network. Salt Strategy Beyond. 2012. Available online: https://responsibilitydeal.dh.gov.uk/wp-content/uploads/2013/03/Salt-Strategy-Beyond-2012.pdf (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. F2. Salt Reduction. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=9 (accessed on 25 June 2015).
- Department of Health. Responsibility Deal: Three New Catering Pledges Launched. Available online: https://www.gov.uk/government/news/responsibility-deal-three-new-catering-pledges-launched (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. F.5 Salt Catering. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=42 (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. F5(a). Salt Catering: Training and Kitchen Practice. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=26 (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. F5(b). Salt Catering: Reformulation of Products as Purchased by the Customer. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=27 (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. F5(c). Salt Catering: Procurement. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=28 (accessed on 25 June 2015.
- Department of Health Public Health Responsibility Deal. F.10 Out of Home Maximum per Serving Salt Targets. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=50 (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. F9. Salt Reduction. 2017. Available online: https://responsibilitydeal.dh.gov.uk/pledges/pledge/?pl=49 (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. Salt Reduction—On Wards and Downwards. Available online: https://responsibilitydeal.dh.gov.uk/salt-reduction-onwards-and-downwards/ (accessed on 25 June 2015).
- Jaworowska, A.; Blackham, T.; Stevenson, L.; Davies, I.G. Determination of salt content in hot takeaway meals in the United Kingdom. Appetite 2012, 59, 517–522. [Google Scholar] [CrossRef] [PubMed]
- Department of Health; Food Standards Agency; The Scottish Government. Guide to Creating a Front of Pack (FoP) Nutrition Label for Pre-Packed Products Sold Through Retail Outlets. Available online: https://www.gov.uk/government/publications/front-of-pack-nutrition-labelling-guidance (accessed on 25 June 2015).
- Abdulla, H. Brussels Starts Proceedings Against UK Over Traffic Light Labels. Just-Food, 2 October 2014; Available online: http://www.just-food.com/news/brussels-starts-proceedings-against-uk-over-traffic-light-labels_id128026.aspx (accessed on 25 June 2015).
- Department of Health Public Health Responsibility Deal. Our Partners. Available online: https://responsibilitydeal.dh.gov.uk/partners/ (accessed on 25 June 2015).
- Hashem, K.; Haigh, C.; Powell, C. The Irresponsibility Deal? Why the Government’s Responsibility Deal is Better for the Food Industry than Public Health. Available online: http://www.sustainweb.org/publications/?id=188 (accessed on 25 June 2015).
- Panjwani, C.; Caraher, M. The Public Health Responsibility Deal: Brokering a deal for public health, but on whose terms? Health Policy 2014, 114, 163–173. [Google Scholar] [CrossRef] [PubMed]
- Quinn, I. Salt Reduction Plan “Hampered” by Out-of-Home Sector. The Grocer. 18 January 2014. Available online: http://www.thegrocer.co.uk/topics/salt-reduction-plan-hampered-by-out-of-home-sector/353655.article (accessed on 25 June 2015).
- Bryden, A.; Petticrew, M.; Mays, N.; Eastmure, E.; Knai, C. Voluntary agreements between government and business—A scoping review of the literature with specific reference to the Public Health Responsibility Deal. Health Policy 2013, 110, 186–197. [Google Scholar] [CrossRef] [PubMed]
- Kraak, V.I.; Swinburn, B.; Lawrence, M.; Harrison, P. A Q methodology study of stakeholders’ views about accountability for promoting healthy food environments in England through the Responsibility Deal Food Network. Food Policy 2014, 49, 207–218. [Google Scholar] [CrossRef]
- Foodstuffs, Cosmetics and Disinfectants Act 1972 (South Africa): Regulations Relating to the Reduction of Sodium in Certain Foodstuffs and Related Matters, RG 36274/2013. Available online: http://faolex.fao.org/cgi-bin/faolex.exe?rec_id=122848&database=faolex&search_type=link&table=result&lang=eng&format_name=@ERALL (accessed on 25 June 2015).
- Charlton, K.; Webster, J.; Kowal, P. To legislate or not to legislate? A comparison of the UK and South African approaches to the development and implementation of salt reduction programs. Nutrients 2014, 6, 3672–3695. [Google Scholar] [CrossRef] [PubMed]
- Collins, M.; Mason, H.; O’Flaherty, M.; Guzman-Castillo, M.; Critchley, J.; Capewell, S. An economic evaluation of salt reduction policies to reduce coronary heart disease in England: A policy modeling study. Value Health 2014, 17, 517–524. [Google Scholar] [CrossRef] [PubMed]
- Murray, C.; Lauer, J.; Hutubessy, R.; Niessen, L.; Tomijima, N.; Rodgers, A.; Lawes, C.; Evans, D. Effectiveness and costs of interventions to lower systolic blood pressure and cholesterol: A global and regional analysis on reduction of cardiovascular-disease risk. Lancet 2003, 361, 717–725. [Google Scholar] [CrossRef]
- Mason, H.; Shoaibi, A.; Ghandour, R.; O’Flaherty, M.; Capewell, S.; Khatib, R.; Jabr, S.; Unal, B.; Sözmen, K.; Arfa, C.; et al. A cost effectiveness analysis of salt reduction policies to reduce coronary heart disease in four Eastern Mediterranean countries. PLoS ONE 2014, 9. [Google Scholar] [CrossRef] [PubMed]
- Black, J. Decentring regulation: Understanding the role of regulation and self-regulation in a “post-regulatory” world. Curr. Leg. Probl. 2001, 54, 103–146. [Google Scholar] [CrossRef]
- Braithwaite, J. Regulatory Capitalism: How It Works, Ideas for Making It Work Better; Edward Elgar Publishing: London, UK, 2008. [Google Scholar]
- Levi-Faur, D. The global diffusion of regulatory capitalism. Ann. Am. Acad. Polit. Soc. Sci. 2005, 598, 12–32. [Google Scholar] [CrossRef]
- Sinclair, D. Self-regulation versus command and control? Beyond false dichotomies. Law Policy 1997, 19, 529–559. [Google Scholar] [CrossRef]
- Clarke, J. Dissolving the public realm? The logics and limits of neo-liberalism. J. Soc. Policy 2004, 33, 27–48. [Google Scholar] [CrossRef]
- Black, J. Constitutionalising self-regulation. Mod. Law Rev. 1996, 59, 24–55. [Google Scholar] [CrossRef]
- Bartle, I.; Vass, P. Self-regulation within the regulatory state: Towards a new regulatory paradigm? Public Adm. 2007, 85, 885–905. [Google Scholar] [CrossRef]
- Ayres, I.; Braithwaite, J. Responsive Regulation: Transcending the Deregulation Debate; Oxford University Press: London, UK, 1992. [Google Scholar]
- Baldwin, R.; Black, J. Really responsive regulation. Mod. Law Rev. 2008, 71, 59–94. [Google Scholar] [CrossRef] [Green Version]
- Gunningham, N.; Sinclair, D. Regulatory pluralism: Designing policy mixes for environmental protection. Law Policy 1999, 21, 49–76. [Google Scholar] [CrossRef]
- Gunningham, N.; Grabosky, P.N.; Sinclair, D. Smart Regulation: Designing Environmental Policy; Clarendon Press: Oxford, UK, 1998. [Google Scholar]
- Nuffield Council on Bioethics. Public Health: Ethical Issues. Available online: http://nuffieldbioethics.org/project/public-health/ (accessed on 25 June 2015).
- Gostin, L.O. Public Health Law: Power, Duty, Restraint,, 2nd ed.; University of California Press: Berkeley, CA, USA, 2000. [Google Scholar]
- Webb, K. Understanding the voluntary codes phenomenon. In Voluntary Codes: Private Governance, the Public Interest and Innovation; Webb, K., Ed.; Carleton Research Unit for Innovation, Science and Environment, Carleton University: Ottawa, ON, Canada, 2004; pp. 3–34. [Google Scholar]
- Cohen, D. The role of the state in a privatized regulatory environmen. In Voluntary Codes: Private Governance, the Public Interest and Innovation; Webb, K., Ed.; Carleton Research Unit for Innovation, Science and Environment, Carleton University: Ottawa, ON, Canada, 2004; pp. 35–56. [Google Scholar]
- Vincent-Jones, P. Values and purpose in government: Central-local relations in regulatory perspective. J. Law Soc. 2002, 29, 27–55. [Google Scholar] [CrossRef]
- Osborne, D.; Gaebler, T. Reinventing Government: How the Entrepreneurial Spirit is Transforming the Public Sector; Plume: London, UK, 1992. [Google Scholar]
- Swinburn, B.; Kraak, V.I.; Rutter, H.; Vandevijvere, S.; Lobstein, T.; Sacks, G.; Marsh, T.; Magnusson, R. Strengthening accountability systems to create healthy food environments and reduce global obesity. Lancet 2015. [Google Scholar] [CrossRef]
- Taskforce on Industry Self-Regulation. Industry Self-Regulation in Consumer Markets. Available online: http://archive.treasury.gov.au/contentitem.asp?ContentID=1131 (accessed on 25 June 2015).
- Reeve, B. Private governance, public purpose? Assessing transparency and accountability in self-regulation of food advertising to children. J. Bioeth. Inq. 2013, 10, 149–163. [Google Scholar] [CrossRef] [PubMed]
- Magnusson, R.S.; Reeve, B.H. Regulation and the prevention agenda. Med. J. Aust. 2013, 199. [Google Scholar] [CrossRef] [PubMed]
- Gunningham, N.; Sinclair, D. Leaders and Laggards: Next-Generation Environmental Regulation; Greenleaf Publishing: Sheffield, UK, 2002. [Google Scholar]
- Sharma, L.L.; Teret, S.P.; Brownell, K.D. The food industry and self-regulation: Standards to promote success and to avoid public health failures. Am. J. Public Health 2010, 100, 240–246. [Google Scholar] [CrossRef] [PubMed]
- Gunningham, N.; Rees, J. Industry self-regulation: An institutional perspective. Law Policy 1997, 19, 363–414. [Google Scholar] [CrossRef]
- Olson, M. The Logic of Collective Action: Public Goods and the Theory of Group; Harvard University Press: Cambridge, MA, USA, 1965. [Google Scholar]
- Australian Competition and Consumer Commission (ACCC). Guidelines for Developing Effective Voluntary Industry Codes of Conduct. Available online: https://www.accc.gov.au/publications/guidelines-for-developing-effective-voluntary-industry-codes-of-conduct (accessed on 25 June 2015).
- Yeung, K. Government by publicity management: Sunlight or spin? Public Law 2005, 2, 360–383. [Google Scholar]
- Braithwaite, J. To Punish or Persuade: Enforcement of Coal Mine Safety; State University of New York Press: Albany, NY, USA, 1985. [Google Scholar]
- Spencer, S.; Kneebone, M. FOODmap: An Analysis of the Australian Food Supply Chain; Department of Agriculture Fisheries and Forestries: Canberra, Australia, 2012. [Google Scholar]
- Sugarman, S.D. Enticing business to create a healthier American diet: Performance-based regulation of food and beverage retailers. Law Policy 2014, 36, 91–112. [Google Scholar] [CrossRef]
- Sugarman, S.D. Salt, high blood pressure, and performance-based regulation. Regul. Gov. 2009, 3, 84–102. [Google Scholar] [CrossRef]
- Grynbaum, M. De blasio administration wants high-sodium warnings on menus. New York Times. 9 June 2015. Available online: http://www.nytimes.com/2015/06/10/nyregion/de-blasio-administration-wants-high-sodium-warnings-on-menus.html (accessed on 25 June 2015).
- Kraak, V.; Swinburn, B.; Lawrence, M.; Harrison, P. An accountability framework to promote healthy food environments. Public Health Nutr. 2014, 17, 2467–2483. [Google Scholar] [CrossRef] [PubMed]
- Australian Securities and Investments Commission Act 2001 (Australia) ss 93AA-93A. Available online: http://www5.austlii.edu.au/au/legis/cth/consol_act/asaica2001529/ (accessed 25 June 2015).
- Competition and Consumer Act 2010 (Australia) s 87B. Available online: http://www5.austlii.edu.au/au/legis/cth/consol_act/caca2010265/ (accessed 25 June 2015).
- Water Act 2007 (Australia) ss 163-164. Available online: http://www5.austlii.edu.au/au/legis/cth/consol_act/wa200783/ (accessed 25 June 2015).
- Brownell, K.D. Thinking forward: The quicksand of appeasing the food industry. PLoS Med. 2012, 9, e1001254. [Google Scholar] [CrossRef] [PubMed]
- Moodie, R.; Stuckler, D.; Monteiro, C.; Sheron, N.; Neal, B.; Thamarangsi, T.; Lincoln, P.; Casswell, S. Lancet NCD Action Group. Profits and pandemics: Prevention of harmful effects of tobacco, alcohol, and ultra-processed food and drink industries. Lancet 2013, 381, 670–679. [Google Scholar] [CrossRef]
- Ludwig, D.S.; Nestle, M. Can the food industry play a constructive role in the obesity epidemic? J. Am. Med. Assoc. 2008, 300, 1808–1811. [Google Scholar] [CrossRef] [PubMed]
- Urquhart, C. Childhood Obesity: Jeremy Hunt Threatens Food Industry with Legislation. The Guardian. 6 January 2014. Available online: http://www.guardian.co.uk/society/2013/jan/05/childhood-obesity-fatty-sugary-foods (accessed on 25 June 2015).
- Gunningham, N.; Johnstone, R. Regulating Workplace Safety: Systems and Sanctions; Oxford University Press: Oxford, UK, 1999. [Google Scholar]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Magnusson, R.; Reeve, B. Food Reformulation, Responsive Regulation, and “Regulatory Scaffolding”: Strengthening Performance of Salt Reduction Programs in Australia and the United Kingdom. Nutrients 2015, 7, 5281-5308. https://doi.org/10.3390/nu7075221
Magnusson R, Reeve B. Food Reformulation, Responsive Regulation, and “Regulatory Scaffolding”: Strengthening Performance of Salt Reduction Programs in Australia and the United Kingdom. Nutrients. 2015; 7(7):5281-5308. https://doi.org/10.3390/nu7075221
Chicago/Turabian StyleMagnusson, Roger, and Belinda Reeve. 2015. "Food Reformulation, Responsive Regulation, and “Regulatory Scaffolding”: Strengthening Performance of Salt Reduction Programs in Australia and the United Kingdom" Nutrients 7, no. 7: 5281-5308. https://doi.org/10.3390/nu7075221
APA StyleMagnusson, R., & Reeve, B. (2015). Food Reformulation, Responsive Regulation, and “Regulatory Scaffolding”: Strengthening Performance of Salt Reduction Programs in Australia and the United Kingdom. Nutrients, 7(7), 5281-5308. https://doi.org/10.3390/nu7075221




